3.4.7 HORMONES AND THE CONTROL OF BLOOD GLUCOSE CONCENTRATION
1/123
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
124 Terms
What are factors that influence blood glucose concentration?
- Eating food containing carbohydrates → glucose absorbed from intestine to blood
- Exercise → increased rate of respiration of glucose
Draw a labelled flow chart of how blood glucose is controlled when its above and below normal levels.
Look at image and compare.
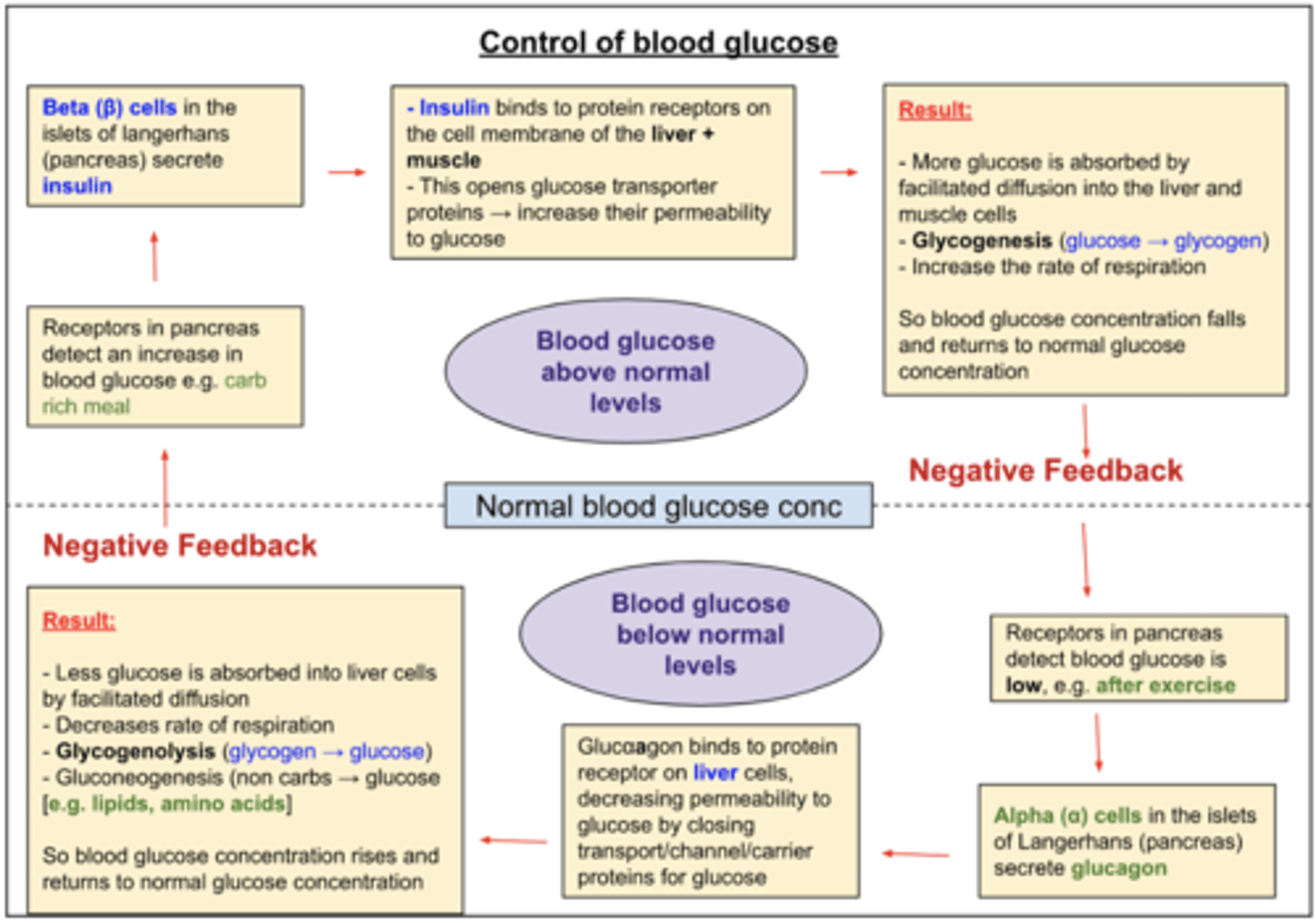
Describe how blood glucose is controlled when it is above normal levels.
1. Receptors in the pancreas detect high blood glucose, E.g. carb-rich food
2. Beta (β) cells in the islets of Langerhans (pancreas) secrete insulin
3. Secretion of insulin inhibits the action of alpha cells
4. Insulin binds to protein receptors on the Liver + Muscle cell membrane, This increases their permeability for glucose
5. Binding on receptors causes adenyl cyclase to convert ATP to cAMP. cAMP activates certain enzyme-controlled reactions in the cells to stimulate the opening of glucose channels in the cell surface membrane, which opens more transport/channel/carrier proteins for glucose
Result…
- More glucose is absorbed into Liver + Muscle cells by facilitated diffusion and removed from blood
- Glycogenesis: glucose → glycogen
- Increases the rate of respiration → helps burn more glucose
BLOOD GLUCOSE FALLS AND RETURNS TO NORMAL GLUCOSE CONCENTRATION
Describe how blood glucose is controlled when it is below normal levels.
1. Receptors in the pancreas detect low blood glucose, E.g. after exercise
2. Alpha (α) cells in the islets of Langerhans (pancreas) secrete glucagon
3. Secretion of glucagon inhibits the action of beta cells
4. Glucagon binds to protein receptors on the liver cell membrane, This decreases its permeability to glucose
5. This closes transport/channel/carrier proteins for glucose
Result…
- Less glucose is absorbed into liver cells by facilitated diffusion
- Gluconeogenesis: Non-carbs → glucose (e.g. lipids, fats)
- Glycogenolysis: glycogen → glucose (second messenger model)
- Decreases the rate of respiration
BLOOD GLUCOSE CONCENTRATION RISES AND RETURNS TO NORMAL GLUCOSE CONCENTRATION
Describe an alternative way in which glycogen can be broken down into glucose to raise blood glucose levels.
Secondary messenger adrenaline:
1. Adrenaline fuses to a receptor on the cell surface membrane of liver cell and causes the receptor to change shape on the inside of the membrane
2. The changing of the shape on the inside of the membrane activates the enzyme adenyl cyclase which converts ATP to cyclic AMP (cAMP). This acts as a second messenger.
3. The cAMP then changes shapes and activates protein kinase enzyme which catalyses the conversion of glycogen into glucose.
BLOOD GLUCOSE CONCENTRATION RISES AND RETURNS TO NORMAL GLUCOSE CONCENTRATION
Draw a flow chart linking glycogenolysis, glycogenesis & gluconeogenesis.
Look at image and compare.
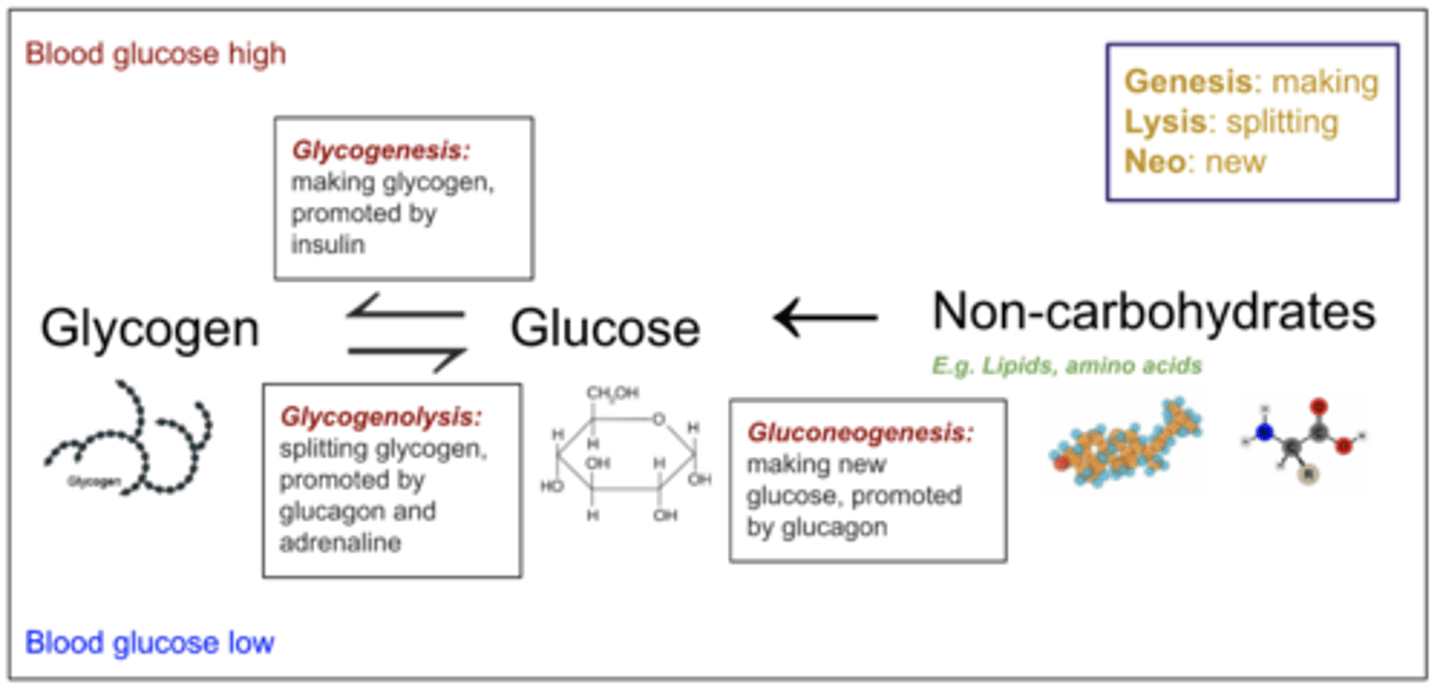
Define diabetes.
Where blood glucose concentration can’t be controlled properly. Blood glucose concentration peaks higher and takes longer to decrease / remains high (after meal)
What is hyperglycemia?
Dangerously high blood glucose concentration
What is hypoglycemia?
Dangerously low blood glucose concentration
Whats the cause of Type 1 diabetes?
- Gene mutation → Autoimmune response of immune system killing/destroying β cells of islets on Langerhans → Body can't produce insulin
Whats the cause of Type 2 Diabetes?
- Poor diet/lack of exercise/obesity →
- Glycoprotein/receptor loses responsiveness to insulin (faulty) → cells less responsive to insulin / don't take up enough glucose
- OR β cells don't make enough insulin
Whats the age of people who have Type 1 diabetes?
Children + young adults
Whats the age of people who have Type 2 diabetes?
Adults / elderly
What is the effect of Type 1 Diabetes on blood glucose after a meal?
- Rise after eating carbohydrates → hyperglycaemia
- Stays high → kidneys cant remove all glucose from urine
What is the effect of Type 2 Diabetes on blood glucose after a meal?
- Rise after easting carbohydrates → hyperglycaemia
How can you control Type 1 Diabetes in respect of insulin?
- Injections of insulin (not by mouth as protein is digested)
- Dose of insulin matched to glucose intake / use biosensors
- Too much insulin can result in hypoglycaemia
How can you control Type 2 Diabetes in respect of insulin?
- Use of drugs which target insulin receptors / use of insulin
- More glucose uptake by cells / tissues
How can you control Type 1 Diabetes in respect of diet manipulation?
- Eating regularly, control diet/sugar intake e.g. carbs which are broken down / absorbed slower
- Avoid sudden rise in glucose → avoid simple carbohydrates (sugars)
- Regular exercise to use up glucose (less insulin needed)
How can you control Type 2 Diabetes in respect of diet manipulation?
- Reduced sugar intake (carbs) in diet / eat food with low glycaemic index → Less sugar absorbed into blood
- Reduced fat intake → Less fat converted to glucose
- More (regular) exercise → Uses glucose / fats by increasing respiration
- Lose weight → Increased sensitivity of cells to insulin / increased uptake of glucose by cells
- Eat healthly
- Lose weight
- Drugs to: reduce the amount of glucose released, increase sensiivity to inuslin, make more insulin
- insulin injections
Describe the role of insulin.
- Protein hormone secreted by beta cells in islets of Langerhans in pancreas when blood glucose concentration is too high
- Insulin binds to specific receptors on cell surface membranes of liver & muscle cells (target cells called hepatocytes):
- Increases permeability of muscle cell membrane to glucose → Glucose carrier proteins are stored in vesicles inside liver and muscle cells → insulin binds with receptors on the cell membrane of the target cells, this causes the vesicles to fuse with cell membrane → carrier proteins join the membrane and so there's an increasing number of channel proteins (GLUT4) in cell surface membrane → more glucose is absorbed by facilitated diffusion from blood
- Activation of enzymes in liver / muscle cells that convert glucose to glycogen → glycogenesis → store glycogen in cytoplasm
- Rate of respiration of glucose also increases
- DECREASES blood glucose concentration
When is insulin secreted and by what?
Protein hormone secreted by beta cells in islets of Langerhans in pancreas when blood glucose concentration is too high
Describe the role of glucagon?
- Secreted by alpha cells in islets of Langerhans in pancreas when blood glucose concentration is too low
- Binds to specific receptors
- On cell surface membranes of liver cells (target cells)
- Activates enzymes involved in the hydrolysis of glycogen to glucose → glycogenolysis
- Activates enzymes involved in the conversion of glycerol/amino acids (non-carbs) to glucose → gluconeogenesis
- Facilitated diffusion of glucose out of (liver cells) cells
- Rate of respiration of glucose also decreases
- INCREASES blood glucose concentration
When is glucagon secreted and by what?
Secreted by alpha cells in islets of Langerhans in pancreas when blood glucose concentration is too low
Describe the role of adrenaline.
- Secreted by adrenal glands (found above kidneys) when blood glucose concentration is low / stressed/exercising
- Binds to specific receptors on cell surface membranes of liver cells (target cells)
- Activates enzymes involved in the conversion of glycogen to glucose → glycogenolysis
- Inhibits glycogenesis
- Activates secretion of glucagon
- Inhibits secretion of insulin
- INCREASES blood glucose concentration (more glucose for respiration)
When is adrenaline secreted and by what?
Secreted by adrenal glands (found above kidneys) when blood glucose concentration is low / stressed/exercising
What hormone is secreted when blood glucose is too low?
- Adrenaline
- Glucagon
What hormone is secreted when blood glucose is too high?
- Insulin
Describe and explain the secondary messenger model.
Adrenaline and glucagon (first messenger) demonstrate this because they cause glycogenolysis to occur inside cell even though they bind to receptors on the outside of the cell
1. Hormones e.g. adrenaline/glucagon (first messenger) bind to specific complementary receptor proteins on the cell membrane of target cells, e.g. liver cell
2. The protein receptor changes shape, which activates adenyl cyclase (enzyme)
3. Activated adenyl cyclase converts ATP to cyclic AMP [cAMP] which is a secondary messenger
4. cAMP (second messenger) activates enzyme called protein kinase A by altering 3D structure/phosphorylation
5. Protein kinase A activates a cascade which causes conversion of glycogen to glucose → glycogenolysis
![<p>Adrenaline and glucagon (first messenger) demonstrate this because they cause glycogenolysis to occur inside cell even though they bind to receptors on the outside of the cell</p><p>1. Hormones e.g. adrenaline/glucagon (first messenger) bind to specific complementary receptor proteins on the cell membrane of target cells, e.g. liver cell</p><p>2. The protein receptor changes shape, which activates adenyl cyclase (enzyme)</p><p>3. Activated adenyl cyclase converts ATP to cyclic AMP [cAMP] which is a secondary messenger</p><p>4. cAMP (second messenger) activates enzyme called protein kinase A by altering 3D structure/phosphorylation</p><p>5. Protein kinase A activates a cascade which causes conversion of glycogen to glucose → glycogenolysis</p>](https://knowt-user-attachments.s3.amazonaws.com/2cdbb2fe-168b-408e-a3c5-652e9f4fcf72.png)
What is the role of the pancreas in regulating blood glucose?
Have hormone-producing cells called islets of Langerhans:
- Have alpha cells, which are larger and produce the hormone glucagon
- Have beta cells, which are smaller and produce the hormone insulin
What is the role of the liver in regulating blood glucose?
- Intiates glycogenesis: glucose → glycogen
- Intiates glycogenolysis: glycogen → glucose
- Intiates gluconeogenesis: amino acids/glycerol → glucose
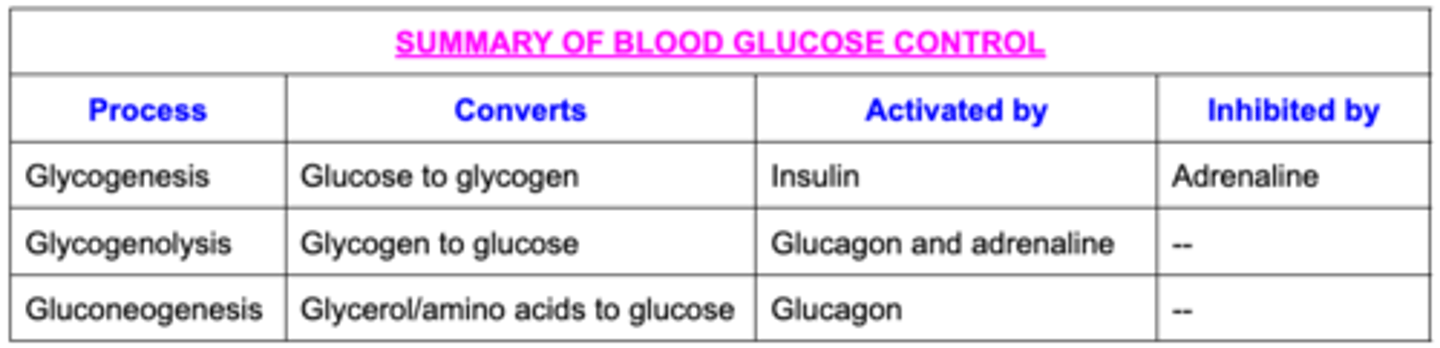
Draw a table of the summary of blood glucose control including:
- Processes
- What the convert
- What activates the process
- What they are inhibited by
Look at image attached and compare.
Q: A student ate a meal containing carbohydrates at 07:00. He ate nothing else for the next five hours.
At 9:00 the concentration of glucose in his blood (in mg per 100cm3 blood) was 70.
At 10:00 it rose to 85
At 1:00 it rose to 110
At 12:00 it fell to 80.
Describe the role of hormones in the fluctuation of glucose concentration between 9:00 and 12:00. (4 MARKS)
- 09:00 to 11:00 glucagon secreted
- (Glucagon) stimulates breakdown of glycogen to glucose
- 11:00 to 12:00 insulin secreted
- Insulin stimulates uptake of glucose by cells / conversion to glycogen
Q: Scientists investigated the control of blood glucose concentration in mice. They kept a group of normal mice without food for 48 hours. After 48 hours, the blood glucose concentrations of the mice were the same as at the start of the experiment.
Explain how the normal mice prevented their blood glucose concentration falling when they had not eaten for 48 hours. (3 MARKS)
- Release of glucagon
- Leads to formation of glucose in liver (cells)
- From non-carbohydrates / amino acids / fatty acids [accept: gluconeogenesis/references to glycogen as a source of glucose]
Q: Describe how negative feedback is used to control blood glucose concentration. (9 MARKS)
- Receptors detect change / increased / decreased in blood glucose (concentration)
- If higher glucose concentration beta cells (in pancreas) release insulin
- (increased) uptake / absorption of glucose by liver / muscle cells
- Enters through glucose transport proteins (in cell surface membrane) OR glucose absorbed by facilitated diffusion
- Glucose converted to glycogen / glucogenesis
- Increased (use of glucose in) respiration / ATP production
- If lower glucose concentration alpha cells (in pancreas) release glucagon
- (increased) conversion of glycogen to glucose / glycogenolysis
- (increased conversion of other compounds (amino acids / lipids) to glucose / gluconeogenesis
Q: After a meal, the concentrations of glucose and insulin in the blood increase. Explain why there is a delay in the increase of insulin concentration following the increase in blood glucose concentration. (2 MARKS)
- Increase (in blood sugar) is detected (by beta cells)
- Idea that takes time for depolarisation (in beta cells) OR time needed for beta cells to produce / release / secrete insulin
Q: Where precisely in the body are the insulin and glucagon each secreted. (4 MARKS)
- Insulin - beta cells
- Glucagon - alpha cells
- In the islets of Langerhans
- In the pancreas
Q: Figure 11 shows how the blood glucose concentration of a healthy, non-diabetic person varied over 24 hours.
The person ate 3 carbohydrate-rich meals at the times shown in figure 11
i) Write the letter X on figure 11 to show one time when the insulin concentration would be highest (1 MARK)
ii) Explain why you chose this time (1 MARK)
iii) Figure 11 shows blood glucose concentration in a healthy, non-diabetic person. Describe two ways in which a similar graph, drawn for a diabetic person, would differ from this. (2 MARKS)
i) ‘X’ on either side or both of the glucose peaks at 08:30 / 16:30
ii) - Insulin lowers blood glucose / stimulates uptake of glucose by cells / by liver / by muscles
- OR High blood glucose stimulates insulin secretion
iii) - Higher glucose concentrations in diabetic
- Takes longer time to decrease / remains high (after each meal)
Q: Type 1 diabetes inject insulin.
Different forms of modified human insulin are available for diabetics to use.
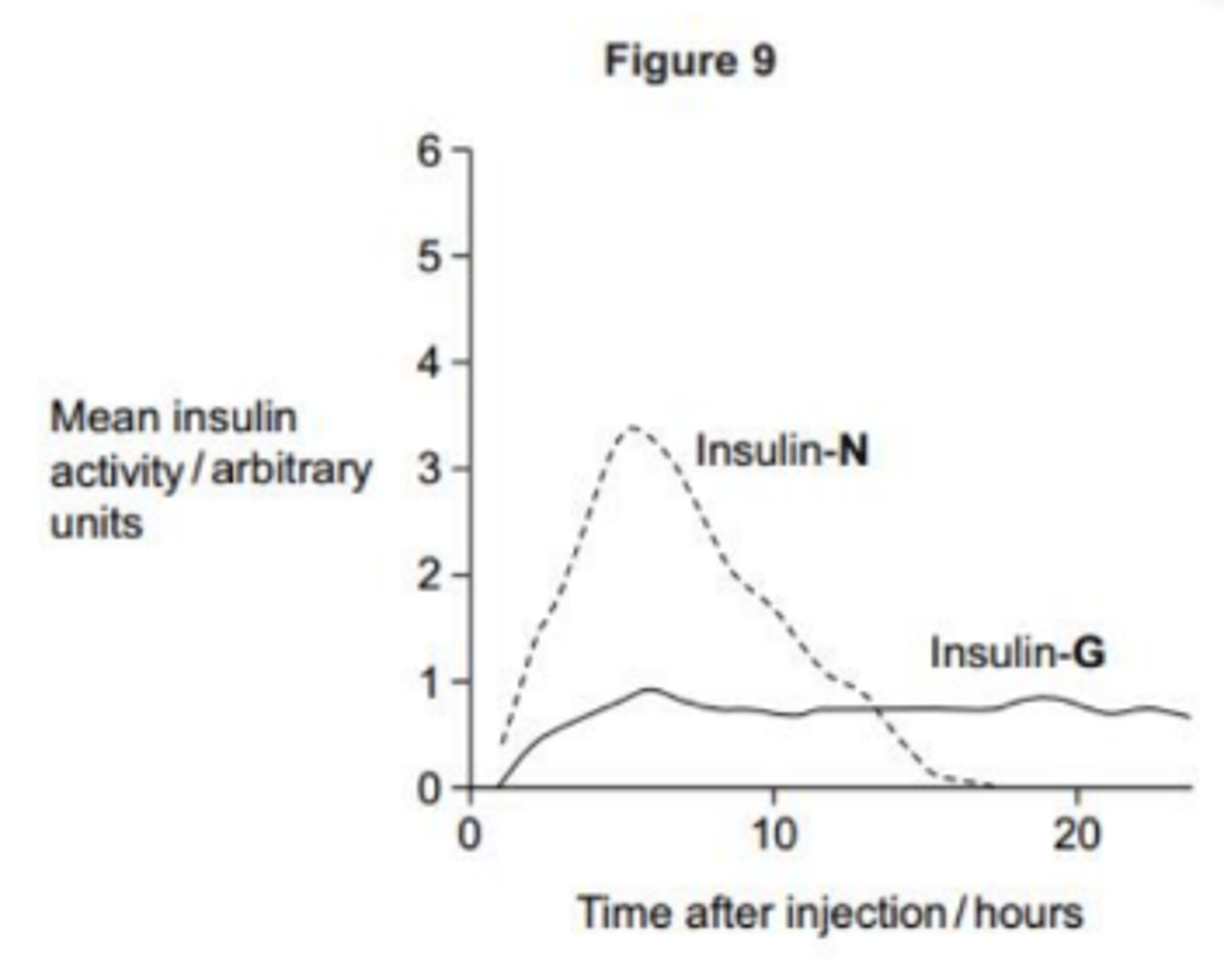
Scientists investigated the activity in the blood of two modified forms of human insulin, N and G. One group of diabetics injected themselves with insulin-N. The second group injected themselves with insulin-G. The scientists then measured the activity of the insulin in blood samples taken from each group at hourly intervals over the next 24 hours.
Their results are shown in figure 9.
Suggest how each of these two types of insulin might be used to manage a patient’s diabetes. (4 MARKS)
- N - has high activity / acts quickly
- N - will lead to greater/faster lowering of blood glucose (than G)
- N - (relatively) short-lived effect
- N - may need >1 injection per day
- N - useful around meal times
- G - fairly constant level of insulin (activity)
Q: When insulin binds to receptor on liver cells, it leads to the formation of glycogen from glucose. This lowers the concentration of glucose in liver cells.
Explain how the formation of glycogen in liver cells leads to a lowering of blood glucose concentration. (4 MARKS)
- Glucose concentration in cell / liver falls
- Below that in blood (plasma)/ higher in blood
- creates/maintains glucose concentration/diffusion gradient
- Glucose enters cell/leaves blood by facilitated diffusion/via carrier (protein)/channel (protein)
Q: Describe how glucagon is involved in the regulation of blood glucose concentration in a person who is able to regulate their blood glucose correctly. (5 MARKS)
- (When blood glucose concentration decreases) glucagon released by the alpha cells
- In islets of Langerhans / pancreas
- Promotes/initiates/leads to conversion of glycogen to glucose/glycogenolysis (in liver/muscle cells)
- Promotes / initiates / leads to gluconeogenesis/conversion of non carbs / lipids / amino acids to glucose
- Negative feedback reduces / inhibits the secretion of glucagon
Q: Diabetic people who do not control their blood glucose concentration may become unconscious and go into a coma. A doctor may inject a diabetic person who is in a coma with glucagon. Explain how glucagon would affect the person’s blood glucose concentration. (3 MARKS)
- Glycogen to glucose/glycogenolysis
- By activating enzymes
- Gluconeogenesis
Q: Adrenaline binds to receptors in the plasma membranes of liver cells. Explain how this causes teh blood glucose concentration to increase. (2 MARKS)
- Adenylate cyclase activated / cAMP produced / second messenger produced OR activates enzyme(s) (in cell)
- (So) glycogenolysis / gluconeogenesis occurs / glucogenesis inhibited
Q: Insulin only remains in the bloodstream for a relatively short time. It is broken down in the liver. Explain what might happen to a person if the liver did not break down insulin. (3 MARKS)
- Blood glucose (concentration) would fall too low / below normal level
- Idea that glucose would continue to be taken up by cells /liver / muscle (results in low blood glucose) OR idea that glucose is continually converted into glycogen / would store too much glucose as glycogen
- (Mitochondria eventually) cannot release enough energy / generate enough ATP (as less available glucose in blood) OR (leads to) coma / death
Q: Adrenaline affects a range of target tissues in the body. Suggest how the adrenaline molecule can cause different effects in different target tissues. (2 MARKS)
- Different tissues have different (types of adrenaline) receptors
- (causing) cAMP concentration to increase or decrease OR second messenger (may be) different OR cAMP / second messenger activates different / other enzymes / enzyme reactions (in different target cells)
Q: Hormonal control of heart rate is achieved by hormones acting on the sino-atrial node (SAN). Suggest how adrenaline brings about a response inside the cells of the SAN. (3 MARKS)
- Adrenaline binds to receptor(s) on cell surface membrane (of SAN cell(s))
- Activates adenyl(yl) cyclase OR ATP converted to cyclic AMP / cAMP or cyclic AMP / cAMP / second messenger synthesised
- Results in depolarisation (of SAN cell membrane)
Q: Scientists made an artificial gene which codes for insulin. They put the gene into a virus which was then injected into rats with type I diabetes. The virus was harmless to the rats but carried the gene into the cells of the rats. The treated rats produced insulin for up to 8 months and showed no side effects.
The scientists measured the blood glucose concentrations of the rats at regular intervals. While the rats were producing insulin, their blood glucose concentrations were normal. The rats were not fed for at least 6 hours before their blood concentration was measured. Explain why. (2 MARKS)
- Glucose/sugar in food would affect the results/food/eating would affect blood glucose (level)
- (allows time for) blood glucose (level) to return to normal
Q: Scientists made an artificial gene which codes for insulin. They put the gene into a virus which was then injected into rats with type I diabetes. The virus was harmless to the rats but carried the gene into the cells of the rats. The rats used in the investigation had type I diabetes.
This form of gene therapy may be less effective in treating rats that have type II diabetes. Explain why. (1 MARK)
Type 2 diabetes is a failure to respond to insulin / still produces insulin / is not insulin-dependent
Q: Describe three factors that increase a person’s risk of developing Type 2 diabetes. (3 MARKS)
- Increasing age/older/ageing/more prevalent over 40
- (idea of) family history / genetic/hereditary
- (more common in) males
- (more common in) some ethnic groups / African / Aro-caribbean / Asian / Hispanic / oceanic
- Obese/overweight/fat abdomen
- High/frequent intake of sugar / highly processed food / high GI food
- Lack of physical activity / sedentary lifestyle
- High blood pressure OR excessive alcohol intake
Q: A 55-year-old man visited the doctor and was newly diagnosed with diabetes
- The doctor initially recommended to the man that he should change his diet to cut out excess carbohydrates, including sugars such as glucose and make a further appointment to check his progress
- At this second appointment, however, it was discovered that the dietary changes had not been effective, which was unexpected
- It turns out that the man had a form of diabetes that required daily hormone injections to control his blood sugar concentration.
Using only the information given above, state how this man’s form of diabetes is similar to:
1. Type 1 diabetes
2. Type 2 diabetes
(2 MARKS)
1. Requires (daily) insulin/hormone injections OR is not affected by dietary changes ACCEPT insulin not being produced in sufficient quantities
2. Idea that has developed in an old(er) person / middle age / a 55 year old
Q: A doctor arranged for a 59-year-old patient to have a series of blood tests. One of these tests was to determine the patients ‘fasting blood glucose’ concentration.
- The result of this test indicates whether or not the patient's blood glucose concentration is being regulated within the normal range
- The validity of the result relies on the patient not having eaten for at least 8 hours before the test
- The patient confirmed to the doctor that he had not eaten since the previous evening
1. What condition was being tested for in this 59-year-old patient? (1 MARK)
2. Why was it important that the patient had not eaten for at least 8 hours before the test? (1 MARK)
1. Diabetes (meliltus)
2. Idea that time needed to restore normal (blood) glucose concentration/for insulin to act (fully)
Q: A patient shows severe symptoms of unregulated blood glucose concentration. Under certain circumstances, this condition may need to be treated with glucagon injections.
Under what circumstances might this patient need to be given a glucagon injection? (1 MARK)
- If blood glucose falls extremely/dangerously/too/very low
- OR if patient cannot produce (enough) glucagon / produces little glucagon
- OR idea that glucose source cannot be taken by mouth
Q: Hormonal control of heart rate is achieved by hormones acting on the sino-atrial (SAN). The adrenaline molecule is not lipid-soluble, therefore it cannot pass directly through the cell surface membrane. Suggest how adrenaline brings about a response inside the cells of the SAN. (4 MARKS)
- Adrenaline binds to receptor(s) on cell surface membrane (of SAN cell(s))
- Activates adenyl(yl) cyclase
- ATP converted to cyclic AMP / cAMP OR cyclic AMP / cAMP / second messenger synthesised
- Results in depolarisation (of SAN cell membrane)
Q: Adrenaline affects a range of target tissues in the body. Suggest how the adrenaline molecule can cause different effects in target tissues. (2 MARKS)
- Different tissues have different (types of adrenaline) receptors
- (causing) cAMP concentration to increase or decrease OR second messenger (may be) different OR cAMP / second messenger activates different / other enzymes/enzymes reactions (in different target cells)
Q: The adrenaline molecule is not lipid-soluble, therefore it cannot pass directly through the cell surface membrane. In order to bring about changes in the cell, adrenaline relies on a second messenger system.
The second messenger system is a multi-step mechanism. It enables large changes in cell metabolism to occur rapidly, although only relatively small number of adrenaline molecules are involved.
Suggests how having a number of steps in the signalling pathway enables a small number of adrenaline molecules to rapidly cause large effects. (1 MARK)
- Idea that one molecule causes production/activation of many others
- OR idea that this multiplying effect is repeated at next / every / later step
- OR idea of recycling / temporary binding of cAMP
Q: Adrenaline binds to receptors in the plasma membranes of live cells. Explain how this causes the blood glucose concentration to increase. (3 MARKS)
- Adenylate cyclase activated / cAMP produced / second messenger produced
- Activates enzyme(s) (in cell)
- (So) glycogenolysis / gluconeogenesis occurs / glycogenesis inhibited
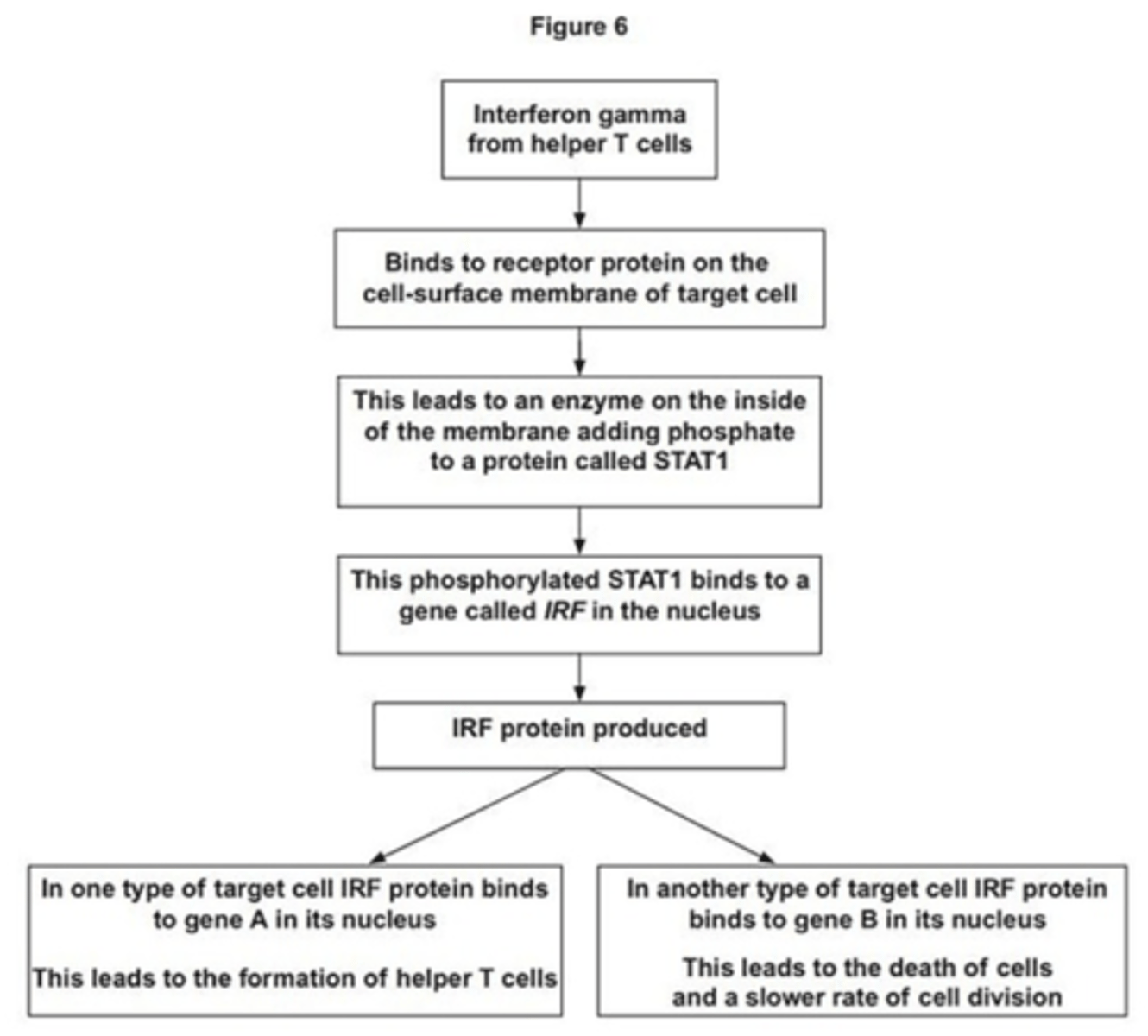
Q: Interferon-gamma is a substance secreted by some types of white blood cells, including helper T cells. It regulates the production of a number of proteins by target cells. Which protein is produced depends on the type of target cell.
Figure 6 shows how interferon gamma regulates three genes. Use information in Figure 6 to suggest how the binding of interferon-gamma to its receptor protein leads to the production of phosphorylated STATI. (2 MARKS)
- Binding (of interferon-gamma) change shape/tertiary structure of receptor (protein)/ Accept reference to second messenger mechanism/process
- This activates/switches on the enzyme
- Use of ATP (to phosphorylate STAT1);
EQ: Each year, a few people with type I diabetes are given a pancreas transplant. Pancreas transplants are not used to treat people with type II diabetes.
Give two reasons why pancreas transplants are not used for the treatment of type II diabetes. (2 MARKS)
1. (Usually)Type II produce insulin;
2. Cells/receptors less sensitive/responsive (to insulin) OR Faulty (insulin) receptors;
3. (Treated/controlled by) diet/exercise;
EQ: The pancreas produces the hormone insulin. Put a tick (x) in the box next to the statement which describes incorrectly the action of insulin.
1. Activates enzymes involved in the conversion of glucose to glycogen.
2. Controls the uptake of glucose by regulating the inclusion of channel proteins in the surface membranes of target cells.
3. Attaches to receptors on the surfaces of target cells.
4. Activates enzymes involved in the conversion of glycerol to glucose.
4th one.
EQ: Describe the role of glucagon in gluconeogenesis. Do not include in your answer details on the second messenger model of glucagon action. (2 MARKS)
1. (Attaches to receptors on target cells and) activates/stimulates enzymes;
2. Glycerol/amino acids/fatty acids into glucose;
EQ: The gene that codes for glucagon is 9.531kilobases in length. The DNA helix makes one complete turn every 10 base pairs. Every complete turn is 3.4 nm in length.
Use this information to calculate the length in micrometres (µm) of the gene for glucagon. Give your answer to 3 significant figures. (2 MARKS)
1. Correct answer of 3.24 = 2 marks;;
2. Incorrect but multiplies by 34 (with decimal point in any position) = 1 mark OR Incorrect but shows sequence 324 = 1 mark OR 3.2 = 1 mark;
EQ: Metformin is a dru box g commonly used to treat type II diabetes. Metformin’s ability to lower the blood glucose concentration involves a number of mechanisms including:
• increasing a cell’s sensitivity to insulin
• inhibiting adenylate cyclase.
Explain how increasing a cell’s sensitivity to insulin will lower the blood glucose concentration. (2 MARKS)
1. (More) insulin binds to receptors;
2. (Stimulates) uptake of glucose by channel/transport proteins OR Activates enzymes which convert glucose to glycogen;
EQ: Metformin is a dru box g commonly used to treat type II diabetes. Metformin’s ability to lower the blood glucose concentration involves a number of mechanisms including:
• increasing a cell’s sensitivity to insulin
• inhibiting adenylate cyclase.
Explain how inhibiting adenylate cyclase may help to lower the blood glucose concentration. (3 MARKS)
1. Less/no ATP is converted to cyclic AMP/cAMP;
2. Less/no kinase is activated;
3. Less/no glycogen is converted to glucose OR Less/no glycogenolysis;
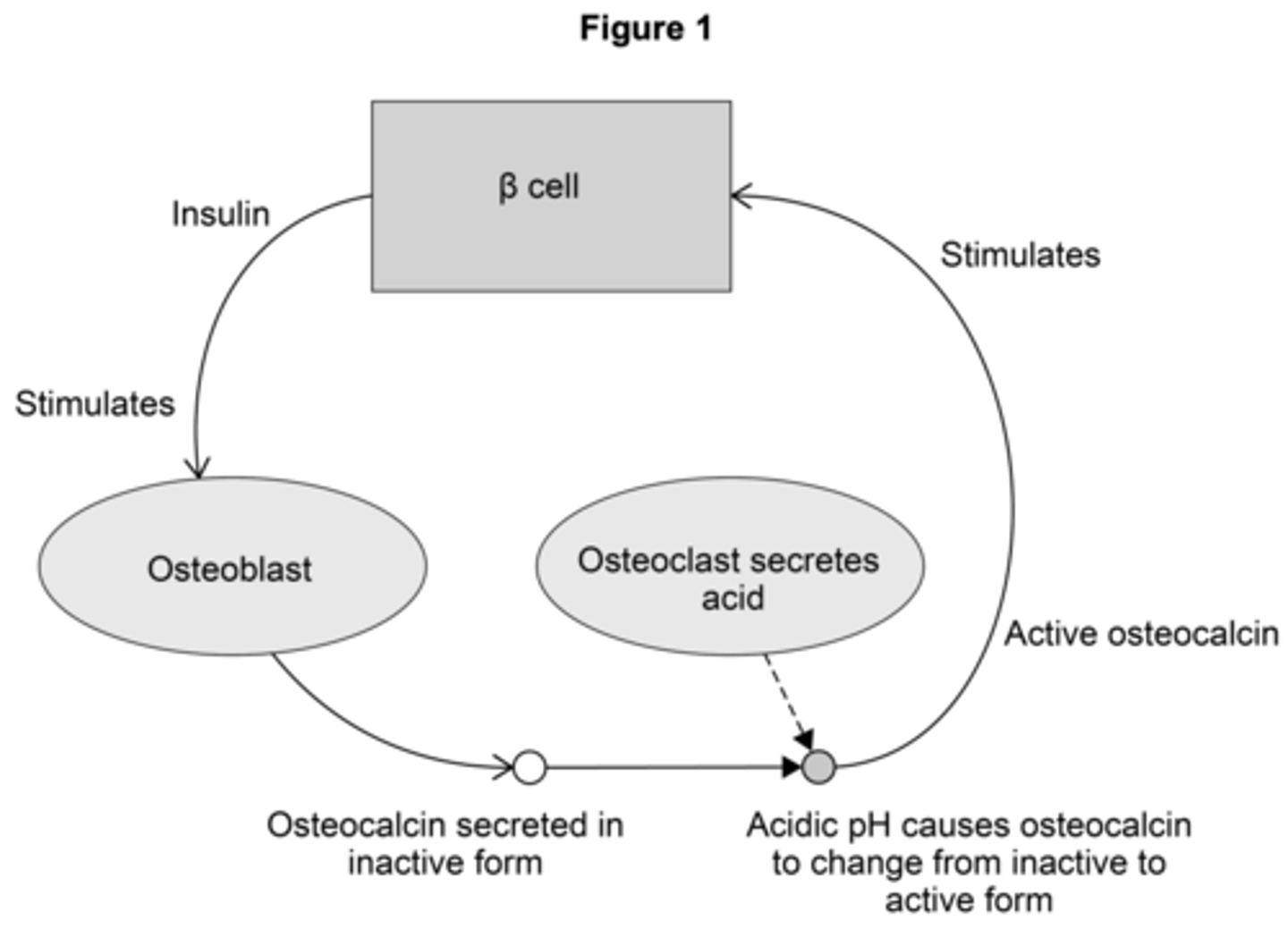
EQ: Broken bones are repaired by cells called osteoclasts and osteoblasts.
Osteoblasts secrete a hormone called osteocalcin in an inactive form. Osteocalcin is a protein. The active form of osteocalcin binds to a receptor on beta (β) cells in the pancreas, stimulating them to release insulin. Osteoblasts have receptors for insulin.
Figure 1 shows how the production of osteocalcin by osteoblasts is controlled by positive feedback.
The acidic pH conditions created by osteoclasts cause the inactive form of the protein osteocalcin to change into the active form of osteocalcin. Suggest how. (2 MARKS)
1. (Change in pH) changes / breaks ionic / hydrogen bonds;
2. Changes tertiary structure;
EQ: Broken bones are repaired by cells called osteoclasts and osteoblasts.
Osteoblasts secrete a hormone called osteocalcin in an inactive form. Osteocalcin is a protein. The active form of osteocalcin binds to a receptor on beta (β) cells in the pancreas, stimulating them to release insulin. Osteoblasts have receptors for insulin.
Figure 1 shows how the production of osteocalcin by osteoblasts is controlled by positive feedback.
Binding of insulin leads to an increase in the rate of respiration in cells such as osteoblasts. Explain how. (2 MARKS)
1. (Insulin) leads to more transport proteins / channel (proteins) / carrier (proteins) for glucose;
2. More glucose (for respiration / glycolysis) enters cell;
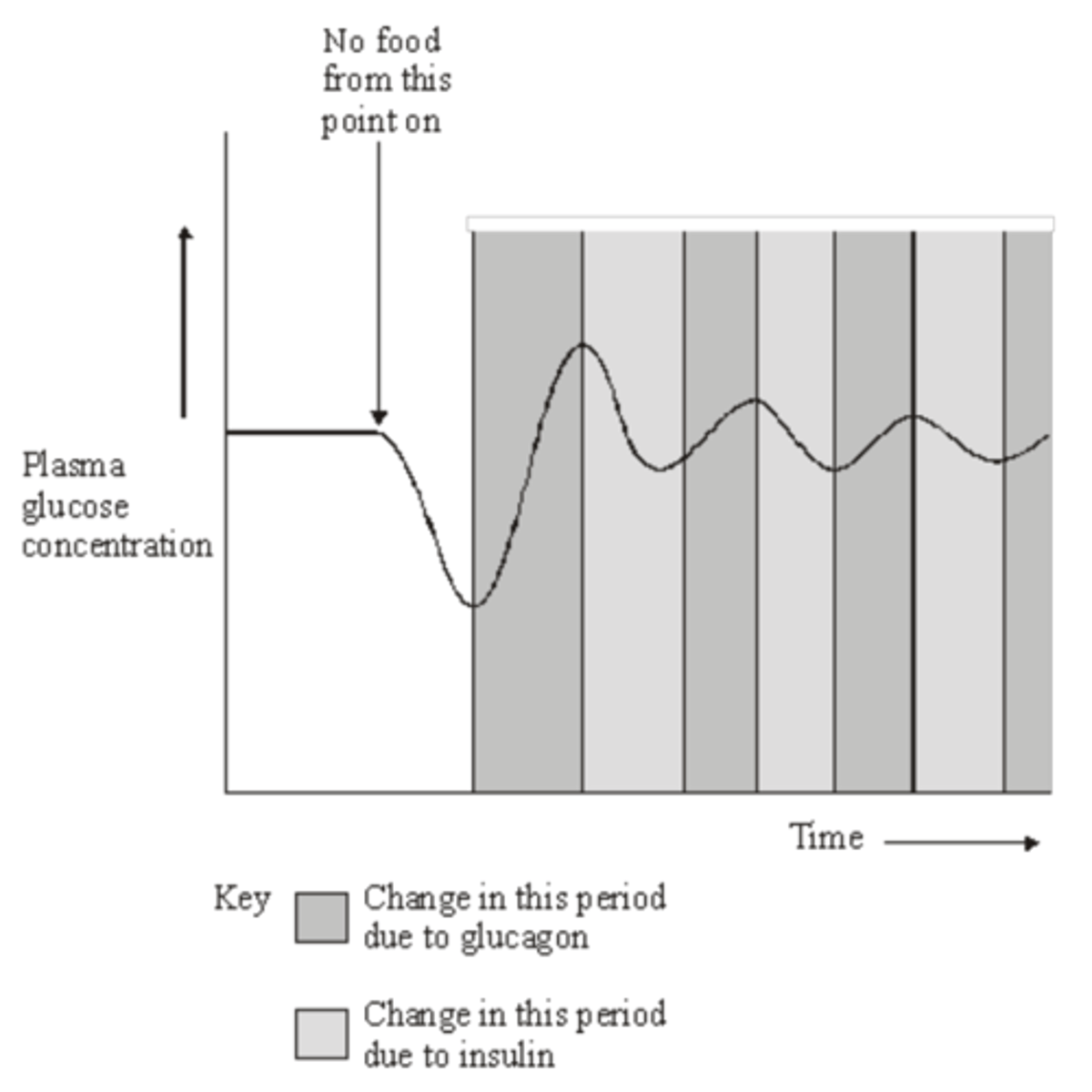
Q: Homeostatic mechanisms maintain a constant environment in the body.
The graph shows changes in plasma glucose concentration that occurred in a person who went without food for some time.
Use evidence from the graph to explain the role of negative feedback in the control of plasma glucose concentration. (5 MARKS)
1. Deviation of a value from norm initiates corrective mechanisms;
2. fluctuations in plasma glucose concentration detected by hypothalmus / islet cells in pancreas;
3. initial decrease, no food given (in plasma glucose) stimulates (increased) secretion of glucagon;
4. increases (in plasma glucose) stimulate (increased) secretion of insulin from β cells as secretors;
5. correct ref. to interconversion of glycogen / glucose / increased / decreased uptake of glucose by cells (as appropriate) / correct ref to change in membrane permeability;
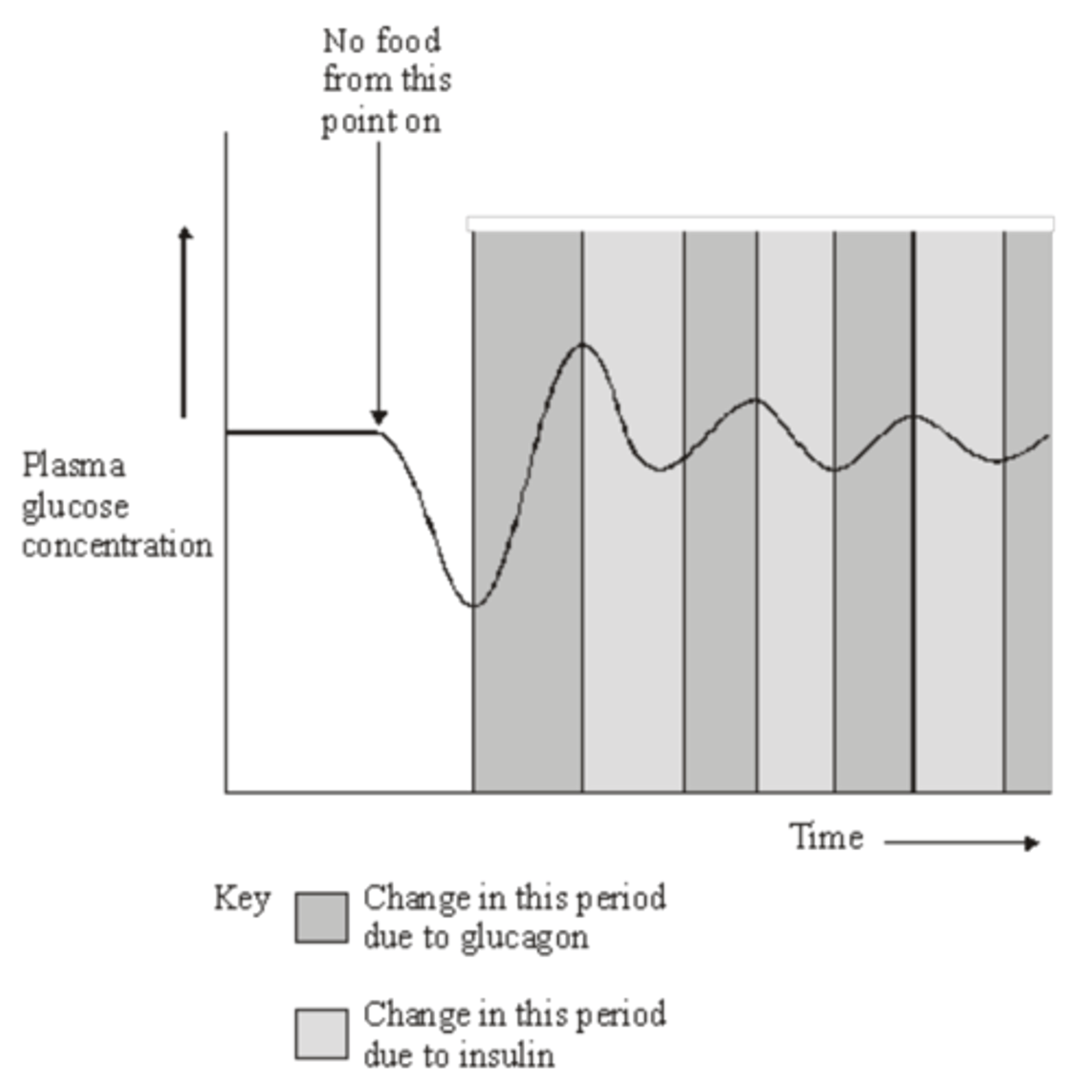
Q: Homeostatic mechanisms maintain a constant environment in the body.
The graph shows changes in plasma glucose concentration that occurred in a person who went without food for some time.
How does maintaining a constant body temperature allow metabolic reactions in cells to proceed with maximum efficiency? (5 MARKS)
1. Body temp. / 37 °C is optimum temp for enzymes;
2. excess heat denatures enzymes / alters tertiary structure / alters shape of active site / enzyme so substrate cannot bind / eq;
3. reactions cease / slowed;
4. too little reduces kinetic energy of molecules / moleculesmove more slowly;
5. fewer collisions / fewer ES complexes formed'
Q: Adrenaline binds to receptors in the plasma membranes of liver cells. Explain how this causes the blood glucose concentration to increase. (2 MARKS)
1. Adenylate cyclase activated / cAMP produced / second messenger produced;
2. Activates enzyme(s) (in cell so) glycogenolysis / gluconeogenesis occurs / glycogenesis inhibited;
Q: Scientists made an artificial gene which codes for insulin. They put the gene into a virus which was then injected into rats with type I diabetes. The virus was harmless to the rats but carried the gene into the cells of the rats.
The treated rats produced insulin for up to 8 months and showed no side-effects. The scientists measured the blood glucose concentrations of the rats at regular intervals. While the rats were producing the insulin, their blood glucose concentrations were normal.
(i) The rats were not fed for at least 6 hours before their blood glucose concentration was measured. Explain why. (1 MARK)
(ii) The rats used in the investigation had type I diabetes. This form of gene therapy may be less effective in treating rats that have type II diabetes. Explain why. (1 MARK)
(iii) Research workers have suggested that treating diabetes in humans by this method of gene therapy would be better than injecting insulin. Evaluate this suggestion. (4 MARKS)
(i) 1. Glucose / sugar in food would affect the results; 1. Accept references to starch / carbohydrate
Or 2. Food / eating would affect blood glucose (level);
Or 3. (Allows time for) blood glucose (level) to return to normal; 3. Neutral: allows time for insulin to act
(ii) Type 2 diabetes is a failure to respond to insulin / still produces insulin / is not insulin-dependent;
(iii) (For) - 3 max
1. Avoids injections / pain of injections;
2. Long(er) lasting / permanent / (new) cells will contain / express gene; Ignore references to methodology e.g. sample size not known
3. Less need to measure blood sugar / avoids the highs and lows in blood sugar;
4. Less restriction on diet;
(Against) - 3 max
5. Rats are different to humans;
6. May have side effects on humans; 6. Accept: virus may be harmful / disrupt genes / cause cancer
7. Long(er) term effects (of treatment) not known / may have caused effects after 8 months;
8. (Substitute) insulin may be rejected by the body;
Q: A diabetic person and a non-diabetic person each ate the same amount of glucose. One hour later, the glucose concentration in the blood of the diabetic person was higher than that of the non-diabetic person. Explain why. (3 MARKS)
1. Lack of insulin / reduced sensitivity of cells to insulin;
2. Reduced uptake of glucose by cells / liver / muscles;
3. Reduced conversion of glucose to glycogen;
The urine of a non-diabetic person does not contain glucose. Explain why. (2 MARKS)
- Leaves the blood at kidney;
- Taken back into blood / reabsorbed (from kidney tubule);
- (Reabsorbed) in 1st convoluted tubule;
Q: A high blood glucose concentration could cause glucose to be present in the urine of a diabetic person. Suggest how. (2 MARKS)
- Large amount / high concentration of glucose in filtrate;
- Cannot all be reabsorbed / 1st convoluted tube too short to reabsorb all of glucose / saturation of carriers;
Q: A test for glucose in urine uses immobilised enzymes on a plastic test strip. One of these enzymes is glucose oxidase. Explain why the test strip detects glucose and no other substance. (2 MARKS)
- Enzyme has specific shape to active site / active site has specific tertiary structure;
- Only glucose fits / has complementary structure / can form ES complex;
Q: Some people who have diabetes do not secrete insulin. Explain how a lack of insulin affects reabsorption of glucose in the kidneys of a person who does not secrete insulin. (4 MARKS)
1. High concentration of glucose in blood;
2. High concentration in tubule / in filtrate;
3. Reabsorbed by facilitated diffusion / active transport;
4. Requires proteins / carriers;
5. These are working at maximum rate / are saturated;
6. Not all glucose is reabsorbed / some is lost in urine;
Q: Neonatal diabetes is a disease that affects newly born children. The disease is caused by a change in the amino acid sequence of insulin.
This change prevents insulin binding to its receptor. Explain why this change prevents insulin binding to its receptor. (2 MARKS)
1. Changes tertiary structure;
2. No longer complementary (to receptor);
Q: Phosphoinositide 3-kinase (PI3K) is an enzyme in several metabolic processes.
The figure below shows the role of PI3K in the control of blood glucose concentration.
A decrease in the activity of PI3K can cause type II diabetes. Use the figure above to explain why. (3 marks)
1. Less/no AKT activated;
2. Fewer/no vesicles move to membrane OR Fewer/no (channel) proteins in membrane;
3. Less/no glucose diffuses into cell (so high blood glucose);
Q: Interferon-gamma is a substance secreted by some types of white blood cells, including helper T cells. It regulates the production of a number of proteins by target cells. Which protein is produced depends on the type of target cell.
Name the two transcription factors in the diagram. (2 MARKS)
1. Phosphorylated STAT1;
2. IRF (protein);
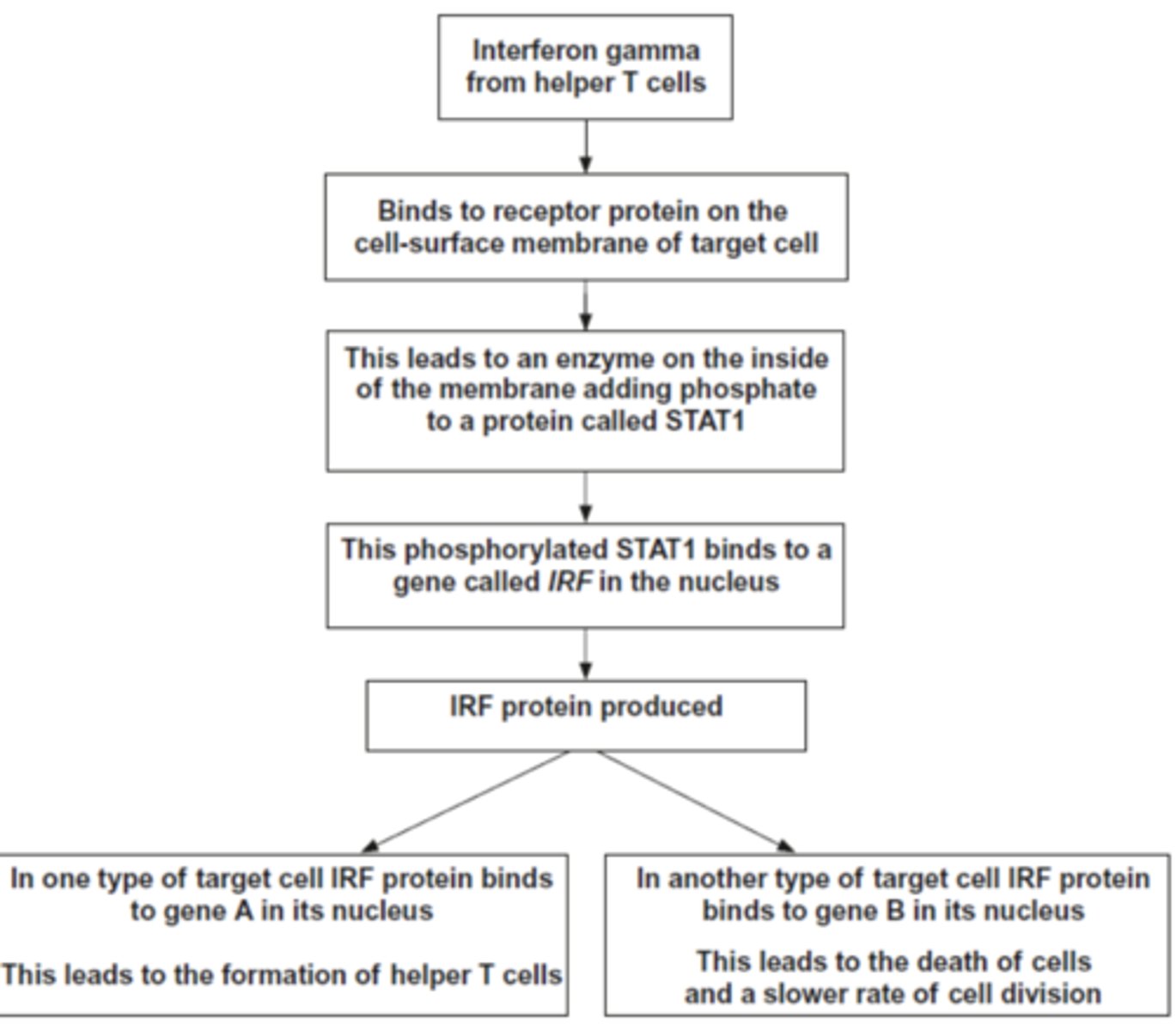
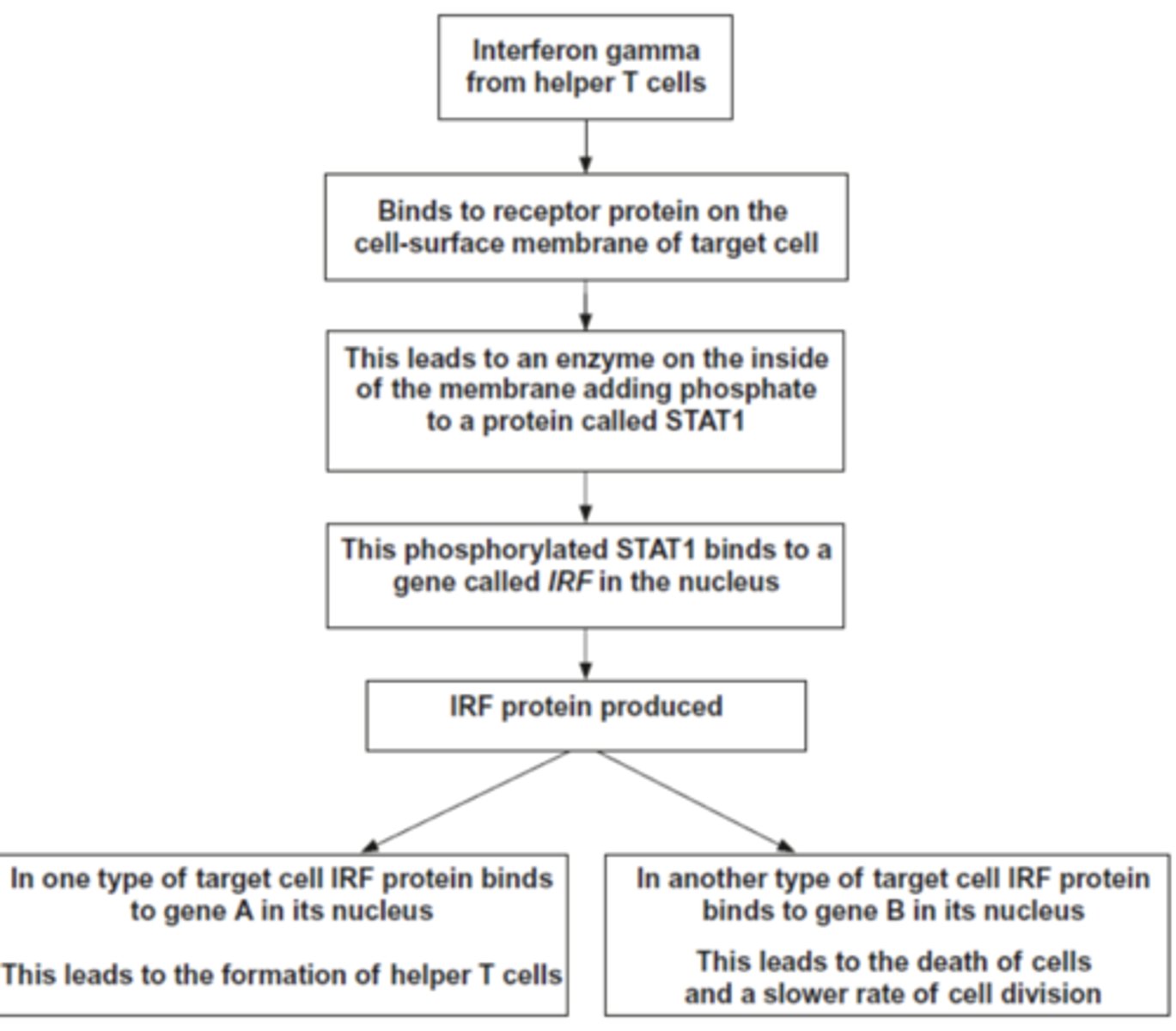
Q: Interferon-gamma is a substance secreted by some types of white blood cells, including helper T cells. It regulates the production of a number of proteins by target cells. Which protein is produced depends on the type of target cell.
The regulation of the formation of helper T cells by interferon gamma is an example of positive feedback. Explain why it is an example of positive feedback. (2 MARKS)
1. Causes more helper T cells to form;
2. (So) more interferon (gamma) production (by helper T cells);
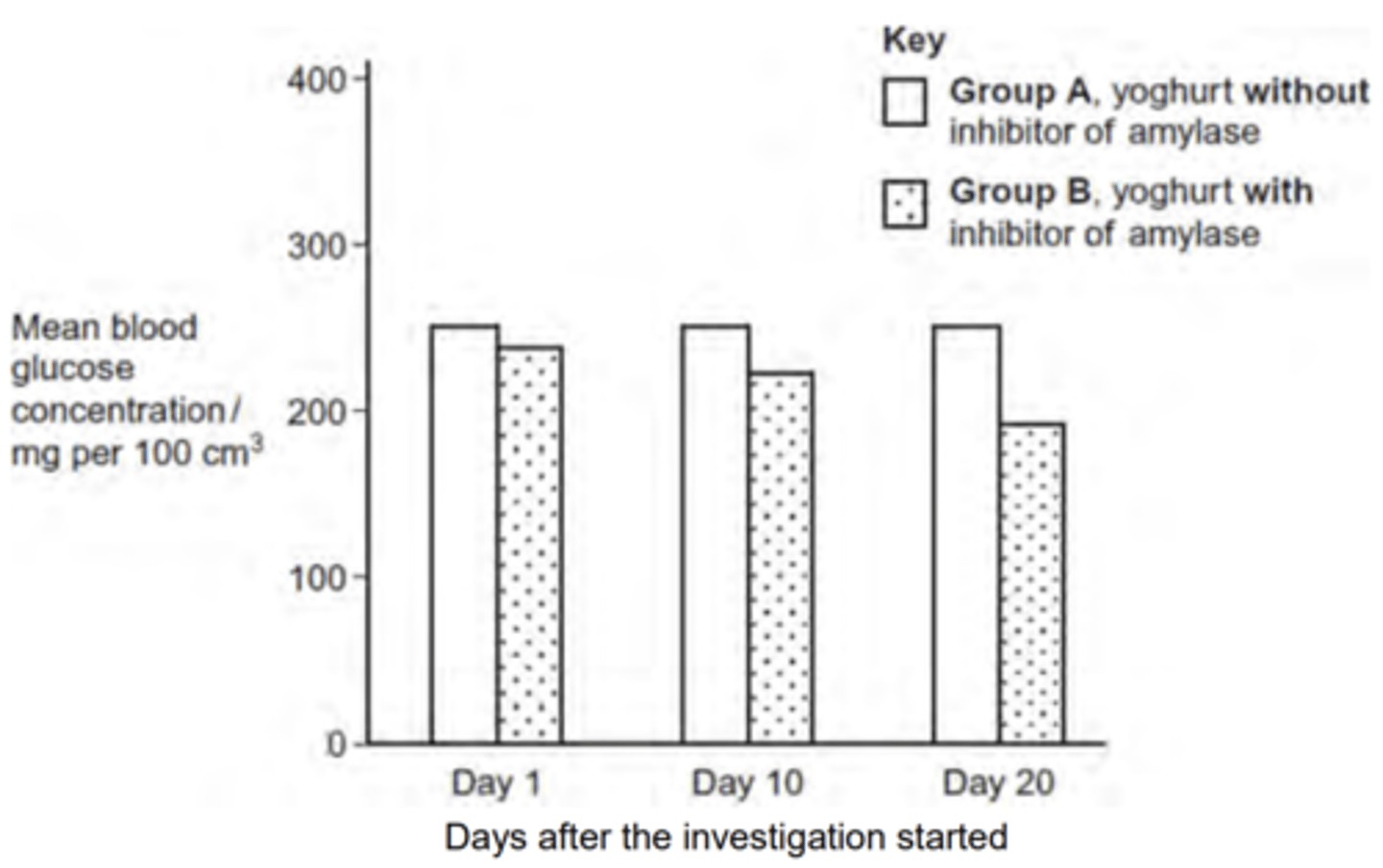
Q: Some mice have diabetes. The diabetes causes the blood glucose concentration to become very high after a meal. Scientists investigated the use of an inhibitor of amylase to treat diabetes.
The scientists took 30 mice with diabetes and divided them into two groups, A and B.
• Group A was given yoghurt without the inhibitor of amylase each day.
• Group B was given yoghurt with the inhibitor of amylase each day.
Apart from the yoghurt, all of the mice were given the same food each day.
The scientists measured the blood glucose concentration of each mouse, 1 hour after it had eaten. This was done on days 1, 10 and 20 after the investigation started.
The following figure shows the scientists’ results.
Group A acted as a control in this investigation. Explain the purpose of this group. (2 MARKS)
1. To show the effect of the inhibitor / drug;
2. To show the effect of yoghurt (on its own does not affect blood glucose);
Q: Some mice have diabetes. The diabetes causes the blood glucose concentration to become very high after a meal. Scientists investigated the use of an inhibitor of amylase to treat diabetes.
The scientists took 30 mice with diabetes and divided them into two groups, A and B.
• Group A was given yoghurt without the inhibitor of amylase each day.
• Group B was given yoghurt with the inhibitor of amylase each day.
Apart from the yoghurt, all of the mice were given the same food each day.
The scientists measured the blood glucose concentration of each mouse, 1 hour after it had eaten. This was done on days 1, 10 and 20 after the investigation started.
The following figure shows the scientists’ results.
Apart from the yoghurt, it was important that all of the mice were given the same food each day. Give two reasons why it was important that all of the mice were given the same food each day. (2 MARKS)
1. Food is a factor affecting blood glucose / different foods contain different amounts of starch / glucose / sugar / carbohydrate;
2. To keep starch / fibre intake the same / similar;
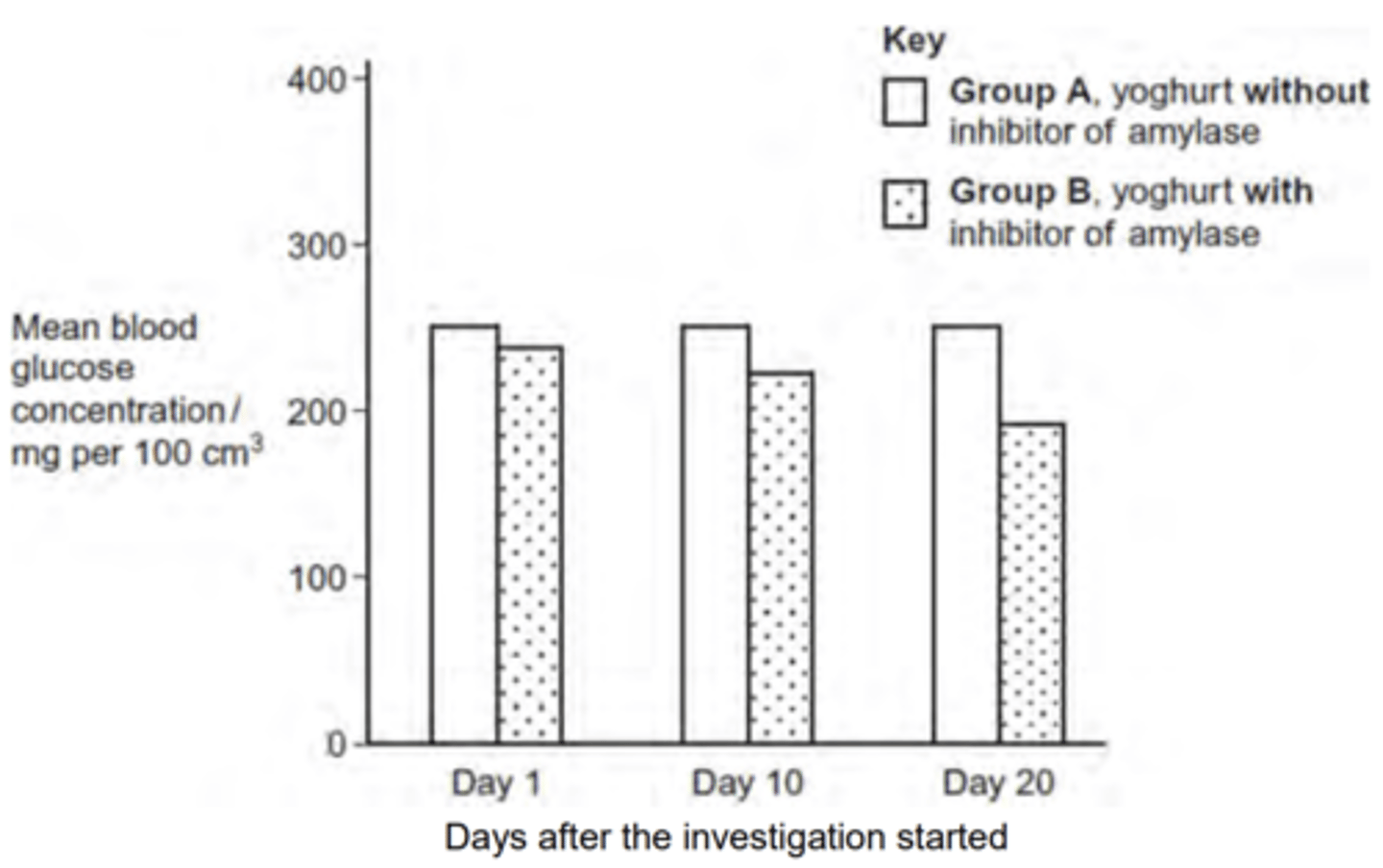
Q: Some mice have diabetes. The diabetes causes the blood glucose concentration to become very high after a meal. Scientists investigated the use of an inhibitor of amylase to treat diabetes.
The scientists took 30 mice with diabetes and divided them into two groups, A and B.
• Group A was given yoghurt without the inhibitor of amylase each day.
• Group B was given yoghurt with the inhibitor of amylase each day.
Apart from the yoghurt, all of the mice were given the same food each day.
The scientists measured the blood glucose concentration of each mouse, 1 hour after it had eaten. This was done on days 1, 10 and 20 after the investigation started.
The following figure shows the scientists’ results.
The scientists’ hypothesis was that adding the inhibitor of amylase to the food would lead to a lower blood glucose concentration.
Use your knowledge of digestion to suggest how the addition of the inhibitor could lead to a lower blood glucose concentration. (2 MARKS)
1. Fewer E-S complexes formed;
2. (With inhibitor) less / no starch digested to maltose ;
3. (So) less / no glucose from maltose;
4. (So) less absorption of glucose (from gut);
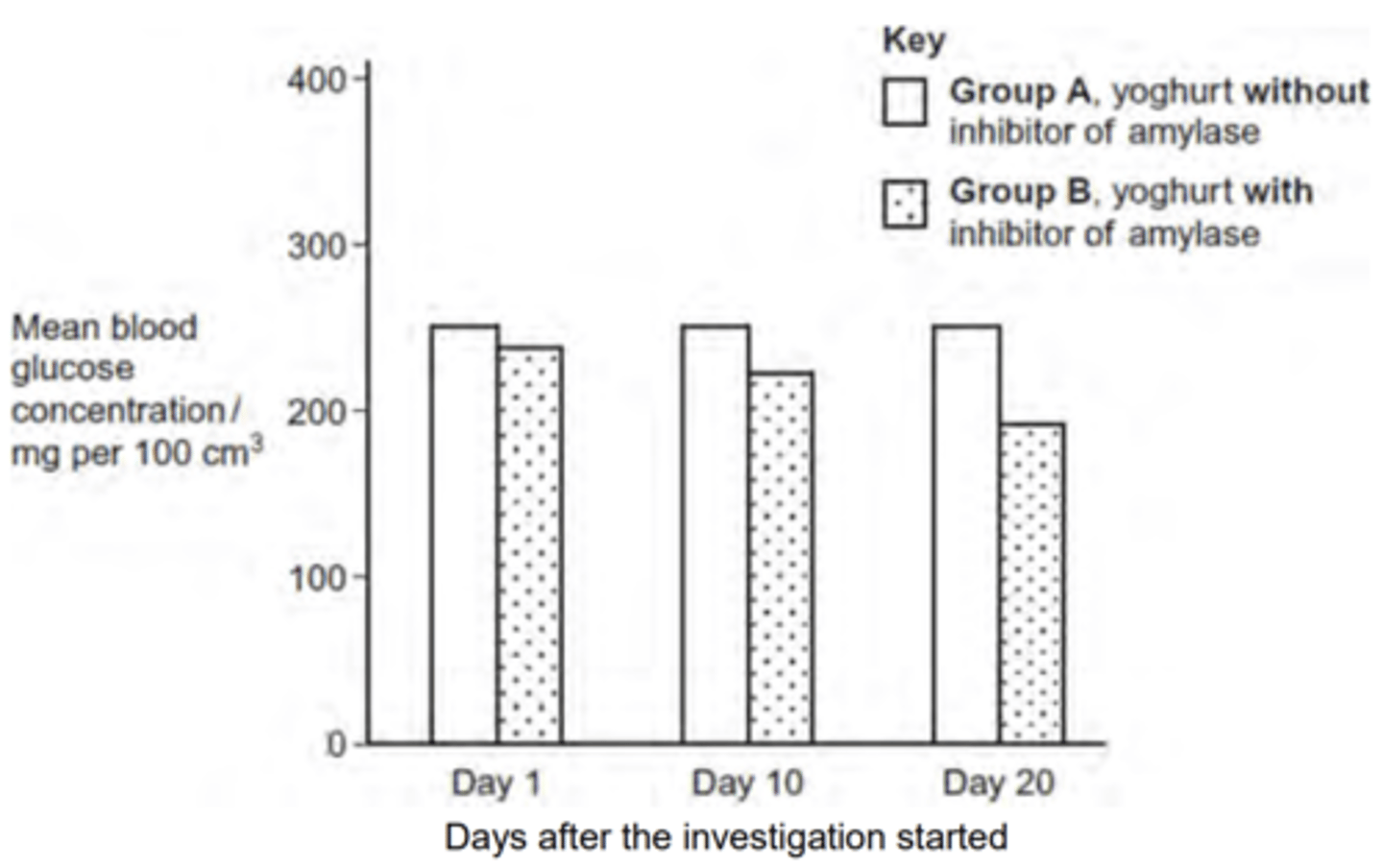
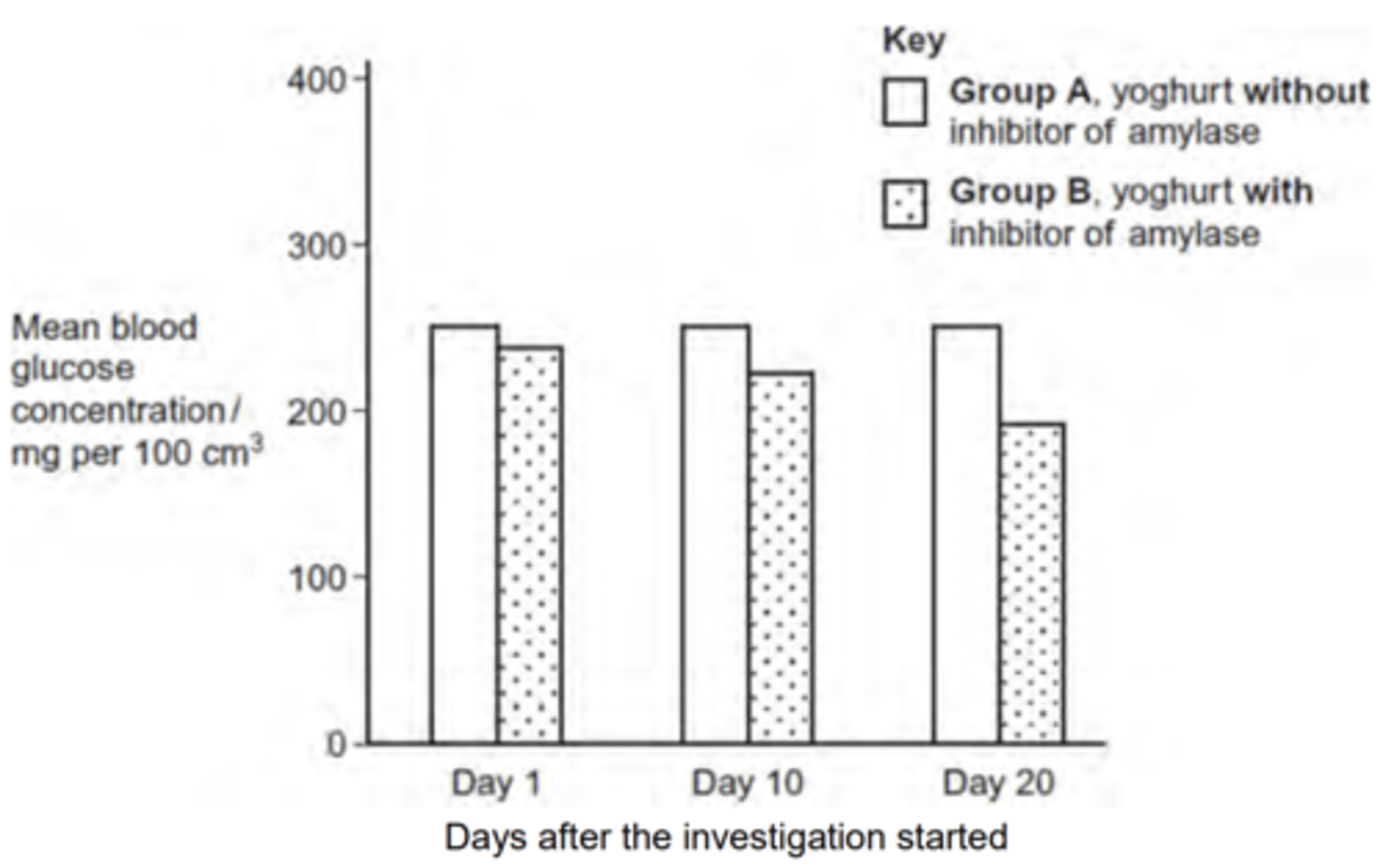
Q: Some mice have diabetes. The diabetes causes the blood glucose concentration to become very high after a meal. Scientists investigated the use of an inhibitor of amylase to treat diabetes.
The scientists took 30 mice with diabetes and divided them into two groups, A and B.
• Group A was given yoghurt without the inhibitor of amylase each day.
• Group B was given yoghurt with the inhibitor of amylase each day.
Apart from the yoghurt, all of the mice were given the same food each day.
The scientists measured the blood glucose concentration of each mouse, 1 hour after it had eaten. This was done on days 1, 10 and 20 after the investigation started.
The following figure shows the scientists’ results.
Give one reason why these results may not support the use of the inhibitor of amylase to treat diabetes in mice. (2 MARKS)
1. Need larger sample / only 30 mice / only 15 mice in each group; Accept small sample size
2. Might not be representative / anomalies might have a bigger or smaller effect; Accept mean not reliable
OR 3. Investigation only lasted 20 days; Experiment was not long enough
4. Can’t see what longer term effects are;
OR 5. Fall in blood glucose is small / numbers from graph;
6. Mice with inhibitor still have a large rise in blood glucose / so don’t know if differences significant;
OR 7. No stats / SDs / SEs;
8. So don’t know if differences significant;
OR 9. Blood glucose could continue to fall;
10. which could be harmful;
OR 11. No group without yoghurt;
12. So cannot compare to other groups;
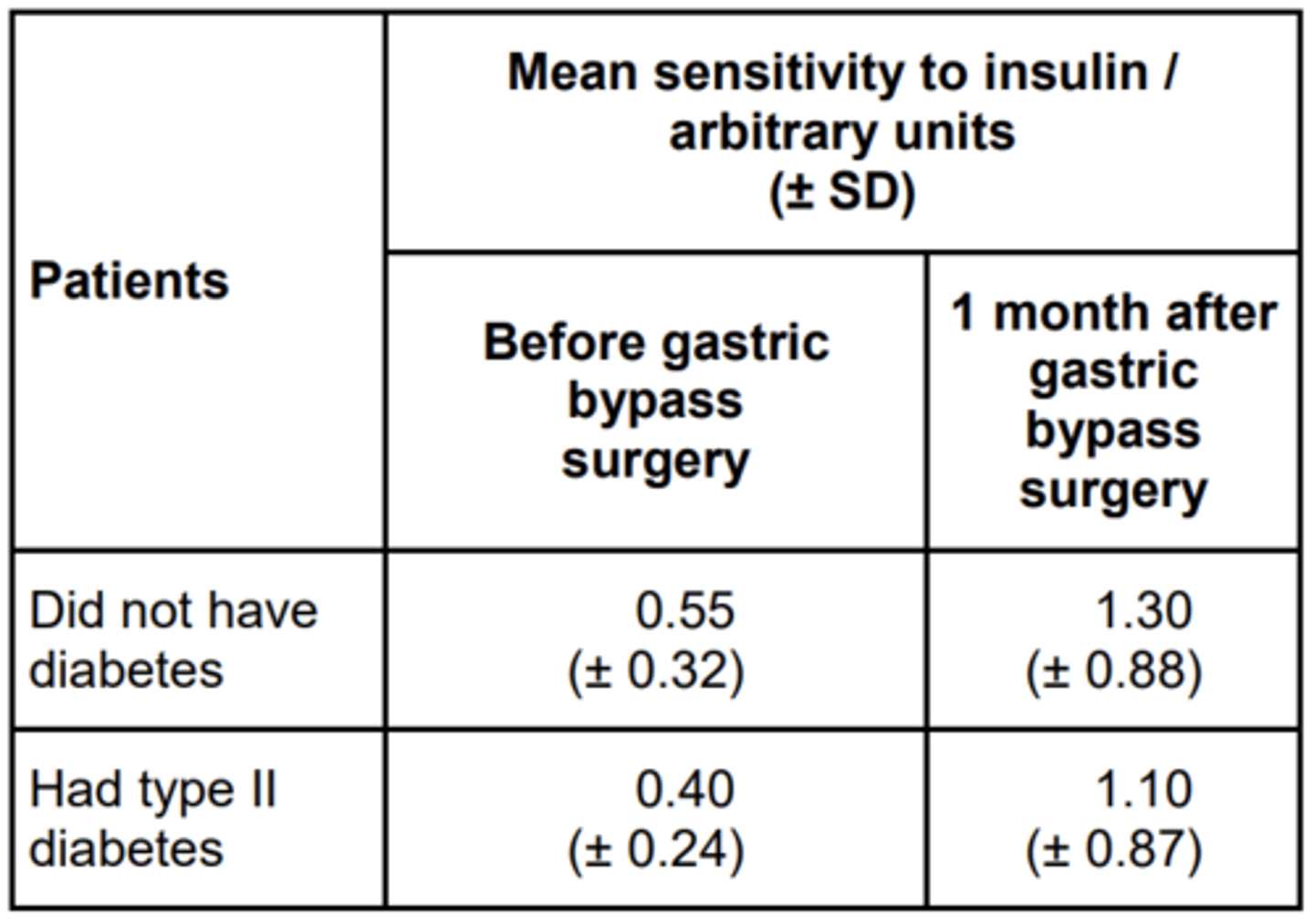
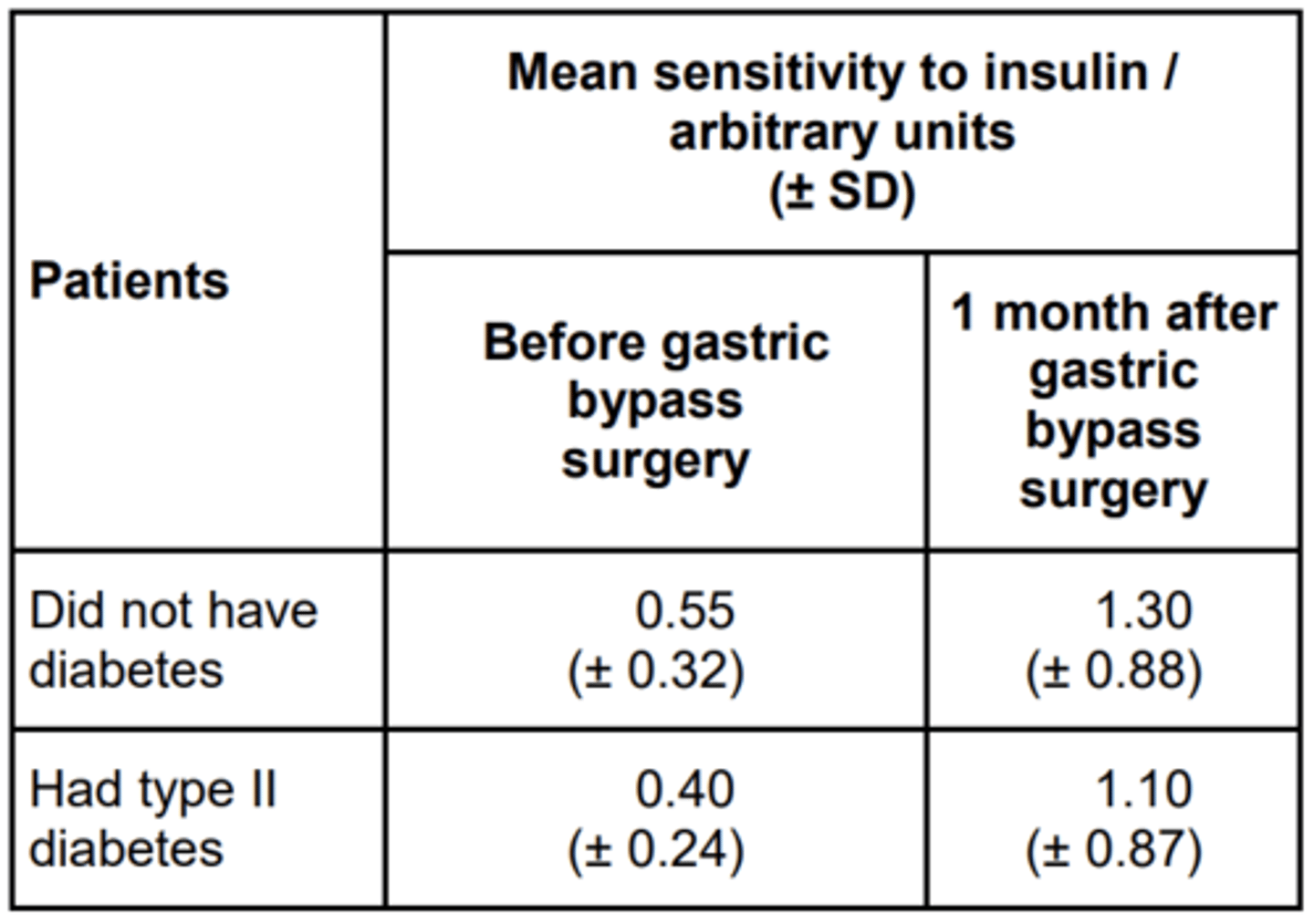
EQ: People with type II diabetes have cells with low sensitivity to insulin. About 80% of people with type II diabetes are overweight or obese. Some people who are obese have gastric bypass surgery (GBS) to help them to lose weight.
Doctors investigated whether GBS affected sensitivity to insulin. They measured patients’ sensitivity to insulin before and after GBS. About half of the patients had type II diabetes. The other half did not but were considered at high risk of developing the condition.
The table below shows the doctors’ results. The higher the number, the greater the sensitivity to insulin.
The doctors concluded that many of the patients who did not have type II diabetes were at high risk of developing the condition. Use the data in the table to suggest why they reached this conclusion. (2 MARKS)
1. Insulin sensitivity similar to / not (significantly) different from those with diabetes;
2. Overlap of SDs;
3. Their sensitivity (to insulin also) improved by GBS;
EQ: People with type II diabetes have cells with low sensitivity to insulin. About 80% of people with type II diabetes are overweight or obese. Some people who are obese have gastric bypass surgery (GBS) to help them to lose weight.
Doctors investigated whether GBS affected sensitivity to insulin. They measured patients’ sensitivity to insulin before and after GBS. About half of the patients had type II diabetes. The other half did not but were considered at high risk of developing the condition.
The table below shows the doctors’ results. The higher the number, the greater the sensitivity to insulin.
The doctors also concluded that GBS cured many patients’ diabetes but that some were not helped very much. Do these data support this conclusion? Give reasons for your answer. (3 MARKS)
1. Sensitivity (to insulin) does increase;
2. But large SD / large variation (after GBS);
3. (So) some patients showing no/little change
4. (So) some showing no / little change / get worse;
5. Do not know what sensitivity to insulin is of non-diabetics (who are not obese);
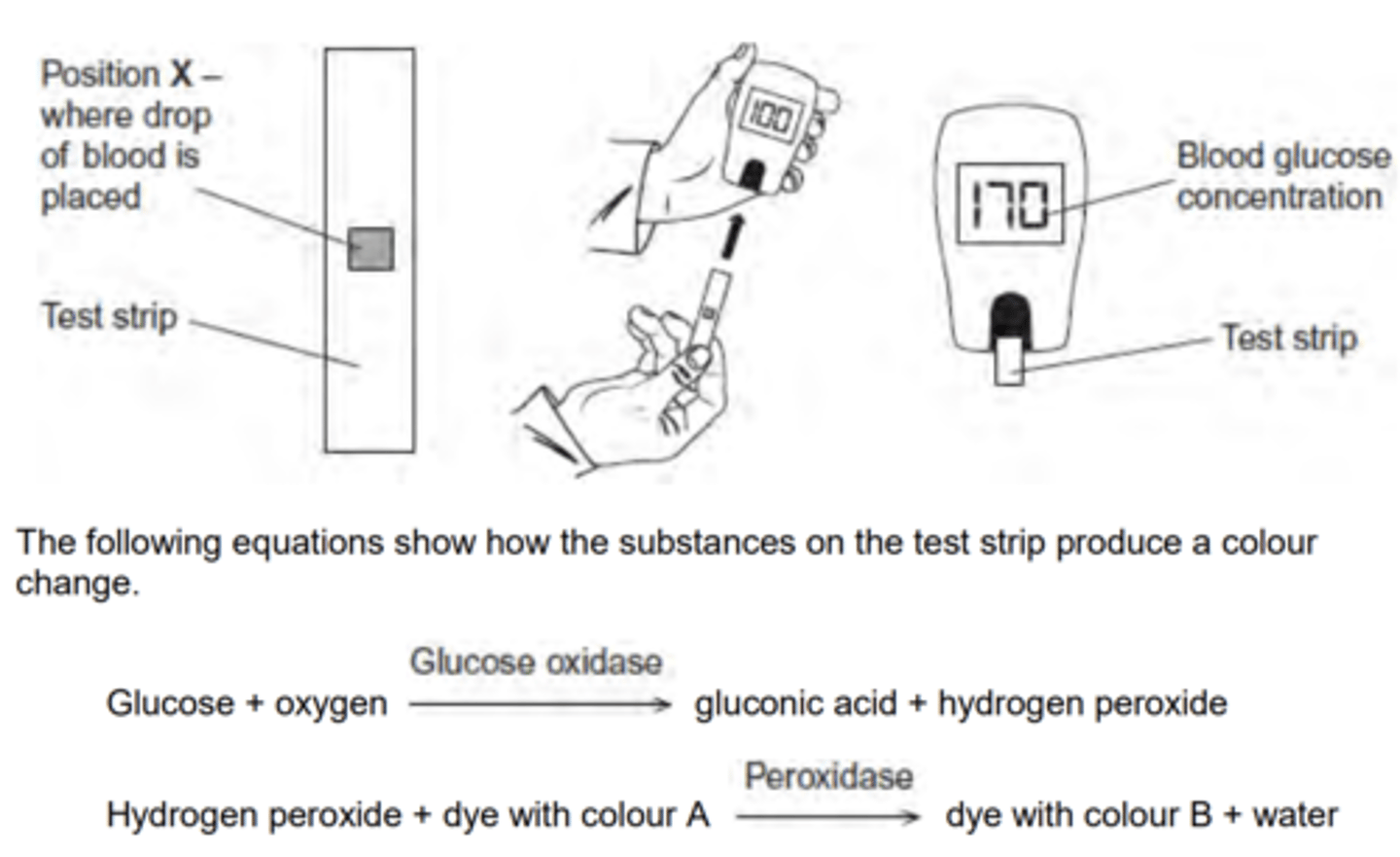
Q: A glucometer is a device used to measure blood glucose concentration. A person uses a test strip that goes into the glucometer. They put a drop of blood onto the test strip. There are substances on the test strip that produce a colour change with glucose. The higher the concentration of glucose, the deeper the colour produced. The glucometer measures the depth of colour produced and converts this into a glucose concentration. A new test strip is used for each blood test.
The following equations show how the substances on the test strip produce a colour change. (IN IMAGE)
Non-diabetics have no glucose in their urine. Diabetics have glucose in their urine if their blood glucose concentration rises above about 170 mg 100 cm–3 . Before the glucometer was available, diabetics used test strips to measure the concentration of glucose in their urine as a means of measuring their blood glucose concentration. When testing urine, the colour of the test strip is compared against a colour chart which gives a glucose concentration range for the colour produced.
Identify all the substances located at position X on the test strip before a drop of blood is added. (2 MARKS)
1. Glucose oxidase and peroxidase; Both enzymes required
2. Dye (with colour A);
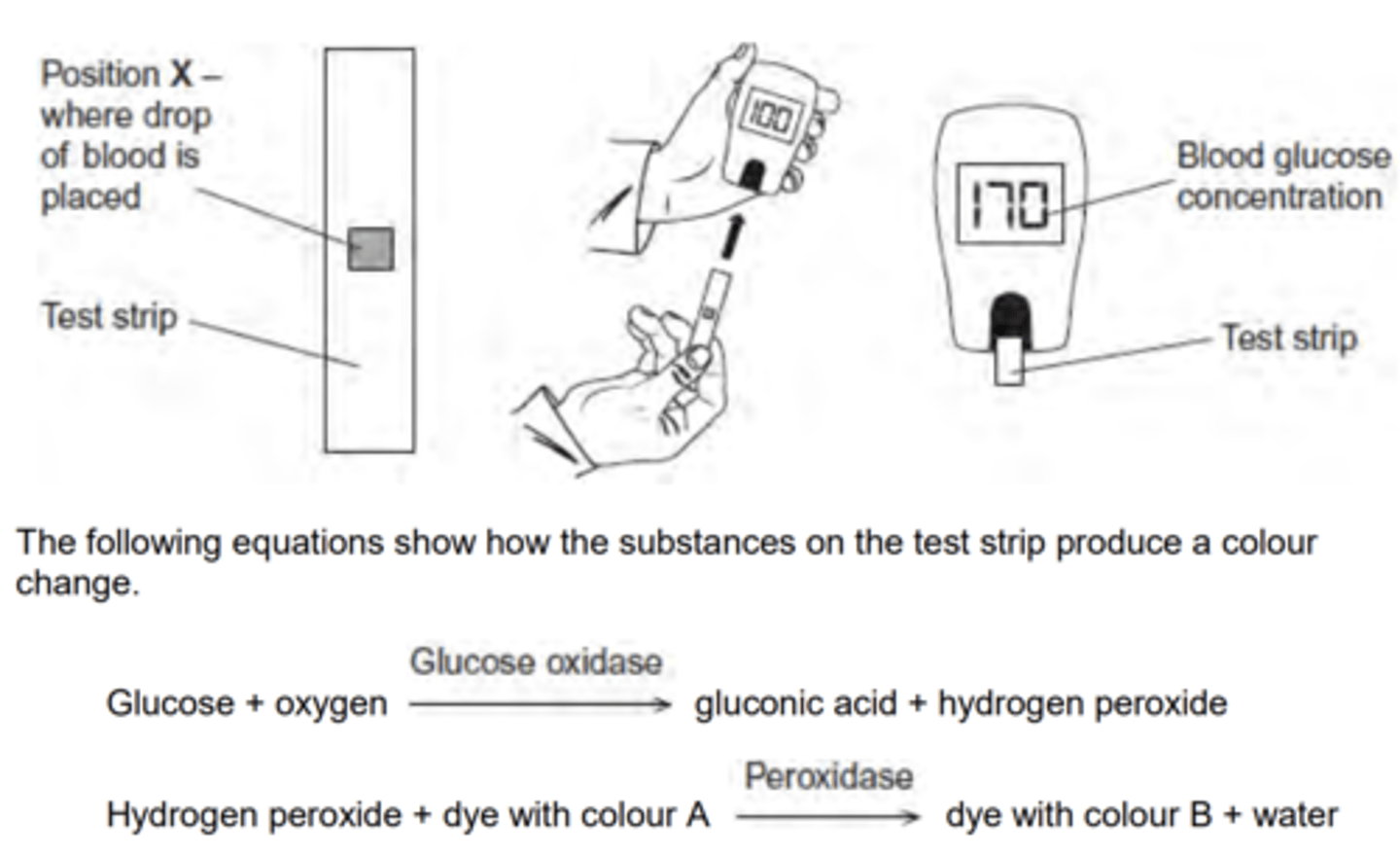
Q: A glucometer is a device used to measure blood glucose concentration. A person uses a test strip that goes into the glucometer. They put a drop of blood onto the test strip. There are substances on the test strip that produce a colour change with glucose. The higher the concentration of glucose, the deeper the colour produced. The glucometer measures the depth of colour produced and converts this into a glucose concentration. A new test strip is used for each blood test.
The following equations show how the substances on the test strip produce a colour change. (IN IMAGE)
Non-diabetics have no glucose in their urine. Diabetics have glucose in their urine if their blood glucose concentration rises above about 170 mg 100 cm–3 . Before the glucometer was available, diabetics used test strips to measure the concentration of glucose in their urine as a means of measuring their blood glucose concentration. When testing urine, the colour of the test strip is compared against a colour chart which gives a glucose concentration range for the colour produced.
Before the glucometer was available, diabetics used test strips to measure the concentration of glucose in their urine as a means of measuring their blood glucose concentration. Give two reasons why this method of testing urine would not give an accurate measurement of blood glucose concentration. (2 MARKS)
1. Concentration is given as a range (for each colour) / measurement is not precise;
2. Only measures glucose concentration above normal / above 170 (mg 100 cm−3) (in blood);
3. 170 (mg 100 cm−3) is an average figure / concentration for loss to urine varies (between people);
4. Difficult to match colour against chart / colour match is subjective;
Q:
RESOURCE A:
A glucometer is a device used to measure blood glucose concentration. A person uses a test strip that goes into the glucometer. They put a drop of blood onto the test strip. There are substances on the test strip that produce a colour change with glucose. The higher the concentration of glucose, the deeper the colour produced. The glucometer measures the depth of colour produced and converts this into a glucose concentration. A new test strip is used for each blood test.
The following equations show how the substances on the test strip produce a colour change. (IN IMAGE)
Non-diabetics have no glucose in their urine. Diabetics have glucose in their urine if their blood glucose concentration rises above about 170 mg 100 cm–3 . Before the glucometer was available, diabetics used test strips to measure the concentration of glucose in their urine as a means of measuring their blood glucose concentration. When testing urine, the colour of the test strip is compared against a colour chart which gives a glucose concentration range for the colour produced.
RESOURCE B:
There are two types of diabetes: type 1 and type 2.
• People with type 1 diabetes do not produce enough insulin.
• People with type 2 diabetes do produce insulin but have cells which do not respond to insulin.
Doctors use a glucose tolerance test to help diagnose people with diabetes. They start each test after a person has not eaten overnight. They measure a person’s blood glucose concentration. The person then drinks a solution containing 75 g of glucose. The doctors measure the person’s blood glucose concentration 2 hours later. During the test, the person remains at rest.
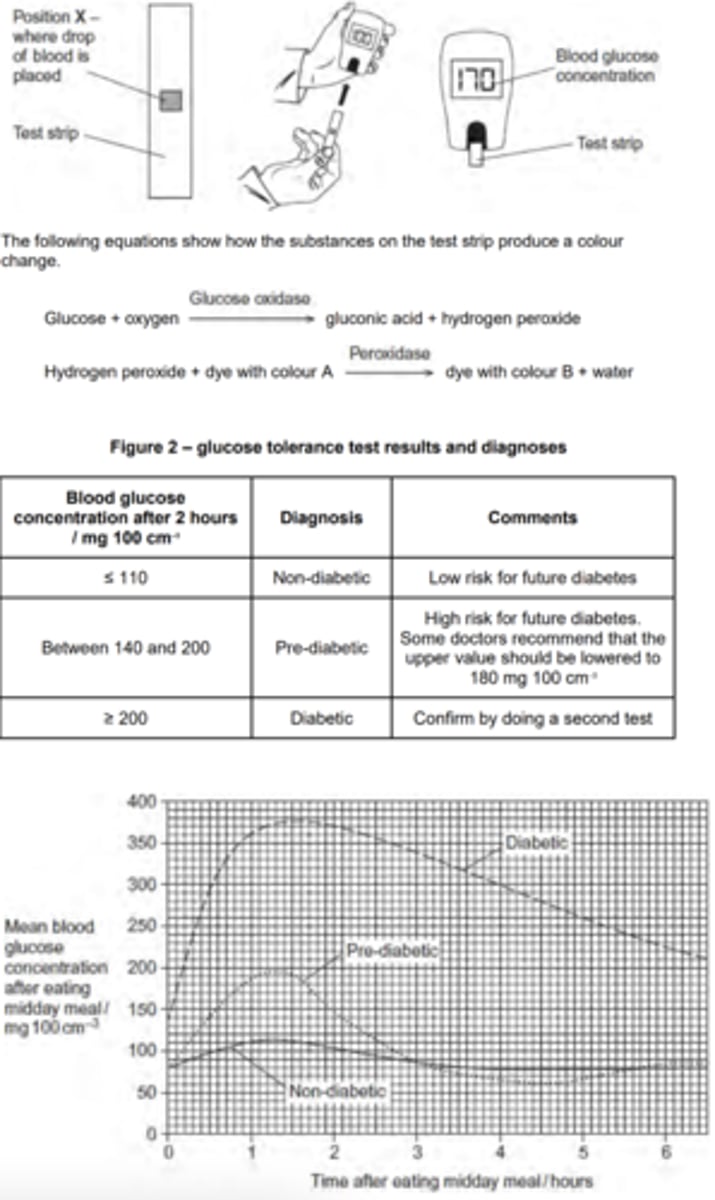
Figure 1 shows three diagnoses that can be made from the results of the test.
A researcher monitored the mean blood glucose concentration of a non-diabetic, a pre-diabetic and a diabetic after they had each eaten a midday meal. His results are shown in Figure 3.
A laboratory worker suspected she had type 2 diabetes but did not have a glucometer. Instead she added a drop of her blood to a test strip and used a colour chart to estimate her blood glucose concentration as 140 mg 100 cm–3 . Is it valid to conclude that she did have type 2 diabetes?
Use this information, and Resource A and Resource B, to explain your answer. (3 MARKS)
1. Diabetics have (blood glucose) concentration greater than 140 mg cm−3 / than her estimate / estimate suggests she is pre-diabetic;
2. Colour change is subjective / blood on test strip masks colour change;
3. Concentration given as a range / estimation is not reliable;
4. May not have fasted;
5. May not have had a drink with 75 g glucose;
6. Only one test carried out;

Q: Technicians in a hospital laboratory tested urine and blood samples from a girl with diabetes at intervals over a one-year period. Each time the technicians tested her urine, they also measured her blood glucose concentration. Their results are shown in the graph.
The girl who took part in this investigation was being successfully treated with insulin. The graph shows that on some occasions, the concentration of glucose in her blood was very high. Suggest why. (2 MARKS)
- Eaten;
- Containing carbohydrate / sugar;
- Glucose absorbed from intestine / into blood;
- Long time after insulin injection / needs more insulin / has not taken insulin;
- Does not convert glucose to glycogen / glucose not taken up from blood;
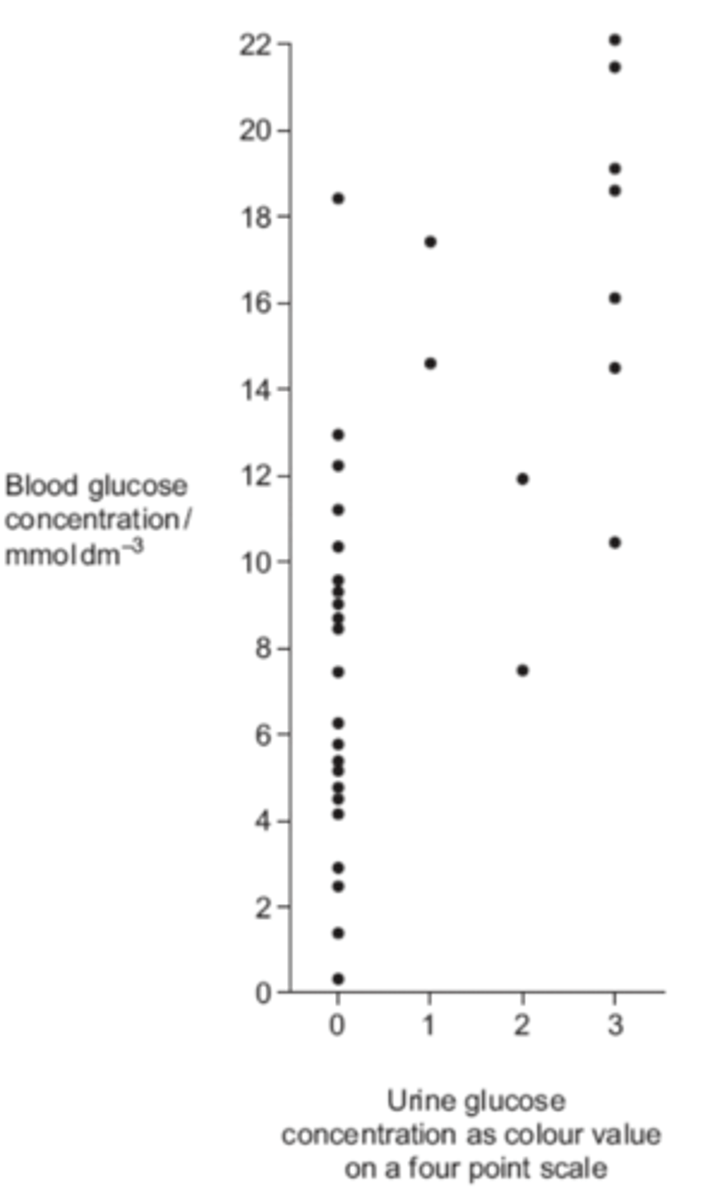
Q: Technicians in a hospital laboratory tested urine and blood samples from a girl with diabetes at intervals over a one-year period. Each time the technicians tested her urine, they also measured her blood glucose concentration. Their results are shown in the graph.
Use the graph to evaluate the use of the urine test as a measure of blood glucose concentration. (3 MARKS)
- Shows positive correlation / directly proportional;
- A range of results for a particular value / values (for different colours) overlap;
- Urine test only an arbitrary scale / not directly related to concentration / colour is subjective / few colour values;
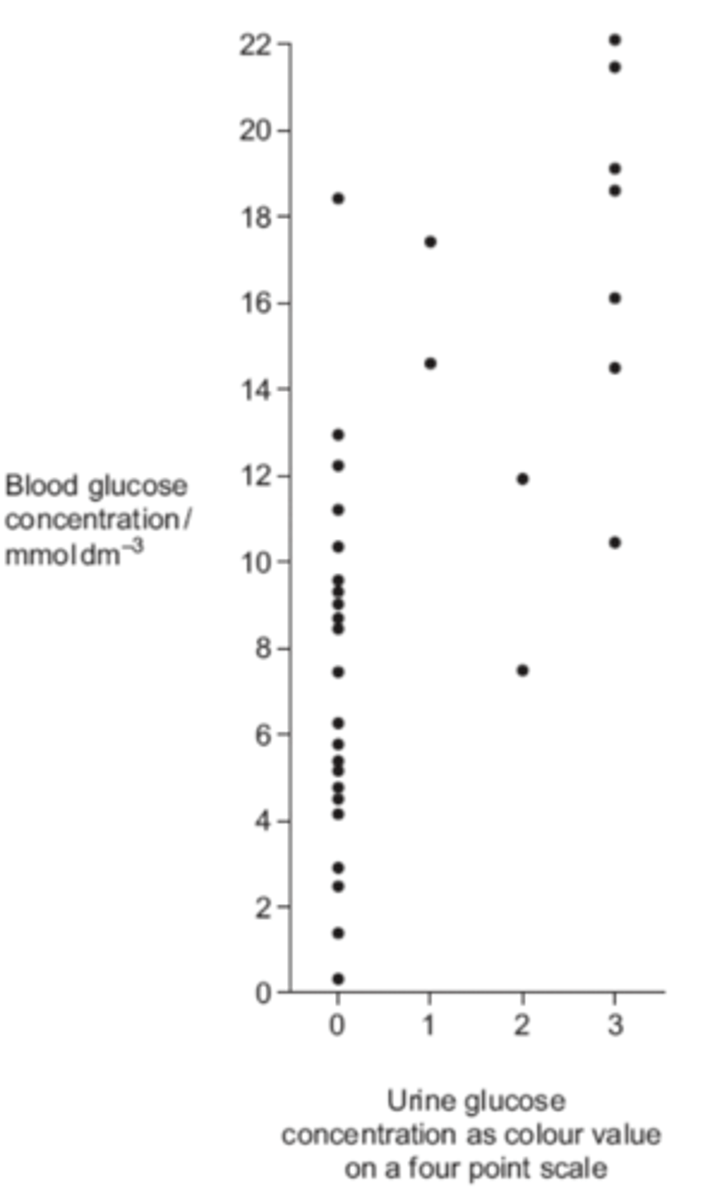
Q: Technicians in a hospital laboratory tested urine and blood samples from a girl with diabetes at intervals over a one-year period. Each time the technicians tested her urine, they also measured her blood glucose concentration. Their results are shown in the graph.
Diabetic people who do not control their blood glucose concentration may become unconscious and go into a coma. A doctor may inject a diabetic person who is in a coma with glucagon. Explain how the glucagon would affect the person’s blood glucose concentration. (2 MARKS)
- Glycogen to glucose / glycogenolysis by activating enzymes;
- Gluconeogenesis;
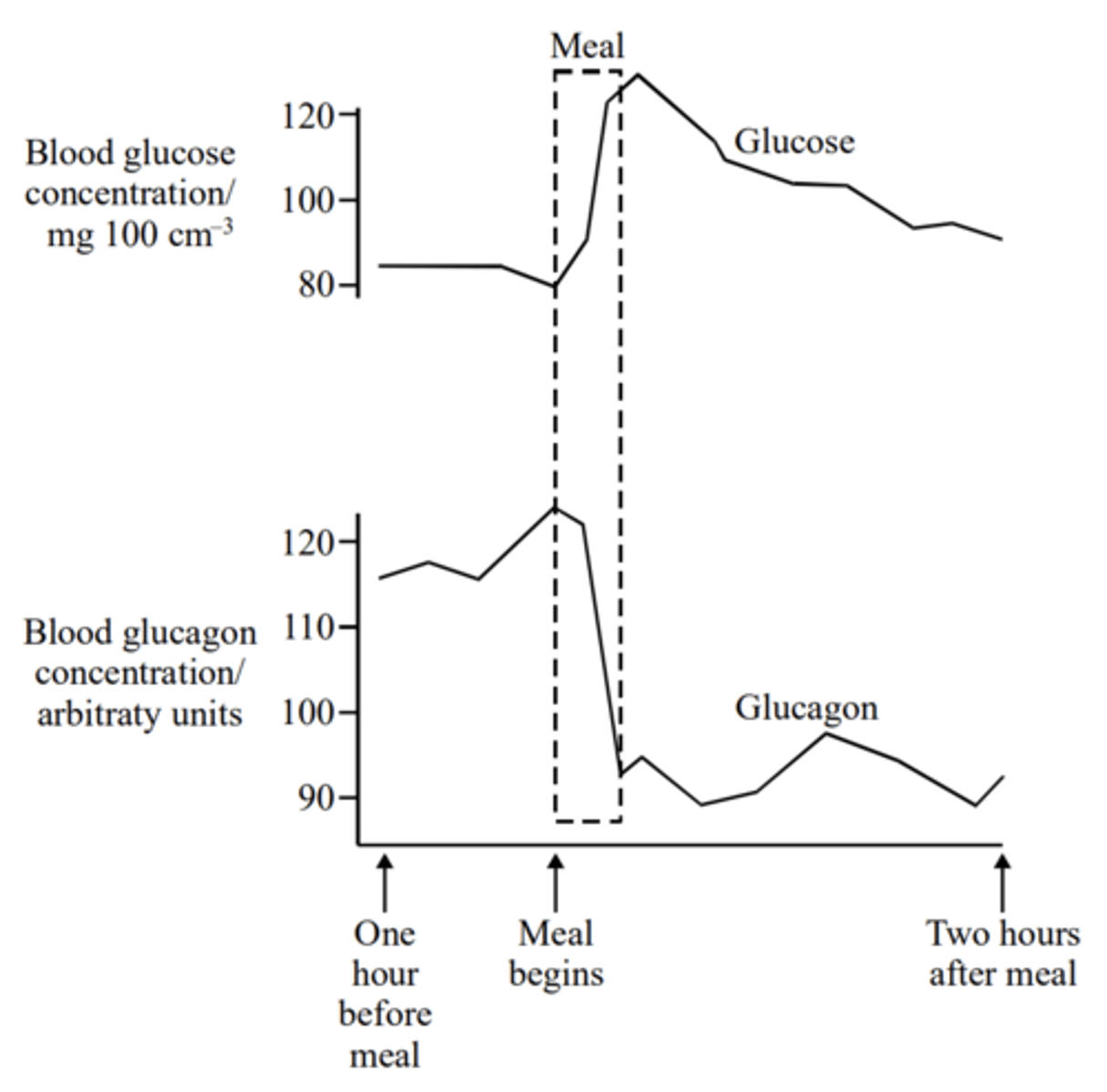
Q: The graph shows the blood glucose and glucagon concentrations in a healthy person during and after eating a meal.
Explain the changes that occur in the glucagon concentration over the period on the graph. (2 MARKS)
- High glucagon because - eg stimulated by low glucose/ glycogen must be converted to glucose;
- Low glucagon because - e.g. body has absorbed glucose;
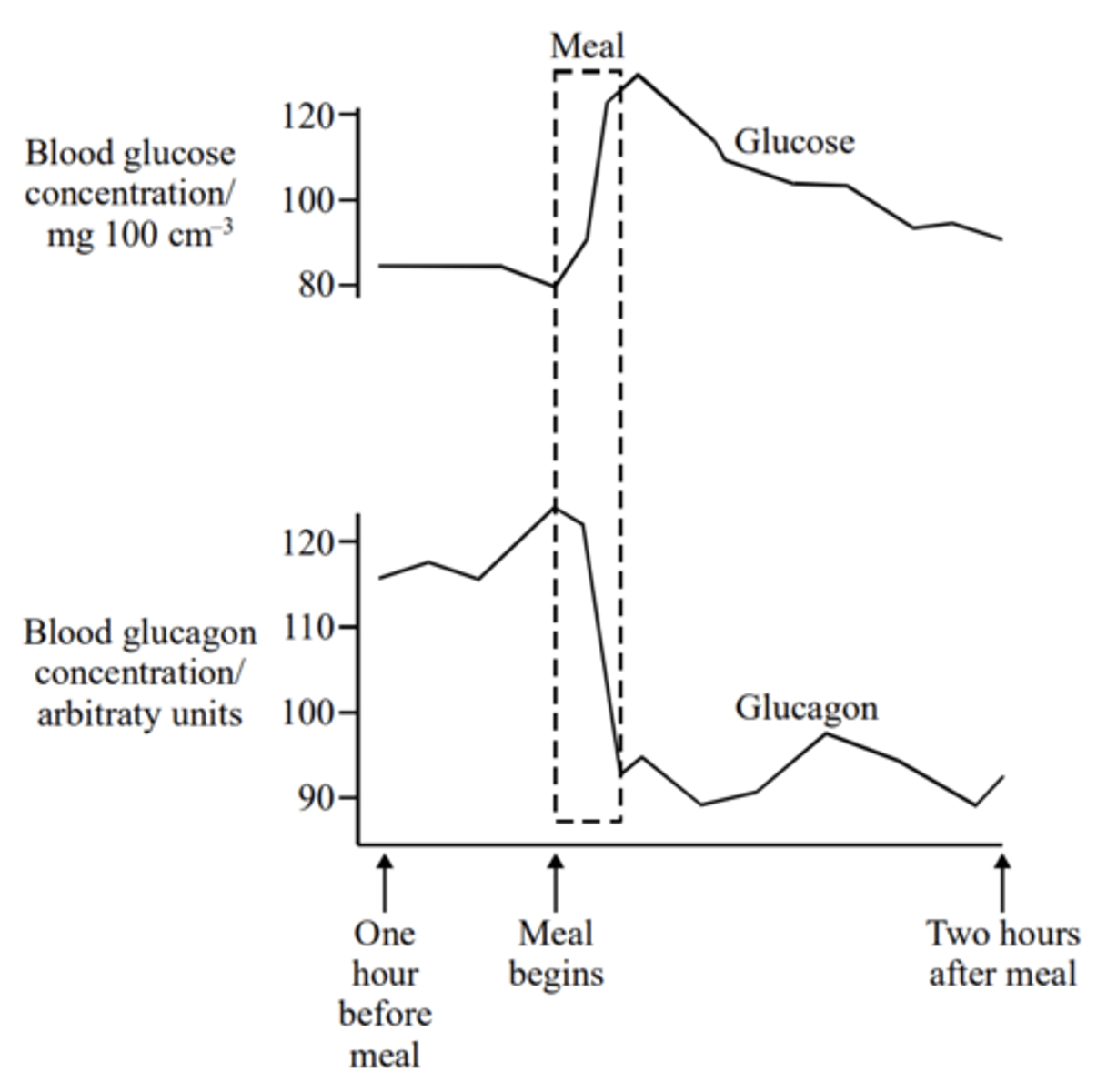
Q: The graph shows the blood glucose and glucagon concentrations in a healthy person during and after eating a meal.
Explain how the information shown in the graph provides an example of negative feedback. (2 MARKS)
Clear understanding that a change from the set level initiates mechanism returning it;
low glucose --> secretion of glucagon --> glucose level increases/ glucagon increase --> glucose increase --> glucagon decrease;
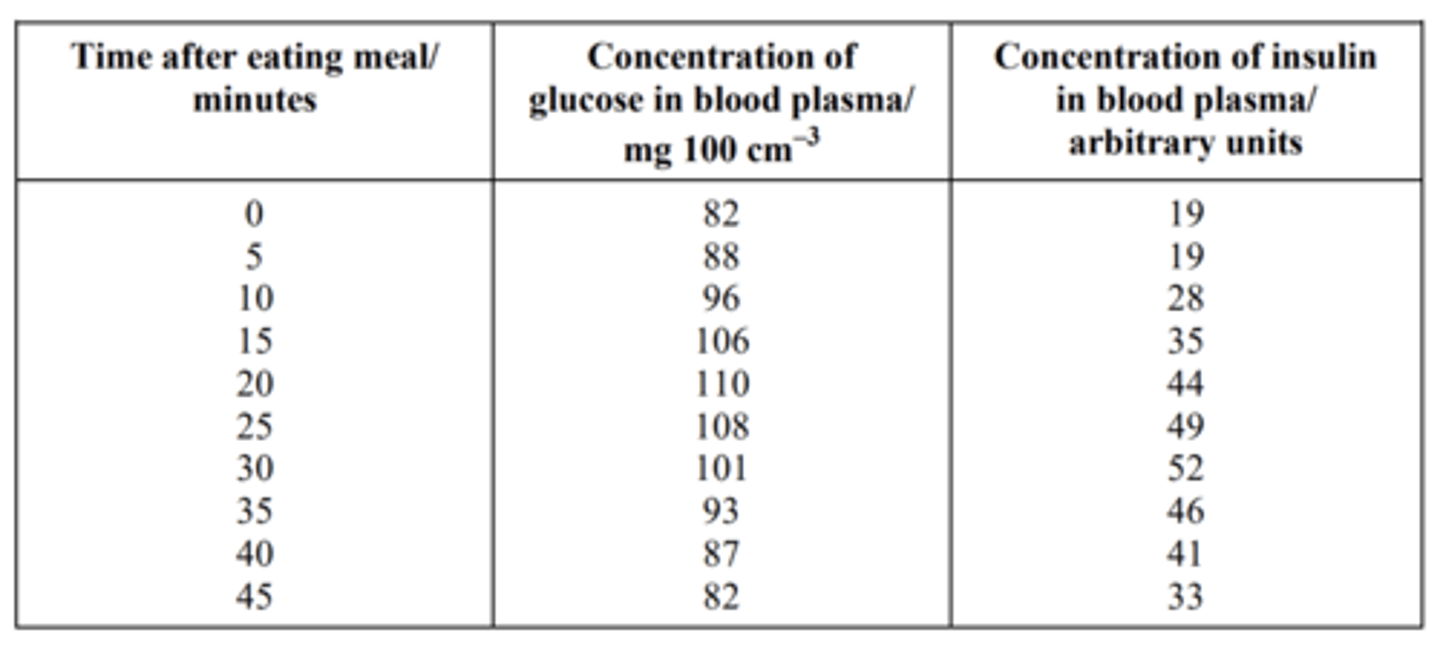
Q: The table shows the concentrations of glucose and insulin in the blood plasma before and after a meal.
Use information in the table to explain how insulin controls the concentration of blood glucose by negative feedback. (2 MARKS)
- High / increasing glucose causes high / increasing insulin;
- Insulin (concentration) reduces glucose;
- Back to original level;
- This results in / subsequent decrease in insulin level / release;
Q: Diabetes can occur when the pancreas cells are unable to secrete insulin. In a test, a person who is suspected of suffering from diabetes is given a solution of glucose to drink. Then blood samples are taken at regular intervals and the concentration of blood glucose is measured. If the person is diabetic, the blood glucose concentration rapidly peaks before slowly returning to its original level.
(i) The test is carried out on the same person a second time. Apart from drinking the same volume and same concentration of glucose solution, suggest two ways in which the test should be carried out to produce reliable results. (2 MARKS)
(ii) The blood plasma glucose concentration falls in diabetics even when there is no insulin present in the blood plasma. Explain why. (1 MARK)
(i) - Drink in a specified (short) time;
- Idea of fasting / controlled diet shortly before test;
- Same level of activity (as 1st test);
- Same (specified) temperature of drink;
- Ensure glucose level returns to normal before test;
(ii) Excreted in urine / respired;
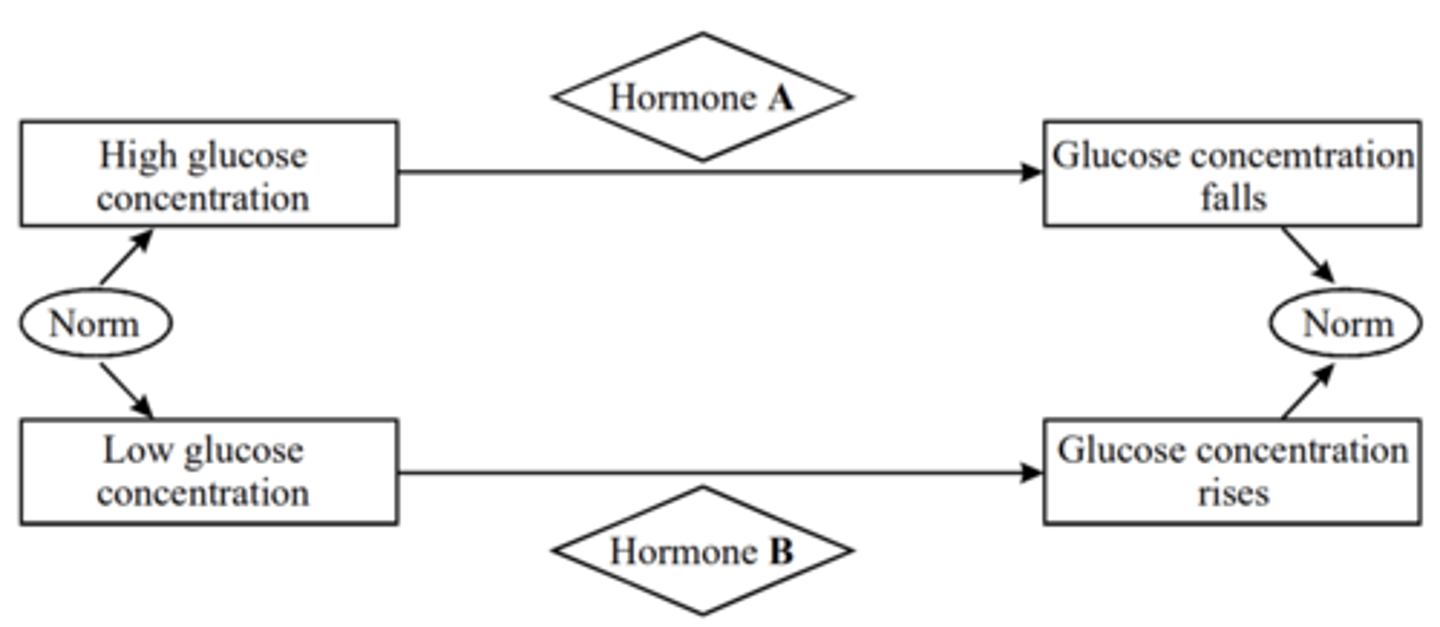
Q: The diagram shows some of the events which maintain blood glucose concentration in a mammal.
(a) Name
(i) hormone A
(ii) organ B
(2 MARKS)
(b) Explain why the events shown in the diagram can be described as an example of negative feedback. (1 MARK)
(a) (i) glucagon
(ii) liver
(b) A change to the normal level initiates a response which reduces the effect/ reverses/acts against the change;
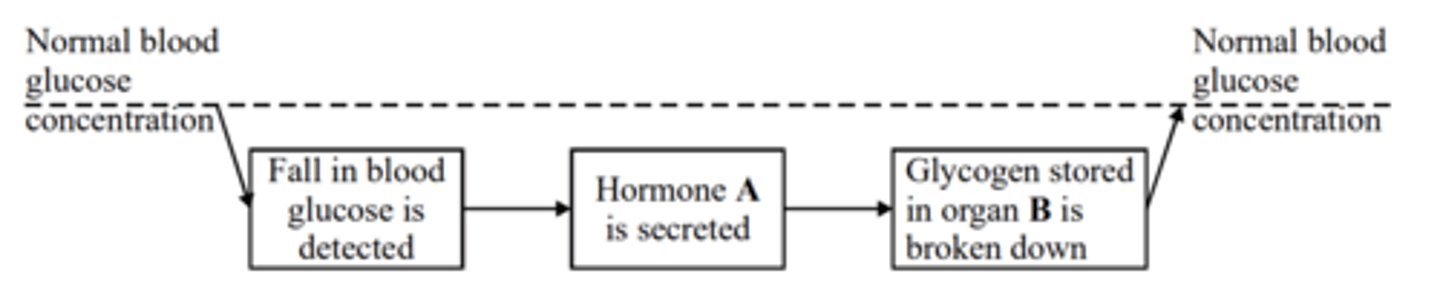
Q: Homeostatic mechanisms maintain a constant environment in the body.
The graph shows changes in plasma glucose concentration that occurred in a person who went without food for some time.
Explain how normal core body temperature is maintained when a person moves into a cold room. (5 MARKS)
1. Sensors in skin/hypothalmus detect reduced temperature;
2. heat gain centre activated/inhibition of heat loss centre;
3. vasoconstriction/constriction of arterioles in skin surface; (R capillaried)
4. dilation of shunt vessels/constriction of - capillary sphincter;
5. less blood to skin surface/capillaries
6. reduced heat loss by radiation;
7. incresed heat gain by increased metabolic rate/respiration/ movement/shivering;
8. decreased heat loss by putting on clothes/huddling/reduced sweating;
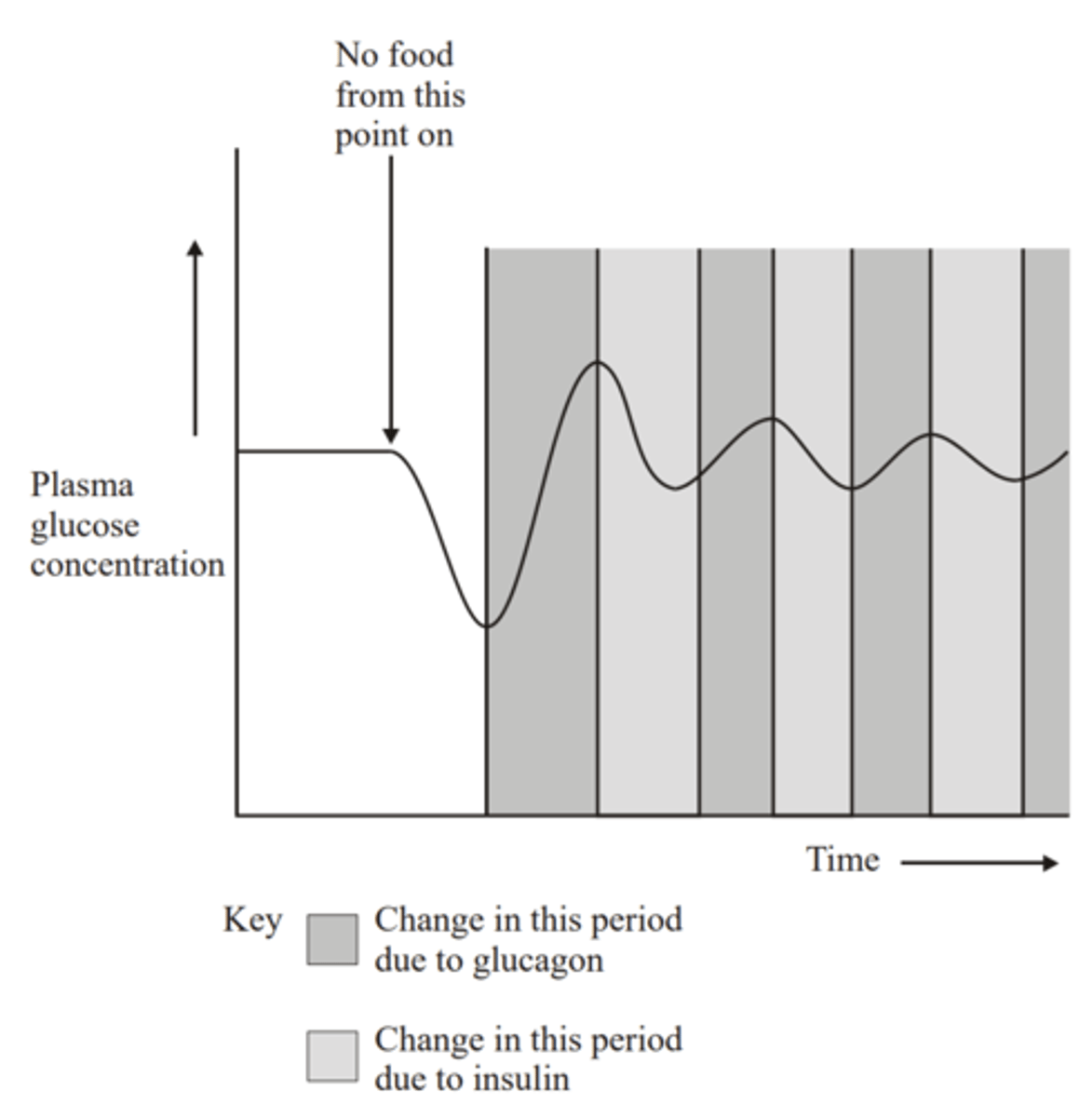
Q: The diagram shows how the concentration of glucose in the blood is regulated.
(a) Name
(i) hormone A
(ii) hormone B
(2 MARKS)
(b) Explain how hormone B brings about the change shown in the diagram. (2 MARKS)
(a) (i) A = insulin
(ii) B = glucagon
(b) - Hormone B acts on liver cells;
- causing conversion of glycogen into glucose;
- via action of an enzyme; gluconeogenesis;
Q: Describe how blood glucose concentration is controlled by hormones in an individual who is not affected by diabetes. (6 MARKS)
For principle, maximum of one mark
- Process involves insulin and glucagon;
For detail, up to a total of 6 marks
- Insulin / glucagon secreted by pancreas / islets of Langerhans;
- Hormone receptors in membrane (of target cells); (insulin stimulates) conversion of glucose to glycogen / glycogenesis:
- activates / involves enzymes;
- stimulates uptake by cells; conversion of glucose to lipid / protein;
- glucagon stimulates conversion of glycogen to glucose;/ glycogenolysis;
- glucagon stimulates conversion of lipid / protein to glucose / gluconeogenesis;
Q: The glucose tolerance test is used in hospitals to assess insulin production. A patient fasts for several hours before swallowing 5Og of glucose in 150 cm3 water. The concentration of glucose in the patient‟s blood is then measured immediately and at 30-minute intervals over a period of two to three hours. The graph shows changes in the blood glucose concentration of three patients who have taken this test.
Explain why it was necessary for the patients to fast for several hours before the test was carried out. (1 MARK)
So that readings are not affected by food recently eaten/ insulin secretion will be low;
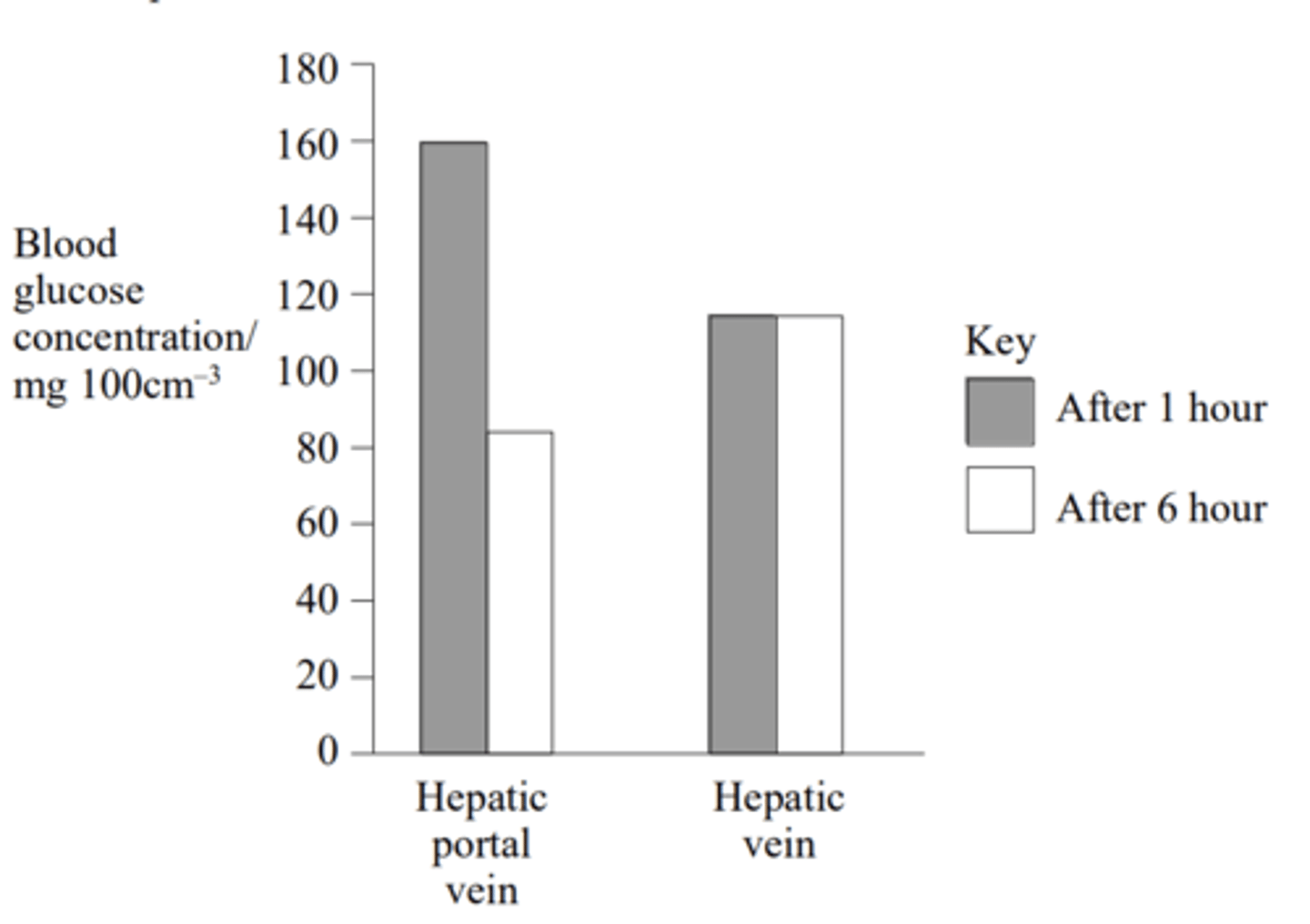
Q: There are two veins associated with the liver. The hepatic portal vein brings blood from the intestine to the liver while the hepatic vein takes blood from the liver. The concentration of glucose was measured in samples of blood from the hepatic portal vein and the hepatic vein. The samples were taken 1 hour and 6 hours after a meal. The results are shown in the graph.
(a) Explain the difference between the blood glucose concentration in the hepatic vein and that in the hepatic portal vein 1 hour after a meal. (1 MARK)
(b) Six hours after the meal, there is a higher concentration of glucose in the hepatic vein than in the hepatic portal vein. Describe the role of hormones in producing this higher concentration. (3 MARKS)
(c) In a person who has not eaten for two days, the blood glucose concentration in the hepatic vein is still approximately 110 mg 100cm3 . What causes the blood glucose concentration to remain at this level? (1 MARK)
(a) Glucose is being removed from the blood/processed in liver Glucose converted to glycogen;
(b) - Glucagon;
- Converts glycogen to glucose;
- By activating enzymes;
- Insulin is inhibited;
(c) Gluconeogenesis/glucose produced from non-carbohydrate sources/ named example;
Q: The hormones which control the concentration of glucose in the blood affect some cells in the body but not others. Use your knowledge of the structure of cell surface membranes to explain why. (3 MARKS)
- Only target cells have appropriate receptors;
- These are the proteins in cell surface membrane;
- Receptor sites/hormones with a particular shape;
- Concept of fitting/binding between receptor and hormone;