Week 11: Physical Changes Associated with Aging
1/24
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
25 Terms
Aging Immune System (things that happen) (5)
Amount of active bone marrow decreased → lower production of leukocytes needed for function of immune system.
Innate (non-specific) immunity declines
Thymus gland (maturation of T-cells for adaptive specific immunity) regresses making T-cells less effective.
Ability to make antibodies (B cells) decreases
Low-grade inflammation increases with age
Aging Immune System (effects) (5)
Increased vulnerability to infections → influenza and pneumonia
Cancer is more common
Vaccines are less effective
Slow wound healing
Inflammation increases risk of other diseases: Alzheimer’s disease, diabetes, atherosclerosis, arthritis
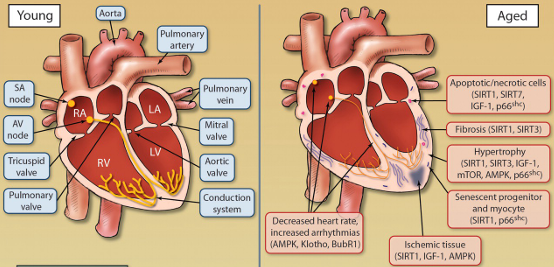
Aged heart (4)
Greater stiffness/rigidity of heart muscle
Increase in thickness of heart walls
Decreased HR and possible arrhythmias
Heart fills with blood more slowly
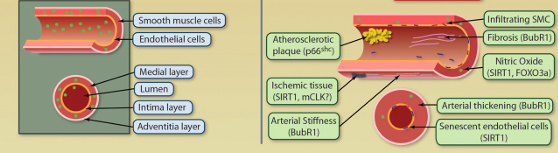
Blood vessels
Increase in thickness and stiffness in arteries
Decrease in lumen (opening)
Accumulation of plaques in arteries (atherosclerosis - normal part of aging)
Aging Cardiovascular system (effects) (6)
Increased BP
Maximum heart rate decreases
Reduced blood flow to cells and tissues
Normal older heart functions well under moderate activity
Slightly less able to tolerate increased physical exertion or other stressors (illness, infections, injuries, emotional stress)
Decrease in performance of elite athletes
Disorders in Aging Cardiovascular System
Cardiovascular diseases (atherosclerosis: fibrous plaques full of lipids, WBCs, platelets) and hypertension
Increased risk for heart attack (acute myocardial infarction), stroke
Stages of plaque development
Plaque build up begins when endothelial artery cells are damaged- excess cholesterol particles collect beneath these cells.
In response to damage, platelets and other cells collect at site, forming fibrous cap, isolating the plaque within the artery wall. Early-stage plaque is called a fatty streak.
Chemical released by cells in and around plaque cause further inflammation and build-up. Advanced plaque has (LDL, white blood cells, connective tissue, smooth muscle cells, platelets)
Narrowed artery is vulnerable to blockage by clots. The risk of blockage and heart attack rises if fibrous cap cracks (due to destructive enzymes released by white blood cells)
Aging Respiratory system (what happens) (5)
Stiffening of CT in lungs
Muscles of breathing (diaphragm) weaken
Number of functional alveoli and capillaries in lungs decrease
Number and activity of cilia declines
Weaker cough
Aging Respiratory system (effects) (5)
Decrease in maximum breathing capacity
More difficult to expand lungs to full volume
Less able to clear mucus
Less able to fight respiratory infections
Daily activities not affected, exercise becomes more difficult
Secondary aging (related to respiratory system)
Increase in chronic lower respiratory diseases (COPD, Emphysema)
Aging Muscular System (5) caused by what + sarcopenia
Decrease in muscle mass (greater loss in fast-twitch than slow-twitch muscles) (10-15% decline)
Decrease in contractile force
Sarcopenia - severe loss of muscle from disease or inactivity, increased fatigue and risk of falls
Caused by decreases in GH and testosterone (in men)
Decreased motor performance in athletes
Fast-twitch v Slow-twitch muscles
Fast-twitch - speed and explosive strength
Slow-twitch - endurance muscles
What can delay loss in mass and strength
Regular resistance training
When is atrophy reversible?
If atrophy due to disuse → reversible
If atrophy due to sarcopenia → non-reversible
Loss in Bone Density (6)
Reduction in thickness of compact bone
Reduction in number and size of trabeculae in spongy bone
Osteoclast activity > osteoblast activity
Menopause and decrease in estrogen accelerates loss for women
Loss in calcium → body absorbs less
Bones most affected are ends of femur at hip, end of arm bones at wrist, and bones of spine (vertebra)
Bone loss with aging
Bone density peaks at about 30 years of age. Past peak, the rate of resorption exceeds rate of bone formation. Women lose bone mass more rapidly than men.
Osteroporosis
Osteoporotic bone is thin, porous, and fragile. Leads to easier fractures.
Aging Bones and Joints (what happens)
Cartilage that lines joints thins and cracks (wear & tear)
Leads to degenerative joint disease - osteoarthritis (inflammation, pain, and stiffness in joints.
Ligaments (bind joints together) and tendons (bind muscle to bone) stiffen and weaken
Aging Bones and Joints (effects)
Increase risk of fracture
Increase risk of tearing of ligaments
Stiffness
Decrease in height
Mobility problems and frailty in severe cases
Changes in endocrine system
Production and secretion of hormones decreases
Somatopause - steady decline in GH and IGF-1 levels with age
Decrease in insulin sensitivity and decrease in insulin secretion → blood glucose levels spike quickly and take longer to recover
Changes in secretion of sex hormones
Why does the production and secretion of hormones decrease as we age?
Result of decreased blood flow and vascularization and increase in connective tissue in endocrine glands.
Type II Diabetes
Cells become resistant to effects of insulin
Beta cells cannot keep up, leads to hyperglycemia
Early symptoms - excessive urination and thirst, fatigue, blurred vision
High glucose levels damage tissues - blood vessels & nerves (atherosclerosis, kidney damage and failure, blindness, and reduction in circulation to limbs and neuropathy)
80-90% of people with T2D are overweight/obese
Diabetes increases risk of heart disease and stroke
Climacteric
Climacteric - fertility decline in men and women
Andropause
Type of climacteric for men.
Gradual decline in testosterone but minimal effect on fertility until very old age.
Menopause
Climacteric for women.
End of menstruation and reproductive capacity (early 50s)
Oocyte atresia → no follicles left to respond to FSH and LH to produce estradiol
Perimenopause (40s), in which cycles become irregular and anovulatory
Estradiol and progesterone decrease, FSH and LH increase (no negative feedback from estrogen or progesterone)