L14 Communicable disease control in HK
1/36
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
37 Terms
What are the elements in epidemiology triangle ? Suggest examples
Host
Humans
Environment
Temperature, humidity, altitude, housing, water, pollution…
Agent
bacteria, viruses, fire, radiation, trauma, poison, alcohol…
Break one side of the triangle or remove an element can stop the disease transmission
What are the 4 main categories of infectious agents ? Which one is the weakest ?
bacteria, fungi, parasites, and viruses.
In terms of infectivity, fungi is the weakest
everyone have many on the skin, only immunocompromised individuals will be affected by fungi
What are the possible host factors leading to communicable disease transmission
Age
Heredity
Resistance to infection
Host resistance
Immunity
Herd immunity
Infectiousness of the host
Explain what is active immunity
Protection produced by person’s own immune system.
Can result from having the disease or from vaccinations.
Long-lasting and usually gives life-time immunity
Explain what is passive immunity
Acquired naturally or artificially
Usually short-lived and often used as stop-gap measure 臨時措施
e.g. IgG, maternal antibodies
Explain what is herd immunity
If number of immune people is high enough, it is unlikely that a susceptible person will have contact with an infected person, the population is said to have “herd immunity”.
enough people are immunized, protecting most in the community
Even though there are some susceptible persons in the population, epidemics are not sustained because between infected persons and susceptible persons is minimal.
Level of immunity required in population to attain herd immunity is dependent on characteristics of disease & how readily a disease spreads.
What means by infectiousness
A measure of the potential ability of an infected host to transmit the infection to other hosts.
Which types of influenza usually responsible for pandemics and annual outbreaks + further explain the time course of the outbreak
Influenza A
(The only one that will cause pandemic, outbreak)
outbreaks typically begin abruptly, peak over a 2-to-3-week period, last for two to three months
Describe the earliest indication of influenza A outbreak in the community
an increase in febrile respiratory illnesses in children
followed by increases in influenza-like illnesses in adults
Attack rates of 10 to 20% in the general population and 50% in pandemics
Which types of influenza is more stable and causes outbreaks every 2-4 years.
Influenza B
Which types of influenza is poorly understood and usually associated with sporadic 零星的 and subclinical infection.
Influenza C
What is the most common s/s of influenza for children ?
fever
What is the most common s/s of influenza for adults ?
cough (non-productive)
fever
What is the most common s/s of influenza for elderly ?
cough (non-productive)
malaise
Explain the major complication of influenza
Primary influenza Pneumonia
Occurs when influenza virus infection directly involves the lung
Not common, but very severe
s/s: bilateral reticular or reticulonodular opacities with or without superimposed 疊加的 consolidation
Secondary influenza Pneumonia
An important complication of influenza &
Contributes to approximately 25% of all influenza-associated deaths
s/s: exacerbation of fever and respiratory symptoms after initial improvement in the symptoms of acute influenza
Influenza virus leads to a decrease in the size of the tracheobronchial epithelium cells and loss of cilia
What is the difference between influenza and common cold
Influenza is not caused by the same virus that causes the common cold
Influenza is not just bad cold
Influenza is a much more severe disease
Describe the transmission of influenza
Via large particle droplets after close contact with an infected individual
large particles do not maintain suspended in the air and travel only short distances (~6 feet)
How long should the infection-control precautions after influenza infection should last for ?
The length of time for which infection-control precautions are required varies with the kind of infection and age of the patient
For adults and adolescents: precautions should last 5 days after symptoms have started
For infants and children aged 12 years or younger: precautions should last 7 days from the onset of symptoms
What is viral shedding ?
viral shedding (spreading, infectivity) of influenza can be detected 24 to 48 hours before illness (s/s onset)
Shedding of influenza virus peaked on the 2nd day, and then rapidly declined
Shedding ceased after six or seven days
for Avian influenza, may shed virus from their respiratory tracts for up to 2–3 weeks
Longer periods of shedding can occur in children, elderly adults, patients with chronic illnesses, and immuno-compromised hosts
infants can shed seasonal influenza viruses for up to 21 days
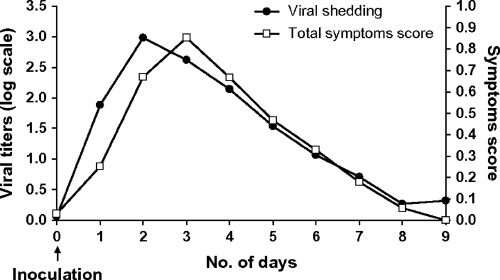
How can duration of shedding be controlled ?
Individuals who received antiviral drug (oseltamivir/Tamiflu) by symptom day had an accelerated decrease in viral RNA concentration and clearance by one week
Suggest 3 classification of influenza
Seasonal influenza
winter surge, summer surge
totally different from Avian influenza & influenza pandemic
Pandemic influenza
Avian influenza (animal)
When does seasonal influenza outbreaks usually occurs ?
Occurs in distinct outbreaks of varying extent every year, 2 seasonal flu in HK (summer and winter surge)
The viruses that cause influenza are constantly changing and people are not always immune to new variants of the virus.
These variants may then cause epidemics
More common in winter
Illnesses resembling influenza that occur in the summer are usually due to other viruses
What is the difference between winter and summer surge of seasonal influenza ? (Characteristics of seasonality of influenza outbreaks)
January to March (WINTER SURGE) – enchanted virus’s stability and indoor crowding
common in northern hemispheres, e.g. HK
July to August. (SUMMER SURGE) – hot and humid enhances influenzas A activity.
common in southern hemispheres, e.g. Australia
In tropical regions, e.g. Malaysia, Brazil, Thailand, Philippines... influenza may occur throughout the year in the tropics
Define what is influenza pandemic (3)
Occurs roughly every 10 – 50 years and may strike anytime.
Caused by emergence and global spread of a novel influenza virus originated from an animal influenza virus e.g., avian influenza virus,
undergoing major genetic changes resulting in efficient human-to- human transmission.
human population has low or no immunity against the emerging pandemic influenza virus, that’s why higher severity of illness
Improved medical care can reduce the dramatic increases in the proportion of young people affected in subsequent pandemics
Suggest an example of influenza pandemics in HK at 1968-1969
H3N2
Moderate severity of pandemic
death toll 1 million
List 3 pandemic prevention strategies
Reducing contact rates in the population through social distance measures.
Reducing the infectiousness of infected individuals through treatment or isolation.
Reducing the susceptibility of uninfected individuals by vaccination or antiviral prophylaxis.
What are the 6 criteria for the success of pandemic containment 遏制
Rapid identification of original case cluster.
Rapid case detection and delivery of treatment to targeted groups (within 48 hours).
Effective delivery of treatment to high proportion of targeted population (>90%).
Sufficient stockpiles 庫存 of drugs, E.g. 3 million or more courses of Tamiflu.
Population cooperation with the containment strategy by social distance measures.
International cooperation in epidemic surveillance and control strategy implementation.
What is avian influenza, suggest an example
Mainly affect birds and poultry, such as chickens or ducks or turkeys
does not commonly infect human (ie. little or no immune protection against them in the human population)
EXAMPLE: H5N1
Highly contagious among birds
Less Human to human
How will people become infected with avian influenza ?
direct contact with infected birds and poultry 家禽 (live or dead),
their droppings or contaminated environments.
Broken contaminated eggs may infect chicks in the incubator
What is the seriousness difference between H1N1 and H5N1 ?
H1N1: 豬流感 Easily spread, rarely fatal
H5N1: 禽流感 Spreads slowly, often fatal
What are the measures for avian influenza infection
Do not require hospitalization
Cohort yourself is okay, hand-washing, respiratory hygiene (mask)
Explain the difference between genetic reassortment of virus, Antigenic shift and drift
Antigenic Shift | Antigenic Drift |
Gradual change | Sudden change, explosive spread |
Point mutation (minor change) in H and N viral protein | Occurs through ressortment of genes (between human and animal reservoirs): result in emergence of pandemic strains |
Occurs in A, B, C viruses | Occurs ONLY in influenza A viruses |
Explain H1N1
A subtype of influenza A virus
One of the seasonal influenza strains in Hong Kong (complete dominant type)
Most common cause of human influenza (flu) in 2009 (豬流感, swine flu pandemic)
Also high level of disease in winter months, unusual in the summer
How was influenza vaccine made ? (the ingredients)
Is made from highly purified, egg-grown viruses that have been inactivated.
should not be administered to persons with a known history of anaphylactic hypersensitivity to eggs
Also have live intranasal influenza vaccine version, nasal spray
Strain composition similar to inactivated vaccine
Flexible administration
What is trivalent influenza vaccine ?
Two influenza "A" viruses and one influenza "B" virus are selected
WHO provides a recommendation on the strains to be included in the influenza vaccine for the northern hemisphere every year
(p.65-66 supp exam ?)
Explain the effectiveness of influenza vaccine (5)
Vaccine effectiveness depends on the similarity between vaccine strains and the strains in circulation during influenza season
With a good "match" influenza immunization prevents disease in 70 to 90% of healthy individuals
This drops to 30 to 40% in the frail and elderly
It does, however, prevent death in 85% of the frail and elderly
It prevents hospitalization in 50 to 60% of individuals immunized
Even with an imperfect match, Canadian studies show the vaccine still reduces the overall risk of infection by about 40-60%
A vaccine that is not perfectly matched can still offer
What are the possible side effects of the inactivated seasonal influenza vaccine ?
Usually well tolerated apart from occasional soreness, redness or swelling at the injection site
Some recipients may experience fever, muscle pain and tiredness beginning 6 to 12 hours after vaccination and lasting up to two days
Immediate severe allergic reactions like hives 麻疹, swelling of the lips or tongue, and difficulties in breathing are rare and require emergency consultation.
Influenza vaccination may be rarely followed by serious adverse events such as
Guillain-Barré syndrome (1 to 2 cases per million vaccinees),
meningitis or encephalopathy (1 in 3 million doses distributed) and
severe allergic reaction (anaphylaxis) (9 in 10 million doses distributed).
However, influenza vaccination may not necessarily have causal relations with these adverse events.