MCBL 121 final
1/147
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
148 Terms
Why might we use anti-viral treatments combining different targets of action?
Viruses can mutate rapidly to avoid the action of some drugs
How is the Baltimore classification system organized?
Virus replication mechanisms and genomes
You run an animal infection experiment with a mutant and wild-type pathogenic bacterium, mixed together and phenotypically tagged, in order to calculate a competitive index. The input ratio (mutant/wt) is 10/1 and the output ratio (mutant/wt) is 10/1. What can you conclude?
The two genotypes have similar fitness in the host
What is a primary function of antibodies?
opsonization- using opsonins to tag foreign pathogens for elimination by phagocytes
Which of the following accurately characterizes innate immunity?
active at birth
A phage genome integrated into the bacterial chromosome is known as a(n):
prophage
A culture of E coli does not exhibit visible turbidity after growth with antibiotic A at 100ug/ml, while a culture with 10ug/ml of antibiotic A shows about the same level of growth as a culture with no antibiotic. Which of the following statements best describes the MLC?
Not determinable with the given information
An operon contains 4 genes (in order: A, B, C, D). What best describes the effects of a missense mutation in B?
All genes are expressed
A bacterial surface protein that binds antibody Fc would inhibit which immune functions?
Neutralization
What is a measure for how easily pathogens can move from one human to another?
Infectivity
What does the viral capsid do?
packages viral genome and delivers it into the host cell
Envelope
encloses capsid, formed from cell membrane. contains glycoprotein spikes which are encoded by the virus
tegument proteins may be found between envelope and capsid
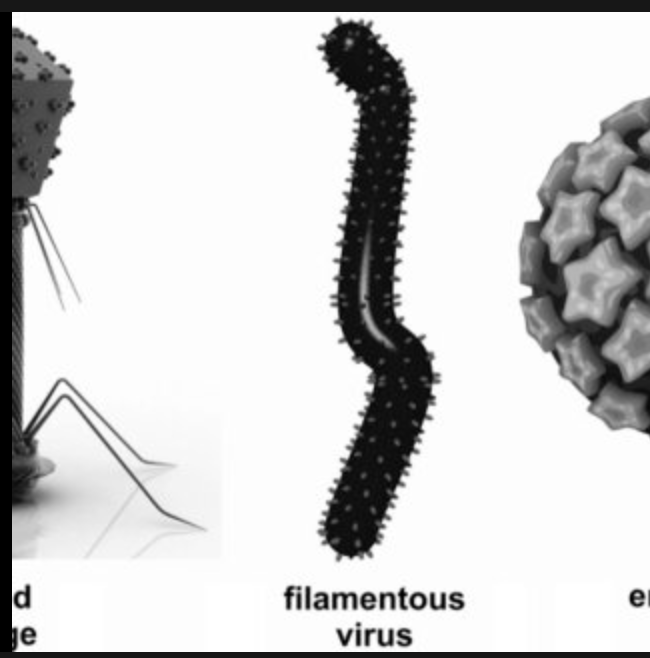
filamentous virus
capsid forms a long tube of protein with the virus coiled inside it; capsid monomers form a tube around genome, which usually winds helically w/in the tube
What are the seven groups of the Baltimore Classification?
I. dsDNA virus
II. ssDNA
III. dsRNA
IV. +ssRNA
V. -ssRNA
VI. RNA reverse transcribing viruses (w/ reverse transcriptase)
VII. DNA transcribing viruses (RNA intermediate)
Are bacteriophages enveloped?
No
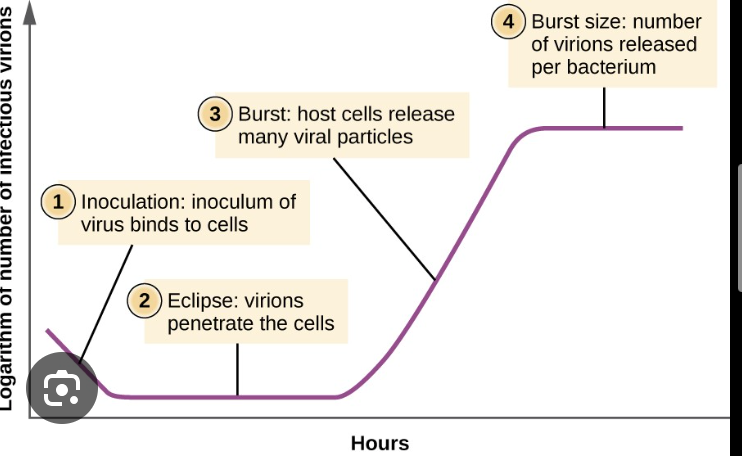
What are the different phases of the viral growth curve and what does each represent?
eclipse period: viruses bound to host cells, and are making proteins, genomes and assembling particles. No free virus can be detected
rise period: bacterial cell lysis. bacteriophage is making more copies of phages, virions bursting out of cell. A large amount of free packaged virus can be detected
curve plateaus when cell lysis is complete
Positive sense single-stranded RNA viruses can…
be directly translated into protein
Negative sense single-stranded RNA viruses….
are transcribed to mRNA and then translated into viral protein
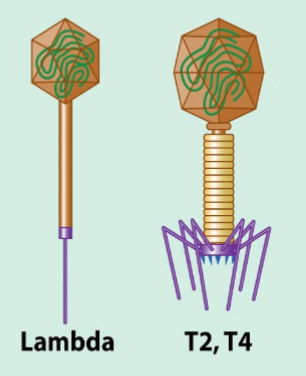
What are the two different types of viruses we discussed that infect E.coli & how do they differ?
T4 and lambda coliphages
T4- intemperate → lytic
lambda: temperate → lysogenic
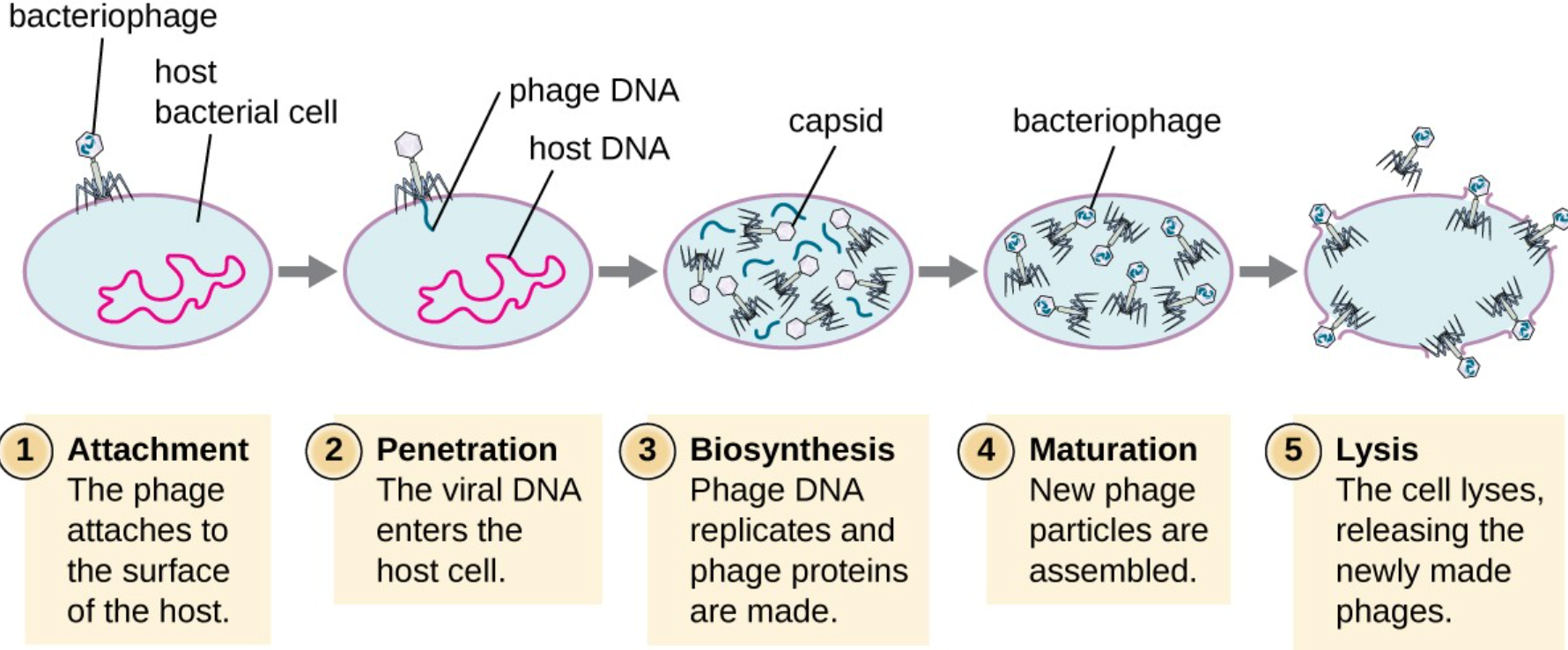
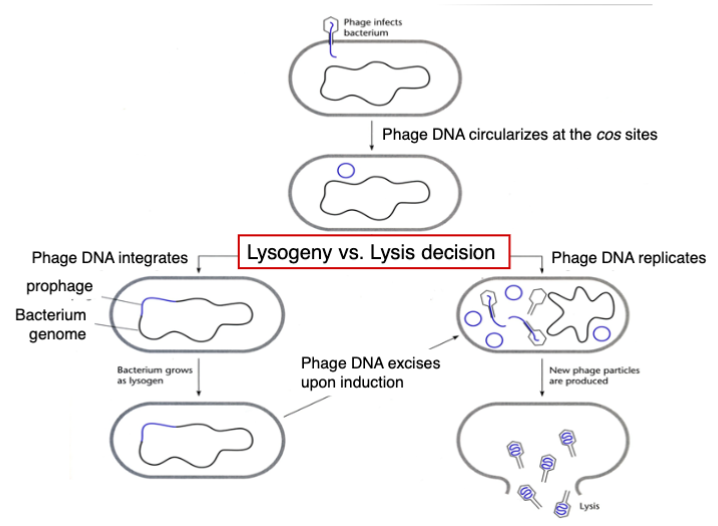
Lytic (intemperate) phages
phage infects bacterium
Phage DNA replicates & makes phage proteins
new phage particles are produced
cell lysis
Lysogenic (temperate) phages
maintain a stable relationship with the host cell in which they neither multiply nor are lost from the cell
integrate viral genome (prophage) into host DNA- cell is a lysogen
phage DNA excises upon induction (DNA damage to host cell) & new phage particles are produced
then cell lyses
What are the different forms of defense against bacteriophage infection?
genetic resistance
altered receptor proteins
restriction endonucleases
cleave viral DNA lacking methylation
CRISPR integration of phage DNA sequences
foreign DNA chewed up and integrated into the genome & can be transcribed, serves as a memory card; will use the sequence to guide trageted degradation of another copy of the viral genome in 2nd infection
What does it mean receptors determine tropism of the virus?
tropism of virus → what kind of cell a virus infects, different receptors of different cells (cellular tropism, tissue tropism, host tropism)
DNA viruses utilize what for replication?
host replication machinery
RNA viruses utilize what for their replication?
use an RNA-dependent RNA Polymerase to transcribe their mRNA
Retroviruses utilize what for their replication?
use reverse transcriptase to copy their genome sequence into DNA for insertion into the host genome
Coronavirus is what kind of virus?
positive sense ssRNA, binds to ACE2 receptor
What kind of virus is HIV?
retrovirus, attaches to CD4 receptor
uses reverse transcriptase and integrase to get DNA copy of genome & insert it into host DNA
Why is it useful that viruses are error-prone in their replication?
they can change their tropism by modification of their surface proteins
they can escape from host immune system
they can change the interaction with therapeutics by changing molecular targets; enzymes/drugs do not interact
How should viral treatments be made to lessen the likelihood of escape mutations?
make drugs that target multiple viral pathways (fusion, reverse transcription, receptor-binding, integration)
Highly Active Antiretroviral Therapy for HIV is an example
What is a plaque forming unit?
quantifies the number of viral particles capable of forming plaques in a viral culture, indicating viral infectivity.
1 plaque is formed from infection of 1 virion
PFU assay shows 100 plaques at 10-2 dilution, from 100ul plated
from the original phage mixture. What is the concentration of phages in the original sample in PFU/ml?
[(Plaque count) * (Dilution factor)] / volume mL = PFU / mL
100 plaques * 100(dilution factor)/0.1 mL= 100,000 pfu/mL
Infection
a pathogen grows & multiplies within or on another organism
infection does not always cause disease
infectious disease
due to presence and multiplication of pathogens, part of all of the host is not capable of performing its normal function
direct transmission
direct contact (touch) or aerosolization (sneeze)
indirect transmission
animal vectors of disease
zoonotic infection
disease spreads from animals → humans or vice versa
pneumonic plague
when Yersenia pestis travels to the lungs, spreads much easier than bubonic plague
What are the steps to infection?
Attach & invade host tissues
suppress host defenses
acquire nutrients from the hosts
propagate in the hosts
transmit to a new host
Pathogenicity
ability of organism to cause disease
infectivity
how easily pathogen spreads or causes infection
virulence
measure of degree/severity of a disease
What is ID50?
infectious dose; number of organisms to colonize 50% of hosts
lower ID50 → more infectious, higher ID50 → less infectious
What is LD50?
lethal dose; number of organism to kill 50% of hosts
lower LD50 → more virulent/pathogenic
What are the pitfalls of using ID50 & LD50?
Need a lot of animals
insensistive to attenuated (weakened) or low-pathogenicity
need to define measurements clearly (time points & sites)
virulence factor
individual characteristics of a pathogen that allow it to invade host and cause disease
all enhance the disease-producing ability of the pathogen
encoded by virulence genes, are highly regulated
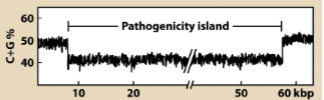
What are pathogenicity islands?
section of genome that contains multiple virulence genes that often encode related functions
often planked by a phage or plasmid genes
often have G-C content different from the rest of the genome
Koch’s Postulates for Pathogenesis
Suspect microbe is present in diseased tissues but absent from healthy tissues
Suspect microbe must be isolated and maintained in pure culture
Inoculation of the cultured microbe into a susceptible host should reproduce original symptoms
The same microbe must be isolated again from the inoculated diseased host
What do molecular Koch’s Postulates do?
they can assign role of a gene or gene product to pathogenesis
only relates to genes of a bacterium
involves mutagenesis and complementation
Complementation
restoration of mutated gene to original function
polar mutation
A mutation that affects the transcription or translation part of the gene or operon downstream of the mutant site.
If wild type phenotype is restored just by restoring the mutated gene, what does this mean?
no other genes are involved in the phenotype
How can we examine the effects of a mutation?
measure loss of pathogenicity, can do a competition assay
competition assay
based on a corrected ratio of strains after infection as a measure of pathogenicity/fitness in the host
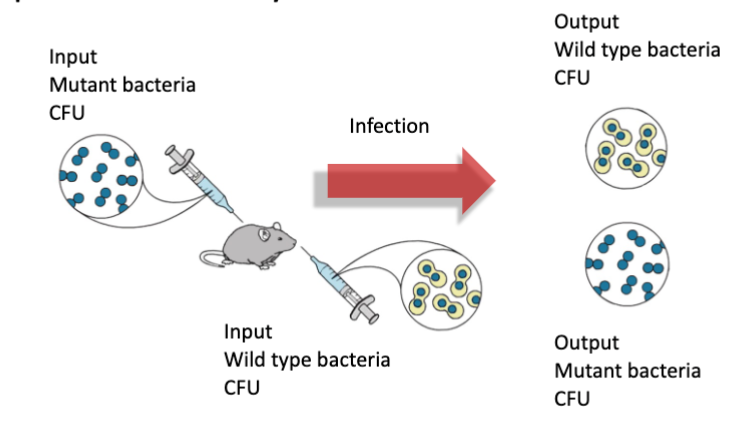
Competitive Index
indicates whether the mutant gene is a putative virulence factor
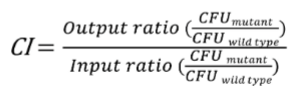
When CI equals 1…
WT and mutant grow equally; gene does not have anything to do with virulence
When CI < 1,….
WT outcompete mutant bacteria; the gene is important for virulence
When CI > 1,…
mutant outcompete WT bacteria; this gene suppresses virulence
What is the drawback of competition assay?
trans complementation of phenotype can occur, where WT bacteria can compensate for defects of the mutant and allow both to colonize
Why is our epithelium important?
it is the 1st barrier of defense against foreign objects and organisms
lines body cavities, blood vessels, & organs (mucosa)
secretes glycoproteins, secretes chemical antimicrobials, keep cell interface w/ environment clear of microbes, physical barrier, etc.
autoimmunity
The immune system mistakenly attacks healthy cells and tissues in the body, leading to chronic inflammation and tissue damage.
allergen
substance that induces immune response against otherwise harmless stimuli
antigen
substance that induces production of antibodies
intrinsic immunity
innate defense system of a cell that provides immediate protection against pathogens without prior exposure or activation of specific immune responses.
innate immunity
present at birth, limited diversity of responses, non-specific defense, no memory, fast responses, constant during response, uses phagocytes, uses pattern recognition receptors (PRRs) of microbes
adaptive/acquired immunity
acquired after contact with pathogen/antigen, includes a vast diversity of responses, is specific (antibodies), memory responses, slow responses, improves during response, uses T-cells & B-cells, generates antigen-specific antibody responses, and uses antigen-specific recognition
Pattern recognition receptors
proteins made by cells within the body that recognize pathogen-associated molecular patterns (PAMPs)
when PAMPs associate w/ PRRs → immune cells are activated and produce anti-microbial compounds to clear infection
what do phagocytes do?
they ingest foreign particles, microbes, or parts of dead or dying cells.
form acidified phagosomes, fuse w/ lysosome to form phagolysosome and enzymes digest foreign particles, then waste products are discharged
humoral immunity
involves antibodies produced by B cells to neutralize pathogens in body fluids, providing defense against bacteria, viruses, and toxins.
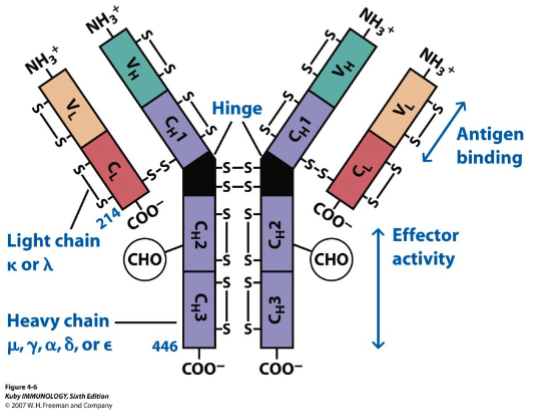
antibodies (immunoglobulins)
glycoproteins produced by B cells; identify and neutralize specific pathogens based on the antigens that are exposed by the host
What are the 2 major functions of antibodies?
opsonization- antibody coats bacteria & promotes phagocytosis
neutralization- preventing biological activity by binding Fc r
major histocompability complexes
cell surface proteins that present antigens to immune cells in immune synapse, crucial for immune response and self-recognition.
two-signal hypothesis
proposes that T cell activation requires two signals: antigen recognition by T cell receptor (Signal 1) and co-stimulation (Signal 2) for full activation.
What does triggering T-cell receptor alone lead to?
tolerant state (anergy)
T-cell
type of white blood cell that play a central role in the immune response, recognizing and destroying infected or abnormal cells.
How is complement/neutralization activated?
by binding to antibodies (in Fc region) that are bound to antigens (in Fab region), triggering a cascade of reactions to destroy or neutralize the invader (opsonization or membrane attack complex → cell lysis
What does activating complement do?
Activating complement enhances the immune response by promoting inflammation, opsonization, and cell lysis to eliminate pathogens.
How do vaccines work?
by stimulating the immune system to produce antibodies against pathogen-specific antigens, providing immunity by generating memory without causing the disease.
phase variation
a strategy used by bacteria to switch between different phenotypes (cell wall, capsule, external structures) by mutations, aiding in immune evasion and adaptation to changing environments.
What are the different ways in which bacteria can avoid being detected and killed by immune mechanisms?
phase variation
binding of host antibodies via Fc to prevent Fab binding & complement activation
degradation of antibody
formation of structures to prevent access to immune cells and components (biofilm, capsule)
go intracellular to avoid humoral immunity
kill host immune cells (via toxins)
Microbial toxins
products of pathogens that alter normal metabolism of the host
directly damage host cells
endotoxins: intrinsic to bacterial cell, but can enter bloodstream → sepsis
exotoxins: proteins secreted out of the pathogens
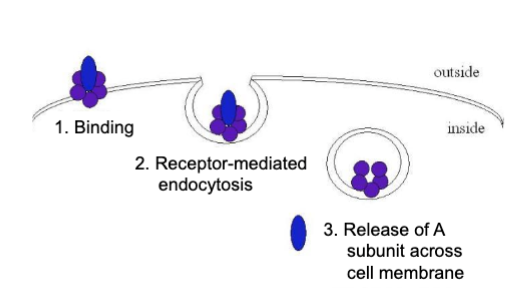
AB toxins
common structure of bacterial exotoxins- consist of two subunits - A is the active component causing harm, while B binds to target host cell receptors for entry.
How do you fulfill Molecular Koch’s Postulates?
need to manipuate presence of microbes in order to observe symptoms and transmission
inoculating microbe into susceptible host should produce same symptoms, need a good model of disease (animal)
What are characteristics of a good animal model of infection?
anatomical similarity, similar symptoms and courses of diseases, similar bacterial distribtuion, similar routes of transmission, similar immune system, inexpensive to obtain & maintain, no endangered species, & genetic modification available (?)
How can fermentation be used to preserve foods? How do fermentation products contribute to food production?
fermentation can produce products that inhibit microbial growth, by
pH changes (acid/base acts as an effective preservative), &
alcohols that act as detergents for growth inhibition
products of fermentation in food include: cheese, tempeh, miso, soy sauce, pickles, kimchi, natto, century eggs, chocolate, bread, beer, wine, etc.
What is the difference between food spoilage and food contamination?
food spoilage refers to microbial changes that renders a product unfit for consumption; food contamination is food poisoning, which contains human pathogens
What is the difference between rancidity and putrefaction?
rancidity: due to oxidation of fats
putrefaction: due to decomposition of proteins
What are some methods for preserving food from microbial breakdown?
eat it before it spoils
heat treatment
pasteurization
sterilization via heat
cooking
autoclave/UHF
remove liquid water (changing osmolarity)
freezing, drying, salting, jamming
radiation
organic acids
useful microbes in controlled fermentation
Biological Safety levels
BSL-1: safest (Saccharomyces cerevisiae) → BSL-4: most dangerous (extreme health risk to humans; Ebola)
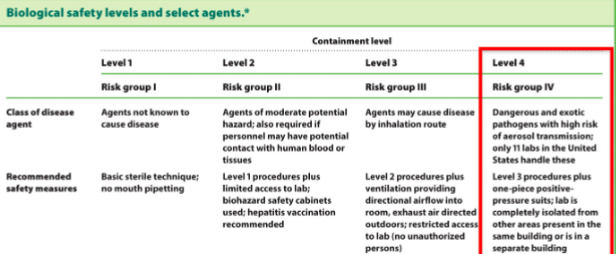
In which BSL are most microbes found in?
BSL-2
Garbage in garbage out (GIGO)
A concept emphasizing that flawed input results in flawed output.
samples must be collected aseptically
What are the different ways in which microbes can be identified?
by structure, by metabolism, using Triple Iron Sugar Agar, PCR, quantitative real time PCR, antibody binding (fluorescent antibody staining or ELISA), & point-of care tests
In Gram-staining procedure, gram positive & gram negative bacteria show up as what colors?
gram negative- pink
gram positive- purple/blue
Why is differential media helpful for identification (MacConkey Agar)?
strains grow, but differ in indicator color, helps to identify
Triple Iron Sugar (TSI) Agar
a differential medium used to differentiate bacteria based on their ability to ferment sugars and produce hydrogen sulfide gas
yellow @ acidic pH
red → purple @ alkaline pH or >
fermentation of lactose/sucrose → yellow
bacteria that cannot ferment break down proteins instead, raising pH → deep purple/red
How are TSI results evaluated?
Score is A (acid/yellow) or K (alkaline/red)
slant/butt tells us about aerobic v. anaerobic conditions
hydrogen sulfide gas produced or not (black precipitate)
gas produced can give cracks in the agar

restriction analysis
technique that uses restriction enzymes to cut DNA at specific sequences, helping to create a genetic fingerprint for identification purposes.
quantitative real time PCR
Quantitative real-time PCR measures DNA amplification during each cycle, providing accurate quantification of initial DNA template.
utilizes reverse transcriptase to generate complementary DNA from RNA templates
involves measurement of fluorescence that increases with target copy number
either using TaqMan (custom, specific probe) or SYBR (more amplicon → more signal)
Which region of antibody binds antigen?
Fab region, Fc is constant region