CVD - CVD in women + Arrhythmias
1/89
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
90 Terms
Define Heart Failure.
Heart is not pumping blood as well as it should
How is heart failure diagnosed?
using ejection fraction
List the types of Heart Failure.
1) Right-sided
2) Left-sided
3) Congestive
Define Right-sided, Left-sided & Congestive heart failure.
Right-sided heart failure: Back-ups in the area that collects "used" blood
Left-sided heart failure: Failure to properly pump out blood to the body
Congestive heart failure: Fluid collects around the heart
What type of heart failure is seen in people with end-stage heart failure?
Congestive HF
List the 2 types of left-sided heart failure.
1) Systolic failure
2) Diastolic failure
What is Systolic failure?
LV loses its ability to contract → ↓ ejection fraction
↓ ejection fraction due to ↓SV
What is Diastolic failure?
LV can't properly fill → preserved ejection fraction (but they still have heart failure)
LV loses its ability to relax
b/c the muscle has become stiff from stretching too much (this causes fibroblasts to be added instead of new muscle cells → increases stiffness)
What is the most common type of heart failure?
Systolic failure
What is the ratio of ejection fraction? Write out its formula.
blood pumped out : blood left in left ventricle
EF = (SV/EDV) x 100
List the percentages of blood pumped out under normal, borderline and reduced conditions.
Normal - 50-70% of blood is pumped out
Borderline - 41-49% of blood is pumped out
Reduced - <40% of blood is pumped out
What is the main contributing factor to heart failure?
Ischemia – Responsible for 50% of heart failure cases
What percentage of heart failure cases are linked to HTN? Why?
25% of cases
HTN causes ↑BV, ↑PVR, ↑ LV pressure → HF
List 4 complications that occur after MI.
↓ CO
Damming of blood outside heart (congestion of blood)
Fibrillation of the heart
Rupture of the heart (rare but still happens)
Describe Complication #1: CO.
Who is it seen in?
What effect does it have on the heart?
→ Seen in ppl who have systolic LEFT heart failure
Healthy portion of ventricle contracts, ischemic portion doesn’t
pressure in LV pushes out “dead”/ischemic portion of muscle → systolic stretch, regional thinning, dilatation
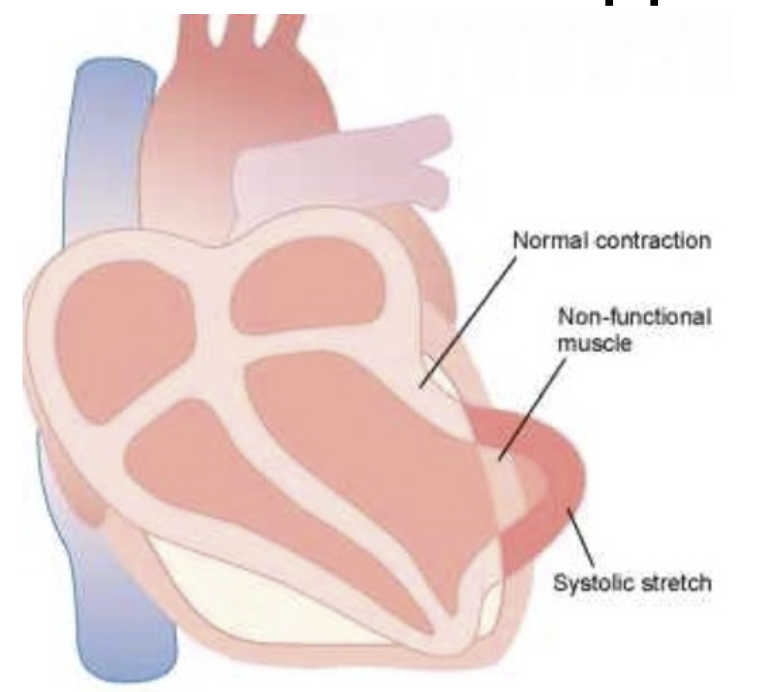
Complication #1: CO
Outline Pathophysiology of Heart Failure Leading to Cardiac Shock.
Heart muscle stretches excessively
No cardiomyocytes (contractile cells) are added to compensate
Fibroblasts (non-contractile cells) are added instead
This leads to heart muscle hardening (fibrosis)
↓ contraction → ↓ SV
Inadequate blood flow to the body → Cardiac shock
Complication #1: CO
Cardiac shock accounts for ____ of heart failure deaths.
85%
Complication #1: CO
Research suggests that people with congestive heart failure (end-stage heart failure) have a certain physical heart adaptation. What is it?
Ppl with congestive heart failure (end-stage heart failure) have left ventricular hypertrophy
↑ left ventricular hypertrophy = ↑ hazard ratio for congestive heart failure (this means ↑ LVH is linked to a ↑ risk of developing or worsening CHF)
Describe Complication #2: Congestion of blood.
Who is it seen in?
What effect does it have on the heart?
→ Seen in ppl who have congestive heart failure
Blood is backed up in atria, pulmonary circuit or systemic circuit leading to:
↑ capillary pressure (esp in lungs)
↓ blood flow to kidneys → ↓ urine output → ↑ blood volume
Complication #3: Ventricular Fibrillation
What is it caused by?
Loss of blood supply (due to blockage in coronary vessel)
ions can't travel to the cardiomyocytes (due to block) → cardiac muscle can't repolarize
↑ SNS activity after a MI
↑ blood perfusion to body
↑ contractility
Ventricular stretch ↑ pathway length for conduction
↑ pathway length = electrical activity has to travel ↑ distance across the heart → interfere with normal contraction → fibrillation
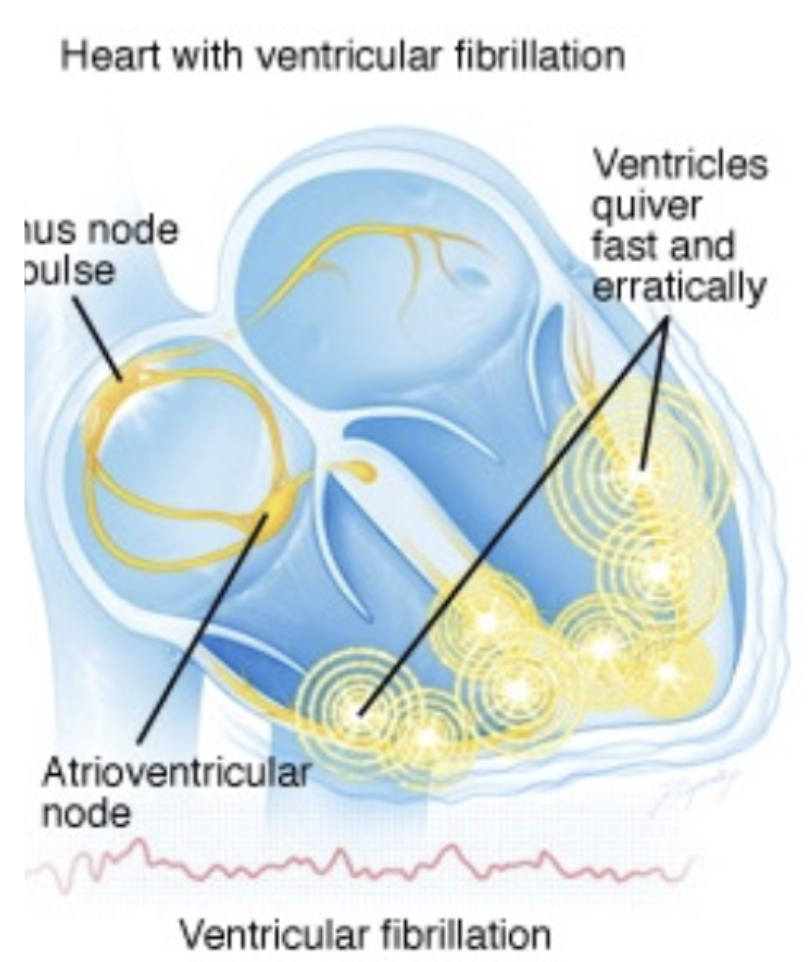
Complication #3: Ventricular Fibrillation
When can it occur?
occur after the first 10 min post-MI and/or 1-3 hours post-MI
Complication #4: Rupture of infarcted area
How does it occur?
occurs when systolic stretch reaches a detrimental (↑↑↑) level → regional thinning of the heart muscle + ischemic muscle fibers degenerate → rupture
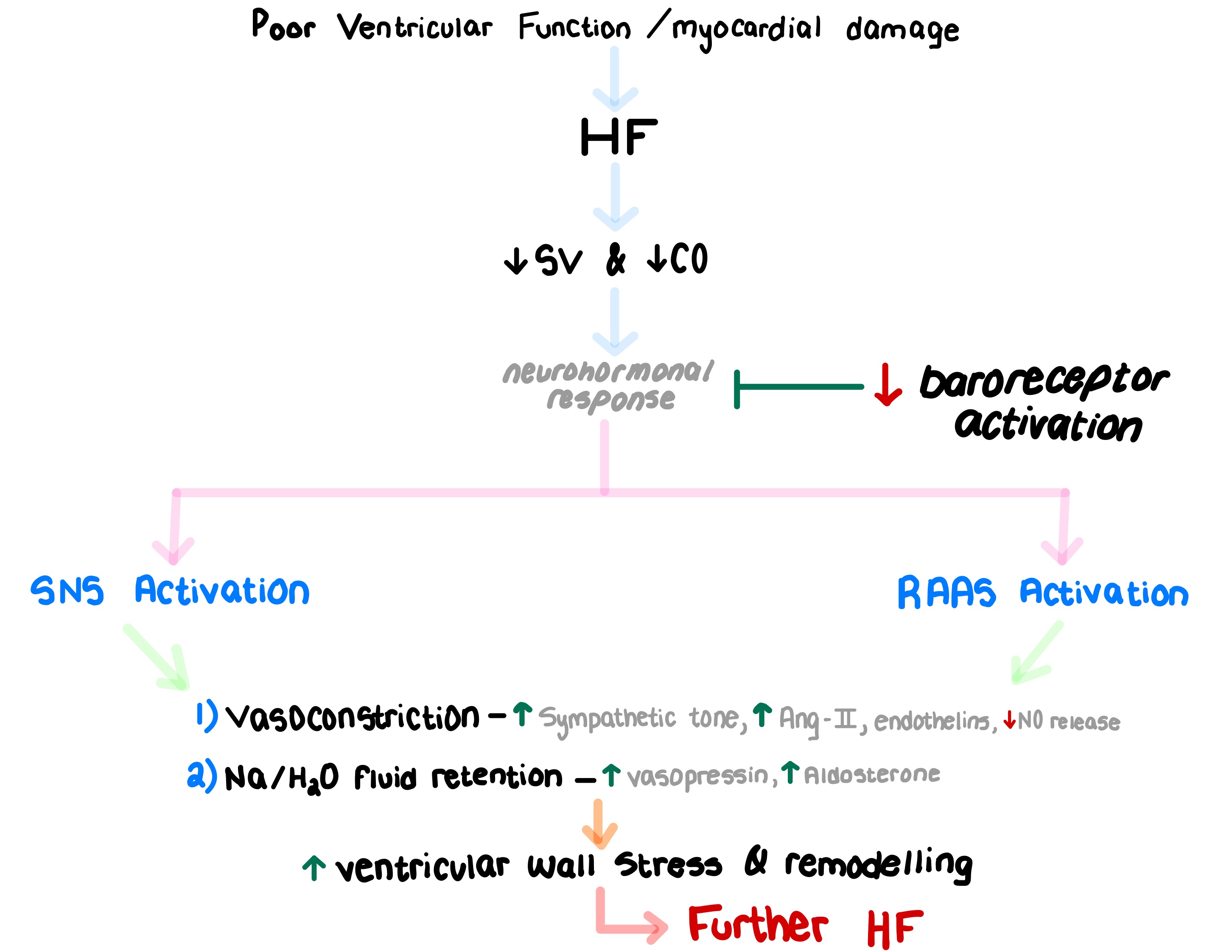
What is the acute impact of ↓ SV and ↓ CO on the heart after an MI?
↓ SV & ↓ CO
↓ Baroreceptor activation
↑ SNS activation to compensate
↑ Contractility & ↑ HR
What is the chronic impact on the heart after a MI?
Concentric Remodeling (Acute Phase)
Eccentric Remodeling (Chronic Phase)
Chronic Impact: What is Concentric Remodeling? What is it this remodelling mediated by?
Occurs right after an MI
Characterized by hypertrophy in the non-infarcted area to maintain function & apoptosis in infarcted area
hypertrophy is mediated by - stretch, Ang II, ACE & GFs → promote heart muscle growth
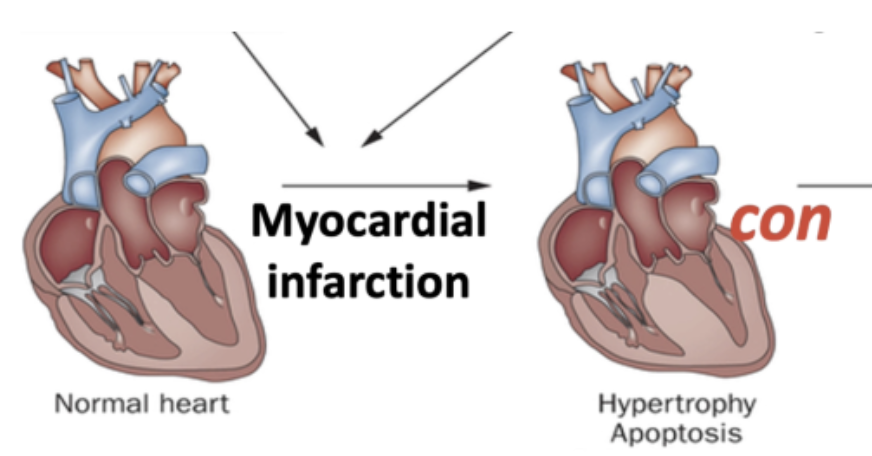
Chronic Impact: What is Eccentric Remodeling?
→ Caused by thinning infarcted zone and lengthening of conduction pathways
Leads to ventricular dilatation and contractile dysfunction over time
associated with ↑ EDV & ↑ ESV → ↓ SV
progressive ↑ pressure and ↓ contractility further weakens the heart
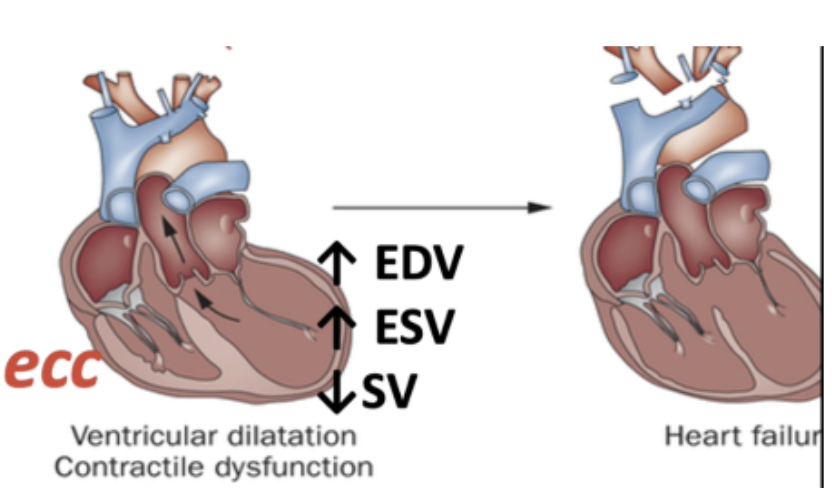
What are the key neurohormonal responses triggered by heart failure, and how do they worse heart failure progression? Draw the pathway.
Study # 1 - HF-ACTION Randomized Controlled Trial
This study wanted to test the effects of exercise on HF patients. How can exercise help HF patients?
Exercise is beneficial even for patients with severe heart failure b/c can help maintain heart function and prevent further progression
Note: Heart failure is irreversible (can’t return to a completely healthy heart)
Study # 1 - HF-ACTION Randomized Controlled Trial
What are some barriers to exercise for someone with HF?
Deal with swelling and edema due to lack of proper blood flow (can be painful)
↑ risk of falls
↓ muscle function
People may be concerned about their heart working too hard
Study # 1 - HF-ACTION Randomized Controlled Trial
Compare the hospitalization rates b/w the exercise training group & usual care group.
Exercise Training Group: 37 patients (3.2%) hospitalized due to an event occurring during or within 3 hours after exercise
Usual Care Group: 22 patients (1.9%) hospitalized, despite not undergoing a formal exercise program
Study # 1 - HF-ACTION Randomized Controlled Trial
Compare the HF progression/worsening HF b/w the exercise training group & usual care group.
29% in the usual care group
26% in the exercise training group
→ No significant difference between groups
Study # 1 - HF-ACTION Randomized Controlled Trial
Did MI prevalence or HF outcomes worsen in the exercise training group & usual care group.
In exercise group
No ↑MI prevalence
No worsening of HF outcomes
Study # 1 - HF-ACTION Randomized Controlled Trial
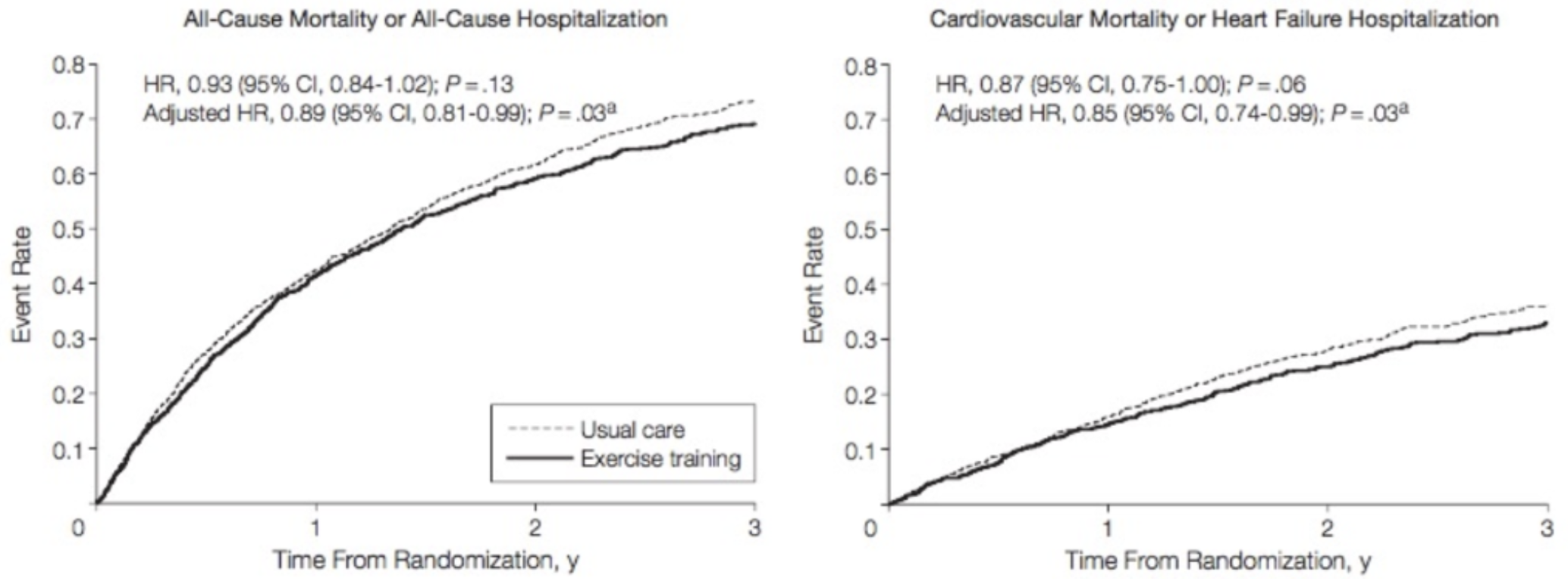
What does the exercise training (———) line lying below the usual care (- - - - - -) line indicate?
People who exercised, showed a ↓ Hazard ratio (↓ risk) for:
all-cause mortality/hospitalization (11% reduction)
CV mortality & HF hospitalization (15% reduction)
Study # 1 - HF-ACTION Randomized Controlled Trial
List the additional benefits of exercise for HF patients.
Improved functional capacity:
↑ 6-minute walking distance
↑ O2 consumption (VO₂ max)
↑ cardiopulmonary exercise duration
What is a heart arrhythmia?
abnormal heart rhythm
What is normal HR vs Heart arrhythmia (bradycardia & tachycardia) HR?
Normal
Bradycardia: slow HR (<60 bpm)
Tachycardia: fast HR (>100 bpm)
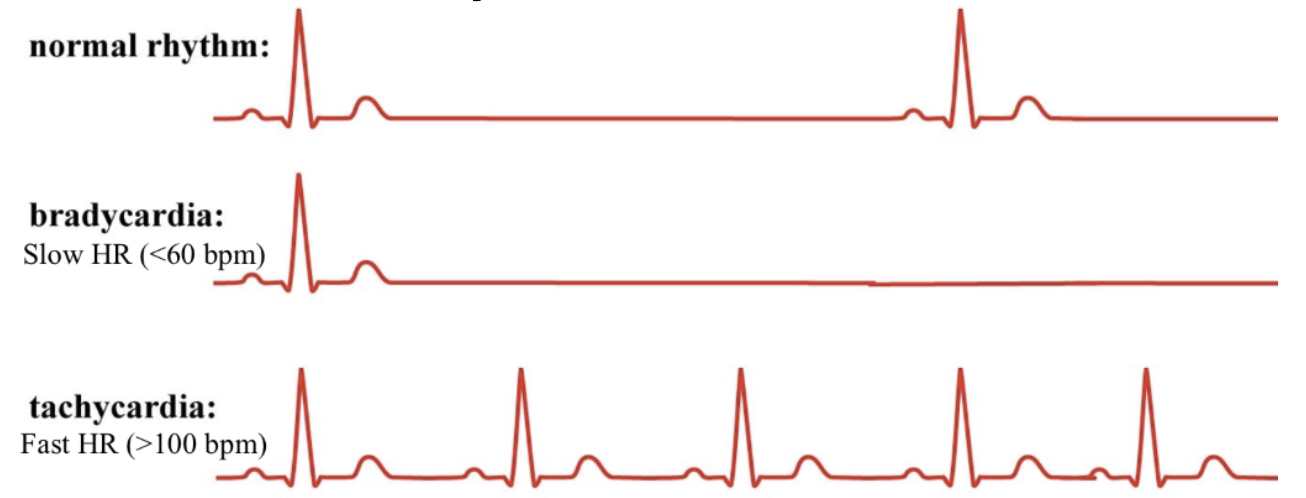
What is Fibrillation?
periods of fast and slow contractions/uncoordinated contractions
What is commonly noticed in people with atrial fibrillation?
Periods of fast HR are noticed
Why is an ECG important for people with AFib?
ECG helps doctors monitor HR and electrical complex freq, allowing them to assess the severity and pattern of AFib
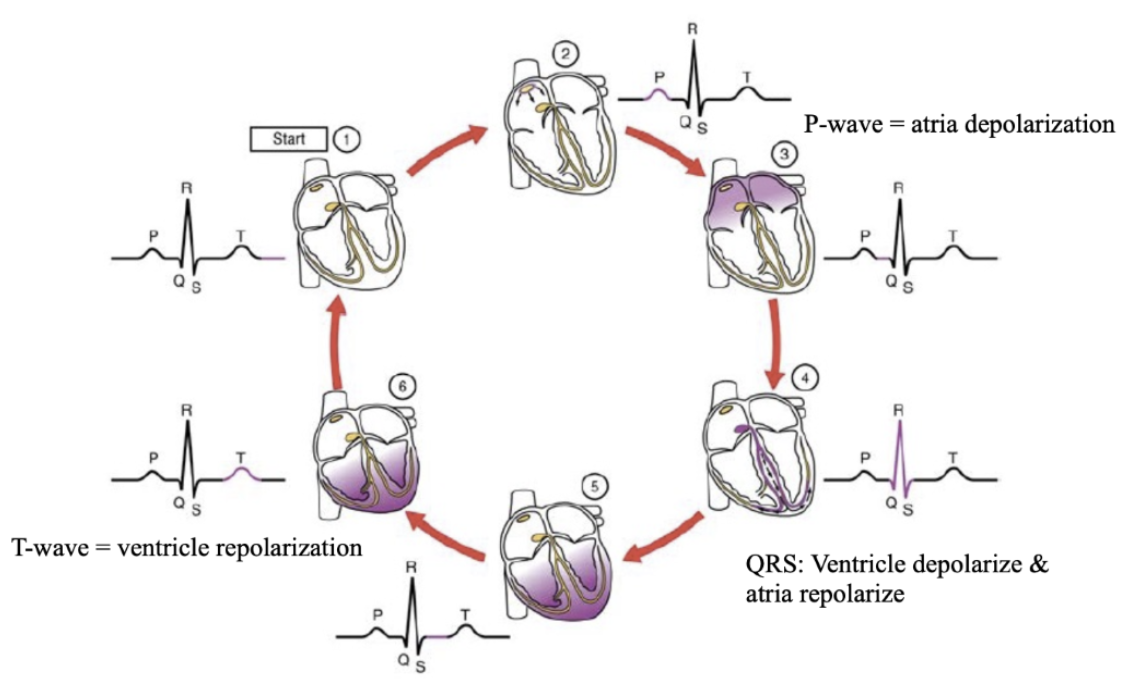
Outline the main phases of an ECG.
P-wave - atria depolarization
QRS-wave - ventricle depolarization + atria repolarization
T-wave - ventricle repolarization
What is (Paroxysmal) Tachycardia?
rapid HR that happens without any known cause
Paroxysmal = Sudden onset and termination
Tachycardia = Fast heart rate (>100 bpm)
List the 2 types of (Paroxysmal) Tachycardia.
Supraventricular fibrillation
Ventricular fibrillation
What is Supraventricular fibrillation?
rapid heart beats in atria or AV node
seen in people with A-fib
What is Ventricular fibrillation?
unconscious within 4-5 secs, death of tissues within mins
most serious form
causes huge disruption in coronary blood flow → cardiac tissue death
What is Postural orthostatic tachycardia syndrome (POTS)?
difficulty adjusting to standing position from lying
rapid heart beat (120 bpm) within 10 min of standing
sometimes due to medications (vasodilators, diuretics, antidepressants)
What happens to the atria vs ventricles during AFib?
Atria - chaotic electrical activity causes the atria to quiver instead of contracting properly
Ventricles - pump irregularly and fast (125-150 bpm)
How is Coronary blood flow affected by AFib?
reduced by 20-30%
What are the major risks associated with AFib, often caused by irregular ventricle pumping + reduced coronary blood flow?
Thrombosis
Pulmonary embolism
Stroke
What is the biggest risk (from Thrombosis, Pulmonary embolism, Stroke) for people with Afib?
Stroke
4-5x higher in people with AFib
How long must atrial fibrillation last to be diagnosed?
More than 30 seconds
Why is Sporadic Afib easier to diagnose than persistent Afib?
Sporadic Afib - hard to diagnose b/c episodes happen randomly
Persistent AFib - easy to diagnose b/c episodes occur more frequently
How prevalent is Afib?
Trend: rising prevalence (1.68% increase in 2000 to 2.36% in 2014)
Most common arrhythmia, affecting ~350,000 Canadians
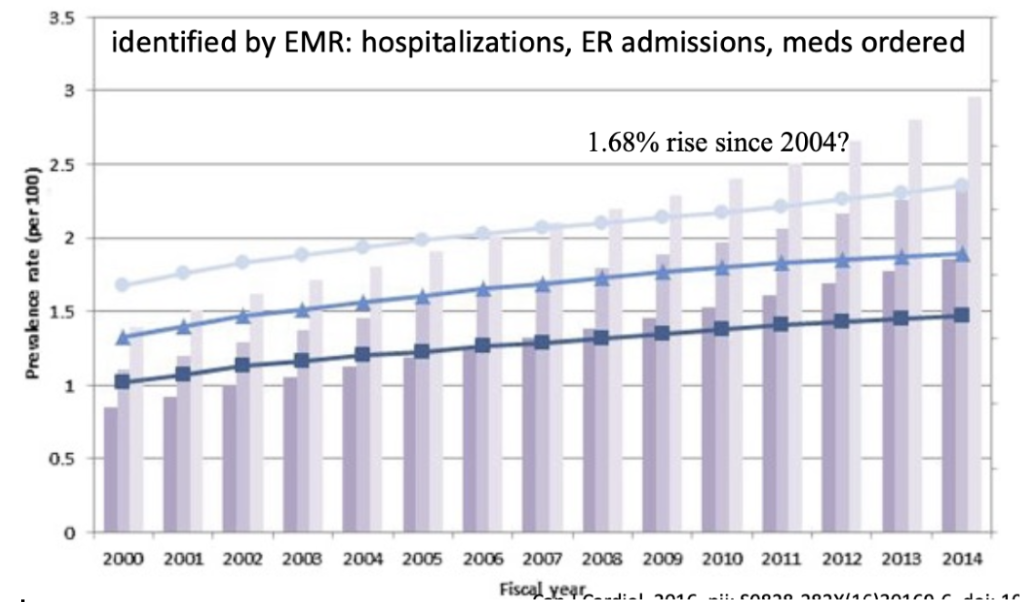
Why is there a rising prevalence of Afib?
Aging population
↑ awareness
Better detection methods
Why is it difficult to accurate data regarding the prevalence of Afib?
Some people experience symptoms, while others have silent (asymptomatic) AFib and go undiagnosed
Outline the pathway on how AFib can lead to stroke.
AFib causes blood pooling in the heart → clot formation
Clots can travel to the brain → blocking blood flow → stroke
Outline the pathway on how AFib can lead to MI.
AFib causes blood pooling in the heart → clot formation → clot moves to the heart
Why does Afib increase HF risk?
↓ Coronary blood supply decreases.
Irregular heartbeats reduce the heart's efficiency
What is Virchow’s Triad? How is it related to AFib?
→ Virchow’s Triad explains the 3 main factors that contribute to blood clot formation
Stasis (↓ blood flow) → Blood pools in the atria.
Endothelial Injury → Heart’s inner lining may be damaged.
Hypercoagulability → Blood clots form more easily
→ All 3 factors work together to make AFib patients more likely to develop dangerous blood clots leading to ↑Stroke & ↑HA risk for people with
How does AP progress in a Cardiac Muscle? List the steps.
1) Depolarization
Voltage-gated Na+ channels open
Na+ enter cardiomyocytes
Rapid upstroke occurs in the action potential
2) Plateau Phase - prevents immediate repolarization
Na+ channels close.
Ca2+ channels open, allowing Ca2+ to enter the cardiomyocytes
K+ channels open, allowing K+ to exit
3) Repolarization
Ca2+ channels close
K+ channels remain open, and K+ continues to exit the cardiomyocytes
Membrane potential returns to resting level (~ -90 mV)
What is a ganglia? Where are ANS Ganglia located?
Ganglion: a cluster of neuron cell bodies in the peripheral NS
Located inside and outside the heart
Intrinsic Cardiac Nerves
Where are they found?
What is their role?
Found in the atria
Helps control conduction through the heart
Extrinsic Sympathetic Nerves Innervating the Heart
Where are they found?
List the key extrinsic sympathetic nerves.
Found outside the heart and influence heart function
Cervical – arises from the vagus nerve
Cervicothoracic (Stellate) – most important extrinsic nerve for heart regulation
Thoracic – contributes to sympathetic control
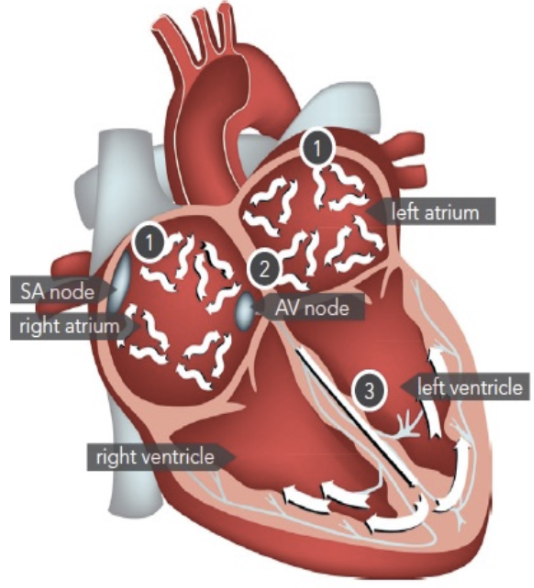
Intrinsic Cardiac Innervation
What is the function of Bachman’s bundle?
acts as a “highway” on top of the heart to ensure both atria contract at the same time
Intrinsic Cardiac Innervation
Where is autonomic nerve density the highest in the heart?
5mm from the left atrium (LA)-pulmonary vein junction
Intrinsic Cardiac Innervation
What does "co-localized" mean in cardiac innervation?
Adrenergic (SNS) and cholinergic (PNS) nerves are found in overlapping areas of the atria
both work intrinsically to regulate heart activity
Extrinsic Cardiac Innervation
The vagus nerve affects both the PNS & SNS. Compare it's effect on both systems.
PNS (↓HR)
75% of PNS action on the heart is controlled by the vagus nerve
SNS (↑ HR)
25% of SNS action on the heart is controlled by the vagus nerve
Extrinsic Cardiac Innervation
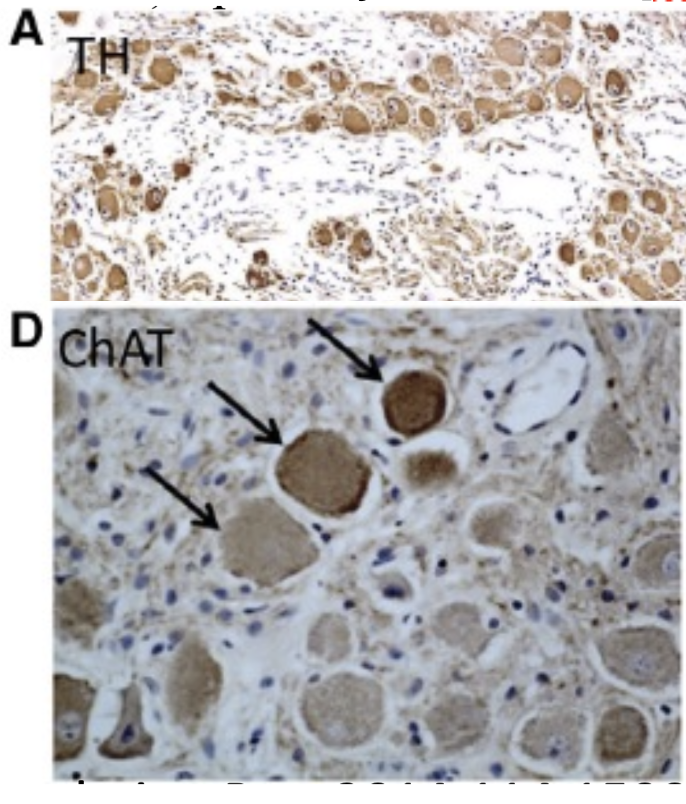
Since the vagus nerve controls both the SNS and PNS, it secretes enzymes involved in both PNS & SNS neurotransmitter synthesis. What are they? Describe them.
1) Tyrosine hydroxylase (TH): makes catecholemines (NE) in the SNS
2) Choline acetyltransferase (ChAT): makes ACh in the PNS
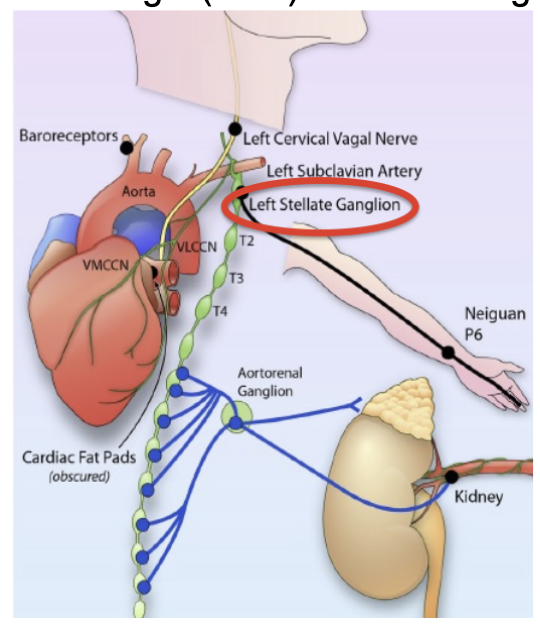
Extrinsic Cardiac Innervation
If 25% of SNS innervention comes from the vagus nerve, what is the major source of SNS innervation to the SNS?
Stellate Ganglion
also has SNS and PNS nerves
secretes TH & ChAT
What does SNS do to the heart?
↑ Na+ & Ca2+ permeability to enter the cell via cAMP
Depolarizes cardiomyocytes so that AP occurs faster
↑ SA node spontaneous depolarization
↑ conduction to AV branches
↑ contractility, ↑ SV
Max SNS stimulation = 200 bpm
What does PNS do to the heart?
↑ K+ permeability to leave cell → K+ efflux → cardiomyocyte hyperpolarization → ↓ rate for next depolarization and AP to occur
↓ SA node spontaneous depolarization
↓ conduction to AV branches
No change in contractility or SV
Max PNS stimulation = 25 bpm
Autonomic Remodeling Post-MI
What is the purpose of autonomic remodeling post-MI?
superload other parts of heart with autonomic nerves and innervation to compensate for the injury to the infarcted area during a MI
Autonomic Remodeling Post-MI
What happens when the heart compensates by superloading other parts with autonomic nerves?
↑ Afib duration
↑ SNS innervation
↑ HR
↓ PNS innervation
Autonomic Remodeling Post-MI
How long after a MI do nerve growth factor (NGF) levels increase?
NGF levels increase within 1 month post-MI
Autonomic Remodeling Post-MI
What does increased NGF levels lead to? What molecular mechanism drives nerve growth after a MI?
↑ NGF levels → Nerve "sprouting"
growth of new nerves in non-infarcted areas, such as the atria
- NGF stimulates ↑ growth factor proteins (GAP43) which promotes nerve growth and regeneration
What did staining for ChAT show in post-MI studies? What does this conclude?
Staining for ChAT (PNS) didn’t show a specific ↑ in PNS innervation, even though nerve growth occurred
Conclusion: Nerve growth was likely dominated by sympathetic nerves.
Outline the pathway of SNS activation after a MI.
SNS nerve activation causes NE release
NE binds to β-adrenergic receptors on cardiomyocytes
Binding activates PKA via cAMP signaling
PKA:
phosphorylates RyR in SR → ↑ Ca²⁺ influx into the sarcoplasm
activates L-type Ca²⁺ channels on cardiomyocytes' membranes → allows more Ca²⁺ to enter
phosphorylates phospholamban (PLB) → SERCA inhibition (↓ Ca²⁺ reuptake into SR)
More Ca²⁺ available → more contractions occur
Ca²⁺ binds to calmodulin → forms a Ca²⁺-calmodulin-dependent kinase complex
This complex interacts with genes inside the cell, activating genes responsible for:
Hypertrophy
Fibrosis
What are the overall effects of SNS activation on the heart after a MI?
Prolonged depolarization.
Greater contraction strength.
Increased nerve sprouting in Afib → More sympathetic nerve activity releases norepinephrine, further amplifying these effects.
Outline the pathway of PNS activation after a MI.
PNS nerve activation causes Ach release
Ach binds to M₂ type 2 muscarinic receptors on cardiomyocytes
K⁺ channels are activated → K⁺ efflux
↑ K⁺ efflux causes:
Faster repolarization of the cardiac membrane
↓ AP duration
Slower HR (b/c a longer time needed for depolarization before the next contraction)
What happens to HR when both Ach and NE are released?
HR depends on which one is stronger
NE usually dominates in Afib due to sympathetic overactivity, so HR increases
List the effects of NE on the heart.
Faster depolarization → faster HR
↑ contraction strength
Activation of hypertrophic and fibrotic gene programs
List the effects of Ach on the Heart.
More hyperpolarization → Slower HR
Shorter depolarization duration
Faster repolarization
List the combined effects of Ach and NE on the heart.
Irregular HR → Alternating fast & slow beats
↓ SV → Heart can't fill properly
Heart remodeling → Hypertrophy & fibrosis
What is the difference b/w Lone Afib & Pathological Afib?
Lone AF – 1er afib
occurs without any other underlying heart conditions
Pathological AF – 2er afib
occurs due to another heart condition
List some factors that cause pathological AF.
Genetics
Sex
SEF (Type A, acute life stress, coffee)
Alcohol
Sports (marathon running)
Sleep Apnea syndrome (ANS imbalance, ↑ SNS activation, ↓ PNS activation)
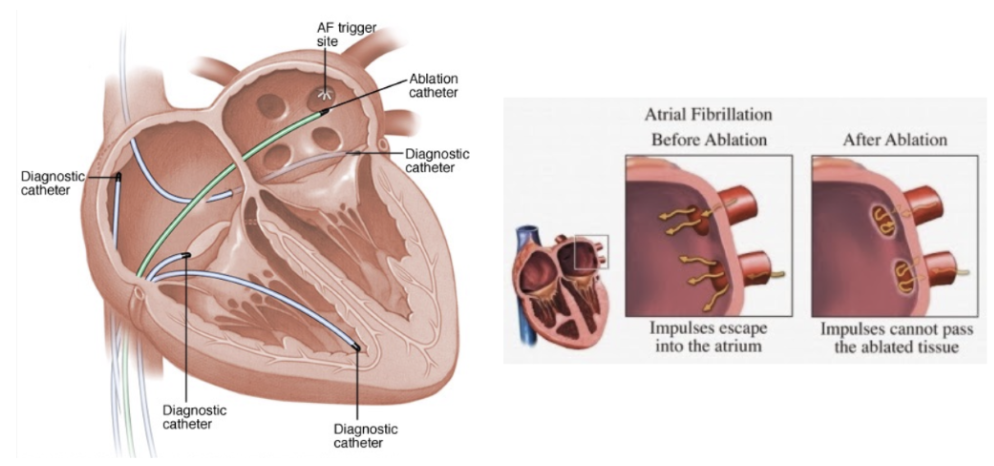
What is Ablation?
Green – ablation catheter
Problem: Nerve sprouting tends to be worse around the LA pulmonary vein junction
Solution: Burning off nerve endings around the LA-pulmonary vein junction to:
treat abnormal heart rhythms
restore heart's electrical activity
control neuron innervation to heart
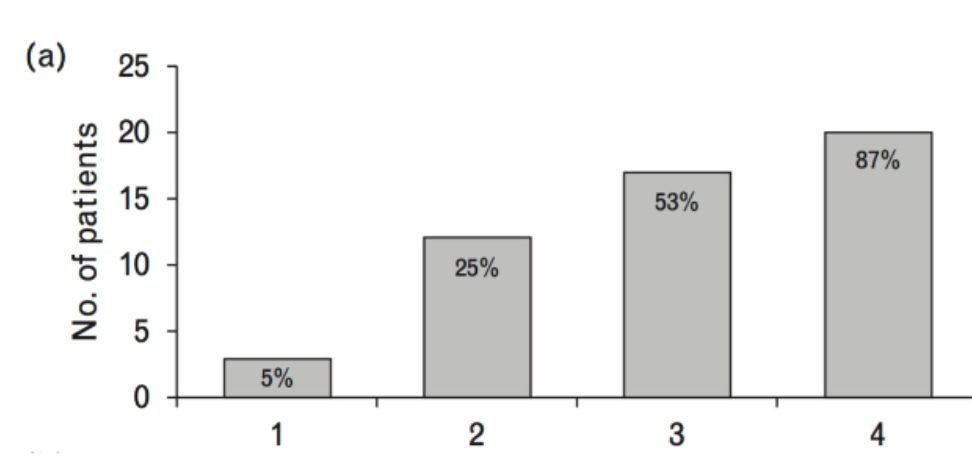
Study # 2 - ARREST-AF Cohort Study
What were the main finding of the 165 patients undergoing ablasion therapy?
↑ ablation procedures = ↑ success rate in restoring normal heart rhythm
majority of patients achieve normal rhythm by the 4th ablation
Ablation is not always successful after one attempt, and some patients require multiple procedures
What is an effective way of lowering A-fib?
Lifestyle Changes + Ablation Therapy = ↓ Afib severity
reduces reliance on anti-arrhythmic meds
Effect: restores heart's physical structure to a healthier state
List the structural improvements occur in the heart after risk factor management + ablation.
↓ Atrial Volume Index - good b/c it means there’s less atrial enlargement
LA volume returned to normal → regains normal heart shape
↓ LV size → helps reverse ventricular hypertrophy and restore normal function
Study # 3 - YOGA My Heart Study
How does yoga affect the following groups?
Symptomatic non-Afib.
Asymptomatic Afib
Symptomatic Afib
↓ Afib symptoms in all 3 groups
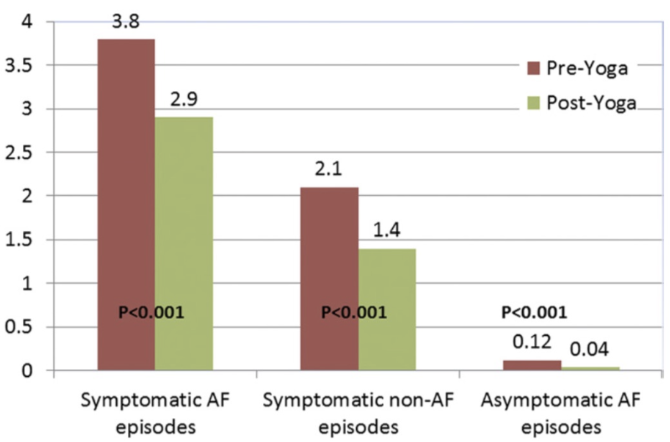
Why might yoga be helpful for people with Afib?
↓ HPA axis activation (↓ SNS activity)
Enhance PNS activity via vagus nerve
↓ risk factors for Afib progression and consequences
↓Systemic stress, ↓BP, ↓Inflammation
Improves endothelial function → upregulate NOS → ↑ NO
↓ atrial remodelling → ↓ hypertrophy & ↓ fibrosis