Diseases of the Lacrimal System + Miscellaneous
1/72
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
73 Terms
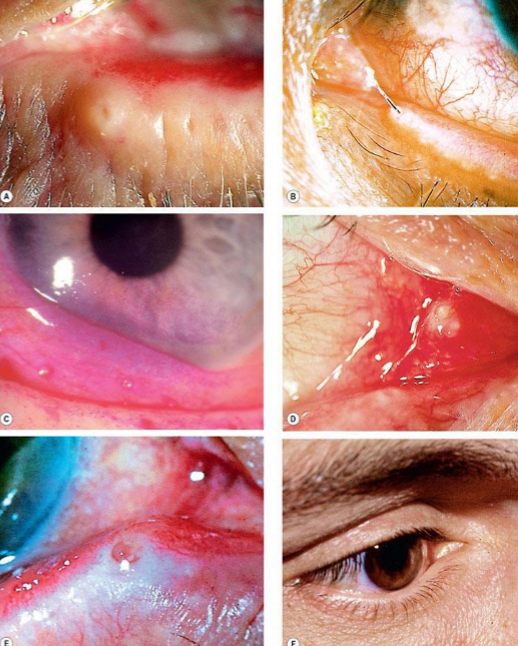
What are the causes of epiphora?
Hypersecretion
Ocular surface irritation or inflammation
Infectious conjunctivitis
Entropion
Trichiasis
Defective drainage
Malposition
Obstruction
Lacrimal pump failure

Evaluate the tear meniscus height prior to eyelid manipulation or instillation of medication
Patients with c/o excessive tearing = high meniscus
Normally, little to no dye remains after 5 minutes
Prolonged retention is indicative of inadequate lacrimal drainage and can be graded from 1-4
Fluorescein disappearance test
Indicated in patients with suspected partial obstruction of the drainage system
Jones dye testing
If dye is present on Jones I is that a positive or negative test?
Positive
Identifies the probable site of partial obstruction
Jones II
If fluorescein dye is passed during Jones II, is that positive or negative?
Positive
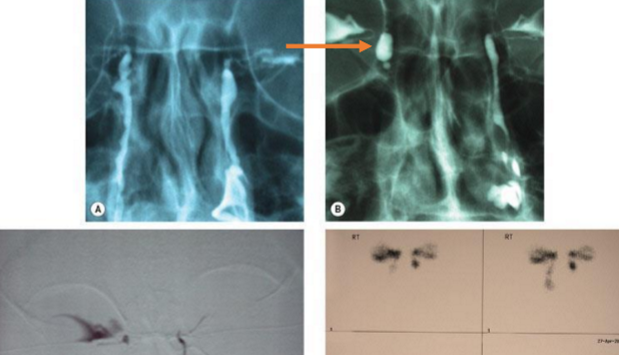
Injection of radio-opaque contrast medium into the canaliculi followed by capture of magnified images.
Indications: confirm site of lacrimal drainage obstruction
Technique:
Inferior puncta dilated
Plastic catheters inserted into inferior canaliculi
Contrast medium injected
Radiographs taken
Interpretation
Failure of dye reaching nose = anatomical obstruction
Contrast dacryocystography
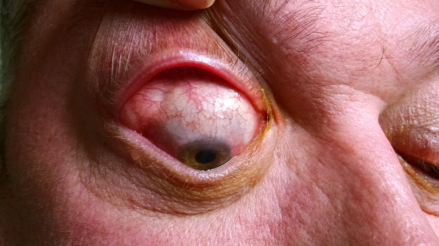
Inflammation of the lacrimal gland
Acute
Chronic
Infectious or inflammatory
Pathophysiology not completely understood
Dacryoadenitis
Causes of viral infectious acute dacryoadenitis…
Mumps (common previously, especially in childhood)
Epstein-Barr virus
Herpes zoster
Mononucleosis
Cytomegalovirus
Echoviruses
Coxsackievirus A
May result in severe dry eye due to lacrimal gland fibrosis
Causes of bacterial, fungal, and parasitic infectious acute dacryoadenitis…
Bacterial (less common)
Staphylococcus aureus and Streptococcus
Neisseria gonorrhoeae
Treponema pallidum
Chlamydia trachomatis
Mycobacterium leprae
Mycobacterium tuberculosis
Haemophilus
Moraxella
Pseudomonas
Fungal (rare)
Histoplasmosis
Blastomycosis
Parasitic (rare)
Schistosoma haematobium
Acute dacryoadenitis symptoms
Unilateral pain
Redness
Swelling (outer 1/3 of upper lid)
Tearing
Discharge
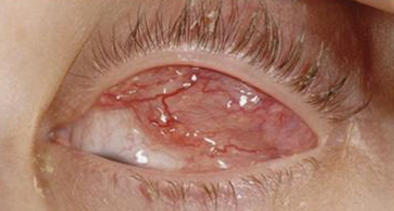
Acute dacryoadenitis signs
Erythema
Swelling
Tenderness
Hyperemia of palpebral lobe of lacrimal gland
Prolapsed and enlarged
S-shaped upper lid
Fever — need CBC
Elevated WBC
Conjunctival injection and chemosis
Lymphadenopathy
Proptosis
EOM restriction
Parotid gland enlargement
Upper respiratory infection
Malaise
Chronic dacryoadenitis etiology (inflammatory)
Sarcoidosis
Wegener’s granulomatosis
Graves’ disease
Sjogren’s syndrome
Orbital pseudotumor
Benign lympho-epithelial lesion
Chronic dacryoadenitis clinical manifestations…
Can be bilateral
Painless enlargement of the lacrimal gland present for more than a month
More common than acute
Less severe presentation than acute
Enlarged gland but motile
Minimal ocular signs
Mild ptosis
Mild to severe dryness
How do we manage dacryoadenitis?
CT scan for both acute and chronic
Should see enlargement of the gland, but NO changes to the bone or globe
Suspect tumor if there is
Viral (most common): self limiting
Cool compress
NSAID
Bacterial or infectious:
Keflex
Adults: 250-500mg PO qid 10-14 days
Children: 25-50mg/kg/day PO qid
Augmentin
Adults: 250-875mg bid 5-7 days
Children: 20mg/kg/day to 40mg/kg/day for no more than 10 days
Inflammatory: investigate
Consider biopsy
Narrowing, occlusion, closure of the punctum
Occurs in the absence of punctal eversion
Primary punctal stenosis
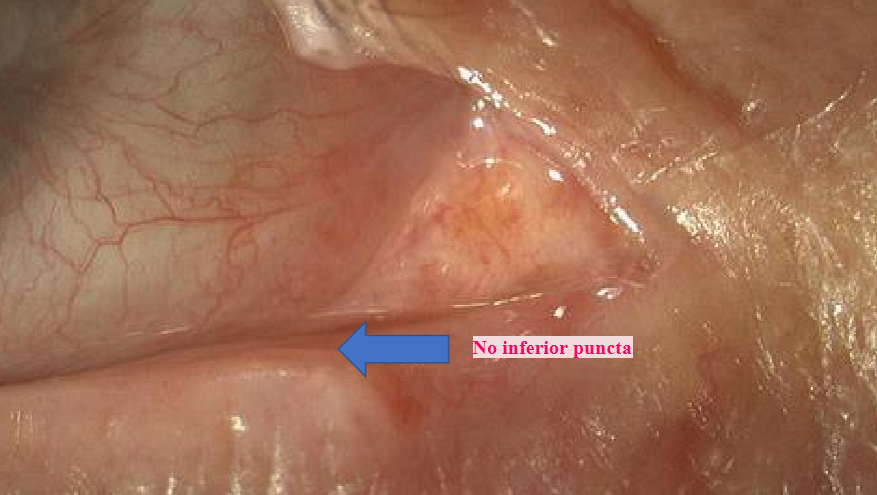
Causes of primary punctal stenosis…
Chronic blepharitis
Idiopathic
HSV HZO
How do we treat primary punctal stenosis?
Dilation
Punctoplasty
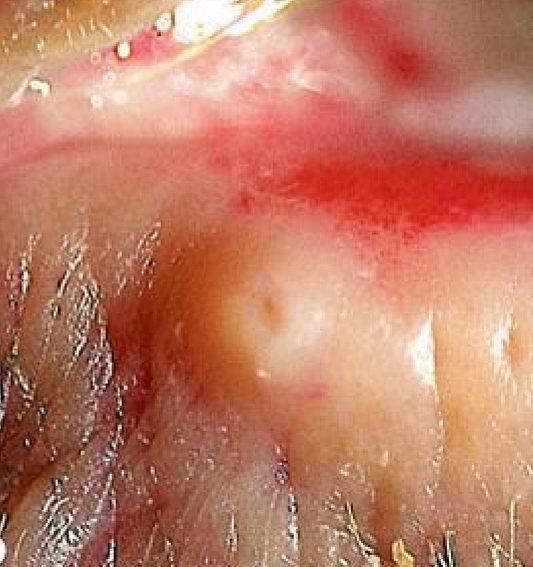
Causes of secondary punctal stenosis…
Punctal eversion
Treatment of secondary punctal stenosis…
Ziegler cautery
Medial conjunctivoplasty
Lower lid tightening
What are the causes of canalicular obstruction?
Congenital
Trauma
Herpes simplex infection
Drugs
Irradiation
Chronic dacryocystitis
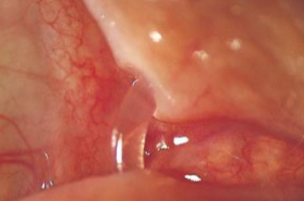
How do we treat canalicular obstruction?
Intubation with stents (3-6 months)
What causes canaliculitis?
Bacteria, fungi, or viruses (actinomyces israelii bacteria)
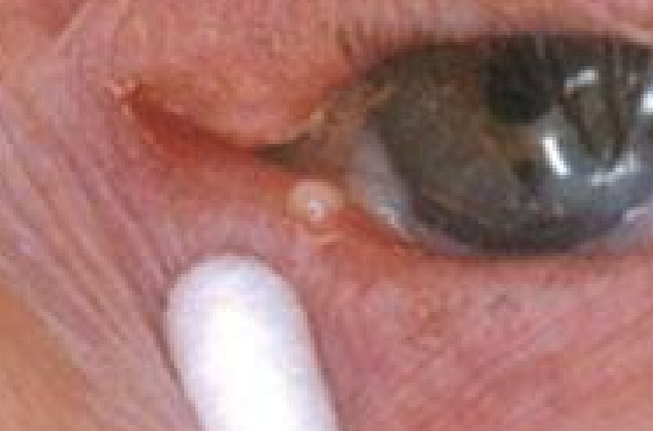
Unilateral epiphora
Redness
Blurry vision
Discomfort
Swollen punctum
Mucopurulent conjunctivitis
Canaliculitis
What are the signs of canaliculitis?
Pounting punctum
Edema of the canaliculitis
Discharge on pressure
Concretions
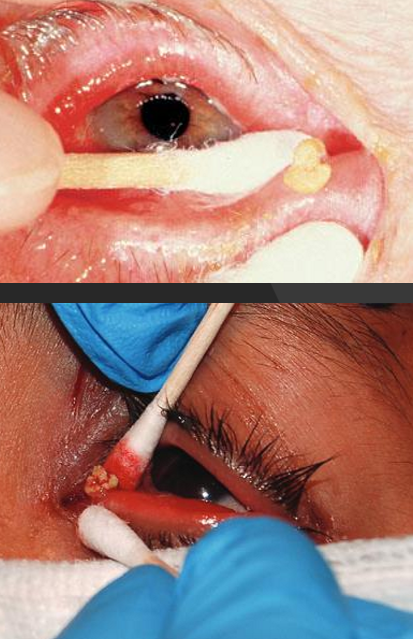
How do we treat canaliculitis?
NEVER D&I
Antibiotics (oral)
Keflex 250-500mg qid 10-14 days
Augmenting 250-875 bid 5-7 days
Topical steroids
Lotemax qid
Canaliculotomy
Linear incision into the conjunctival side of the canaliculitis and curetting of the concretions
Stenting
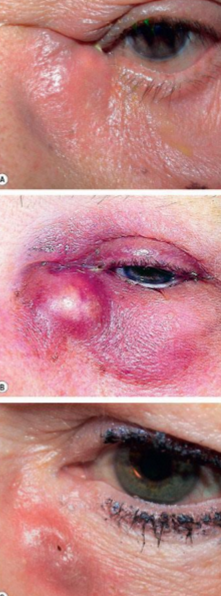
Infection or inflammation of the lacrimal sac
Usually secondary to obstruction
Dacryocyctitis

Frequent complication of congenital dacryostenosis
Subacute (mild to moderate tenderness on palpation)
Chronic (painless) presentation for weeks to months
May be unilateral or bilateral
Congenital Dacryocystitis
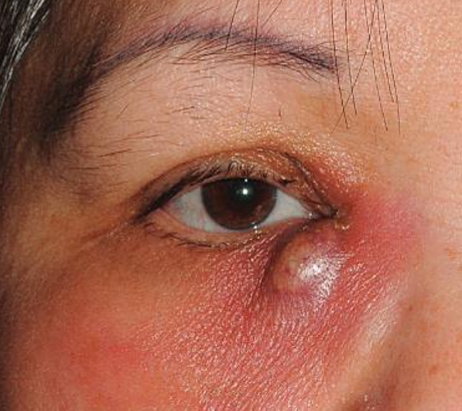
Unilateral
Acute onset with moderate to severe pain
Epiphora
Tenderness
Diffuse pain around eye and orbit (headache)
May present with pain only on firm palpation of inner canthus
Acquired Dacryocystitis
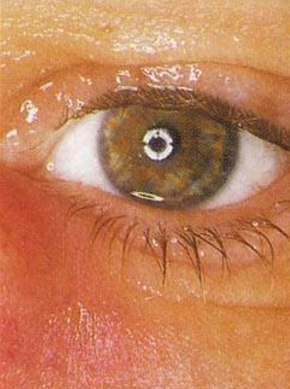
Signs of acute dacryocystitis
Moderate swelling of sac
Mild to moderate localized edema and erythema throughout inferior nasal region
Purulent discharge
Secondary conjunctivitis
In severe cases, a secondary preseptal cellulitis
Almost always epiphora
Signs of chronic dacryocystitis
Less severe
More common congenital presentation
Purulent discharge
May persist up to 9-12 months in congenital form with spontaneous remission (opening of the valve of Hasner)
What workup should you do for dacryocystitis?
Problem oriented questions:
Previous episodes?
Concomitant ear, nose, or throat infection?
Evaluation
Gentle compression of the lacrimal sac
Extraocular motility
Check for proptosis
Gran’s stain and blood agar culture
Consider CT scan
How do we treat dacryocystitis?
Systemic antibiotic
Children: afebrile, mild case, systemically well
Amoxicillin clavulanate (Augmentin) 20-40mg/kg/day po
Cephalexin (Keflex) 25-50mg/kg/day
Cefaclor (Ceclor) 20-40 mg/kg/day po
Children: febrile or acutely ill, moderate-severe case, or unreliable parent
Hospitalize and treat
Adult: afebrile, systemically well, mild case, reliable patient
Cephalexin (Keflex) 500mg po qid
Amoxicillin clavulanate (Augmentin) 250-875mg po bid
Febrile or acutely ill
Hospitalize and treat
Topical antibiotic drops
Warm compresses and gentle massage (Crigler massage) qid
Pain med (acetaminophen) PRN
Consider surgical correction: DCR
Follow-up every 3-5 days
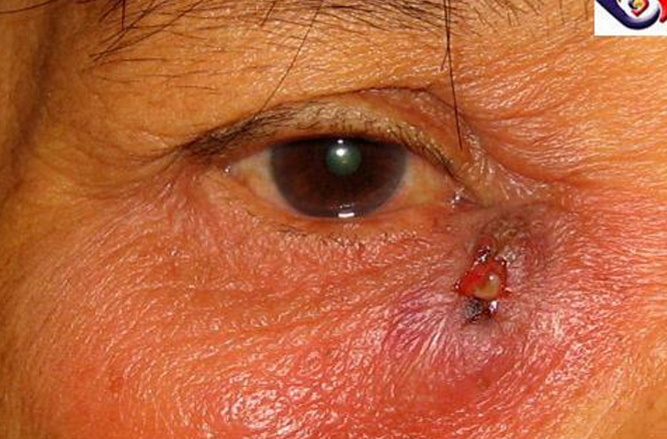
Chronic, untreated dacryocystitis has inflamed the lacrimal sac to the point of perforation
Lacrimal fistula
What are the causes of nasolacrimal duct obstruction?
Acquired or congenital
Idiopathic stenosis
Naso-orbital trauma
Previous nasal and sinus surgery
Infiltration by nasopharyngeal tumors
Granulomatous disease
How do we treat nasolacrimal duct obstruction?
Dacryocystorhinostomy
Intubation
Stent insertion
Balloon dilation
How do we treat congenital nasolacrimal duct obstruction?
Often resolves on its own
Massage
Lid hygiene
Topical antibiotics
Probing and/or stenting
Signs of congenital nasolacrimal duct obstruction…
Epiphora and matting of lashes
Gentle pressure over the lacrimal sac causes reflux of purulent material
Uncommon
Delayed diagnosis
Common cause of lacrimal sac mass
Clinical presentation
Epiphora
Dacryocystitis
Epistaxis (nosebleed)
Mass
Nasolacrimal tumor
A number of histologies are encountered including:
Squamous cell papilloma
Squamous cell carcinoma (most common)
Transitional cell papilloma
Transitional cell carcinoma
Oncocytoma
Adenocarcinoma
Adenoid cystic carcinoma
Malignant melanoma
Biopsy, CT and MRI scans
Treatment — surgery, chemotherapy, immunotherapy
Nasolacrimal tumor
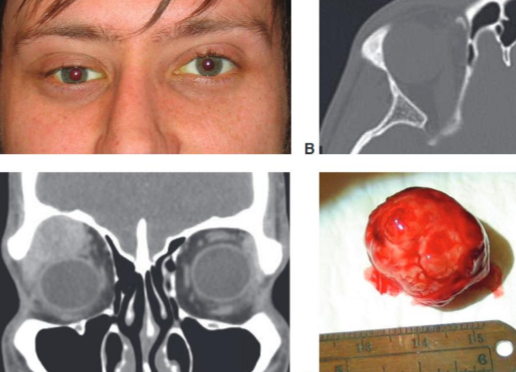
Most common epithelial tumor of the lacrimal gland
Progressive, painless, inferior and medial displacement of the globe >12 months
Proptosis
Firm lobular mass located near the superior orbital rim
Treatment = removal
Pleomorphic adenoma of the lacrimal gland
Most common malignant epithelial tumor of the lacrimal gland
Pain
Perineural invasion and bond destruction
Rapid course (<1 year)
Extends to posterior orbit
Adenoid cystic carcinoma (ACC) of the lacrimal gland
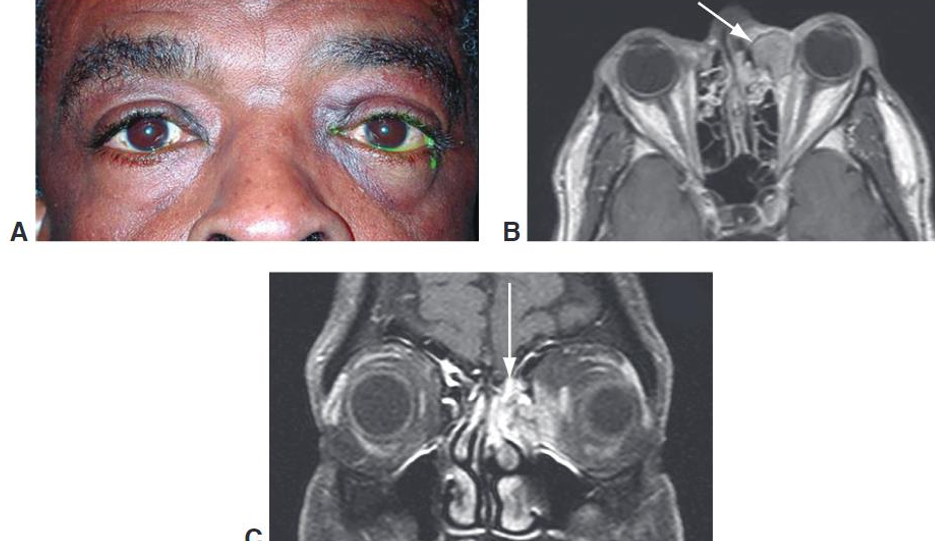
Nonepithelial tumor
Usually arise in the maxillary sinus, followed by the nasopharynx
Nasal obstruction or epiphora may be associated with tumor growth
Characterized by proliferation of keratinizing malignant squamous cells
Treatment = surgical excision and radiation
Primary squamous cell carcinoma and adenocarcinoma of the lacrimal gland
Type of non-Hodgkin lymphoma
Originates in the conjunctiva, lacrimal gland, soft tissues of the eyelids or EOMs
Primary or secondary
Constitutes 55% of all malignancies
Unilateral or bilateral
Orbital lymphoma
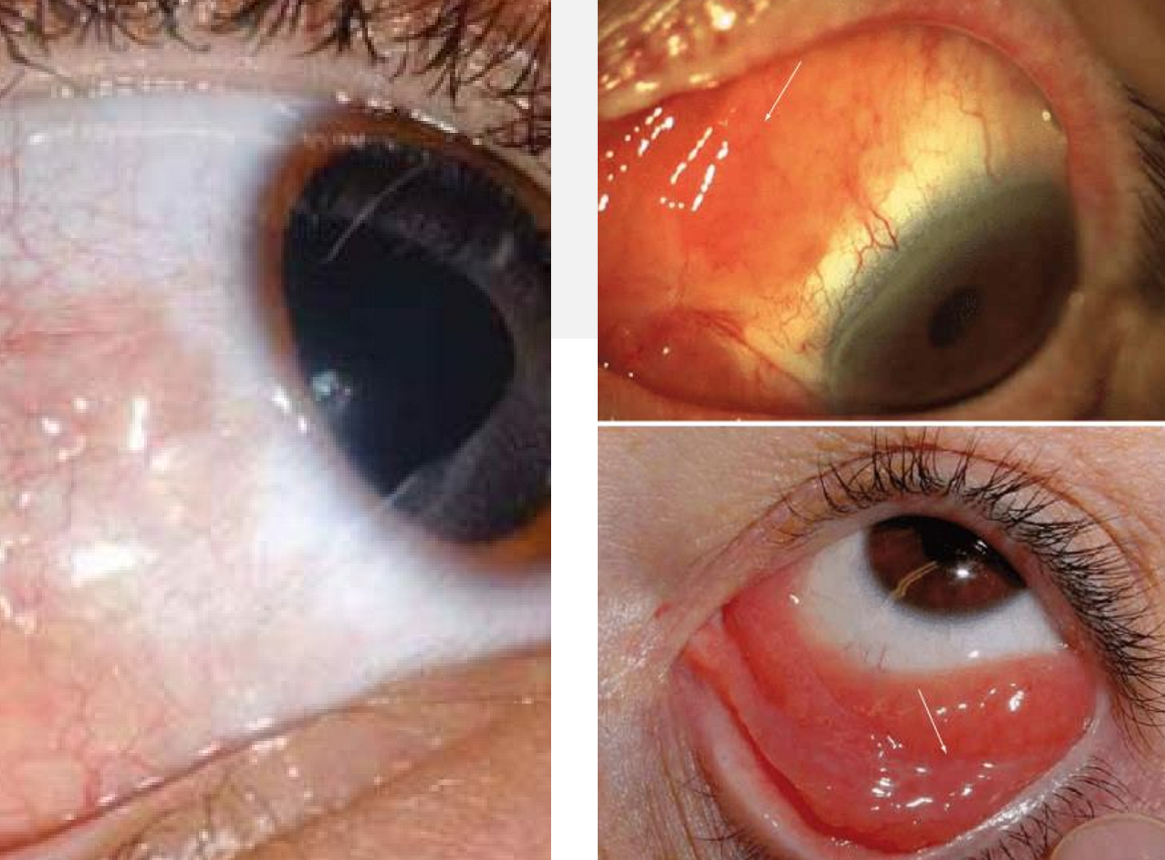
Vision usually preserved
Conjunctiva: pink or red batch of swollen conjunctiva or conjunctival hyperemia (often feeder vessels)
Orbit: painless mass in ST quadrant, proptosis, diplopia, abnormal EOMs
LG: displaces the eye IN
Eyelids: swelling and prolapse
Orbital lymphoma
How do you treat orbital lymphoma?
Imaging
Molding of tumor to normal structures
Surgery, radiotherapy, chemotherapy, immunotherapy
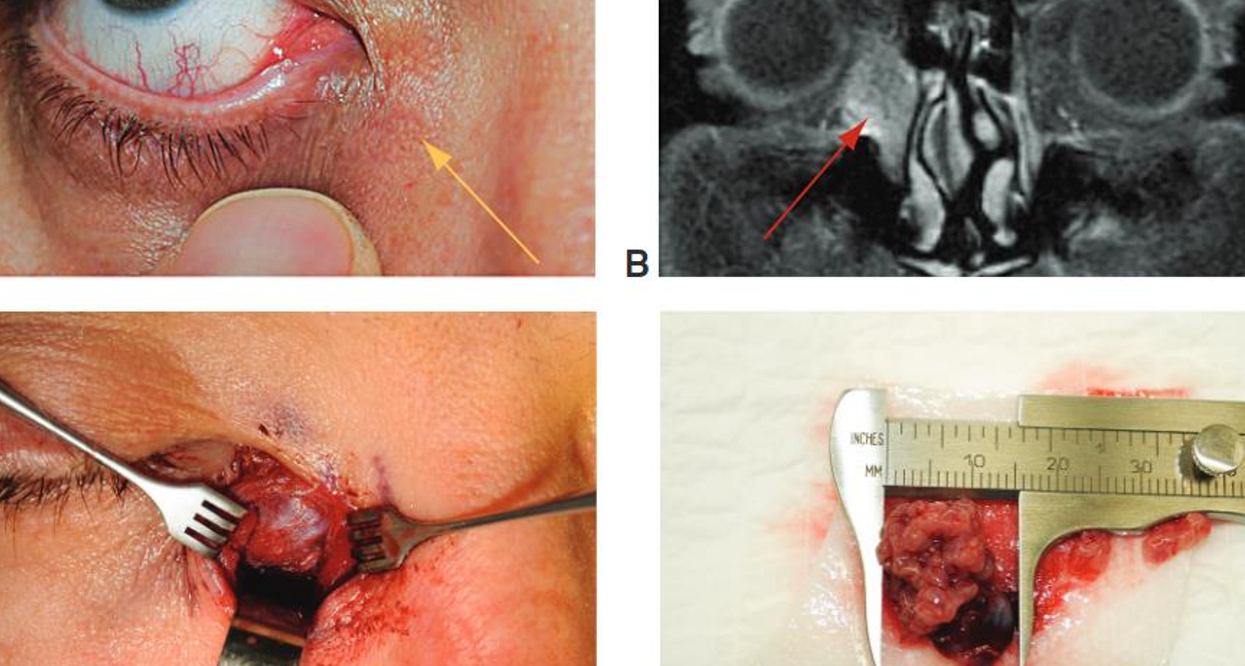
Rare
Associated with epiphora or chronic dacryocystitis
Spontaneous bleeding from punctum
Tumors that invade the skin may produce ulceration with telangiectasia over the lacrimal sac
Metastasis to reginal lymph nodes may occur
CT and MRI
Treatment = dacryocystectomy
Primary lacrimal sac tumor
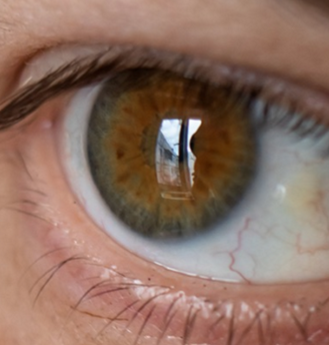
Adjacent to limbus— nasal & temporal
UV exposure
Epithelium may be normal, thin or thick
Yellow-white in color
Grow over time
Recurrent inflammation/irritation common
Treatment = ocular lubrication
Pinguecula
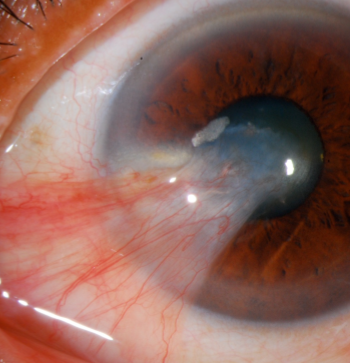
Wing shaped fibrovascular growth of conjunctiva involving the superficial cornea
Caused by UV exposure, environmental insults, dryness
Typically preceded by pinguecula
Prevalence increases with proximity to the equator
Irregular astigmatism with increasing size
Measure size/topography
Stocker line - iron line at leading edge
Treatment - lubrication, excision is VA decreased
Pterygium
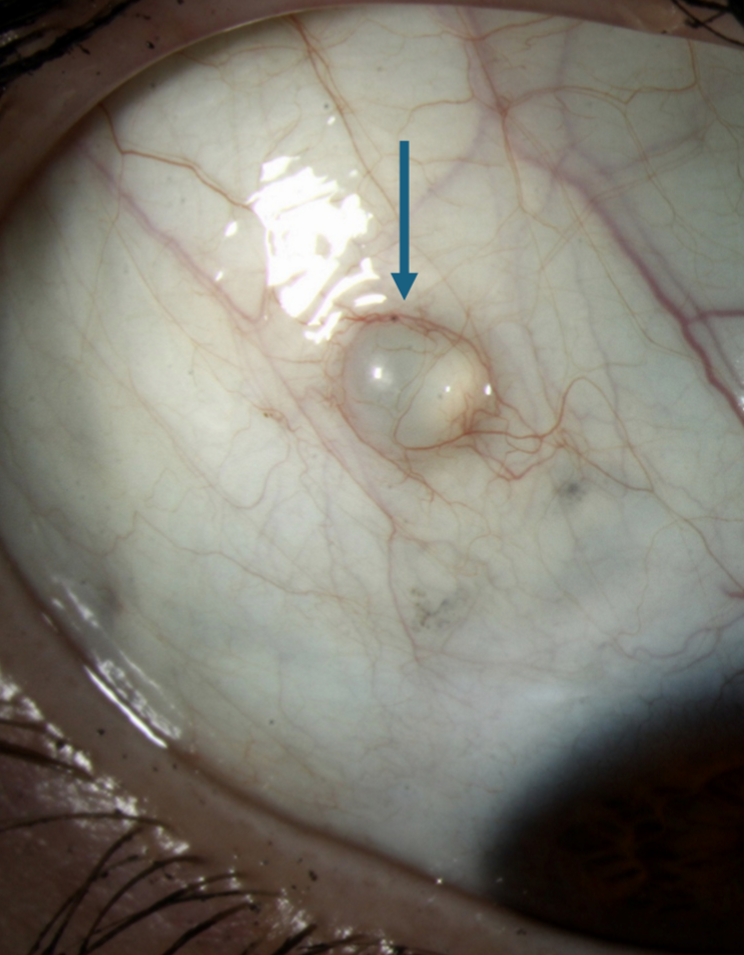
Asymptomatic
Congenital or acquired
Chronic inflammation
Trauma
Surgery
Derived from inclusion of conjunctival epithelium in the substantia propria
Central cavity filled with clear fluid and lined with nonkeratinized conjunctiva epithelium
Bulbar conjunctiva or fornix
Treatment = drain or excise
Need to differentiate from dilated lymphatic channels
Inclusion cyst of the epithelium
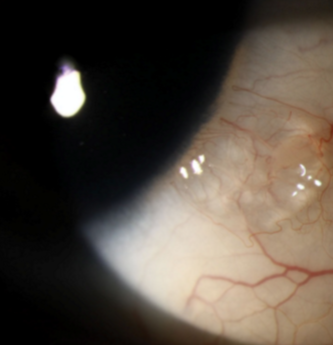
"bubble" on the eye
"string of pearls"
Dilated conjunctival lymphatic channel
Unknown etiology
Benign
Possible connection with Fabry's Disease
Conjunctival lympangiectasis
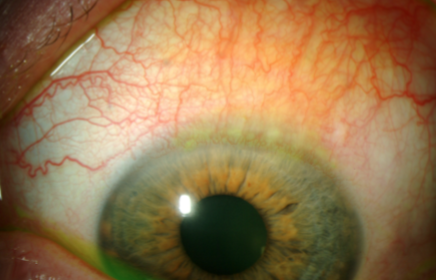
Chronic, recurrent inflammation involving the superior bulbar and tarsal conjunctiva as well as superior limbus and cornea
Associated with TED
Mechanical trauma from upper lid
Clinical signs:
Papillae
Injection and edema of superior conjunctiva
(+) NaFl and LG staining
Hypertrophy of superior limbus
Blepharospasm
Superior corneal filaments
Superior Limbic Keratoconjunctivitis
How do you treat SLK?
Lubrication
Punctal plugs
Topical cyclosporin, steroids
Autologous serum
BCL
Co-manage
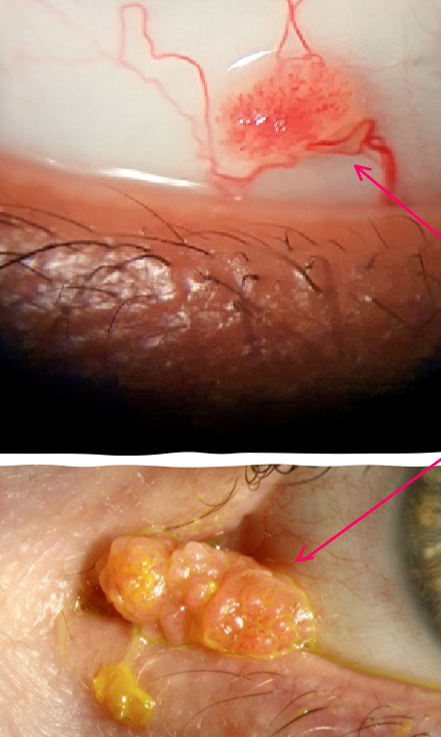
Pedunculated - fleshy growth with fibrovascular core
Sessile - found near limbus and has a flat base
Glistening surface with red dots
Benign
When caused by HPV may be carcinomatous
Conjunctival papilloma
How do you treat a conjunctival papilloma?
Regress spontaneously
Observe
Excision and cryotherapy
Dysplasia
Premalignant that is at risk for becoming squamous cell carcinoma
Analogous to actinic keratosis of the skin
Does not invade underlying basement membrane
Develops on exposed area of bulbar conjunctiva near the limbus
Older males, light complexion
Smokers
Three variants
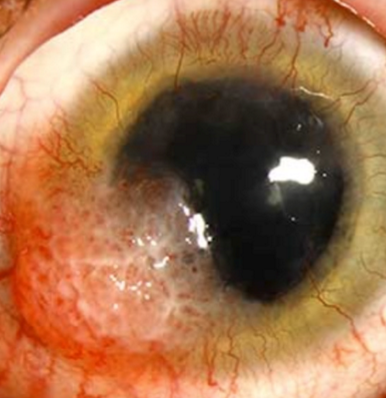
Mild inflammation and various forms of abnormal vascularization
Large feeder vessels - invasion to BM
Slow growing, rapid in AIDS patient
Can invade cornea
Stains with LG
Recurrent
Conjunctival Intraepithelial Neoplasia (CIN)
What is the most common conjunctival malignancy in the US?
Conjunctival Intraepithelial Neoplasia (CIN)
How do we treat conjunctival intraepithelial neoplasia (CIN)
Excision including 3-4mm of surrounding tissue
Chemotherapeutic agent
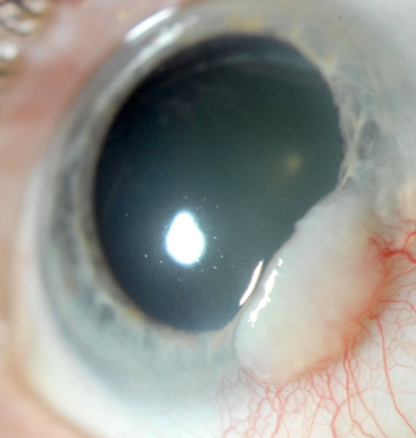
Cornea involvement with minimal conjunctival involvement
Granular, translucent, gray epithelial sheet at the limbus extending to the cornea
Stains with LG
No corneal neo
Corneal intraepithelial neoplasia
How do you treat corneal intraepithelial neoplasia?
Apply absolute alcohol to the cornea for 30-40 seconds, then irrigate and debride
Cryotherapy
Surgical excision
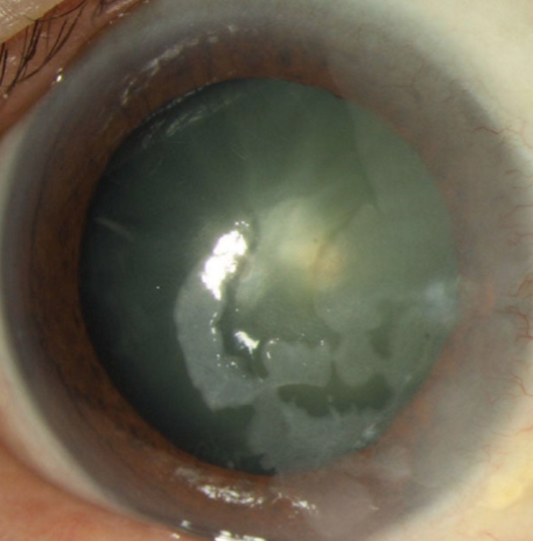
Plaque-like, gelatinous or papilliform growth
Limbal and bulbar conjunctiva
UV radiation, viral and genetic factors
Compromised immunity, xeroderma pigmentosa
Grows outward with sharp borders
Invades through basement membrane
Engorged conjunctival vessel feeds the tumor
Treatment = excision followed by cryotherapy
Squamous cell carcinoma
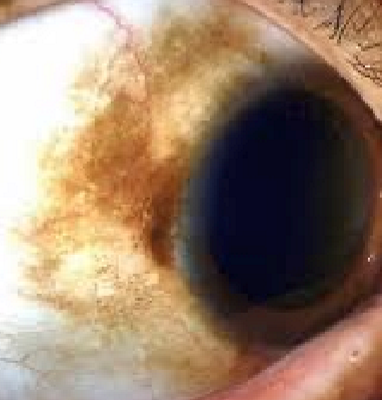
Benign
Freckle
Bulbar conjunctiva near limbus
Present at early age
Management: monitor
Congenital epithelial melanosis
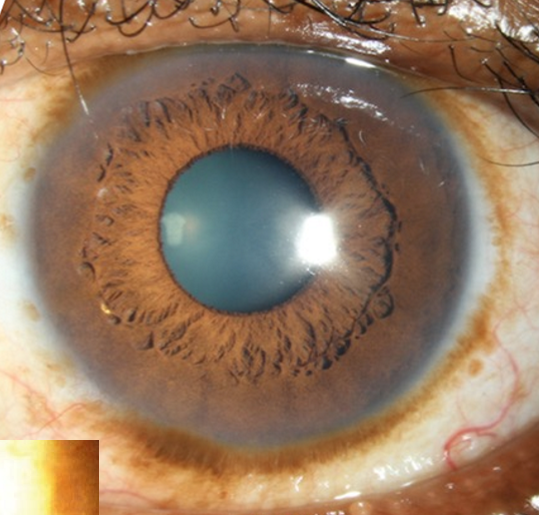
Increasing pigmentation of the conjunctiva
Can extend on the cornea (striate melanokerotosis)
Bilateral
Sunlight exposure
Management: monitor
Benign melanosis (racial, complexion associated)
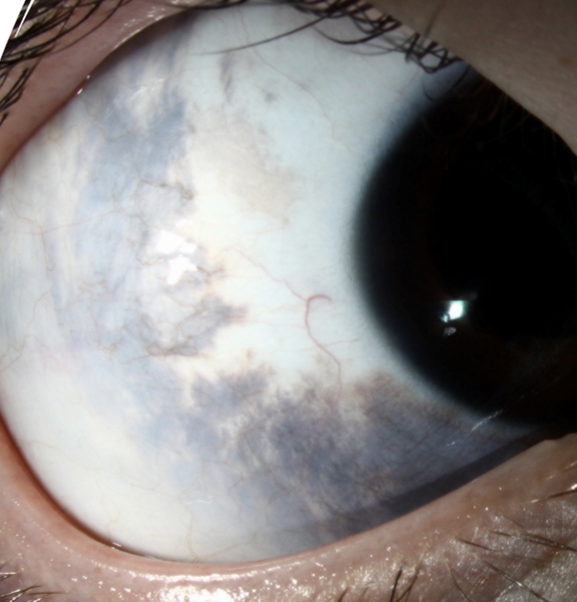
1 in every 2500
More common in Black, Hispanic,
Asian populations
Focal proliferation of subepithelial melanocytes (blue nevus)
Patches of episcleral pigmentation appear slate gray
Unilateral
Immobile
Management: Monitor
50% have ipsilateral dermal melanocytosis of periorbital skin
Nevus of Ota
Increased risk of secondary glaucoma
Increased risk of uveal melanoma
Ocular Melanocytosis
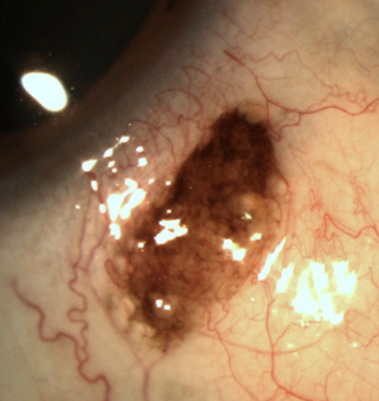
1st or 2nd decade of life
Flat
Tan, light brown or amelanotic
Epithelial inclusion cysts may occur
Secretions of mucin may cause nevus to enlarge
Management: monitor 6-12 months
Biopsy if change
Conjunctival nevus
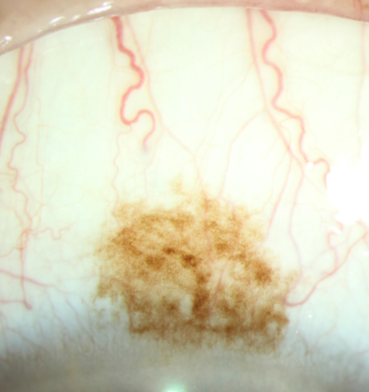
Acquired pigmentation — hyperplasia of melanocytes
Unilateral
Light-skinned individuals
Flat, brown lesion
Changes in size may be associated with inflammation
Pre-cancerous (rare)
Larger size
Caruncle, fornix or palpebral
Progressive enlargement
Nodular component
Thickening
Feeder vessel
Management: monitor 8-12 months
Biopsy
Primary acquired melanosis (PAM)
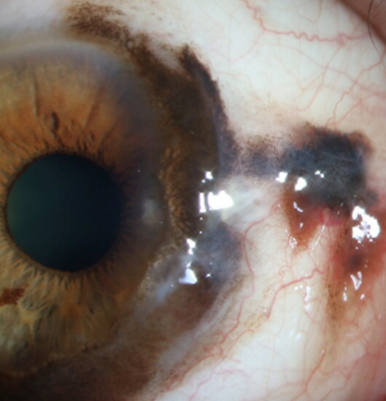
2% of ocular malignancy
European ancestry
Arise from PAM, nevi or de novo
Mortality rate = 25%
25% are amelanotic
High recurrence rate
Heavy vascularization
Nodular
Invade the globe or orbit
May metastasize to regional lymph nodes, brain, lungs, liver and bone
Melanoma
How do we treat melanoma?
Biopsy
Excision
Cryotherapy
Orbital exteneration
Enucleation
Abnormal increased distance between the eyes
Hypertelorism
Abnormal decreased distance between the eyes
Hypotelorism
Remove the contents of the globe, leaving the scleral shell
Better preservation of the anatomy
Better motility for prosthetic
CONTRAINDICATED in intraocular malignancy
Evisceration
Removal of the eyeball (globe) leaving orbital content (fat & musculature) behind
Allows for histologic examination of intact globe and optic nerve
Indications
Intra ocular malignancy
Severe trauma
Blind, painful eye
Enucleation
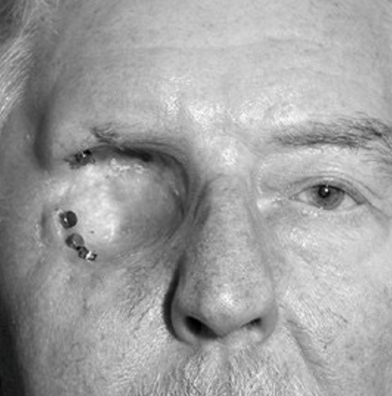
Removal of the entire globe and ALL orbital contents
Indications
Orbital malignancy
Life-threatening infection
Exteneration