Eating and Sleep–Wake Disorders: Criteria, Types, Causes, and Treatments
1/81
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
82 Terms
What are the criteria for determining abnormality?
Unusualness, social deviance, faulty perceptions, significant personal distress, maladaptive behavior, and dangerousness.
What are the main types of eating disorders?
Anorexia nervosa, bulimia nervosa, binge-eating disorder, and obesity.
What is anorexia nervosa characterized by?
Severe weight loss due to significant restriction of calorie intake, excessive fear of gaining weight, and distorted body image.
What is the lifetime prevalence of anorexia nervosa in women?
Approximately 0.9% (9 in 1,000 women).
What are the two subtypes of anorexia nervosa?
Binge-eating/purging type and restricting type.
What are common medical complications of anorexia nervosa?
Anemia, cardiovascular complications, gastrointestinal problems, and increased risk of death.

What characterizes bulimia nervosa?
Recurrent episodes of binge eating followed by compensatory behaviors such as purging.
What is the lifetime prevalence of bulimia nervosa in women?
Between 0.9% and 1.5%.
What are common features of bulimia nervosa?
Feelings of lack of control over eating, fear of gaining weight, and excessive concerns about body shape.
What are the medical complications associated with bulimia nervosa?
Repeated vomiting, skin irritation, decay of tooth enamel, and potassium deficiency.
What is binge-eating disorder?
Recurrent binge eating without compensatory purging.
What is the lifetime prevalence of binge-eating disorder in women?
Approximately 3.5%.
What psychosocial factors may contribute to eating disorders?
Feelings of insecurity, body dissatisfaction, and problems with interpersonal relationships.
What sociocultural factors influence eating disorders?
Social pressure, body dissatisfaction from media images, and dieting behaviors.
At what age does body dissatisfaction typically begin to manifest?
As early as 8 years of age.
What is the impact of media images on body image perception?
They can lead to disturbed eating behaviors and body dissatisfaction.
What is the typical age range for the onset of anorexia nervosa?
Between the ages of 12 and 18.
What is the average frequency of binge-purge episodes in bulimia nervosa?
At least one episode per week for three consecutive months.
What are the two types of anorexia nervosa and their characteristics?
Binge-eating/purging type (binge eating or purging) and restricting type (rigid control of diet).
What is the significance of the term 'maladaptive behavior' in the context of eating disorders?
Behaviors that are self-defeating and hinder an individual's ability to function effectively.
What role does emotional gratification play in eating disorders?
Food may be used as a means to cope with emotional distress.
What are the psychological features of anorexia nervosa?
Intense fear of becoming fat, intentional starvation, and distorted body image.
What is the relationship between dieting and eating disorders?
High rates of dieting among young women can lead to increased risk of developing eating disorders.
What is the role of family factors in the development of eating disorders?
Family dynamics and pressures can contribute to the onset and maintenance of eating disorders.
What is the common demographic affected by anorexia nervosa?
Typically affects young, European American women.
What are the potential consequences of binge-eating disorder?
Compulsive overeating and associated health risks.
How does the prevalence of eating disorders differ between genders?
Eating disorders are more common in women, but men can also be affected.
What is the impact of excessive exercise in bulimia nervosa?
It is often used as a compensatory behavior to prevent weight gain.
What is the significance of amenorrhea in anorexia nervosa?
It indicates a serious health risk and is characterized by the absence of three or more menstrual cycles.
What is anorexia nervosa?
An eating disorder characterized by an attempt to relieve upsetting emotions by seeking control over body.
What is bulimia nervosa?
An eating disorder that involves coping with emotional distress, often accompanied by other diagnosable disorders.
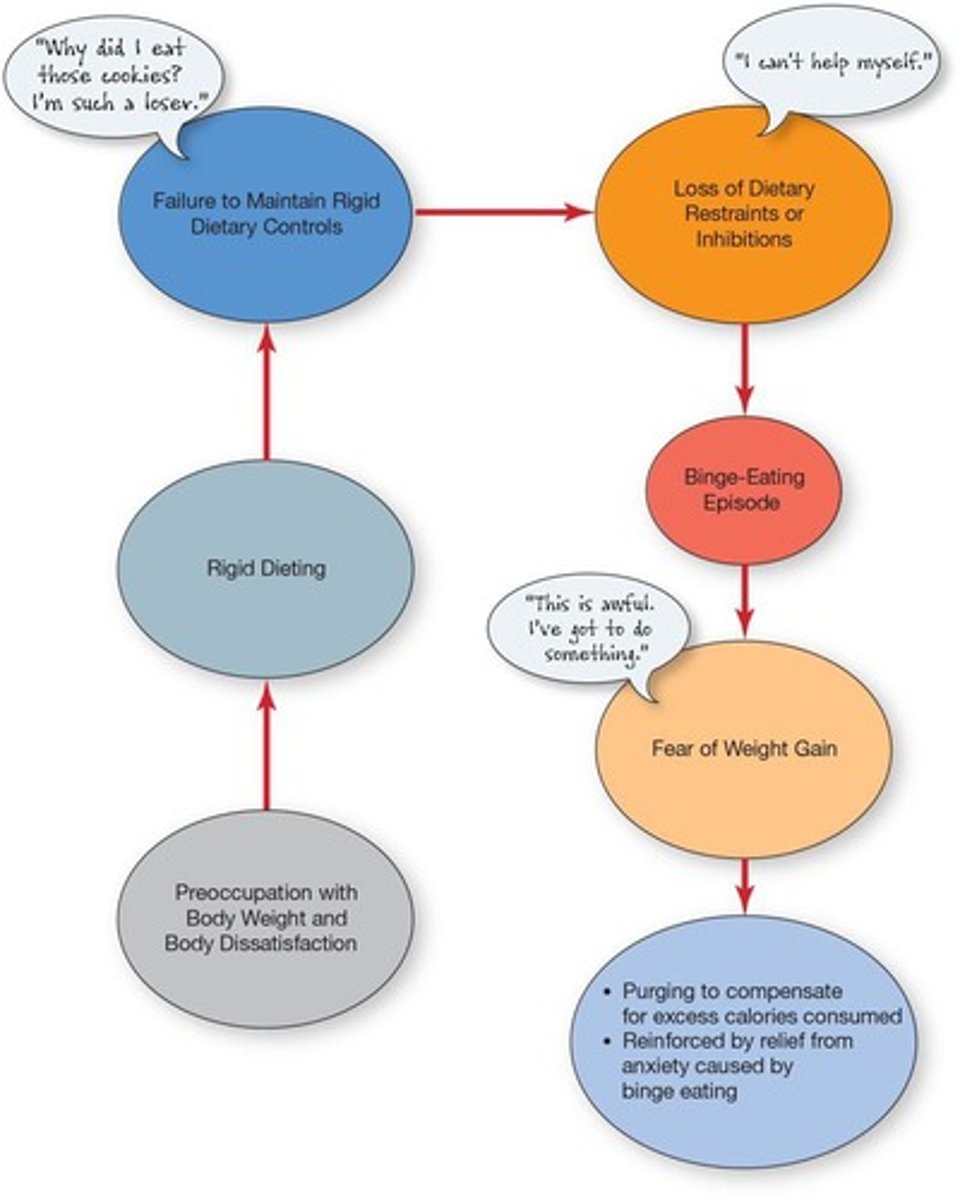
How can bulimia be negatively reinforced?
Purging produces relief from anxiety over gaining weight.
What psychological factors contribute to eating disorders?
Perfectionism, overconcern about mistakes, and a strong need for control.
What family dynamics are associated with anorexia nervosa?
Dysfunctional families with high conflict and overprotective but less nurturing parents.
What biological factors are linked to eating disorders?
Serotonin imbalance, genetic factors, and heredity.
What treatments are available for anorexia nervosa and bulimia nervosa?
Hospitalization, cognitive behavior therapy, interpersonal psychotherapy, and SSRI-type antidepressants.
What is insomnia disorder?
A sleep disorder characterized by chronic difficulties falling asleep, remaining asleep, or achieving restorative sleep.
What are the types of insomnia?
Transient, short-term, and chronic insomnia.
What is hypersomnolence disorder?
A pattern of excessive sleepiness during the day, causing distress or difficulties in daily functioning.
What characterizes narcolepsy?
Sudden, irresistible episodes of sleep, often transitioning directly into REM sleep.
What is cataplexy?
A sudden loss of muscular control often associated with narcolepsy.
What is the relationship between social media use and body dissatisfaction?
Comparing oneself to others on social networking sites may negatively affect body image.
What is the prevalence of binge-eating disorder?
It is the most common eating disorder overall and occurs more often in women than men.
What are the effects of insomnia on daily functioning?
Insomnia affects concentration, attention, response time, problem solving, and memory.
What is the significance of serotonin in eating disorders?
Serotonin imbalance is a biological factor linked to the development of eating disorders.
What are common co-morbid conditions with insomnia?
Anxiety, unipolar affective disorder, bipolar disorder, and substance abuse.
What is the role of cognitive behavior therapy in treating eating disorders?
It helps address the cognitive distortions and behaviors associated with eating disorders.
How does weight control relate to energy balance?
Weight is determined by the balance between calories consumed and calories used.
What is the impact of family problems on eating disorders?
Family conflicts and dysfunction can contribute to the development of eating disorders.
What is a common treatment for hypersomnolence disorder?
Stimulant medication is often used to manage excessive daytime sleepiness.
What is the typical duration for chronic insomnia?
Chronic insomnia lasts for a month or longer and is associated with impairments in daily functioning.
What is the relationship between perfectionism and eating disorders?
Perfectionism can lead to unreasonable pressure to achieve the 'perfect body,' contributing to eating disorders.
What are the symptoms of insomnia disorder?
Chronic difficulties with sleep that cause significant personal distress and impaired functioning.
What is the significance of the hypocretin deficiency in narcolepsy?
It is associated with the most common type of narcolepsy and may indicate an autoimmune disease.
What are breathing-related sleep disorders?
Disruptions of sleep due to respiratory problems.
What is obstructive sleep apnea hypopnea syndrome?
A condition with repeated episodes of complete or partial obstruction of breathing during sleep.
What are common symptoms of obstructive sleep apnea?
Excessive daytime sleepiness and fatigue.
Which demographic is most affected by obstructive sleep apnea?
Middle-aged and older adults.
What is central sleep apnea?
A type of sleep apnea that may involve heart-related problems or chronic use of opioid drugs.
What is sleep-related hypoventilation?
A condition associated with lung disease or impaired lung function.
What is a sign of obstructive sleep apnea?
Loud snoring.
What is a circadian rhythm sleep-wake disorder?
Persistent disruptions of the natural sleep-wake cycle.
What can circadian rhythm sleep-wake disorders lead to?
Insomnia disorder or hypersomnolence.
What is non-24-hour circadian rhythm disorder?
A disorder that occurs in people who are totally blind, disrupting their circadian rhythm.
What causes non-24-hour circadian rhythm disorder in blind individuals?
Lack of light exposure to the retina, which prevents synchronization of the circadian rhythm.
What are parasomnias?
Sleep disorders involving abnormal behavior patterns associated with partial or incomplete arousals.
What are examples of parasomnias associated with non-REM sleep?
Sleep terrors and sleepwalking.
What characterizes sleep terrors?
Repeated episodes of terror-induced arousals that usually begin with a panicky scream.
What is sleepwalking?
Performing motor behavior while sleeping without conscious awareness.
What are examples of parasomnias associated with REM sleep?
Rapid eye movement sleep behavior disorder and nightmare disorder.
What is rapid eye movement sleep behavior disorder?
Acting out dreams during REM sleep due to incomplete muscle paralysis.
What is nightmare disorder?
Recurrent episodes of disturbing and well-remembered nightmares during REM sleep.
What are biological approaches to treating sleep disorders?
Sleep medications like antianxiety drugs and sleep-inducing agents.
What are some problems associated with sleep medications?
Suppression of REM sleep, rebound insomnia, chemical dependence, and psychological dependence.
What are cognitive-behavioral techniques for treating sleep disorders?
Techniques that focus on lowering physiological arousal and modifying maladaptive sleeping habits.
What is the goal of stimulus control in sleep therapy?
To create a stimulus environment associated with sleeping.
What sleep hygiene measures can improve sleep?
Avoiding eating, reading, or using electronic devices in bed.
What challenges do pregnant women face regarding sleep?
Increased sleep problems due to physical symptoms and emotional concerns.
What is a recommended sleep position for pregnant women in the third trimester?
Sleeping on the left side.
What factors contribute to sleep difficulties in menopausal women?
Hot flashes, sweating, and anxiety.
What medications have been shown to improve sleep in post-menopausal women?
Zolpidem (Ambien) and Eszopiclone (Lunesta).
What lifestyle changes can help reduce insomnia in menopausal women?
Stretching, morning exercise, and keeping the bedroom cool.