Ch18: Heart
1/26
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
27 Terms
Pulmonary circuit
The right side of the heart receives oxygen-poor blood from body tissues and then pumps this blood to the lungs to pick up oxygen and dispel carbon dioxide
The blood vessels that carry blood to and from the lungs from the pulmonary circuit
Left atrium receives blood returning from pulmonary circuit
Right ventricle pumps blood into the pulmonary circuit
System Circuit
Left side of heart receives oxygenated blood returning from lungs and pumps blood throughout body to supply oxygen and nutrients to body tissues
Blood vessels that carry blood to and from body tissues form systemic circuit
Right atrium receives blood from systemic circuit
Left ventricle pumps blood into systemic circuit
Blood floor
Deoxygenated blood from extremities and body go to the superior and inferior vena cava and coronary sinus
Blood goes to right atrium
Blood passes through the tricuspid valve into the right ventricle
Deoxygenated blood passes through the pulmonary semilunar valve into the pulmonary trunk
Pulmonary arteries brings blood to lungs to be oxygenated
Blood enters back from lungs through 4 pulmonary veins into left atrium
Bicuspid valve opens for blood to enter left ventricle
Blood leaves through aortic semicircular valve into aorta to go to body
Size and location
Heart is about the size of a fist, is hollow and cone-shaped
Mass of 250-350 grams
Enclosed within the mediastinum or medial cavity of thorax
Heart extends obliquely for 12 to 14 cm from the 2nd rib to the 5th intercostal space
Rests on superior surface of diaphragm and lies anterior to the vertebral column and posterior to the sternum
⅔ of mass lies left of midsternal line and balance projects to the right
The flat base, or posterior surface is about 9 cm wide and directed toward right shoulder
Its apex pointed inferiorly toward left hip
Apical impulse: caused by beating heart’s apex where it touches chest vali
Coverings
Heart is enclosed in pericardium(double walled sac)
Fibrous pericardium (outermost)
Tough, dense connective tissue layer
Protects heart
Anchors heart
Prevents overfilling
Serous pericardium
Forms closed sac around heart
Parietal layer: lines internal fibrous pericardium
Visceral layer (epicardium): is integral part of heart wall
Pericardial cavity: contains serous fluid for lubrication
Pericarditis
Inflammation of pericardium
Roughens serous membrane surface
Heart rubs against pericardial sac
Pain beneath sternum
Impedes function
Cardiac tamponade
3 Layers
Epicardium: visceral layer of the serous pericardium
Often infiltrated with fat
Myocardium: the middle layer is composed mainly of cardiac muscle and forms the bulk of the heart. This is the layer that contracts
Branching cardiac muscle cells are tethered to one another by criss crossing connective tissue fibers and arranged in spiral or circular bundles. interlacing bundles link all parts of the heart together.
Connective tissue fibers form a dense network, the fibrous cardiac skeleton reinforces the myocardium internally and anchors the cardiac muscle fibers
Cardiac skeleton allows action potentials to spread only via specific pathways in the heart
Endocardium: 3rd layer of the heart wall is a glistening white sheet of endothelium resting on a thin connective tissue layer. Located on the inner myocardial surface, it lines the heart chambers and covers the fibrous skeleton of the valves
Atria: Receiving Chambers
Auricles: small, wrinkled appendages which increase atrial volume
Internally, the right atrium has two basic parts
smooth-walled posterior part
anterior portion in which bundles of muscle tissue form ridges in the walls
(bundles are pectinate muscles)
The left atrium is mostly smooth and pectinate muscles are found only in the auricle.
Function: the atria are receiving chambers for blood returning to the heart from the circulation
Interatrial septum: where it separates the atria
Interventricular septum: where it separates the ventricles
Blood enters right atrium
The superior vena cava returns blood from body regions superior to the diaphragm.
The inferior vena cava returns blood from body areas below the diaphragm.
The coronary sinus collects blood draining from the myocardium.
Blood enters left atrium
4 pulmonary veins: transport blood from the lungs back to heart
Ventricle: Discharging Chambers
Make up most volume of the heart
irregular ridges of muscle called trabeculae carneae ("crossbars of flesh") mark the internal walls of the ventricular chambers.
Other muscle bundles, the papillary muscles, which play a role in valve function, project into the ventricular cavity
Right ventricle: pumps blood into the pulmonary trunk, which routes the blood to the lungs where gas exchange occurs.
Left ventricle: ejects blood into the aorta, the largest artery in the body.
Interventricular septum: where it separates the ventricles
Valves
2 atrioventricular valves. One located at each atrial-ventricular junction
Prevents backflow into the atria when ventricles contract
Tricuspid valve: right AV valve that has 3 flexible cusps
Mitral valve: left AV valve that has 2 cusps, also called bicuspid valve
Each AV valve flap has a white collagen cord attached called Chordae tendineae
Anchors the cusps to papillary muscles protruding from the vascular walls
Semilunar valves are made up by the aortic and pulmonary valves
Guard the bases of large arteries from the ventricles
Coronary circulation
Coronary arteries provide an arterial supply of the coronary circulation
Left C.A. = runs toward left side of the heart and then divides into 2 major branches
Anterior interventricular artery: follows anterior ventricular sulcus and supplies blood to the interventricular septum and interior walls of both ventricles
The circumflex artery: Supplies left atrium and posterior walls left ventricle
Right coronary artery courses right side of the heart, where it gives rise to 2 branches:
Right marginal artery serves the myocardium of the lateral right side of the heart
Posterior interventricular artery runs to the heart apex and supplies the posterior ventricular walls. Merges anastomoses with the anterior interventricular artery
Branches of right coronary artery supply right atrium and nearly all right ventricle
Arterial supply of the heart varies for everyone
Right side blockage shows pitting edema in limbs and jugular vein distention where left side blockage causes respiratory emergencies (loss breath, cyanosis)
Skeletal vs Cardiac muscle
Skeletal
Striated, long, cylindrical, multinucleate
No gap junctions
No motor units, must be individually stimulated
Abundance of T tubules
Elaborate SR with terminal cisterns
Ca for contraction comes from SR
CA binds to troponin
No pacemaker cells
Tetanus possible
Gets ATP from aerobic and anaerobic respiration
Cardiac
Striated, short, branchedd, 1-2 nuclei per cell
Has gap junctions
Gap junctions create functional syncytium (contracts as unit)
T tubules are less numerous, wider
SR less elaborate, no terminal cisterns
Ca for contraction from SR and ECF
Ca binds to troponin
Tetanus not possible
ATP from aerobic respiration (more mitochondria)
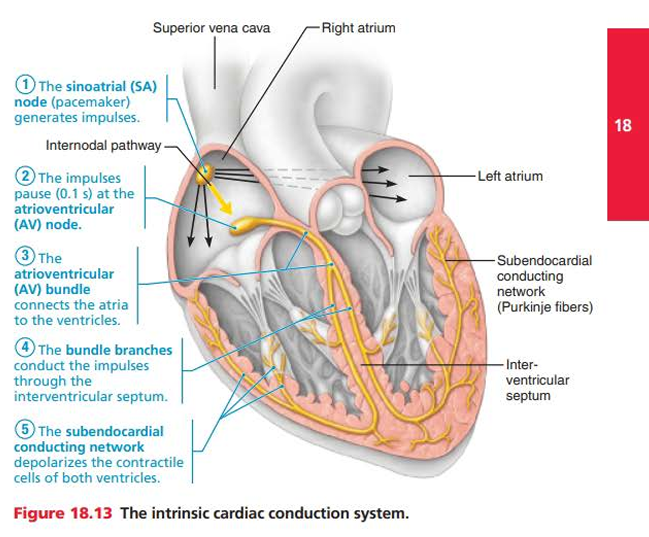
Sequence of Excitation ***
The sinoatrial (SA) node generates impulses (pacemaker)
The impulses pause (0.1 s) at the atrioventricular (AV) node
The atrioventricular bundle connects the atria to the ventricles
The bundle branches conduct the impulses through interventricular septum
The subendocardial conducting network depolarizes the contractile cells of both ventricles
Autonomic Nervous System
Fibers of ANS modify the beat of the heart
Sympathetic NS increases heart rate
Parasympathetic NS decreases heart rate
Cardiac centers are located in medulla oblongata. The cardioacceleratory center projects to sympathetic neurons in the spinal cord. The postganglionic fibers run thru cardiac plexus to heart where they innervate the SA + AV nodes, heart muscle + coronary arteries
The cardioinhibitory center sends impulses to sympathetic dorsal vagus nucleus in the medulla which sends inhibitory impulses to heart via branches of vagus nerves
Most parasympathetic postganglionic motor neurons are in ganglia in heart wall
Fibers project to SA and AV nodes
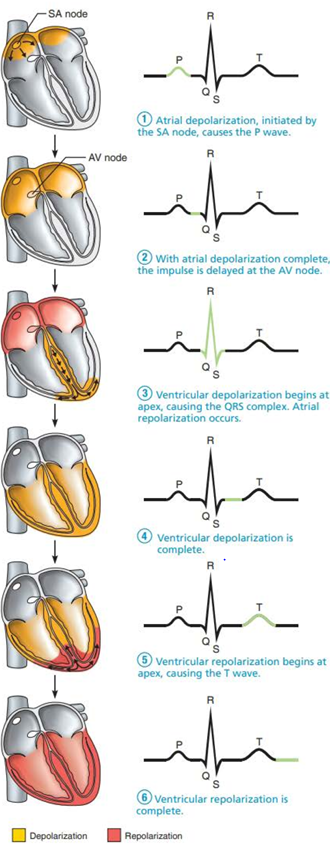
ECG/EKG
Electrocardiogram: graphic record of heart activity
The electrical currents generated in and transmitted through the heart spread throughout the body and can be detected with an electrocardiograph
And ECG is a composite of all the APs generated by nodal and contractile cells at a given time
To record an ECG, electrodes are placed at various sites on body surfaces → typical 12 lead ECG:
3 electrodes form bipolar leads that measure voltage between arms or between an arm and leg
9 electrodes form unipolar leads
Together, 12 provide a comprehensive picture of heart electrical activity
Typical ECG has 3 waves/deflections:
P wave: 1st wave, small, lasts 0.09 seconds. Results from movement of the depolarization wave from SA node through atria; approximately 0.1 seconds after P wave begins the atria contracts
QRS complex: large, results from ventricular depolarization and precedes ventricular contraction, complicated shape be the paths of depolarization waves through ventricular walls change contraction and produces corresponding changes in current direction
T wave: caused by ventricular repolarization, lasts 0.16s, more spread out and has a lower amplitude than QRS complex because repolarization is slower.
P-R interval: time from beginning of atrial excitation to beginning of ventricular excitation
S-T segment: APs of ventricular myocytes are in plateau phases
Phases of cardiac cycle
Ventricular filling: mid to late diastole
Ventricles fill with blood and the aortic + pulmonary valves are closed
Atria contract and propels residual blood into ventricles
Isovolumetric contraction
Ventricles contract and pressure increases
Phase is when ventricles are completely closed chambers
SL valves are forced open
Ventricular ejection
Blood rushes from ventricles into aorta + pulmonary trunk
Isovolumetric relaxations: early diastole
Ventricles relax and the SL valves close
End is the beginning of isovolumetric relaxation phase
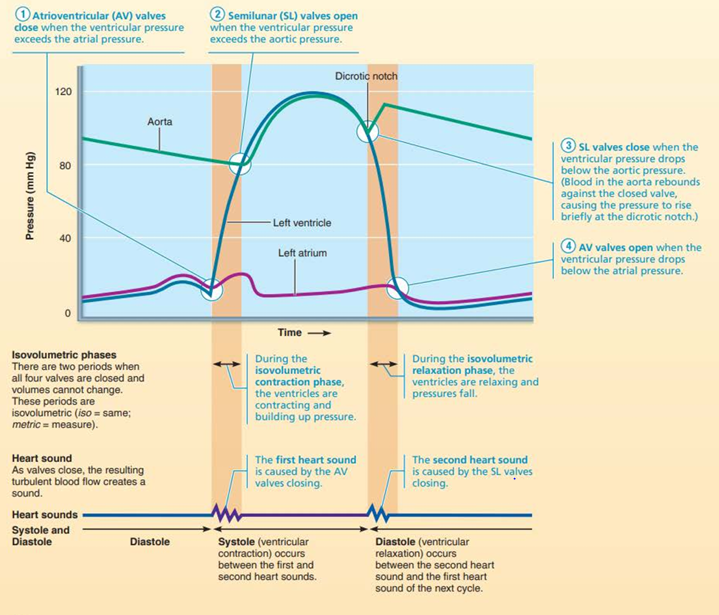
Heart Sounds
2 sounds
First: closing of AV valves at beginning of ventricular systolic
Second: closing of SL valves at beginning of ventricular diastole
Pause between (lub-dub) indicates heart relaxation
Mitral valve closes slightly before tricuspid, and aortic closes slightly before pulmonary valve
Differences allow auscultation of each valve when the stethoscope is placed in 4 diff regions.
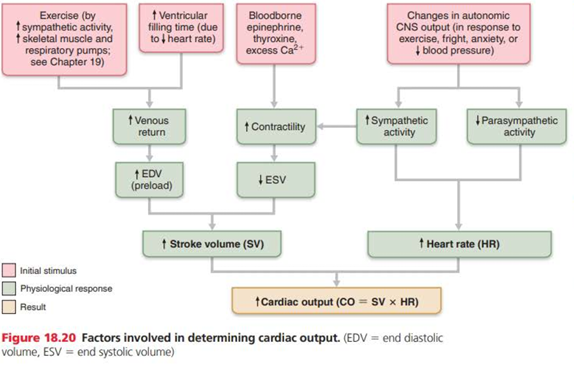
Cardiac Output
Amount of blood pumped out by each ventricle in 1 minute
CO = HR (heart rate) x SV (stroke volume)
Stroke volume
Volume of blood pumped out by 1 ventricle with each beat
Correlated with force of ventricular contraction
Measured in LPM
Increases with increase in SV or HR
Cardiac reserve: difference between resting and maximal cardiac output
Higher in trained athletes
Regulation of Stroke Volume
Difference between end diastolic volume (EDV) and end systolic volume (ESV)
end diastolic volume (EDV): amount of blood that collects in ventricle during diastole
end systolic volume (ESV): volume blood in ventricle after it contracted
Preload
Degree to which cardiac muscle cells are stretched just before they contract. Increase preload and increase SV
Venous system: amt of blood returning to heart and distending its vesicles, most important factor stretching cardiac muscle. higher venous return is higher cardiac output.
Frank-starling is relation between SV and preload
Contractility
Contractile strength achieved at given muscle length
Rises when increased Ca enters cytoplasm from SR and EC fluid
Afterload
Pressure that the ventricles must overcome to eject blood
Not a major determinant in SV
In people with hypertension = important, afterload reduces ability of ventricles to eject blood
Regulation of Heart Rate
Positive chronotropic factors increase heart rate, negative chronotropic decreases
HR is regulated by ANS, chemicals, other factors
Increases
ANS: sympathetic NS activated by emotional/physical stressors
Norepinephrine release: pacemaker fires more rapidly, increased contractility
Atrial (bainbridge) reflex: sympathetic reflex initiated by increased venous return, hence increased atrial filling
Hormone release (epinephrine/thyroxine) influences HR
Decreases
PNS has opposite effects
Acetylcholine release: opens K channels
Heart at rest exhibits vagal tone
Parasympathetic = dominant influence
Decreases rate about 25 bpm
Cutting vagal nerve leads to HR of 100
Intra/extracellular ion concentration need to be maintained
Age, gender, exercise, body temp also influences
Homeostatic imbalance of cardiac output
Hearts pumping action maintains balance between Cardiac output and venous return
In congestive heart failure, heart is an inefficient pumped blood circulation does not meet tissue needs
Reflects weakening of myocardium
Most common causes:
Coronary atherosclerosis: fatty build up that clogs arteries and impairs blood and oxygen delivery. Cells and heart becomes hypoxic
Increased Blood pressure: myocardium must exert more force to open aortic valve
Stress causes weaker myocardium
Multiple myocardial infarction: heart attack depresses pumping because noncontractile fibrous tissue replaces dead heart cells
Dilated cardiomyopathy: ventricles stretch and myocardium deteriorates
intrinsic cardiac conduction system
noncontractile cardiac cells specialized to initiate and distribute impulses throughout the heart, so that it depolarizes and contracts in an orderly, sequential manner
Cardiac pacemaker cells: having the special ability to depolarize spontaneously and so pace the heart
Pacemaker potentials: initiate action potentials that spread throughout the heart to trigger contractions
cardiac reserve
different between resting and maximal cardiac output
Angina pectoris
thoracic pain caused by a fleeting deficiency in blood to myocardium
blockage of coronary arterial circulation
may result from spasms of coronary arteries or increased physical demands of heart
Myocardial infarction
Heart attack
prolonged coronary blockage in which cells do die
Cardiac Muscle differences
Some cardiac muscle cells are self-excitable
Heart contracts as a unit
Influx of Ca from extracellular fluid triggers Ca release from SR
Tetanic contractions cannot occur (multiple contractions)
Relies on aerobic respiration
3 Parts of action potential in pacemaker cells
Pacemaker potential: Slow Na channels open and Na influx occurs. (depolarization in action potential tracing)
Depolarization: Ca channels open and influx of Ca occurs. (plateau in action potential tracing)
Repolarization: Ca channels inactivate and K efflux from the cell