38 - Antimicrobials and Resistance
1/23
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
24 Terms
What is PRSA?
Penicillin Resistant Staphylococcus aureus
What allows for antibiotic resistance?
Over perscription
Prescribing below the optimum dose
True or False: we induce antibiotic resistant bacteria
False → bacteria are constantly mutation and selectively encourage growth of bacteria that is resistant due to mutations
What is constitutive resistance? Examples?
Bacteria are reistance because that don’t have the systems to uptake ABX or don’t have the targets the ABX is looking for → their structure ain’t right!
Mycoplasma + B-lactam ABX → lack of cell wall
Penicillin G + Enterobacteriaceae → tiny channels and lipid layer won’t allow PG to enter
Obligate anaerobes are resistant to aminoglycosides (active transport requires oxygen → anaerobes don’t have that system)
What type of resistance is related to previous ABX exposure?
Acquired
What is acquired resistance? Examples?
Bacteria become resistant to ABX via mutations in uptake system and targets
Staphylococci + Penicillin G → make enzymes that inactivate ABX (penicillinase/beta-lactamase)
What is the mechanism of acquired resitance?
Alter drug target
Modify target site (Ex. methylation of rRNA changes macrolide binding site on 50S ribosomal subunit)
Reduce target site → alternative pathways so ABX doens’t change their function (ex. alternative folic acid synthesis pathway)
Alter drug uptake
Inhibit uptake → decrease pore size so ABX is too big
Increase excretion of ABX (tetracyclines)
Inactivate Drug
Enzymes (ex. beta-lactamases, make into anti-binding form)
How is bacteria resistant to multiple drugs?
Multi-ABX resistance
Different resistance mechanisms = different classes
Ex. Resistance to aminoglycosides (altered ribosomal protein) and penicillin (via beta-lactamase production)
Cross-resistance
Resistance due to the same mechanism = same class
What does it mean that cross-resistance is unidirectional?
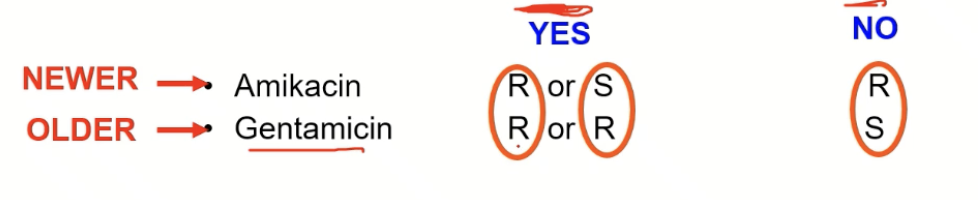
Resistance in older class drug means that the bacteria could be sensitive or resistant to new class drug BUT
Resistance in newer class drug means that the bacteria MUST be resistant to older class drug
How to bacteria acquire resistance?
DNA Mutation
Acquisition of new DNA with mutations
What type of mutations results in antibiotic resistance and what is required?
Selective Advantage Mutations
Must have ABX present → “Selective Pressure”
Describe the different kinds of mutations that can cause bacteria to be resistant (or not) to ABX
Most mutations are lethal → bacteria dies
Mutations can give them
disadvantages (die out over time)
no advantage
selective advantage (become dominant type → ABX resistance)
Describe how bacteria acquires mutations from other bacteria
Genetic transfer → between strains → genetic diversity
Conjugation → plasmid transfer via sex pilli
Transduction → transfer through virus, bacteriophage delivers viral genes which are integrated into chromosome
Transformation → free genes in environment from dying bacteria (least effective)
What type of mechanism is responsible for multi-antibiotic resistance?
Genetic Transfer between bacteria
Besides antibiotic resistant genes, what can bacteriophages also introduce into the bacterial chromosome?
Virulence factors
What mechanism allows multiple antibiotic resistance genes to be introduced to bacteria?
Conjugation
What mechanism is more common in gram negative bacteria? Why?
Conjugation → gram + doesn’t have sex pillus and has a thick peptidoglycan layer
What should we consider when selecting an antibiotic?
Gram + or -?
Route
Historical data
In vitro sensitivity
ABX sensitiivty testing
What ABX are used for gram - vs. gram + bacteria?
Positive = Penicilin
Negative = Gentamicin
What ABX are used for rickettsia?
Tetracyclines
What ABX are used for Streps?
Penicillin
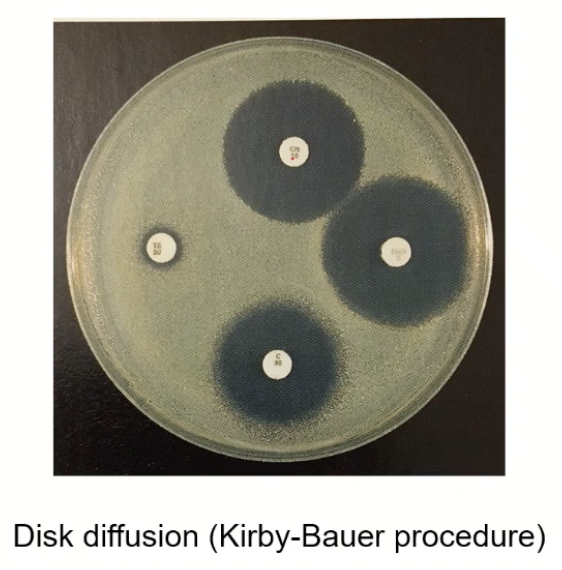
How does Kirby Bauer determine ABX sensitivity?
Spread bacteria on plate
Put a disk of ABX on there → not able to grow by ABX = not resistant
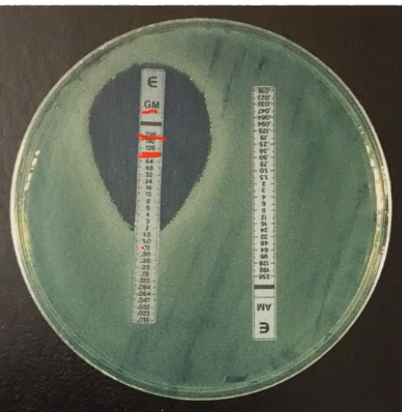
How does E Test determine ABX sensitivity?
Spread bacteria on plate
Strips have different levels of ABX in them
Able to see minimum concentration inhibiting bacteria
How does Broth Dilution Method determine ABX sensitivity?
Dilute ABX across a bunch of tubes
Add same amount of bacteria to each one
See what dilution the bacteria doesn’t grow
Able to see minimum concentration inhibiting bacteria