Lecture 11: Special Circulations
1/114
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
115 Terms
Resistance
Blood flow and distribution are regulated by _________________ in the arterial microcirculation
Arterioless
-vessels that regulate bulk flow
Precapillary Spincters
-regulate number of perfused capillaries for exhchange
-affect oxygen extraction
Cardiac Output (CO)
the quantity of blood pumped into the aorta per unit time and is the sum of all factors that control tissue perfusion
Acute Control
-control of flow
-rapid changes in vessel diameter (autoregulation)
Long-term Control
-control of flow
-slow, progressive changes in vessel and number
seconds to minutes
time span of acute regulation of blood flow
Baroreceptor Reflex
The primary reflex pathway for homeostatic control of blood pressure
Decreased
low blood pressure leads to _______________ baroreceptor firing
Decreased
_____________________ parasympathetic outflow leads to increased heart rate and contractility
Decreased; increased
Low BP and decreased baroreceptor firing leads to _________________ parasympathetic and _____________________ sympathetic outflow
Norepinephrine and Epinephrine
Increased Sympathetic Flow results in release of __________________ and ________________________ from adrenal gland
Arginine Vasopressin (AVP)
a peptide hormone from the posterior pituitary that promotes water conservation
Atrial Natriuretic Peptide (ANP)
A hormone, secreted by the heart, that normally reduces blood pressure, inhibits drinking, and promotes the excretion of water and salt at the kidneys.
Decreased
low blood volume results in __________________ atrial filling and myocyte stretch
Vasodilation
Vasodilation or Vasoconstriction?
-smooth muscle relaxation
-resistance decreases
-blood flow increases
Vasoconstriction
Vasodilation or Vasoconstriction?
-smooth muscle contraction
-resistance increases
-blood flow decreases
Compresses
high pressure in surrounding tissue ______________________ vessels
Distends
Low pressure in surrounding tissue _________________ vessels
Myogenic Response
Increased intravascular pressure causes active _____________________________
remains relatively constant
As pressure increases, resistance increases, and Flow __________________________
remains relatively constant
As pressure increases, radius decreases,
Wall tension ___________________________
Vasodilator Metabolites
Increased metabolic rate in active tissues promotes release of ______________________________
Vasodilation
Multiple contributors to
metabolic ________________________:
• Adenosine
• decreased O2
• CO2
• H+
• Lactic acid
• Decreased ATP
• K+
• Osmolality
• Arachidonic acid metabolites
Acute
which would be an example of hypertensive crisis?
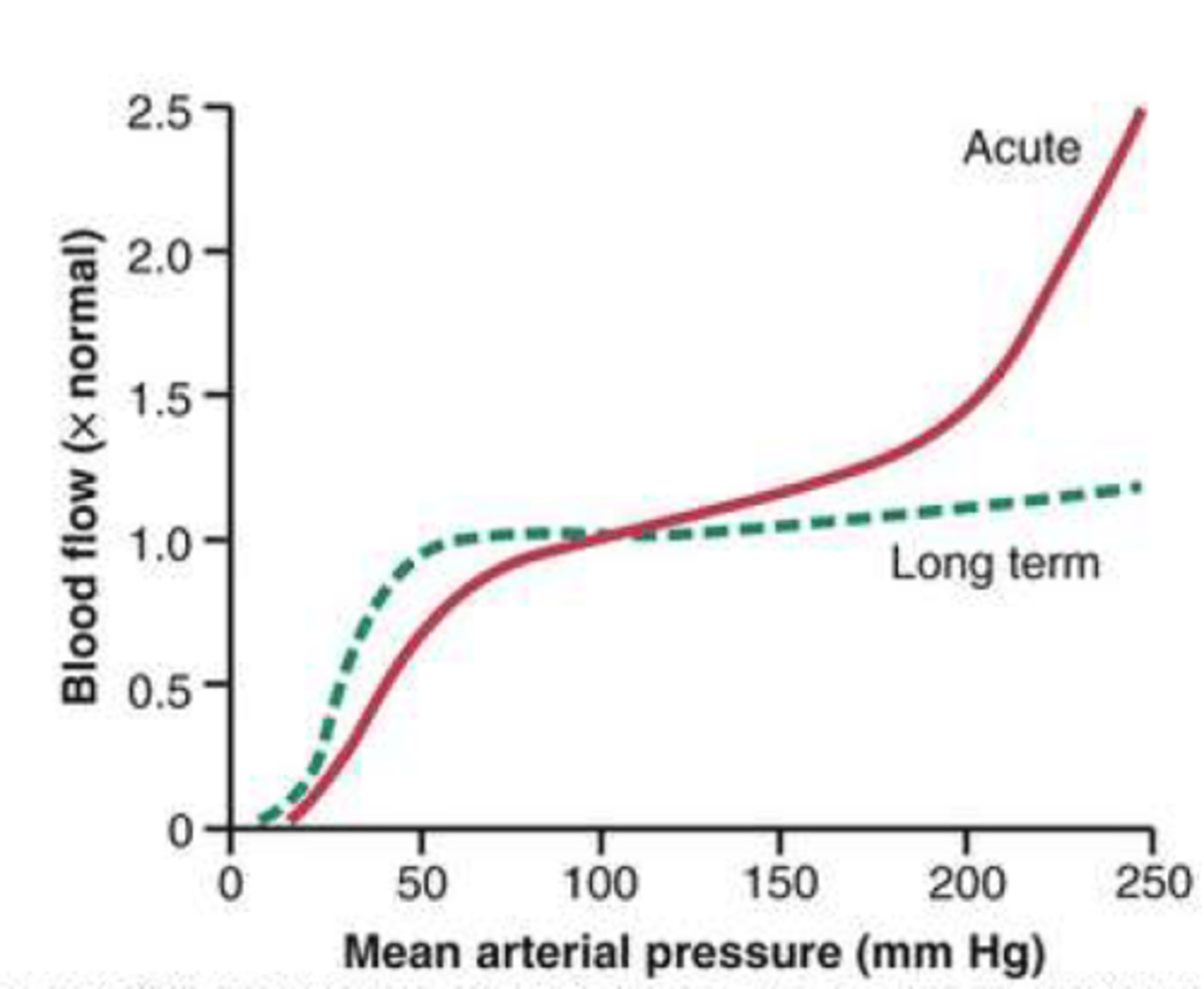
Long term
which would be an example of chronic HTN
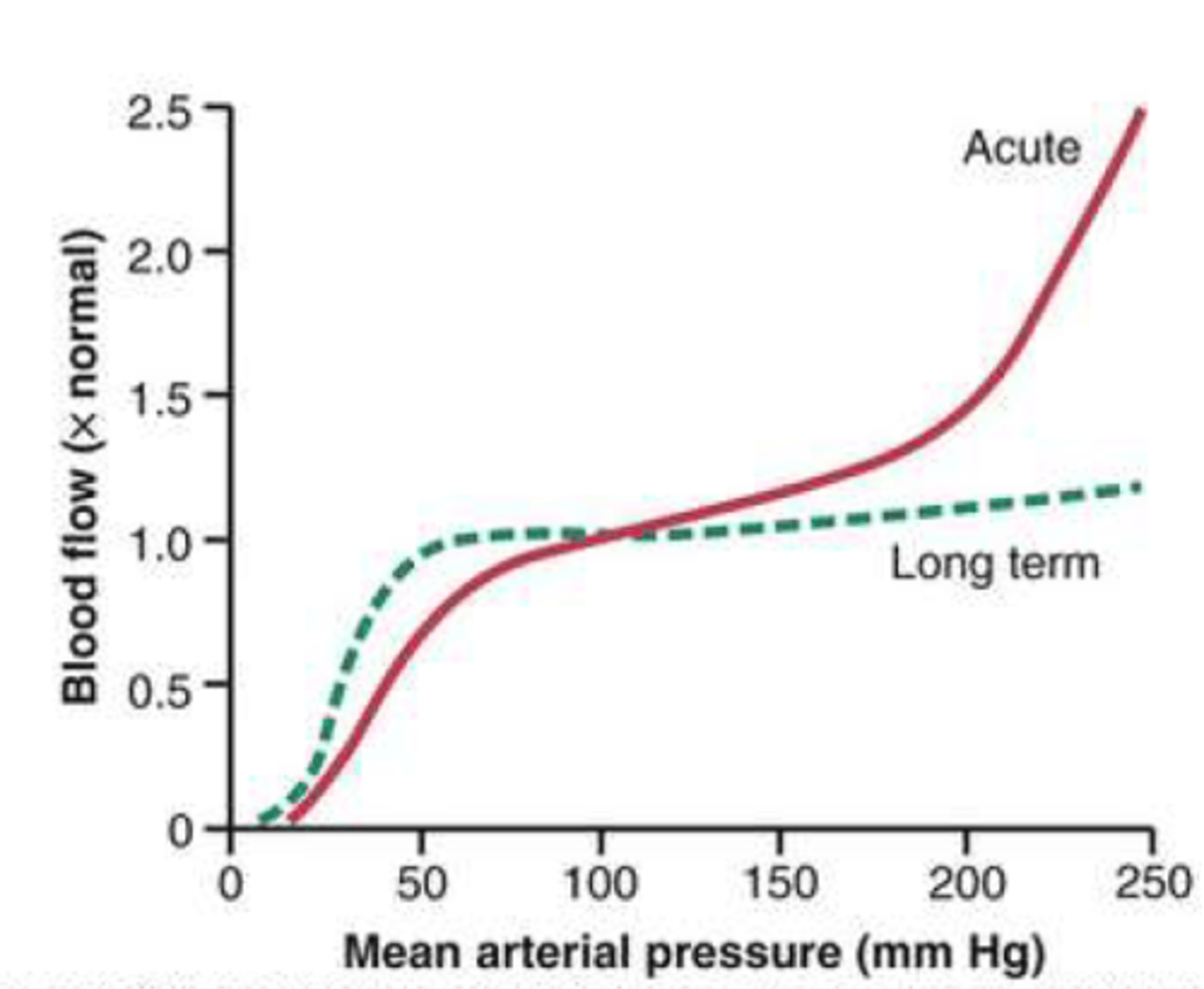
Pressure-Flow Autoregulation
Intrinsic ability of a vascular bed to regulate its own flow over a wide range of intravascular pressures
Reserve
-The capacity for increasing flow within a bed at any given pressure
-No additional capacity to increase flow
Reserve
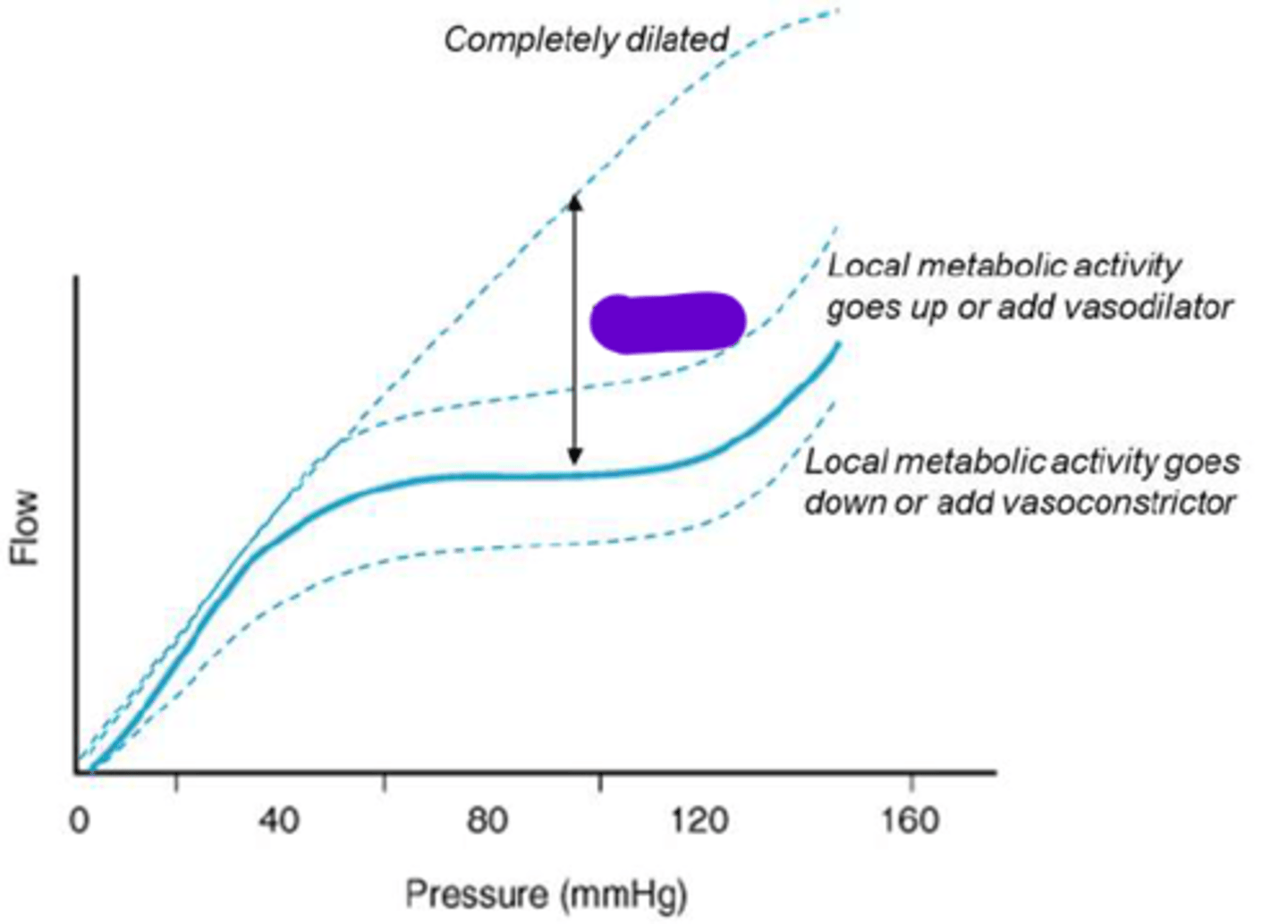
Autoregulatory Range
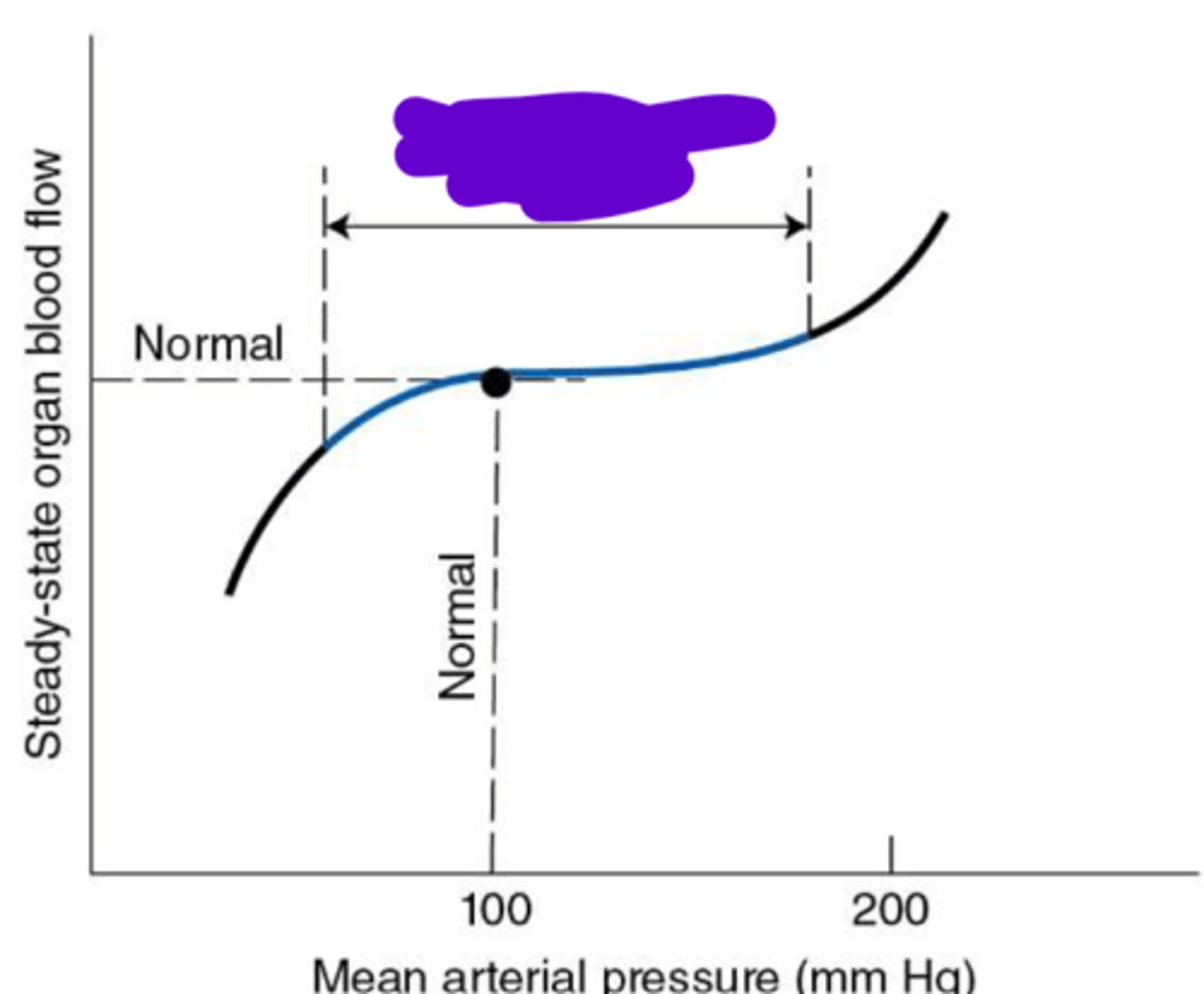
60-140 mmHg
range where flow is independent of pressure due to autoregulation
Endothelial-derived relaxing factors
EDRF
Endothelial-derived constriction factors
EDCF
Endothelial-derived hyperpolarizing factor
EDHF
Myoendothelial Junction
-communication between endothelium and smooth muscle cells
-gap junctions can be found here
-Prostaglandins
-EDHF
-Nitric Oxide (NO)
Substances synthesized by endothelial cells lining the blood vessels that when released, alter the degree of relaxation or contraction of vascular smooth muscle
Vasodilation
Lipophilic gas released from endothelial cells in response to stimuli to cause ___________________
NO
viscous flow of blood (or some vasoconstrictors, ANG II) causes shear stress on vascular walls that contorts endothelial cells to induce _______ release
M3
receptor for parasympathetic dilation of vascular smooth muscle
α1
recepor for sympathetic constriction of vascular smooth muscle
Histamine
• Causes arteriolar dilation and venous constriction
• The combined effects cause ↑Pc and increased filtration out of the capillaries resulting in local edema
• Released in response to tissue trauma
Bradykinin
• Causes arteriolar dilation and venous constriction
• Produces increased filtration out of capillaries and local edema
Serotonin
• Causes arteriolar constriction and is released in response to blood vessel damage to help prevent blood loss
Vasodilators
E-series prostaglandins are ____________________
Vasoconstrictors
F-series prostaglandins are _____________________
Vasodilator
Prostacyclin is a ____________________ in several vascular beds
Vasoconstrictor
Thromboxane A2 is a ______________________
Endothelin
• Potent vasoconstrictor, present in endothelial cells via endothelin converting enzyme (ECE)
• Binds to G-protein receptors in VSMCs and endothelial cells
• Formation & release stimulated by Ang II, ADH, thrombin, cytokines, ROS, & shear stress
Endothelin
• Inhibited by endothelial derived vasodilators (e.g., NO), specifically when ETB receptors are bound
• Implicated in pathogenesis of HTN, coronary vasospasm, and HF
• Presence increased with endothelial damage
Endothelial Dysfunction
-Major role in the development of atherosclerosis
-associated with diabetes/metabolic
syndrome, hypertension, smoking, and physical inactivity
-shift to a proinflammatory, prothrombic state with impaired vasodilation
• Involves decreased NO bioavailability
• Impaired flow mediated dilation (FMD); assessed by ultrasound in brachial artery
Hours to Weeks
time span fo long term control of blood flow
Normal
If MAP is chronically elevated over time, local blood flow approaches _____________ despite increased pressure
Vascular Remodeling
-important when metabolic needs change
-arterioles and capillaries can change in number and size to adapt
Vascular Remodeling
1. ↑ in Angiogenic factors & formation of new blood vessels
2. Rarefaction of vessels
3. Development of collateral circulation in response to occlusion
4. Vascular remodeling in response to chronic changes in blood flow or pressure
Vascular Remodeling
Ability to form blood vessels is the defining characteristic of an endothelial cell
Hyperemia
redness of the skin due to increased blood flow
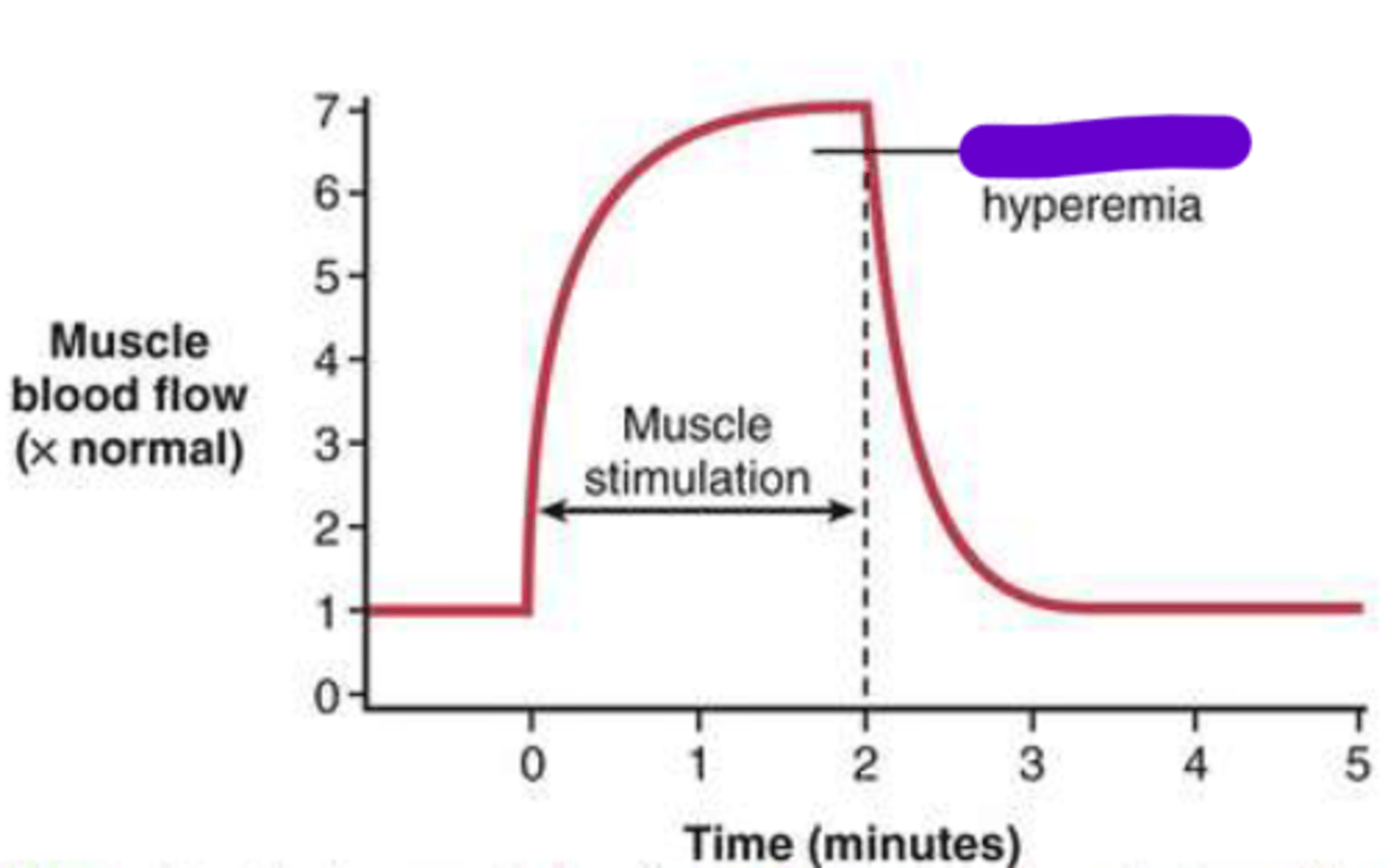
Active Hyperemia
Increased blood flow to a tissue when its energy demands/metabolism increase
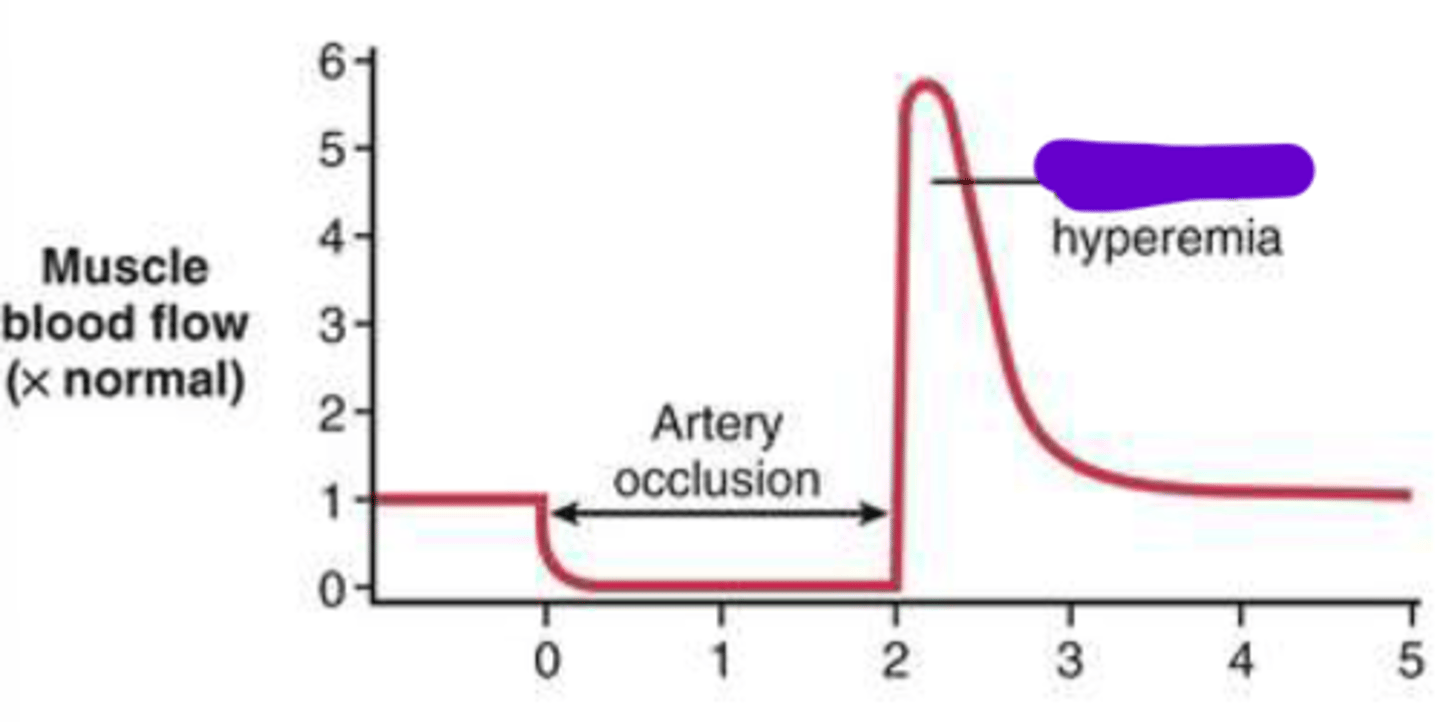
Reactive Hyperemia
-Exaggerated flow that occurs after temporary ischemia
-accumulation and washout of metabolites
-continues until O2 debt is repaid
Reactive Hyperemia
Active Hyperemia
Splanchnic Circulation
blood flow through the stomach, small intestine, large intestine, pancreas, spleen, & liver
Splanchnic Circulation
-Vascular supply is highly interconnected & primarily occurs by way of celiac, superior & inferior mesenteric arteries
-Provides collateral pathways, lessens the risk of ischemia in the event of occlusion
No
does the circulatory system distribute splanchnic blood flwo equally to all digestive organs
increases
Blood flow _______________ sequentially as food progresses along GI tract
Liver
what organ is in parallel AND series with other splanchnic organs?
30%
Splanchnic Circulation receives _____% of CO
Constrict
During high sympathetic output (exercise, hemorrhage); splanchnic arteries and veins __________________
Postprandial Hyperemia
Blood flow to GI tract increases 8 fold following meal
Countercurrent Exchange
the exchange of a substance between two fluids flowing in opposite directions
Microvessels in villi
in splanchnic circulation, what vessels branch into numerous capillaries that are highly permeable to facilitate absorption of nutrients from GI tract
15%
Cerebral Circulation receives about _____% CO
Cerebral Circulation
• Averages 50-60 mL/min/100g
• Remains relatively constant (autoregulation)
-neural, myogenic, and metabolic control
vasoconstriction
in cerebral circulation: increase in transmural pressure results in _______________________
Oxidative
(therefore intolerant of ischemia)
describe brain metabolism
Cerebral Circulation
-no lymphatics
• Blood flow highly autoregulated:
• Localized active hyperemia primarily via increased pH
-BBB
Respiratory Acidosis
-hypercapnia (high blood Pco2) cayses global drop in brain pH and global brain hyperemia
Stroke
-any disruption of brain blood flow
-can be ischemic or hemorrhagic
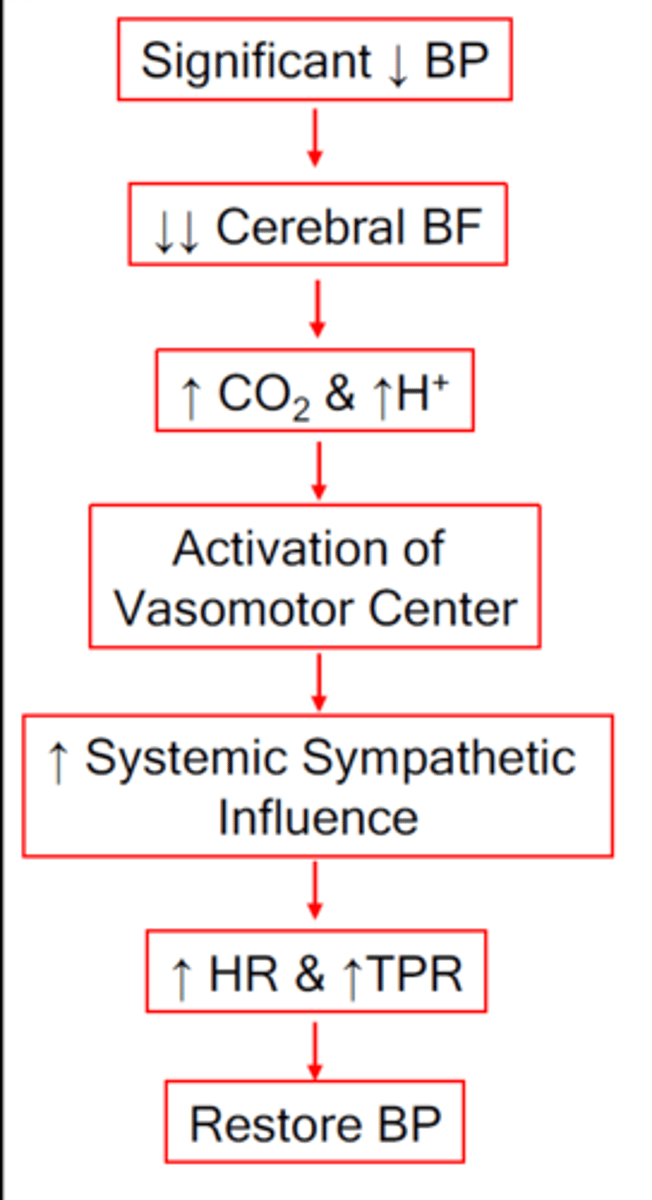
[CO2] & [H+]
If blood flow severely decreases causing cerebral ischemia, local ______________ and _______________increases greatly
Medulla
In the ischemic pressor response, there is stimulation of the sympathetic vasomotor control areas in the _________________
Ischemic Pressor Response
-stimulation of sympathic vasomotor control
-systemic arterial pressure rises as high as the heart can pump to clear out CO2 and H+
-can elevate MAP
-can cause occlusion of peripheral vessels
Ischemic Pressor Response
-operates as emergency pressure control system when cerebral arterial pressure and blood flow decreases to lethal levels
• <60 mmHg, with greatest stimulation at 15-20 mmHg
Cushing's Reflex
-special type of ischemic response resulting from ↑CSF pressure
• Initiates CNS ischemic response that causes the arterial pressure to rise
Ischemic Pressor Response
Aerobic Exercise
Capacity to increase blood flow > 20-fold during __________________
At Rest
At Rest or During Exercise:
• Sympathetic (and myogenic) tone; high
vascular resistance and low flow
• Low O2 extraction
During Exercise
At Rest or During Exercise:
• active hyperemia
• Low vascular resistance and high flow
• High O2 extraction
Cutaneous Circulation
• Sympathetic inputs
• Sympathetic adrenergic
• Sympathetic cholinergic
• Temperature regulation
Vasoconstriction
in cutaneous circualtion, cold results in sympathetic adrenergic response causing __________________
Vasodilation
in cutaneous circualtion, heat results in withdrawal of sympathetic response causing __________________
Sweating/Vasodilation
in cutaneous circualtion, High heat and stress results in sympathetic cholinergic response causing __________________
Right and Left Coronary Artery
Entire blood supply to myocardium derives from ______________________________
5%
Coronary Circulation receives ______% of CO
Coronary Circulation
• Averages 70 mL/min/100g
• Work of heart can increase 6-9x and coronary flow can increase 3-4x to supply heart
• Adenosine and NO - most important vasodilators here
Resting
In coronary circulation, High O2 extraction under ________________ conditions (70 - 80%) - meet
increased demand by increasing flow.
Adenosine
key metabolic dilator of coronary circulation
Endothelial NO
important for flow mediated filation in coronary circualtion
Sympathetic
___________________ stimulation of the heart increases coronary flow due to increased heart rate, and contractility (active hyperemia).
Endocardium
in reference to coronary circulation, what is susceptible to ischemia due to vascular compression during systole
Left coronary artery
What artery?
Early Systole: isovolumetric contraction of ventricle compresses vessels & aortic pressure is low, reversed flow
Mid-Late Systole: as aortic pressure increases so does coronary
flow, but doesn’t peak
Diastole: ventricles relaxed & aortic pressure still high, coronary
flow is high (~80%)
Right Coronary Artery
Which Artery?
Systole: contributes more flow due to lower wall tension of right ventricle, no reversal
Diastole: virtually negligible augmentation of flow