NS 3310 Lecture 24
1/94
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
95 Terms
Choline deficiency (very rare) causes what 3 things?
Muscle Damage
Liver damage
NAFLD
Fatty liver arises from the requirement for ___in the synthesis of?
PtdCho; VLDLs
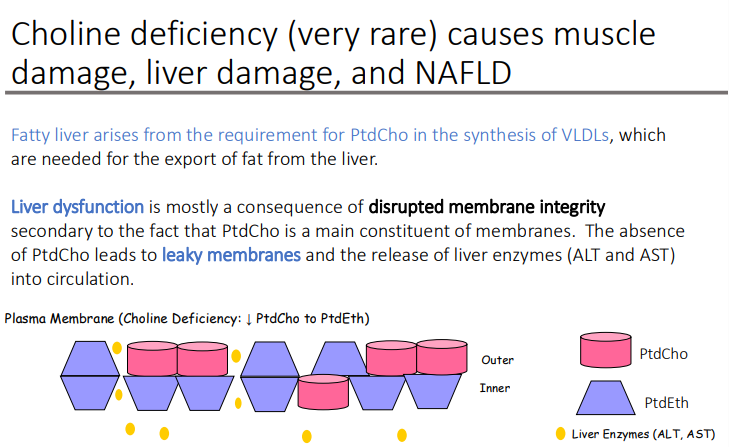
Fatty liver arises from the requirement for PtdCho in the synthesis of VLDLs, which are needed for?
the export of fat from the liver
Liver dysfunction is mostly a consequence of disrupted? secondary to the fact that PtdCho is a main constituent of membranes
membrane integrity
The absence of PtdCho leads to? and the release of?
leaky membranes
Liver enzymes (ALT and AST)
What are three other health outcomes of Choline deficiency?
Cancer
Birth outcomes → Higher maternal choline intakes during pregnancy have been associated with a lower risk of having a baby with an NTD.
Cognition → Higher maternal choline intakes during pregnancy have been found to improve measures of cognitive functioning in infants and children.
Cancer: Relationships between biomarkers of choline status and cancer risk are?
inconsistent
some studies reporting a positive relationship and others reporting a negative relationship.

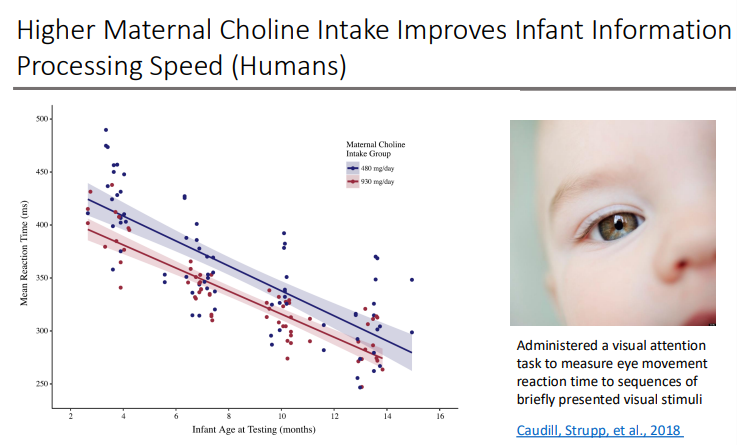
Higher Maternal Choline Intake Improves Infant Information Processing Speed (Humans)

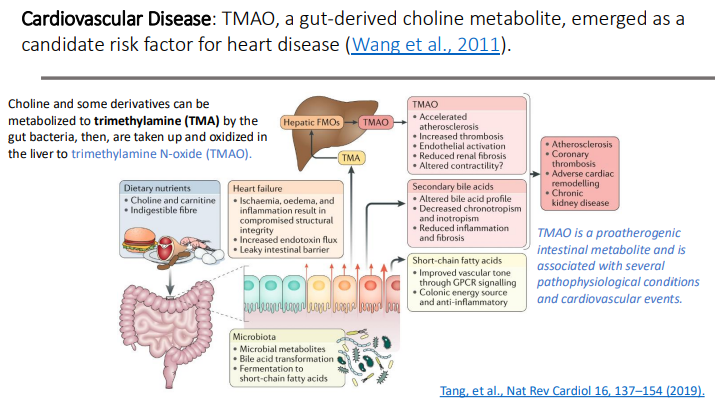
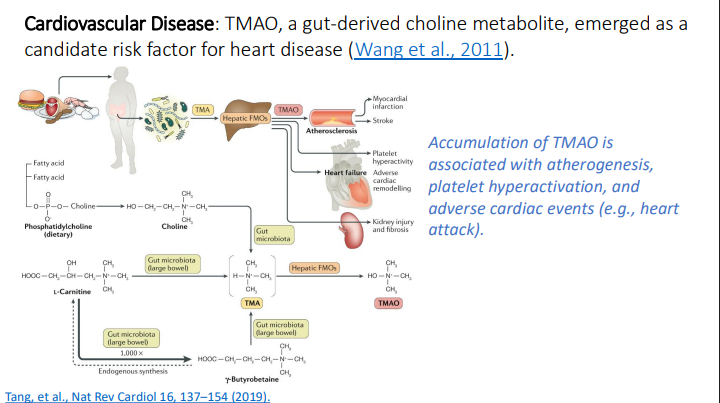
Cardiovascular Disease: What emerged as a candidate risk factor for heart disease?
TMAO, a gut-derived choline metabolite
Choline and some derivatives can be metabolized to? by the?
trimethylamine (TMA)
gut bacteria
Choline and some derivatives can be metabolized to trimethylamine (TMA) by the gut bacteria, then, are taken up and oxidized in the liver to?
trimethylamine N-oxide (TMAO)
TMAO is a ____ intestinal metabolite and is associated with several _____conditions and ____ events.
proatherogenic; pathophysiological; cardiovascular
Accumulation of TMAO is associated with what 3 things?
Atherogenesis
Platelet hyperactivation
Adverse cardiac events (ex: heart attack)
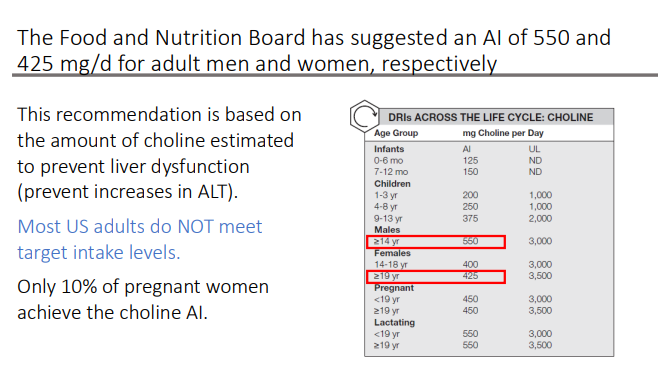
The Food and Nutrition Board has suggested an AI for choline of? This recommendation is based on?
550 and 425 mg/d for adult men and women, respectively
This recommendation is based on the amount of choline estimated to prevent liver dysfunction (prevent increases in ALT)
The UL is 3.5 g choline/d and is based on the amount of choline that could result in what two things?
Fishy body odor (caused by TMA)
Hypotension (acetylcholine, which slows heartbeat)
Are there good biochemical indicators of choline status?
No
(problems with specificity and sensitivity)

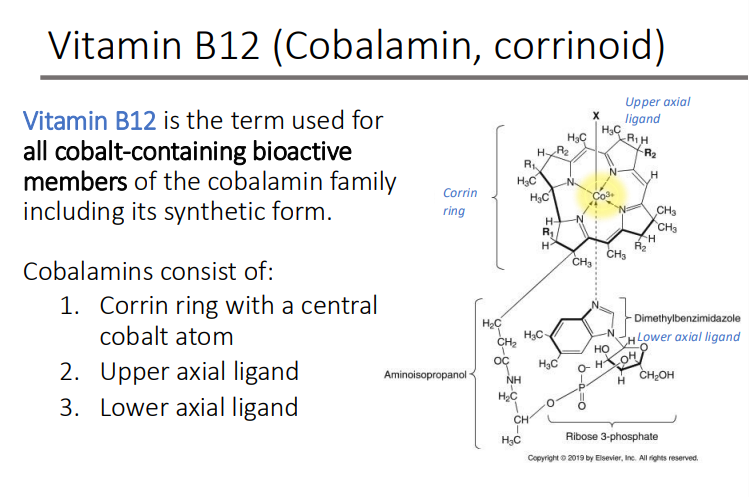
Vitamin B12 is the term used for all?
cobalt-containing bioactive members of the cobalamin family
including its synthetic form
Cobalamins consist of what 3 things?
Corrin ring with a central cobalt atom
Upper axial ligand
Lower axial ligand
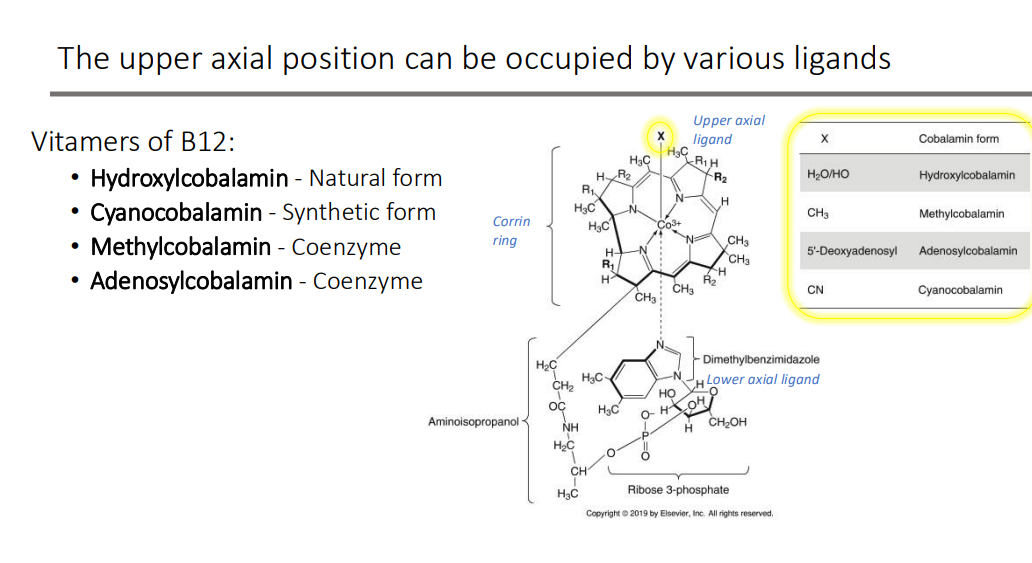
The upper axial position can be occupied by?
various ligands
What are the 4 Vitamers of B12?
Hydroxylcobalamin - Natural form
Cyanocobalamin - Synthetic form
Methylcobalamin - Coenzyme
Adenosylcobalamin - Coenzyme
Dietary sources of vitamin B12 come primarily from animal products. What 5 things are good sources of vit b12?
Meat
milk
eggs
fish
shellfish
Synthetic forms of vitamin B12 are present in what 2 things?
fortified foods (e.g., many ready-to-eat cereals)
multivitamins
This vitamin is fairly stable and resistant to what three things?
Light
Heat
Oxidation

With few exceptions, plant sourced foods do NOT contain vitamin B12: Diets low in animal-source foods, either by choice or by circumstance, provide very low amounts of the vitamin and can lead to?
vitamin B12 deficiency.
For vegans, what 3 things can help them meet their vitamin B12 needs?
Supplements
Nutritional yeast
Fortified products

Neither plants nor animals can synthesize vitamin B12. A. True B. False

Digestion and absorption: The majority of vitamin B12 is absorbed bound to? via what process?
intrinsic factor (IF)
carrier-mediated process.
A small amount (~1% of total intake) can be absorbed via passive diffusion.
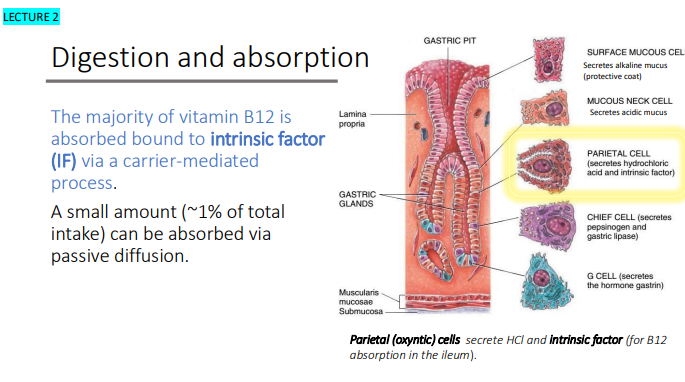
Vitamin B12 requires release from food proteins and transport via what 2 things?
Haptocorrin
Intrinsic factor
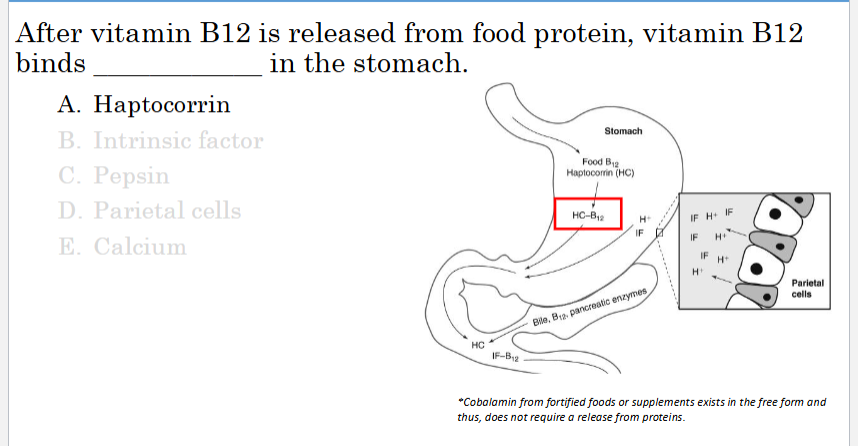
Protein-bound cobalamin in foods* is released from proteins by the actions of what 2 things?
Pepsin
HCL
*Cobalamin from fortified foods or supplements exists in the free form and thus, does not require a release from proteins.
Within the stomach, ‘free’ B12 binds?
haptocorrin (HC)
Within the stomach, ‘free’ B12 binds haptocorrin (HC), which is produced by?
glandular cells
(salivary glands, gastric mucosa, and others)
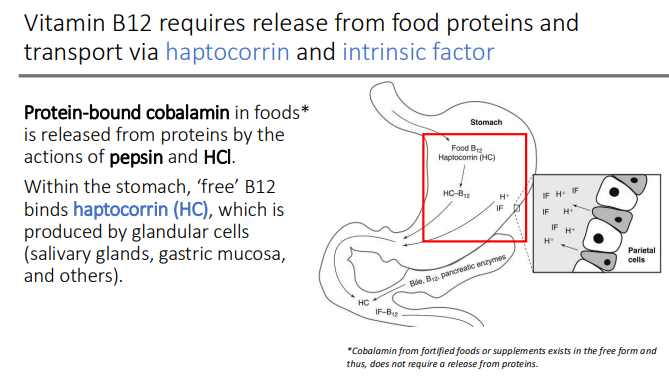

Can antiacids interfere with vitamin B12 absorption?
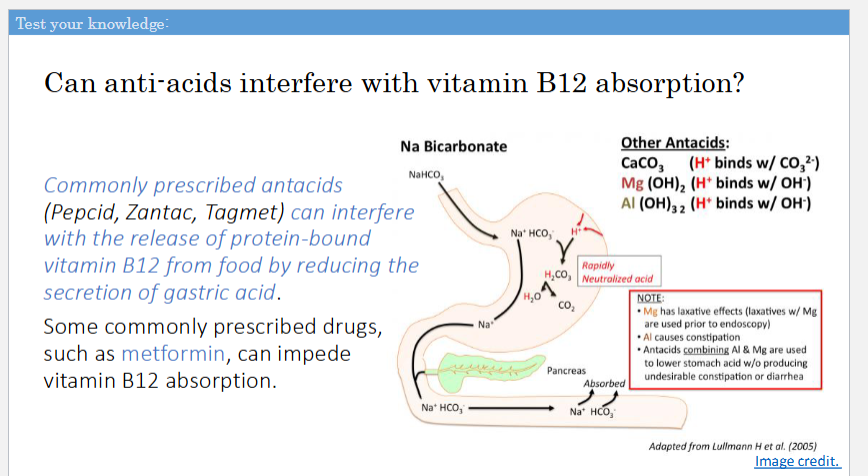
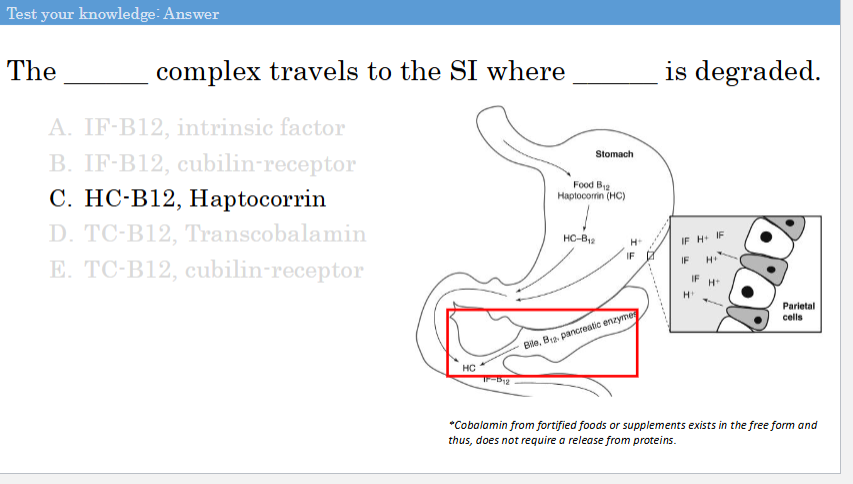
The vitamin HC-B12 complex passes into the small intestine where the HC is hydrolyzed by?
pancreatic proteases
Free vitamin B12 binds to?
IF
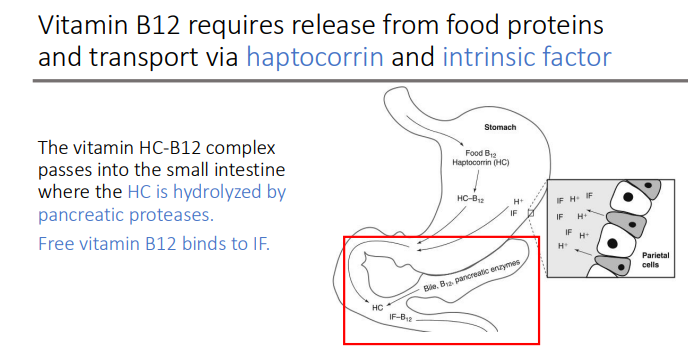
vitamin B12 and bile acids are absorbed in the?
ileum
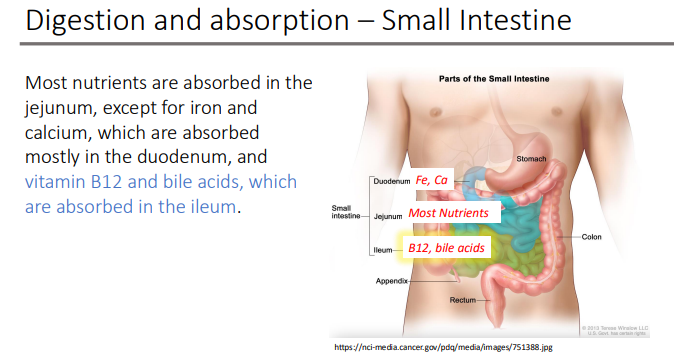
The IF-B12 complex is absorbed via?
cubilin receptor-mediated endocytosis
The IF-B12 complex is recognized by a cubilin-receptor on the? of what type of cells?
brush border membrane of ileal cells
Cubilin interacts with an?
amnionless (AMN) protein
Cubilin interacts with an amnionless (AMN) protein, which is required for the localization of cubilin to the?
membrane of intestinal cells
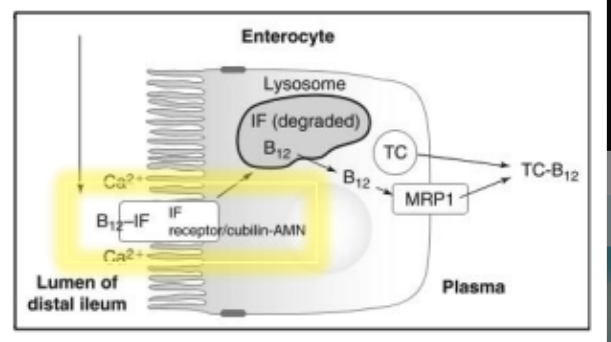
Most ingested vitamin B12 is absorbed as part of this IF-B12 complex. Cubilin does not recognize?
unbound B12 or free IF

IF-B12 binds to the cubilin-AMN receptor in the presence of?
Ca2+
When IF-B12 binds to the cubilin-AMN receptor (in the presence of Ca2+), the receptor and the IF-B12 complex are? by?
internalized
by endocytosis with the subsequent recycling of the receptor to the membrane
To a lesser extent (1-3%), vitamin B12 is also absorbed by?
passive diffusion

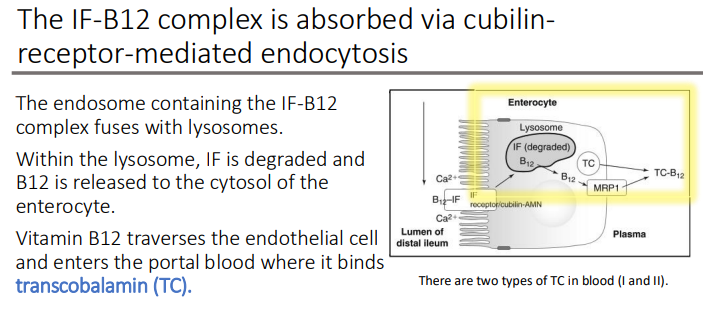
The endosome containing the IF-B12 complex fuses with?
lysosomes
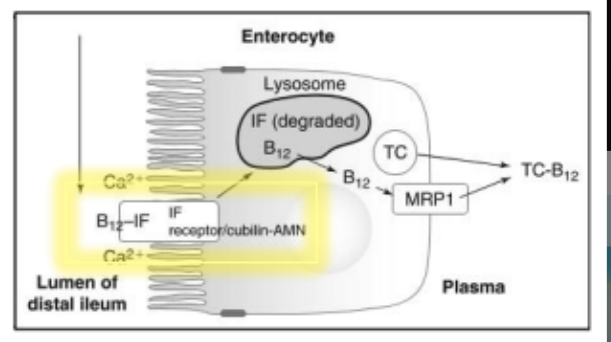
Within the lysosome, IF is ____ and B12 is released to the cytosol of the ____.
degraded
enterocyte
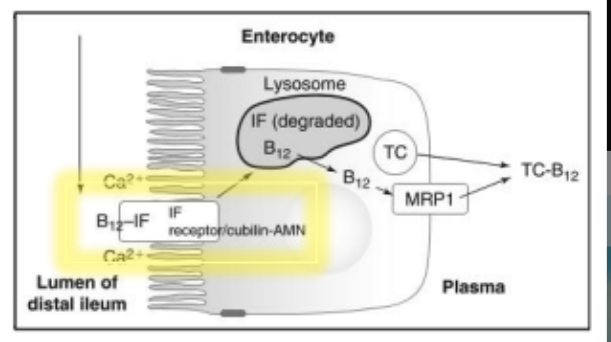
Vitamin B12 traverses the ____ cell and enters the portal blood where it binds?
endothelial; transcobalamin (TC)

______ and _____ are required for the release of vitamin B12 in the stomach


After vitamin B12 is released from food protein, vitamin B12 binds ____________ in the stomach.

The ______ complex travels to the SI where ______ is degraded

In the intestines (ileum), free B12 binds to ______ and is taken up by the ________ (receptor)


Within the enterocyte, _________ is degraded and free B12 enters portal blood where it binds ________________.

Upon uptake of B12-TC by receptor-mediated endocytosis, B12 can be metabolized to what two things?
Methylcobalamin
deoxyadenosylcobalamin
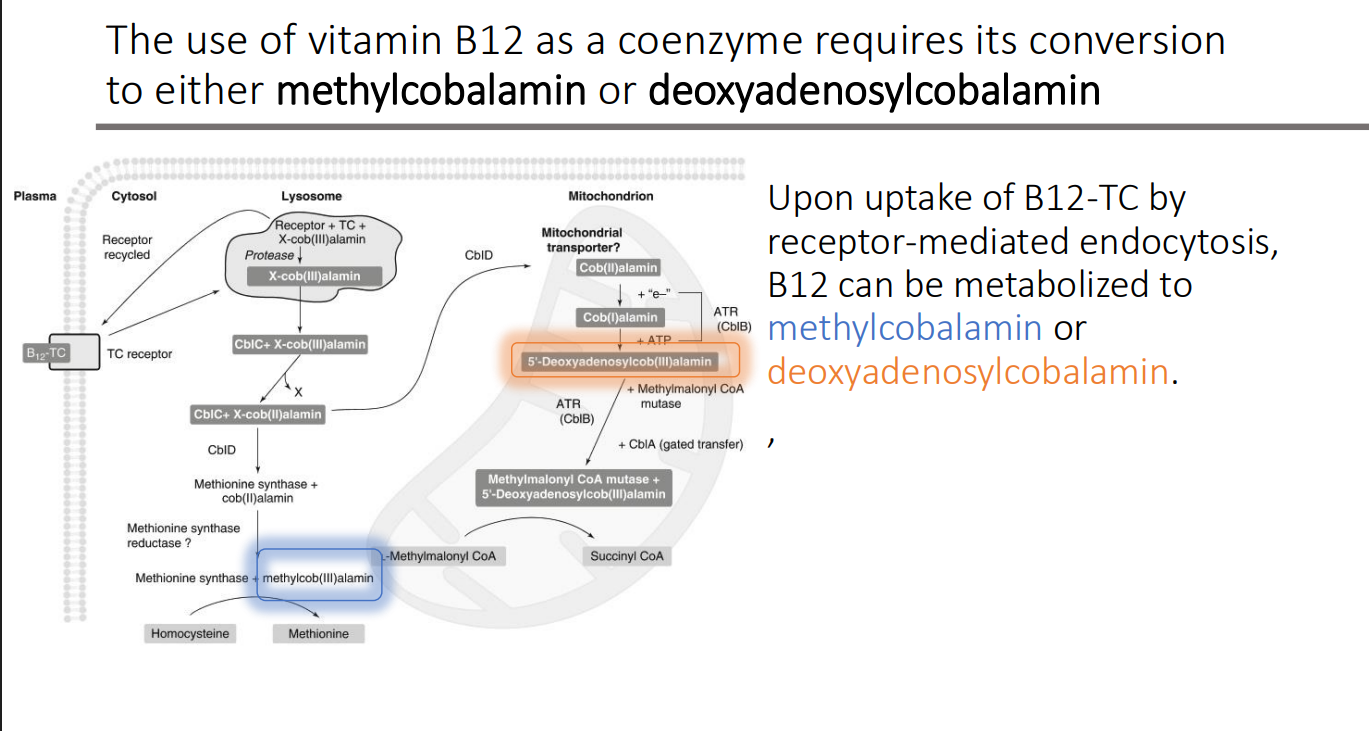
Methylcobalamin serves as the coenzyme for what in the cytoplasm?
methionine synthase
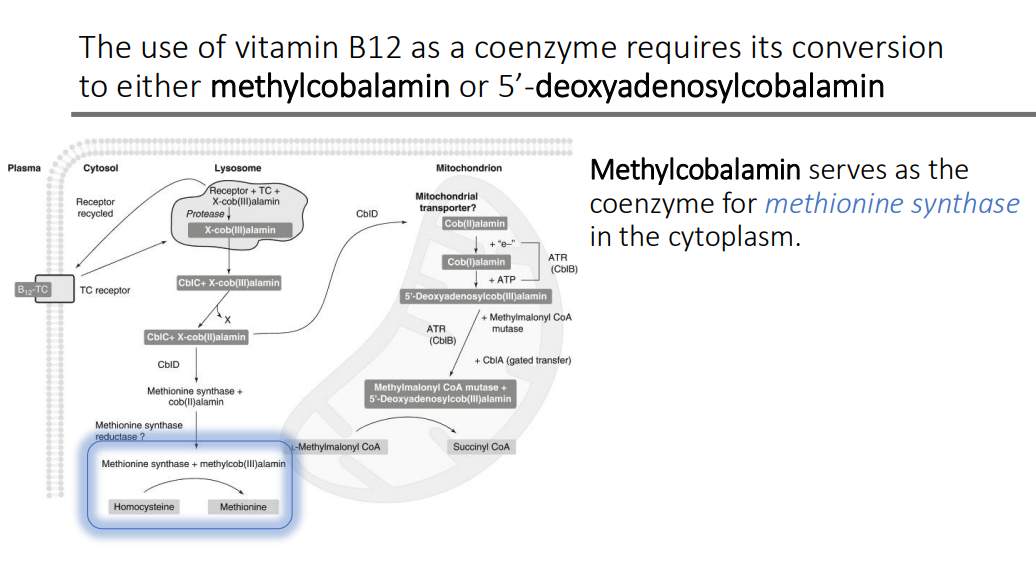
Methionine synthase, in the folate-dependent pathway, requires?
B12 as a coenzyme.
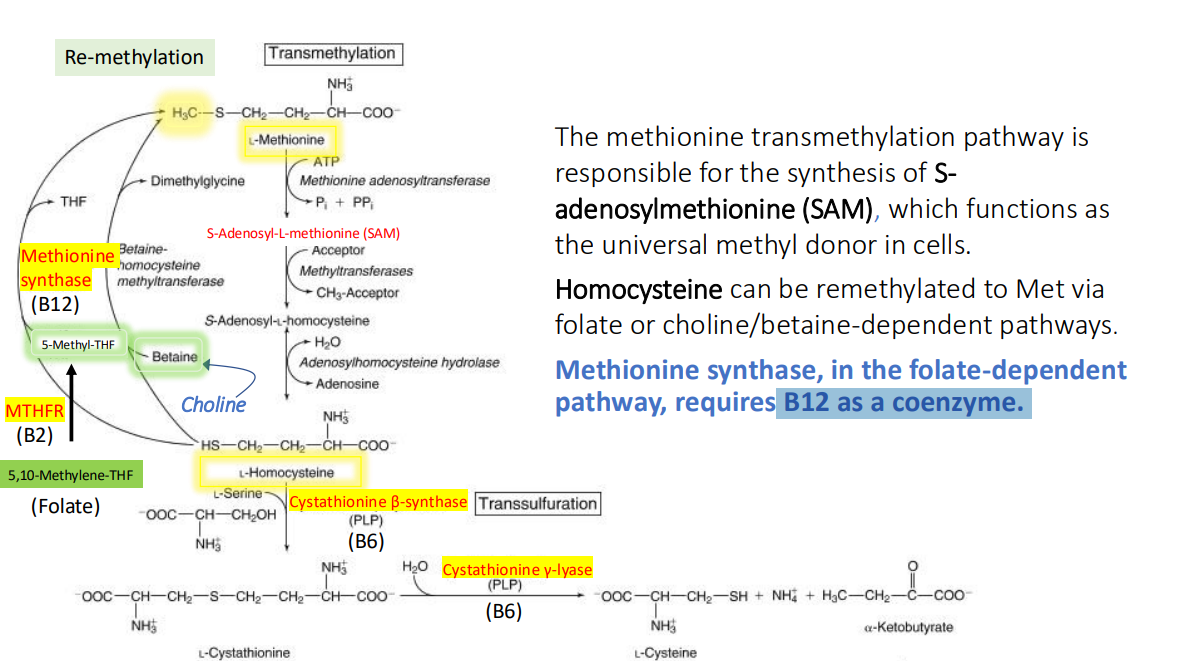
Methylcobalamin is used by cytosolic methionine synthase to?
remethylate homocysteine to methionine in a two-step process
Methylcobalamin is used by cytosolic methionine synthase to remethylate homocysteine to methionine in a two-step process: Step 1. The methyl group is transferred from 5-methyl-THF to? forming?
cobalamin forming methylcobalamin
Step 1. The methyl group is transferred from 5-methyl-THF to cobalamin forming methylcobalamin, which is bound to what two things?
Methionine synthase
THF
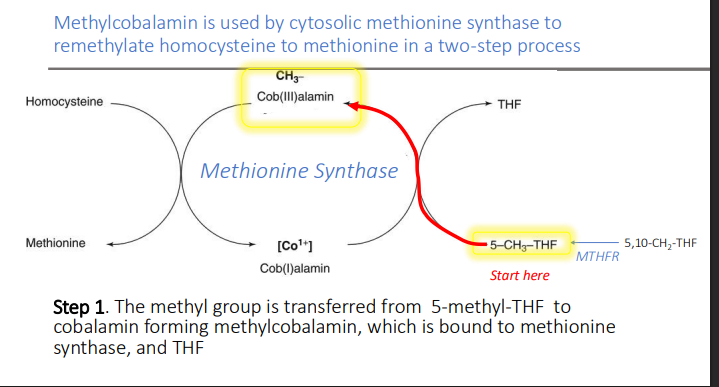
Methylcobalamin is used by cytosolic methionine synthase to remethylate homocysteine to methionine in a two-step process: Step 2. The methyl group from methylcobalamin is transferred to? forming what two things?
homocysteine
Methionine
Cobalamin
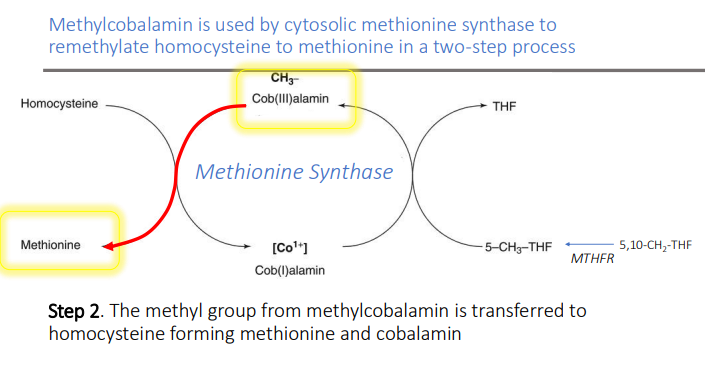
Methionine synthase’s activity depends on the transfer of labile methyl groups from what to what?
5-methyl THF to vitamin B12
Methionine synthase’s activity depends on the transfer of labile methyl groups from 5-methyl THF to vitamin B12, in which methylcobalamin serves as an? to convert what to what?
immediate methyl donor to convert Hcy to Met
Vitamin B12 deficiency ”traps” folate in what form?
5-methyl-THF form
Vitamin B12 deficiency ”traps” folate in the 5-methyl-THF form, which will accumulate at the expense of other folate groups (↓folate pool) and will cause a?
secondary folate deficiency
The reason behind either folate or vitamin B12 can cause what type of anemia?
megaloblastic (macrocytic) anemia
5’-Deoxyadenosylcobalamin serves as the coenzyme for what in the mitochondria?
methylmalonyl CoA mutase
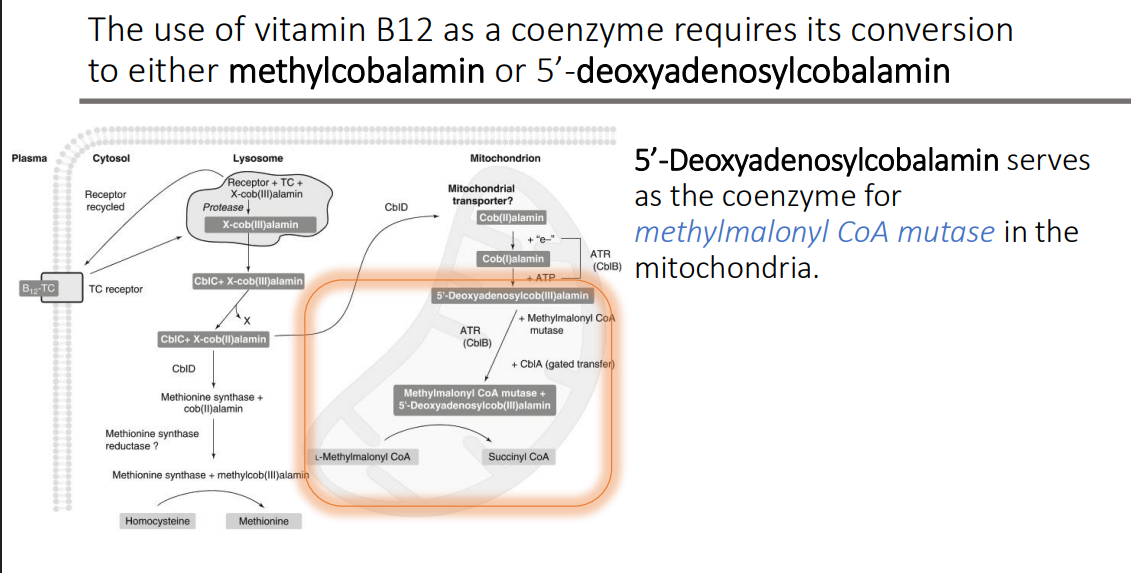
Lecture 9: 5’-Deoxyadenosylcobalamin is used by mitochondrial methylmalonyl CoA mutase: Propionyl-CoA is generated during the catabolism of?
odd-numbered fatty acids and several amino acids (e.g., isoleucine, valine, methionine, threonine)
Methylmalonyl CoA mutase catalyzes the last step of this pathway, which is the conversion of what to what?
L-methylmalonyl CoA to succinyl CoA

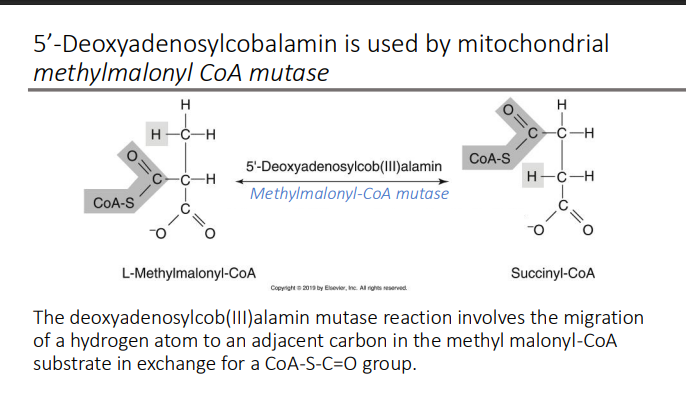
5’-Deoxyadenosylcobalamin is used by mitochondrial methylmalonyl CoA mutase: The deoxyadenosylcob(III)alamin mutase reaction involves the migration of a hydrogen atom to an adjacent carbon in the methyl malonyl-CoA substrate in exchange for a _____ group
CoA-S-C=O group.
Lecture 23: Folate (and B12) deficiency causes megaloblastic anemia

Megaloblastic anemia occurs in both folate and vitamin B12 deficiency because vitamin B12 deficiency causes a secondary _______ of folate via the ____ trap
functional deficiency; methyl-folate
What activity is reduced in vit B12 deficiency?
Methionine synthase activity
Methionine synthase activity is reduced in vitamin B12 deficiency: There is an accumulation of? because the methionine synthase reaction is the only reaction capable of ?
5-methyl-THF
converting 5-methyl-THF back to free THF
The lack of folate for other reactions of 1-C metabolism impedes what 3 things? and thus what is compromised?
thymidylate
purine synthesis
methylation
Nucleotide synthesis and repair are compromised

Vitamin B12 deficiency is relatively common among? due to?
older adults due to malabsorption
The prevalence of atrophic gastritis increases with age, perhaps exceeding 30% in older adults (age >65 y) thus accounting for most cases of vitamin B12 deficiency in older adults
Atrophic gastritis is a condition of reduced? and consequent reduced capacity to release?
stomach acid production (hypochlorhydria/achlorhydria
protein-bound vitamin B12.
Individuals with atrophic gastritis can efficiently absorb _____ from fortified foods and supplements because vitamin B12 is not bound to proteins.
crystalline vitamin B12
Vitamin B12 deficiency is also affected by frequent use of?
antiacids

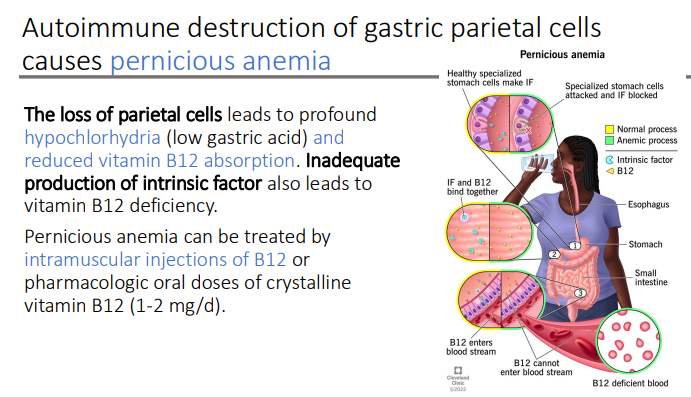
Autoimmune destruction of gastric parietal cells causes?
pernicious anemia
The loss of parietal cells leads to profound? and reduced?
hypochlorhydria (low gastric acid)
vitamin B12 absorption
Inadequate production of intrinsic factor also leads to?
vitamin B12 deficiency
Pernicious anemia can be treated by what two things?
Intramuscular injections of B12
Pharmacologic oral doses of crystalline vitamin B12 (1-2 mg/d)
Undetected vitamin B12 deficiency can result in neurological disorders: The neurological manifestations of vitamin B12 deficiency can be severe and are often irreversible, affecting what three locations?
Spinal cord
Peripheral nerves → peripheral neuropathy
Brain → memory loss, dementia, and depression
These neurological deficits are the consequence of the? and are likely related to metabolic disturbances in?
Demyelination of neuronal axons
1-C metabolism

What often precedes neurological diseases and allows for the detection and treatment of vitamin B12 deficiency before the development of neurological damage?
Megaloblastic anemia
What can prevent secondary folate deficiency whereby megaloblastic anemia does not develop, allowing the vitamin B12 deficiency to go undetected?
High folic acid intake

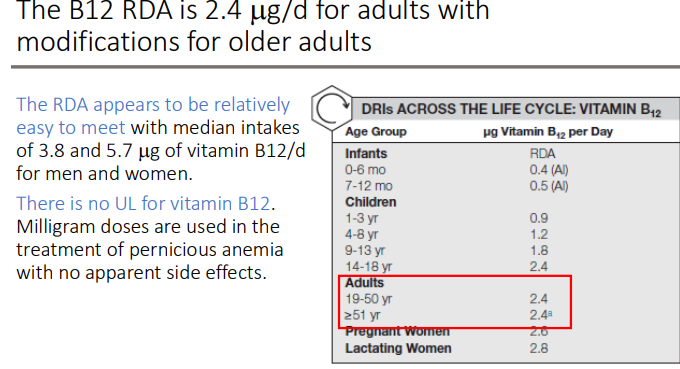
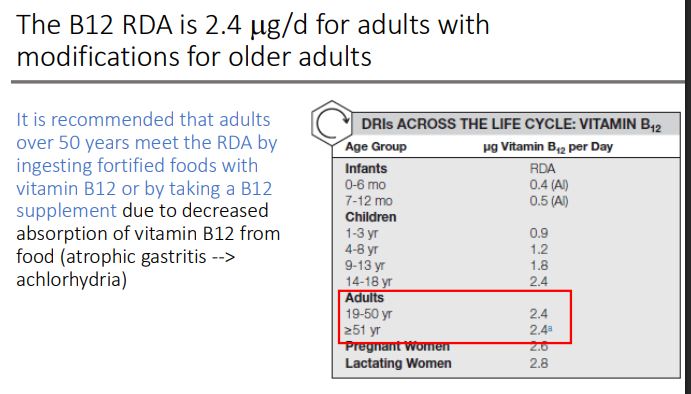
The B12 RDA is ____for adults with modifications for older adults. Is it easy to meet?
2.4 ug/d
The RDA appears to be relatively easy to meet with median intakes of 3.8 and 5.7 ug of vitamin B12/d for men and women.
Is there an UL for Vit B12
There is no UL for vitamin B12. Milligram doses are used in the treatment of pernicious anemia with no apparent side effects.
It is recommended that adults over 50 years meet the RDA by ingesting?
fortified foods with vitamin B12 or by taking a B12 supplement due to decreased absorption of vitamin B12 from food (atrophic gastritis --> achlorhydria
Biochemical Indicators: What is used clinically but it may not be a reliable biomarker?
Total Vitamin B12 in plasma (HC-B12 + transcobalamin-bound B12
Total Vitamin B12 in plasma (HC-B12 + transcobalamin-bound B12) is used clinically but it may not be a reliable biomarker because it does not indicate the amount of? available for?
bioactive vitamin B12
cellular uptake
What is a marker of bioactive vitamin B12 and appears to be of greater diagnostic value than total vitamin B12
Holotranscobalamin (transcobalamin-bound B12) plasma

Elevations in what can occur in response to vitamin B12 (methylcobalamin) or folate deficiency?
homocysteine
In populations exposed to folic acid fortification, B12 has become the major nutritional determinant of increases in? and thus represents a specific?
homocysteine
functional indicator of vitamin B12 status
(enzymatic activity of methionine synthase is impaired in B12 deficiency)

Elevations in what are used as a functional indicator of vitamin B12 deficiency?
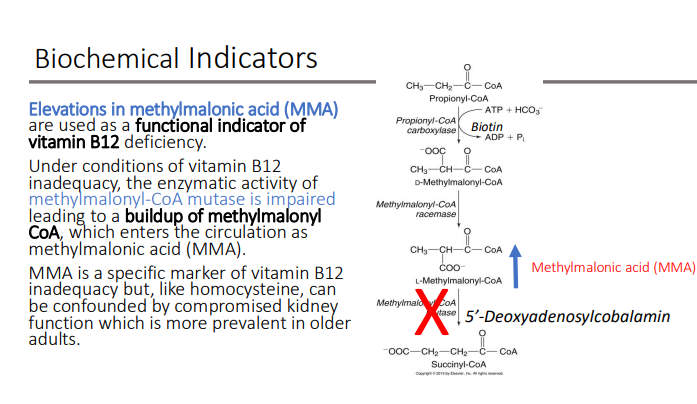
methylmalonic acid (MMA)
Under conditions of vitamin B12 inadequacy, the enzymatic activity of methylmalonyl-CoA mutase is impaired leading to a buildup of?
methylmalonyl CoA, which enters the circulation as methylmalonic acid (MMA).
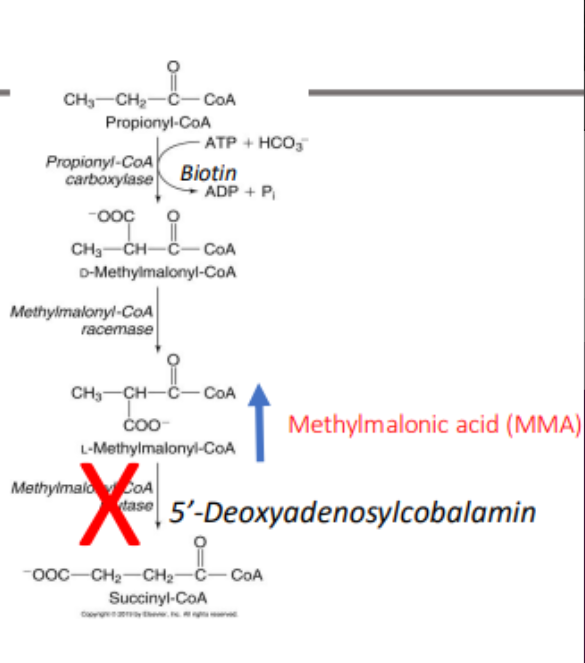
MMA is a specific marker of vitamin B12 inadequacy but, like homocysteine, can be confounded by compromised what function?
kidney function which is more prevalent in older adults.