Topic 4: Plasma Proteins; Pathological Markers in Blood
1/38
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No study sessions yet.
39 Terms
What is the difference between plasma and serum
plasma = complete straw coloured fluid without cells
serum = the straw coloured fluid left after clotting without clotting factors or cells
What are some functions of plasma proteins
transport and storage
balance of electrolytes and water
acid/base regulation
acute phase response
enzymes
hormones
clotting
What are some cation binding proteins and their ligands
albumin - divalent and trivalent cations: Cu2+ and Fe3+
ceruloplasmin - Cu2+
transferrin - Fe3+
What are some hormone binding proteins and their ligands
thyroid binding globulin - thyroxine (T4), tri-iodothyrine (T3)
cortisol binding globulin - cortisol
sex hormone binding globulin - androgens, estrogens
What are some haemoglobin/protoporphyrin binding proteins and their ligands
albumin - haem, bilirubin, biliverdin
haptoglobin - Hb dimers
What are some FFA binding proteins and their ligands
albumin - FFA, steroids
Why are proteins measured?
A change in plasma level of a protein can be indicative of disease affecting circulation or the tissue that synthesises the protein
proteins with physiological function in circulation
A change in level of plasma can be indicative of disease affecting tissue that synthesises protein
proteins that leak from cells/tissues
Clinical Biochemistry labs measure:
total protein
albumin
Ig’s
serum protein electrophoresis
protein and peptide hormones
enzymes, fibrinogen, clotting factors
CRP - inflam marker
transferrin - transport
complement - immune
alpha-1-antitrypsin - protease inhibitor
ceruloplasmin - transport
haptoglobin - binding protein
What are some reasons for the body to alter plasma protein levels/activity
changes in cellular prolif, cell turnover or damage, protein synth
inherited protein variants with altered activity
altered protein conformation
How are enzymes used as disease biomarkers?
cellular damage triggers release of certain enzymes from affected tissues
elevated enzyme levels can be measured in serum, saliva, urine
measurable changes in enzyme activity can serve as disease biomarkers, often before clinical symptoms appear
What is proteomics
the systematic, high-throughput approach to protein expression analysis of a cell or organism
cells respond to internal and external changes by regulating activity and level of proteins therefore can be used to understand structure, function and interactions of the entire protein content in specific organism
What are the four types of protein assays used in clinical biochemistry labs
spectrophotmetric
total protein
albumin
electrophoresis
protein
immunochemical
nephelometry
rate nephelometry
turbidimetric immunoassay
immunoassay
immunoassay
ELISA
western blotting
protein hormones
How is total protein measured?
Biuret assay
Cu2+ ions and peptide bonds in alkaline medium form violet coloured complex and is measured at 540nm
How can serum albumin be measured?
Bromocresol green
Bromocresol purple
Bradford assay
Lowry assay
Describe the bromocresol green assay for total protein/albumin measurement. What absorbance does it measure it at? What is a limitation?
albumin binds BCG
absorbance at 628nm: increases in proportion to protein concentration
some non specific A changes over time
Describe the bromocresol purple assay for total protein/albumin measurement. What absorbance does it measure it at?
albumin binds BCP
absorbance at 603nm: increases in proportion to protein concentration
more specific for albumin
does not bind animal albumin
Describe the bradford assay for total protein/albumin measurement. What absorbance does it measure it at?
red form of coomassie blue donates free e- to ionisable groups on protein
causes disruption of proteins exposing hydrophobic pockets
negatively charged coomassie blue binds to protein and forms stabilised blue form in proportion to amount of protein
absorbance at 595nm
Describe the lowry assay for albumin measurement. What absorbance does it measure it at?
divalent copper ions in folin-ciocalteu reagent form complex with peptide bonds at alkalkine pH and reduced to monovalent copper ions
monovalent copper and radical groups of tyrosine, tryptophan and cystein react to folin reagent to produce unstable product that becames reduces to tungsten blue
blue = proportional to amount of tyrosine, trytophan and cysteine in protein
absorbance at 650nm
what is the clinical significance of measuring total protein. Include the RR and what low and high levels indicate.
RR = 60-80g./L
limited clinical value, concentration reflects protein and fluid content
low levels
dilution
hypoalbuminaemia
profound Ig deficiency
high levels
loss of protein free fluid, or stasis during venipuncture
major increase in Ig
what is the clinical significance of measuring albumin? What does it assess?
RR = 32-50g/L
assesses:
Ca2+ concentration (binds to albumin)
severity of liver disease, myeloma
contribution to oedema formation
dehydration resulting in haemoconcentration (increased Hct)
What is the principle of protein electrophoresis. What does migration depend on
migration of charged particles in support medium due to electric field
proteins = zwitterionic = can be negatively or positively charged depending on pH of solution
migration depends on:
electric charge
size and shape
electric field strength
properties of support material
temp
How is the velocity of a molecule moving in an electric field calculated?
v = Eq/d6 pi r n
v = velocity of molecule
E = electric field strength
q = net charge on molecule
d = distance between electrodes
r = radius of molecule
n = solution viscosity
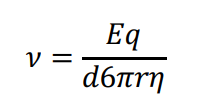
What are the uses of protein analysis
determine MW
analyse protein purity
protein ID
western blotting
What is the difference between Native PAGE and SDS PAGE
Native
proteins separated based on native conformation and charge
used to analyse serum proteins
SDS
uses SDS to break disulfide bonds and denature proteins
SDS unfolds proteins into their linear shape and masks charged groups
separate based on MW
What are types of solid support gels for electrophoresis. What molecules are they used for.
polyacrylamide
for proteins
chemically inert and electrically neutral
hydrophilic
does not interact with solutes
agarose
for nucleic acids
melted and set polysaccharide
sieving effect based on MW
uncharged support
What are the PAGE protein stains and their sensitivities?
Coomassie blue
sensitivity = 30ug protein
normal/common
Amido black
sensitivity = 75ug protein
used when lots of protein and not concerned about sensitivity
Silver
sensitivity = 0.2ug protein
What are the functions of acute-phase proteins?
mediators: CRP
modulators: fibrinogen
inhibitors: alpha-1-antitrypsin
scavengers: haptoglobin
immunomodulators: alpha-acid glycoprotein
repair: alpha-1-AT
What is the acute phase response? What are some systemic effects and by how much do acute phase proteins increase by in the first 7 days.
physiological events that follow tissue damage and inflammation
systemic effects = fever, muscle proteolysis, leukocytosis
acute phase proteins increase by >25% in first 7 days following tissue damage
How do some plasma proteins increase in APR?
CRP, alpha-1-AT, haptoglobin, ferritin, ceruloplasmin, C3, C4
CRP = 1000x increase in 6-10 hours
alpha-1-AT, haptoglobin and ferritin = 2-4x increase in 10-24 hours
ceruloplasmin and C3 and C4 = 0.5x increase in 48-72 hours
What is CRP (and its normal concentration) and what are some conditions with elevated CRP?
pentraxin family of proteins that bind phosphocoline, microbial cell walls and microbial and host chromatin
0.8mg/L
inflammatory = systemic vasculitis, rheumatoid arthritis
infections = bacterial and restricted viral
malignant = carcinoma, sarcoma
ischaemic necrosis = MI
trauma = surgery, burns
What is the function of complement proteins?
removal or destruction of antigen by opsonisation and lysis of microorganisms
peak 5 days after APR
classic: Ag-Ab complexes, C1q, C4, C2
alternate: bacterial cell wall components, endotoxins
both activate C3 → C5-9 MAC
What is the function of haptoglobin and what is its signicance i.e. when is it increased/decreased
binds free Hb released from RBC during intravascular haemolysis
1 HAP binds 2 Hb
rapid endocytosis and recovery of iron
Significance:
decreased in intravascular haemolysis and haem turnover
used up
increased in APR and burns + nephrotic syndrome
What is alpha-1 antitrypsin and its functions?
A mutation of this protein causes what? Which conditions/symptoms can it cause and how can it be diagnosed?
a major inhibitor of neutrophil elastase which is released from WBC to fight infection, and inhibits trypsin
changes conformation and tightly binds to inactivate protease
neutrophil elastase may attack normal tissues if not controlled by a1AT
uncontrolled → emphysema
smoking causes oxidation of a1AT → prevents inhibition
Z mutation (PiZZ)
poorly secreted a1AT and it aggregates in liver
homozygotes develop emphysema and liver disease at early age
dyspnoea
cirrhosis
infection and dehydration
defining symptoms:
cholestasis in infants
cirrhosis of unproven etiology
emphysema
diagnosis:
electrophoresis: decrease in a1 band
functional decrease in ability of serum to inhibit trypsin
What is ceruloplasmin and its functions? how many molecules can it bind and what enzymatic role does it have. Low levels of this protein can cause what disease?
multifunctional copper binding protein that has transport and enzymatic activities
binds 95% of serum Cu - 6-8 molecules at a time
oxidises Fe2+ to Fe3+ for incorporation into apotransferrin
antioxidant activity
low levels = wilsons disease (excess Cu) and menkes disease
results in increased total body Cu and liver Cu
What is a serum paraprotein
a monoclonal Ig or complement light or heavy chain
produced by clonal prolif of plasma cells or other B-cell lineage cells
What is monoclonal gammopathy and its characteristics?
an abnormal overproduction of specific clone of B cells/plasma cells producing Ig’s
monoclonal gammopathy of undetermined significant (MGUS)
paraprotein production with no associated organ damage
benign phenotype
serum paraprotein conc <30ug/L
<10% affected BM plasma cells
no anaemia, renal failure or hypercalcaemia
What is Multiple Myeloma and its characteristics? What are the symptoms associated?
proliferation of malignant plasma cells in the BM → producing abnormal monoclonal paraprotein and evidence of end-organ damage
symptoms: hypercalcaemia, anaemia, renal impairment and or bone pain
serum paraprotein > 30g/L or BM plasmacytosis of >10%
How can paraproteins be detected?
immunofixation - serum protein electrophoresis
serum separated on native PAGE
lanes with seperated proteins incubated with specific anti-Ig antisera
monoclonal Ig detected as bands
anti-IgG
anti-IgA
anti-IgM
anti-kappa light
anti-lambda light
What are bence jones proteins? What does their presence indicate?
free monoclonal light chains of kappa or lambda
ligh chains are filtered at glomerulus due to low MW to give heavy BJP proteinuria
presence of light chains implies de-differentiation due to their synthesis in excess of heavy chains (G, A, M)