Retinal Vascular Disease 1
1/51
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
52 Terms
Different types of blood vessels?
arteries, arterioles, capillaries, venules, veins
What does microvascular mean?
comprised of capillaries
What does macrovascular mean?
comprised of all other blood vessels
Key blood vessels in the Ocular Blood Supply?
Internal carotid artery
Ophthalmic artery
Posterior ciliary arteries
Central retinal artery
Other arteries that feed into anterior ciliary arteries
What are the two circulations of the eye
Central retinal artery and Ciliary arteries
What do the Central retinal artery / vein supply?
inner retina to OPL
What do the posterior and anterior ciliary arteries / vortex veins supply?
Uvea ,
outer retina to OPL (Photoreceptors)
What do the short posterior ciliary arteries supply?
Posterior uvea
Anterior optic nerve
why is the CRA described as ‘end arteriole’
there are no channels between artierioles so if there isa blockage anything distal to it will be susceptible to ischaemic damage
why is ischaemic changes rare in the uveal circulation
its robust so there are any intercommunicating channels so that any bloackage can be bypassed without interferring with the overall oxygenation o the tissues
4 Key features of retinal arterioles?
cross OVER veins, Share outer coat (adventitia), Site of BRVO, site of Arteriolosclerotic changes
How do venules compare to arterioles?
Darker red
Wider
More tortuous
Capillaries structure?
Wall is single cell thick, Thick basement membrane, Pericytes, Astrocyte foot processes, Selectively permeable
How is Fundus photography / SLO used to investigate of ocular vascular disease
Retinal vasculature, Haemorrhage, Exudates / Cotton wool spots
How is Fluorescence angiography used to investigate of ocular vascular disease
Structural integrity of vessels
Dynamic integrity of circulation- leaking of blood
Fluorescein: retinal circulation- capillary beds
Indocyanine green: choroidal circulation- any new abnormal blood vessels arising from choroid
How is OCT used to investigate of ocular vascular disease
Oedema, Macula
How is OCT angiography used to investigate of ocular vascular disease
Retinal circulation, Work in progress
Congenital anomalies of retinal blood vessels?
Congenital vascular tortuosity,
Anomalous blood vessels,
Bergmeister's papilla (hyaloid artery remnant at optic disc),
Cilioretinal artery
Telangiectasia
Coats disease
Key features of Cilioretinal artery
From short posterior ciliary arteries
Same supply as choroid
Common (20 - 30%)
Vascular pathology
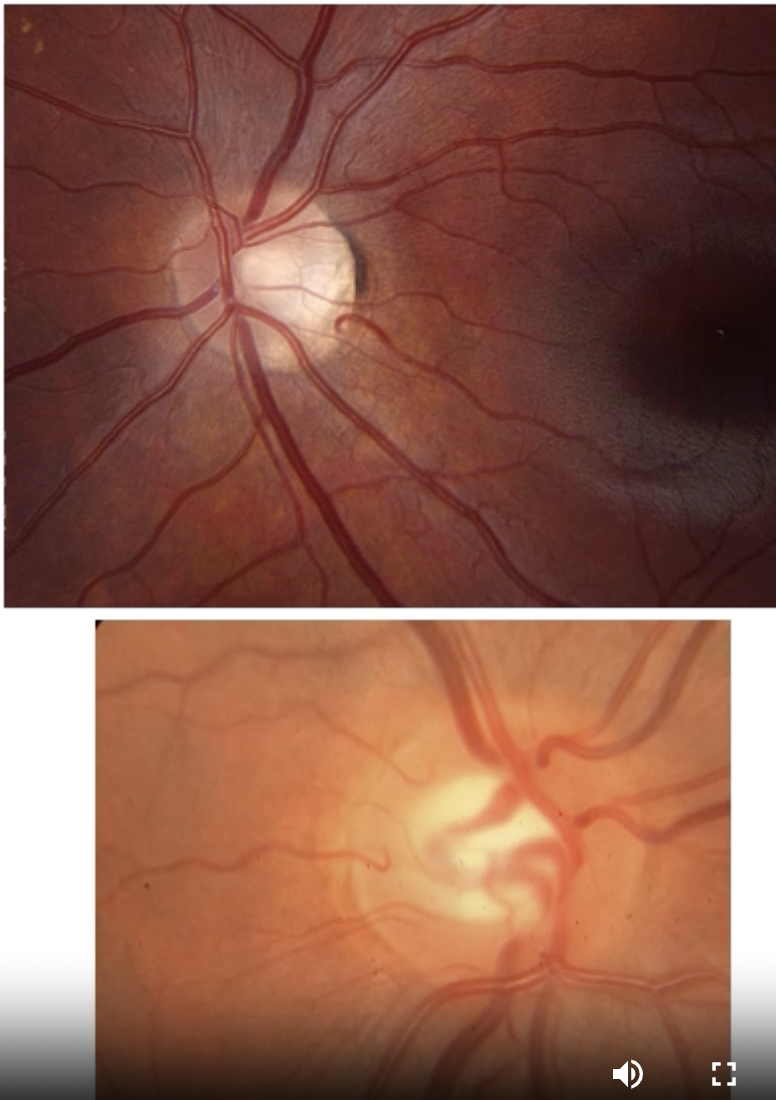
What is Telangiectasia
abnormal dilation of a blood vessel
types of telangiectasis for eye
Congenital retinal telangiectasia
Idiopathic juxtafoveal retinal telangiectasia
Key features of Coat's disease?
Rare
Children (boys)
Squint
Leukokoria / yellow or absent red reflex
Reduced vision
Dilated abnormal leaky vessels
Gross exudate,
Exudative retinal detachment
Progressive,
Treatment difficult
Result of acquired vascular disease?
cell damage and death (necrosis)
What causes cell damage and death in acquired vascular diseases?
Ischaemia and infarction due to disordered circulation because of damaged blood vessels
Vascular diseases within the lumen?
Haemodynamic: hyperviscosity and sluggish circulation
Thrombosis: in situ blood clot in a blood vessel e.g chlosterol
Embolus: abnormal mass (including a thrombus) travelling in bloodstream
Vascular disease within vascular wall?
Thinning and increased permeability, leakage
Oedema
Haemorrhage.
Thickening - Arteriosclerosis • Atherosclerosis • Spasm • Inflammation.
Dilatation • Tortuosity • aneurysm
Vascular disease external to vessel?
Compression
IOP / glaucoma
Risk factors for vascular disease including ocular vascular disease
Hypertension • Diabetes mellitus • Hyperlipidaemia • Obesity • Smoking • Age • Haematological = blood disorders
What blood disorders can be a risk factor for vascular disease?
Hyperviscosity e.g. polycythaemia, leukaemia
Increased clotting
Anaemia
What is Atherosclerosis
fatty deposits in arterial wall
Large / medium sized arteries
leads to Thrombosis • Embolism
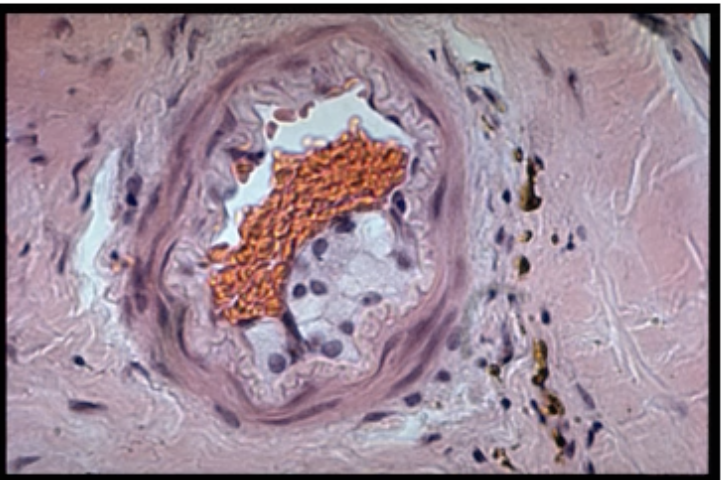
What is Arteriolosclerosis
Thickening of walls / narrowing of lumens of small arteries and arterioles e.g. retina
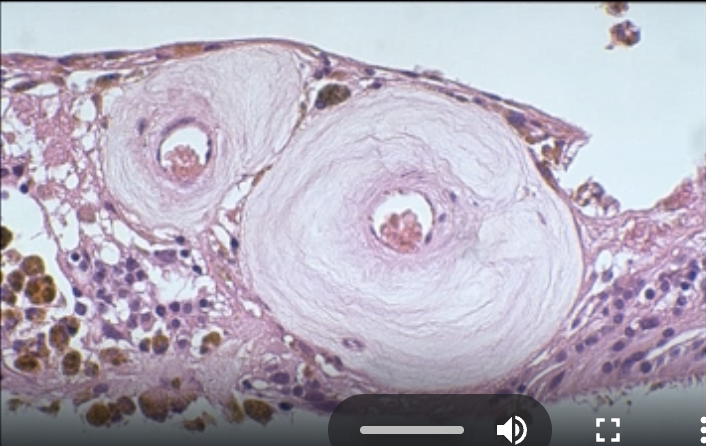
Key features of Hypertensive retinopathy
Systemic hypertension - BP consistently > 140/90
Chronic changes - Accelerated ageing changes
Arteriolosclerosis - Accentuated light reflex: 'silver wiring' - Arteriovenous crossing changes so nipping - Focal arteriolar narrowing
Changes do not significantly correlate with hypertensive control
Common
What are features of Accelerated hypertension/ malignant hypertension
Recent, often severe, elevation in baseline BP associated with target organ damage: CNS (including eye), CVS and renal system
Medical emergency
Due to damage (fibrinoid necrosis) of small arteries, arterioles and capillaries
due to increased permeability from fibrinoid necrosis causing leakage from damaged blood vessels causing Nerve fibre haemorrhages (flame-shaped) or Exudates e.g. macular star
Retinal ischaemia / infarction - Cotton wool spots
Disc oedema
Rare
What is an aneurysm?
pathological dilatation of a blood vessel
Key features of Retinal Macroaneurysm?
Hypertension
Arterial disease
Bifurcations of arterioles
Leakage, retinal oedema and exudate
May be asymptomatic
What is Transient retinal ischaemia: amaurosis fugax?
fleeting loss of vision, A form of "transient ischaemic attack
Sx of Transient retinal ischaemia?
transient loss of vision
typically all or part of their vision
returns to normal after a few seconds or minutes.
What is Transient retinal ischaemia an important indicator of?
Systemic vascular disease
Carotid artery disease
Retinal emboli
Giant cell arteritis
What does Transient retinal ischaemia increase risk of?
CRAO or BRAO, cerebrovascular accident (CVA)
What are the 2 types of Anterior ischaemic optic neuropathy (AION)?
Arteritic = inflammation of ciliary arteries or Non-arteritic = embolic /atherosclerotic/ thrombotic occlusion
AION Clinical Features
Sudden painless profound loss of vision
> 60 yrs
Initially unilateral, May be preceded by amaurosis fugax
Unilateral pale swolen optic disc
APD
Profound visual field loss
Later optic atrophy
Key features of Non-arteritic AION?
No other symptoms,
Typically unilateral
Some recovery possible
PHM: vascular risk factors
Untreatable
Key features of arteritic AION?
Symptoms of Giant Cell (Temporal) Arteritis
95% bilateral if not treated
Recovery rare
Urgent treatment of underlying vasculitis is essential
What is an embolus?
an abnormal mass/particle that travels through the bloodstream and is capable of blocking a blood vessel distant from its point of origin
Origin of a Retinal artery emboli?
anywhere between heart and eye
Key features of Retinal artery emboli?
May be transient - platelet embolus
May be permanent and lodge in retinal arteriole, calcific / cholesterol embolus.
Often difficult to see
What is Retinal Arterial Occlusion?
Abrupt cessation of blood flow through a retinal artery/arteriole sufficient to cause inner retinal ischaemia
central retinal artery is typically thrombotic or embolic
thrombotic
branched retinal artery is typically thrombotic or embolic
embolic
Retina Arterial Occlusion: Risk factors
History of amaurosis fugax / retinal emboli
Smoking
Hypertension,
Diabetes mellitus
Hyperlipidaemia,
Obesity
Known cardiovascular disease
Giant cell arteritis
RAO: Clinical Features?
Sudden profound painless loss of vision (6/240 or worse). Whole field (CRAO), Part field (BRAO), Central sparing if intact CilRA
Pupils: - APD (CRAO) - RAPD (BRAO)
Ophthalmoscopy:
Inner retinal oedema
'Cherry Red Spot' for 4 - 6 weeks
Sluggish / segmentation of arterial blood flow
Retinal atrophy
Disk pallor
No recovery
Retinal arterial occlusion management?
Immediate
try to re-establish circulation
Rebreathing CO2 from bag
Lower intraocular pressure
Digital massage of globe
Immediate referral to eye clinic (see that day)
Lower intraocular pressure
Anterior chamber paracentesis
Look for underlying causes
Medical examination of heart and carotid arteries
Treat underlying disorders