Health Psych Exam 3
1/90
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
91 Terms
What is the core premise of the Diathesis-Stress Model?
Psychological disorders develop from a combination of long-term vulnerability (diathesis) and immediate triggers (stress).
What are three common predisposing factors (diathesis) in the Diathesis-Stress Model?
Genetics, personality, and early life experiences.
What are three common precipitating factors (stress) in the Diathesis-Stress Model?
Trauma, life events, and acute stress.
According to the Diathesis-Stress Model, when does a disorder actually manifest?
When the combination of vulnerability and stress crosses a specific threshold.
How does chronic stress contribute to weight gain?
Stress increases cortisol, which boosts appetite, triggers cravings for high-fat/sugar foods, and promotes abdominal fat storage.
Why does the body promote fat storage during chronic stress?
The body perceives stress as a survival threat and attempts to store energy for future use.
What are the three stages of General Adaptation Syndrome (GAS)?
1. Alarm stage, 2. Resistance stage, 3. Exhaustion stage.
What occurs during the Alarm stage of GAS?
The fight-or-flight response is activated and adrenaline levels increase.
What characterizes the Resistance stage of GAS?
The body attempts to adapt to the stressor while cortisol levels remain elevated.
What happens during the Exhaustion stage of GAS?
The body's resources are depleted, leading to an increased risk of illness.
What does the SAM system stand for and what is its primary function?
Sympathetic-Adreno-Medullary system; it handles the immediate, short-term stress response.
What hormones are released by the SAM system?
Adrenaline and norepinephrine.
What does the HPA axis stand for and what is its primary function?
Hypothalamic-Pituitary-Adrenal axis; it handles the longer-lasting stress response.
What hormone is primarily released by the HPA axis?
Cortisol.
What is the key difference between the SAM system and the HPA axis?
The SAM system provides a fast, short-term response, while the HPA axis provides a slow, long-term response.
What is the 'freeze response' in the context of stress?
A state where the body becomes immobile or unable to act in response to a perceived threat.
Which individuals are more likely to experience the freeze response?
People with high trauma exposure, chronic stress, or anxiety/PTSD.
What is 'allostatic load'?
The cumulative 'wear and tear' on the body resulting from chronic stress.
What are the long-term health effects of high allostatic load?
A weakened immune system, increased disease risk, and various mental and physical health problems.
Approach Coping
Directly tackles the problem head on
Avoidant Coping
Avoids dealing with the problem
Problem-Focused Coping
Focus on fixing the problem itself
Emotion-Focused Coping
Focus on managing emotions
Relationship-Focused Coping
Focus on maintaining relationships
Instrumental Support
Tangible help
Informational Support
Advice or guidance
Emotional Support
Comfort and care
Mindfulness
Being present in the moment and aware of thoughts/emotions without judgment
Relaxation Response
Body's calm, opposite response to stress
How to activate the Relaxation Response
Meditation, Deep breathing, Visualization
BIG IDEA of the Relaxation Response
Reduces stress by calming the body and lowering physiological arousal
Social Determinants of Health
Conditions in which people are born, live, work, and age that impact health
Economic Stability
Income, employment, financial security
Education Access & Quality
Schooling, literacy, education level
Healthcare Access & Quality
Insurance, access to providers, quality care
Neighborhood & Built Environment
Housing, safety, environment, transportation
Social & Community Context
Relationships, support systems, discrimination
Justice as Fairness (Rawls)
Society should be structured to ensure fairness
Rawls' Key Ideas
Equal basic rights (freedom, participation), Equal opportunity for all, Inequalities are only okay if they benefit the least advantaged
Daniels (applies Rawls to health)
Health is necessary for equal opportunity
Daniels' Key Takeaways
Society must provide: Access to healthcare, Resources like education & childcare; Focus should NOT just be profit → should reduce health inequalities
Whitehall I (1978)
British civil servants (all employed, not poor); Lower job status = higher death rates
Whitehall II
Same results (even with women included)
Whitehall Main Finding
Health follows a social gradient; Lower status = worse health; NOT just income → position in hierarchy matters most
CARDIA (U.S. study)
Looked at race + socioeconomic status
CARDIA Main Findings
Lower social status = Worse self-rated health, Higher depression, Higher hypertension (most groups)
CARDIA Trend
Effects weaker in some groups, but trend still exists
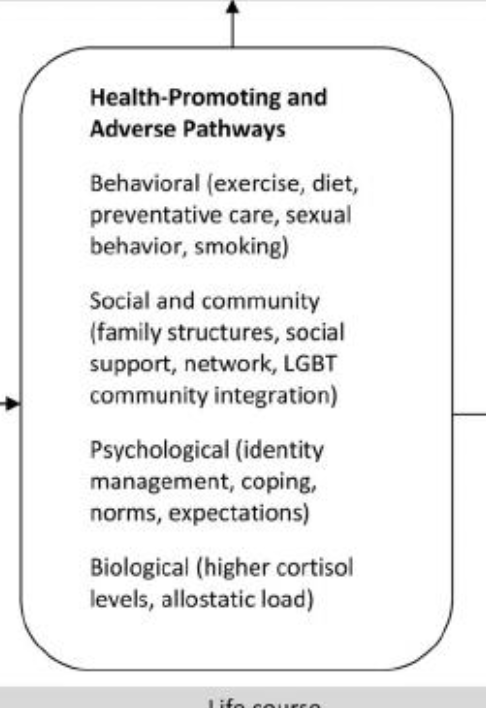
Health-Promoting Pathways
Factors that improve health
Health-Adverse Pathways
Factors that harm health
BIG IDEA: How is health shaped?
Health is shaped by multiple levels (individual + social + structural)
BIG IDEA: How do pathways influence health?
These pathways influence physical + mental health over time (life course)
Implicit Bias
Automatic, unconscious attitudes or beliefs about others
What does Implicit Bias come from?
Comes from socialization
What does Implicit Bias affect?
Healthcare decisions, Communication, Patient outcomes
Minority Stress
Stress experienced by marginalized groups due to their identity
Key Takeaways: What are the three characteristics of stress in Minority Stress Theory?
Unique (specific to minority status), Chronic (ongoing, not one-time), Socially based (comes from society, not the individual)
Distal (external) stress
discrimination, violence
Proximal (internal) stress
fear of rejection, concealment, internalized stigma
What does Minority Stress Theory explain?
Why marginalized groups have worse mental & physical health outcomes and that their stress does not come because of their color it is due to the way society has treated them.
Stigma
Negative attitudes, beliefs, and discrimination toward a group
Public Stigma
Negative attitudes/actions from others
What does Public Stigma include?
Enacted (actual discrimination), Perceived (believed discrimination happened), Anticipated (expected discrimination)
Internalized Stigma (Self-Stigma)
Person applies negative beliefs to themselves
Structural Stigma
Institutional/system-level discrimination
What constitutes Structural Stigma?
Laws, policies, societal systems that disadvantage groups
Health promoting and Health adverse pathways
Premium
Monthly payment for insurance
Deductible
Amount you pay before insurance starts covering
Copay
Fixed cost per visit/service (e.g., $20 doctor visit)
Coinsurance
Percentage you pay after deductible (e.g., 20% of bill)
Medicare
For people 65+ (EXAM HINT); Also for some disabilities; NOT income-based; Same rules nationwide
Medicaid
For low-income individuals; Not age-based (varies by state); Eligibility varies by state
Affordable Care Act (ACA) Main Impacts
Makes insurance more affordable & accessible; Expands Medicaid (low-income coverage); Creates Marketplace for buying insurance
ACA Required Coverage
Pre-existing conditions; Preventive care (screenings, vaccines); Mental health services
Age limit for staying on parents' insurance
Until age 26
Emergency Medical Treatment and Labor Act (EMTALA)
Hospitals must treat & stabilize ANY patient in emergency, regardless of ability to pay or insurance
Health Insurance Portability and Accountability Act (HIPAA) Rights
You have a right to your medical records; You can share your records with others if you choose; Your health information cannot be shared without your consent
Patient Safety and Quality Improvement Act (PSQIA)
Protects healthcare workers who report unsafe conditions
Physical Noise
External distractions (e.g., loud environment)
Physiological Noise
Body-related issues (e.g., hearing problems, fatigue)
Psychological Noise
Mental/emotional interference (e.g., stress, bias)
Sociocultural Noise
Differences in culture, language, beliefs affecting understanding
Source
Where the message originates
Transmitter (Encoder)
Converts message into signals (e.g., speaking, typing)
Channel
Medium message travels through (e.g., slides, phone)
Receiver (Decoder)
Interprets the message
Destination
Final target of the message
Health Literacy
Ability to receive, understand, and use health information to make decisions
Gain-Framed Message
Focuses on benefits of taking action
Loss-Framed Message
Focuses on consequences of NOT taking action