Oral Medicine OSCE
1/117
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
118 Terms
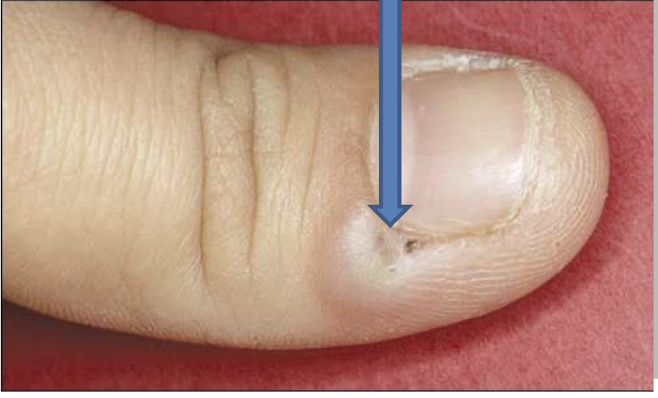
what is this lesion and how is it caused
herpetic whitlow
direct contact with an infected lesion without gloves
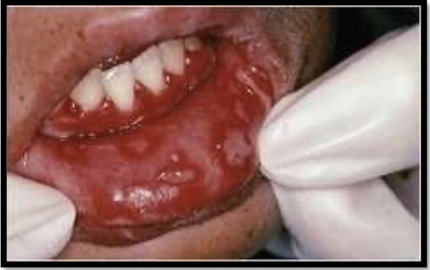
what is this lesion
acute herpetic gingivostomatitis
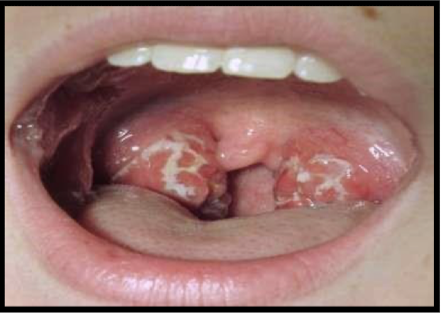
what is this lesion associated with and what are they called
acute herpetic gingivostomatitis
vesicles on the tonsilar pillars
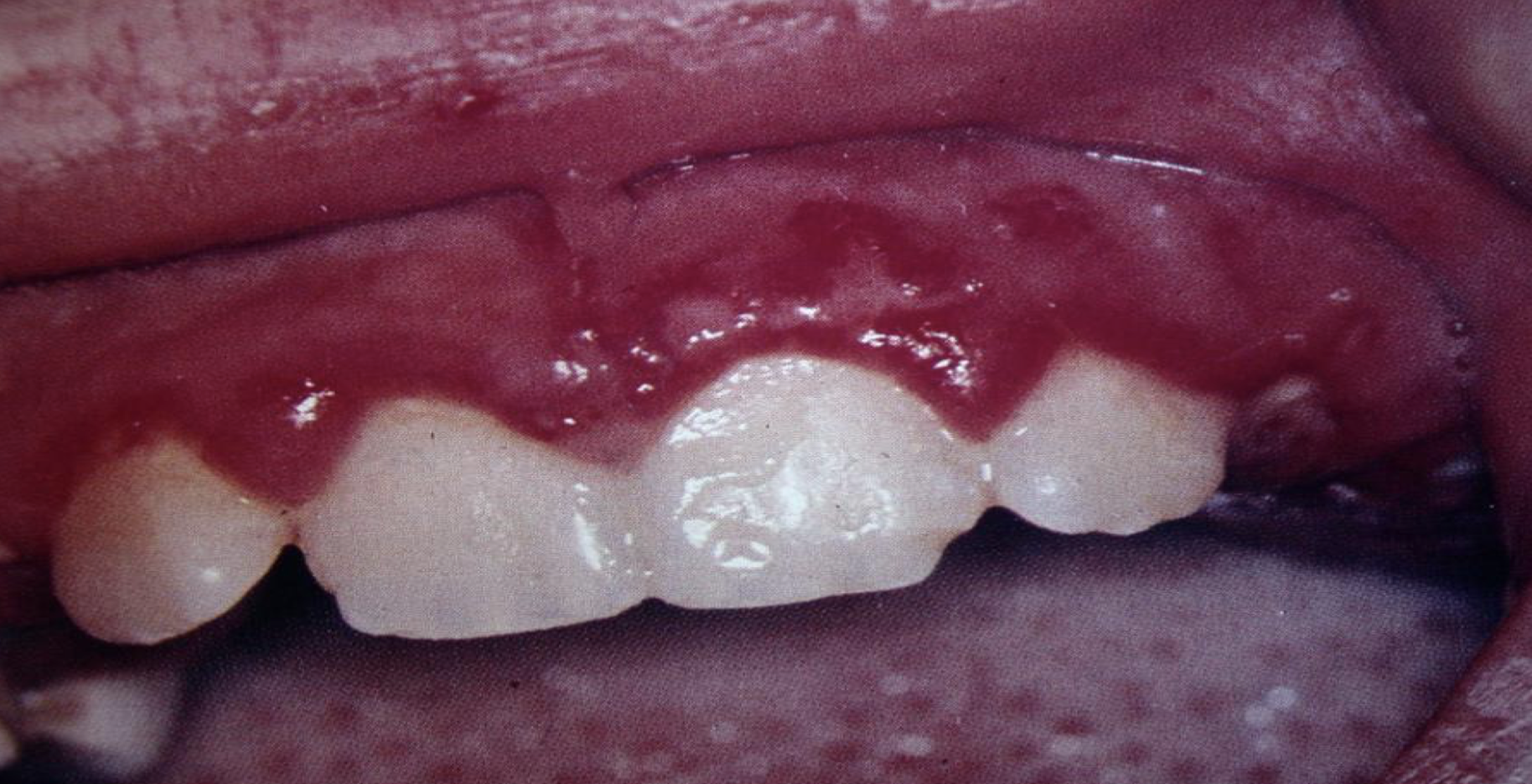
what is this lesion and what is it associated with
acute marginal gingivitis
HSV 1
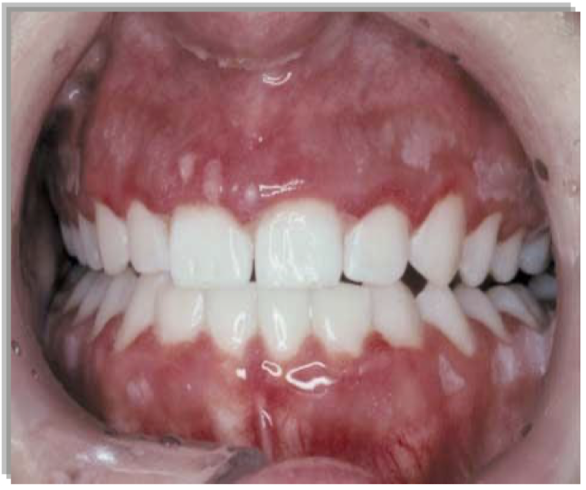
what is this lesion and what is it associated with
Acute marginal gingivitis
HSV-1
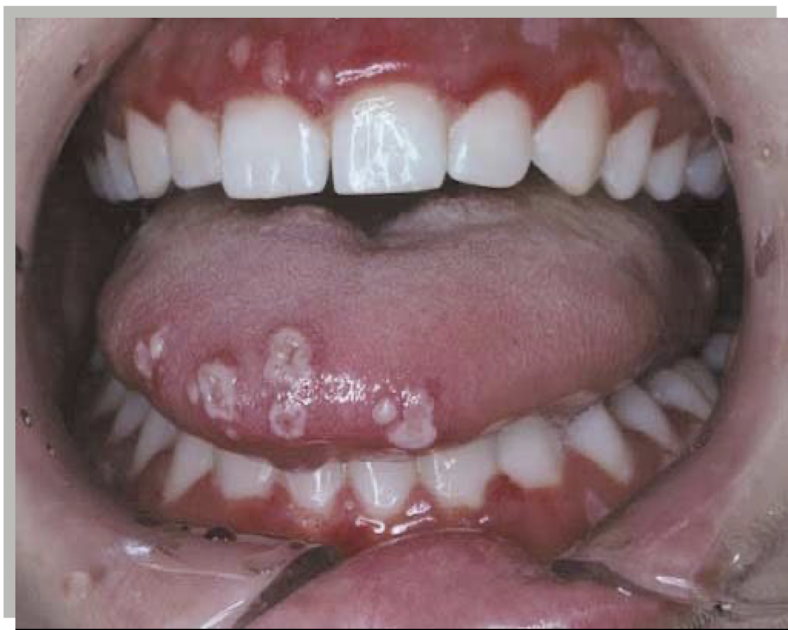
what is this lesion and what is it associated with
acute generalized gingivitis
HSV 1
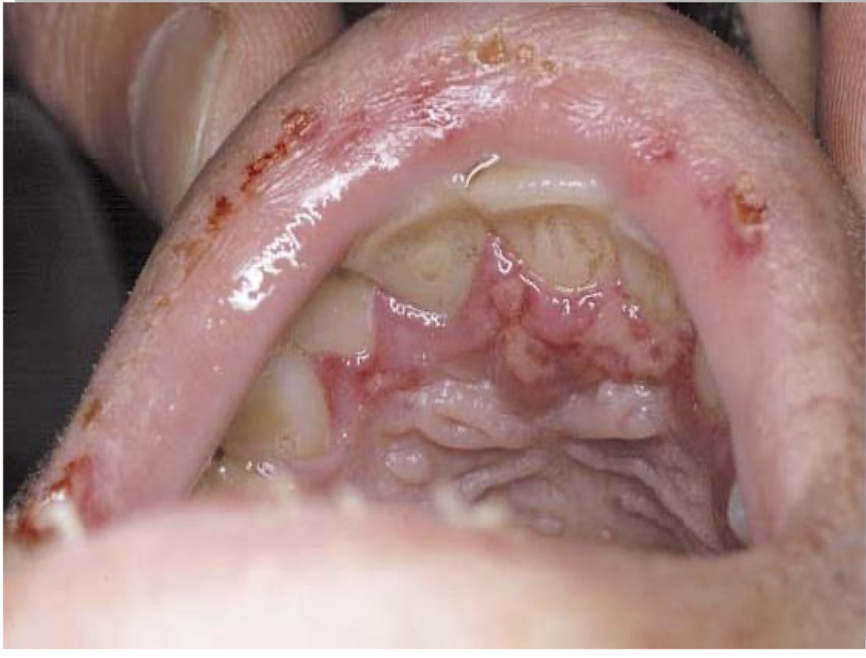
what is this lesion
recurrent intraoral herpes simplex
vesicles/ulcers
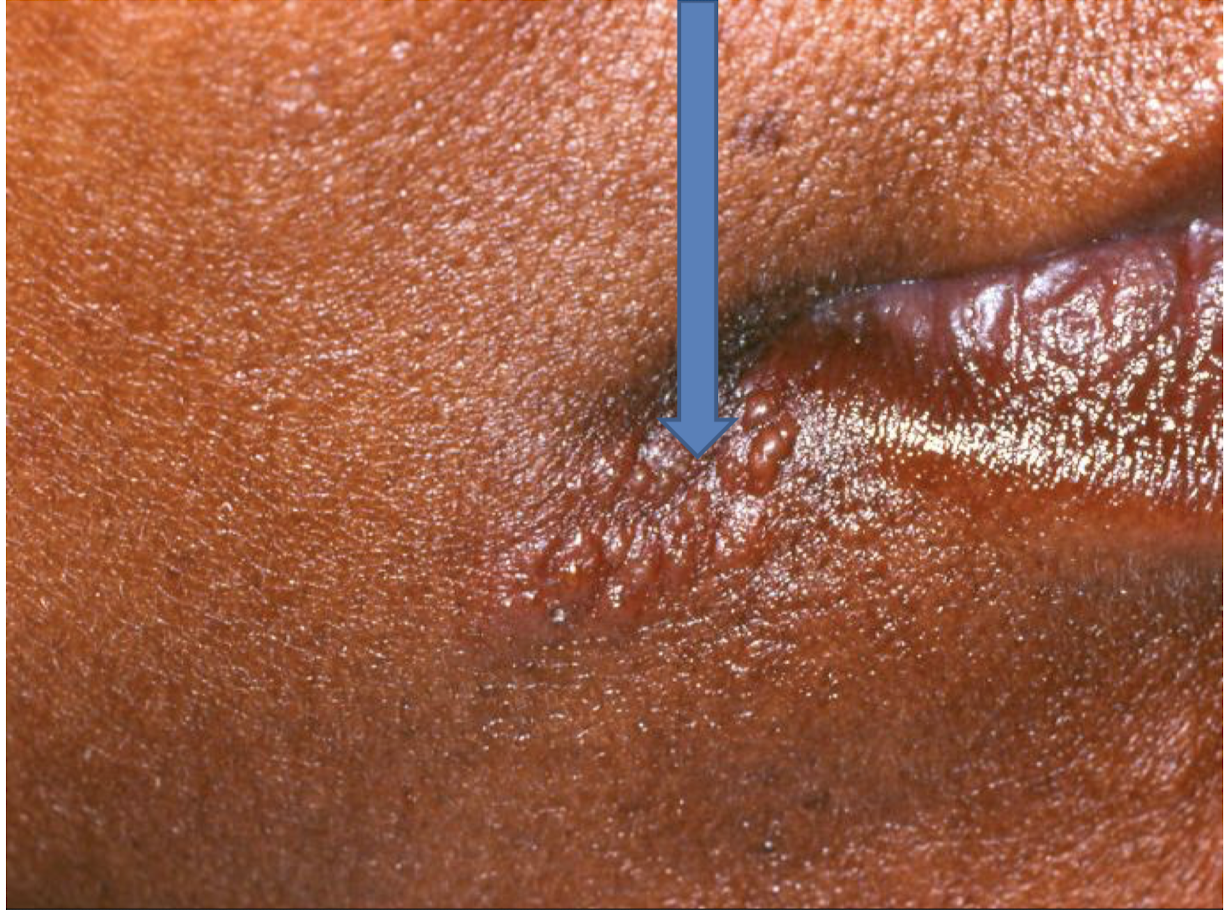
what is this lesion
herpes labialis
vesicles
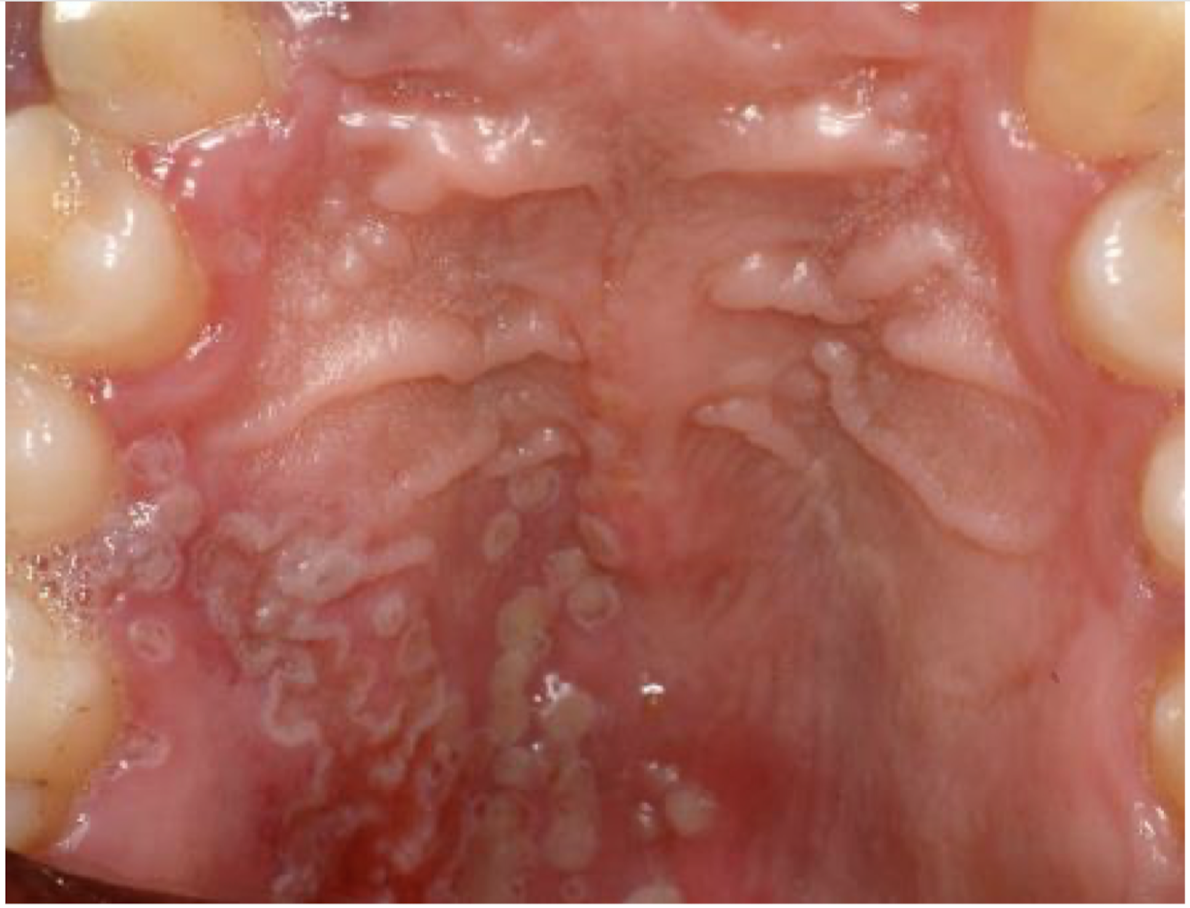
what is this lesion
recurrent intraoral herpes simplex
vesicles
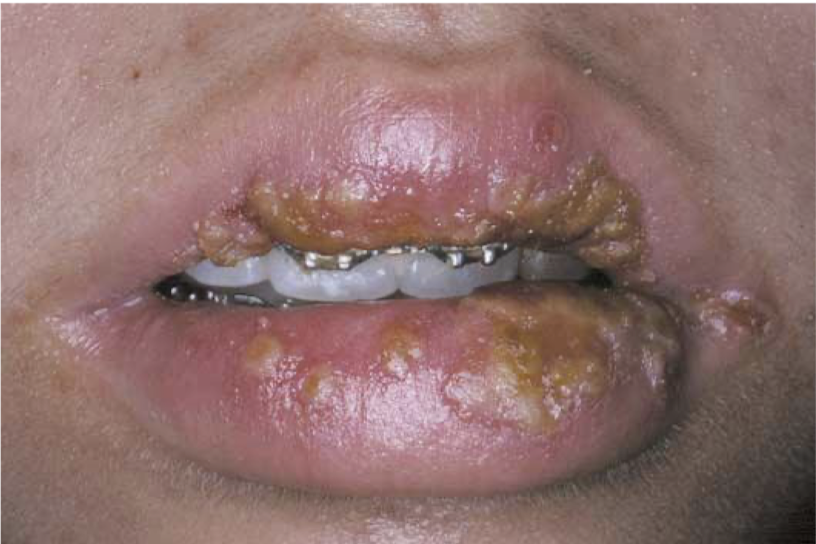
what is this lesion associated with and how did it form
recurrent intraoral herpes simplex
coaslesced vesicles
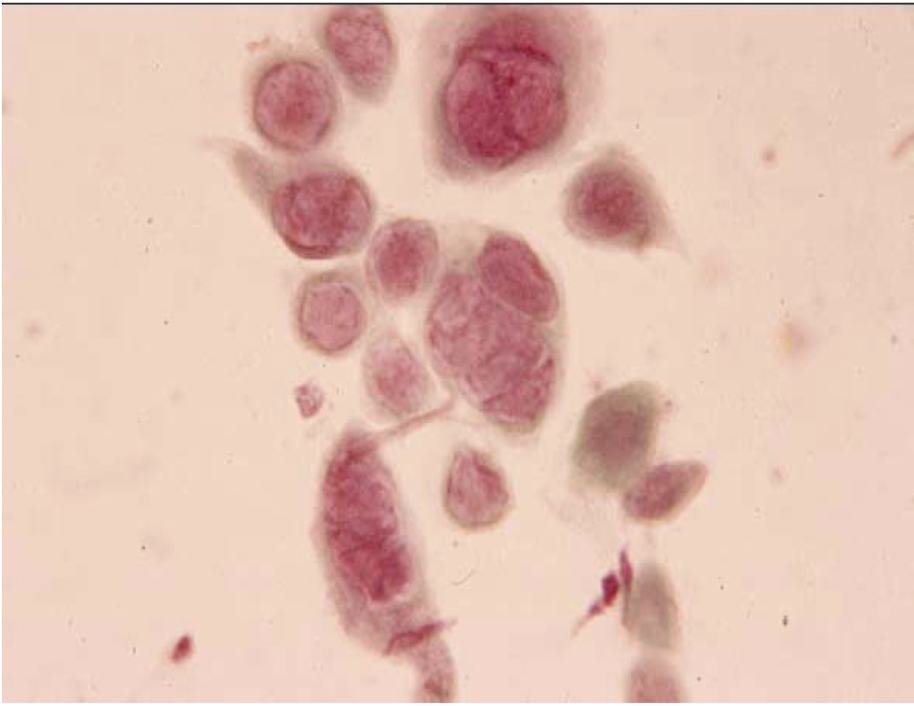
what are these cells called and which disease can you see these cells
multinucleated giant cells
herpes simplex virus

what is this medicine used for and what is the dose
herpes simplex virus
Acyclovir suspensions/ cream 5g 5 times a day

what is this medicine used for and what is the dose
Acyclovir (Zovirax) - Herpes simplex virus
400 mg TID (3x a day) × 7days

what is this medicine and what is the dose
penciclovir 1% - Herpes Simplex Virus
every 2 hours
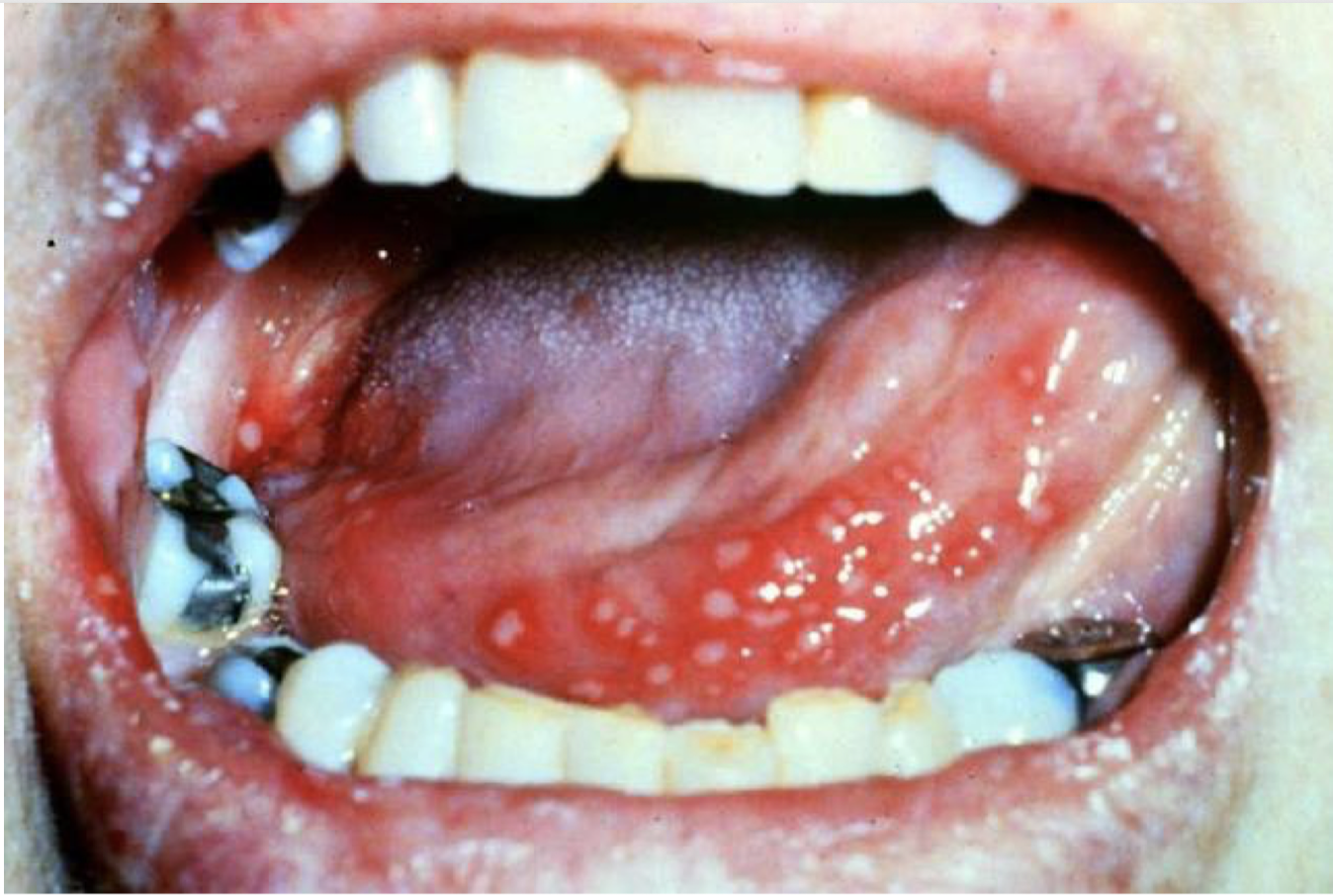
what are these lesions associated with
Herpangina - Coxsackie A4
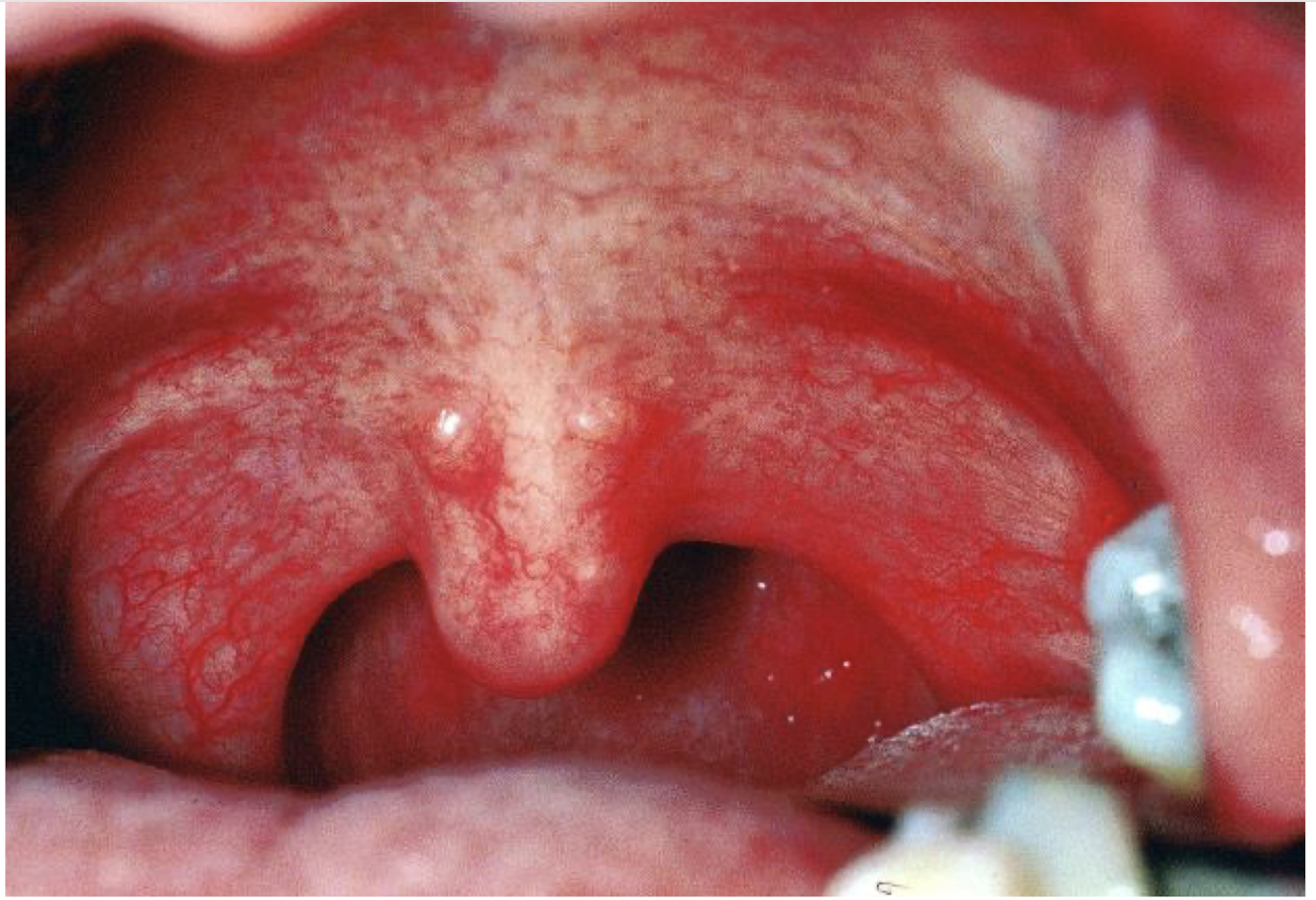
what are these lesions associated with
Acute lymphonodular pharyngitis - Coxsackie A10
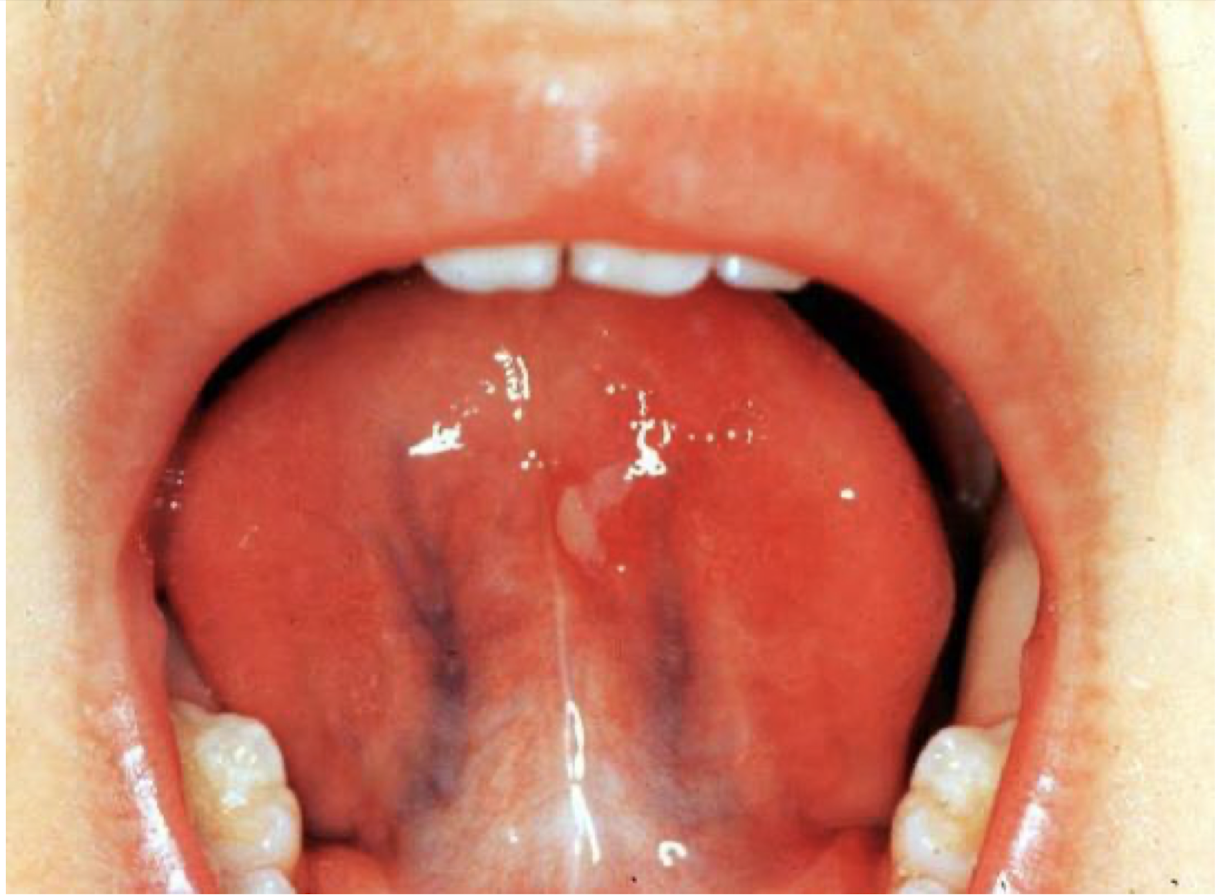
what is this lesion and what is it associated with
oral vesicle/ulcer
hand foot and mouth disease - A16
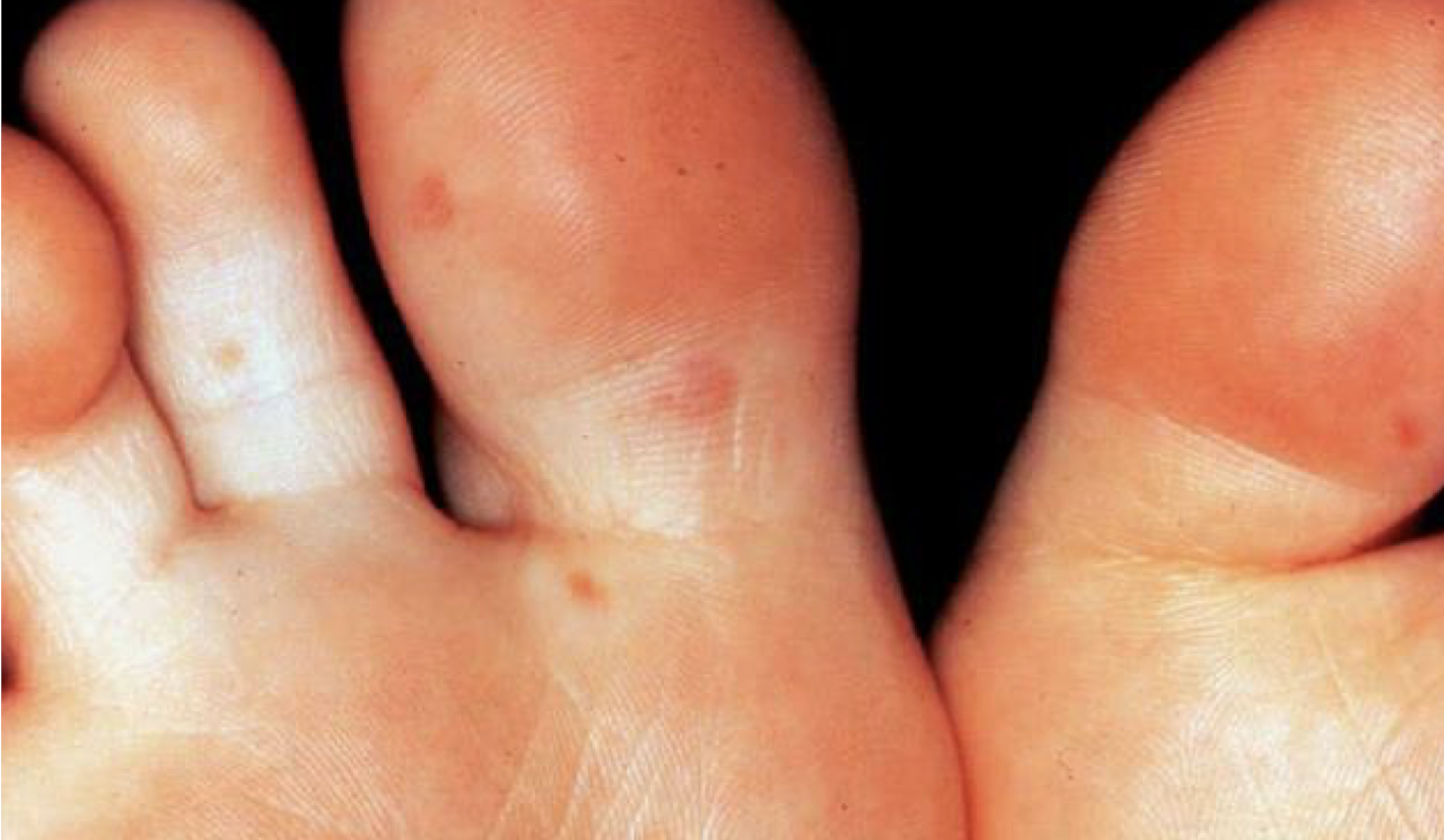
what are these lesions associated with
hand foot and mouth disease
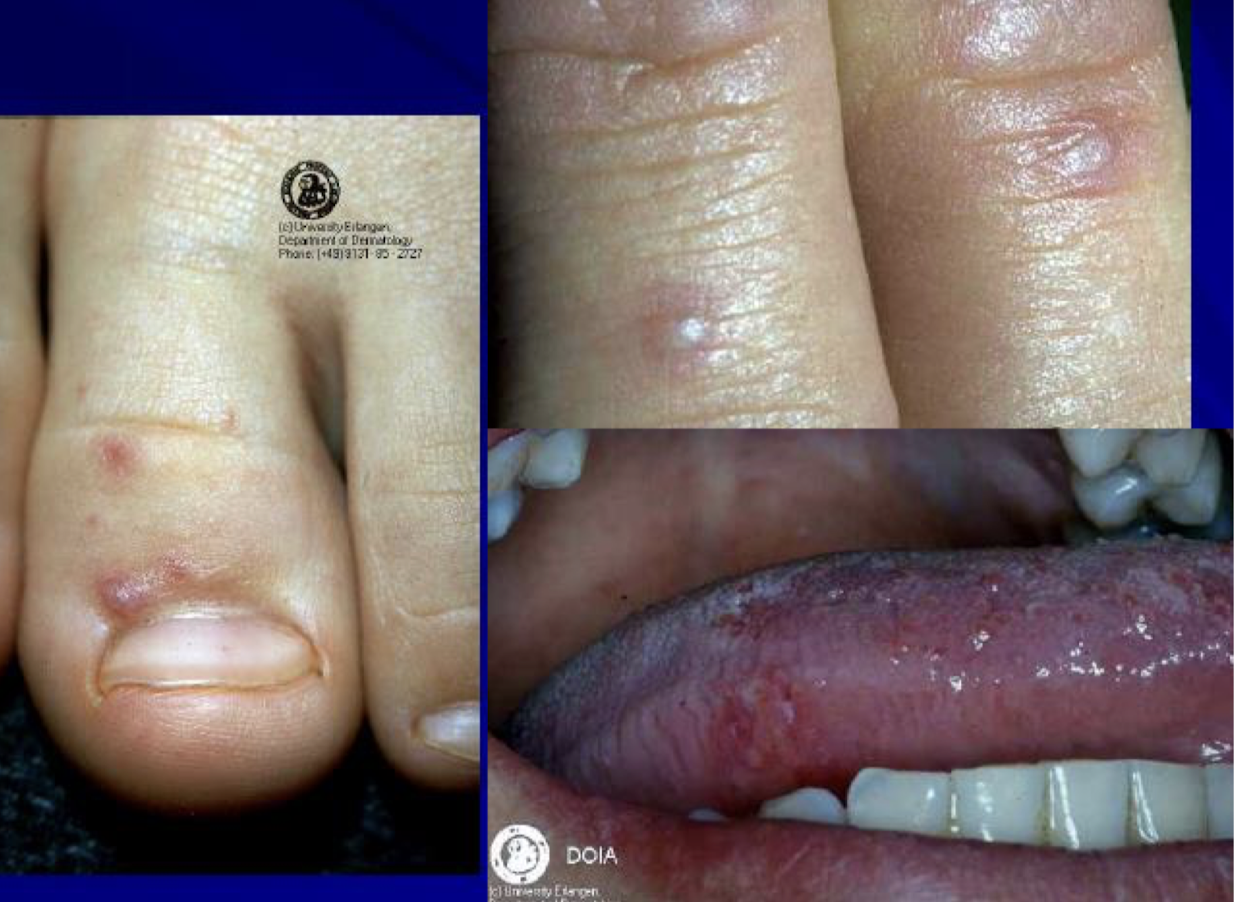
what are these lesions associated with
hand foot and mouth disease
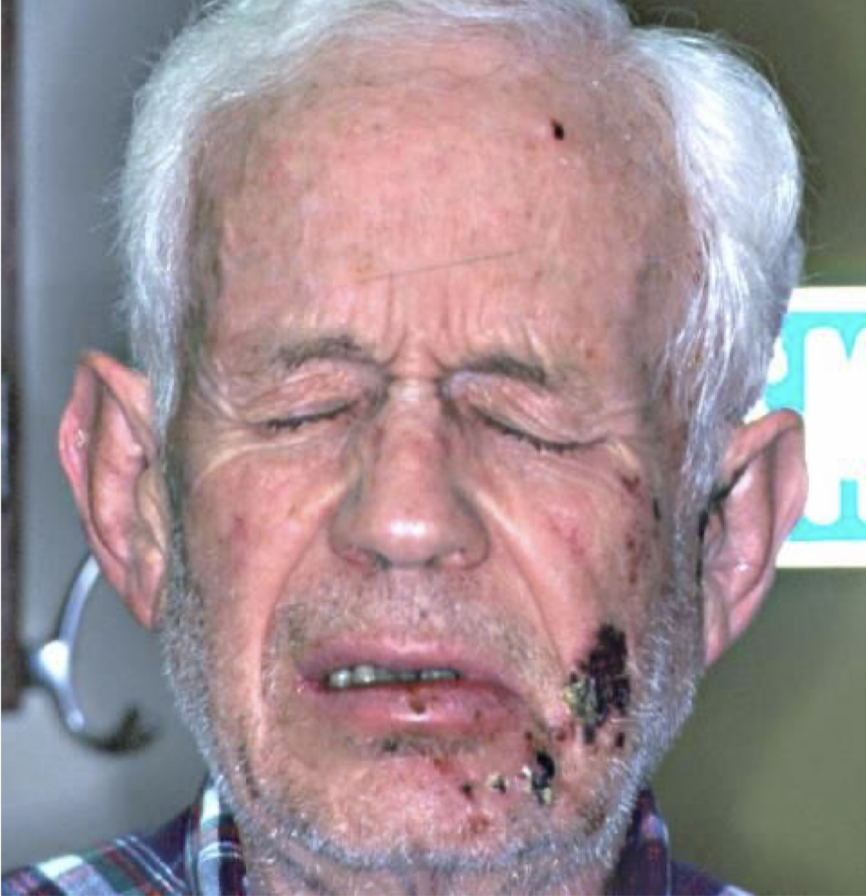
what is this lesion associated with and why is it black
shingles/herpes zoster
the vesicles turned into ulcers which turned into scabs
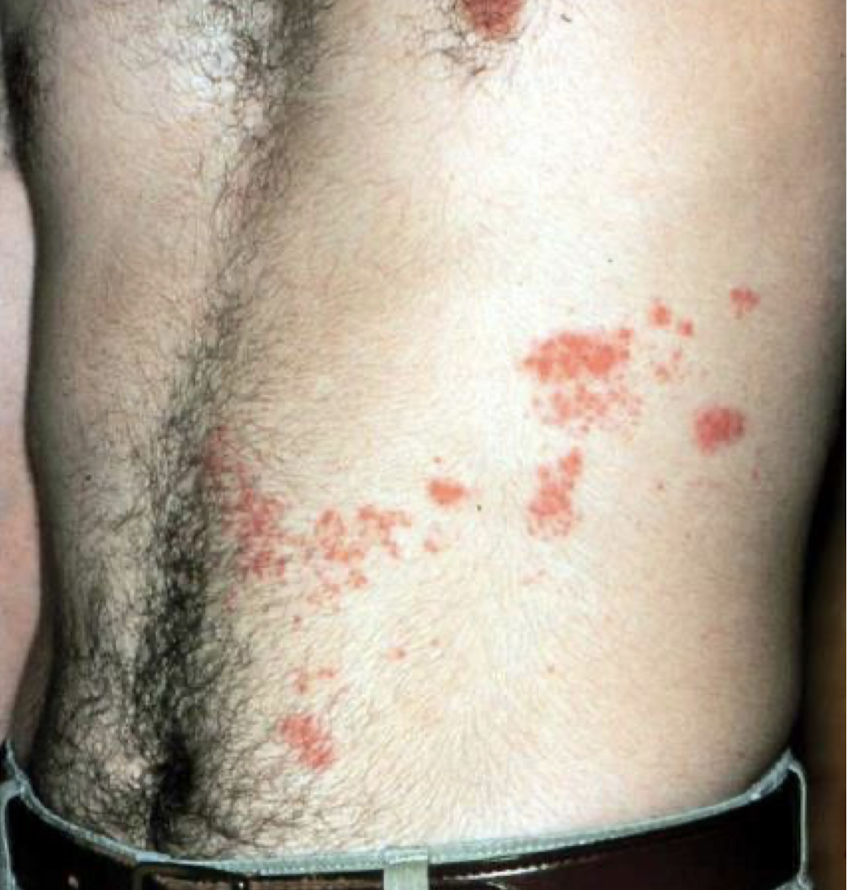
what are these lesions associated with and what is it called
shingles/herpes zoster
post-herpetic neuralgia
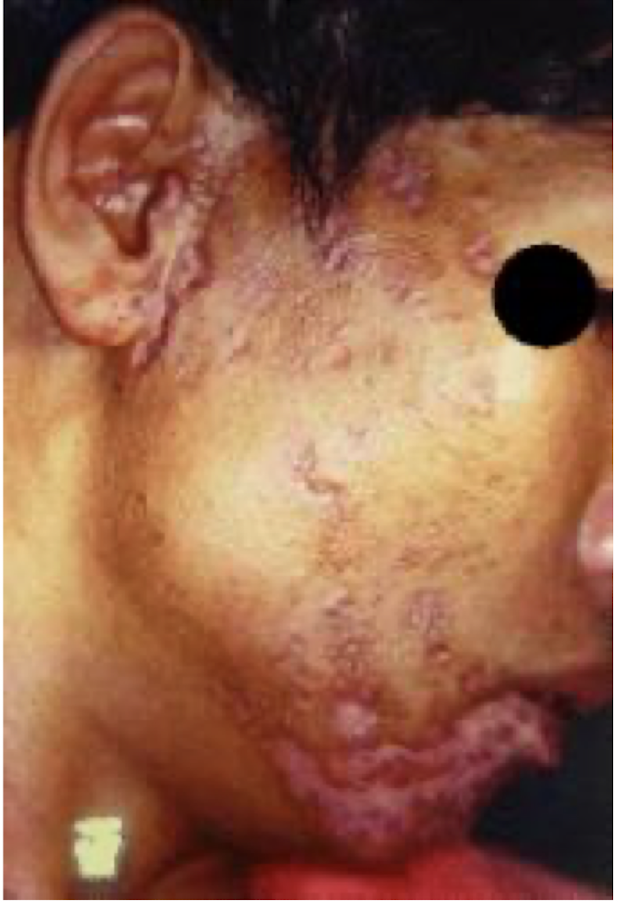
what are these lesions associated with
herpes zoster/shingles
post-herpetic neuralgia
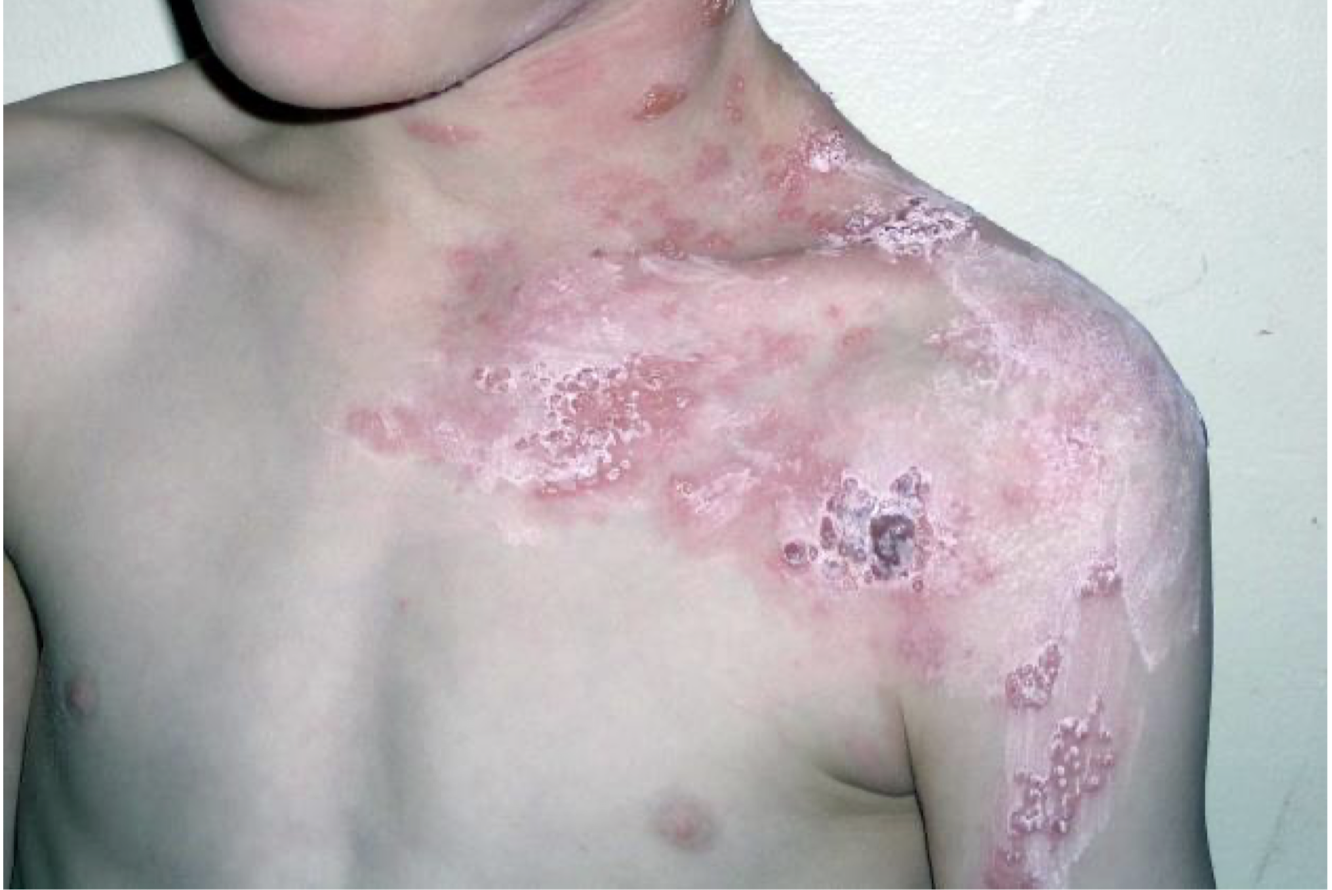
what is this lesion associated with
herpes zoster/shingles
post-herpetic neuralgia (spinal nerve)
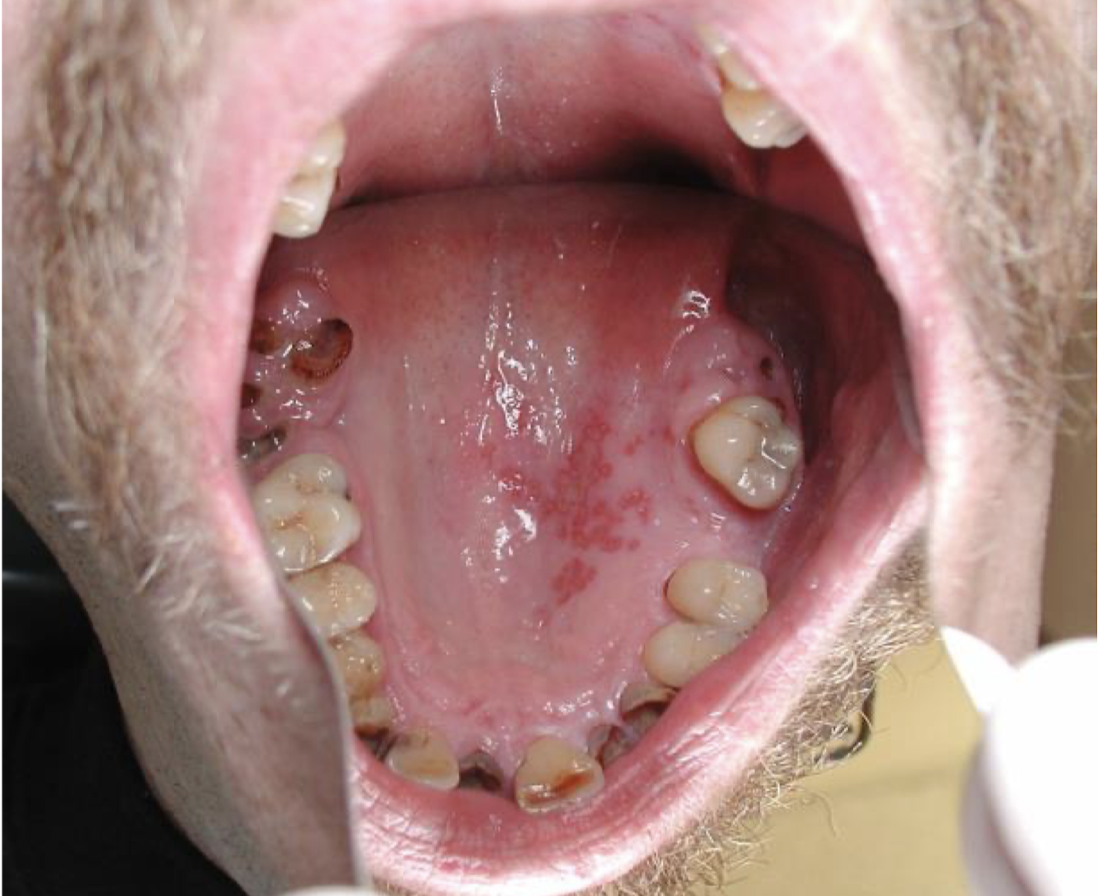
what virus is this lesion associated with and how do you determine?
Herpes Zoster (shingles)
the lesion doesnt cross the midline
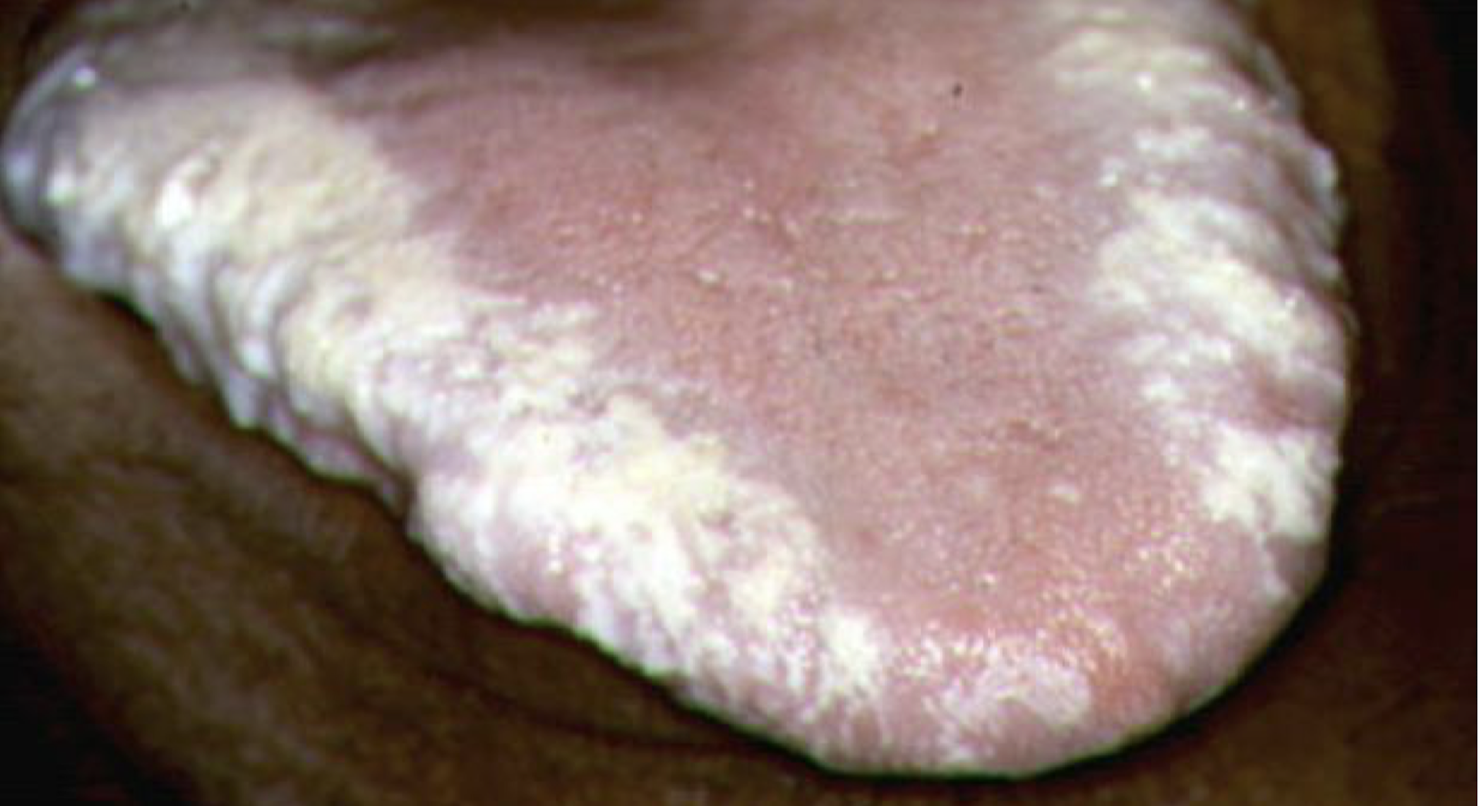
what is this lesion called and what virus is it associated with
oral hairy leukoplakia
Epstein-Barr virus
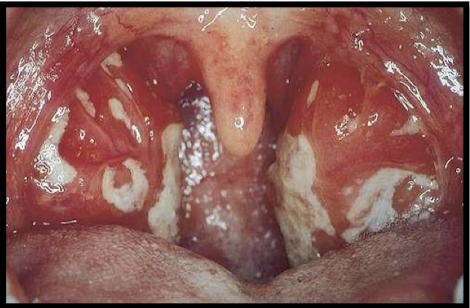
what is this associated with
pharyngitis and tonsilitis
infectious mononucleosis/glandular fever
epstein barr virus
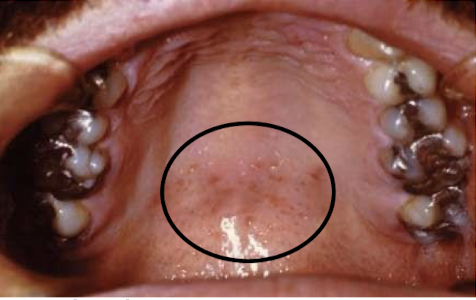
what are these lesions associated with
Infectious mononucleosis/glandular fever
Epstein Barr Virus
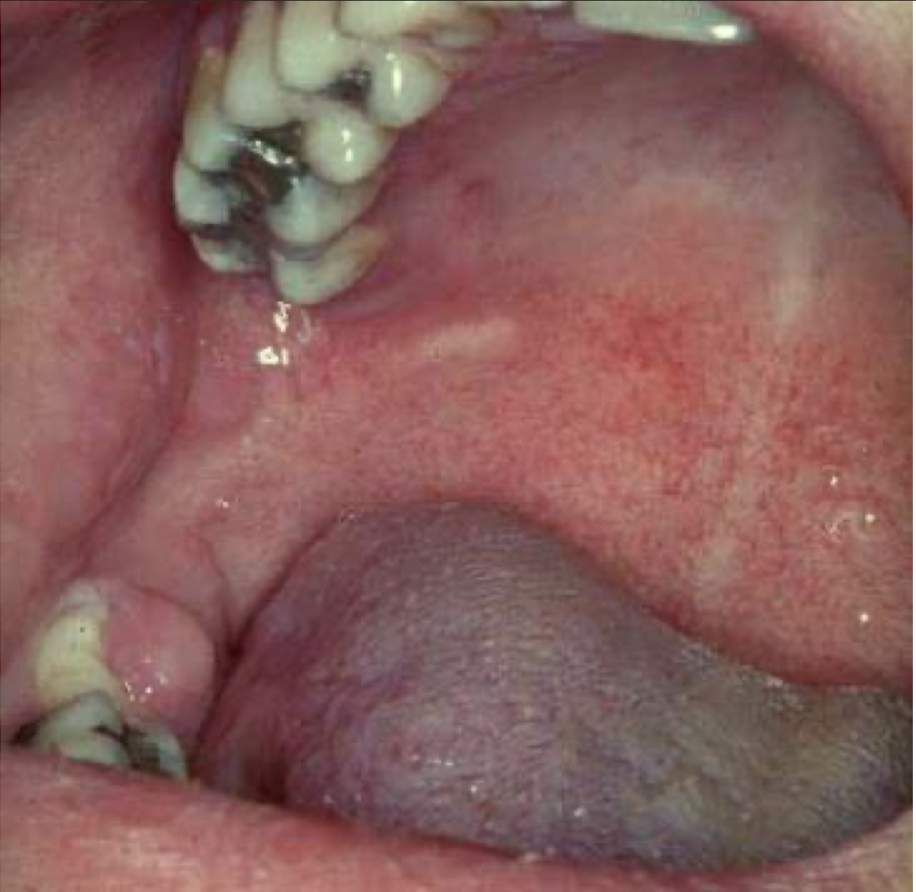
what are these lesions associated with
Rubeola/measles
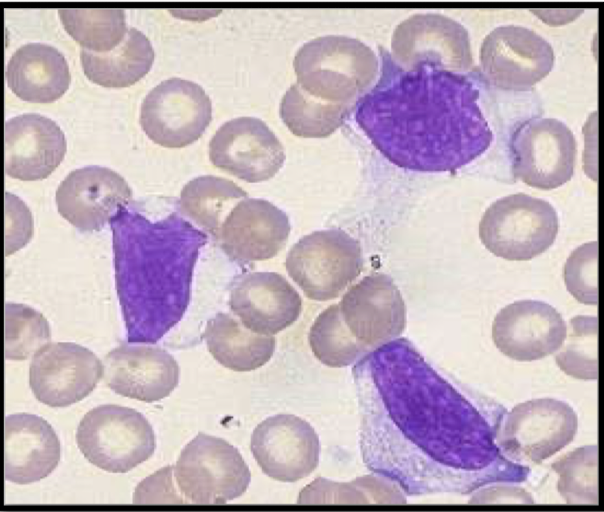
what are these cells and what are they associated with
Downey cells - atypical lymphocytes
infectious mononucleosis/EBV
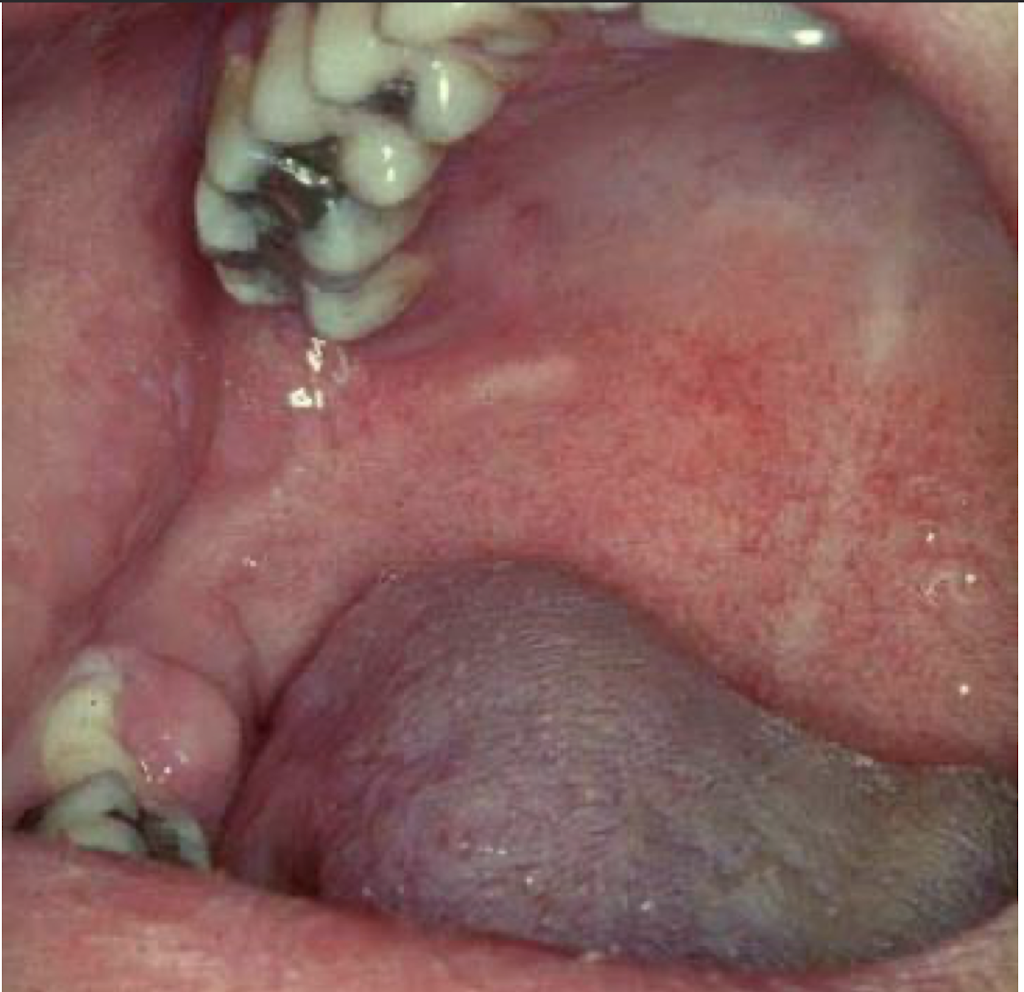
what is this disease
Rubeola/mumps/measles
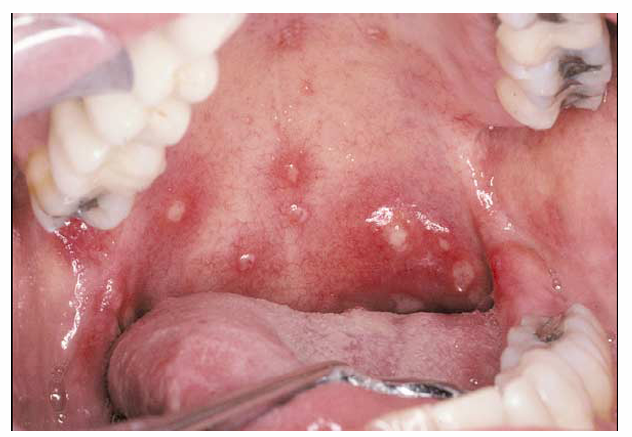
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
multiple apthous, Recurrent, painful mouth ulcers (canker sores), often appearing as multiple small or numerous ulcers on non-keratinized oral mucosa. Includes minor, major, or herpetiform types depending on size/severity.
Mild cases: topical corticosteroids (e.g., triamcinolone), pain relief (lidocaine/benzydamine), chlorhexidine mouthwash, correct iron/B12/folate deficiencies.Severe or persistent cases: systemic steroids, colchicine, dapsone, or specialist evaluation for underlying systemic disease.
group 2 less commonly associated
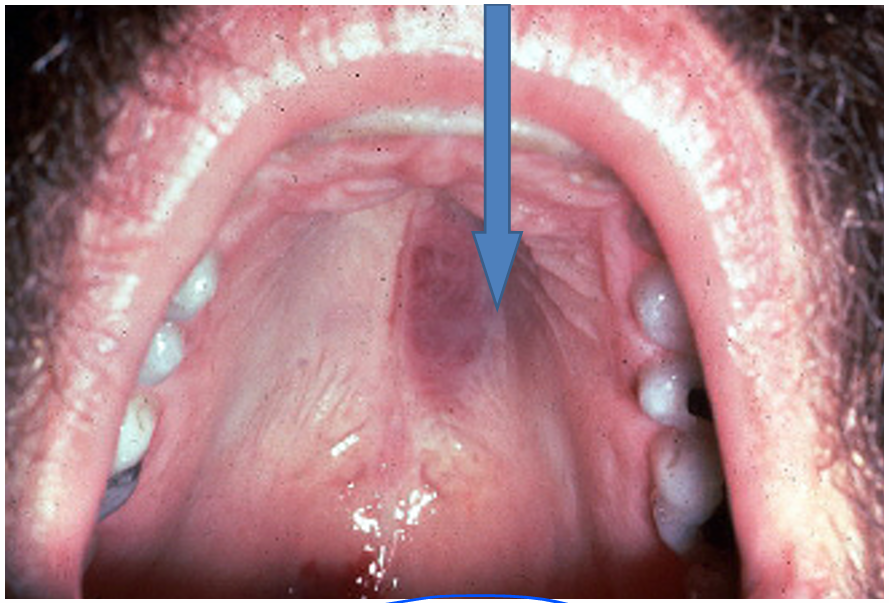
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
kaposi sarcoma
antiretroviral therapy (ART)
group 1 strongly associated
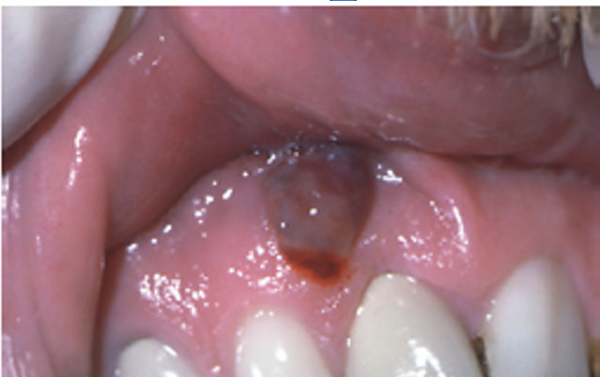
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
kaposi sarcoma
antiretroviral therapy (ART)
group 1 strongly associated
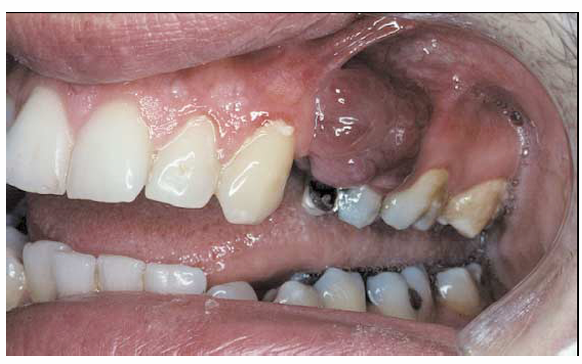
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
kaposi sarcoma
antiretroviral therapy (ART)
group 1 strongly associated
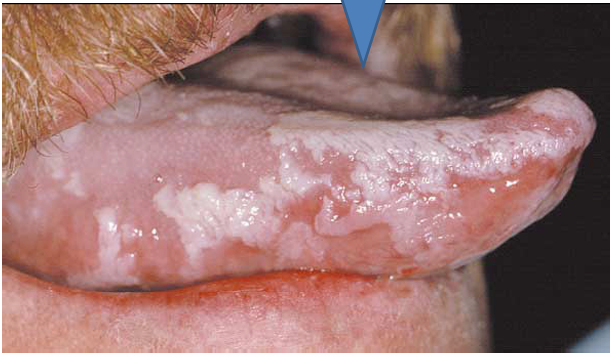
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
oral hairy leukoplakia
antiretroviral therapy (ART)
group 1 strongly associated
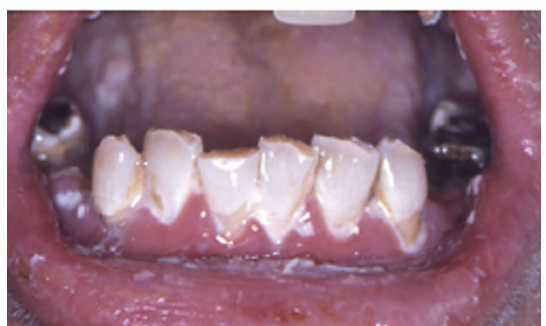
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
oral candidiasis
Topical antifungals: nystatin suspension, clotrimazole troches. Severe/recurrent cases: systemic antifungals like fluconazole.
group 1 strongly associated
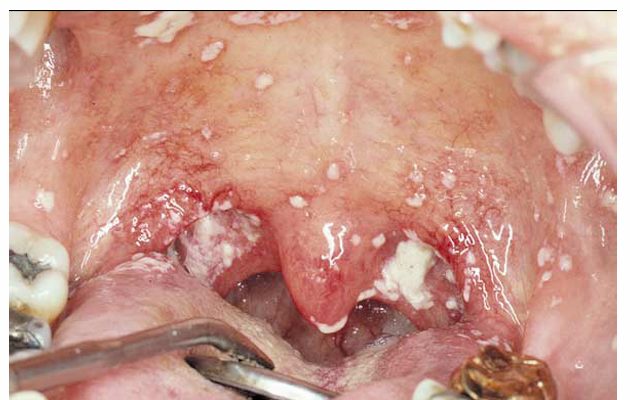
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
Pseudomembraneous candidiasis
First-line: topical antifungals such as nystatin oral suspension or clotrimazole troches. Severe/recurrent cases: fluconazole orally.
group 1 strongly associated
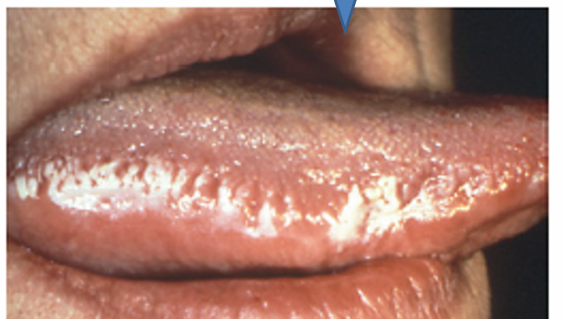
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
oral hairy leukoplakia
antiretroviral therapy (ART)
group 1 strongly associated
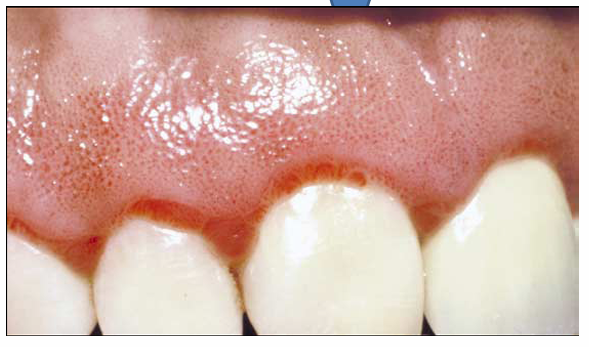
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
linear gingiva erythema
Professional cleaning + meticulous oral hygiene, chlorhexidine mouth rinse, and often antifungal therapy if Candida is involved.
group 1 strongly associated
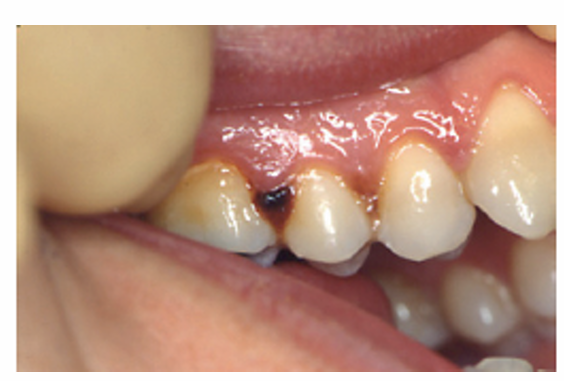
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
NUG(necrotizing ulcerative gingivitis)
Immediate gentle debridement, chlorhexidine mouthwash, improved oral hygiene, pain control, and removal of contributing factors. Metronidazole may be used in severe cases or systemic involvement; ensure nutrition and hydration.
group 1 strongly associated
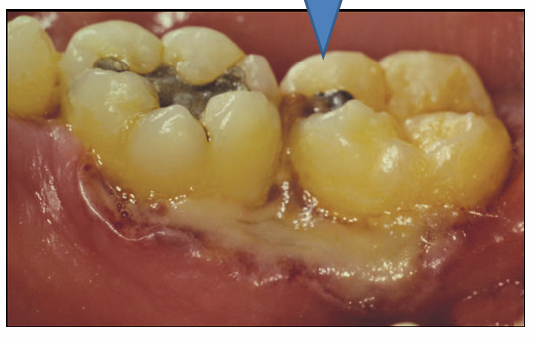
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
Necrotizing ulcerative periodontitis
Urgent debridement, chlorhexidine rinses, pain control, and systemic antibiotics (commonly metronidazole). Intensive periodontal care, improved oral hygiene, nutritional support, and treatment of underlying immune suppression (e.g., HIV management).
group 1 strongly associated
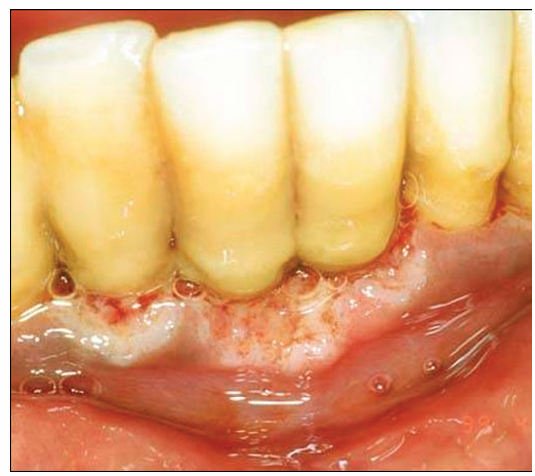
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
Necrotizing ulcerative periodontitis
Urgent debridement, chlorhexidine rinses, pain control, and systemic antibiotics (commonly metronidazole). Intensive periodontal care, improved oral hygiene, nutritional support, and treatment of underlying immune suppression (e.g., HIV management).
group 1 strongly associated
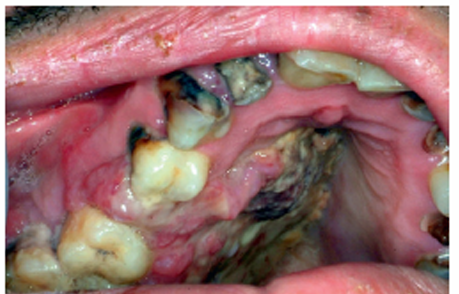
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
Oral lymphoma
Requires urgent biopsy and oncologic diagnosis. Main treatment: chemotherapy ± radiotherapy depending on type/stage; HIV-associated cases also require antiretroviral therapy (ART).
group 1 strongly associated
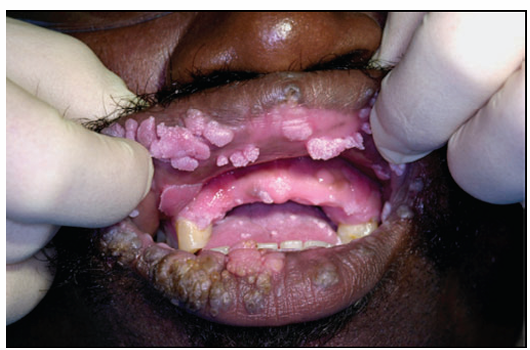
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
Human papilloma virus infection
Benign lesions: surgical excision, laser removal, cryotherapy, or observation depending on lesion type. Prevention: HPV vaccination and reducing transmission risk. Suspicious/persistent lesions require biopsy to rule out dysplasia or malignancy.
group 2 less commonly associated
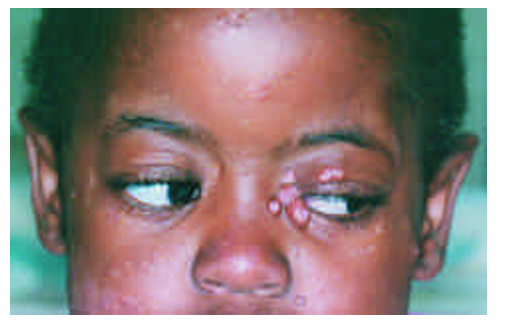
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
Pox virus infection
Often supportive care (pain control, hydration, hygiene); many lesions are self-limiting depending on the specific virus. Severe, extensive, or immunocompromised cases may need antiviral/specialist management depending on the poxvirus type.
group 3 possibly associated
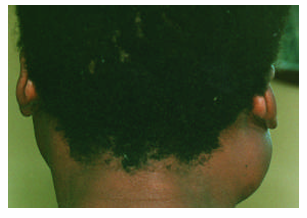
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
Parotid enlargement, salivary gland disease causing facial swelling and sometimes dry mouth.
Evaluate cause (infection, stones, tumors, autoimmune disease, HIV-related disease). HIV-related cases: antiretroviral therapy (ART), monitoring, aspiration/surgery if symptomatic, and xerostomia management.
Group 2 less commonly associated
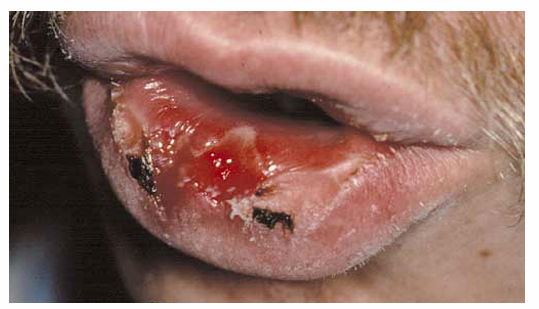
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
Recurrent herpes , Recurrent reactivation of Herpes Simplex Virus (usually HSV-1) causing repeated painful vesicles/ulcers, commonly on lips (herpes labialis) or oral mucosa.
Antivirals: acyclovir, valacyclovir, or famciclovir. Pain relief, hydration, and trigger avoidance (stress, trauma, sun exposure). Severe or chronic cases may need prolonged antiviral therapy.
Group 2 less commonly associated
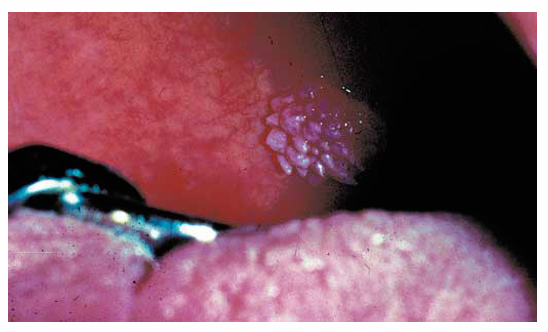
1.what is this lesion?
2. how to treat/ manage it?
Squamous papilloma, A benign epithelial growth, usually caused by low-risk HPV types (6, 11), appearing as a small painless papillary or cauliflower-like oral lesion (common on tongue, palate, uvula).
Surgical excision is the standard treatment. Laser or cryotherapy may also be used. Biopsy confirms diagnosis and excludes dysplasia.

describe the pic
Gross specimen
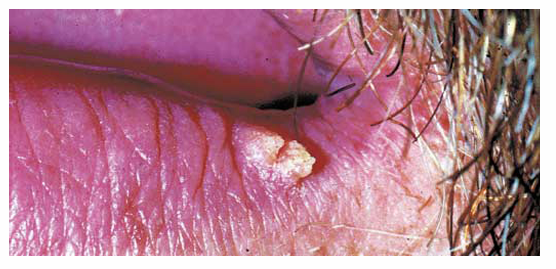
1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
Verruca vulgaris, A benign HPV-related lesion (commonly HPV 2, 4) that may occur orally as a painless, rough, papillary or verrucous growth, often on lips, tongue, or labial mucosa.
Surgical excision, laser, cryotherapy, or observation depending on size/location. Biopsy may be needed to confirm diagnosis.
Group 2 less commonly associated

1.what is this lesion?
2. how to treat/ manage it?
3. classification of oral lesion in HIV?
Condyloma accuminatum, A STI HPV-related lesion (commonly HPV 6, 11) presenting as soft, pink, multiple sessile papillary/cauliflower-like growths in the oral cavity.
Surgical excision, laser removal, cryotherapy, or other lesion-directed therapy. Biopsy may be needed, and sexual health evaluation is important due to STI association.
Group 2 less commonly associated
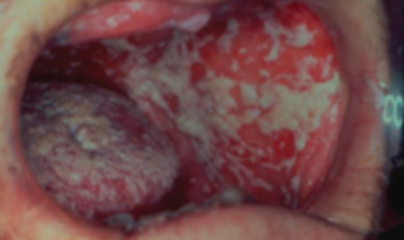
what is this condition
acute pseudomembranous candidiasis (thrush)
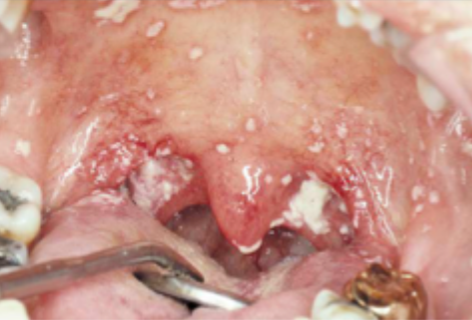
what is this condition
pseudomembranous candidiasis
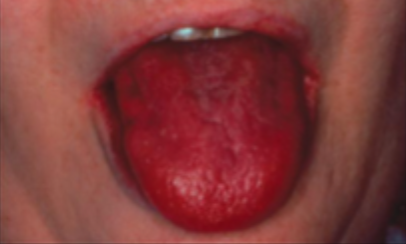
what is this condition
acute atrophic candidiasis
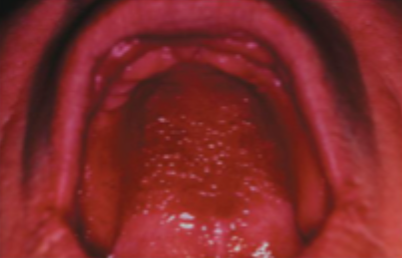
what is this condition
chronic atrophic candidiasis
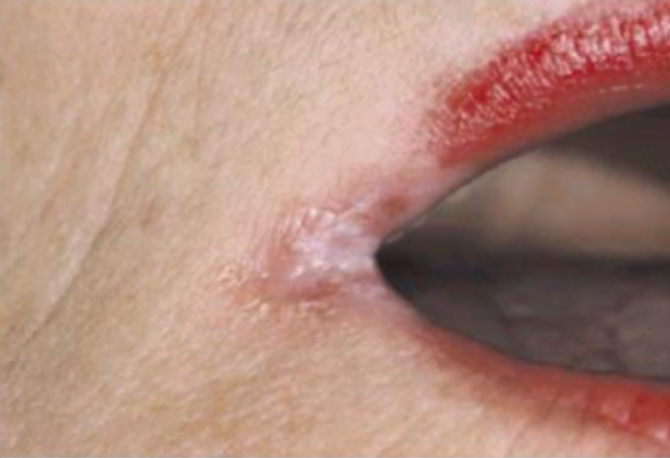
what is this condition
angular chelitis
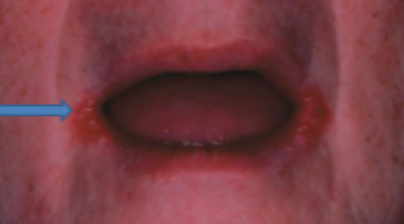
what is this condition
angular chelitis
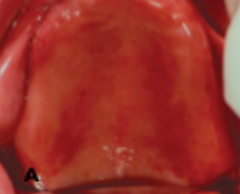
what is this condition
angular stomatitis (perieche) stage 1
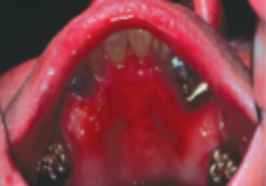
what is this condition
denture stomatitis (stage 2)
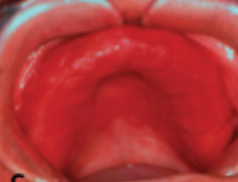
what is this condition
denture stomatitis (stage 2)
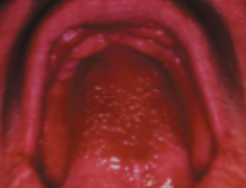
what is this condition
denture stomatitis (stage 3)
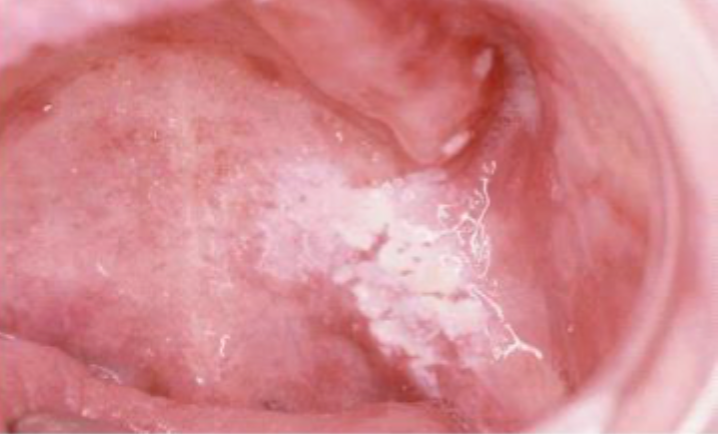
what is this condition
chronic hyperplastic candidiasis
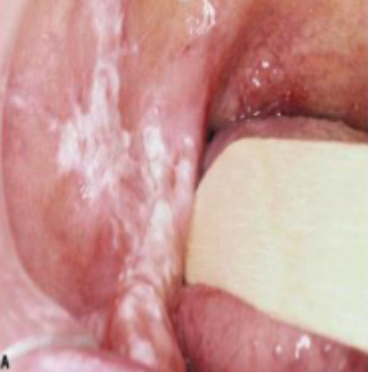
what is this condition
chronic hyperplastic candidiasis
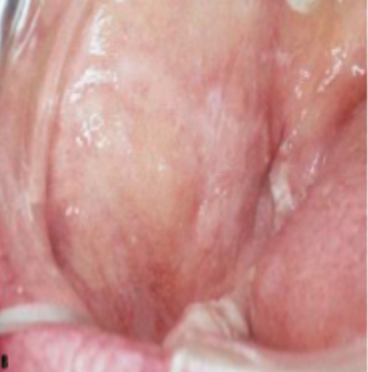
what is this condition
chronic hyperplastic candidiasis
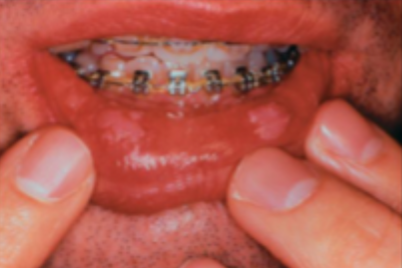
what is this condition
chronic hyperplastic candidiasis
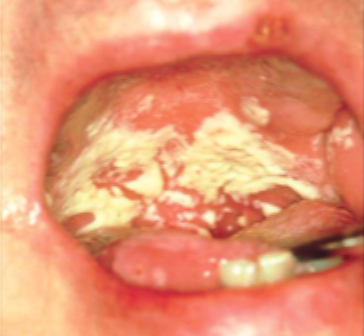
what is this condition
hyperplastic candidiasis
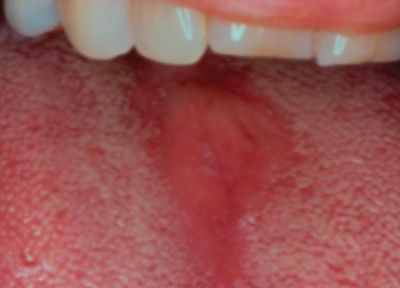
what is this condition
median rhomboid glossitis
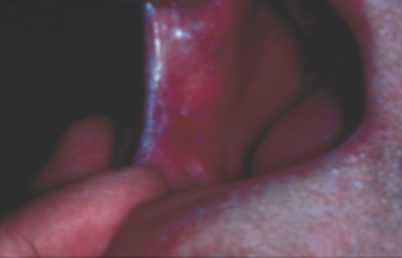
what is this condition
candidal leukoplakia
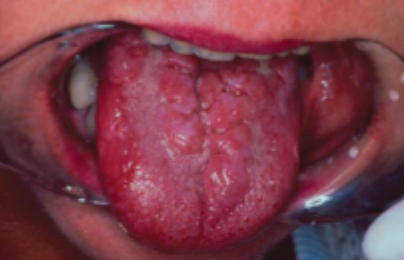
what is this condition
chronic mucocutaneous candidiasis
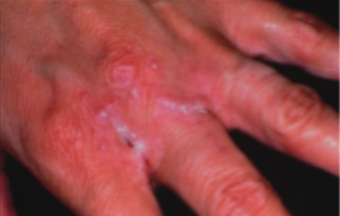
what is this condition
chronic mucocutaneous candidiasis
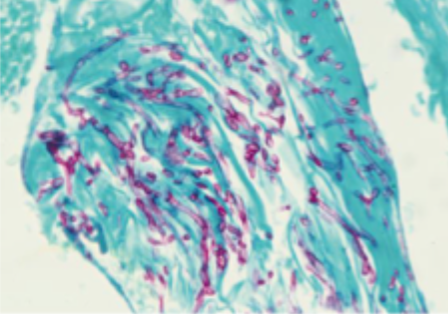
what is this test, and what is it used for
pas stain » used to diagnose candida
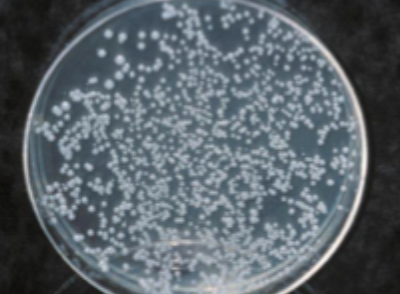
what is this test called, and what is it used for
corn meal agar candidate growth » used to diagnose candida
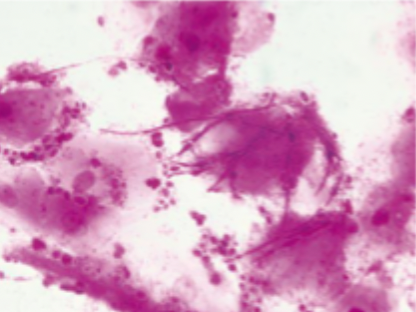
what is this test called, and what is it used for
gram stain with hyphae and myceliae » used to diagnose candida
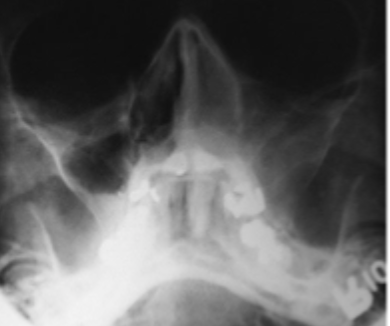
what is this condition
mucormycosis
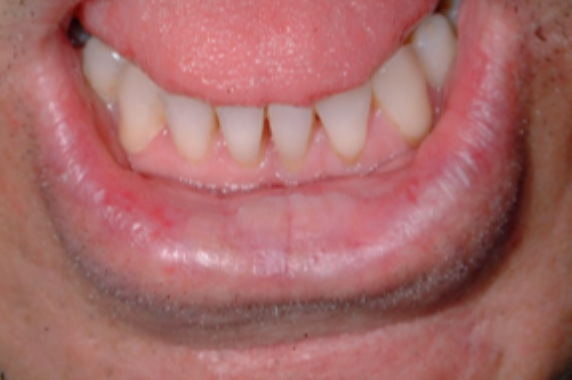
what is this condition
actinic chelitis
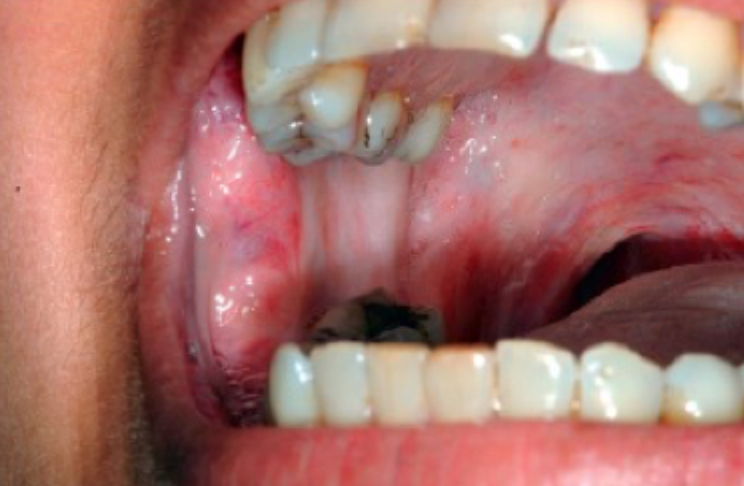
what is this condition
oral submucous fibrosis
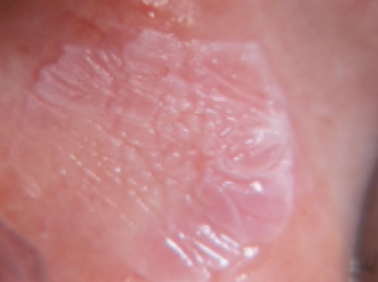
what is this condition
homogenous leukoplakia
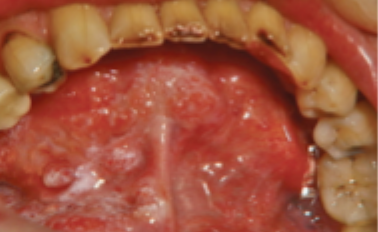
what is this condition
non-homogenous oral leukoplakia
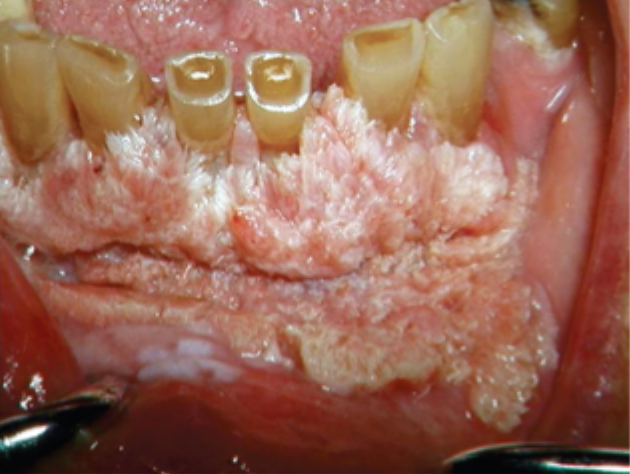
what is this condition
verrucous oral leukoplakia
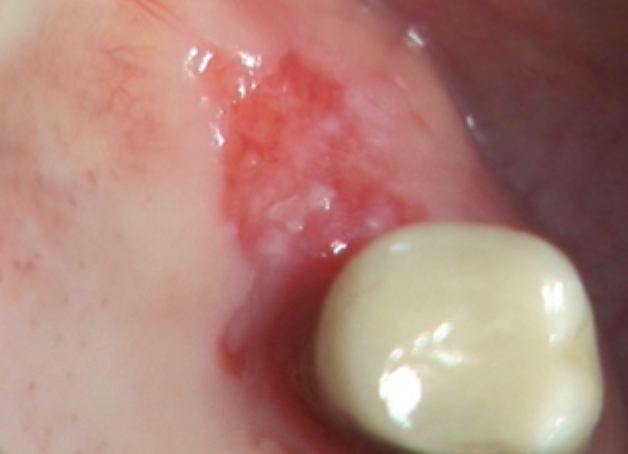
what is this condition
erythroplakia
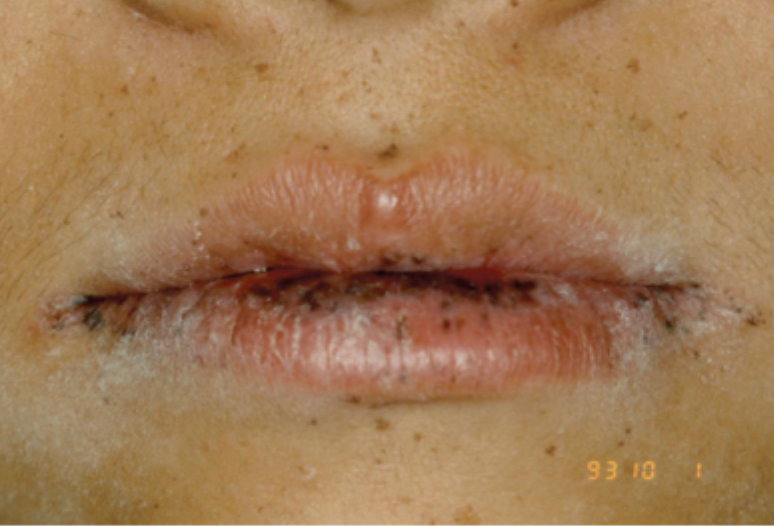
what is this condition
peri-oral melanosis
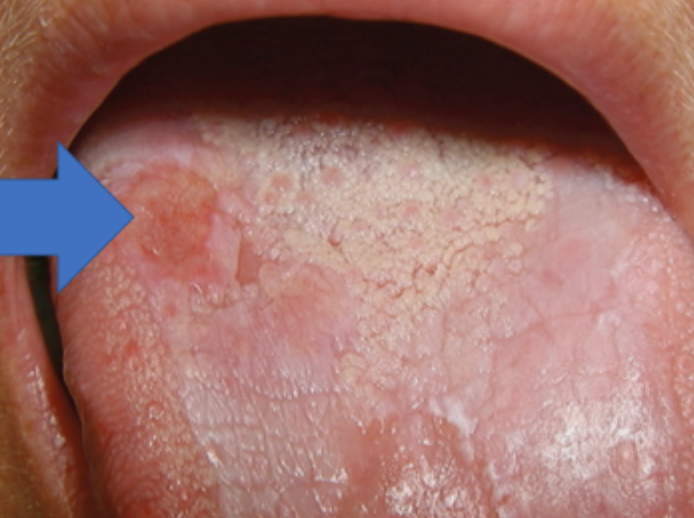
what is this condition
OSCC developed in plaque-like oral lichen plants
actinic chelitis features
sun overexposed individuals
smooth or scaly friable patch OR may involve entire lip
palpably thick with small grey-white plaques
develops into warty nodules » OSCC
management of actinic chelitis
PREVENTION » esp for high risk (photosensitive, xeroderma pigmentosum, transplant)
wearing broad brimmed hats
use UV sunscreen
oral submucous fibrosis features
betel quid chewers
tightening of buccal, palatal and lingual mucosa
trismuis
grade 1 oral submucous fibrosis
oral opening >35mm
grade 2 oral submucous fibrosis
oral opening 20-35mm
grade 3 oral submucous fibrosis
oral opening <20mm
grade 4 oral submucous fibrosis
oral opening <20mm + premalignant disease
grade 5 oral submucous fibrosis
oral opening <20mm + oral squamous cell carcinoma
which grades of OSMF should be sent for biopsy
grade 4 and 5
management of oral submucous fibrosis
physiotherapy (jaw opening exercises) + correcting nutritional deficiencies (iron and vitamin B)
cox-2 inhibitors » hyaluronidase, intralesional corticosteroids
ineffective but may be used: surgery, placenta, interferon gamma

what is this device and what is it used for
physic device for grade 1 and 2 OSMF
features of homogenous leukoplakia
white
well demarcated plaque
identical pattern throughout entire lesion
features of non-homogenous leukoplakia
white patches or plaques
intermingled with red
features of verrucous leukoplakia
white papillary projections
management of oral leukoplakia
excision
cessation of tobacco, betel, alcohol
ineffective: physio, retinoids (temporary effect, only used if difficult to access), radio/chemo (because it isn’t malignant)
when to excise vs wait+watch oral leukoplakia
no dysplasia » wait and watch
mild dysplasia (buccal, hard palate, dorsal tongue) » wait or remove
mild dysplasia (anywhere else) » remove
moderate/severe dysplasia » remove
features of erythroplakia
red lesion
asymptomatic; sometimes burning sensation when eating
reverse smoking chutta
peutz-jeghers syndrome features
multiple small pigmented macule of lips + perineal skin, hands, feet