structure and function of the respiratory system
1/53
Earn XP
Description and Tags
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
54 Terms
componentss of URT
nasal cavity
oral cavity
nasopharynx
pharynx
oropharynx
epiglottis
larynx
trachea
oesophagus
what is the diaphragm innervatd by and what kind of nerve is this
phrenic nerve- which is a somatic motor nerve
what are the external intercostal muscls innervated by
intercostal nerve
respiration in horses
biphasic ventilation
locomotion ventilation coupling
layers of the blood gas barrier
surfactant
type 1 alveolar epithelial cell
basal laminar of epithelial cell
connective tissue
basal lamina of endothelial cell
endothelial cell
plasma
rbc membrane
0.2-0.6 um thick
large surface ae to volume
ficks law
rate of transfer of gas through a sheet of tissue is proportional to the tissue area and the difference in partial pressure between the two sides and inversely proportional to the tissue thickness
oxygen transport in the blood
most carried by haemoglobin in red blood cells
3 percent dissolved in plasma
reversible binding o2 to heme- high po2 is binding, low po2 is release
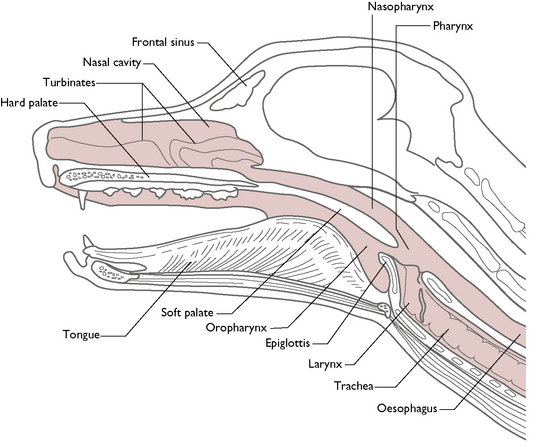
anatomy of urt
where is oesophagus relative to the larynx
where is the trachea relative to the oesophagus
oesophagus lies dorsal to larynx
trachea lies ventral to oesophagus
what is the blood gas barrier
surfactant
type 1 alveolar epithelial cell
basal laminar of epithelial cell
connective tissue
basal lamina of endothelial cell
endothelial cell
plasma
rbc membrane
0.2-0.6um thick
large surface area to volume
diffusion of oxygen and carbon dioxide in the lung
lower partial pressure in venous end compared to arterial end for oxygen
vice versa for carbon dioxide
move from an area of low to high partial pressure
diffusion of oxygen from capillary into tissue
what is the systemic arterial blood pressure
what is the pressure in the interstitial fluid
what does this mean
systemic arterial blood partial pressure 95mmHg
Interstitial fluid 40mmHg
large pressure difference meaning rapid diffusion
partial pressure of blood leaving the capillaries drop
oxygen carriage in blood
most carried by haemoglobin, some dissolved in plasma
reversible binding oxygen to haem
high po2 is binding, low po2 is release
carbon dioxide carriage in blood
most as bicarbonate ion which is important for acid base balance
some carried by Hb
some dissolved in plasma
reversible binding of carbon dioxide to amine radicals of Hb- carboaminohaemoglobin
importance of ventilation and perfusion
to maintain proper concentrations of oxygen, carbon dioxide and hydrogen ion concentration in tissues
features of the upper respiratory system
respiratory epithelium- nose to terminal bronchioles, lined by mucus which keeps epithelium moist and traps small particles
cilia beats mucus towards the pharynx
nasal cavity warms, humidifies and filters air, turbulent precipitation
features of the lower respiratory tract
what are the 2 zones
features of the 2 zones
CONDUCTING ZONE
structural support (cartilage which decreases as descend to lower levels)
modulation of airway diameter (smooth muscle)
defence ( mucociliary escalator, mucus production by goblet cells and glands, ciliated epithelium
RESPIRATORY ZONE
gas exchange (type 1 pneumocytes- very thin, and capillaries in intimate contact with air spaces)
redistribution of ventilation (limited smooth muscle)
maintain open alveoli (type 2 pneumocytes- produce surfactant)
pleural cavity
what is it
what does it contain
what does it surround
is a potential space between the paritiel and visceral pleura
contains small volume of serous fluid which helps lubrication
surrounds lungs in the thoracic cavity
is a vaccum
negative pressure essential to pull lungs out when ribcage and diaphragm expand thoracic cavity
the pleura
visceral plura
attached to surface of lung inc fissures
elastic fibres
continuous with parietal at the hilium
parietal pleura
covers internal suface of thoracic cavity
mediastinal- lines mediastinum
costal- lateral wall of rib cage
cervical- extension of pleural cavity into neck
diaphragmic- lines cranial surface of diaphraghm
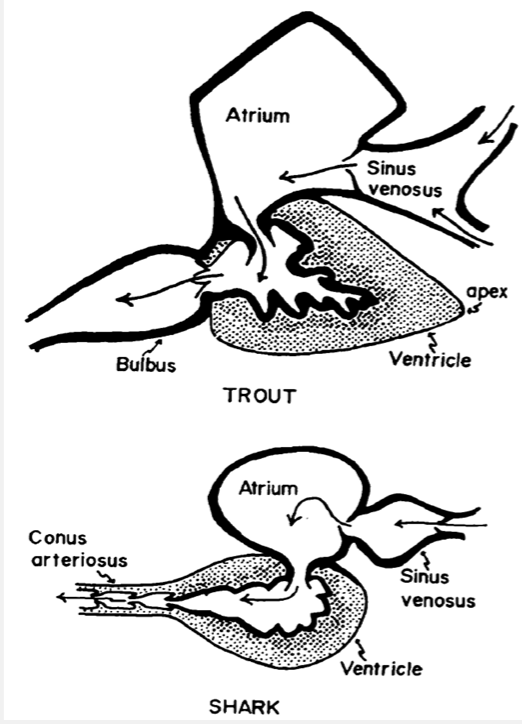
fish circulatory
type
what does the sinus venosus recieve and what does it contain
where does the bulbus arteriosus extend between. what does this structure allow
what is the conus arteriosus
fish have a single circulatory system where there is a single atrium and a single ventricle.
the sinus venonus recieves deoxygenated blood and acts as a reservoir and contains the pacemaker
bulbus arteriosus is a thick walled chamber that extends between the single ventricle and the ventral aorta. allows maintenance of continuous blood flow into the gill arches. elastic
conus arteriosus is the whole of the headward portion of the heart in fish which interveenes between the ventricle and anterior boundary of the pericardiac space. not all fish have- mostly replaaced by the non muscular bulbus arteriosus.
amphibian heart
double
2 atria and a single ventricle
spiral valve
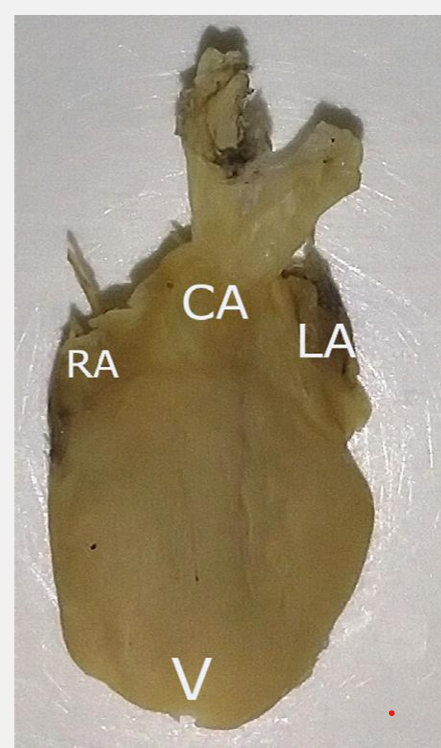
mammals, birds and crocadilians
fully developed septum between the atria (all) and ventricles (mammals and birds)
cranial vena cava
pulmonary veins- from lung
aorta- to body
pumonary artery- to lungs
vena cava caudal
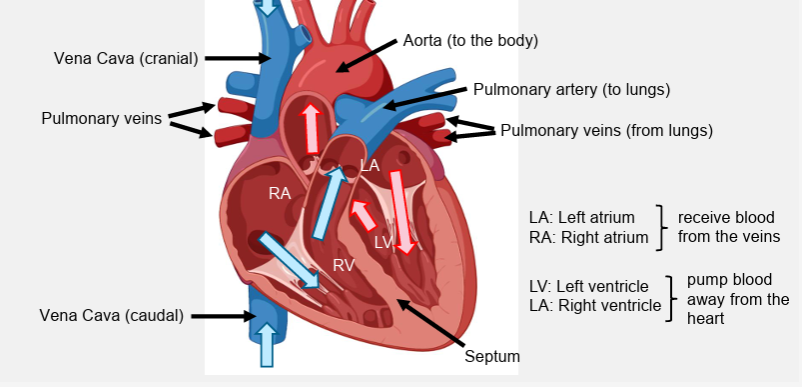
pulmonary vs systemic circulation
pulmonary- to and from lung. right pumps deox to pulmonary circulation at low pressure
systemic- to and from body. left side pumps oxygenated to systemic at high pressure
exterior anatomy
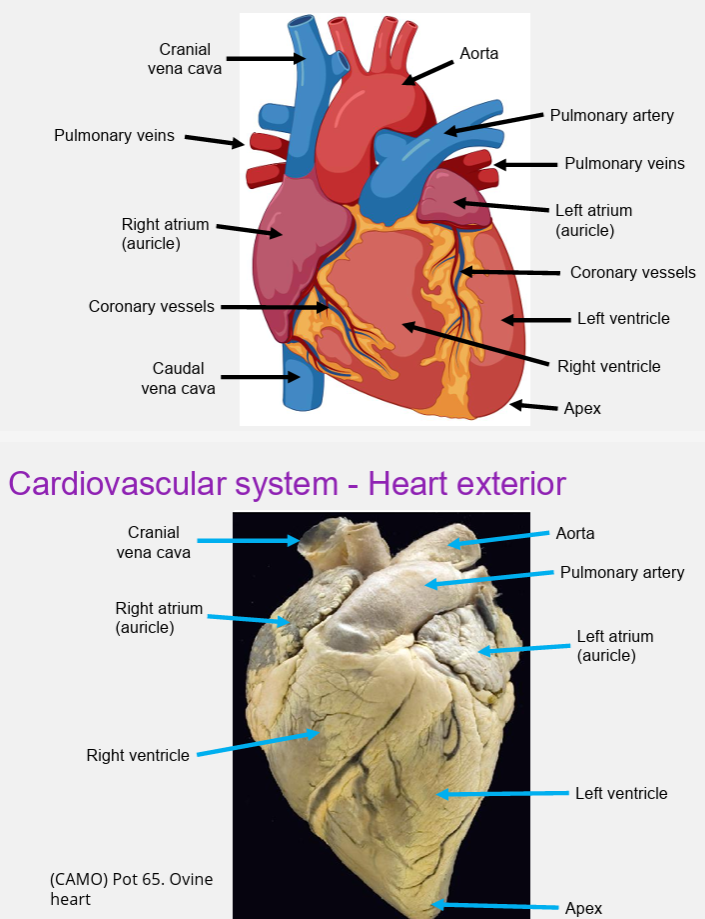
dog vs pig vs sheep
pressure of
cranial vena cava
aorta
pulmonary artery
pumnonary vein
cranial vena cava- deoxygenated blood at 3mmHg
aorta to rest of body 100mmHg systemic
pulmonary artery to lungs 12mmHg pulmonary
pulmonary vein oxygenated blood 7mmHg
what surrounds the heart
pericardial sac
epicardium- visceral pericardium
parietal pericardium
layers of the heart wall
endocardium
myocardium
epicardium
what connects the papillary muscles to the tricuspid and mitral valves
chordae tendinae
when the ventricles contract what is evasion of the cusps prevented by
action of the papillary muscles through the chordae tendinae
how many cusps do the semilunar valves hve each
3
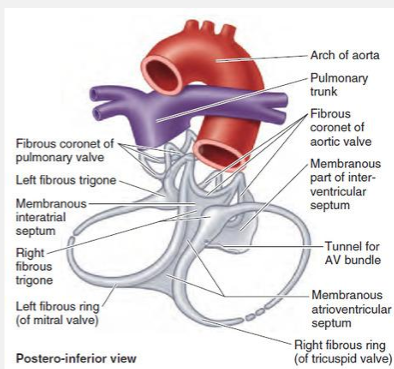
cardiac skeleton
function
structure
helps provide structural integrity to the heart with fibrous tissue
breaks up continuity between cardiac muscle cells of the atria and the ventricles
four fibrous rings, right and left fibrous trigones, and finally the membranous aspects of the interatrial, interventricular and atrioventricular septa.
surround the orifices of the pulmonary, aortic and atrioventricular valves,
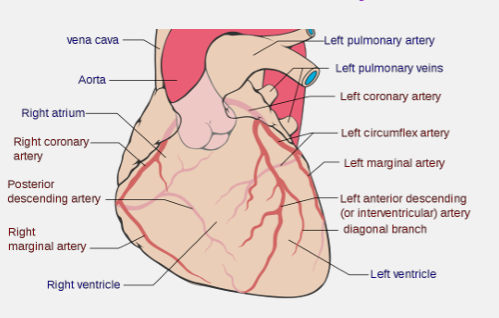
coronary arteries
where do they branch off of
how much percent of cardiac output is delivered directly into the myocardium
left and right branch from the base of the aorta
are the first branches off the aorta, 5 percent of cardiac output is delivered directly into the myocardium
extensive capillarisation
function of elastic vessels
large artries
accomodate stroke volume- high elastance
convert intermittent ejection into continuous flow
conduit ad feed vessels
medium to small
conduct blood flow to organs
resistance vessels
examples
what do they control
arterioles, terminal arteries
control arterial blood pressure
control local blood flow
exchange vessels
capillaries
nutrient delivery to cells
lymph formation
removal of metabolic waste
removal of metabolic waste
capacitance vessels
example
what do they control
what do they act as
venules, veins
control cardiac filling pressure
reservoir of blood
distribution of blood
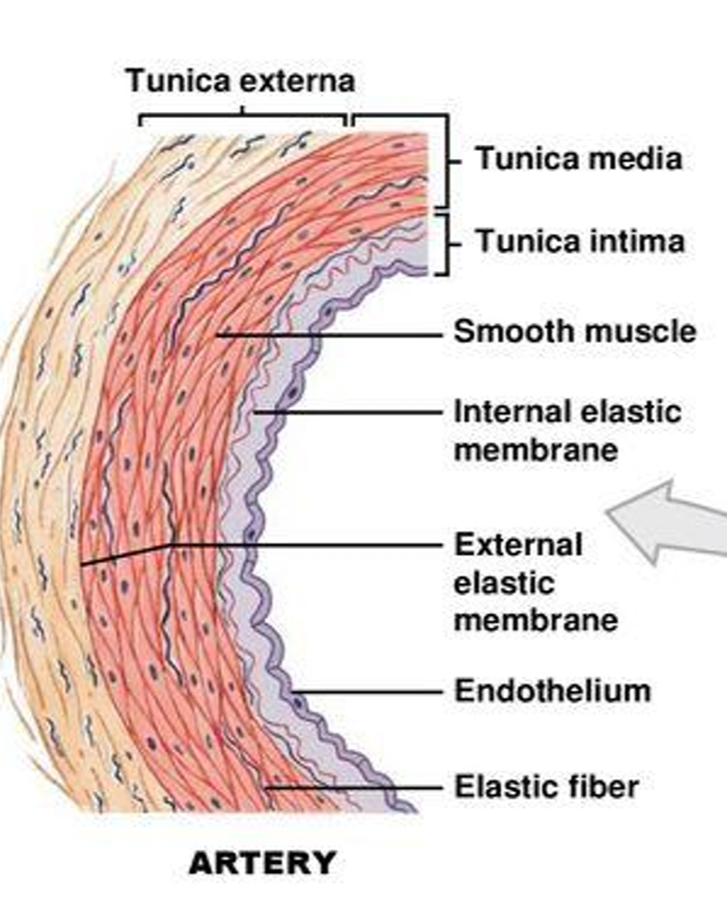
artery structure
transverse section- usually round with relatively thick wall
rippled tunica intima and has internal elastic membrane. single layer of endothelial cells, simple squamous
thick, dominated by smooth circular muscle cells and elastic fibre in tunica media. has externall elastic membrane
tunica externa- collagen and elastic fibres, nerve terminals, vasa vasorum
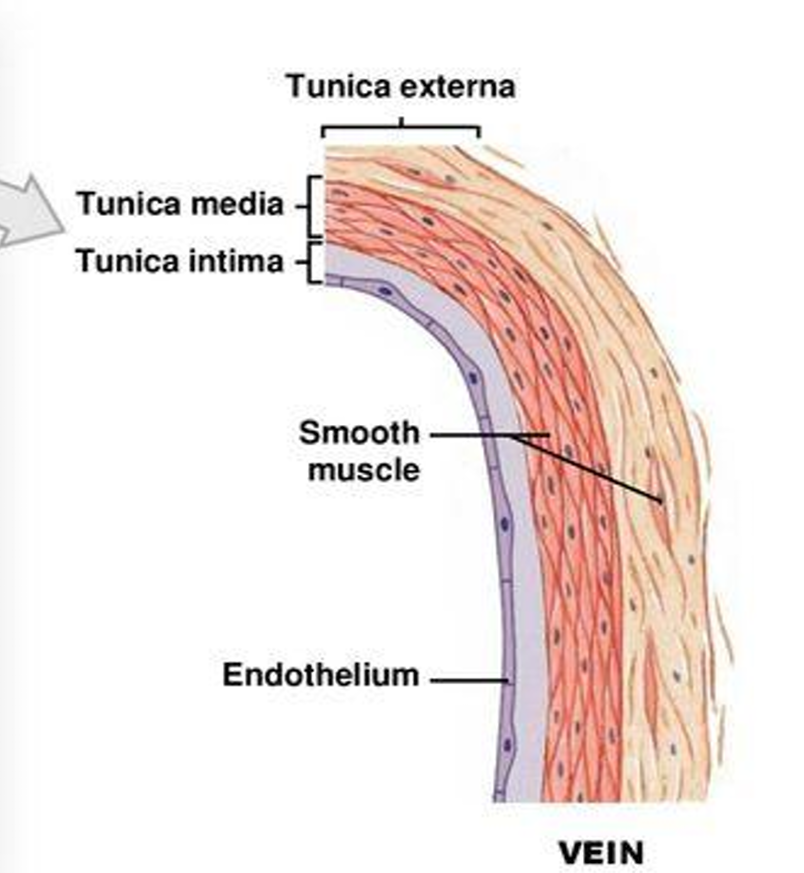
vein structure
transerse section-usually flattened or collapsed with relatively thin wall
tunica media- often smooth, no internal elastic membrane
tunica media- thin, dominated by smooth muscle cells and collagen fibres, no external elastic membrane
tunica externa- collagen and elastic fibres, smooth muscle cells, nerve terminals
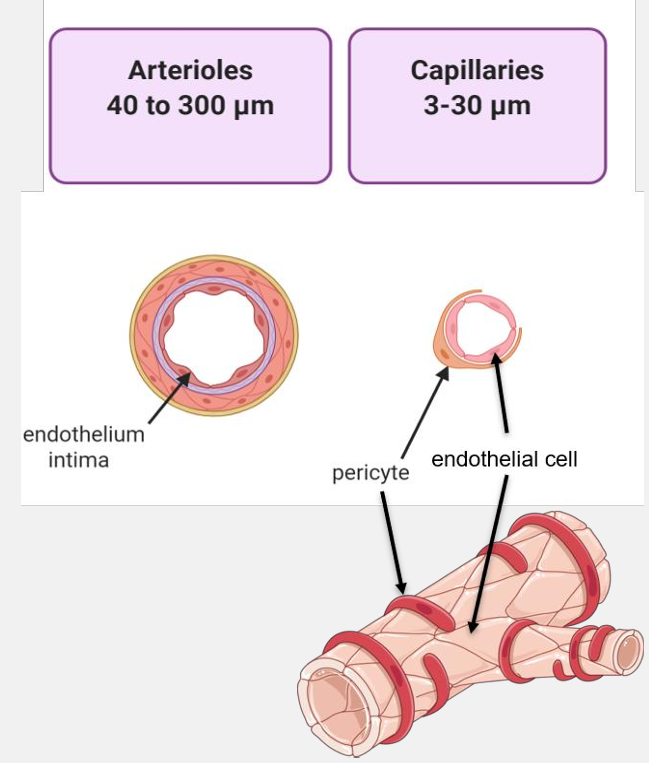
arterioles and capillaries diameter
what is flow
amount of blood flowing through a vessel at a given time
what is perufsion
flow per unit mass of tissue
calculating resistance to flow in a tube

what is the relationship between flow, pressure and resistance
blood flow is directly proportional to the blood (hydrostatic) pressure gradient. if hydrostatic pressure gradient increases blood flow speeds
blood flow (F) is inversely proportional to peripheral resistance (R)
F= ΔP/R
resistance is more important in influencing local blood flow because it is easily changed by alteirng vessel diameter
generation of interstitial fluid
oncotic pressure- pressure exerted by the proteins
hydrostatic pressure- pressure exerted by the blood
movement of fluid depends on four variable known as starling forces
lymph formation- what pressure does the blood enter and leave the capillary
blood enters the capillary around 35mmHg and leaves around 15mmHg
filtration process provides continuous supply of intersitital fluid to form lymph
lymphatic system
lymphatic vessles carry intersitital fluid to the cardiovascular system
abnormal accumulation of interstitial fluid is known as oedema
excess filtration
defective resorption
defective lymphatic drainage
increased capillary permeability, increased capillary pressure, decreased plasma protein, decreased lymphatic drainage
mammalian foetus
what connects the atria and what does this become
what connects the pulmonary trunk and aorta and what does this layr become
foramen ovale connecting the atria (becomes fossa ovalis)
ductus arteriosus- vessels between the pulmonary trunk and aorta becomes the ligamentum arteriosum
pneumothorax
pleural effusion
haemothorax
pyothorax
air
fluid
blood
pus
where do these chemical mediators in the regulation of cardiovascular function have their site of origin?
noradrenaline
adrenaline
acetylcholine
renin
angiotensin ii
aldosterone
ADH/ vasopressin
ANP atrial natriuretic peptide
nitric oxide NO
sympathetic nerve terminals
adrenal medulla
parasympathetic nerve terminals
kidney (juxtaglomerular apparatus)
lung endothelium
adrenal cortex (glomerulosa)
posterior pituitary gland
atrial myocardium
vascular endothelial cells