Bio 240W Exam 3
5.0(1)
Card Sorting
1/61
Earn XP
Description and Tags
Study Analytics
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
62 Terms
1
New cards
Define water potential and explain how it is influenced by solutes, pressure, and gravity
* Water potential is the water’s capacity to perform work.
* Water flows from regions of higher water potential to regions of lower water potential
* Adding solute causes water to diffuse to the place with the solute
* Adding positive pressure causes the water to move away from the pressure
* Adding negative pressure causes the water to move toward the pressure
* Overall, water moves from an area of high water potential to low water potential
* Water flows from regions of higher water potential to regions of lower water potential
* Adding solute causes water to diffuse to the place with the solute
* Adding positive pressure causes the water to move away from the pressure
* Adding negative pressure causes the water to move toward the pressure
* Overall, water moves from an area of high water potential to low water potential
2
New cards
Describe how water potential, evapotranspiration, and stomatal regulation influence how water is transported in plants
* Evapotranspiration- the loss of water from the plant through evaporation at the leaf surface
* Creates a negative pressure at the leaf surface (water potential)
* Pulls water from the roots up towards the leaf
* Happens during the day when the stomata are open, at night the stomata close and transpiration stops.
* Stomata are open when there is a K+ influx, closed when the K+ is moving out
* Creates a negative pressure at the leaf surface (water potential)
* Pulls water from the roots up towards the leaf
* Happens during the day when the stomata are open, at night the stomata close and transpiration stops.
* Stomata are open when there is a K+ influx, closed when the K+ is moving out
3
New cards
Explain how photosynthates are transported in plants
In the phloem
* need a pressure difference, and its caused by high sucrose concentrations at source
* using Active transport, move sucrose against its concentration gradient from source to phloem
* Water moves in from xylem to reduce water potential
* generates positive pressure to move sucrose down the phloem
* unloads sucrose into the sink and relieves pressure
In xylem
* Water is pushed back into xylem from phloem
* transpiration occurs to push water along potential gradient to top of xylem
* need a pressure difference, and its caused by high sucrose concentrations at source
* using Active transport, move sucrose against its concentration gradient from source to phloem
* Water moves in from xylem to reduce water potential
* generates positive pressure to move sucrose down the phloem
* unloads sucrose into the sink and relieves pressure
In xylem
* Water is pushed back into xylem from phloem
* transpiration occurs to push water along potential gradient to top of xylem
4
New cards
Plants do not have a circulatory system like that of some animals. If a water molecule in a plant did "circulate" **it would require…**
both the xylem and the phloem
5
New cards
Plants need to **control stomatal opening** primarily so they can…
prevent water from leaving the cell, allow oxygen to leave, and allow CO2 into the cell
6
New cards
**Most of the water** taken up by a plant is...
lost through transpiration (90%)
7
New cards
The **opening** of stomata is thought to involve...
movement of K+ into the guard cells, an increase in turgor pressure in guard cells, and movement of water into guard cells
8
New cards
For sucrose to be moved from a leaf (source) cell to a root (sink) cell, **sucrose is first actively transported into the phloem** from the source cell. **What happens next?**
Water diffuses from the xylem to the phloem
9
New cards
Describe the mechanisms of inspiration including the muscles used and changes in pressure gradients
* Inhaling
* Diaphragm contracts (moves down)
* Rib cage expands
* Rib muscles contract
* more volume, less pressure
* Diaphragm contracts (moves down)
* Rib cage expands
* Rib muscles contract
* more volume, less pressure
10
New cards
Describe the mechanisms of expiration including the muscles used and changes in pressure gradients
* Exhaling
* Diaphragm relaxes (moves up)
* Rib cage gets smaller
* Rib muscles relax
* volume decreases, pressure increases
* Diaphragm relaxes (moves up)
* Rib cage gets smaller
* Rib muscles relax
* volume decreases, pressure increases
11
New cards
Describe how gas exchange occurs in the alveoli of the lungs and in the body cells
* Air enters alveoli (have a large surface area)
* Gases equilibrate with gasses of blood in capillaries
* Gases move down their pressure gradients via diffusion
* This is a similar process for capillaries and body cells
* Gases equilibrate with gasses of blood in capillaries
* Gases move down their pressure gradients via diffusion
* This is a similar process for capillaries and body cells
12
New cards
Contrast hemoglobin and myoglobin
* both protein + iron
* increases the amount of oxygen in the blood and body tissues
\
Hemoglobin
* in almost all vertebrates and many invertebrates
* oxygen is bound to it in red blood cells
\
Myoglobin
* found in muscle cells
* increases the amount of oxygen in the blood and body tissues
\
Hemoglobin
* in almost all vertebrates and many invertebrates
* oxygen is bound to it in red blood cells
\
Myoglobin
* found in muscle cells
13
New cards
Explain how oxygen and carbon dioxide are transported in the blood
Oxygen transport
\-98% bound to **hemoglobin** in red blood cells
\-2% dissolved in blood plasma
\-high pressure in alveoli, low in body cells, so oxygen goes into body cells
\
CO2 transport
\-10% dissolved in blood plasma
\-20% bound to hemoglobin
\-70% in the form of **Plasma bicarbonate**
* More important in determining the respiratory rate
\-high pressure in body cells, lower in alveoli, so co2 goes into alveoli
\-98% bound to **hemoglobin** in red blood cells
\-2% dissolved in blood plasma
\-high pressure in alveoli, low in body cells, so oxygen goes into body cells
\
CO2 transport
\-10% dissolved in blood plasma
\-20% bound to hemoglobin
\-70% in the form of **Plasma bicarbonate**
* More important in determining the respiratory rate
\-high pressure in body cells, lower in alveoli, so co2 goes into alveoli
14
New cards
Describe how the carbonic acid equation is related to blood pH
\-Putting Co2 into the body cells decreases pH by increasing the amount of H+ in the cells.
\-Decreasing CO2 in the body cells would increase pH because we decrease the H+ ions
\-Decreasing CO2 in the body cells would increase pH because we decrease the H+ ions
15
New cards
Describe the factors that affect oxygen loading and unloading from hemoglobin
O2 pressure
\-O2 saturation increases as the partial pressure of O2 increases
\-starts to level off and plateau as partial pressure of O2 increases
\
pH differences
\-hemoglobin retains less O2 at lower pH
\-lower pH has a higher CO2 concentration
\-O2 saturation increases as the partial pressure of O2 increases
\-starts to level off and plateau as partial pressure of O2 increases
\
pH differences
\-hemoglobin retains less O2 at lower pH
\-lower pH has a higher CO2 concentration
16
New cards
Explain the Bohr effect
* Arises from the relationship between pH and oxygen’s affinity for hemoglobin
* A lower pH promotes oxygen dissociation from hemoglobin.
* A higher pH inhibits oxygen dissociation from hemoglobin.
* The greater the amount of carbon dioxide in the blood, generates hydrogen ions and lowers blood pH.
* blood pH may decrease when certain byproducts of cell metabolism, such as lactic acid, carbonic acid, and carbon dioxide, are in the bloodstream.
* A lower pH promotes oxygen dissociation from hemoglobin.
* A higher pH inhibits oxygen dissociation from hemoglobin.
* The greater the amount of carbon dioxide in the blood, generates hydrogen ions and lowers blood pH.
* blood pH may decrease when certain byproducts of cell metabolism, such as lactic acid, carbonic acid, and carbon dioxide, are in the bloodstream.
17
New cards
Analyze how changes in carbon dioxide levels alter pH (based on protons and the carbonic acid equation)
\-CO2 increase, decreases pH by increasing H+ ions
\-CO2 decrease, increases pH by decreasing H+ ions
\-CO2 decrease, increases pH by decreasing H+ ions
18
New cards
Describe the different components of the neural circuit that helps to regulate respiratory rate
* afferent (sensory) neurons, interneurons, and efferent (motor) neurons
* afferent neurons conduct signals from receptors to CNS
* interneruons are confined to the CNS
* efferent neurons conduct signals from CNS to effectors such as muscles and glands
* afferent neurons conduct signals from receptors to CNS
* interneruons are confined to the CNS
* efferent neurons conduct signals from CNS to effectors such as muscles and glands
19
New cards
Explain how the respiratory system works with the cardiovascular system to help regulate pH
\-When the pH is too low, the chemoreceptors signal the respiratory system to increase ventilation and remove carbon dioxide.
\-The chemoreceptors initiate the contraction of the diaphragm and intercostal muscles.
\-High pH leads to a decrease in breathing rate
\-The chemoreceptors initiate the contraction of the diaphragm and intercostal muscles.
\-High pH leads to a decrease in breathing rate
20
New cards
Explain the importance of carbon dioxide in determining breathing rate
\-Carbon dioxide levels increase H+ ions which decreases pH
\-If pH is too low chemoreceptors cause breathing to quicken and get rid of the carbon dioxide faster
\-If pH is too low chemoreceptors cause breathing to quicken and get rid of the carbon dioxide faster
21
New cards
Contraction of intercostal muscles causes which of the following to occur?
A) The diaphragm moves downward
B) the rib cage is compressed
C) The thoracic cavity volume decreases
D) The rib cage expands
A) The diaphragm moves downward
B) the rib cage is compressed
C) The thoracic cavity volume decreases
D) The rib cage expands
D) The rib cage expands
22
New cards
The partial pressure of carbon dioxide is 46 mm Hg in the blood and 40 mm Hg in the alveoli. What happens to the carbon dioxide?
It diffuses into the alveoli
23
New cards
Describe the structure of a neuron and how it relates to its function.
\-Cell body (soma)- keeps cell functional
\-Cell membrane- protects the cell
\-Axon- passes signal away from neuron to cell body, other neurons, muscles, or glands
\-Dendrites- receives messages from other cells
\-Myelin sheath- covers axon and helps speed neural impulses
\-Synapse- allows neurons to communicate with each other
\-Cell membrane- protects the cell
\-Axon- passes signal away from neuron to cell body, other neurons, muscles, or glands
\-Dendrites- receives messages from other cells
\-Myelin sheath- covers axon and helps speed neural impulses
\-Synapse- allows neurons to communicate with each other
24
New cards
Compare and contrast a current and a potential
\-A **current** is the flow of charged particles from one point to another
\-A current requires an electrical **potential**
* Potential is a concentration gradient of charged particles/difference in charge
* Potential of charged particles is called an electrochemical gradient
\-A current requires an electrical **potential**
* Potential is a concentration gradient of charged particles/difference in charge
* Potential of charged particles is called an electrochemical gradient
25
New cards
Describe the two components of an electrochemical gradient
Chemical gradient- uneven distribution of **molecules**
Electrical gradient- uneven distribution of **charge** (because these molecules are ions)
Electrical gradient- uneven distribution of **charge** (because these molecules are ions)
26
New cards
Explain in your own words the importance of an electrochemical gradient (in this case, the resting membrane potential, RMP) to neuron function.
* electrochemical gradient generates energy that is especially important in establishing and maintaining the membrane potential of neurons and pH homeostasis within the cytosol of the cell
* also allows the cells to communicate with each other and respond to signals quickly.
* also allows the cells to communicate with each other and respond to signals quickly.
27
New cards
Describe how the sodium/potassium pump and leak channels contribute to the negative RMP of neurons.
* A neuron’s RMP inside of a cell is approximately 70 mV more negative than the outside
* caused by differences in the concentrations of ions inside and outside the cell and the selective permeability created by ion channels.
* Sodium-potassium pumps in the membrane produce the different ion concentrations
* bring in two K+ ions and remove three Na+ ions.
* Potassium ions (K+), higher inside the cell, can move out of the neuron through potassium leak channels
* this loss of positive charge produces a net negative charge inside the cell.
* Sodium ions (Na+), low inside cell, have a driving force to enter the neuron but there are many fewer sodium leak channels.
* Their channels are voltage-dependent and open when there is a slight change in the membrane potential
* caused by differences in the concentrations of ions inside and outside the cell and the selective permeability created by ion channels.
* Sodium-potassium pumps in the membrane produce the different ion concentrations
* bring in two K+ ions and remove three Na+ ions.
* Potassium ions (K+), higher inside the cell, can move out of the neuron through potassium leak channels
* this loss of positive charge produces a net negative charge inside the cell.
* Sodium ions (Na+), low inside cell, have a driving force to enter the neuron but there are many fewer sodium leak channels.
* Their channels are voltage-dependent and open when there is a slight change in the membrane potential
28
New cards
Identify the parts of a generic neural circuit and their relationship to the structure of the nervous system.
Sensory input (afferent neurons) (PNS)
* receptors respond to external/internal stimuli
* relay message to brain and spinal cord
Integration (interneurons) (CNS)
* brain, spinal cord integrate data and send back out nerve impulses
Motor output (efferent neurons) (PNS)
* impulses go to effectors-muscles and glands
* receptors respond to external/internal stimuli
* relay message to brain and spinal cord
Integration (interneurons) (CNS)
* brain, spinal cord integrate data and send back out nerve impulses
Motor output (efferent neurons) (PNS)
* impulses go to effectors-muscles and glands
29
New cards
Identify the different part of neurons and how they help the cells function in a circuit.
\-Axon- passes signal away from neuron to cell body, other neurons, muscles, or glands
\-Dendrites- receives messages from other cells
\-Myelin sheath- covers axon and helps speed neural impulses
\-Synapse- allows neurons to communicate with each other
\
Synapse attaches to dendrites and allows messages from one neuron to another. Axon and myelin sheath sends the message from one to another very quickly with action potential
\-Dendrites- receives messages from other cells
\-Myelin sheath- covers axon and helps speed neural impulses
\-Synapse- allows neurons to communicate with each other
\
Synapse attaches to dendrites and allows messages from one neuron to another. Axon and myelin sheath sends the message from one to another very quickly with action potential
30
New cards
Compare and contrast the types of gated ion channels
Mechanically gated ion channels
* change occurs in the surrounding tissue, such as pressure or touch, the channel is physically opened
* Thermoreceptors work on a similar principle
* When local tissue temperature changes, the protein reacts by physically/mechanically opening the channel
\
Ligand-gated ion channels
* Ion channels that change structure in response to a chemical (ligand) binding to a receptor
* typical ligands include neurotransmitters
\
Voltage-gated ion channels
* ion channels that change their structure in response to voltage changes
* Structural changes in protein channel allow or prevent ion movement
* change occurs in the surrounding tissue, such as pressure or touch, the channel is physically opened
* Thermoreceptors work on a similar principle
* When local tissue temperature changes, the protein reacts by physically/mechanically opening the channel
\
Ligand-gated ion channels
* Ion channels that change structure in response to a chemical (ligand) binding to a receptor
* typical ligands include neurotransmitters
\
Voltage-gated ion channels
* ion channels that change their structure in response to voltage changes
* Structural changes in protein channel allow or prevent ion movement
31
New cards
Define depolarization, repolarization, and hyperpolarization and how they relate to sodium vs. potassium gated channels.
Depolarized- becoming less negative
* opening of Voltage-gated Na+ channels after threshold is reached
* letting Na+ in to cell
* inside becomes more positive
Repolarize- becoming more negative till the threshold
* Na+ channels close
* K+ channels open and K+ leaves the cell
* inside becomes less positive
hyperpolarize- becoimg more negative past the threshold
* K+ channels stay open longer to allow more K+ to diffuse out of the cell
* inside becomes even less positive
* opening of Voltage-gated Na+ channels after threshold is reached
* letting Na+ in to cell
* inside becomes more positive
Repolarize- becoming more negative till the threshold
* Na+ channels close
* K+ channels open and K+ leaves the cell
* inside becomes less positive
hyperpolarize- becoimg more negative past the threshold
* K+ channels stay open longer to allow more K+ to diffuse out of the cell
* inside becomes even less positive
32
New cards
Describe how local potentials are initiated using ligand-gated channels
* neurotransmitter binds to ligand-gated Na+ channel on postsynaptic neuron
* Local potential in cell body reaches threshold (-55mV)
* Neuron “fires” or starts an action potential
* Na+ starts to enter the cells
* Local potential in cell body reaches threshold (-55mV)
* Neuron “fires” or starts an action potential
* Na+ starts to enter the cells
33
New cards
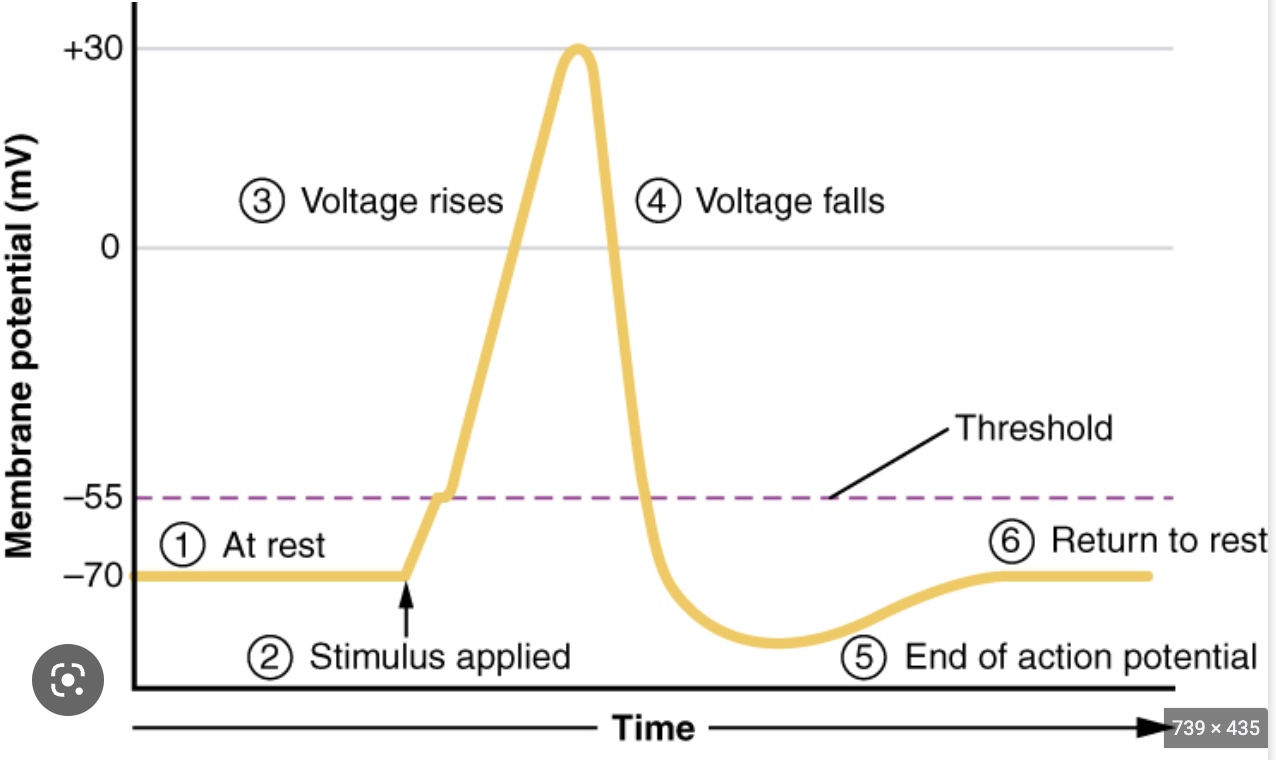
Draw and label all steps of an action potential including the ion channels being used at each step
1. at resting membrane potential of -70 mV
\
2) Presynaptic neuron releases a neurotransmitter that binds to the ligand-gated Na+ channel on the postsynaptic neuron. Na+ enters the postsynaptic neuron cell body. If enough Na+ enters, then the postsynaptic neuron will be depolarized to its threshold voltage.
\
3) Voltage-gated Na+ channels open and allow Na+ into the cell. voltage becomes less negative
\
4) Membrane potential reaches 30 mV, which is peak depolarization. Na+ channels close, and voltage-gated K+ channels open to let K+ out of the cell. Inside becomes more negative. Repolarization and hyperpolarization
\
5) Sodium/potassium pumps actively transport ions back to their original state. Membrane at resting potential and ready to receive next signal
34
New cards
Explain why an action potential can only travel AWAY from a cell body
* Sodium channels can’t open again after a certain period so it ensures the signal can only move in one direction
* “all or nothing" once it depolarizes and reaches the threshold of the action potential
* “all or nothing" once it depolarizes and reaches the threshold of the action potential
35
New cards
Explain the process of secretion and describe the role of vesicles in secretion.
Secretion is the process of converting the electrical signal of the presynaptic neuron to a chemical signal in the synapse and then back to an electrical signal in the postsynaptic neuron.
\-neuron to neuron or neuron to muscle cells
* The presynaptic neuron synthesizes and packages the neurotransmitter in synaptic vesicles located in the synaptic terminal
* The action potential causes the release of the neurotransmitter
* The neurotransmitter diffuses across the synaptic cleft and is received by the postsynaptic cell
\-neuron to neuron or neuron to muscle cells
* The presynaptic neuron synthesizes and packages the neurotransmitter in synaptic vesicles located in the synaptic terminal
* The action potential causes the release of the neurotransmitter
* The neurotransmitter diffuses across the synaptic cleft and is received by the postsynaptic cell
36
New cards
Describe the components of the autonomic nervous system
Sympathetic- fight or flight
Parasympathetic- rest and digest
Parasympathetic- rest and digest
37
New cards
Differentiate between the sympathetic and parasympathetic divisions in the autonomic nervous system
Sympathetic—arouses body for “fight or flight”
* Neurotransmitter released by sympathetic neurons is norepinephrine (similar to adrenaline)
* cardioacceleratory centers
* post-absorptive state- glucagon, epinephrine, norepinephrine
\
Parasympathetic—predominates during relaxation, “rest and digest”
* Neurotransmitter is acetylcholine—the same neurotransmitter used at the neuromuscular junction
* cardioinhibitory centers
* absorptive state- insulin
* Neurotransmitter released by sympathetic neurons is norepinephrine (similar to adrenaline)
* cardioacceleratory centers
* post-absorptive state- glucagon, epinephrine, norepinephrine
\
Parasympathetic—predominates during relaxation, “rest and digest”
* Neurotransmitter is acetylcholine—the same neurotransmitter used at the neuromuscular junction
* cardioinhibitory centers
* absorptive state- insulin
38
New cards
Contraction of the **intercostal muscles** causes which of the following to occur?
A) The diaphragm moves downward.
B) The rib cage is compressed.
C) The thoracic cavity volume decreases.
D) The ribs and sternum move upward.
A) The diaphragm moves downward.
B) The rib cage is compressed.
C) The thoracic cavity volume decreases.
D) The ribs and sternum move upward.
D) The ribs and sternum move upward.
39
New cards
If the **pH of the blood has decreased**, this means that the ________.
A) amount of carbon dioxide has increased
B) amount of bicarbonate in the blood is unchanged
C) amount of oxygen in the blood has decreased
\
D) amount of protons in the blood has decreased
A) amount of carbon dioxide has increased
B) amount of bicarbonate in the blood is unchanged
C) amount of oxygen in the blood has decreased
\
D) amount of protons in the blood has decreased
A) amount of carbon dioxide has increased
40
New cards
During most daily activities, the human **respiration rate** is most closely **linked to the blood levels** of ________.
\
\
carbon dioxide
41
New cards
Which of the following events would you predict as **carbon dioxide** is released **from your muscles into the surrounding capillary bed?**
Oxygen delivery to muscle is increased when more carbon dioxide is produced by the muscle.
42
New cards
The partial pressure of carbon dioxide is 45 mm Hg in the **blood** and 40 mm Hg in the **alveoli**.
* **What happens to the carbon dioxide?**
* **What happens to the carbon dioxide?**
It diffuses into the alveoli.
43
New cards
**Oxygen** saturation (loading/unloading) of **hemoglobin** depends on.
Oxygen pressure differences in the tissues
and pH differences in the blood
and pH differences in the blood
44
New cards
The **sensory (afferent) and motor (efferent)** divisions are part of the...
the peripheral nervous system
45
New cards
The region of the neuron that carries **the nerve impulse away from the cell body** is called the...
axon
46
New cards
For a neuron at **resting membrane potential**…
a higher concentration of potassium ions is found inside the membrane
a higher concentration of sodium ions is found outside the membrane
a higher concentration of sodium ions is found outside the membrane
47
New cards
The **"threshold" potential** of a membrane is the…
minimum depolarization needed to operate the voltage-gated sodium and potassium channels.
48
New cards
Why does **hyperpolarization of the neuron membrane** occur?
The potassium channels close more slowly, allowing more potassium to flow from inside to outside the membrane.
49
New cards
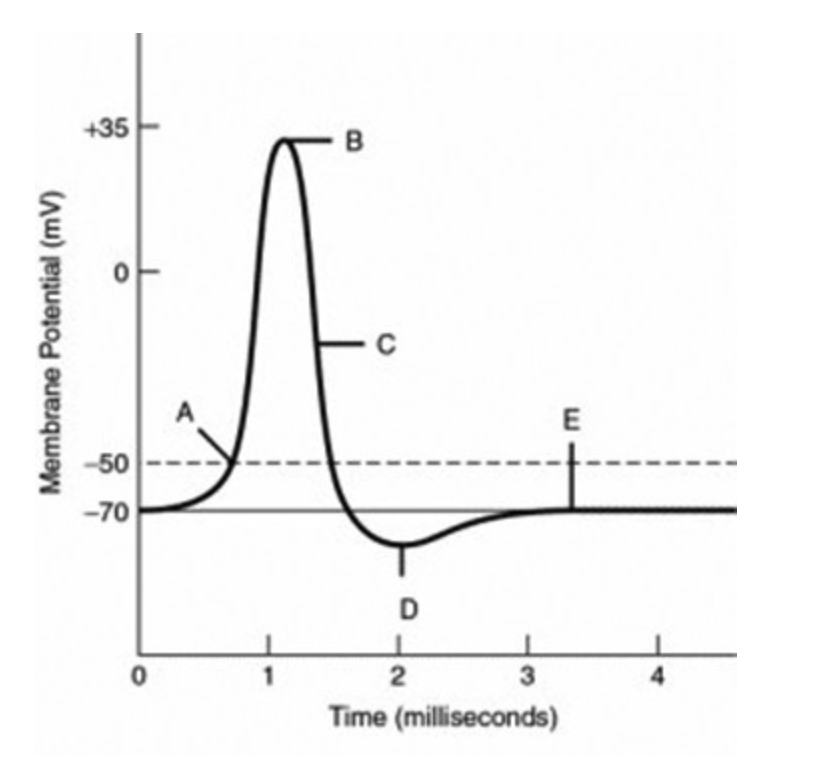
The minimum **local/threshold** depolarization needed to operate the voltage-gated sodium and potassium channels is **indicated by the label ________**.
A
50
New cards
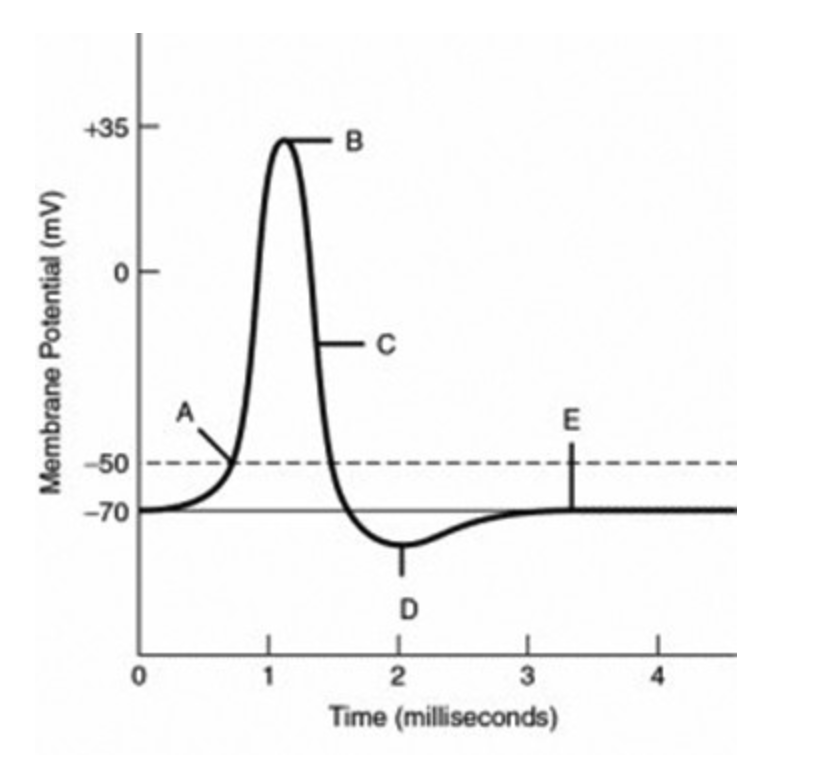
The neuronal membrane is at its **resting membrane potential at label ________.**
E
51
New cards
If you wanted to **inhibit a signal from propagating along the axon**, which of the following **ion channels would you want to ONLY open**?
potassium
52
New cards
The following steps refer to various stages in **transmission of the signal at a chemical synapse.**
Put them in order
1. Neurotransmitter binds with receptors associated with the postsynaptic membrane.
2. Calcium ions rush into neuron's cytoplasm.
3. An action potential depolarizes the membrane of the presynaptic axon terminal.
4. The ligand-gated ion channels open.
5. The synaptic vesicles release neurotransmitter into the synaptic cleft.
Put them in order
1. Neurotransmitter binds with receptors associated with the postsynaptic membrane.
2. Calcium ions rush into neuron's cytoplasm.
3. An action potential depolarizes the membrane of the presynaptic axon terminal.
4. The ligand-gated ion channels open.
5. The synaptic vesicles release neurotransmitter into the synaptic cleft.
3→2→5→1→4
53
New cards
Which **cardio center in the brain** is paired with the correct division of the **autonomic nervous system transmitting that signal to the heart**?
A) cardioacceleratory center : parasympathetic system
B) cardioacceleratory center : sympathetic system
C) cardioinhibitory center : sympathetic system
A) cardioacceleratory center : parasympathetic system
B) cardioacceleratory center : sympathetic system
C) cardioinhibitory center : sympathetic system
B) cardioacceleratory center : sympathetic system
54
New cards
Contrast the roles of Chemoreceptors, proprioceptors, and baroreceptors
Proprioceptors (sensory input from muscles and tendons)
* Informs brain on changes in physical activity
Baroreceptors (sensory input from blood vessels)
* Informs brain on changes to pressure in vessels
Chemoreceptors (sensory input from blood vessels)
* Informs brain on changes of carbon dioxide or oxygen levels in the blood
* Important in respiratory system but has some affect on heart rate
* Informs brain on changes in physical activity
Baroreceptors (sensory input from blood vessels)
* Informs brain on changes to pressure in vessels
Chemoreceptors (sensory input from blood vessels)
* Informs brain on changes of carbon dioxide or oxygen levels in the blood
* Important in respiratory system but has some affect on heart rate
55
New cards
What type of receptors provide afferent signals? efferent signals?
Afferent
* baroreceptors
* chemoreceptors
Efferent
* baroreceptors
* chemoreceptors
* proprioceptors
* baroreceptors
* chemoreceptors
Efferent
* baroreceptors
* chemoreceptors
* proprioceptors
56
New cards
What is re-uptake? When does it occur?
* When a neurotransmitter, such as Acetylcholine, dopamine, epinephrine, is bound to a receptor it will continue to stimulate nerve cell
* To stop nerve impulse, neurotransmitter must be broken down by enzyme
* re-uptake is when the impulse is taken back up by neuron.
* need receptor on pre-synaptic neuron
* To stop nerve impulse, neurotransmitter must be broken down by enzyme
* re-uptake is when the impulse is taken back up by neuron.
* need receptor on pre-synaptic neuron
57
New cards
Describe ADHD, why it occurs, and what works to counteract it
* Attention Deficit Hyperactivity Disorder
* may be due to overabundance of dopamine receptors on pre-synaptic cell
* Prevent continued stimulation of post-synaptic cell and prevent nerve impulse from being propagated
* Ritalin acts by blocking actions of dopamine re-uptake receptor
* Dopamine stays around and can transmit impulse to post-synaptic cell
* may be due to overabundance of dopamine receptors on pre-synaptic cell
* Prevent continued stimulation of post-synaptic cell and prevent nerve impulse from being propagated
* Ritalin acts by blocking actions of dopamine re-uptake receptor
* Dopamine stays around and can transmit impulse to post-synaptic cell
58
New cards
What parts of the PNS are used to contract a muscle?
efferent nerves and somatic motor nerves
59
New cards
Describe the channels used to contract a muscle
* Action potential from motor neurons reaches end of axon
* Voltage-gated calcium channels open
* Ca2+ enters the neuron and causes synaptic vesicles to release acetylcholine (ACh) into the synapse
* ACh binds to ligand-gated ion channel in the motor plate
* The channel is a non-specific cation channel, allows diffusion of both sodium and potassium
* called a cholinergic receptor
* Sodium rushes into the cell →depolarization
* Potassium leaves the cell→ hyperpolarization
* More sodium enters than potassium leaves, end result is depolarization
* Depolarization causes muscle cell to reach threshold leading to action potential
* The action potential involves same voltage-gated channels as neurons
* Voltage-gated calcium channels open
* Ca2+ enters the neuron and causes synaptic vesicles to release acetylcholine (ACh) into the synapse
* ACh binds to ligand-gated ion channel in the motor plate
* The channel is a non-specific cation channel, allows diffusion of both sodium and potassium
* called a cholinergic receptor
* Sodium rushes into the cell →depolarization
* Potassium leaves the cell→ hyperpolarization
* More sodium enters than potassium leaves, end result is depolarization
* Depolarization causes muscle cell to reach threshold leading to action potential
* The action potential involves same voltage-gated channels as neurons
60
New cards
What is needed in order for a muscle to contract
Ca2+ ions remain in the sarcoplasm, and as long as ATP is available, the muscle fiber will continue to shorten.
61
New cards
Describe the respiratory response to exercise
* Increased rate and depth of breathing (Exercise hyperventilation or hyperpnea)
* Arterial O2 pressure, CO2 pressure, and pH do not change significantly during mild to moderate (submaximal) exercise due to exercise hyperventilation
* Arterial O2 pressure, CO2 pressure, and pH do not change significantly during mild to moderate (submaximal) exercise due to exercise hyperventilation
62
New cards
What does creatine phosphate do?
Some ATP is stored in a resting muscle. As contraction starts, it is used up in seconds. More ATP is generated from creatine phosphate for about 10 seconds (short duration exercises.)