Bio - Excretion and Kidneys
1/59
Earn XP
Description and Tags
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
60 Terms
define excretion
the process of removing waste products of metabolic processes
define osmoregulation
a form of homeostasis where the concentrations of hemolymph or blood is kept within a particular homeostatic range
define hemolymph
the circulating fluid in arthropods
What are included in arthropods?
insects, crustaceans, and arachnids
what does it mean if an animal is an osmoregulator?
animals that maintain a constant internal solute
what does it mean if an animal is an osmoconformer?
animals whose internal solute concentration tends to be the same as the concentration of solutes in the environment
what does the liver do in terms of excretion?
transforms toxins such as alcohol, drugs, heavy metals, and products of protein metabolism into soluble compounds that can be eliminated by the kidneys
what is the function of the urinary system?
remove waste, balances blood pH, and maintains water balance
what three waste products are excreted by the kidney and what is their origin of waste
ammonia: deamination of amino acids by liver
urea: deamination of amino acids by liver and ammonia combined with CO2
uric acid: products of the breakdowns of nucleic acids, such as DNA
which waste product is excreted by the lungs and what is its origin of waste
carbon dioxide: waste products of cellular respiration
what two waste products are excreted by the liver and what are their origins of waste
bile pigments: breakdown of red blood cell pigment, hemoglobin
lactic acid: products of anaerobic respiration
which product is excreted by the large intestine and what is its origin of waste
solid waste: by product of digestible and indigestible materials
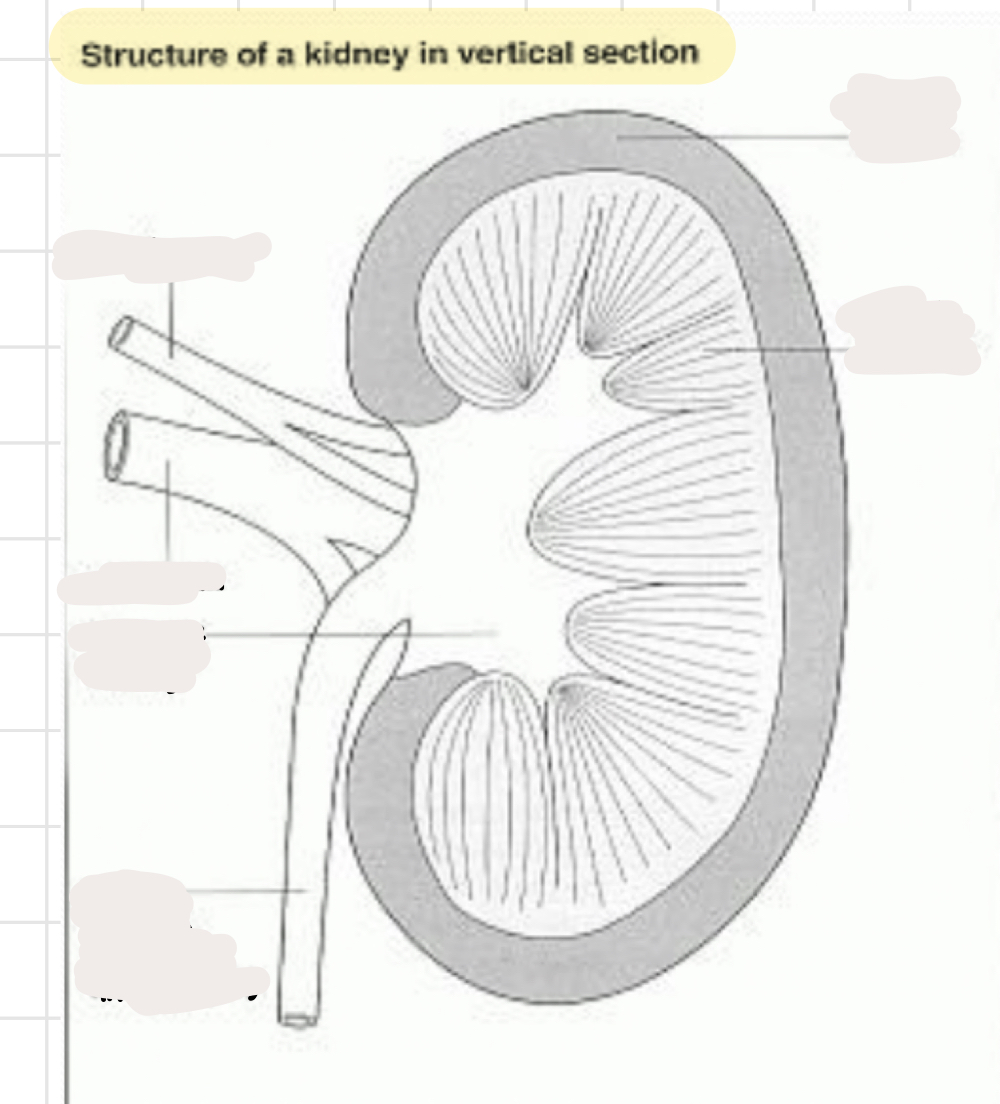
label the kidney!
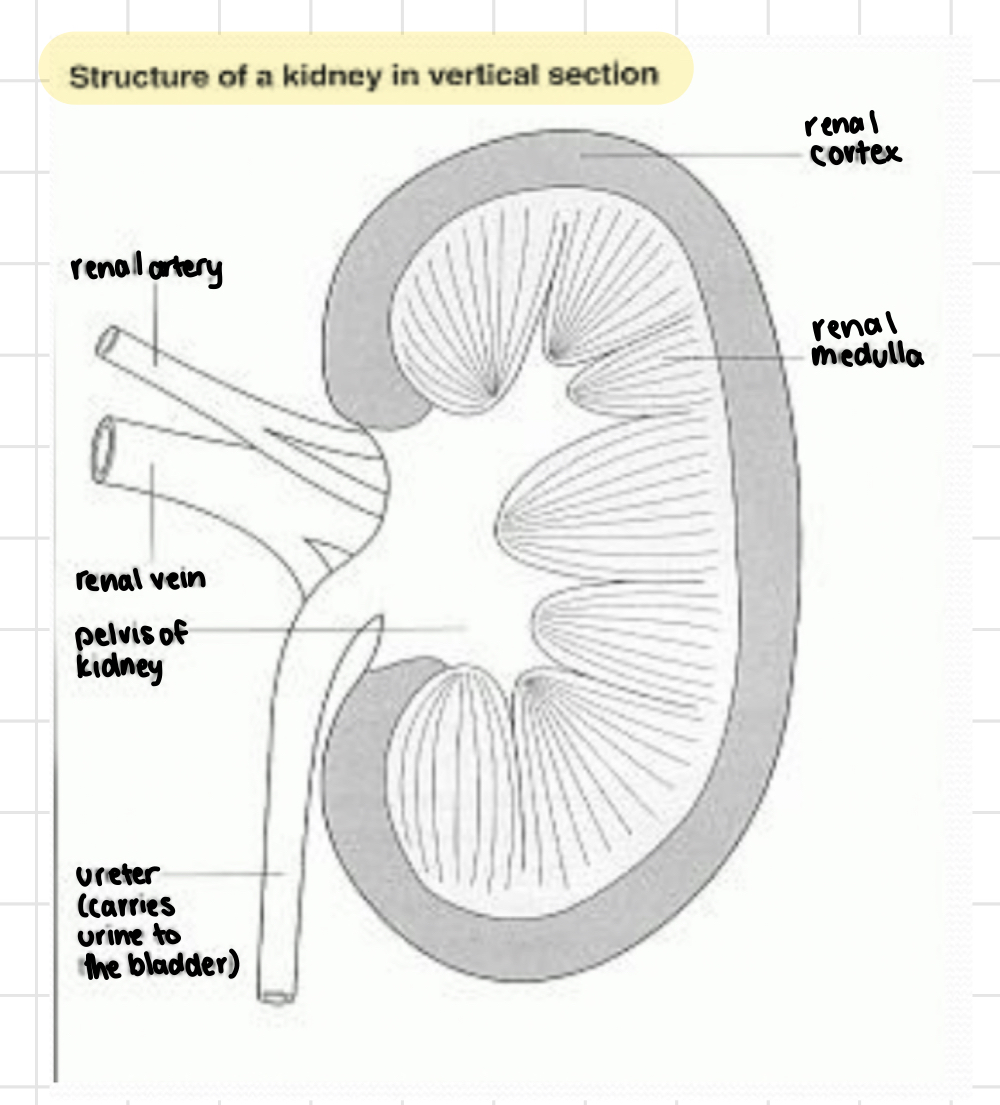
what is the function of proteins in the diet
maintain tissues
promote cell growth
direct cell processes
what are excess proteins often converted into and how does this result in nitrogenous bases as a waste product? what is this process called and what other waste product does it produce?
often converted into carbs which are broken down for ATP
since carbs do NOT have nitrogenous bases, they need to be removed
called deamination
produces ammonia
what is the nephron and what is its function?
functional unit of the kidney
where urine is formed
give the pathway of blood through the kidneys
renal artery —> afferent arteriole —> glomerulus —> efferent arteriole —> peritubular capillaries —> renal vein
give the pathway of urine through the kidney starting at the glomerulus
glomerulus —> Bowman’s capsule —> proximal tubule —> loop of Henle —> distal tubule —> collecting ducts —> renal pelvis —> ureter
what are the three steps of the formation of urine?
filtration
reabsorption
secretion
what is filtration in the formation of urine and how does it work?
fluids move from blood to Bowman’s capsule
ultrafiltration: volume forced out of the glomerulus is 100x greater than in other tissues
filtration occurs because of pressure difference pushing blood into the Bowman’s capsule through the fenestrations of the glomerulus
what three things are NOT filtered into the Bowman’s capsule?
red blood cells
plasma proteins
platelets
what is reabsorption in the formation of urine and how does it work?
transfer of essential solutes and water from nephron back to the blood
both active and passive transport are used
occurs until homeostatic threshold is reached and the excess material is excreted in urine
what is secretion in the formation of urine?
movement of materials from paratubular capillaries into nephron at location other than Bowman’s capsule
what things are secreted into the nephron from the paratubular capillaries?
nitrogen-containing wastes
excess H+ ions
minerals
drugs and poisons
in what form do aquatic animals secrete their waste and why?
directly as ammonia
easily diluted in their environment
what is the feature of echinoderms and what are three examples?
show radial symmetry
sea urchins, star fish, sea cucumbers
what is the feature of coelenterates and what are two examples
tube or cup-shaped body and single opening with tentacles
jelly fish, coral
in what form do insects excrete waste and how?
the form of uric acid
have tubes that branch off large intestine called the Malpighian tubes
what happens in the glomerulus and bowman’s capsule? how does it work?
site of filtration
glomerulus is fenestrated: small slits that open when pressure is increased
high pressure in glomerulus forces fluids into the Bowman’s capsule
blood pressure is high because the afferent arteriole is wider than the efferent
only molecules small enough to fit through the fenestrations will move to the Bowman’s capsule
what is filtrate and what three things must it pass through?
filtrate: fluid that enters the Bowman’s Capsule
must pass through:
glomerular walls
basement membrane
podocytes
define the basement membrane and podocytes?
basement membrane:
covers and supports walls of the glomerulus
made of glycoproteins
prevents plasma proteins from being filtered out
podocytes:
cells that form the inner wall of the Bowman’s capsule
wrap around the capillaries
what happens in the proximal tubule? how does it work?
site of most reabsorption of useful materials via active and passive transport
epithelial cells lining proximal tubule have:
lots of mitochondria (for active transport)
brush border of microvilli into lumen (increase surface area)
almost all of the filtrate is reabsorbed into the blood
exterior side has smaller surface area so as to minimize movement of salt and water back into the tubule
what is reabsorbed into paratubular capillaries? what is secreted into the nephron?
reabsorbed
80% of water
glucose and amino acids
vitamins
hormones (small ones)
sodium and other mineral ions
secreted
H+ and NH3 to manage pH
drugs and poisons that didn’t pass through Bowman’s capsule
what is moved by active transport? what is moved by passive transport? (in proximal tubule)
active transport:
Na/K pump: pumps Na+ out into interstitial fluid and K+ into tubule lumen
passive transport:
Na+: moves into tubule lumen (b/c of Na/K pump creating concentration gradient)
Cl-: follows Na+ (electrochemical gradient)
glucose: CO- transported into interstitial fluid (because of Na+ movement)
water: osmotic force b/c of Na+ movement causes reabsorption into interstitial fluid
what happens in the loop of henle?
creates gradient of solute concentration in the medulla that is essential for H2O reabsorption
what happens in the descending limb of the loop of Henle?
only water is reabsorbed, therefore sodium chloride concentration increases inside nephron
what happens in the ascending limb of the loop of Henle and what are the two parts?
thin segment:
passive transport of NaCl into interstitial fluid (because of concentration gradient)
inner medulla
thick segment:
active transport of NaCl into interstitial fluid (against concentration gradient)
outer medulla
what is the countercurrent multiplier system?
countercurrent: because flow of fluid in the descending and ascending limb are in opposite directions
multiplier: a steeper osmotic gradient is produced
osmotic gradient is produced because of “u” shape
NaCl leaves nephron in ascending limb to make solute concentration in interstitial fluid high, moving water out of the descending limb
what happens in the distal tubule and how does it work?
selective reabsorption of nutrients to maintain homeostasis in blood
regulates K+ and NaCl of body fluids by varying amount secreted/reabsorbed
note: less mitochondria and microvilli here compared to proximal tubule / not as much transfer of nutrients occurs
how is pH and blood solute concentration regulated in the distal tubule?
pH: regulated by secretion of H+ ions and reabsorption of HCO3- ions
blood solute concentration:
if low, little water will be reabsorbed
if hight, ADH will be released by pituitary gland and water reabsorption is increased in distal tubule
what happens in the collecting duct? what happens in what areas?
carries filtrate to renal pelvis
water reabsorption continues
outer medulla: NaCl reabsorbed in interstitial fluid
inner medulla: small amount of urea diffuses into interstitial fluid due to high concentration in fil
what six things are left in the nephron to make up urine?
sodium chloride (NaCl)
water
urea
liver metabolites
uric acid
minerals
what happens in the renal pelvis?
collecting ducts merge to the ureter which takes urine to the bladder
Draw the nephron
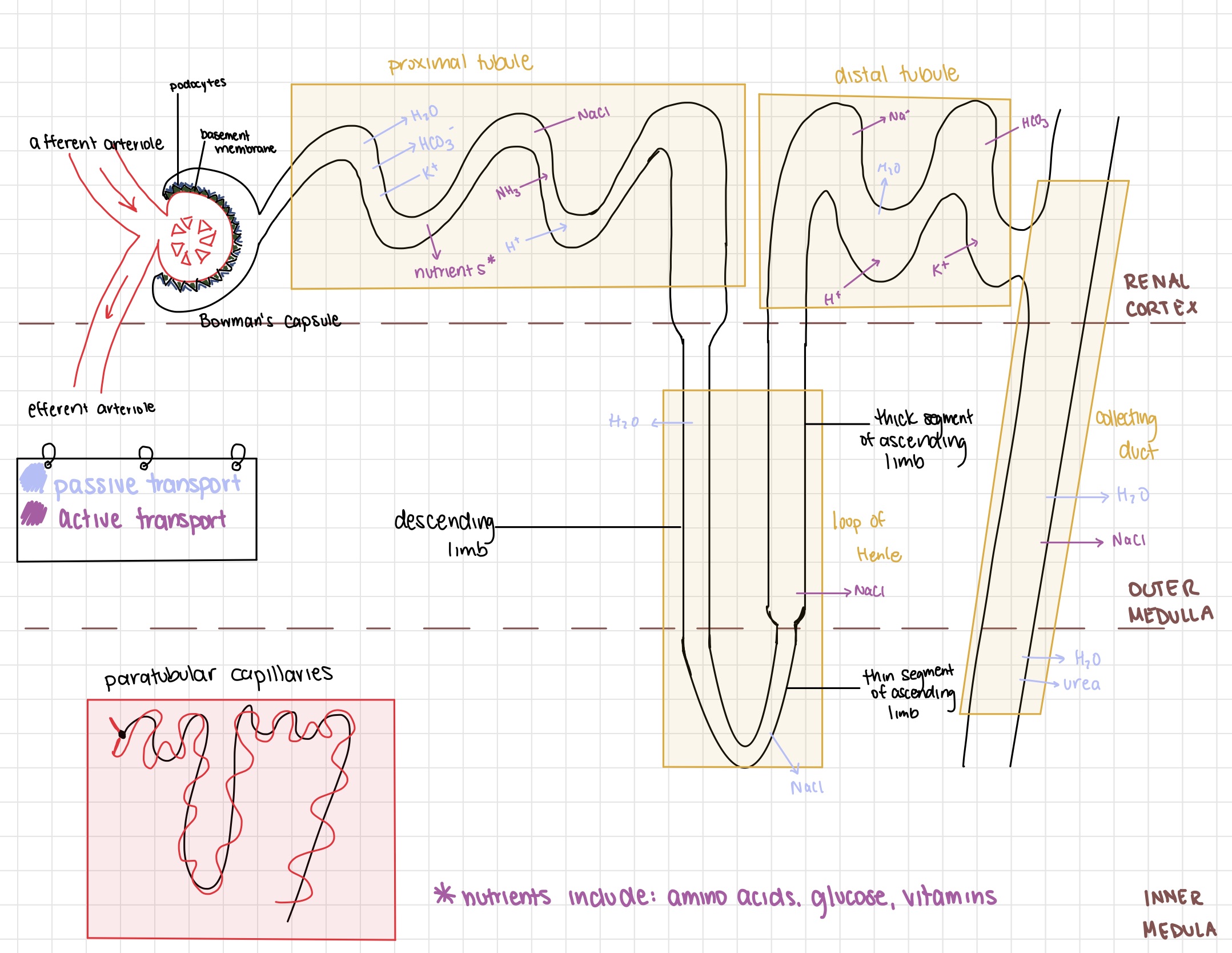
Annotate the nephron

what does diabetes mellitus cause?
excess sugar in the nephrons because inadequate secretion of insulin
excess sugar provides osmotic pressure which leads to more water secreted and excreted in the urine
as a result, release large volume of urine
what is diabetes insipidus and what does it cause?
destruction of ADH producing cells (regulate water reabsorption) or inability of the distal tubules to respond to ADH
as a result, water is not reabsorbed and too much water is lost through urination
what is Bright's Disease (nephritis) and what is it caused by? what does it effect?
inflammation of the nephrons
can be caused by toxins which destroy blood vessels in the glomerulus
affects the permeability and allows larger molecules such as proteins to pass into the nephron
since proteins do not often pass through, there is no mechanism for reabsorption
results in excess water in nephron and increased urine output
what are kidney stones caused by and where are they lodged? why are they so painful?
caused by precipitation of mineral solutes from the blood
stones become lodged in the renal pelvis or may move into the ureter
as it moves through the ureter, the jagged edges can tear the delicate tissues and pain
what three ways can kidney stones be removed?
surgery
shock-wave lithotripsy
shock waves break apart stones into small fragments that can be passed
medication to widen urinary tract
what is dehydration and what can cause it? what is a sign of dehydration?
when more water leaves the body than enters
can be a result of exercise, insufficient water intake, diarrhea, water loss during overheating
sign: darker, more concentration urine with stronger odour due to increased solute concentration
what is over hydration? what can cause it? what does it result in?
when there is over consumption of water, diluting blood solutes
may result from excessive water consumption after exercise without replacing lost electolytes
results in swelling of body cells resulting in headaches and disruption of nerve function
two treatments of kidney failure
dialysis
transplant
what is dialysis?
exchange of substances across a semipermeable membrane
what hormone is responsible for osmoregulation? what does it do?
ADH - antidiuretic hormone
increases water reabsorption in the kidney
outline the steps of the negative feedback loop for osmoregulation when blood osmotic pressure is high (water is low)?
1) osmoreceptors in hypothalamus detect change in osmotic pressure
2) cells of hypothalamus shrink (bc water leaves cells and moves into blood) and a nerve message is sent to the pituitary gland to release ADH
3) water reabsorption is increased in distal tubules and collecting duct
4) water reabsorption prevents the osmotic pressure of body fluids from increasing any further, preventing dehydration
Osmoreceptors also cause you to get thirsty and drink water which lowers the osmotic pressure back to homeostasis
once returned to homeostasis, water moves from plasma to hypothalamus cells which swell and stops ADH release
what hormone is responsible for maintaining homeostatic blood pressure and blood volume in the kidneys? what does it do?
aldosterone
maintains homeostatic blood pressure (raises it when low)
increases sodium concentration in blood by increasing sodium reabsorption in the distal tubule and collecting ducts
water follows concentration gradient, increasing volume of blood plasma and therefore blood pressure
outline the steps of the negative feedback loop for when blood pressure and blood volume is low?
1) specialized cells within the apparatus release renin (enzyme)
2) renin converts angiotensinogen into angiotensin
3) angiotensin does the two following things:
stimulates release of aldosterone which acts on nephrons to increase sodium absorption and therefore water absorption
causes constriction of blood vessels
what is the low blood pressure detector called?
juxtaglomerular apparatus