9. Systemic hypertension primary and secondary, blood pressure measurement
1/209
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
210 Terms
What is systemic hypertension?
Systemic hypertension, commonly known as high blood pressure, is a prevalent condition globally that impacts a significant portion of the adult population.
What is Systemic Hypertension?
Defined as a sustained increase in blood pressure, typically diagnosed when blood pressure readings consistently exceed 140/90 mmHg.
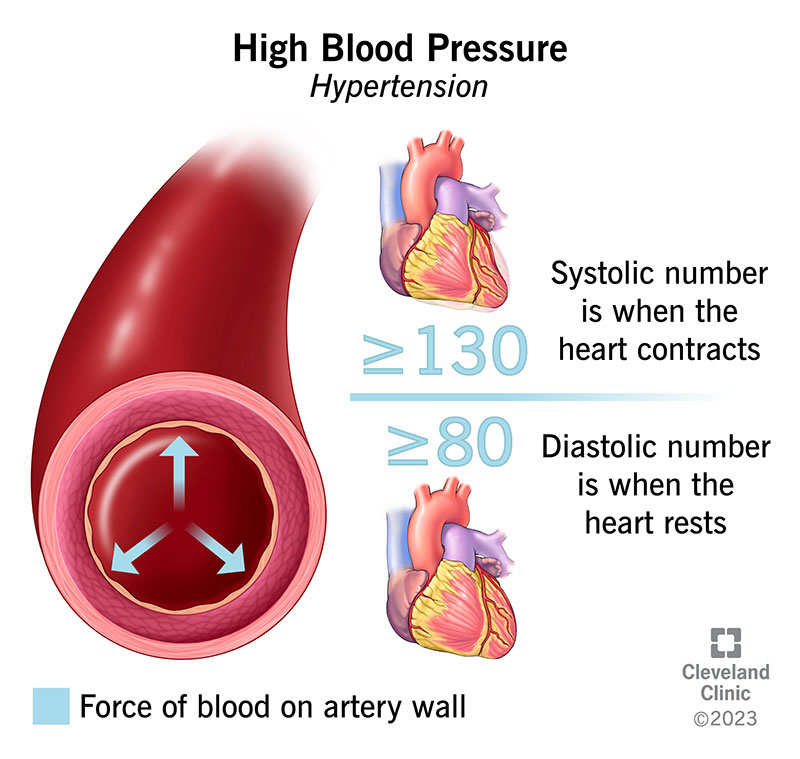
What is the Prevalence of Systemic Hypertension?
Affects about 30-45% of the general population, with incidence increasing with age—65% of individuals over the age of 60 are affected.
Risk Factors and Associations
Age
Race
Gender
Associated Risks
What is a significant risk factor for cardiovascular diseases such as stroke and heart failure?
Risk increases with age due to the natural loss of arterial elasticity.
In which communities is a higher prevalence and severity of hypertension observed?
Higher prevalence and severity observed in African American communities.
How does the prevalence of hypertension vary between genders as they age?
Initially more common in men but becomes equally prevalent in older age groups.
What are some cardiovascular diseases associated with hypertension?
Hypertension is a major risk factor for cardiovascular diseases including stroke, myocardial infarction (MI), sudden cardiac death, and heart failure.
Besides cardiovascular diseases, what other conditions can hypertension contribute to?
It also contributes to peripheral artery disease and end-stage renal disease.
Blood Pressure Categories
Optimal
Normal
High Normal
Hypertension Grades according to severity
Isolated Systolic Hypertension
What blood pressure range is considered optimal?
Blood pressure below 120/80 mmHg.
What blood pressure range is considered normal?
Systolic 120-129 mmHg and diastolic 80-84 mmHg.
What blood pressure range is classified as high normal?
Systolic 130-139 mmHg or diastolic 85-89 mmHg.
What are the three grades of hypertension based on severity?
Grade I Hypertension, Grade II Hypertension, Grade III Hypertension
what is Grade I Hypertension
Systolic 140-159 mmHg or diastolic 90-99 mmHg.
what is Grade II Hypertension
Systolic 160-179 mmHg or diastolic 100-109 mmHg.
what is Grade III Hypertension
Systolic greater than 180 mmHg or diastolic greater than 110 mmHg.
What is Isolated Systolic Hypertension?
Defined as systolic pressure above 140 mmHg with diastolic pressure below 90 mmHg, often due to arterial stiffness.
PRIMARY HYPERTENSION
PRIMARY HYPERTENSION refers to high blood pressure with no identifiable cause, often developing gradually over time. It is the most common type of hypertension.

What is primary hypertension also known as?
Essential hypertension
What percentage of hypertension cases in adults does primary hypertension account for?
Approximately 85-95%
What is the main cause of primary hypertension?
Combination of genetic predispositions and lifestyle factors
Risk Factors
Positive Family History
Age
Ethnicity
Obesity
Diabetes
Smoking and Excessive Alcohol or Caffeine Intake
High Sodium Diet
Physical Inactivity
Physiological Stress
What role does genetic predisposition play in the risk of developing hypertension?
Genetic predisposition plays a significant role in the risk of developing hypertension. Studies have shown that individuals with a family history of hypertension are more likely to develop the condition themselves. Genetic factors can influence blood pressure regulation and contribute to the development of hypertension.
How does age influence the risk of developing hypertension?
The risk of developing hypertension increases with age. It typically begins to manifest between the ages of 25 and 55.
Which ethnic group is more prone to hypertension and why?
Hypertension is more prevalent and tends to appear earlier and with more severity in the African American population compared to other ethnic groups.
How does obesity contribute to the risk of hypertension?
Excess body weight is a strong risk factor. Adipose tissue produces several substances that can increase blood pressure, such as leptin, which may not only increase sympathetic nervous system activity but also cause direct effects on blood vessels.
How are type 1 and type 2 diabetes linked to hypertension?
Both types of diabetes are associated with an increased risk of developing hypertension due to shared risk factors like obesity and inflammation.
How can smoking and excessive alcohol or caffeine intake impact blood pressure?
These substances can acutely increase blood pressure and, with chronic use, can lead to long-term hypertension.
What effect does a high sodium diet have on blood pressure?
Excessive salt intake leads to increased fluid retention, raising blood pressure, and can cause alterations in vasoactive substances balance and arterial stiffness over time.
How does physical inactivity contribute to hypertension risk?
A sedentary lifestyle contributes to weight gain and poor cardiovascular health, predisposing individuals to hypertension.
How does physiological stress affect blood pressure?
Chronic stress can lead to increased adrenal activity, resulting in higher levels of cortisol and adrenaline, tightening blood vessels and raising blood pressure.
Pathophysiology of Primary Hypertension
Neurohormonal Activation
Renal Function
Vascular Dysfunction
What is one of the underlying mechanisms of primary hypertension involving overactivity of the sympathetic nervous system and the renin-angiotensin-aldosterone system?
Neurohormonal Activation: Overactivity of the sympathetic nervous system and the renin-angiotensin-aldosterone system can lead to increased vascular resistance and water retention.
How can changes in kidney function impact blood pressure control in primary hypertension?
Changes in kidney function can affect salt and water balance, influencing blood pressure control.
What role does vascular dysfunction play in contributing to elevated blood pressure in primary hypertension?
Changes in the endothelial function and reduced arterial elasticity can increase peripheral resistance, contributing to elevated blood pressure.
SECONDARY HYPERTENSION
SECONDARY HYPERTENSION is high blood pressure caused by an underlying condition like kidney disease or hormonal disorders, different from primary hypertension with no identifiable cause.
What is secondary hypertension?
High blood pressure resulting from an identifiable underlying secondary cause.
What percentage of hypertension cases does secondary hypertension account for?
About 5-15% of all cases.
Causes of Secondary Hypertension
1. Renal Parenchymal Disease
2. Renovascular Disease
3. Endocrine Disorders
4. Structural Abnormalities
5. Lifestyle Factors and Conditions
6. Other Types of Hypertension
What are two common causes of secondary hypertension mentioned in the text?
Renal parenchymal disease and renovascular disease.
What is Renal Parenchymal Disease?
The most common cause of secondary hypertension involving conditions that impair kidney function.
Renal Parenchymal Disease refers to damage or abnormalities in the functional tissue of the kidneys. It can result from various conditions like diabetes, hypertension, infections, or autoimmune disorders, leading to impaired kidney function.
What are some causes of Renal Parenchymal Disease?
Urinary Tract Infections, Analgesic Abuse, Glomerulonephritis, Hereditary Polycystic Kidney Disease, Lupus Nephritis, and Renal Tumors.
What can lead to chronic kidney damage along with analgesic abuse?
Urinary Tract Infections (UTI)
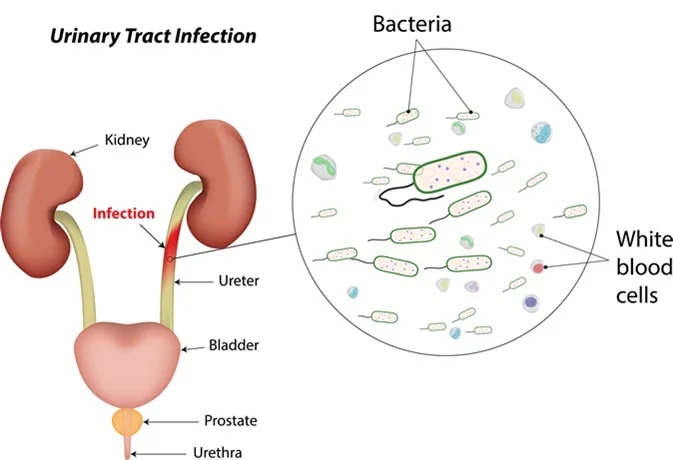
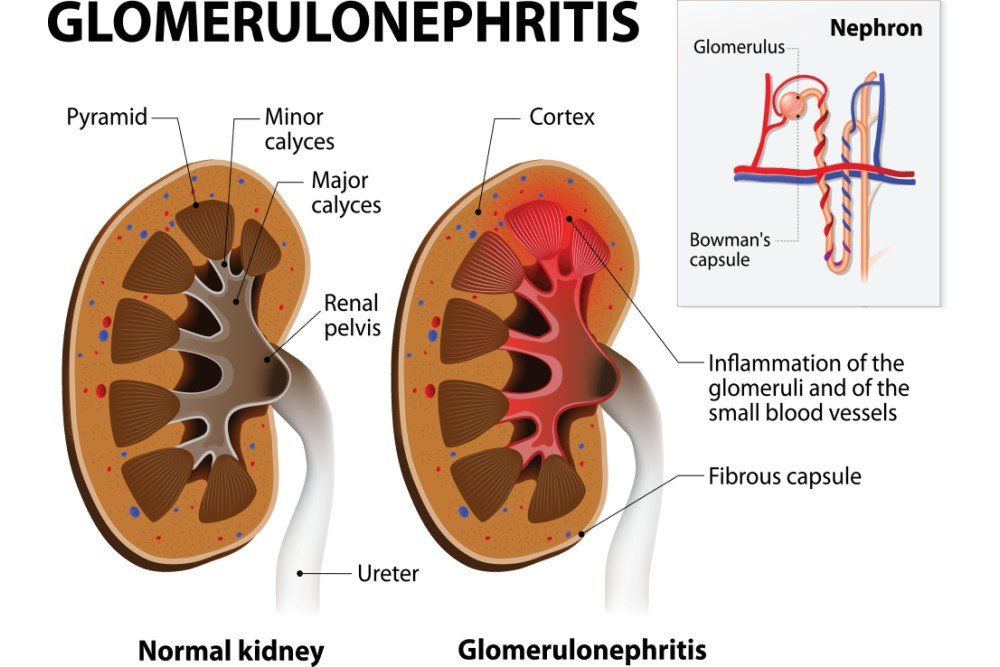
What are glomeruli and what happens during glomerulonephritis?
Tiny structures in the kidneys that filter blood; inflammation occurs.
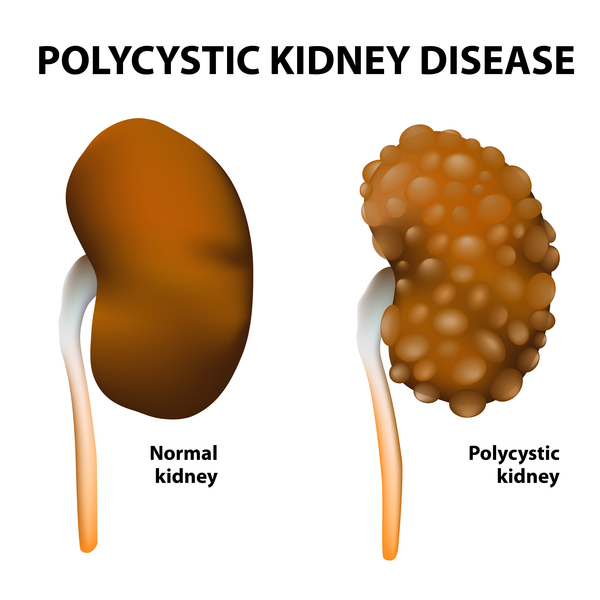
What is Hereditary Polycystic Kidney Disease characterized by?
Growth of numerous cysts in the kidneys due to a genetic disorder.
What is Lupus Nephritis?
An autoimmune disease causing kidney inflammation.
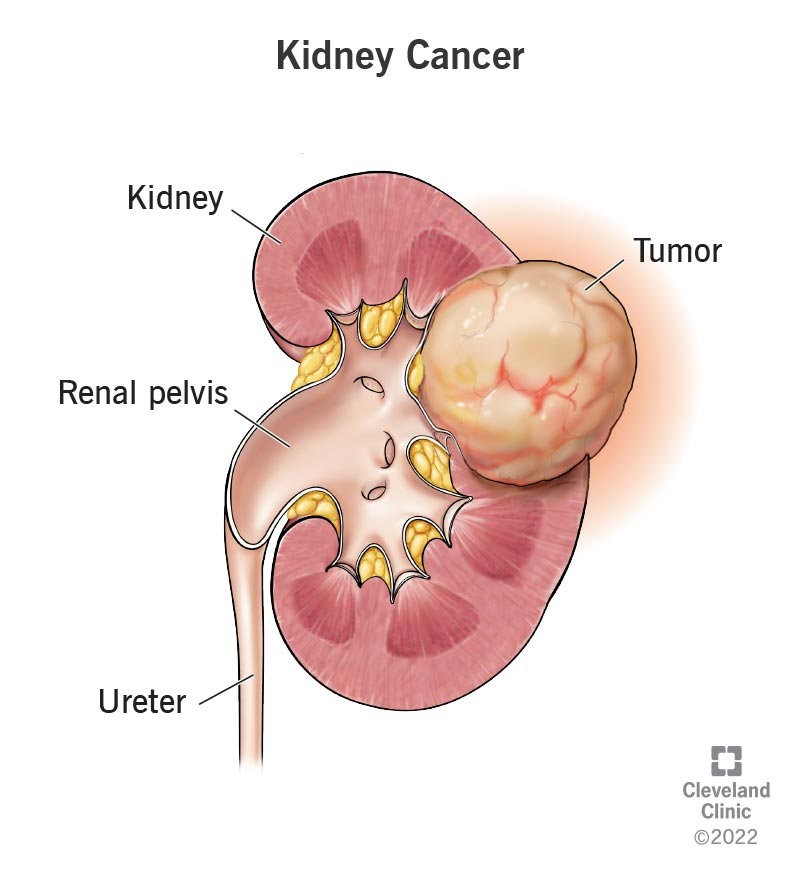
How can Renal Tumors impact kidney function and blood pressure regulation?
They can impair kidney function and affect blood pressure regulation.
Renal tumors can disrupt kidney function by impairing filtration and causing blockages. They can also affect blood pressure regulation by secreting hormones that raise blood pressure or by compressing blood vessels.
Symptoms and Diagnosis of Renal Parenchymal Disease
Creatinine levels
Urine concentration
Ultrasound
Hormonal changes
What might rising creatinine levels indicate in patients?
Kidney dysfunction.
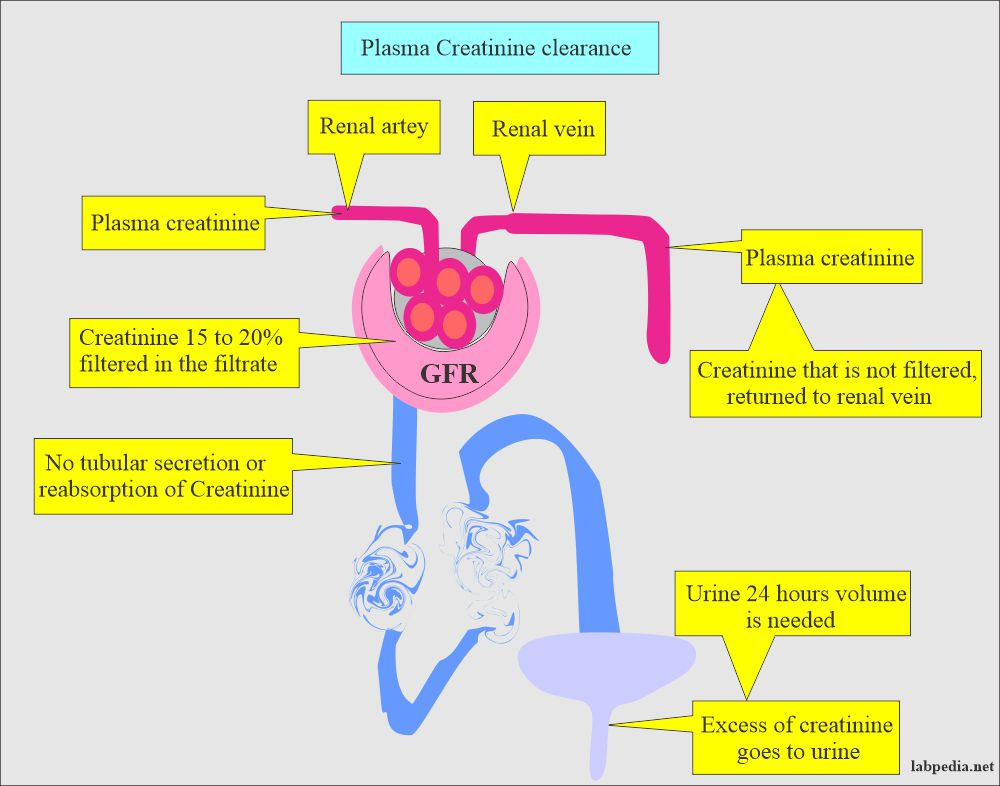
What can an inability to concentrate urine indicate as kidney damage progresses?
There is typically an inability to concentrate urine, which can become more apparent as kidney damage progresses.
An inability to concentrate urine can indicate kidney damage progressing towards renal failure.
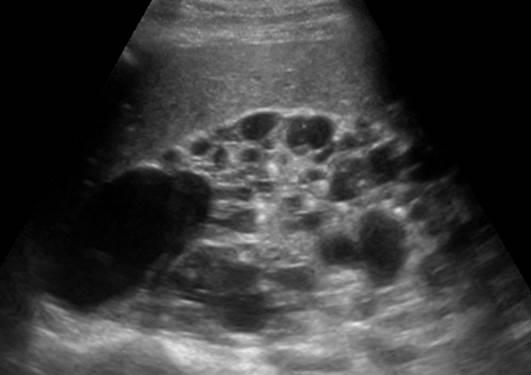
What might an ultrasound reveal in cases like polycystic kidney disease?
Enlarged kidneys.
What hormonal changes are often seen in patients with kidney damage?
Low aldosterone and renin activity, unless compensatory overactivation has occurred.
Secondary Hypertension- Renovascular Disease
What is Renovascular Disease characterized by?
This condition involves the narrowing (stenosis) of one or both renal arteries, which can be caused by atherosclerosis or fibromuscular dysplasia.
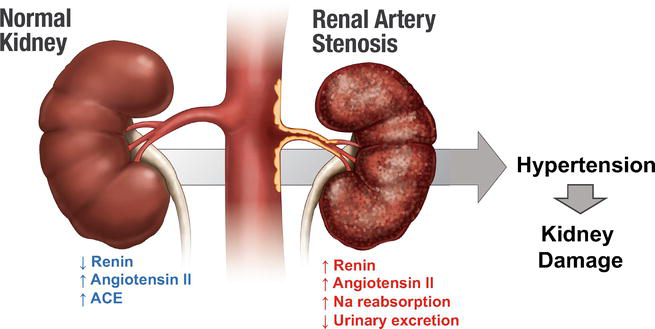
What are the two main causes of Renovascular Disease?
Atherosclerosis
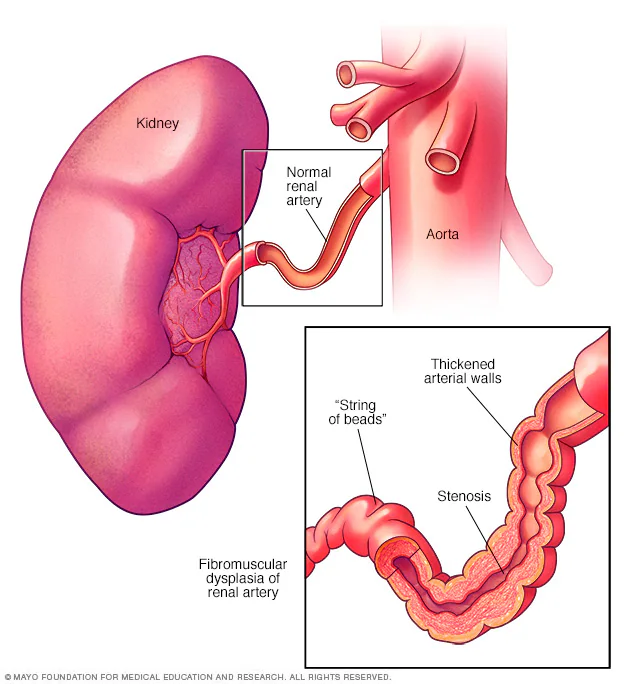
Fibromuscular Dysplasia
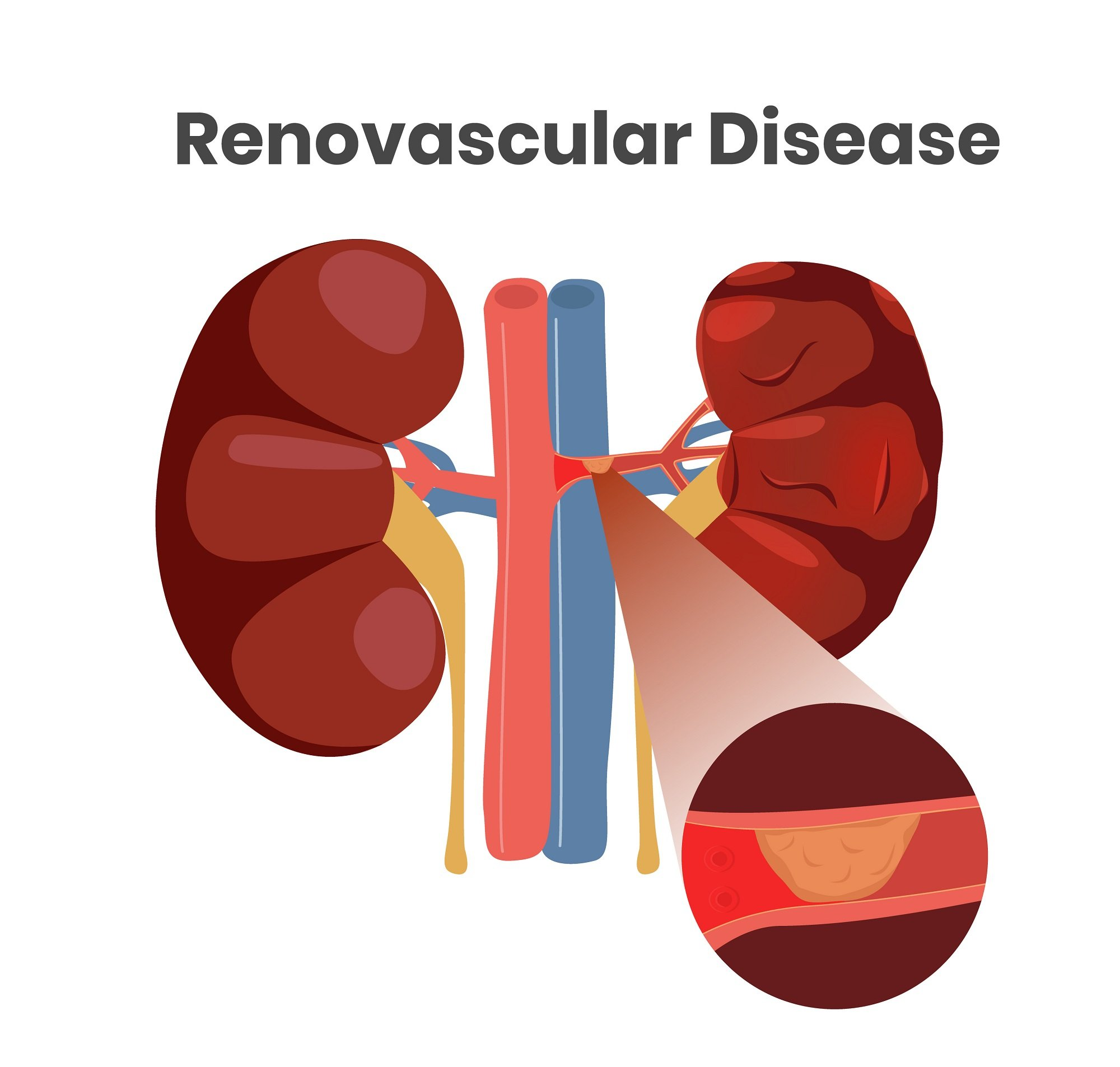
What is the most common cause of atherosclerosis?
Plaque buildup in the arteries.
Who is fibromuscular dysplasia more common in?
Young women.
Fibromuscular dysplasia is a non-inflammatory, nonatherosclerotic vascular disease that primarily affects medium-sized arteries, leading to abnormal cell development in the arterial walls.
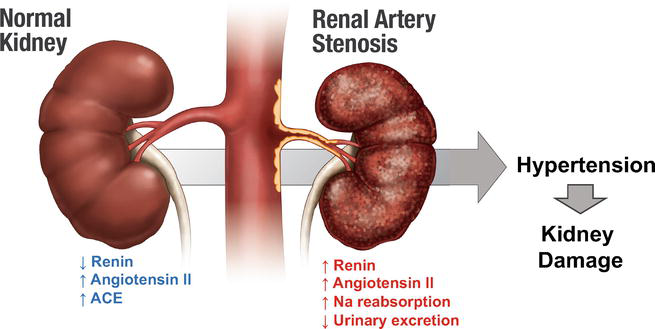
How does renal artery stenosis lead to increased blood pressure in the body?
The stenosis causes reduced blood flow to the kidneys, which triggers the activation of the renin-angiotensin-aldosterone system (RAAS), increasing blood pressure throughout the body.
Symptoms and Diagnosis of renal artery stenosis —> renovascular disease
Urine concentration
Aldosterone and Renin levels
Ultrasound and CT Angiography
What are some symptoms and diagnostic methods associated with renal artery stenosis?
Symptoms include normal urine concentration but possibly increased creatinine levels. Diagnostic methods like ultrasound and CT angiography are useful for assessing blood flow to the kidneys and confirming the stenosis.
Normal urine concentration, but possibly increased creatinine levels.
Elevated levels of aldosterone and renin due to RAAS activation.
Ultrasound and CT Angiography: Useful for assessing blood flow to the kidneys and confirming renal artery stenosis.
3. Endocrine Disorders- As a Cause of Secondary Hypertension
Primary Hyperaldosteronism (Conn's Syndrome)
Cushing's Syndrome (Hypercortisolism)
Hyperthyroidism
Pheochromocytoma
Primary Hyperparathyroidism
Acromegaly
Congenital Adrenal Hyperplasia
Primary Hyperaldosteronism
What are the characteristics of Primary Hyperaldosteronism (Conn's Syndrome)?
Overproduction of aldosterone, leading to sodium retention, potassium loss, and metabolic alkalosis.
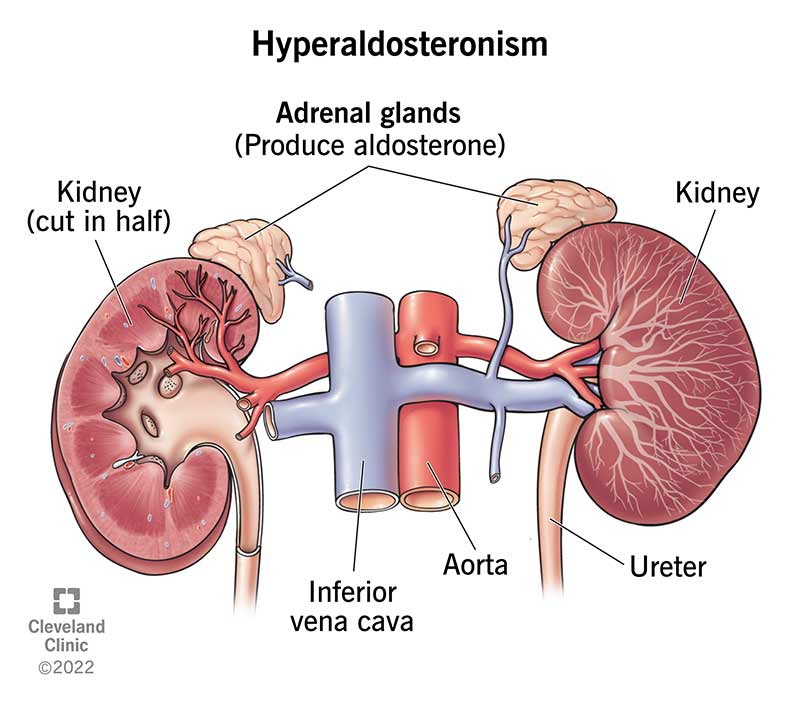
Primary Hyperaldosteronism
How does potassium loss causes metabolic alkalosis?
Potassium loss causes metabolic alkalosis by reducing hydrogen ion excretion in the kidneys, leading to increased bicarbonate retention and alkalinity in the blood.

Primary Hyperaldosteronism
What is the diagnostic marker for Primary Hyperaldosteronism (Conn's Syndrome)?
Increased aldosterone/renin ratio, with decreased renin activity due to negative feedback.
Primary Hyperaldosteronism causes increased aldosterone/renin ratio due to excessive production of aldosterone by the adrenal glands, leading to low renin levels and high aldosterone levels in the blood.
Cushing's Syndrome (Hypercortisolism)
What are the symptoms of Cushing's Syndrome (Hypercortisolism)?
Central obesity, thin limbs, moon face, and possibly a buffalo hump.
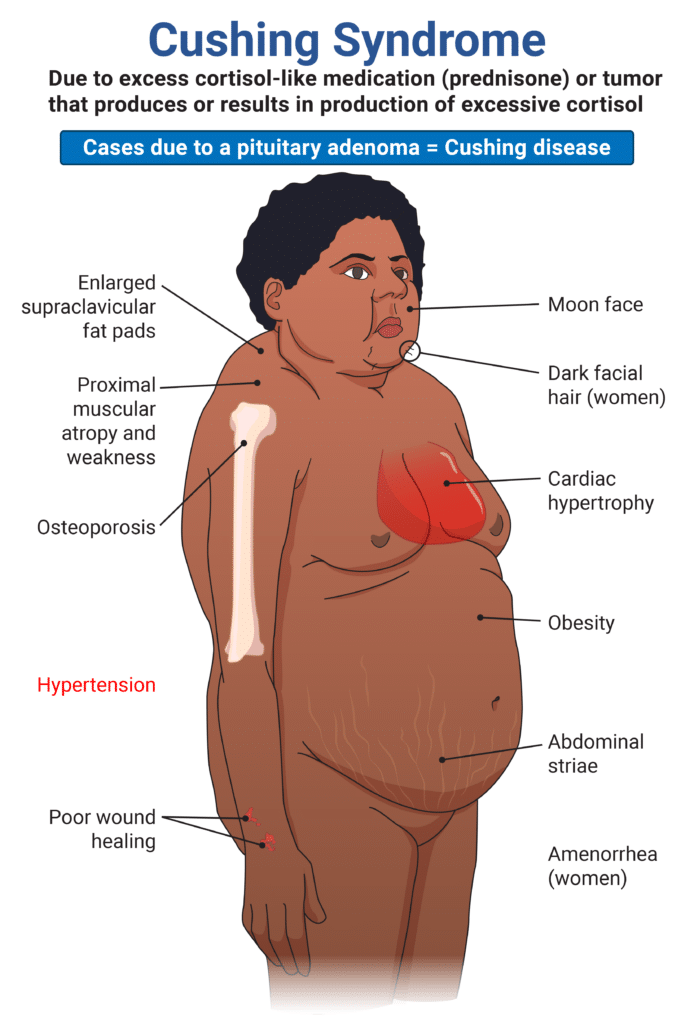
Cushing's Syndrome (Hypercortisolism)
What is the cause of Cushing's Syndrome (Hypercortisolism)?
Excess cortisol, which increases glucose and has mineralocorticoid effects that increase sodium and water retention, raising blood pressure.
Hyperthyroidism:
What are the effects of hyperthyroidism?
Increased metabolism and enhanced sensitivity to sympathetic stimulation due to excess thyroid hormones (T4), leading to increased heart rate and blood pressure.
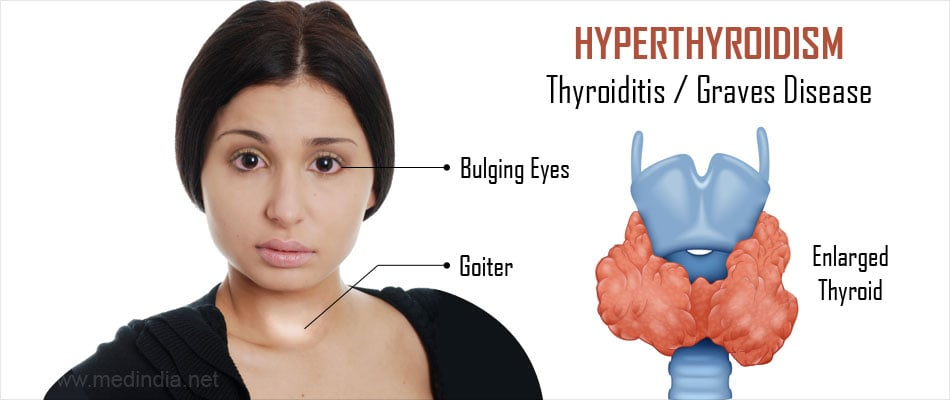
What are the laboratory findings associated with hyperthyroidism?
Elevated T4 levels and suppressed TSH.
In hyperthyroidism, elevated T4 levels signal excess thyroid hormone production, leading to negative feedback on the pituitary gland, suppressing TSH secretion.
pheochromocytoma
How does pheochromocytoma typically present?
Episodic or sustained hypertension due to catecholamine-secreting tumors typically found in the adrenal medulla.
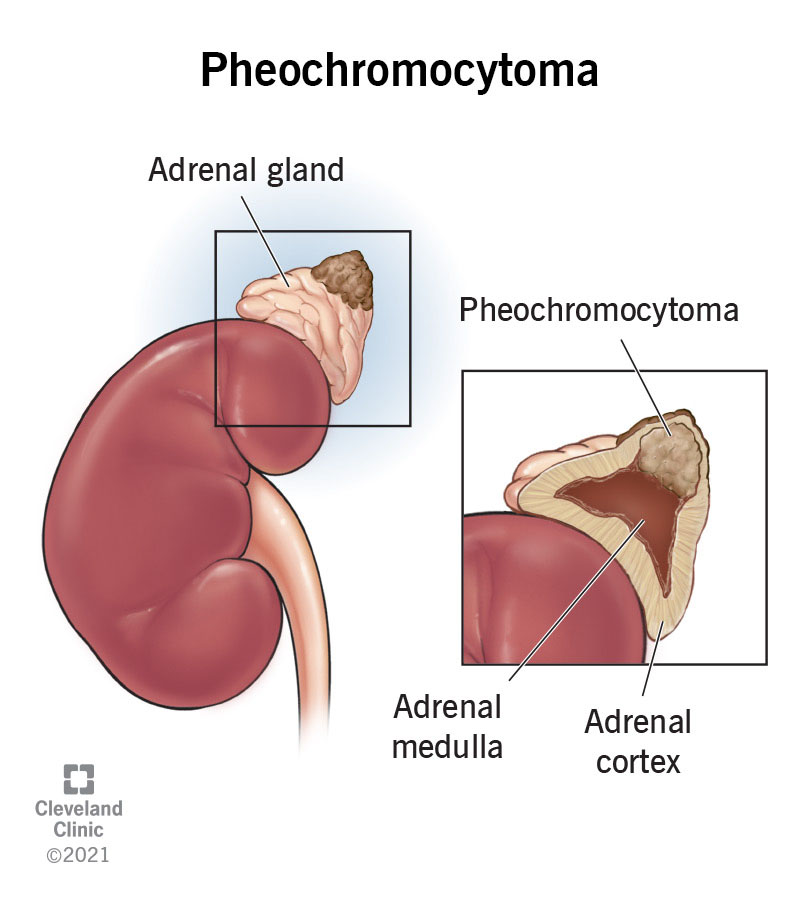
How is pheochromocytoma diagnosed?
High levels of urinary metanephrines, which are catecholamine metabolites.
primary hyperparathyroidism
What is the mechanism behind primary hyperparathyroidism?
Excess parathyroid hormone (PTH) leads to increased calcium levels; hypercalcemia can increase vascular resistance.
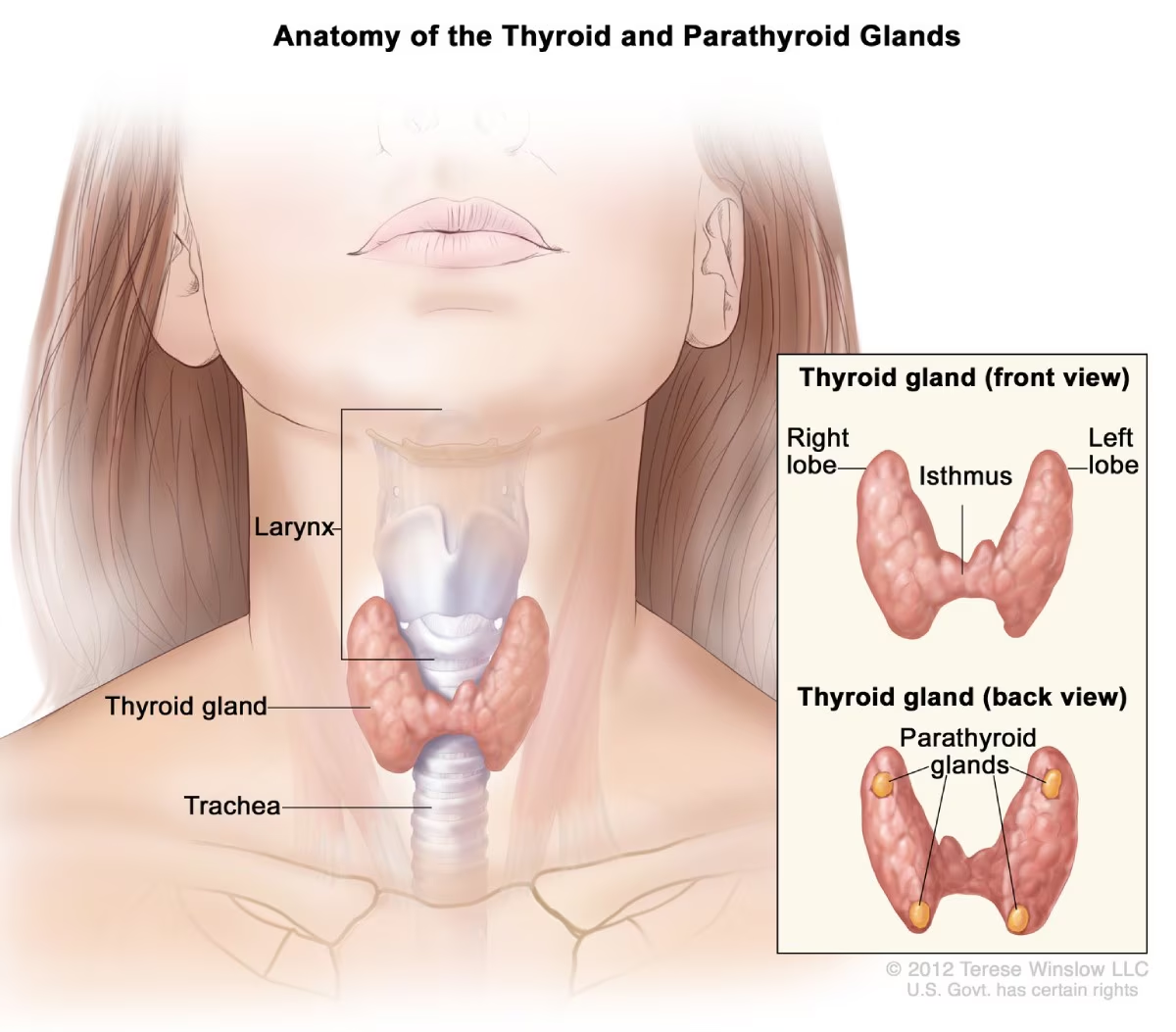
What are the lab values associated with primary hyperparathyroidism?
High calcium, high PTH, and low phosphate levels.
Acromegaly
What is the cause of Acromegaly?
Overproduction of growth hormone usually due to a pituitary adenoma.
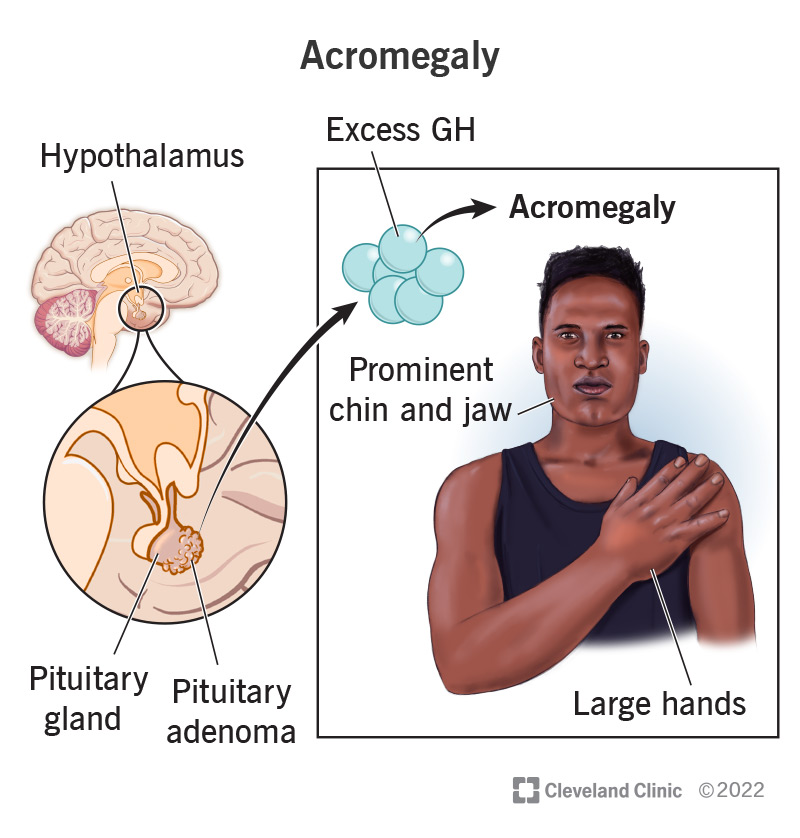
What effect does increased growth hormone and IGF-1 levels have in Acromegaly?
They cause fluid retention and increase cardiac output, contributing to hypertension.
What are the specific forms of Congenital Adrenal Hyperplasia?
Deficiencies in 17alpha- and 11beta-hydroxylase can lead to overproduction of mineralocorticoids, which mimic aldosterone effects.
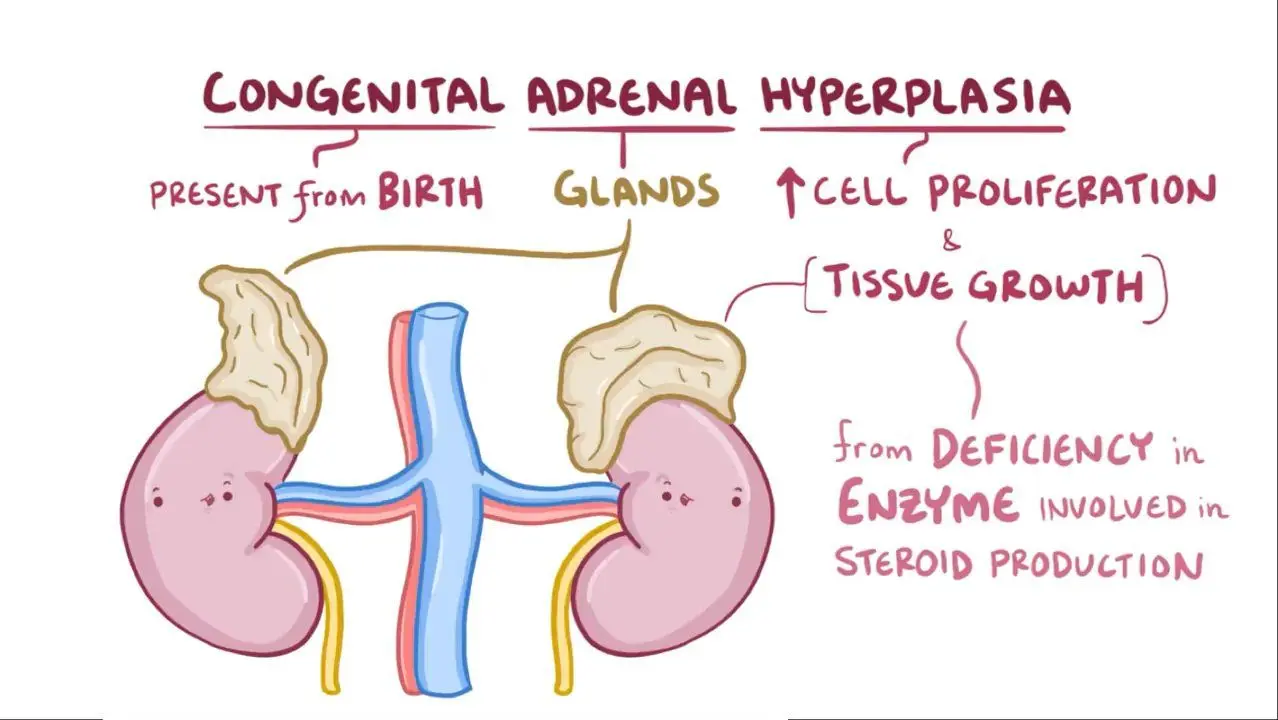
What result can deficiencies in 17alpha- and 11beta-hydroxylase lead to in Congenital Adrenal Hyperplasia?
Deficiencies in 17alpha- and 11beta-hydroxylase can lead to excess androgen production in Congenital Adrenal Hyperplasia.
Deficiencies in 17alpha- and 11beta-hydroxylase can lead to overproduction of mineralocorticoids, which mimic aldosterone effects.
Sodium retention and potassium loss, which elevate blood pressure.
4. Structural Abnormalities (As a cause of Secondary Hypertension)
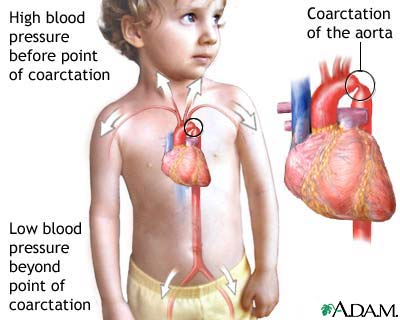
Coarctation of the Aorta
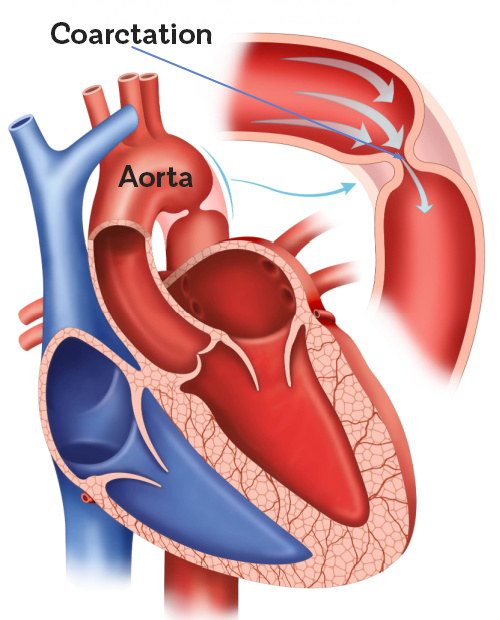
What is coarctation of the aorta?
Narrowing of the aorta, typically distal to the left subclavian artery branch.
What are the symptoms of coarctation of the aorta?
Higher blood pressure in the arms than in the legs, and delayed or weaker femoral pulses compared to radial pulses.
5. Lifestyle Factors and Conditions (As a cause of secondary hypertension)
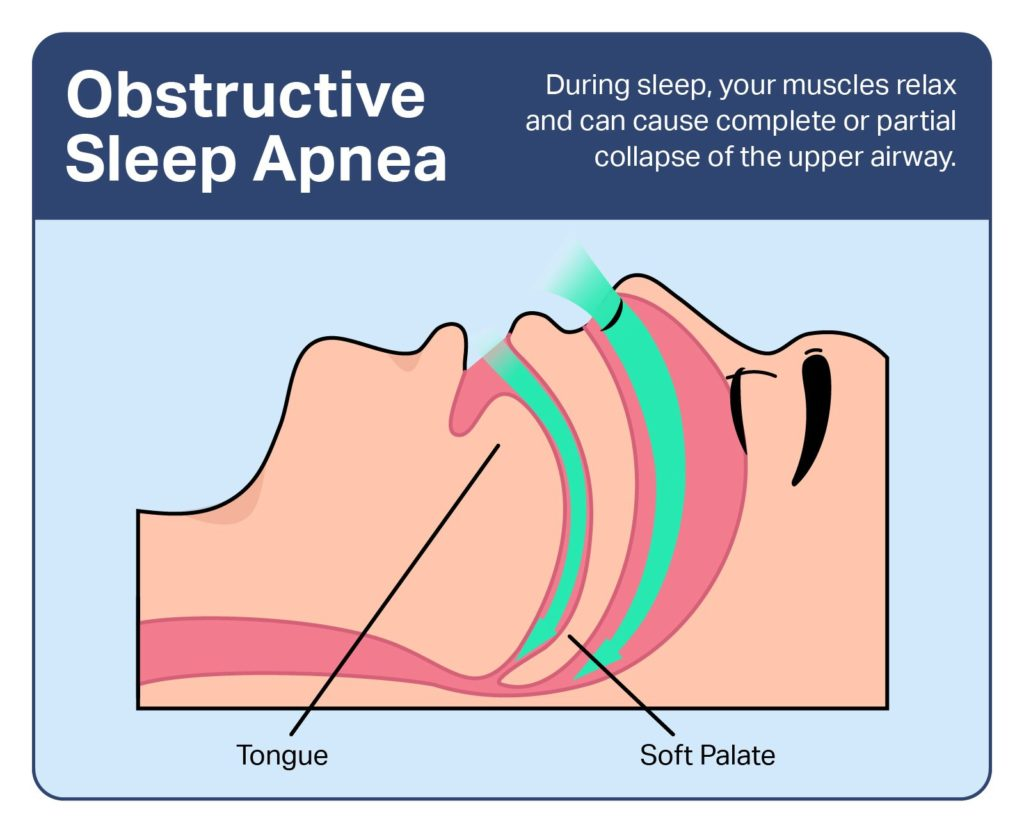
Obstructive Sleep Apnea (OSA)
Drug-Induced Hypertension
Hypertension
Chronic Stress
What is the mechanism behind hypertension in obstructive sleep apnea (OSA)?
Intermittent hypoxia and hypercapnia from repeated airway closures increase sympathetic activity and blood pressure.
What are some substances that can induce drug-induced hypertension?
Includes substances like sympathomimetics, corticosteroids, NSAIDs, oral contraceptives, amphetamines, and cocaine, all of which can raise blood pressure through various mechanisms.
What is the mechanism by which pregnancy can lead to increased blood volume and water retention?
Increased estrogen stimulates the renin-angiotensin system, enhancing water retention and expanding blood volume.
How does chronic stress affect the cardiovascular system in terms of heart rate and vascular resistance?
Persistent elevation of catecholamines (adrenaline and noradrenaline) increases heart rate and vascular resistance.
Other Types of Hypertension
White Coat Hypertension
Masked Hypertension
Isolated Systolic Hypertension
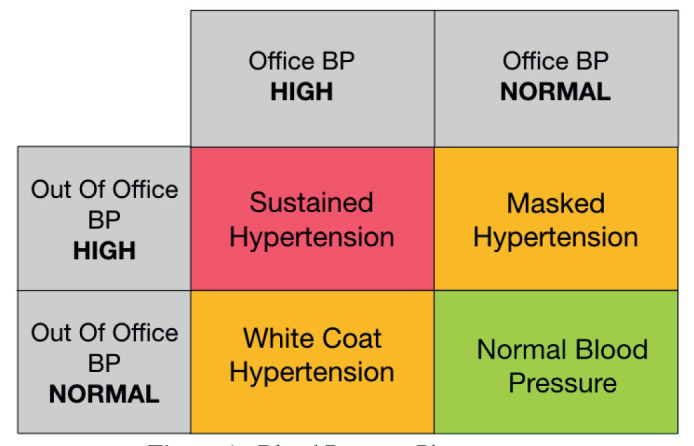
What is White Coat Hypertension?
This condition occurs when patients exhibit high blood pressure readings in a clinical setting but have normal readings elsewhere.

What is the prevalence of White Coat Hypertension?
About 13% of people may experience this form of hypertension.
How can true blood pressure levels be confirmed in patients with White Coat Hypertension?
Ambulatory blood pressure monitoring over 24 hours can help confirm true blood pressure levels, as this method provides readings in a variety of settings and times, reducing the influence of anxiety associated with doctor's visits.
What is Masked Hypertension?
Opposite of white coat hypertension, where patients show normal blood pressure readings in a clinical setting but have high readings in their daily life.
What is the prevalence of Masked Hypertension?
Also affects an estimated 13% of individuals.
Why is Masked Hypertension risky?
Often goes undetected without the use of ambulatory or home blood pressure monitoring, potentially leading to untreated hypertension and its complications.
What is Isolated Systolic Hypertension characterized by?
Elevated systolic pressure (>140 mmHg) while diastolic pressure remains normal (<90 mmHg).

What are some common causes of Isolated Systolic Hypertension?
Decreased arterial elasticity in the elderly, anaemia, hyperthyroidism, chronic aortic regurgitation, and arteriovenous fistulas.
What are the symptoms of Isolated Systolic Hypertension?
Often asymptomatic, but may present with signs of increased pulse pressure, such as visible pulsation of the head (De Musset's sign).
Clinical Features and Symptoms of Hypertension
Headaches
Dizziness and Tinnitus
Visual Changes
Epistaxis
Cardiac Symptoms
Nervous System Symptoms
Why is hypertension often undetected until serious health issues arise?
Hypertension is typically asymptomatic in its early stages, which is why it is so dangerous and often goes undetected until serious health issues arise.
What are common characteristics of headaches associated with hypertension?
Often occur in the morning, can be intense, and located at the back of the head.
What nonspecific symptoms are common in individuals with high blood pressure?
Dizziness and ringing in the ears (Tinnitus).
How can hypertension affect the eyes?
Hypertension can affect the blood vessels in the eyes, leading to blurred vision.
What can nosebleeds sometimes indicate in relation to hypertension?
Nosebleeds can sometimes be a sign of chronically high blood pressure.
Nosebleeds can sometimes indicate hypertension due to increased pressure in blood vessels, leading to vessel fragility and bleeding.