Ortho I: Lumbopelvic Spine Examination
1/218
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
219 Terms
Limiting factors during lumbar flexion
-PLL
-ligamentum flavum
-interspinous
-supraspinous
-intertransverse
-anterior disc compression
Limiting factors during lumbar extension
-ALL
-posterior disc compression
Fryette's laws: if the segments are in full flexion or full extension, rotation and side bending are in what direction?
if the segments are in full flexion or full extension, rotation and side bending are in the same direction
Fryette's Laws: if the motion is introduced into a segment in any plane,
if the motion is introduced into a segment in any plane, motion in the other planes is reduced
Fryette's Laws: if the segments are in neutral, rotation and side bending are in what direction?
if the segments are in neutral, rotation and side bending are opposite
Why should caution be used when applying Fryette's laws in treatment?
due to inconsistency in reported patterns of coupled motions
Form closure in the pelvis
pelvis has significant form closure because of the shape of the sacrum creates natural stability in standing and with the influence of gravity
Force closure
additional stability provided by ligaments, muscles, and fascia that crosses a joint
Sagittal plane motion at the SIJ occurs about a transverse axis at the
2nd sacral body
Nutation
sacral flexion
-sacral base moves anteriorly and inferiorly
-iliacs approximate
-ischial tubs separate
Counternutation
sacral extension
-base moves posteriorly and superiorly
-iliacs move apart
-ischial tuberosities approximate
Sacral torsions occur around the ___________ axes
oblique
Forward sacral torsion
sacral sulcus moves anteriorly and contralateral ILA moves posteriorly
-LOL or ROR
Backward sacral torsion
sacral sulcus moves posteriorly and contralateral ILA moves anteriorly
-LOR or ROL
Contractile and fascial influences on the pelvic girdle during posterior rotation - innominate
abdominals, gluteus maximus, hamstrings (esp biceps femoris)
Contractile and fascial influences on the pelvic girdle during anterior rotation - innominate
iliopsoas, rectus femoris, TFL
Contractile and fascial influences on the pelvic girdle during transverse shear
pelvic floor fascia
Contractile and fascial influences on the pelvic girdle during anterior rotation - pelvis
erector spinae, lat dorsi (via fascia) and thoracolumbar fascia
Contractile and fascial influences on the pelvic girdle during flexion - sacrum
piriformis
Contractile and fascial influences on the pelvic girdle during inferior shear - pubis
hip adductors
Contractile and fascial influences on the pelvic girdle during lateral pelvic tilt
TFL
___________ _________is necessary for effective load transfer through the pelvic girdle
joint stability
Lumbopelvic functional considerations
-lumbopelvic rhythm
-lumbopelvic mobility
-lumbar disc mechanics
How is epidemiological data useful in patient care?
clinical reasoning and using likelihood ratios
What is the difference between incidence and prevalence?
-incidence is number of new cases in a time period/population at risk
-prevalence is number of existing cases at a point in time/population at risk
Example: Lots of new cases but ending in death means there's ________ incidence but ________ prevalence
high incidence but low prevalence
__________ and ________ pain are the leading cause of global disability in years lived with disability (increasing burden from 1990 and 2005)
LBP and neck pain
Annual prevalence of occupational LBP
2-8% of workforce affected by LBP
Chronic low back pain (CLBP) has increased from
3.9% to 10.2%
Lifetime prevalence of LBP
50-80% have at least 1 episode in a lifetime
Epidemiology of LBP: estimated between ___-___% have SIJ pain
13-30% (recurrence rate? ..no studies)
Annual incidence of developing an episode of LBP is
4-93%
What is a strong predictor of future episodes of LBP?
prior episodes (recurrent episodes are common)
LBP is a multifactorial disorder predominantly _________ and ___________
occupational and psychosocial
Risk factors of LBP
1. comorbidities
2. psychological factors
3. occupational factors
4. lifestyle/social demographic
5. age
6. gender
Risk factors of LBP: comorbidities
-increased cost and disability: diabetes, RA, anxiety, psychiatric illness, and depression
-risk comorbidity prevalence highest for anxiety (depression 5th)
Risk factors of LBP: psychological
anxiety, depression, catastrophizing, kinesiophobia, and somatization
Risk factors of LBP: occupational
-heavy lifting, pushing, pulling
-physical workload
-job demands
-stressful and monotonous work
-dissatisfaction with work
Risk factors of LBP: lifestyle/social demographic
-BMI - increased risk with obesity
-smoking 47 studies reviewed; favor a causal link
-BMI and smoking
-male and African American are significant predictors for claims related LBP
-lower education
-social class
-lower income
-overindebtedness 11x increase in probability of LBP
Risk factors of LBP: age
-"wear and tear"
-DDD
-higher rates of LBP in those >65
-highest frequency of LBP sxs from 35-55 (sickness, absence, symptom duration increase with age)
Risk factors of LBP: gender
-females > males
-more than 2/3 pregnant women report LBP
-LBP during pregnancy
Prognostic factors of lumbar disc herniation: favorable factors
-absence of crossed SLR
-spinal motion in extension that does not reproduce leg pain
-large extrusion or sequestration
-relief of >50% reduction in leg pain within the first 6 weeks onset
-positive response to corticosteroid treatment
-limited psychosocial issues
-self employed
-motivated to recover and return to function
-educational level >12 years
-good fitness level
-motivated to exercise and participate in recovery
-absence of spinal stenosis
-progressive return from neurologic deficit within the first 12 weeks
Prognostic factors of lumbar disc herniation: unfavorable factors
-positive crossed SLR
-leg pain produced in spinal extension
-subligamentous contained LDH
-lack of >50% reduction in leg pain within the first 6 weeks of onset
-negative response to corticosteroid treatment
-overbearing psychosocial issues
-worker's compensation
-unmotivated to return to function
-educational level <12 years
-illiteracy
-unreasonable expectation of recovery time frames
-poorly motivated and passive in recovery process
-concomitant spinal stenosis
-progressive neurologic deficit
-cauda equina syndrome
Prognostic factors of lumbar disc herniation: neutral factors
-degree of SLR
-response to bed rest
-response to passive care
-gender
-age
-degree of neurologic deficit (except progressive deficit and cauda equina syndrome)
Prognostic factors of lumbar disc herniation: questionable factors
-actual size of LDH
-canal position of LDH
-spinal level of LDH
-multi level disc abnormalities
-LDH material
Why is differential diagnosis difficult?
-functionally independent on adjacent joints
-joint mobility is minimal; radiographs are not helpful
-poor inter rater and intra reliability for positional and mobility clinical testing
-no true "gold standard" for diagnosis
Musculoskeletal causes of LBP
any innervated structure in the lumbar spine can cause symptoms of low back and referred pain into extremities
What makes associating anatomy with symptoms so difficult?
high rate of false positive findings with imaging studies
Non musculoskeletal causes of LBP
-visceral
-neurogenic
-vasculogenic
-spondylogenic
-psychogenic
-primary/secondary cancer
Lumbopelvic exam sequencing
-patient first
-test uninvolved/less involved side/direction first
-active motions done before passive, passive before resistive
-painful/provocative testing should be done towards the end of the exam
-special orthopedic testing done after motion and strength assessments
-do not repeat testing unnecessarily
-consider positional changes of the patient
Red flag indications

Cauda equina syndrome/widespread neurologic disorder indications
-difficulty with micturition
-loss of anal sphincter tone or fecal incontinence
-saddle anesthesia about the anus, perineum or genitals
-widespread (>one nerve root) or progressive motor weakness in the legs or gait disturbance
-sensory level
Inflammatory disorders (ankylosing spondylitis and related disorders) indications
-gradual onset before age 40
-marked morning stiffness
-persisting limitation of spinal movements in all directions
-peripheral joint involvement
-iritis, skin rashes (psoriasis), colitis, urethral discharge
-family history
Lumbopelvic examination viscerogenic: cancer
-prostate, testicular, and pancreatic cancer
-metastatic lesions
Lumbopelvic examination viscerogenic: cardiac
-abdominal aortic aneurysm (AAA)
-endocarditis
Lumbopelvic examination viscerogenic: renal
kidney involvement including UTI
Lumbopelvic examination viscerogenic: GI
-ulcerative colitis
-neoplasms and obstructions
-irritable bowel syndrome and Crohn's disease
-colon cancer
Lumbopelvic examination viscerogenic: other
-spinal tuberculosis
-reiter's syndrome (reactive arthritis)
-ankylosing spondylitis
-pagets disease
Red flags with the highest positive LR for cancer
1. age ≥ 50
2. failure to improve after 1 month of therapy
3. previous history of cancer
4. unexplained weight loss (more than 4.5 kg in 6 months)
*absence of all 4 confidently R/O malignancy
Red flags that may increase the likelihood of metastatic cancer
-history of cancer
-night pain or pain at rest
-unexplained weight loss
-age > 50 or < 17
-failure to improve over the predicted time interval following treatment
Red flags that may suggest the presence of an infection within the disc or vertebra
-patient is immunosuppressed
-a prolonged fever with a temp over 100.4 F
-history of intravenous drug abuse
-history of a recent UTI, cellulitis, or pneumonia
Red flags suggesting an undiagnosed vertebral fracture
-prolonged use of corticosteriods
-mild trauma > age 50 years
-age > 70 years
-a known history of osteoporosis
-recent major trauma at any age (motor vehicle accident or a fall from greater than 5 ft
-bruising over the spine following trauma
Red flags that may indicate a dangerous abdominal aortic aneurysm
-a pulsating mass in the abdomen
-a history of atherosclerotic vascular disease
-a throbbing, pulsing back pain at rest or with recumbency
-age > 60
Is cauda equina syndrome an emergency?
Yes, surgical emergency
Cauda equina syndrome
-progressive neurological deficits
-urine retention or incontinence
-fecal incontinence
-bilateral sciatica
-global or progressive LE weakness
-numbness in saddle distribution
-sensory deficits in the feet L4, L5, S1
-ankle DF, toe extension, and ankle PF weakness
Yellow flags are predictors of
chronicity - first 6 to 8 weeks
Yellow flags
-nerve root pain or specific spinal pathology
-reported severity of pain at the acute stage
-beliefs about pain being work related
-psychological distress
-psychosocial aspects of work
-compensation
-time off work
-the longer someone is off work with back pain, the lower the probability that they will return to work
Psychosocial barriers to recovery
-belief that pain and activity are harmful
-"sickness behaviors" such as extended rest
-low or negative moods, social withdrawl
-treatment that does not fit best practice
-problems with claim and compensation
-history of back pain, time off and other claims
-problems at work, poor job satisfaction
-heavy work, unsociable hours
-overprotective family or lack of support
Other associated symptoms with lumbopelvic pain
-paresthesias
-weakness
-crepitus
-swelling
-discoloration
-PM pain
-changes with eating
-B and B changes
Non mechanical LBP
-typically not made worse with loading
-referred (pelvis/abdomen)
-neoplasm
-vascular
-other medical
Mechanical LBP
-decreased pain with rest or unloading
-pain pattern with activity, motion, load
-pain provocation with specific motion, load, positioning
-usually cyclic
-low back pain is often referred to the buttocks and thighs
-morning stiffness or pain is common
-start pain (i.e. when starting movement) is common
-there is pain on forward flexion and often also on returning to the erect position
-pain is produced or aggravated by extension, side flexion, rotation, standing, walking, sitting, and exercise in general
-pain becomes worse over the course of the day
-pain is relieved by a change of position
-pain is relieved by lying down, especially in fetal position
Risk factors for development of recurrent LBP
-history of previous episodes
-excessive mobility in the spine
-excessive mobility in other joints
Risk factors for development of chronic pain
-presence of symptoms below the knee
-psychological distress or depression
-fear of pain, movement, and re injury or low expectations of recovery
-pain of high intensity
-passive coping style
Fear avoidance beliefs questionnaire
-16 item questionnaire
-2 sub scales: physical activity and work
Reliability and internal consistency of fear avoidance belief questionnaire
ranged between moderate and substantial
__________ relationships between measures of fear and avoidance beliefs and pain/disability among patients with mechanical neck pain as compared to patients with LBP
weaker
Scoring of fear avoidance beliefs questionnaire
0-6 points/item
-work max = 42 points
-physical activity max = 24 points
*higher the score the greater degree of fear and avoidance beliefs
Lower fear avoidance belief questionnaire predict what?
better functional outcome and less LBP in chronic unilateral radiculopathy
Work FABQ and depression were significant variables in predicting what?
short term pain and disability following lumbar disc surgery
Fear avoidance beliefs in LBP <6 months resulted in what outcomes?
-greater disability, higher pain and delayed RTW
-decreasing fear avoidance beliefs results in improved outcomes
-early treatment in patients with higher fear avoidance beliefs may result in less chronicity and better outcomes, if treatment addresses fear avoidance beliefs
Indication scores of poor return to work status in FABQ with patients with acute occupational LBP
>29 in working population or >22 in non working
Indication scores of poor outcomes in patients seeking care from PCP
>14
2 separate PT clinical trials found FABQ-W cutoff >_____ better predictor of self reported disability at 6 months
>29
Subgrouping and targeting treatment (STarT back screening questionnaire)
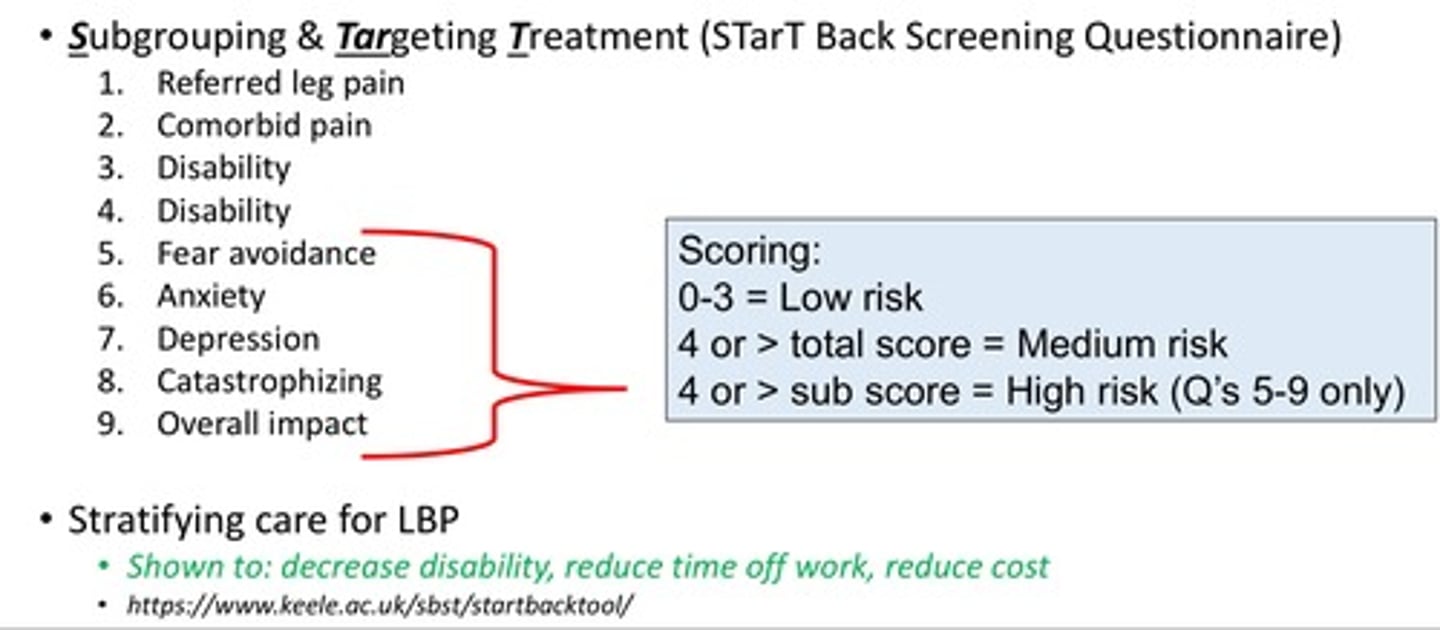
STarT back screening tool created by Keele University
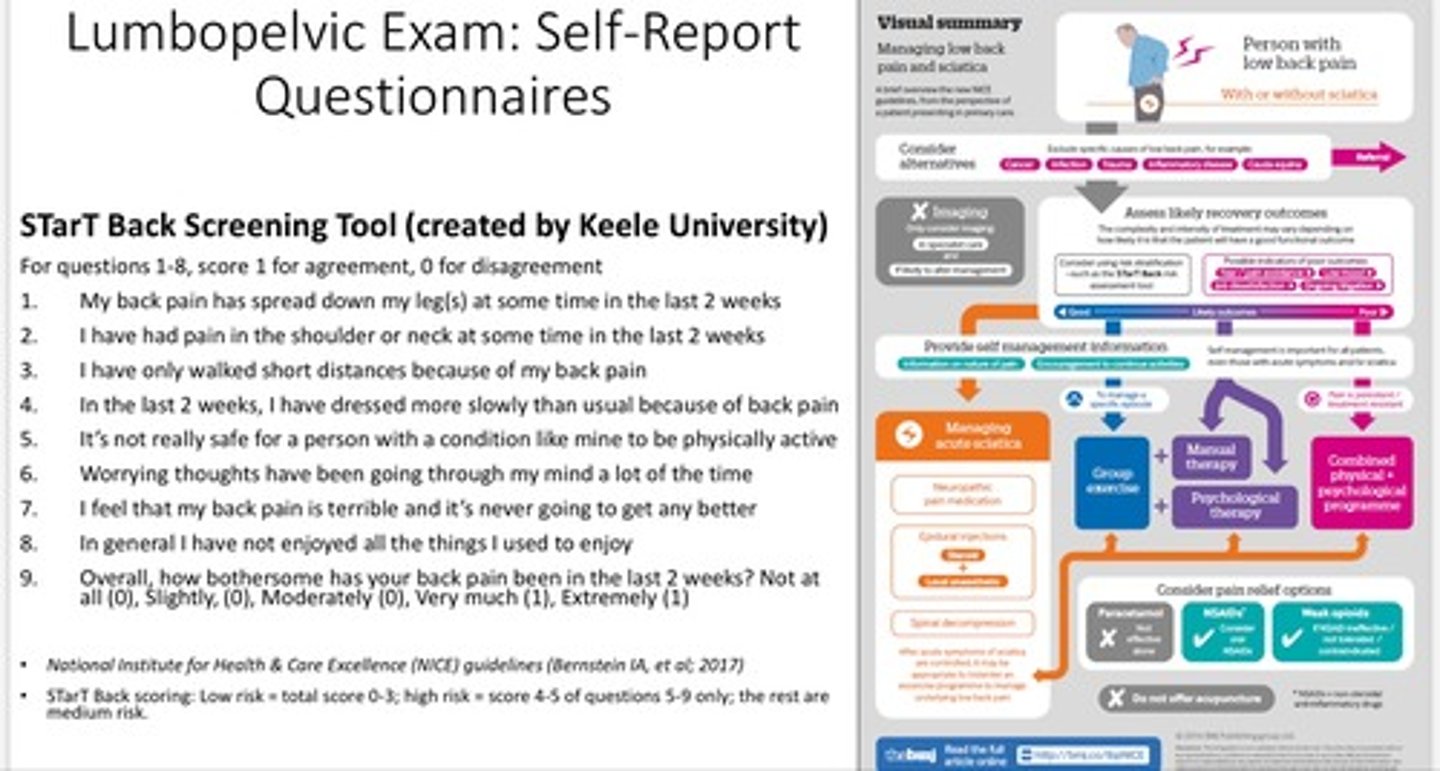
Roland Morris Low back pain and disability questionnaire
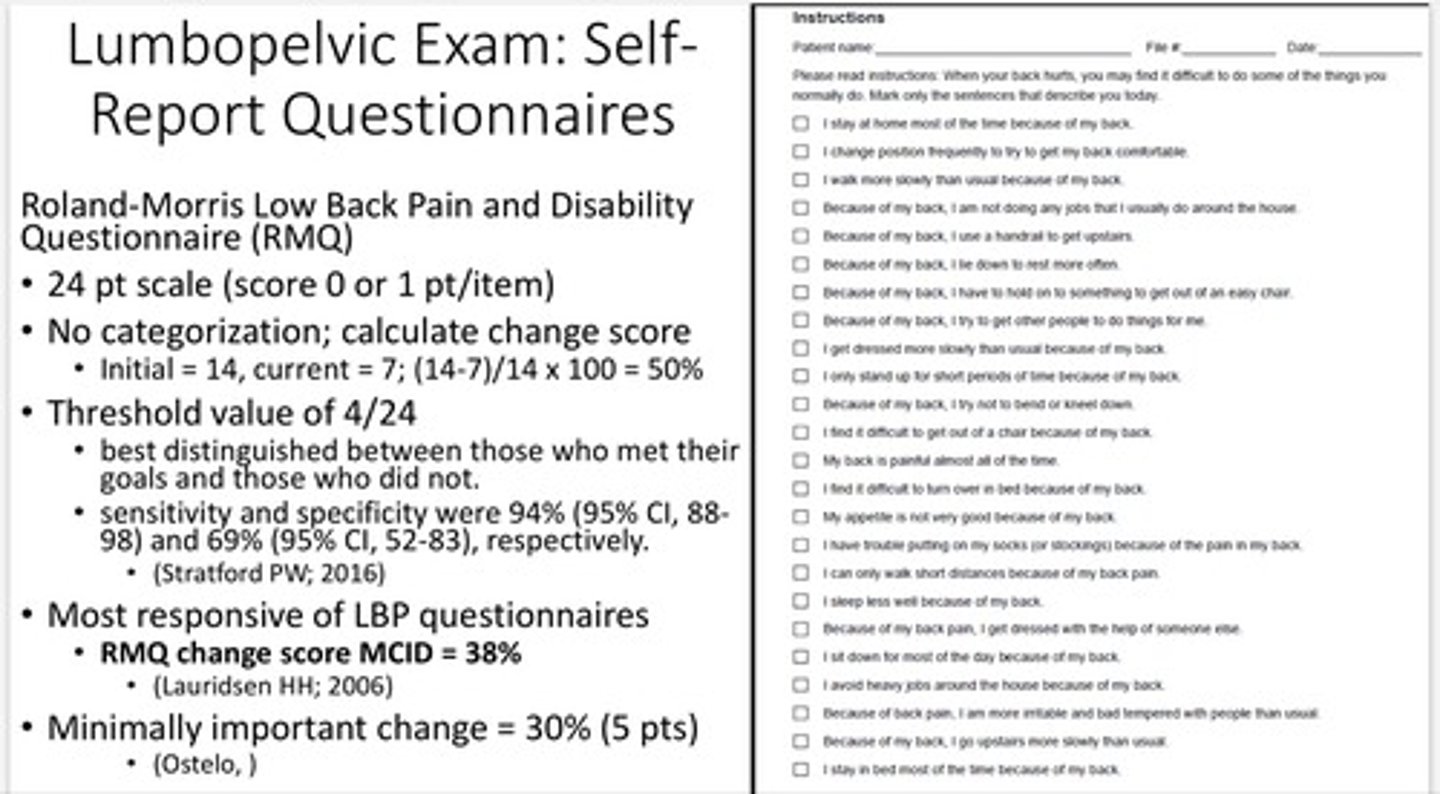
Modified Oswestry Low Back Pain Disability Questionnaire
10 sections:
1. pain intensity
2. personal care
3. lifting
4. walking
5. sitting
6. standing
7. sleeping
8. social life
9. traveling
10. employment/homemaking
scored 0-5 pts; total 50 pts

Clinical prediction tool for prediction of poor 2 year outcome in persistent LBP
1. (+) feeling everything is an effort
2. (+) difficulty getting breath
3. (+) hot/cold spells
4. (+) numbness/tingling in parts of body
5. (+) pain in heart/chest
Overpressure rules: If patient has full painfree AROM,
apply OP at end range in standing
Overpressure rules: if patient has full AROM but is painful,
move the lumbar spine passively through the full ROM in sidelying and OP at end range to assess effect of motion on pain
Overpressure rules: if patient does not have full AROM,
move the lumbar spine passively and find if there is a difference in quantity of motion and pain; check end feel with OP
Neurodynamic tests
1. passive neck flexion
2. slump test
3. straight leg raise
4. crossed straight leg raise
5. prone knee bend
Special tests lumbar stability: prone instability test
-test is positive if pain is present in first part but subsides in second part
-has been used for CPR for lumbar instability: <40, (+) PIT, aberrant flexion AROM, ("instability catch"), SLR > 91 degree; if >2 present = (+) LR 4.0
Special tests lumbar stability: stork standing test is positive for
(+) for pars interarticularis defect
Special tests for SIJ/innominate dysfunction
-upslip/downslip
-ant/post rotations
-forward torsions
-backward torsions
-flexed/extended sacrum
Gillet test technique
-palpate inferior PSIS with one thumb and S2 with the other thumb
-patient actively flexes ipsilateral hip greater than 90 degrees
Gillet test is positive when
no inferior movement of thumb on PSIS
Alternate gillet test technique
-palpate the innominate bone, PSIS, and sacrum by placing the R thumb directly on the R PSIS with the rest of the R hand contacting the R innominate bone; palpates the S2 spinous process with the L thumb
-patient actively flexes the contralateral hip into 90 degrees of hip flexion and 90 degrees of knee flexion
Alternate gillet test is positive when? and negative when?
(+) when R PSIS moves cephalad; (-) if it remains unchanged
Standing forward flexion test technique
-patient standing. examiner palpates inferior PSIS with one thumb and S2 with the other thumb
-patient actively forward flexes