Final - Awasthi’s study guide
1/120
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
121 Terms
Obj. 1
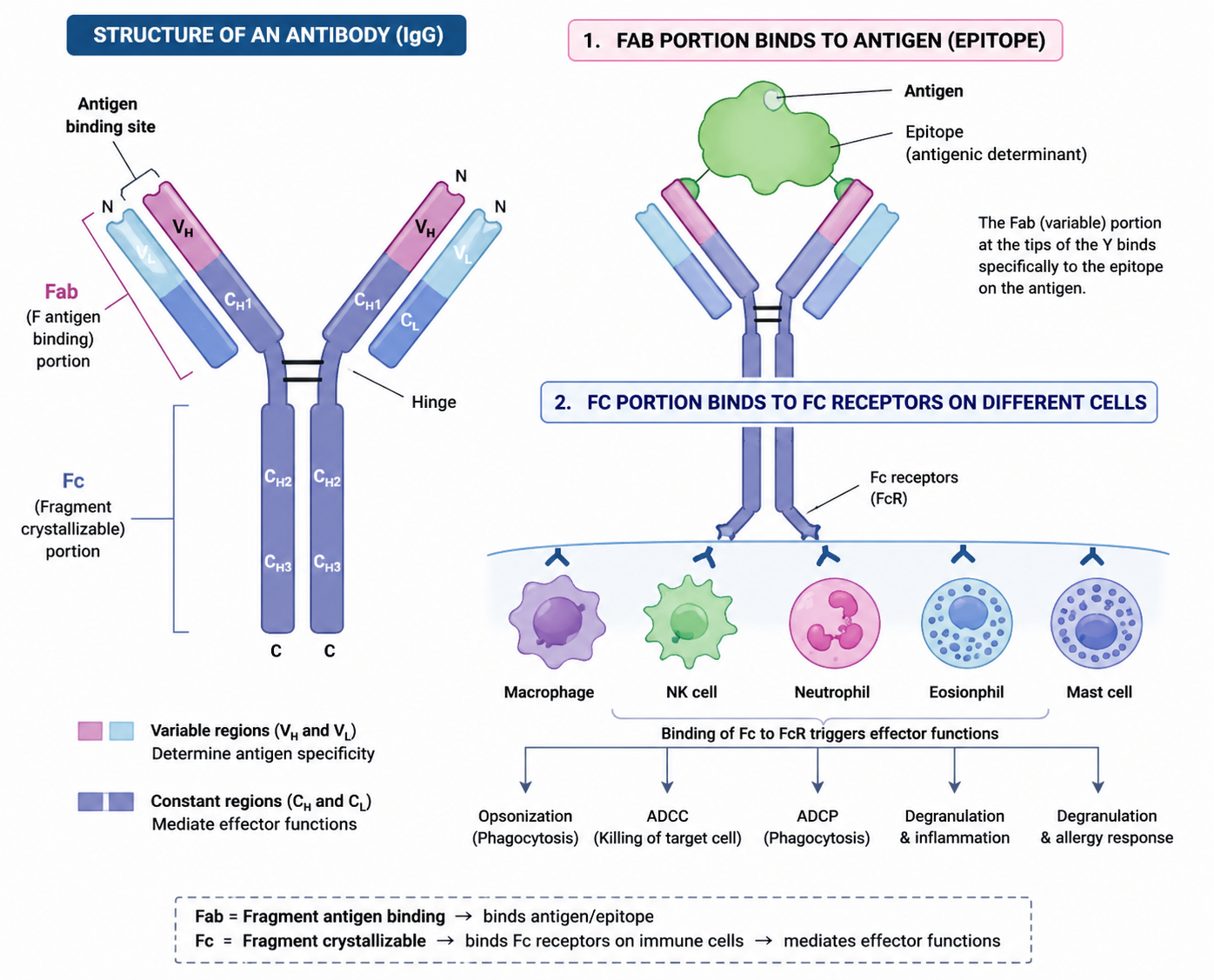
Antibody structure and types, parts of antibodies, and their unique characteristics.
🔹What is an ANTIBODY (Ab)?
A Y-shaped protein produced by Plasma cells that specifically BINDS an ANTIGEN.
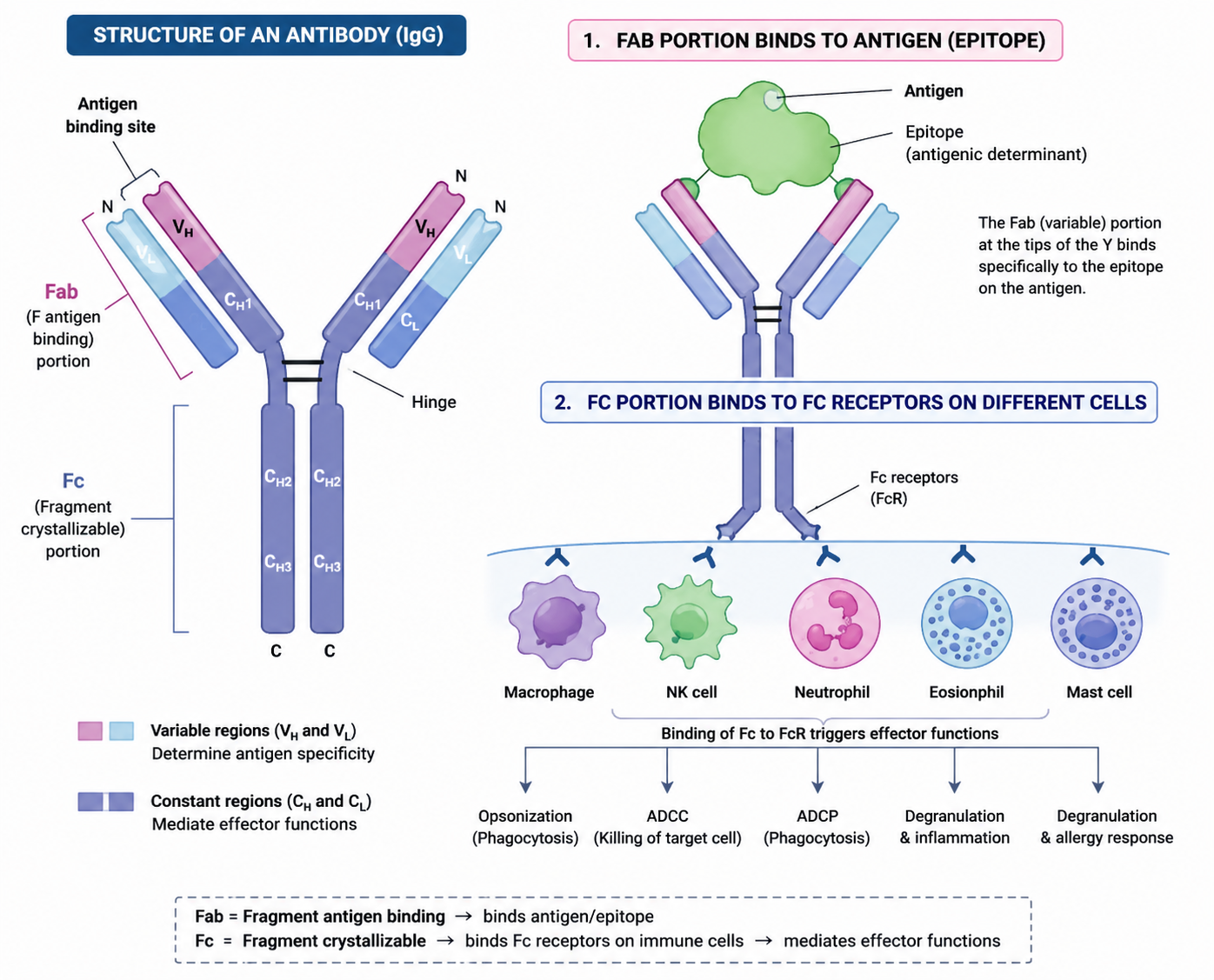
What are the 4 chains that make up an Ab?
2 Light chains + 2 Heavy chains
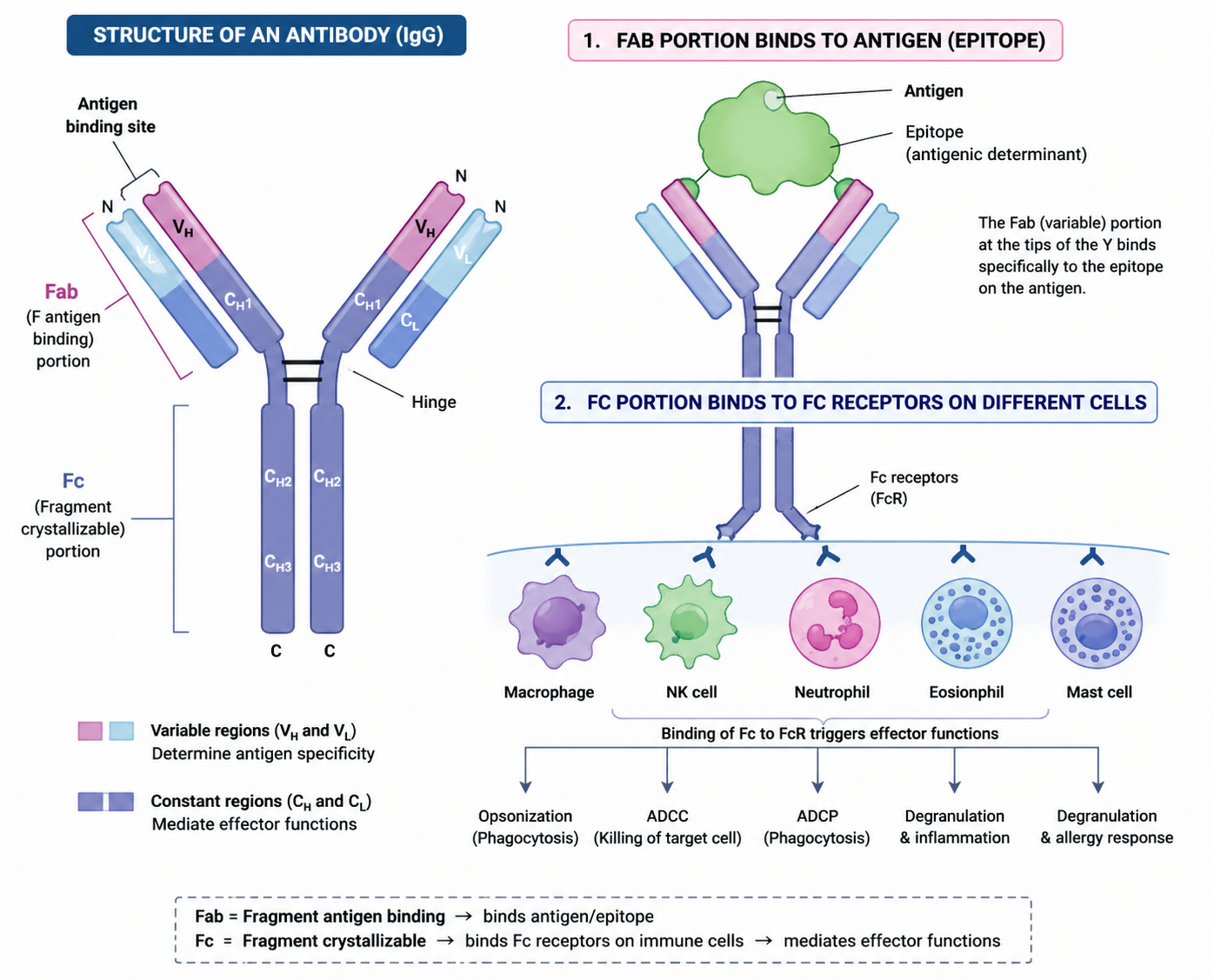
What connects the heavy chains & light chains?
Disulfide bonds.
Which part of the Ab binds to Antigen?
Fab region.
What does Fab stand for?
Fragment Antigen Binding.
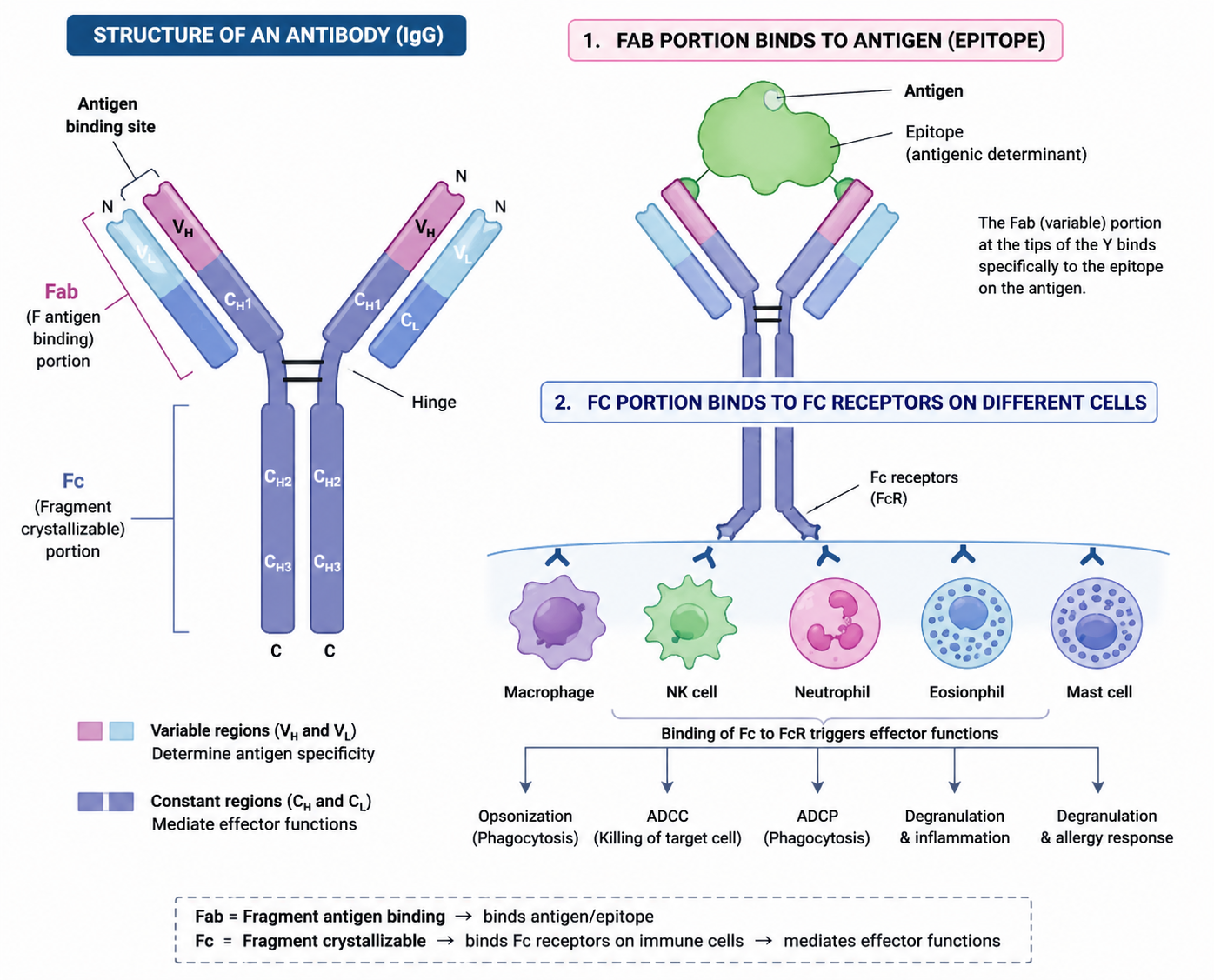
What is the function of the Fab region?
Binds antigen/epitope
Determines specificity
What is the Fc region?
What is it responsible for?
The Fragment crystallizable region of the Ab.
It is responsible for biologic effect/effector functions.
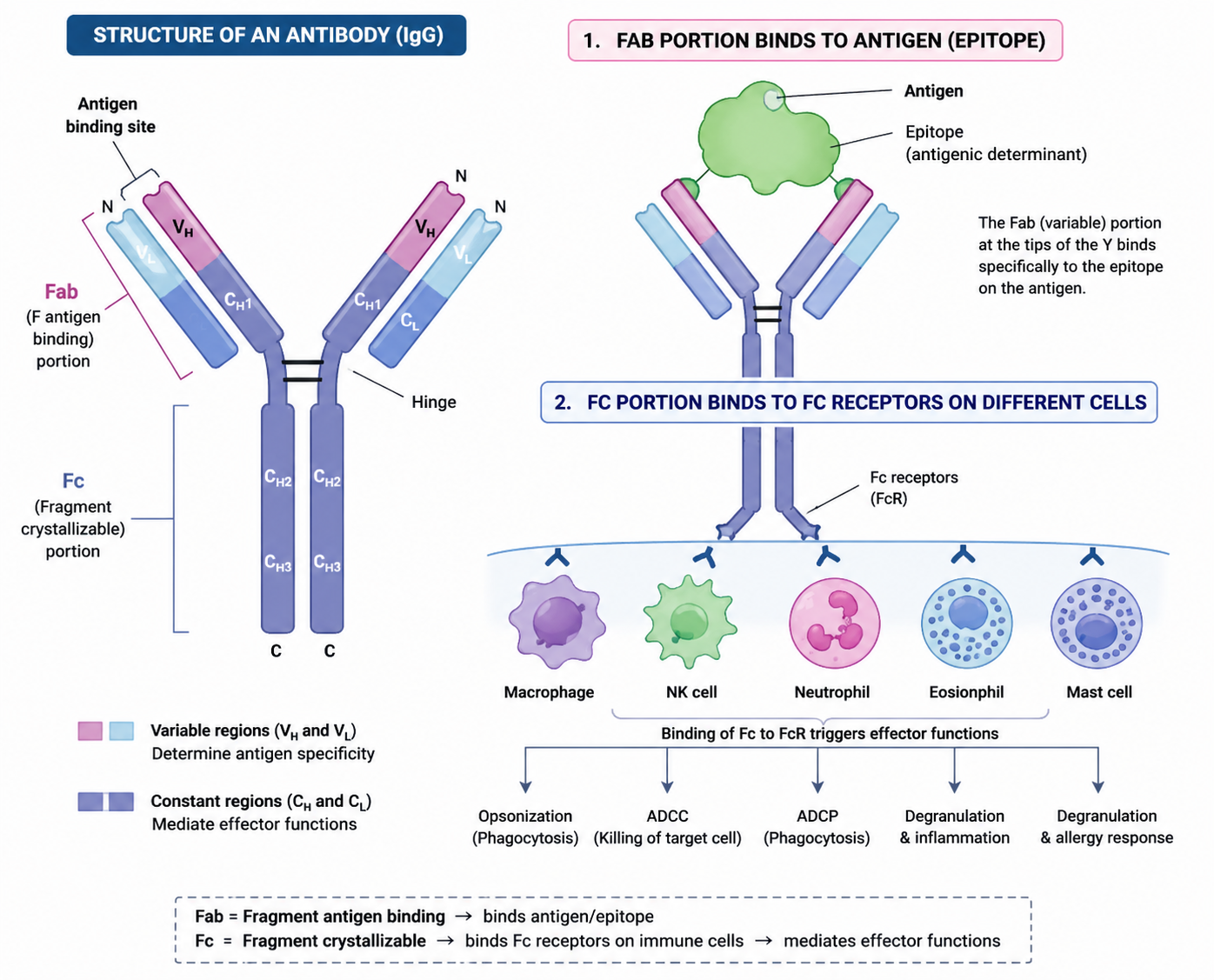
What are Fc region functions?
Complement activation
Opsonization
ADCC
Mast cell sensitization
What is the Variable region?
Located @ the tips of the Fab arms & determines:
Antigen specificity
Epitope recognition
What is the Constant region?
Determines:
Ab class (IgG, IgM, etc.)
Biologic function
What is a Paratope?
Ab binding site that recognizes the Antigen.
Located: on the Ab
What is an Epitope?
Specific part of an antigen recognized by the antibody.
Located: on the Antigen
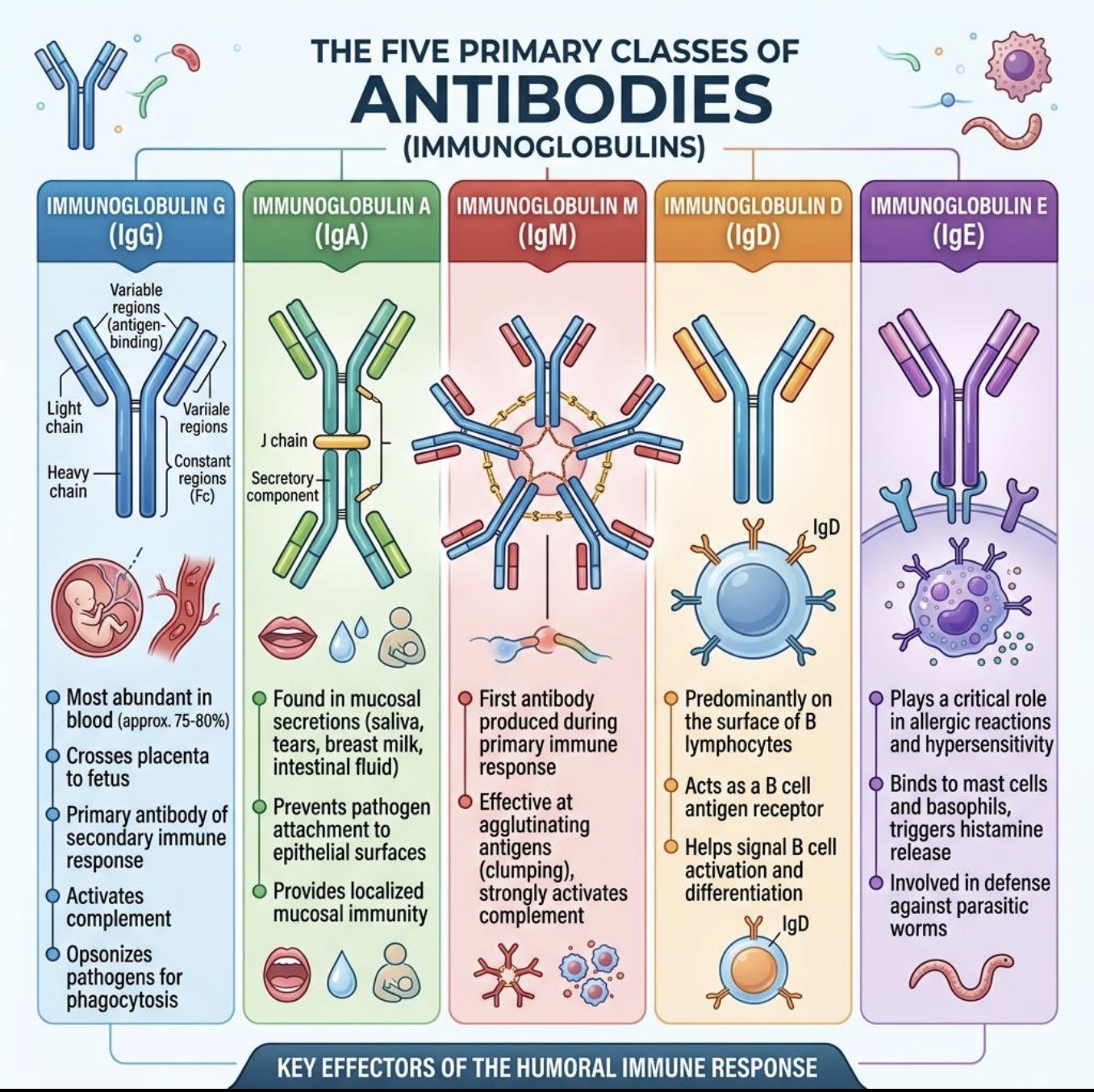
What are the 5 Ab classes?
IgG
IgM
IgA
IgE
IgD
💭Think: DAMAGE => Ig - “DAMGE”
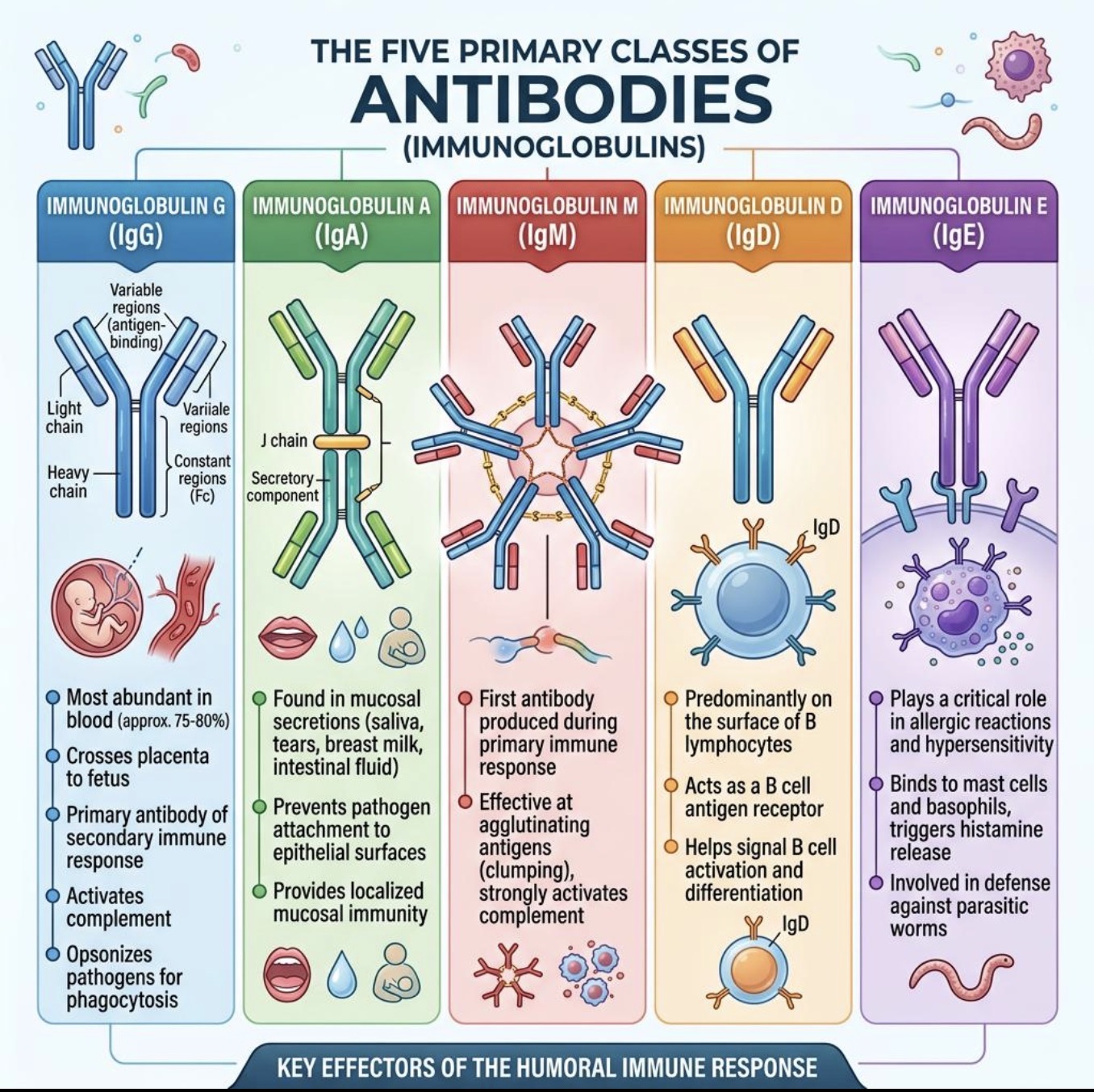
What is the most abundant Ab in the SERUM?
IgG
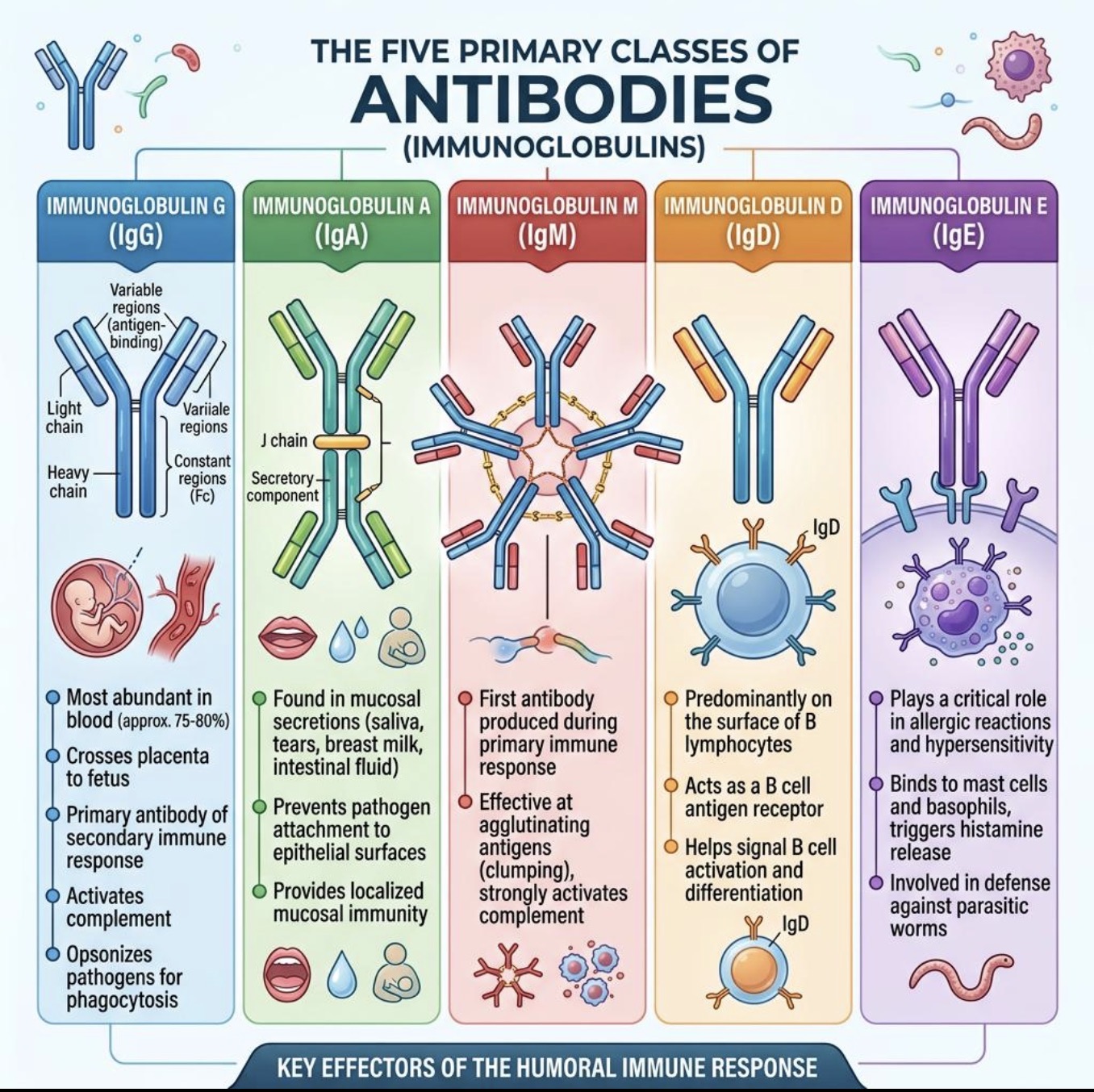
Which antibody crosses the placenta?
IgA
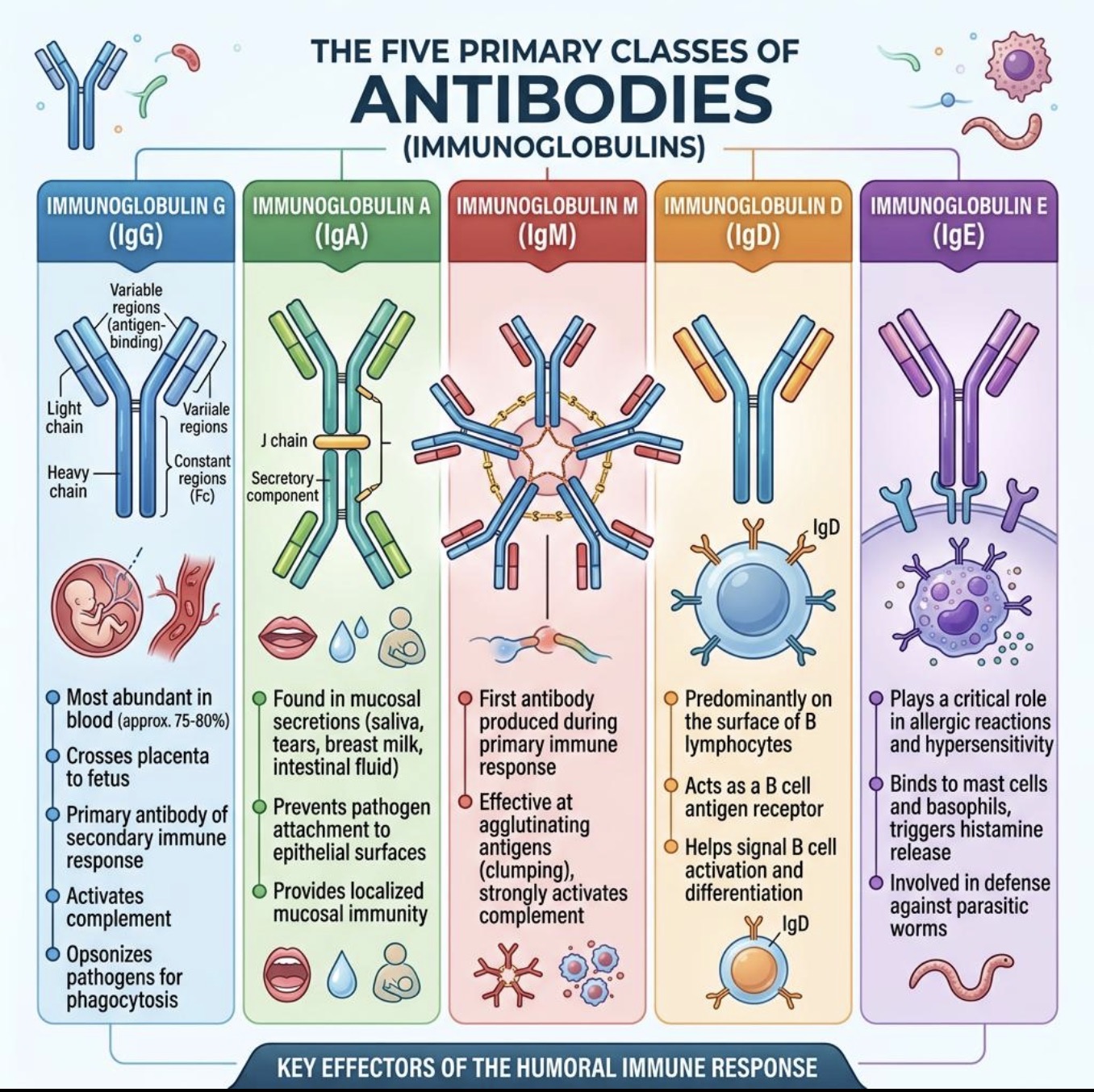
Which antibody is most important for toxin neutralization?
IgG
Main functions of IgG?
Neutralization
Opsonization
Complement activation
Secondary immune response
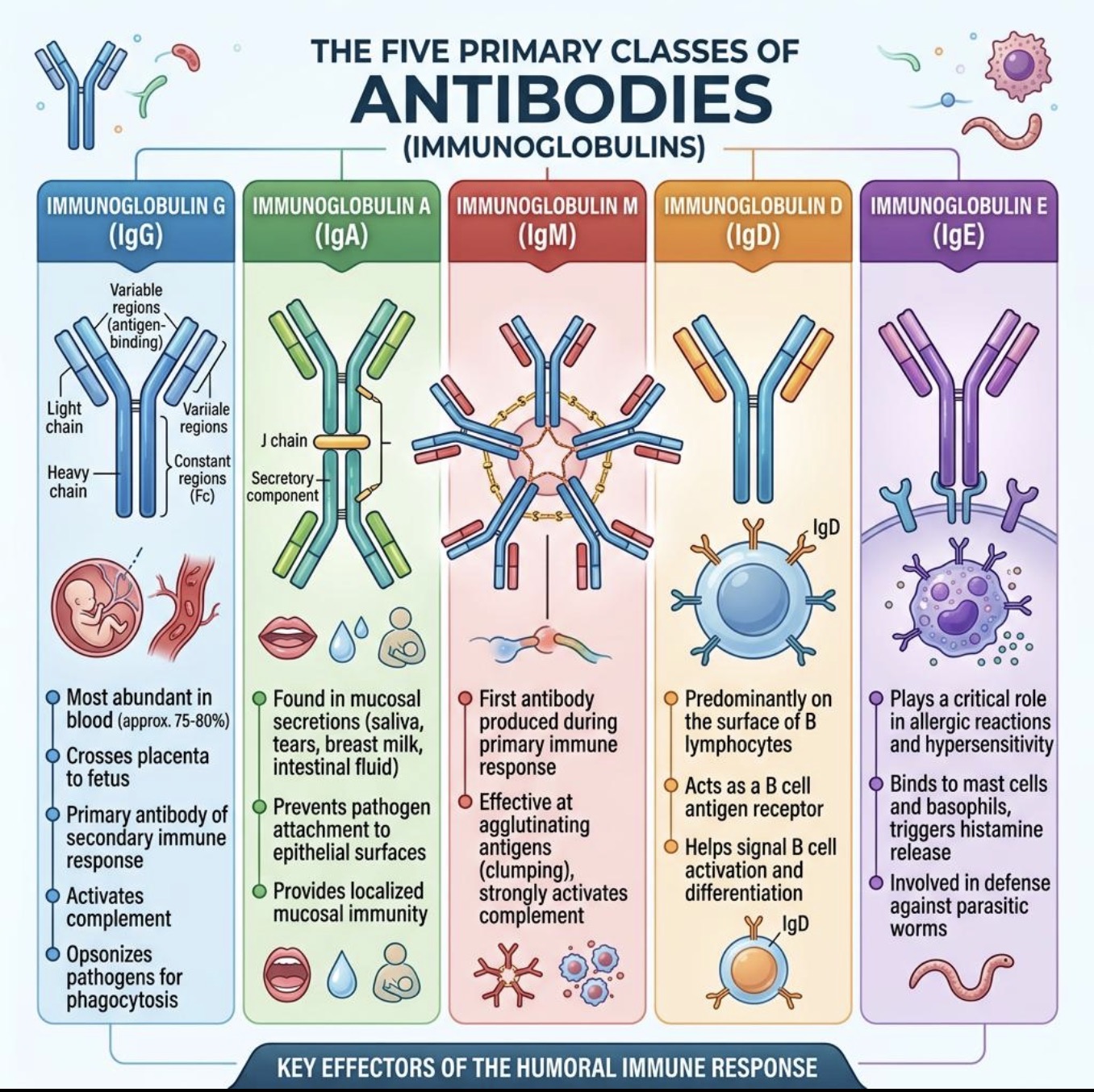
Which antibody is produced first in a primary immune response?
IgM
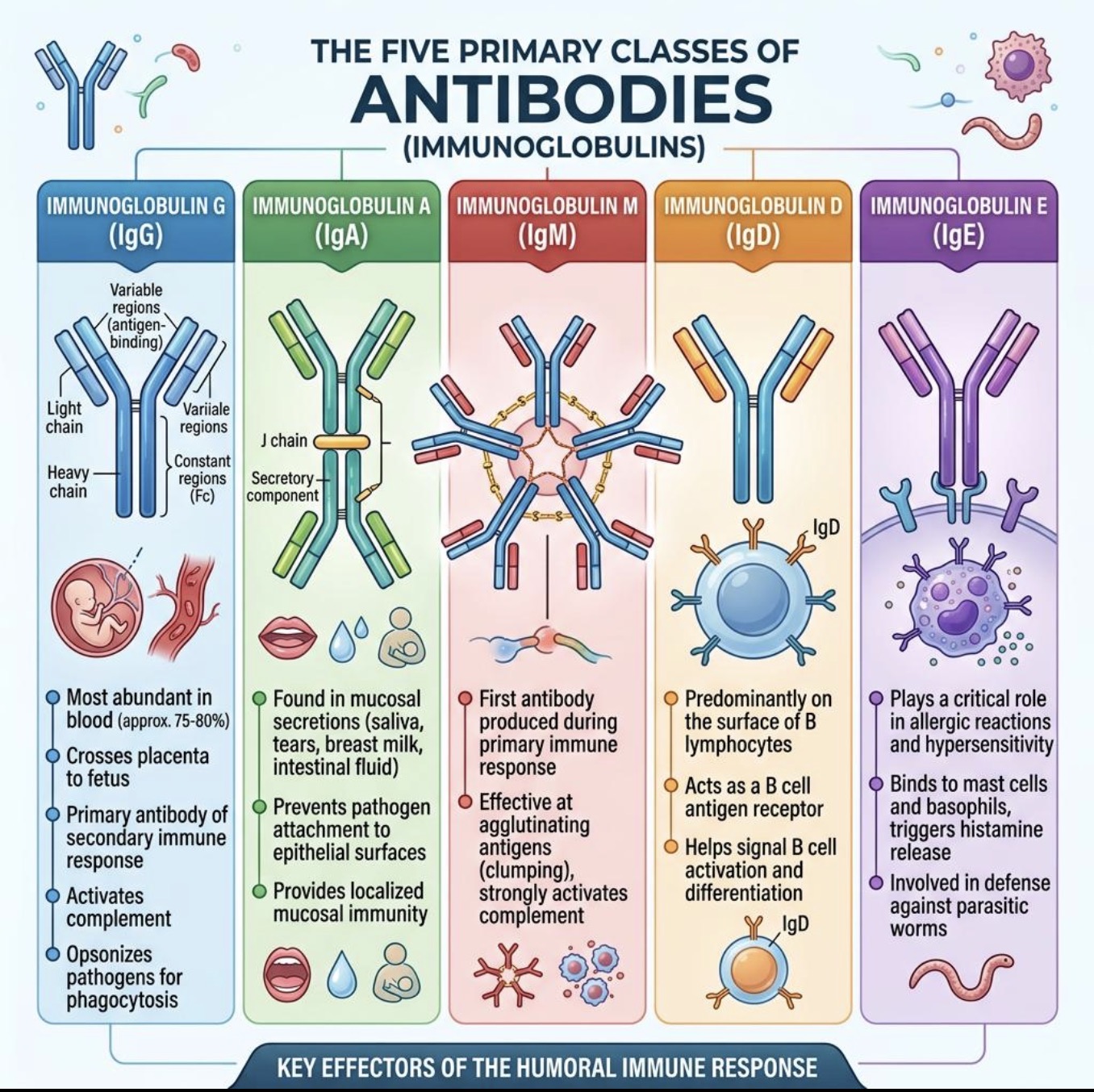
What is unique about IgM structure?
pentamer
Which antibody is best at activating complement?
IgM
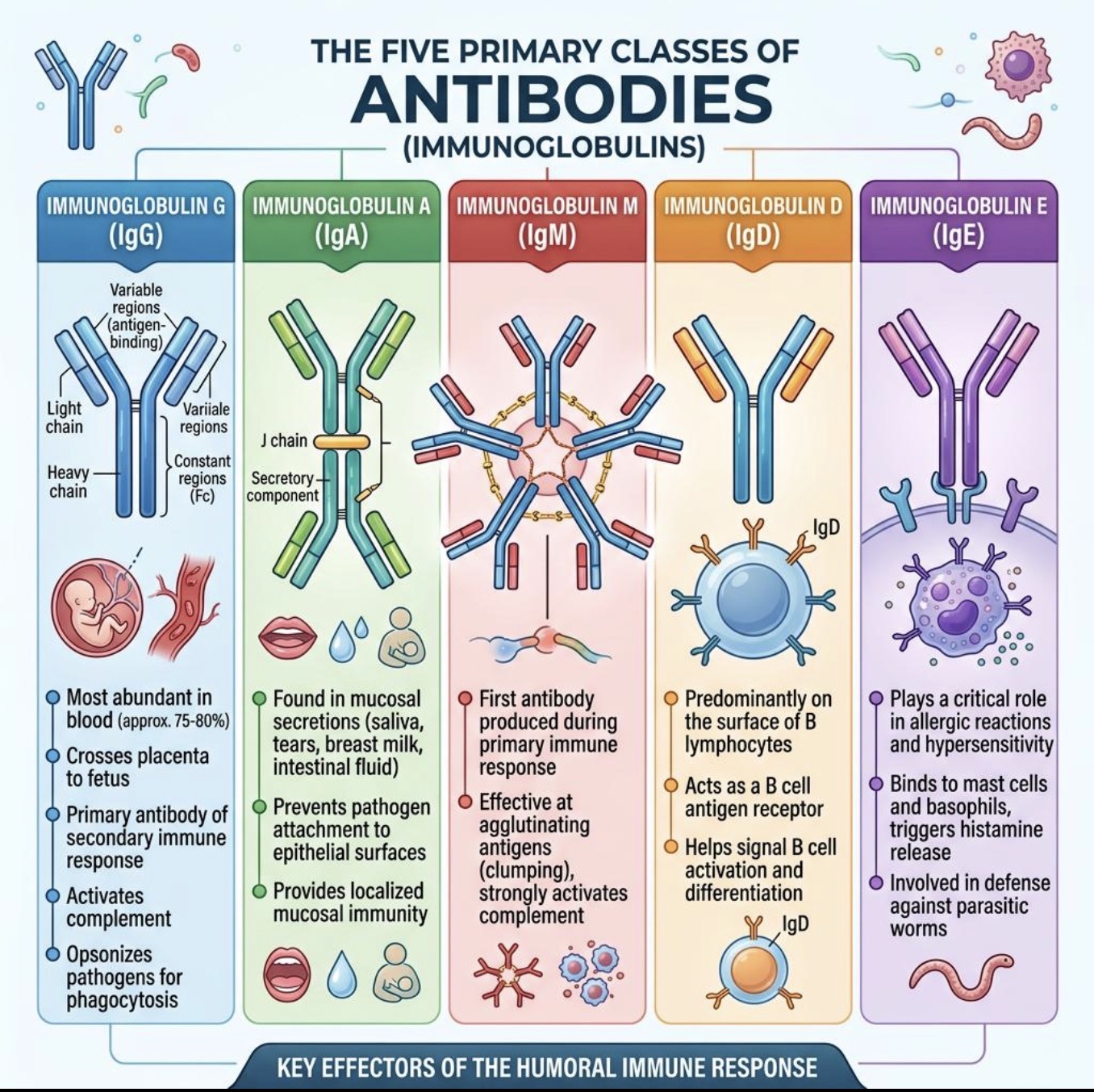
Why does IgM have high avidity?
Because the pentamer has many antigen-binding sites.
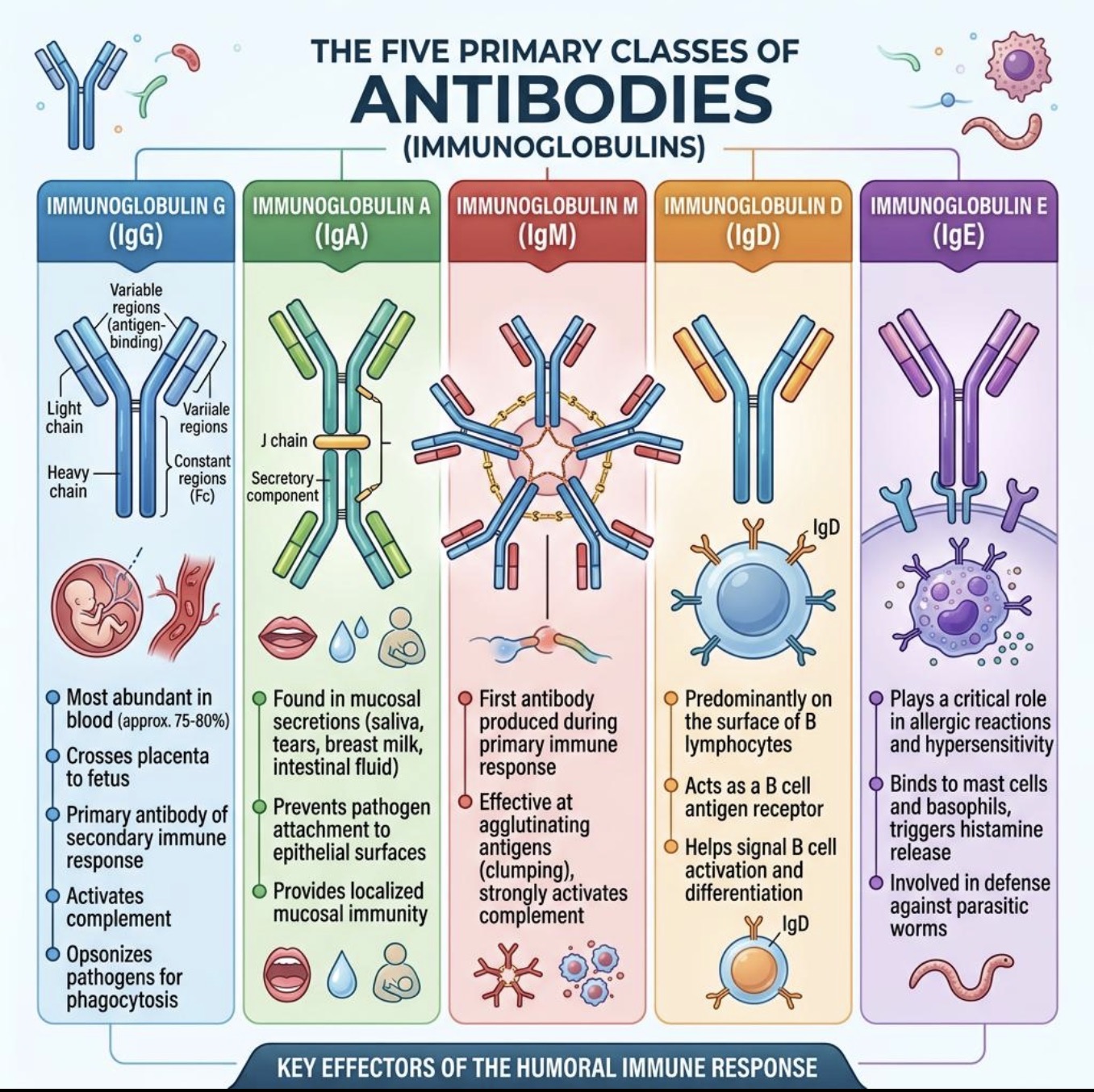
What is the major mucosal antibody?
IgA
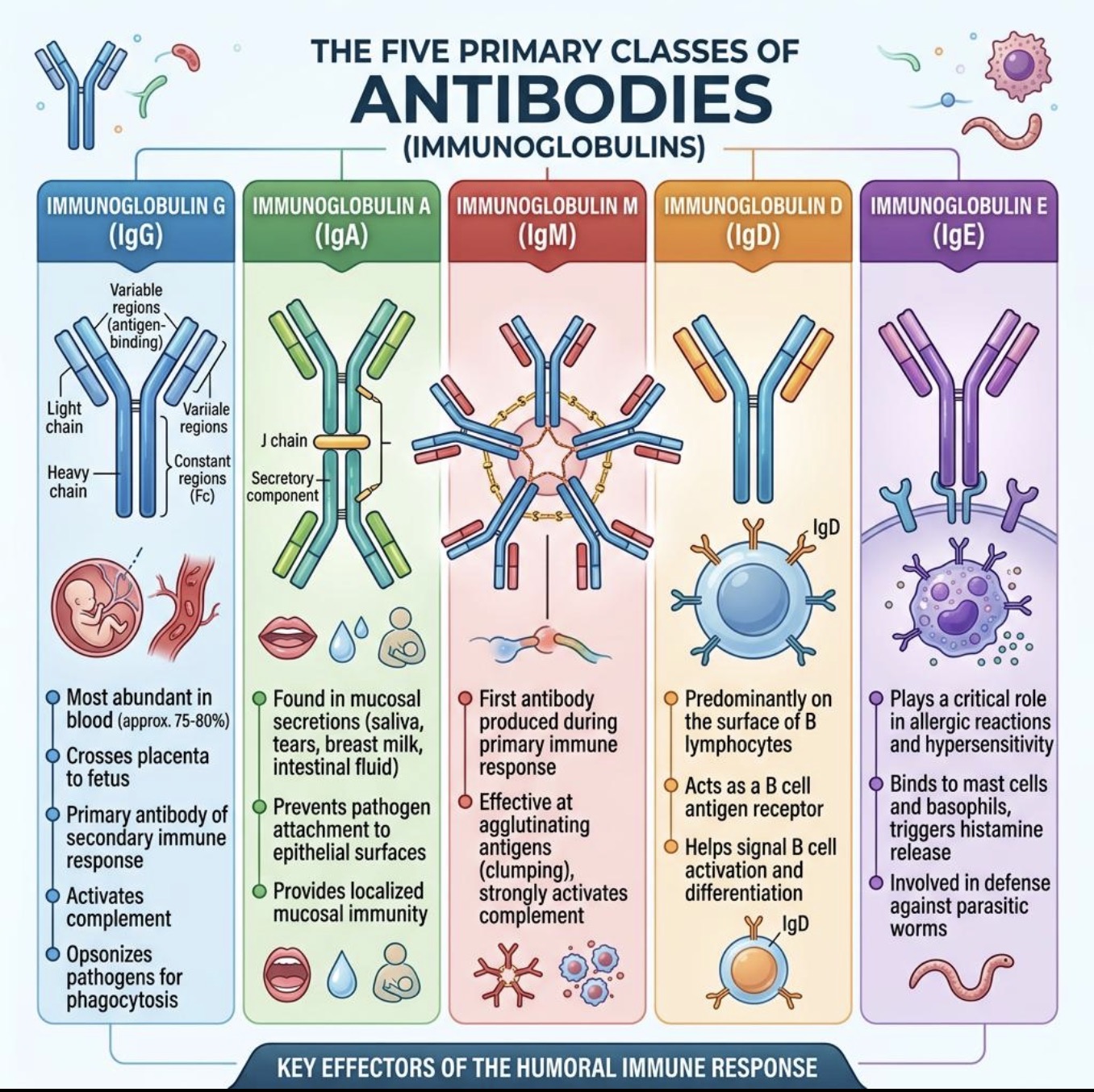
Where is IgA found?
Saliva
Tears
Mucus
Breast milk
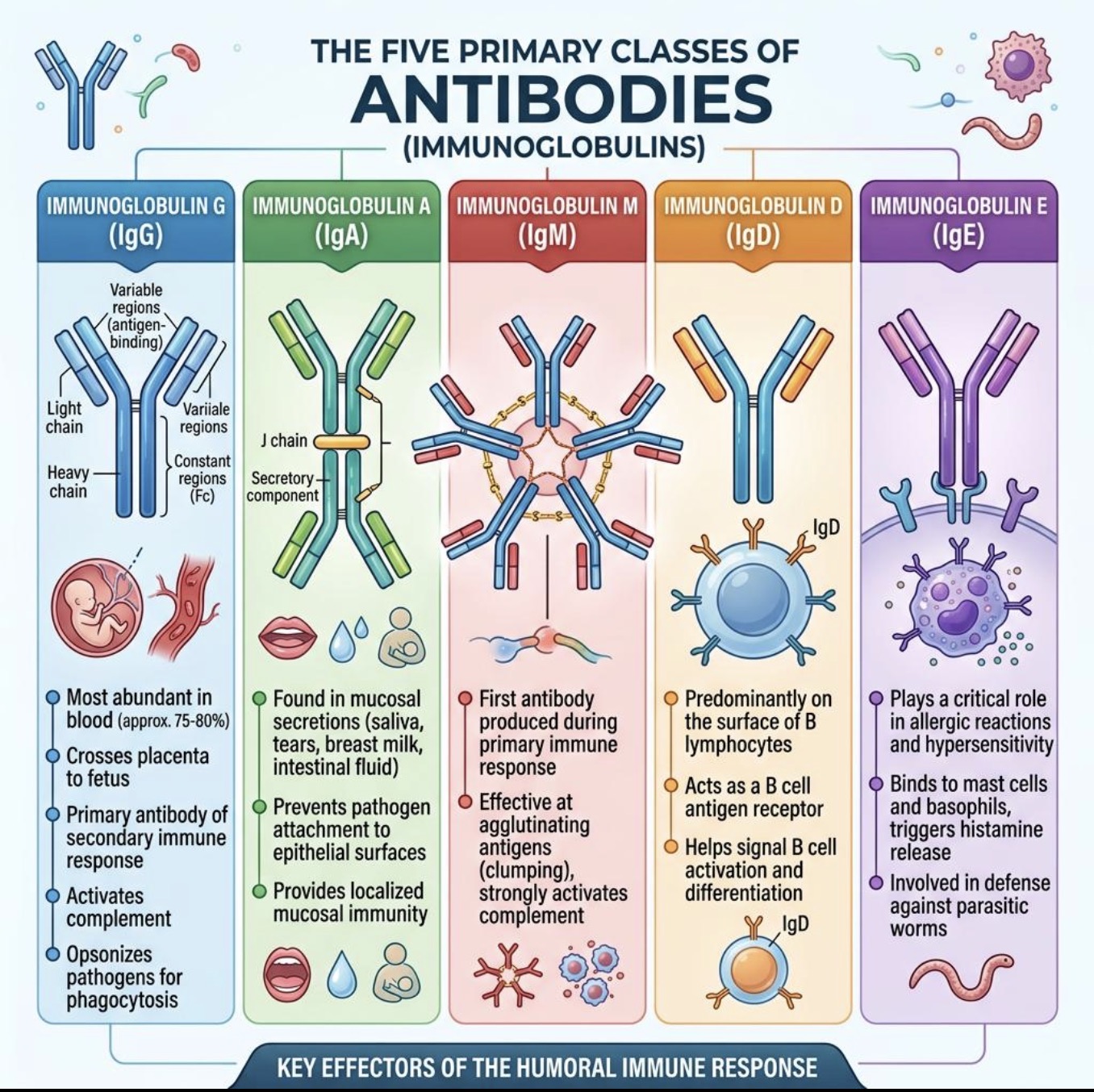
Main function of IgA?
Saliva
Tears
Mucus
Breast milk
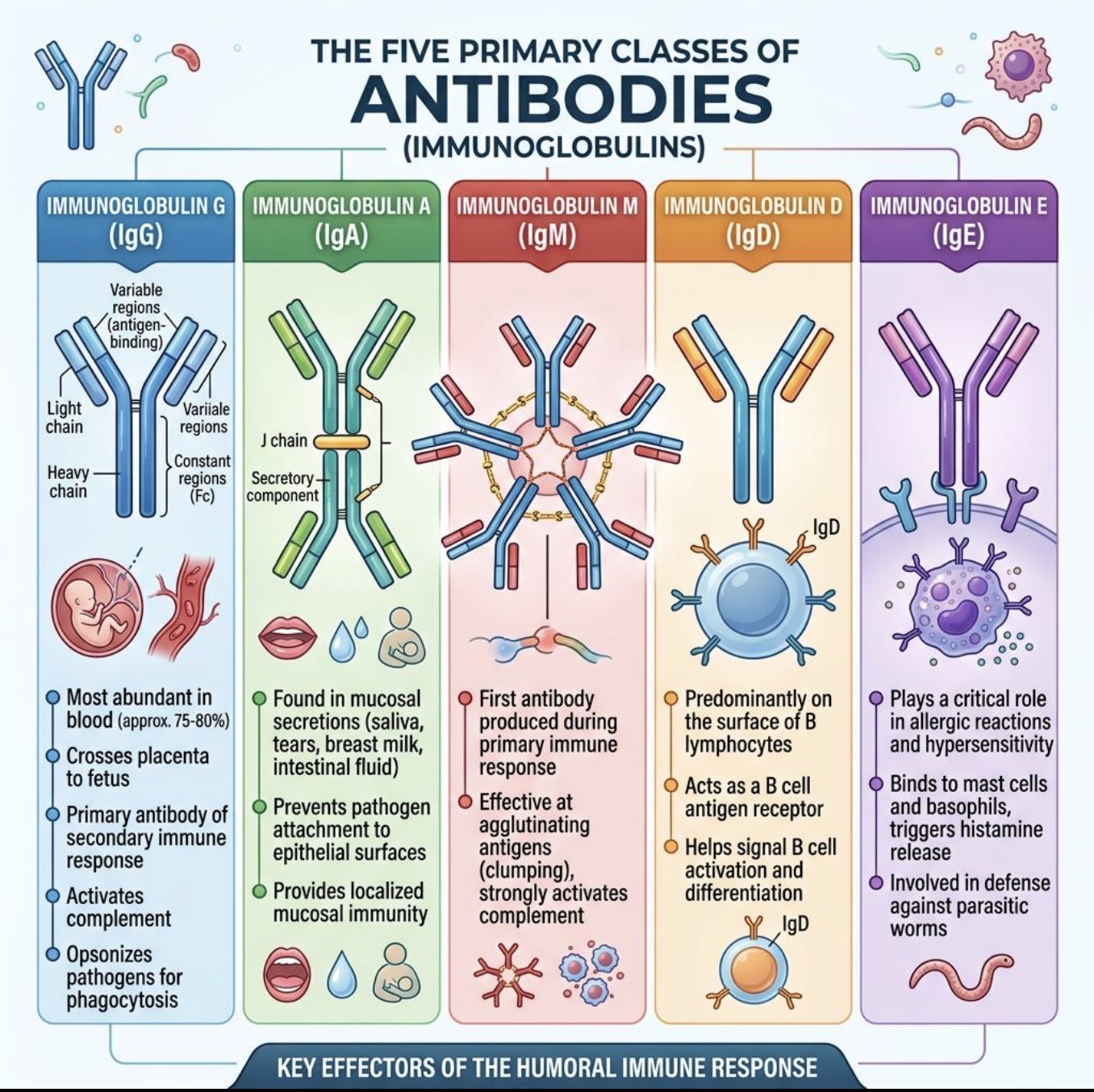
What does secretory IgA (sIgA) do?
Protects mucosal surfaces and helps prevent reinfection.
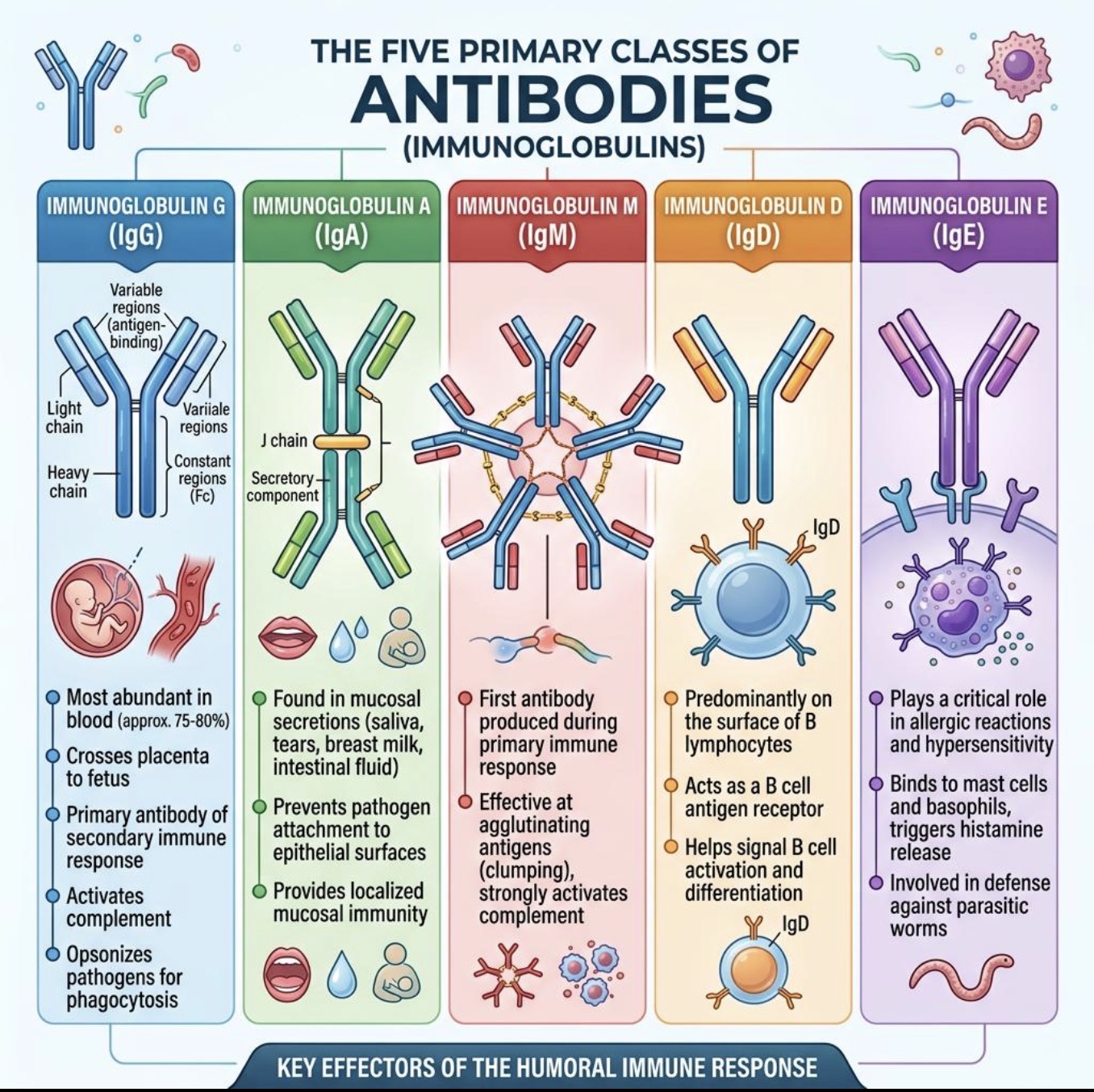
Which antibody mediates allergy?
IgE
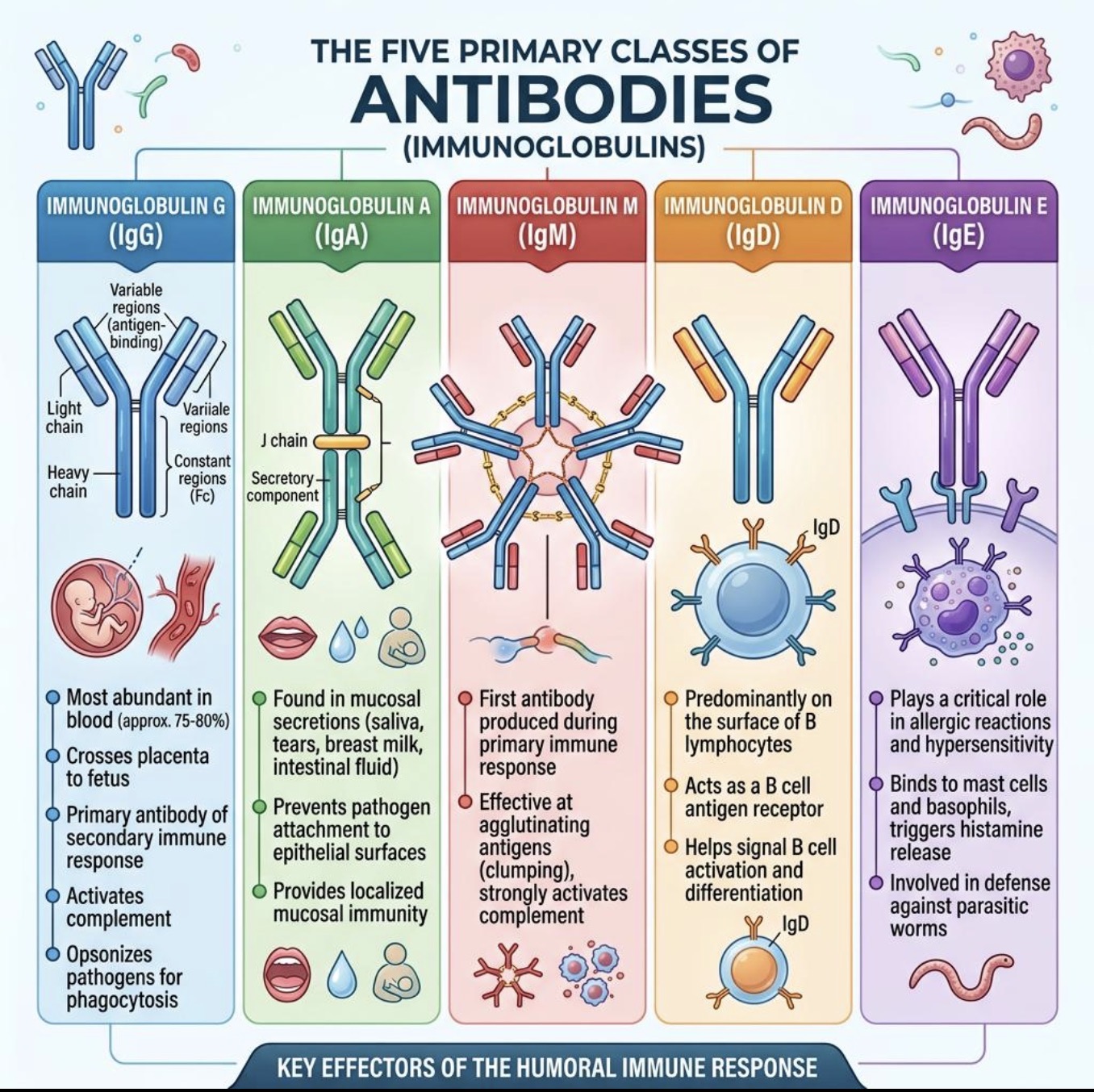
Which cells does IgE bind?
Mast cells
Basophils
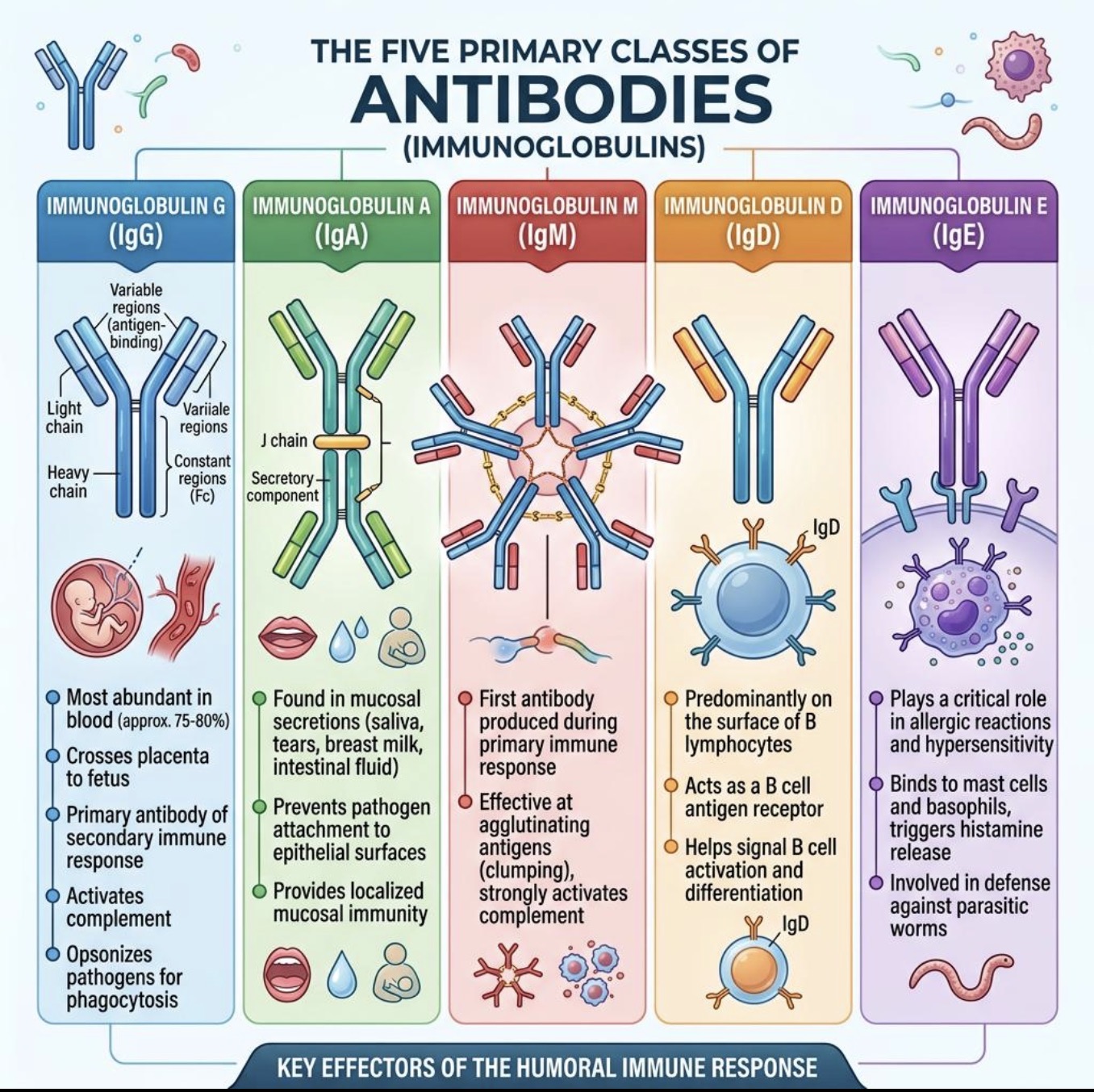
What else is IgE involved in besides allergy?
Parasitic infections.
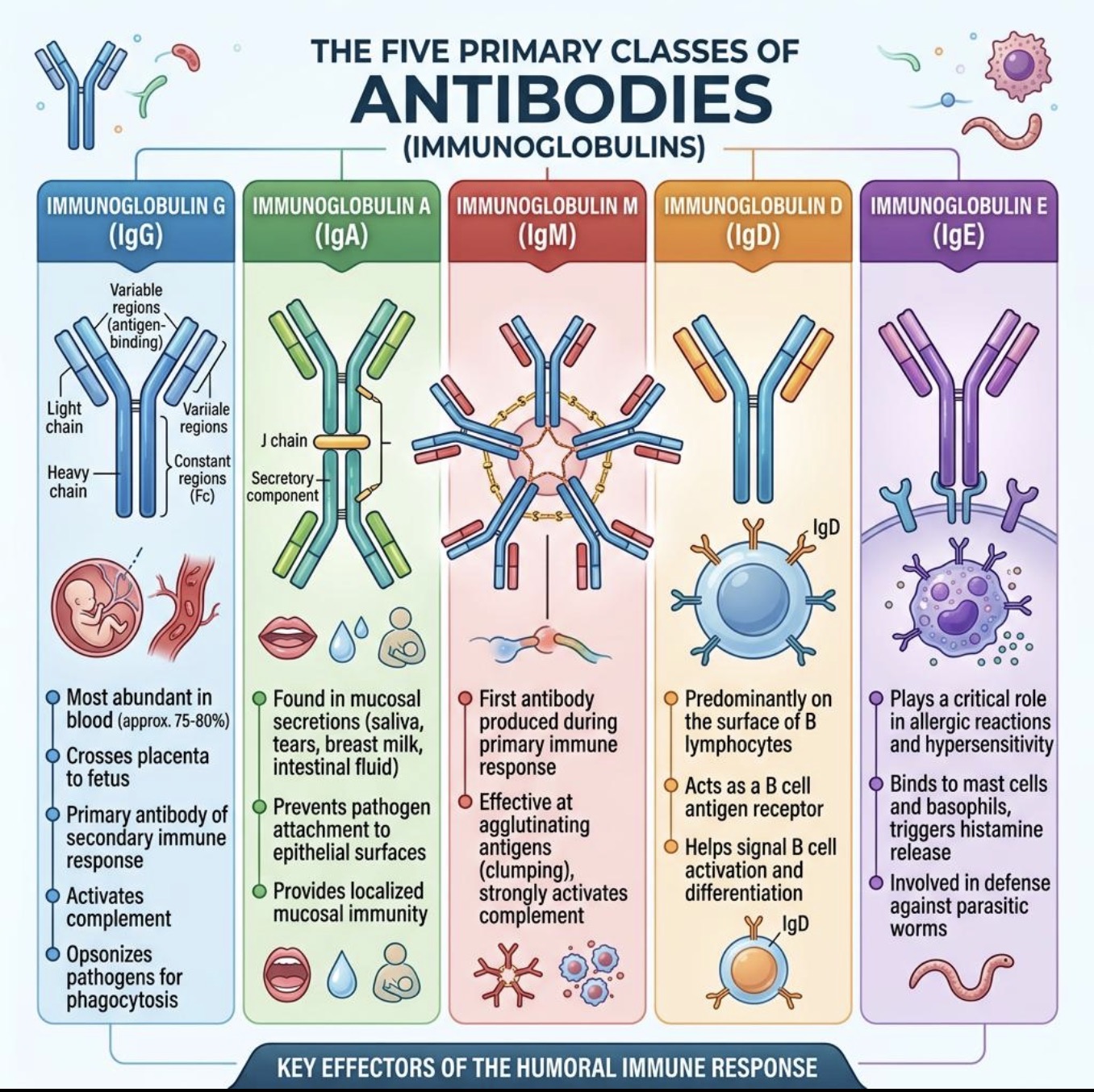
Which monoclonal antibody targets IgE?
Omalizumab (Xolair)
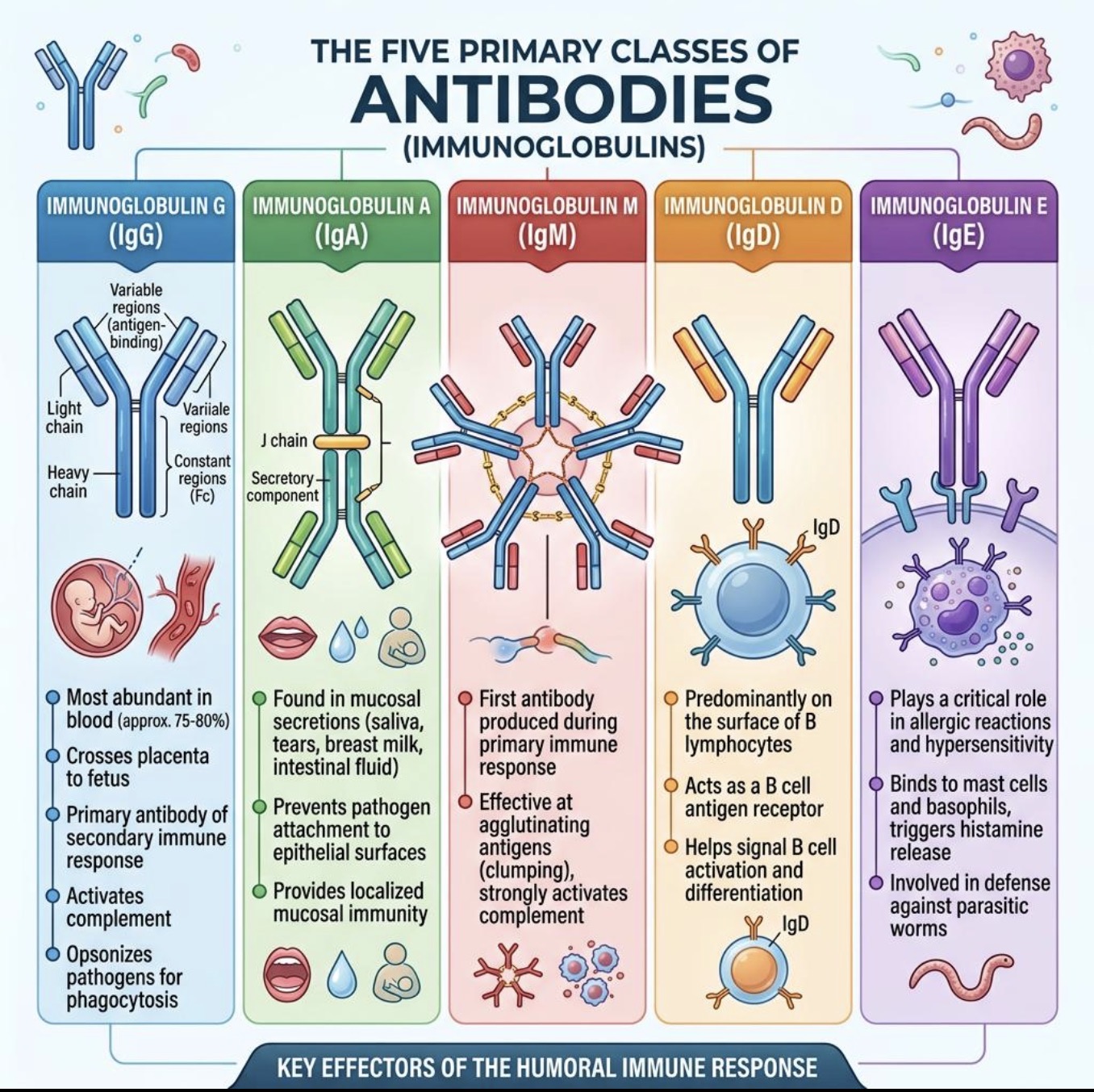
Where is IgD mainly found?
On naïve B-cell surfaces
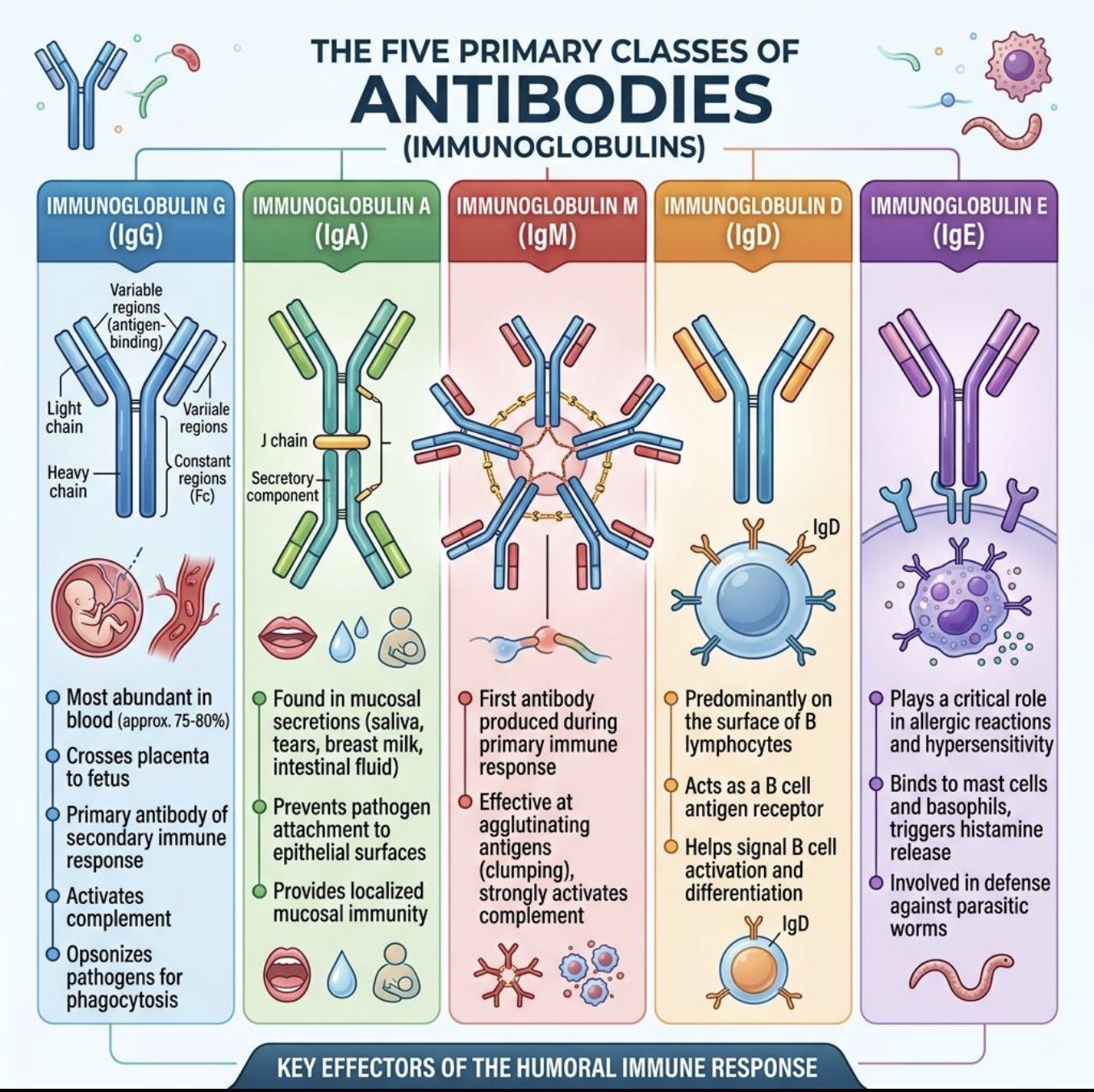
Main function of IgD?
Acts as a B-cell receptor.
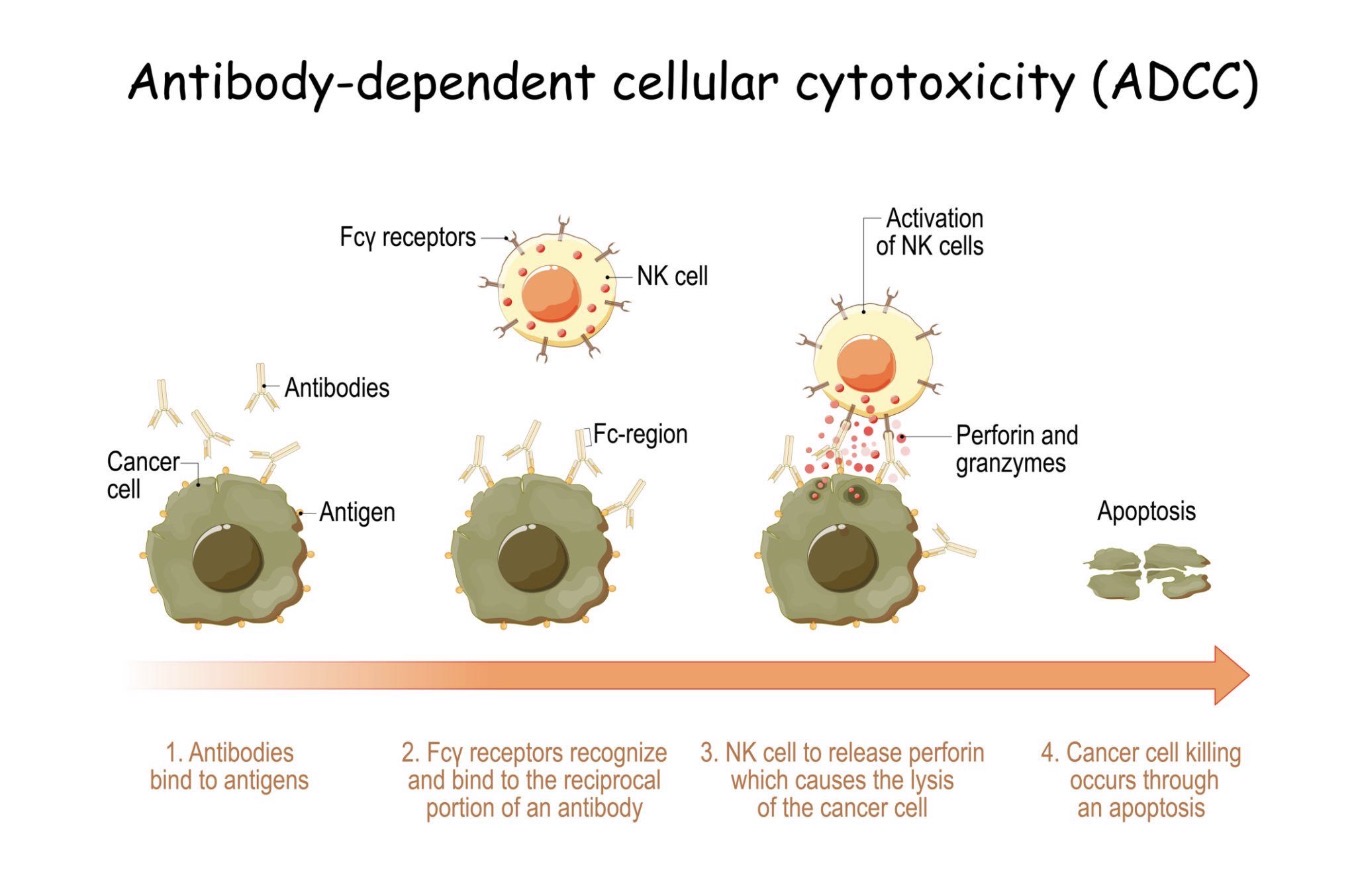
What does ADCC stand for?
Antibody-Dependent Cellular Cytotoxicity
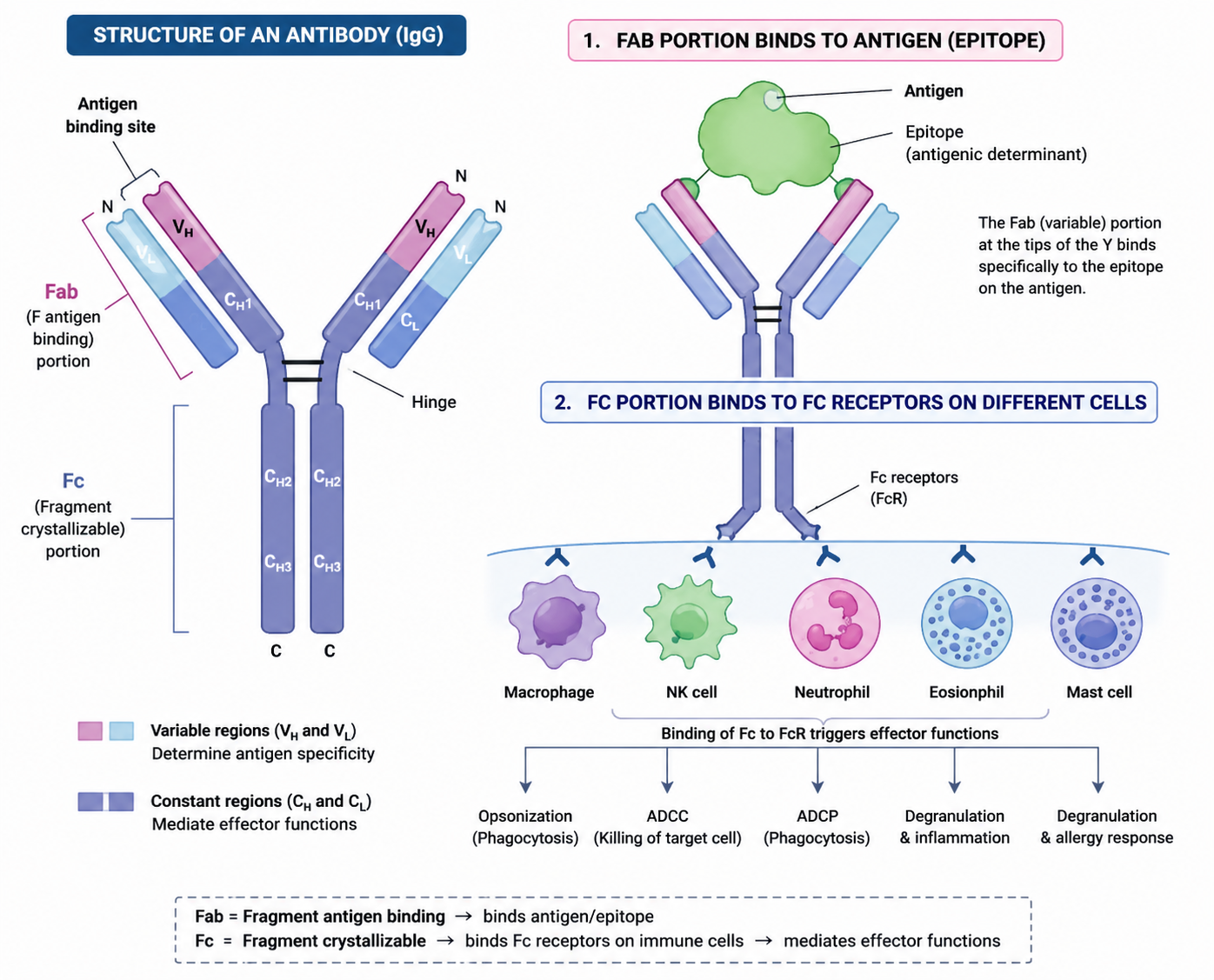
Which antibody region is involved in ADCC?
Fc regions binds Fc receptors on NK cells.
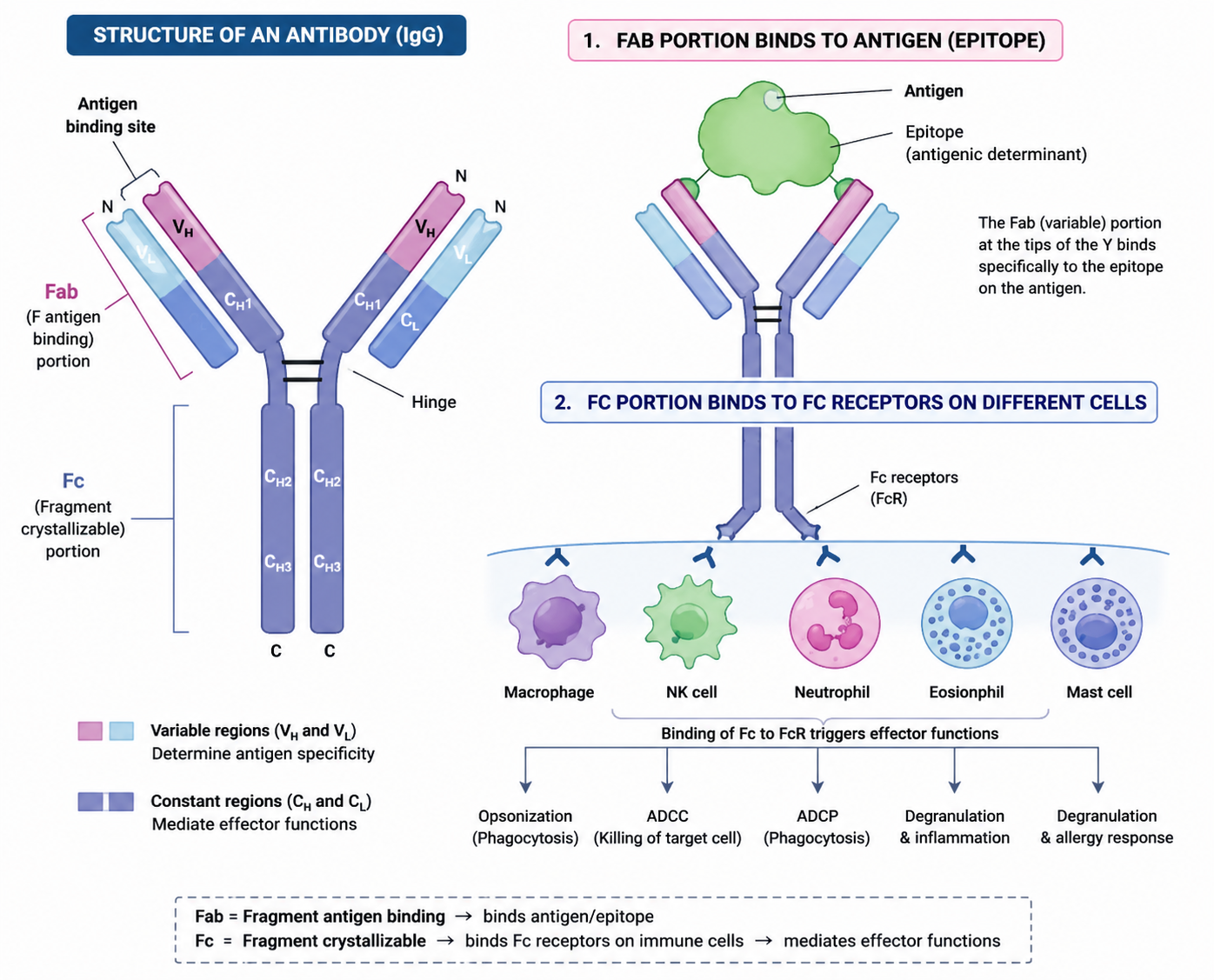
Which antibody region activates phagocytosis?
Fc region.
What is opsonization?
Coating a pathogen with antibody to improve phagocytosis.
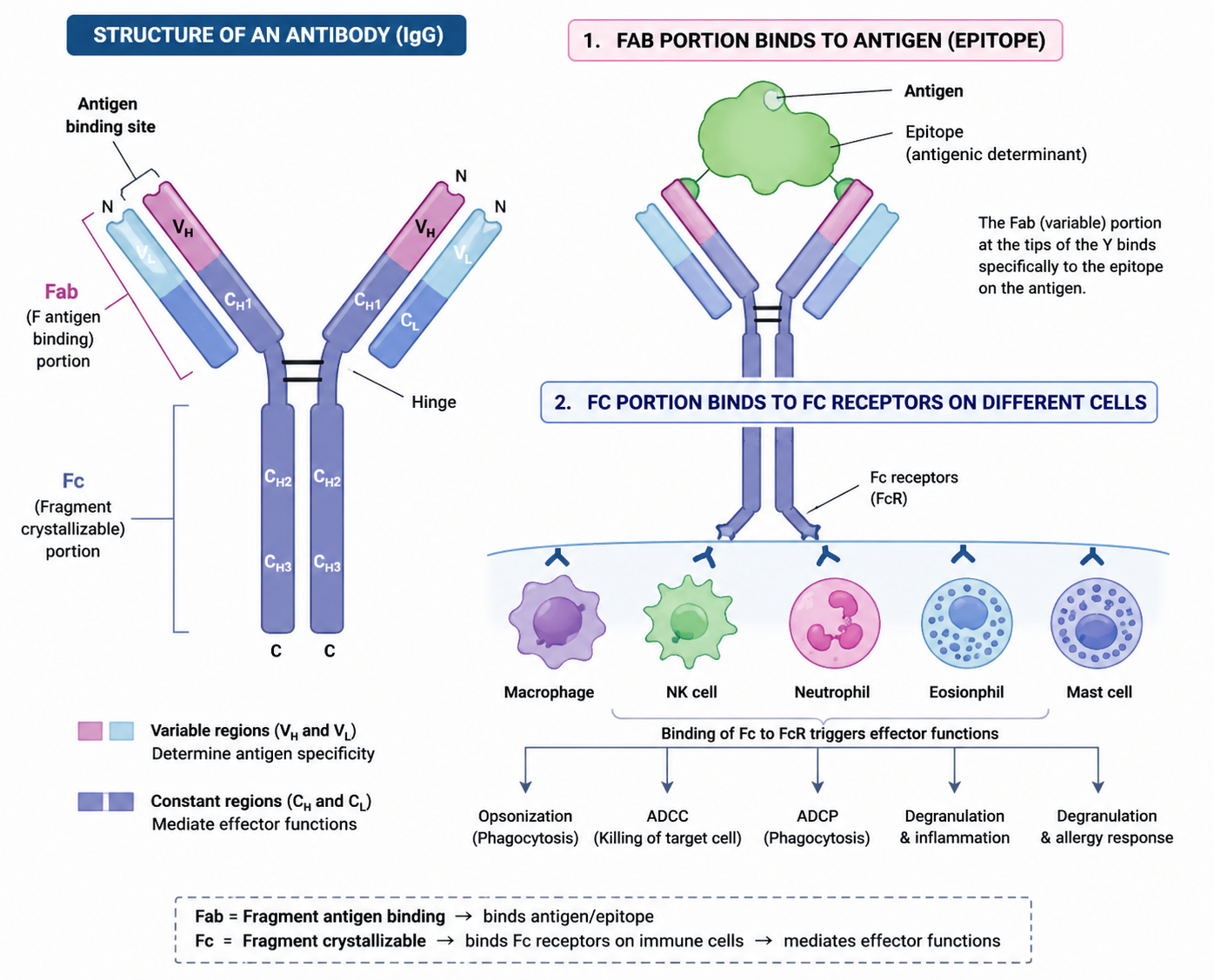
What is the hinge region?
The flexible region connecting Fab and Fc portions.
It allows movement/flexibility of the antibody arms.
⚙Mech of ADCC
Fab region of Ab binds Antigen on infected/tumor cell.
Fc portion of Ab binds to Fcγ receptor on the NK cell.
NK cell is activated and releases perforins and granzymes, inducing apoptosis of the cancer cell.
Obj. 2
Agglutination, precipitation, affinity, avidity, specificity, cross-reactivity.
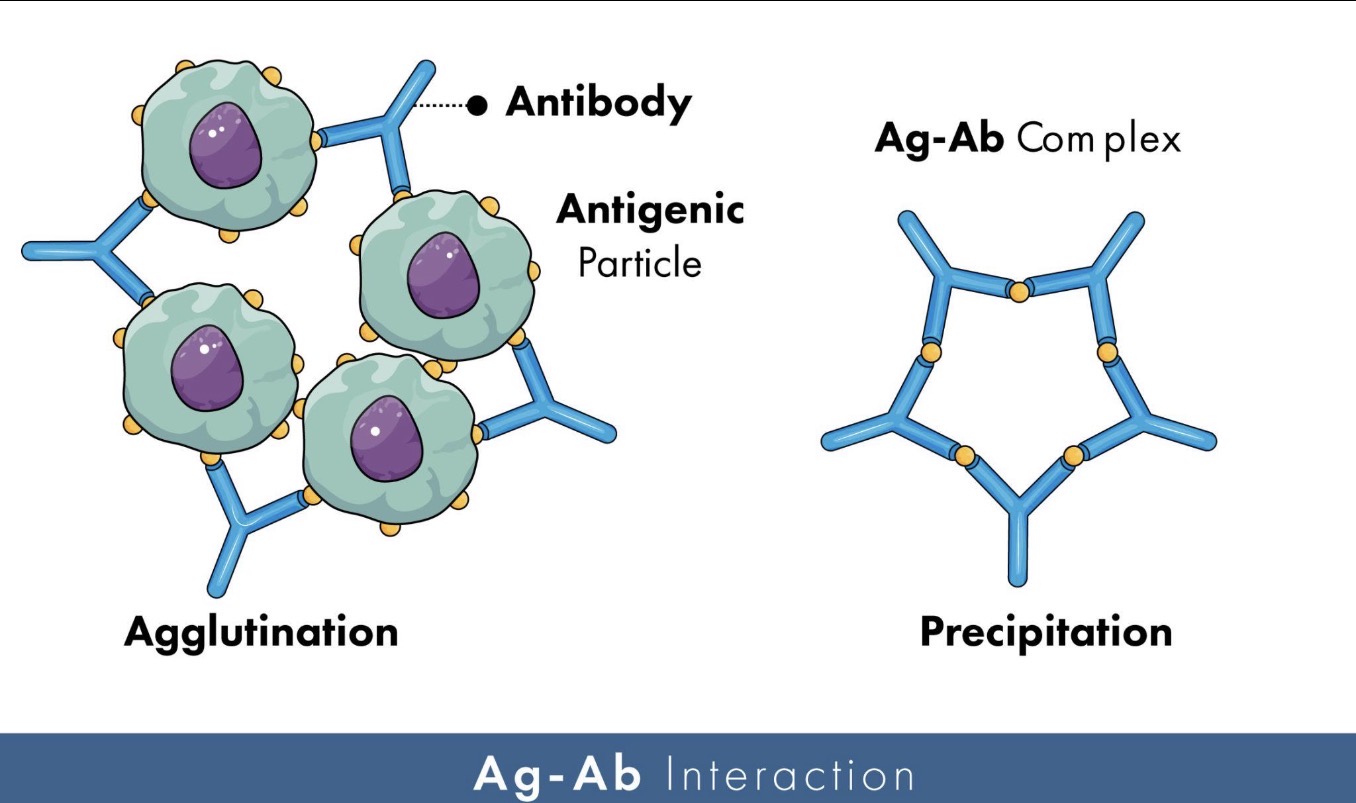
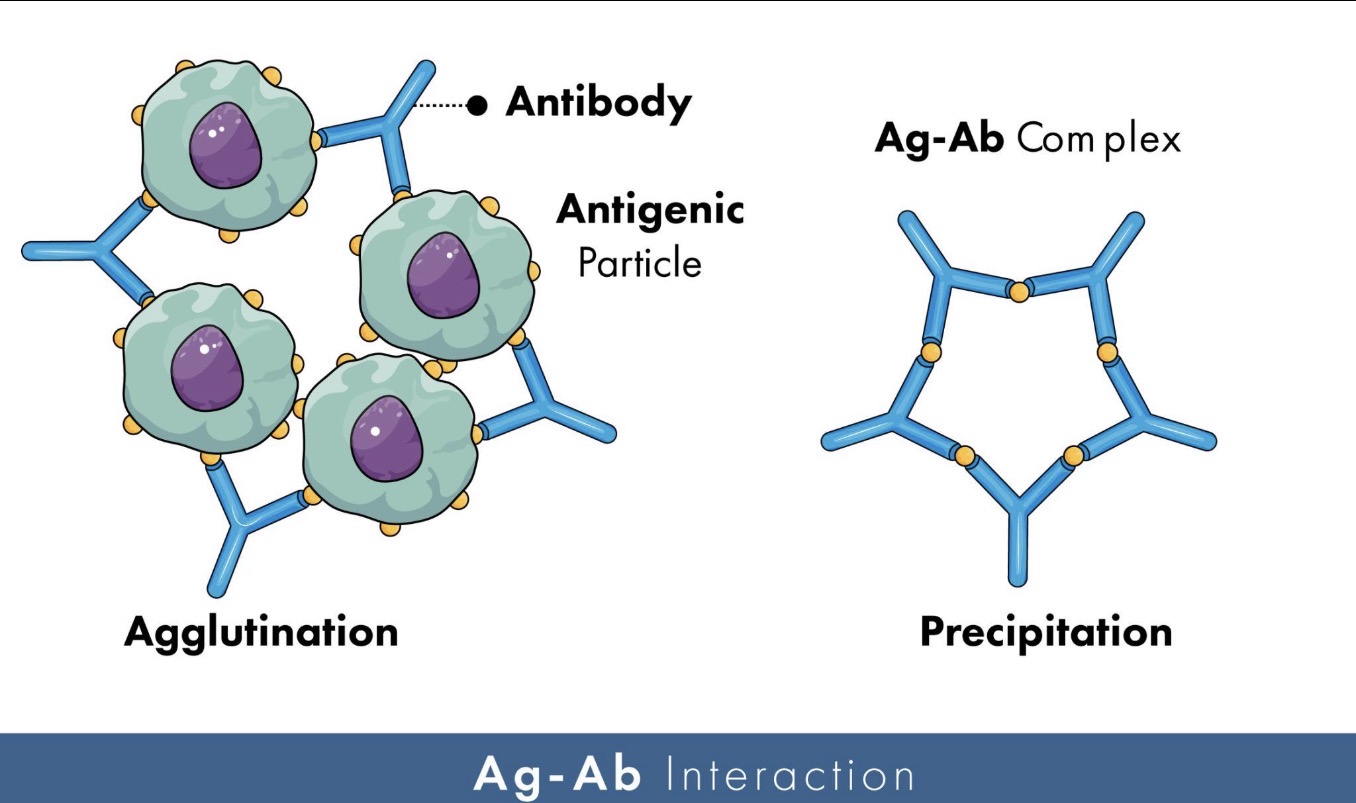
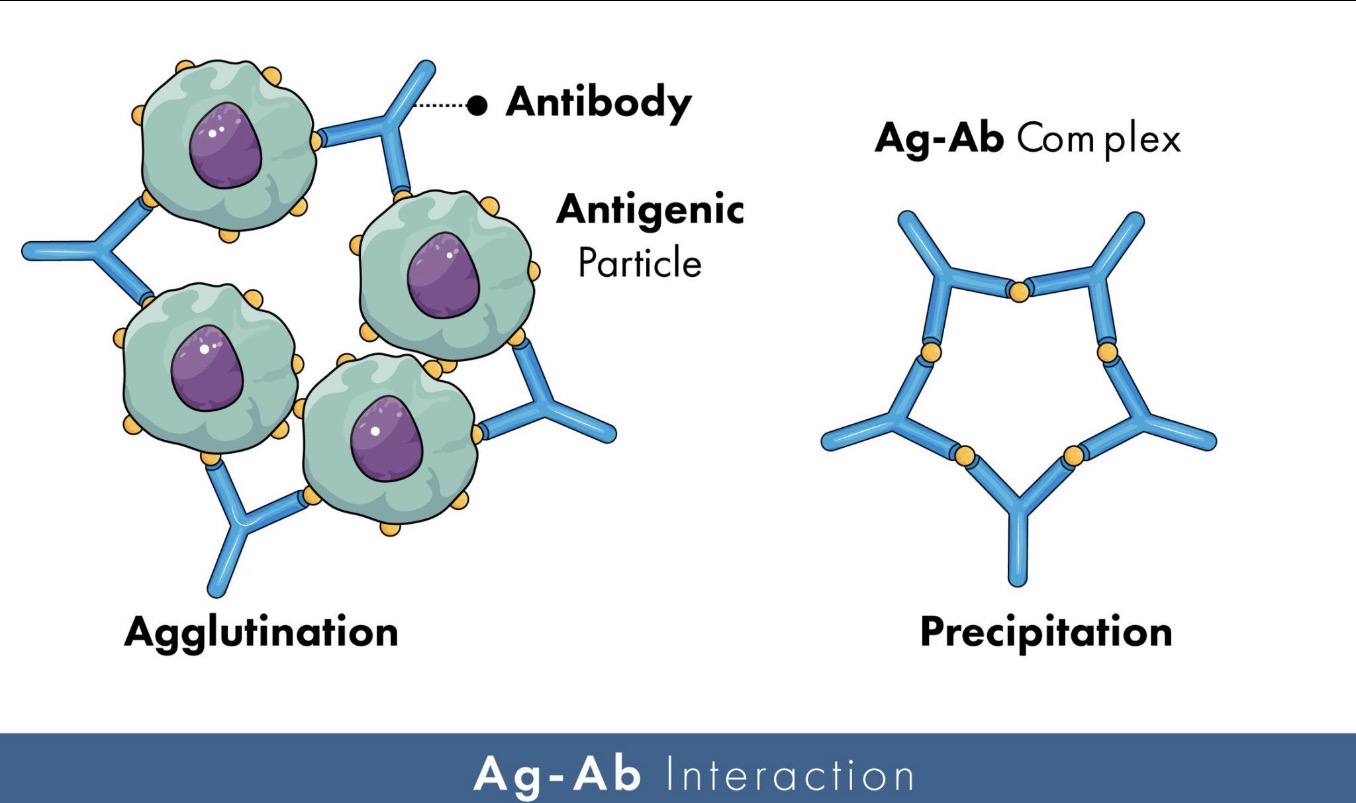
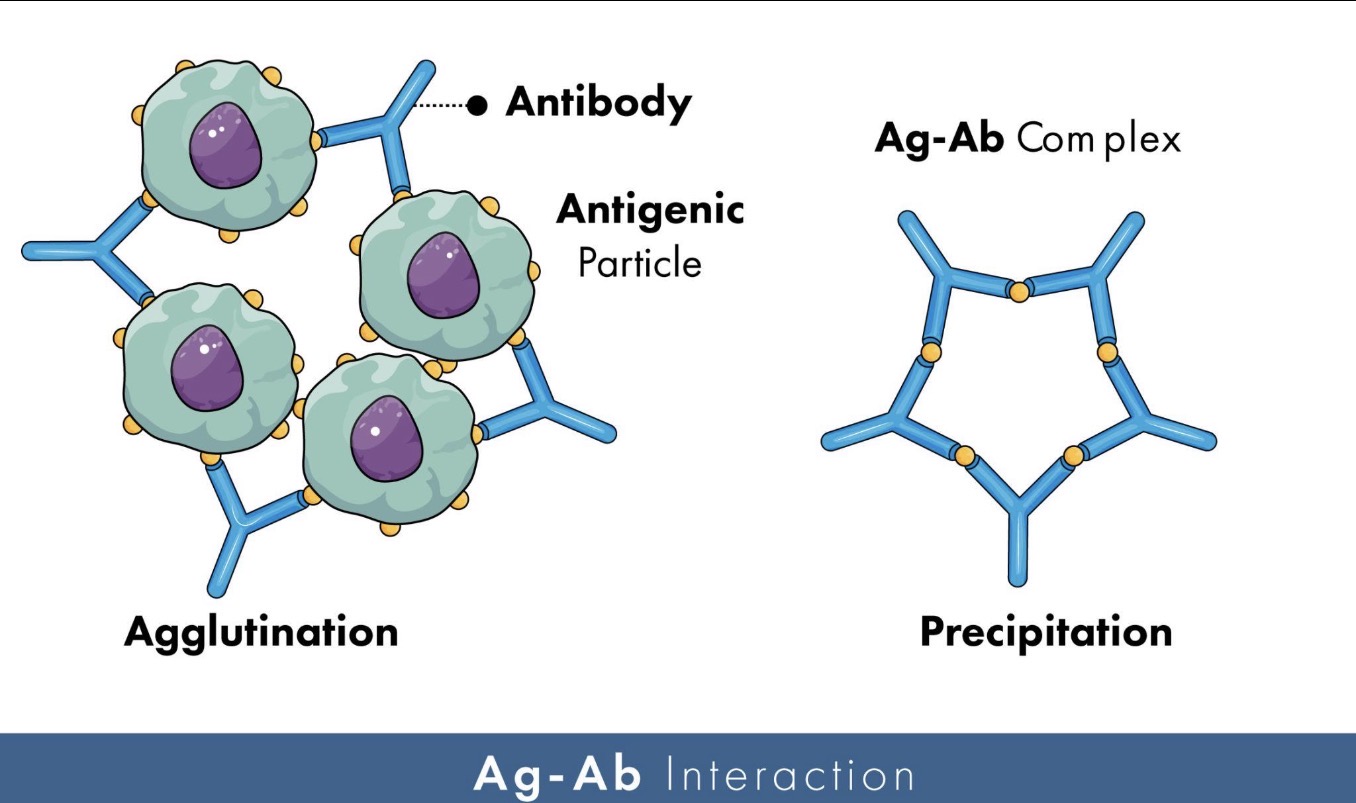
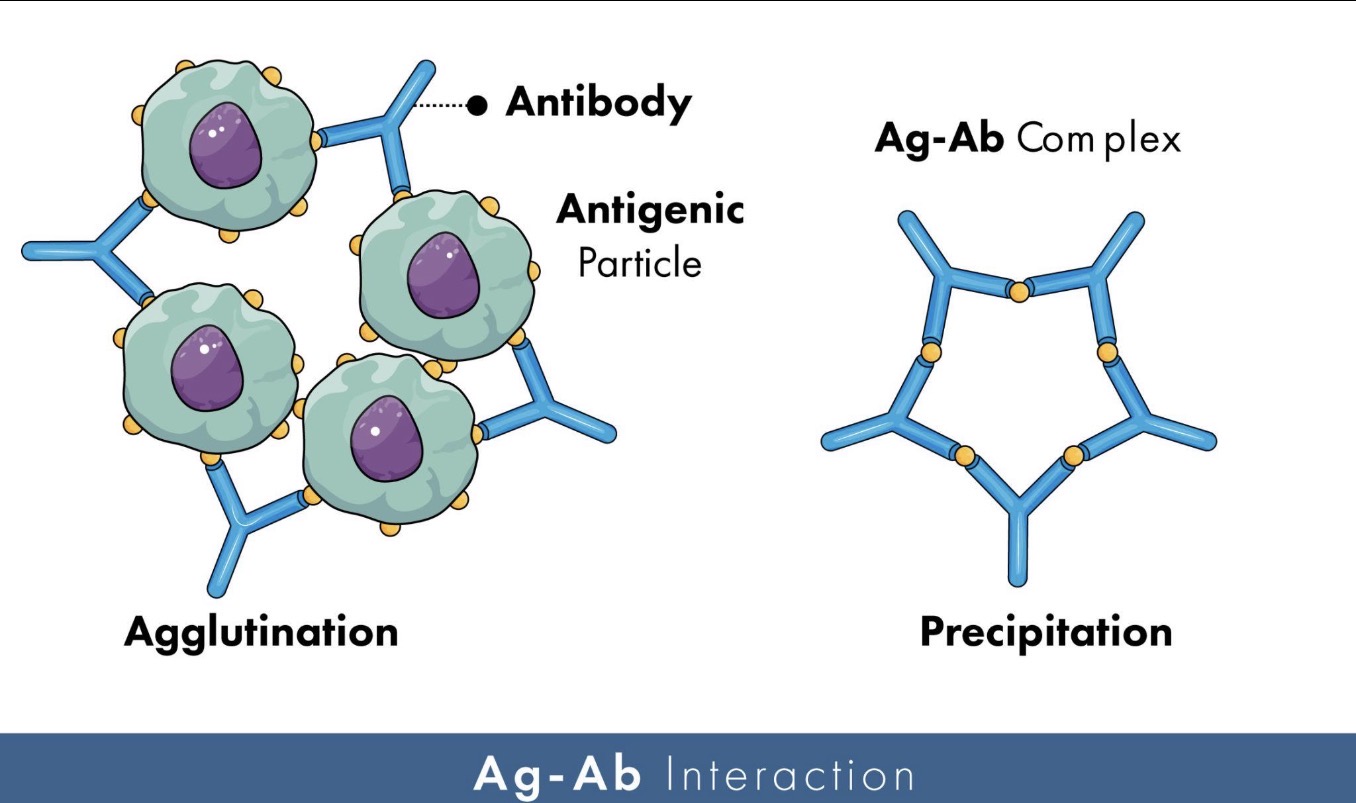
🔹What is agglutination?
Agglutination is the clumping of particles or cells caused by antibodies binding multiple antigens together.
What kinds of things undergo agglutination?
Bacteria
RBCs
Particles
Cells
What kinds of things undergo agglutination?
Bacteria
RBCs
Particles
Cells
Why is IgM very good at agglutination?
Because IgM has very high valency and can bind many antigens simultaneously.
What is the purpose of agglutination?
Immobilizes pathogens
Enhances phagocytosis/removal
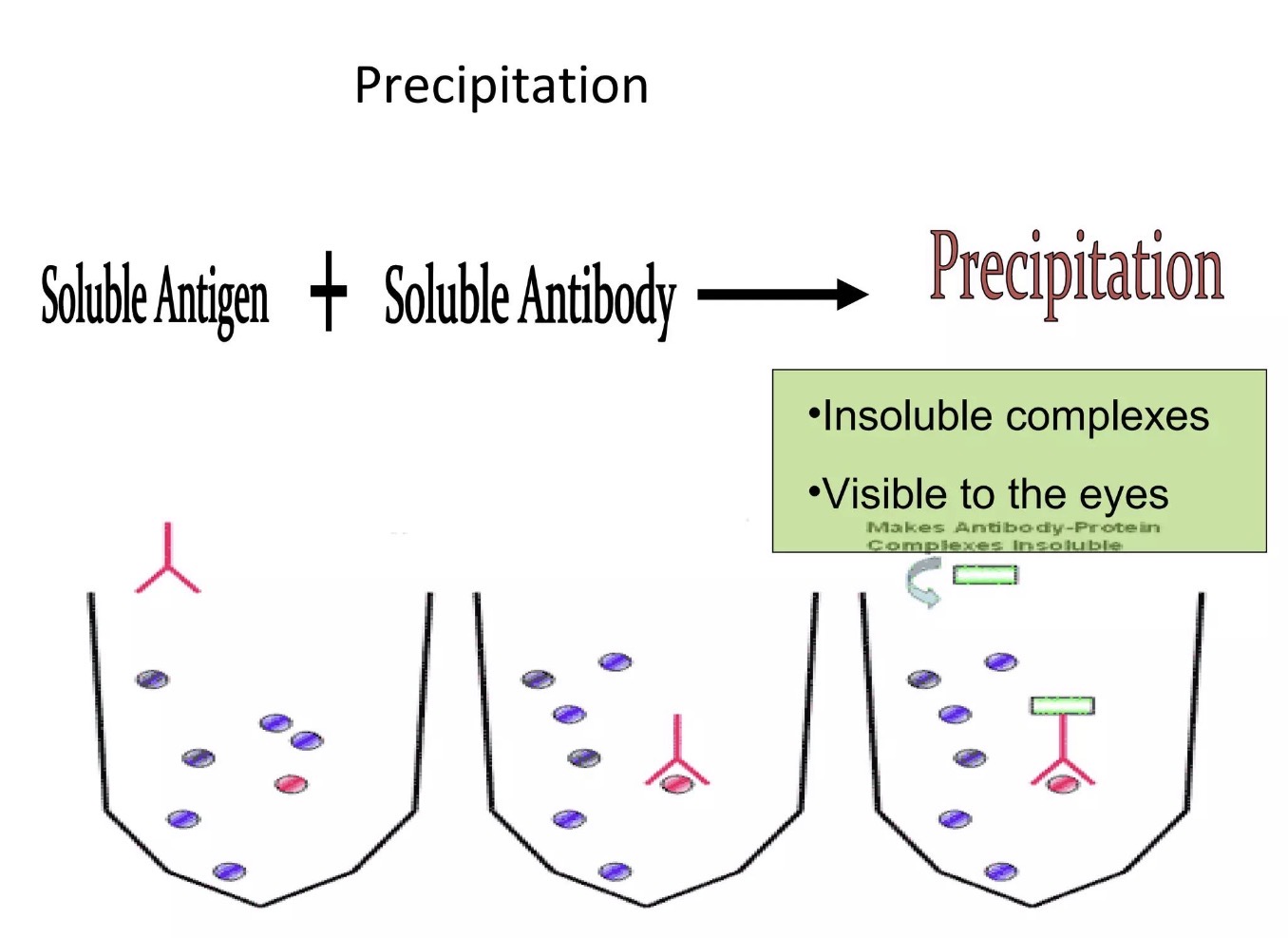
What is precipitation in immunology?
Precipitation occurs when antibodies bind soluble antigens and form insoluble immune complexes that precipitate out.
What is the difference between agglutination and precipitation?
Agglutination | Precipitation |
Insoluble particles/cells | Soluble antigens |
Visible clumping | Insoluble precipitate formation |
What forms during precipitation?
Large antigen-antibody lattice network
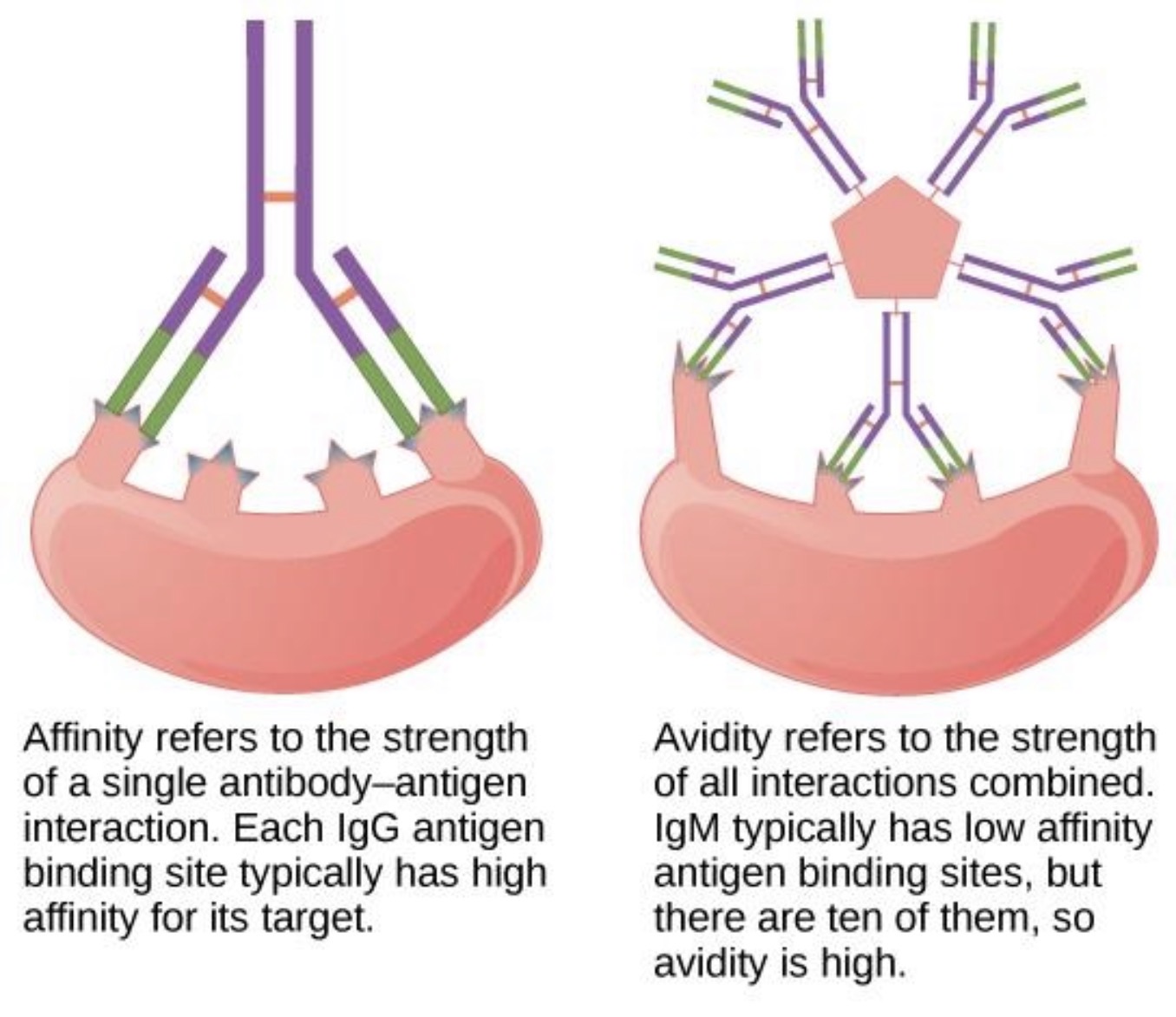
What is affinity?
Affinity is the strength of binding between ONE epitope and ONE antibody binding site (paratope).
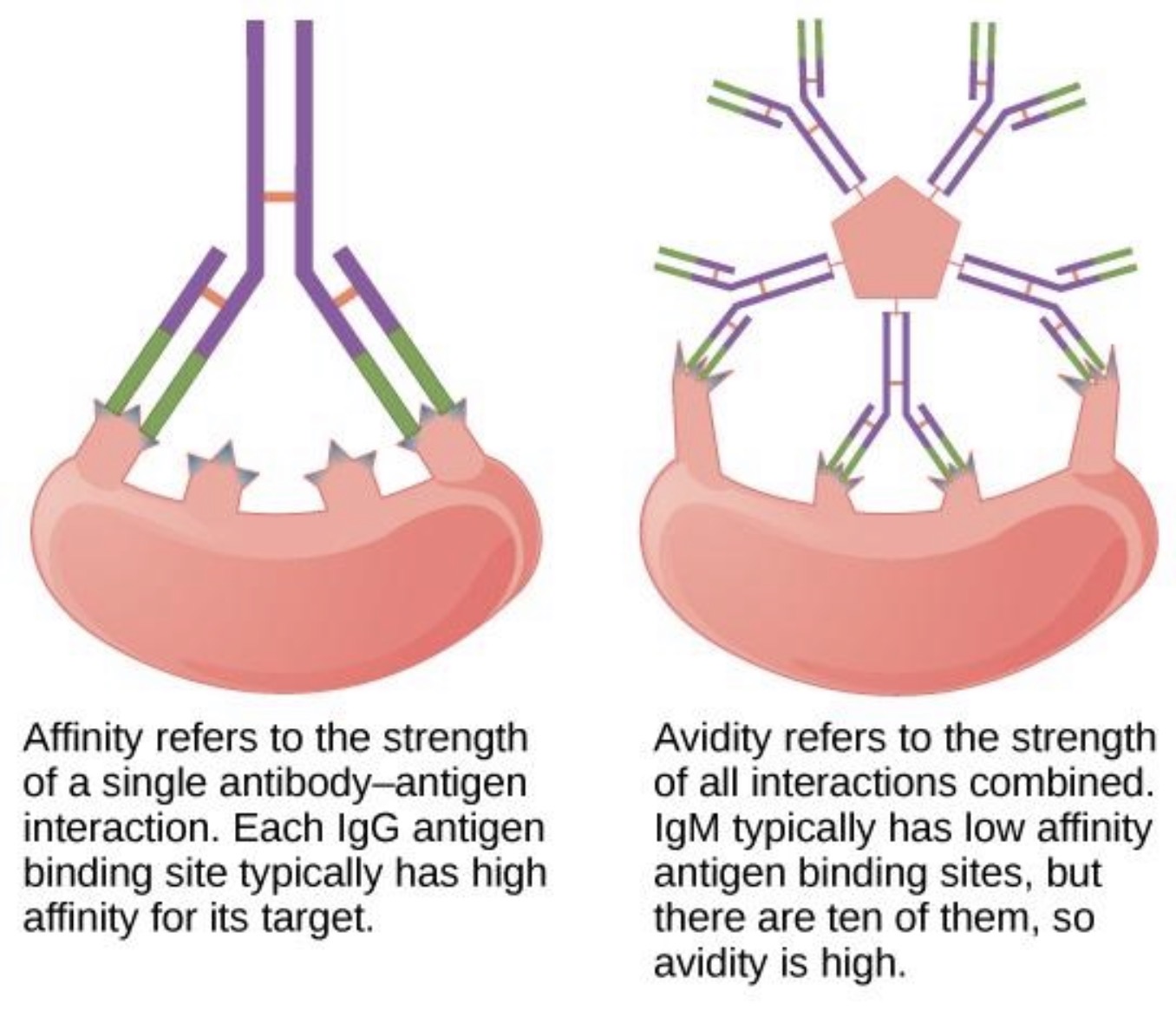
Affinity measures binding between what?
ONE epitope + ONE paratope.
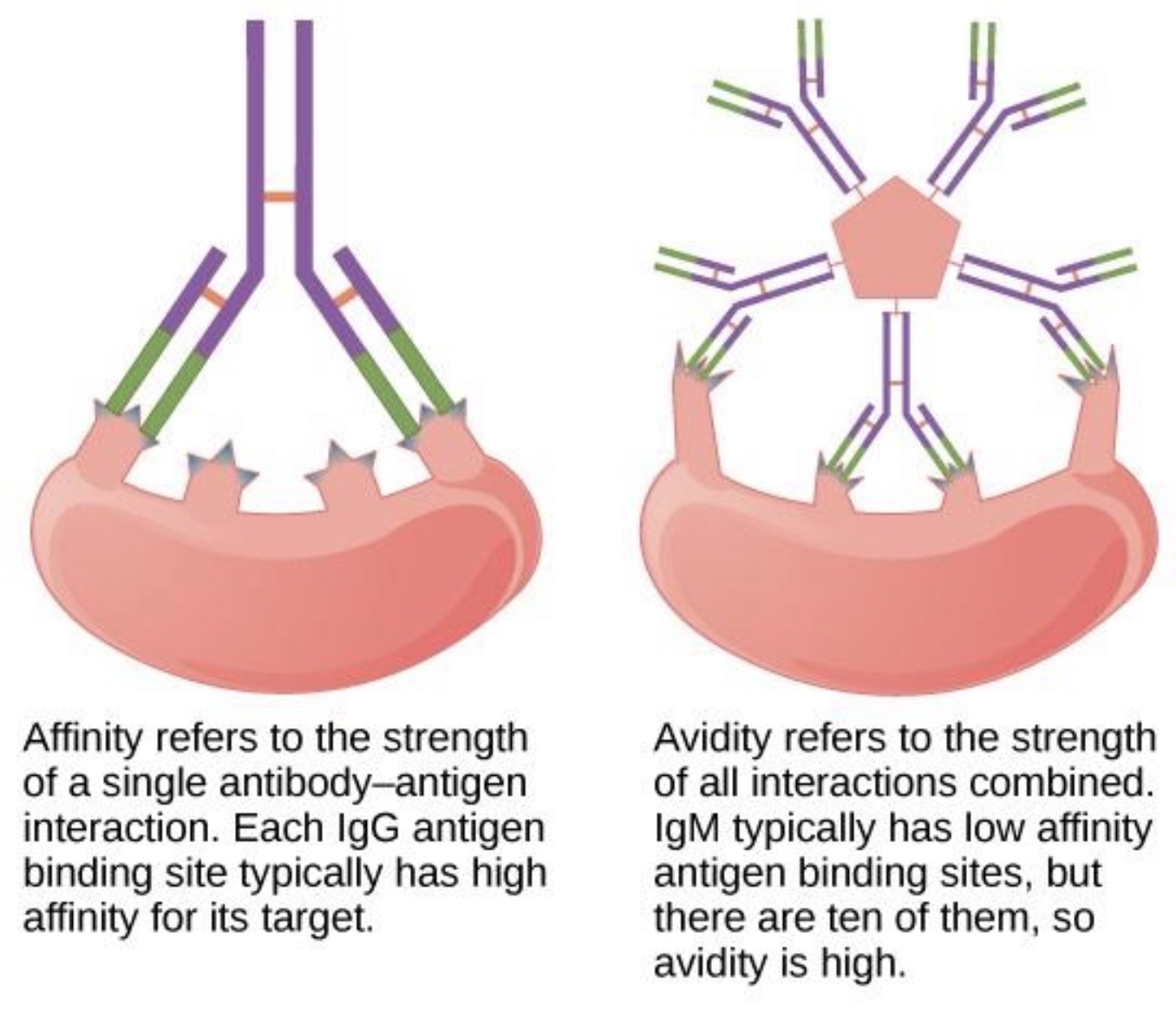
High affinity means what?
Very strong antigen-antibody binding.
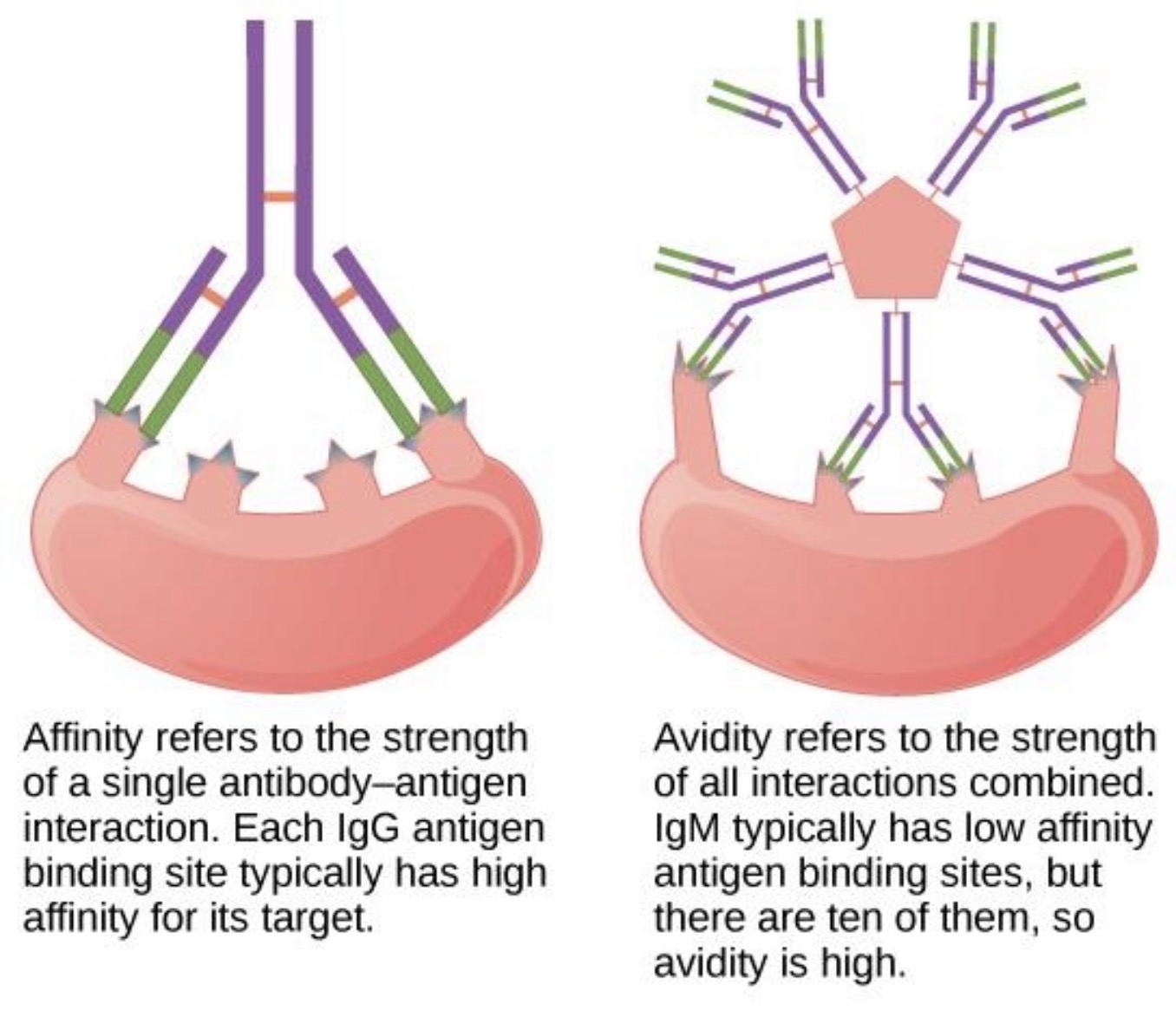
Which region determines affinity?
The variable region/Fab region
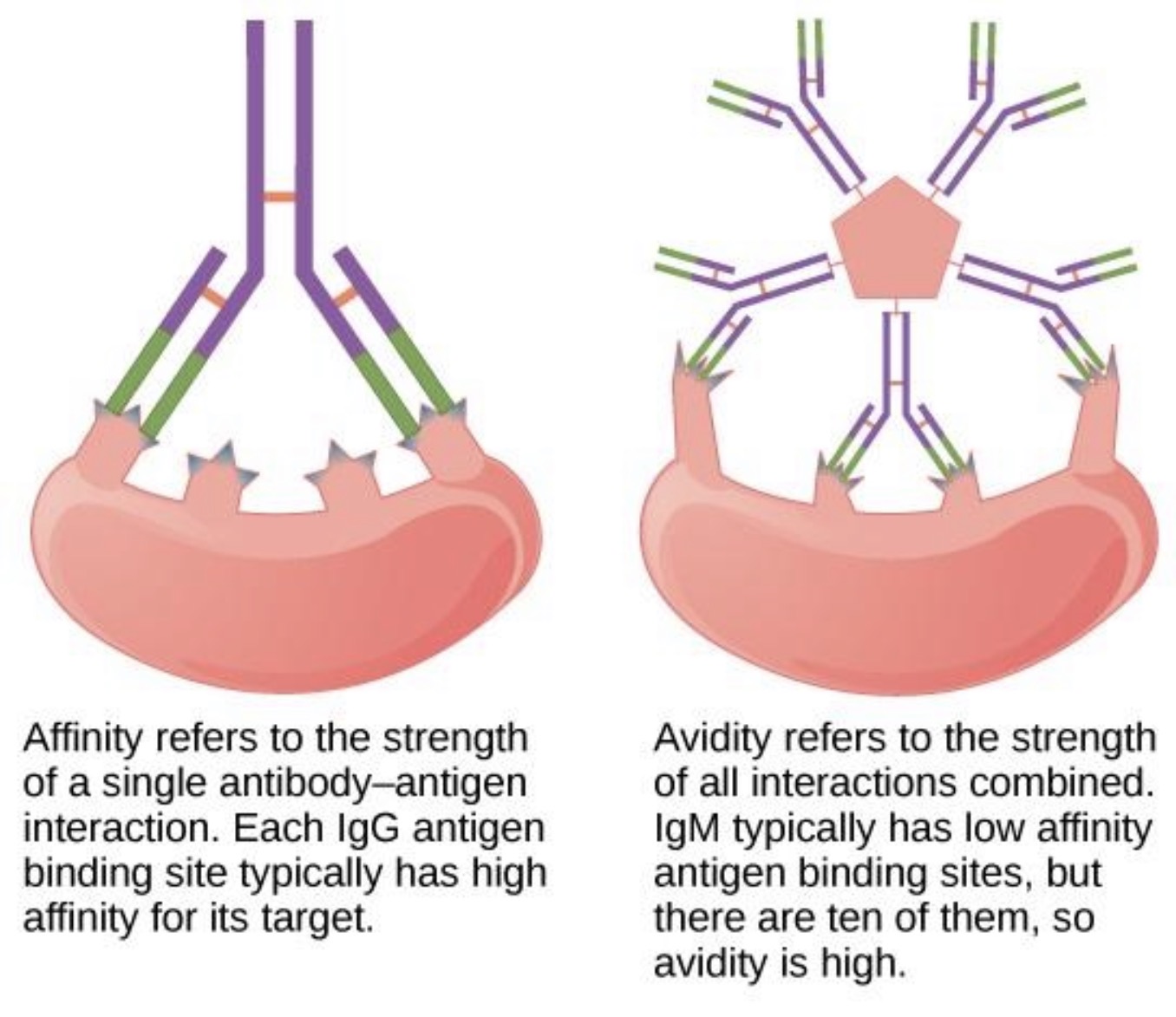
What is avidity?
Avidity is the overall binding strength of ALL interactions between antibody and antigen.
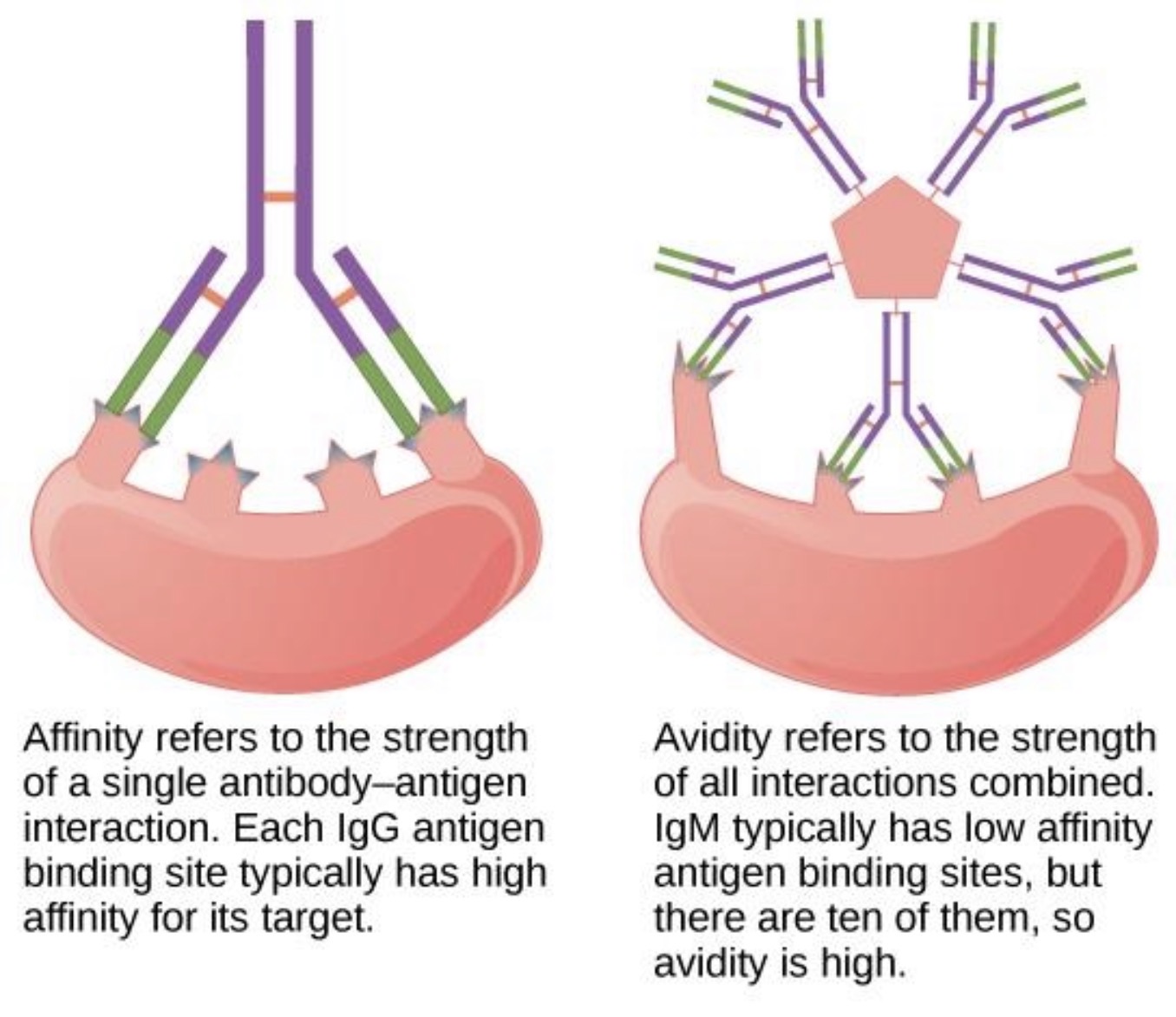
Difference between affinity and avidity?
Affinity | Avidity |
ONE binding interaction | TOTAL combined binding strength |
ONE epitope + ONE paratope | ALL bindings together |
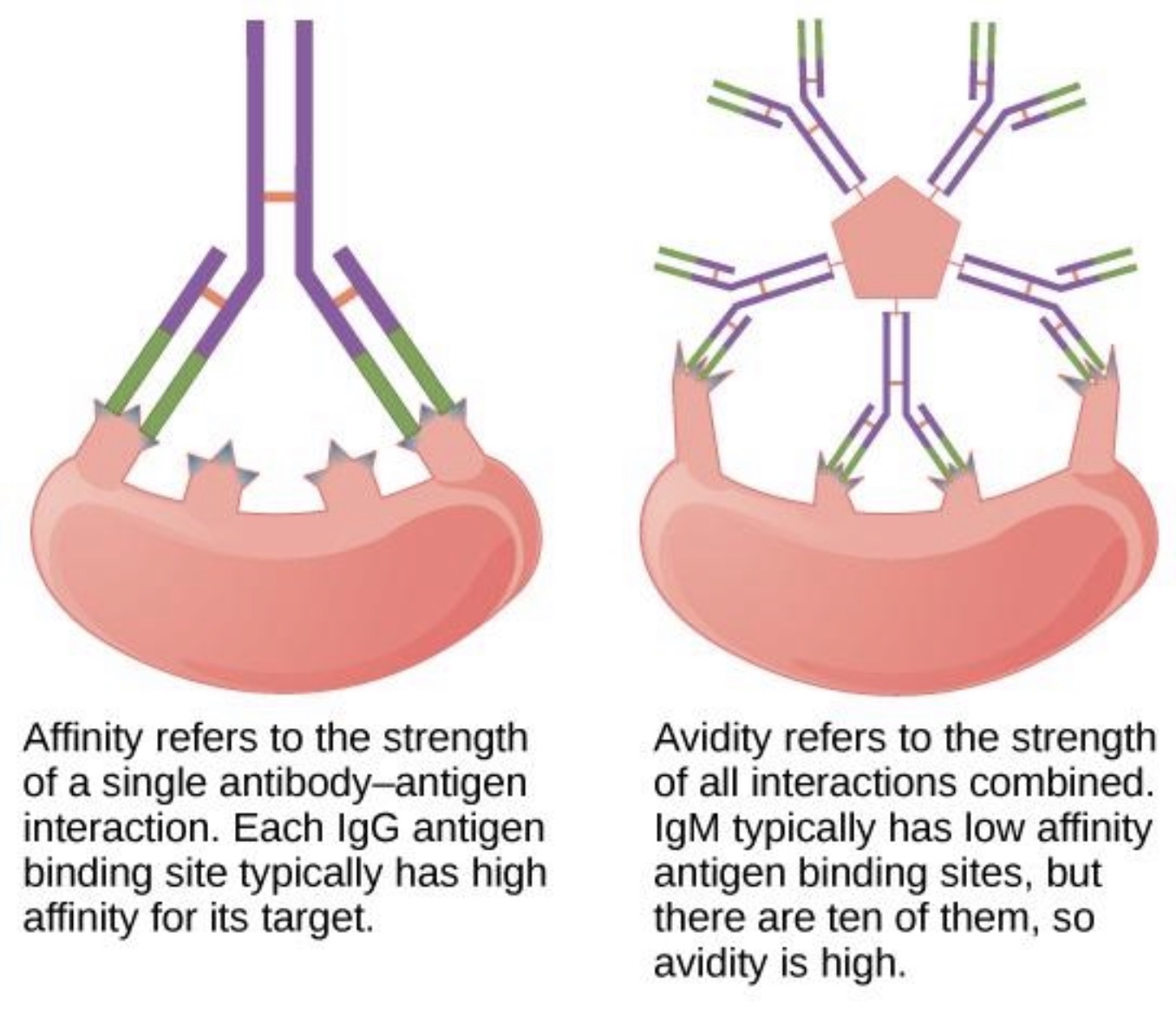
Which antibody has especially high AVIDITY?
IgM
👉Reason:
Pentamer structure
Many binding sites
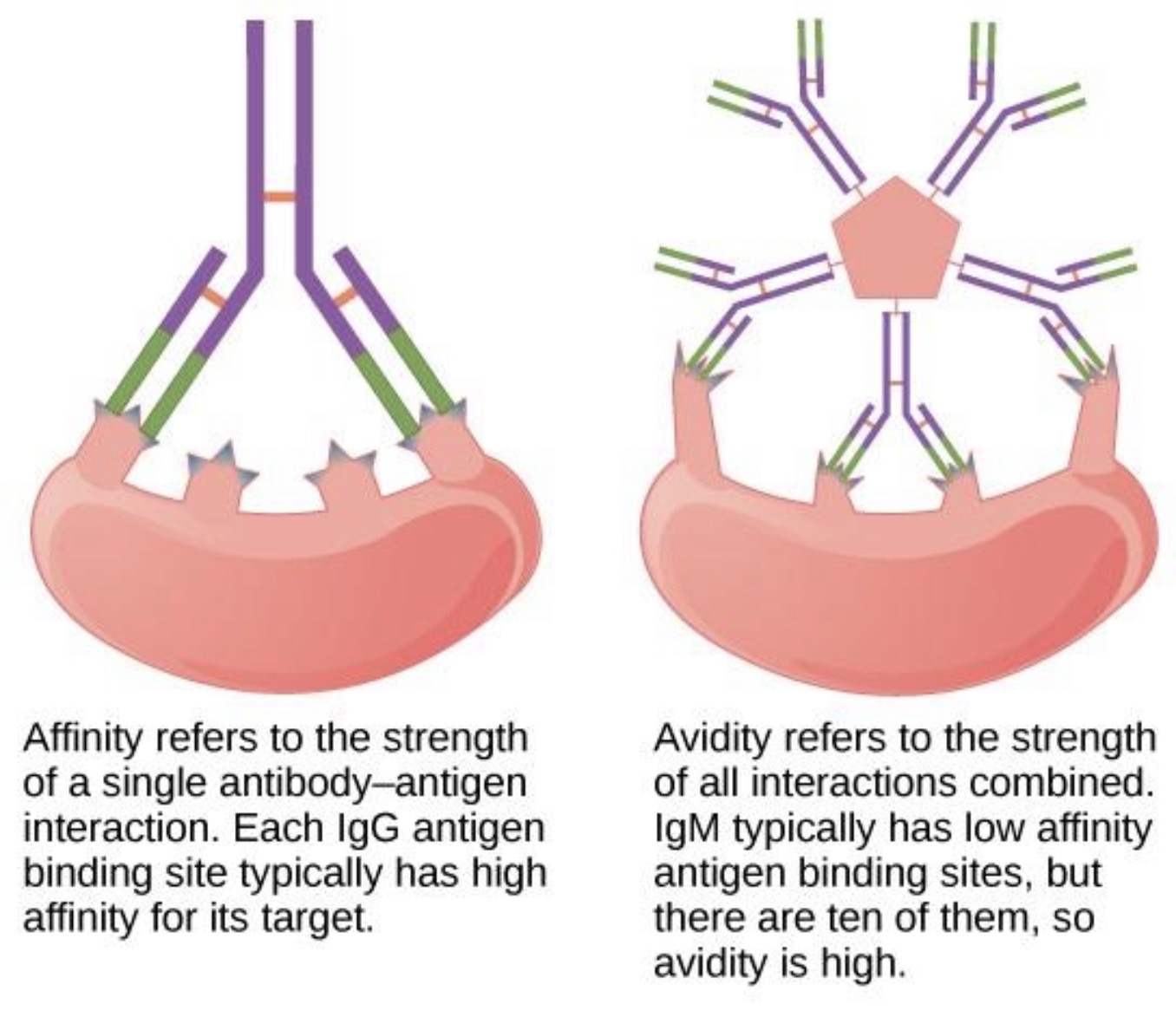
Can low-affinity interactions still produce high avidity?
Yes — if many binding interactions occur simultaneously.
Ex: IgM
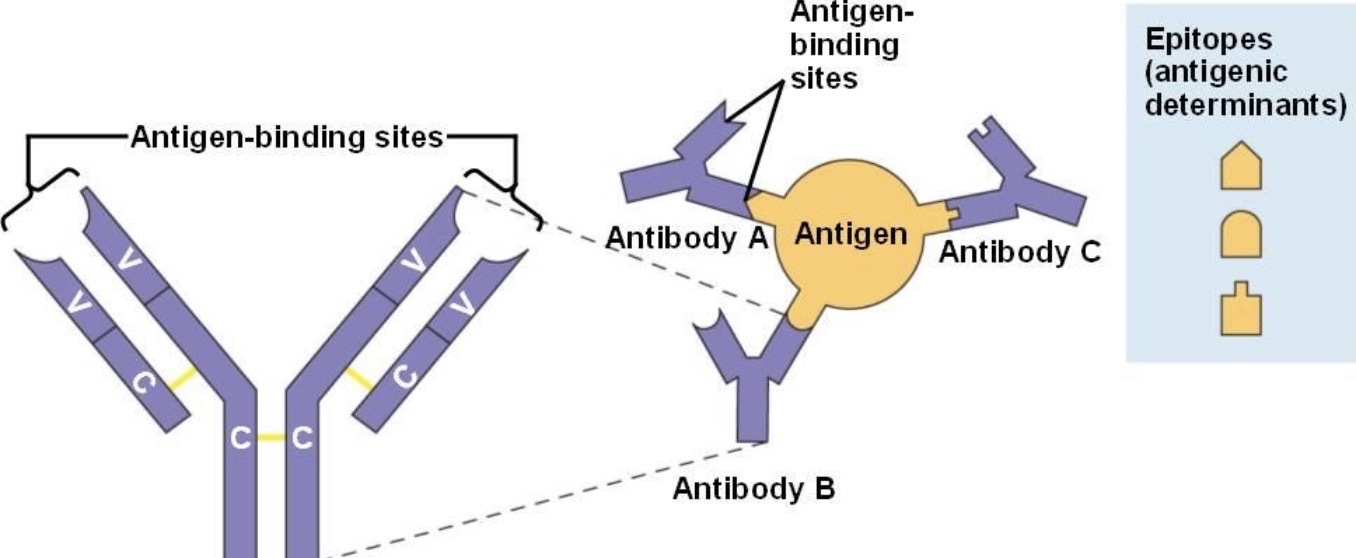
What is specificity?
Specificity is the ability of an antibody to bind a PARTICULAR epitope/antigen.
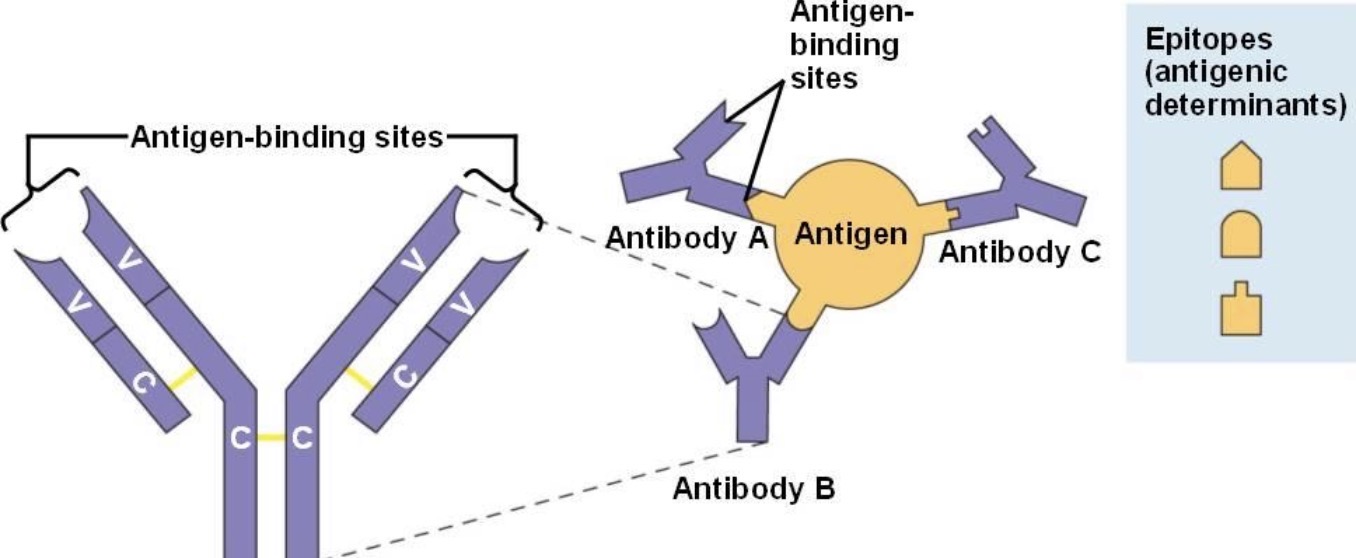
What determines specificity?
The variable region (Fab region).
Why are monoclonal antibodies highly specific?
Because they bind a single epitope.
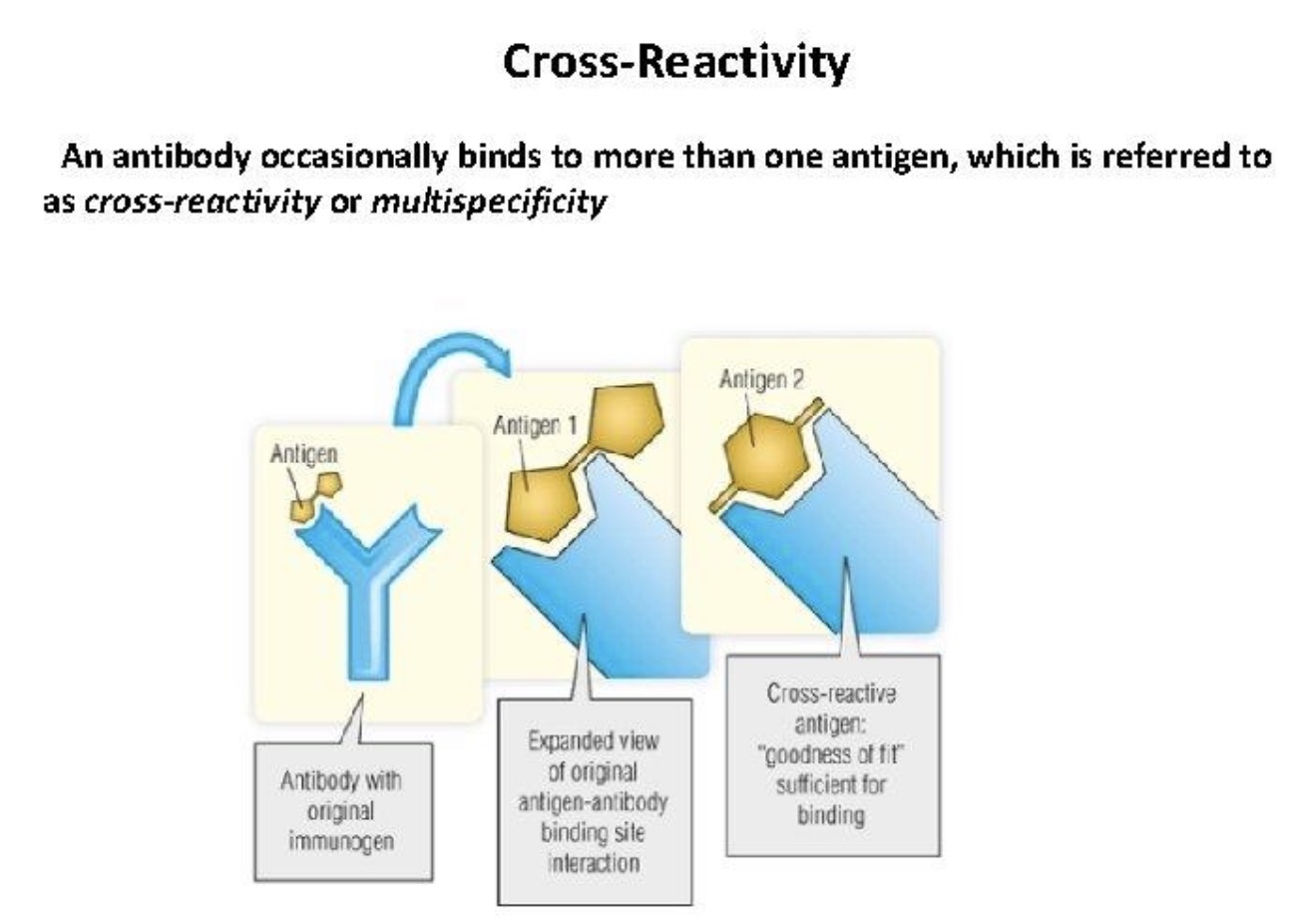
What is cross-reactivity?
Occurs when an Ab binds a different antigen that has a similar epitope.
Why does cross-reactivity happen?
Because different antigens may share structurally similar epitopes.
Is cross-reactivity always beneficial?
No.
👉It can provide Protection.
OR
👉Contribute to Autoimmune reactions/allergy.
What is molecular mimicry?
When pathogen epitopes resemble host epitopes, causing cross-reactive immune responses.
⭐️Sometimes a pathogen has an epitope that looks very similar to one of your own body’s proteins.
The immune system:
Makes antibodies/T cells against the pathogen
Those antibodies accidentally recognize your own tissues too
This causes a cross-reactive immune response
Can lead to autoimmune damage
This is called molecular mimicry.
Obj. 3
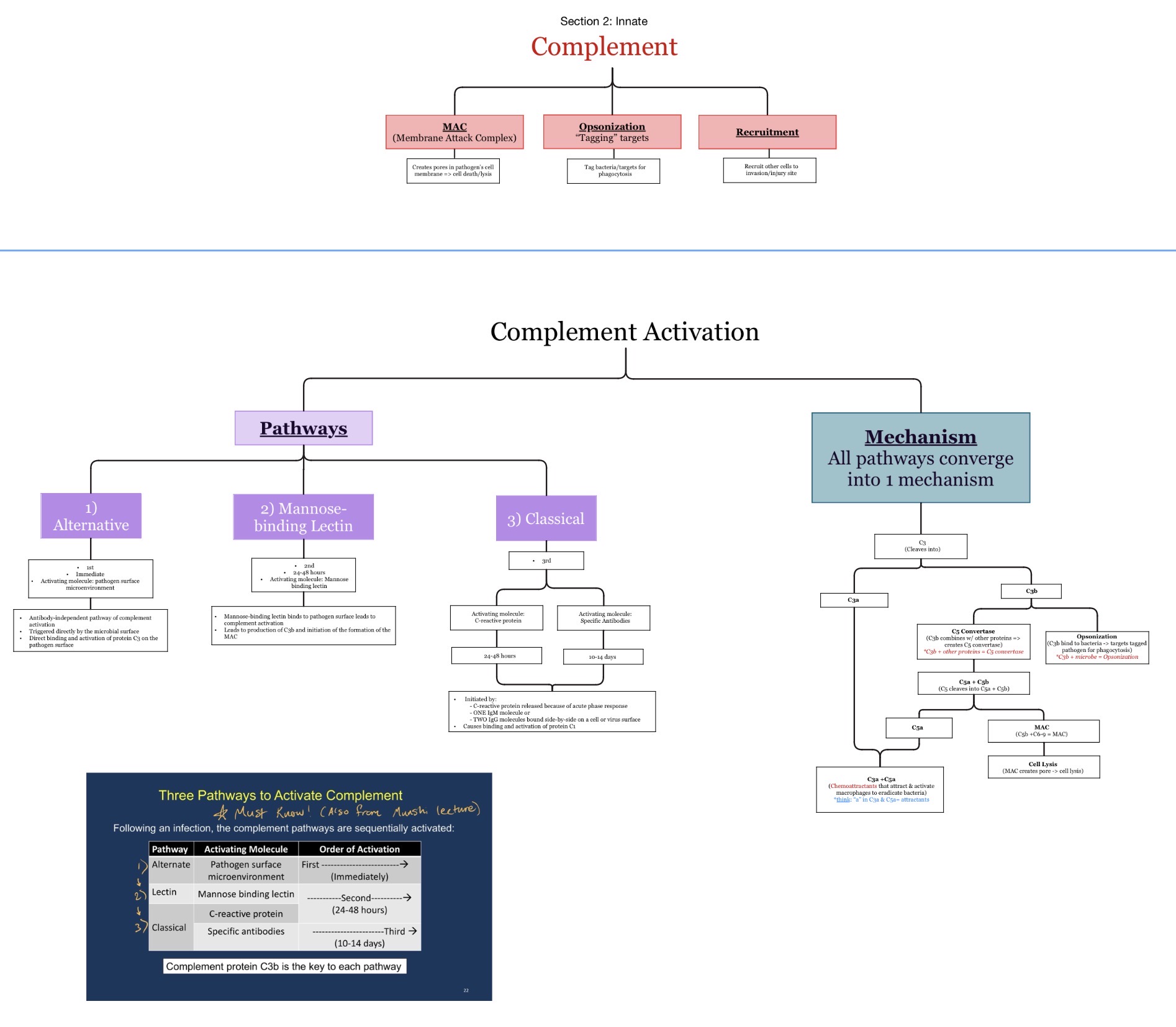
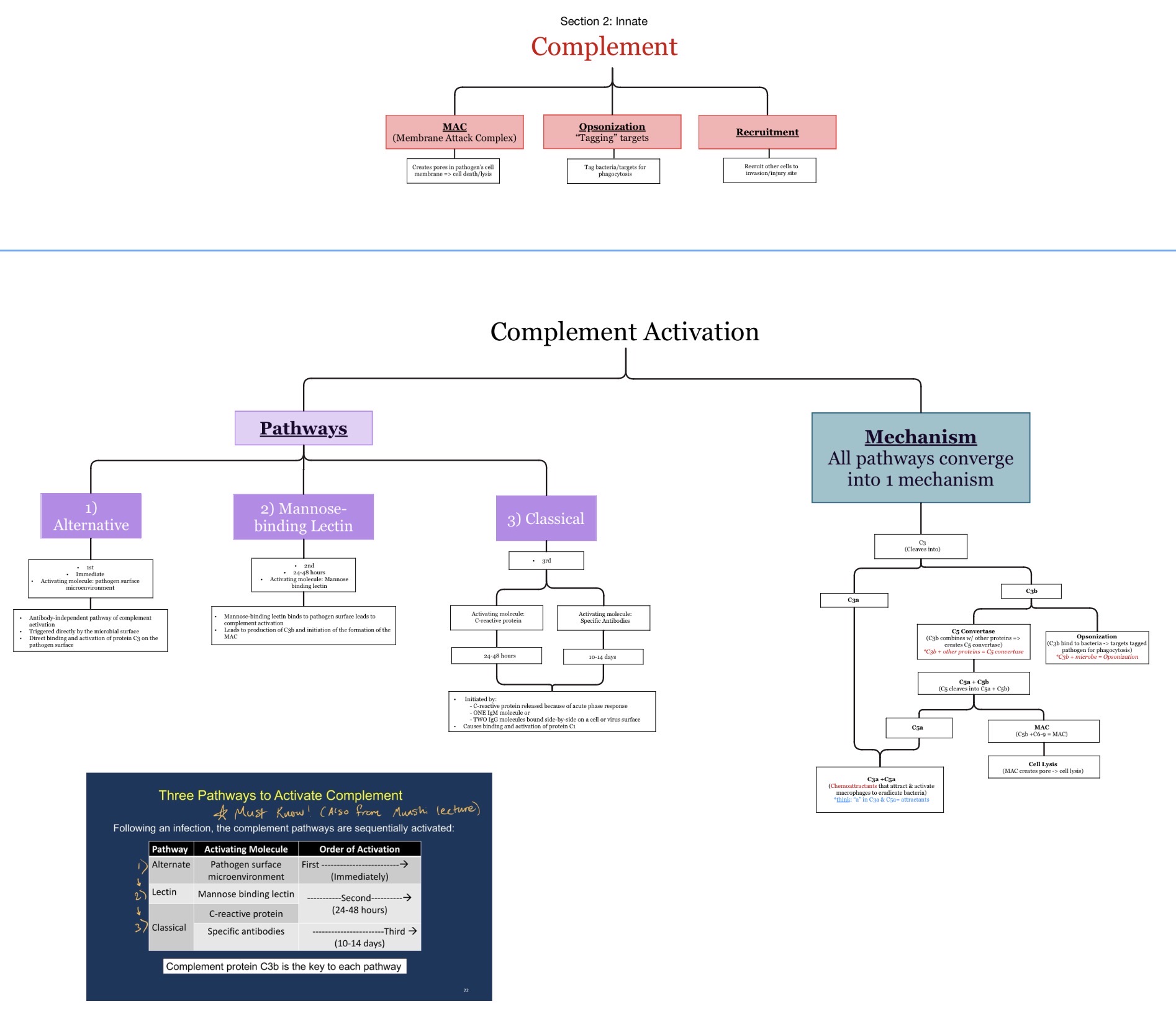
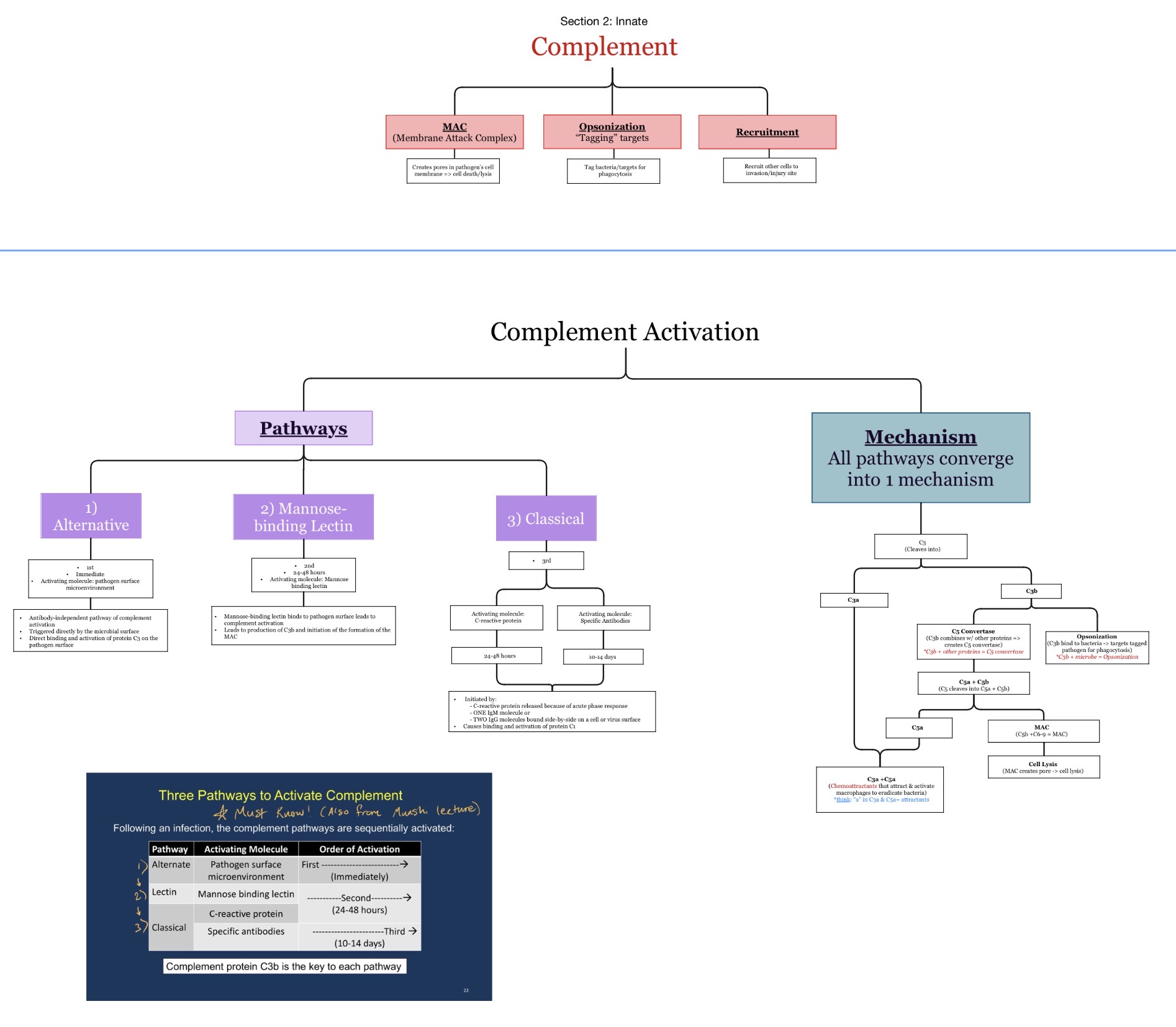
What is complement? What are three pathways, timeline of their stimulation, and functions of the complement components (opsonization, phagocytosis, inflammation). Anaphylactic shock reaction by which of the released complement factors?
🔹What is Complement?
Complement is a group of plasma proteins that work together to:
destroy pathogens
enhance inflammation
promote phagocytosis
assist antibodies and innate immunity
Is complement part of innate or adaptive immunity?
Mainly innate immunity, but it also interacts with antibodies/adaptive immunity.
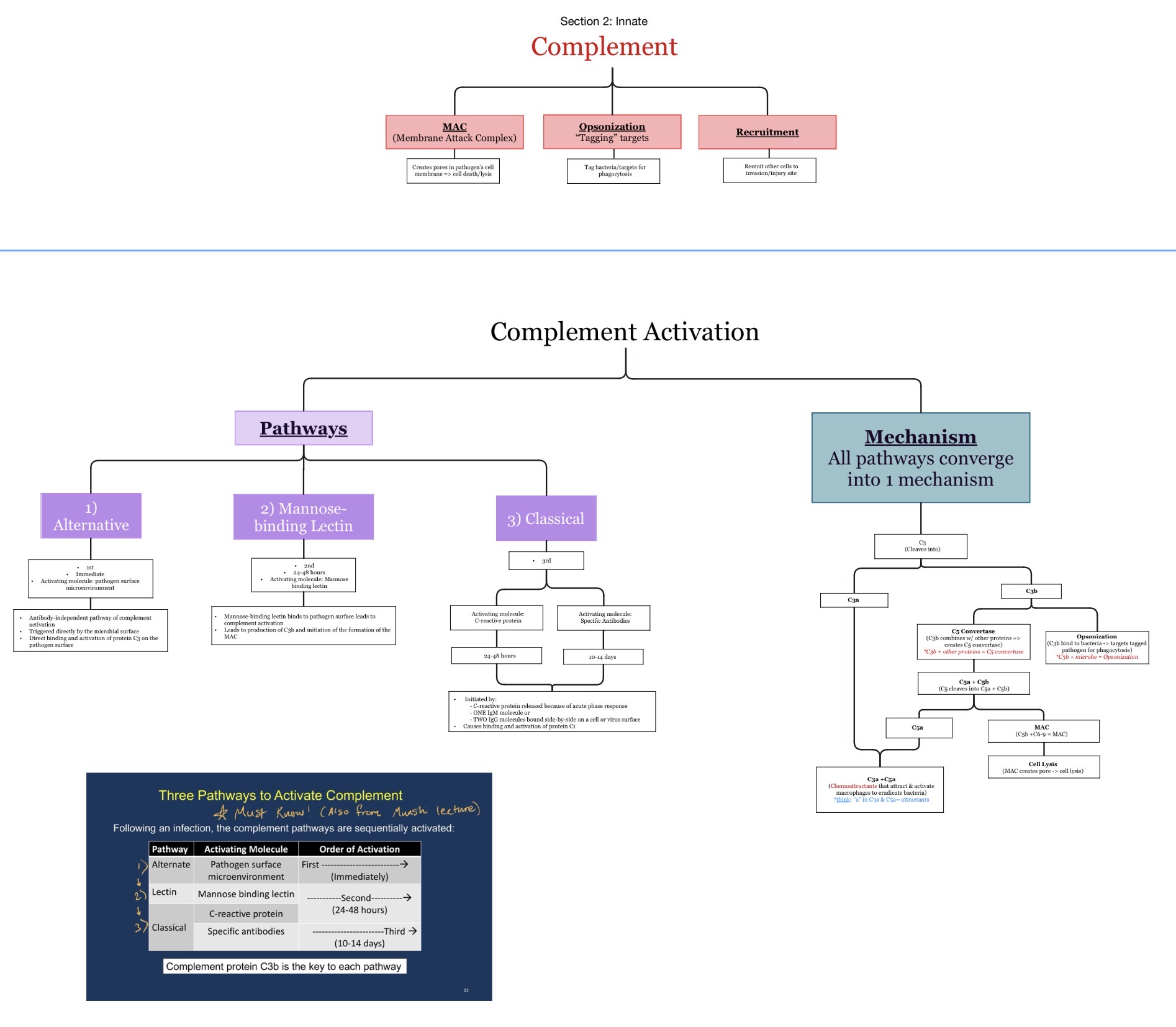
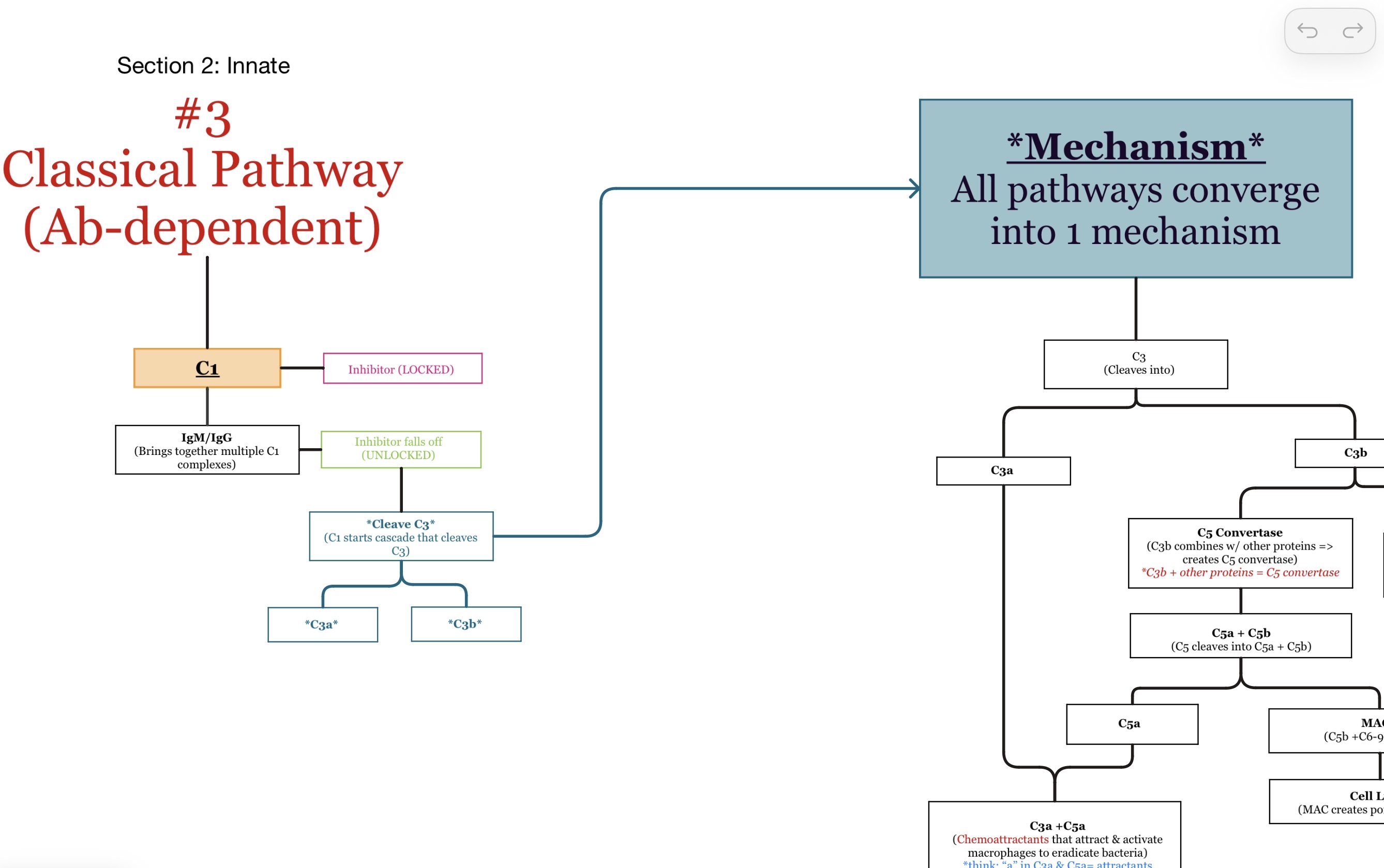
What are the 3 complement pathways?
Classical pathway
Alternative pathway
Lectin pathway
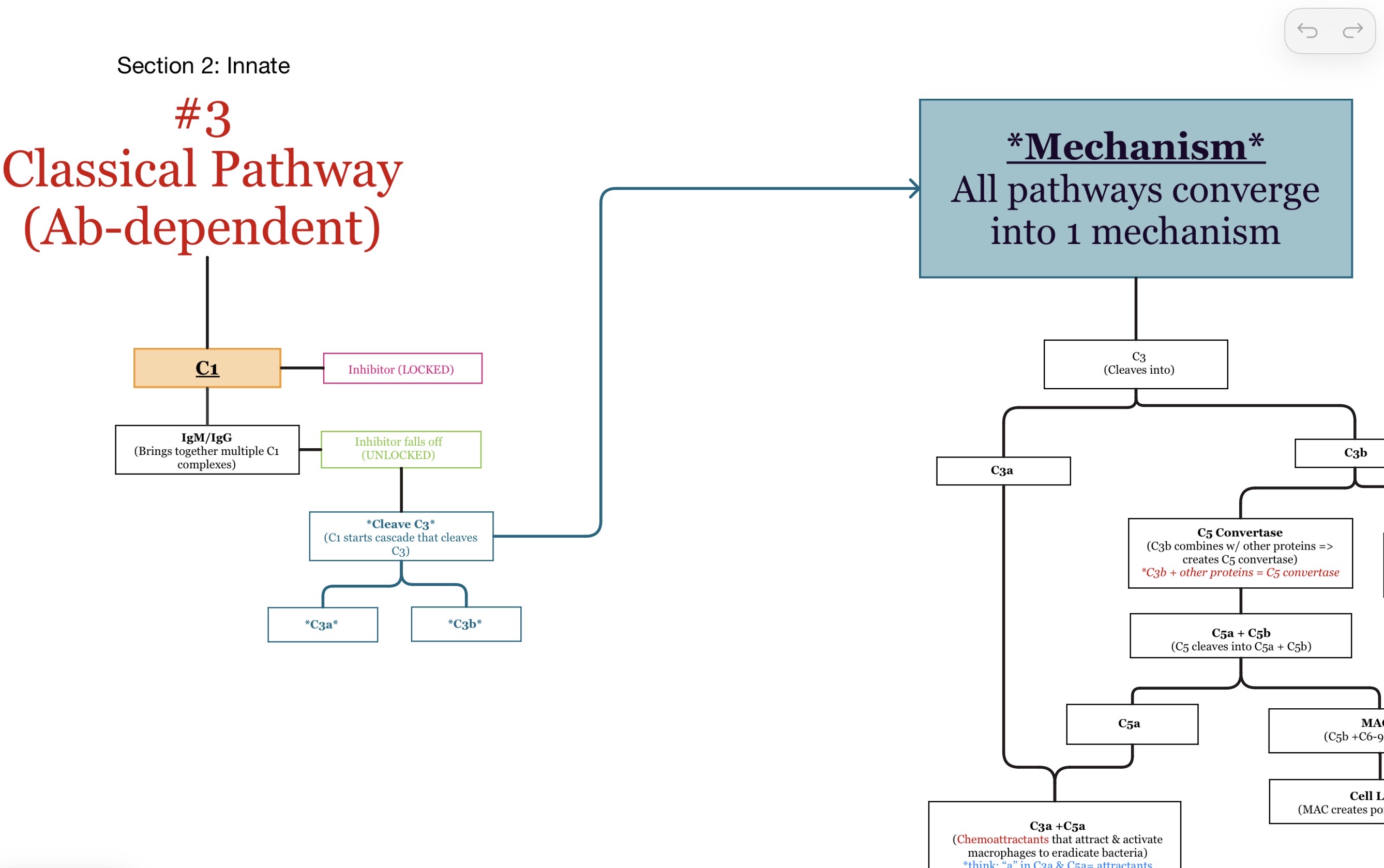
What activates the classical pathway?
Antigen-antibody complexes.
Usually:
IgG
IgM
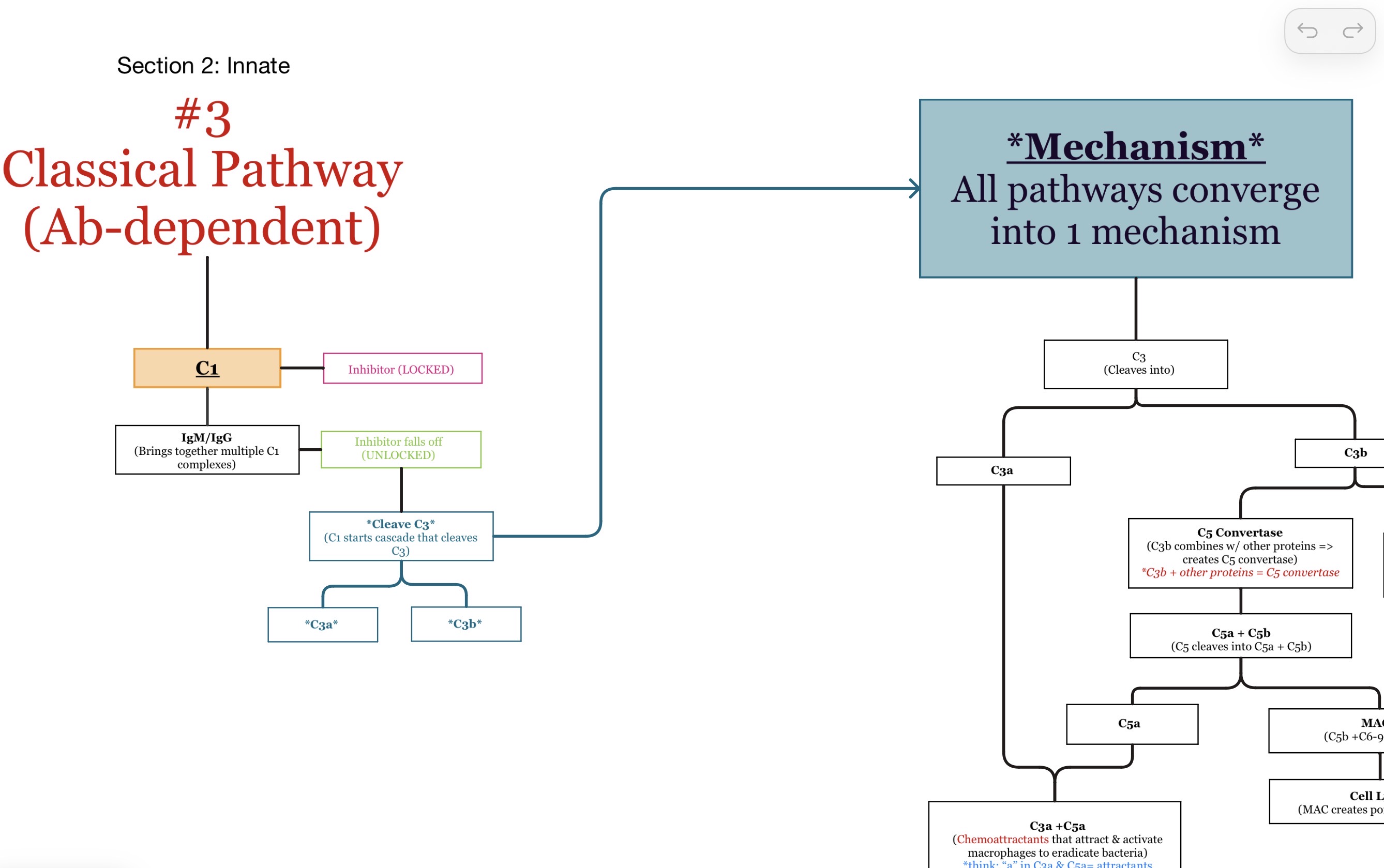
Which complement protein starts the classical pathway?
C1
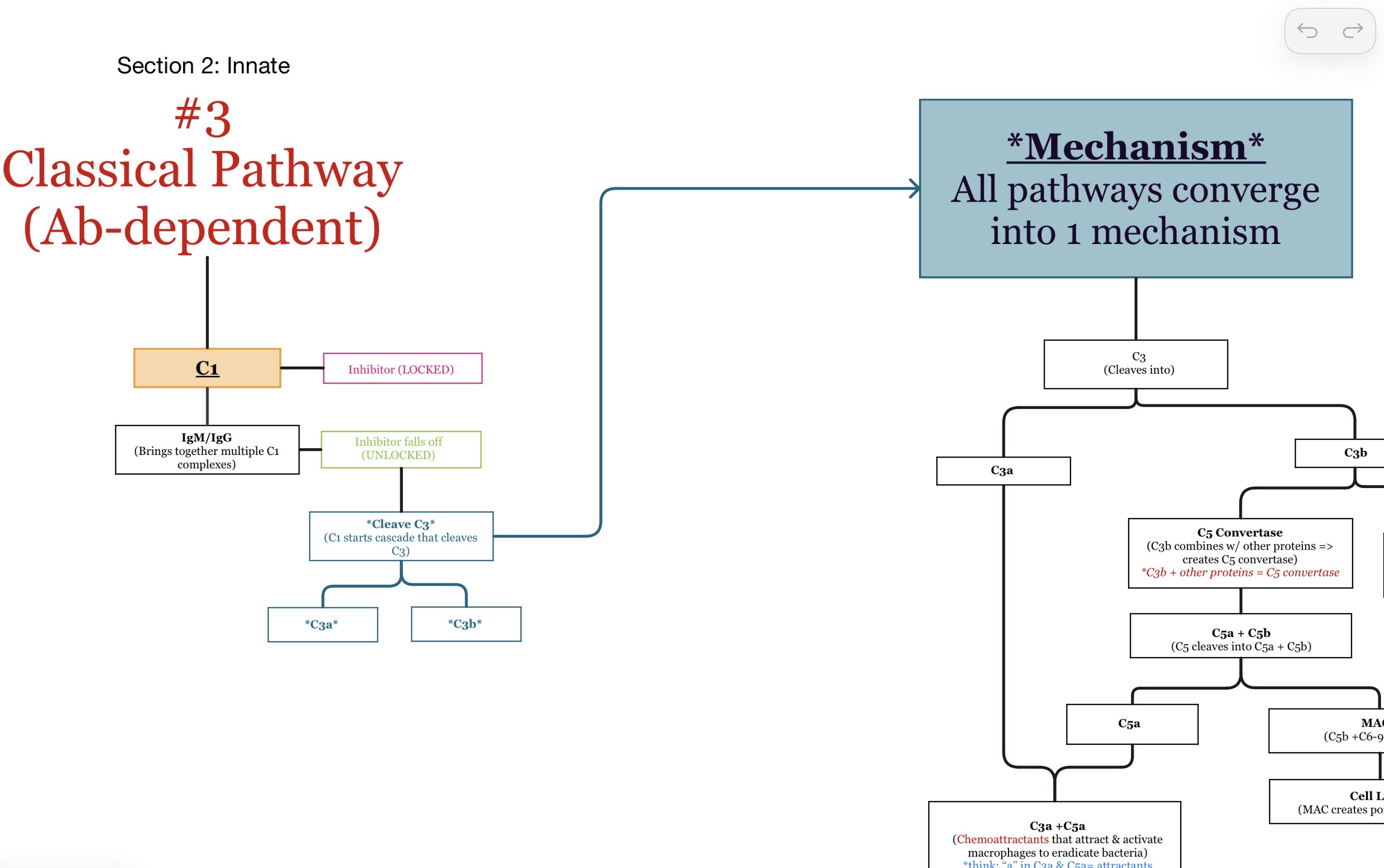
Which immune system branch is the classical pathway associated with?
Adaptive immunity b/c Ab activate it.
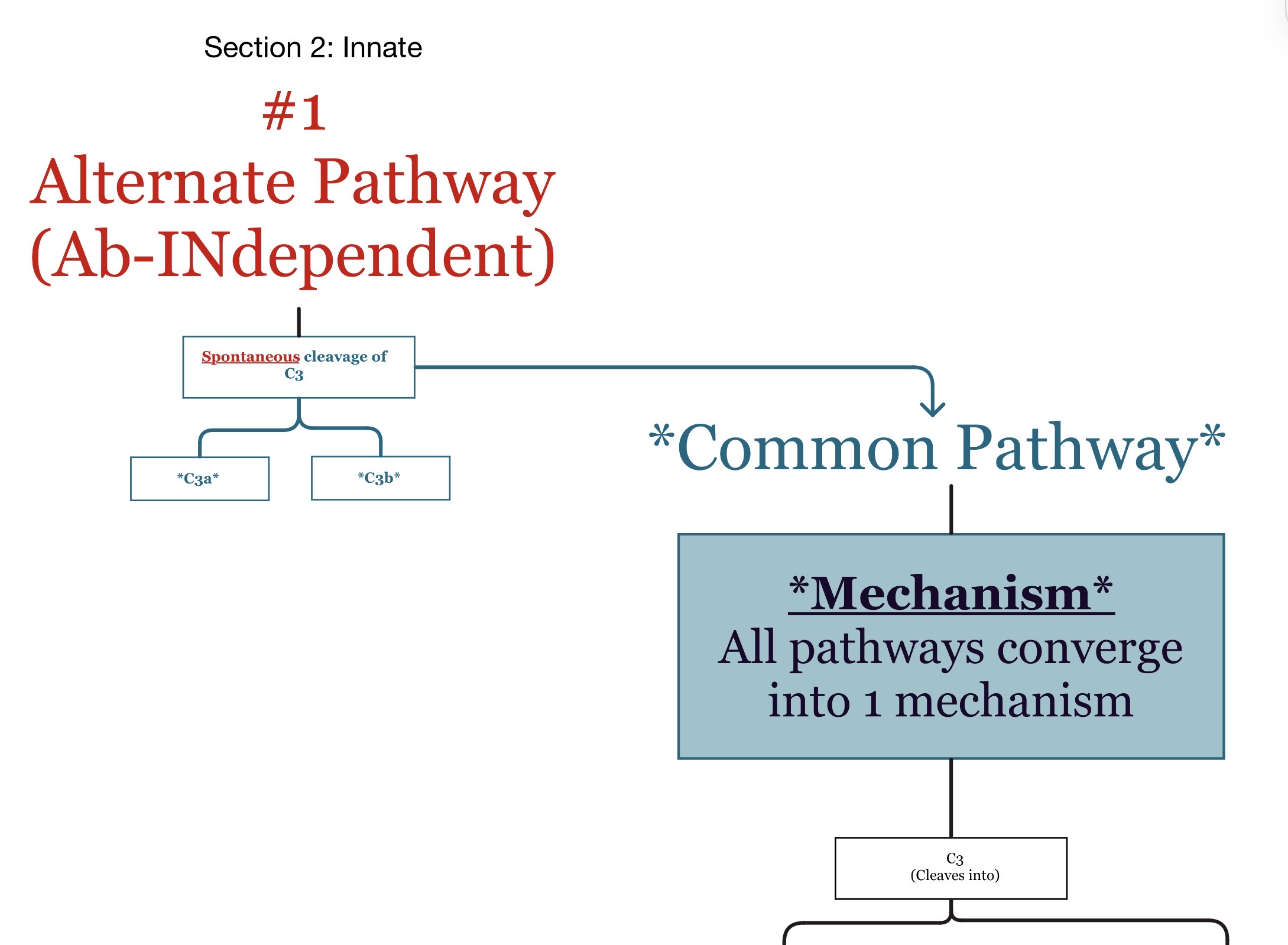
What activates the alternative pathway?
Direct microbial surfaces/pathogens.
No antibody required.
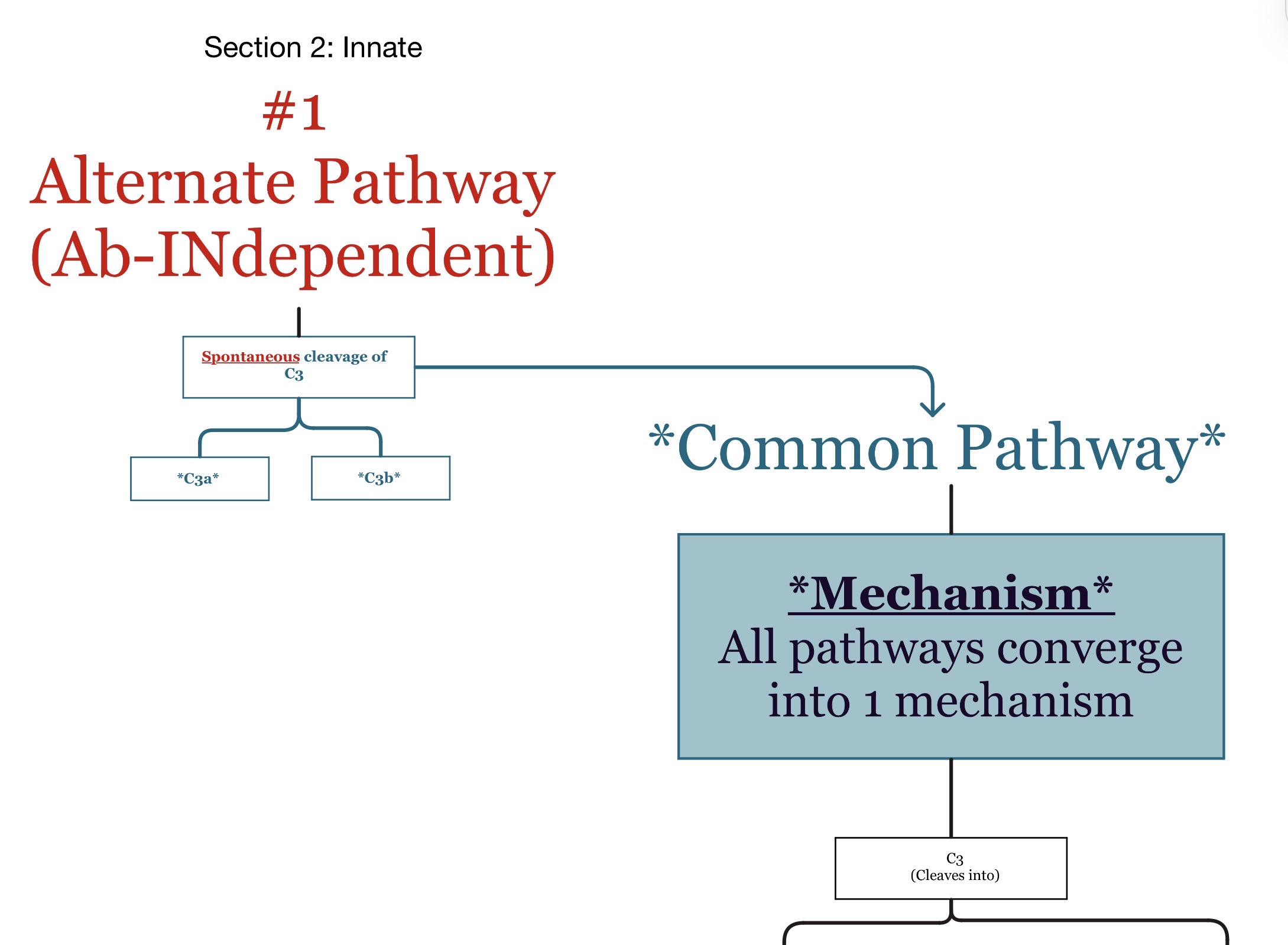
Which immune system branch is the alternative pathway associated with?
Innate immunity.
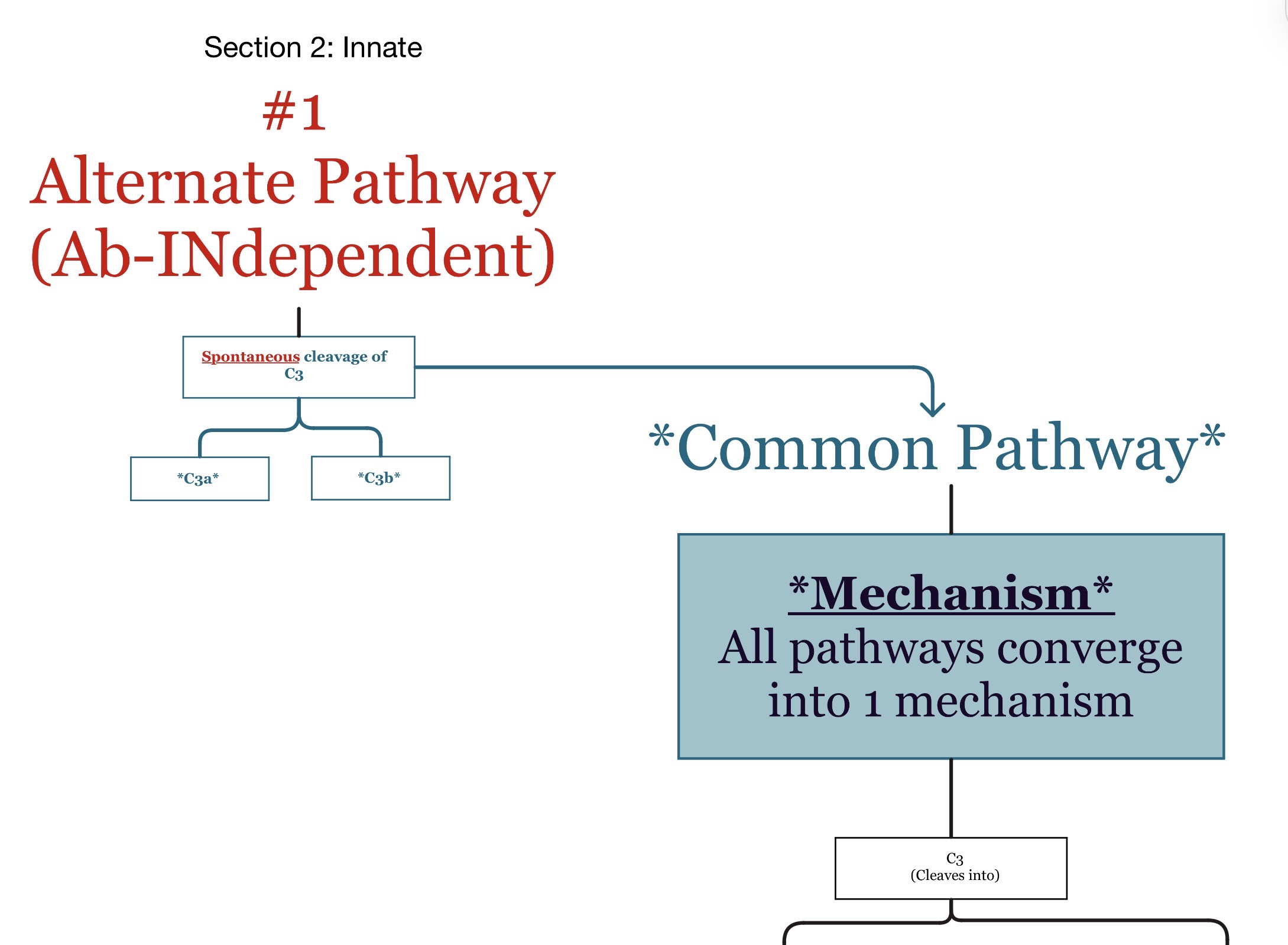
What is unique about the alternative pathway?
It can activate immediately W/OUT antibodies
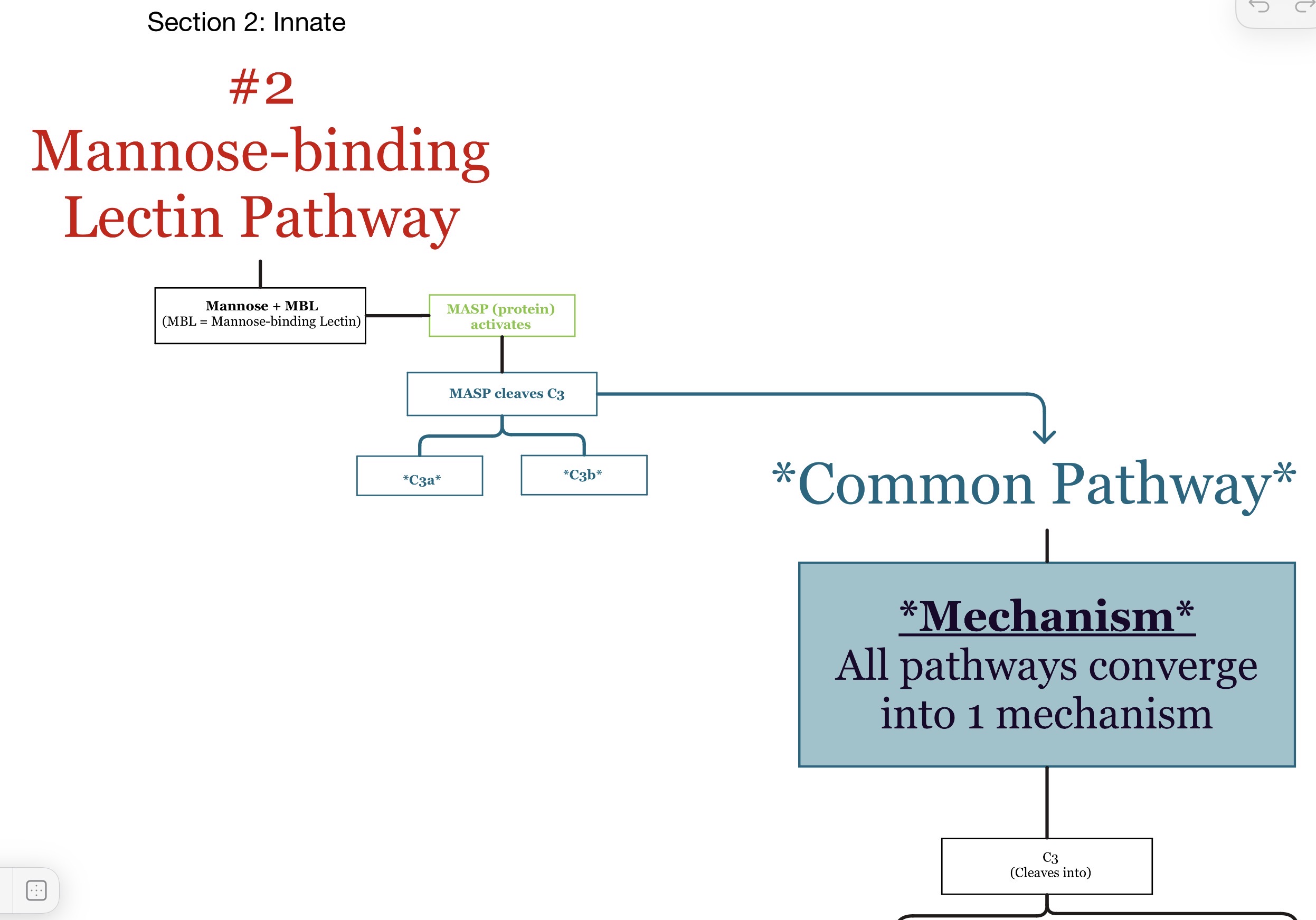
What activates the lectin pathway?
Mannose-binding lectin (MBL) binding to microbial carbohydrates.
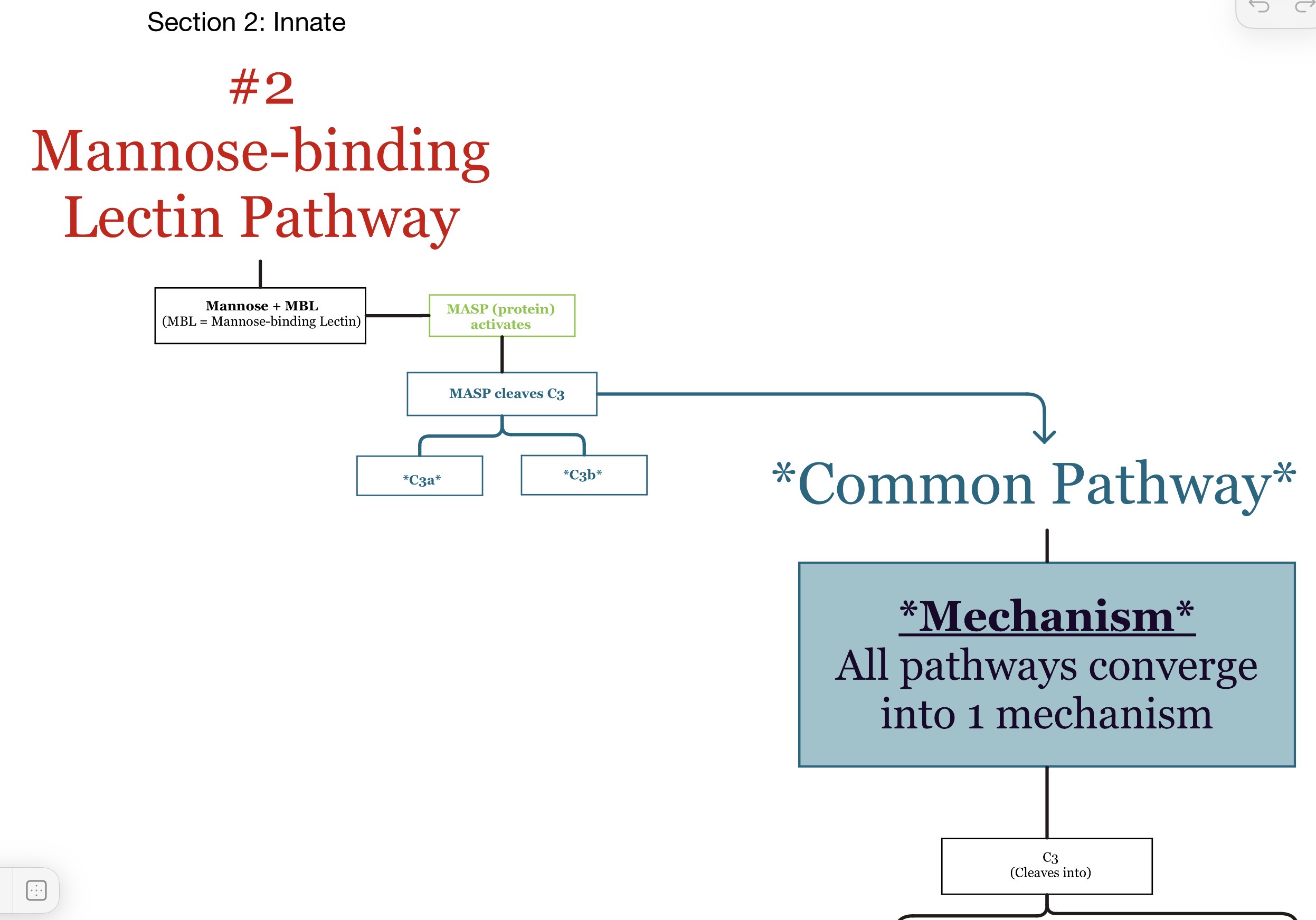
What does MBL recognize?
Mannose sugars on pathogen surfaces.
Is the lectin pathway innate or adaptive?
Innate immunity.
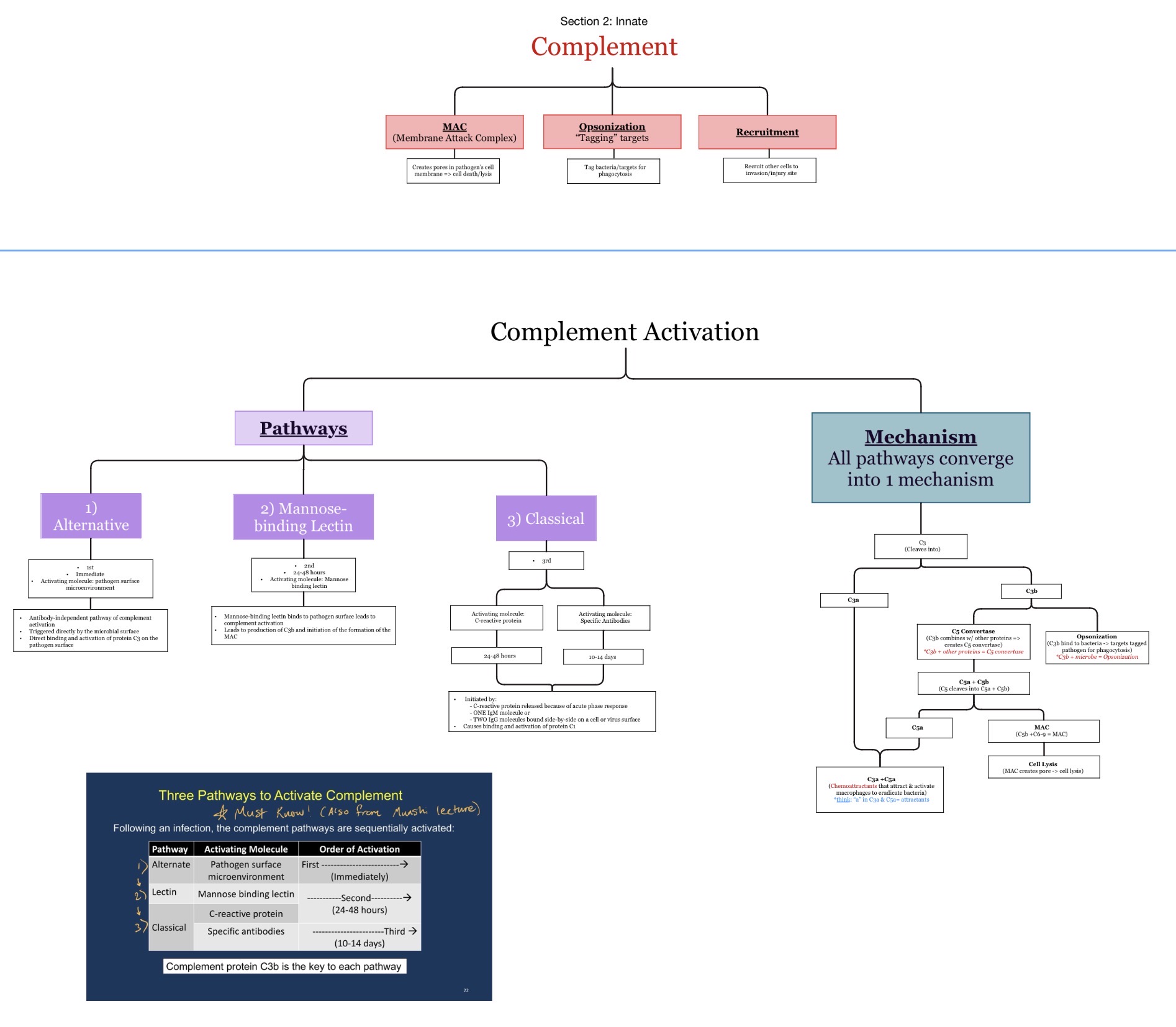
Which complement pathways activate FIRST to LAST during infection?
Alternative → Lectin → Classical
Alternative & Lectin: b/c they do NOT require Ab.
Classical: b/c it requires that Ab must FIRST be produced.
What is opsonization?
Coating pathogens to enhance phagocytosis.
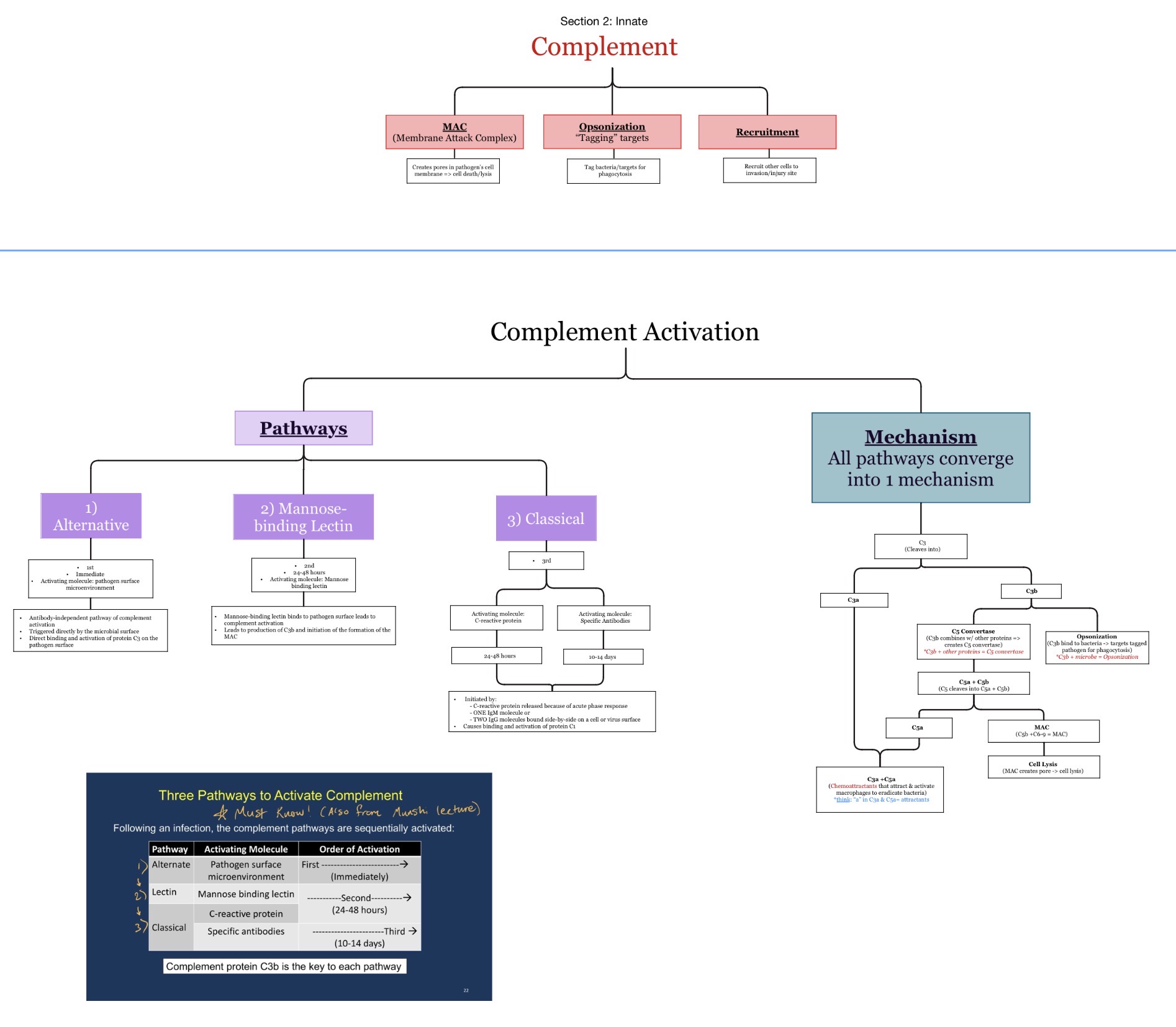
Which complement component is the major opsonin?
C3b
What does C3b do?
C3b coats microbes and helps phagocytes bind and ingest them.
Which cells perform phagocytosis?
Neutrophils
Macrophages
How does complement enhance phagocytosis
C3b binds microbes and phagocyte complement receptors recognize C3b.
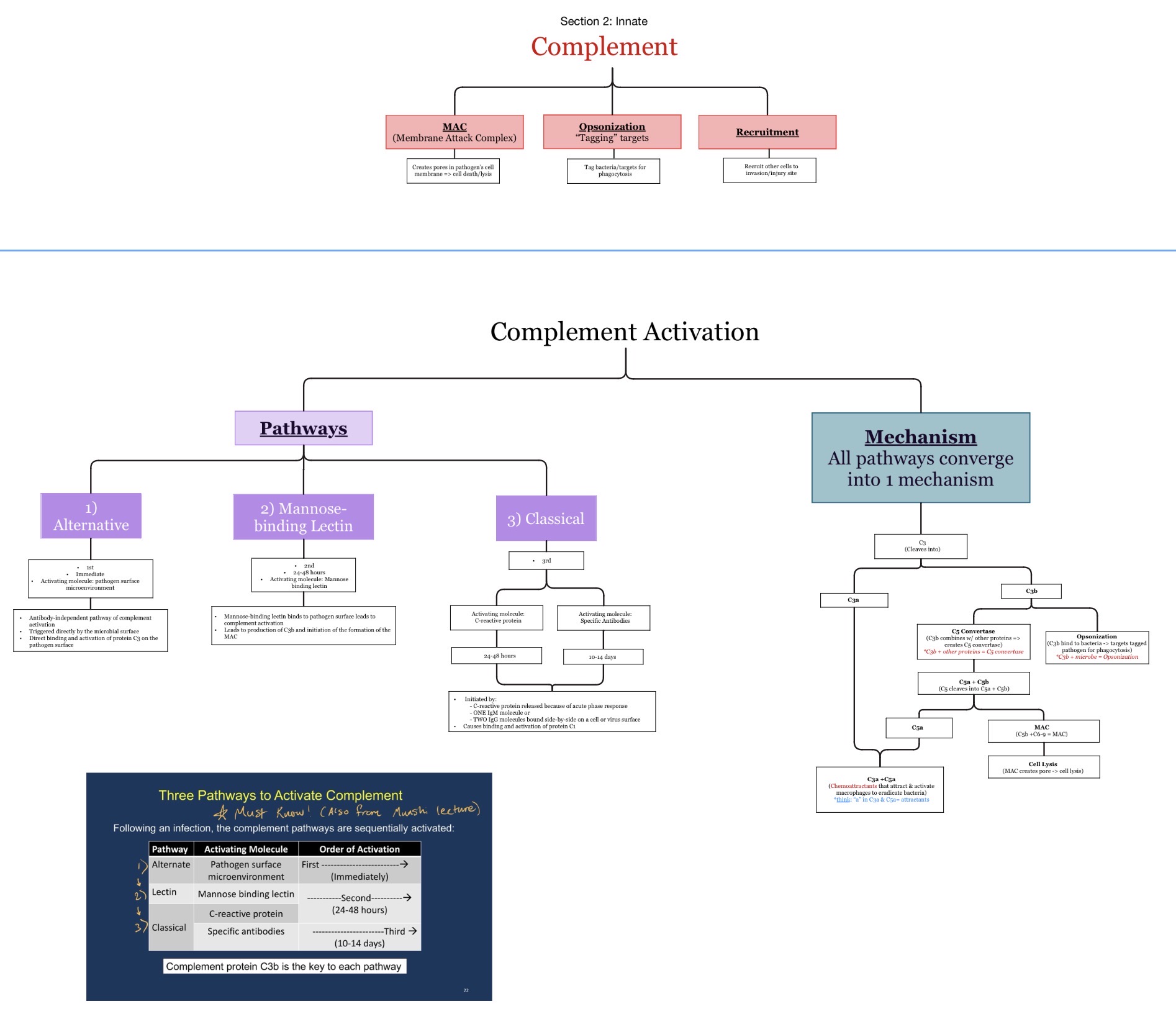
Which complement fragments are important inflammatory mediators?
The chemoattractants:
C3a
C5a
What are anaphylatoxins?
Complement fragments that trigger inflammation and mast-cell degranulation.
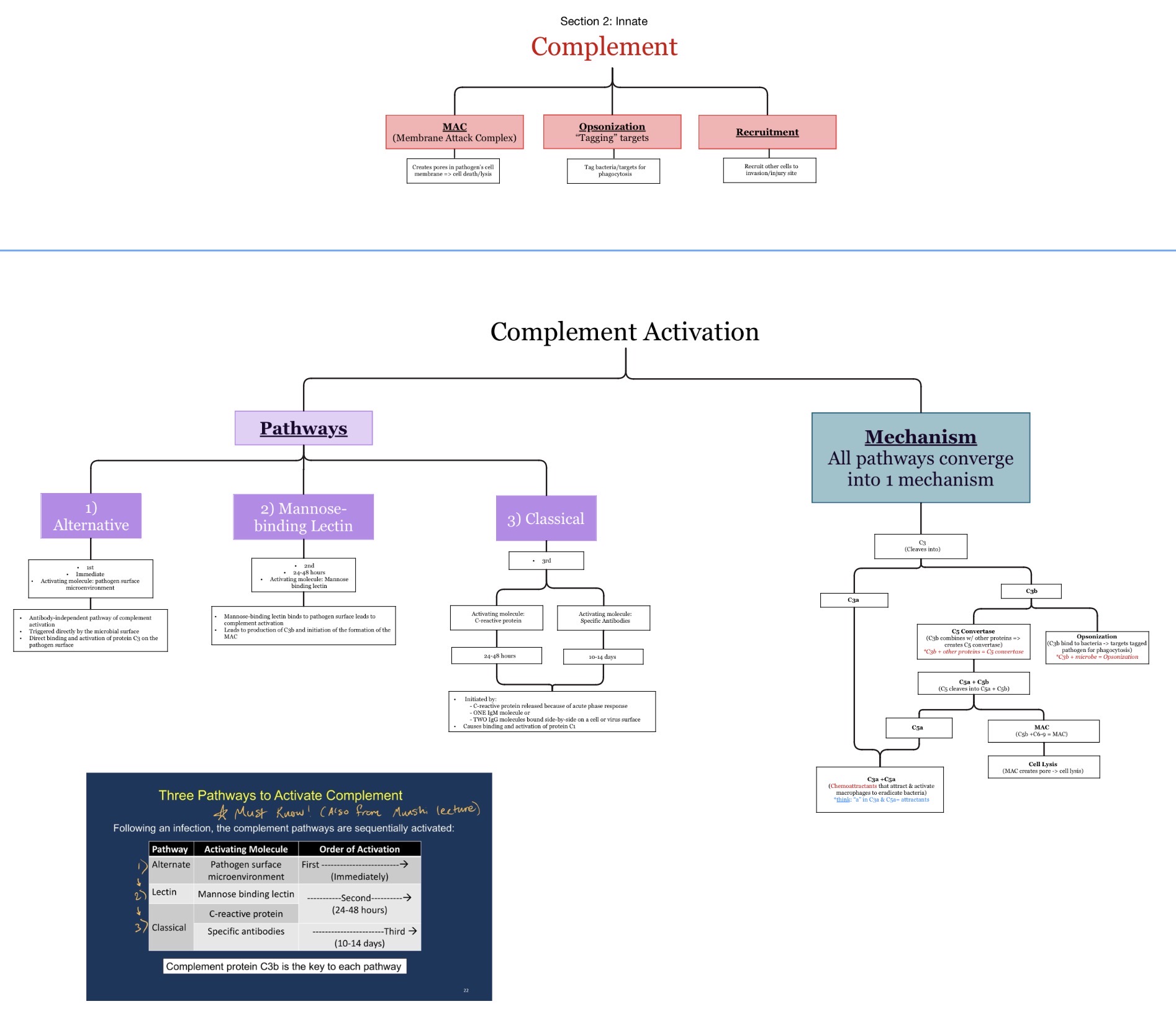
Which complement factors can cause anaphylactic shock reactions?
C3a and especially C5a.
These are called anaphylatoxins.
Which complement factor is the MOST powerful anaphylatoxin?
C5a
What does C5a do?
Mast-cell degranulation
Histamine release
Increased vascular permeability
Neutrophil chemotaxis
Strong inflammation
What does chemotaxis mean?
Movement/recruitment of immune cells toward infection.
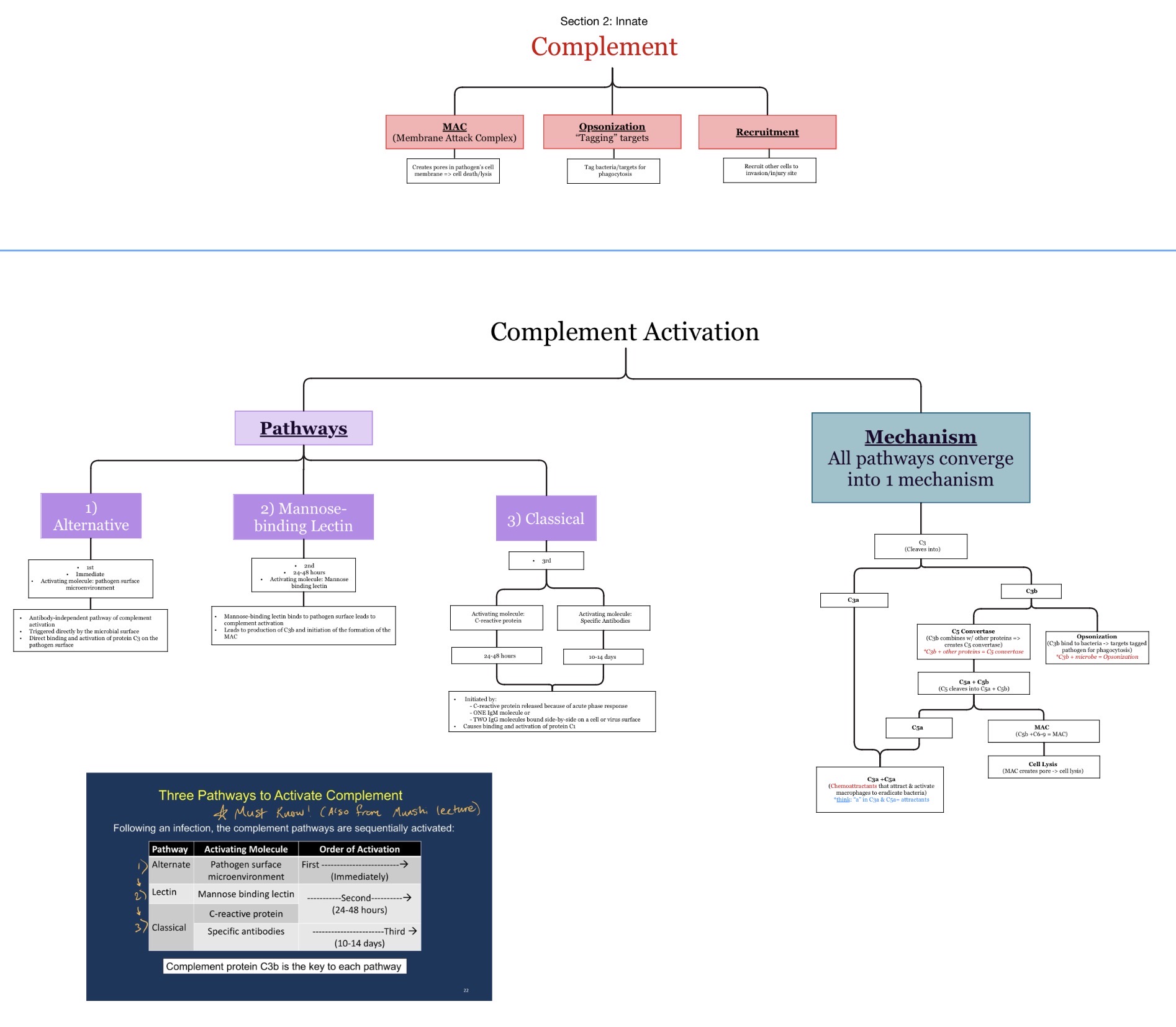
What is the membrane attack complex (MAC)?
A pore-forming complement complex that lyses pathogens.
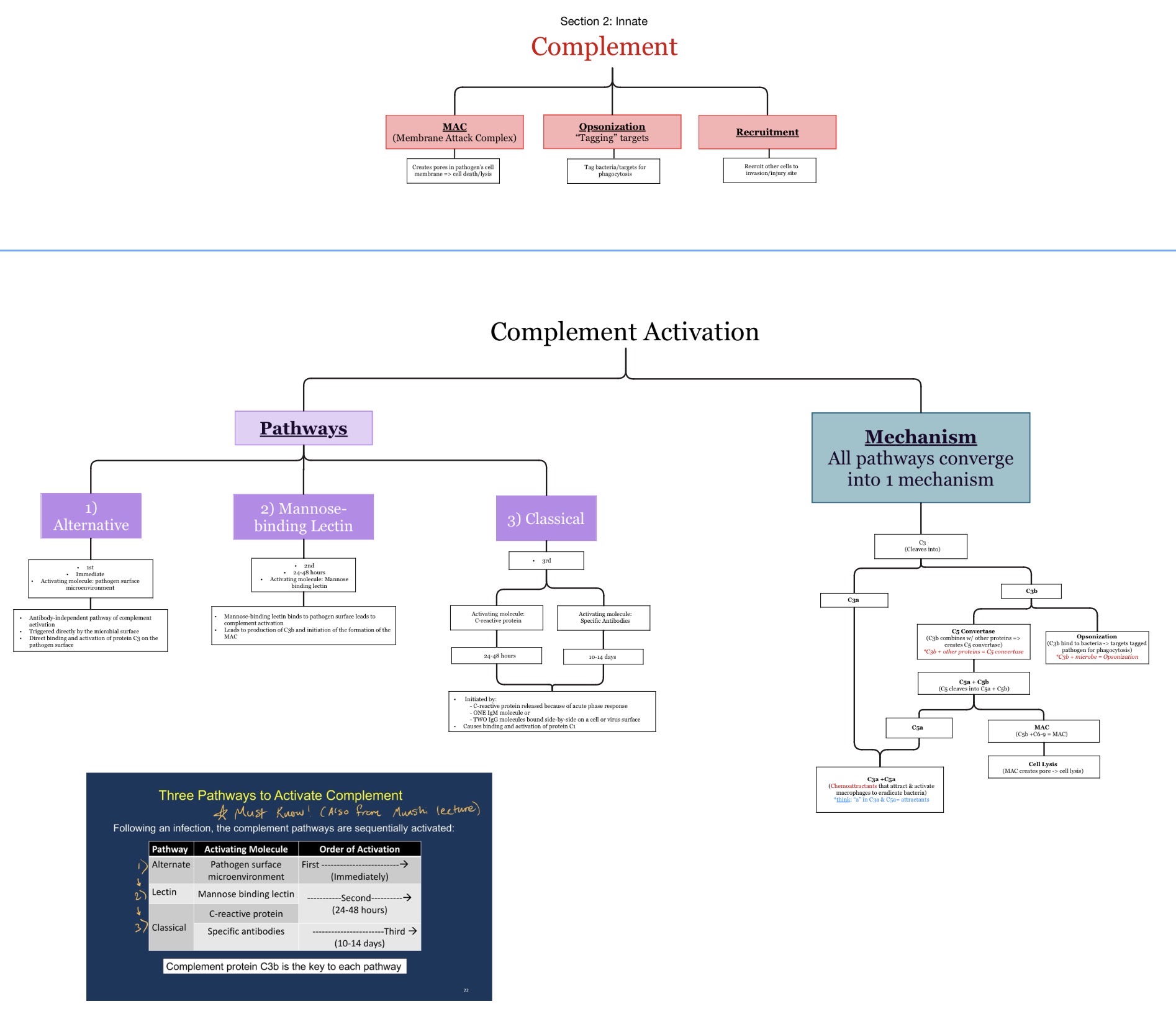
Which complement components form the MAC?
C5b-C9
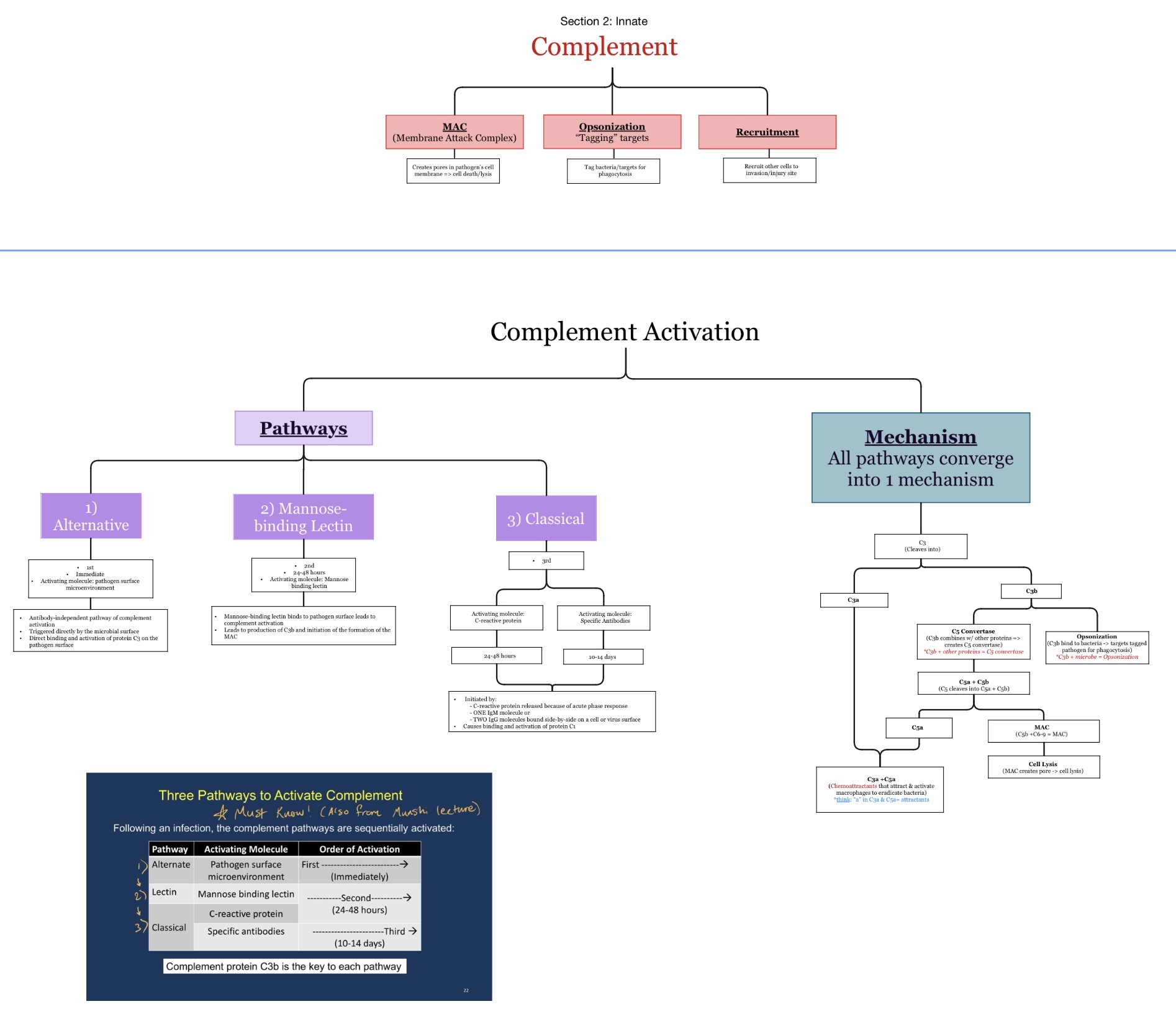
What does the MAC do?
Creates pores in microbial membranes causing lysis.
🔥Complement Components table
Complement Component | Function |
C3b | Opsonization |
C3a | Inflammation/anaphylatoxin |
C5a | Strong inflammation + chemotaxis |
C5b-C9 | Membrane attack complex |
Obj. 3
Membrane attack complex formation steps and its function.
🔹What does MAC stand for?
Membrane Attack Complex
How does the MAC kill bacteria?
The MAC forms pores in the membrane causing:
ion imbalance
water influx
osmotic lysis
What type of killing does MAC cause?
Cell lysis
Obj. 5
Phases and characteristics of immune response (innate immunity, adaptive immunity, and immunological memory).
🔹What are the two major phases/types of immunity?
Innate immunity
Adaptive immunity
What is innate immunity?
Innate immunity is the immediate, nonspecific first-line defense against pathogens.
Is innate immunity specific or nonspecific?
Nonspecific
How quickly does innate immunity respond?
Immediately or within minutes/hours.
Does innate immunity have memory?
No. No significant immunologic memory.
Main cells involved in innate immunity?
Neutrophils
Macrophages
Dendritic cells
NK cells
Mast cells
Main components of innate immunity?
Physical barriers
Complement
Phagocytes
Cytokines
Inflammation
NK cells
Which complement pathways are part of innate immunity?
Alternative pathway
Lectin pathway
What are the characteristics of innate immunity?
Rapid
Nonspecific
No memory
Same response with repeated exposure