PBI380-final exam objectives
1/26
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
27 Terms
Describe the mechanisms involved in the synthesis and release of 5-HT, and the processes involved in terminating 5-HT signalling
Step 1 (making 5-HT): tryptophan (from turkey, egg, bananas) –> tryptophan hydroxylase (enzyme 1) turns tryptophan into 5-HTP –> AADC (enzyme 2) turns 5-HTP into 5-HT (FINAL PRODUCT ASF)
Step 2 (releasing 5-HT): 5-HT stored in vesicles (little bags in neurons)–> brain says “need 5-HT” & vesicles move to edge of neuron to dump 5-HT into synapse
Step 3 (doing it’s job): once in synapse, 5-HT floats around & binds to 5-HT receptors on post-synaptic neuron, this sends a message
Step 4 (stopping signal): 2 ways
Reuptake: SERT (like special vacuum cleaner) sucks 5-HT back into neuron so it can be reused
Breakdown: some 5-HT gets destroyed by an enzyme called MAO (monoamine oxidase)
Recognize the receptor types that bind 5-HT
Think of them like clubs!
5-HT1 (chill clubs): calming and migraine related
5-HT1A: anti-anxiety, helps mood
5-HT1B & 5-HT1D: involved in blood vessels, especially in migraines
5-HT2 (hype crew): party drugs, heart risks, & hunger control
5-HT2A: trippy one, involved in hallucinations (LSD, shrooms mess with this one)
5-HT2B: mostly heart, can be bad if overstimulated
5-HT2C: helps control appetite
5-HT3 (nausea boss): no subtypes; mostly in gut, controlling nausea
5-HT4 (gut crew): no major subtypes, helps digestion and GI movement
5-HT5 (mystery receptor): sleep and brain stuff
5-HT5A: only confirmed subtype, seems to help with sleep & learning (we don’t fully understand in yet)
5-HT6 (memory booster): almost entirely in brain; seems to help with memory, learning, and maybe mood regulation
5-HT7 (mood & body clock regulator): found in brain, blood vessels, and GI tract; seems to help regulate mood, body temp, and sleep-wake cycles; blocking it might help with depression & sleep disorders
Give examples of behaviours that are affected by 5-HT signalling
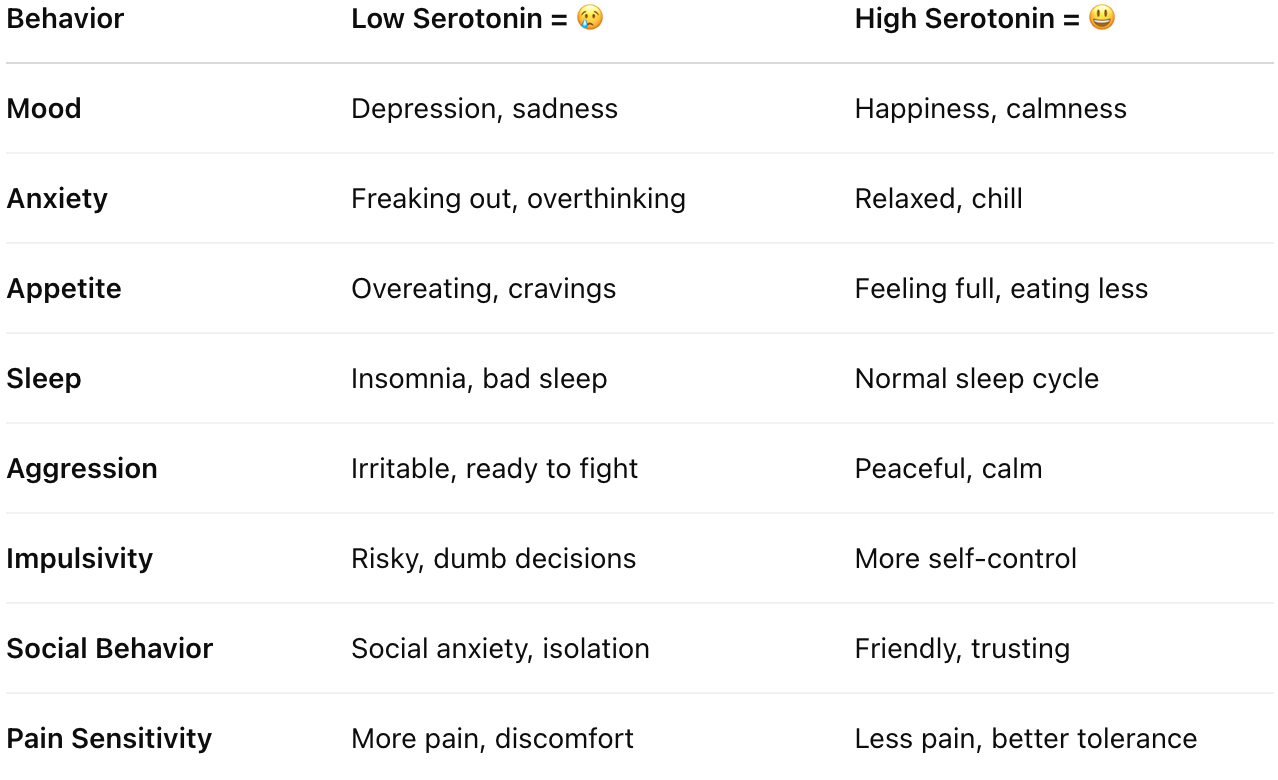
Give examples of drugs that enhance the activity of 5-HT at the synapse
Antidepressants: increase serotonin in brain to help with anxiety and depression
SSRIs (selective serotonin reuptake inhibitors): block 5-HT from being sucked back up, so it stays in the synapse (e.g. Prozac, Zoloft, Lexapro)
SNRIs (serotonin-norepinephrine reuptake inhibitors): like SSRIs but also boost norepinephrine (Effexor, Cymbalta)
MAOIs (monoamine oxidase inhibitors): stop serotonin from getting broken down (Nardil, Parnate)
Psychedelics: over-activate serotonin receptors, especially 5-HT2A, leading to hallucinations:
LSD (acid), Psilocybin (shrooms), DMT, Mescaline: all mess with 5-HT2A causing visual & sensory distortions
Like serotonin fireworks: too much 5-HT activity = trippy thoughts
MDMA: dumps a TON of serotonin into the synapse all at once, making you feel euphoric & social
Ecstasy, Molly: serotonin on steroids; super happy, super loving – until you crash
Give examples of drugs that interfere with the activity of 5-HT at the synapse
Antipsychotics: block 5-HT2A receptors to help with schizophrenia & mood disorders
5-HT ‘mute buttons’: less activity = fewer hallucinations (e.g: Risperdal, Seroquel, Clozaril)
Migraine Meds
Target 5-HT to stop headaches; 5-HT ‘on switches’ for pain relief (e.g: Sumatriptan, Rizatriptan)
Triptans activate certain receptors to shrink blood vessels & stop migraines
Anti-nausea drugs: block serotonin to stop vomiting
Ondansetron (Zofran) blocks 5-HT3 receptors to prevent nausea (especially from chemo or surgery)
5-HT ‘off switch’ for puking
Summarize the mechanisms of action of first-generation antidepressants
MAOIs - Serotonin Protectors:
MAO breaks down serotonin, dopamine, norepinephrine, but MAOIs stop this from happening (more NTs stay in the brain); more 5-HT = better mood
Downside: can interact badly with certain foods (cheese, wine, cured meats)
e.g: Nardil, Parnate
TCAs (Tricyclic Antidepressants) - Reuptake Blockers:
TCA blocks serotonin & norepinephrine reuptake, more stays in synapse; more NTs = betters mood
Downside: side effects (drowsiness, weight gain, heart risks)
e.g. Amitriptyline, Imipramine
Summarize the mechanisms of action of second-generation antidepressants
SSRIs - Serotonin Hoarders 2.0
`Only block 5-HT reuptake; more serotonin stays in the synapse = better mood; most commonly perscribed
Advantage: fewer side effects than MAOIs or TCAs
e.g: Prozac, Zoloft, Lexapro
SNRIs - SSRIs with extra powers
Block reuptake of both serotonin & norepinephrine; boost in mood & energy (good for depression & fatigue)
Advantage: more energizing than SSRIs, good for people with both depression & low energy
e.g: Effexor, Cymbalta
Describe the synthesis and release of acetylcholine (ACh), and how its signal is terminated at the synapse
Step 1 (making ACh): Choline (from fish, eggs, peanuts) + Acetyl-CoA (made in neurons) –> Choline Acetyltransferase (ChAT, enzyme 1) sticks them together –> Acetylcholine (ACh, aka FINAL PRODUCT)
Step 2 (releasing ACh): VAChT (vesicular ACh transporter) loads ACh into vesicles to be transported & released at synapse, vesimacol blocks VAChT
Step 3 (doing its job): ACh floats around in the synapse & binds to ACh receptors on the post-synaptic neuron –> sends message for movement, memory, or whatever ACh is controlling
Step 4 (stopping signal #nomoreAChdafuq): only 1 way (ACh doesn’t get reuptaken); breakdown – AChE (enzyme) DESTROYS ACh in the synapse –> Chloine gets taken back up into the neuron to make new ACh later
Give examples of where in the brain and body ACh is found
In the brain:
Basal forebrain (memory & attention HQ)
ACh helps you focus, learn, & remember stuff
Damage linked to Alzheimer’s disease (memory loss)
Pons & Midbrain (sleep control)
ACh helps you stay awake & controls REM sleep (dreaming)
Low ACh = might sturggle with sleep problems
In the body:
Neuromuscular Junction (tells muscles to move)
ACh released onto muscles to make them contract
No ACh? PARALYSIS!
Parasympathetic Nervous System (rest & digest)
ACh slows heart rate, increases digestion, chills you out
messed up ACh = body goes into overdrive
Sympathetic Nervous System (fight or flight)
ACh helps send signals before adrenaline kicks in
messed up ACh = messed-up stress response
Recognize the receptor types that bind ACh
Nicotinic Receptors (nAChRs) - Fast Ones
in muscles, brain, ANS
instant activation with ACh binds to nicotinic receptors; found in places where quick reactions are needed (muscle movement, brain signals linked to focus & addiction)
e.g: Nictotine (overactivates receptors), Curare (blocks receptors = paralysis)
Muscarinic Receptors (mAChRs) - Slow & Steady Ones
in brain, heart, lungs, digestive system
slower, long-lasting effects (more fine-tuned control)
heart: ACh binds –> heart rate slows (relax mode AF)
lungs: ACh binds –> airways tighten (too much ACh = breathing issues)
brain: ACh binds–> memory & attention (damaged in Alzheimer’s)
e.g: Atropine (blocks muscarinic receptors–speeds up heart rate, dilates pupils), Poisonous Mushrooms (overactivate muscarinic receptors–sweating, diarrhea, slowed heart rate, death)
Give examples of behaviours that are affected by ACh signalling
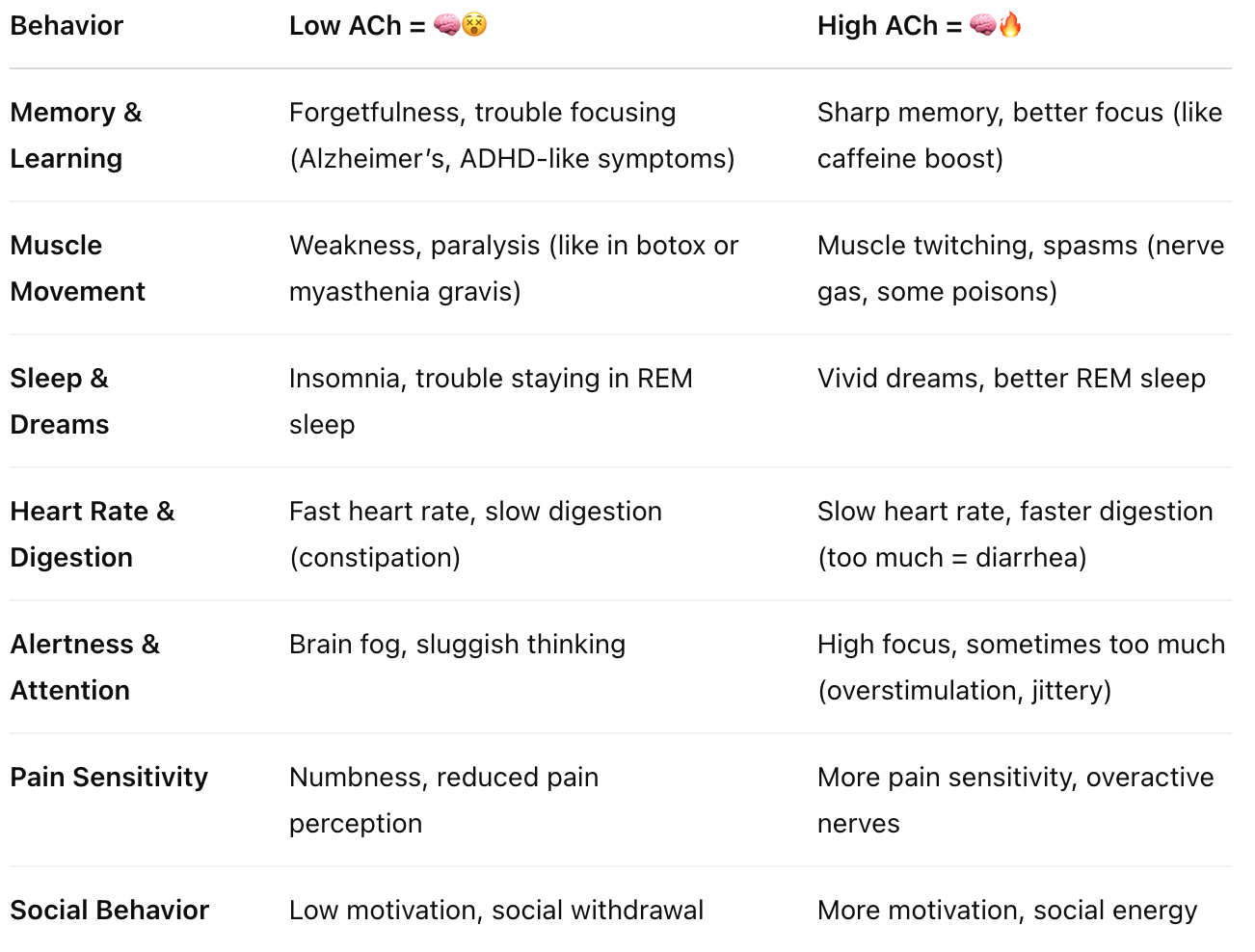
Give examples of drugs that enhance the activity of ACh at the synapse
Cholinesterase Inhibitors: block AChE (enzyme), ACh stays in synapse longer
Donepezil, Rivastigmine, Galantamine –> boost memory in Alzheimer’s disease
Physostigmine, Neostigmine –> help muscle strength in myasthenia gravi (disorder that causes muscle weakness)
Nicotinic Receptor Agonists: activate nicotinic ACh receptors –> brain & body stimulation
Nicotine (cigs, vapes, patches) –> increases alertness & focus, but also highly addictive
Muscarinic Receptors Agonists: activate muscarinic ACh receptors –> affect organs like heart eyes, & saliva glands
Pilocarpine –> increases saliva & tears (used for dry mouth & glaucoma)
Toxic Overload: too much ACh = muscle spams, seizures, death
Organophosphates (pesticides, nerve gas) –> permanently block AChE, leading to uncontrolled ACh buildup –> paralysis & death (used in chemical warfare & insect killers)
Give examples of drugs that interfere with the activity of ACh at the synapse
Cholinergic Antagonists: block ACh receptors –> less ACh activity
Atropine –> blocks muscarinic ACH receptors –> speeds up heart rate, dilates pupils (used for eye exams & treating slow heart rate)
Scopolamine –> blocks muscarinic ACh receptors in brain –> reduced nausea & motion sickness (also causes memory issues at high doses)
Neuromuscular Blockers: stop ACh from activating muscles –> paralysis
Curare –> blocks nicotinic ACh receptors at muscles –> paralysis (used poison dart & surgery anesthesia)
Botulinum Toxin (Botox) –> prevents ACh release at muscles –> muscles can’t contract = paralysis & wrinkle reduction (used to treat migraines & muscles spasms)
Acetylcholinesterase Reactivators: reverse too much AChE blockage
Pralidoxime (2-PAM) –> reactivates AChE after nerve gas poisoning –> restores normal muscle function
Toxic Overload: blocking too much ACh = dry, slow, confused
Anticholinergic Toxicity (too much ACh blockage) –> dry mouth, blurry vision, confusion, fast heart rate, trouble urinating (can be caused by overdose on antihistamines, antidepressants, or atropine)
Summarize the synthesis pathways of glutamate
Glutamine Route (Main Way!)
Step 1: glutamine (precursor) is floating around in the brian
Step 2: glutaminase (enzyme) converts glutamine to glutamate (FINAL PRODUCT ASF)
Krebs Cycle Route (Backup Plan!)
Step 1: cells break down glucose –> a-ketoglutarate (part of Krebs cycle, energy production)
Step 2: glutamate dehydrogenase or transaminase (enzymes) convert a-ketoglutarate –> glutamate (FINAL PRODUCT ASF)
Releasing glutamate
VGLUT (vesicular glutamate transporters) load glutamate into vesicles to be transported & released at the synapse, rose bengal & similar dyes can block VGLUT but no major drug used clinically to target it
Describe how glutamate signals are terminated at the synapse
Step 1: Reuptake (Vacuum Mode)
EAATs (excitatory amino acid transporters) act like tiny vacuum cleaners & suck glutamate out of the synapse so it stops activating neurons
important because if glutamate stays in synapse too long –> neurons overfire = bad (toxic, seizures, cell death)
Step 2: Glutamate –> Glutamine (Safe Mode)
glial cells (astrocytes) grab the extra glutamate & convert it into glutamine; glutamine synthetase (enzyme) does that job; glutamine is harmless & gets sent back into neurons to be reused
important because glutamine can be stored & safely turned back into glutamate when needed (#recycling)
Step 3: Breakdown (Destroy Mode)
in somes cases, glutamate can also be broken down into other molecules; reuptake & conversion to glutamine is the main way the brain prevents glutamate overload
important because it helps fine-tune levels despite being less common
Recognize receptor subtypes for glutamate
Ionotropic Receptors = FAST & DIRECT
act like doors; open when glutamate binds–> ions rush in–> neuron gets excited
like light switches (on/off instantly)
too much activation = brain overload –> seizures, cell death
e.g: NMDA (lets Ca2+ in; memory, learning, brain plasticity), AMPA (lets Na+ in; super-fast signlas, reflexes, movement); Kainate (letsNa+ & K+; less common, still speeds things up)
Metabotropic Receptors = SLOW & LONG-LASTING
wokr through G-proteins & second messengers –> gradual effects on neuron activity
like dimmer switches (gradually turn up/down activity)
too little activation – brain = slow/sleepy
group I (excitatory): activates cells; increases firing; matters for learning, memory, emotions
groups II & III (inhibitory): lowers neuron activity; regulates mood, anxiety, motor control
Give examples of behaviours influenced by glutamate release
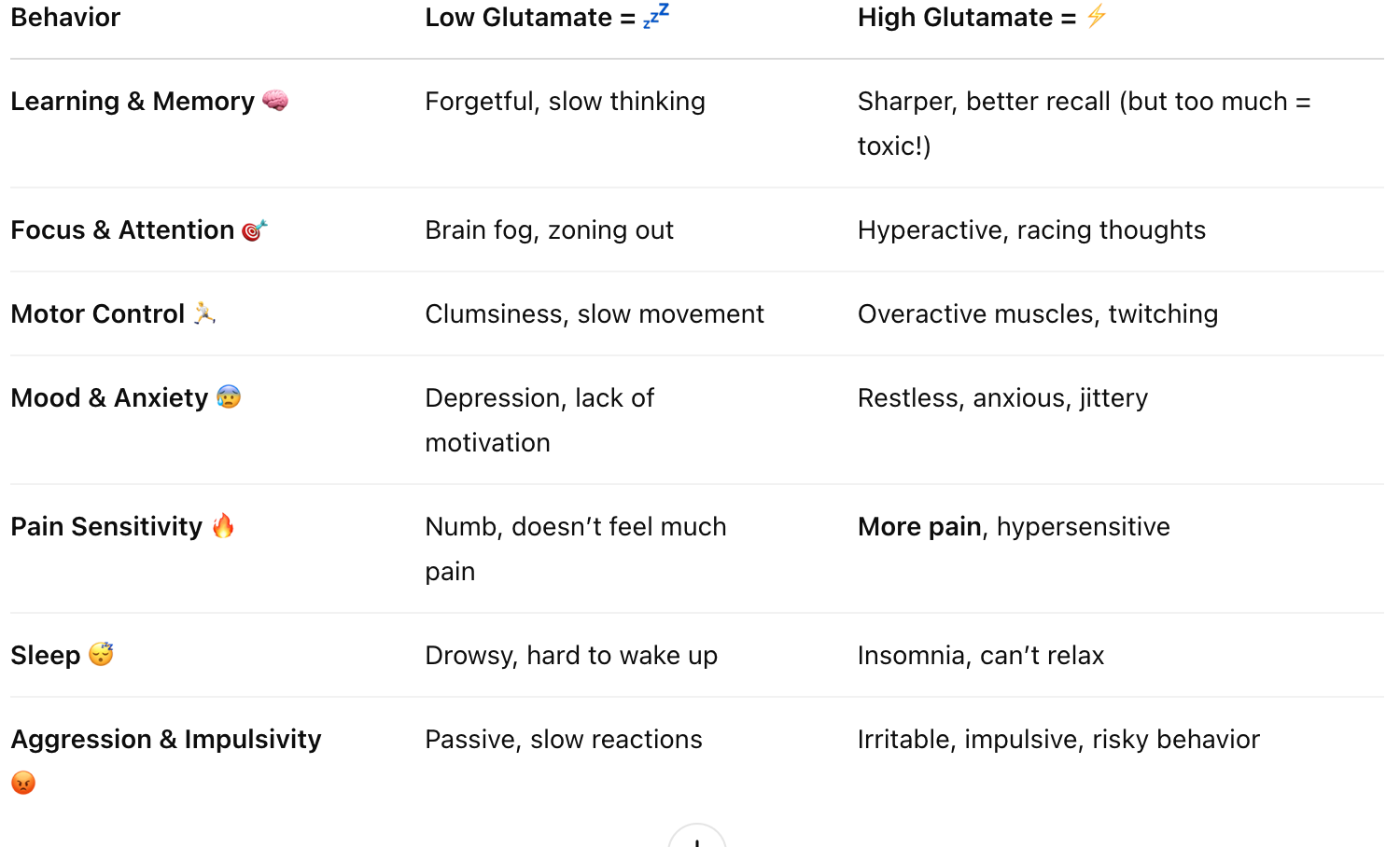

Summarize the synthesis pathways of GABA
Most GABA comes from glutamine, which gets turned into glutamate first!
Glutamine Route (Main Way ASF):
Step 1: glutamine floating around in the brain
Step 2: glutaminase (enzyme) converts glutamine → glutamate
Step 3: glutamate decarboxylase (GAD) (MVP enzyme) chops off a piece of glutamate → BOOM GABA (FINAL PRODUCT ASF)
Krebs Cycle Route (Backup Plan):
Step 1: cells break down glucose → a-ketoglutarate (a molecule from the Krebs cycle)
Step 2: glutamate dehydrogenase or transaminase (enzymes) convert a-ketoglutarate → glutamate
Step 3: GAD enzyme (again, MVP) converts glutamate → GABA (FINAL PRODUCT ASF)
Releasing GABA
VGAT or VIAAT packages GABA into vesicles to be transported & released at the synapse, no major clinically used VGAT blockers currently
Describe how GABA signals are terminated at the synapse
Reuptake (sucking GABA back up):
GAT-1, GAT-2, GAT-3 (special proteins) suck GABA back into neurones & glial cells for neuron to reuse or get rid of
e.g: tiagabine blocks GAT-1 → more GABA stays in synapse = extra chill, anti-seizure vibes
Breakdown (destroying GABA):
GABA-T breaks GABA down into inactive metabolites (succinic semialdehyde); metabolites go into Krebs cycle to make energy; no more GABA = no more chill → brain can wake back up
e.g: vigabatrin blocks GABA-T → GABA doesn’t get destroyed = extra inhibition, anti-seizure effects
Recognize receptor subtypes for GABA
GABA-A (Fast & Strong - the knockout switch)
ligand-gated ion channel (door that opens when GABA binds)
lets Cl- in → neuron gets super negative → no firing = CALM
GABA-A boosters: benzos (xanax, valium) – make GABA work better = anti-anxiety, muscle relaxant; barbiturates (phenobarbital) → super strong sedation; alcohol (ethanol) → enhances GABA-A = tipsy, drowsy; neurosteroids → body’s natural chill enhancers
GABA-B (Slow & Steady - the gentle brake)
metabotropic receptor (g-protein-coupled, slower effects)
tells neuron to stop firing by blocking Ca2+ entry & opening K+ channels → neuron chills out
effects = long-term calm, muscle relaxation
GABA-B boosters: baclofen (muscle relaxer) → used for spams, alcohol withdrawal; GHB (club drug, aka liquid ecstasy) → sedative effects, but also abuse potential
Give examples of behaviours influenced by GABA release

Recognize the families of endogenous opioid neurotransmitters in the human nervous system and the ‘preferred’ receptor types
Endorphins (Runner’s High Crew)
most famous opioids; released during exercise, laughter, sex, etc
preferred receptor: Mu (μ) receptors
effects: pain relief, pleasure, euphoria, sedation
“feel amazing” chemicals
Enkaphalins (Chill Under Pressure Squad)
found in brain & spinal cord; released during mild/moderate stress
preferred receptor: Delta (δ) receptors
effects: mild pain relief, emotional regulation, antidepressant-like effects
mood balance & mental resilience
Dynorphins (Too Much Stress Gang)
released during intense stress or trauma
preferred receptor: Kappa (κ) receptors
effects: pain relief, BUT ALSO dysphoria, stress, anxiety
“I feel weird/bad but I don’t hurt” chemicals
Nociceptin (Reality Check Crew)
involved in stress, learning, addiction, & pain modulation
preferred receptor: nociceptin/orphanin FQ peptide receptor (NOP)
effects: reduces pain, spinal cord, but may increase pain in brain, affects mood, cognition, & stress response
“Wait, what’s really going on?” chemical, complex and context-dependent
Compare and contrast various opiate drugs in terms of their affinity and efficacy at opioid receptors
Best tip to remember:
Full Agonists = Full Effect!
Morphine, Heroin, Fentanyl, Methadone
Partial Agonists = Stick hard, weak effect
Buprenorphine (used in Suboxone)
Antagonists = Stick super hard, block everything
Nalaxone (Narcan), Naltrexone
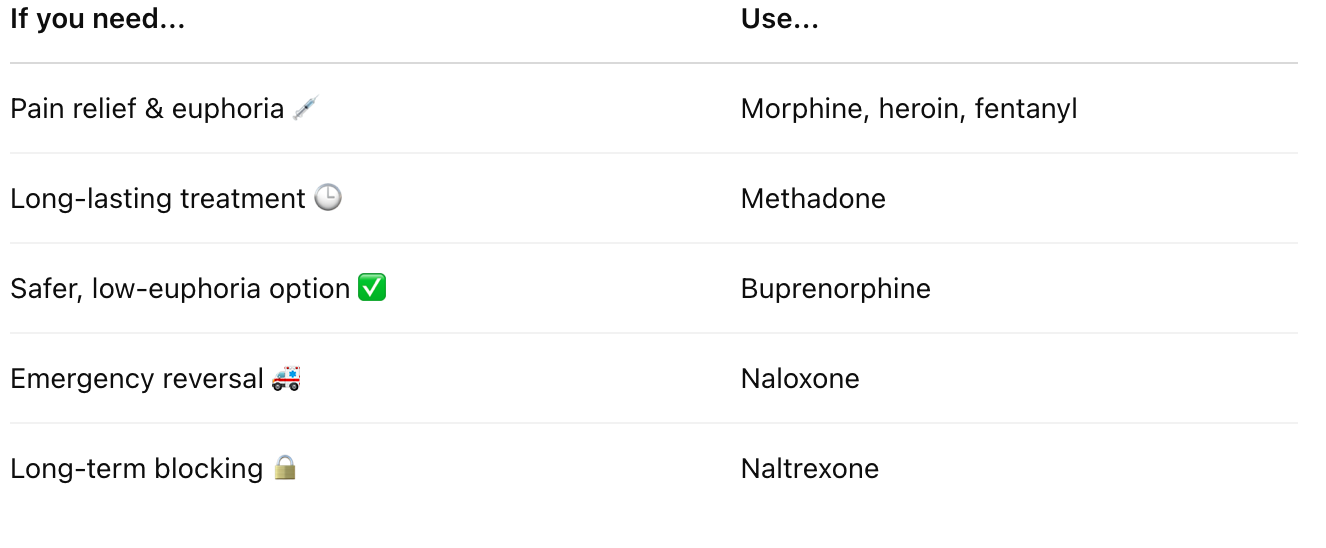
Describe some processes involved in the development of tolerance to opiate drugs
Receptor Downregulation - “Too Much = Shut It Down”
opioids activate mu receptors to block pain and make you feel good
if they’re activated too often → fewer receptors = less effect = you need more drug to get the same high
Receptor Desensitization - “Still There, But Not Listening”
even if receptors don’t disappear, they stop responding as strongly (like brain hitting mute on opioid signal)
same amount of drug = weaker effect
Increased Metabolism - “Get Rid of It Faster”
liver gets better at breaking down the drug; doesn’t last as long or hit as hard
need more and more, more often
Opponent Processes - “Brain Tries to Balance”
brain doesn’t like being overly relaxed & euphoric all the time
starts ramping up opposite systems (pain, stress, alertness)
when opioids wear off, you feel worse than before = withdrawal, cravings
you don’t even take drug to feel good anymore, you take it to feel normal
Identify which brain circuits are active when feeling a high (a ‘reward’) from an opiate drug
Mesolimbic dopamine system:
Ventral Tengmental Area (VTA) → makes dopamine
Nucleus Accumbens (NAc) → feels the reward through the dopamin release
Prefrontal Cortex → helps with decision-making, craving
Opiates also affect the amygdala (emotions) and brainstem (bodily effects like slowed breathing)