Test 2 (Pharmacology Concepts, Screening CV and Respiratory, Screening GU, Renal and Integumentary)
1/104
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
105 Terms
What are racial, ethnic, and genetic factors that many increase risk of CV conditions?
heart disease is the leading cause of death for people of most racial and ethnic groups in the US (including African American, American Indian, Alaska native, hispanic, and white men)
What are risk factors for cardiac issues?
- age (males >45, women >55)
- family history of heart disease
- cigarette smoking
- physical inactivity
- obesity
- hypertension
- dyslipidemia
- diabetes
What risk factors can PTs help with?
- blood pressure
- blood sugar/diabetes
- BMI
- chronic inflammation
- diet
- exercise
- HDL cholesterol
- smoking
- stress
- total cholesterol
Do PTs typically get patients (referrals or direct access) based on constitutional signs/symptoms?
NO
What constitutional signs/symptoms might suggest CV system involvement?
palpitations, angina, extreme fatigue, pallor, chest pain
What are possible physical examination skills that we can use if report of possible CV involvement is provided during intake?
vitals
What pain patterns may indicate CV involvement?
pain referrals are variable and extensive!
most likely not instigated or responsive to movement (rules out MSK injuries)
most common: chest pain, LUE, discomfort in jaw, neck, back, arm, or shoulder
most common for women: feeling nauseous, light-headed or unusually tired
What are other causes of chest pain?
chest pain can happen more many reasons, often other signs that occur with it will give an idea of why chest pain occurs
Which artery carries deoxygenated blood away from the heart?
pulmonary artery
Which vein carries oxygenated blood to the heart?
pulmonary vein
What is the only cardiac muscle?
heart
Which ventricle in the heart is thicker?
LEFT = pumps blood through the whole body
What are signs/symptoms for respiratory system issues?
- dyspnea
- cough (duration, positional, productive, sputum)
- palpitations
- syncope (fainting)
- sweats
- edema
- cold distal extremeties
- skin discoloration
- open wounds/ulcers
- clubbing of the nails
- wheezing, stridor
What is dyspnea?
shortness of breath
What are some common causes for dyspnea?
medications, allergies, CV/pulmonary issues, etc.
When is a referral for dyspnea indicated?
when there is little effort exerted and there is shortness of breath, when pt experiences dyspnea when laying down and during sleep
What is dyspnea often associated with?
chronic heart and lung disease
What is a common pulmonary condition that mimics MSK conditions?
pneumonia > makes overall body weak, COPD, pulmonary embolism
What is the number one cause of pneumonia, and common risk factors?
aspiration > nursing facilities, patients who are not upright when eating
Can PT positively impact/ make it less likely that someone will develop pneumonia?
YES, movement is key to not pool liquid in the lungs
exercise lets gravity do work on the body
How do structures which contact the diaphragm influence pain referral to the shoulder?
phrenic nerve (C3, C4, C5) has the same nerve roots for the diaphragm and the shoulder
Why is it often difficult to detect pulmonary disorders? (think parietal vs visceral pleura)
referral of pain is less localized, different layers of pleura, parietal pleura isn't innervated whereas the visceral pleura is
What are considered to be immediate referrals for the pulmonary system?
pulmonary embolism, significant changes/pain, low O2 stats over prolonged period, ongoing cough, symptom after traveling/scuba diving
What constitutional signs/symptoms might suggest respiratory system involvement?
- fever
- diaphoresis (unexplained perspiration)
- sweats
- nausea
- vomiting
- diarrhea
- pallor
- dizziness/syncope
- fatigue
- weight loss
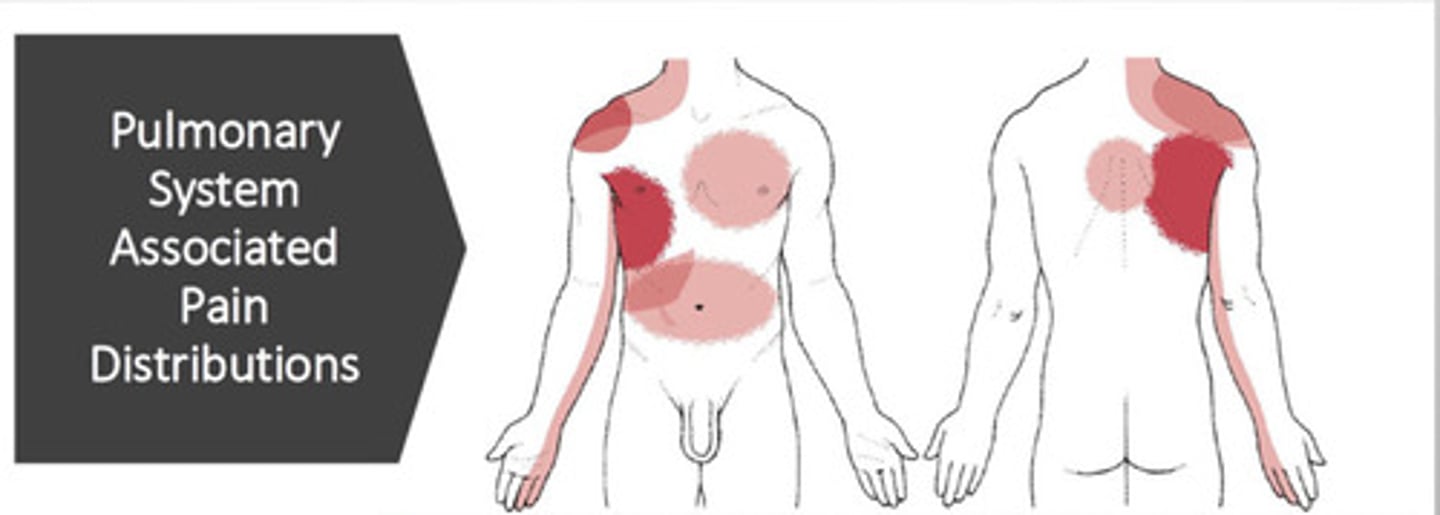
What pain patterns may indicate respiratory/pulmonary involvement?
not localized to a specific area
Wells Score for pulmonary embolism
score > 6 = high probability
score 2-6 = moderate probability
score < 2 = low probability
What does a Wells Score for PE > 4 indicate?
PE likely, consider diagnostic imaging
What does a Wells score for PE < 4 indicate?
PE unlikely, consider D-dimer to rule out PE
What are symptoms of hypertension?
- facial flushing
- headaches
- altered vision
- dizziness
- nose bleeds
- shortness of breath
- chest pain
- unsteady "rubbery" legs
- feeling faint, syncope
Untreated, _______ can lead to CVA, MI, CHF, PVD, renal failure, neuropathy, retinopathy. It is the "silent killer"
hypertension
What is heart failure?
complex clinical syndrome in which there is inability of the heart to eject blood to meet the demands of the body
What are symptoms of heart failure?
shortness of breath, fluid retention, fatigue, orthopnea, paroxysmal nocturnal dyspnea
What are complications of heart failure?
impaired exercise tolerance, increased risk of vent arrhythmias, and shortened life expectancy
Why do we study pharmacology?
for its impact on patients!
medications can affect response to exercise, pain perception, motivation, interactions between drugs can have adverse affects, affect modalities
Only ___% of the time do providers know ALL the medicines/substances someone takes
2%
What are factors influencing pharmacokinetics (ADME)
absorption, distribution, metabolism, excretion
What are examples of routes of administration for medications?
- oral
- sublingual (under tongue)
- buccal (cheek)
- rectal
- inhalation
- IV
- intra-arterial
- subcutaneous
- intramuscular
- intrathecal
- topical
- transdermal (patch)
What is important in medications regarding the distribution?
where in the body the medication goes
With aging, total body water (decreases/increases), total body fat (decreases/increases)
decreases, increases
If a medication is hydrophilic (water loving) what happens if the patient is dehydrated?
increased effect of medication = more medicine per amount of water
If a medication is lipophilic (fat loving) what happens when a patient loses 40 pounds?
increases affect of medication = higher concentration
What is important in regards to metabolism of medications?
break down- how the medication is broken down in the body
What organ is mainly responsible for metabolism?
liver
Why does it matter if some enzymes in the liver aren't active until around age 5?
some medications could be deadly and have adverse effects on a child when it has normal effects on an adult
Why does it matter if some enzymes in the liver aren't active in older ages?
the same dosage of medication they have been taking since their 40s might have a different effect in their 80s
How is the medication eliminated from the body?
feces, urine
_____________ function gradually declines with age after about the age of 40
renal
What are beta blockers used for?
blood pressure, heart failure, after a myocardial infarction
What are beta agonists used for?
asthma treatment
What are possible systemic effects of medications?
- upregulation or downregulation of receptors
- alterations in the physiologic response to medications
What are key factors we should consider that people bring to the table regarding medications?
age, sex, concomitant medical conditions, diet, exercise, environment, smoking, alcohol, genetics
T/F: Pharacokinetics can be both linear and nonlinear
TRUE
What is important regarding nonlinear pharmacokinetics?
it is important for prescribers to understand that different medications have different potencies depending on their dosage
an increased dosage of one medication can have little effect, whereas an increased dosage of another can have a significant change
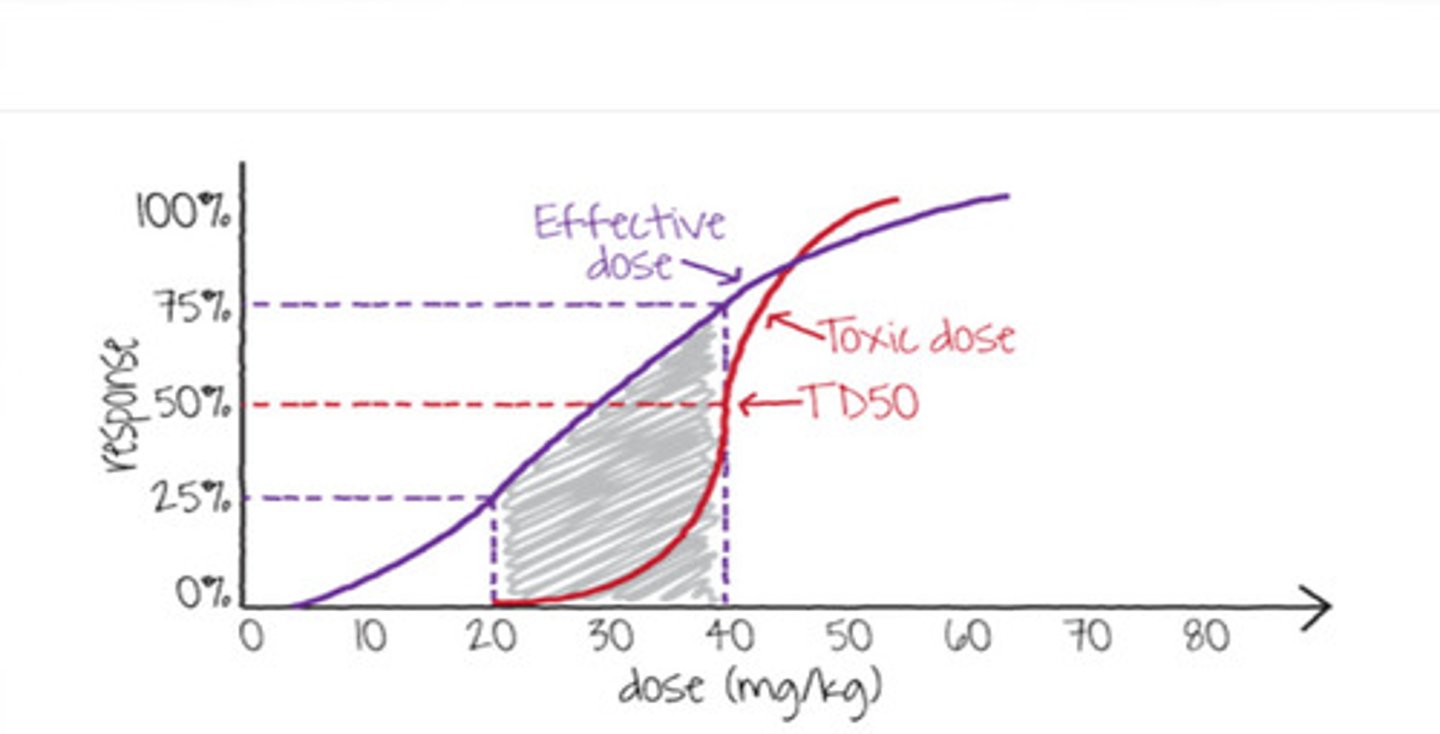
What is important in regards to the "narrow therapeutic index" in pharmacokinetics?
there are some drugs where small differences in dose or blood concentration may lead to serious therapeutic failures and/or adverse drug reactions that are life-threatening or result in persistent or significant disability or incapacity
aka: become toxic quickly!
Where can GU/Reproductive system issues refer pain?
low back, thighs, abdominal wall
_____________ is filtered by the glomerulus and secreted by the proximal tubule
creatinine
Creatinine clearance can be a good estimate of?
glomerular filtration rate
What is the BIG DEAL with CYP450?
enzymes essential for medication metabolism; these enzymes can have a lot of genetic variability where they can be inhibited or induced > chance of clinically significant drug-drug interactions and adverse effects
What are the advantages for the new labeling for medications during pregnancy?
align with physician labeling rule format, helps to assess benefit vs. risk, counsel patient appropriately, removed perception that one drug might be better than others
What does the new/current pregnancy and lactation labeling rule include?
- pregnancy, includes labor and delivery
- lactation, includes nursing mothers
- females and males of reproductive potential
Many medications have cough, flu, cold symptoms in their list of possible adverse effects? Why?
the clinical trials were most likely conducted during the winter/flu season, therefore they couldn't rule out these symptoms during testing
What are important factos to consider when deprescribing?
- triage changes
- coordinate changes
- one or very few at a time
- taper, especially if impacts thinking
- closely monitor during taper
How many schedules are there for controlled substances?
5
What are the 5 schedules of controlled substances based on?
- currently accepted medical use
- relative abuse potential
- likelihood to cause dependence
examples of schedule 1
non-regulated: heroin, LSD, canabis, peyote, ecstacy, qualuuds
examples of schedule 2
most regulated/approved: morhpine, hydromorphone, oxycodone, codeine, Adderall, Ritalin
examples of schedule 3
Tylenol with codeine, suboxone, ketamine, Depo-testosterone
examples of schedule 4
alprazolam (xanax), lorazepam (ativan), diazepam (valium)
examples of schedule 5
codeine cough syrup (up to 2 mg/ml)
What are some medication-related problems?
- medication errors
- suboptimal drug, dose, regimen, dosage form, and duration of use
- unnecessary drug therapy
- therapeutic duplication
- drug-drug disease, drug-food, or drug-nutrient interactions
- drug allergies/intolerances
- adverse drug effects, clinically significant (some are preventable)
- not take a medication when one can help
What is the GI system?
vast, complex system of organs that functions to digest and absorb ingested nutrients, and to excrete waste products of digestion
What system supports the GI system?
biliary
What system is considered the "second brain" due to its millions of neurons, neuropeptides, and hormonal influences?
GI system
Where can GI disorders refer pain in the body?
sternal region, shoulder/neck, scapular region, midback, lower back, hip, pelvis, sacrum
What is a visceral pain?
site of pain corresponds to dermatomes from which the diseased organ receives its innervation; not well-localized; multi-segmental innervation
What are clinically meaningful symptoms for GI?
- abdominal pain
- dysphagia
- odynophagia
- melena
- epigastric pain radiating to the back
- symptoms affected by food
- constipation
- diarrhea
- referred shoulder pain
- arthralgia
- McBurney's point
Where is referred pain common of GU/Reproductive systems?
low back, thighs, abdominals
Conditions of GU/Reproductive systems can have symptoms often mimicking MSK pathology!
Who are the main patient populations affected by UTIs?
women, older adults
What is the main symptom of an older adult with a UTI?
quick onset of confusion
What can UTIs develop into if left untreated?
pyelonephritis (kidney infection)
What is the largest organ of the body that forms a physical barrier between the external and internal environment that serves to protect and maintain?
integumentary system
Wy can PTs detect integumentary system conditions?
PTs see the skin a lot more than other providers during examination and treatment, longevity of care
How to test dehydration?
pinch the skin, lift up slightly, then release
testing locations: under the clavicle, extensor surface of forearm, dorsum of hand
What is seen with a negative dehydration assessment? Positive?
negative: the skin should lift up easily and return to place quickly
positive: pinched skin remains lifted for 5 seconds or more after its release and returns to normal very slowly
(Positive/Negative) dehydration assessment indicates signs of dehydration
positive
What patient populations is the dehydration test commonly seen?
children, older adults
What does unilateral edema usually indicate?
DVT/post-thrombotic syndrome (blood clot), local inflammation
What does bilateral edema usually indicate?
chronic heart failure, chronic venous insufficiency, liver failure, renal disease
What does pitting edema usually idicate?
chronic condition
What are signs of skin infection?
warm.hot skin
What are signs of arterial insufficiency?
cool skin
What are signs of venous insufficiency?
warm skin
What does cyanosis ("blue colored fingers") usually indicate?
lung disease, CHF, venous obstruction, or cold environments (hypothermia, etc)
What does Rubor of Dependency (redness) usually indicate?
peripheral vascular disease
What does yellowing/jaundice of skin usually indicate?
bilirubin levels, hepatic (liver) disease
WHat does darkening-hyperpigmentation of skin usually indicate?
Addison's disease
Where is it best to observe skin color changes?
white part of eyes, palms of hand, soles of feet
What are the ABCs for skin cancer screening?
Asymmetry, Border, Color, Diameter
Evolution
Round, symmetric skin lesions such as common moles, freckles, and birthmarks are considered?
normal
Common moles or other "normal" skin changes usually have what types of borders?
usually smooth, even borders or edges