respiratory exam 2402
1/71
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
72 Terms
What is the difference between ventilation and respiration?
Ventilation: also known as breathing. allows gas exchange in lungs
Respiration: gas exchange between atmosphere and body cells
What is external respiration?
Ventilation or breathing; allow gas exchange in lungs
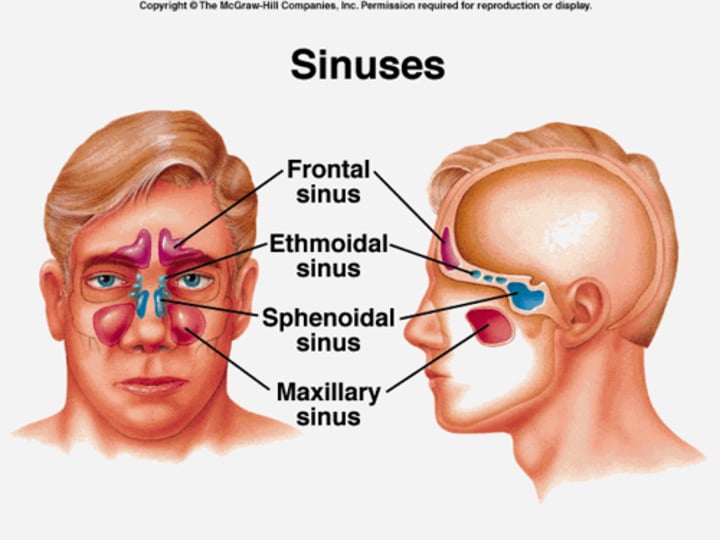
What are paranasal sinuses? Know the facial bone involved.
Air-filled spaces in the maxillary, frontal, ethmoid, and sphenoid bones of the skull
Which laryngeal cartilage is unpaired?
Thyroid (Adam's apple): Largest cartilage; thyroid gland covers lower part. Cartilage more prominent in males.
Cricoid: Below thyroid cartilage
Epiglottic: Central portion of flap-like epiglottis. This is elastic cartilage not hyaline like the other laryngeal cartilages
What helps you hit the high notes when singing?
Larynx: Increase tension of vocal cords
What disorders are considered COPD? Name two of them.
Chronic Bronchitis: long-term inflammation of the bronchi; leads to increased mucus production (cilia does not function correctly anymore); most likely to form from smoker's cough
Emphysema: progressive, degenerative disease; aveoli are damaged; leads to decreased respiratory function; loss of breath
Where do you find vocal cords?
In Larynx
False vocal cords:
Upper (vestibular) folds
No sound production
Help close airway during swallowing
True vocal cords:
Lower folds
Vocal sounds
Sound created as air is forced between them, vibrating them
What is the function of mucus lined nasal passages?
Warms, moistens, and filters incoming air and traps dust and pathogens
What determines the intensity or volume of a vocal sound?
-Force of air passing over the vocal cords.
-**Stronger blasts of air result in greater vibration of the vocal cords and louder sounds.
Know the location of the frontal sinus. You can transmit light into that sinus in a dark room.
-forms the lower forehead, and above eyebrows.
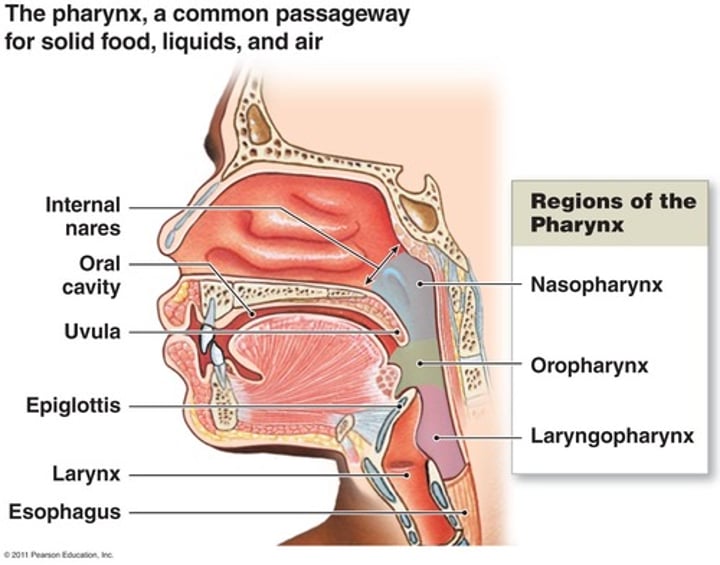
List the order of the sections of the pharynx from superior to inferior.
Nasopharynx: Superior to soft palate; air passage; contains openings to auditory tubes
Oropharynx: Posterior to mouth, inferior to nasopharynx; passageway for food and air
Laryngopharynx: Inferior to oropharynx; continuous with larynx and esophagus
What is laryngitis? (you may have to Google this) Symptoms?
an inflammation of your voice box (larynx)
Symptoms:
Hoarse/raspy voice
What type of cells would you find in the nasal cavity?
pseudostratified ciliated epithelium (mucous membrane)
What is the difference between the trachea and the esophagus?
Trachea is for air passageway and esophagus is for food and air passageway
Is the pharynx located superiorly or inferiorly to the trachea and the esophagus?
located superiorly
What is the difference between the tracheal cartilage and the bronchial cartilage?
Tracheal cartilage: Has 20 C-shaped rings of HYALINE cartilage
Bronchial cartilage: Has cartilaginous plates
What happens to the epithelial lining as you go deep into the respiratory tract?
Epithelial lining gets thinner
-Pseudostratified ciliated columnar, simple cuboidal, simple squamous
How many lobes does the right and left lung have?
Right lung has 3 lobes
left lung has 2 lobes
How does air enter the lungs during inspiration?
Diaphragm (moves downward) and intercostal muscles (thoracic cavity expands) contract, intra-alveolar pressure atmospheric pressure is less than atmospheric pressure
**DUE TO pressure gradient between atmosphere and alveoli
Define atmospheric pressure? Why is Boyle's law important?
Atmospheric pressure: Force that moves air into the lungs (atmospheric and alveolar pressure are equal)
What forces air out of the lungs during quiet expiration? (Look under Expiration-normal resting expiration)
The forces responsible for normal resting expiration come from elastic recoil of lung tissue and surface tension
Define inspiratory reserve volume.
maximum amount of additional air that can be drawn into lung by extra effort after normal inspiration
Look at table 19.4. Memorize all volume numbers. There will be general questions and You will need these numbers to solve problems. Memorize definitions of all volumes as well.
tidal volume (TV) - 500 mL - volume pf air moved in or out of lungs during a respiratory cycle.
inspiratory reserve volume (IRV) - 3,000 mL - additional amount of air that can be drawn into lung by extra effort after normal inhalation
expiratory reserve (ERV) - 1,000 mL - maximum additional amount of air that can be exhaled after normal exhalation.
residual volume (RV) - 1,200 mL - volume of air that remains in the lungs even after a maximal exhalation
vital capacity (VC) - 4,600 mL - maximum volume of air that can be exhaled after taking the deepest breath possible:
VC = TV + IRV + ERV
inspiratory capacity (IC) - 3,500 mL - maximum volume of air that can be inhaled after exhalation: IC = TV + IRV
functional residual capacity (FRC) - 2,300 - volume of air that remains in the lungs following exhalation:
FRC = ERV + RV
total lung capacity (TLC) - 5,800 mL - total volume of air that the lungs can hold:
TLC = VC + RV
Why will a newborn develop respiratory distress syndrome?
They don't produce enough surfactant (crucial for keeping lungs expanded); infant's lung can collapse.
You need to know what a respiratory cycle is as well if you don't know that.
-One inspiration + the following expiration = a respiratory cycle
-Volume of air moved in and out of lungs during quiet (normal) respiration
What holds the visceral and parietal pleural membranes together?
Serous fluid
Define pneumothorax.
-Caused by puncture in thoracic wall
-Collapse of lung
-Air within the pleural pace in between the membranes (should be fluid not air)
What happens to intrapleural pressure and intra-alveolar pressure during inspiration and expiration. (Figure 19.22 will help you)
Inspiration: Intra-alveolar and intrapleural pressure decreases
- Expiration: Intra-alveolar and intrapleural pressure increases
List the events of inspiration. (Table 19.2)
1- Impulses on phrenic nerves to diaphragm, causing contraction
2- Diaphragm moves downward, the thoracic cavity expands.
3- External intercostal muscles may contract, raising the ribs and expanding the thoracic cavity further.
4- The intra-alveolar pressure decreases.
5- Atmospheric pressure, greater than intra-alveolar pressure, forces air into the respiratory tract through the air passages.
6- The lungs fill with air.
What is the first thing to occur during expiration?
The diaphragm and external intercostal muscles relax.
What is the relationship between volume and pressure according to Boyle's Law?
****Inverse relationship****
-Volume increase = decrease in pressure
-Volume decrease = increase in pressure
What is a hiccup? Look at the mechanism. Table 19.5
-Diaphragm contracts spasmodically while glottis is closed.
-Sudden inspiration of air can cause spasmodic contraction
Where would you find respiratory control centers?
Medullary oblongata and pons
What do the dorsal and ventral respiratory groups control?
-Ventral respiratory group: Sets basic rhythm of breathing and controls abdominal muscles
-Dorsal respiratory group: Controls the diaphragm and external intercostal muscles
Your child stops their breathing on purpose because you won't get them a toy. Should you panic? What will happen to prevent them from dying?
DON'T PANIC
- Increase of CO2 stimulates chemoreceptors which will soon trigger breathing (the need for air is greater)
What causes adult sleep apnea?
Usually obstructive, caused by airway blockage
Where do you find central chemoreceptors?
In ventral part of medulla oblongata
Look at Table 19.6 and list the factors that affect breathing.
- Stretch of tissues
- Low plasma PO2
- High plasma PCO2
- High cerebrospinal fluid hydrogen ion concentration
What happens when peripheral chemoreceptors are stimulated?
Respiratory rate and tidal volume increases
What has to happen to the P02 in order for peripheral chemoreceptors to be stimulated?
Has to hall below 50%
Look at Figure 19.35. What is the percentage of hemoglobin saturation when you have a Po2 of:
30 mm/Hg = 60%
60 mm/Hg = about 92%
100 mm/Hg = 100%
What has an effect on pH of the blood?
Pco2 and H+ ion
Where are the peripheral chemoreceptors located?
located in the aortic arch and carotid bodies
Why do we use a gas mixture in a clinical setting?
Increase the rate and depth of breathing.
What happens to Pco2 (partial carbon dioxide and ph when you hyperventilate?
-lowers the blood CO2 below normal
-followed by a rise in pH (alkalemia)
When you exercise your breathing rate changes (increases). What happens to your Po2 and your Pco2?
Blood levels of O2 and CO2 do not change significantly (remains unchanged)
What happens to hydrogen ions if there is an increase in carbon dioxide?
Hydrogen ion and carbon dioxide increase (direct relationship)
What type of tissue does the alveoli wall have?
simple squamous epithelium
What forms the respiratory membrane?
-Alveolar wall: simple squamous epithelium
-Blood capillary wall: simple squamous epithelium
-Fused basement membranes: bottom of the cells (where cells connect)
What type of cell would ensure particles that you may inhale are removed for the respiratory tract?
Alveolar macrophages: help clean alveoli from airborne agents, including bacteria.
Differentiate between type I and type II cells
-type I cells: simple squamous epithelium
-type II cells: secrete pulmonary surfactant
Know what is chloride shift.
-an exchange that maintains the ionic balance between th RBC and plasma
-bicarbonate ions leave RBC's, chloride ions move from plasma to RBC's
-chloride ions leave the RBC's, bicarbonate ions enter RBC's (upon reaching the lungs)
What would cause the amount of oxygen to be released from oxyhemoglobin?
increase in blood PCO2 (partial pressure of carbon dioxide)
What enzyme is used to catalyze the carbon dioxide reaction with water?
carbonic anhydrase
What protein will transport carbon dioxide in the blood?
hemoglobin
What is globin?
protein part of hemoglobin
Why is carbon monoxide dangerous? What does it bind to?
- binds to the oxygen binding site on hemoglobin
- O2 carrying ability will be reduced
List the changes in the respiratory system that occur with aging.
- ciliated epithelium cells become fewer numbered
swallowing, gagging, and coughing reflexes slow
- connective tissue replaces muscles in bronchioles, hindering dilation
- macrophages in lungs lose efficiency
What two systems can be severely affected if you are a smoker or if you have exposure to secondhand smoke?
Respiratory and Cardiovascular
What cells undergo changes with smoking? Why are smokers more susceptible to respiratory infections?
- epithelial cells
- respiratory passages lose cilia which aid in removing bacteria
What is affected with emphysema?
alveoli degenerate and decrease surface area for gas exchange
What usually causes bronchial asthma?
an allergen (to something)
Define anatomic dead space.
-air in respiratory tract that remains in the conduction structures
-doesn't reach the alveoli
What is minute ventilation?
volume of air moved into the respiratory passages each minute
What is alveolar ventilation?
volume of air that reaches the alveoli each minute
How is minute ventilation calculated?
TV (Tidal Volume) x breathing rate
What respiratory volumes are added together that equal vital capacity?
TV (Tidal Volume) + IRV (Inspiratory Reserve Volume) + ERV (Expiratory Reserve Volume)
Define atelectasis.
collapsed lung or region of lung
How is oxygen transported in the blood? What you need to look at is what is it bound to? What percentage?
-98% bonded to hemoglobin
-2% is dissolved in plasma
How is carbon dioxide transported in the blood? Same as above, look at the percentages and the overall way it is transported.
- 70% transported as bicarbonate ion
- 23% bound to hemoglobin
- 7% dissolves in plasma
What is the difference between the pharynx and the larynx? Same answers as trachea and esophagus
Pharynx is for food passageway and larynx is for air ONLY passageway
Why is Boyle's law important?
Pressure and volume of gases are inversely proportional. (HIGH TO LOW) (i.e. intra-alveolar pressure decrease, atmospheric pressure increase)