BIOS 3755- Human Physiology Exam 3
1/146
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
147 Terms
how much blood does heart pump
60 mL per contraction
~54 gal per hr
components of blood
plasma, wbc, rbc, platelets
plasma: function and components
Transports carbon dioxide, digested food, urea, hormones and heat energy
pt, nutrients, inorg subst, metabolic waste, hormones
hematocrit
% of blood that is RBC; 45%
how much % is plasma in blood
55%
what is the "buffy coat" in blood
leukocytes and platelets
rbc made from
bone marrow`
rbc properties (4)
no nucleus
120 day life cycle
bilirubin made when broken down
most fe recycled back to bone marrow
low rbc means ______ which includes (4)
anemia:
fe deficiency
bone marrow failure
hemorrhage
blood cell production issue
sickle cell
abnormal hemoglobin; sickle shape causes blockage to blood flow
treatment for sickle cell (5 steps)
1. bone marrow makes diseased hemaglobin
2. stem cells extracted
3. stem cells modified (silence BCL11A gene)
4. new stem cells
5. production of healthy hemaglobin
wbc made in ___________; do they have a nucleus?
bone marrow;
have nuclei
circ sys: 3 components
fluid for nutrient/gas exchange
tubes for transport (vessels)
musc pump for movement
3 types of circulatory systems
none, simple (open), closed
how eukaryotic cells obtain O2 and expel CO2
1. ventilation
2. gas exchange
3. circulation
4. cellular respiration
open circ (3)
blood bathes organs directly (circ fluid IS interstit fluid)
may or may not exchange o2; has o2 carrying pigment but not in cells, free in hemolymph
low Pressure = less e cost
insect circ sys does NOT have
o2 exchange
closed circ sys (3)
blood is confined to vessels
transports co2 and o2
high pressure = more e cost
annelid (worm) circ sys is ... and has ....
closed circ sys; mult hearts and no lungs
single circulation
bony fishes, rays, and sharks
2 chambered heart.
blood passes 2 cap beds (gill and systemic) before returning to heart
drawbacks of simple circulatory system
after passing through gill caps, blood enters system caps slowly; fish cannot handle high bp
do some fishes have lungs?
yes (lungfish); direct return of blood to heart from lung
amphipians hearts have ...
3 chambered-hearts (2 atria, 1 ventricle)
in amphibians, the pulmonary and systemic circuits are
partially separated
in amphibians, the these fluids mix in the ventricle
oxygenated and deoxygenated blood
what does the pulmonary vein return to in amphibians?
left atrium
reptiles heart
still 3 chambers, but partially divided ventricles w septum
how does the septum in reptiles make their heart better than amphibians
improves separation of pulmonary and systemic circulation
birds/mammals heart
4 chambers. septum completely separates ventricle into 2 parts.
pulmonary and systemic circ completely separated!
advantage of bird/mammal heart
high rate of oxygen delivery to tissues/ more activity
which animals have double circulation
amphibians, reptiles, and mammals
where does oxygen-poor blood flow through to pick up O2 through the lungs?
the pulmonary circuit
amphibians have what kind of circuit?
pulmocutaneous circuit (skin)
What is the adaptive advantage of having a double circulation system and three-chambered heart of amphibians, over the single circuit and two-chambered heart of fish?
A. There can be capillary beds in both the respiratory organ and body systems.
B. The additional chamber increases the pressure of blood flow to the respiratory organ.
C. Oxygenated blood can return to the heart for additional pumping before going to systemic flow.
D. Oxygenated blood is kept completely separate from deoxygenated blood in the heart.
C. Oxygenated blood can return to the heart for additional pumping before going to systemic flow.
pulmonary circuit
flow from/to lungs
systemic circuit
flow to/from rest of the body
capillaries connect
arterioles and venules
Flow of blood in the cardiovascular system is (11 parts)
r ventricle> pulmonary artery> cap of r&l lung> pulmonary vein> l atrium> l ventricle> aorta> cap of head/forelimbs> cap of lower limbs> superior vena cava> inf. vena cava> r atrium
do veins have high or low pressure
low bp; carry blood from capillaries
why do cap. have such low bp?
to permit for gas/nutrient exchange b/t blood and interstitial fluid
Veins always carry deoxygenated blood.
True or False?
False! Veins carry blood to the heart w or w/o oxygen
mammalian hearts are 2 pumps operating in _
parallel
which side of the heart receives venous blood from systemic circulation? from lungs?
right side; ;left side
what kind of valves in human heart
1 way valves. prevent backflow
blood flow rate changes depending on circumstances. t or f
true
systole and diastole
Contraction and relaxation of the ventricles
what is the function of the "one-way" valves in the heart?
separates the atria and ventricle;
prevents backflow of blood into atria and continues in one direction
cardiac cycle steps
1. AV entrances are open/ SL valves are closed (atrial and ventricular diastole)
2. atrial systole; ventricular diastole
3. AV are closed/ SL valves are open. (atrial diastole, ventricular systole)
There are no valves at the point where venous blood flows into the atria.
T or F
true
atrioventricular and semilunar valves
separates atria from ventricle
separates ventricles from arteries
coronary skeleton function
supports one-way valves and helps w conduction of action potentials
what initiates depolarization in heart? also called pacemaker of heart
SA node
Electrical pathway of the heart
SA node, AV node, Bundle of His, Purkinje fibers
the sa node depolarization propogates from
bundle of His along Purkinje fibers in ventricles
skeletal vs cardia musc graph
cardiac: has plateau after AP!
repolarization is much slower due to fibers propagating. prevents tetany
how does the heart avoid tetany (musc. spasms)?
repolarization happens much more slowly
AP in heart diff from other cells (SA node pacemaker potential)
depolarization from Ca2+ influx rather than Na+, efflux K+. though Na+ does enter before Ca2+, it is Ca2+ causes dep
Na+ channels open at ~60mV
K+ diminishes as MP rises
SA node depolarize to threshold
during _ in heart, dep cannot occur
absolute refractory period
in heart, plateau phase is longest for fibers that contract _
ventricles
this is bc prolonged contractions in ventricles are more fatal than those in atria
Why is there a plateau of membrane potential despite Ca and K entering and exiting?
...
what can a change in ECG pattern mean? (3)
cardiac rhythmic disturbances
inadequate coronary artery blood flow
electrolyte disturbances
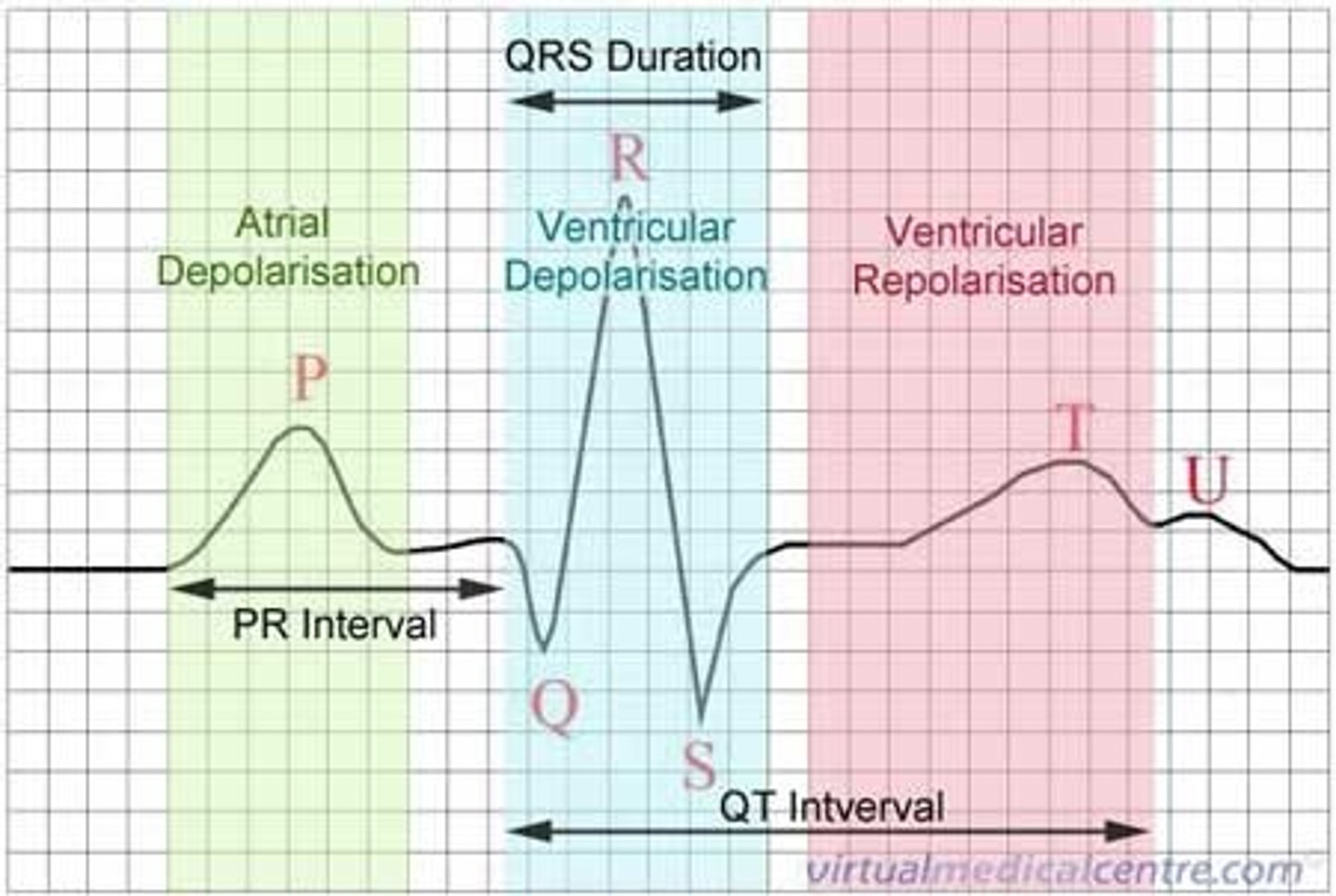
EKG 3 parts
P wave, QRS complex, T wave
what sets rate and timing for cardiac musc contraction
pacemaker cells in SA node. initiate dep
intercalated discs def and f(x)
specialized connections between myocardial cells containing gap junctions and desmosomes
branching network. allows pulse to spread quickly
does the AV node start contraction immediately after SA node?
no, slightly delayed so that the ventricles can fill up
electrical activation of heart pathway: (5 steps)
1. signal starts at SA,
2. spread to both atria, atria contract,
3. signal delay at AV
4.signal spread down fibers to apex then reach ventricles, ventricles contract
5. ventricles relax
atrial excitation (beginning and ending)
begins: SA node
end: AV node
ventricular excitation (beginning and ending)
begins: atrial relaxation
ends: ventricle contracting
vagus nerve vs accelerator nerve
para, symp
baroreceptors
arterioles constrict, veins constrict, cardiac output constrict
cardiac acceleration (4 steps)
sympathetic ns
epi/norepi -> B1 receptor -> Na and Ca influx increased, dep -> increased HR
cardiac deceleration (5 steps); what system is it apart of
parasymp ns
ACh -> muscarinic receptors -> K efflux increased and Ca influx decreased -> increased time to depolarize -> HR decreased
Frank-Starling Law
The greater the stretch, the stronger is the heart's contraction. This increased contractility results in an increased volume of blood ejected (Increased SV)
more stretch -> more force
fetal heart: 2 bypasses due to no lungs
foramen ovale: allows deoxy blood to flow directly from left to right atrium
ductus arteriosis: connects pulmonary artery to aorta
physical differnce bt arteries and veins
thicker elastic layer in arteries
Do veins or arteries have valves?
veins
thinner walls
low pressure/resistance
are veins or arteries thicker
arteries
also more elastic
high pressure
blood velocity in diff vessels
artery > vein > capillary
total area diff in vessels
cap > vein > artery
BP in diff vessels
artery > cap > vein
role of musc in regulating BP
SMOOTH musc
contract/relax
local vasocontraction
same volume of blood in smaller cross sectional area will increase speed and bp
local vasodilation
same volume of blood in larger cross sectional area will decrease speed and bp
what brings back blood in veins to heart?
skeletal musc and valves!
neg pressure applied by heart
circulating blood pushing in the back
what system controls blood flow to specific tissues? what are they called and where are they located? how do they work?
autonomic ns
smooth muscles calles precapillary sphincters. in arterioles
These muscles can constrict or relax, either completely cutting off circulation or flooding specific tissues with blood.
Can respond immediately to physiological demands placed on the body
what happens when BP drops?: kidneys
kidneys release renin -> renin circulation activates angiotension -> vessels constrict
what happens when BP drops?: hypothalamus
stretch sensors decrease firing -> hypothalamus release vasopressin -> vessels constrict ->
what causes BP to keep falling
decreased blood to tissues -> wastes accumulate -> vessels widen
Poiseuille's Law
-calculates rate of flow through a pipe of confined space (laminar flow)
Q= (πr^4 ∆P)/8ηL
η: viscosity of the fluid
Q: flow rate (volume flowing per time)
ΔP: pressure gradient
r: radius of tube
L: length of tube
Thus resistance is inversely proportional to the fourth power of the radius (i.e., reduction of vessel diameter by a factor of 2 causes a 16-fold increase in resistance!)
3 types of capillaries
Continuous
Fenestrated
Sinusoidal
continuous cap: permeability, location
lowest permeability
found in muscle, brain, lungs, connective tissues, exocrine glands
fenestrated cap: permeability, location
intermediate permeability, found in kidneys, intestines, endocrine glands
has pores
sinusoidal cap: permeability, location
very permeable, found in liver, bone marrow, spleen, lymph nodes, adrenal cortex
paracellular gap
what determines permeability of capillary beds?
junctions bt endothelial cells
what makes capillaries leaky
hydraulic pressure
forces fluid out arteriole end
Large molecules remain, increasing osmotic concentration of blood; coupled with dropping blood pressure in the capillary as it progresses towards the venule results in a net inward flow of fluid.But, volume out is slightly greater than volume in!
at arterial end of capillary, BP and osmotic P
BP > osmotic P
fluid flows out cap into interstit. fluid
at venule end of cap: BP and osmotic P
BP < osmotic P
fluid flow from interstit. fluid to cap
direction of osmotic pressure in capillaries
increases from arteriole to venule
what happens to excess lymph
The fluid (lymph) which accumulates in the interstitial spaces is collected into small ducts (lymphatic vessels). These drain into larger lymphatic ducts which merge into large thoracic duct that is connected to vena cava adjacent to heart (returning lymph to general circulation)
lymph carries _ to _
pathogens to nodes
where they are destroyed or stimulate production of antibodies to fight infection