Week 6: Urinary Elimination, Fluid Balance, and Assessing Input and Output
1/56
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
57 Terms
What two distinct compartments is a human's body fluids divided into? (Potter and Perry 1015)
Intracellular fluid (60%/ 28L)- fluid within the cells (cytosol)
Extracellular fluid (14L) - fluid outside the cells
What three compartments is extracellular fluids of the human body divided into? (Potter and Perry 1015)
Interstitial fluid (11L) - fluid between and outside of cells
Intravascular fluid (3L) - blood plasma
Transcellular fluid - separated by other fluids by epithelium, includes cerebral spinal,. pleural, peritoneal, synovial, and GI fluids
What are three passive transport methods of fluids and electrolytes across a membrane? (Potter and Perry 1016)
Osmosis - movement of water from less solute conc to more solute conc
Diffusion - movement of ions + molecules from high conc to low conc (inclu. facilitated diffusion)
Filtration - water moves into and out of the capillaries as a result of hydrostatic and colloid osmotic pressures (high on arteriole end, low on venous end)
What is active transport? What is primary vs secondary active transport? (Potter and Perry 1016)
Facilitating movement of molecules across the plasma membrane against a concentration gradient via ATP
Primary active transport - Protein binds with solute to carry it across a concentration gradient
Secondary active transport - Pump uses ATP to create an artificial concentration gradient, allowing a molecule to enter/exit a cell
(Fluid) Output (Potter and Perry 1016)
Loss of body's fluid through various mechanisms involving the kidneys, the skin, the lungs, and the GI tract
Includes urine, diarrhea, vomit, gastric suction, and drainage from wounds
What is the kidney's role in fluid output? (Potter and Perry 1016)
Kidneys filter plasma and produce urine (~1200ml - 1500ml) which is part of the body's obligatory and sensible water loss
What is the skin and respiratory system role in fluid output? (Potter and Perry 1016)
Both contribute to insensible water loss, which is a continuous, gradual loss of water.
The respiratory system contributes to water loss by changes in respiratory rate and depth.
The skin contributes to water loss via the sympathetic NS, which activates sweat glands. It also occurs during a fever and exercise
What is insensible water loss? (Potter and Perry 1016)
Continuous gradual loss of water via the lungs and the skin
What is the GI tract's role in fluid output? (Potter and Perry 1017)
Filters and absorbs 9L of fluid which is ingested, leaving only 100ml of fluid excreted via feces, or excessively during diarrhea , which may affect the body's homeostasis
(Fluid) Intake (Potter and Perry 1017, 1031)
Gain of body's fluids, primarily through the body's thirst mechanism
Includes all liquids taken by mouth or through nasogastric + jejunostomy feeding
How is fluid intake monitored by the body? (Potter and Perry 1017)
Osmoreceptors detects osmolarity and plasma levels. If osmolarity increases (more solute) or if plasma levels decrease, the thirst center is stimulated which causes you to feel thirsty
The thirst center is also stimulated by the RAA pathway, potassium depletion, psychological factors, and oropharyngeal dryness
What 5 health history factors can increase the risk of fluid imbalances? (Potter and Perry 1026)
1. Age - differences in water proportions and compensation
2. Environmental factors - excessive sweating from intense exercise or temperatures
3. Diet - Lack of amino acids -> hypoalbuminemia -> serum colloid oncotic pressure decreases -> circulating plasma leaks into interstitial fluid spaces
4. Lifestyle - substances, damage to regulatory organs (kidneys, liver, lungs)
5. Medication (use of diuretics or laxatives)
How does age influence fluid balances in the body? (Potter and Perry 1026)
Infants - greater water proportion, greater risk for fluid volume deficits
Children (2-12) - less stable regulatory responses to fluid imbalances + frequent response to illnesses
Adolescence - increased metabolic processes + compensation
Older ppl - less ability to compensate for imbalances (results in reduced ability to excrete medication)
What 6 acute medical history factors may influence the risk of a fluid imbalance? (Potter and Perry 1027)
Acute illnesses
-Burns (greater burn = greater water loss)
-Respiratory disorders
-GI disturbances (gastroenteritis + nasogastric suctioning)
-Trauma (hemorrhage, crush injuries)
-Head injury (edema causing pressure to pit. gland)
-Recent surgery (extensive surgery= big fluid loss, stress response from surgery)
What 5 chronic medical history factors may influence the risk of a fluid imbalance? (Potter and Perry 1029)
Chronic illnesses
-Diabetes mellitus (results in FVD, end stage renal disease)
-Cancer
-Cardiovascular disease (reduced kidney perfusion = reduced urinary output = increased water retention)
-Renal disorders (abnormal retention of water)
-GI disorders (Inflammatory bowel disease, liver failure, vomiting diarrhea)
Fluid volume deficit (FVD) (Potter and Perry 1030)
aka hypovolemia, condition where body losses an excessive amount of fluid
Fluid volume excess (FVE) (Potter and Perry 1030)
aka hypervolemia, condition where body contains/retains an excessive amount of fluid
What are 11 physical assessment techniques done by the nurse to assess fluid imbalances? (Potter and Perry 1030, PG)
1. Daily weight assessment (>1kg loss = FVD, >1kg gain= FVE)
2. BP (hypotension + orthostatic hypotension= FVD)
3. Pulse (Rapid+thready= FVD, Bounding= FVE)
4. Capillary refill (>2 sec = FVD -> poor perfusion)
5. Lung auscultation (crackles or wheezing = FVE)
6. Urine output (<30-50ml/hr = FVD, yellow=FVD)
7. Edema (presence = FVE)
8. Mucous membranes (dry, decreased of tearing = FVD)
9. Skin turgor (poor = FVD)
10. LOC (Restlessness + mild confusion = severe FVD)
11. Thirst (presence = FVD)
Whereas FVD = fluid volume deficit (low fluids in body) and FVE = fluid volume excess (high fluids in body)
What are physical assessment characteristics that are indicative of fluid volume deficit (FVD)? (Potter and Perry 1030, PG, Lec)
1. Loss of weight greater than 1kg per day
2. Hypotension or orthostatic hypotension
3. Rapid thready pulse
4. Greater than 2 second capillary refill
5. Less than 30-50ml/hr urine output
6. Dry mucous membranes
7. Poor skin turgor, sign of dry skin
8. Restlessness and mild confusion
9. Thirst
10. Dizziness, headaches, impaired mental status
11. Weakness/Lethargy/Irritable
12. Fever
13. Nausea/Vomiting
14. Urine amount + concentration (<30ml/hr - very yellow)
What are physical assessment characteristics that are indicative of fluid volume excess (FVE)? (Potter and Perry 1030, PG)
1. Gain of weight greater than 1kg per day
2. Bounding pulse
3. Cracking or wheezing sounds of lungs upon auscultation
4. Presence of edema
What are 7 clinical tools that nurses can use to assess fluid imbalances within a patient? (Potter and Perry 1030)?
1. Fluid balance chart - including all intake and output (time+amount) and 24 hour balance (deficit or excess) summary
2. Patient weight
3. Urine sample via calibrated receptacle (pls pee into this cup) or a catheter
4. Lab data (including serum + electrolyte levels, hematocrit, blood creatinine, blood urea nitrogen levels, and urine specific gravity)
5. Arterial Blood Gases
6. Chest X-Ray (detect fluid in lungs)
7. ECG (cardiac status + rhythm)
(Urinary) Incontinence (Potter and Perry 1164)
Any complaint of involuntary loss of urine (including storage, voiding, and postmicturition symptoms)
How can a UTI affect fluid imbalances in the body? (Potter and Perry 1164)
-obstruction to urinary tract
-spread to kidneys causing disease
-pain + burning sensation during urination
-development of fever, chills, nausea, vomiting, and malaise
-inflammation of bladder may cause incontinence
What is nocturia? (Potter and Perry 1164)
Prevalent and bothersome lower urinary tract symptom, defined as the need to get up at night on a regular basis to urinate, often increases with age
How can urinary retention affect fluid imbalances in the body? (Potter and Perry 1165)
Accumulation of urine in the bladder due to the bladder's inability to empty , causing feelings of discomfort, pressure, tenderness, restlessness, and diaphoresis. Can result in UTI and UI
How can renal failure affect fluid imbalances in the body? (Potter and Perry 1167)
Damage to glomeruli or renal tubules causes decline in kidney function, leading to end-stage renal disease, resulting in severely reduced or absent urine output from the bladder
What are 4 alterations in the urinary system that can cause fluid imbalances in the body? (Potter and Perry 1164)
- Urinary Tract Infections
-Urinary Incontinence (nocturia)
-Urinary retention
-Renal failure
What are 7 types of urinary incontinences? (Potter and Perry 1166)
Transient UI= caused from factors outside of urinary system
Urge UI= Involuntary loss of urine with urgency, frequency, or nocturia
Stress UI= Involuntary loss of urine upon physical exertion
Mixed UI= Urge + Stress UI
UI assoc with chronic retention of urine = involuntary loss of urine when bladder does not completely empty with a high residual urine volume
Functional UI = loss due to inability to reach toilet
Neurogenic bladder dysfunction = lower urinary tract dysfunction, causing urge incontinence, frequency, and retention
How does the patient's ability to control urination develop throughout the lifespan? (Potter and Perry 1168)
Infants + Children - excrete large volume of urine
2-3 yrs - able to associate sensations of bladder filling and urination -> should be able to recognize feeling of bladder fullness, hold urine 1-2 hours, and communicate to adult
Toddlers - control of urethral sphincter + toilet training
4-5 yrs - full control of micturation via toilet training
Pregnancy - increased urinary freq + UTI
Older pts - lack of kidney ability to concentrate urine or reabsorb water + sodium -> often experiences nocturia, elevated postvoid residual, increased susceptibility to UTI
What should be included in a nursing health history of a patient's urinary system? (Potter and Perry 1169, PG)
1. Patterns of Urination (usual daily voiding patterns + changes)
2. Factors Affecting Urination
-Medical/Surgical history
-Constipation (Bowel elimination pattern)
-Medication
-Catheter
-ADLS
-Symptoms such as pain
-Frequency
-Urgency
-Polyuria
-Dysuria
-Nocturia
-Hematuria
-Hesitancy
-Dribbling
-Elevated post void residual volume
-Mobility
What should be included in a nursing physical assessment of a patient's urinary system? (Potter and Perry 1170, PG)
1. Assessment of skin (turgor) and mucosal membranes (dryness)
2. Kidneys (flank pain, renal artery bruit)
3. Bladder
-Inspection - swelling or convex curvature of lower abdomen
-Palpitation - light palpitation, should feel smooth and rounded
-Percussion - should yield a dull note
4. Perineum (note any rash, discharge, inflammation, and lesions)
What urine characteristics should be noted during a urinary assessment? (Potter and Perry 1172, PG)
Color - Normal: pale straw - amber/ Bleeding: dark red from kidney or liver dysfunction, bright red from bladder or urethra/ also influenced by food and medication
Clarity - Normal: transparent/ Cloudy+Foamy: renal disease, bacteria/ Mucous: normal w/ pts with urinary diversions, increased production= UTI
Odor - more concentrated = stronger/Incontinent = ammonia odour/ Diabetes mellitus or starvation = sweet-fruity odor
Amount - (<30ml/hr for 2 hours is concerning)
How should urine collection be adjusted for pediatric patients? (Potter and Perry 1173)?
- Offering water 30 minutes before collection
- Using terms that children can understand
-Use of potty chair or toilet seat instead of receptacles
-Use of clear plastic single use bags for toddlers that are not potty trained
What should be part of a nursing intervention in regards to patient education of urinary elimination as part of a urinary assessment? (Potter and Perry 1182)
-Focusing on teaching patient specific problems related to urination
-Teaching patients significance of symptoms related to urinary alterations so that early preventive health care can be initiated
-Incorporating teaching while providing nursing care (teaching benefits of fluid intake while giving fluids to pt)
What should be part of a nursing intervention in regards to promoting regular micturition as part of a urinary assessment? (Potter and Perry 1182)
-Reinforce importance of voiding regularly to maintain a normal bladder capacity (every 3-4 hours)
-Emphasize normal bowel movements and methods of enhancing regularity (stool can compress urethra)
-Educate normal position of voiding to enhance micturition reflex (female - easier while squatting or sitting, male - easier while standing)
-Providing urinals for patients with limited mobility and unable to reach toileting facilities
-Providing sensory stimuli to promote relaxation and voiding (sounds of rushing water)
-Pouring warm water over perineum to create urge to urinate
-Inquiring and incorporating pt's normal urination patterns/habits
-Encourage fluid intake (even with pt's with incontinence), without caffeine, can also include fruits
-Establishing a routine for fluid intake
-Avoiding tobacco, alcohol, caffeinated drinks, carbonated beverages, and artificial sweeteners
Urinal (Potter and Perry 1184)
A metal or plastic receptacle for urine
For females, contains an elongated spout

What should be part of a nursing intervention in regards to promoting complete bladder emptying as part of a urinary assessment? (Potter and Perry 1183)
-Residual urine can cause incontinence and bacterial growth (leading to UTI)
-Encouraging pt to take their time while voiding, try to encourage them to feel when they have not emptied their bladders fully
-Pts with constant post-void residuals may need catheterization
-Use of bladder scanner to scan for post-void residuals
What should be part of a nursing intervention in regards to preventing UTIs as part of a urinary assessment? (Potter and Perry 1183)
- Encouraging good perineal hygiene (cleaning after voiding or bowel movement)
-Use of squirt bottle with pt's w/ limited dexterity
-Encouraging hand hygiene
-Drinking sufficient amounts of fluid to maintain constant urine output based on weight
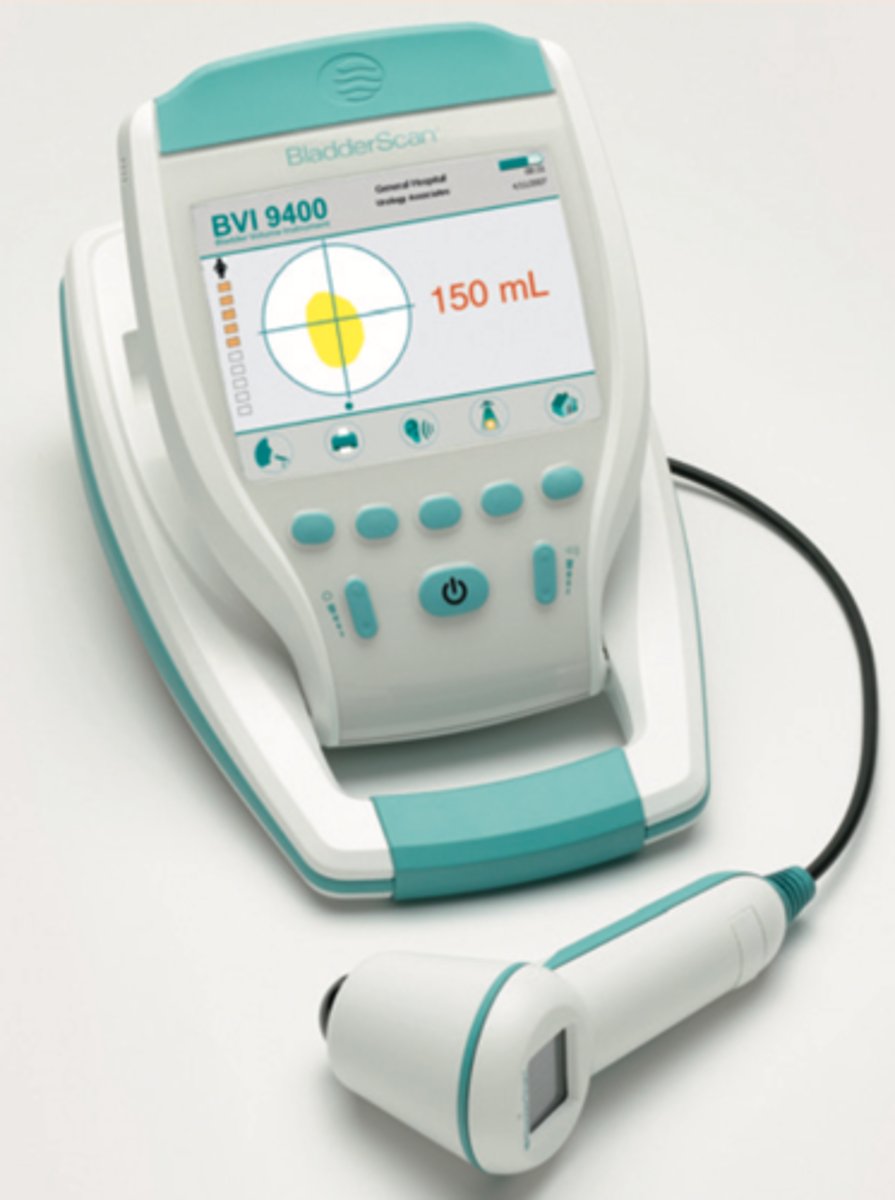
Bladder scanner (Potter and Perry 1185)
Used to measure bladder volume, especially useful with pts with post-void residuals
NPO
Abbreviation for "nothing by mouth"
A medical instruction to not eat or drink anything for a period of time
Positive/Negative fluid balance
Positive fluid balance - body has too much fluids (aka hypervolemia, FVE)
Negative fluid balance - body has too little fluids (aka hypovolemia, FVD)
Which body system is primarily responsible for regulating fluid balance? (Lec)
Renal system
Which age groups are primarily vulnerable to fluid imbalances? (Lec)
Infants + Older adults
What functions does body water have in the body? (Lec)
1. Transporting Nutrients, Electrolytes, and Oxygen to cells (important to tissue oxygenation, renal function, and acid-base balance)
2. Carrying waste products away from cells
3. Regulation of body temperature
4. Lubrication of joints and membranes
What are osmotic pressures? (Lec)
Pressure needed to counter movement of water across a membrane (prevent osmosis)
A solution with a high solute concentration, and thus a high osmotic pressure, draws water into itself
What is colloid osmotic pressure? What causes this pressure? (Potter and Perry 1016)
Water being pulled from the intracellular fluid into the intravascular compartment (bvs) due to a greater solute concentration in the plasma
This solute concentration exists due to plasma proteins such as albumin (greatest), globulins, and fibrinogen
What is hydrostatic pressure? What causes this pressure? (Potter and Perry 1016)
"Force exerted by fluids within a compartment", in the case of intravascular fluid, is caused by heart contractions. Thus, hydrostatic pressure (bp) is greater in the arterioles than the veins, causing a pressure gradient, allowing blood to flow through the capillaries
How is weight an indicator of fluid volume loss or gain? (Lec)
1kg = 1L of water
Therefore,
loss of 1kg = loss of 1L of water
What are general nursing interventions to dehydration? (Lec)
1. Measure inputs and outputs (insertion of foley catheter)
2. Vital Signs
3. Fluids as ordered
4. Skin/mouth care (dry mucous membranes + skin)
5. Increase Na+ levels
6. Measure daily weights (1kg=1L)
7. Cognitive assessment (dehydration has lots of cognitive signs)
8. Urine specific gravity
9. Skin turgor assessment
10. Color of urine
11. Health teaching
What is a symptom of hypervolemia observable on the surface of the body, and why does this occur? (Lec)
Edema on tissues (appears as swelling)
Occurs due to excess fluid in the body being forced out of blood vessels and moving into interstitial space
May be severe and cause pulmonary edema, fluid in lungs
What are physical characteristics of patients with hypervolemia? (Lec)
1. Tachypnea
2. Dyspnea
3. Crackles in lungs
4. Rapid/bounding pulse
5. Hypertension
6. Distended neck and hand veins
7. Acute weight gain (1kg = 1L)
8. Edemas
9. S3 gallop
10. Pulmonary congestion (pulmonary edema)
What are general nursing interventions in response to hypervolemia? (Lec)
1. Measuring inputs and outputs (insertion of foley catheter)
2. Na+ and fluid restrictions
3. Mouth and skin care
4. Diuretic therapy upon prescription
5. Daily weights
6. Urine specific gravity/osmolarity
7. Cognitive assessment
9. Cardiovascular assessment
10. Respiratory assessment
11. Color of urine (more diluted)
12. Possible need for dialysis if kidney function impaired
What intakes and outputs are measured during an I/O assessment? (Lec)
Intakes
-Oral intake (food)
-Enteral intake (feeds into GI)
-Parenteral intake (IV fluids, TPN - nutrition via veins)
Outputs
-Urine
-Diarrhea
-Emesis (Vomiting)
-Drainage tubes
-Suctioning
What are factors that can influence urination? (Lec)
1. Psychological (Anxiety + Stress)
2. Sociocultural (culture, gender, practices)
3. Fluid balance (Caffeine, alcohol)
4. Developmental level
5. Activity
6. Medical conditions/diagnoses
7. Surgical procedures (anesthesia)
8. Pathological conditions (neuro disease, altered mobility, renal disease)
9. Medication (diuretics)
What are normal urine amounts across the lifespan?
>Age 2 =(>1ml/kg/hour)
Adults= (>30ml/hr)
What are nursing methods to prevent catheter associated UTI? (Lec)
- Only use catheter when necessary (surgery, I/O, immobilization, urinary retention/obstruction, end of life care, sacral pressure injury)
-Use should be re-assessed daily
-Maintain a closed system
-Properly secure tubbing
-Allow unobstructed urine flow
-Routine hygiene and perineal care
-No routine use of antibiotics needed
What are the steps to using a bladder scanner (Potter and Perry 1185, Lec)
1. Identify patient and perform hand hygiene
2. Place patient supine with head slightly elevated, expose abdomen
3. Turn scanner on, clean before use
4. Palpate pubic bone, apply ultrasound gel to midline abdomen above pubic bone
5. Place scanner on gel and apply light pressure, point downward slightly toward bladder