pt centered care families exam 3 week 2
1/61
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
62 Terms
externalizing disorders
outward directed, disrupting behaviors that may affect executive functioning and social functioning
oppositional defiant disorder (ODD)
conduct disorder
neurodevelopmental disorders ex: ADHD, autism spectrum disorder (ASD)
internalizing disorders
emotional, mood-related (sefl)
depression and mood disorders
anxiety disorders
feeding and eating disorders
trauma and stressor related disorders ex: PTSD, reactive attachment disorder
etiology and risk factors for externalizing disorders?
genetic vulnerability
child abuse hx
environmental adversity
poor family functioning
parent w/anti-social personality, substance abuse, mood disorder, thought disorder, ADHD
socioeconomic disadvantages may also be a factor
temperament
externalizing disorders with behaviors like…
high anxiety
distractibility
high intensity
poor reaction to new stimuli
poor adaptability
strong willed - negative persistence
low sensory threshold
negative mood
oppositional defiant disorder (ODD)
persistent pattern (negative way!)
resists authority - disobeys, breaks rules
argues
has anger outbursts
blames others never their own fault
behaviors may be more evident in one setting and not another
conduct disorder
persistent pattern (negative way!)
BREAKS LAWS - antisocial behavior
aggressive towards people and/or animals
destroys property
steals
deceives others
may be present in adolescents w/ADHD.
breaks laws, doesn’t just bend rules…
attention deficit disorder (ADD)
often lifelong, affects 5 million children ages 3-17, subtypes are inattentive, hyperactive/impulsive, combined
criteria for diagnosis
inattentive: to details, cannot stay on task, trouble organizing
hyperactivity: excessive compared to age expectations
impulsivity: “blurts" out answers and “interrupts”
ADD risk factors
exposure to lead or pesticides, low birth weight, premature birth, brain injury
risk of serious consequences like accidents, school or job failure, substance abuse, depression, anxiety, relationship/family stress and disruption, delinquency, etc…
autism spectrum disorder
boys 4x more likely to be diagnosed (all ethnic groups, all socio between age 2-6 yrs, by age 3-4 for sure diagnosed)
persistent deficits in social communication and interaction
restricted, repetitive patterns of behavior, interests, or activities
must be present in early developmental period
may cause significant impairment in functioning
risk factors: older parents, genetics, environmental exposure
nursing considerations for mental health in general
ensure safety
provide structure
work on coping skills and self esteem
model social skills
nursing considerations for ADD/autism
short clear instructions
daily routine
break tasks into small portions
get child’s attention
cue transitions
manage stimulation (ex: fidgets, slime, glasses…)
nursing considerations ODD/CD
teach collaborative problem-solving (can do well if supported early on!)
set clear rules and consequences
be nonjudgemental
work on talking vs acting out
de-escalation
separate child from behaviors…
reactive attachment disorder (RAD)
affects less than 2% of children
risk factors: early trauma, removed from caregivers, multiple parent figures, neglect, institutional care
symptoms: lack of positive emotions, avoidant of eye contact/touch, tantrums/anger, limited social interactions, withdrawn…
symptoms (DSED): break rules, attention seeking, overly affectionate, poor boundaries, inappropriate social behavior
nursing considerations for RAD
at risk for…
developmental delays
mood disorders (anxiety, depression, PTSD, eating disorders, substance use disorder)
school isues
relationship issues
risk taking
nursing approach: consistent limits, consistent approach
treatment: psychology, family therapy, social skills, educational supports, parenting skills
anxiety
most common mental health condition (more common females than males) (25.1% of children age 13-18)
strong co-existence of depression and anxiety disorders
physical comorbidities ie. heart disease, etc…
3-5 times more likely to visit the doctor and 6 times more likely to be hospitalized
anxiety and mood disorders involve what changes?
physiological, emotional changes, cognitive changes…
physiological changes in anxiety and mood disorders
increased HR
increased RR
increased brain alertness
increased muscle tone
increased blood glucose
increased perspiration
increased blood volume
increased epinephrine, NE, cortisol
decreased GI/GU functioning
decreased speaking
decreased sleeping
decreased immune functioning
pupil dilation
emotional changes in anxiety and mood disorders
feelings of worthlessness/helplessness/depression
suspiciousness/jealousy
withdrawal/decreased personal involvement
crying/sobbing
blaming self/others
lack of interest
“not themselves”
cognitive changes in anxiety and mood disorders?
forgetful/distracted
ruminative thoughts
anticipatory worries
intrusive memories
cognitive distortions (“awfulizing”)
lack of attention, decreased concentration
focus on past, rather than present or future
reduced productivity/interest/creativity
nursing considerations for mental health
biological interventions: improve sleep, reduce stimulating substances, maintain adequate diet and eating patterns
behavioral interventions: muscle relaxation and breathing, imagery/meditation, behavioral modification, behavioral activation
cognitive interventions: distraction, positive self-talk, cognitive behavioral therapy, psychoeducation
social interventions: stress and time management, family psychoeducation and/or therapy, increased social contact, group therapy…
nursing care in mental health
ensure safety
help pt to identify and express stressful feelings
identify to strengthen coping and strategies
work on self-esteem
medication and side effect teaching
screen for suicide (routine in many EDs and clinics from ages 8-10+ yrs. if at risk refer to social work, ensure safety, 1:1 care, and create safe room if on suicide protocol)
trauma informed care
prevention is the best form of de-escalation…
shift judgement to “I wonder…”
have a universal approach (trauma is hidden and prevalent)
create safety through words and body language
create trust/transparency
create space
ensure choice/voice
strength based approach to build resilience
be aware of warning signs (pacing, agitation, forced speech)
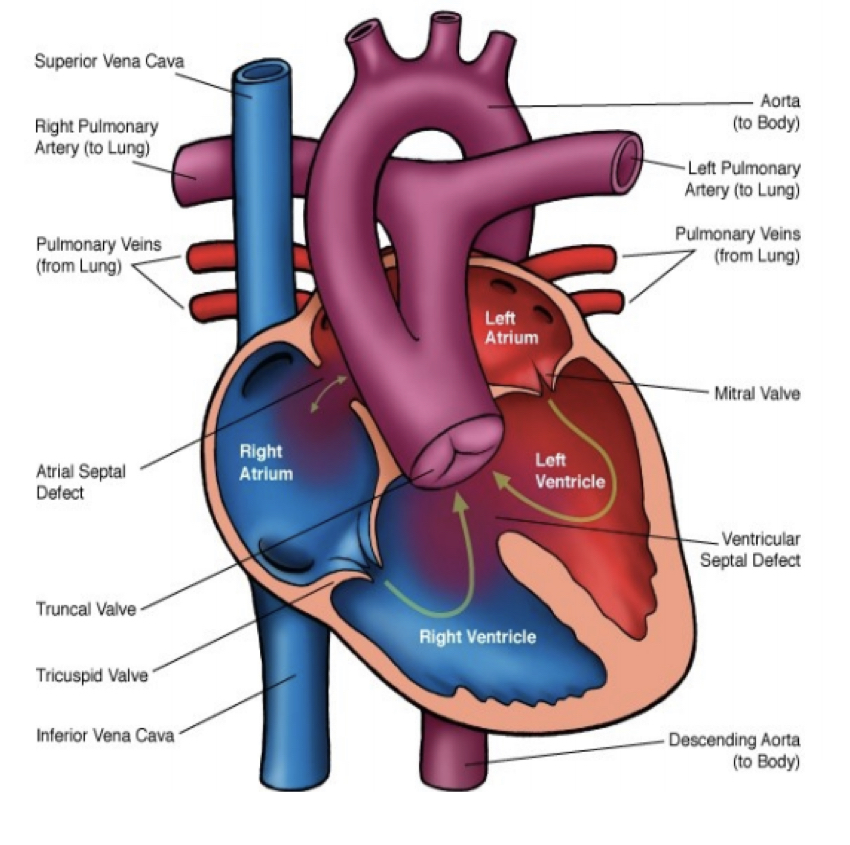
coronary arteries
bring oxygen-rich blood to the heart
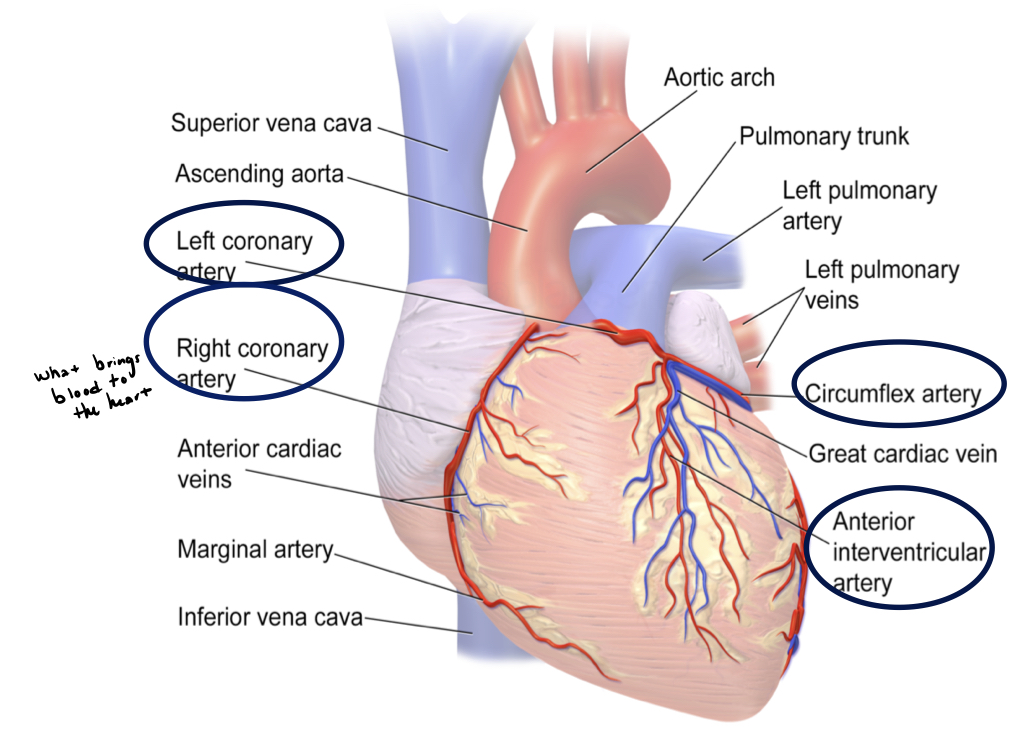
coronary veins
return oxygen-depleted blood from the heart muscle back to the heart to be sent to the lungs
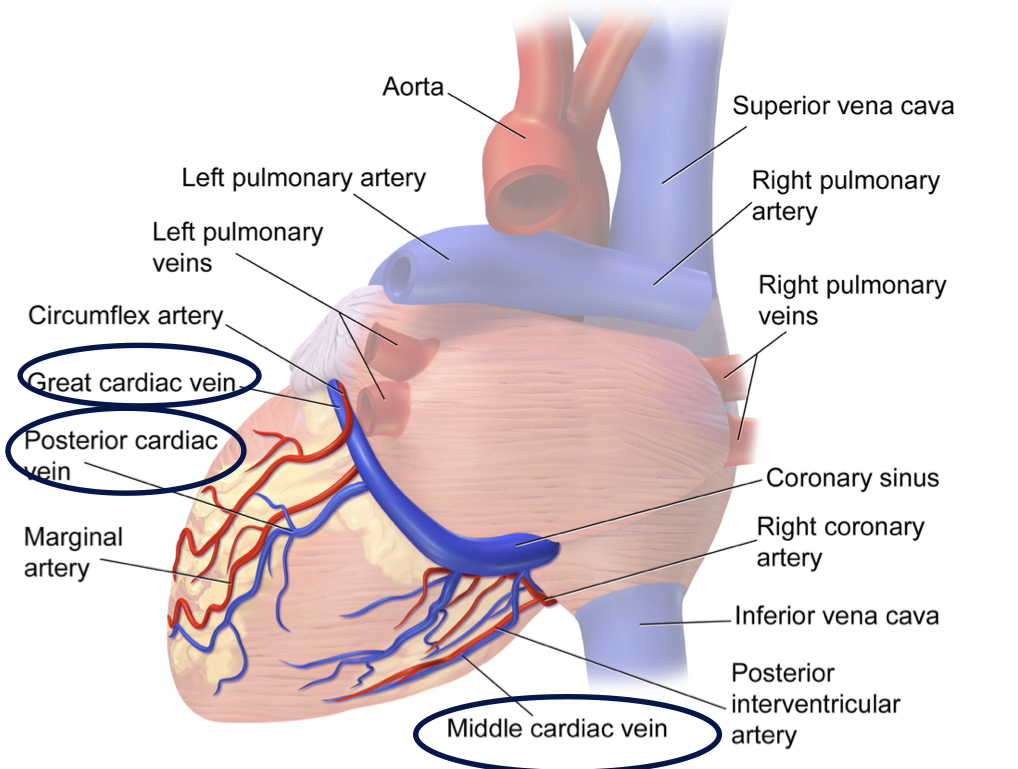
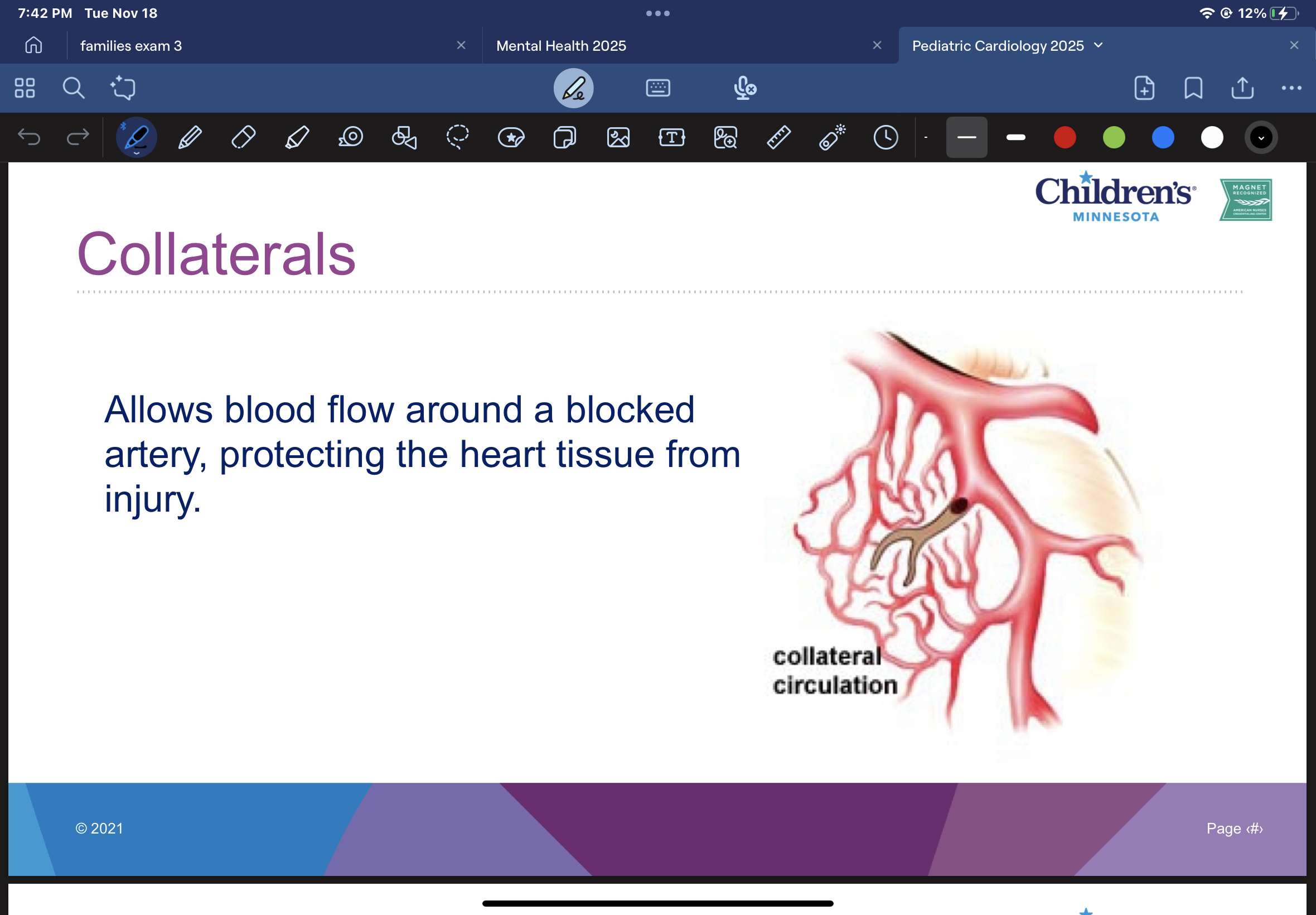
collaterals
allows blood flow from a blocked artery, protecting the heart tissue from injury
at what phase of the cardiac cycle are the coronary arteries perfused?
diastole
what is the most common congenital heart disorder?
ventricular septal defect
general post-op recommendations
airway
- ETT - where is it? secure? suction?
breathing
ventilator settings, ABG results
circulation
vasoactive drips
heart rate and rhythm
pulses, perfusion
disability
bleeding, pain/sedation
exposure
temperature
how are cardiac defects classified?
pulmonary vascularity: increased, normal, none
acyanotic: left to right shunts (VSD, PDA, ASD, AVSD), obstructive lesions (AS, PS, COA, cardiomyopathy), or none
cyanotic: admixture lesions (D-TGV, TAPVR, truncus, single ventricle lesions, none, obstruction to pulmonary blood flow + septal defects TOF, tricuspid atresia, ebstein’s malformation
what are acyanotic defects with increased pulmonary blood flow?
(left → right shunts)
patent ductus arteriosus (PDA)
atrial septal defect (ASD)
ventricular septal defect (VSD)
AVSD
patent ductus arteriosis (PDA)
begins to constrict 10 to 15 hours after birth
born, placenta removed, onset of respiration, PVR drops, rise in PaO2 and a fall in prostaglandin → ductus constricts
FULLY CLOSES AT 2-4 WEEKS
doesn’t fully close because of prematurity or hypoxia…

PDA nursing considerations pre-op
normal newborn cares
decide on treatment plan (premature infant, larger kids)
monitor respiratory symptoms (tachypnea, increased work of breathing…)
failure to thrive
PDA nursing considerations post-op
phrenic or recurrent larengeal nerve injury
hemorrhage
pain management
PDA cath lab care
pre: NPO time, antibacterial bath, meds taken
intra: positioning, VS monitoring, labs
post: pt MUST lay flat for 4-6 hours, pain controlled, eating/voiding
atrial septal defect (ASD)
hole in the wall separating the atrium
creates a left to right shunt
results in increased workload on the right heart
small shunts do not require therapy!
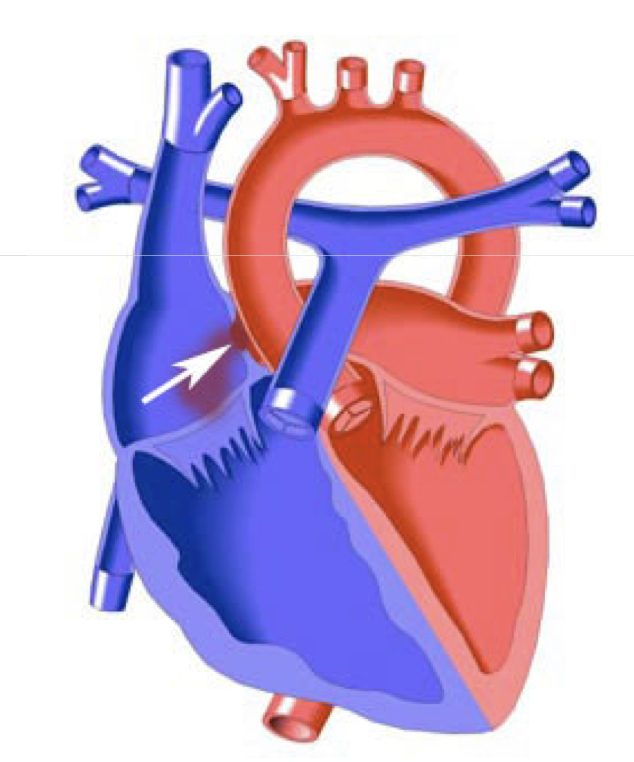
ASD nursing considerations pre-op
admission from home
antibacterial bath
NPO time
ASD nursing considerations post-op
right ventricular dysfunction (arrhythmias)
prolonged pulmonary overcirculation (pulmonary disease)
pain
bleeding
ventricular septal defect (VSD)
hole between the ventricles
blood flow pathway
increased workload on the RIGHT side of the heart
size of defect and pressures in the lungs and body determine magnitude of symptoms
different types of VSD based on WHERE THEY ARE IN THE VENTRICLE
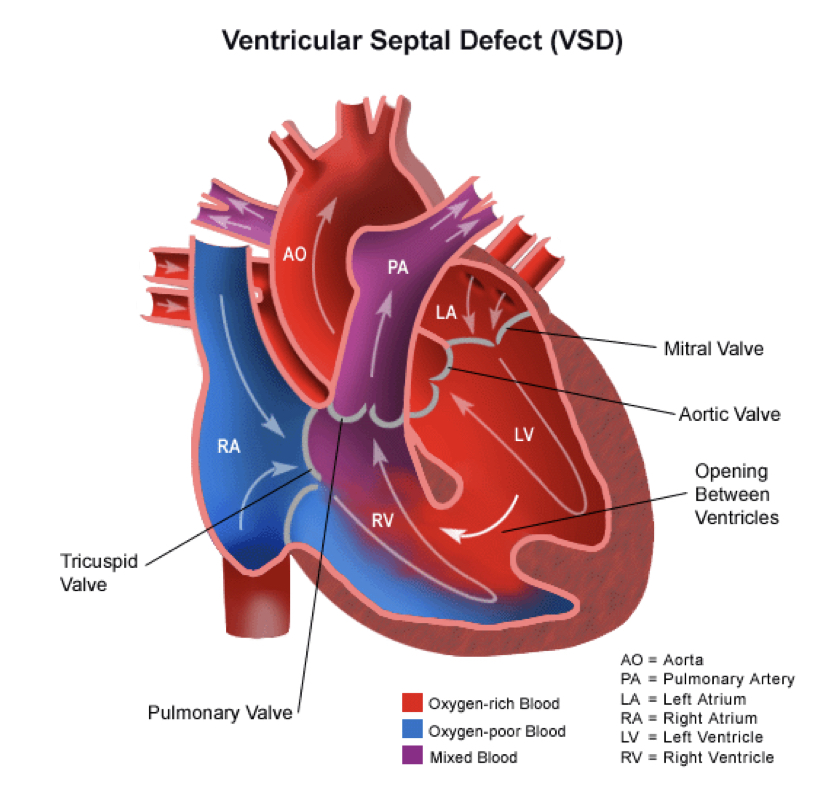
VSD nursing considerations pre-op
CHF
pulmonary hypertension
VSD nursing considerations post-op
arrhythmias
pulmonary hypertension
low cardiac output syndrome
residual VSD
acyanotic defects that obstruct blood flow?
obstructive lesions (AS, PS, COA, cardiomyopathy)
obstructive acyanotic lesions
coarctation of the aorta
aortic stenosis
pulmonary stenosis
increase in LV work
no intracardiac connections
no shunting
PBF normal, cyanosis absent
coarctation of aorta
increased resistance to blood flow to body
left ventricle
elevated pressure to maintain flow
proximal to narrowing: pressures are high
disal to narrowing: pressures are low
collateral pathways
presentation
cardiac collapse at birth
as a teenager
overall goal is to prevent end organ damage
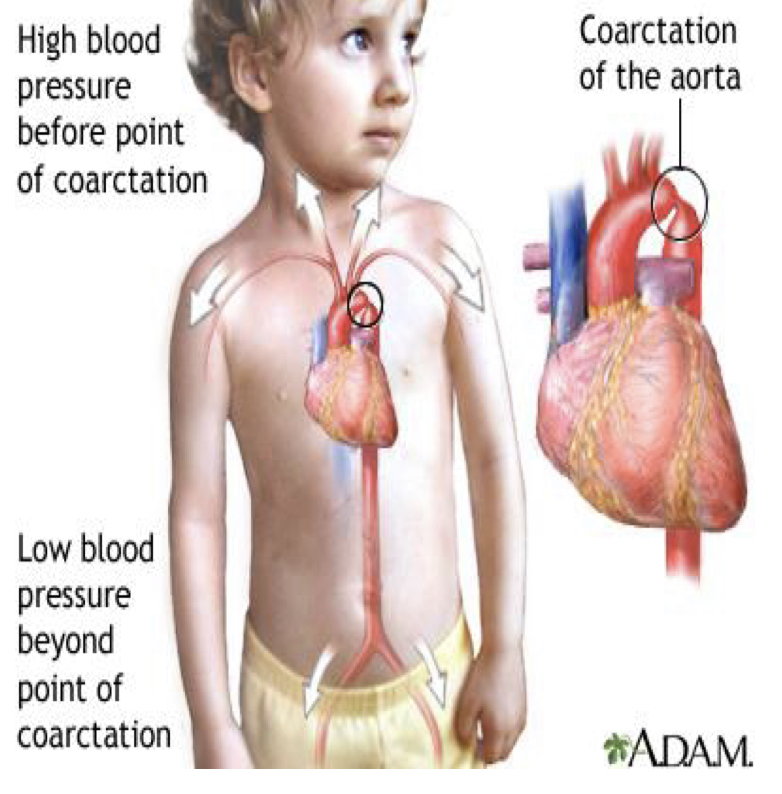
coarctation nursing considerations pre-op
infant
monitoring for PDA to close
difference in upper and lower extremity pulses and pressure
teenager
probably asymptomatic
extremely elevated BP
OR
admission from home
antibacterial bath
NPO time
coarctation nursing considerations post-op
hypertension
post-coarctectomy syndrome
spinal cord hypoperfusion - paralysis
cyanotic defects w/increased pulmonary vascularity
admixture lesions: D-TGV, TAPVR, truncus, single ventricle lesions
d-transposition of the great arteries
blood flow pathway
aorta rises from the right ventricle - no opportunity to be oxygenated in lungs
the pulmonary artery arises from the left ventricle - no opportunity for oxygenated blood to reach the body
the child requires intracardiac mixing to survive
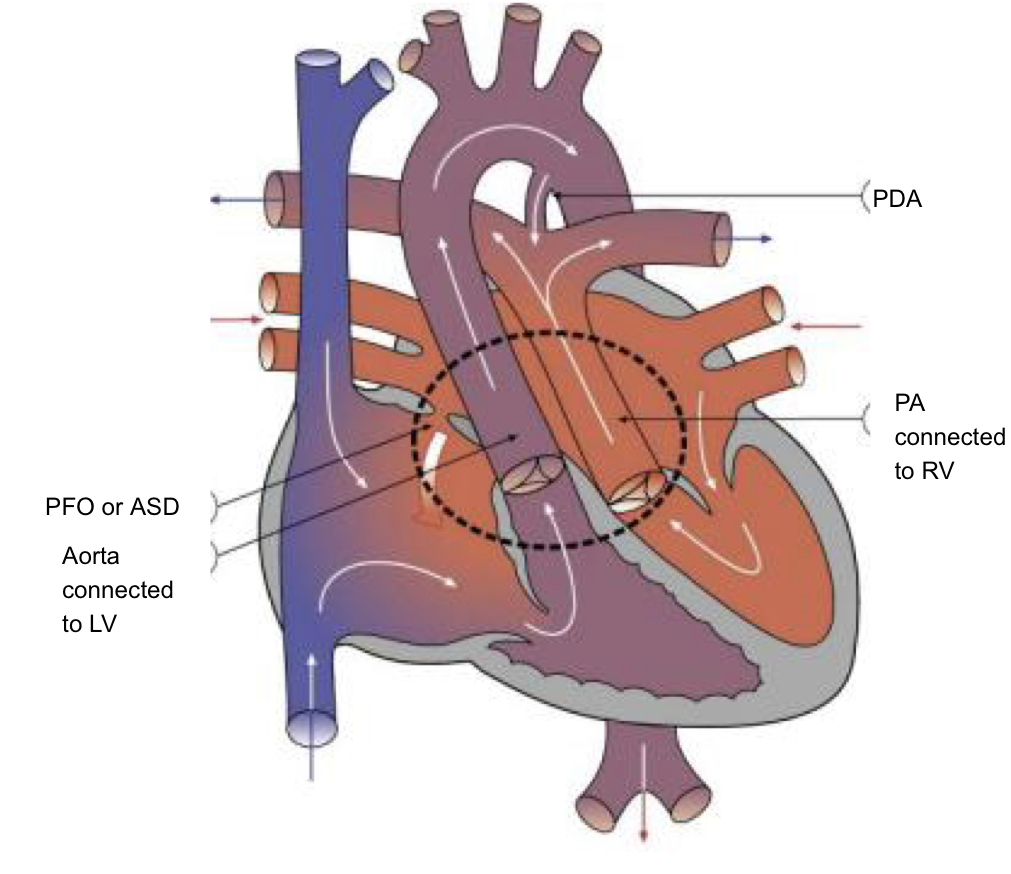
d transposition pre-op considerations
prostaglandins (PGE1) to maintain ductal patency
monitor pre and post-ductal O2 saturations
intracardiac shunting necessary to survive - will go to cath lab if needed
transposition post-op considerations
cardiac output
BP control
pain/sedation
monitor for myocardial infarction (MI)
telemetry monitor
anticoagulation
provide coronary artery patency
total anomalous pulmonary venous return (TAPVR)
pulmonary veins have no connection to the left side of the heart
blood flow pathway
results in over circulation of right side of heart and lungs and inadequate blood flow to the body
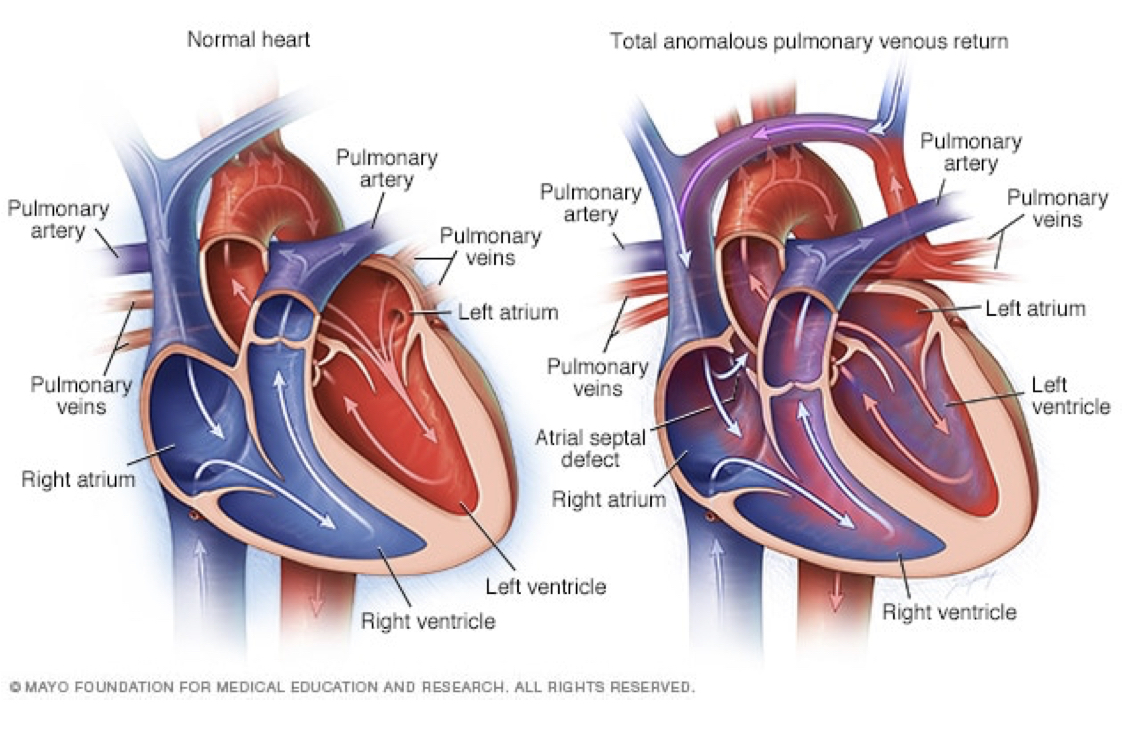
TAPVR nursing considerations pre-op
patients are dependent on an ASD
assess the structure of pulmonary veins - dictate timing of repair
TAPVR nursing considerations post-op
at risk for pulmonary hypertension
pain/sedation
oxygenation
at risk for low cardiac output
bleeding
vasoactive infusions
truncus arteriosus
results from inadequate division of the common great vessel during fetal development
blood flow pathway
a single arterial trunk gives rise to pulmonary, systemic, and coronary circulations
usually a single large truncal valve with 2-6 cusps
truncus nursing considerations pre-op
maintain adequate but not excessive pulmonary blood flow
room air-no increased FiO2
lasix
vasoactive
post-op considerations
truncal valve insufficiency
pulmonary hypertension
arrhythmias
low cardiac output syndrome
residual pulmonary stenosis
fontan stage III
all blood returning to the heart bypasses the heart and goes DIRECTLY TO TGE LUNGS (connects the IVC to the PA)
the right ventricle becomes the pumping ventricle
no pump propelling blood forward
normal ish sats after this operation
accomplished at 3 yrs of age
exubate ASAP

VAD/transplant
bridge to healing, transplant, or destination
berlin VAD is the only pediatric approved VAD (others on teenagers)
nursing considerations: VAD safety (no cracks or clots), cardiac output, neurodevelopment
cyanotic defects w/decreased pulmonary blood flow and septal defects?
TOF, tricuspid atresia, ebstein’s malformation
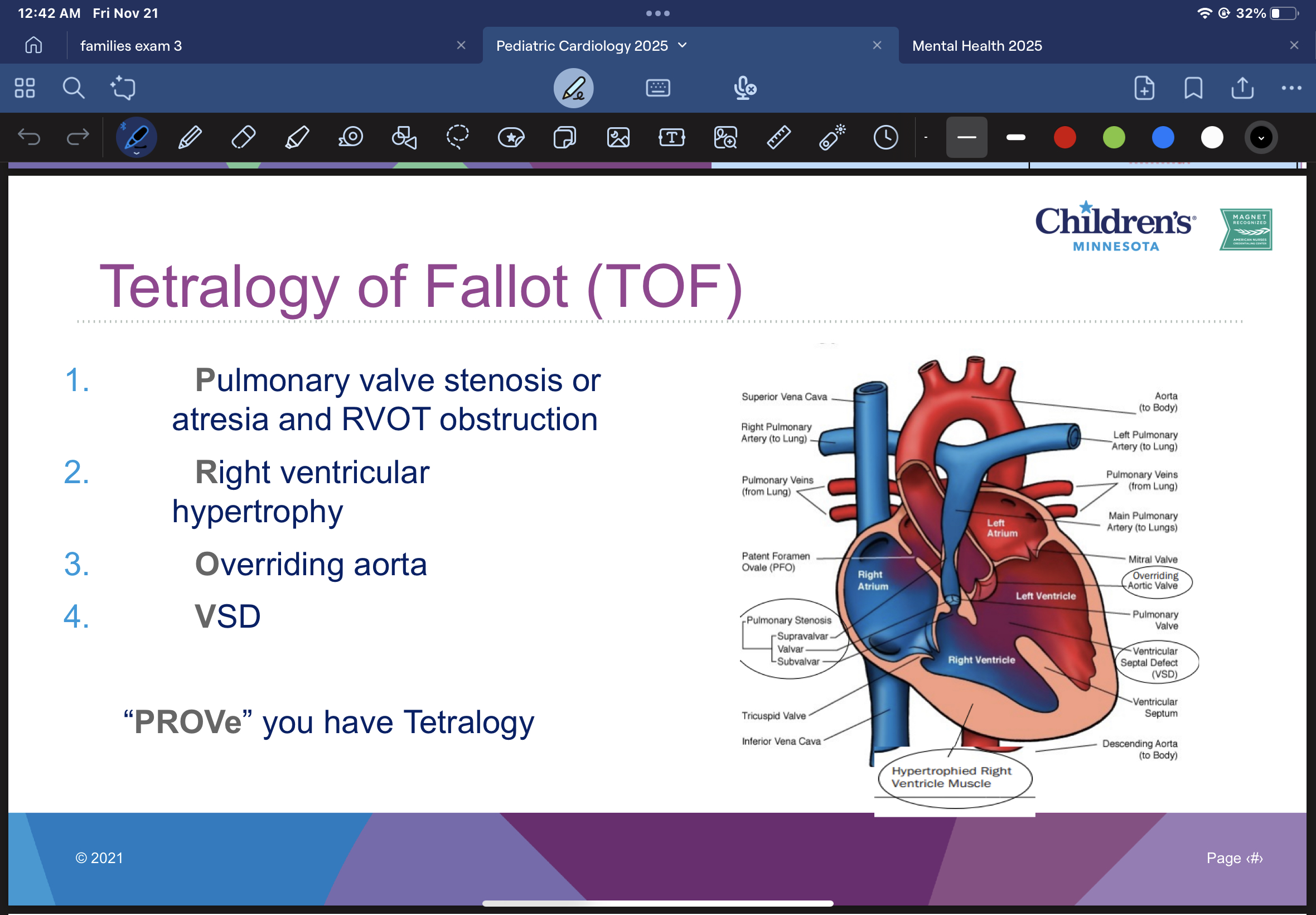
tetralogy of fallot (TOF)
pulmonary valve stenosis or atresia and RVOT obstruction
right ventricular hypertrophy
overriding aorta
VSD
“PROVe” you have tetralogy
hypercyanotic or “tet” spells
increased RVOT resistance coupled w/decreased SVR:
significantly increased R to L shunting via VSD
precipitates hypoxemia
causes
increased RVOT resistance: crying, stooling, feeding, noxious stimulus such as lab draws, IV starts, any stressors
decreased SVR: fever, dehydration
TOF nursing considerations
pre op: elevate HOB, squatting knee-chest during tet spells, O2 via best tolerated means, goal sats >85%
post op: monitor for arrhythmias, temp goal of 36-36.5, bleeding, low cardiac output
heart failure
the heart muscle can’t pump enough blood to meet the body’s needs for blood and oxygen
diagnosis: CXR-enlarged heart, ECHO - normal ejection fraction is 50-70%