4. Diseases of the lacrimal glands and duct. Keratitis sicca
1/56
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
57 Terms
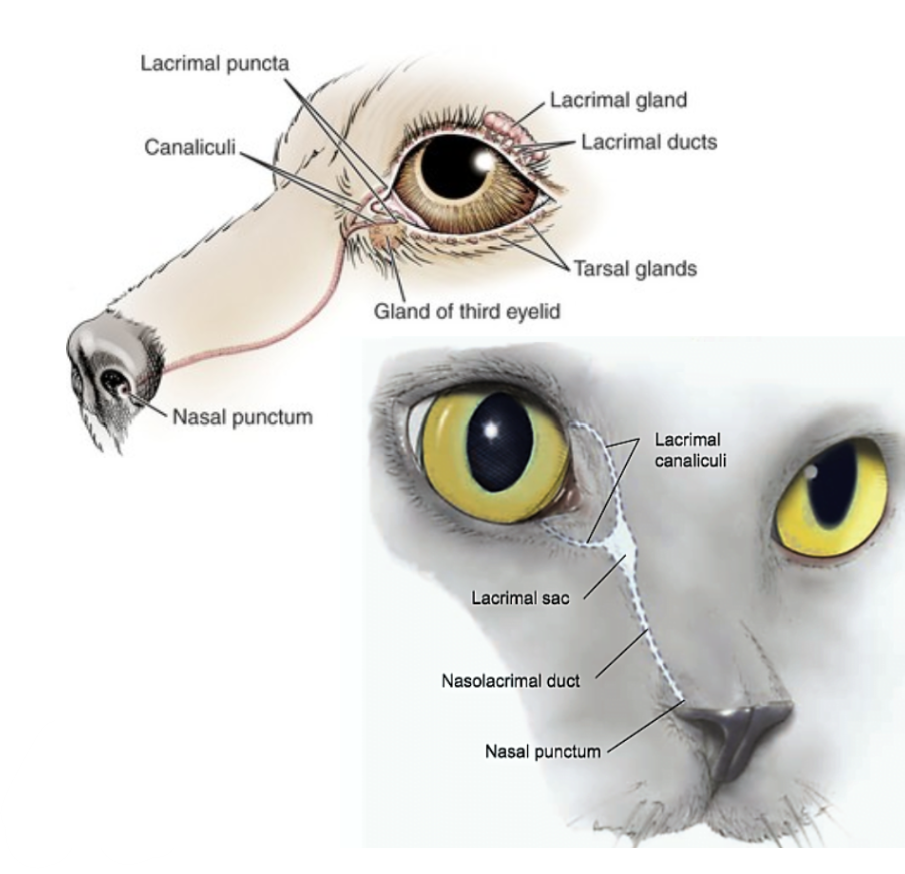
What are examples of causes of epiphora/wet eye?
Imperforate puncta/congenital puncta
Obstruction of nasolacrimal system (tear duct)
Dacryocystitis
What are the clinical signs of imperforate puncta?
How is imperforate puncta diagnosed?
Clinical signs, inability to cannulate the duct (ballooning on flushing), culture, fluorescein testing (John’s test), and imaging studies with contrast
What are the differential diagnoses for imperforate puncta?
How is imperforate puncta treated?
Topical lubricants/ointments. For chronic epiphora, surgery (punctoplasty [opening or widening of puncta] or dacryocystorhinostomy [creation of a new tear drainage pathway]) may be performed
![<p>Topical lubricants/ointments. For chronic epiphora, surgery (punctoplasty [opening or widening of puncta] or dacryocystorhinostomy [creation of a new tear drainage pathway]) may be performed</p>](https://knowt-user-attachments.s3.amazonaws.com/30e4fb7c-0c49-4e6d-b9bd-79e94bfd4723.png)
Congenital absence of the inferior canaliculus, imperforate puncta
Acquired factors (dacryocystitis, foreign bodies, scarring from trauma/inflammation)
Clinical signs, negative fluorescein passage into nasal cavity (John’s test), and dacryocystorhinography (fluoroscopic contrast examination of nasolacrimal apparatus)
Flushing, fluorescein passage check, topical antibiotics and corticosteroids, and conjunctivorhinostomy (create passage)
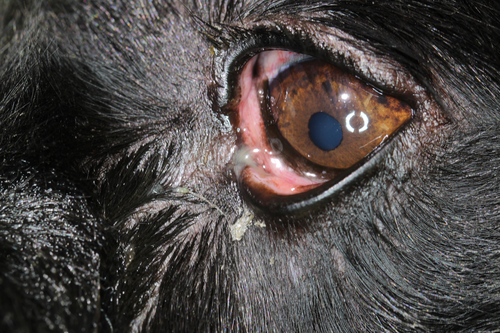
Negative fluorescein passage and X-ray with contrast
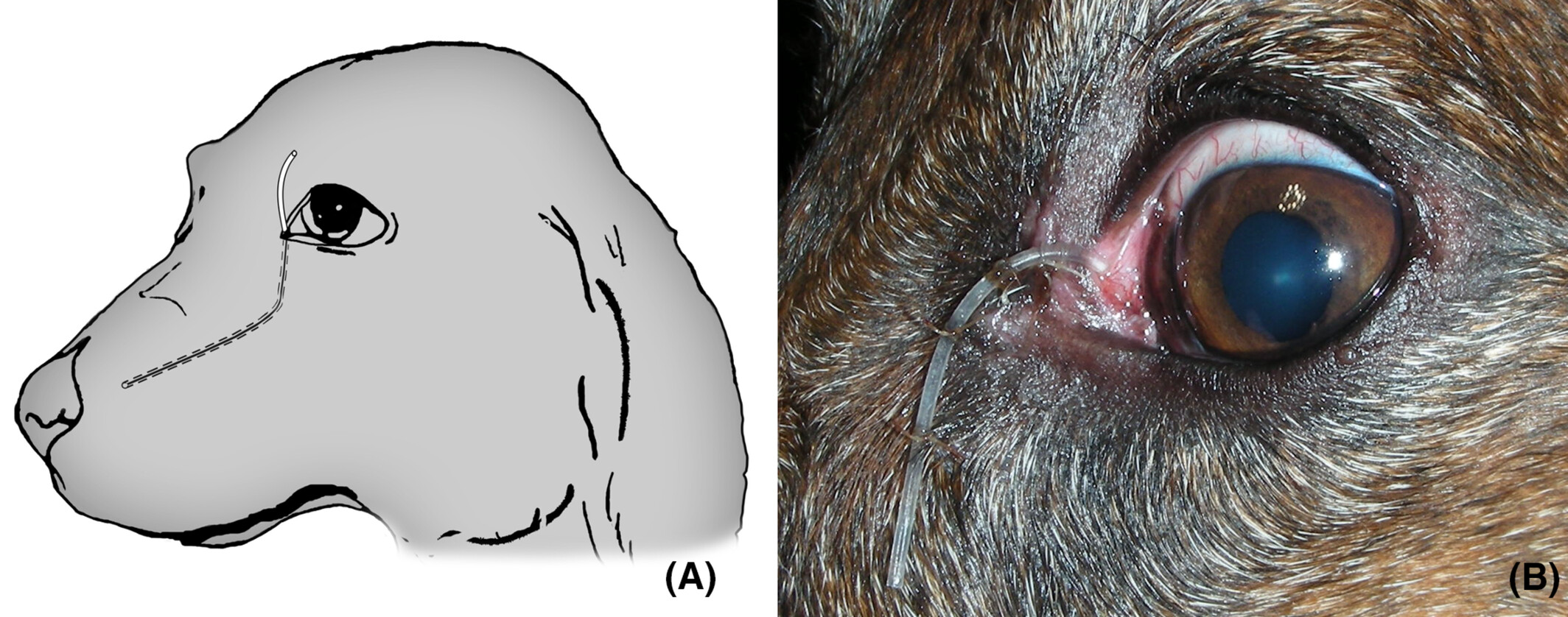
What are types of disorders causing dry eyes?
Dry eye syndrome/keratoconjunctivitis sicca
Meibomian gland dysfunction
Mucin abnormality
Cysts and neoplasia of the lacrimal secretory system
Infectious causes: Canine distemper virus, chronic blepharoconjunctivitis, and other ocular surface infections
Congenital: Acinar hypoplasia, lacrimal gland hypoplasia
Drug-induced: Systemic sulfonamide or topical atropine
Metabolic disease hypothyroidism, cushings, diabetes mellitus
Immune-mediated: lacrimal gland adenitis
Vary depending on the stage.
Early stage: red and inflamed eyes with intermittent mucoid/mucopurulent discharge. Blepharitis and periocular dermatitis are common.
Progressive disease: increased discomfort and persistent blepharospasm
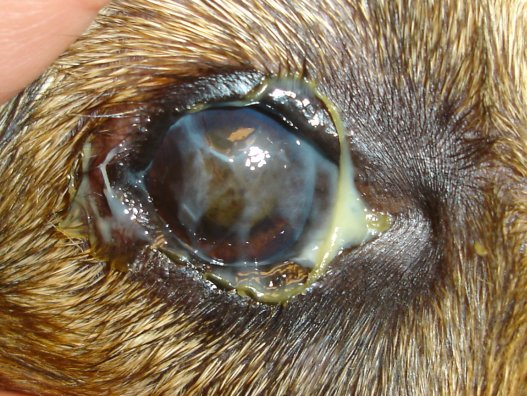
Epithelial defects, inflammation, vascularisation, and scarring.
Decreased tear production or altered tear composition on microscopic examination of tear film
Clinical signs, ocular staining, Schirmer tear test (less than 15 mm/min is suggestive; < 8 mm/min is severe), and Rose Bengal stain (detect devitalised cells). IOP is normal.
Tear stimulation with pilocarpine (oral or topical)
Artificial tear replacement/lubrication
Topical/oral ATB
Mucolytics (sodium hyaluronate & cyclorine A)
Cyclosporine ointment (immunosuppressive for 4 weeks)
Anti-inflammatories
Parotid duct transposition: saliva & tear are nearly normal in osmolality & pH, & may substitute lack of tears
Partial tarsorrhaphy: May be beneficial in some dogs to protect cornea.
Replacement of prolapsed nictitans gland
Conjunctival or nictitans flap for ulcers & protection of cornea
Inflammation, hyperkeratosis, glandular duct obstruction/dilation (chalazion), and glandular atrophy
How is the tear break-up time test carried out?
Add fluorescein, let blink and hold eye to see how fast the fluorescein forms dark spots on cornea aka breaks (normal: 20 seconds in dog)
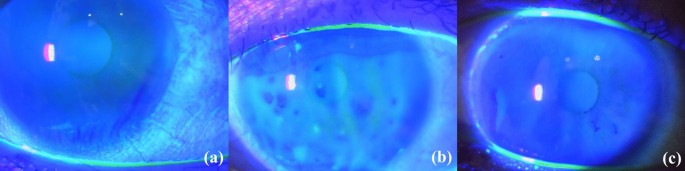
A problem with the production or distribution of mucin (a component of the tear film that helps the aqueous layer adhere to the cornea) → evaporative dry eye.
Where is the mucin layer produced?
Goblet cells of the conjunctiva
Genetic disorders
Autoimmune diseases (e.g., Stevens-Johnson syndrome)
Inflammatory conditions (e.g., allergic conjunctivitis, chronic blepharitis)
Environmental factors (toxins or pollutants)
Clinical signs, fluorescein break-up test (TBUT <5 seconds is suggestive), and conjunctival biopsy to quantify goblet cells

Cysts: cystic structures lined by epithelial cells.
Neoplasms: abnormal cell proliferation
Treatment depends on the type, nature, and extent of the lesion.
Options include surgical excision, drainage/aspiration of cysts, anti-inflammatory/antimicrobial therapy, and radiation/chemotherapy for neoplasia
What is instability of the tear film (paradox in poodles)?
Certain breeds or dogs will have epiphora or normal eyes but suffer from dry eyes. So they may have enough tear volume, but if the mucin layer is insufficient or the lipid layer is compromised, the tear film cannot effectively adhere to the ocular surface.
What drugs are used for KCS?
Topical cyclosporine, lubricant and daily cleaning with NaCl