Periodontal Anatomy and Occlusion – Vocabulary Flashcards
1/68
Earn XP
Description and Tags
Vocabulary flashcards covering key terms from periodontal anatomy and occlusion concepts.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
69 Terms
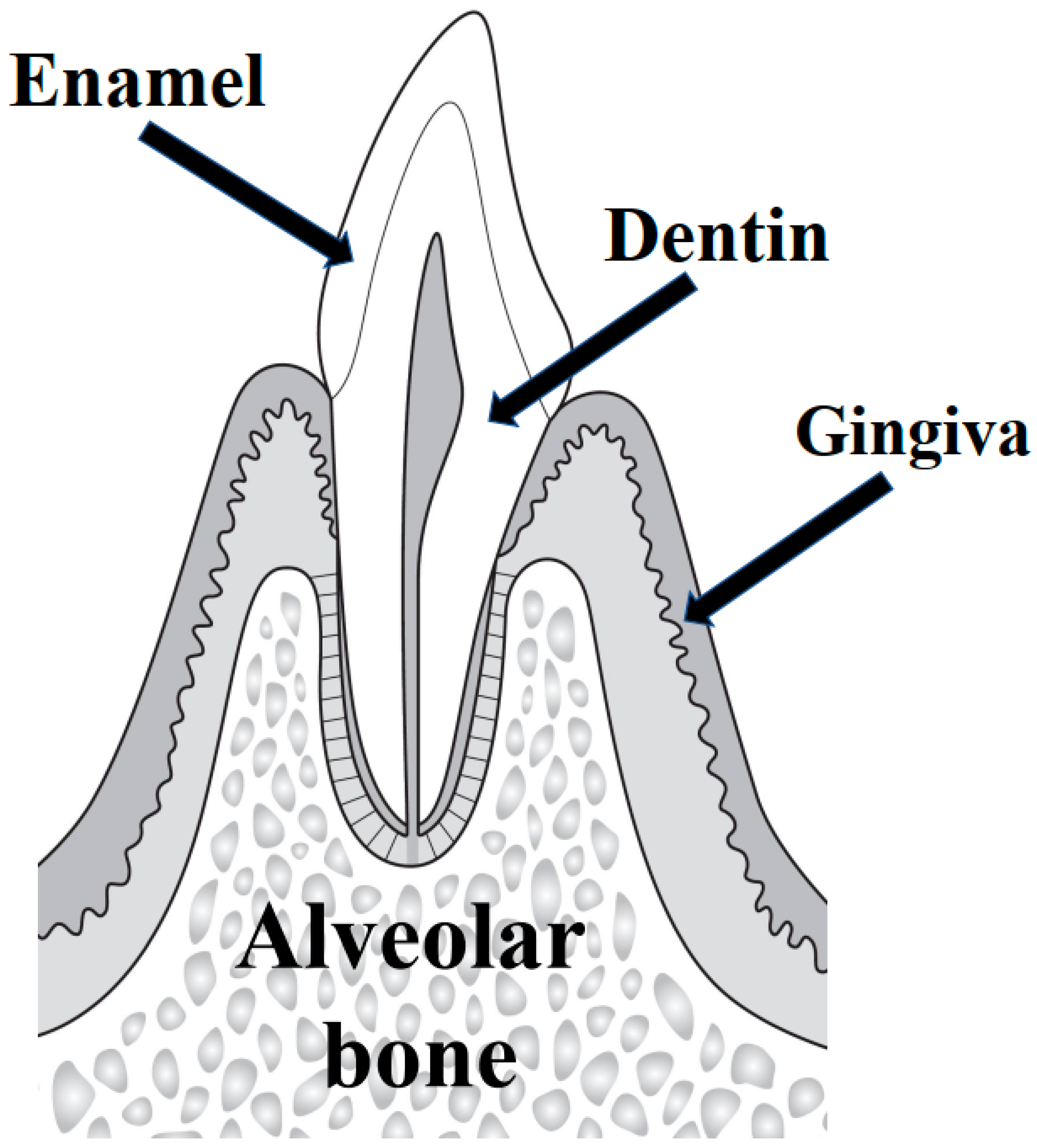
Alveolar bone
The bone that surrounds tooth roots, forms the tooth socket, and provides support for teeth with the periodontal ligament.
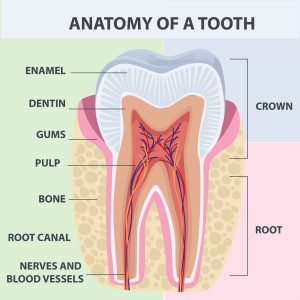
Tooth root surface
The portion of a tooth root covered by cementum where the periodontal ligament attaches.
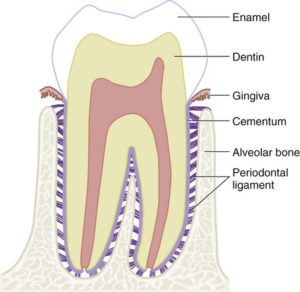
Periodontal ligament (PDL)
Fibrous connective tissue between cementum and alveolar bone that supports the tooth; cushions forces and contains Sharpey’s fibers. It is also apical, oblique, horizontal, alveolar crest, and transseptal.
Gingiva
The gum tissue around teeth, comprising free gingiva and attached keratinized gingiva; forms the gingival sulcus.
Free gingiva
Gingiva surrounding the tooth but not attached to bone; forms the gingival sulcus.
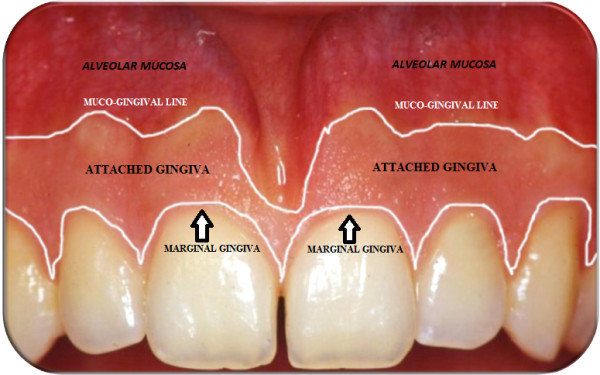
Attached gingiva
Keratinized gingiva tightly bound to underlying bone, extending from the free gingival margin to the mucogingival junction.
Gingival sulcus
The shallow crevice between the tooth surface and the free gingiva that can be probed.
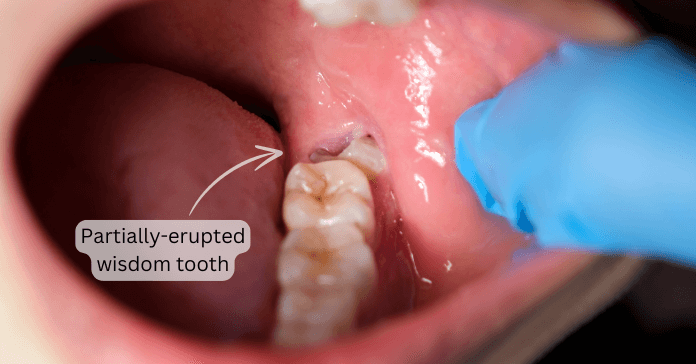
Operculum
Is a flap of gingiva over the last molar that can be inflamed
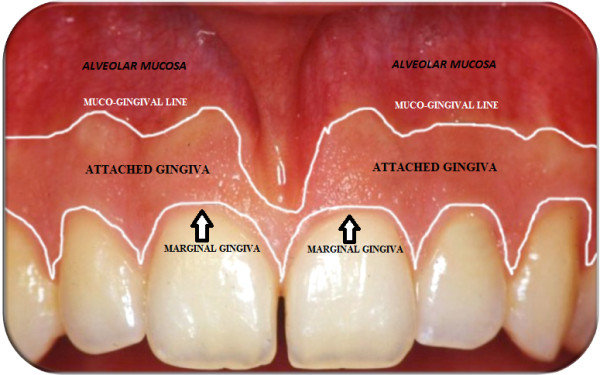
Gingival margin
The edge of the gingiva closest to the tooth crown.
Functions of healthy gingiva
Support
Protection
Esthetics
Phonetics
Phonetics
Affected by open embrasures that allow air to “whistle” through spaces
Anatomy of diseased periodontium
Gingivitis
Periodontists: bone loss
Gingival recession
Interdental papilla
Gingival tissue between adjacent teeth.
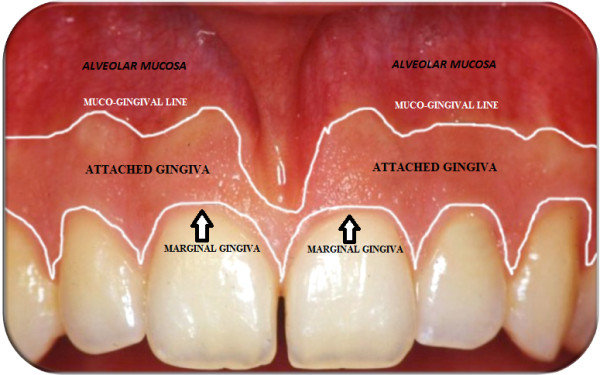
Zone of attached gingiva
The portion of gingiva that is firmly bound to underlying bone and does not move with the mucosa.
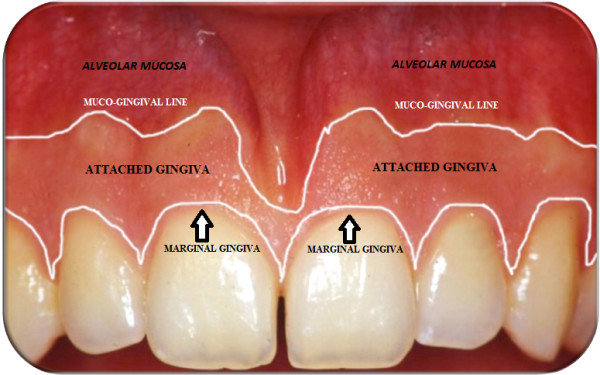
Mucogingival junction
The boundary between keratinized attached gingiva and nonkeratinized alveolar mucosa.
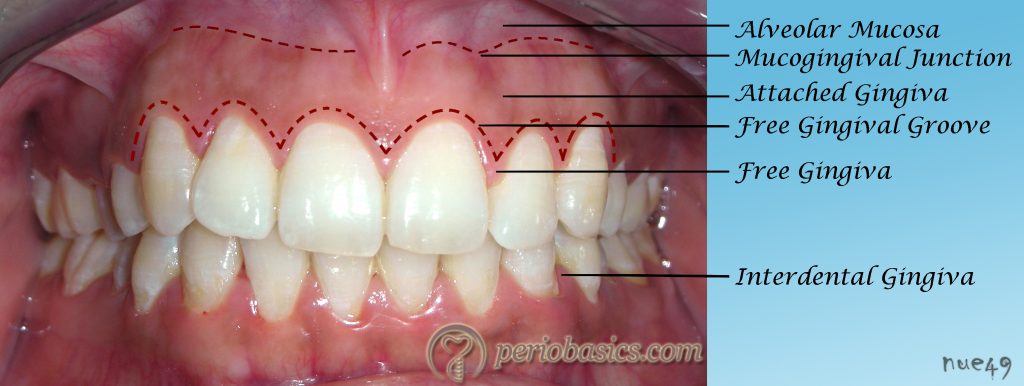
Free gingival groove
A shallow groove marking the boundary between free and attached gingiva.
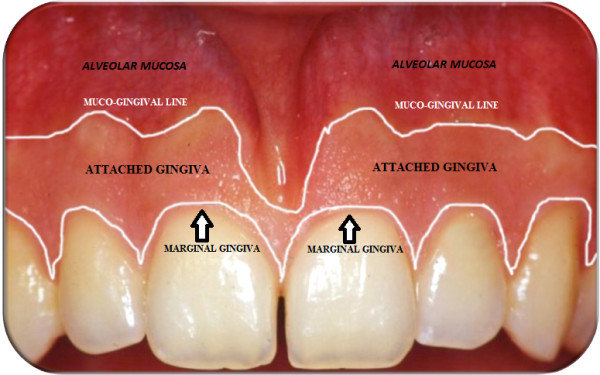
Alveolar mucosa
Movable, nonkeratinized mucosa located apical to the attached gingiva.
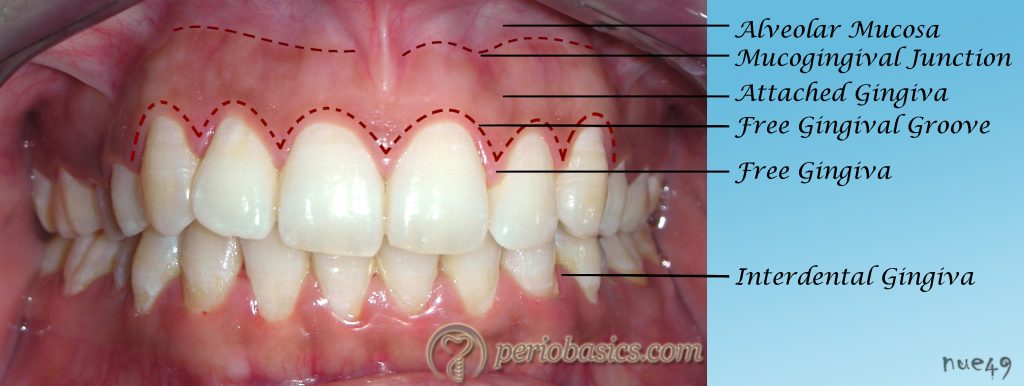
Zones of gingiva
Regions including alveolar mucosa, zone of attached gingiva, gingival groove, gingival margin, and interdental papilla.
Gingivitis
Inflammation of the gingiva; mild cases show slight bleeding on probing (BOP).
Periodontitis
Inflammation with bone loss around teeth, evidenced by radiographic bone loss.
Gingival recession
Apical migration of the gingival margin; may include gingival clefting.
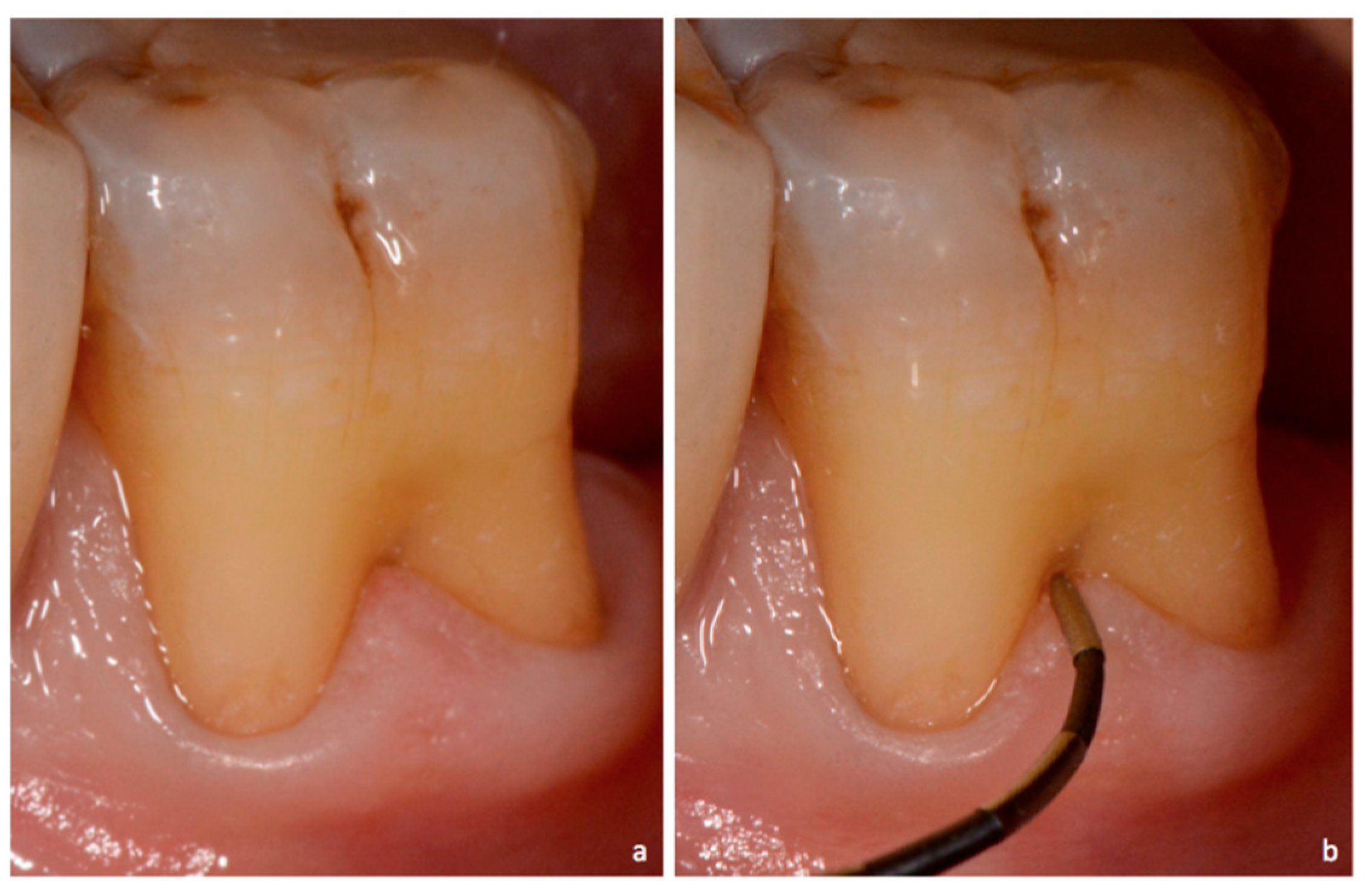
Furcation involvement
Involvement of the furcation area on multi-rooted teeth; assessed with a furcation probe and can harbor calculus.
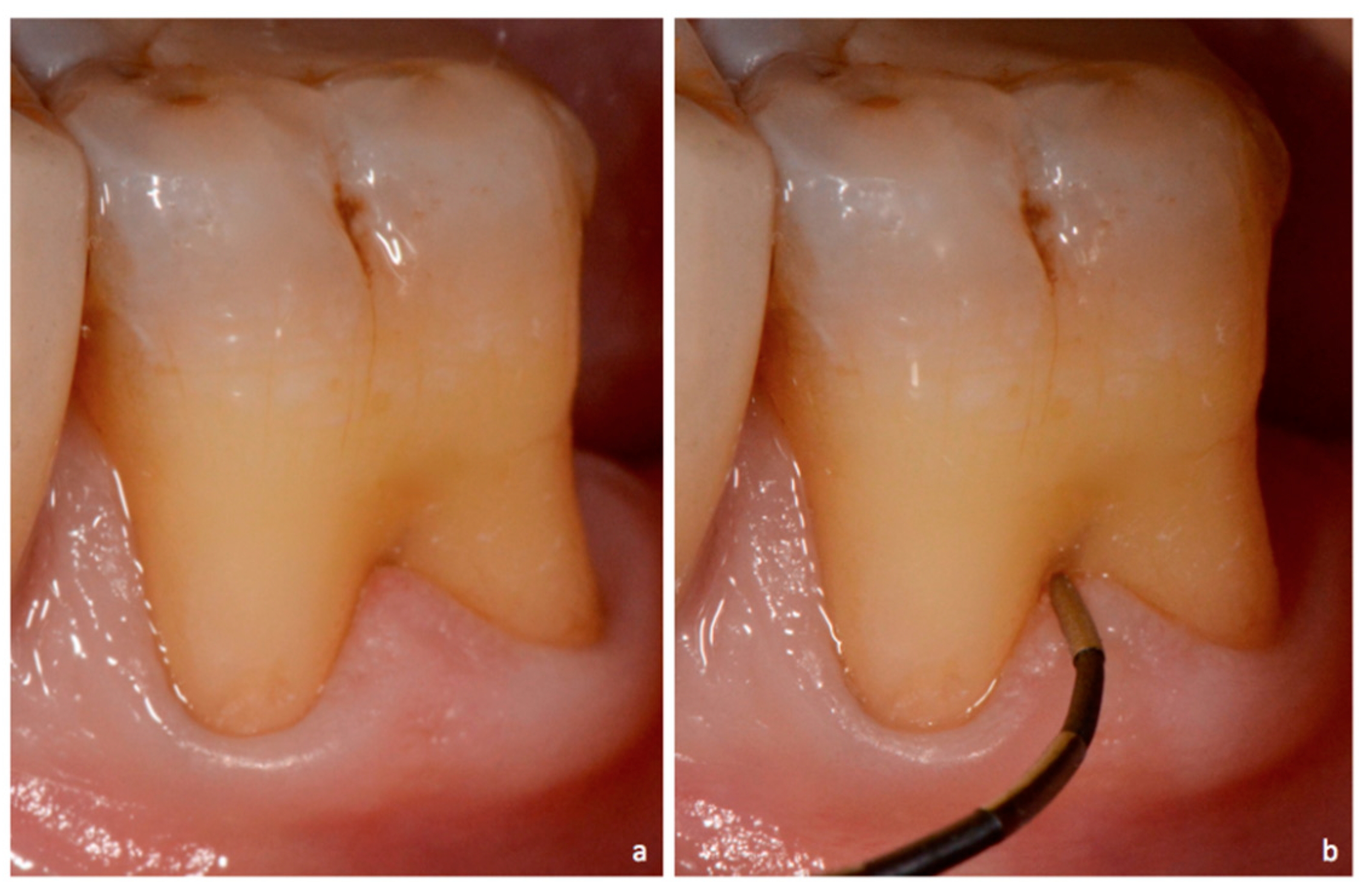
Furcation probe
A specialized periodontal probe used to assess involvement of the furcation area. This can be with facial/lingual and proximal.
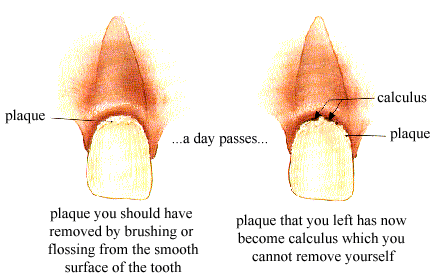
Plaque vs Calculus
Plaque is a soft biofilm on teeth; calculus is mineralized plaque that can form supragingival or subgingival. Difficult areas to clean are CEJ,Concavities, Furcations, Contours at the line angles.
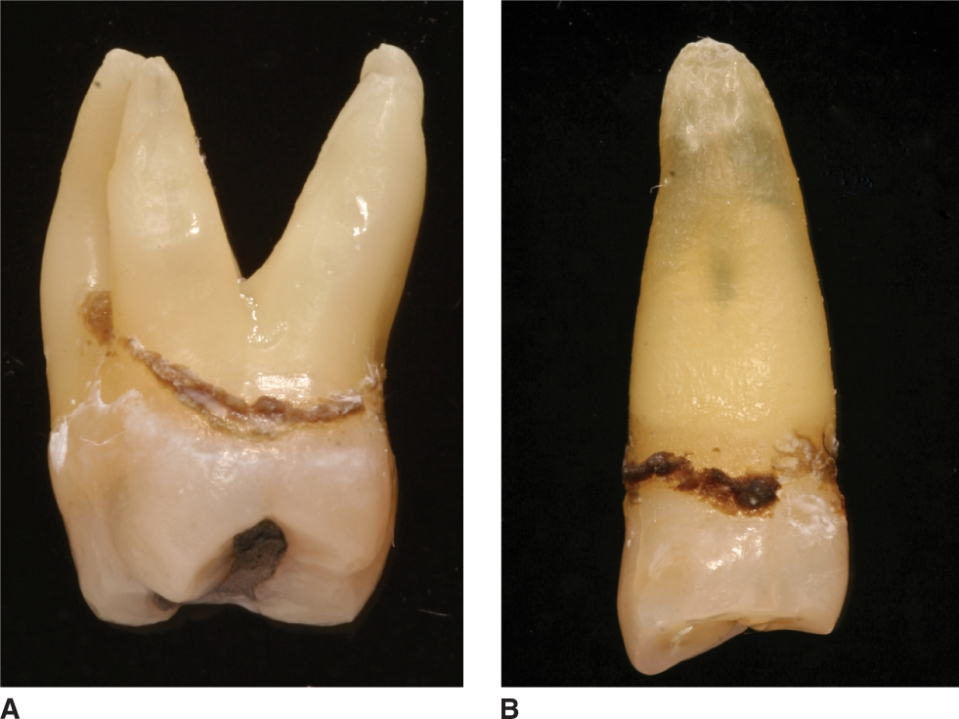
Subgingival calculus
Calculus located below the gingival margin, often harder to remove.
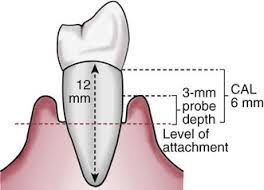
Clinical Attachment Loss (CAL)
Distance from the CEJ to the bottom of the pocket; measures loss of periodontal support.
Bleeding on probing (BOP)
Bleeding elicited by periodontal probing; indicator of gingival inflammation.
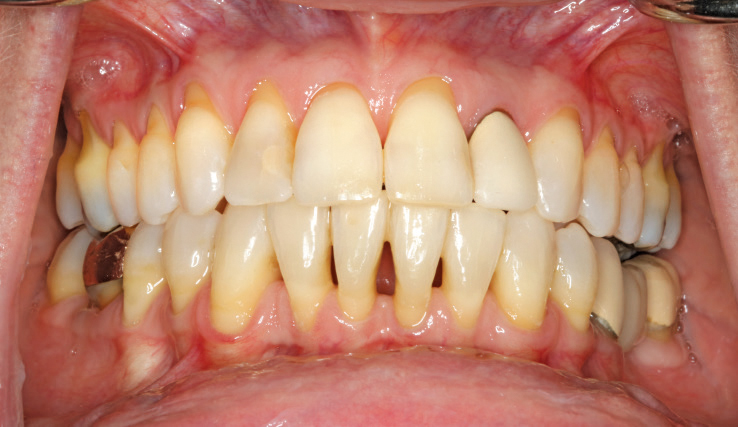
Lack of Attached Gingiva
Insufficient or absent attached gingiva, a mucogingival defect.
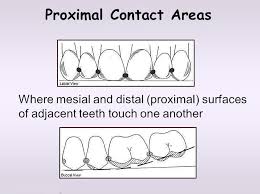
Proximal contact areas
Areas where adjacent teeth touch; influence embrasures and plaque control.
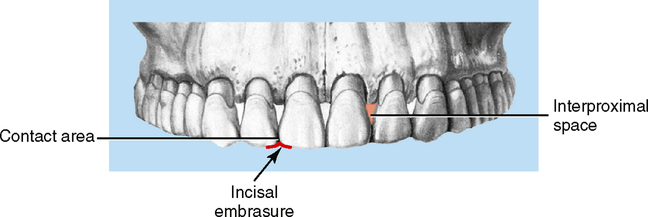
Interproximal spaces
Spaces between adjacent teeth, which may be open or closed depending on contact points.
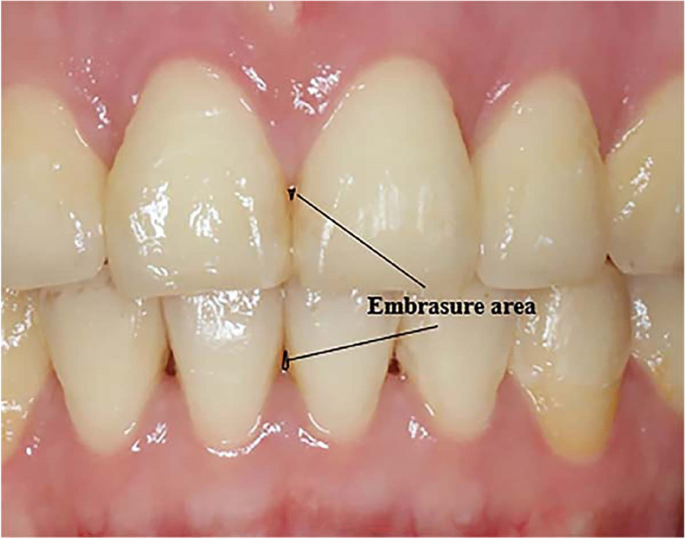
Embrasures
Spillways around contact areas between teeth; affect self-cleaning and esthetics.
CEJ (Cementoenamel junction)
The junction where enamel meets cementum on a tooth; used as a reference point for CAL.
Cementum
Thin calcified tissue covering the root; provides attachment for PDL fibers.
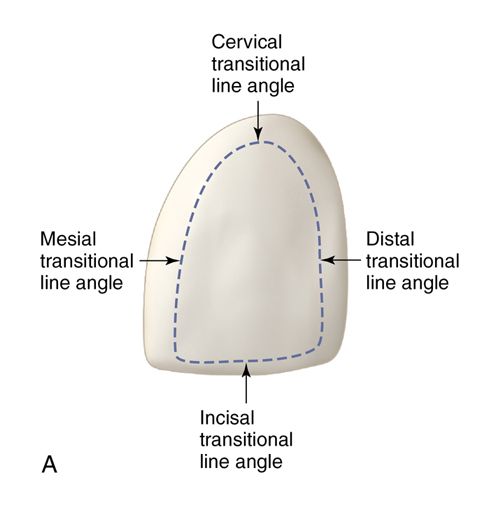
Facial Line Angles
The lines are more prominent than lingual line angle of the same teeth. Overall we got different line angles.
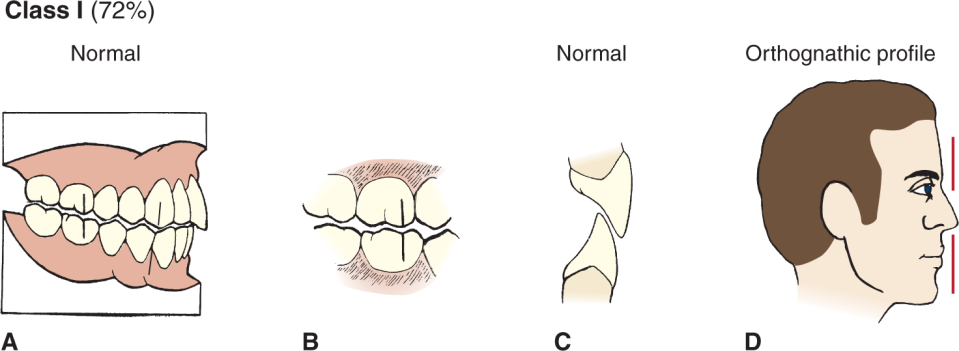
Ideal Class I Occlusion (Normal or Neutroclusion)
This is when both the maxillary teeth have good alignment. Normal bite to say. But is the front teeth stick out to much that is an over jet.
Crowding
The most common contributor to malocclusion, one or many teeth are involved in misplacement
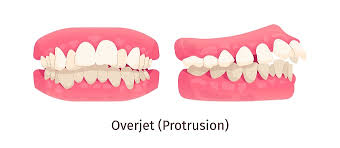
Overjet
The maxillary incisors are sticked more out so its not touching the mandíbulas incisors
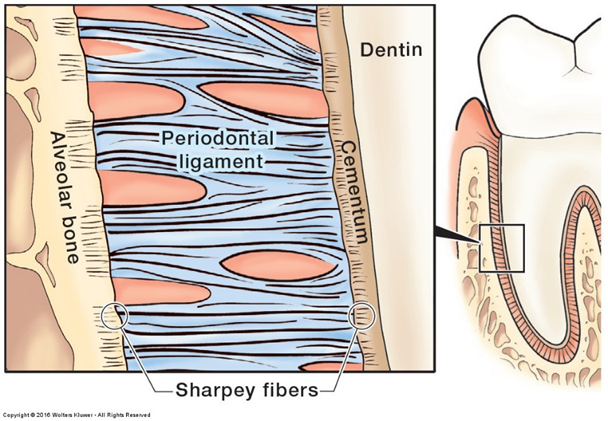
Sharpey’s fibers
Ends of periodontal ligaments inserting into cementum and bone to suspend the tooth.
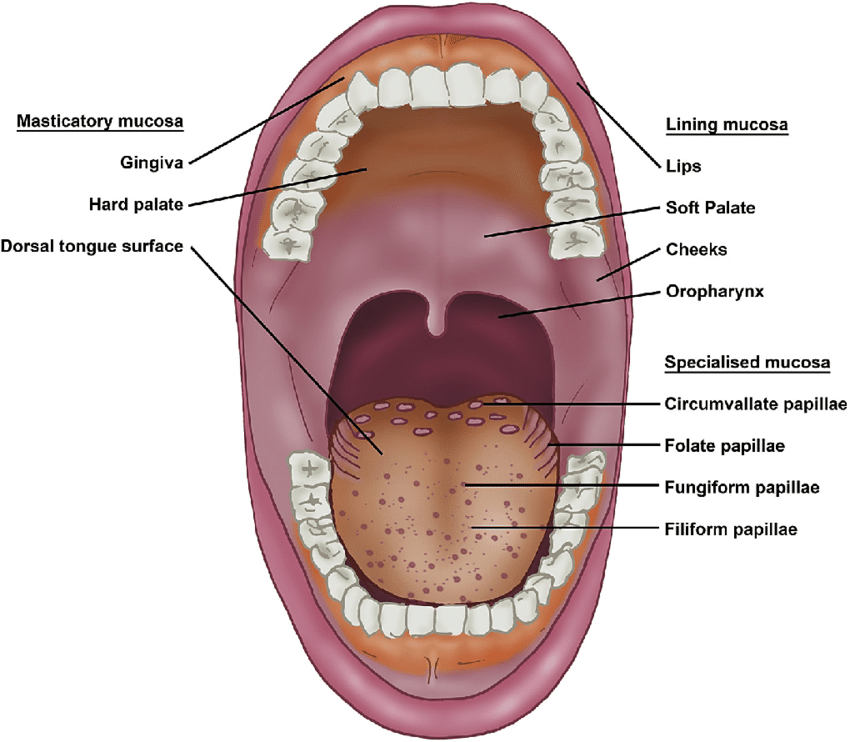
Masticatory mucosa
Keratinized mucosa including gingiva and hard palate that withstands mastication.
Articulations
How the entire masticatory system (the jaws, teeth, and supporting structures) act ask a complete single entity like chewing or breakdown of foods.

Centric Relation
A stable bone to bone (maxillary and mandible) relationship that occurs when the mandible condyles are in their most superior and anterior position within the temporomandibular joint (TMJ)
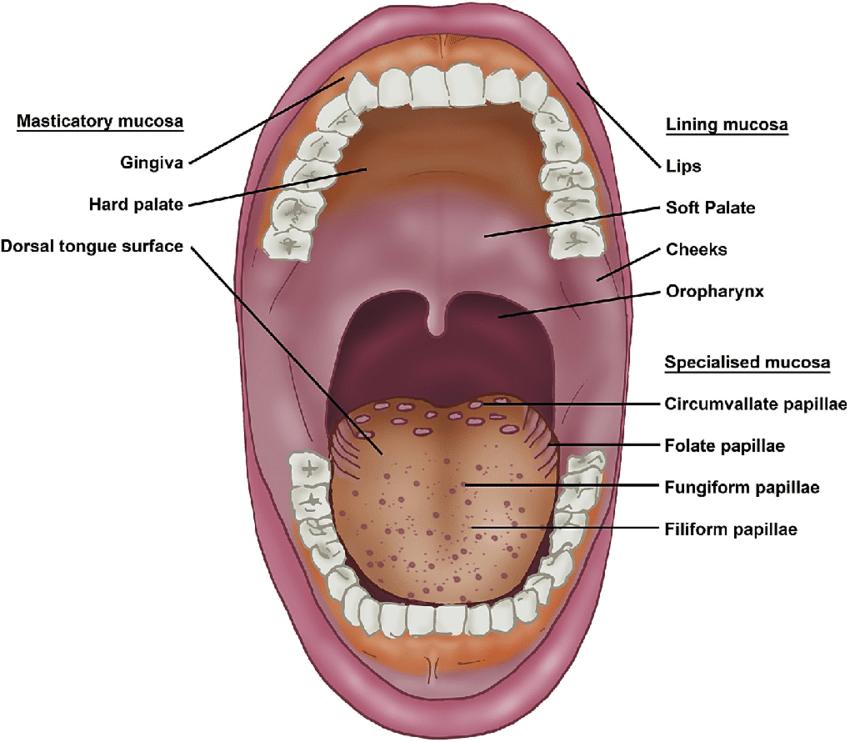
Lining mucosa
Nonkeratinized mucosa lining lips, cheeks, floor of mouth, and other areas.
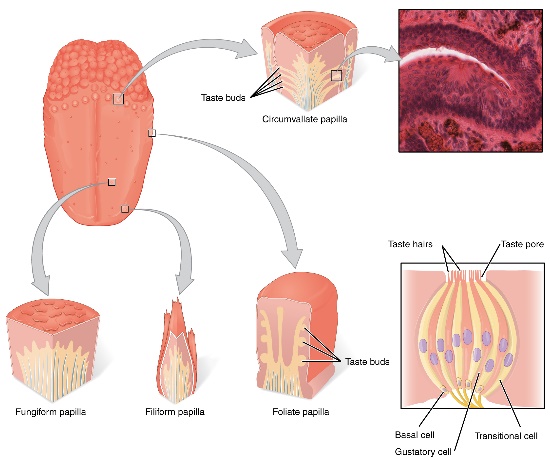
Specialized mucosa
Mucosa on the dorsum of the tongue containing taste papillae.
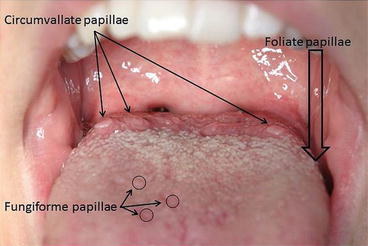
Circumvallate papillae
Large taste papillae located at the posterior part of the tongue.
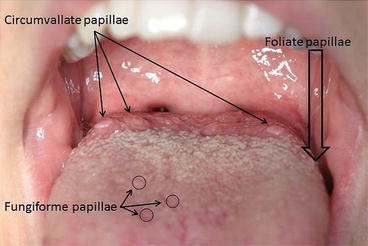
Filiform papillae
Thread-like papillae covering most of the tongue; do not contain taste buds.
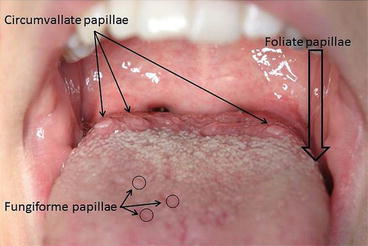
Fungiform papillae
Mushroom-shaped taste papillae scattered on the tongue.
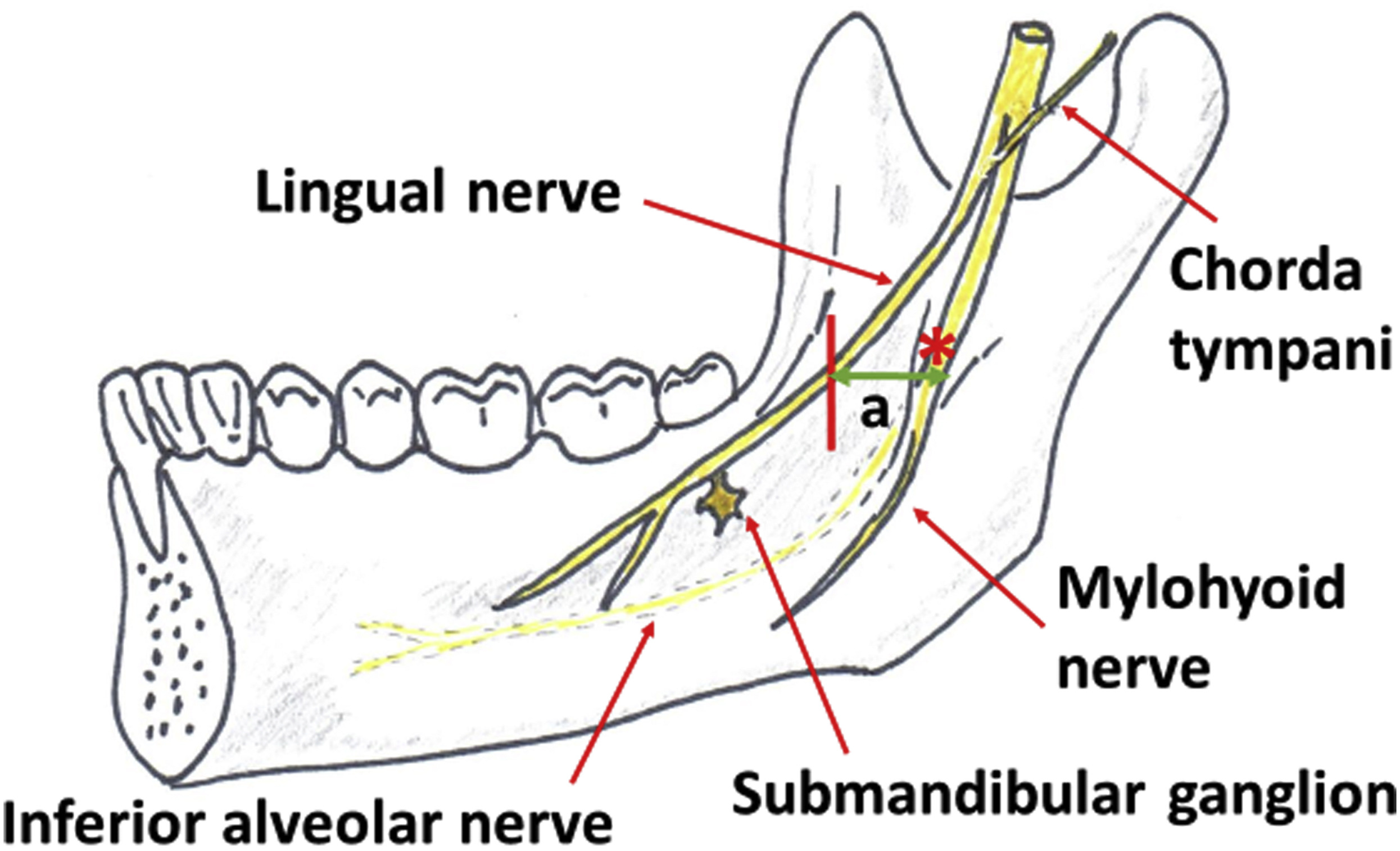
Lingual nerve
Branch of the mandibular nerve providing sensation to the tongue.
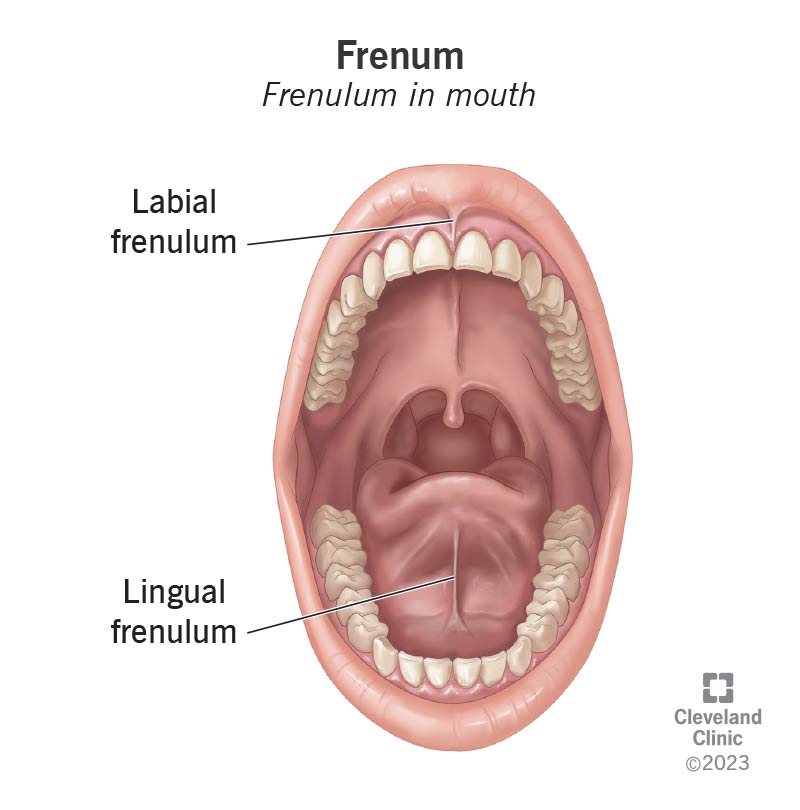
Frenum
Fold of tissue attaching lips or cheeks to the gingiva (labial or buccal frenum).
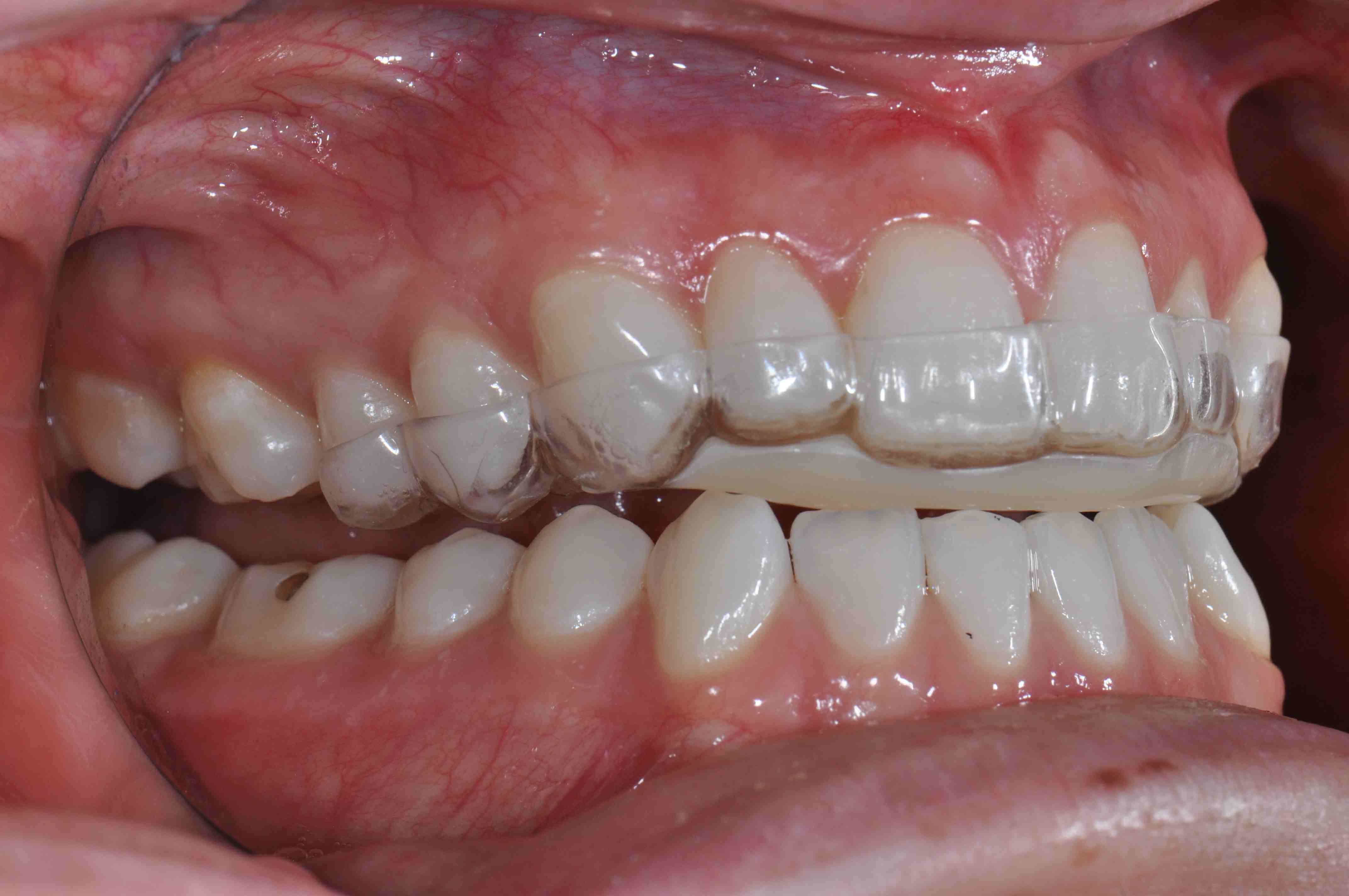
Occlusal device (bite plane)
An appliance worn to reduce tooth wear and modify occlusion (night guard).
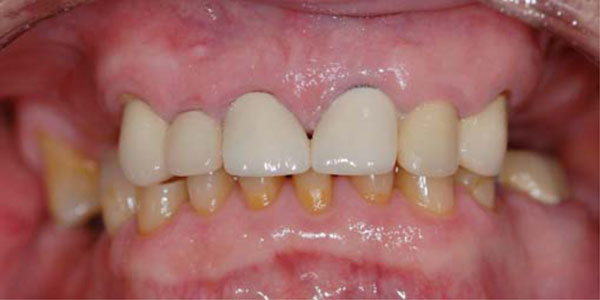
Maximal intercuspal position (MIP)
The position of maximum tooth contact when the jaws are in centric occlusion.
overbite
this is an icreased vertical overlap of the maxillary incisors
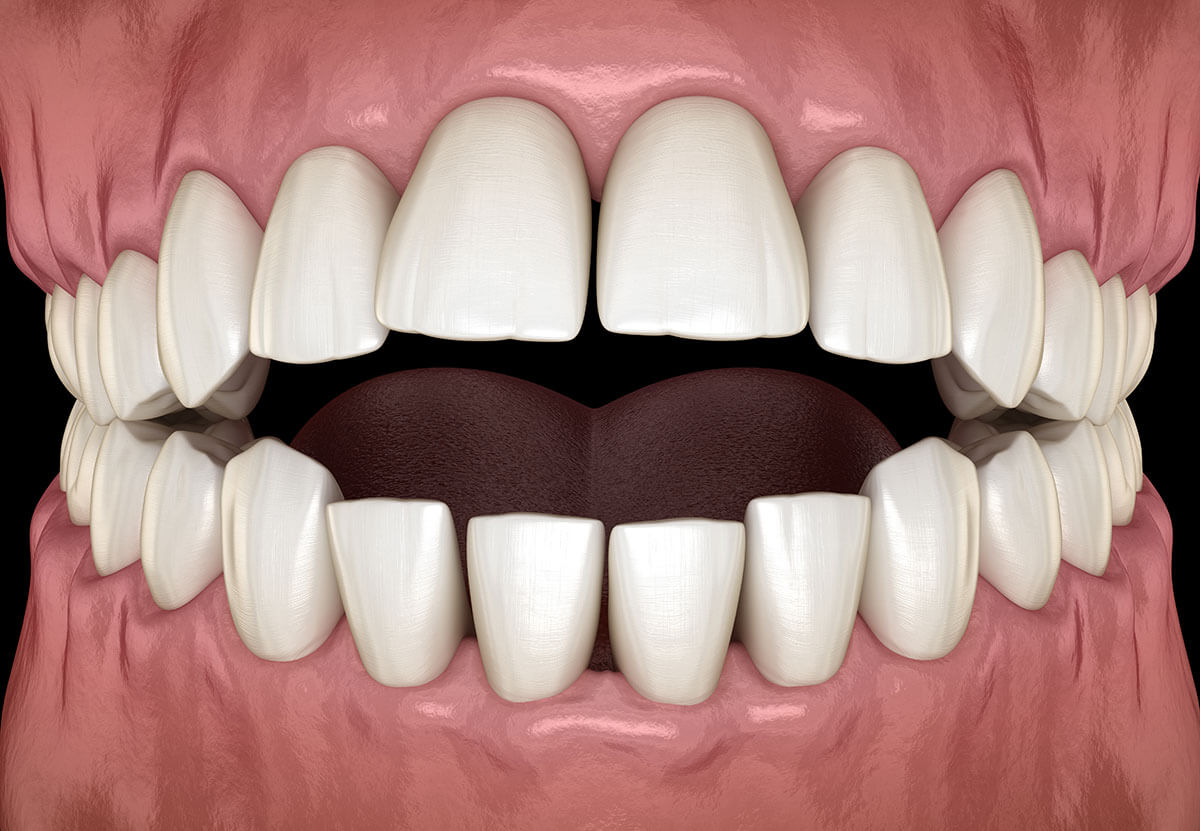
open bite
a lack of vertical overlap of the maxillary inciors results in an opening of the anterior teeth when occluded
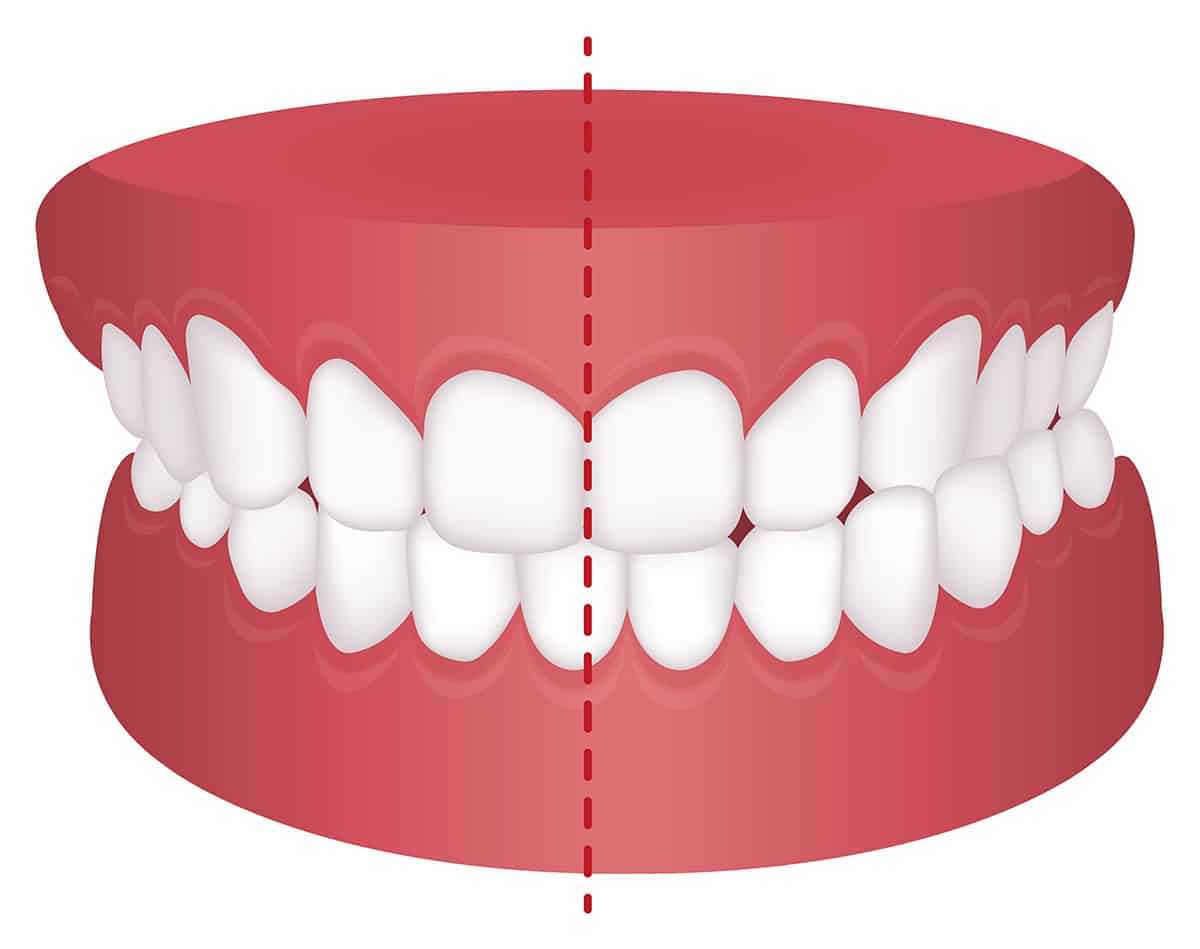
cross-bite
a tooth is not properly aligned with its opposing tooth
How Malocclusions are caused?
The most common cause is disproportion in size between the jaw and teeth or between the upper and lower jaws. But its also cause by genetics/hereditary
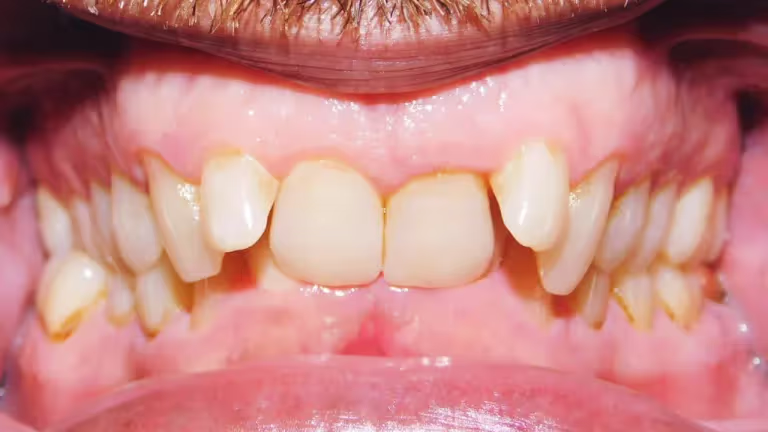
Class II Malocclusion (Distal Occlusion)
your jaw is back (retro) also your central incisiors are in but the laterals are out
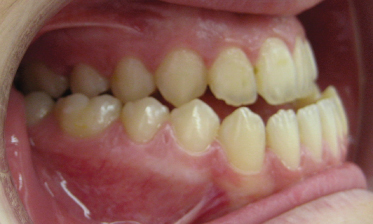
Class III Malocclusion
This is when your jaw is sticked out
Functional Movements: Chewing and Swallowing
Incising
Masticating (Chewing)
Swallowing
Examples of parafunctional contacts
clenching
bruxing (teeth grinding)
biting on pipe stem, pencil, fingernails
cheek biting etc..
overall doing something that your teeth are not made to do
Possible symptoms related to parafunctional contacts
ringing in ears
sinus pain
dizziness
head, neck, and or/back aches
TMJ pain (also from arthritis, injury)
Tired muscles of mastication
sore tooth (sensitive to percussion)
Possible symptoms related to parafunctional contacts
Tooth mobility (fremitus)
Tooth wear (flat, shiny facets)
Widened periodontal ligament
Angular bone loss
Thickened lamina dura (seen on radiographs)
Root resorption
Benefits of orthodontic treatment
Psychosocial problems
Severe malocclusion and dental facial deformities can be a social handicap
Oral malfunction
Malocclusion can compromise all aspects of oral function
Dental disease
****Malocclusion can contribute to dental decay and periodontal disease
Developmental causes of malocclusion
Congenitally missing teeth
Malformed teeth
Supernumerary teeth
Interference with eruption
Ectopic eruption
Periodontal ligament
Composed of fibers that attach to the alveolar bone and the cementum
Provides a hammock that the tooth sits in
Acts as a shock absorber
Socket the tooth sits in is called the alveolus
Sharpey’s fibers--the ends of the collagen fibers from the PDL that are inserted into the cementum on one side and the bone
Periodontl ligaments fibers
Principal fiber groups (5 types):
alveolar crest
horizontal
oblique
apical
interradicular--between roots of multirooted teeth
Periodontal Ligament: Gingival Fiber Groups
Dentogingival (free gingiva)
Alveologingival (attached gingiva)
Circumferential (circular)
Dentoperiosteal (alveolar crest)
Transseptal
Cementum
Thin layer of calcified connective tissue
Covers anatomical root
Provides attachment for periodontal fiber groups
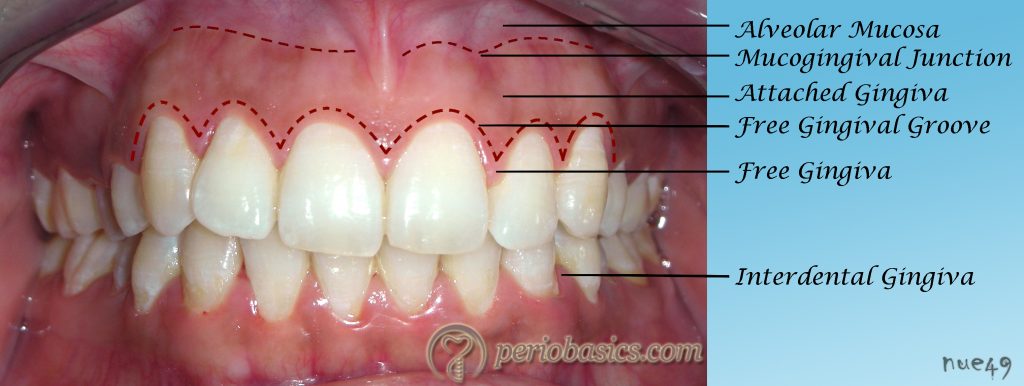
Free Gingival Groove
A shallow linear groove that demarcates the free and the attached gingiva
Can be seen in 1/3rd of teeth with healthy gingiva
Is approximately at the
bottom of the gingival
sulcus
Mucosa
3 divisions or categories
Masticatory
Gingiva and
Hard palate
Lining
Inner surfaces of lips & cheeks,
Floor of the mouth,
Ventral surface of the tongue,
Soft palate, and
Alveolar mucosa
Specialized mucosa:
Dorsum of tongue
Lining Mucosa
Thin, movable, easily injured
Nonkeratinized
Not firmly attached to underlying tissues
Components are the:
Alveolar mucosa
Inside of lips & cheeks
Floor of the mouth
Ventral surface of tongue
Soft palate