[9.1] Pediatric Nursing (Increased ICP, Seizure Disorder / Epilepsy, Bacterial Meningitis, Head Trauma, & Congenital Cardiovascular Disorders)
1/205
Earn XP
Description and Tags
From Sir Archie Alviz' Lecture Last August 11, 2025
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
206 Terms
Increased ICP
Seizure Disorder / Epilepsy
Bacterial Meningitis
Head Trauma
What are the discussed neurological disorders of the pedia?
5 to 15 mmHg
What is the normal range of ICP?
>20 mmHg
What ICP value is life-threatening?
Cushing’s Triad (HyperBradyBrady)
Hypertension
Bradycardia
Bradypnea
Triad to WOF in increased ICP and its components
b. Wide pulse pressure
Increased ICP
a. Narrow pulse pressure
b. Wide pulse pressure
30-40 mmHg
Normal range of pulse pressure
NO
Bulging fontanels
YES
NO
Increased HEAD circumference
YES
NO
Projectile Vomiting
NO
Diplopia
YES
NO
Sunset Eyes
YES
YES
Identify if the following is a s/sx of increased ICP (YES or NO):
Sunken fontanels
High-pitched cry
Increased chest circumference
Headache
Scant Vomiting
Nystagmus
Pupillary Changes
Sundowning
Anorexia, nausea, weight loss
Seizures
Crying
Comfort and properly timed feeding
Increased ICP (S/Sx): Bulging fontanels are aggravated by what? What should be done to avoid this?
a. Anterior Fontanel
Diamond
a. Anterior fontanel
b. Posterior fontanel
b. Posterior fontanel
Triangle
a. Anterior fontanel
b. Posterior fontanel
12 to 18 months
Increased ICP (S/Sx): When does the anterior fontanel close?
2-3 months
Increased ICP (S/Sx): When does the posterior fontanel close?
a. Anterior fontanel
Bigger
a. Anterior fontanel
b. Posterior fontanel
b. Posterior fontanel
Closes first
a. Anterior fontanel
b. Posterior fontanel
High-pitched cry
Increased ICP (S/Sx): Early sign of increased ICP
Headache
Sasakit muna ang ulo nila bago sila iiyak nang high pitched
Increased ICP (S/Sx): Earliest/Initial sign of increased ICP
High-pitched cry
Increased ICP (S/Sx): Irritable cry; shrill cry
High-pitched cry
Irritability and agitation
Restlessness
Confusion
What are the early signs of increased ICP in the following age group?
Infant
Child
Adult
Geria
Tape measure
Increased head circumference
Increased ICP (S/Sx): What should always be at the bedside (1) to measure this s/sx of increased ICP (2)?
Every shift of q8 hours
Increased ICP (S/Sx): How often should the head circumference of a pediatric patient be measured?
Compression of medulla → Compression of the CTZ (Chemoreceptor Trigger Zone) d/t Cerebral Edema
Increased ICP (S/Sx): Explain why there is projectile vomiting among pediatric patients with increased ICP.
Cerebral Edema
There is 80-95% chance that increased ICP or vomiting in increased ICP is caused by this.
Skull X-ray or CT Scan
How is Cerebral Edema diagnosed in the ED?
Diplopia
Increased ICP (S/Sx): Double Vision
Inc. ICP = Inc. IOP → Optic Nerve damage → Blurring of vision
→ Blindness (latter stages)
Increased ICP (S/Sx): Explain why there is diplopia in pediatric patients with increased ICP.
PERRLA (Pupils Equally Round and Reactive to Light and Accommodation)
Increased ICP (S/Sx): What is the normal reaction of the pupils?
TRUE
TRUE or FALSE: PERRLA implies that there should be consensual eye movement
Brain damage (Uneven pupil size)
Shock
Narcotic overdosage
Increased ICP (S/Sx): Identify the cause of the following pupillary changes
Anisocuria
Dilated pupils
Constricted pupils
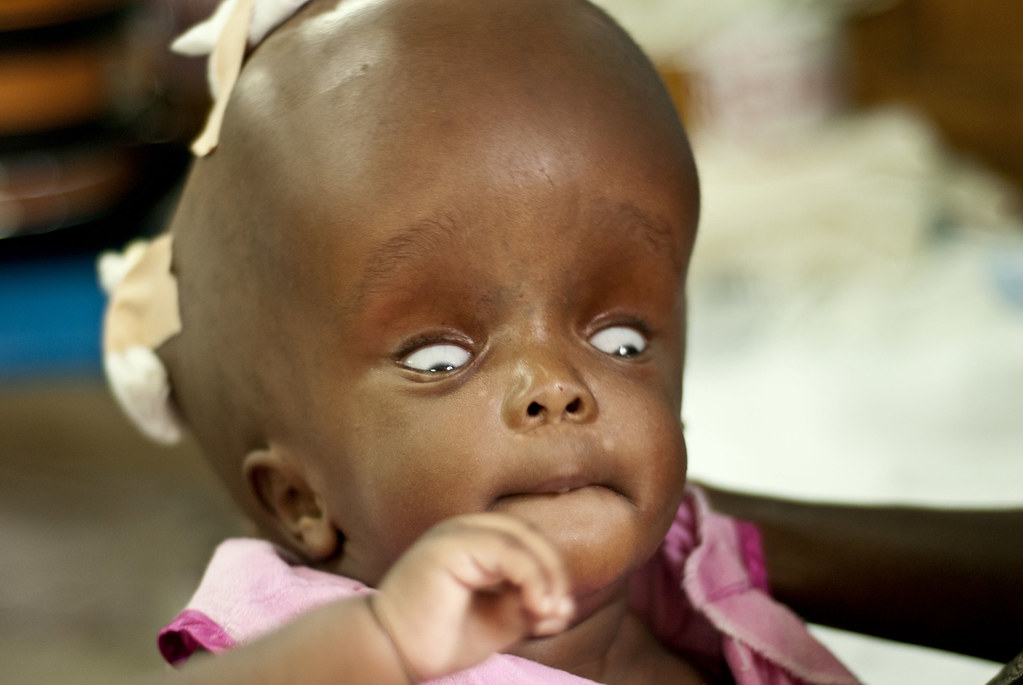
Sunset Eyes
Increased ICP (S/Sx): eyes are directed downward, with the iris covered by the lower eyelid
FALSE
You should still assess further
TRUE or FALSE: If the pediatric patient’s pupils are widely distributed to the whiter portion, this rules out increased ICP.
Weight / Weight Loss
Increased ICP (S/Sx): This is an important general indicator of health among pediatric patients
Increased neuronal firing
Vomiting
Increased ICP (S/Sx): What are the two main reasons for the seizure of the pediatric patients?
Increased neuronal firing → erratic transmission of electrical impulses → Seizures
Vomit → decreased fluid levels → DHN → Increased temperature → Convulsions → Seizures
Parang kotseng walang tubig, mag-ooverheat
Increased ICP (S/Sx): Explain the development of seizure based on its two main causes?
Semi-fowler’s (Dec ICP by the virtue of gravity)
Increased ICP: What should the patient’s position be?
Coughing and Sneezing
Increased ICP: What activities should be avoided?
1,200 - 1,500 mL/day
Increased ICP: How much fluid intake should be given?
FALSE
It could aggravate the ICP due to increased fluids
TRUE or FALSE: Since dehydration is a cause for seizure in increased ICP, then the OFI should also be increased.
1, 2, 4, 6, 9
Which of the following are included in the pharmacotherapy for increased ICP among pediatric patients?
Diuretics
Decadron
Hydrochlorothiazide
Anticonvulsants
Benzodiazepines
Antacids
PPIs
Antiplatelets
Anticoagulants
Beta Blockers
a. Lasix (Furosemide)
Increased ICP (Pharmacotherapy): Localized
a. Lasix (Furosemide)
b. Mannitol
b. Mannitol
Increased ICP (Pharmacotherapy): Generalized
a. Lasix (Furosemide)
b. Mannitol
Both a and b
Increased ICP (Pharmacotherapy): K Wasting
a. Lasix (Furosemide)
b. Mannitol
a. Lasix (Furosemide)
Increased ICP (Pharmacotherapy): Loop / Loop of Henle
a. Lasix (Furosemide)
b. Mannitol
b. Mannitol
Increased ICP (Pharmacotherapy): Osmotic
a. Lasix (Furosemide)
b. Mannitol
Decadron (Dexamethasone)
Increased ICP (Pharmacotherapy): Prevent Cerebral Edema
Anticonvulsants
Increased ICP (Pharmacotherapy): Prevent/minimize seizure episodes
Anticonvulsants
Increased ICP (Pharmacotherapy): Muscle relaxants
Antacids
Increased ICP (Pharmacotherapy): Neutralizes Acidity
Magnesium (Magtatae)
Increased ICP (Pharmacotherapy: Antacids): Side effect is diarrhea
Aluminum (Alang Tae)
Increased ICP (Pharmacotherapy: Antacids): Side effect is constipation
Increased ICP → Increased Stress → Increased HCL Production
Dexamethasone → Gastric irritation (stomach easily ulcerated)
Both causes increased acidity
Increased ICP (Pharmacotherapy): Why are antacids indicated?
Anticoagulants
Increased ICP (Pharmacotherapy): Prevents clumping of blood
IV/SQ (ptt)
Oral (pt)
Increased ICP (Pharmacotherapy): Identify the route of the following and the lab parameter that should be monitored
Heparin
Warfarin
Increased ICP → Increased BP in the brain → High risk for blood vessel injury → Clotting
Increased ICP (Pharmacotherapy): Why are anticoagulants indicated?
Opiates and Sedatives
Can cause cardiac and respiratory depression especially that RR and HR are down in the Cushing’s Triad
Increased ICP (Pharmacotherapy): What drugs are contraindicated? Why?
Seizure Disorder / Epilepsy
Caused by erratic transmission of electrical impulses
Grand Mal (Generalized)
Petit Mal / Absent
Jacksonian Seizure
Psychomotor
Febrile Seizure
Status Epilepticus
What are the types of Seizures?
Tonic-Clonic
Post-Ictal
Type of Seizure: What are the subtypes or parts of grand mal seizures?
a. Tonic
Type of Seizure (Grand Mal): Mild Contractions
a. Tonic
b. Clonic
b. Clonic
Type of Seizure (Grand Mal): Severe contractions
a. Tonic
b. Clonic
Supine/flat position and protect the head
During a seizure episode, the patient may experience d_______, s______, and u______. With that, what should be the position of the patient and what should you do?
Post-ictal
Type of Seizure (Grand mal): Exhaustion
Side-lying/Recovery to prevent aspiration
Type of Seizure: What should be the position during the post-ictal phase? Why?
Petit mal/Absent
Type of Seizure: Blank facial expression
Automatisms
Lip-smacking
Type of Seizure (Petit Mal/Absent): Repeated purposeless behavior in petit mal. What is the most common of these?
Jacksonian Seizure
Type of Seizure: Tonic-clonic of a group of muscle leading to grand mal
Psychomotor
Type of Seizure: Not common among pediatric patients; more common among adults.
Psychomotor
Type of Seizure: Mental clouding and intoxication
Psychomotor
Type of Seizure: Delirium, Hallucinations, and Delusions leading to seizure
Febrile Seizure
Hypothalamus not yet developed → Thermoregulation impaired → Temperature widely fluctuating
Type of Seizure: Common for those under 5.
Why is it so?
Febrile Seizures
Type of Seizure: Associated with high levels of temperature
38.5 deg. C to 39 deg. C to 40 deg. C
42 deg. C; Paracetamol RTC
Type of Seizure: What range of temperature often leads to febrile seizure?
What temperature leads to damage? What is the drug order for this?
Status Epilepticus
Type of Seizure: 30 minutes; Brain damage could occur
Medications
Surgery
Seizure Disorder: Main way to manage is through ______(1)______. If not effective, _____(2)_____.
1, 4, 5, 6
Seizure Disorder: Select all the medications indicated
Hydantoins
Antacids
Lithium
Benzodiazepines
Iminostilbenes
Valproates
Dexamethasone
Phenytoin
Gingival Hyperplasia
Seizure Disorder: What is the most popular hydantoin and what should you watch out for?
Pinkish-red
Seizure Disorder: What urine color is expected when the patient is taking phenytoin?
Benzodiazepines
Seizure Disorder: Minimizes seizure episodes (relaxants). Ends in -pam/-lam
Iminostilbenes
Seizure Disorder: Prevent seizure reoccurrence
Carbamazepine
Seizure Disorder: What are the common Iminostilbenes?
Refractory Seizure
Seizure Disorder: What do you call reoccuring seizures?
Valproates
Seizure Disorder: Last resort seizure medications for children
Valproic acid
Seizure Disorder: What is the most common valproate used?
Hepatotoxicity
Seizure Disorder: What is the side effect of valproic acid?
Can cause neural tube defects (NTDs) especially in 1st semester (Organogenesis)
Seizure Disorder: Why is valproic acid not given among pregnant patients?
Neurectomy
Seizure Disorder: What is the surgery of choice?
Cranial Nerve
Seizure Disorder: Neurectomy is the surgical resection of the _______ involved in the seizure
FALSE
This is considered the last resort because it can cause permanent damage/effects
TRUE or FALSE: Neurectomy is the 1st line of management for seizure disorders among pediatric patients to directly resolve the root cause and avoid future complications.
It depends on the assessment of the neurosurgeon
Seizure Disorder: What cranial nerve is resected in patients undergoing neurectomy?
Bacterial Meningitis
Bacterial infection of the meninges
b. Viral meningitis
Self-limiting; the patient can survive without any permanent effects
a. Bacterial meningitis
b. Viral meningitis
Lumbar Puncture
What is the main diagnostic tool for bacterial meningitis?
L3, L4, and L5
Bacterial Meningitis: What are the vertebrae or parts to be aspirated CSF from in lumbar puncture tests?
C-shape, fetal position, knee chest to access L3, L4, and L5
Bacterial Meningitis (Lumbar Puncture): What should be the position of the patient?
Genupectoral
What is knee-chest position also known as?
Clear
Bacterial Meningitis (Lumbar Puncture): What should be the normal result of a CSF analysis?
Cloudy
There is elevated WBC (to fight Bacteria)
There is elevated CHON (by-product or waste-product of bacteria)
Bacterial Meningitis (Lumbar Puncture): What should be expected of the CSF analysis if there is bacterial meningitis? Why?
Neisseria meningitidis
Bacterial Meningitis: What is the causative agent?
1, 2, 5, 7, 12
Bacterial Meningitis: Which of the following are signs and symptoms of bacterial meningitis?
Kernig’s Sign
Brudzinski’s Sign
Herman’s Sign
Cullen’s Sign
Nuchal Rigidity
Rovsing’s Sign
Seizures
Dunphy’s Sign
Blumberg Sign
Obturator sign
Psoas Sign
Opisthotonus
Torticolis
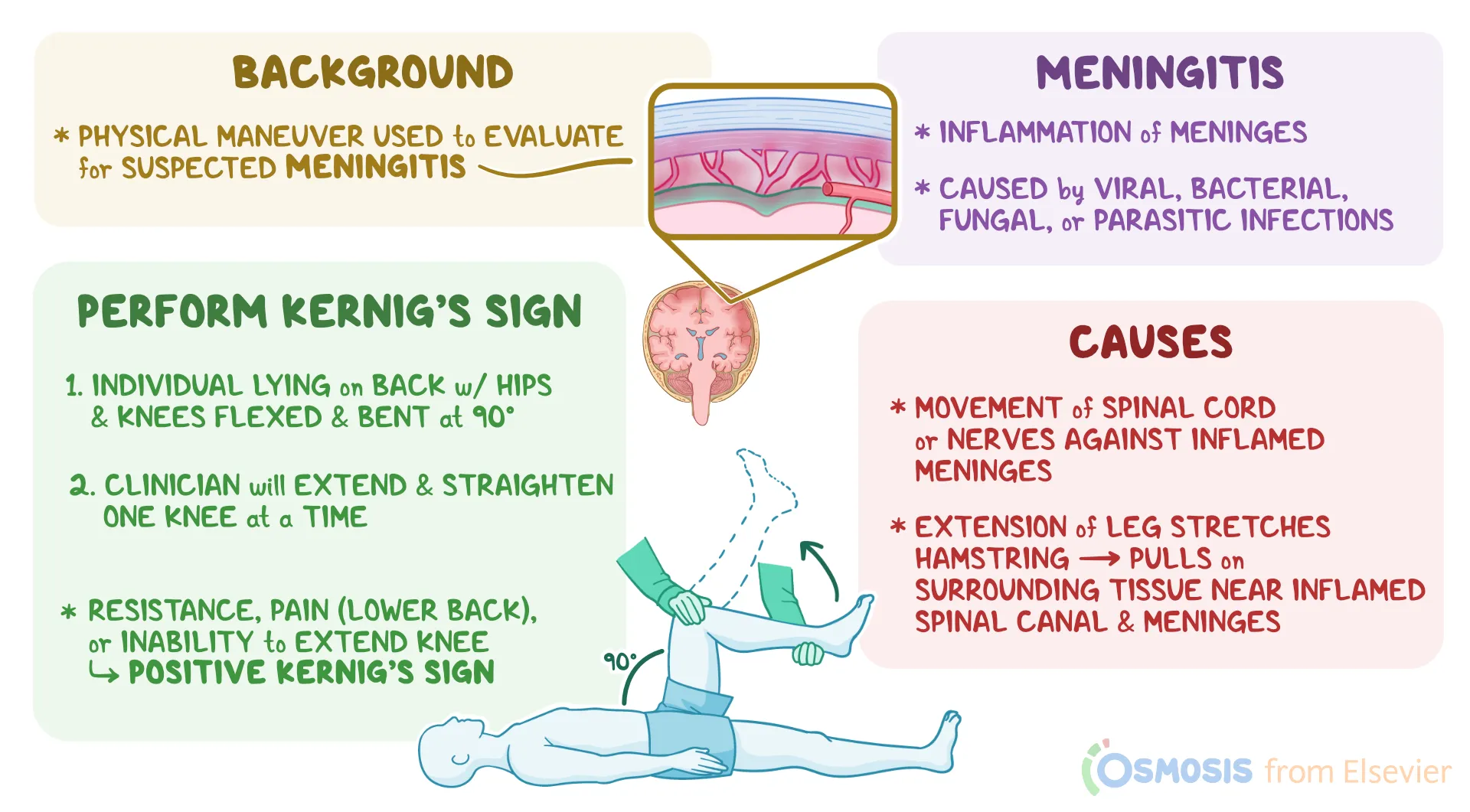
Pain in the hamstring, back, and neck
Bacterial Meningitis (Kernig’s sign): When you flex the knee, where should the pain be for it to be positive?
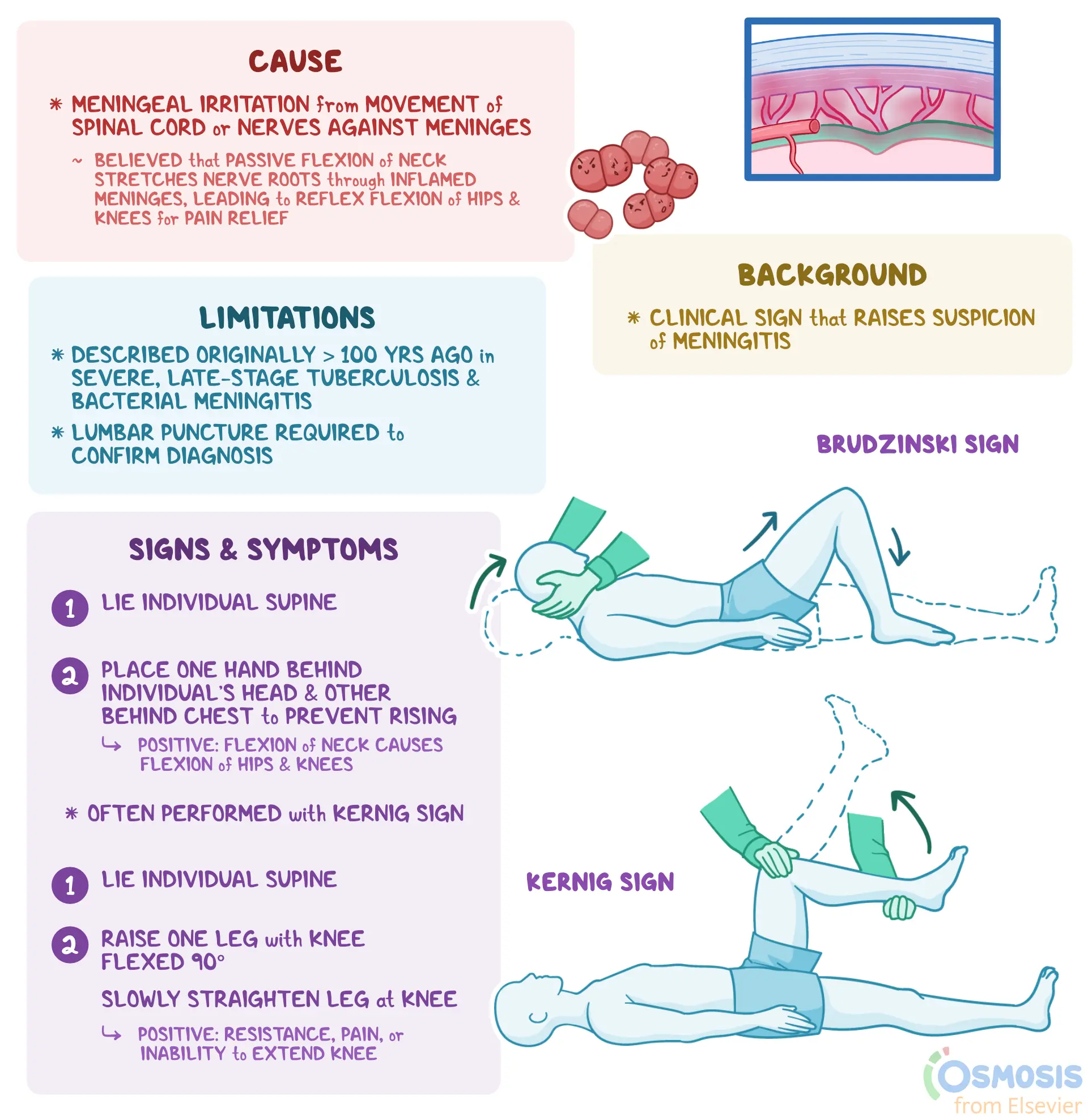
Pain in the neck and back
Bacterial Meningitis (Brudzinski’s sign): When you flex the nape, where should the pain be?