Block 6: Week 4: Psychosis
1/56
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
57 Terms
stat for schizophrenia - deaths?
People with schizophrenia are 2 to 3 times more likely to die early than the general population (often due to cardiovascular, metabolic, and infectious diseases).
stat for schizophrenia - treatment?
More than two out of three people with psychosis in the world do not receive specialist mental health care.
what is psychosis?
fundamental and characteristic distortions of thinking and perception, and by inappropriate or blunted affect.
ICD 11 vs ICD 10 in schizophrenia diagnosis?
no more schizophrenia substypes - focus on course and symptoms.
what are requirements of schizophrenia diagnosis on the ICD-10?
1 syndrome or 2 symptoms for most of the time (or at some time during most of the days) for at least 1 month.
Not a manic or depressive episode or at least present before these.
Not attributable to organic brain disease.
Not attributable to alcohol or drug-related intoxication, dependence or withdrawal.
what are the positive symptoms of schizophrenia? (syndromes)
Thought echo, insertion, withdrawal or thought broadcasting.
Delusions of control, influence or passivity of thought, action or sensation delusional perception.
Persistent delusions that are bizarre or impossible (allowing for cultural factors)
Catatonic behaviour, such as stupor, mutism, posturing, excitement
what are the positive symptoms of schizophrenia?
Disordered thought (derailment, incoherence, neologisms, irrelevance).
Hallucinatory voices in 3rd person, discussing, running commentary or coming from part of the body.
“Negative symptoms” (apathy, blunting or incongruity of emotional response, poverty of speech, NOT due to medication.
Other persistent hallucinations (accompanied by delusions).
what are negative symptoms of schizophrenia?
7As:
Apathy (loss of feeling).
Avolition (loss of motivation).
Anergia (loss of energy).
Alogia (loss of speech).
Anhedonia (loss of pleasure).
Asociality (loss of sociability).
Affective flattening (flat affect).
Impaired Attention.
what are the cognitive symptoms of schizophrenia?
Average IQ = 95 and may decline after 1st episode.
Discrepancy in verbal / non-verbal IQ.
Impaired attention.
Executive function - problem solving, response inhibition, planning.
Overinclusiveness, verbal redundancy.
what is Liddle’s 3-syndrome model of schizophrenia?
Reality distortion - hallucinations, delusions
Disorganization - thought disorder, inappropriate affect
Psychomotor poverty – poverty of speech, blunt affect
what are the associated findings with schizophrenia?
Increased volume of ventricles.
Decreased volume of cortex.
More neurons with less connections.
what has functional imaging shown patterns of in schizoprenia?
patterns of activity reflect symptoms:
- Auditory hallucinations - Broca’s area
- Negative Symptoms - prefrontal cortex
- Passivity - Cingulate gyrus
describe the epidemiology of schizophrenia? (M/F)
M = F BUT depends on criteria
Earlier peak onset in males (mean 22 v 26).
describe the epidemiology of schizophrenia? (incidence)
Incidence 1-2/10000/year
describe the epidemiology of schizophrenia? (populations)
Present in all populations:
Urban > Rural (2-3 X risk).
Most common in SocioEconomicClass IV & V (poorer).
what is the aetiology of schizophrenia? (heritability).
identical twins = 48% concordance rate.
fraternal twins = 17% concordance rate.
strong evidence for genetic component.
what are prenatal risk factors for schizophrenia development?
Premature births.
Unwanted pregnancy (4X).
Maternal influenza.
Rubella.
IUGR (Intrauterine growth restriction) or malnutrition.
Associated medical problems eg:DiabetesMellitus.
what are obstetric/neonatal risk factors for schizophrenia development?
obstetric complications,
low birth weight,
hypoxia,
association with structural brain abnormalities.
what are early childhood risk factors for schizophrenia development?
mixed handedness,
mixed hand and eye dominance,
late milestones.
what are adult risk factors for schizophrenia development?
age (earlier onset in those with biological risk factors).
gender effects (males present earlier).
urban vs rural birth and rearing.
migrants risk 4-6 times greater in 2nd generation, decline in subsequent generations.
what are late/precipitant risk factors for schizophrenia development?
life events (more frequent in the few weeks before onset of psychosis).
stress.
substance abuse
what substance abuse particularly is a risk factor for schizophrenia?
cannabis, CBD:THC ratio important, the lower the ratio the worse the risk.
(also amphetamines/cocaine/crack).
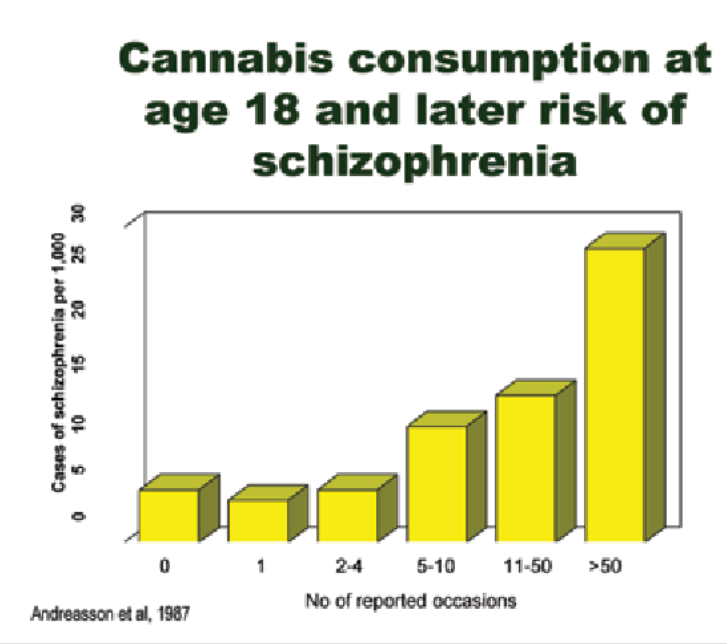
what are dopamine levels like in acutely psychotic individuals?
Individuals who are acutely psychotic, they show an excessive striatal release of dopamine.
what is the role of dopamine?
Dopamine is involved in reward learning and normally mediates attachment of salience to ideas and objects.
what does excessive dopamine release lead to? (salience)
aberrant assignment of salience (unimportant stimuli) - delusions may arise from here?
what are the 4 dopamine pathways?
mesolimbic,
mesocorticol,
nigrostriatal,
tuberohypohyseal.
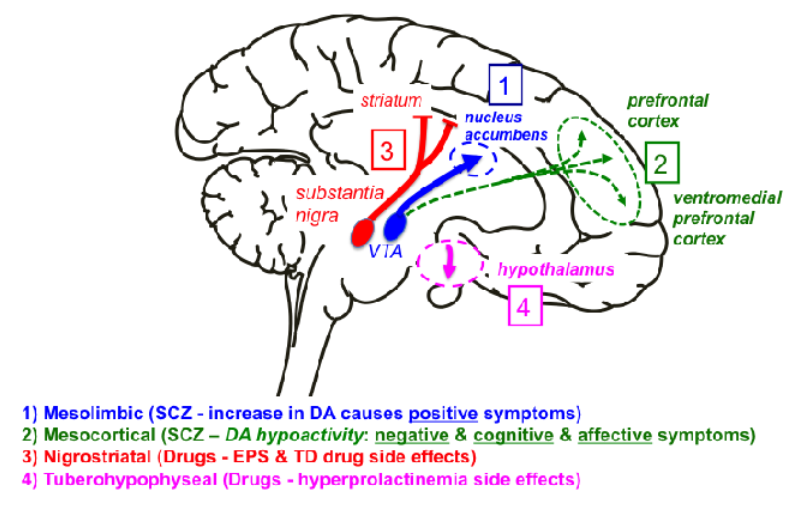
what happens to mesolimbic pathway in schizophrenia?
increase in dopamine causes positive symptoms - reward, motivation, and reinforcement.
what happens to mesocorticol pathway in schizophrenia?
dopamine hypoactivity leads to negative / cognitive / affective symptoms - cognition, executive functions, motivation, and emotional responses.
what happens to the nigrostriatal pathway in schizophrenia?
drugs: extrapyramidal symptoms and Tardive Dyskinesia.
involuntary repetitive movement.
what happens to the tuberohypohyseal pathway in schizophrenia?
drugs: hyperprolactinemia side effects
what is the glutamate hypothesis?
dysfunctional NMDA receptors lead to lower glutaminergic transmission (-ve symptoms).
lower glutaminergic transmission leads to lower GABA transmission,
so less inhibitory effect on dopamine neurons, meaning more dopamine release (+ve symptoms).
differential diagnosis of schizophrenia?
Depressive psychosis.
Mania.
Autistic spectrum disorder.
Acute and Transient psychotic episode.
Schizoaffective Disorder (F25).
Intoxication (NOT drug induced psychosis).
Delirium and other medical problems.
organic causes of psychosis/psychosis-like symptoms: autoimmune?
e.g encephalitis
organic causes of psychosis/psychosis-like symptoms: tumours?
temporal lobe - auditory.
occipital lobe - visual.
limbic and hypothalamus - delusions.
organic causes of psychosis/psychosis-like symptoms: neurological conditions?
Parkinson’s (secondary to mood, dementia or medication),
MultipleSclerosis, MotorNeuronDisease, Huntington’s…
organic causes of psychosis/psychosis-like symptoms: infection?
HIV, Neurosyphilis,
Neuroborreliosis (Lyme disease),
meningitis/encephalitis
organic causes of psychosis/psychosis-like symptoms: endocrine?
Hypo/hyperthyroidism,
Hypo/hyper parathyroidism,
Adrenal disorders
organic causes of psychosis/psychosis-like symptoms: medications?
cardiac (digoxin/betablockers), antiparkinsons, corticosteriods…
what are acute and transient psychotic disorders?
Acute onset of delusions, hallucinations, incomprehensible or incoherent speech with disruption of normal behaviour.
Complete recovery usually occurs within a few months.
what are criteria for acute/transient psychotic disorder diagnosis?
Interval from first appearance to presentation is < 2 weeks.
Not due to drugs or organic cause.
Not fulfilling criteria for mania or depression.
what are pharmacological treatments for psychosis?
antipsychotics - first and second generation.
what are psychological treatments for psychosis?
family therapy, CBTp, trauma focus, help with voice hearing…
what are social treatments for psychosis?
housing, employment/education support, social connections, community engagement
what are lifestyle interventions for psychosis?
smoking, exercise, meaningful activity.
treatment for substance use and other comorbid problems.
what is the timeline for antipsychotic use?
Treatment with lowest effective dose for at least 1-2 years after 1 episode
or 3-5 years after recurrent episode (potentially lifelong).
treatment approaches - clozapine?
Clozapine is used for resistant symptoms (where 2 other antipsychotics including at least one SecondGenerationAntipsychotic have failed or not been tolerated).
what are the main side effects of antipsychotics?
sedation, weight gain (& metabolic).
hyperprolactinaemia, involuntary movements,
QTc prolongation on ECG & associated risks.
what do antipsychotics typically target?
Dopamine (D2) antagonists (except for clozapine).
what monitoring is used with antipsychotic treatment?
Physical Healthcare and monitoring commencing proactively as early as possible to address the reduced life expectancy and mitigate side-effects.
e.g ECG for QT interval prolongation.
what routine checkups are carried out in primary care for patients with Schizophrenia?
BMI (weekly for first 6 weeks, then 3 months, then yearly).
Serum electrolytes and urea (yearly).
FBC (yearly).
Plasma glucose or HbA1c (3 months post treatment then yearly).
Pulse/BP (at each dose change).
ECG monitoring.
Prolactin + sexual health (6 months post treatment, then yearly).
LFT (every 12 months).
what risks to general health does schizophrenia pose? - CVD risk
increased CVD risk (stress, genetic risk, lifestyle issues, social disadvantage, antipsychotics (weight gain/insulin resistance).
what risks to general health does schizophrenia pose? - Type 2 diabetes risk
antipsychotics (weight gain/insulin resistance) and lifestyle (poor diet/exercise)…
also impaired glucose homeostasis more commonly present at disease onset in people with schizophrenia.
what risks to general health does schizophrenia pose? - smoking-related issues
increased COPD/smoking-related issues (psychotic disorders more likely to smoke than general pop.).
what risks to general health does schizophrenia pose? - cancer risk
cancer (late recognition and undertreatment, women with schizophrenia 31% more likely of developing breast cancer)
what areas increase risk of premature death for those with schizophrenia?
increased risk of suicide,
increased risk of physical disorders (CVD, type 2 diabetes, COPD, cancer…).
why are those with schizophrenia at higher risk of social exclusion?
negative symptoms, such as emotional blunting, reduced speech, loss of motivation, self-neglect, and social withdrawal, are often the major cause of social exclusion by impairing the person's ability to learn, work, and maintain relationships.
what are the risks of social isolation on health?
Heart disease and stroke.
Type 2 diabetes.
Depression and anxiety.
Suicidality and self-harm.
Dementia.
Earlier death.