Visual problems
1/49
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
50 Terms
Normal IOP =
10-21 mm Hg
Group of disorders characterized by increased IOP and subsequent optic nerve atrophy. Tissue damage starts in the periphery, causing peripheral vision loss
Incidence increases with age; unaware
Early detection and tx important to prevent blindness
Glaucoma
Most common type of glaucoma
The outflow of aqueous humor is decreased in the trabecular meshwork
The drainage channels become clogged
Damage to the optic nerve results
POAG
Pathophysiology of glaucoma
Aqueous production (inflow) and aqueous reabsorption (outflow) must be balanced to maintain IOP
Outflow occurs at angle where iris meets cornea
Inflow > outflow → increased IOP
Increased IOP → permanent loss of vision
Outflow of aqueous decreased; drainage channels clogged → optic nerve damage
Primary open-angle glaucoma (POAG)
Reduced outflow from angle closure
Angle-closure glaucoma (ACG)
Clinical manifestations of POAG
Initially asymptomatic (develops slowly w/o sx of pain or pressure)
Gradual loss of peripheral vision (visual field loss may not be noticeable until severe peripheral vision loss
Late or untreated: tunnel vision
Clinical manifestations of AACG
Severe, sudden pain in or around eye
NV
Colored halos around lights
Blurred vision
Ocular redness (may be mistaken for eye infection)
A reduction in the outflow of aqueous humor that results from angle closure
Caused by the lens bulging forward (can occur because of the aging process)
May occur because of pupil dilation in the patient with anatomically narrow angles
PACG
Acute attack of PACG may be precipitated by:
Prolonged pupil dilation, causing increase in IOP
Drug-induced mydriasis (ophthalmic and systemic medications)
Emotional excitement
Darkness
What can cause prolonged pupil dilation and increase IOP, resulting in an acute PACG attack?
Drug-induced mydriasis (ophthalmic and systemic medications)
Emotional excitement
Darkness
Check before administering drugs that may cause pupil dilation
POAG IOP →
22-32 mm Hg
AACG →
IOP > 50 mm Hg
Diagnostic studies for glaucoma
IOP measurement
POAG—IOP 22 to 32 mm Hg
AACG —IOP > 50 mm Hg
Slit lamp microscopy
Visual acuity measurements
Ophthalmoscope: optic disc cupping
Diagnostic studies for retinal detachment
Visual acuity measurements
ophthalmoscope or slit lamp examination
US
Health promotion for glaucoma:
Early detection and treatment
Eye examination: Age 40 to 64 every 2 to 4 years
Age 65+ every 1 to 2 years
Blacks—more frequent → ↑ incidence
Postoperative considerations for retinal detachment
Bedrest/Activity restrictions
Medications: analgesia and topical
Patient education
A clouding or opacity within the lens of the eye that distorts the images projected on the retina causing blurred vision.
Cataract
What is the pathophysiology of cataracts?
Caused by an abnormal metabolic process within the lens Water and protein accumulate in the lens fiber structure. This affects lens transparency and vision
What are risk factors for cataracts?
Advanced age
Eye trauma
Congenital infection (i.e., maternal rubella)
Radiation or UV light exposure (Sun is bad!)
Long-term corticosteroid use
Ocular inflammation
What are clinical manifestations of cataracts?
Decreased vision
Abnormal color perception
Glare, especially at night
No pain or eye redness is associated with age-related cataract formation
No pain or eye redness is associated with age-related cataract formation. True or false?
True
Interprofessional care for age-related macular degeneration:
Medications injected every 4 to 6 weeks into vitreous cavity to stop new vessel formation and slow vision loss
Photodynamic therapy (PDT) uses dye and laser to damage abnormal blood vessels
Patients must avoid sunlight and intense light for 5 days
Nutrition: vitamin C and E; beta-carotene, zinc, lutein
Smoking cessation
What is nursing education for PDT to treat age-related macular degeneration?
Patients must avoid sunlight and intense light for 5 days
What does dietary management of age-related macular degeneration involve?
Vitamin C and E; beta-carotene, zinc, lutein
Smoking cessation
Diagnosis of cataracts =
Ophthalmoscope or slit lamp examinatio
Health promotion for cataracts:
No specific preventative measures
Wear sunglasses, avoid unnecessary radiation
Antioxidant vitamins (C and E); adequate nutrition
Intraoperative care for cataracts
Decrease lighting for photophobia
Administer abx and corticosteroids
Post-op care for cataracts
Mild analgesia, monitor for complications, understand and adhere to therapy, physical and emotional comfort.
Postoperative phase for cataract care:
Discharged after sedation wears off
Post-op medications: abx and corticosteroids drops
Activity restrictions: avoid IOP such as bending, stooping, coughing, or lifting
Nighttime shielding
Follow-up for visual acuity; may or may not need glasses/lenses
Surgical therapy for cataracts in preoperative phase:
Give anti-inflammatory and pupillary dilating drops
Mydriatic = alpha-adrenergic agonist → dilation
Cycloplegic = Anticholinergic—paralysis of accommodation and dilation
Drug Alert: Patients wear dark glasses to reduce photophobia; monitor for systemic toxicity (tachycardia and CNS effects)
Surgical therapy for cataracts in intraoperative phase:
Phacoemulsification—ultrasonic vibrations dissolve lens ; fragments are removed
Extracapsular cataract extraction procedure—remove lens in one piece; requires sutures
Intraocular lens (IOL) implantation
Administration of abx and corticosteroids
Nonsurgical therapy for cataracts
Is only temporary (need surgery to treat)
prescription eyewear; visual aids; increased light; change lifestyle
A deterioration of the macula (area of central vision) and is related to retinal aging. It is the most common cause of irreversible central vision loss in people over the age of 60.
Macular cells start to atrophy, leading to a slow, progressive, and painless vision loss
Age-related Macular Degeneration
Predisposing factors to AMD
Smoking
HTN
Caucasian ethnicity
Family hx of AMD
Chronic inflammatory conditions
What are clinical manifestations of AMD?
Blurred and darkened vision
*Decline in central vision
*Blind spots in the visual field (scotomas)
*Distortion of vision (metamorphopsia)
Acute vision loss (wet AMD)
Nonexudative
Atrophy of macular cells
More common
Slow, progressive, painless vision loss
Dry AMD
Exudative
More severe; abnormal blood vessels develop in or near macula
Rapid onset of vision loss; AMD related blindness
Wet AMD
Diagnostic studies for AMD
Visal acuity measurements;
Ophthalmoscopy
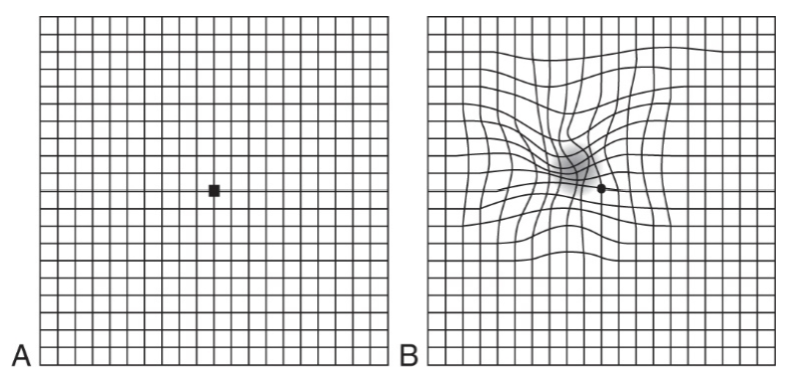
Amsler grid test
*Sudden, excruciating pain in or around the eye
*NV
*Halos around lights
Blurred vision
Ocular redness that may be mistaken for an eye infection
These are clinical manifestations of what condition?
AACG
Appears gradually
Hx of *halos around lights, blurred vision and ocular redness, or eye/brow pain
PACG (gradual)
Surgical therapy for retinal detachment:
Surgical therapy—seal retinal breaks
by inflammation/adhesion or scar
Laser photocoagulation—inflammation
蚠 Cryopexy—freezing scar
蚠 Scleral Buckling—band placed around globe (Fig. 22-
14
What are post-op considerations for surgery of retinal detachment
Bedrest/Activity restrictions
Medications: analgesia and topical
Patient education
What are clinical manifestations of retinal detachment?
Photopsia (light flashes)
Floaters, and cobweb/hairnet or ring in field of vision
Curtains closing slowly
Separation of retina and underlying epithelium; fluid accumulation between layers
Etiology: Breaks—holes (spontaneous) or tears (aging)
Retinal detachment
Photopsia (light flashes)
Floaters, and cobweb/hairnet or ring in field of vision
Curtains closing slowly
These are clinical manifestations of what condition?
Retinal detachment
Intraocular procedures for retinal detachment?
Pneumatic retinopexy—intravitreal injection of gas to form bubble to close retinal break
Vitrectomy—removal of vitreous
Initially asymptomatic (develops slowly w/o sx of pain or pressure)
Gradual loss of peripheral vision (visual field loss may not be noticeable until severe peripheral vision loss
Late or untreated: tunnel vision
These are clinical manifestations of what condition?
POAG
Blurred and darkened vision
*Decline in central vision
*Blind spots in the visual field (scotomas)
*Distortion of vision (metamorphopsia)
Acute vision loss (wet)
These are clinical manifestations of what condition?
AMD
Decreased vision
Abnormal color perception
Glare, especially at night
No pain or eye redness is associated with age-related cataract formation
These are clinical manifestations of what condition?
Cataracts