9) Single fields
1/13
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No study sessions yet.
14 Terms
What are examples of single field treatment?
1) megavolt (4-6Mv)
2) Orthovoltage
3) e-
What can single fields be used to treat for (review Q)?
1) scalp
2) breast boost (lumpectomy scarr)
3) eye orbits
4) parotid
5) superficial bony metastases (rib, sternum, skull, scapula)
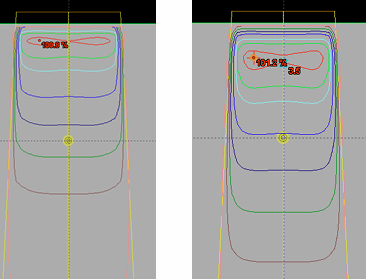
Which beam has higher energy (review q)?
RIGHT
deeper dmax
more horns
as photon energy INCREASES, range of 2ndary e- increases
→ more energy deposited DEEPER in tissue

1) The depth of a given isodose curve __ with beam quality.
2) Greater lateral scatter is associated with __.
3) for MEGAVOLTAGE beams, scatter OUTSIDE the field is __ due to _
1) increases
2) lower energy beams.
3) minimized, forward scattering
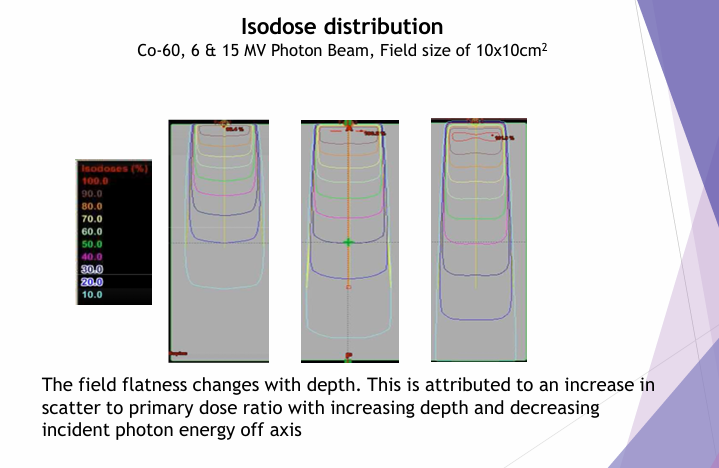
What are the considerations for selecting beam energy (review q)?
1) Prescription point/region
(where the dose is prescribed)
2) Variation of dose within tumor
(will there be significant dose variation within PTV - ideally no; we want homogeneity aka beam coming from all sides. single field will not be homogenous- NEVER)
3) Maximum dose in tissue
(minimize hotspots; only worry about in POP, not in single field)
4) Exit dose
(what critical structures in the path of beam)

Identify photon beam quality for different beam energies
6MV
- 10×10
- 100cm SSD
- %DD @ 10cm = 67%
15MV
- 10×10
- 100cm SSD
- %DD @ 10cm = 77%

Effects of field size & shape on beam:
increase field size
→ increase PDD (more scatter radiation)
(increase in PDD also depends on beam quality)
→ change field size → PDD affected more w/ lower energy (high energy less effect)
When is orthovoltage used?
Single field
-skin lesion
-superficial bone met
What are orthovoltage considerations (review q)
1) low PDD
2) no skin sparing (100% surface dose)
3) increased absorption in bone
4) available resources (wa??)
5) tumor volume accessibility
(it better be superficial)
When is e- used?
Single field
- skin
- vulva
- breast
- superficial lymph
- parotid
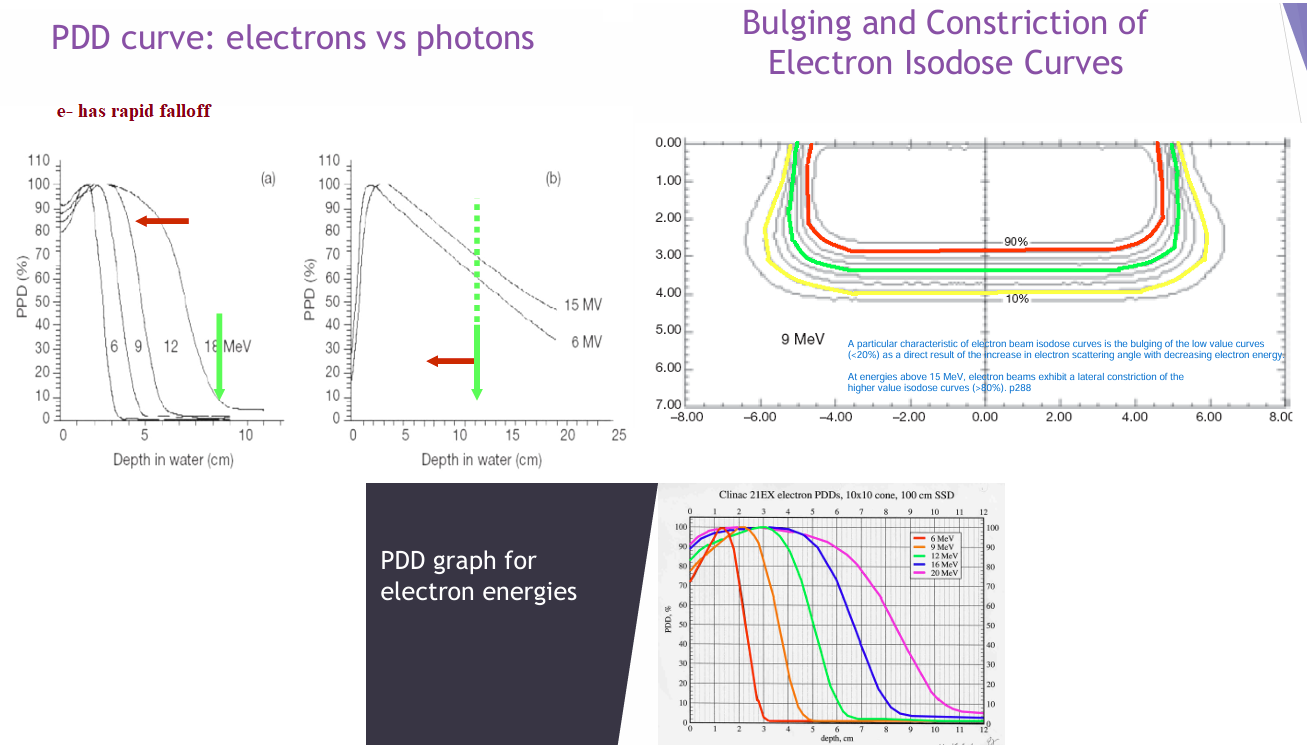
What are e- considerations (review q)?
-rapid falloff (compared to MV-xray)
-high surface dose (compared to MV-xray)
-bulging + pinching of isodose curves (@deeper doses)
-difficult to predict passing through nonhomogenous (ex. lung tissue → air)
-available resources (wuhh)
(just to refresh your mind)
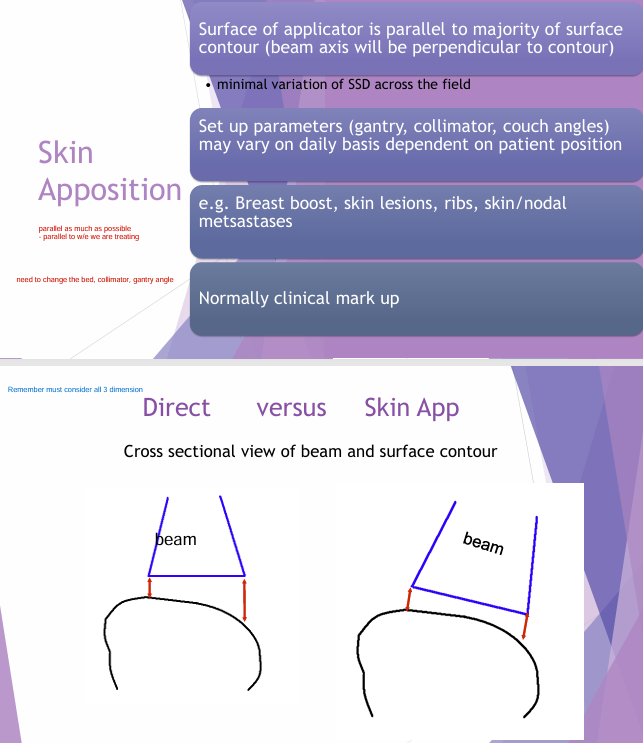
Differentiate b/w skin apposition & direct field
Skin apposition = surface applicator PARALLEL to majority of surface
Direct = just directly on top (might be lopsided surface - not uniform dose distribution)
→ you can use bolus to make it better