Clinical Path exam 3
1/70
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
71 Terms
Cystitis/urethritis (UTI)
Cystitis (inflammation of the bladder), Urethritis (inflammation of the urethra)
S/S: bacteriuria, cloudy/bloody urine, dysuria
Renal calculi (kidney stones)
Common cause of urinary obstruction; concentration of various mineral salts in the renal pelvis or the calyx
S/S: excruciating pain in the flank and upper outer quadrant of the abdomen on the affected side, nausea, vomiting, chills and fever, hematuria, abdominal distention
BPH (Benign Prostatic Hyperplasia)
Enlarged prostate
S/S: urinary obstruction, nocturia, dribbling, urinary frequency, hematuria, weak urine stream, and incontinence
Tx: “watchful waiting” then alpha blocker medication to shrink the prostate
Prostatitis
Inflammation of the prostate gland (can be acute or chronic)
S/S: low back pain, pain in pelvic region, perineal fullness or pain, fever, dysuria, hematuria, and urinary frequency and urgency
Tx: antibiotic
Epididymitis
Inflammation of the epididymis due to infection
S/S: epididymis enlarged, hard, and causing pain, scrotal and groin tenderness, fever, and malaise
Tx: antibiotoic
Testicular torsion
a medical emergency occurring when a testicle twists on the spermatic cord, cutting off the blood supply
S/S: sudden, severe scrotal pain, swelling, and nausea
Tx: immediate surgery
Ovarian cysts/tumors
Benign cysts of the ovary are derived from ovarian follicles that do not break open to release the egg
S/S: Some cysts are asymptomatic. Large can have pelvic pain, low back pain, and dyspareunia. Cysts that are mobile can twist, producing spasmodic abdominal pain
Watchful waiting
Endometriosis
Appearance and growth of endometrial tissue in areas outside of the endometrium, the lining of the uterine cavity
S/S: Dysmenorrhea with lower back and vaginal pain, Pain at the ectopic site during menses. Clients might have profuse menses, infertility, dyspareunia, dysuria, and even painful defecation
Pelvic inflammatory disease
infection of the uterus, fallopian tubes, or ovaries
S/S: no symptoms, while serious damage is being done to reproductive organs. acute: sudden pelvic pain, foul-smelling vaginal discharge, fever, sexual dysfunction, metrorrhagia (abnormal uterine bleeding), and rebound pain.
Polycystic ovary syndrome (PCOS)
Numerous cysts in the ovaries disrupt the monthly reproductive cycle
S/S: irregular menstrual periods, excess hair growth, and obesity, enlarged polycystic ovaries, infertility, pre-diabetes or type 2 diabetes, hypertension, sleep apnea, amenorrhea or irregular menses
Menstrual disorder (amenorrhea, dysmonorrhea and menopause)
Amenorrhea - the absence of menstruation
Dysmenorrhea - painful, crampy menstrual periods, affecting the lower abdomen, back, or thighs.
Menopause - not a disease, but can be a RF for osteoporosis, HTN, high cholesterol, depression
Breast Cancer
Occurs when breast cells mutate and grow uncontrollably, often forming tumors
S/S: breast thickening/lump, pain/swelling in armpit, breast size change, nipple discharge/irregular shape/crustiness, skin changes (dimpling)
Testicular/prostate cancer
Prostate cancer - S/S: dysuria, nocturia, frequent urination, low back pain, hematuria, bone pain, erectile dysfunction, weakness/numbness in legs and feet, incontinence, weight loss
Testicular cancer - S/S: lump/swelling in the testicle (may be painless), breast growth/soreness; LBP, SOB, abdominal pain in advanced cases
Hyperpituitarism/hypopituitarism
Hyperthyroidism/hypothyroidism
Hyperparathyroidism/hypoparathyroidism
Cushing syndrome - adrenal dysfunction
Too much cortisol
Enlargement
weight gain
waist weight gain
stretchmarks
Addison syndrome - adrenal dysfunction
A lot of atrophy
muscle weakness
GI issues
Hyperpigmentation (darkening of skin)
Diabetes mellitus
pancreatic dysfunction (insuffiicnet insulin poduction or inadequate utilization of insulin)
Diabetes mellitus - Type 1
immune-mediated
Abrupt onset, earlier in life
Diabetes mellitus - Type 2
age related
gradual onset, later in life
Gestational diabetes
hormonal changes d/t pregnancy
cut off of supply to the pancreas
Consequences/comorbidities of DM (untreated)
Chronic kidney disease, renal failure
Diabetic neuropathy
Cardiovascular diseases (including hypertension)
Diabetic retinopathy (and blindness)
Build-up of pressure in the eye because of blood glucose
Comorbidities
PCOS
thyroid dysfunctions
hyperlipidemia
obesity
psychological disorder
celiac disease and other GI complications (gluten sensitivity)
Diagnosing DM
Non-fasting sugar test >200mg/dL (normal before meal is 70-130 mg/dL; post-meal normal is <180 mg/dL)
Fasting blood glucose test >126mg/dL (normal is 70-100 mg/dL)
A1C >6.5% (normal is below 5.7%)
(A1C is how much sugar is included in hemoglobin part of RBC)
Diabetes Tx & Management
Medications
Insulin (for sure for type 1)
Metformin and others for lowering blood glucose levels (T2DM)
Cholesterol-lowering medication
Exercise, diet, and other lifestyle/habit modification
Regular assessment of blood glucose and A1C
Preventing hypoglycemia and hyperglycemia
Metabolic acidosis - pH, S/S
pH<7.35
Accumulation of ketones and lactic acid, renal failure, drug/toxins, GI issues (diarrhea)
Metabolic alkalosis - pH, S/S
pH>7.45
Prolonged vomiting (acid loss), hypovolemia, diuretic use, hypokalemia
(pH is increased bc of vomiting)
GERD (gastroesophageal condition)
Malfunction of the lower esophageal sphincter
S/S: heartburn, regurgitation, nausea
Peptic ulcers (gastroesophageal condition)
Mucous membrane lesion due to excess acid, H. pylori infection, excess NSAID use
S/S: bloody stool, lack of appetite
Gastroenteritis (chronic gastroesophageal condition)
No specific cause, but stress, food ant other habits RFs
S/S: intermittent abdominal pain without bowel issues
Celiac disease (intestinal condition)
gluten-induced enteropathy - an autoimmune disorder affecting the villi (absorption ability is affected)
S/S: flatulence, bloating, loose bowel, indigestion, nausea/vomiting, anemic osteoporosis, dry/itchy skin, weight loss
IBS
3 types of inflammatory bowel disease: diverticulitis, crohn’s, ulcerative colitis
Diverticulosis, diverticulitis
Bulging pouches (diverticula) cause issues when inflamed or rupture
S/S: fever, pain (may be relieved by bowel movement), constipation/diarrhea, muscle spasm
Crohn’s disease
Chronic inflammation causing intenstinal wall (all layers) to thicken/toughen
Mix of healthy and diseased sections
S/S: RLQ pain, diarrhea, appetite loss
ulcerative colitis
Chronic inflammation of the mucosal lining of the colon
S/S: bloody diarrhea, abdominal pain, urgency for bowel movement, fever, dehydration
Pancreatitis
Cholecystitis, cholelithiasis
Acute inflammation of the interior wall of the gallbladder
Lasting URQ pain, nausea/vomit, low-grade fever, lack of appetite
Cirrhosis
Chronic degenerative disease of the liver; build-up of fibrotic scar tissues
Various causes (alcohol, diet, toxins, CHF, hepatitis)
S/S: nause/vomiting, lack of appetite, dull abdominal pain, weakness/fatigue, pruitus, edema and ascites, jaundice, neuritis
Hepatitis (A, B, C) liver condition
Necrosis of liver cells
A: acute infection; fecal-oral route infection; vaccine present
B: blood/serum transmission; more serious than A; vaccine present
C: chronic infection; blood transmission; high risk for cirrhosis and liver failure; vaccine not present
Flu like symptoms: dark urine; clay colored stools; pruitis/hives, nausea, vomiting; loss of appetite; pain; jaundice
Appendicitis (acute)
*Perforation is life-threatening
S/S: Local LRQ pain (McBurney point), rebound tenderness, rigidity, muscle spasms, constipation, fever and malaise (later)
Spleen injury (not in textbook)
MOI: blunt force trauma
Rupture is a medical emergency
Tx: depends on vascular supply; non-surgical preservation to splenectomy
Monitor for decreased immune function
Kidney functions
Waste removal
Body fluid, electrolyte, and pH balance
Hormone release for regulating blood pressure
Regulation of RBC production
Chronic kidney disease stages (1-5)
Stage 1 - normal, eGFR>90
Stage 2 - mild decrease, eGFR 60-89
Stage 3 - moderate damage, eGRF 30-59
Stage 4 - moderate/severe damage, eGFR 15-30
Stage 5 - severe damage/failure, eGFR <15, aka end-stage renal disease or ESRD
Typical S/S of kidney disease
May remain asymptomatic until a more serious failure
Swelling in the body (face, extremities)
Foamy and brown urine
Sharp back pain (and tenderness at CVA)
Dysuria
Reduced urine volume
Itchy skin
Specific assessment (urinary, reproductive system conditions)
Pain in the CVA (costovertival angle), flank, or abdomen
Perineal, genital, groin, or low-back pain (common w/ ovary issues)
Painful intercourse
enlarged, painful nodes
abnormal discharge
Specific assessment - urine
Frequency of urination
Amount of urine, urgency
Dysuria - difficulty/pain w/ urination
Nocturia - having to pee at night
urinary retention - bladder isn’t empty all the way
Incontinence - cannot hold pee in the bladder
Change in color and odor of urine (including blood)
Stones or sediment in urine
Systemic issues (fever, chills, excess sweat)
Abnormal colors of urine: Pink/red
kidney disease, tumors, UTI, prostate problems, lead or mercury poisoning, trauma causing internal bleeding (rhabdomyolysis - could be brown)
Abnormal colors of urine: orange/brown
Liver disease, porpuria (genetic disorder), bile duct issues, severe dehydration
Abnormal colors of urine: green/blue
Bacterial infection, bilirubin (too much excreted in body)
Abnormal colors of urine: bright yellow
Excess bilirubin (bile production), vitamin B supplement
USG (hydration status)
Urine specific gravity
measured through a refractometer
USG <1.010: hydrated
USG > 1.020: dehydrated
Dipstick analysis
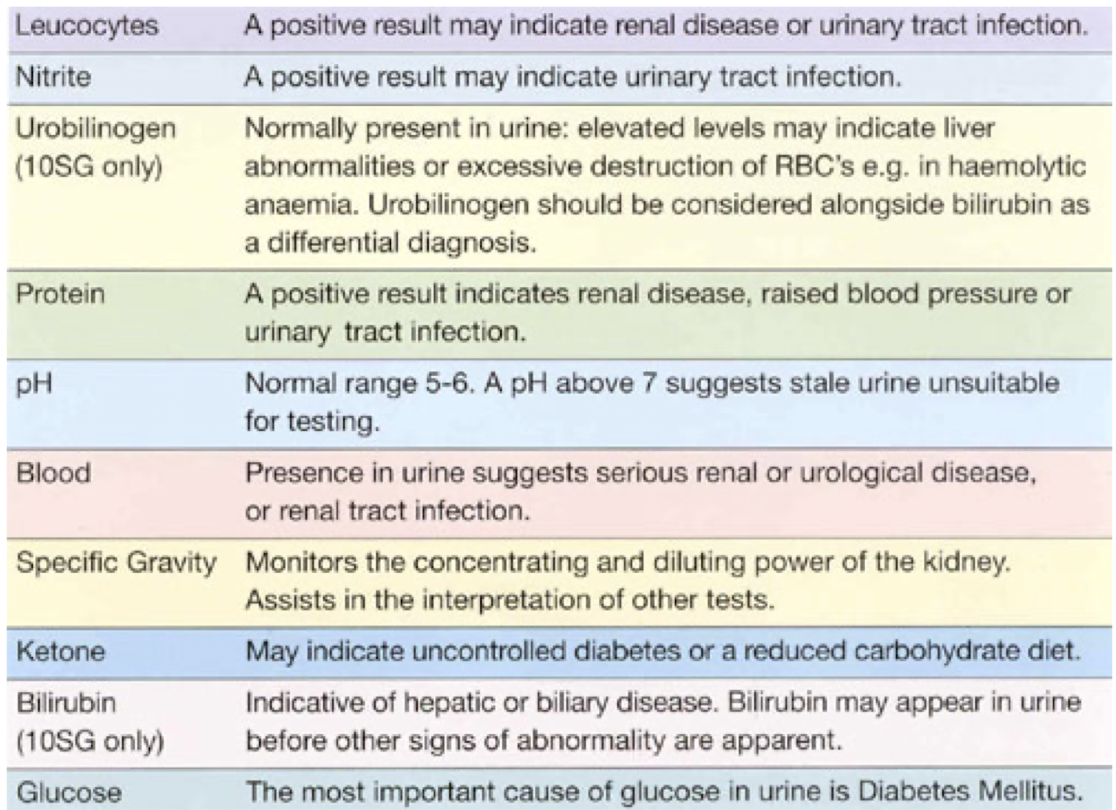
Endocrine dysfunctions
Lack of hormone production
Excess of hormone production
Dysfunctions of the target organs
receptor malfunction
Other diseases and mediation that contribute to above diagnoses
Common issues associated with endocrine dysfunctions
decreased energy level, increased fatigue
Intolerance to heat or cold
Changes in sexual function
development of 2nd degree sex characterics
changes in mood and ability concentrate
changes in memory and sleep patterns
weight changes
hypotension or hypertension
diminished or excessive growth
Immune system disruption
Thyroid gland (T3 and T4 - triiodothyronine and thyroxine)
Protein synthesis
Maintenance of BP, HR, digestion, metabolism, body temp, brain functions and reproductive functions
Thyroid gland (calcitonin)
Ca2+ regulation can cause:
Over storing - kidney stones
Over release - osteoporosis
Parathyroid gland (parathyroid hormone - PTH), what does it do? possible tx?
Maintains normal blood calcium level via a negative feedback loop
possible tx: take a gland out… then might need to watch heart and keep an eye out for increased muscle injury…
Adrenal glands (cortex - cortisol, aldosterone, androgen)
Cortisol functions
Regulating blood sugar level for brain functions
Convert fat, protein, glucose to energy
Regulate BP and CV functions
Aldosterone
Targets the kidneys for maintaining a balanced blood Na+ level
Androgen
Secondary male sexual characteristics
Adrenal glands (adrenal medulla - Epinephrine and NE)
Fight or flight response
Epinephrine (adrenaline)
Increased HR, blood flow to muscles + brain
Increased blood sugar
Norepinephrine
Increased vasoconstriction - increased BP
Pancreas (insulin vs glucagon jobs)
Insulin (beta cells)
Reduce blood glucose (signal muscle, blood, and fat cells to absorb glucose)
Glucagon (alpha cells)
Increased blood glucose (activate the liver to release glucose)
Endocrine-Specific assessment
Family Hx
Frequency, hx of infection
diet + physical activity level
stress (hormones are regulated by the hypothalamus)
environmental factors
medication hx, supplement use
pregnancy, menopause
Endocrine “inspection” points
Hair - thinning, growth
skin - itchiness, darkness/redness, scaling, sweat
nails
eyes — deer in headlights (?)
tremors
breast development in men
body shape (fat distribution, atrophy, muscular tone)
deformity, swellling
General Tx for endocrine dysfunction
Medications (for treating symptoms)
Hormone replacement (e.g., insulin shots)
Surgical removal of affected glands
Side effects, consequences for above options
Monitored exercises and diet
dietary modifications
Addressing underlying cause or comorbidities
Alimentary canal
Open tract of major organs through which food travels from mouth → anus
Accessory organs
Secrete fluids into digestive tract to assist in digestion and absorption in nutrients
Functions of the digestive system
Food is INGESTED
Food is DIGESTED
Water and nutrients in food are ABSORBED
Undigested food is ELIMINATED
Digestive issue S/S that warrent emergency care
Vomiting bright red blood, black material (resembling coffee grounds)
Fever >101, accompanied by severe abdominal pain
Persistent vomiting (inability to keep any fluid down for 24-36 hours)
Unstable vital signs, altered mental status
Digestive system inspection
Typically with patient in supine position
Scars (hx of appendectomy, cholecystectomy)
bruising, discoloration
Swelling, distention, visible mass
Abdomen movement during regular breathing
Guarding (protective) position
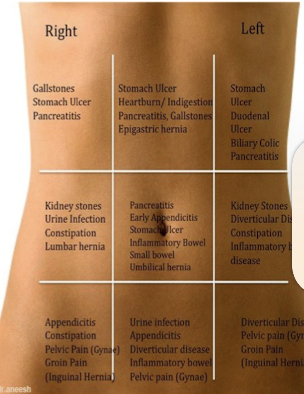
Abdominal Auscultation (normal vs abnormal)
Normal - some clicking and gurgling (also assess vascular sounds esp. abdominal aorta)
Abnormal - hyperactive, hypoactive, absence
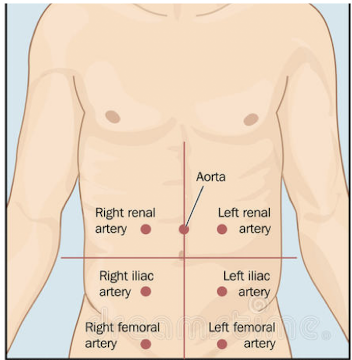
Abdominal percussion
Tympanic or resonant (high pitch, drum-like)
Over air-filled structures
Dull sounds (thuds)
Over solid or fluid-filled structure
Abdominal palpation
tenderness (rebound tenderness), rigidity
Superficial (light) vs deep
Spleen, liver, kidneys (especially CVA), appendix (McBurney’s point)