Ultrasonography and image viewing techniques
1/209
Earn XP
Description and Tags
Includes Week 3 of CAR radiographic faults, echocardiology etc.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
210 Terms
What is ultrasound
longitudinal pressure waves that produce compressions and rarefactions of ‘particles’
how can the pressure waves be represented
as sinusoidal waves
what is a)wavelength, b)frequency and c)velocity
a)shortest distance b/w 2 points that are in phase (l)
b)the number of waves that would pass a given point in 1 second (f)
c) l x f
what are common diagnostic frequencies and what’s the max human fq that we can hear?
3,5,7 and 10 MHz up to 18MHz
humans can hear up to 20,000Hz
how are images generated with ultrasound (general)
generated based on returning echos reflected at tissue boundaries
What do we use ultrasound for in veterinary medicine?
imaging soft tissue structures
guiding certain types of tissue sampling (biopsy)
view blood flow in circulation (Doppler flow colour)
what’s one limitation of ultrasound use in veterinary medicine
in larger animals some structures are too deep for the wave to reach and return with enough energy to form an image.
how can we adapt ultrasonography for large animals
In cows to view their ovaries, we use a rectal transducer and observe the ovaries directly from above through the rectal wall
What are the general principles of ultrasound imaging
an ultrasound transducer/probe and coupling transmission gel is applied to the surface
transducer emits ultrasound and acts as a receiver for incoming echoes
echoes create an image, depending on strength, time of return and direction of return
Image is an aggregate of multiple echoes and is updated many times per second
Images can be paused/frozen, labelled, measured, saved as stills or short loops of moving image.
How is ultrasound generated
Transducer has ‘piezoelectric’ ceramic crystals which deform and vibrate when electrical signal is applied, emitting ultrasound
To generate an image the transducer generates an electrical signal proportional to the strength of the returning echo
approx 1% emit, 99% receive
How is an image created
Amplitude of the returning echo sets the whiteness on the screen (higher = whiter)
Time taken for echo to return sets the position on the screen
Distance = (time taken for echo to return x assumed speed through tissue) / 2
Multiple lines of sound are collected to create a cross-sectional image
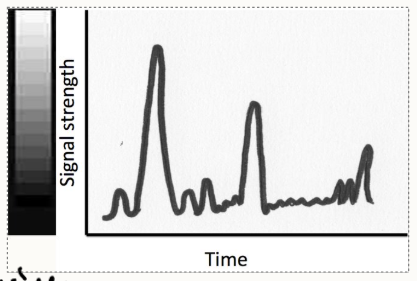
How does the machine convert amplitude into grey-scale?
loudness or amplitude of returning echoes are displayed on the screen with increasing signal strength depicted as whiter.
Grey scale is used for diagnostic interpretation.
What happens to ultrasound in tissues (4 things)
When sound strikes a boundary b/w two tissues of different acoustic impedance:
Transmitted beam = sound continues unaffected
Reflected beam = sound is reflected the way it came through
Refracted beam = sound changes path, continues through the tissue in a different direction
Scattered beam = happens where there are many small uneven boundaries, reflection and refraction in multiple directions
What affects the ability to generate images of deep tissues
Attenuation
When are we able to visualise within tissues when performing ultrasound
when some sound is reflected in passage through a structure
when is reflection the strongest?
at boundaries b/w different tissues especially ones that have a large difference in acoustic impedance
what is acoustic impedance related to
tissue density and speed of the sound in the tissue
what may scattered beams contribute to in an image?
artefacts or improper positioning of an organ or incorrect iconicity.
what do we need to consider with regards to orientation of the image
a thin slice of tissue image is created
orientation of the transducer is key
rotating the transducer enables movement b/w the different ‘cut face’ views.
What do we need to consider for prepping for an ultrasound?
Patient: starvation, sedation, clipping, cleaning, gel application, comfort and position
Room: dim lighting, quietness, comfort for yourself, patient and handler
why is coupling gel used?
it’s water based with similar acoustic impedance to soft tissues so the ultrasound beam can be transmitted into the body and not reflected at the air on the skin.
What types of transducer are there
usually have several different crystals mounted to permit electrical impulse and frequency variation
Types:
linear
curvilinear
phased array
Outline linear array transducers
multiple crystals arranged in a line and sequentially triggered
Advantages:
good near field resolution, parallel beams, no moving parts
Disadvantages:
large contact area, limited field of view
Common uses:
abdominal organs, muscles, joints and tendons
Outline curved array/curvilinear
multiple crystals arranged in an arc and sequentially triggered
Advantages:
good near field resolution
no moving parts
diverging beam
Disadvantages:
large contact area (less than linear)
difficult to use on the cranial abdomen (ribs) (solve by using the ones below)
HOWEVER: microcurved or microconvex transducers have a smaller footprint
common uses:
abdominal organs, pregnancy diagnosis.
outline phase array transducers
Sector (single crystal) scanner with electronic steering of crystal emission
Advantages:
small contact area
diverging beam
good resolution
Disadvantages:
reduced near field resolution
Common uses:
echocardiography, thoracic structures, abdominal organs, regions with small contact area (brain, eye, joints)
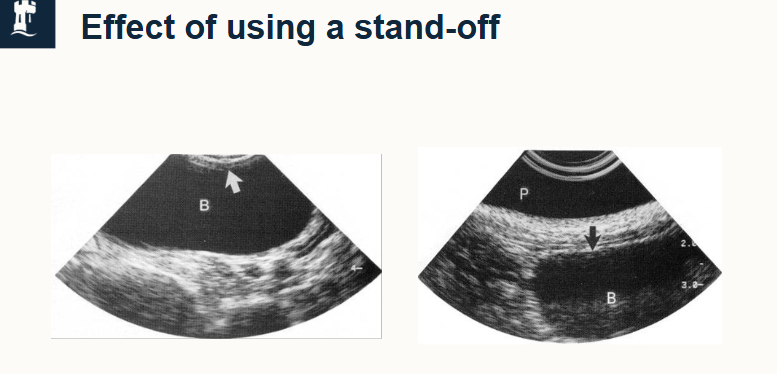
what are stand off pads
used to increase distance b/w transducer and superficial structures, moving the image down the screen to enable interpretation of near structures
adjust to uneven contours to give better contact
can be built in or pre-shaped removable pads.
Outline 4 aspects of the ultrasound machine that affect how it works?
frequency of the ultrasound wave
gain applied to the returning echo
time-gain compensation
where the ultrasound is focused
Often these have been set up initially but change as you move b/w structures
what do we mean by ‘driving skills’
learning how to adapt the settings of the ultrasound machine to each situation, not just learning numbers.
Outline transducer frequency
most operate at an optimal frequency governed by the crystal thickness
some have dual crystals that can operate at more than 1 frequency
some fire over a broad range of fq and use filters to block out parts of the range and utilise others.
How does wavelength length and fq affect the image
shorter wavelengths are absorbed and attenuated more easily
low fq have a longer wavelength and penetrate better (but poorer quality)
high fq have short wavelength and penetrate worse (but better quality of shallow structures)
outline frequency and resolution in ultrasonography
resolution = ability to see fine detail in the image
determined by wavelength (shorter = more accurate in discriminating b/w adjacent structures)
WAVELENGTH IS INVERSELY RELATED TO FQ
How do we select transducer frequence?
highest that allows adequate penetration (don’t learn exact, know a range)
if fq is too high, won’t have an image on the deep section (poor penetration)
Give 3 examples of ultrasound frequencies and what they’re used for
5MHz - abdominal in large dogs, and cardiac in med/small dogs
7.5MHz - abdominal and cardiac in small dogs and cats, pelvic and pregnancy in med/small dogs and cats
10MHz - cervical structures (salivary glands, thyroid), superficial structures (eye, skin, mammary glands) and musculoskeletal.
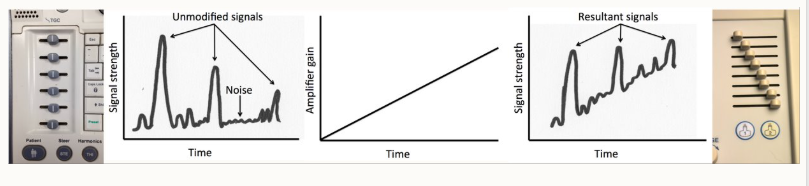
what is Gain?
The amplification applied to the returning echo - makes the overall image look whiter - overall starts at 60%
why would we use gain?
when imaging deep structures, look darker on screen because sound has to travel further so there’s a quieter returning echo.
lower energy echoes have lower amplitude so are shown as darker grey
gain must be adjusted to compensate for this - give a balanced picture
use TIME GAIN COMPENSATION settings to refine this
what is Time Gain Compensation
allows selective amplification of signals from different depth levels
initially all set to 50%
only do once the image is produced on screen.
How and why do we change the focus on an image?
narrows the beam at certain points improving resolution at the chosen depth
adjust focal zone to region of interest by selecting focus and moving the arrow to the required depth.
what does the mark/bump on the side of the transducer mean?
related to the side of the screen marked ‘M’
should be on the LEFT

How do we orientate with respect to the animal?
depends on the location of the organ
use the different planes - frontal, sagittal, transverse
How do we hold our hands when scanning
find the location of the bump
move thumb to the thumb indent, knowing where the bump is.
match the bump to the screen
Sagittal plane:
bump is cranial and thumb is left side of animal
Transverse
bump is on the right side of the animal and thumb moves to cranial
Outline the technique used for viewing images
train your eyes by viewing normal positions
use the bump, thumb position
remember you’re looking at a 2D image of a 3D structure
what 6 main terms are there and one additional thing to look out for
anechoic
hypoechoic
medium echogenicity
hyperechoic
homogenous
heterogenous
note any artefacts
what does anechoic mean
no echo produced
all sound passes through the tissue
non is reflected to the ultrasound transducer
anechoic tissue appears black on an image
examples include fluid (blood, urine, bile)
what does medium echogenicity mean?
produce a medium echo
a medium amount of sound is reflected to the transducer and a medium amount passes through
dark to light grey appearance
examples include soft tissues e.g. liver, spleen, prostate, testes
what does hypoechoic mean
produce little echo
most sound passes through
small is reflected back to the transducer
dark grey appearance
examples: high-water content tissues e.g. cartilage, muscle and renal medulla
what does hyperechoic mean
produce much echo
little sound passes through
most is reflected back to the transducer
often appear white on image
example is dense connective tissue
where else may we get full reflection?
gas and bone interface (may appear as acoustic shadow deep to structure)
what does heterogeneous and homogeneous mean
Heterogeneous (non-uniformed, mixed) = mixed/irregular pattern (common in finding diseased tissue)
Homogeneous (uniform) = similar and regular pattern throughout (most normal tissues)
define an x-ray
electromagnetic radiation used to create an image
what is a radiograph
an image on a display screen
define radiography
the art or process of making the radiographic image
includes radiation safety, radiographic equipment and radiographic technique
define radiology
the interpretation of the radiograph leading to diagnosis of disease using X-rays/radioactive material.
includes normal radiographic anatomy and appearance which changes with different diseases.
How many radiographs should we take, why and how
Minimum of 2 views perpendicular to each other
animal is 3D
images are 2D
need the two images to gain an understanding of 3D structure
called orthogonal views
what are X-rays
a form of short wavelength, high energy electromagnetic radiation
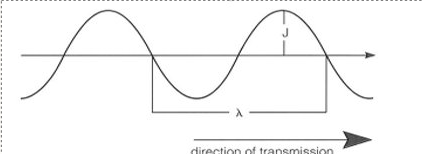
sinusoidal waveform - transverse waves
J= amplitude (height of each wave)
λ is wavelength
frequency = number of wavelengths per second
on the electromagnetic spectrum how does wavelength and energy change
Higher up the spectrum e.g. with gamma, xrays and cosmic waves, higher energy, shorter wavelength
Lower down the spectrum e.g. electric power or Tv shortwave radio, lower energy and longer wavelength
Give 9 properties of X-rays (and gamma rays)
no charge, no mass
invisible
cannot be felt
travel at speed of light
travel in a straight line
penetrate all matter (to some degree)
can cause some substances to fluoresce
expose photographic emulsion
ionise atoms
give 3 important features of X-rays to consider for medical use
high energy and short wavelength
penetrate materials and cause changes atomically
can lead to ionisation which can have potentially damaging effects on living tissue = IONISING RADIATION
outline the risk of ionising radiation on living tissue
harmful to living tissue
single large doses = SOMATIC EFFECTS which includes tissue damage seen or felt e.g. radiation burns or sickness
multiple, very small doses = GENETIC EFFECTS which includes tissue damage to cellular DNA, can cause mutations or cancer
patients are unlikely to have significant risk, however accumulation of small amounts can be a risk.
Outline radiation safety for personnel
ALARP PRINCIPLE:
As Low As Reasonably Practical
Radiation Regulations 2017, enforced by Health and Safety Executive
What are 14 safety considerations for radiation
Never expose to primary beam
U16 and pregnant/breast feeding = not in the room
min. no. people needed
always wear protective clothing
always use vertical beam
only manually restrain in exceptional circumstances
monitor radiation for staff
minimal time for exposure as possible
use lead screens
control from outside the area if possible
lead clothing
wear gloves
cassette holder
x-ray machine holder?
what are dosimeters
a health requirement to track individual ionising radiation exposure IN ADDITION to other sensible practices
site specific
stored outside radiography room
worn on the front of the body, around the torse and clipped to clothing
under leaded PPE too
sent for readings every 1-3 months (for development and interpretation)
how are x rays produced?
Cathode in an X-ray tube generates a stream of electrons from a coiled tungsten wire filament when current passes through
cathode is a cup shape to focus stream
number of electrons generated is determined by mA (miliamperes) and exposure time
electrons hit and interact with atoms w/in target area of tungsten anode which releases X-rays
potential difference is applied across tube, accelerating electrons towards +vely charged anode
electron energy is determined by kV (kilovolts, sometimes kVp = kilovolt peak)
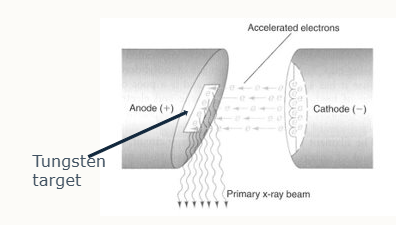
why is tungsten metal used in X-ray production
high melting point
high atomic number
heat is produced during the process
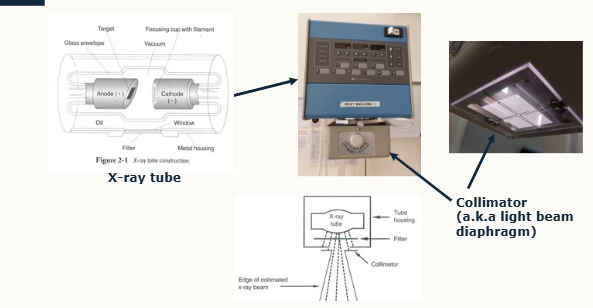
How is an X-ray tube constructed
produced in tube head of machine due to interactions b/w anode and cathode
whole arrangement is kept in evacuated glass envelope surrounded by oil to absorb heat produced
placed in a metal casing
absorbs x-rays with a window to allow them to emerge in only one direction
beam passes through a collimator that has lead plates to adjust size of the x-ray
light shines through the gap to indicate extent of x-ray beam
collimator is referred to as light beam diaphragm
what are the 2 properties of X-ray beam
quality = penetrating power of beam (comes from energy)
Intensity = amount of radiation in the beam (comes from number of xrays)
first x-ray beam = primary beam
what is the effect of increasing kilovoltage
increase kV
increased electron acceleration
increased energy of electrons
grater number of x-rays produced
increased energy = increased penetrating power
what is the effect of mA
governs the current applied to the filament and is applied for a specific time = sec
increased mA
increased tube current
increased number of electrons
GREATER NUMBER OF X-RAYS ARE PRODUCED
energy remains unchanged. (same penetrating power)
what is the effect of exposure time?
if time over which current is implied INCREASES, more x-rays produced, energy remains unchanged
mA x sec = mAs
how can we increase mAs?
increase time
increase mA
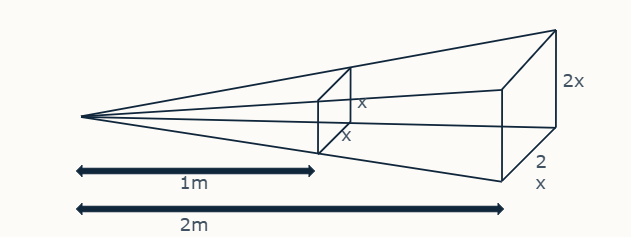
what is source to image-receptor distance (SID)
closer the x-ray tube to the image receptor, the more ‘concentrated’ the x-ray beam (vice versa)
exposure varies according to inverse square law
e.g.
double source to image receptor distance - ¼ amount of radiation lands on given area of image receptor.
How did we use to form radiographic images vs now?
Historically: recorded on photographic film, chemically processed
Now: digital image - recorded on digital detector, electronically processed and displayed on a computer screen.
examples: computer radiography and direct (digital) radiography
uses substantially less energy
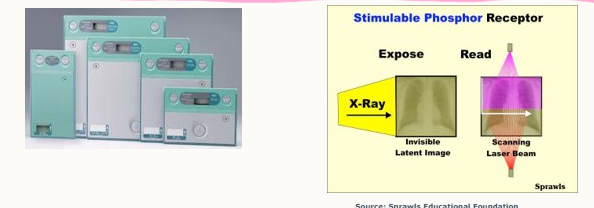
what is computed radiology (CR)?
phosphor plate held in cassette
X-rays strike plate, electrons are energised and form an ‘invisible’, latent image.
cassette placed into reader, plate removed
scanned by a laser, trapped energy is released as visible light
photomultiplier detects light, converts it to an electrical signal
processed by a computer
image is produced and can be manipulated post processing
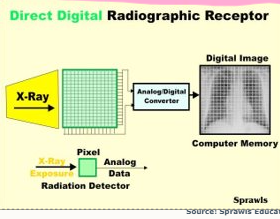
what is Direct Digital Radiography (DR)
x-rays stimulate sensor panel, sends electrical signals direct to computer
image manipulated and stored as before
sensor panel separate/mounted in table
how are images stored and distributed?
stored to enable:
easy searching of archived images
back-up of digital files
PACS (picture archiving and communication system) often used
consider back ups (cloud/physical)
be able to share them with other professionals e.g. for referrals.
what are 3 ways the x-ray interacts with the patient
Absorbed completely
pass through unaffected
interact with atoms and scatter
How is a radiographic image produced
animal is between x-ray tube and image receptor
low energy rays absorbed by patient
differential absorption by tissues/structures produces a radiation pattern from the patient, used to create the image
is it possible to have a thick, low-density structure showing as whiter than a thin high-density structure
YES
e.g. thick area of fat vs thin area of bone
what is meant by radiographic density
ability of tissues to absorb radiation
outline the different radiographic tissue types
5 tissues with relative radiographic densities
air = lowest value, shows as radiolucency
fat is next
water, soft tissue/fluid
bone shows as radiopaque
metal is bright white
note:
all fluid shows same opacity so can’t distinguish type of fluid, same as soft tissue
why do different tissues have different radiographic densities?
atoms get closer/further apart
interact differently with x-rays
outline what scatter is
low energy x-rays emitted in random directions as it bounces off atoms
increases as volume of irradiated tissue increases
why is scatter a problem?
can fall onto image receptor
causes blackening/fogging that’s unrelated to tissue pattern
reduces image quality
increases radiation dose to personnel outside primary beam = health risk
how can we limit impact of scatter?
use a GRID for tissue thicker than 10cm
collimate beam to minimum size necessary
reduce kV
ensure personnel are outside room at exposure
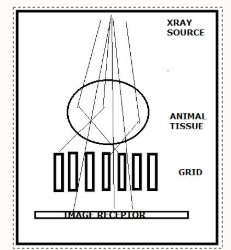
how does a grid work?
series of lead foil strips in a grid pattern
separated by radiolucent spacers
placed between patient and image receptor when tissue depth >10cm
multidirectional scattered radiation is absorbed by lead strips
only radiation in parallel with transmitted beam produces the image
image isn’t affected
what are some practical considerations for using a grid?
exposure needs to be slightly higher (some of the radiation is absorbed by grid)
care is needed to time when exposure is taken with respiratory pauses (blur more likely when animal breathes, increased mAs)
faint grid lines are visible if stationary grid is used
how can we prevent an image having faint grid lines?
bucky tray is used
placed below the table
grid will oscillate slightly at exposure
therefore grid lines blur slightly and aren’t visible on final image
doesn’t give moment blur to patient image as image receptor stays still.
how do we take a good radiograph?
depicts accurate portrayal of structures
enables easy perception, sharp shadows, wide shades of grey
no misleading artefacts
no unnecessary risks to patient or personnel
was taken using a standardised technique for consistent results
take attention to detail and care in radiographic technique
what is a pneumonic for radiograph technique?
PINK CAMELS COLLECT EXTRA LARGE APPLES
Positioning
Centring
Collimation
Exposure
Labelling
Artefacts
choose correct equipment before this
process and store the image
when may blurring occur and how can we overcome this?
if the animal moves when exposure is taken:
involuntary movement e.g. breathing
voluntary movement e.g. limbs, trying to get off table
overcome?
sedation with positioning aids e.g. sandbags (NEVER USE TIES if awake/lightly sedated)
GA - then use ties as well as sandbags
time the exposure to minimise impact of breathing
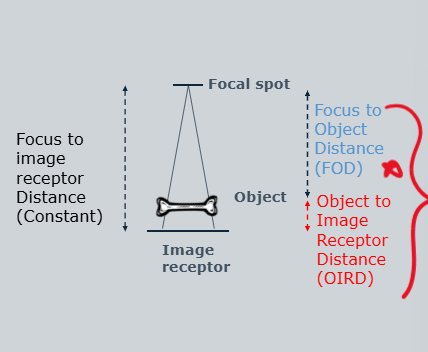
what do we need to consider about magnification during positioning for a radiograph
x-ray beam diverges with distance from tube
position part of interest as close to receptor as possible - clear and accurate image
to minimise magnification:
minimal OIRD (object to image receptor distance)
maximal FOD (focus to object distance)
What do we need to consider about geometric distortion for positioning during a radiograph
position accurately with part of interest parallel to image-receptor
centring point in the middle of cassette and area of interest
what will happen if an object is not parallel to beam/in the centre of the beam for a radiograph?
distortion
structures may appear elongated
may appear foreshortened
shapes won’t be accurate
superimposition
what do we need to consider for rotation for a radiograph
avoid axial rotation of part of interest
ensures accurate portrayal of part
makes positioning for limb views hard
can use foam blocks for example.
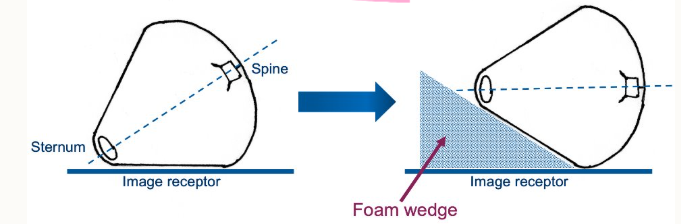
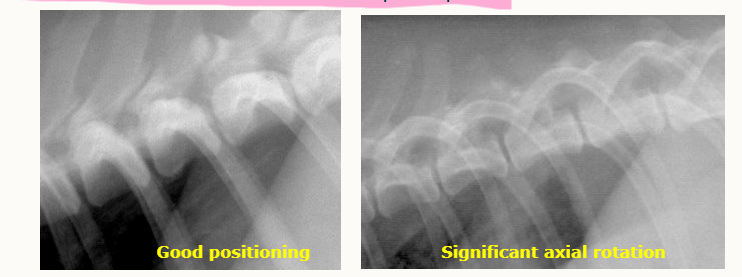
how can we assess axial rotation in lateral thoracic views?
caudodorsal rib heads should be superimposed
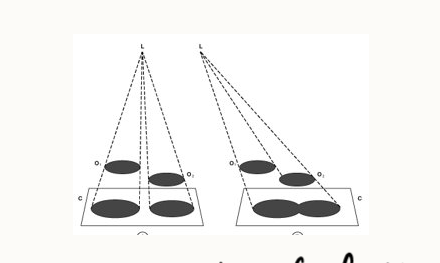
how do we correctly centre?
centre primary beam over area of interest
especially important in large animal limbs, all joints and spines
relative position may shift if not central
outline collimation
scattered radiation contributes to general image opacity and increases radiation hazard
collimation:
reduces production of scattered radiation
beam is collimated to minimize size necessary to include only area of interest
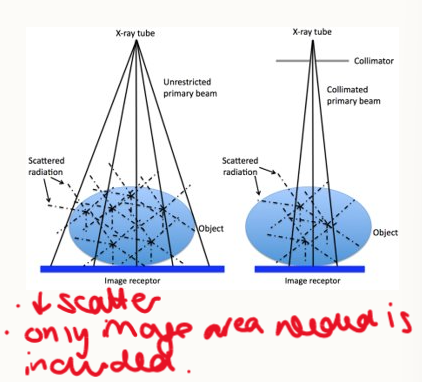
why is collimation important in radiography?
important for appropriate image processing
collimate closely but include area of interest
give examples of how much of the surrounding tissue should be included in radiographs
Joints: include 1/3 of adjacent associated bone
long bones: whole bone, adjacent joints
abdomen OR thorax, not both
when evaluating images: describe how closely it’s been collimated to the area of interest
what are some important concepts for exposure factors in radiography
need a wide range of well differentiated shades of grey
need to balance kV and mAs:
enough penetration with sufficient x-rays for a good image to form
optimum difference b/w different tissues (contrast)
ensure different structures can be viewed.
use exposure factors for consistent results
how does kV affect image
increasing = greater number of x-rays produced and increased energy, therefore increased penetrating power
If
a) increase kV = increase overall amount of radiation emerging from patient (may lead to over exposure), reduces contrast
b) decreasing kV = decreases exposure and increases difference. Energy is reduced therefore absorption is increased = increased contrast