Analgesics & Anesthesia; Diagnostic Imaging & Cutting-Edge Surgical Advances
1/210
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
211 Terms
What is pain in a physiological and neurological context?
Pain is the interpretation of sensory stimuli by the nervous system, resulting in a subjective, unpleasant, and emotional experience often described as suffering, meaning that it is not purely physical but also influenced by perception and emotion.
Why is pain considered subjective?
Pain is considered subjective because its perception varies between individuals depending on factors such as age, gender, cultural background, environment, anxiety levels, and prior experiences, meaning two individuals can experience the same stimulus very differently.
What are the two main types of pain?
The two main types of pain are nociceptive pain, which results from tissue damage such as injury or inflammation, and neuropathic pain, which arises from damage or malfunction of the nervous system itself.
What is nociceptive pain?
Nociceptive pain is pain caused by physical damage to tissues due to trauma, injury, disease, or inflammation, and it can be further categorized into somatic pain (skin, muscles) and visceral pain (internal organs).
What is neuropathic pain?
Neuropathic pain is pain caused by damage or dysfunction in peripheral or central nerves, often resulting in abnormal sensations such as burning or shooting pain, and includes conditions like sciatica, diabetic neuropathy, and post-herpetic neuralgia.
What is nociception?
Nociception is the process by which the somatosensory nervous system detects and responds to harmful stimuli, involving sensory neurons called nociceptors that transmit signals from the site of injury to the brain.
What are nociceptors?
Nociceptors are specialized sensory nerve cells that detect harmful or potentially damaging stimuli and convert them into electrical signals that can be transmitted to the central nervous system.
How does a pain signal travel through the body?
When nociceptors are activated, they generate an electrical signal that travels through afferent neurons to the spinal cord and then to the brain, where it is processed and perceived as pain.
What are the four phases of nociception?
The four phases of nociception are transduction, transmission, perception, and modulation, each representing a step in how pain is detected, sent, interpreted, and regulated.
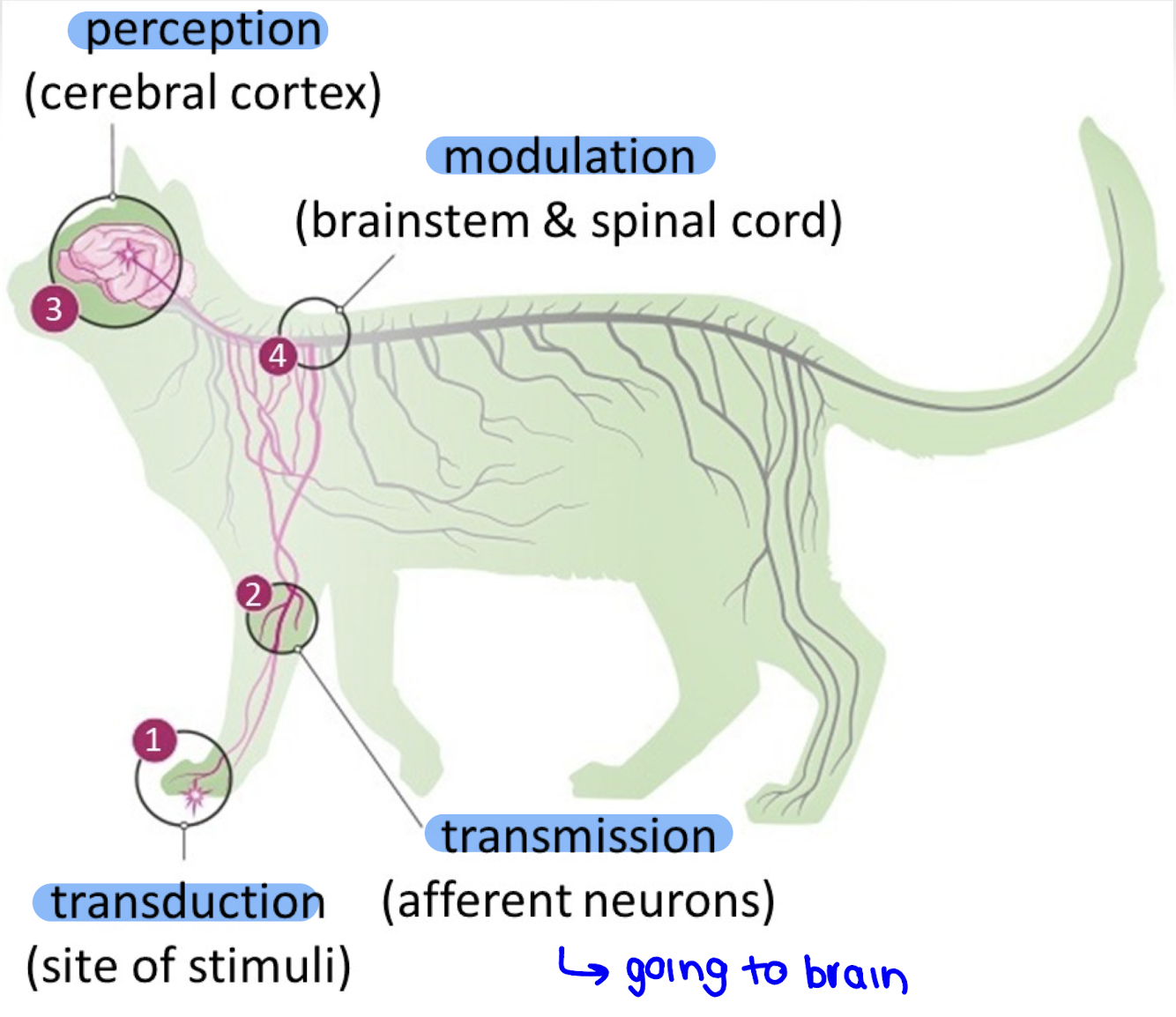
What is transduction?
Transduction is the process by which harmful stimuli such as mechanical pressure, extreme temperatures, or chemical signals are converted into electrical signals (action potentials) in nociceptors.
What types of stimuli initiate transduction?
Transduction can be initiated by mechanical stimuli like pressure or injury, thermal stimuli such as extreme heat or cold, and chemical stimuli including inflammatory mediators and toxins.
What chemical mediators are released during tissue damage during transduction?
Damaged cells release chemical mediators such as prostaglandins, bradykinin, substance P, and histamine, which activate nociceptors and initiate the pain signal.
What is an action potential in the context of pain?
An action potential is an electrical impulse generated in nociceptors that propagates along neurons to carry the pain signal toward the spinal cord and brain.
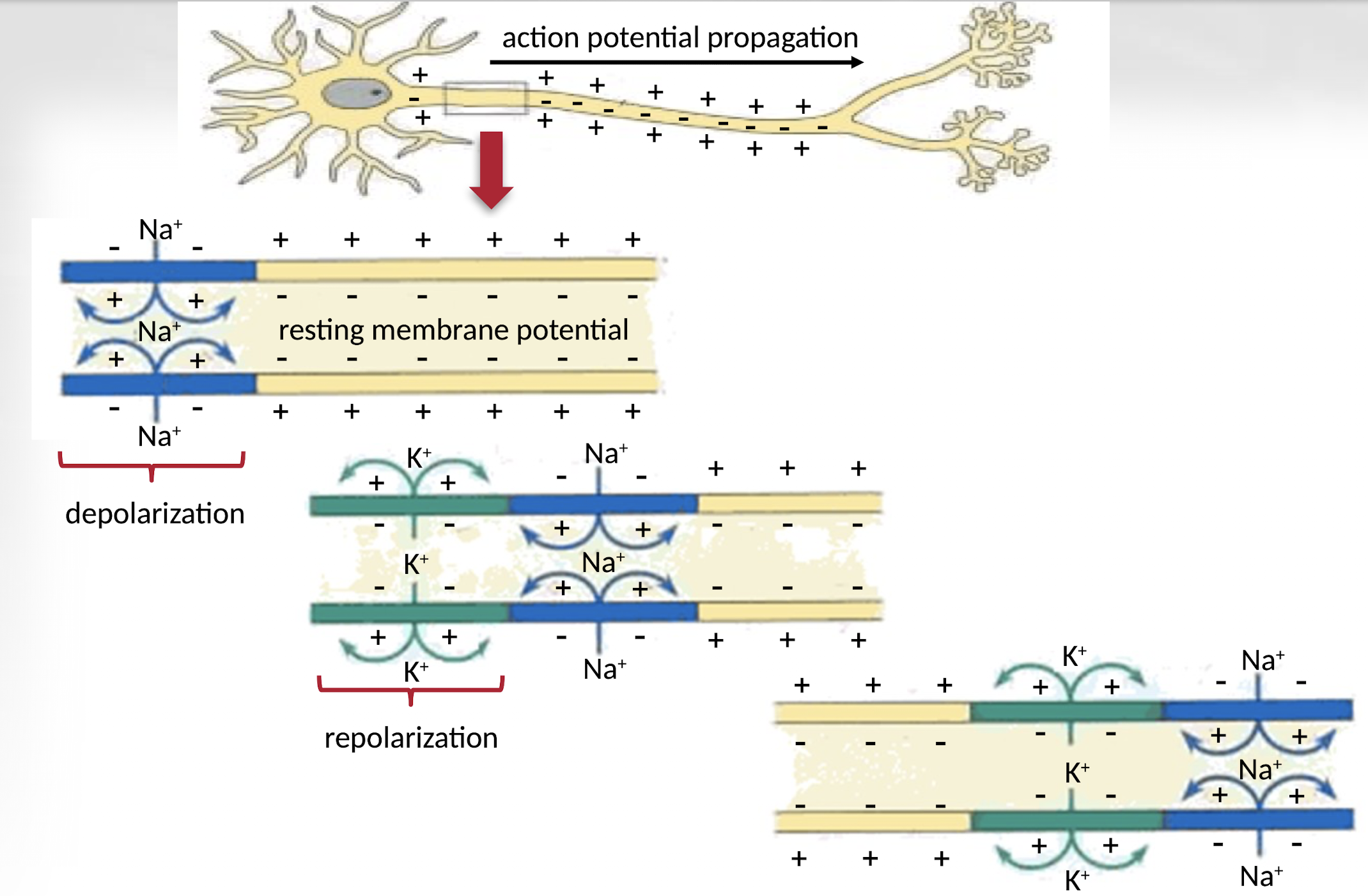
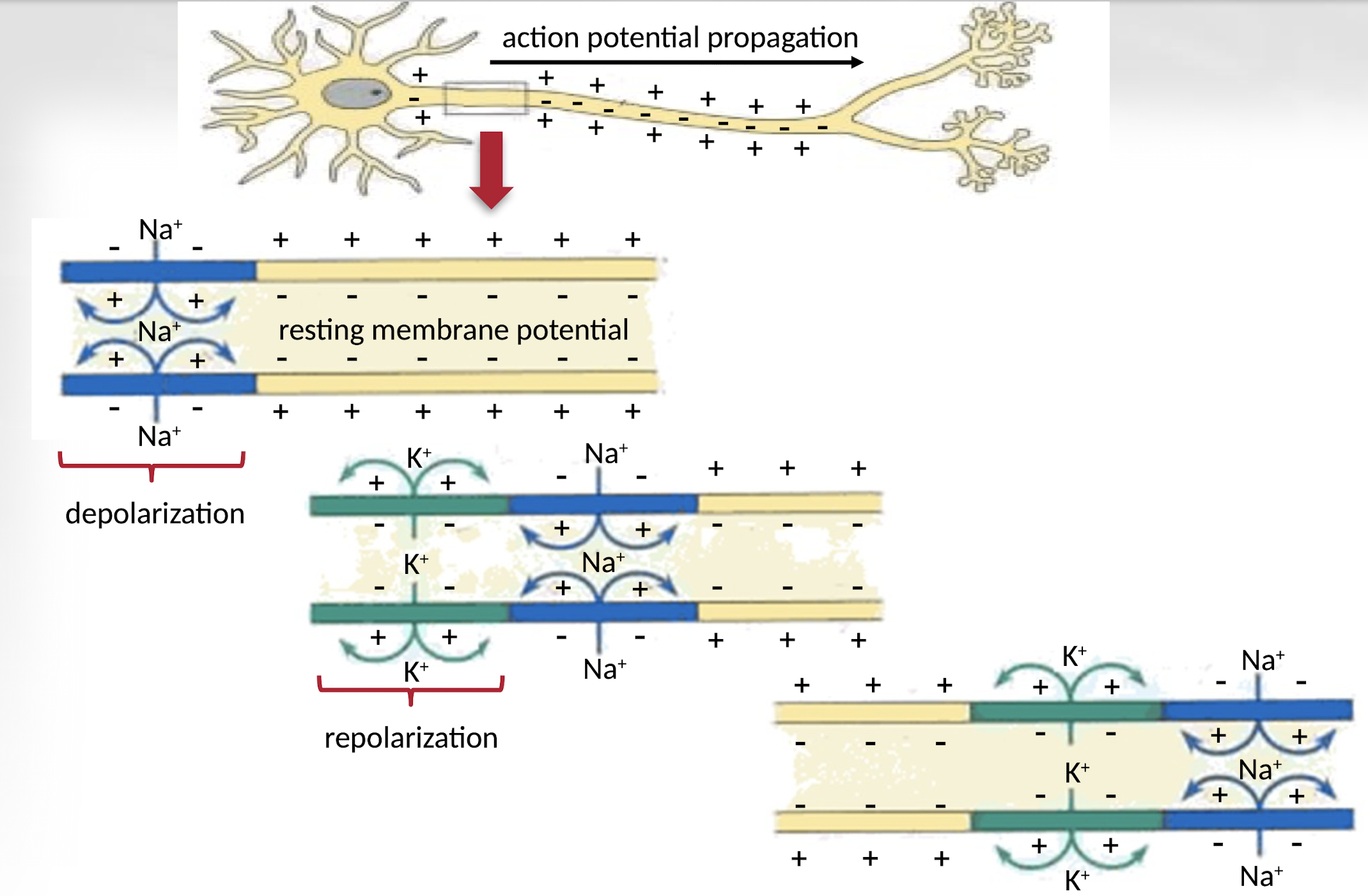
What happens during depolarization and repolarization?
During depolarization, sodium ions enter the neuron causing a positive charge, while during repolarization, potassium ions exit the cell restoring the negative resting membrane potential.
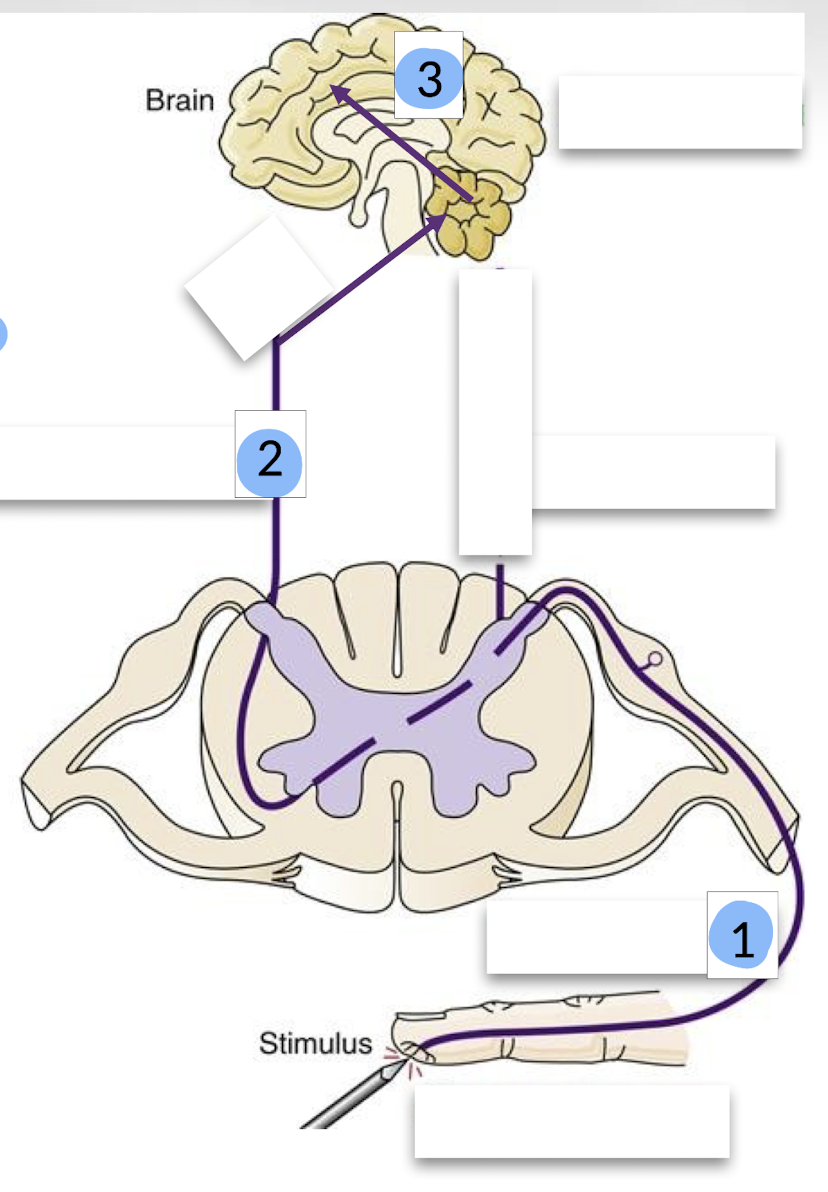
What is transmission in nociception?
Transmission is the process by which pain signals are carried from the site of injury to the brain through a series of neuronal pathways.
What are the three stages of transmission?
The three stages of transmission are from the site of injury to the dorsal horn of the spinal cord, from the spinal cord to the brainstem and thalamus, and from the thalamus to the sensory cortex.
What neurotransmitters are involved in transmission?
Excitatory neurotransmitters such as glutamate, substance P, nitric oxide, calcitonin gene-related peptide (CGRP), and bradykinin facilitate the transmission of pain signals across synapses.
What is perception in nociception?
Perception is the conscious awareness and interpretation of pain that occurs in the brain, involving multiple regions that process intensity, location, and emotional significance.
What role does the reticular activating system play in pain perception?
Autonomic and motor responses: heart rate, respiration, sweating, reflexes.
What role does the somatosensory cortex play in pain perception?
Perception and interpretation: type and location of pain, intensity.
What role does the limbic system play in pain perception?
Emotional and behavioral response: attention, mood, behavior.
What is modulation in nociception?
Modulation is the process by which the brain alters or regulates pain signals through descending pathways that can either amplify or inhibit the signal.
What are descending modulatory pain pathways (DMPPs)?
DMPPs are neural pathways from the brainstem that send signals back down to the spinal cord to regulate pain transmission through excitation or inhibition.
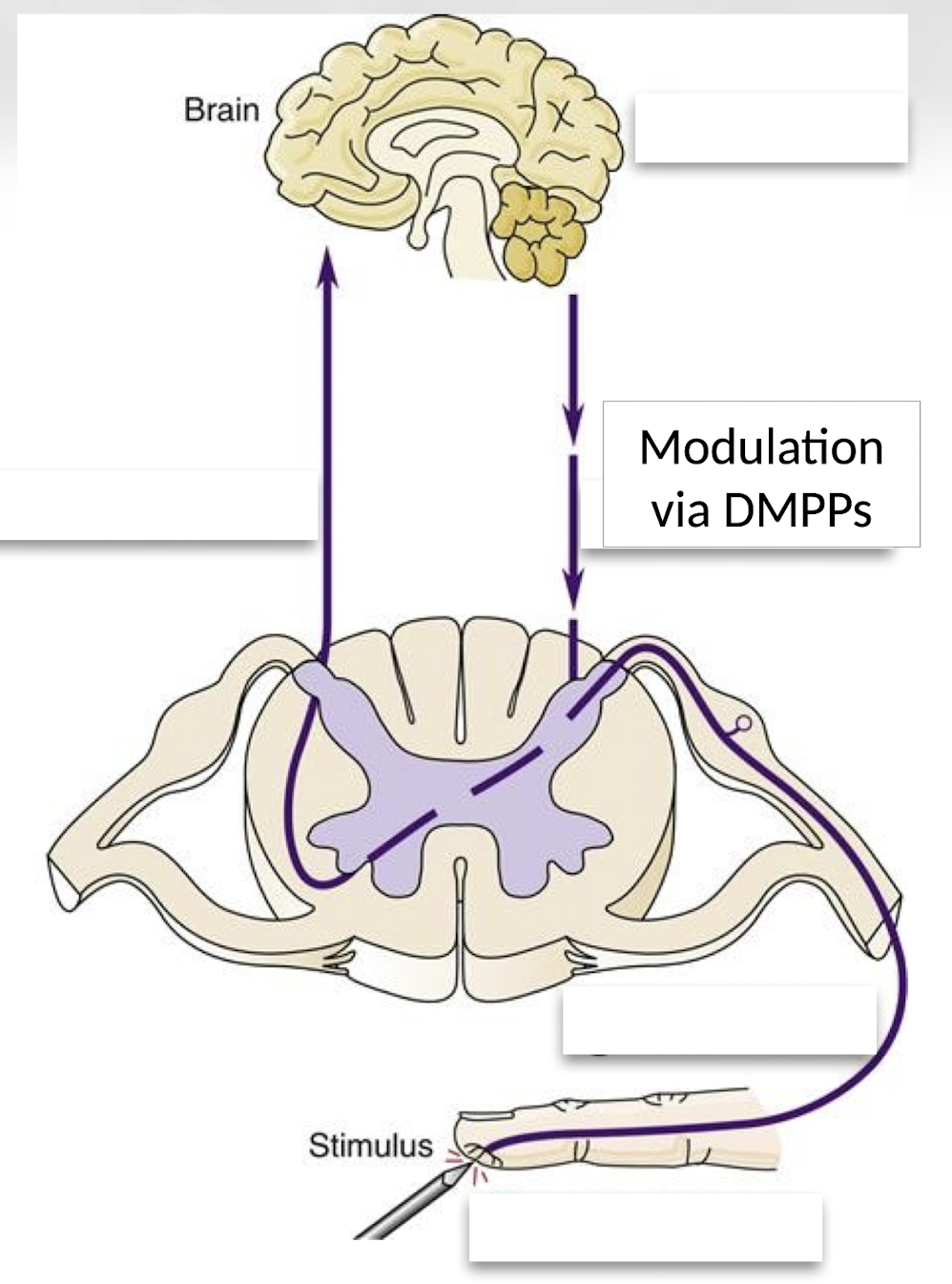
What neurotransmitters inhibit pain during modulation?
Inhibitory neurotransmitters include serotonin (5-HT), norepinephrine, glycine, GABA, and endogenous opioids such as endorphins and enkephalins, which suppress pain signaling.
What is an analgesic?
An analgesic is a medication specifically designed to relieve pain by interfering with one or more stages of nociception.
What are the two main categories of analgesics?
The two main categories are non-opioid analgesics, which are typically used for mild to moderate pain, and opioid analgesics, which are used for more severe pain.
What are common uses of non-opioids vs opioids?
Non-opioids are used for short-term, mild to moderate pain, while opioids can be used for short- or long-term management of severe pain.
What are routes of administration for analgesics?
Non-opioids are typically administered orally or topically, while opioids can be given orally or intravenously.
What are side effects of non-opioids?
Non-opioids can cause liver and kidney damage, gastrointestinal bleeding, ulcers, and potential cardiac issues with prolonged use.
What are side effects of opioids?
Opioids can cause tolerance, dependence, addiction, and respiratory depression due to their effects on the central nervous system.
What are examples of non-opioid analgesics?
Examples include acetaminophen and NSAIDs such as ibuprofen, naproxen, and meloxicam.
What are examples of opioid analgesics?
Examples include codeine, hydrocodone, oxycodone, morphine, methadone, and fentanyl.
How do NSAIDs work?
NSAIDs inhibit cyclooxygenase (COX) enzymes, reducing prostaglandin synthesis, which decreases inflammation and pain at the site of injury. This interferes with transduction of pain perception.
→ NSAIDs primarily inhibit transduction by preventing the formation of prostaglandins that activate nociceptors.
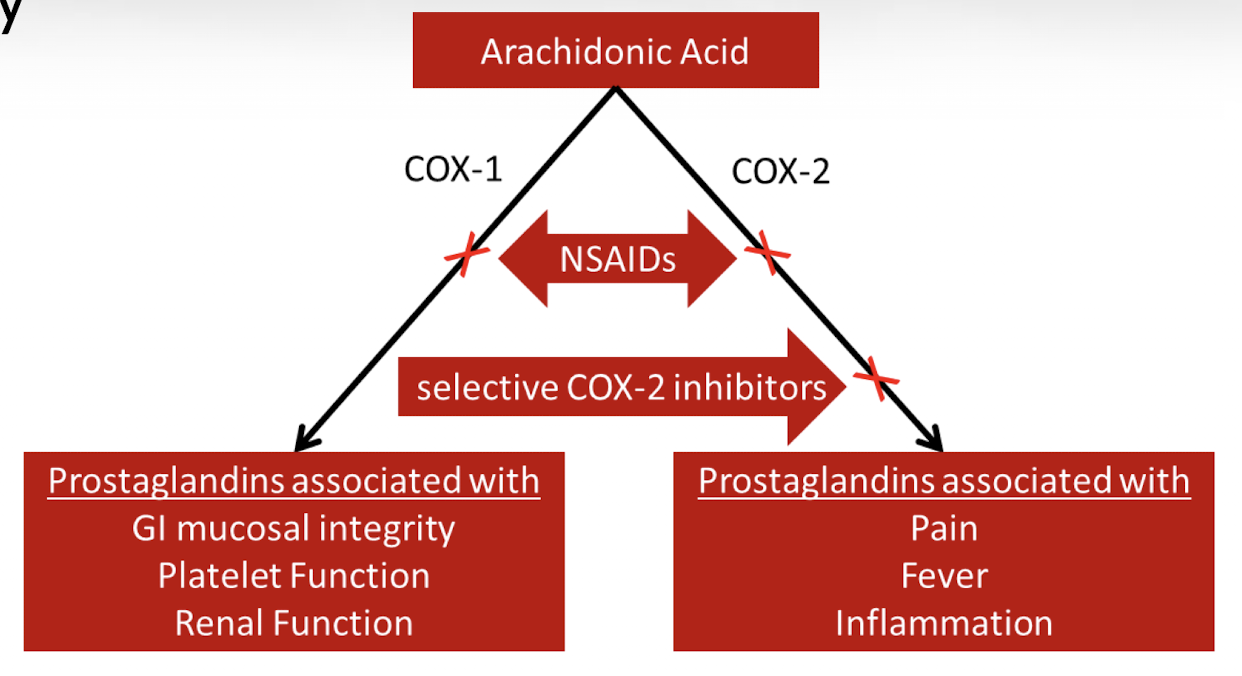
What is the significance of prostaglandins?
Prostaglandins are chemical mediators that promote inflammation, pain, and fever, so reducing their production decreases pain sensation.
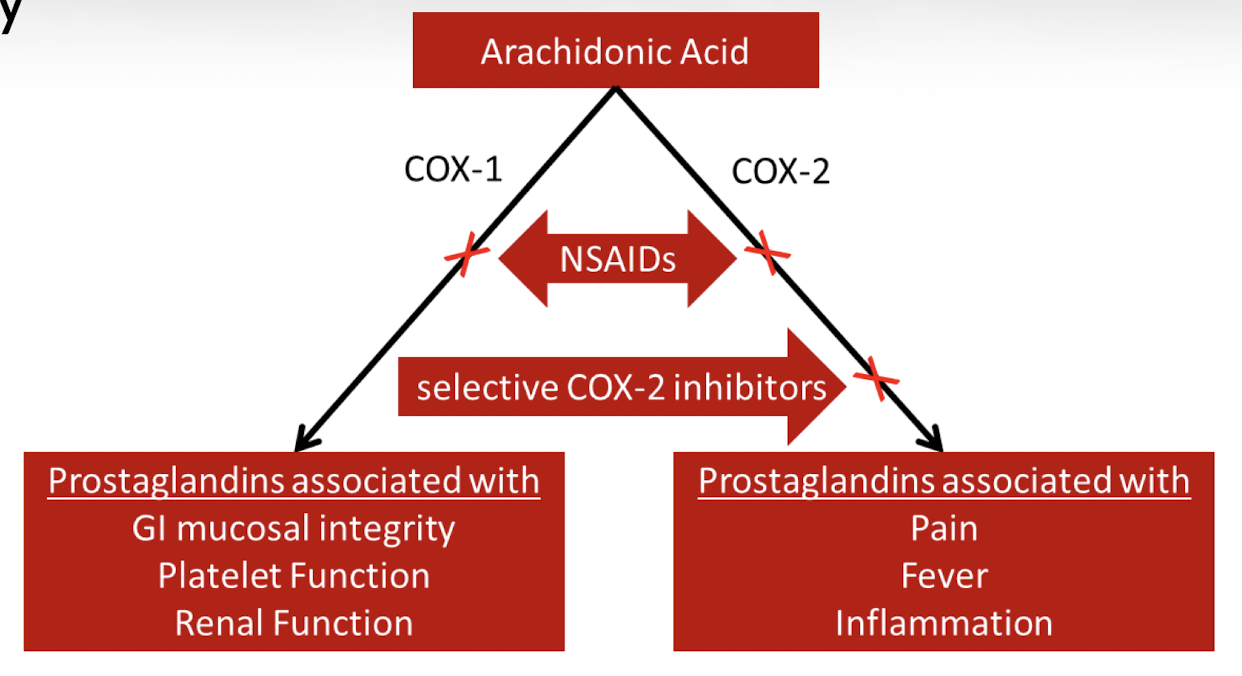
How does acetaminophen differ from NSAIDs?
Acetaminophen does not significantly inhibit peripheral COX enzymes but instead acts centrally in the brain and may influence the endocannabinoid system (interferes with transduction and central pain perception rather than peripheral inflammation).
How do opioids work at the cellular level?
Opioids activate G-protein coupled receptors, leading to decreased neuronal excitability by closing calcium channels, increasing potassium efflux, and reducing cAMP levels.
Which phases of nociception do opioids affect?
Opioids interfere with transmission, modulation, and perception by suppressing neuronal signaling throughout the pain pathway.
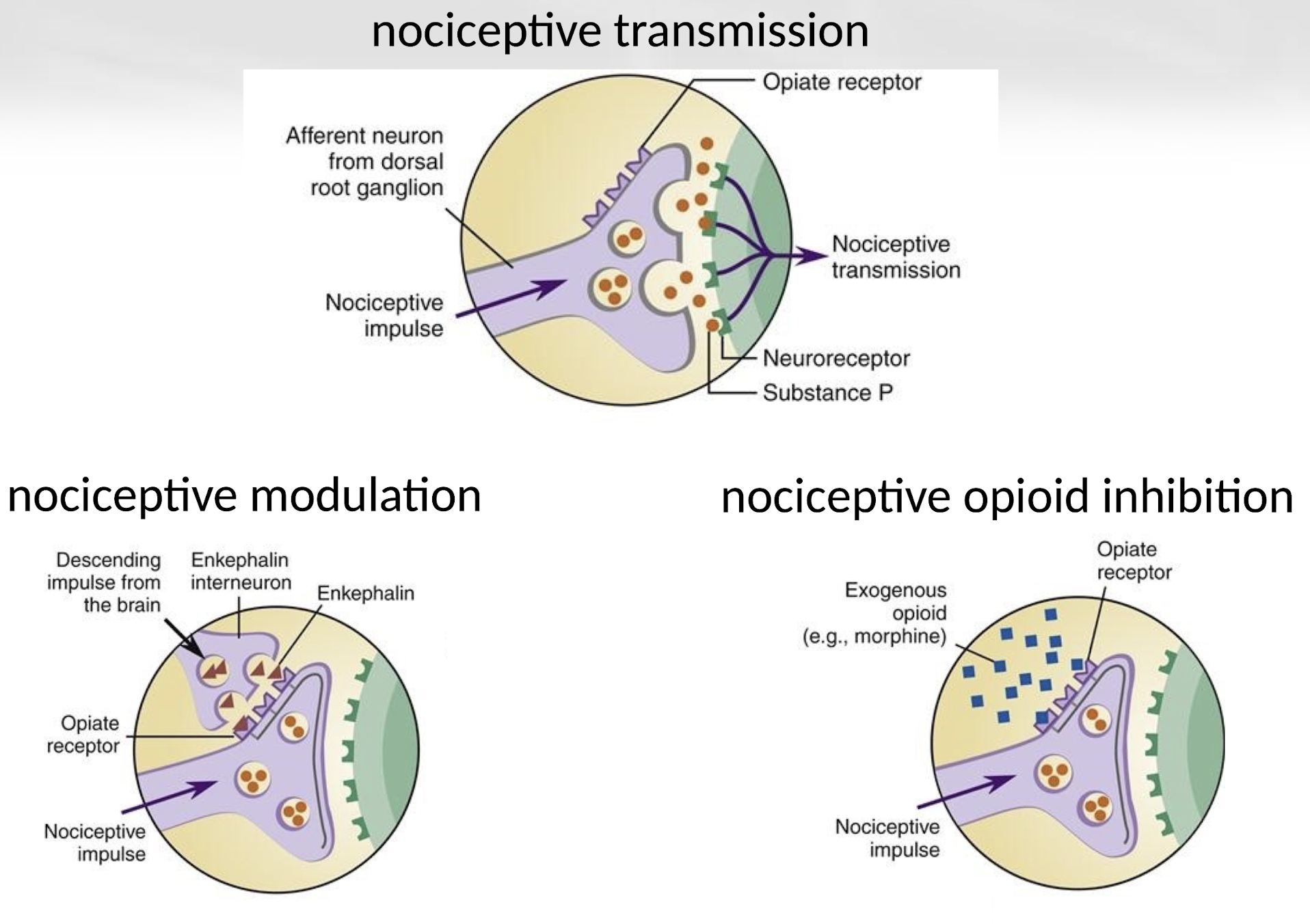
What is the effect of opioids on neurotransmitter release?
Opioids reduce the release of excitatory neurotransmitters from nociceptive neurons, thereby decreasing pain signal transmission.
What does the term “anesthesia” mean?
Refers to an induced, temporary, and reversible loss of sensation or awareness.
What are the three broad categories of anesthesia?
The three categories are local anesthesia, which affects a small area of tissue, regional anesthesia, which affects a larger but specific region, and general anesthesia, which affects the entire body and causes loss of consciousness and sensation.
What are the primary goals of anesthesia?
The goals of anesthesia include analgesia (loss of pain sensation), muscle relaxation, hypnosis (loss of consciousness and memory), and ensuring that these effects are temporary and reversible.
What factors are considered when selecting anesthesia?
The safest and most effective drug should be selected to prevent pain while minimizing recovery time, reducing surgical stress response, and limiting physiological disturbances/complications.
What is the mechanism of action of local and regional anesthetics?
These anesthetics work by blocking sodium (Na⁺) channels in neurons, preventing depolarization and the generation of action potentials, which stops pain signal transmission.
What is the order of sensory blockade in local/regional anesthesia?
Sensory loss occurs in the following order: pain → cold → warmth → touch → deep pressure → motor function
What is a local anesthetic?
A local anesthetic is a drug that produces a reversible loss of pain sensation in a small, specific area without affecting consciousness.
What types of procedures use local anesthesia?
Local anesthesia is commonly used in minor procedures such as dentistry, ophthalmology, dermatology, and podiatry.
How are local anesthetics administered?
They can be applied topically as creams or sprays to skin or mucous membranes, or injected directly into tissues (infiltration) to block nerve endings.
Why are vasoconstrictors added to local anesthetics?
Vasoconstrictors like epinephrine reduce blood flow at the injection site, slowing drug diffusion to make sure it stays localized, prolonging anesthetic effect, and increasing depth of anesthesia.
What is regional anesthesia?
Regional anesthesia blocks pain in a larger part of the body without causing loss of consciousness, often used when local anesthesia is insufficient but general anesthesia is unnecessary.
When is regional anesthesia used?
It is used for surgeries involving larger or deeper areas, such as orthopedic procedures, childbirth, reproductive and urological surgery, gastrointestinal surgery, and thoracic surgery.
What are the main types of regional anesthesia administration?
Regional anesthesia can be delivered through peripheral nerve blocks, spinal anesthesia, or epidural anesthesia.
What is a peripheral nerve block?
A peripheral nerve block involves injecting anesthetic around a specific nerve to block sensation in the area supplied by that nerve.
How is needle placement guided during nerve blocks?
Imaging techniques such as ultrasound, fluoroscopy, or CT scans are used to ensure accurate placement of the anesthetic near the target nerve.
What additional drugs may be used with nerve blocks?
Vasoconstrictors prolong the effect, opioids enhance pain relief, and corticosteroids reduce inflammation.
What is spinal anesthesia?
Spinal anesthesia involves injecting anesthetic into the cerebrospinal fluid in the subarachnoid space, producing a rapid and profound loss of both motor and sensory function below the injection site.
Why must spinal anesthesia be administered below L2?
It must be injected below the L2 vertebra to avoid damaging the spinal cord, which typically ends above this level.
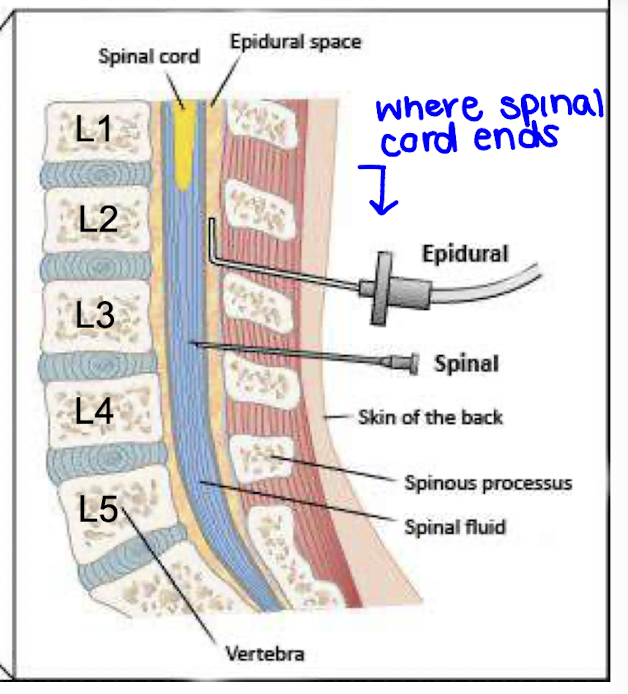
What are key characteristics of spinal anesthesia?
It has a rapid onset (within minutes), requires a small dose, and produces a complete block of motor and sensory function below the injection level.
What is epidural anesthesia?
Epidural anesthesia involves administering anesthetic into the epidural space outside the spinal cord at cervical, thoracic, or lumbar sites, allowing for continuous infusion and controlled anesthesia.
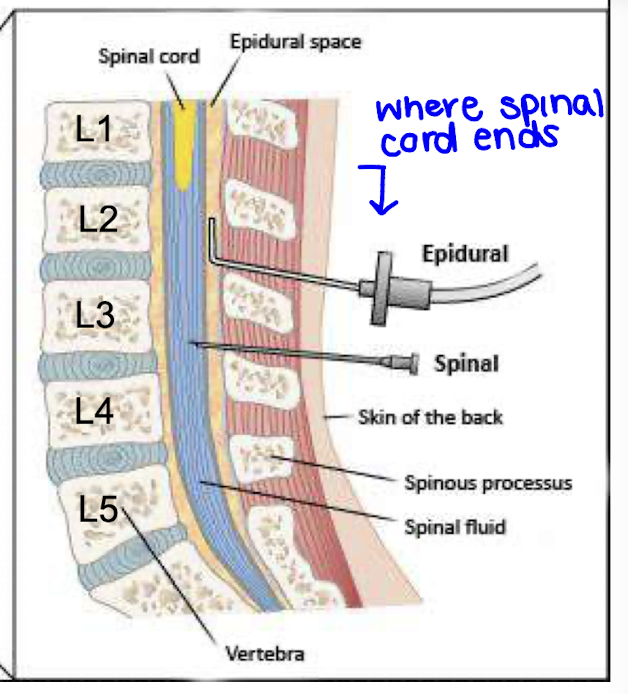
How does epidural anesthesia differ from spinal anesthesia?
Epidurals use larger doses, have a slower onset, and produce a more localized “band” of sensory blockade rather than a complete motor and sensory block.
What are the 5 goals of general anesthesia?
General anesthesia aims to induce analgesia, amnesia, immobility, hypnosis, and paralysis of skeletal muscles.
What is analgesia in general anesthesia?
Analgesia is the loss of pain sensation, preventing the patient from feeling surgical stimuli.
What is amnesia in general anesthesia?
Amnesia is the loss of memory, ensuring the patient does not recall the surgical experience.
What is immobility in general anesthesia?
Immobility is the absence of motor responses to painful stimuli, preventing movement during surgery.
What is hypnosis in general anesthesia?
Hypnosis is the loss of consciousness, meaning the patient is unaware of their surroundings.
What is paralysis in general anesthesia?
Paralysis refers to the relaxation of skeletal muscles and suppression of reflexes, allowing for surgical manipulation.
What physiological effects does general anesthesia reduce?
It decreases respiration, blood pressure, heart rate, and body temperature.
How do general anesthetics work?
They modulate neuronal activity by altering neurotransmitter release and action potential generation, although the exact mechanisms are not fully understood.
How are general anesthetics administered?
They can be administered intravenously or through inhalation.
What are injectable anesthetics?
Injectable anesthetics are drugs given intravenously that rapidly induce unconsciousness, often within 10–20 seconds.
Why are injectable anesthetics often combined with other drugs?
Many lack strong analgesic effects, so they are combined with analgesics to provide complete anesthesia. They are often used to sedate and induce anesthesia prior to maintenance with inhalants
What are examples of injectable anesthetics?
Examples include ketamine, propofol, sodium thiopental, and etomidate.
What are inhalant anesthetics?
Inhalant anesthetics are gases or volatile liquids that are inhaled to maintain anesthesia during surgery.
What properties make inhalant anesthetics effective?
They are non-flammable, non-explosive, lipid-soluble, non-toxic, and non-irritating to the respiratory system.
What are advantages of inhalant anesthetics?
They allow precise control of anesthesia depth, can be maintained for varying durations, and enable rapid recovery after discontinuation.
What are disadvantages of inhalant anesthetics?
They require specialized equipment and may expose medical personnel to anesthetic gases.
What are examples of inhalant anesthetics?
Common inhalants include isoflurane, sevoflurane, desflurane, and nitrous oxide.
How is anesthetic potency measured?
Potency is measured as the dose required to prevent a response to a stimulus in 50% of subjects, expressed as ED50 for injectables or MAC for inhalants.
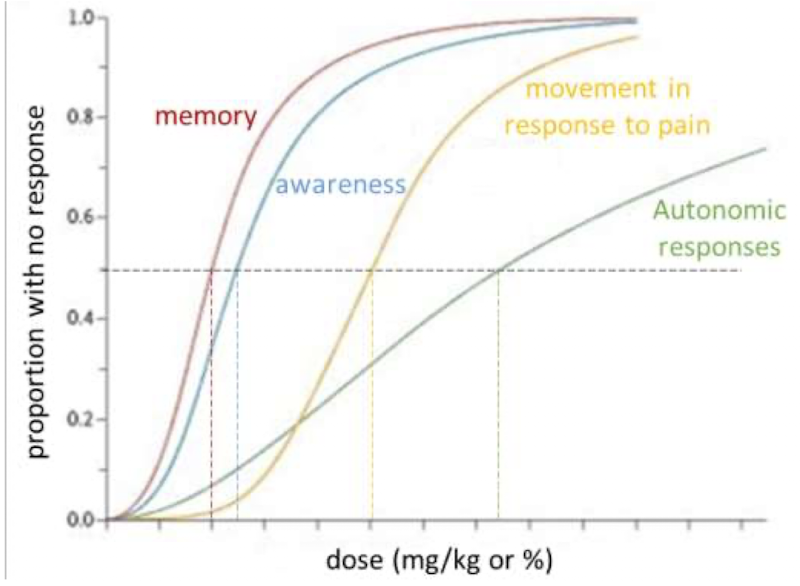
What is MAC (minimum alveolar concentration)?
MAC is the concentration of inhaled anesthetic required to prevent movement in response to a surgical stimulus in 50% of subjects.
How does MAC relate to potency?
MAC is inversely proportional to potency, meaning a lower MAC indicates a more potent anesthetic.
What is MAC50?
MAC50 is the concentration required to prevent motor response to a surgical incision in 50% of patients.
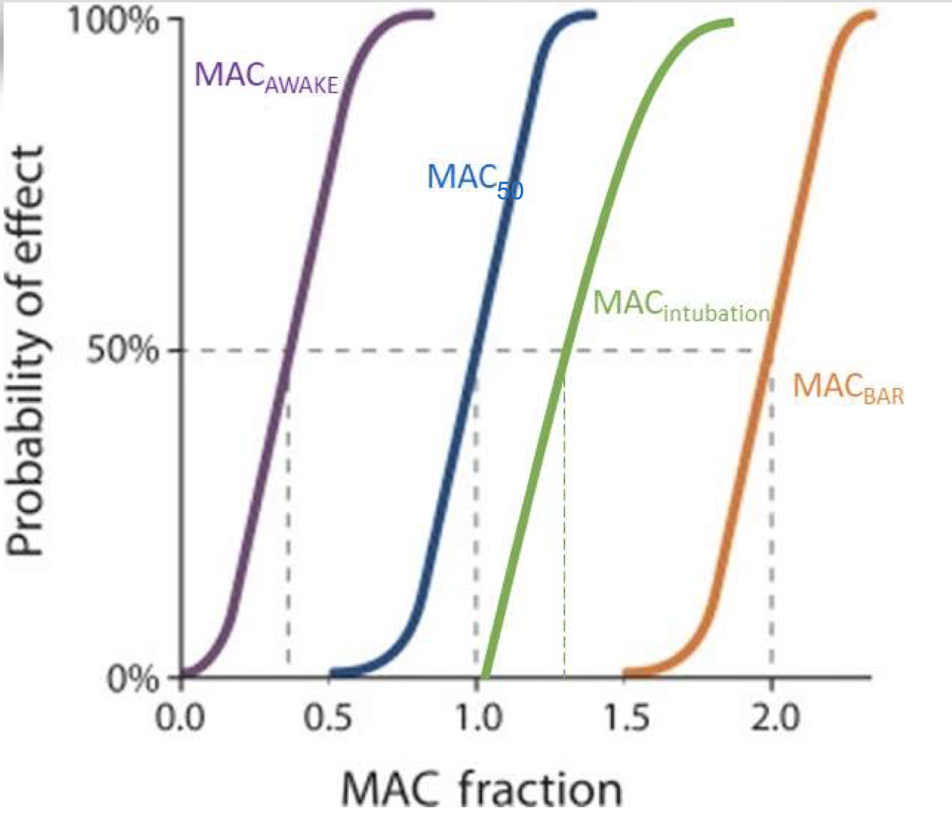
What is MACawake?
MACawake is the concentration at which 50% of patients respond to verbal commands, typically about 30% of MAC.
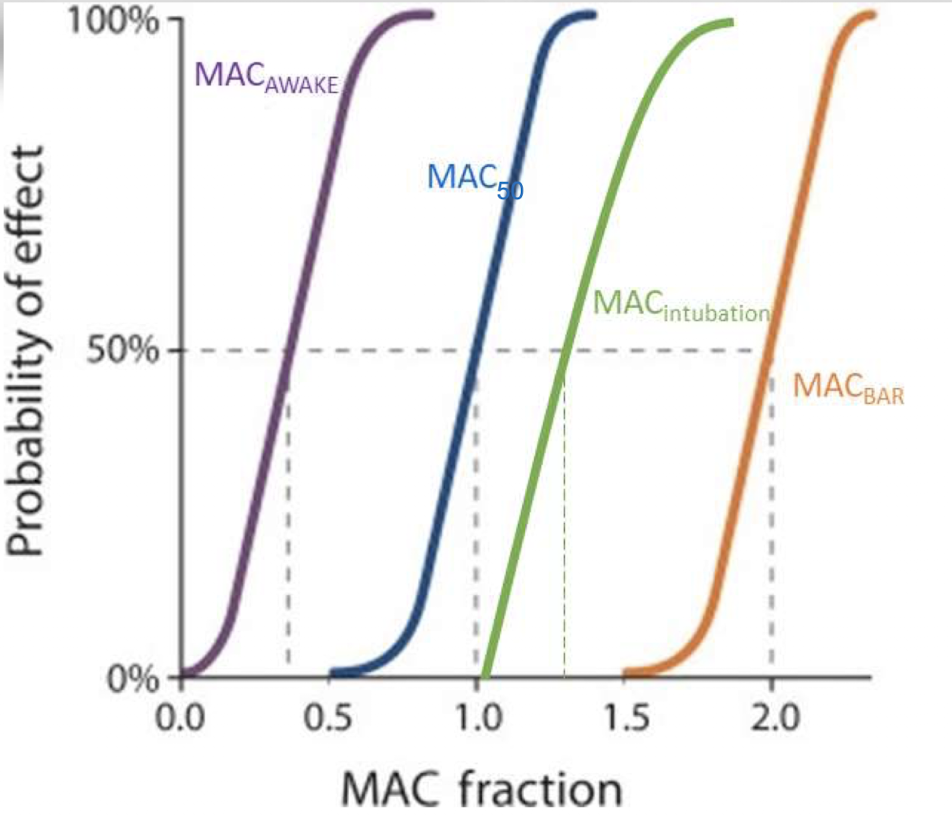
What is MAC95?
MAC95 is the concentration required to prevent movement in 95% of patients.
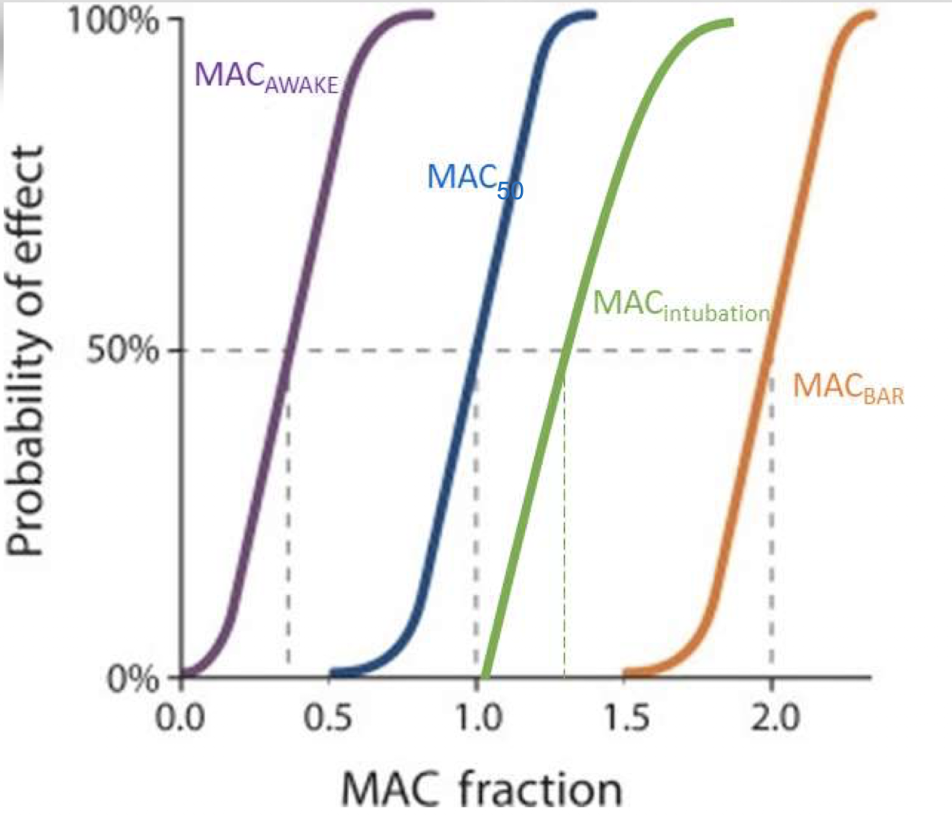
What is MACintubation?
MACintubation is the concentration needed to allow intubation without resistance or coughing in 50% of patients.
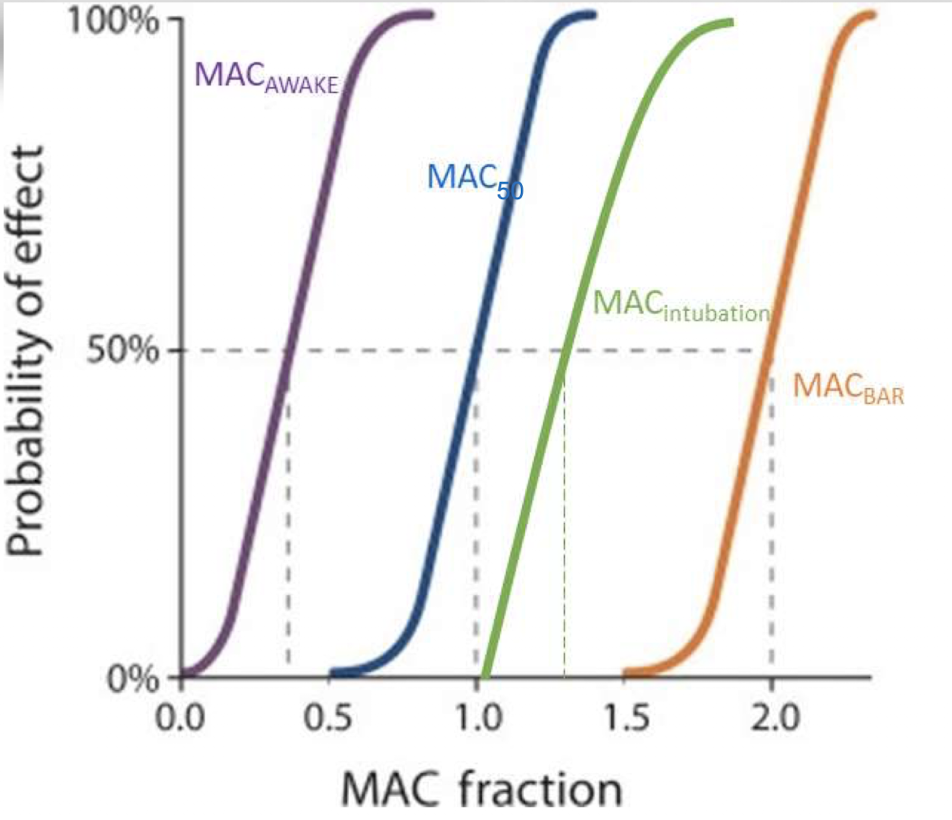
What is MACBAR?
MACBAR is the concentration required to block autonomic responses such as increased heart rate and blood pressure during surgery.
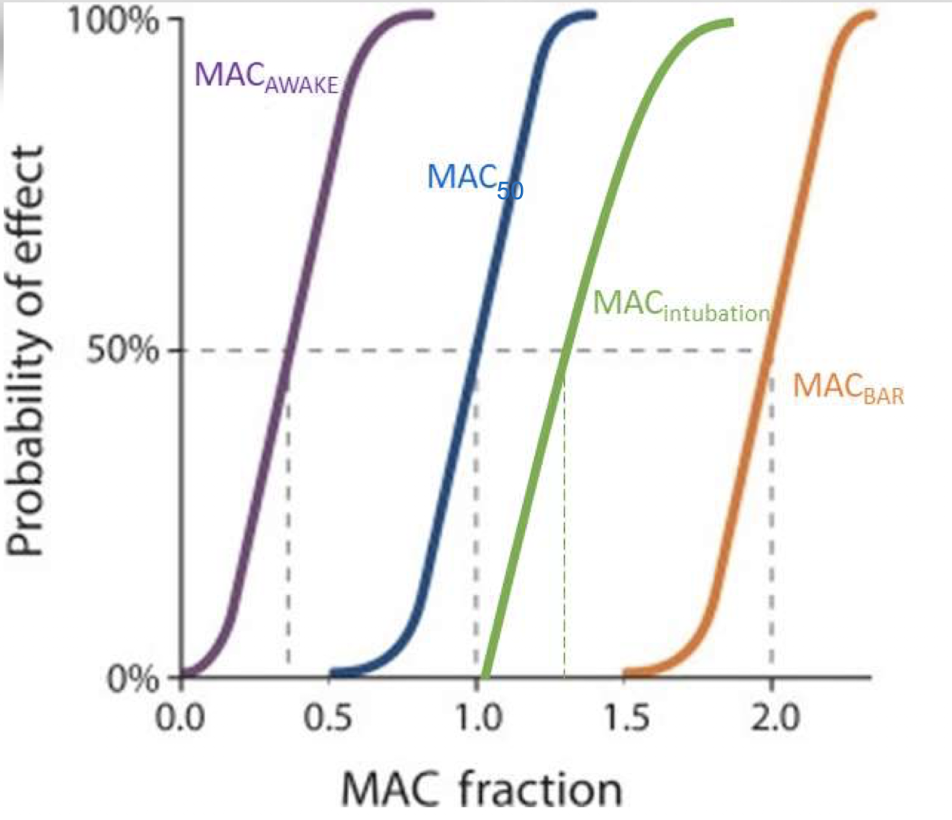
What is the purpose of pre- or co-anesthetic medications?
These medications are used to make anesthesia safer, reduce stress, and improve the overall surgical experience.
What effects do pre-anesthetic drugs provide?
They reduce anxiety, prevent allergic reactions, relieve pain, reduce nausea, and counteract potential side effects of anesthesia.
What types of drugs are used as pre-anesthetic medications?
These include sedatives, antihistamines, opioids, antiemetics, and anticholinergics.
What is the role of sedatives in anesthesia?
Sedatives reduce anxiety and induce relaxation and partial amnesia before anesthesia.
What is the role of antihistamines?
Antihistamines prevent allergic reactions during surgery.
What is the role of opioids in pre-anesthesia?
Opioids provide pain relief before and during surgical procedures.
What is the role of antiemetics?
Antiemetics prevent nausea and vomiting associated with anesthesia.
What is the role of anticholinergics?
Anticholinergics reduce secretions and prevent complications such as bradycardia and hypotension.
What are some predisposing conditions that can increase risk with anesthesia?
Smoking, heavy alcohol use, age, obesity, health problems, medications, drug allergies, history of adverse reactions
What are some common minor side effects of anesthesia?
Confusion, memory loss, drowsiness, dizziness, nausea, vomiting, dry mouth, shivering, sore throat, hoarseness
What are some respiratory and cardiac complications that can occur with anesthesia?
Respiratory arrest, pulmonary edema, persistent bronchospasm, traumatic lung injury, cardiac arrest, stroke, heart failure, heart attack
When is anesthesia awareness more likely to occur?
When neuromuscular blocking agents are also used since patient cannot move or speak to indicate awareness or pain
What is diagnostic imaging?
Diagnostic imaging is the process of creating medical images of the body to identify, diagnose, and monitor diseases or injuries, especially when a condition cannot be determined through physical examination or laboratory testing.
Why is diagnostic imaging important in medicine?
Diagnostic imaging is crucial because it allows for early detection of disease, helps guide treatment planning, and provides internal visualization of structures that cannot be assessed externally.
Why is diagnostic imaging considered noninvasive?
Diagnostic imaging is considered noninvasive because it does not require incisions into the body, although in some cases anesthesia may still be required, especially in veterinary patients.
What are the two most common diagnostic imaging techniques?
The two most common techniques are radiography (x-rays), which uses ionizing radiation, and ultrasonography (ultrasound), which uses sound waves.