Ch 23 Respiratory System Learning Objectives & PPTs
1/94
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
95 Terms
Define the four phases of respiration
Pulmonary Ventilation, External Respiration, Gas Transport, Internal Respiration
Pulmonary Ventilation
movement of air into and out of the lungs
External respiration
exchange of gases between lungs and blood
Gas Transport
the process of carrying gases from the alveoli to the systemic tissues and vice versa
Internal Respiration
Exchange of gases between tissues of the body and the blood
Respiratory zone
where gas exchange occurs, bronchioles and alveoli
Conduction zone
Structures that simply conduct air with no gas exchange; everything but bronchioles and alveoli
Why is air filtered, warmed, and moistened in the conducting zone?
To protect delicate tissues of the respiratory system and allow for efficient gas exchange
Nasal cavity
hollow space behind the nose lined with vibrissae
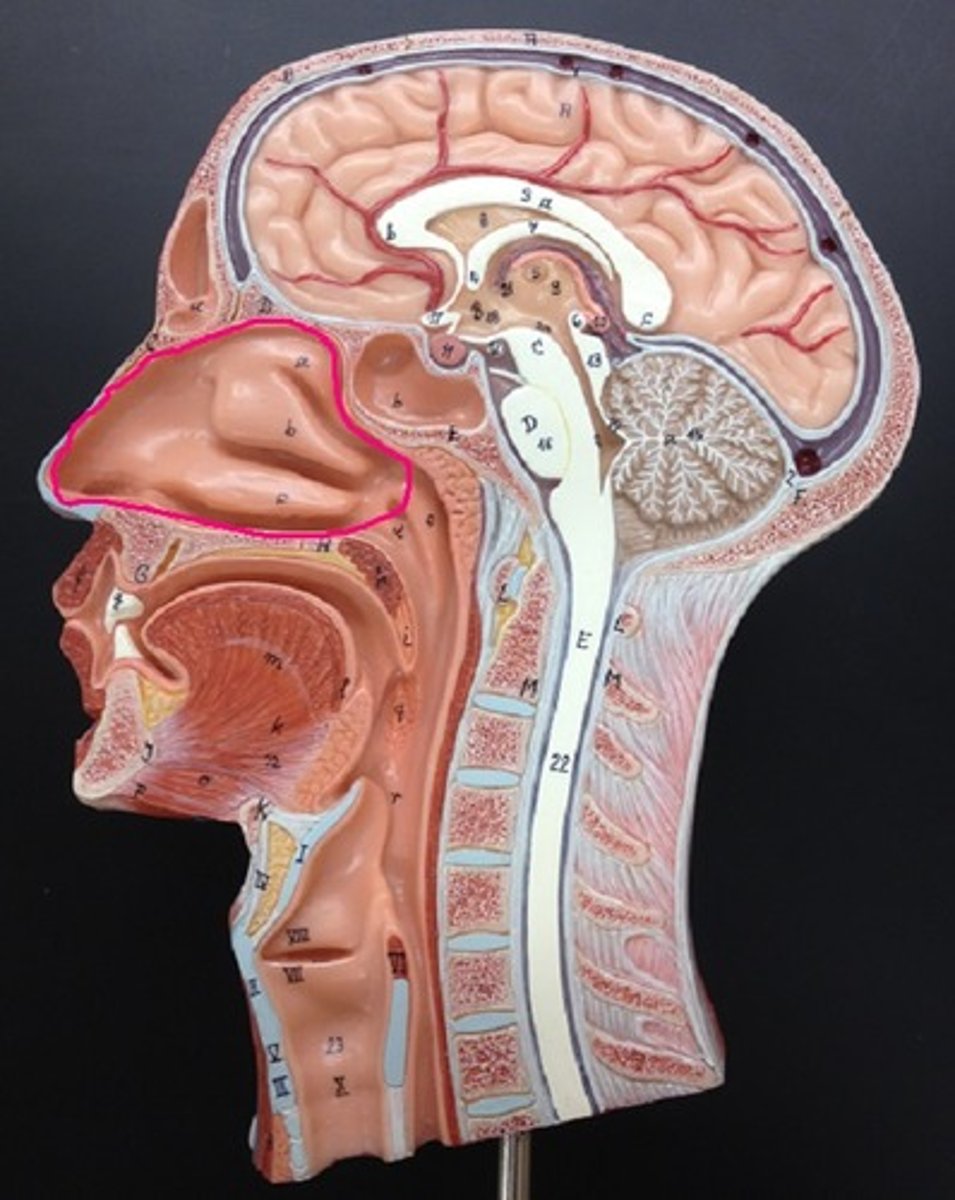
Nasal capillaries
Warm the air within the nasal cavity
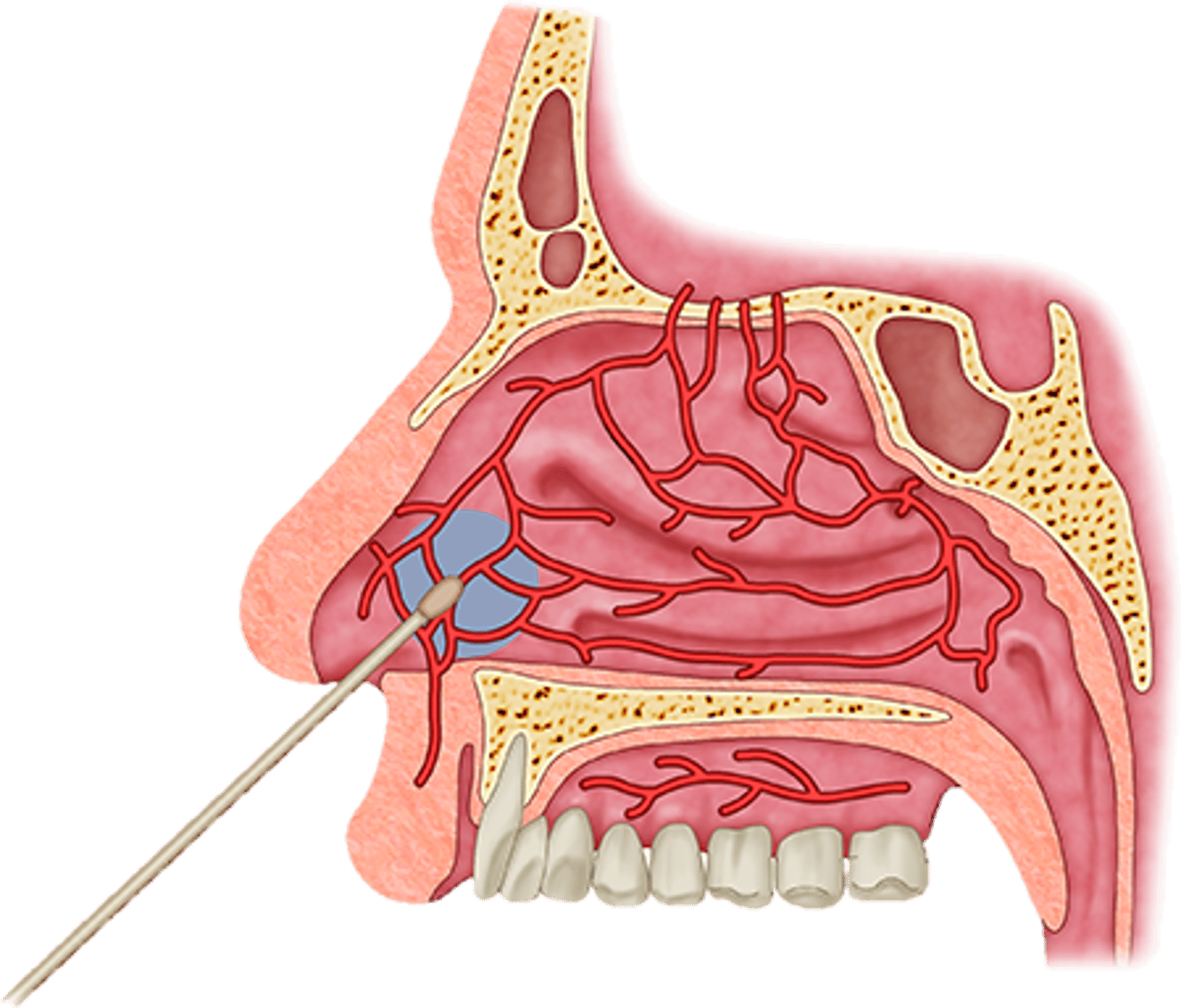
Respiratory mucosa
mucus-covered membrane that lines the tubes of the respiratory tree; filters and moistens
Nasal conchae
The scroll like ridges on the lateral walls of the nasal cavity; filter and moisten on inspiration, retain heat and moisture on expiration
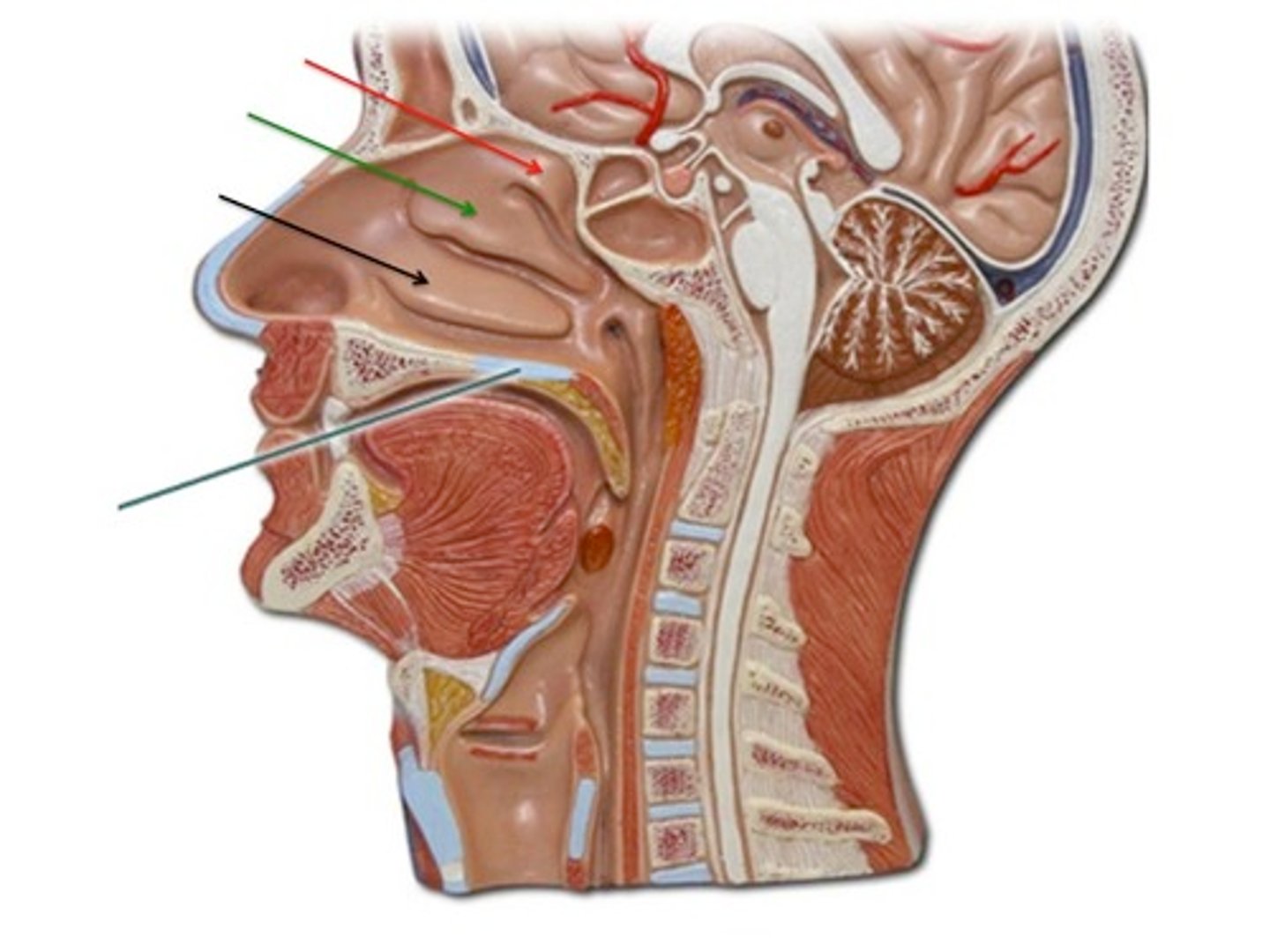
Paranasal Sinuses
Spaces within the skull bones that are lined with pseudostratified ciliated columnar epithelium; warm and moisten air, resonate voice sounds, reduce weight of skull
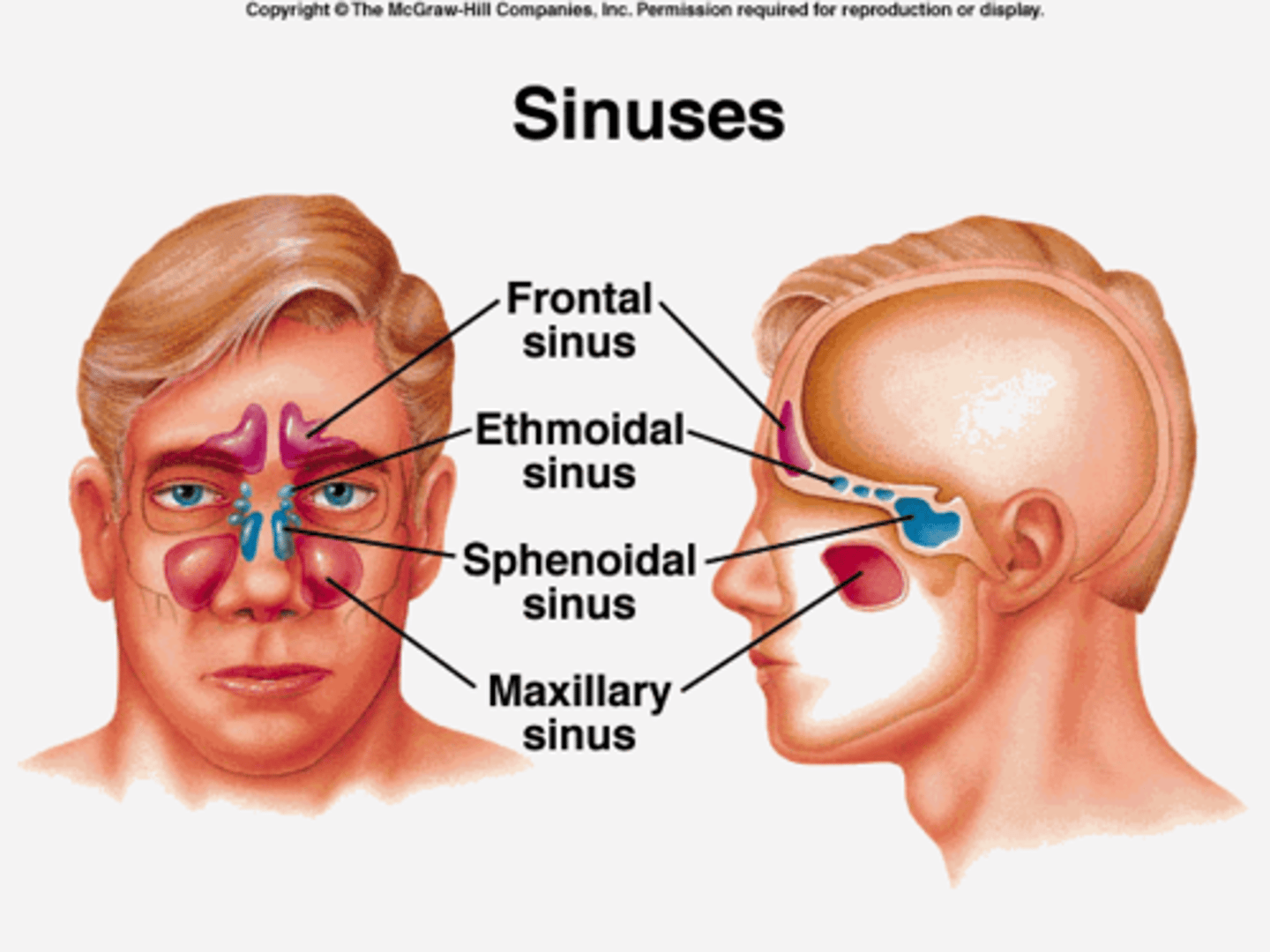
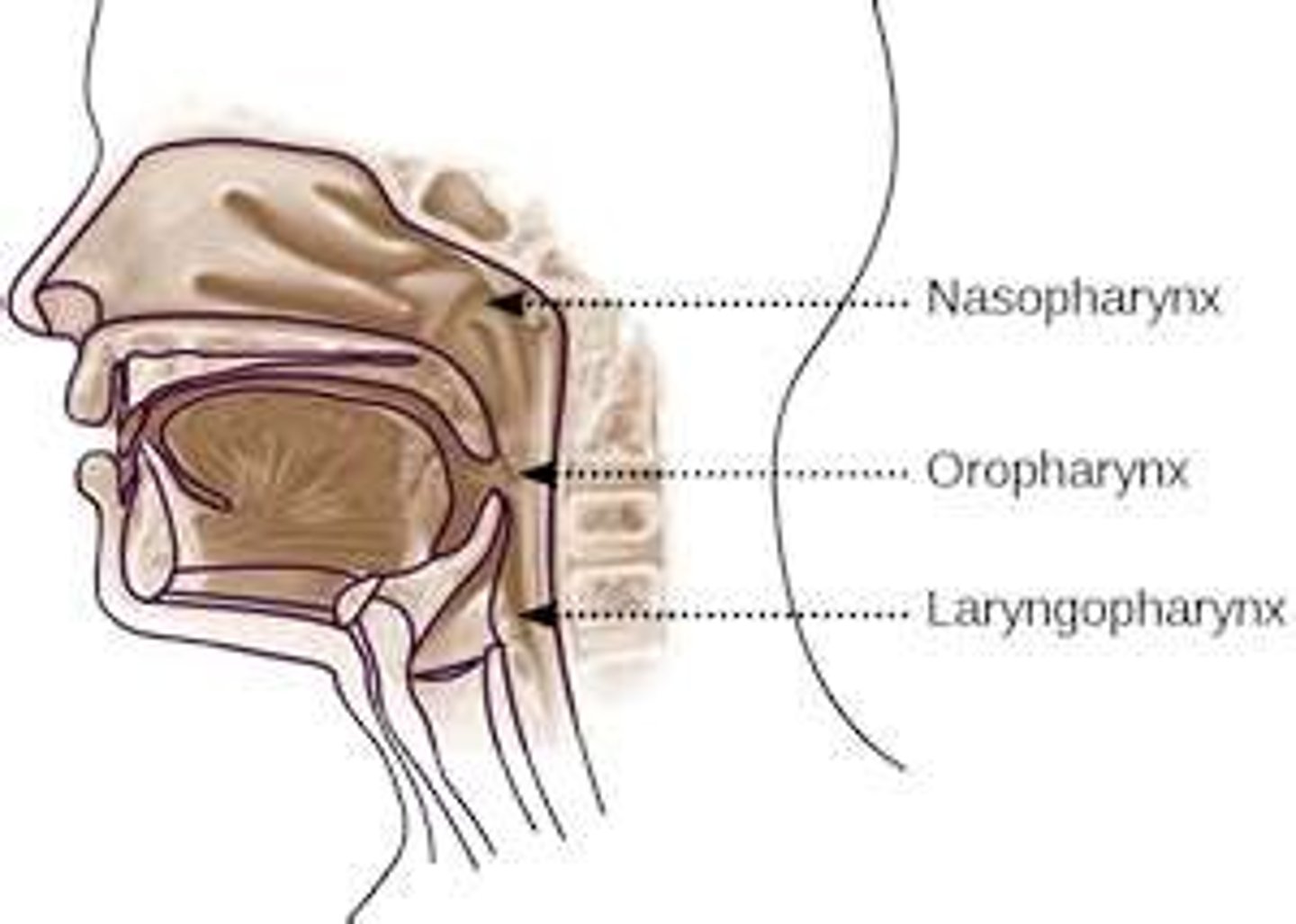
Pharynx
connects the nasal cavity, oral cavity, larynx, and esophagus; nasopharynx, oropharynx, laryngopharynx
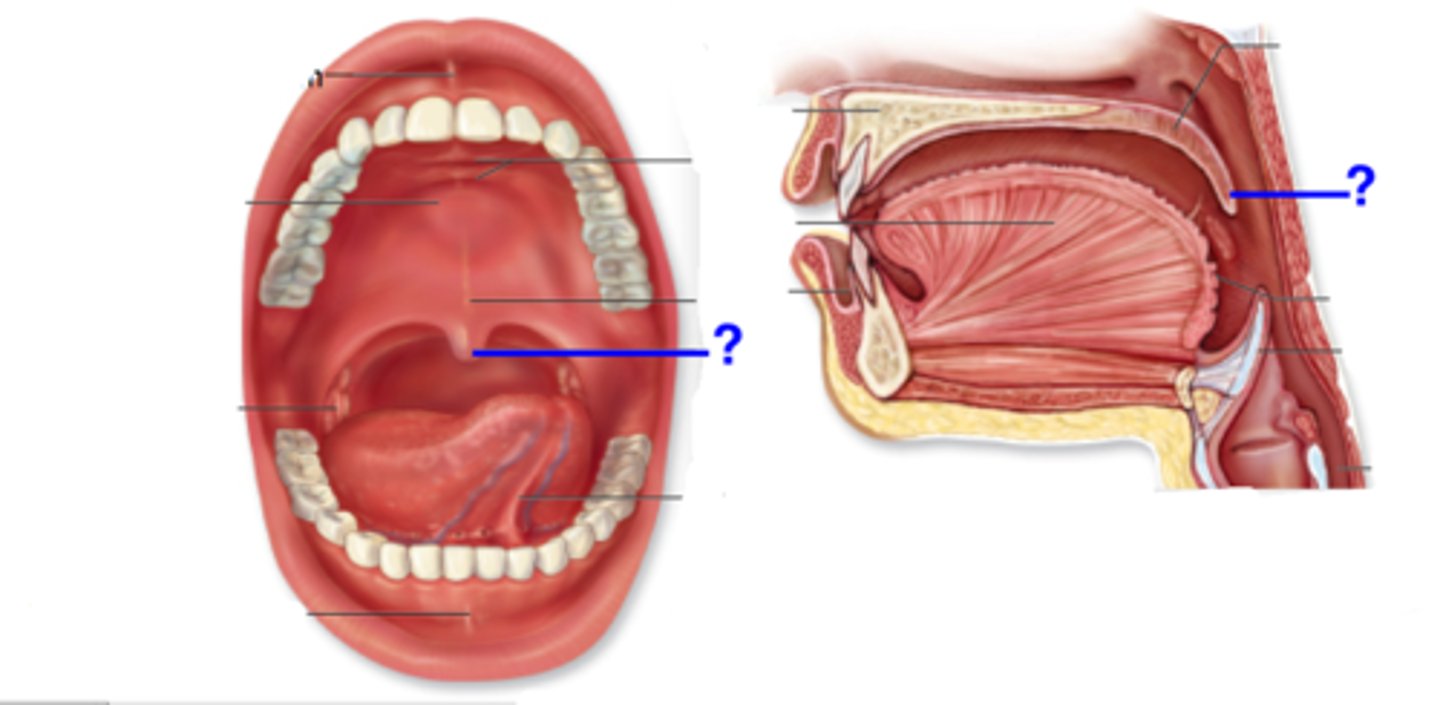
Uvula
small projection hanging from the back middle edge of the soft palate; part of pharynx
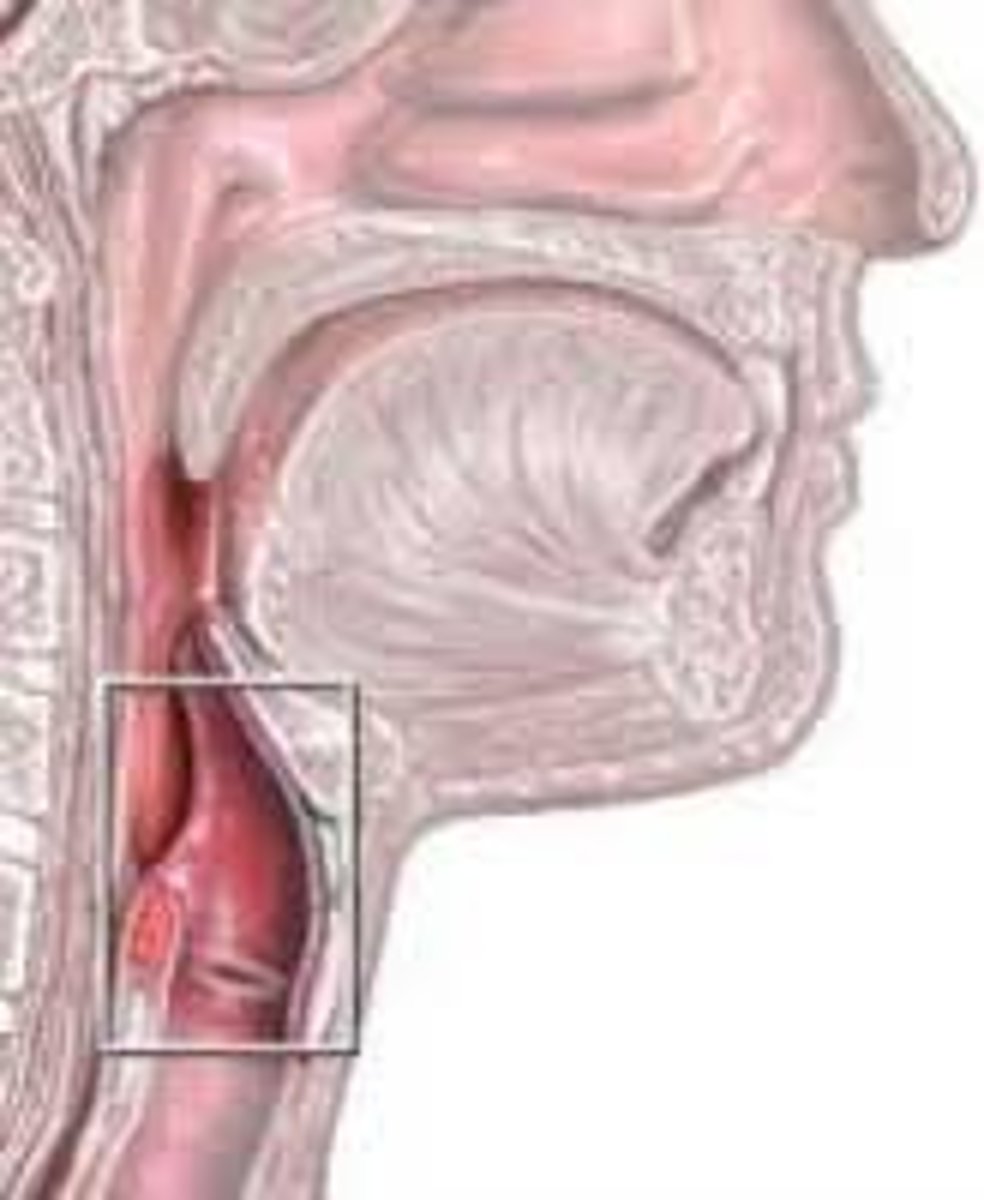
Larynx
voice box; passageway for air moving from pharynx to trachea; contains vocal cords; has cartilaginous structures and rings held together but connective tissue and muscle
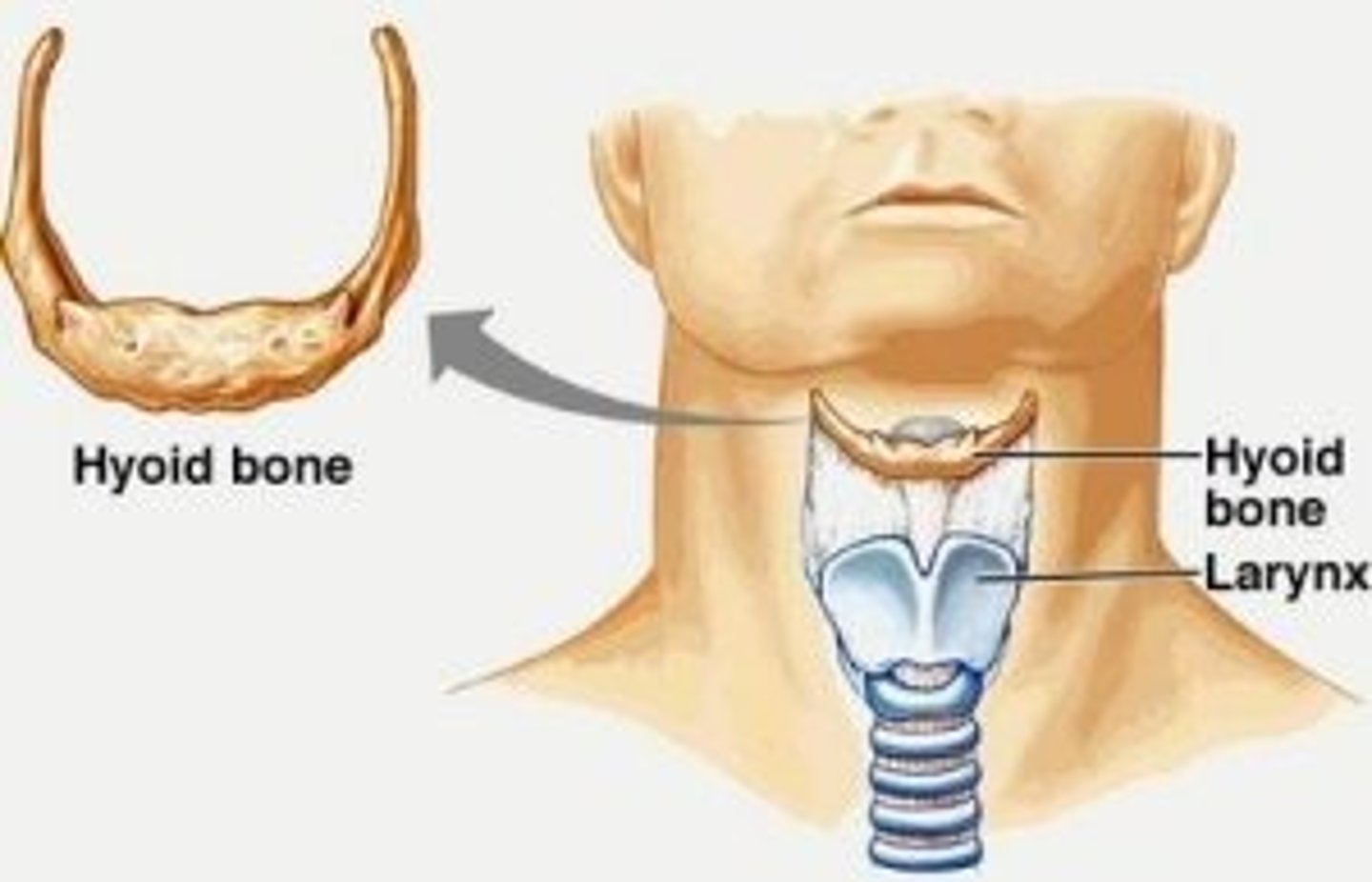
Hyoid bone
a U-shaped bone in the neck that supports the tongue; provides an attachment point for muscles of the tongue, larynx, and mandible
Epiglottis
A flap of tissue that seals off the windpipe and prevents food from entering
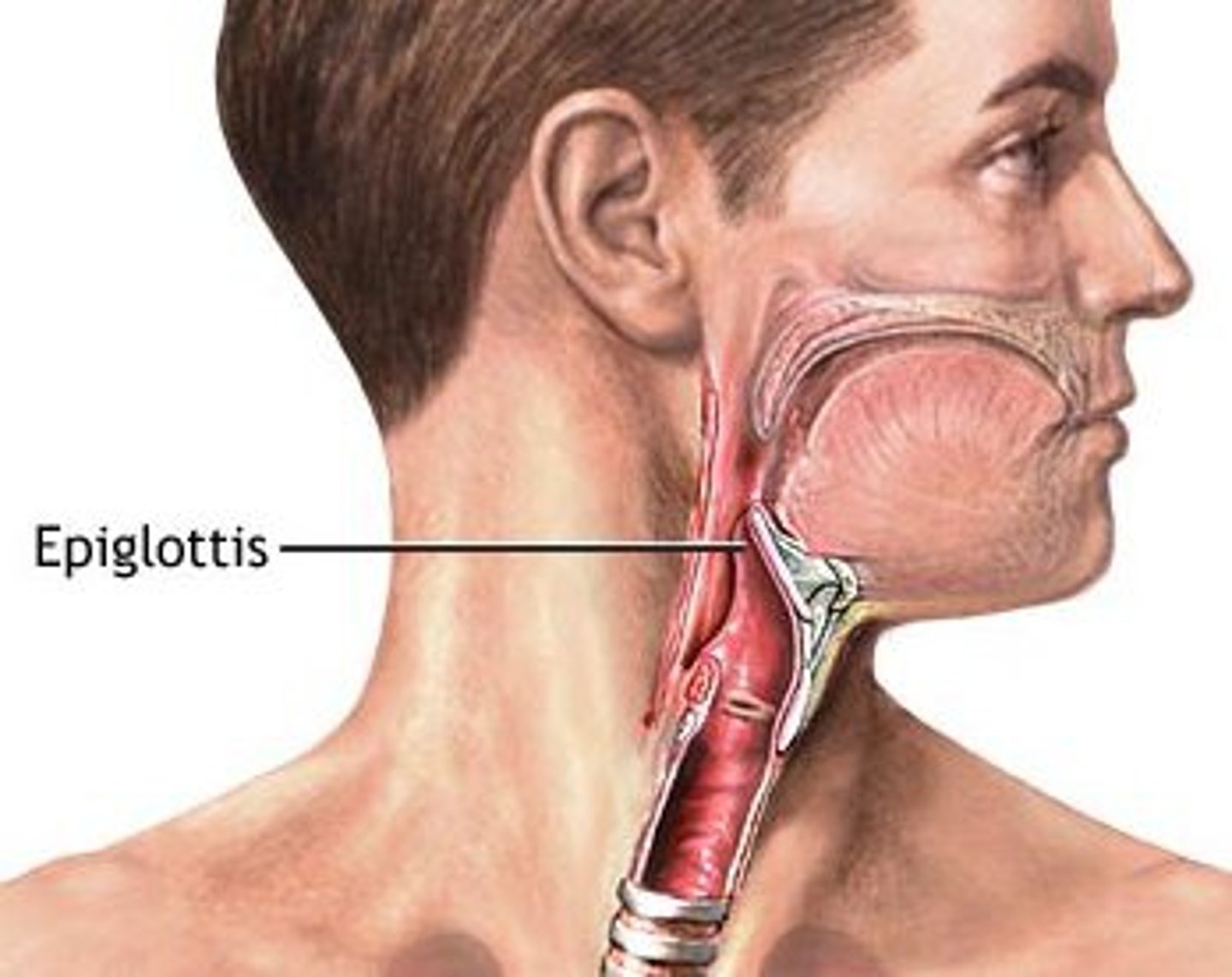
Glottis
opening between the vocal cords in the larynx
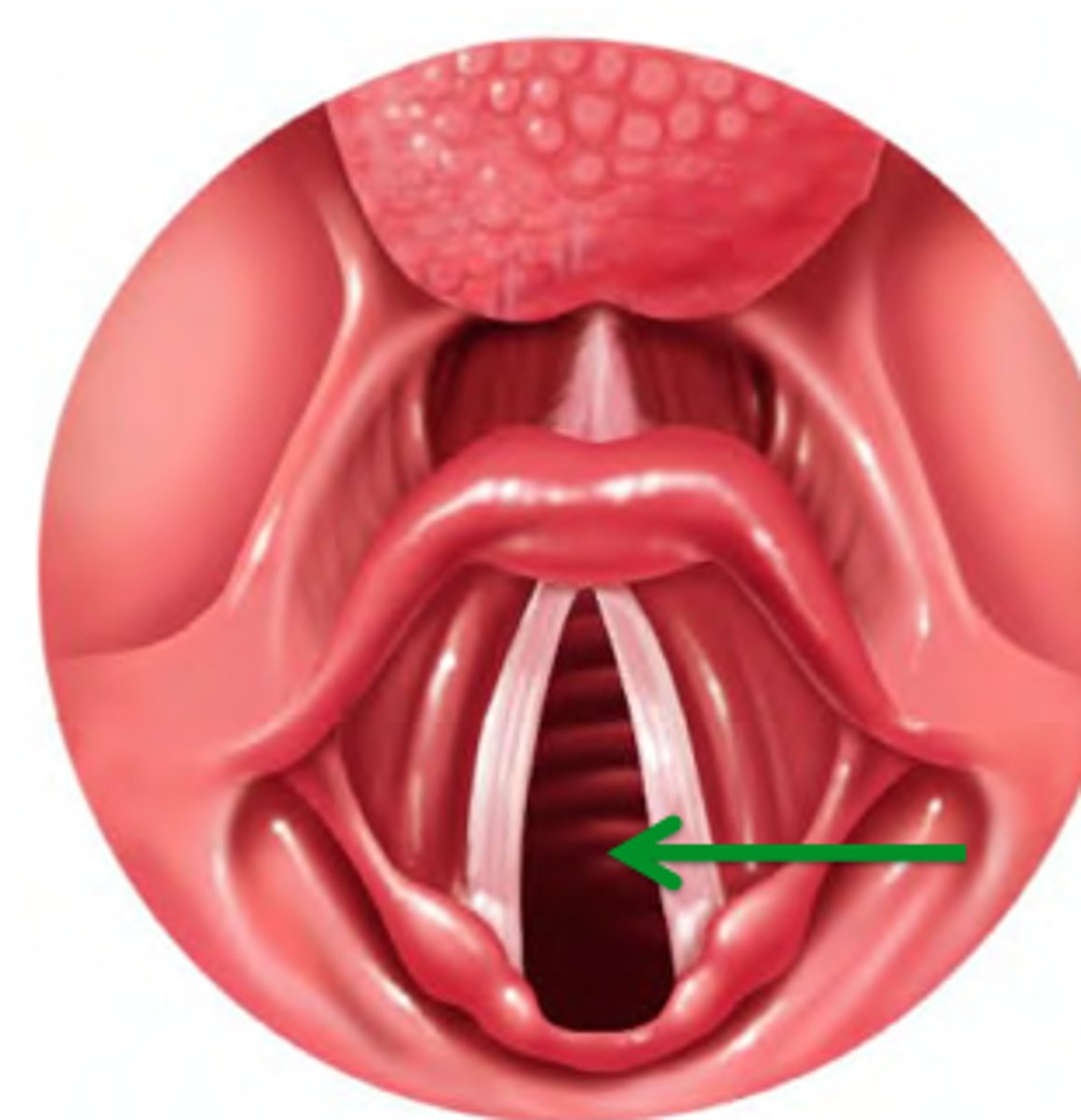
Vocal cords
folds of tissue within larynx that vibrate and produce sounds; elastic fibers that appear white due to lack of blood vessels
Vestibular folds
(false vocal cords)
Superior to vocal folds;
No part in sound production;
Help to close glottis during swallowing
Vocal ligaments
pull on cartilages of the larynx to open and close vocal folds
Trachea
windpipe; extends from larynx into mediastinum, where it divides into main bronchi
Tracheal cartilages
cartilaginous rings that stiffen the tracheal walls and protect the airway
4 Layers of trachea
-Mucosa: ciliated pseudostratified epithelium with goblet cells
-Submucosa: connective tissue with seromucous glands
-Hyaline cartilage: form rings and support trachea
-Adventitia: outermost layer made of connective tissue
Bronchial Tree
highly branched system of air-conducting passages beginning at main bronchi and ending at alveoli of lungs
Main bronchi
division of trachea which divide into each lung; primary
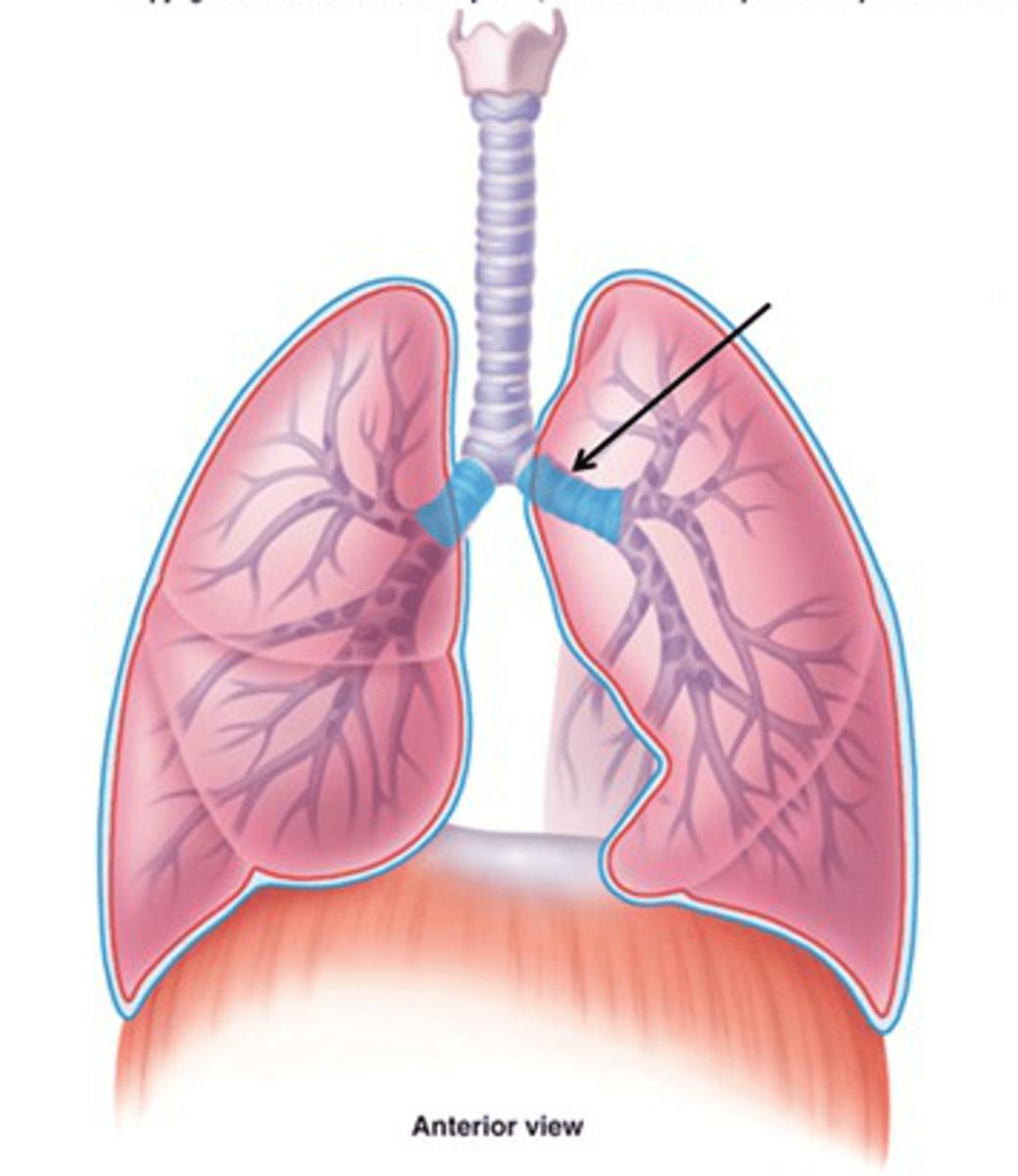
Lobar bronchi
Airway leading into specific lobe of lungs; secondary
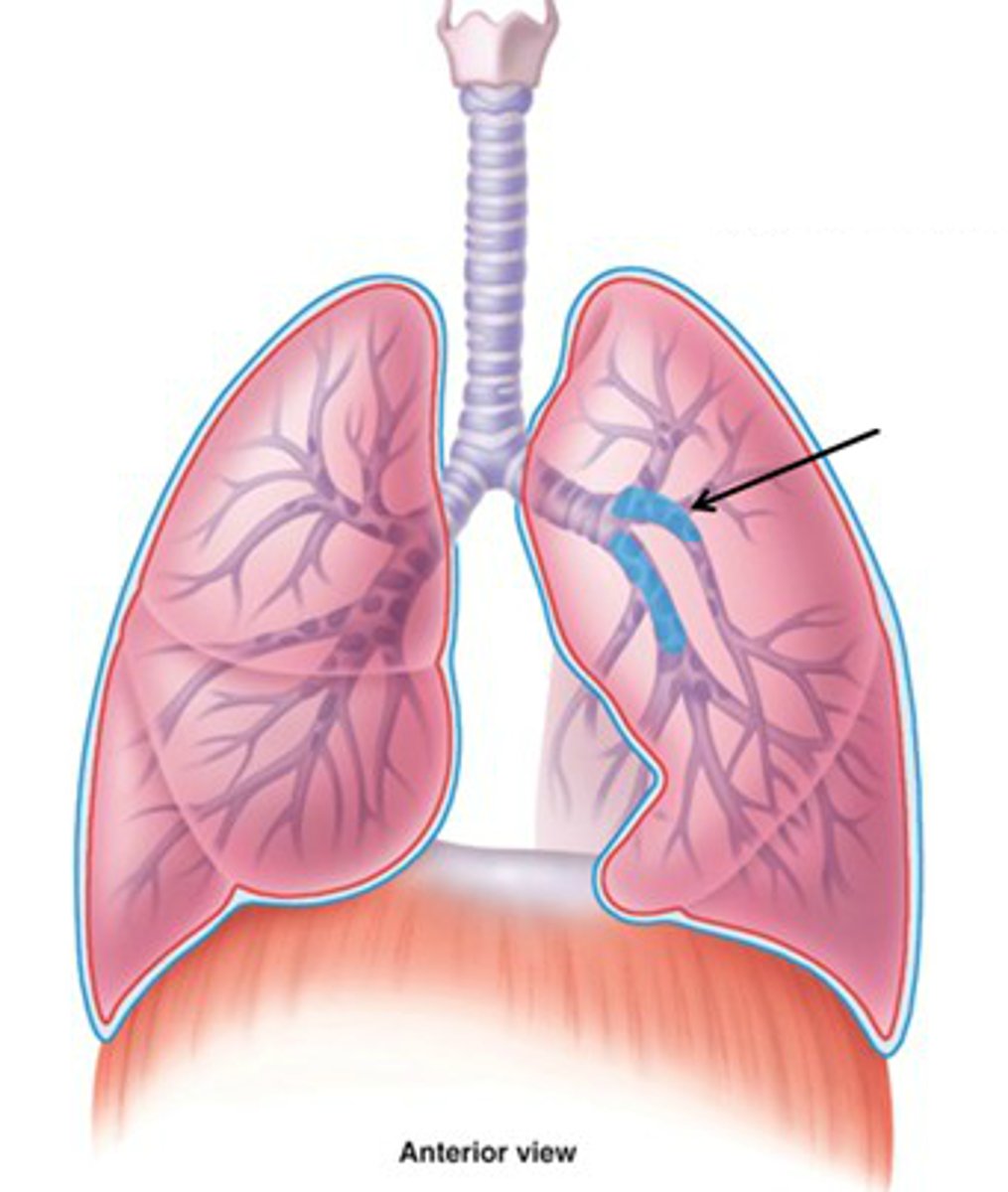
Segmental bronchi
Airways leading into specific lung segments; tertiary
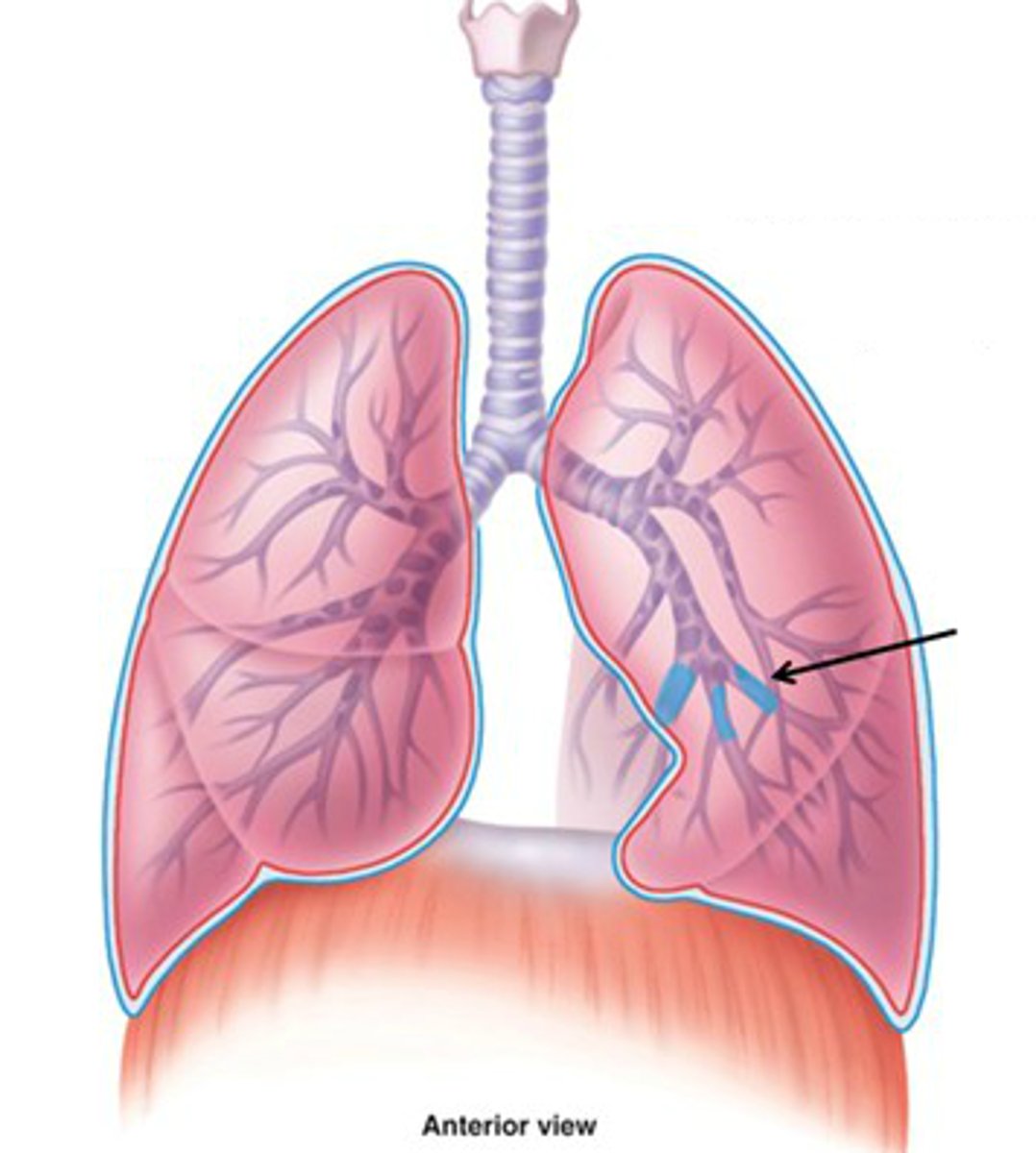
Smaller bronchi
less cartilage and more smooth muscle
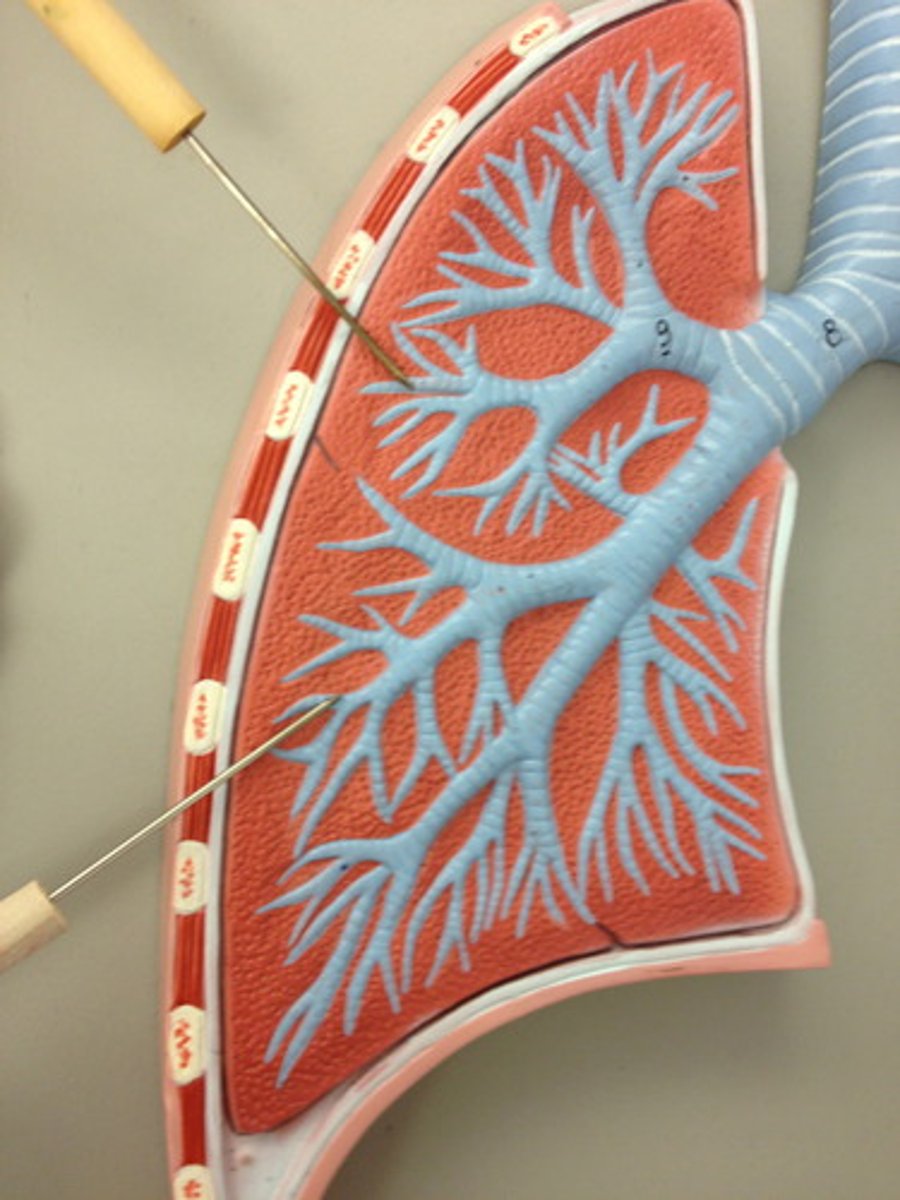
Bronchioles
smallest branches of the bronchi
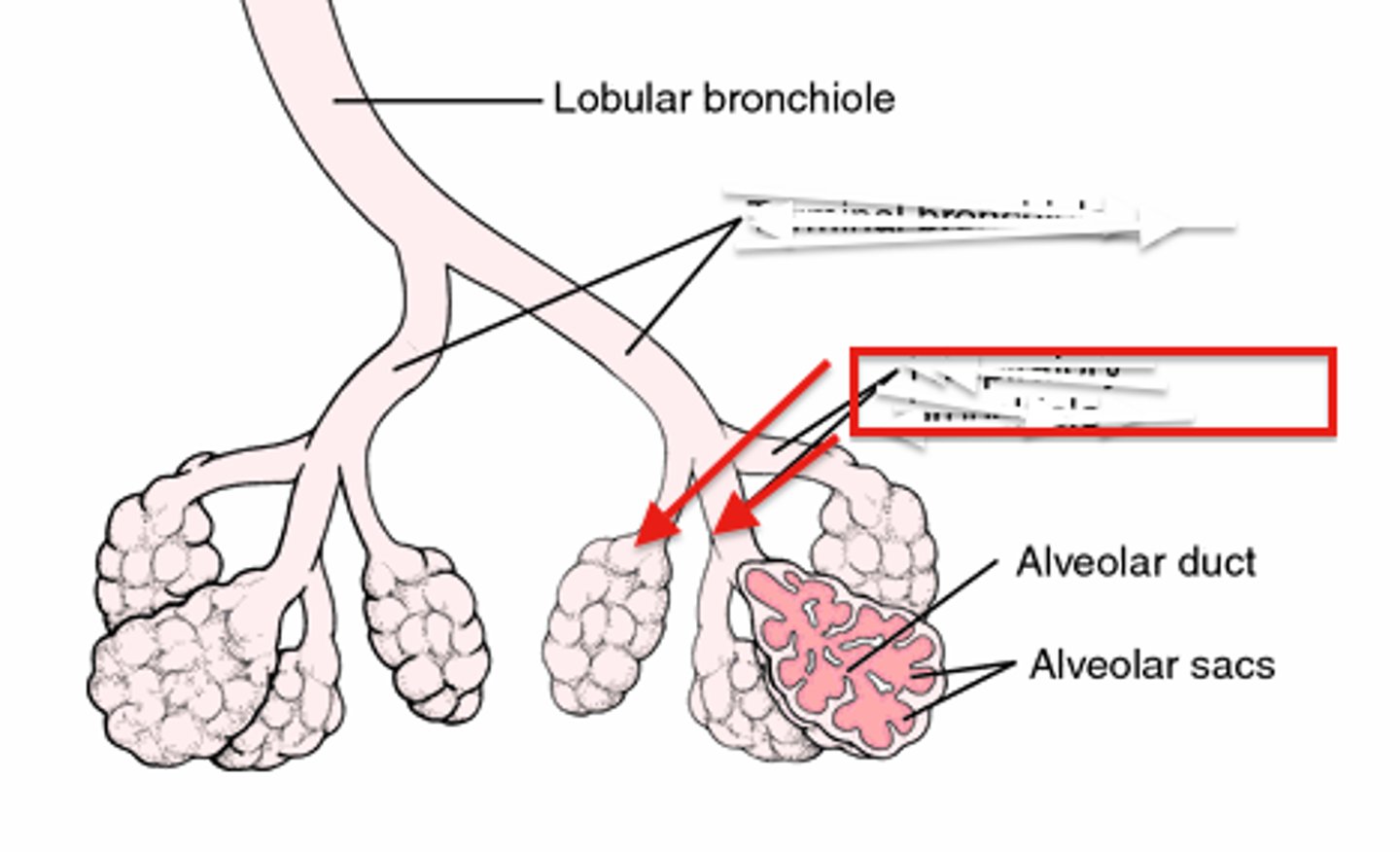
Alveoli
tiny sacs of lung tissue specialized for the movement of gases between air and blood
Alveolar pores
connect adjacent alveoli, equalize air pressure throughout lung
Alveolar type I cells
simple squamous epithelial cells; form walls of alveoli and are included in gas exchange
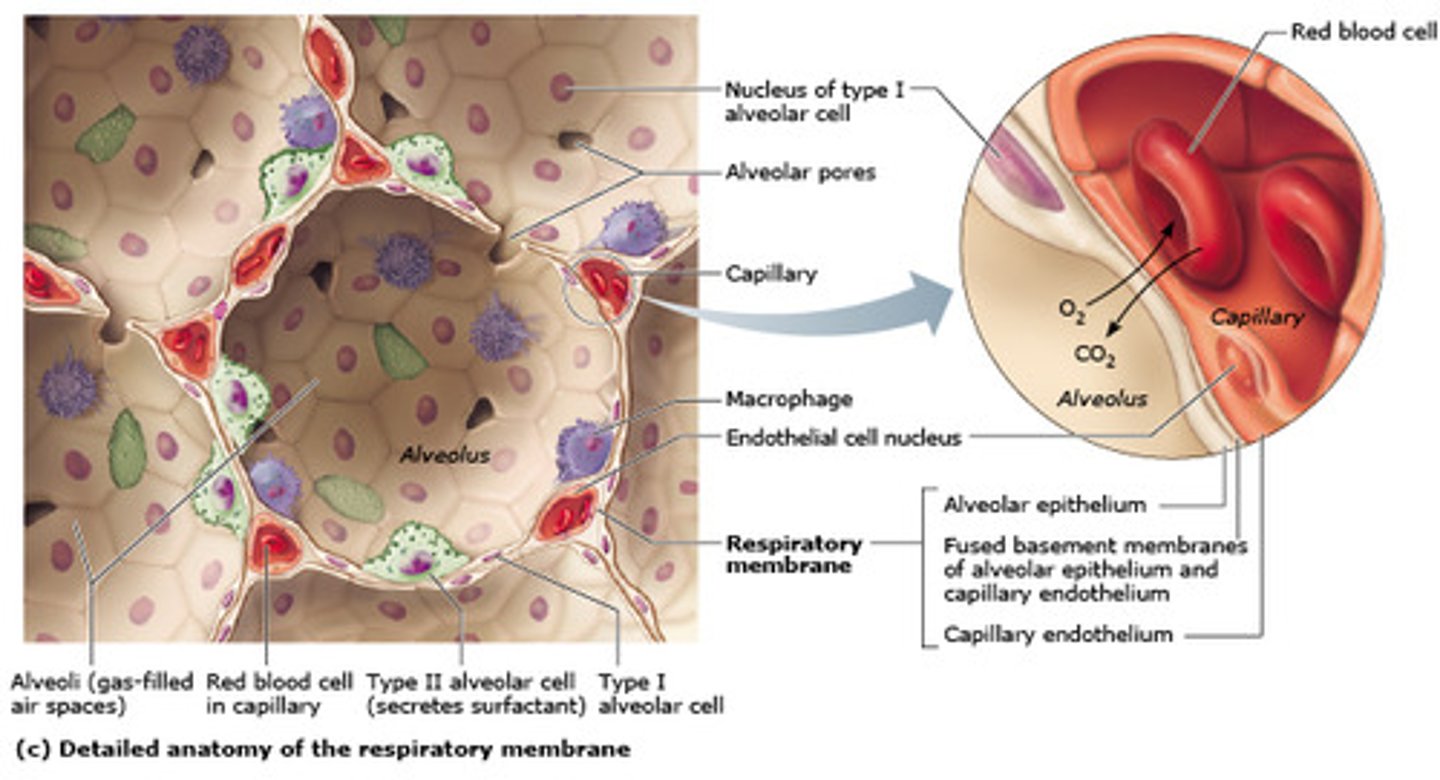
Alveolar type II cells
cuboidal epithelial cells, produce and secrete pulmonary surfactant
Changes in bronchial tree
cartilage rings become irregular plates; cilia and goblet cells become more sparse; amount of smooth muscle increases for bronchioles to provide resistance
Alveolar macrophages
phagocytose small particles in alveoli; dust cells
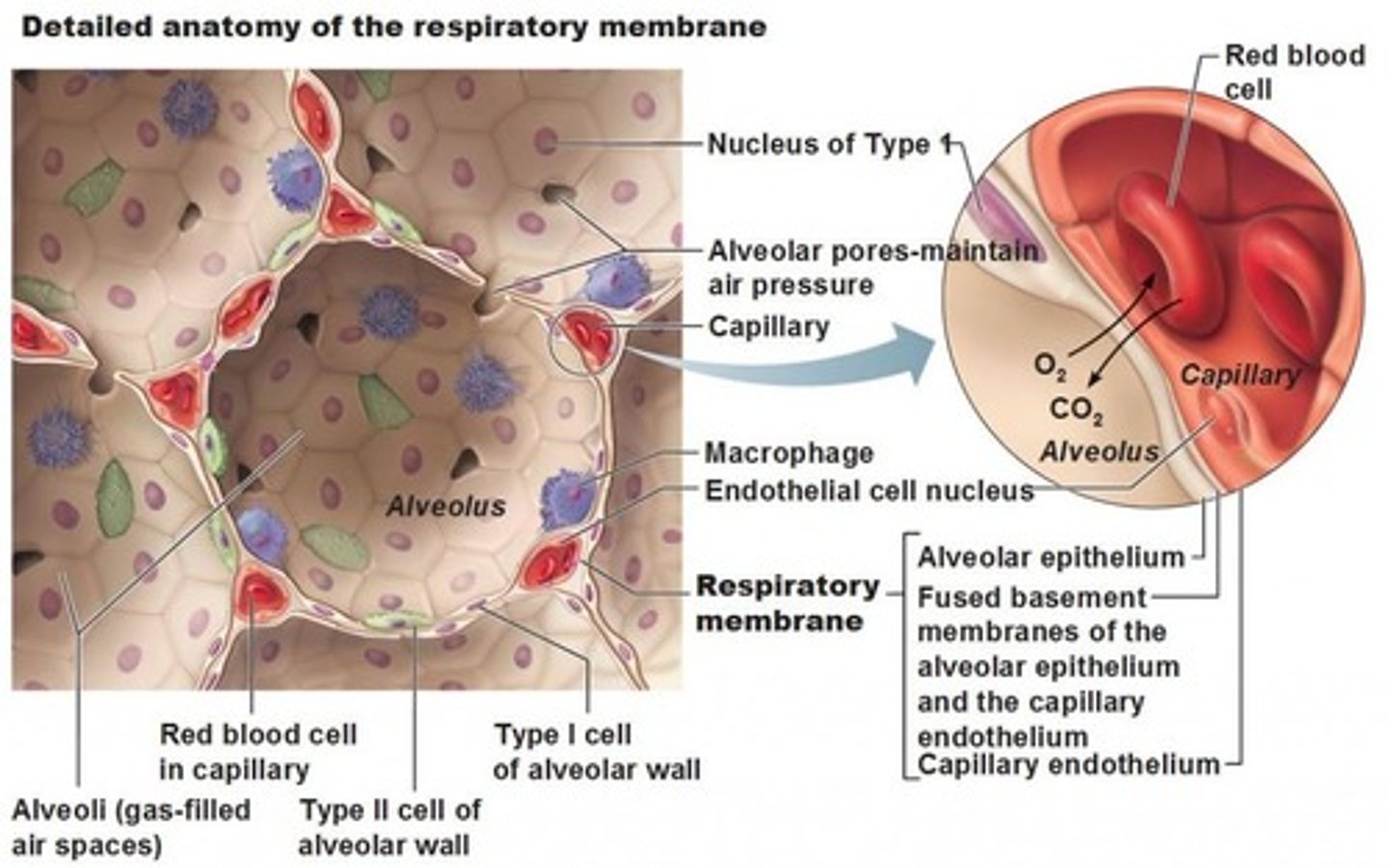
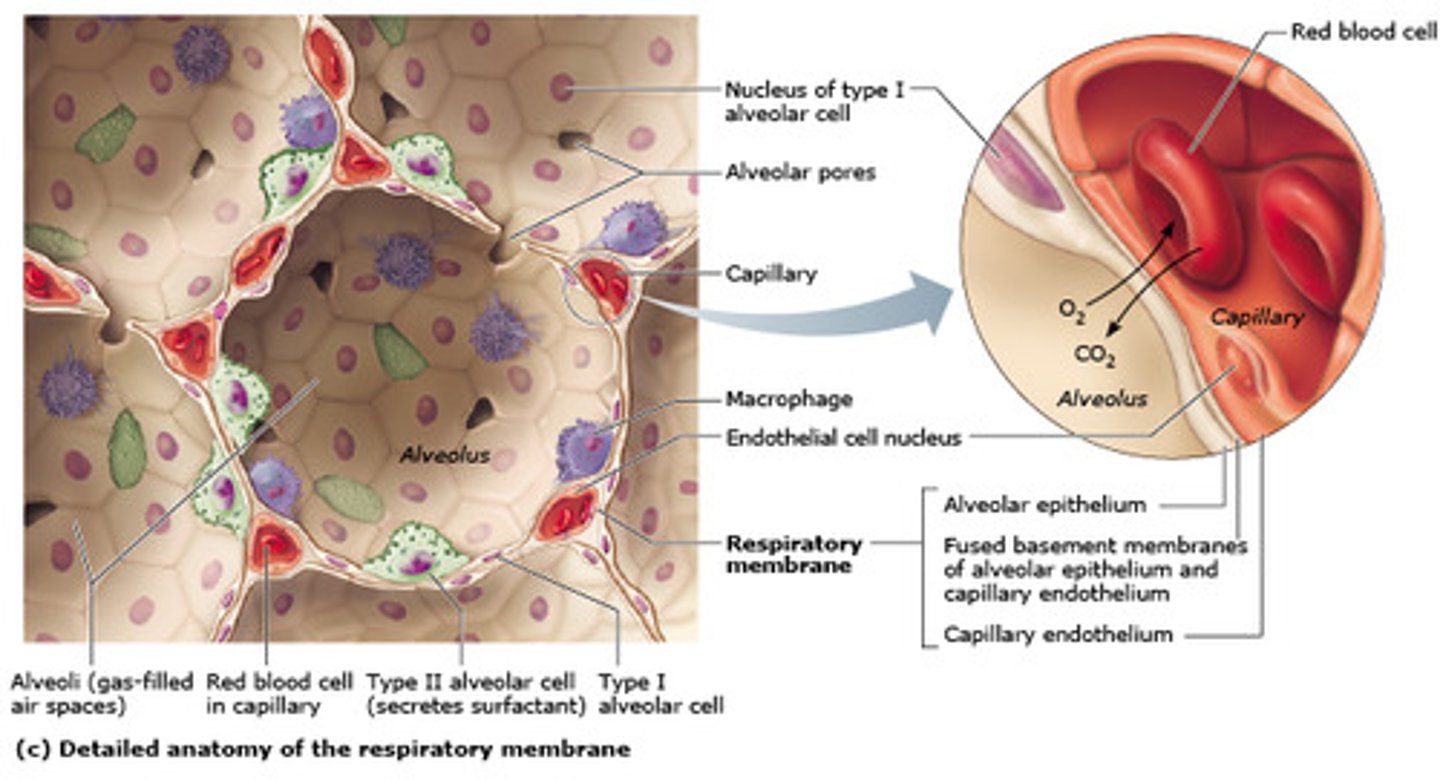
Respiratory membrane
where gas exchange occurs between the air on the alveolar side and the blood on the capillary side; the alveolar and capillary walls form the respiratory membrane
Pleural membranes
double-layered serous membrane surrounding each lung; pleural fluid lies between
Pulmonary arteries
carry deoxygenated blood out of the right ventricle and into the lungs
Bronchiole arteries
provide oxygenated blood to lung tissue
Innervation of Respiratory structures
lungs are innervated by parasympathetic and sympathetic nervous system
Innervation of respiratory muscles
respiratory muscles are innervated by motor fibers of somatic nervous system
Parasympathetic fibers
cause bronchoconstriction via vagus nerve
Sympathetic fibers
cause bronchodilation via sympathetic chain ganglion
Motor fibers
innervate intercostal muscles (intercostal nerves) and diaphragm (phrenic nerve)
Atmospheric pressure
the pressure caused by the weight of the atmosphere
Intrapulmonary pressure
pressure in the alveoli
Intrapleural pressure
pressure in the pleural cavity surrounding the lungs that sucks lung outward; should always be negative
How do pulmonary pressures keep lungs from collapsing?
Intrapleural pressure must be negative and intrapulmonary pressure cannot be zero
How do pulmonary pressures change with inspiration
Intrapleural pressure decreases (becomes less negative), intrapulmonary pressure decreases to -1mmHg of atmospheric pressure
How do pulmonary pressures change with expiration
Intrapleural pressure increases (becomes more negative), intrapulmonary pressure increases to +1mmHG of atmospheric pressure
Boyle's Law
A principle that describes the relationship between the pressure and volume of a gas; if volume increases, pressure decreases; if volume decreases, pressure increases
Respiration
the process involved in supplying the body with oxygen and disposing of carbon dioxide
Muscles of quiet breathing
diaphragm and external intercostals
Muscles of forced inspiration
sternocleidomastoid, pectoralis major, erector spinal
Muscles of forced expiration
internal intercostals, abdominal muscles
How do changes in volume of thoracic cavity affect pulmonary inspiration and expiration
inspiration: muscles of quiet breathing contract, volume of thoracic cavity increases, pressure decreases, and air flows in
expiration: muscles of quiet breathing relax, volume of thoracic cavity decreases, pressure increases, air forced out
Dorsal respiratory group
integrates input from chemoreceptors and other sensory receptors
Ventral respiratory group
generates rhythm by firing during inspiration and expiration; sends impulses to the diaphragm and intercostal muscles; when VRG output stops, muscles relax and recoil
3 Factors that influence pulmonary ventilation
Airway resistance;
Alveolar surface tension;
Lung compliance
Factors that increase airway resistance
increased bronchoconstriction; loss of surfacant; reduced lung compliance
Alveolar surface tension
-Attracts liquid molecules to one another at a gas-liquid interface
Alveolar film
contains surfactant which decreases the cohesiveness of water molecules to prevent the walls of alveoli from sticking together
Lung compliance
the measure of change in lung volume that occurs with a given change in transpulmonary pressure; a measure of "stretch" the lung has
Spirometry
a measurement of breathing (or lung volumes)
Tidal volume
Amount of air that moves in and out of the lungs during a normal breath
Residual volume
Amount of air remaining in the lungs after a forced exhalation
inspiratory reserve volume
The amount of air that can be inhaled after a normal inhalation; the amount of air that can be inhaled in addition to the normal tidal volume.
expiratory reserve volume
Amount of air that can be forcefully exhaled after a normal tidal volume exhalation
Alveolar ventilation rate
the volume of air per minute entering alveoli
AVR Formula
AVR = RR(TV-DS)
Dalton's Law of Partial Pressures
states that the total pressure of a mixture of gases is equal to the sum of the pressures of all the gases in the mixture
Partial Pressure of O2 in alveolar air
high
Partial pressure of O2 in alveolar capillary bed
low
Partial pressure of O2 in arterial blood
high
Partial pressure of O2 in venous blood
low
Partial pressure of CO2 in alveolar air
low
Partial pressure of CO2 in alveolar capillary bed
high
Partial pressure of CO2 in arterial blood
low
Partial pressure of CO2 in venous blood
high
2 Ways oxygen is carried in blood
1) 99% bound to hemoglobin - this represents oxygen saturation of Hgb
2) 1.5% is dissolved in the plasma
Henry's Law
gases dissolve the same in fluid as in gases
Hemoglobin dissociation curve
shows how saturated Hb is at various partial pressures of O2
Oxygen-Hemoglobin saturation in lungs
PO2 high, Hb 99% sat
Oxygen-Hemoglobin saturation in tissue at rest
PO2 low, Hb 75% sat
Oxygen-Hemoglobin saturation in tissues during exercise
PO2 low, Hb 35%, muscles pull O2 from blood
3 ways CO2 is transported in the blood
1) freely dissolved in blood as carbon dioxide
2) bound to globin portion of hemoglobin
3) freely dissolved in blood plasma as bicarbonate
Conversion of CO2 in systemic capillaries
1) CO2 enters RBC
2) CO2 is combined with H2O by enzyme carbonic anhydrase to form bicarbonate
3) bicarbonate diffuses into plasma, in exchange, Cl- ion enters RBC (chloride shift)
Conversion of CO2 in pulmonary capillaries
1) Bicarbonate diffuses into RBC, in exchange, Cl- ion transported out of RBC (chloride shift)
2) Bicarbonate binds to free H+ ion, producing H3CO3, this molecule is broken into H2O and CO2 by carbonic anhydrase
3) CO2 exits RBC, diffuses into alveolus for expiration
carbonic acid-bicarbonate buffer system
chemical system that helps maintain pH homeostasis of the blood
Increasing pH
bicarbonate mops up free H+ ions to become carbonic acid, increases pH
Decreasing pH
carbonic acid dissociates to release H+, decreases pH
Slow/Shallow breathing
CO2 accumulates, carbonic acid accumulates, dissociates more H+, pH decreases
Rapid/Deep breathing
more CO2 blown off, less carbonic acid, H+ binds to bicarbonate, pH increases