wound healing
1/20
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
21 Terms
risk factors for pressure injury
- Impaired sensory perception
- Impaired mobility
- Alteration in LOC
- Shear
- Friction
- Moisture
- Elevated body temperature
- Incontinence
- Diabetes
- Prolonged surgery
- Poor nutrition
- Advanced Age
- Anemia
stage 1 classification
intact skin with nonblanchable redness
usually over a bony prominence
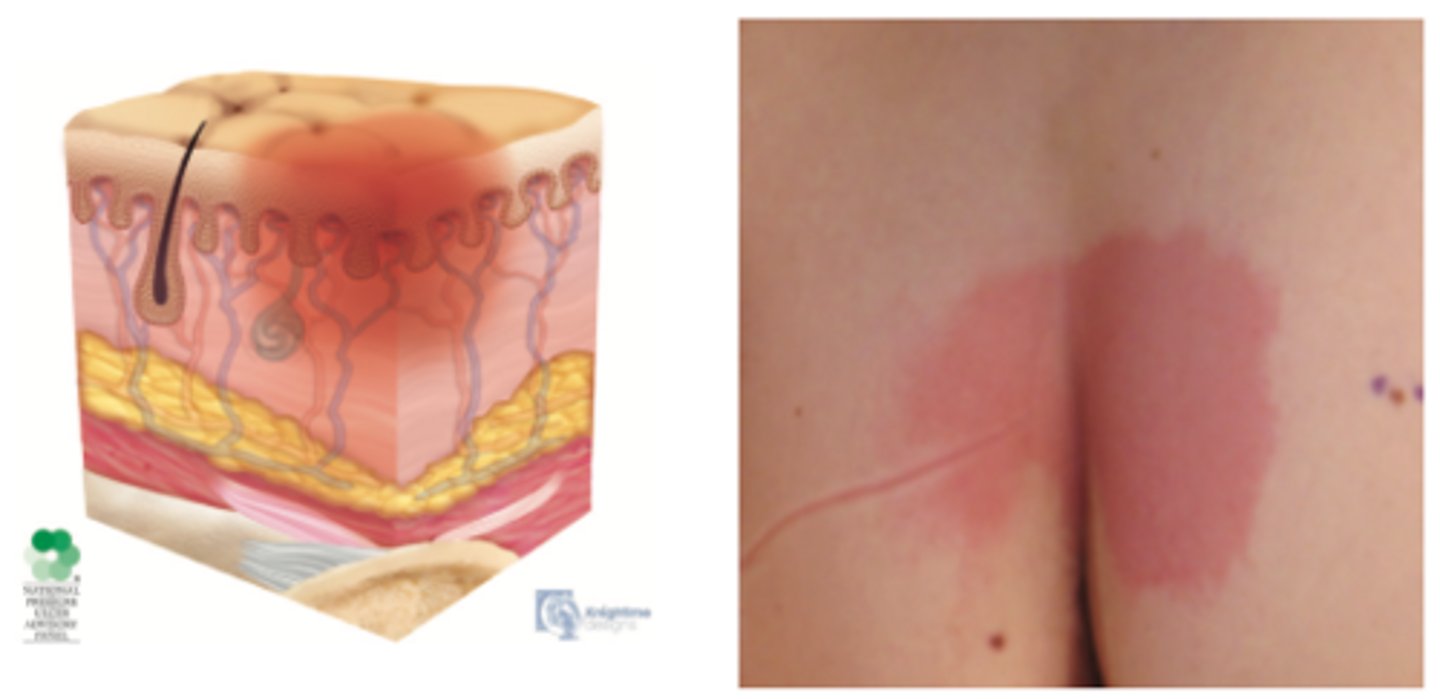
stage 2 classification
partial thickness skin loss involing epidermis, dermis, or both
Can present as an intact or ruptured serum-filled blister
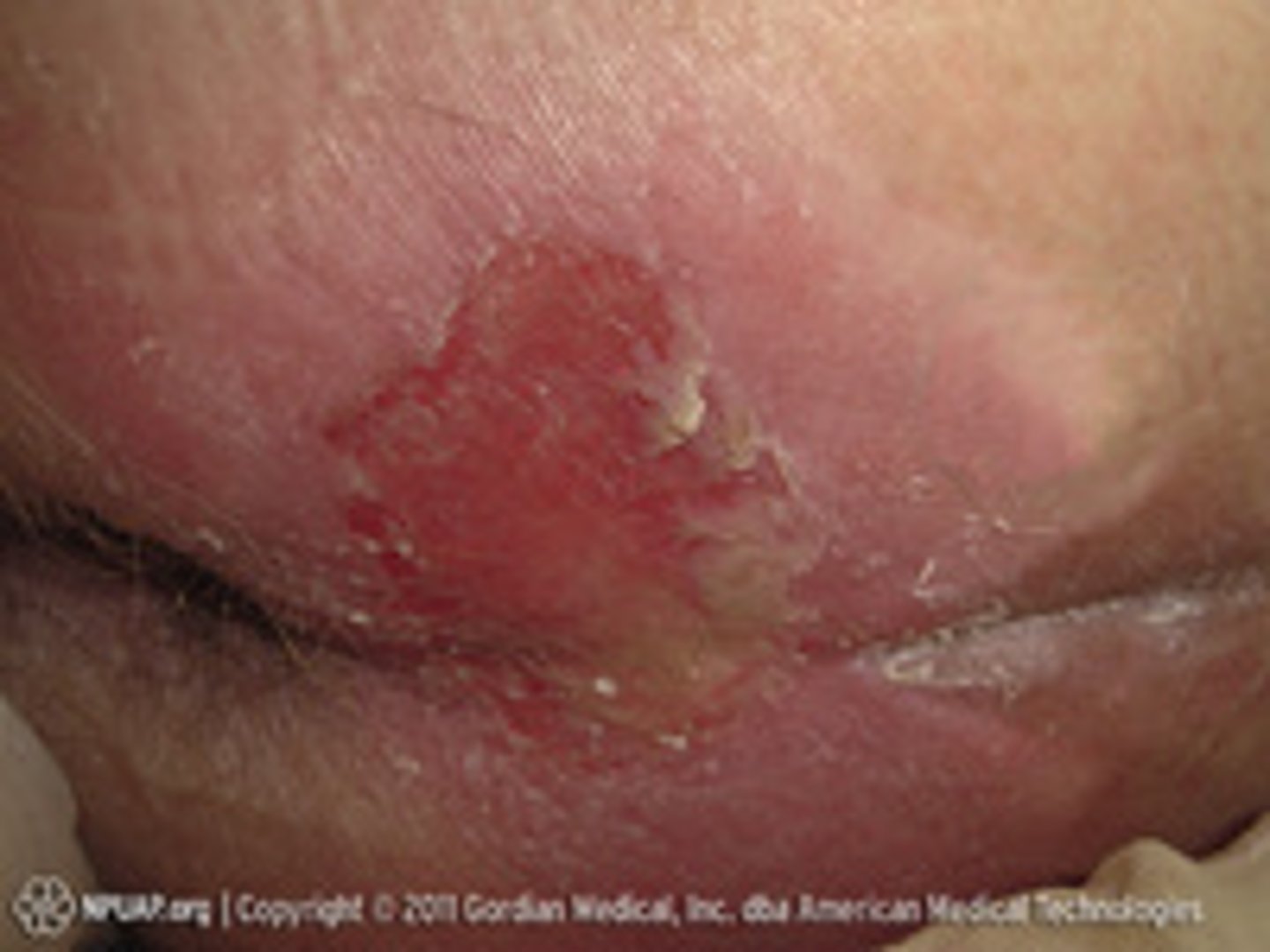
stage 3 classification
Full-thickness tissue loss with visible fat
deep crater
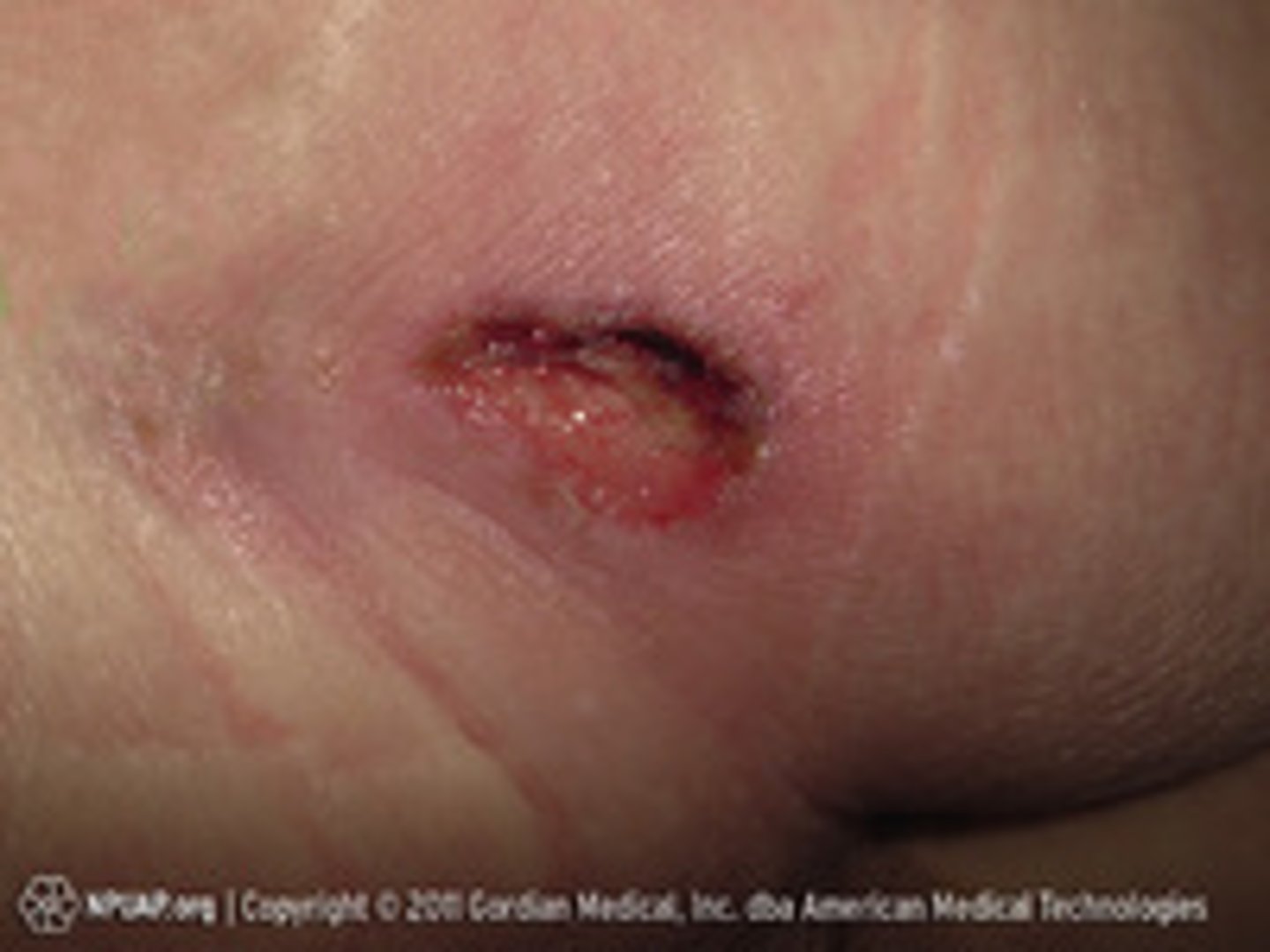
stage 4 classification
Full-thickness tissue loss with exposed bone, muscle, or tendon
Epibole, undermining and tunneling may occur
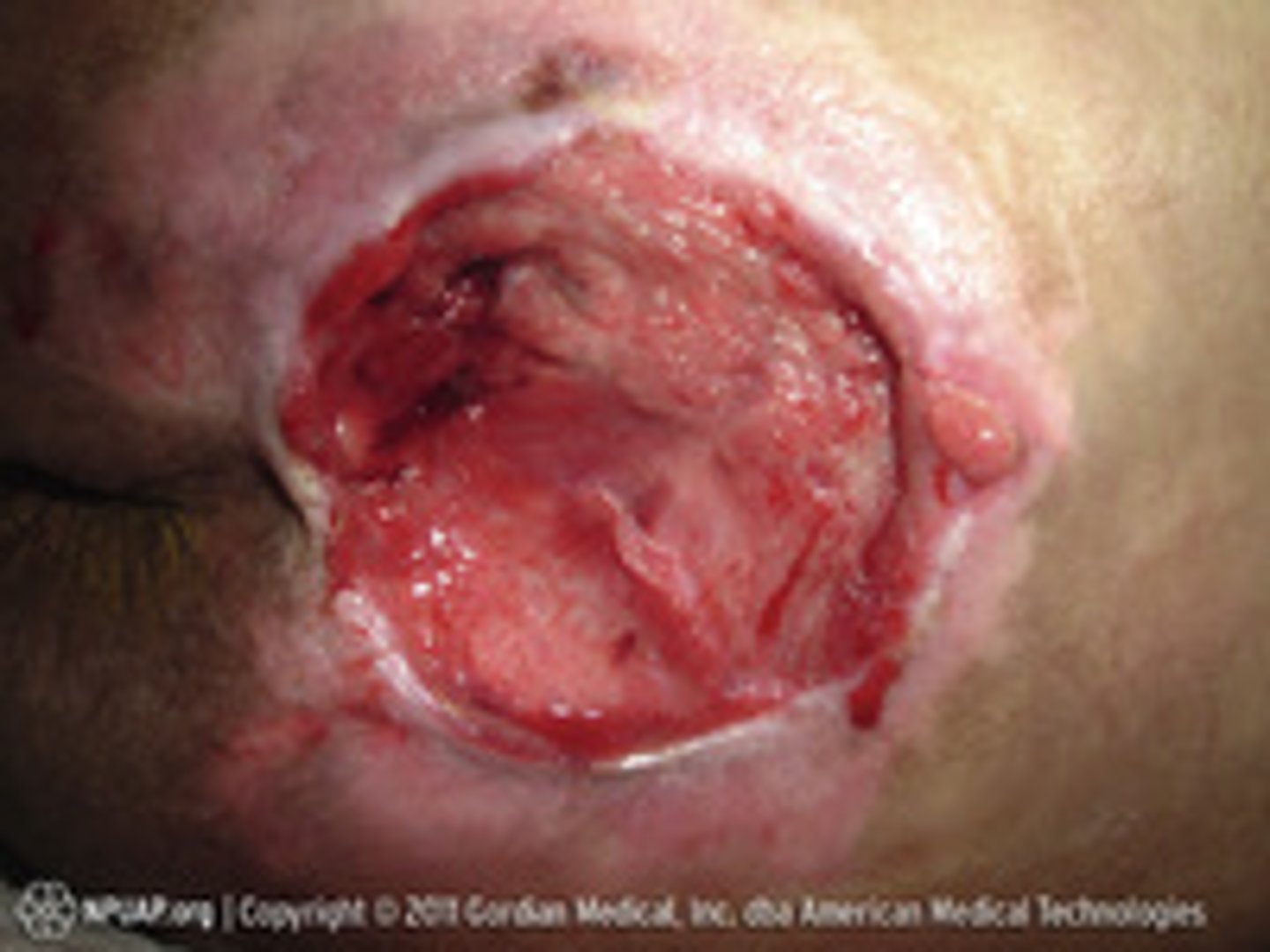
epibole
rolled wound edges
undermining
shelf, pocket, or lip is formed
separation of the wound edges from the surrounding healthy tissue
tunneling
narrow, tube-like channel extending in one specific direction
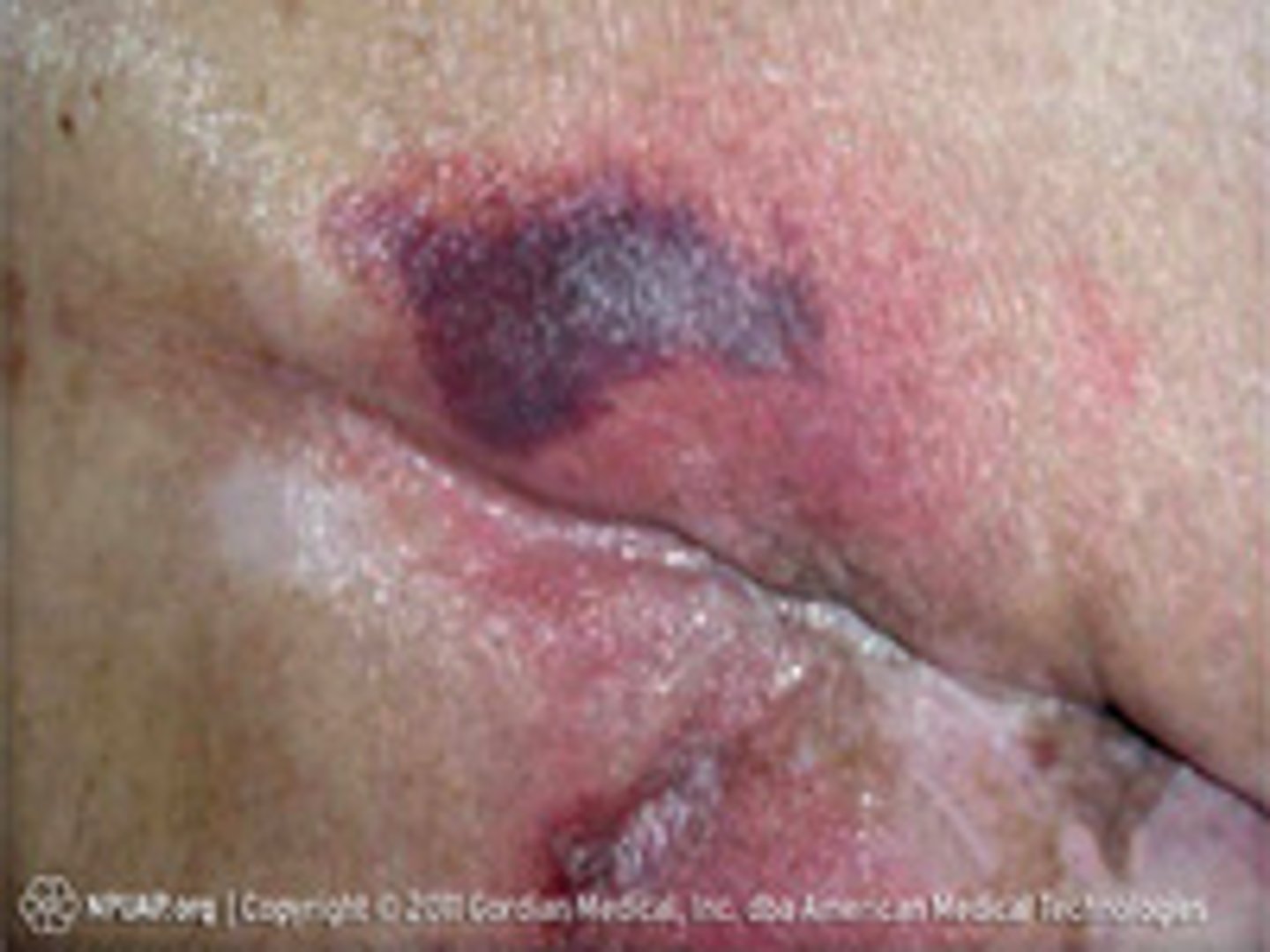
deep tissue injury
Purple or maroon localized area of discolored intact skin or blood-filled blister
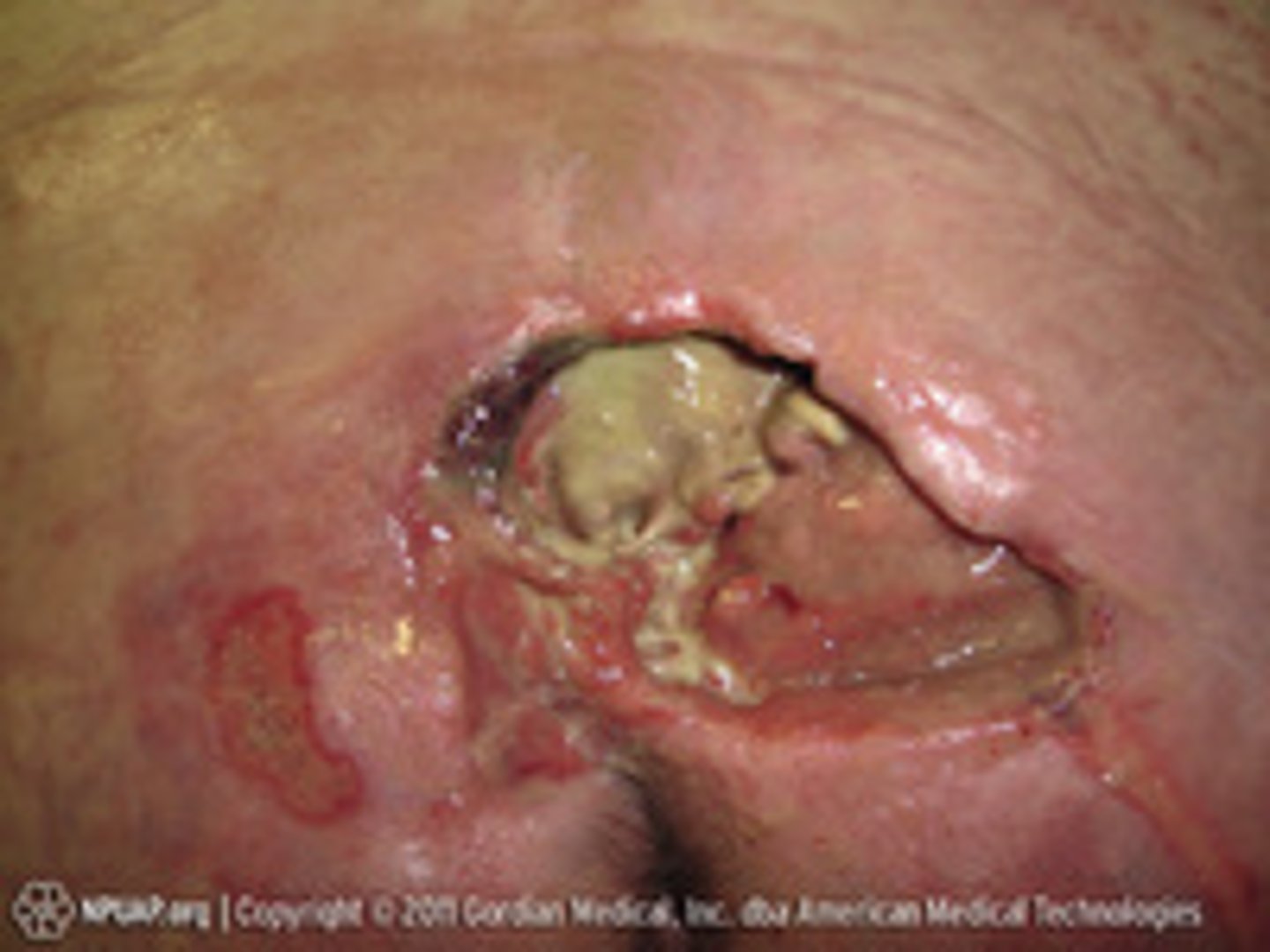
unstageable pressure injury
Full-thickness tissue loss in which actual depth of Injury is completely obscured by slough or eschar
healing process of full thickness wound repair
1. hemostasis
2. inflammation
3. proliferative
4. maturation
Medical-device related pressure injury
The resultant pressure injury generally conforms to the pattern or shape of the device.
The injury should be staged using the staging system.
Mucosal membrane pressure injury:
localized damage to mucous membranes caused by prolonged pressure, usually from medical devices like endotracheal tubes or nasal cannula
common in ICU patients
wound classification
- cause of wound (abrasion, laceration, puncture, skin tear)
- cleanliness of wound
- Descriptive qualities of the wound tissue such as color
- acute vs. chronic
- extent of tissue loss (full vs. partial)
secondary intention wound healing
not enough issue to bring together
tertiary intention
delayed healing of a wound that can be closed with sutures
wound healing for partial thickness
1. Inflammatory response
2. Epithelial proliferation and migration
3. Reestablishment of the epidermal layers
Complications of wound healing
- hemorrhage
- infection (likely 3-5 days post op)
- fistula formation
- dehisence
- evisceration
Factors influencing pressure injury formation and wound healing
Tissue perfusion
Inadequate blood supply
Anemia
Corticosteroid drugs
Infection
Smoking
Advanced Age
Obesity - adipose tissue is not vascularized, doesn't get nutrients
Diabetes
Psychosocial impact
nutrients necessary for wound healing
- calories (cell energy)
- protein (fibroplasia)
- vitamin C (collagen)
- vitamin A (epithelization)
- zinc (collagen formation, protein synthesis)
- fluid
braden scale
- Sensory perception
- Moisture
- Activity
- Mobility
- Nutrition
- Friction and shear
Low score = high risk for injury developing
High score = lower risk