NUR215 Exam 3: Medication Administration, Gas Exchange and Oxygenation, Elimination (Part I: Urinary), & Client Education
1/145
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
146 Terms
Polypharmacy
use of multiple medications
What information makes a medication order/prescription from a provider complete?
date and time ordered, name of meds, strength, route, frequency, signature from provider
TACTIS
therapeutic effect, action, contraindications, toxic effects, interventions, safe dose
Rights of med administration
right medication, dose, client, route, time, documentation
What are the three checks?
remove from storage, take out of packaging, at bedside (compare to EMAR)
When is medication reconciliation performed
admission, transitions of care, discharge
Enteral types
oral, tube
Topical types
transdermal, ophthalmic, otic, nasal, intravaginal, rectal, inhaled
Parenteral types
ID, Subq, IM, IV
Intradermal needle
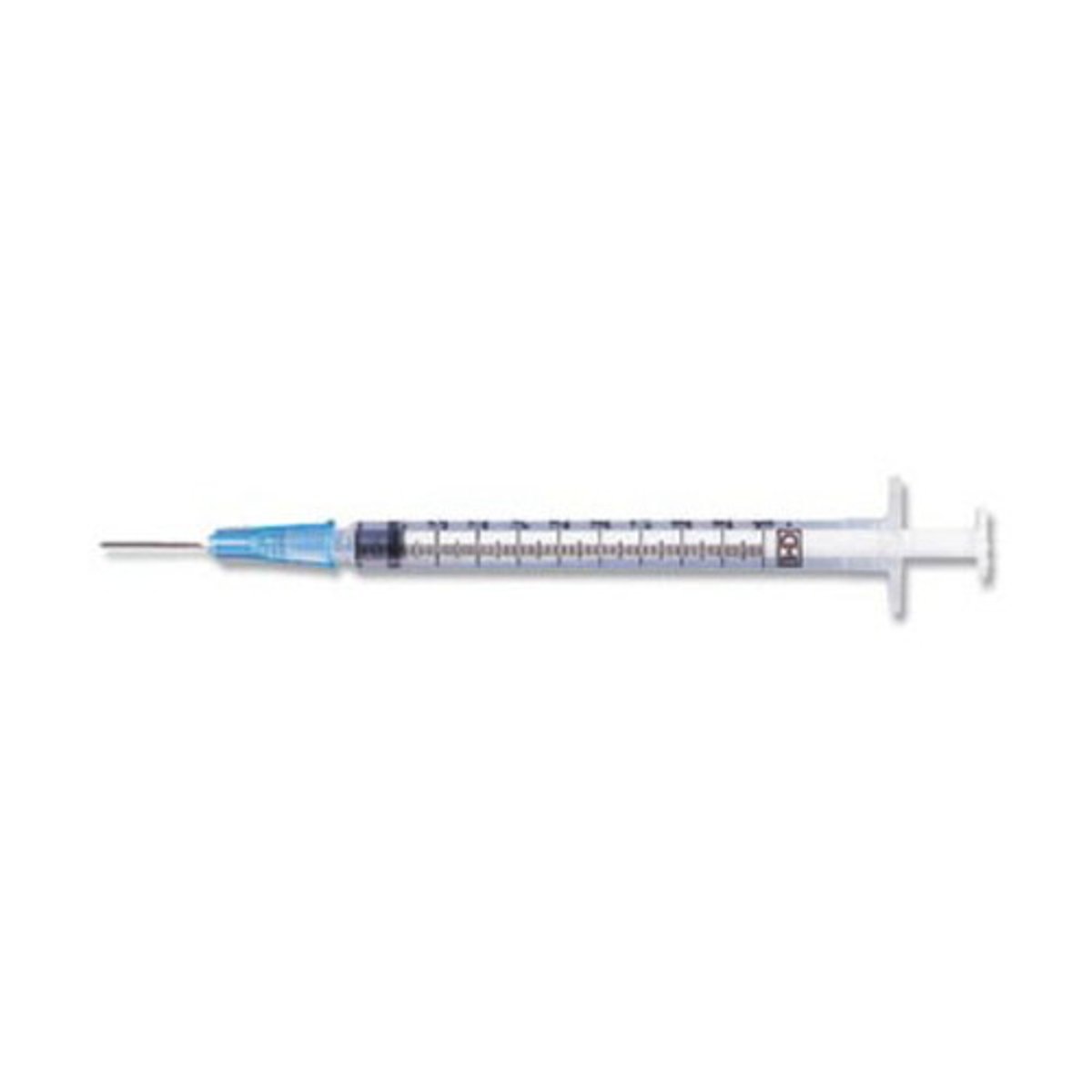
Intradermal angle
5-10 degrees
Subcutaneous needle
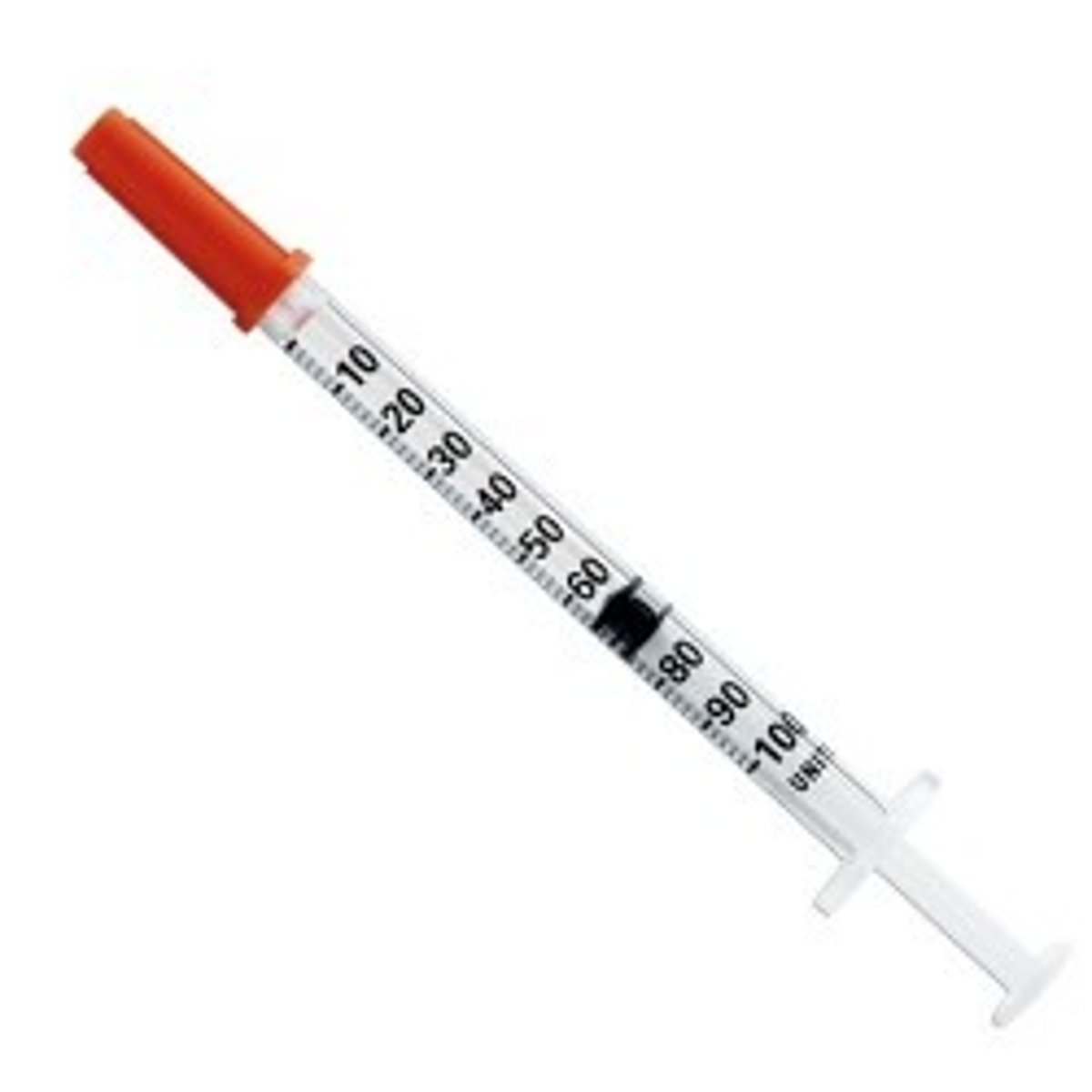
Subcutaneous angle
45-90 degrees
Intramuscular needle
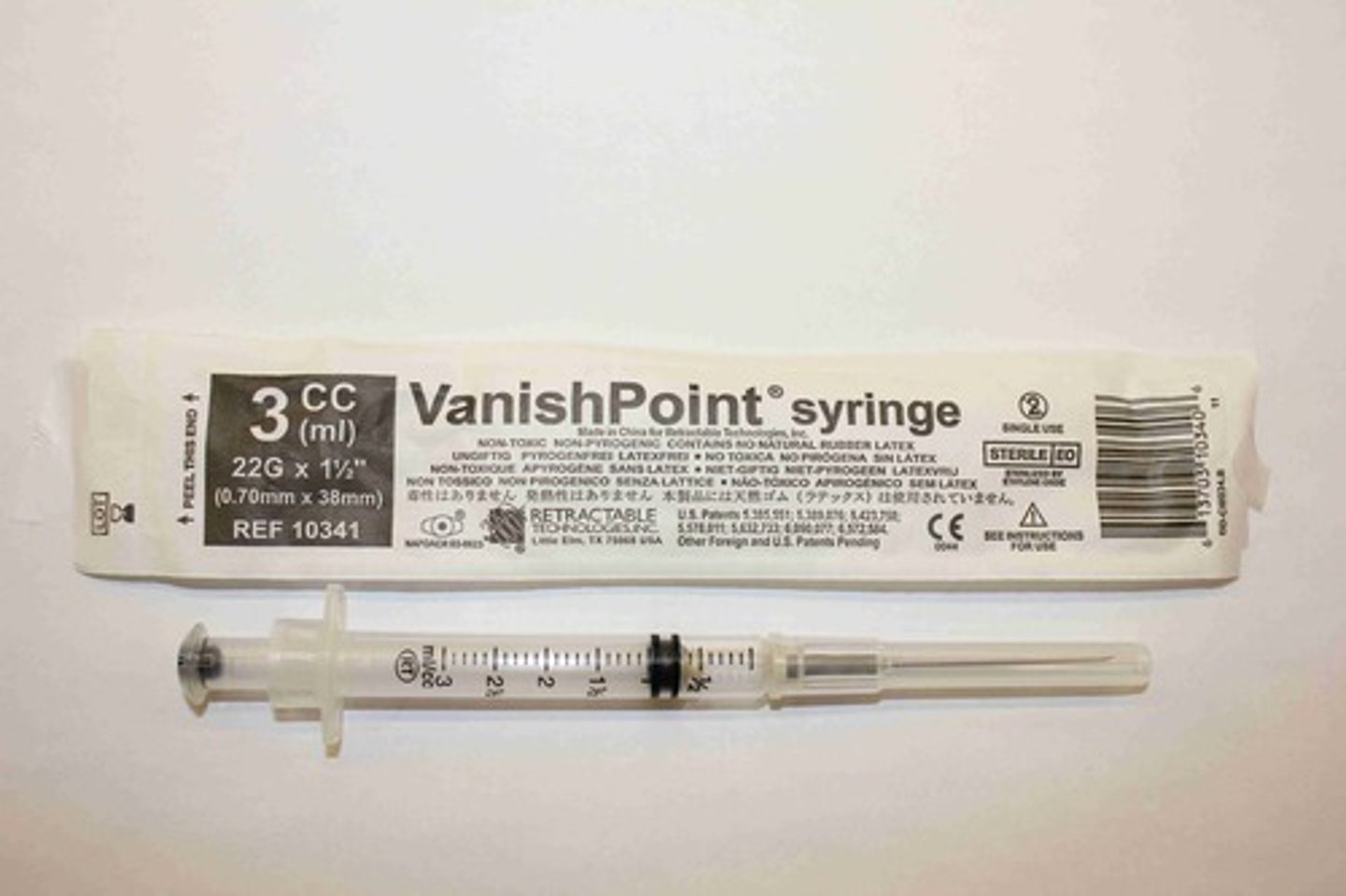
Intramuscular angle
90 degrees
Intravenous needle
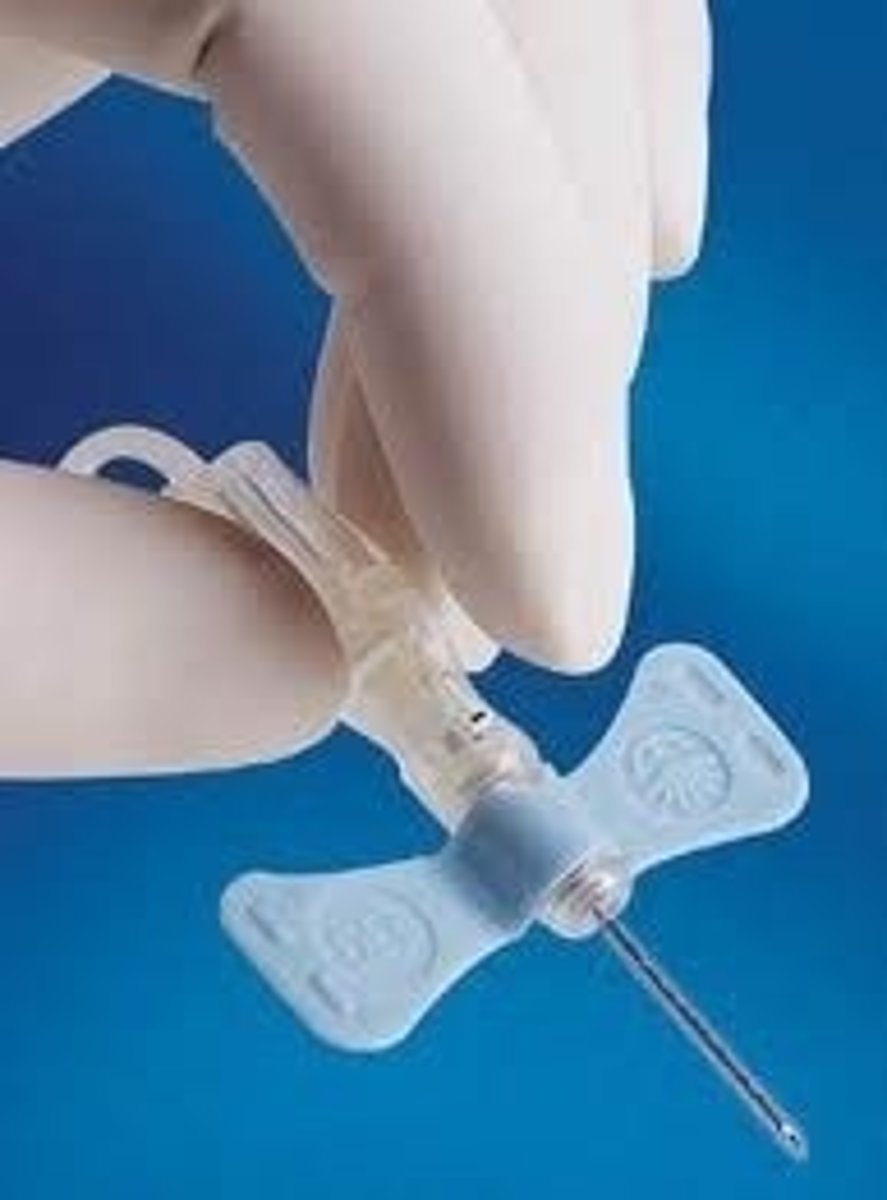
Intravenous angle
25 degrees
Blood flow route
heart, arteries, capillaries, veins, heart
Pulmonary circulation
flow of blood from the heart to the lungs and back to the heart
Respiratory upper airway anatomy
pharynx and larynx
Respiratory lower airway anatomy
trachea, bronchi, bronchioles, alveoli
Inspiration
diaphragm down, thoracic cavity increase
Expiration
diaphragm up, thoracic cavity decrease
Ventilation
moving gases in and out of lungs/alveoli
Diffusion
moving respiratory gases from one area to another by concentration gradients
Perfusion
ability of cardiovascular system to pump oxygenated blood to tissues and return deoxygenated blood to heart
Work of Breathing
effort required to expand and contract the lungs
Increased work of breathing
breathing faster, not enough oxygen
Increased WOB signs
accessory muscle use, increased RR and HR, diaphoresis, nasal flaring
Lung volumes
lung compliance and airway resistance
Lung compliance
ability of lungs to distend or expand
Diastole
rest, mitral and tricuspid valves permit flow to those relaxed ventricles
Systole
AV valves are closed, hear S1, semilunar valves closing - S2
Cardiovascular structure and function
myocardial pump, myocardial blood flow, systemic circulation, coronary artery circulation
Cardiac output
volume of blood pumped by the heart per minute
Stroke volume
amount of blood ejected from the heart in one contraction
Calculating cardiac output
CO = SV x HR
Normal stroke volume
50-75 mL/contraction
Preload
volume of blood in ventricles at end of diastole
Clients w decreased preload
dehydration, hypovolemia, hemorrhage, hypotensive
Clients w increased preload
hypervolemia (too much fluid), heart failure
Afterload
amount of resistance to ejection of blood from the ventricle
Clients w increased afterload
hypertension, coronary artery disease (blockage/clot)
Contractility
ability of heart to squeeze blood from the ventricles
The conduction systems
SA node, AV node, bundle of His, Purkinje network
P wave
atrial depolarization (contraction)
What does the P wave represent
SA node
QRS Complex
ventricular depolarization (contraction)
T wave
ventricular repolarization (getting ready to contract)
Cardiopulmonary risk factors
sedentary lifestyle, smoking, high BMI, diet high saturated fat, heroin abuse
S1 (lub)
closure of AV valves
S2 (dub)
closure of aortic and pulmonic valves
Respiratory acidosis
low pH, high CO2, hypoventilation
Respiratory acidosis S&S
confusion, fatigue, lethargy, SOB
Respiratory acidosis interventions
improve lung function, mechanical ventilation
Respiratory alkalosis
high pH, low CO2, hyperventilation
Respiratory alkalosis S&S
dizziness, muscle spasms, irritability, nausea
Respiratory alkalosis interventions
regulate o2, reduce anxiety, rebreathing
Hypoxemia
deficient amount of oxygen in the blood
Hypoxemia S&S
dyspnea, wheezing, cyanosis, tachycardia
At risk for hypoxemia
COPD, asthma, pneumonia, heart failure, sleep apnea, COVID-19
Hypoxia
deficiency in the amount of oxygen reaching the tissues
Hypoxia S&S
restless, agitated, dizzy, confusion, cyanosis
At risk for hypoxia
those affecting the heart, lungs, and blood (COPD, emphysema or asthma)
Right-sided heart failure S&S
dependent edema, distended jugular veins, GI distress, enlarged organs, weight gain
Left-sided heart failure S&S
pulmonary congestion, tachypnea, orthopnea, cyanosis (respiratory)
Nasal cannula
low concentrations of oxygen through two prongs that rest in nostrils
When to use nasal cannula
chronic illnesses (COPD, Emphysema)
Simple mask
low concentrations of oxygen, little higher than cannula, fits over a client's nose and mouth
When to use simple mask
low blood oxygen levels (chest pain, dizziness, or minor hemorrhages)
Non-rebreather mask
higher levels of oxygen
When to use non-rebreather mask
emergency, require additional oxygen (smoke inhalation, carbon monoxide poisoning, or trauma)
Partial rebreather mask
two-way valves instead of one-way, rebreathe small amount of outside air
When to use partial rebreather mask
need extra oxygen (smoke inhalation, trauma, or carbon monoxide poisoning)
Venturi mask
regulate percentage of oxygen (only one that does this)
When to use venturi mask
risk of hypercapnia, COPD
Oral suctioning
removal of secretions from the mouth
Nasal suctioning
clearing nasal passages to improve breathing
Nasopharyngeal suctioning
removing secretions from the throat through a nasally inserted catheter
Nasotracheal suctioning
removal of secretions from the trachea through a nasally inserted catheter; sterile technique
Oropharyngeal suctioning
removing secretions from the throat through an orally inserted catheter (clean not sterile)
Productive cough
sputum
Non-effective cough
cannot clear airway
Chronic lung disease assessment findings
increased respiratory rate, fatigue, adventitious lung sounds, accessory muscle use
Never suction for an
effective cough and can clear airway
When should you suction using NTS
non effective cough
Emphysema patient looks like
tripod position, barrel chest
How blood flows through the heart
1.Right Atrium (deoxygenated blood from body)
2.Right Ventricle (pushes deoxygenated blood to lungs)
3.Left Atrium (now oxygenated blood from the lungs)
4.Left ventricle (pushes oxygenated blood to aortas, then to rest of the body)
Patients who have a problem diffusing
atelectasis, postoperative, immobile (not taking deep breaths), smokers (can develop COPD)
Structure responsible responsible for returning oxygenated blood to heart
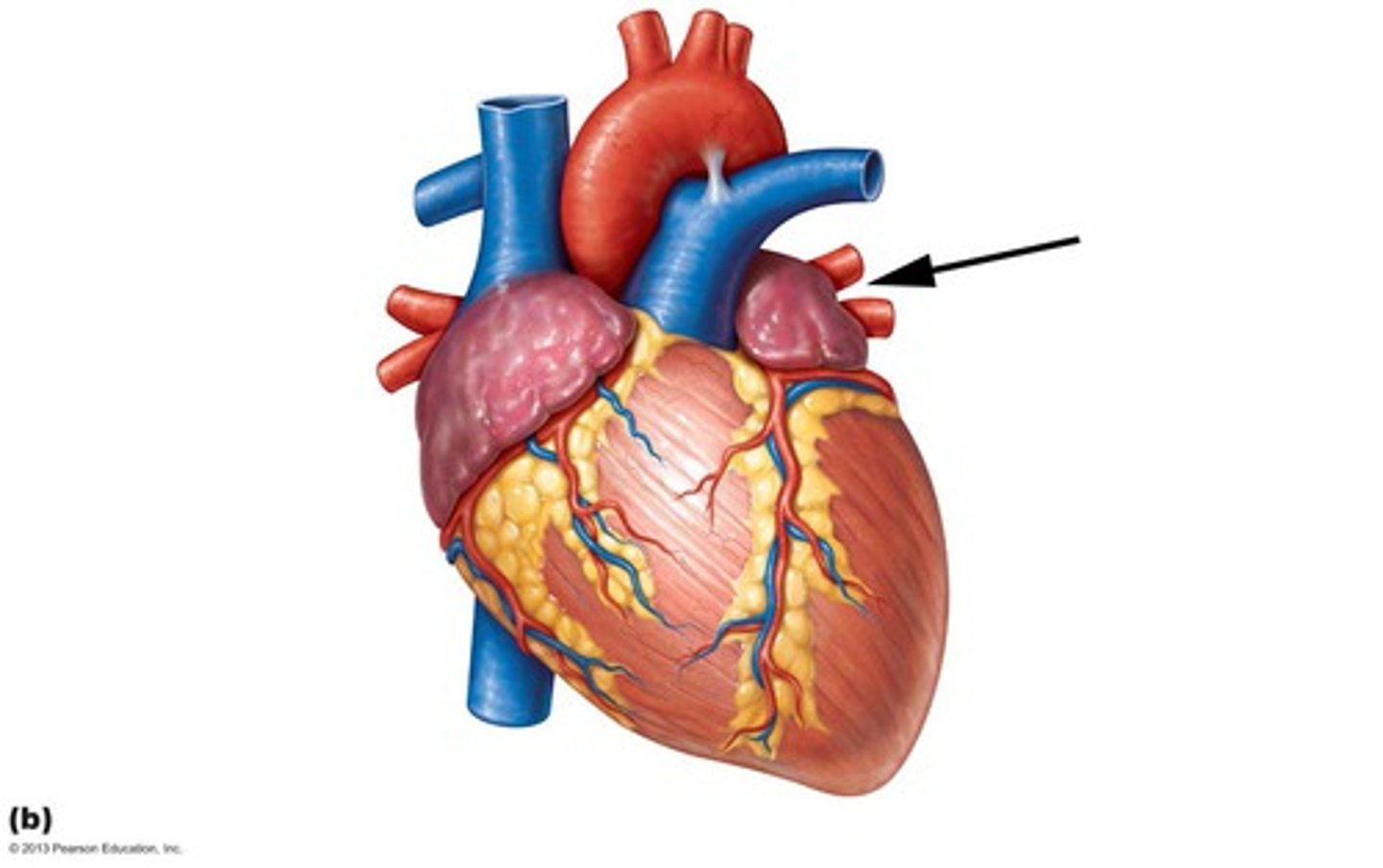
Cognitive learning
knowledge/thinking
Affective learning
emotions/feelings
Psychomotor learning
action/doing
Urine is produced in the
kidneys
Ureters
attached to each kidney, carries urinary waste to bladder
Bladder
holds urine, holds about 2 cups, once full receptors tell brain to empty
Urethra
where urine passes out body
Nephrons
functional unit of kidney, removes waste from blood, role in fluid/electrolyte balance
Production of urine factors
diet, breathing, sweating, meds
Clear urine
too much water