Microbiology, Exam 3 Antibiotics (1/3)
1/47
Earn XP
Description and Tags
antibiotics & their mode of action
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
48 Terms
selective toxicity
the idea that the antibiotic given to an individual should be more harmful/toxic to the microorganism being targeted than to the person its given too (little to no harm to the person)
Are antibiotics completely harmless
No; antibiotics come with risk; the risk goes up with the dosage; ex: some cause teeth staining, tendon damage (cipro), kidney damage (vanco), dull color vision (antebutanal)
bactericidal
antibiotics that target bacteria by killing bacteria; most antibiotics
bacterial static
antibiotics that target bacteria by slowing its growth
How do antibiotics target bacterial cells but not human cells?
they leverage the physical differences between human cells and bacterial cells. as the amount of evolutionary change between humans and bacteria diverged, more targets are made available for antibiotics.
antibiotics target the physical differences between human cells and bacterial cells to remove pathogens; how is the different in the case of funguses?
there are less differences to leverage. this is because fungus is more evolutionarily similar to human cells than bacteria is.
How are ribosome differences in human cells and bacterial cells leveraged by antibiotics
Both bacteria and human cells have ribosomes (which connect to RNA to produce protein that does processes in the cell (structural, enzymes, etc)); but the process of the ribosomes attaching or functioning is different so it can be targeted
How are mitochondrial differences in human cells and bacterial cells leveraged by antibiotics
the endosymbiotic theorem is an idea that mitochondria of eukaryotes originated from evolution with prokaryotes. because of this, mitochondria have similar makeup to their prokaryotic counterparts. because of this, antibiotics that target the mitochondria of bacteria can harm the mitochondrial cells of humans in high dosages.
How are cell wall differences in human cells and bacterial cells leveraged by antibiotics
human cells do not have a cell wall, while bacterial cells have a cell wall. because of this, many antibiotics will target the cell wall or cell membrane
How are DNA differences in human cells and bacterial cells leveraged by antibiotics
both bacterial cell and human cells have DNA made up of nucleic acids, but different methods of transcription. antibiotics will interfere with transcription to prevent DNA synthesis or transcription.
How are metabolite differences in human cells and bacterial cells leveraged by antibiotics
bacterial cells and human cells produce and use different molecules. ex: sulfa drugs work by targeting bacterial metabolism, interfering with folic acid synthesis by inhibiting the enzyme (DPHS) that carries out folic acid synthesis. w/out folic acid, the bacterial cell cannot grow or replicate
what is the makeup of gram negative bacteria & is it effected by antibiotics that target the cell wall
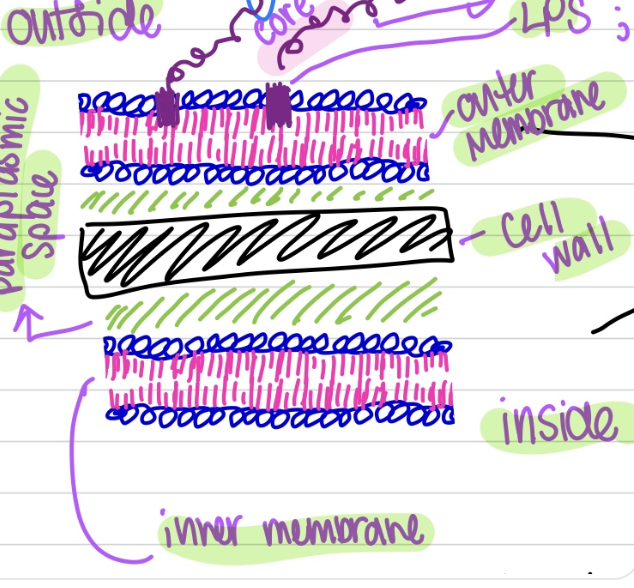
will have two cell membranes (bilayer membrane & the selective barrier) and the cell wall (peptidoglycan) in the middle; antibiotics targeting the cell wall will have a harder time attacking gram negative because there are two selective barriers; making it more difficult for the antibiotic to penetrate
what is the makeup of gram positive bacteria
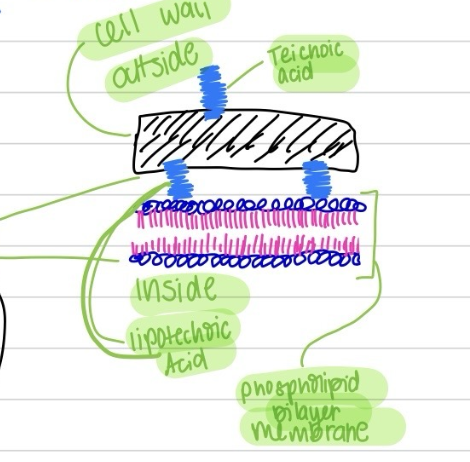
cell wall (peptidoglycan) on outside with bilayer membrane (selective layer) inside; antibiotic that target cell wall is very effective
what is the makeup of acid-fast bacteria
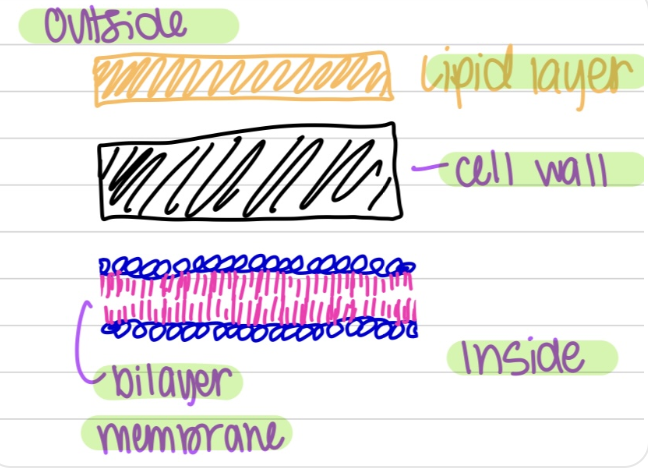
lipid layer on top, middle cell wall (peptidoglycan), and bilayer membrane (selective layer) inside; not as effective due to the lipid layer protecting the cell wall
Bacitracin
targets the transport of cell wall components, thus, preventing growth; primarily used for gram positive
bactericidial
found in neosporin (triple antibiotic cream)
will inhibit bactoprenol phophate (that attaches to cell wall components to move them across the bilayer membrane to the cell wall) from binding with cell wall components
resulting in, cell wall components from crossing the cell mem. → slowing the growth of the bacteria & preventing division → will eventually kill the bacteria
How does the cell wall of a bacteria grow to prepare for binary fission?
for binary fission, the cell wall needs to grow in preparation, so cell components must be added to the cell wall for it to grow. these components are made within the cell and move past the selective layer (bilayer membrane) to reach the cell wall to add on to it. these cell wall components bind with bactoprenol phophate to move across the selective layer.
bactoprenol phophate targeted by bacitracin
narrow spectrum antibiotics
antibiotics that kill not kill all bacteria, but are instead specialized and kill very specific bacteria; used in cases where the bacteria is known
broad spectrum antibiotics
antibiotics that will target and kill many different types of bacteria; used when there is not enough time to determine the type of bacteria causing the infection; can potentially kill “good” bacteria
Clostridium Difisil → C. dif
occurs when “good” bacteria is killed of; broad spectrum antibiotic kills of competing microorganisms good bacteria and allows c. dif to grow.
yeast infection
result of using a broad spectrum antibiotic
what antibiotics are included in the Beta-lactum class (weaken the cell wall of bacteria)
penicillans, monobactums, cephalosporins, carbapenems
Beta-lactums
will weaken the cell wall; think of a brick wall without mortar
in the cell wall, long chains of carbohydrates and short chains of amino acids connecting the carbohydrates are called cross links. these antibiotics will target these cross links, weakening the cell wall
only effects new cell walls → not old or already made cross links
ineffective against slow growing bacteria → new peptidoglycan is not being added → no “new” cross links being made
will be bactericidal → the cell wall protected against osmotic stress, so when in an osmotically stressful env., the weak cross links allow fluid into the cell, causing the cell to flood, rupture, and die (lyse)
penicillins
Beta-lactum
effects crosslinks of peptidoglycan, weakening the cell wall, resulting in osmotic stress & cell lyse
naturally occurring
effects gram negative and gram positive
bactericidal
cephalosporins
Beta-lactums
bactericidal
effects crosslinks of peptidoglycan, weakening the cell wall, resulting in osmotic stress & cell lyse
will have multiple generations; will be separated into 5 generations based on their coverage against gram-positive and gram-negative bacteria; with each successive generation having a broader spectrum of activity
carbapenems
Beta-lactums
bactericidal
effects crosslinks of peptidoglycan, weakening the cell wall, resulting in osmotic stress & cell lyse
modified chemically to prevent the kidneys from breaking them down via metabolism → allows the antibiotic to be in the body for a longer time frame
“last resort antibiotics” → given when all other antibiotics fail
the “heroic antibiotics”
monobactums
Beta-lactums
bactericidal
effects crosslinks of peptidoglycan, weakening the cell wall, resulting in osmotic stress & cell lyse
will have a single ring in chemical makeup → “mono”
are only useful against slow growing bacteria
not strong antibiotics; useful when a strong antibiotic is not necessary
Glycopeptides
effects the cell way by targeting the amino acid alanine / the isomers
isomers = the shape of the compound; classified as D and L, or R and S; corresponding pairs will be opposite (i.e. D and L are opposite, as are R and S)
in the cell wall crosslinks of the bacteria, there is a D-Alanine precursor that is needed to form the cross links (precursor = what something is before it is transformed into something else). glycopeptides will get inserted after this specific D-alanine precursor so that it can not be added to the cell wall (change its shape); thus, shutting down cell wall growth
vanctomyosin is a type of glycopeptide
vanctomyosin “vanc”
type of glycopeptide → will target the cell wall by changing the shape of the amino acids (alanine) in the compound that contribute to building crosslinks of the cell wall (the isomers)
very large compound when compared to the penicillins → more difficult to get within the bacterium
only effective and used against gram positive, since it is more difficult for the large molecules to be past through the cell membrane/bilayer membrane (selective layer)
gram + → will have cell wall on the outside, and bilayer membrane on the inside
gram - → has 2 bilayer membranes around cell wall; vanc not effective
side effects: high dosages can result in long term damage to the kidneys (high dosage = due to antibiotic resistance)
cycloserine
targets the cell wall by targeting the conversion of D-alanine to L-alanine (where D-alanine can convert to L-alanine and vice versa)
the bacteria must convert L-alanine to D-alanine for use in the cell wall; if the bacteria is unable to change L-alanine into the correct shape, then it can not be used in the cell wall → no growth → eventual death
this antibiotic will inhibit the enzyme that converts L-alanine to D-alanine; thus, disrupting bacterial cell wall synthesis
isomers
specific molecules with the same chemical formula but different structural arrangements; will have distinct functions and properties due to the differences in shape; majority amino acids exist as isomers that have two forms (stereoisomers)
L-amino acids are found in proteins in living organisms
D-amino acids are found in bacterial cell walls
ciprofloxacin “cipro”
targets DNA replication of bacteria by inhibiting DNA gyrase in gram negative bacteria and DNA topoimerase in gram positive bacteria
side effects: FDA warnings for tendon damage; especially to achilles tendon
very common antibiotic; broad spectrum
How would ciprofloxacin effect a gram positive bacteria
will inhibit DNA topoisomerase, G+
the replication fork opens, allowing DNA pol to come in and replicate DNA, as it move down and DNA is replicated and the replication fork closes.
however, the new DNA is still connected to the old DNA strand and must be separated by DNA topoisomerase IV
cipro will inhibit DNA topoisomerase IV by binding to it; preventing the processes of DNA replication from occurring
how would ciprofloxacin effect a gram negative bacteria
will inhibit DNA gyrase, or G-
as the replication fork opens to allow DNA pol to connect, the DNA below will be come tightly wound, but there is a limit to the tightness. the strand eventually becomes so tight, that it can not be broken apart / opened up
DNA gyrase will break up one of the phosphodiester bonds in one strand of DNA to allow the DNA fork to continue opening up and then links them back together → allows the replication fork to continue opening
will release some strain and relax the areas of super strain and the corners of the replication fork → allowing for DNA replication to occur
antibiotic will bind to DNA gyrase, causing it to be unable to function; thus the DNA will become so tight the replication fork will seize up and will not be able to be replicated
will stop DNA replication
rifampin
a RNA pol inhibitor that prevents RNA pol from transcribing
no transcription = no proteins = no enzymes, no molecules transportation, no work being done within the cell
oxazolidinone
will target the assembly of the ribosome on the strand of RNA; will prevent translation from occurring
two subunits (large and small) come together on the ribosomes binding site on a strand of RNA to form a ribosome; this ribosome then moves down the strand to create proteins
this antibiotic will prevent the binding of the two subunits / the formation of initiation complex
causing the ribosomes to not actively work
preventing translation from occurring = no formation of proteins
ex: Zyvox → used for MRSA infections that are common in hospitals
isoniazid
targets the enzyme in bacteria that forms mycolic acid
will go after mycobacteria specifically
mycolic acids are chains of fatty acid in the mycobacterial cell wall → cell wall is weaker, resulting in eventual death
ex of mycobacteria: TB and leprosy
TB is one of the top killers globally
ethambutol
will go after mycobacteria specifically
targets the attachment of mycolic acid to the peptidoglycan cell wall → weakening the cell wall, resulting in eventual death
possible side effects: loss of vibrancy of color vision (myopathy)
polymixin B
targets the cell membrane (selective layer) by “punching” holes into the cell membrane
causes the bacteria to lose its selective permeability (or membrane permeability)
most effective against gram positive bacteria since it only has 1 membrane
prevents the ability of ions to diffuse / go against the concentration gradient or exit the cell (could also effect the cells ability to form ATP, since bacterial cells use this method due to not having organelles)
cause the bacteria to “leak” to death → bactericidal
tetracycline
will target the proteins of bacteria by interfering with tRNA docking and slowing protein synthesis
molecular structure has 4 rings
tendency to be bacteriostatic since it slows bacterial growth; but doesn’t kill the bacteria
side effects: can cause teeth staining → why it shouldnt be given to children
What is the process of tRNA docking and how is it effect by tetracycline
tRNA → an adaptor molecule that ensure the correct amino acid is delivered to the ribosome base on the mRNA codon sequence and are at specific sites in the ribosome during translation
in protein synthesis (translation), tRNA must go to the site on the ribosome and “dock” so that the ribosome works correctly (by delivering the correct amino acid to form proteins), once the tRNA bonds, more tRNA will bind, forming polypeptide bond, causing the amino acids to bond together and form proteins. (think of tRNA as carrying ingredients (amino acids) that are the connected together with glue (polypeptide bonds) to form the final product (proteins)
tetracycline will prevent tRNA from docking to the ribosome → preventing amino acids from forming proteins and preventing amino acids from being delivered (slowing protein synthesis)
chloramphenicol
will target the protein peptide bonds
on amino acids, there are two funcitonal groups (NH2 and COOH + R group; where the R group is a “side chain”), when a covalent bond form between 2 amino acids, or a peptide bond, OH and H come off as water (dehydration synthesis)
the formation of a peptide bond is catalyzed (or carried out) by a specific enzyme — this antibiotic targets this enzyme, thus preventing the formation of a peptide bond (i.e. no proteins can be made)
internal form not often used in the U.S., but is in eyedrops
potential side effects: can cause low RBC (aplastic anemia)
aminoglycosides
will target the bacterium’s ability to form the correct protein
protein function is based on the tertiary structure, which is predicated on the secondary structure, which is predicated on the primary structure (or the sequence of amino acids; where 1 codon = specific amino acid)
this antibiotic will decrease the stringency (the ability to correct an incorrect codon) of ribosomes, allowing for extra codons to be put in (typically the 2nd codon, since the 3rd is the least influential), changing the primary structure, in turn changing the secondary and tertiary structure, causing the protein to be different and incorrect
changing the amino acids or codons of the protein changes the shape of the protein, changing the function of the protein so that is does not work correctly
used for gram negative and mycobacteria
mupirocin
will target protein synthesis by effect tRNA containing isoleucine
tRNA containing isoleucine will ensure the correct amino acids are inserted into the polypeptide chain when proteins are made during translation
this antibiotic will make tRNA containing isoleucine less readily available to the bacteria → effecting the ability of the bacteria to insert the correct amino acids into the poly peptide chain
macrolides and lincosamides
two different classes of antibiotics that target the same things
will target translation (making proteins) by acting as “boot” and immobilizing the ribosome from moving down the strand (translocation)
for a ribosome to function ut must move relative down the mRNA, so no translocation = no protein synthesis
ex) when the two subunits of ribosome attach at the ribosome binding site on the mRNA, the antibiotic will block the ribosome from moving down the strand
used for gram positive bacteria
clofazimine
will target guanine, specifically the GTP, the trincleotide before DNA can be incorporated
without guanine, DNA is unable to be incorporated
antibiotic will bind to guanine bases of bacterial DNA, preventing the bacteria from growing its number of cells (or proliferating)
GTP = guanine with 3 phosphates (the pre-incorporated form of guanine)
used for mycobacteria
bedaquiline
will target the ability of a bacteria to produce ATP / ATP synthase
ATP is synthesized by converting one form of energy to another (such as via a proton gradient)
this antibiotic will target the pathway making ATP
used for mycobacteria
Sulfa Drugs
sulfa drugs are analog, or the same structure/shape, as paramine benzoic acid (PABA) → on a substrate level, sulfa drugs look like PABA but with sulfa ends
in bacteria, PABA is used as a precursor in the synthesis of folic acid, which is then used to make nucleotides to make DNA.
PABA will bind with DHPS to form folate (that is then used in synthesis of folic acid)
Sulfa drugs will compete with PABA for binding with DHPS, preventing the formation of folate, in turn preventing the creation of folic acid (hindering bacterial growth and replication)
are bacteriostatic
of the antibiotics studied, which are bacteriostatic
tetracycline and sulfa drugs