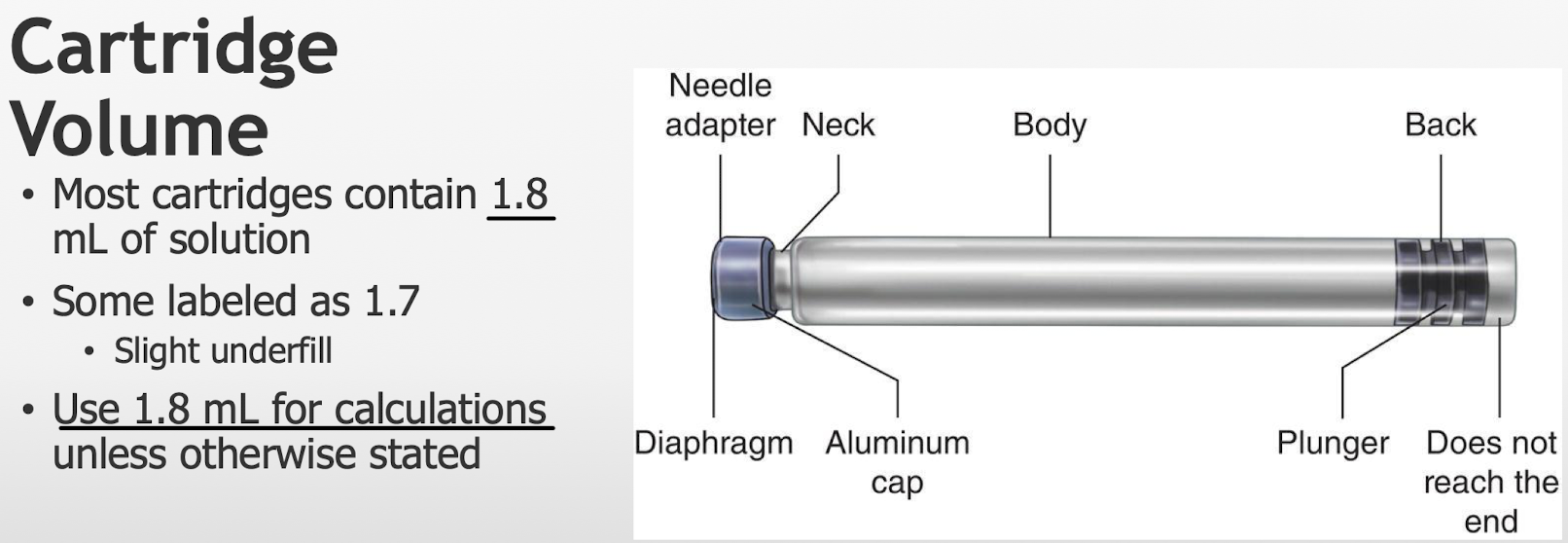
Local Anesthetics and Vasoconstrictors
1/81
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
82 Terms
What are the ideal local anesthetic properties:

Where do pain signals originate from? How do we detect these signals?
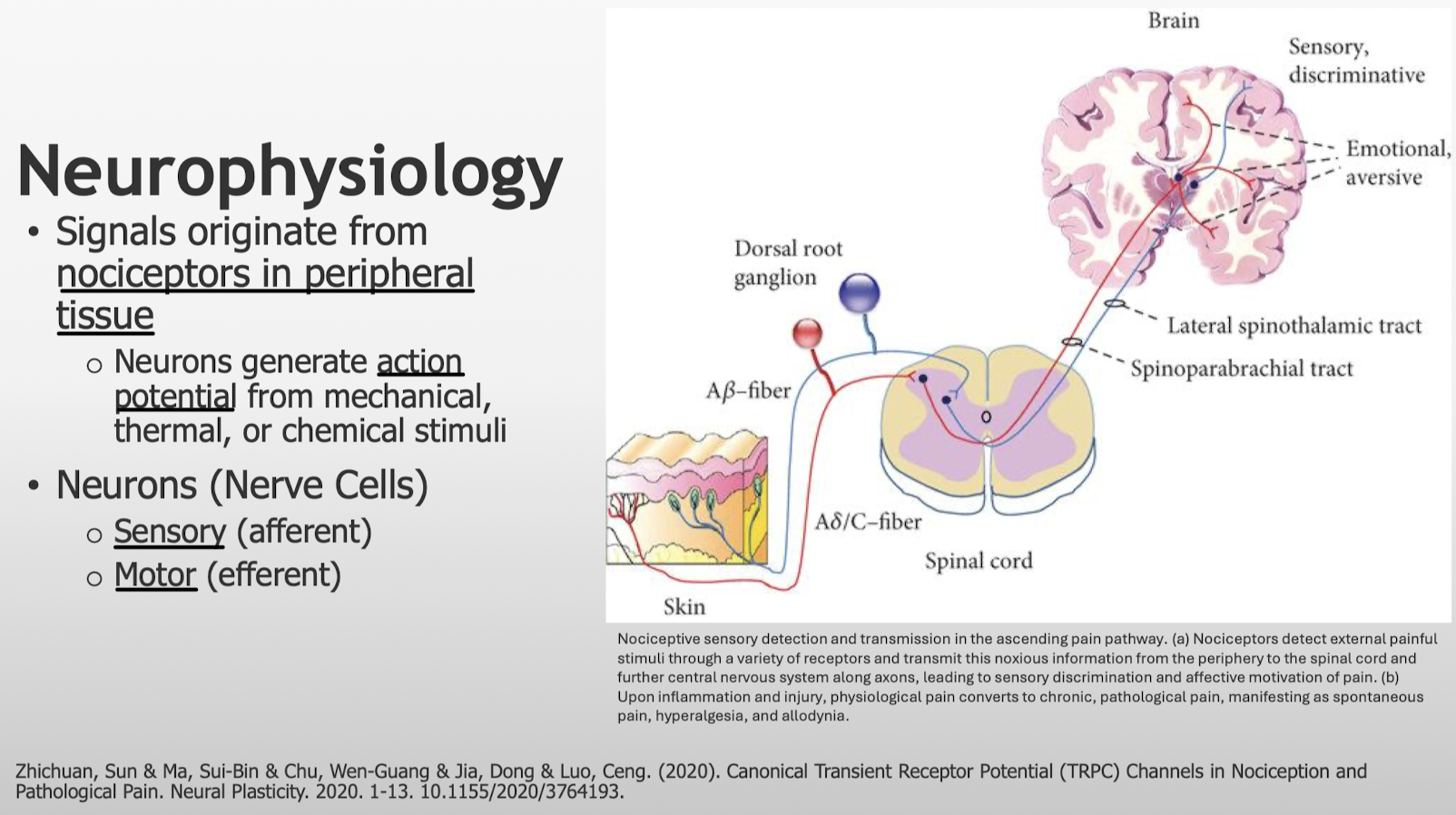
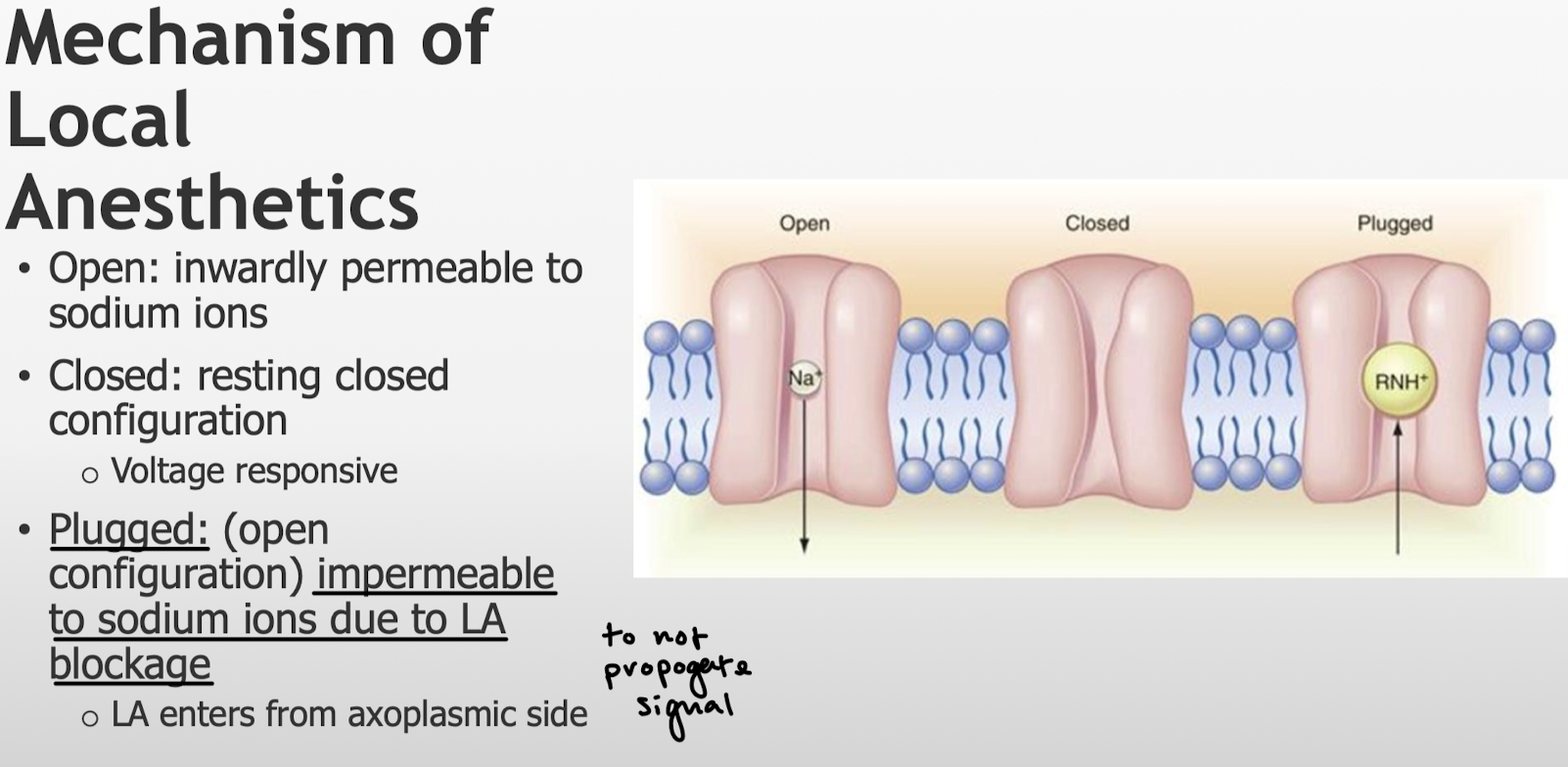
What is the general mechanism of local anesthetics?

Explain the different states of the sodium channels and how local anesthetics work on the sodium channels.
What is the general structure of local anesthetics? What are the two ends? What kind of LAs cannot be used as injections due to their structure?
Hydrophilic end = amine group
Lipophilic/hydrophobic = aromatic ring
LA without hydrophilic end would not be dissolved into liquid form.
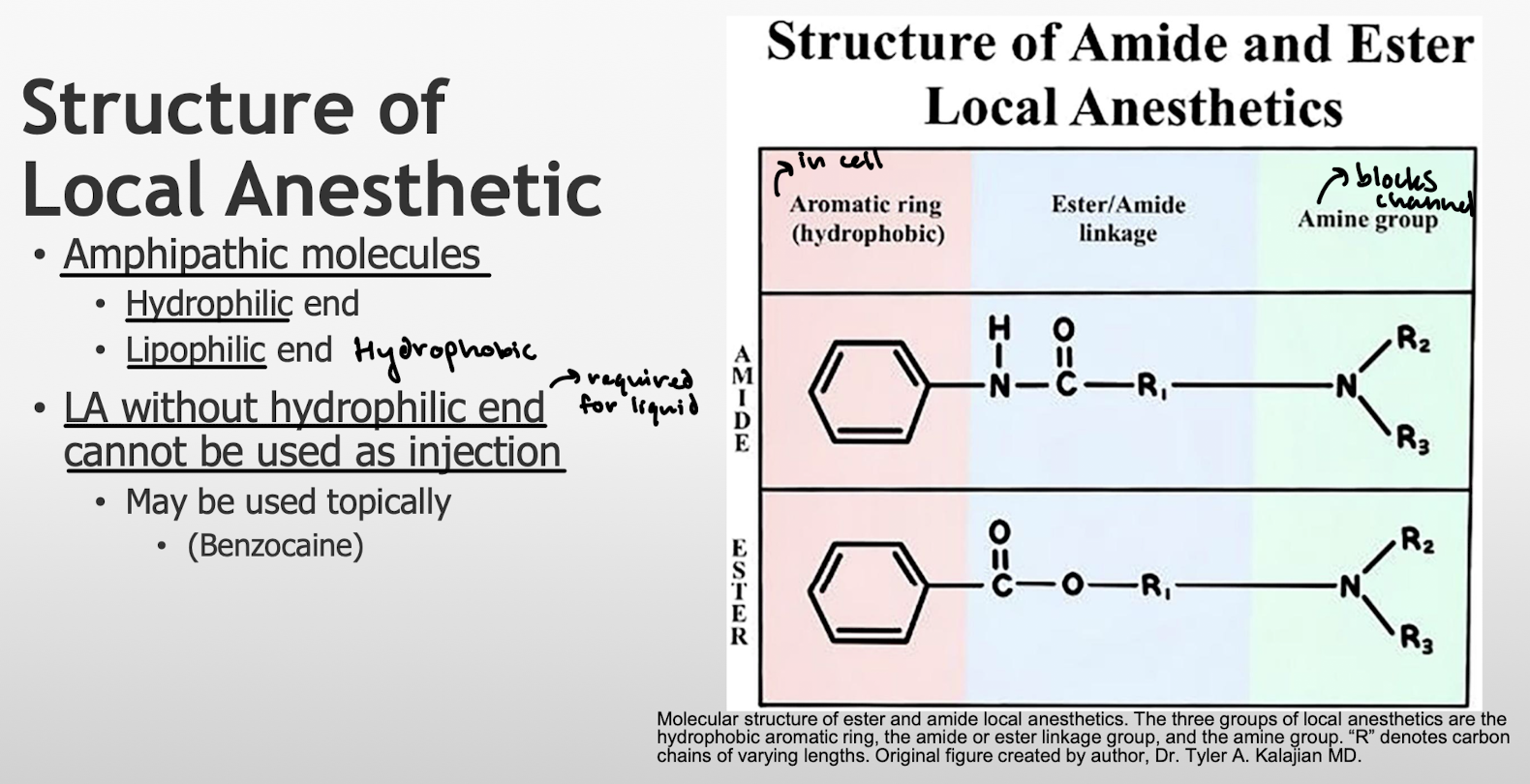
What are the characteristics of amino ester LAs? Duration, elimination, etc.

What are the characteristics of amino amide LAs? How it is metabolized, etc.

What is the physiologic pH of normal oral tissue? Inflammed tissue?

What is the pH of LAs (with and without vasoconstrictor)? Are they soluble in water?

How do local anesthetics absorb across the nerve sheath and bind at receptor sites?

Generally, more acidic = (less/more) pain
more
How does recovery occur after a LA block? Is this process slower or faster than induction of LA?

What is the vasoactivity of LAs? Cocaine? What clinical applications does this have?

What are the forms of absorption of a LA (3)? What do each depend on?

What is the time to achieve peak blood level for IV, topical, IM, and SQ?

Once it is absorbed into blood, where does LA go? What is the rate dependent on?
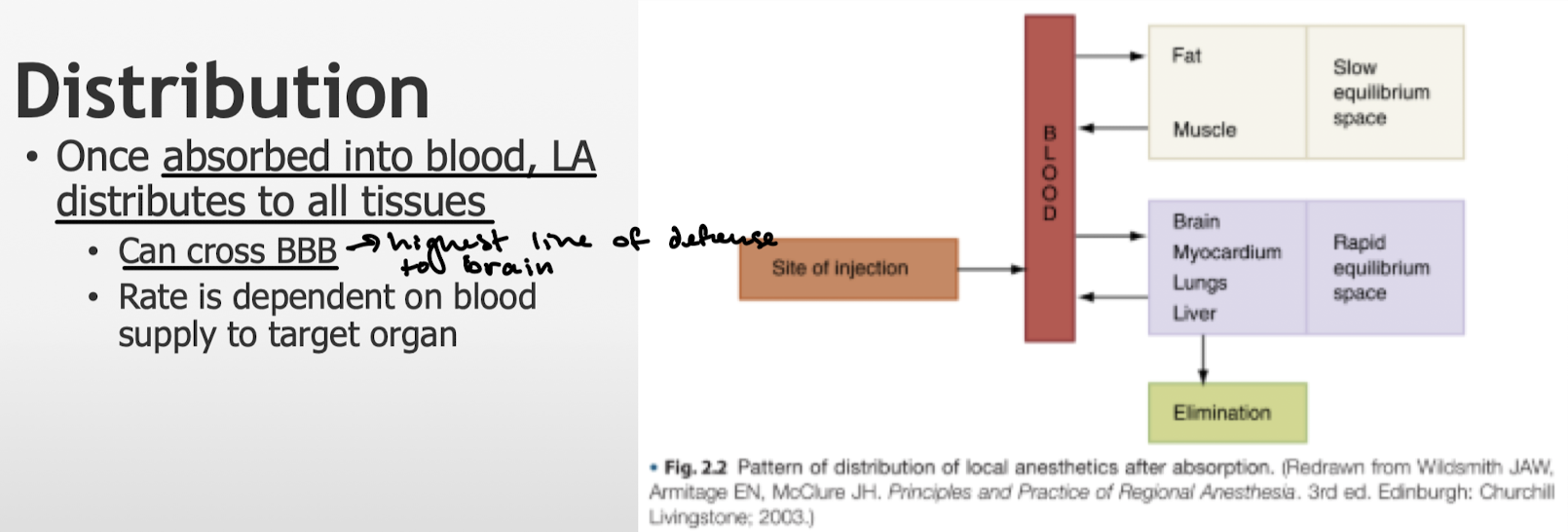
How is an ester LA metabolized? By what enzyme? The rate of hydrolysis impacts _______.
Hydrolyzed by pseudocholinesterase in plasma/blood. Toxicity.

What is the allergenicity of ester LAs?

How are amide LAs metabolized? The liver does nearly all the metabolism for which amides? Which is a hybrid ester/amide and where is it primarily metabolized?

What determines the extent of metabolism of Amide LAs? What are the factors that decrease liver function?
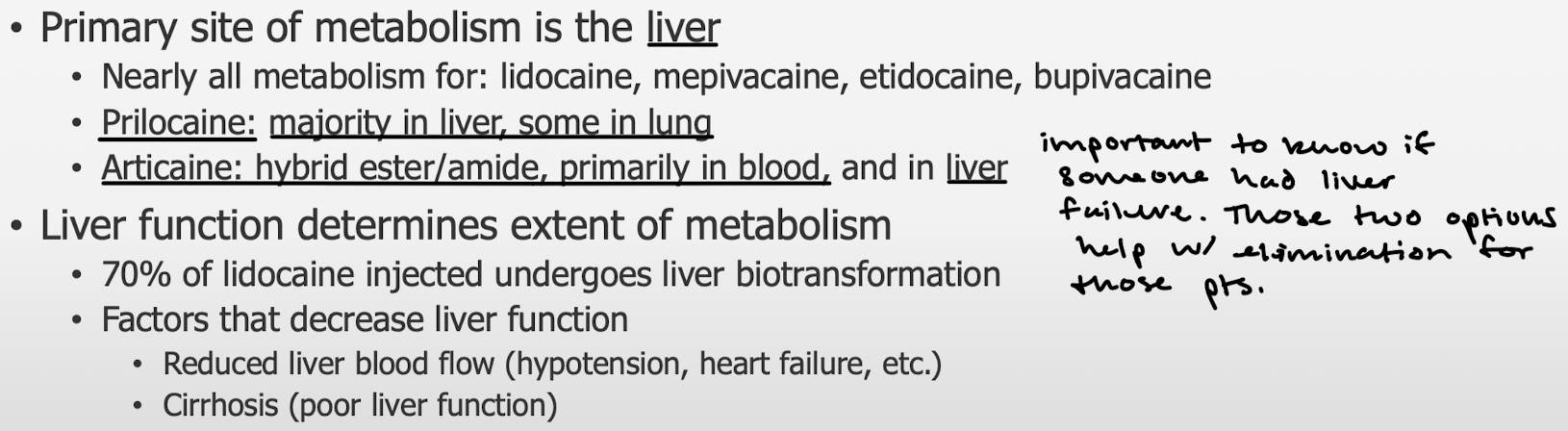
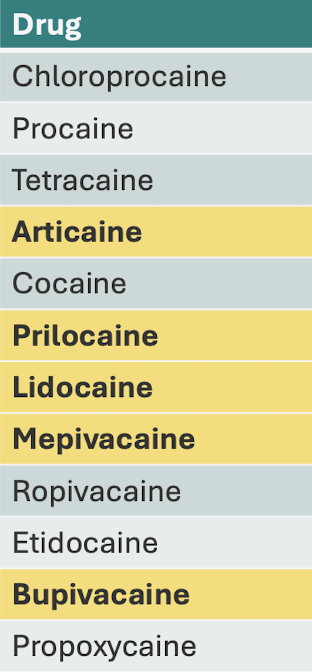
Which drugs are amides? Which are esters?
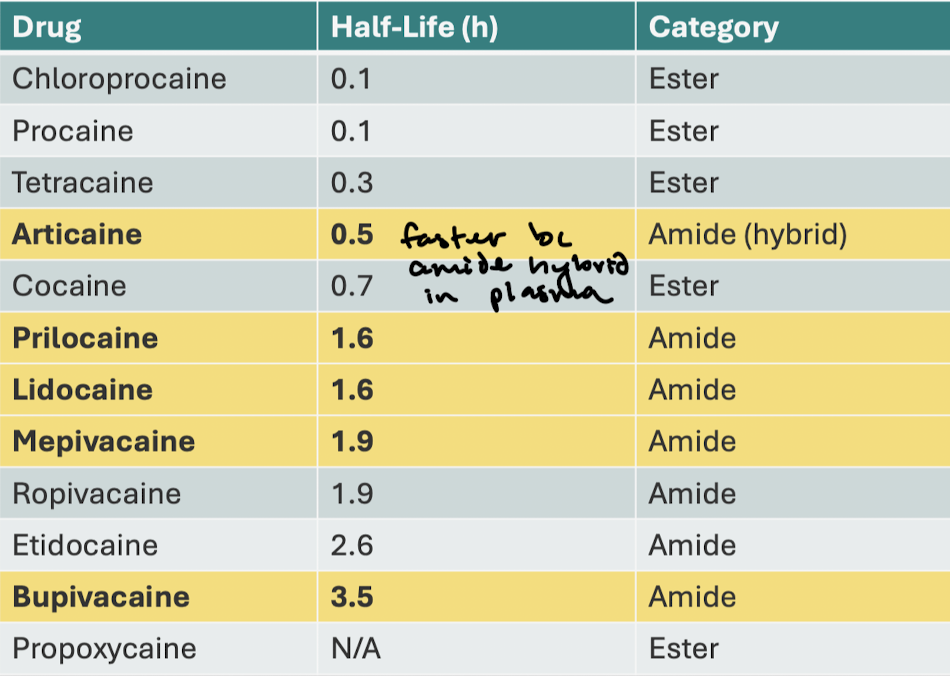
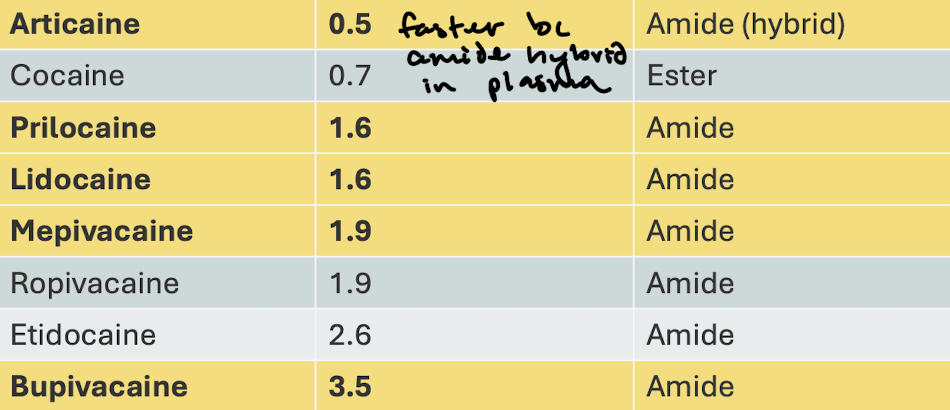
What are the half-lives of the amides?
In hours!
Define half life. What does 1 half life mean? 2, 3, 4, and 5?
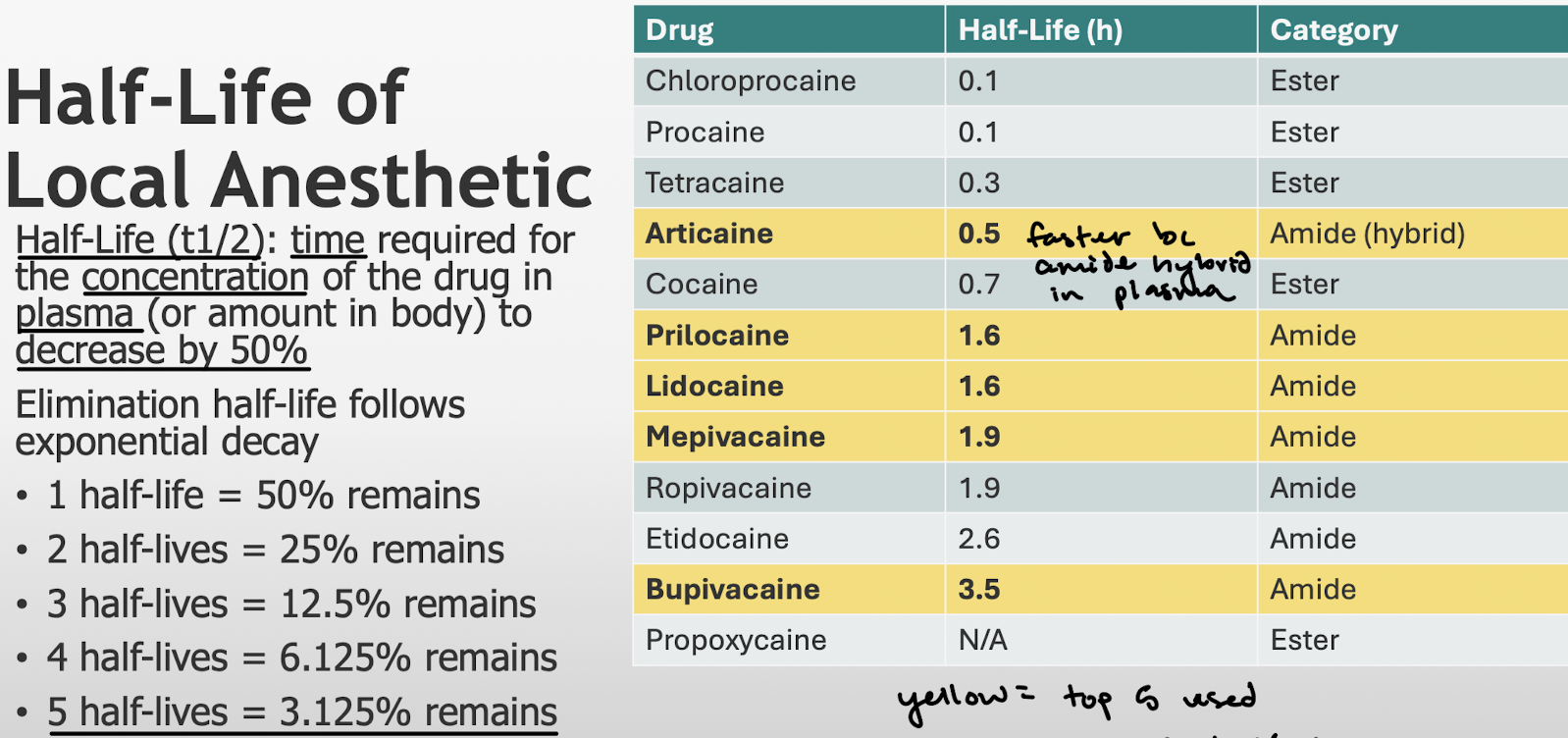
What is the number of half-lives necessary for the drug to be considered not clinically active?
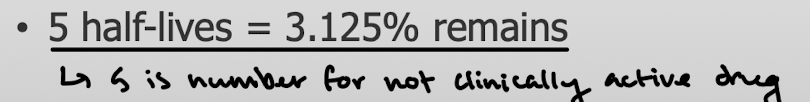
What is the primary form of excretion? What are the clinical implications of this?

What are the relative contraindications for increased risk of toxicity due to renal dysfunction?

Systemic action of LA is dependent on what three things?

What are the main systemic concerns of LAs?

What is the effect of LAs on the CNS? What is the clinical significance of this?

How do low doses and high doses of LAs affect seizure threshold? Know the different level ranges.
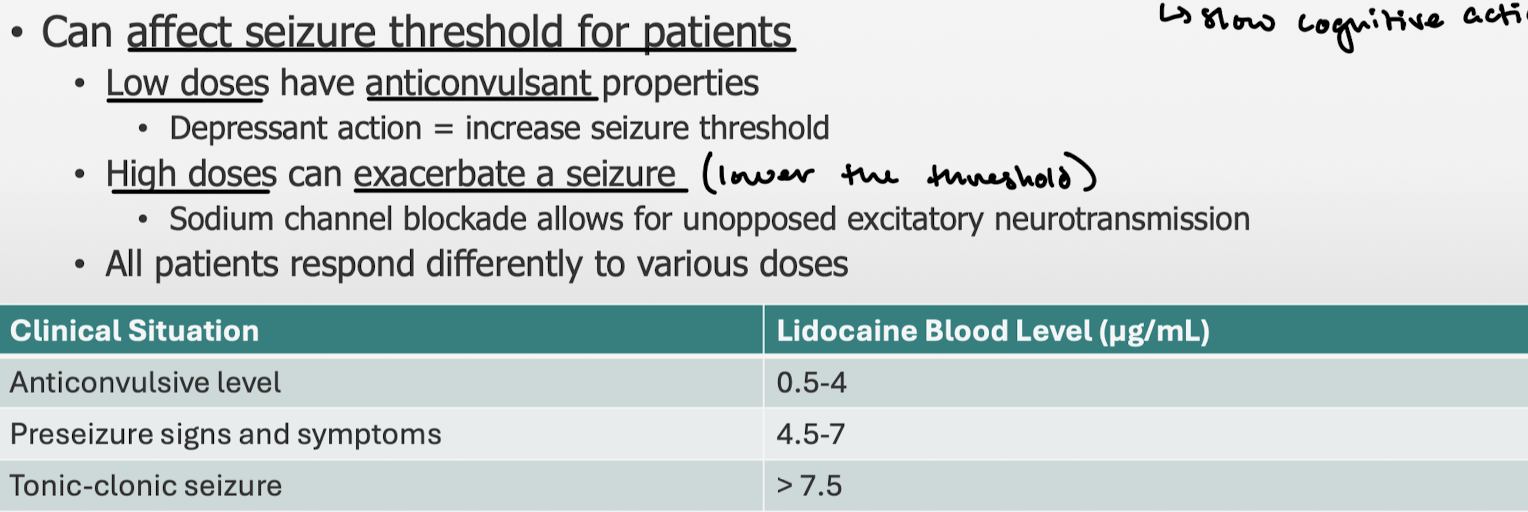
What are the preconvulsive signs and symptoms.

What is the general mechanism for CNS toxicity

What are the effects of LAs on the myocardium? What is the clinical significance of this?

What is the blood level of lidocaine after 1-2 dental cartridges administered intraorally?

What happens if blood levels are above the antidysrhythmic level?

What is the primary effect of LA in peripheral vasculature?
Hypotension
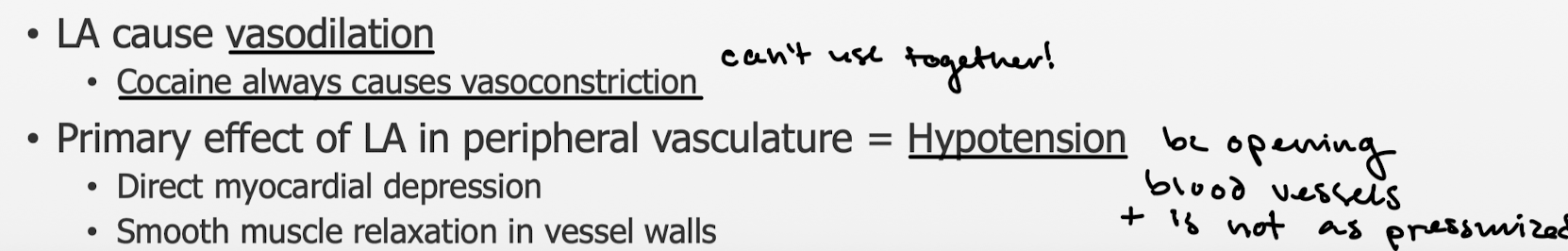
Are peripheral vasculature effects or myocardium effects more concerning? What happens at doses under overdose, at overdose level, and at lethal levels?
Myocardium effects

What are two other systemic effects of LA?

Summary of Systemic Effects of Local Anesthetics
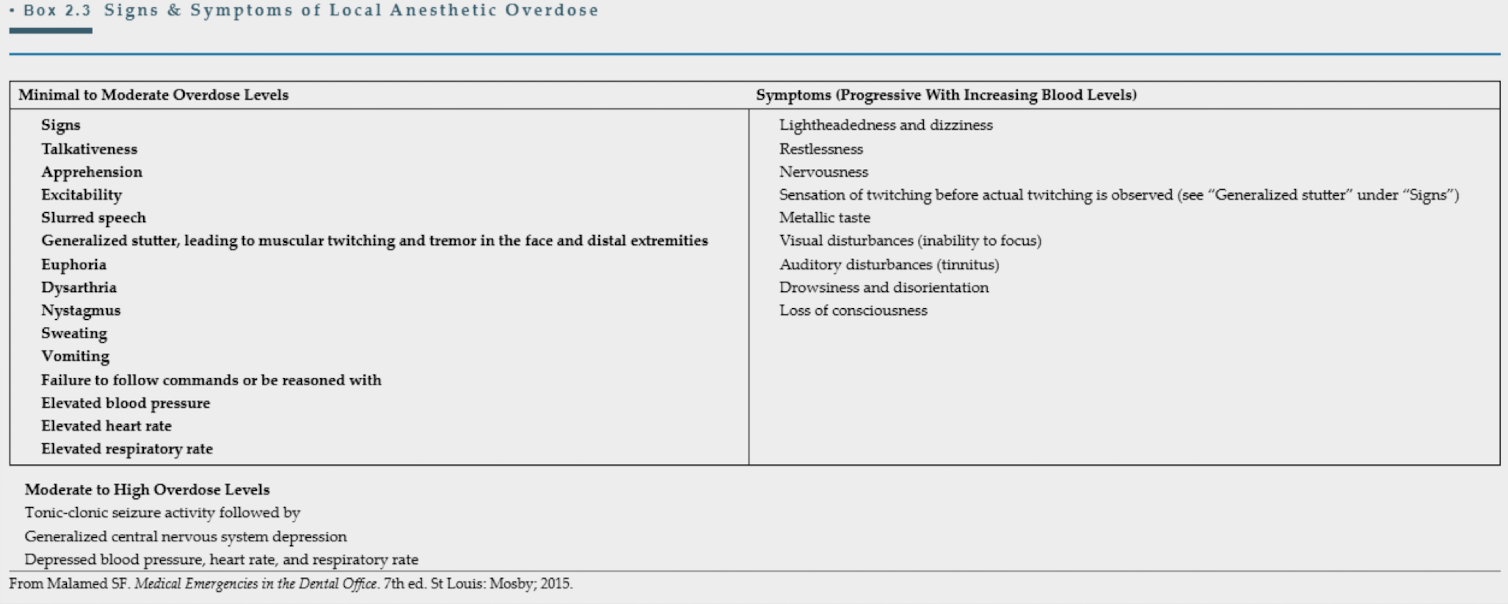
What are the LA administration issues (4)?

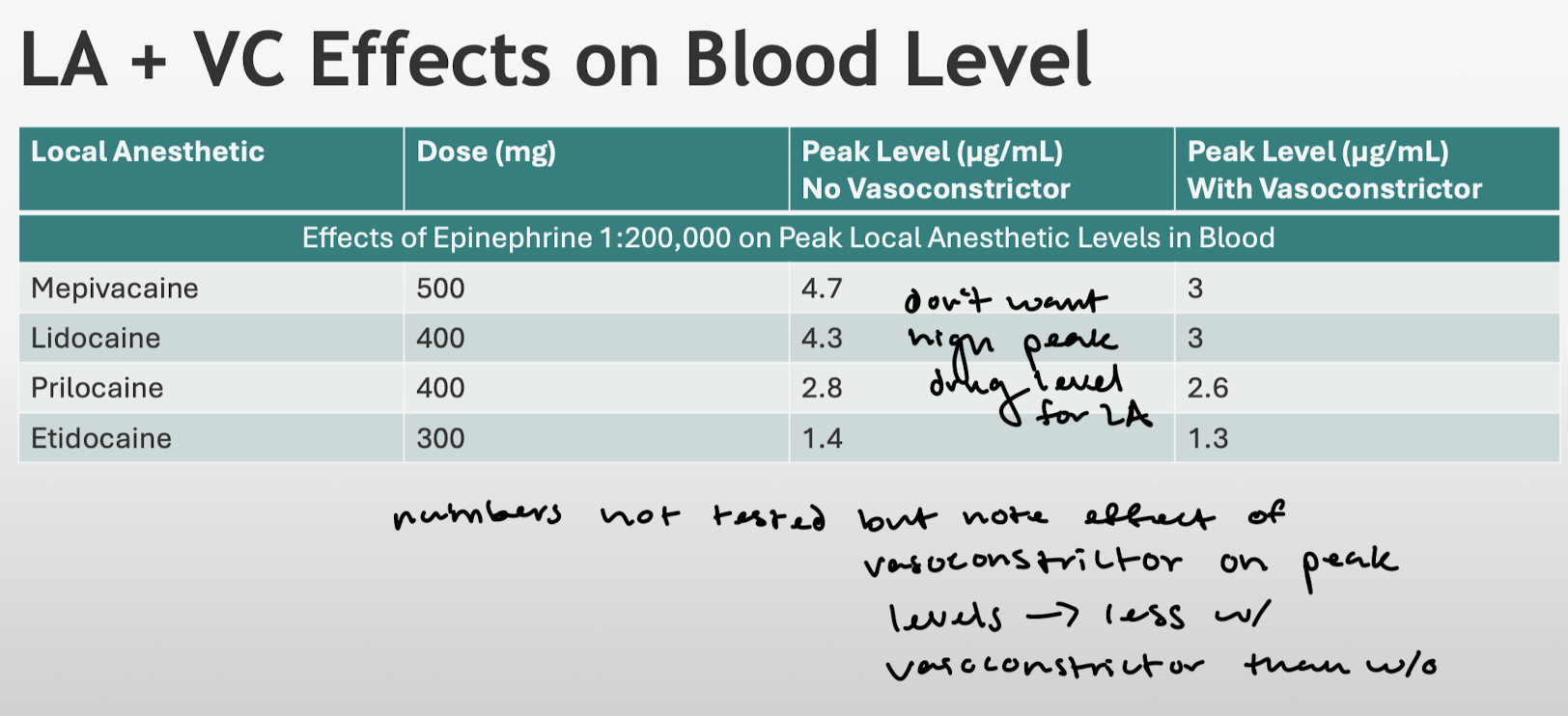
Based on the previous slide, how does adding a vasoconstrictor affect these issues?

What is the effect of adding VC on peak blood levels?
Reduced.

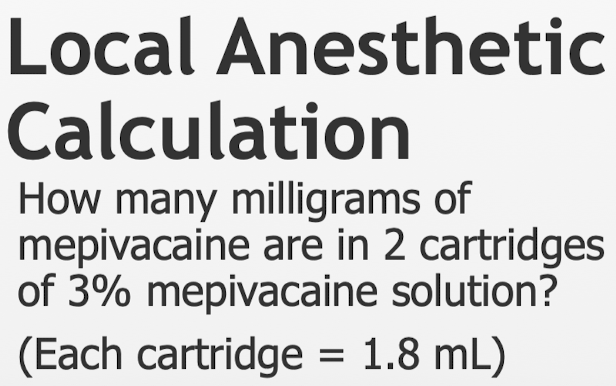
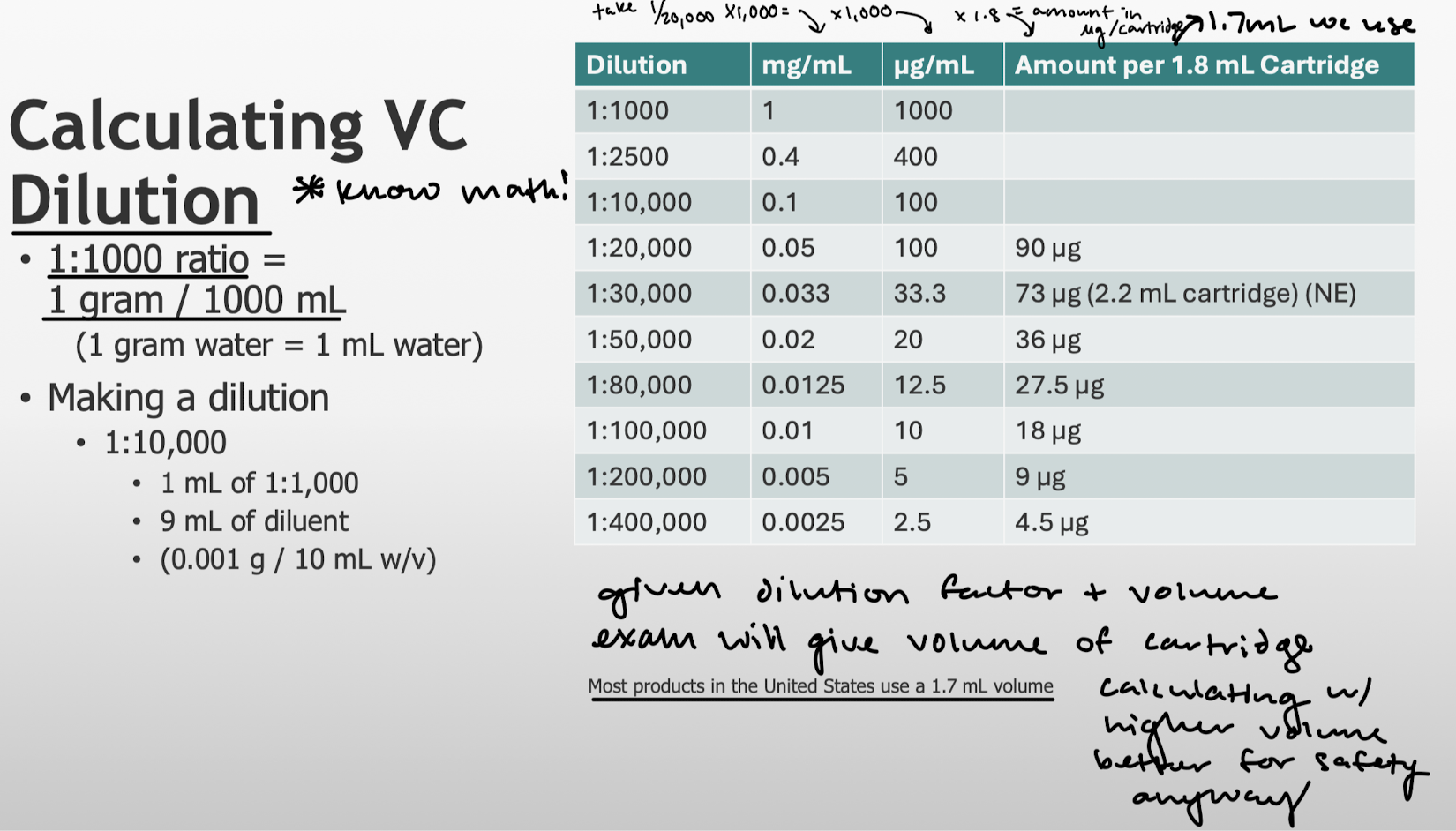
How to calculate for dilution? What is the volume of a cartridge in the US versus elsewhere?
1:1000 ratio = 1 gram/1000 mL
What is the mechanism of action of epinephrine? What are the CV and respiratory effects?
Non-selective adrenergic agonist

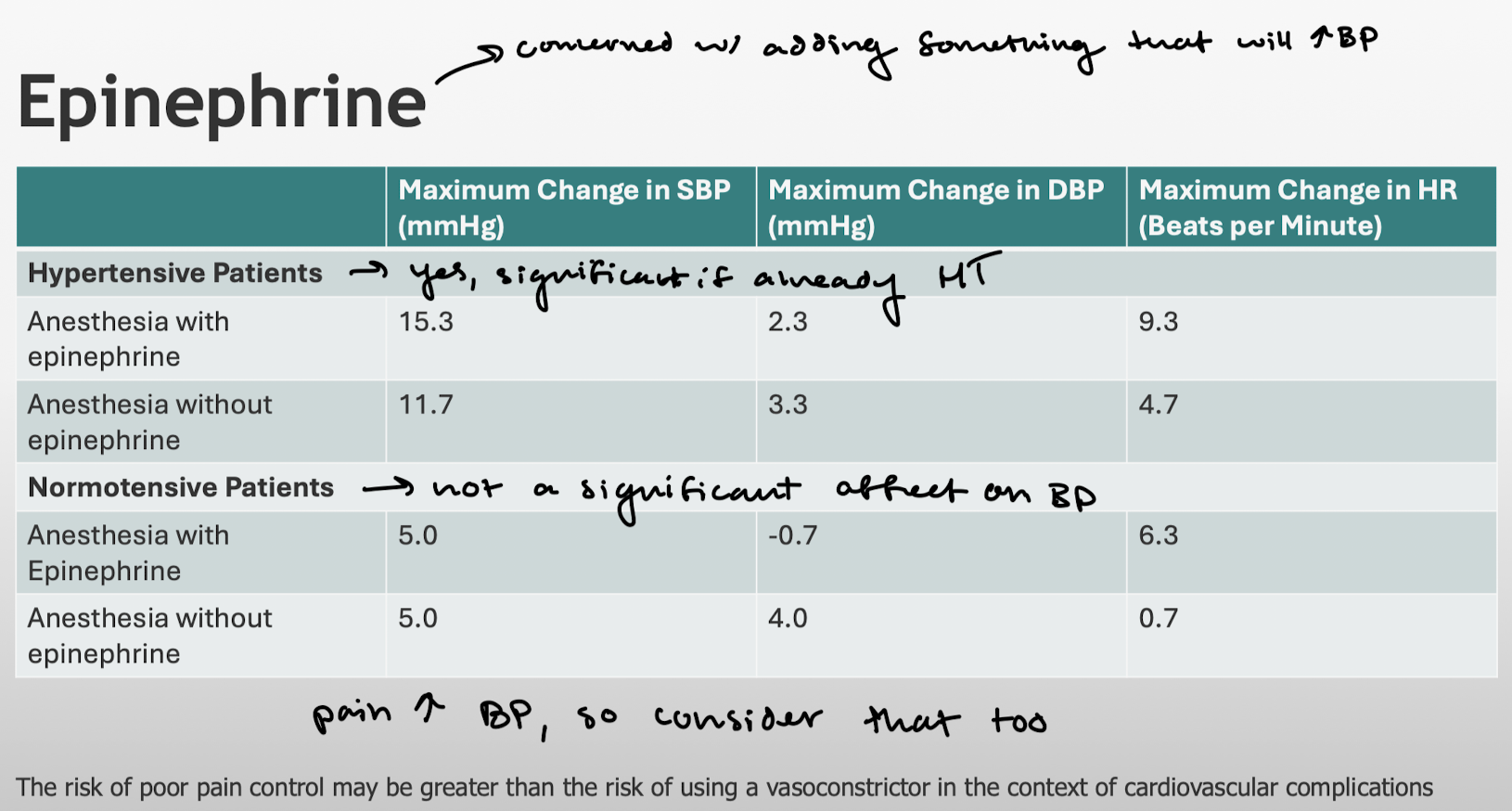
What patients may you be concerned to give a lot of epinephrine?
Hypertensive pts because LA will increase BP. Keep in mind that pain will also increase BP though!!!
What is the general rule about max doses of epinephrine? What are the maximum recommended doses in dentistry for healthy adults and for those with CVD?
Healthy Adult: 0.2 mg
CVD (ASA 3-4): 0.04 mg

What are the effects of epinephrine on cardiac stimulation? What are the signs and symptoms?

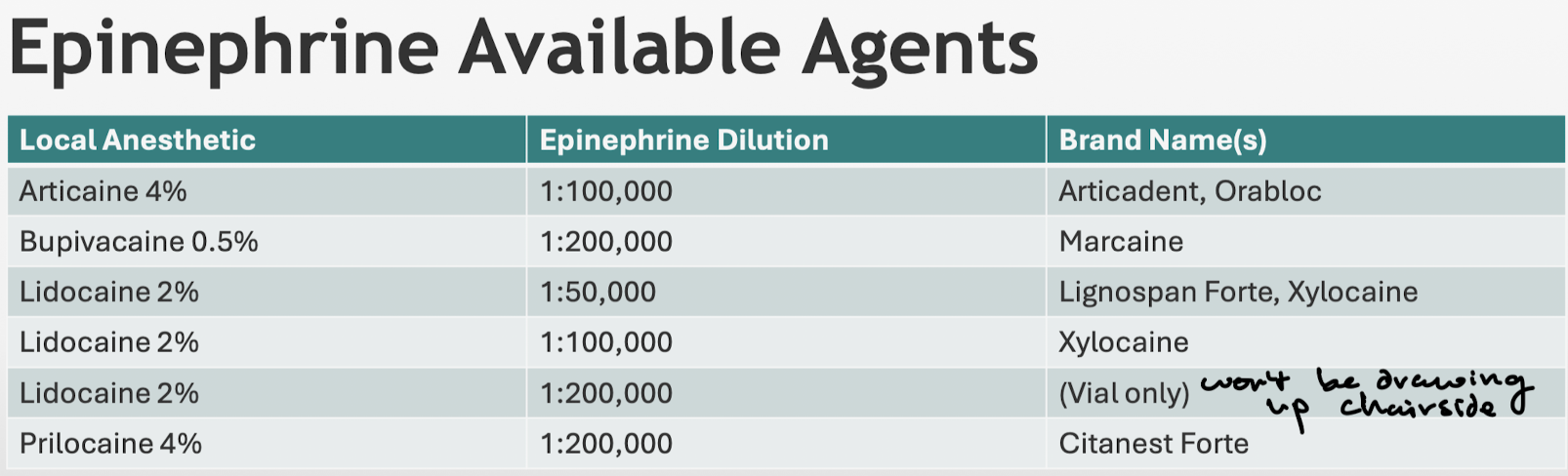
Recognize the epinephrine available agents:
What is the main advantage of Levonordefrin compared to epinephrine?
Less CV concern compared to epinephrine because only 15% of potency

What are the maximum doses of levonordefrin? How is it supplied? Is it currently available?

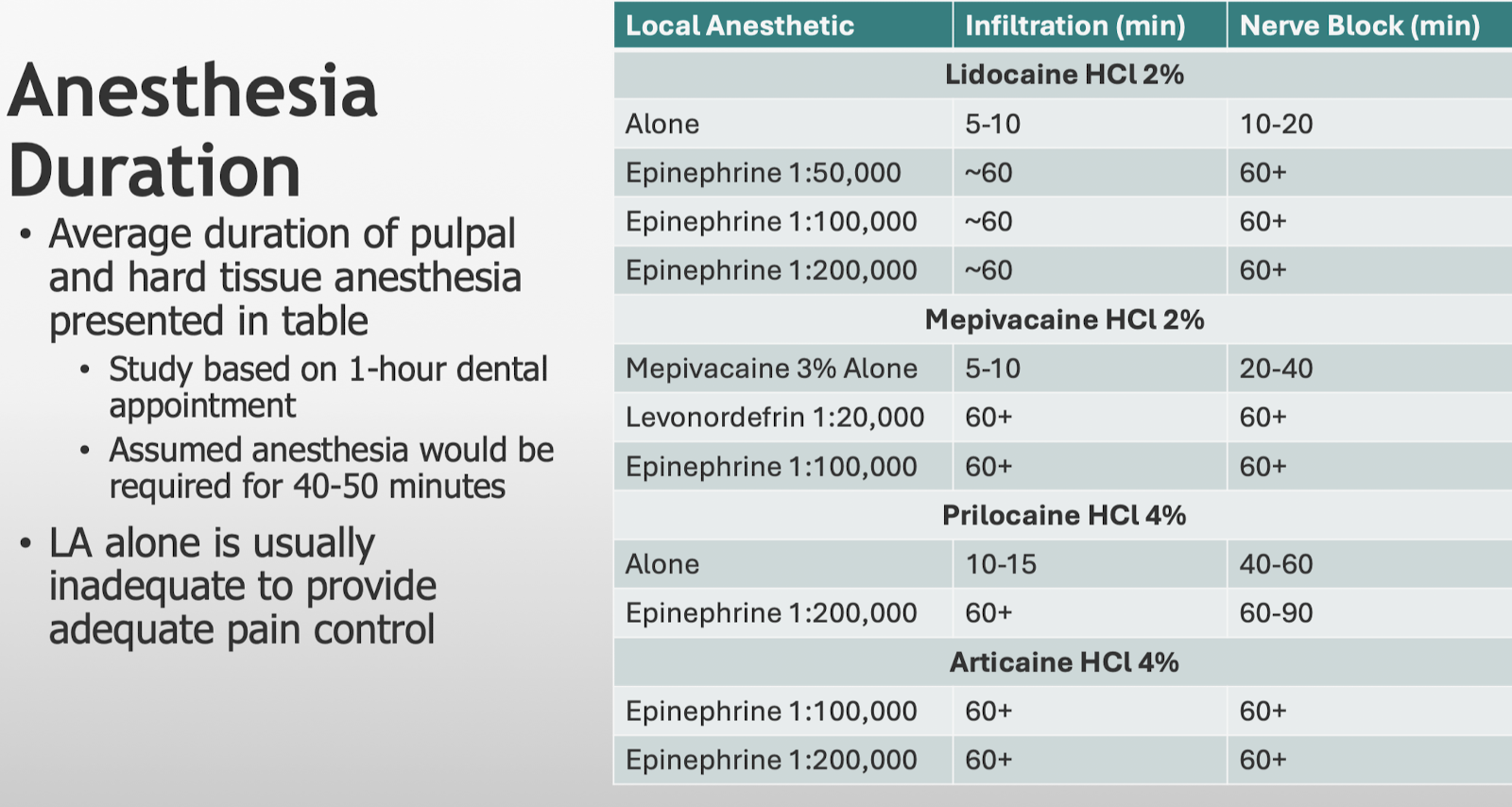
What are the effects of epinephrine on anesthesia duration? What is the main takeaway from this information?
LA alone is usually inadequate to provide adequate pain control!
What are the vasoconstrictor contraindications?
Drug

In what setting should you use a risk vs benefit analysis when deciding to use a vasoconstrictor?

Typically, if medical condition is under control and no drug interactions, a vasoconstrictor may be used. What should you still ensure?

Epinephrine allergies
Typically sodium bisulfite or metabisulfite used as an antioxidant to stabilize the VC can trigger an allergic reaction in sulfite-sensitive patients, but this is not really an allergy to epinephrine.

What are the limitations of epinephrine? (5)

Know the commercially available dental cartridges
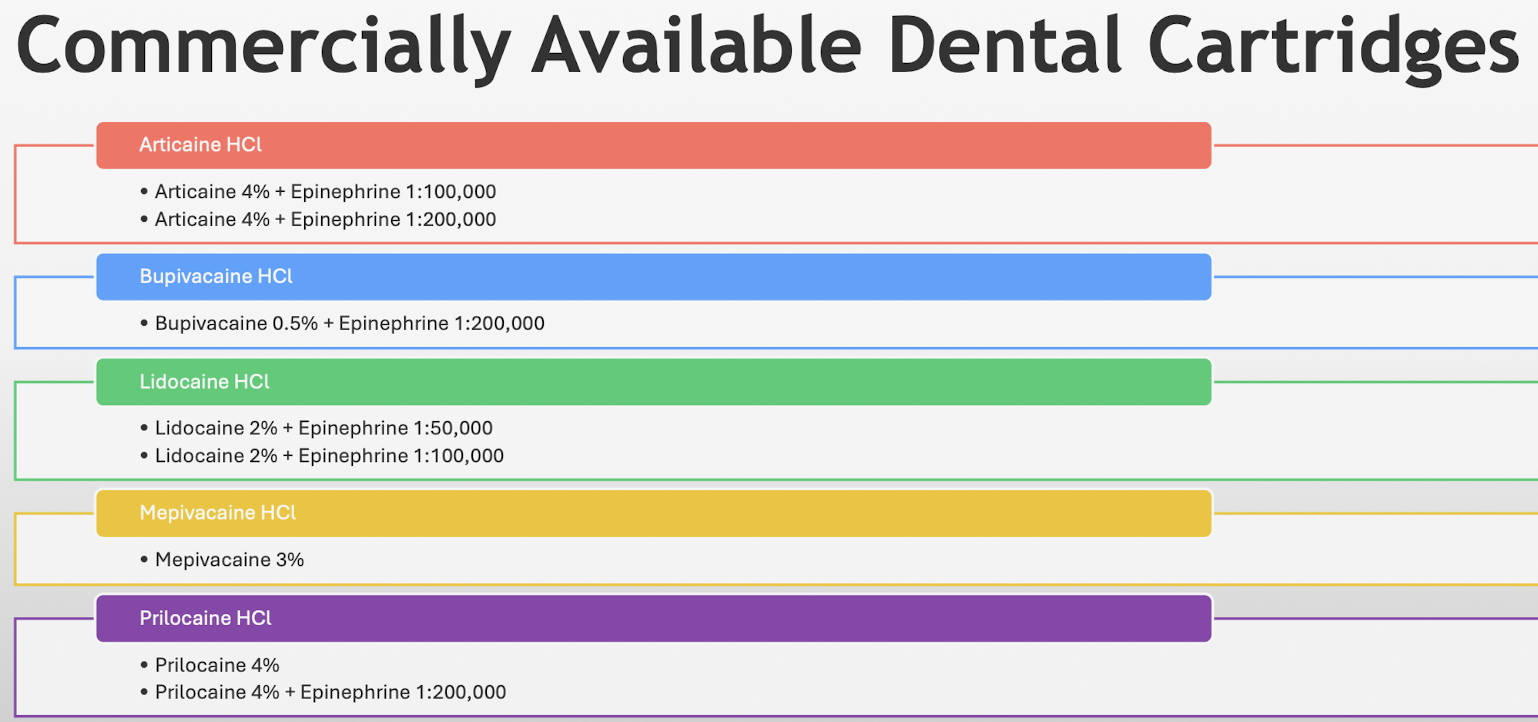
Articaine: classify (ester or amide), pregnancy category, pediatric safety, half-life, max dose

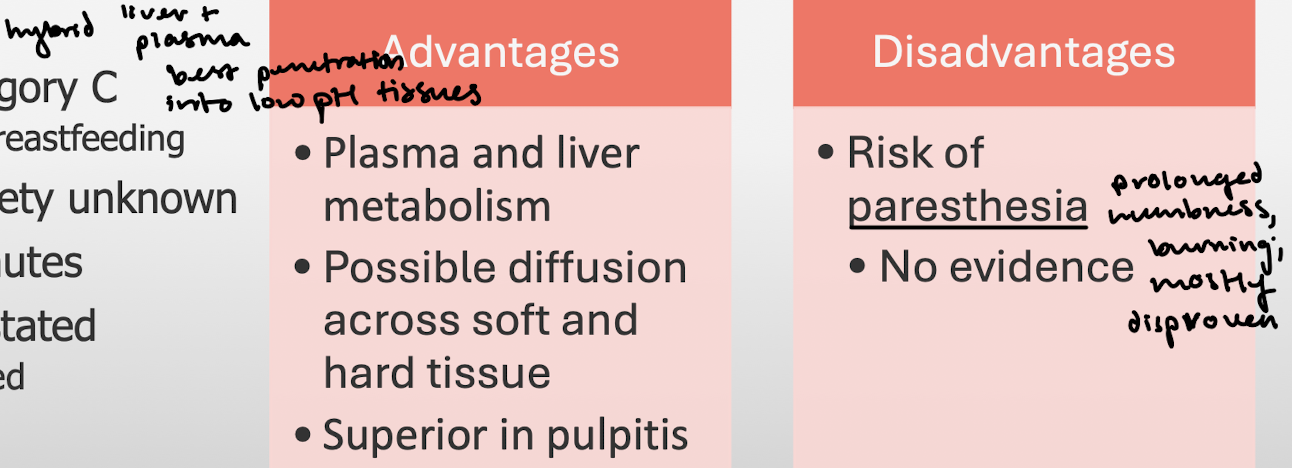
Articaine: Main advantages and disadvantages
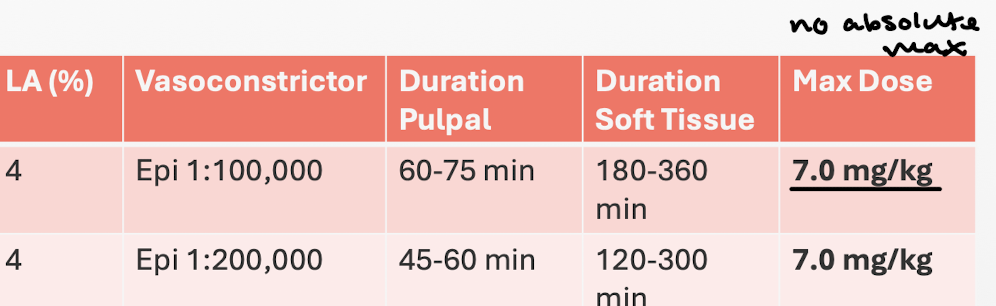
Articain: %s, dilations of VC, pulpal duration, soft tissue duration, max dose
Bupivacaine: category, pregnancy category, peds, half-life, absolute max dose.

Bupivacaine: %s, VC dilution, pulpal duration, soft tissue duration, max dose

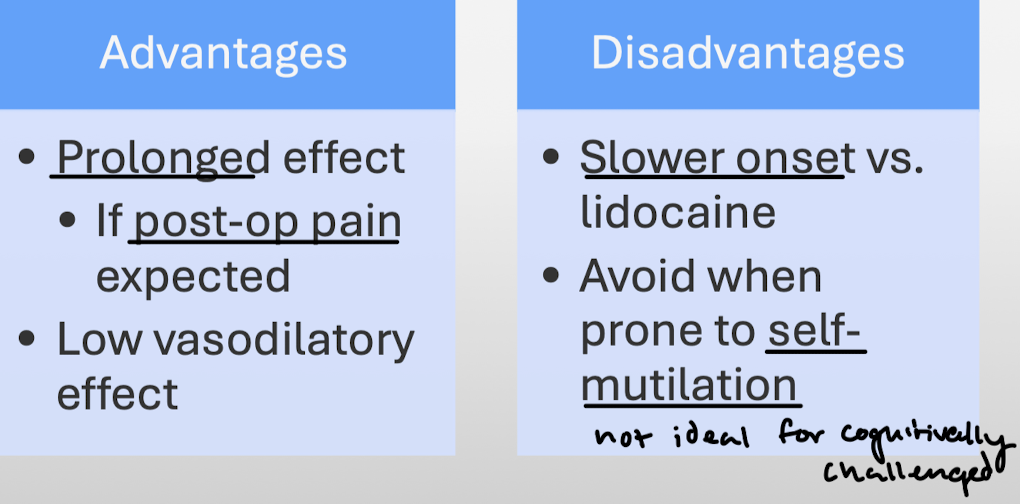
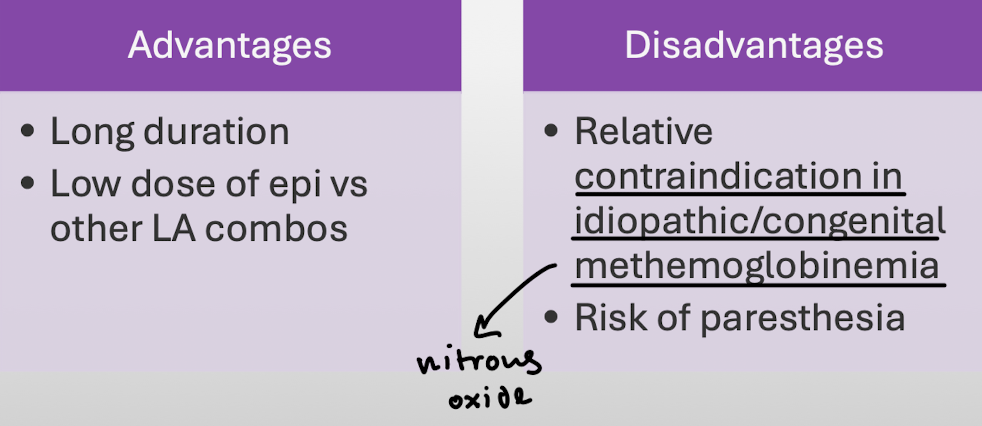
Bupivacaine: main advantages and disadvantages
Lidocaine: classification, pregnancy category, peds, half-life, absolute max dose

Lidocaine: LA %, VC dilution, pulpal duration, soft tissue duration, max dose
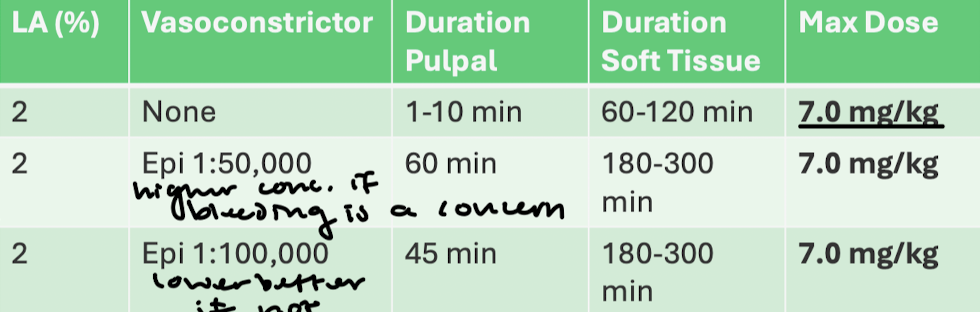
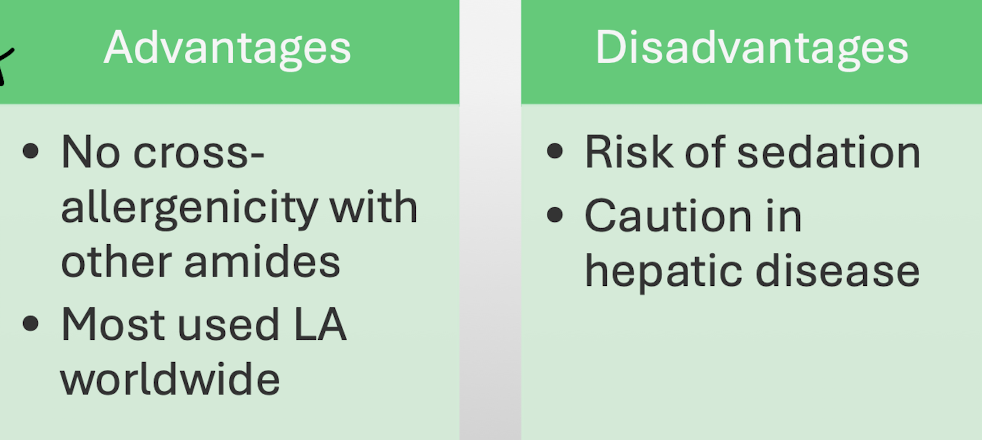
Lidocaine: advantages and disadvantages

What are the different lidocaine dosages? Which is common for perio? Which are topical?

Mepivacaine: category, pregnancy category, pediatric, half-life, absolute max dose.

Mepivacaine: LA, VC dilution, pulpal duration, soft tissue duration, max dose.
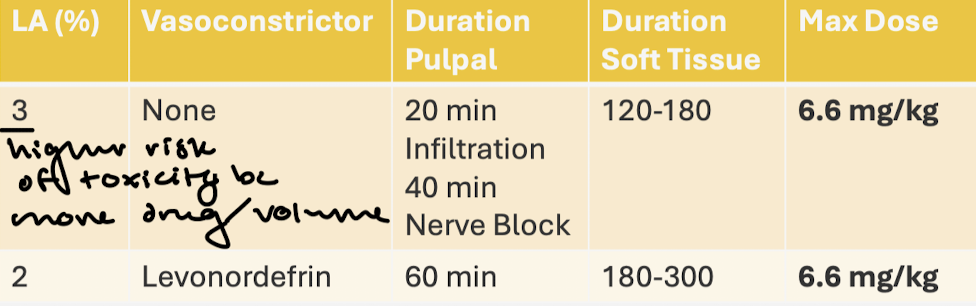
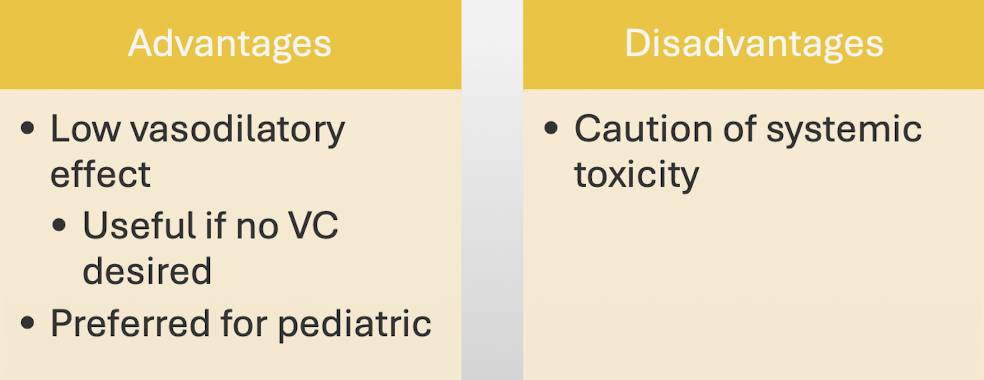
Mepivacaine: advantages and disadvantages:
Prilocaine: category, pregnancy category, peds, half-life, max dose

Prilocaine: LA %, VC dilution, pulpal duration, soft tissue duration, max dose
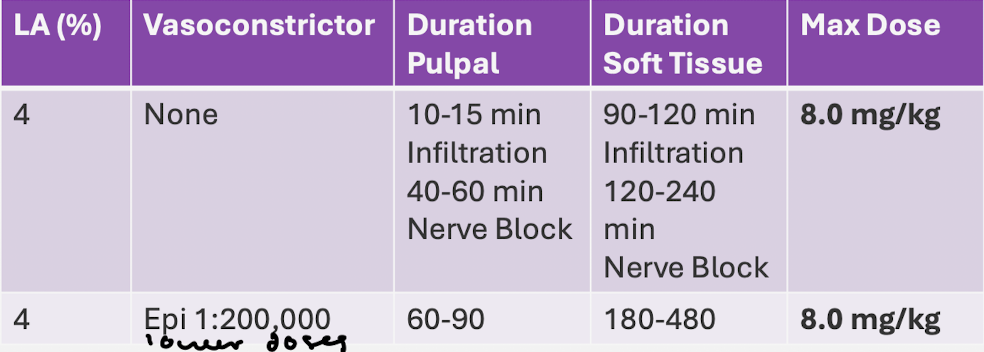
Prilocaine: advantages and disadvantages
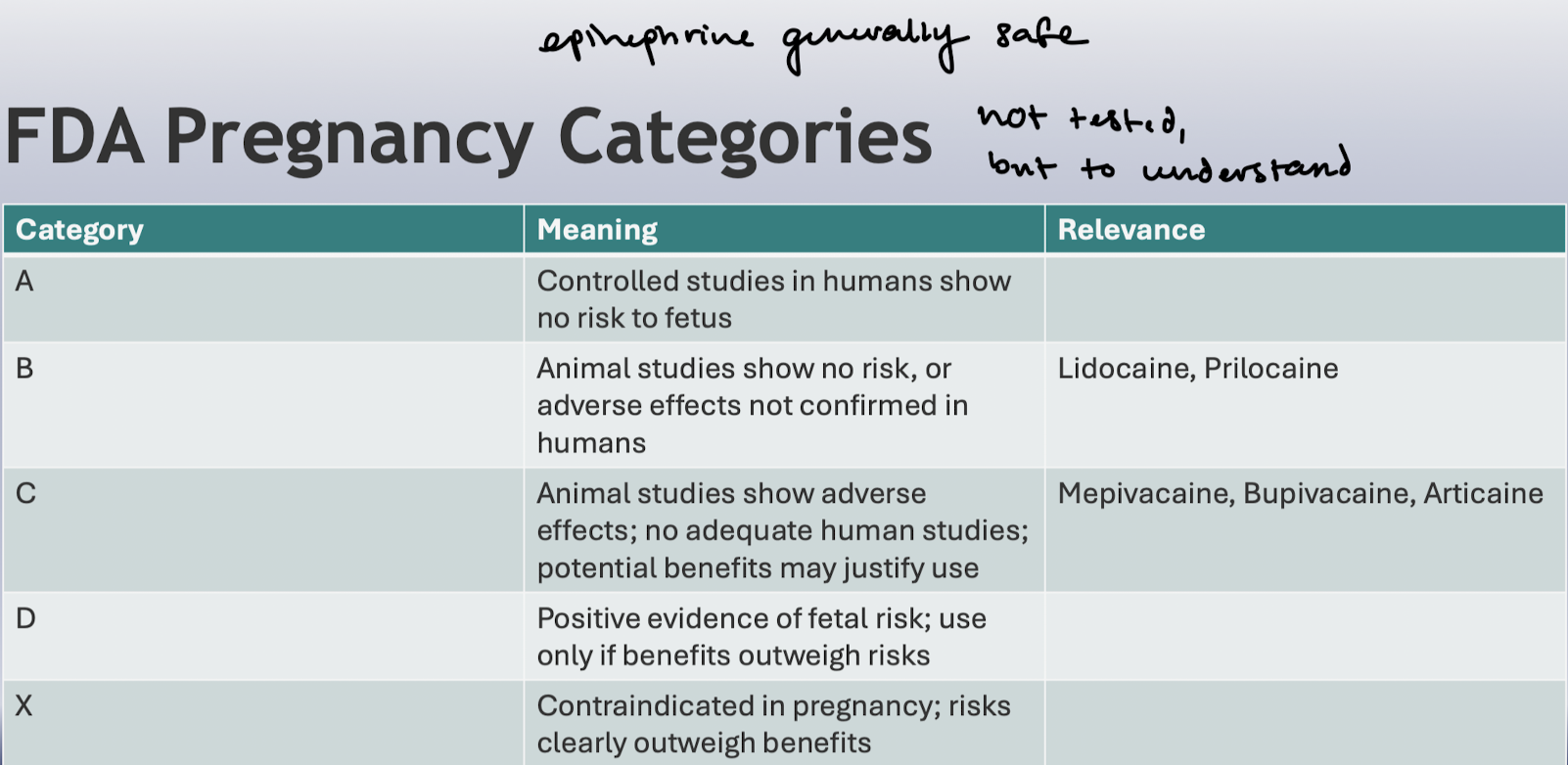
Know which LAs are what pregnancy category
What is OraVerse (Phentolamine Mesylate)? What is the mechanism?
Non-selective alpha-adrenergic antagonist

What is the mechanism of action and efficacy of OraVerse (phentolamine mesylate). For who might this be indicated?

What is the pregnancy category for OraVerse? What children can use OraVerse?

What are the main topical anesthetics? Who might you use a topical anesthetic for?


Dental cartridges volume