PCT - Respiratory System (A&P)
1/102
Earn XP
Description and Tags
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
103 Terms
Anatomy of the upper airway
soft palate
palatine tonsil
epiglottis
vocal fold
esophagus
hard palate
tongue
pharynx (opa, npa, lpa)
larynx
anatomy of the lower airway
trachea
alveoli
main bronchi
smaller bronchi
bronchioles
bifurcation of the lungs
carina
trachea
conduit for air entry, 10-12cm, C-shaped cartilaginous rings, descends to level of fifth or sixth thoracic vertebra
hilum
point of entry for blood vessels and bronchi on each lung
lobes of the lung
3 in right lung
2 in left lung
pleura
visceral pleura lines the lungs
parietal pleura lines the thoracic cavity
small amount of synovial fluid between them to allow reduction of friction when breathing
bronchus
divides into smaller bronchi once it enters lungs
alveoli
balloon-like clusters of single-layer (cell) air sacs, functional site for gas exchange of oxygen and carbon dioxide with the pulmonary capillaries
surfactant
decreases surface tension to keep alveoli open
atelectasis
when alveoli collapse
total lung capacity
6 liters for an adult man
Tidal Volume (Vt)
volume of air that is inhaled/exhaled during a single respiratory cycle, normal is 5-7mL/kg (~500mL)
Inspiratory reserve volume
amount of air that can be inhaled in addition to normal Vt (around 3000mL)
Dead Space (Vd)
amount of space not participating in gas exchange
3 types:
Anatomical
Alveolar
Physiological
Anatomical dead space
includes trachea and larger bronchi, air lingers but does not partake in gas exchange, typically 150mL or 30% of normal Vt
Alveolar dead space
not perfused alveoli
Physiological dead space
Anatomical dead space + alveolar dead space, created by intrapulmonary obstructions or atelectasis (alveolar collapse), mucus, inflammation, mechanical obstruction
Alveolar Volume
volume of air that reaches the alveoli and participates in gas exchange, approx. 350mL participating in gas exchange
Va = Vt - Vd
Minute Volume (Vm)
Amount of air that moves into and out of the respiratory tract per minute
Vm = Vt * RR
Minute Alveolar Volume (Va)
Amount of air that actually reaches the alveoli per minute and participates in gas exchange
Va = Vt- Vd * RR
Functional Residual Capacity (FRC)
Volume of gas remaining in lungs at the end of normal tidal volume exhalation, PEEP limits exhalation (increases FRC and keeps alveoli from collapsing)
Expiratory Reserve Volume
amount of air that can be exhaled following a normal exhalation, approx. 1200mL
residual volume
cannot completely empty your lungs, residual volume is the amount of air that remains in the lungs after maximal expiration, also approx. 1200mL
Vital Capacity
equal to the sum of tidal volume, inspiratory reserve volume, and expiratory reserve volume (Vc = Vt+Vir+Ver)
Fraction of Inspired Oxygen (FIO2)
Percentage of oxygen in inhaled air, increases when supplemental oxygen is given to a patient.
May decrease at altitude, in confined spaces, chemical vat
Expressed as decimal (i.e. breathing room air 21% O2, FIO2 0.21%)
Two phases of Ventilation
Inspiration (Inhalation)
Expiration
One cycle = one inhalation (one third) and one expiration (two thirds)
Regulation of Ventilation
regulated by pH of the CSF (cerebral spinal fluid) - directly related to the amount of CO2 dissolved in the blood (PaCO2)
Involves a series of receptors and feedback loops to sense CO2, pH, and O2 concentrations in the blood and plasma
These receptors send signals to the respiratory centre of the brain to alter ventilations accordingly, increase or decrease ventilation
neural control of ventilation
involuntary control of breathing originates in the brain stem in the pons and medulla, impulses descend through the spinal cord and can be overridden by voluntary control (breath holding)
Two motor nerves affect breathing
phrenic nerve innervates the diaphragm
intercostal nerve - innervates the external intercostal muscles between the ribs
Control center in the brain process to regulate breathing
CO2 increase/pH decrease travels along with nerve signal triggered by O2 sensor in artery indicating low O2 levels to breathing control centers in medulla and pons which send nerve signals to trigger contraction of intercoastal muscles and diaphragm
respiratory center
in the medulla, divided into 3 regions
3 regions of respiratory center
Respiratory rhythmicity center (inferior)
apneustic center
pneumotaxic center (superior)
respiratory rhythmicity center
sets RR, inhalation at 2 seconds, relaxes for 3 seconds allowing for passive exhalation
apneustic center
receives signals from the chest wall (mechanical stretch receptors) and bronchioles via the vagus nerve to inhibit inhalation and thus expiration occurs, PREVENTS OVEREXPANSION, INCREASES NUMBER OF INSPIRATIONS/min
pneumotaxic center
working opposite apneustic center, it inhibits inspiration and in times of increased demand it decreases influence of apneustic influence and increases respiratory rate
Chemical control of ventilation
keeps concentrations of O2 and CO2 in blood, component of acid-base balance, within a narrow range
CO2 is the most powerful stimulant to affect the respiratory center (too much is acidosis), small increases as little as 1% can increase minute volume, whereas small change in PO2 has almost no effect (don’t use all the O2)
Hypercarbic Drive
amount of CO2 in bloodstream controlled by a negative feedback loop, primary stimulus to breathe
Chemoreceptors
monitor levels of CO2, O2, and the pH of the CSF and provide feedback to the respiratory center to modify rate and depth and respiration based on the body’s current needs
hydrogen ions to regulate ventilation
pH of blood has a powerful effect on respiratory center, CO2 and pH inversely rise and fall together causing a combined effect in the control of respirations
CO2 + H2O = H2CO3 = H +HCO3
central chemoreceptors
located adjacent to respiratory center in the medulla, monitor and sense minute changes in the pH of the CSF (H+)
H+ goes up, pH goes down, excitatory response to increase rate and depth of breathing
peripheral chemoreceptors
located in the carotid bodies and aortic arch, monitor and sense reduction in O2 and to a lesser degree CO2, pH in arterial blood
aortic arch detects levels of O2 and CO2 but not pH, carotid detects all three
control of ventilation by other factors
body temperature (febrile), medications, hypoxia, acidosis, metabolic rate
Accomplished mechanic of ventilation
pressure changes brought about by contraction and relaxation of the intercostal muscles and diaphragm
inhalation mechanics of ventilation
active process initiated by the contraction of the respiratory muscles with the net effect to increase the volume of the chest, the lungs undergo a comparable increase in volume and negative-pressure ventilation-air flows into the expanded lungs because pressure inside less than outside
Exhalation Mechanics of Ventilation
passive process at the end of inhalation, the respiratory muscles relax, natural elasticity of the lungs passively exhales the air
3 mechanics of ventilation
relaxation - no movement
inspiration - chest expands, diaphragm contracts
expiration - chest contracts, diaphragm relaxes
**Respiration
Mechanism to ensure a constant oxygen supply and the removal of excess carbon dioxide
2 Kinds of Respiration
external (pulmonary respiration) → environment and lungs
internal (cellular respiration → glycolysis, citric acid, etc.) between blood and cells
4 parts of circulatory system
pulmonary artery
pulmonary vein
arterial system
venous system
hemoglobin carrying capacity
4 molecules of O2
Oxygen dissociation curve
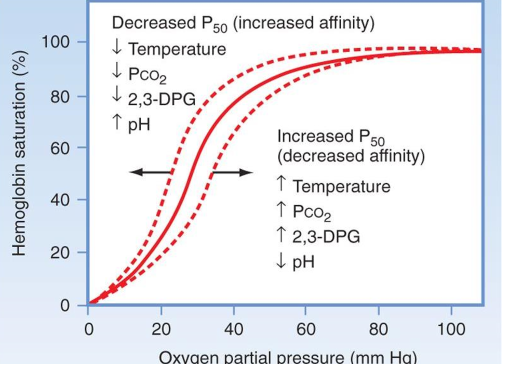
Factors Affecting Affinity of Oxygen to Hemoglobin
3 main
temperature (increase temp, decrease affinity)
pH (increase in H+ ions, decrease affinity)
Carbon dioxide (increase Co2, decrease affinity)
Bohr effect
changes in affinity of oxygen to bind to hemoglobin as a result of the shift in blood pH that occurs on a breath by breath basis, occurs at level of lungs and tissues
when blood is more alkaline, hemoglobin has a greater affinity for O2 and thus O2 is drawn toward hemoglobin at the alveolar/capillary level
when blood reaches tissue level, CO2 from cell. resp. diffuses from the tissue to the capillary blood
this shifts the blood pH toward the acidic side which weakens hemoglobin’’s hold on oxygen
blood that shifts toward acidic side of pH gives up O2 readily to the tissues
hemoglobin dissociation curve
oxygen from lungs
oxygen bonded to hemoglobin
oxygen released to tissue cells
hemoglobin in an alkaline state
strong affinity, draws O2 towards it
(if blood remained alkaline at tissue level, it would not release O2 to the tissues readily)
Hemoglobin in Acidotic state
weak affinity for O2, does not pick it up as readily, O2 bound to hemoglobin is released to tissue easily
(we attempt to compensate for this by providing supplemental oxygen which increases amount of O2 dissolved in blood plasma for transport)
False low Pulse oximetry cause
cold extremities
nail polish
inflating the bp cuff
ambient lighting (ambulance)
states of decreased perfusion
Falsely high O2 Sat readings can be caused by
anemia
CO poisoning
CO affinity for hemoglobin
200 times greater than O2, blocks oxygen off from hemoglobin
cyanide poisoning and O2
prevents utilization of O2 at the cellular level
Oxygenation
to provide oxygen (hyperoxygenate: to provide supplemental oxygen in a high concentration)
PaO2
the partial pressure of oxygen in the arterial blood
SpO2
Saturation percentage of oxygen, should be >90%
ventilation
refers to the movement of air into and out of the lungs
normal Partial pressure of CO2 (PaCO2) is
35-45 mmHg
(hyperventilation blows off CO2 and therefore may result in PaCO2 or ETCO2 level of less than 35mmHg)
ETCO2
End tidal carbon dioxide
Hyperventilation
when minute volume (RR*Vt) exceeds body’s metabolic demands
impaired ventilation of upper airway
obstruction : fboa (foreign body obstruction of the airway), epiglottis, swelling
impaired ventilation of the lower airway
obstruction - asthma, bronchospasm
impaired ventilation in chest wall
pneumo/tension pneumothroax, flail chest
impaired ventilation at the neurological level
Neurogenic dysfunction - CNS depressant drugs, cervical spinal trauma, CVA (cerbrovascualr accident)
Cheyne-Stokes respirations
Gradually increasing rate and depth of respirations followed by gradual decrease of respirations with intermittent periods of apnea, associated with brain stem insult
Kussmaul respirations
deep gasping respirations, common in ketoacidosis (diabetic coma)
biot respirations
irregular pattern, rate, and depth with intermittent periods of apnea, results from increased intracranial pressure
agonal respirations
slow, shallow, irregular respirations or occasional gasps, results from cerebral anoxia, may be seen briefly after the heart has stopped as the brain continues to send signals to the respiratory muscles
hypoxia
not enough oxygen, occurs in acidosis
diffusion
exchange of gases (O2 and CO2) between alveoli and pulmonary capillaries
gas moves from an area of high to low concentration
around 98% of body’s total O2 is bound to hemoglobin
conditions for diffusion
alveolar and pulmonary capillary walls must not be thickened
interstitial spaces between the alveoli and pulmonary capillaries must not be enlarged or filled with fluid
impaired diffusion causes
inadequate oxygen in the air (smoke inhalation, CO poisoning)
alveolar/bronchial pathologies, emphysema, bronchitis
interstitial space pathologies (pulmonary edema, submersion aspiration, interstitial lung disease)
capillary bed pathologies (severe atherosclerosis, pulmonary embolism)
atherosclerosis
hardening of arteries due to gradual plaque buildup
conditions for perfusion to occur
adequate blood volume
adequate hemoglobin within
pulmonary capillaries must not be occluded
there must be a functional left ventricle that allows for the smooth flow of blood through the pulmonary capillary bed
causes of impaired perfusion
inadequate blood volume - shock
inadequate hemoglobin - anemia
impaired circulation or flow - pulmonary embolus, myocardial infarction
general signs and symptoms of respiratory distress
stridor, wheezing, crackles, decreased LOC, accessory muscle use, tripod positioning, diminished breath sounds, tachycardia, tachypnea, pale, cool diaphoresis, bradycardia
stridor
partial obstruction of the upper airway
wheezing
bronchospasm/bronchoedma
decreased loc signs
disoriented, confused, combative, obtunded, (seizure), unconscious
perfusion
refers to circulation and oxygenation of blood as it circulates through the pulmonary capillary bed
Tachypnea, Tachycardia, pale, cool diaphoresis
Respiratory Distress due to SNS
purposes of O2
increase the PO2 in alveoli and blood
reduce ventilatory workload
reduce myocardial workload
Non-Rebreather Mask (NRB Mask) Flow rates (non-COPD)
6 lpm - 60%
7 lpm - 70%
8 lpm - 80%
9 lpm - 90%
10-15 lpm - 95+%
Nasal Cannula Flow Rates (non-COPD)
1 lpm - 24%
2 lpm - 28%
3 lpm - 32%
4 lpm - 36%
5 lpm - 40%
6 lpm - 44%
Simple Face Mask Flow Rate (Non-COPD)
10 lpm - 40-60%
(mostly for peds)
nebulizer flow rate
typically ran at 8 lpm and used to deliver medications such as bronchodilators and epinephrine
BVM flow rate
at 15 lpm - 100% O2 supplied
indicated of apneic pts and those with inadequate respirations
PEEP
Positive End-Expiratory Pressure
BVM Technique
J (modified) jaw thrust
Airways (OPA/NPA)
Work together
Slow, small squeeze - 5-7 cc/kg, over 1-2 seconds at 10-12/min using low pressure
difficulties with BVM
Mask seal
Obese
Age
No teeth
Stiff lungs
Ventilation Correction Steps
Mask adjustment - reapply the mask consider 2-hand
Reposition airway - place head neutral or slightly extended
(Try PPV and reassess chest mvmt)
Suction mouth and nose - use a bulb syringe or suction catheter
Open mouth - lift jaw forward
(Try PPV and reassess chest mvmt)
Pressure increase - increase pressure in 5-10cm H2O increments max 40cm H2O
Alternative airway - place endotracheal tube or laryngeal mask
(Try PPV and assess chest mvmt and breath sounds)
edentulous patient
no teeth