BCIT - Test 1 - ECG / Pacemakers - CARD 3330
1/156
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
157 Terms
phases of action potential
1 - resting state - -90mv - Sodium out, potassium in.
2 - depolarization phase - +20mv sodium in, potassium out
3 - repolarization phase - Close sodium channels, loss of potassium, calcium channels open. Calcium flows out too.
4 - hyperpolarization/terminal - calcium out, potassium in, sodium out.
cardiac conduction system
a system of specialized muscle tissues which conduct electrical impulses that stimulate the heart to beat.
the sinoatrial node (SA node), internodal tracts, atrioventricular node (AV node), bundle of His, right and left bundle branches, and the Purkinje fibres
Cardiac cells can be divided into two basic types
conduction and contraction
cellular properties
excitability, automaticity, conductivity, contractility, and refractoriness
Excitability
the ability of a cell to respond to a given electrical stimulus when it is not in a state of refractoriness
Automaticity
the ability of the cell to spontaneously initiate an action potential. (commonly SA node)
Conductivity
the ability of a cardiac cell to transmit an electrical impulse to another cell. (Gap junctions)
Refractoriness
the cell's inability to be re-stimulated after depolarization. This is a preventive mechanism that allows the cell time to contract.
sinoatrial cells
P - pacemaker calls
T - Transitional cells
Norepinephrine (NE)
the neurotransmitter used by the sympathetic division of the autonomic nervous system at the post-ganglionic organ-level (synapse).
innervates both the atria and ventricles. It governs increases in heart rate and AV conduction. It is also responsible for the "irritability" of cardiac cells.
SA node receives blood from:
SA nodal artery, 2/3 of pop originates in first branch or right coronary artery.
AV nodal delay
The unique crisscross matrix of the AV node provides the necessary delay in impulse conduction so that atrial contraction can precede ventricular contraction.
Starling's law of the heart
the greater the ventricles stretch, enlarging their volume, the more blood will be pumped out.
AV node may assume the role of pacemaker.
If the SA node is diseased or impaired. Beats around 40 to 60 beats per minute (bpm). The resulting rhythm is considered a nodal or junctional rhythm.
Hemiblocks
Involve conduction failure in one of the divisions of the left bundle branch ( anterior or posterior)
Anterior block: affects the superior portion of the ventricle
Posterior: affects the inferior portion
Left Anterior Fascicular Block (LAFB)
This presents with an unexplained left-axis deviation
Left axis deviation, usually >-60 degrees
Small Q in leads I and aVL, small R in II, III and AVF
Usually normal QRS duration
Late intrinsicoid deflection in a VL (>0.045 secs)
Increased QRS voltage in limb leads
Left Posterior Fascicular Block (LPFB)
This presents with an unexplained right-axis deviation
Right axis deviation (usually > +120 degrees)
Small R in leads I and AVL, small Q in II, III and aVF
Usually normal QRS duration
Late intrinsicoid deflection in aVF (>0.045 secs)
No evidence for right ventricular hypertrophy
bifascicular block
Blockage of any combination of two of the fascicles or conduction pathways: a right bundle branch block (RBBB) and anterior hemiblock, a RBBB and posterior hemiblock, or an anterior hemiblock and posterior hemiblock
Trifascicular block (complete 3rd degree block)
A blockage or impairment of all three components of the ventricular conduction system, with one working occasionally to provide AV conduction
Sinus Node Dysfunction
refers to deterioration of the propagation of normal beats originating in the SA node, sometimes coupled with enhanced sinus or atrial automaticity.
sinus arrest, pause, SA block, bradycardia.
chronotropic effect
The effect on the rate of contraction of the heart
Exit block
the SA node depolarizes, but conduction of impulses to atrial tissue is impaired or blocked.
1st degree SA block
the SA node impulse is just slowed, and ECG is normal
type I 2nd-degree SA (Wenckebach) block
impulse conduction slows before blocking, seen on the ECG as a P-P interval that decreases progressively until the P wave drops altogether. This creates a pause and the appearance of grouped beats - the duration of the pause is less than 2 P-P cycles
type II 2nd-degree SA block
conduction of impulses is blocked without slowing beforehand, producing a pause that is a multiple (usually twice) of the P-P interval and the appearance of grouped beats.
3rd degree SA block
all conduction is blocked. P waves are absent, giving the appearance of sinus arrest.
Sinus Pause
Temporary absence of sinus node activity. This results in a pause with the disappearance of the P wave on ECG, usually lasting for seconds.
Sinus Arrest
If the pause becomes prolonged without an escape rhythm occurring.
length greater than 2 seconds
no sinus activation
normal sinus beat post pause
length of the pause not an exact multiple of missed beats.
Tachy-brady syndrome
"sick sinus syndrome"
Refers to alternating rapid and slowing rhythms, often accompanied by pauses.
atrial fibrillation
occurs when the normal rhythmic contractions of the atria are replaced by rapid irregular twitching of the muscular heart wall
Atrial Flutter
has a distinctive sawtooth appearance. It is rhythmic and regular with an atrial rate of 200 - 350 bpm.
1st degree AV block
SA node fires normally and conduction is slowed through the AV node to the ventricles. P-R interval is greater than 0.20 seconds
2nd degree AV block type 1
AV interval prolongs to an increasingly greater degree until 1 P wave is completely blocked, then the timing is reset to a shorter AV Block.
2nd degree AV block type 2
Impulses produced and conducted from the SA node and through the AV node are blocked below the bundle of His.
beats have a normal PR interval, until a P wave is blocked, which creates a delay.
3rd degree AV block (complete heart block)
P waves are still seen in ECG recording, but the QRS complexes are completely dissociated from them.
Junctional Rhythm
beats appear from the junction below the AV node, above the bundle of His. It is the iconic "rescue" rhythm that protects the heart from effects of heart block, pauses or severe bradycardia.
Idioventricular Rhythm
There the QRS is wider, as other ventricular beats. Rates are 20-40 bpm and No P waves are visible.
Below the bundle of His.
mitral valve prolapse
Improper closure of the valve between the heart's upper and lower left chambers.
PVCs, and supraventricular ectopy, which includes atrial fibrillation and flutter.
aortic stenosis
causes a decrease in blood flow through the aorta as the valve becomes stiff and doesn't open fully.
condition is not treatable by any method other than valve replacement.
endocarditis
inflammation of the inner (lining) of the heart (particularly heart valves)
Chordae tendons shorten and thicken, valves thicken and commisures fuse.
cardiomyopathy
disease of the heart muscle, the myocardium.
cardiac hypertrophy
enlargement of the heart by increases in muscle wall thickness or chamber size or both.
Right Ventricular Hypertrophy
increase in thickness of the myocardium of the right ventricle.
culprit is a condition that manifests pulmonary hypertension such as pulmonary edema, mitral stenosis, mitral insufficiency, and chronic obstructive pulmonary disease (COPD).
a shift in QRS axis towards right axis deviation
tall R waves in V1, II and III
deep S in V5, V6
possible RBBB
young children and adolescents
WPW Type A pattern
Posterior wall acute MI
Right Atrial Enlargement (RAE)
This occurs when there is a >2.5 box height of p wave in lead II, III, and aVF to fulfill the criteria for p-pulmonale
left ventricular hypertrophy or enlargement
s characterized by pathologies that increase ventricular volume or pressure such as aortic stenosis, aortic insufficiency, hypertrophic cardiomyopathies, systemic hypertension, and MI
tall R waves in I, aVL and left precordial leads V5 and V6
deep S waves in V1
possible mid axis deviation to the left
T wave inversion in leads I, aVL, V5 and V6
possible increased left ventricular activation time
generally accepted that if the combined S wave (V1) and R wave (V5 or V6) add up to 35 mm or if an R wave in V5 or V6 is larger than 30 mm, the voltage criteria are satisfied.
asymmetrical septal hypertrophy
responsible for obstructing the ventricular outflow tract, which leads to more vigorous contractions and further manifestation myocardial hypertrophy.
Left Atrial Enlargement (LAE)
most common causes are mitral stenosis, mitral insufficiency, heart failure, and myocardial infarction.
broadened P wave (>120 msec) in any lead
wide, notched P wave (p mitrale), seen commonly in lead II
terminal portion of a biphasic P wave in lead V1 which is 0.04 sec in duration and 1 mm in depth
What is the underlying atrial rate of this rhythm? Afib
400-650bpm
Name 2 possible causes of this rhythm: Afib
Metabolic disorders
Ischemia
What are 2 anticoagulants approved for use in Canada in treatment of AFib?
dabigatran
warfarin
Name 2 medical procedures which may be used to terminate AFib and restore normal sinus rhythm.
Direct current cardioversion
pulmonary vein ablation
Describe why tachy-brady syndrome is difficult to treat:
Difficult to treat because medications to slow the tachycardia also worsen the bradycardia.
Atrial flutter is a rhythm which may be treated effectively with cavotricuspid isthmus ablation. An electrophysiology study is commonly done to see that typical AFl is originating in the area of__________ and is conducted in a __________ direction
Tricuspid isthmus, right atrium, inferior vena cava
Counter clockwise
Heart block tends to be progressive. 2nd degree block often progresses to complete heart block, and the risk also increases if the patient has underlying____________block. This type of block rarely causes symptoms initially
bifasicular
Junctional rhythm is an escape rhythm commonly seen. What is the normal rate of junctional rhythm?
40-60bpm
One type of bundle branch block obscures any changes that may be seen in ischemia. What type of bundle branch block is this?
Left BBB
Name the 3 electrolytes responsible for conduction through the SA node.
Sodium
potassium
calcium
Many cardiac medications affect cardiac refractoriness. Describe what refractoriness means.
Inability of the cells to respond to stimulation after depolarization
Conduction is slowed as it passes through the AV node. Conduction is then rapid through the______
bundle of his
Left Ventricular outflow tract obstruction
Systolic anterior motion of the MV, accompanying LVH. It is a physical structural abnormality
increased inotropes
may occur post AVR and with mitral regurgitation present
known LVH or possibly the presence of hypertrophic cardiomyopathy
hypertension
small left ventricle
Tetralogy of Fallot
a congenital malformation of the heart involving four distinct defects:
ventricular hypertrophy
right ventricular outflow tract obstruction
ventricular septal defect
aortic dextroposition
Wellens Syndrome
Deeply-inverted or biphasic T waves in V2-3 (may extend to V1-6)
Isoelectric or minimally-elevated ST segment (< 1mm)
No precordial Q waves
Preserved precordial R wave progression
Recent history of angina
ECG pattern present in pain-free state
Normal or slightly elevated serum cardiac markers
Fontan procedure
the repair of a congenital defect which encompasses a number of structural abnormalities. In general it is most often regarded as a single ventricle anatomy.
Tricuspid atresia
Double inlet left ventricle
Hypoplastic left heart syndrome
Some variations of double outlet right ventricle
Various heterotaxy defects
Eisenmenger's complex
Patent ductus arteriosus (PDA)
Ventricular septal defect (VSD)
Atrial septal defect (ASD)
Atrial canal defect (AV canal)
dyspnea, resting and exertional
fatigue
dizziness or syncope
cyanosis
chest pain or tightness
headache
paresthesia
palpitations
Ebstein's anomaly
Tricuspid flaps fused to inside of right ventricle; creates constant opening between atrium & ventricle
Long QT syndrome
inherited genetic abnormality, hallmark of Long QT is prolongation of the QT interval related to abnormal repolarization. The primary risk in these patients is possibility of ventricular arrhythmia, primarily Torsade de Pointes.
Brugada syndrome
genetic abnormality characterized by 3 subtypes of ECG abnormalities and an increased risk of sudden cardiac death.
underlying AFib in up to 20% of patients
often occurs during sleep or at rest
may be accompanied by syncope
accompanied by nightmares or disturbed, restless sleep
possibly triggered by fever
asymptomatic but abnormal ECG with V1-V3 ST elevation
congential abnormalities, ECG syndromes
Left Ventricular outflow tract obstruction
Tetralogy of fallot
Wellens syndrome
Fontan procedure
Eisenmenger's syndrome
Ebstein's anomaly
Long Qt syndrome
Burgada Syndrome
Hypokalemia
deficient potassium in the blood. excessive loss of body fluids from vomiting, gastric suction, diuretics or diarrhea.
Hyperkalemia
excessive potassium in the blood. renal failure, acidosis (as seen in ketoacidosis and lactic acidosis), and excessive potassium replacement therapy.
Hypocalcemia
deficient calcium in the blood;
occurs most commonly in the setting of chronic conditions.
chronic or acute on chronic renal impairment
hyperphosphatemia
inadequate vitamin D ingestion or absorption
lack of ultraviolet light exposure
Hypercalcemia
excessive calcium in the blood
excessive sunlight exposure
vitamin D overdose with supplements or antiacids
thyrotoxicosis
metastatic cancer
prolonged immobilization causing decreased vitamin D elimination
sarcoidosis
Electrolyte Abnormalities
Hypokalemia
Hyperkalemia
Hypocalcemia
Hypercalcemia
Re-entry Rhythms
the propagation of an impulse through tissue already activated by that same impulse.
Two functionally distinct pathways
Functional unidirectional block of one of the pathways
Differing electrophysiological (EP) properties (that is, conduction velocity and refractoriness)
Drugs can terminate - adenosine, beta blockers or calcium channel blockers.
Accessory pathway connections
Re-entry can result from accessory pathway (AP) connections that bypass the normal function of the AV node.
rapid conduction characteristics often allows for pre-excitation of the ventricles.
Wolff-parkinson-white pattern/syndrome
Atrioventricular Re-entry Tachycardia
Both use accessory pathways and AV node as part of their re-entry
2 types - Orthodromic and Antidromic
Orthodromic tachycardia
Rely on the AV node for the ante grade path and on the (AP) for retrograde conduction (95% of AVRTs are of this variety). Initiation can be either a PAC or a PVC
Antidromic tachycardia
(5% of AVRTs): Use the accessory pathway for antegrade conduction and the AV node or another accessory pathway for retrograde conduction
Wolff-Parkinson-White Syndrome
Most common type of ventriuclar pre-excitation sydnrome. Abnormal fast accessory conduction pathway from atria to venricle bypasses the rate-slowing AV node causing a delta wave and widening QRS with shortened PR interval. Could lead to a reentrant circuit and suprvaventicular tacky. AVRT
Lown-Ganong-Levine Syndrome
A disorder that causes preexcitation of ventricular tissue and which is characterized on the ECG by a short PR interval and a normal QRS duration, does not display a delta wave, and is not a medical condition of concern, simply abnormal ECG.
Three accepted mechanisms of tachyarrhythmia (abnormal automaticity) are:
Abnormal automaticity
Re-entry
Triggered activity
Abnormal automaticity
exaggerated firing of non-sinus tissue (ectopic foci i.e. any site which reaches threshold before or ahead of sinus tissue and depolarizes the heart)
Triggered automaticity
Impulse giving rise to further impulses due to abnormal state of myocardial cells. (they are triggered and then multiply) Ventricular arrhythmias are "triggered" by early afterdepolarizations (EAD) and delayed afterdepolarizations (DAD).
Early Afterdepolarization (EAD)
Caused by slow activation and prolonged action potential. occur near end phase 2 and onset of phase 3.
Delayed Afterdepolarization (DAD)
Caused by calcium overload. Occur frequently in the presence of digitalis toxicity and myocardial ischemia.
pacemaker used to
prevent the heartbeat from going too slowly or to support a regular heartbeat when the intrinsic SA node is incapable of the job.
class I indication for implantation
Conditions for which there is evidence and/or general agreement that a given procedure or treatment is beneficial, useful, and effective.
class II indication for implantation
Conditions for which there is conflicting evidence and/or a divergence of opinion about the usefulness/efficacy of a procedure or treatment.
class IIa indication for implantation
Weight of evidence/opinion is in favour of usefulness/efficacy.
class IIb indication for implantation
Usefulness/efficacy is less well established by evidence/opinion.
class III indication for implantation
Condition for which there is evidence and/or general agreement that a procedure/treatment is not useful/effective and in some cases may be harmful.
Most commonly occurring causes of bradycardia resulting in a ICD include:
1st degree AV Block
2nd degree AV Block Type I (Wenckebach or Mobitz I Block)
2nd degree AV Block Type II (Mobitz II Block)
3rd degree AV Block (Complete Heart Block, AV Dissociation)
Sinus node dysfunction including SSS, SA block, SVT
Bifascicular Block
Chronotropic Incompetence
Slow atrial fibrillation
Neurocardiogenic syncope/hypotension
Hypersensitive carotid sinus syndrome
The following table describes the meaning of each letter in the mode description.
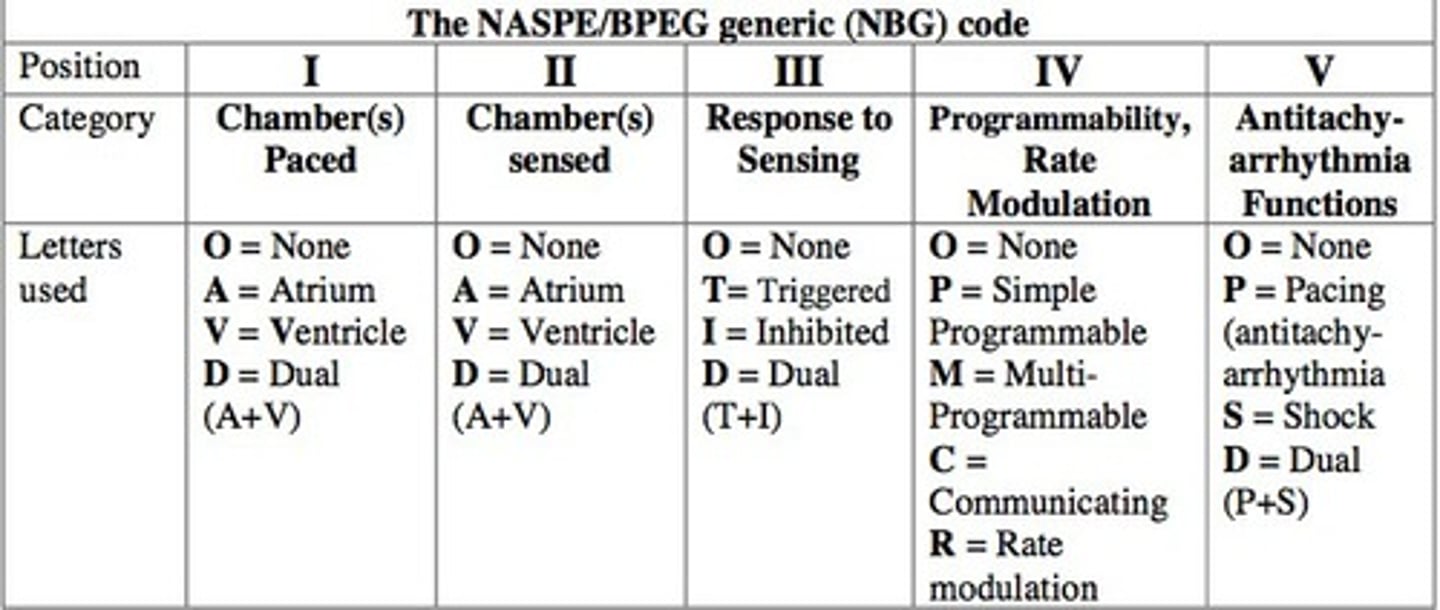
Rate modulation
This refers to the device having the capability of increasing heart rate when necessary to support physiologic response, such as during exercise.
When atrial pacing occurs:
The spike is usually small. This is because the atrium is small and just as a P wave is small, the paced spike generated in the atrium is also small.
When pacing occurs in the ventricle:
you will usually see a larger spike, because the ventricle is a larger mass of muscle. Just as the R wave is usually large, the ventricular spike is also large.
The physician chooses the best device for their patient based on:
individual circumstances, the patient's underlying condition, socioeconomic circumstances, age, co-existing illnesses, access to regular follow-up, and even specific device availability.
Basic functions of a CRMD
Detecting the intrinsic rhythm (sensing)
Pacing when appropriate
Maintaining the timing intervals (V-V, A-V)
Maintaining the base and upper rate limits for pacing
Monitoring safety margins (ensuring enough energy to depolarize the heart)
ICD batteries do not last as long as pacemaker batteries because:
ICD is programmed to respond by monitoring the heart rhythm, delivering therapy when necessary, withholding therapy when necessary, and storing electrograms to be evaluated by the clinician at follow-up. Statistical data collected includes heart rate histograms, lead impedance graphs, capture threshold, and sensing trends. causes more current drain.
The usual incision site is:
beneath the clavicle, usually two finger breadths down (the infraclavicular fossa). This helps to eliminate the possibility of the device rubbing against the bone with arm movement.