Trauma Wk One - P&S Surveys & Trauma Systems
1/38
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
39 Terms
Trauma Triage Immediate Life Threat Criteria & Care
- Airway compromise or threat
- Severe bleeding that cannot be compromised
> closest trauma center, esclate care & signal 1. notify ARV.
Trauma Triage Vital Signs Criteria & Care
- SpO2 <90
- RR <10 or >30
- HR <60 or >120
- BP <90
- GCS <13
> closest trauma center within 60 minutes, esclate care & signal 1. notify ARV & consider HEMS if time to hospital is >60min
Trauma Triage Pattern of Injury Criteria & Care
- Penetrating Trauma (EXCEPT ISOLATED SUPERFICIAL LIMB INJURIES)
- Blunt trauma > serious injury to a single body region, or more than one
- Limb amputation or limb threat
- Suspected spinal chord injury or fracture
- Burns >20% TBSA
- Suspected resp tract burns
- Serious crush injury
- Major compound fracture
- Fracture to two or more long bones
- Pelvis fracture
Highest level of trauma service within 60min, escalate care, HEMS is >60min out, signal ONE
Trauma Triage Mechanism + Vunerability Criteria & Care
- motor cyclist impact >30km/hr
- high speed MCA >60km/hr
- pedestrian impact
- ejection from vehicle
- prolonged extrication
- fall from >3m
- struck on the head object from >3m
- explosion
AND over 55, pregnant, or significant underlying condition (hypertension, obesity, CCF cont/uncont, symptomatic COPD, IHD, renal issues)
Closest trauma service, escalation of care
Trauma Service List
MAJOR TC (Adult >16yrs)
- Royal Melbourne
- The Alfred
MTS Paed (<16yrs)
- Royal Childrens
Metro Trauma Centres
- austin health (A+Paed)
- box hill (A+Paed)
- the northern (A+Paed)
- monash medical (A+Paed)
- dandenong (A+Paed)
- frankston (A+Paed)
- Maroondah (ADULT ONLY)
- St VIncents (ADULT ONLY)
- Western Hospital Footscray
Regional TC
- Geelong, Hamilton, Warrambool
- Ballarat, Horsham
- Bendigo, Mildura
- Albury, Shepparton, Wangaratta
- Traralgon
VSTORM
Victorian State Trauma Outcomes Registry and Monitoring Group - they gather & interpret information about causes of traumatic injury and treatment from trauma centres across Victoria. Aim is to reduce preventable deaths. (in vic since 2001)
Improved Functional Outcomes for Major Trauma Patients in a Regionalized, Inclusive Trauma System
Despite an annual decline in mortality, risk-adjusted functional outcomes improved over time, and cases managed at MTS (level-1 trauma centers) demonstrated better functional outcomes. The findings provide early evidence that this inclusive, regionalized trauma system is achieving its aims.
Paed Trauma Criteria Vitals 0-3mnths
HR <100 - <180
RR >60
BP <50
SPO2 <90%
GCS <15
Paed Trauma Criteria Vitals 4-12mnths
HR <100 - <180
RR >50
BP <60
SPO2 <90%
GCS <15
Paed Trauma Criteria Vitals 1-4yrs
HR <90 - <160
RR >40
BP <70
SPO2 <90%
GCS <15
Paed Trauma Criteria Vitals 5-11yrs
HR <80- <140
RR >30
BP <80
SPO2 <90%
GCS <15
Paed Trauma Criteria Vitals 12-15yrs
HR <60- <130
RR >30
BP <90
SPO2 <90%
GCS <15
What is a 'Major Trauma' ?
Includes all trauma patients with injury as their principal diagnosis who meet the following criteria:
- death after injury
- injury severity score >12
- admission to intensive care for more than 24 hours
- urgent surgery for intracranial, intrathoracic or intraabdominal injury, or fixation of pelvic or spinal fractures
- injury being the principal diagnosis & satisfying any of the victorian state trauma registry patient inclusion criteria
Global Trauma Epidemiology
- 4.4MIL people die each year due to unintentional and violence related injuries
- Persons ages 5-29, top 3/5 causes of death are injury related
- injuries and violence are responsible for an estimated 10% of all years lived with disability
Global MVA Accident Vehicle Distribution Stats
- 25% 4 wheelers
- 30% powered 2/3 wheelers
- 5% bikes
- 21% pedestrians
- 19% other
Aussie Trauma Epidemiology
- 1,,824,454 ED presentations
- 575,345 hospitalisations
- 15,332 deaths
- 7.9% of total burden of disease
- 6.4% of healthcare spending
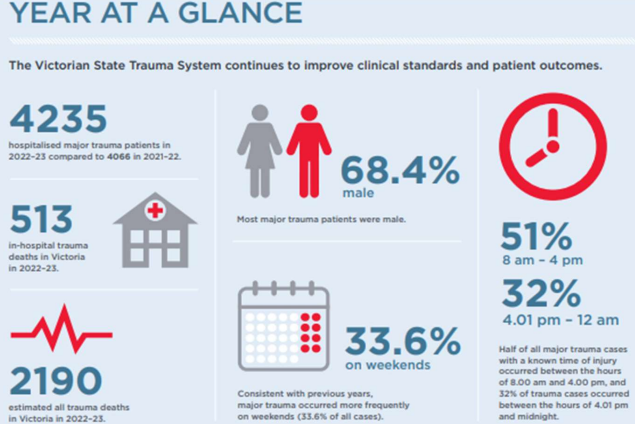
VIC Trauma Epidemiology 22-23
- 4235 major trauma patients hospitalised
- 513 in-hospital trauma deaths
- 2190 estimated trauma deaths
- 68.4% male
- 33.6% occur on weekends
- 51% 8am-4pm, 32% 4.01pm - 12am)
- 34% transport related
- 37% due to falls
- 5.5% cyclists
- 1.3% burns
- 37% at home
Viictorian Epi Stats
'Golden Hour'
The first hour after injury will largely determine a critically injured persons chances for survival
Trimodial Distribution of Deaths
Immediate: targeted with safety features/public health
Early: enhanced pre-hospital care + trauma systems
Late: specialist trauma care - massive reduction
Theoretical Model of an Ideal Trauma System
- advanced prehospital system
- registry research education
- centralised expertise
- expert Advice & retrieval
- satellite recieving centres
- early notification
- rapid transpirt platforms
- rapid identification & dispatch
When was ROTES established?
Review of Trauma & Emergency Services VIC was published in 1999, and established the need for a statewide trauma system, and formalised trauma centres.
Paramedics role in a Trauma case
patient assessment, triage, leadership & choice making, primary survey intervention, supportive management, resource allocation, communication
Four Trauma Triage Pathways
- Life threat
- Vital signs
- Pattern of Injury
- MOI + Vunerability
Three components of pre-hospital trauma triage
Vital signs, Anatomical, Mechanism
Clinical Approach Breakdown
- Dynamic Risk Assessment (throughout)
- Rapid Assessment (WOB, Circ to skin, Appearance) - SICK/NOT SICK
- Haemorrhage (identify & manage early. DP, DP Again, Arterial Pressure, CAT & Haemostatic Dressing)
- Response (AVPU)
- Airway + C-Spine (check for patency, listening for weird sounds) - collar?
- Breathing (Yes? No? Adequate? Manage if required)
- Circulation (Pulse?)
- Disability/Defib (pads on if needed)
- Exposure/Environment
- History (AMPLE + DOLORS), VSS, GCS RSA PSA
- Secondary Survey
Trauma Secondary Survey (HEAD)
- lacerations
- haematomas
- fractures
- mastoid/periorbital bruising (basal skull)
- feel for depressions, boggy masses & other irregularities
Trauma Secondary Survey (FACE)
- symmetry
- CSF from nose/ears
- foreign bodies in eyes
- iris & eye shape
- hyphema
- bruising under eyes
- conjunctival haemorrhage
- pupil size & reactivity
- mid-facial swelling
- upward gaze abaility
- nasal fracture
- alignment of bite
- oral swelling
- palpate bony margins of orbit, maxilla, nose & jaw
Potential Trauma Injuries (FACE)
- fractures (+basal skull & nose))
- high forces
- pressure changes
- TBI
- le forts fracture
- orbital floor fracture
- bleeding into the stomach
- lost teeth
Trauma Secondary Survey (NECK)
- lacerations
- perforations
- gross irregularities
- general pain
- trachea alignment
- wounds
- subcutaneous emphysema
- vein distension
Potential Trauma Injuries (NECK)
- spinal injury
- bone injury
- vessel perforation
Trauma Secondary Survey (CHEST/BACK)
- lacerations
- perforations
- bruising
- equal rise & fall
- paradoxical movements
- lung sounds present?
- wounds (blunt/penetrating)
- subcutaneous emphysema
- seatbelt signs
Potential Trauma Injuries (CHEST/BACK)
- lung contusions
- lung injury/pnemothorax
- large vessel perforations
- pericardial tamponade (FLUID IN HEART)
- Haemothorax
- Flail segment
- rib injuries
Trauma Secondary Survey (ABDOMEN)
- lacerations
- bruising
- perforations
- swelling/rigidity
- tenderness
- penetrating injuries
- genitalia injury
Potential Trauma Injuries (ABDO)
- underlying contusion
- vessel perforation
- internal haemorhhage
Trauma Secondary Survey (PELVIS + LEGS)
- pelvic symmetry (DO NOT SPRING)
- blood from urethra
- genital injury
- neurovasc obs
- deformity
- crepitus
- unnatural movement
- changes in strength & sensation
Potential Trauma Injuries (PELVIS & LEGS)
- fracture
- spinal injuries
Traumatic Arrest Guideline
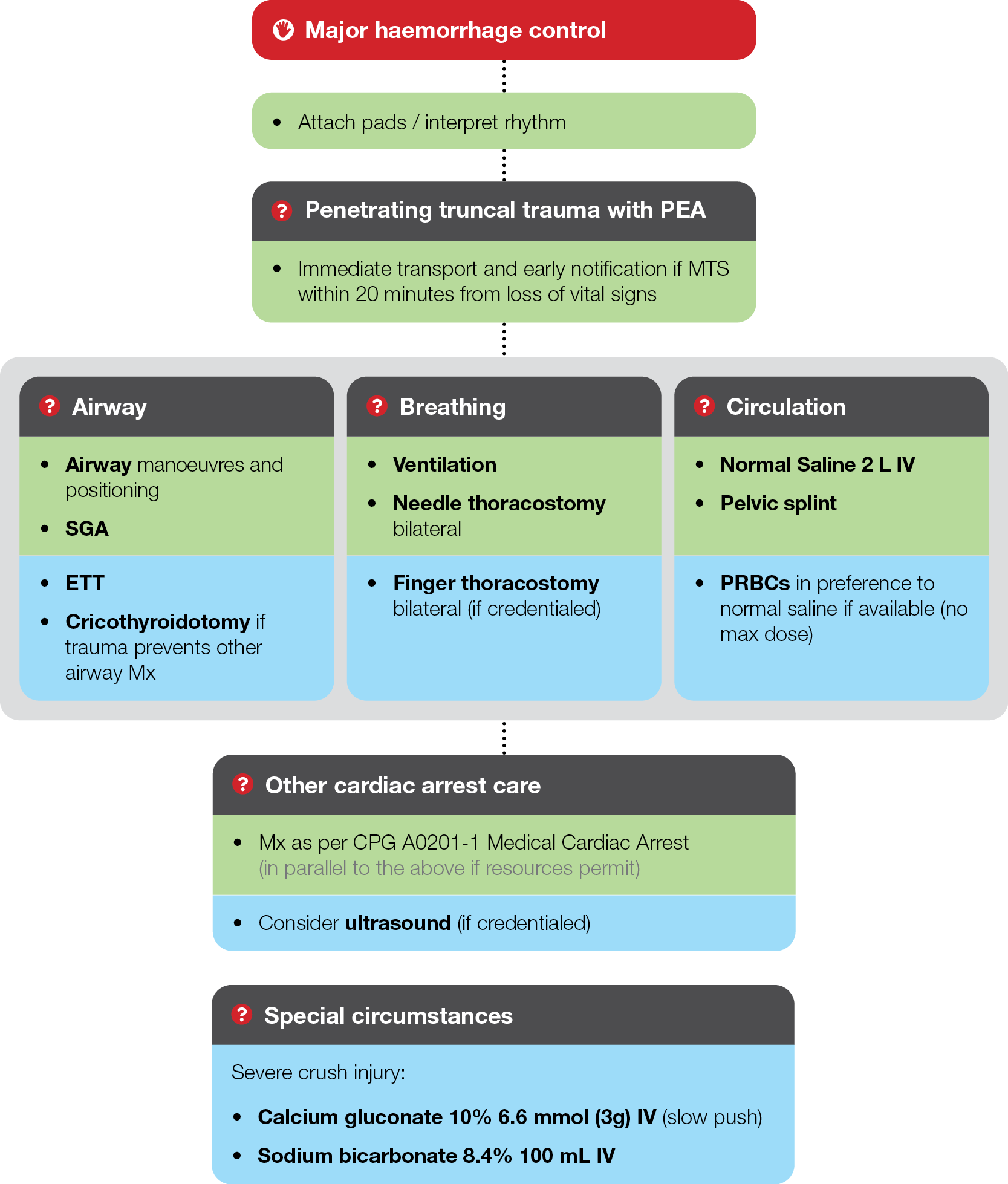
OSCE vs ON ROAD Approach
OSCE: DRSAaBbCcHDE
ON ROAD: DR ABC Hh abc (D)E