physiology test 1
1/236
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
237 Terms
what are levels of organization
how molecules, cells, tissues, and organs work together to make animals function
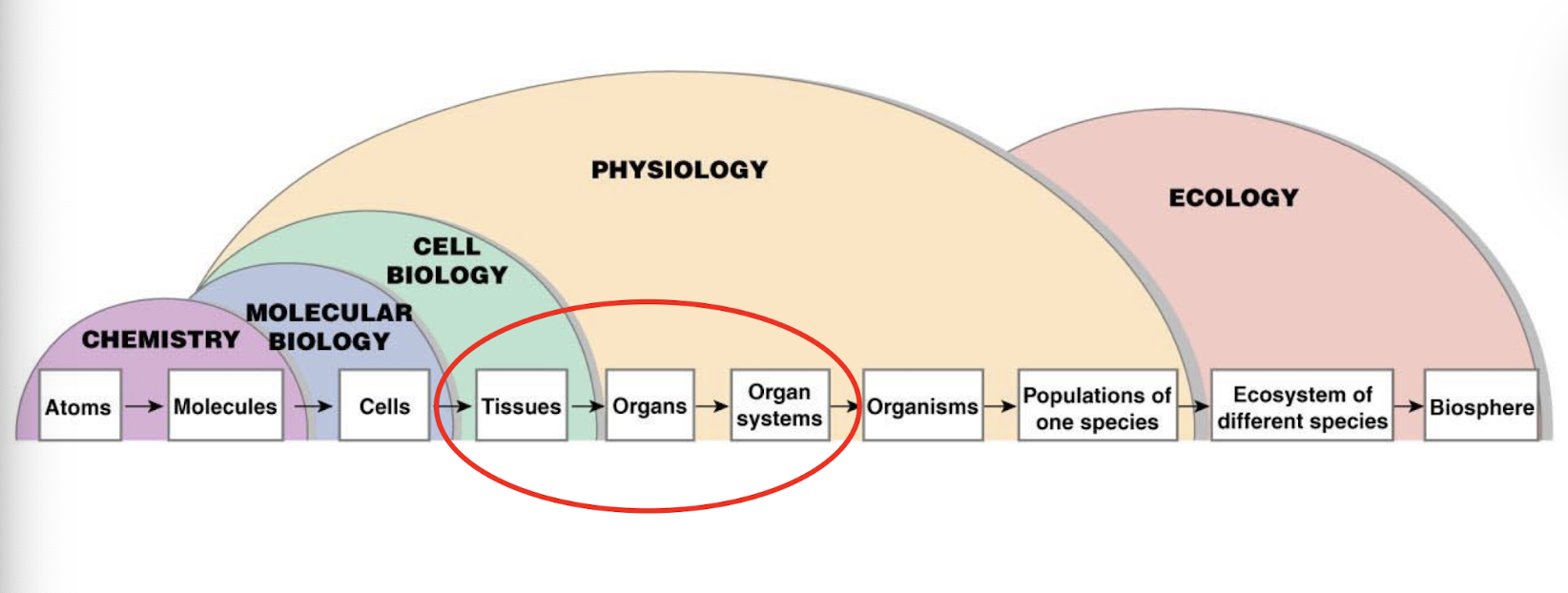
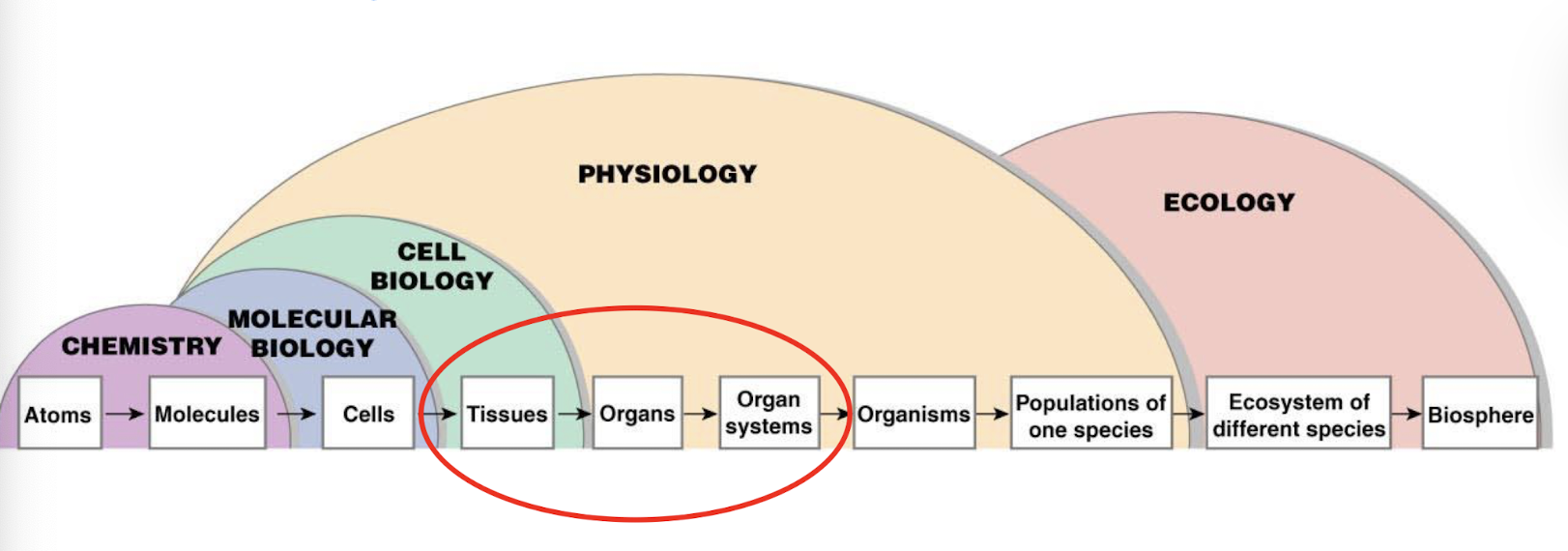
what are the different levels of organization focused on in physiology
molecules, cells, tissues, organs, organ systems, organisms, and populations of one species
we are especially focusing on tissues, organs, and organ systems
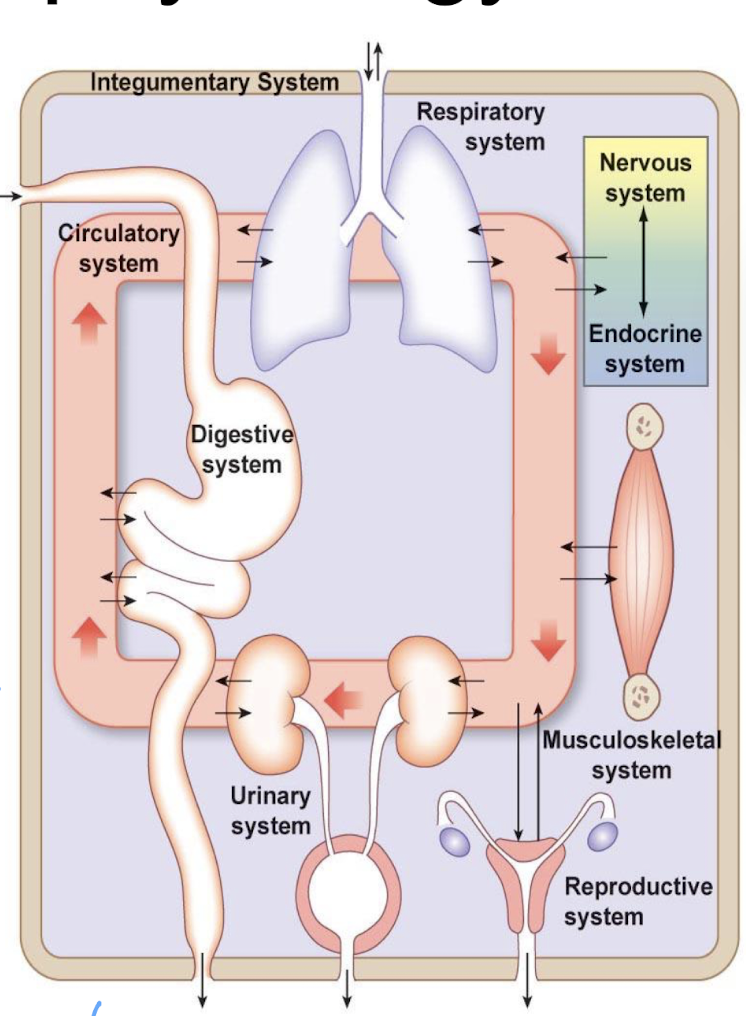
what are the key systems in physiology
communication systems (nervous, endocrine)
internal transport systems (circulatory, lymphatic)
input/output systems (digestive, urinary, respiratory)
mobility systems (musculoskeletal)
immune systems
reproductive systems
how do organisms living in different external environments maintain the same internal requirements
regulate the characteristic using energy
the cells inside of an organism are only exposed to a regulated internal environment, not to the harsh external environment

what is an external environment
anything (air, fluid, solid) that is outside of our barrier cells, including things in the hollow tubes of our digestive, excretory, and respiratory systems
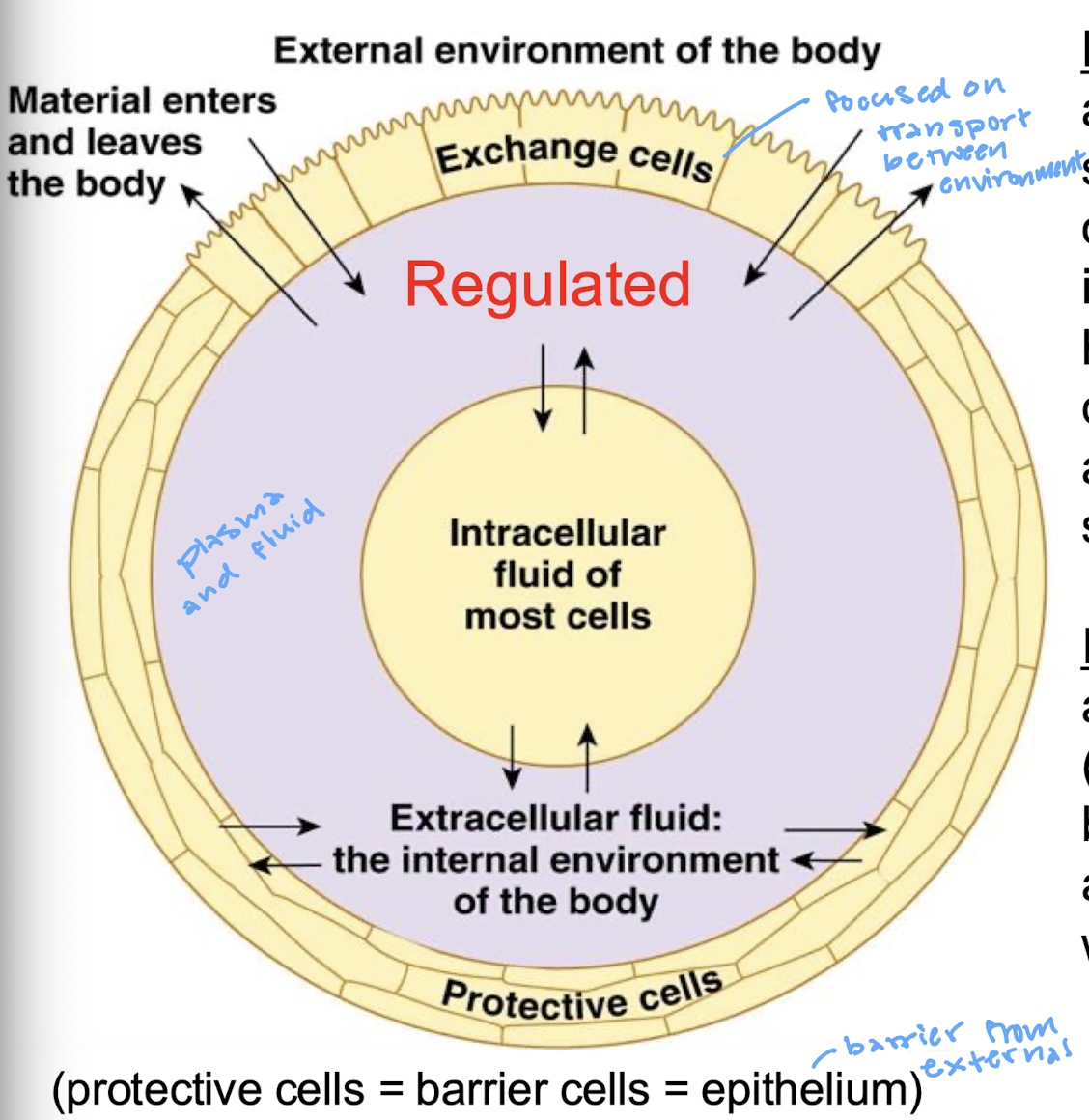
what is the internal environment
any extracellular fluid (ECF) within our bodies that surrounds and is in direct contact with non-barrier cells
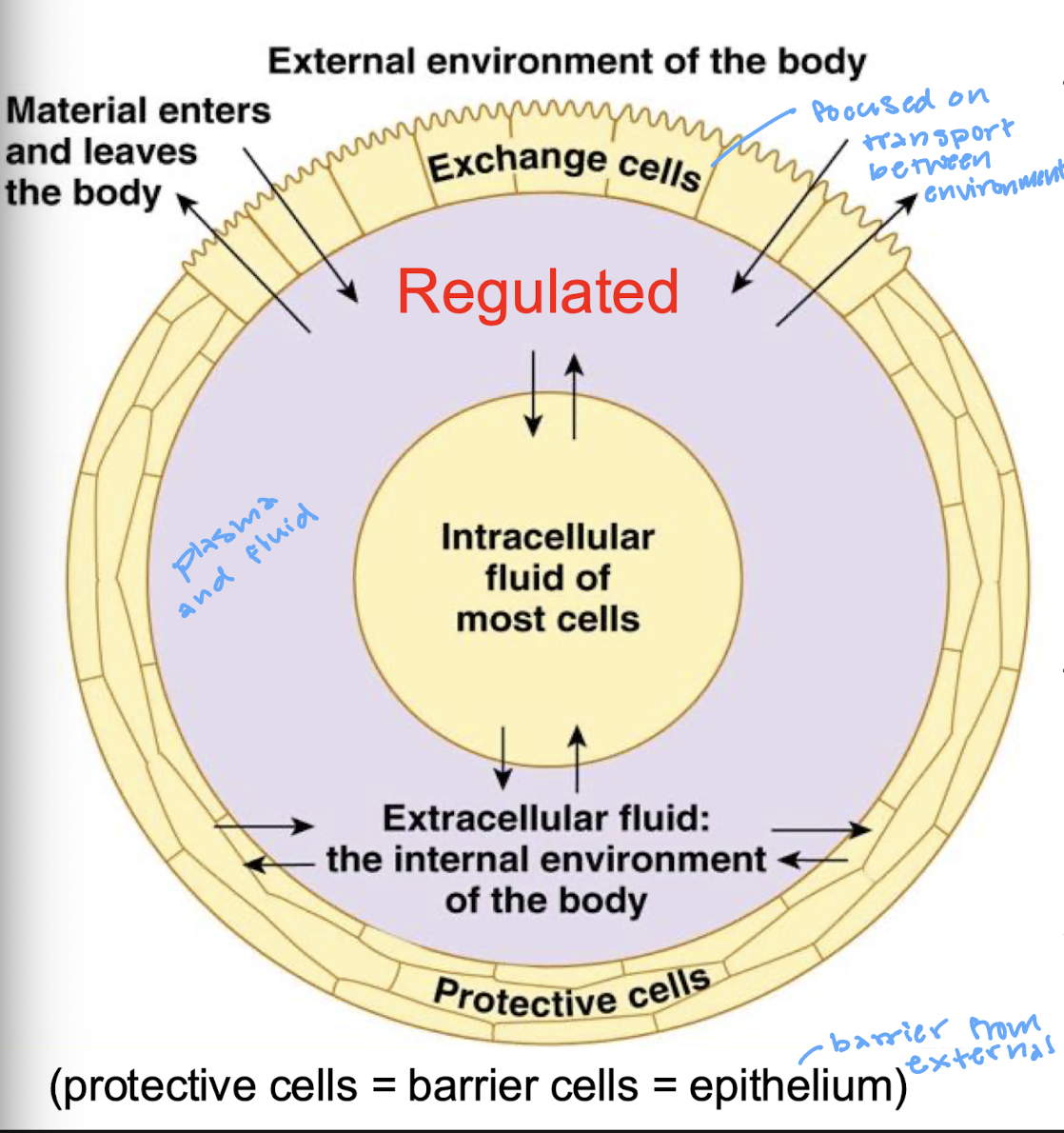
describe barrier cells
protective cells or epithelium that is a barrier from the external environment
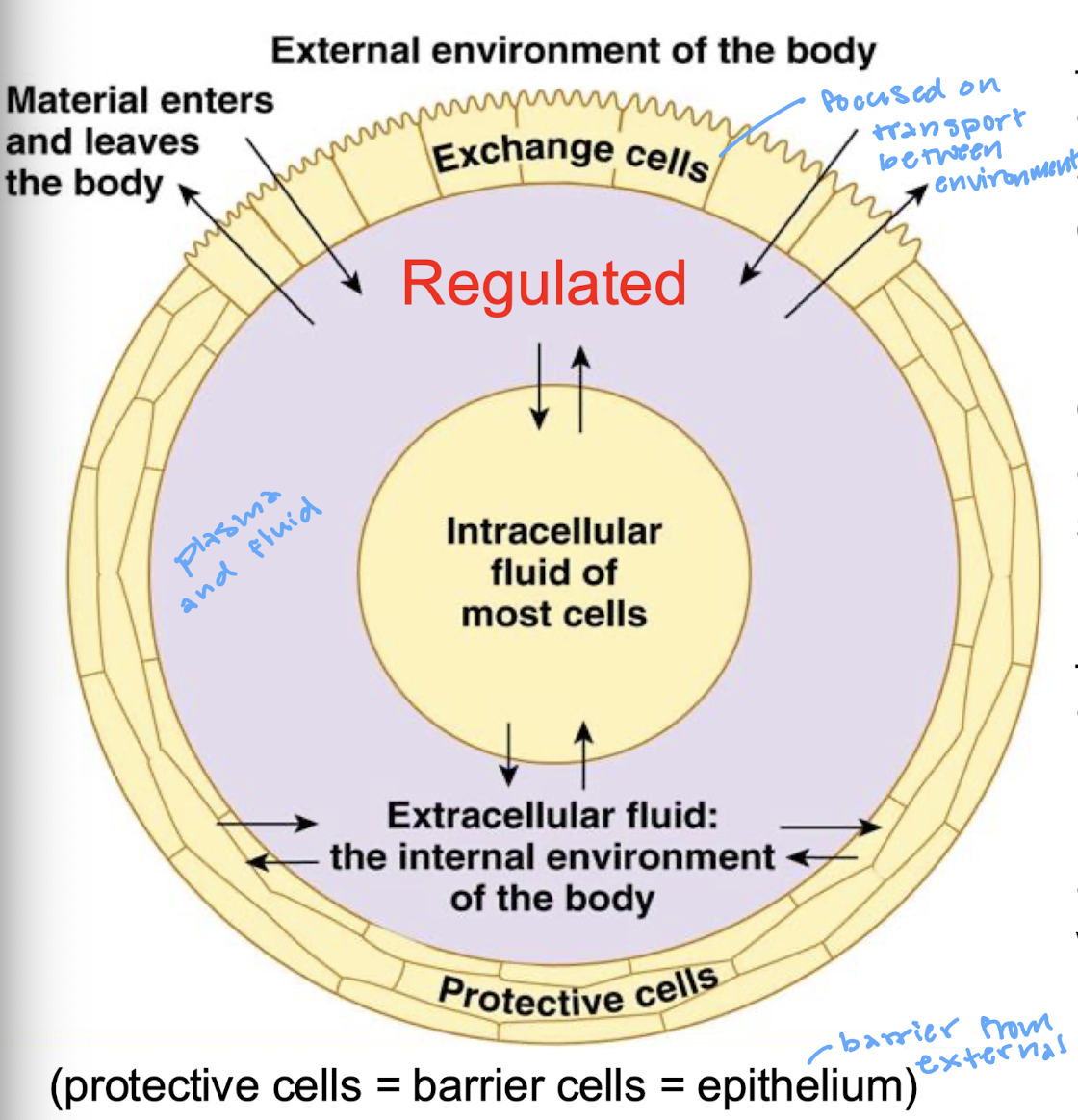
describe the extracellurlar fluid (ECF)
the internal environment of the body (plasma and fluid)
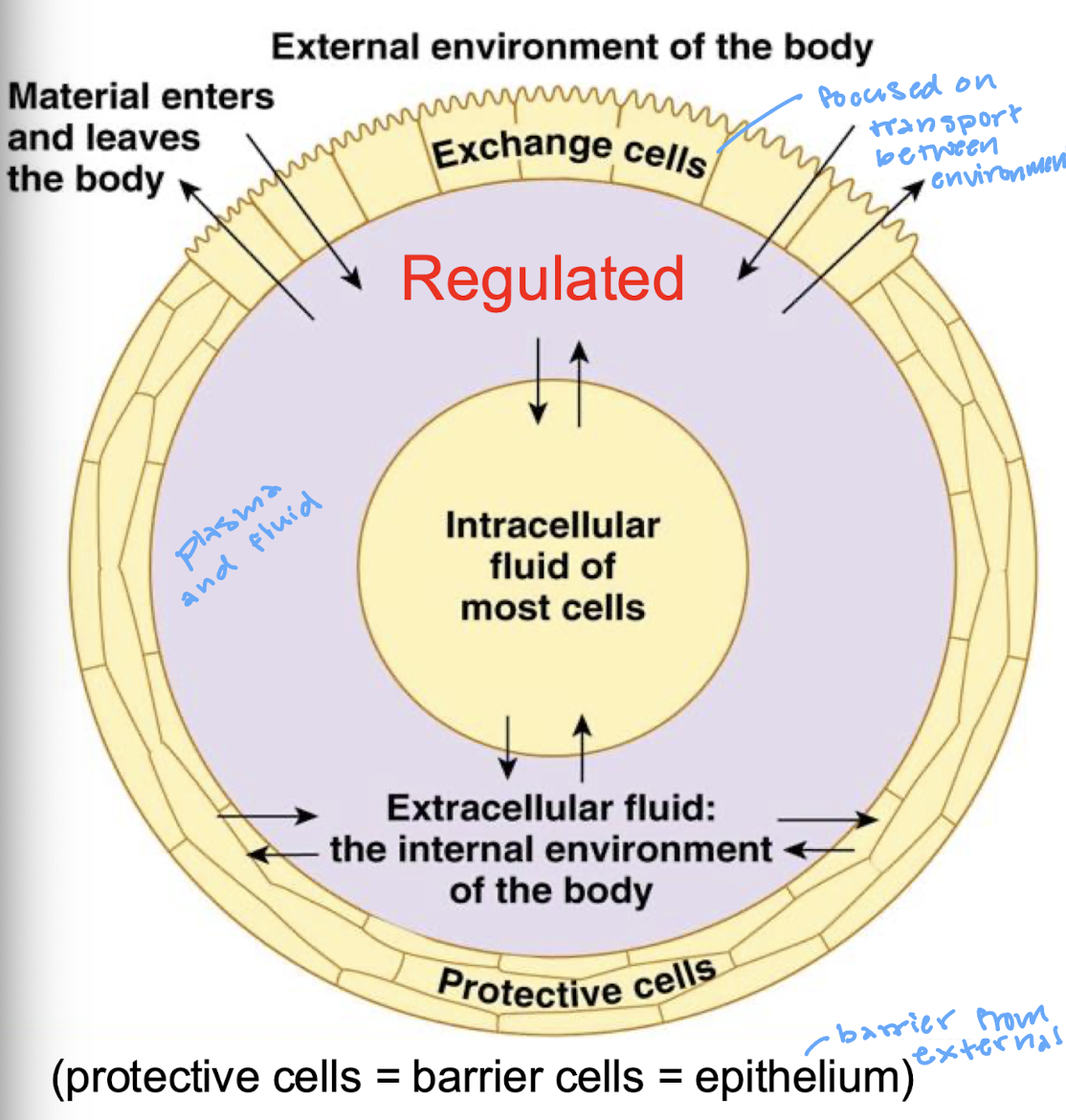
describe epithelial cells
the barrier to and allow for exchange with the internal environment
absorption and secretion
important for the immune system
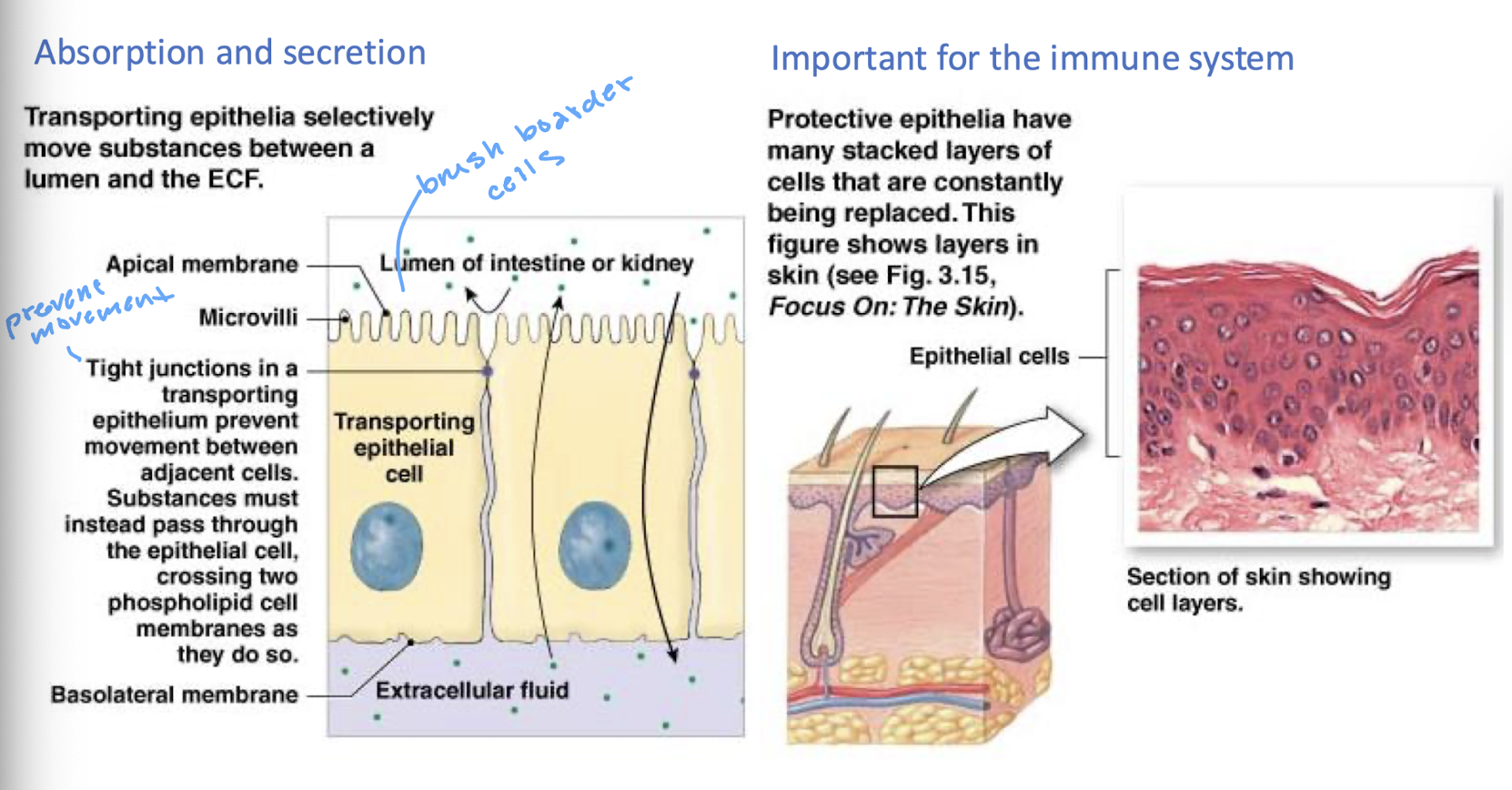
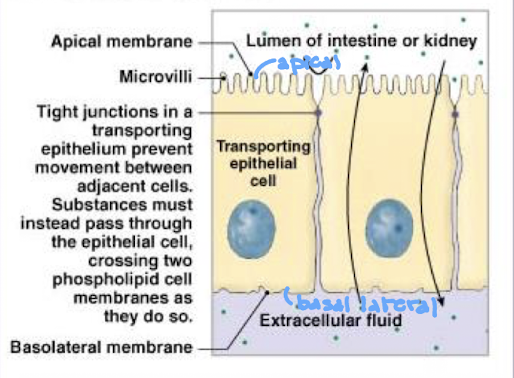
describe how epithelial cells aid in absorption and secretion
transporting epithelia selectively move substances between a lumen and the ECF
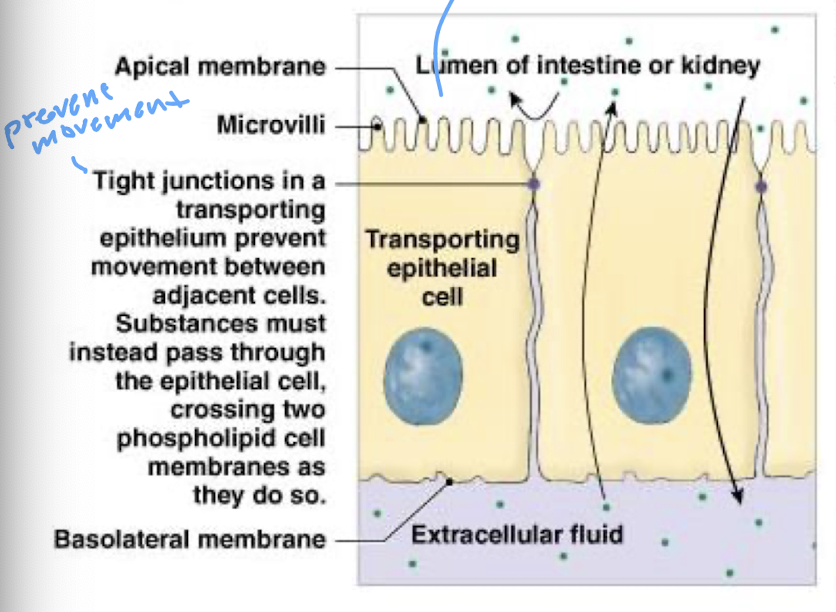
label the lines of the epithelial cells
lumen of intestine or kidney
apical membrane
microvilli
tight junctions
basolateral membrane
extracellular fluid
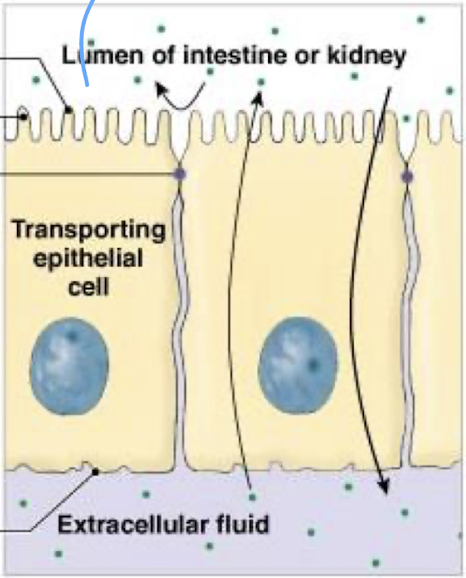
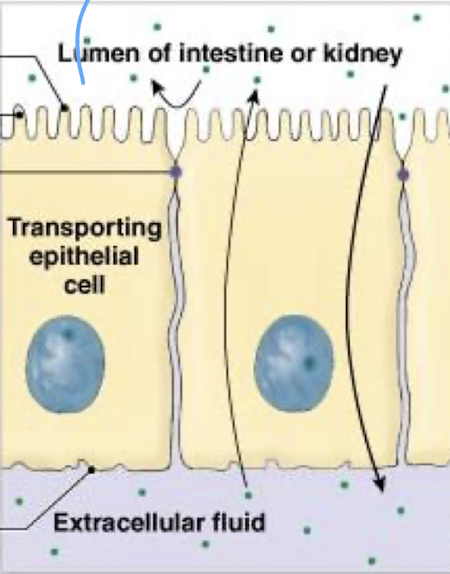
what are tight junctions
a transporting epithelium prevent movement between adjacent cells
substances must instead pass through the epithelial cell, crossing two phospholipid cell membranes as they do so
describe how epithelial cells are important for the immune system
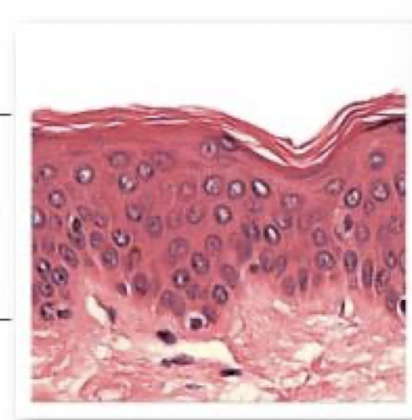
protective epithelia have many stacked layers of cells that are constantly being replaced
example: layers in skin
what are the two fluid compartments of the body
extracellular fluid
intracellular fluid
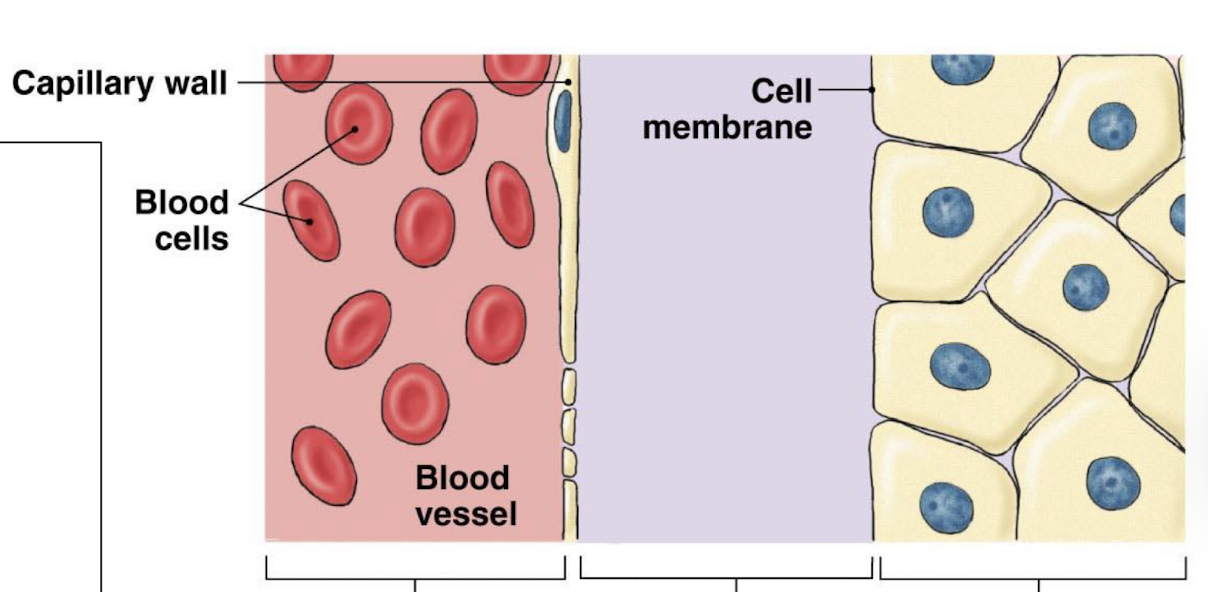
what is included in the extracellular fluid compartment
interstitial fluid
blood plasma
cerebral spinal fluid (CSF)
lymph fluid
divided into the plasma and interstitial fluid and materials moving between cells and ECF must cross the cell membrane
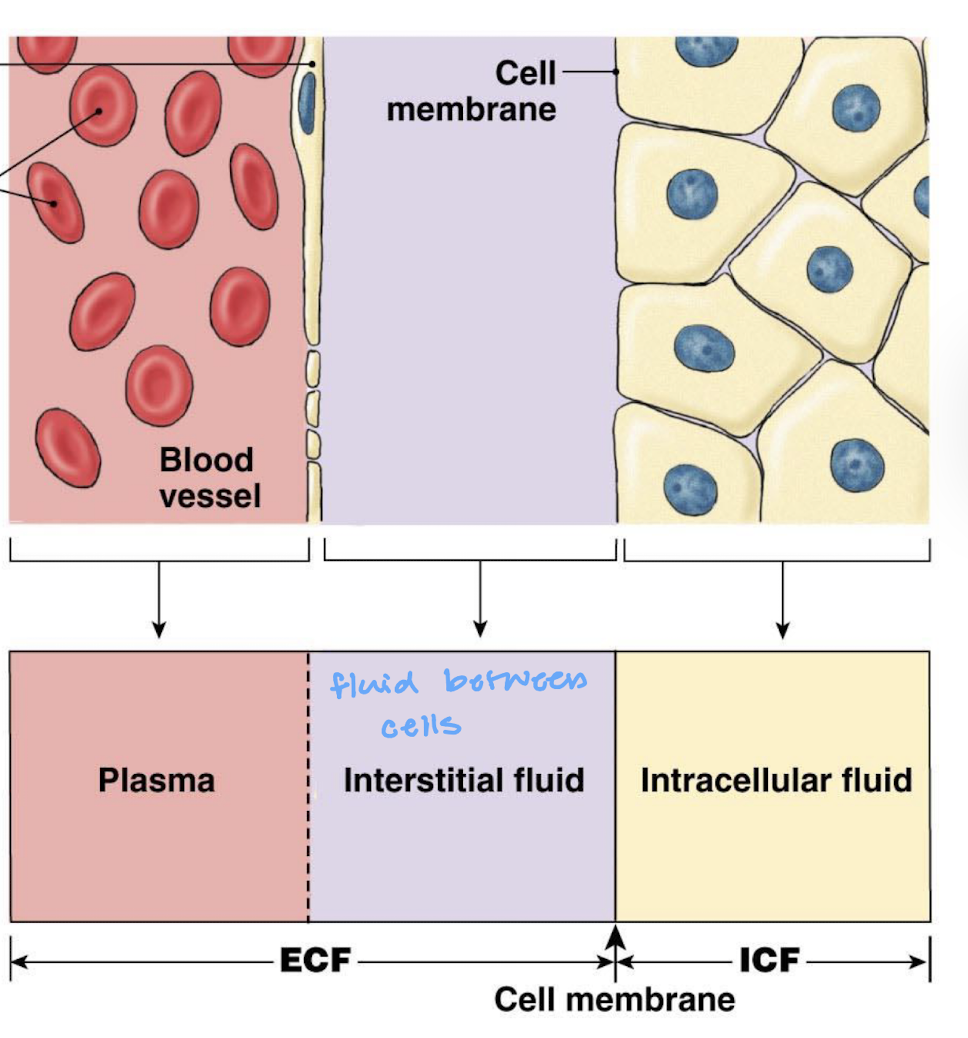
what is included in the intracellular fluid compartment of the body
cytosol
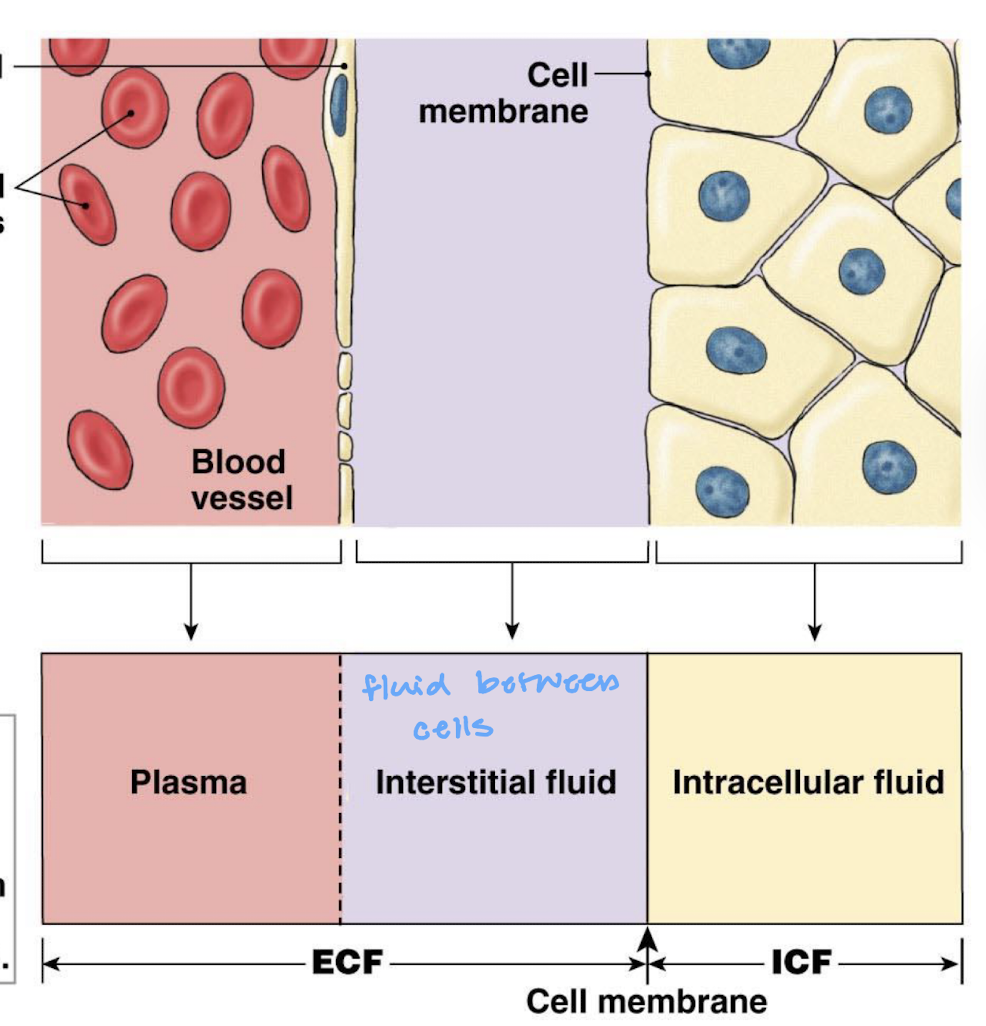
what does it mean by the internal environment does not equal the intracellular fluid, cells, or cytoplasm
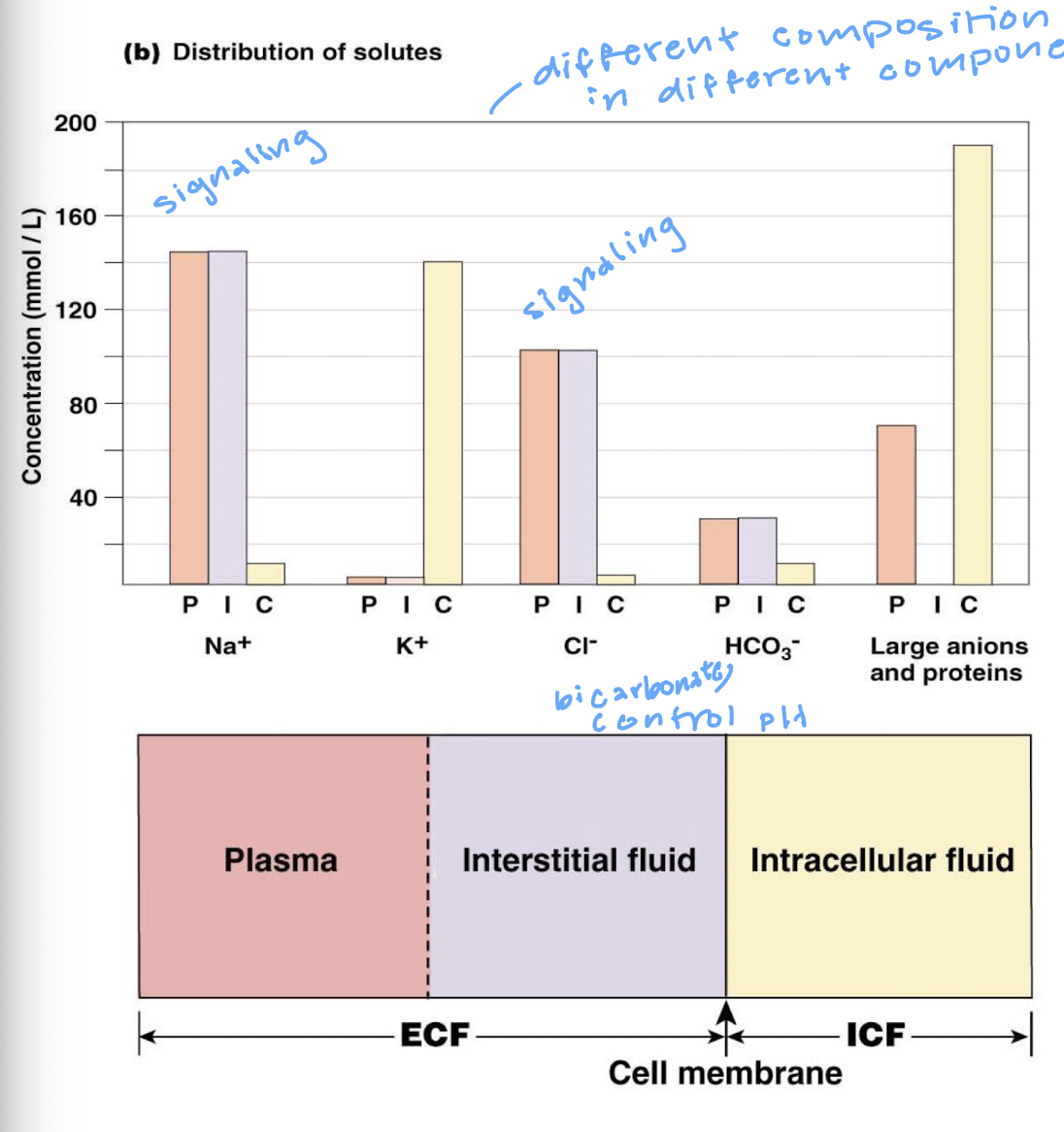
the composition of our internal environment is highly regulated with each having its own distribution
when the ECF compostion changes outside of an acceptable range compensatory mechanisms activate to return the fluid to its normal state
regulated variables include: ion, nutrient, and energy molecule concentrations; pH, gases, temperature, etc
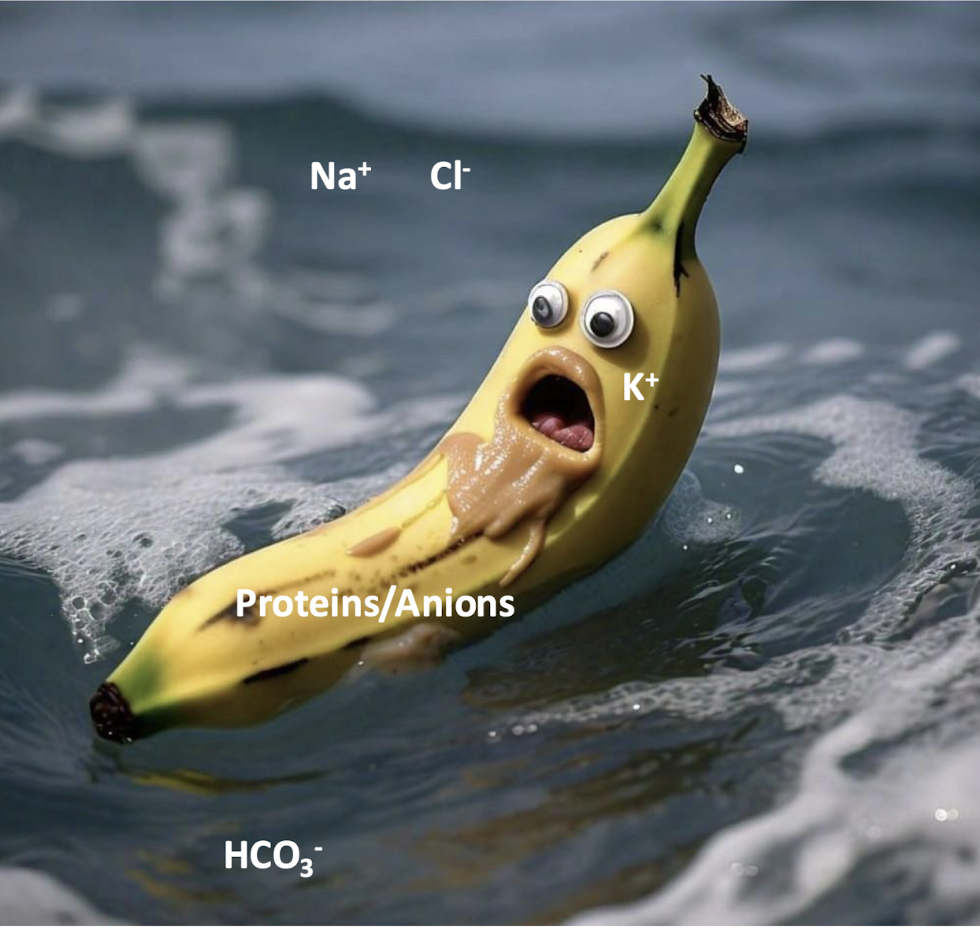
describe the banana in the ocean analogy
the ocean is the ECF with high concentrations of Na+, Cl-, and HCO3-
the banana is the cell that is K+ rich
the peanut butter is proteins and anions
the distribution is important for membrane dynamics
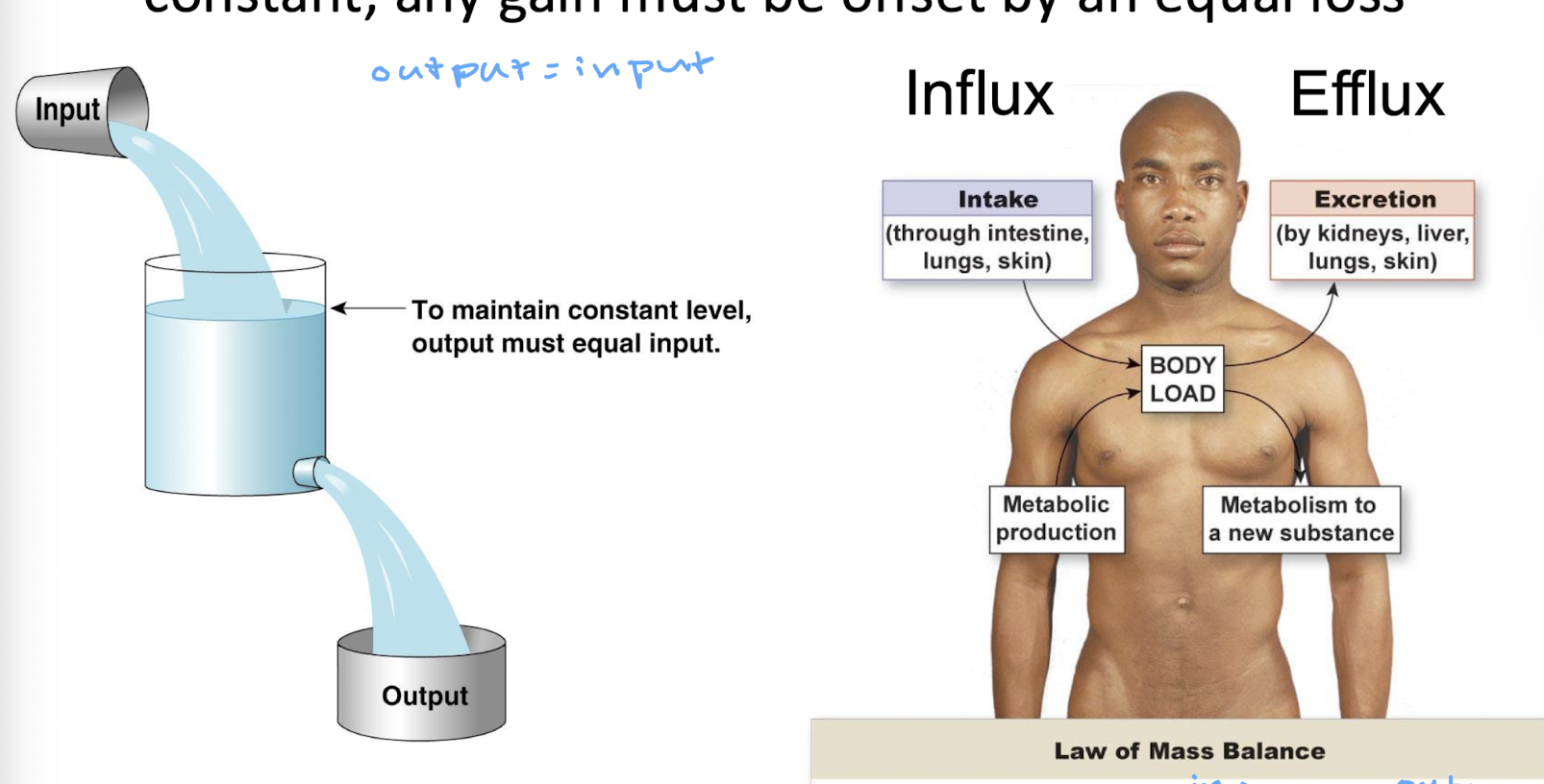
describe the law of mass balance
if the amount of a substance in the body is to remain constant, any gain must be offset by an equal loss (output has to equal input)
mass balance = (existing body load) + (intake or metabolic production) - (excretion or metabolic removal)
regulation doesn’t mean no change, it means no net change
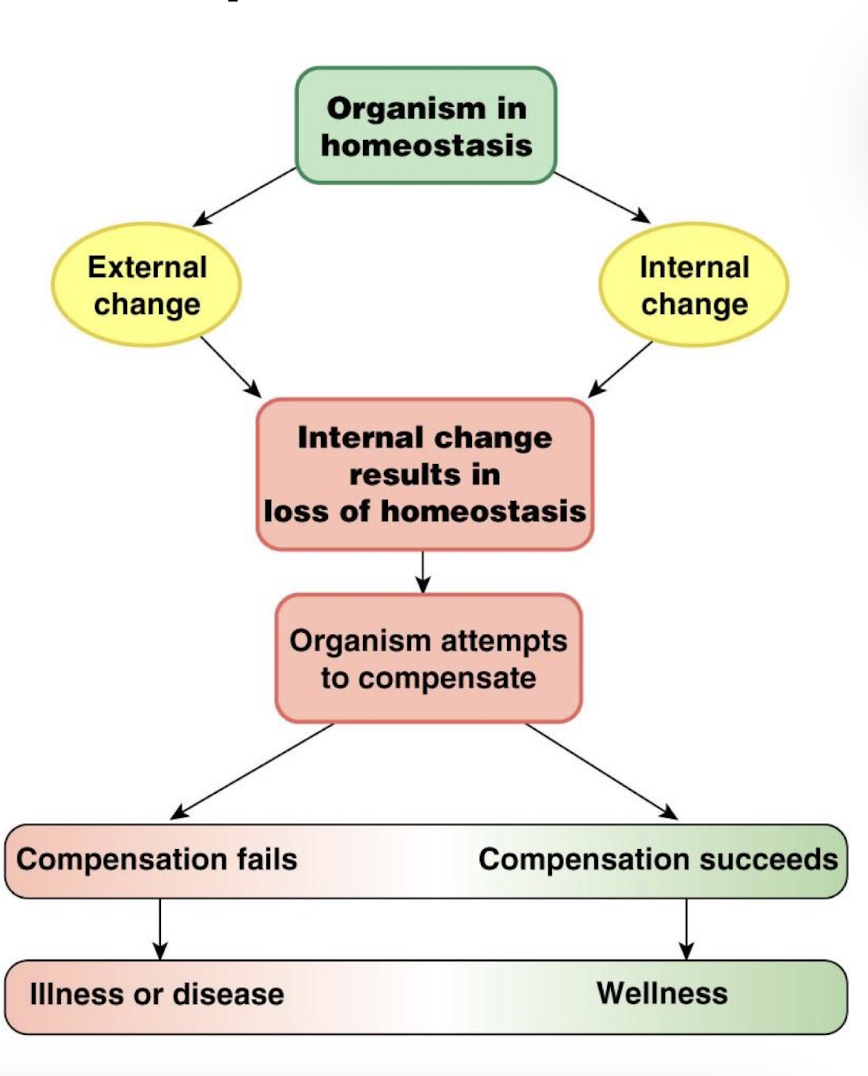
what is equilibrium
a state in which opposing forces or influence are balanced
an animal’s body is NEVER fully at equilibrium with the environment
what is homeostasis
the composition of the body compartments are relatively stable and within the range required by cells for life
O2, CO2, osmolarity, BP, NaCl, temperature, glucose
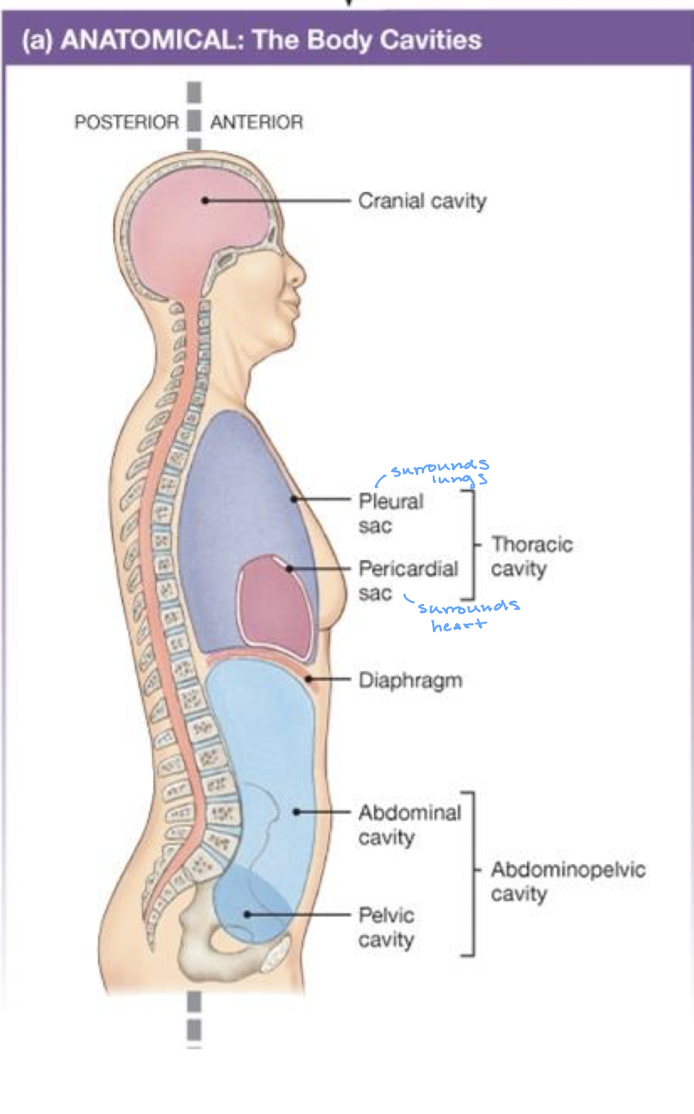
what are the anatomical body compartments
cranial cavity
thoracic cavity
plueral sac surrounding the lungs
pericardial sac surrounding the heart
diaphragm
abdominopelvic cavity
abdominal cavity
pelvic cavity
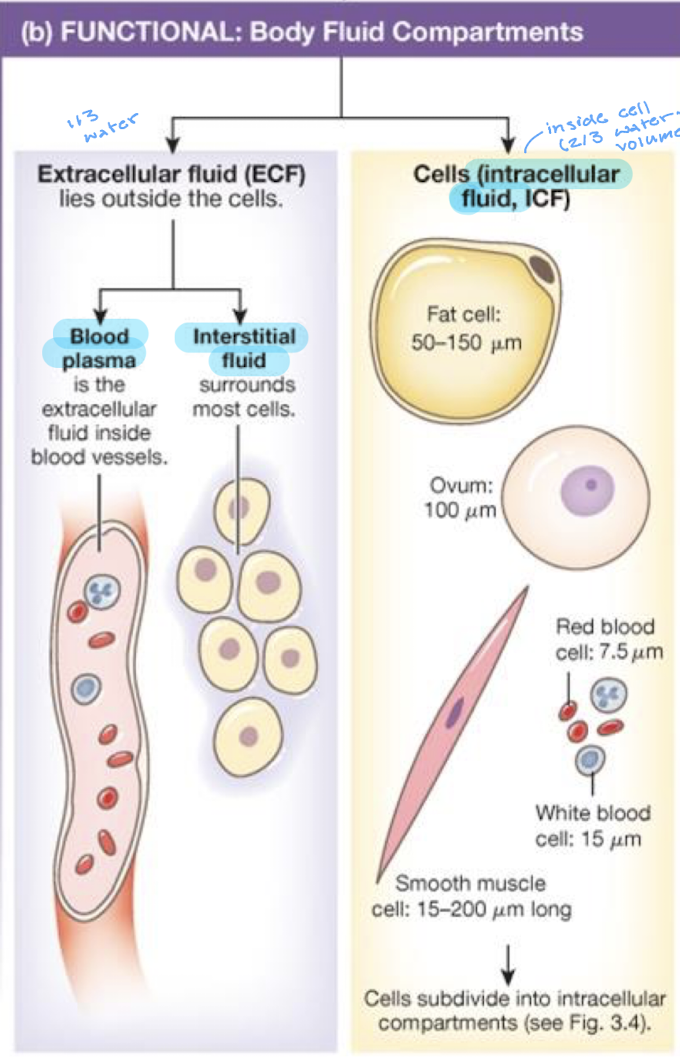
what are the different functional body fluid compartments
extracellular fluid (lives outside the cells)
blood plasma (extracellular fluid inside blood vessels)
interstitial fluid (surrounds most cells)
cells (intracellular fluid, ICF)
describe how all compartments are separated by membranes
the pericardial sac is a tissue that surrounds the heart
tissue membranes have many cells that are supported by connective tissues
each cell has a cell membrane surrounding it
phopholipid bilayers create cell membranes
describe how membranes are composed of a lipid bilayer
phospholipids have 2 fatty acids and a phosphate group
cholesterol and phospholipids are important components of animal cell membranes
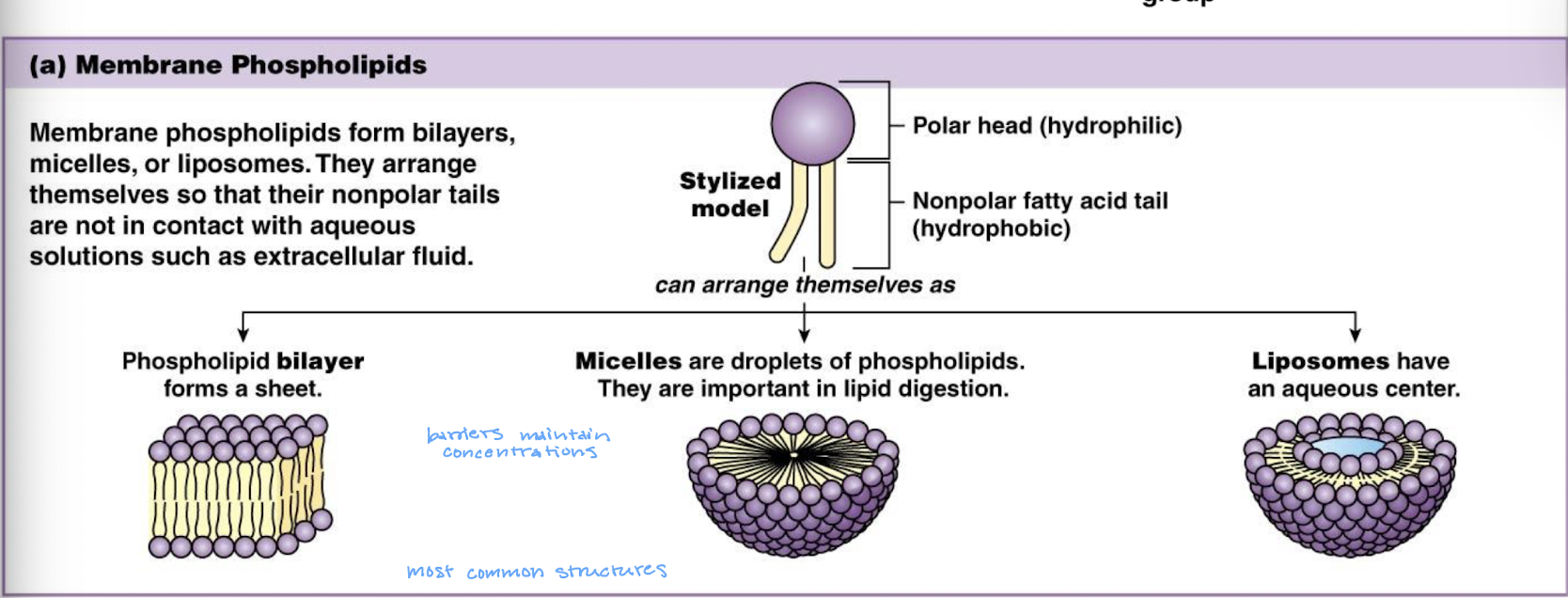
membrane phospholipids can form bilayers (sheets), micelles (droplets of phospholipids), liposomes (have an aqueous center)
they arrange themselves so that their nonpolar tails are not in contact with aqueous solutions such as extracellular fluid
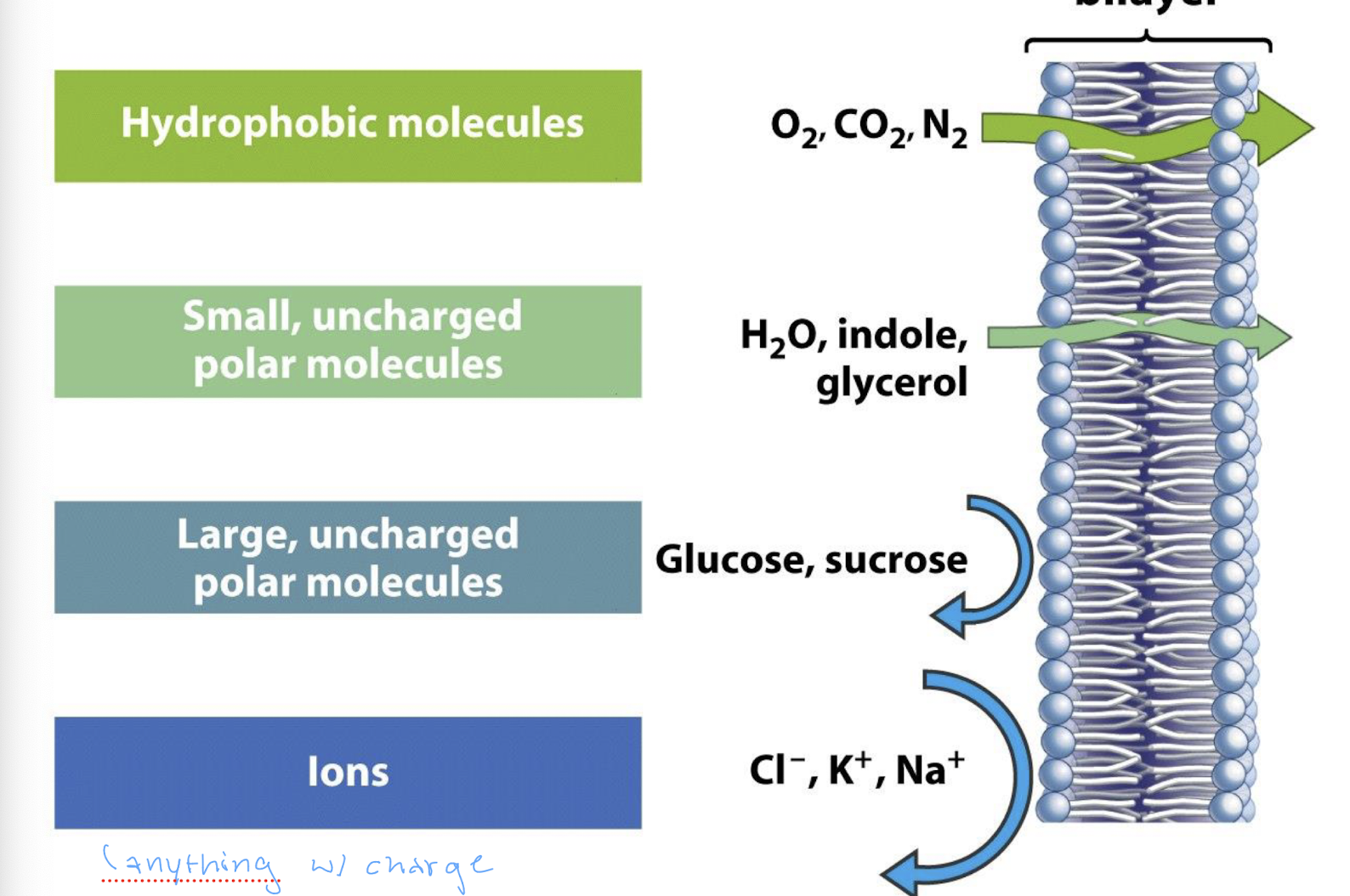
describe how size and charge affect the rate of diffusion across a membrane
hydrophobic molecules (O2, CO2, N2) easily pass through
small, uncharged polar molecules (H2O, indole, glycerol) somewhat easily pass through
large, uncharged polar molecules (glucose, sucrose) rarely pass through and mostly reflect
ions (anything with a charge) almost never pass through
describe how the body is in osmotic equilibrium and chemical disequilinrium (homeostasis)
the ECF and ICF are in osmotic equilibrium but have very different chemical compositions
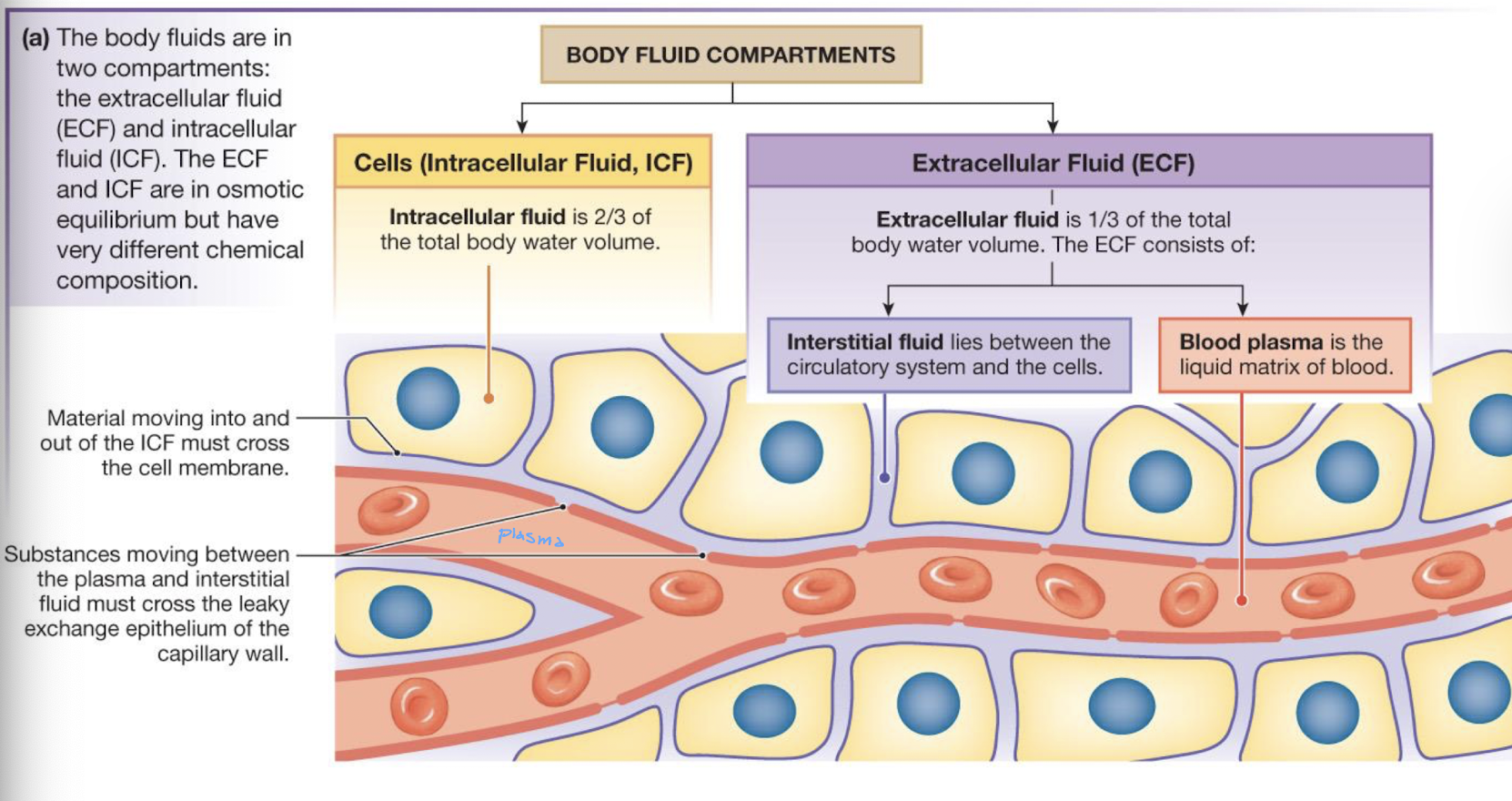
describe osmosis
the passive movement of H2O across a semi-permeable membrane from an area of low SOLUTE concentration to high SOLUTE concentration
direcetion of water is determined by the concentration of impermable solutes on either side of the membrane
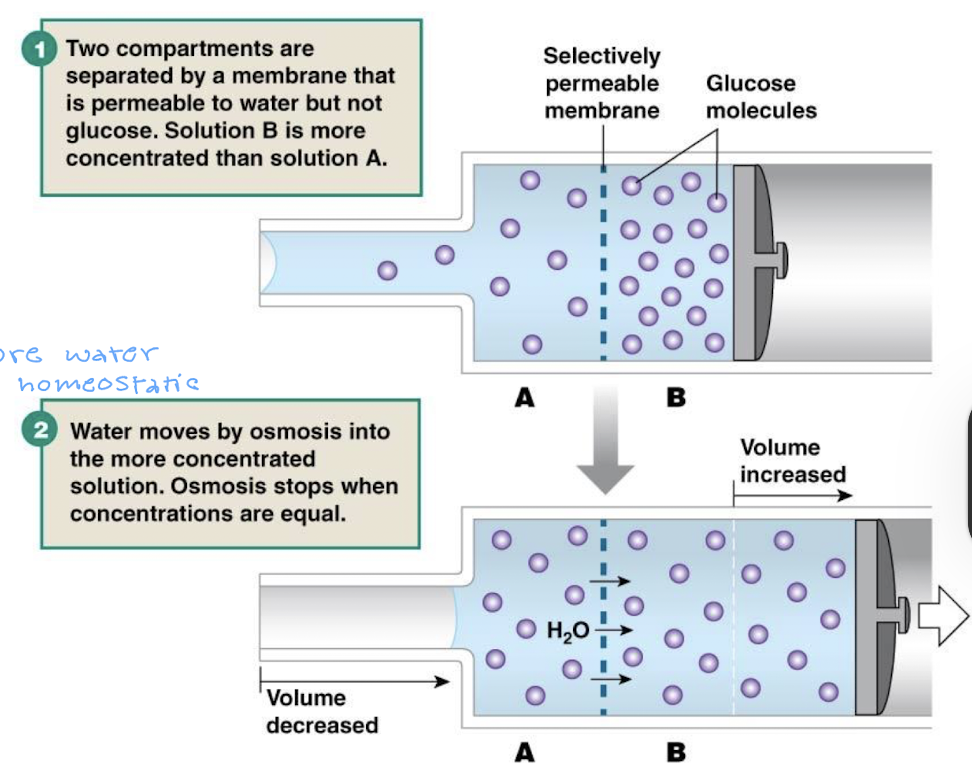
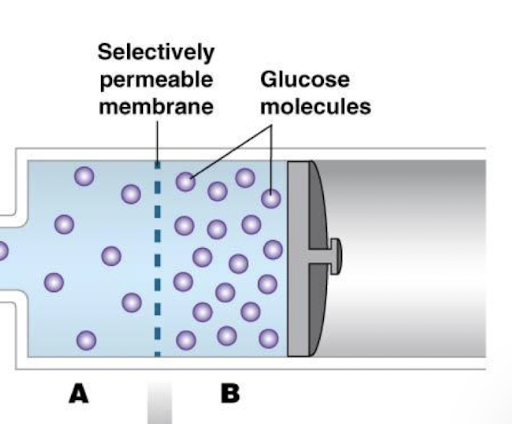
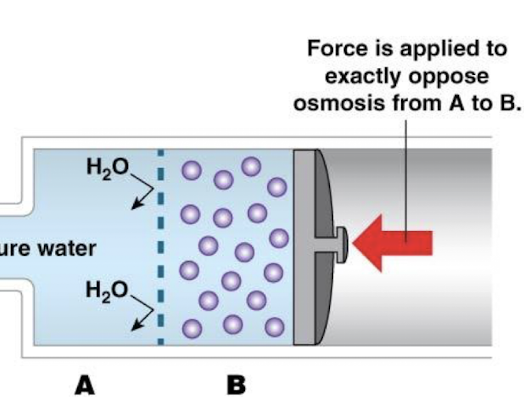
describe what will happen to the image with respect to osmosis
the two comartments are separated by a membrane that is permeable to water but not glucose and solution B is more concentrated than solution A
water moves by osmosis into the more concentrated solution and stops when concentrations are equal
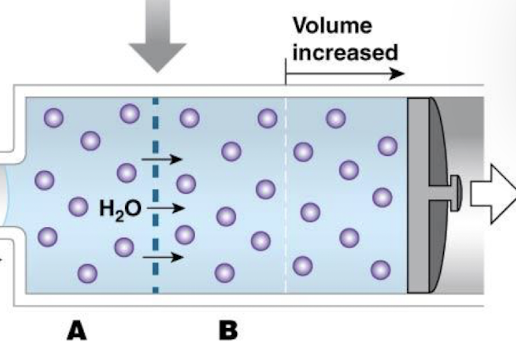
describe osmotic pressure
the amount of physical pressure that must be applied to oppose osmosis
describe the molariity
the number of molecules of EACH solute in solution per unit volume (M)
describe the osmolarity
total concentration of ALL solute PARTICLES in solution per unit volume (OsM)
given the M, calculate the OsM of 1M glucose, 1M glucose and 2M sucrose, and 1M NaCl
1M glucose: 1 OsM
1M glucose and 2M sucrose: 3 OsM
1M NaCl: 2 OsM
what are the three types of tonicity
hypotonic
isotonic
hypertonic
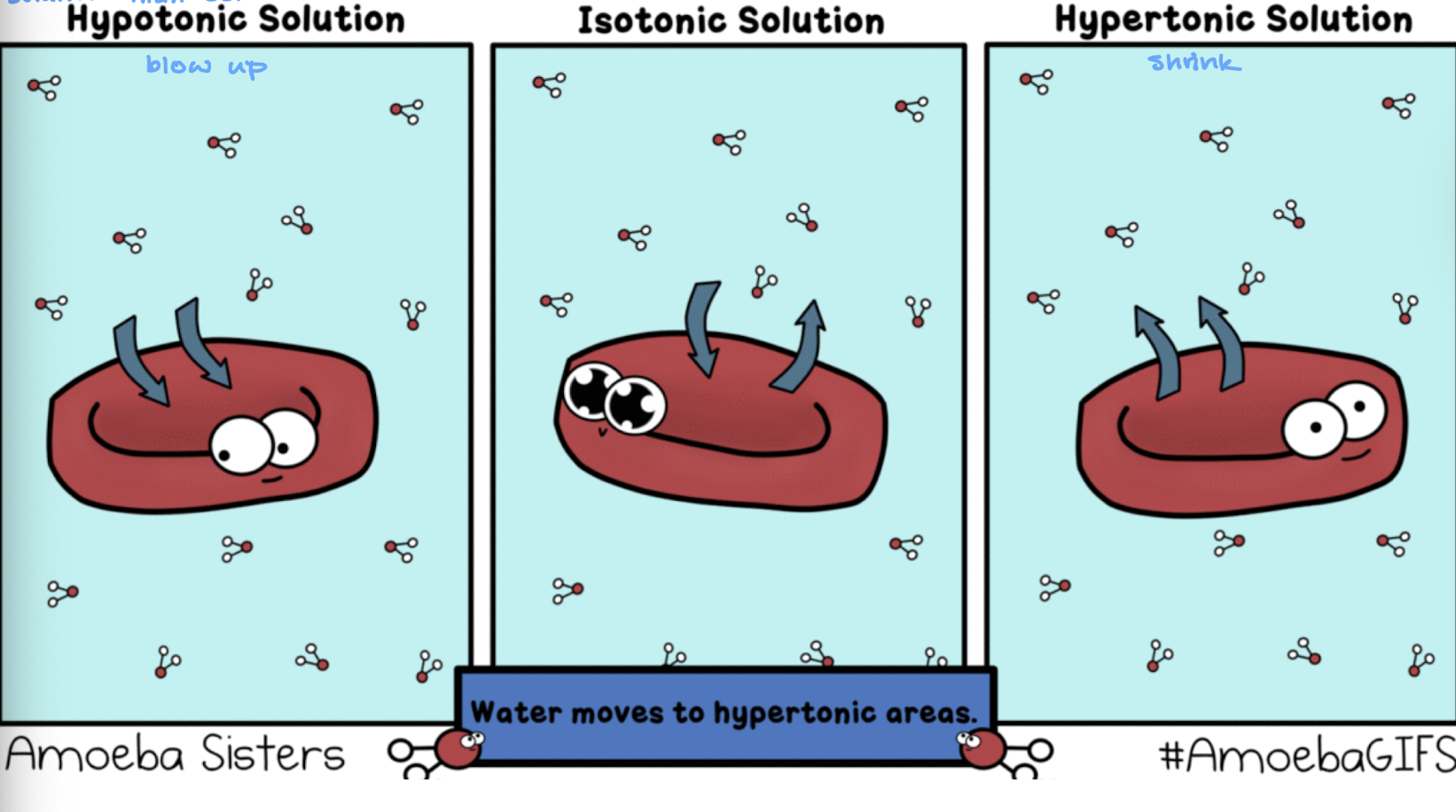
describe a hypotonic solution
less solute in solution than in the cell so the cell blows up

describe an isotonic solution
the amount of solute in the solution and in the cell is the same so the cell is turgid

describe a hypertonic solution
more solute in the solution than in the cells so the cell shrinks

what are the rules for osmolarity and tonicity
assume that all intracellular solutes are nonpenetrating (won’t freely pass membranes)
compare osmolarities before the cell is exposed to the solution (at, equilibrium, the cell and solution are always isosmotic)
tonicity of a solution describes the volume change of a cell at equilibrium
determine tonicity by comparing nonpenetrating solute concentrations in the cell and the solution. net water movement is into the compartment with the higher concentration of nonpenetrating solutes
hyposmotic solutions are always hypotonic
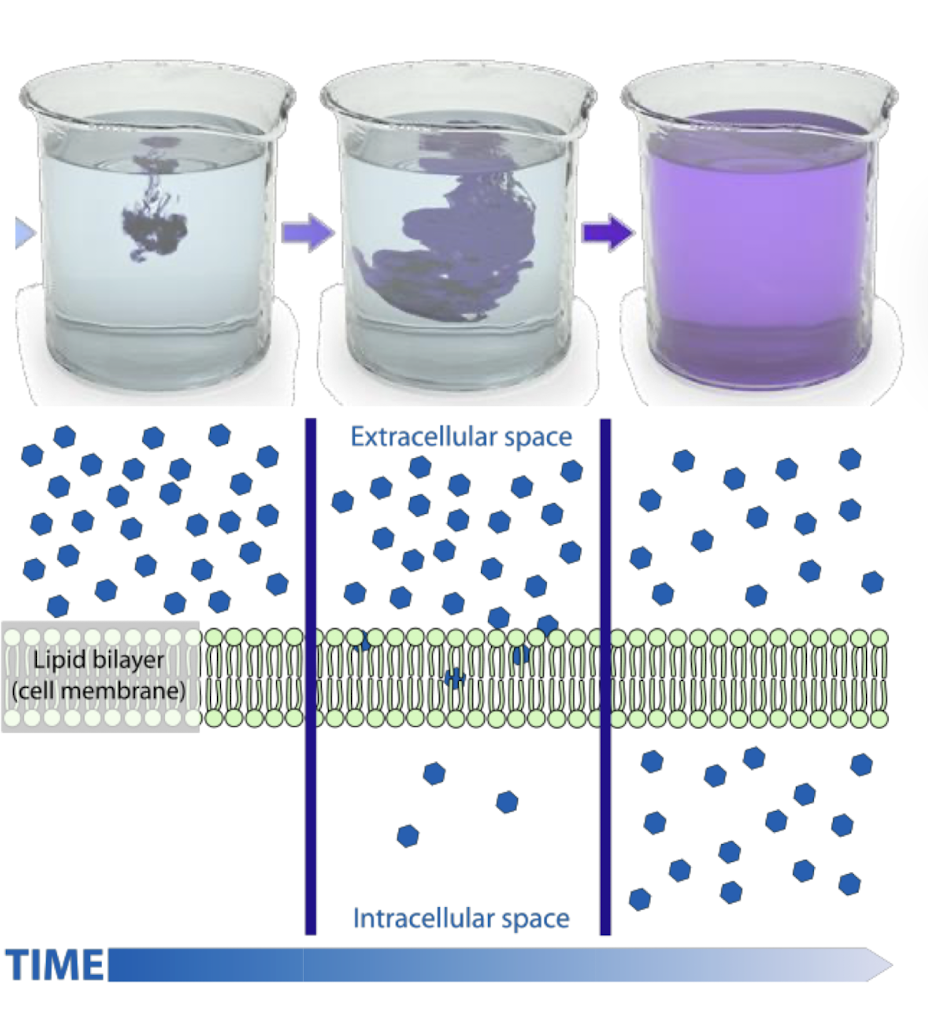
describe diffusion
the passive movement of solutes from an area of higher concentration to an area of lower concentration
does not require any external concentration
happens with or without a barrier
molecular movement continues after reaching equilibrium, just not NET movement
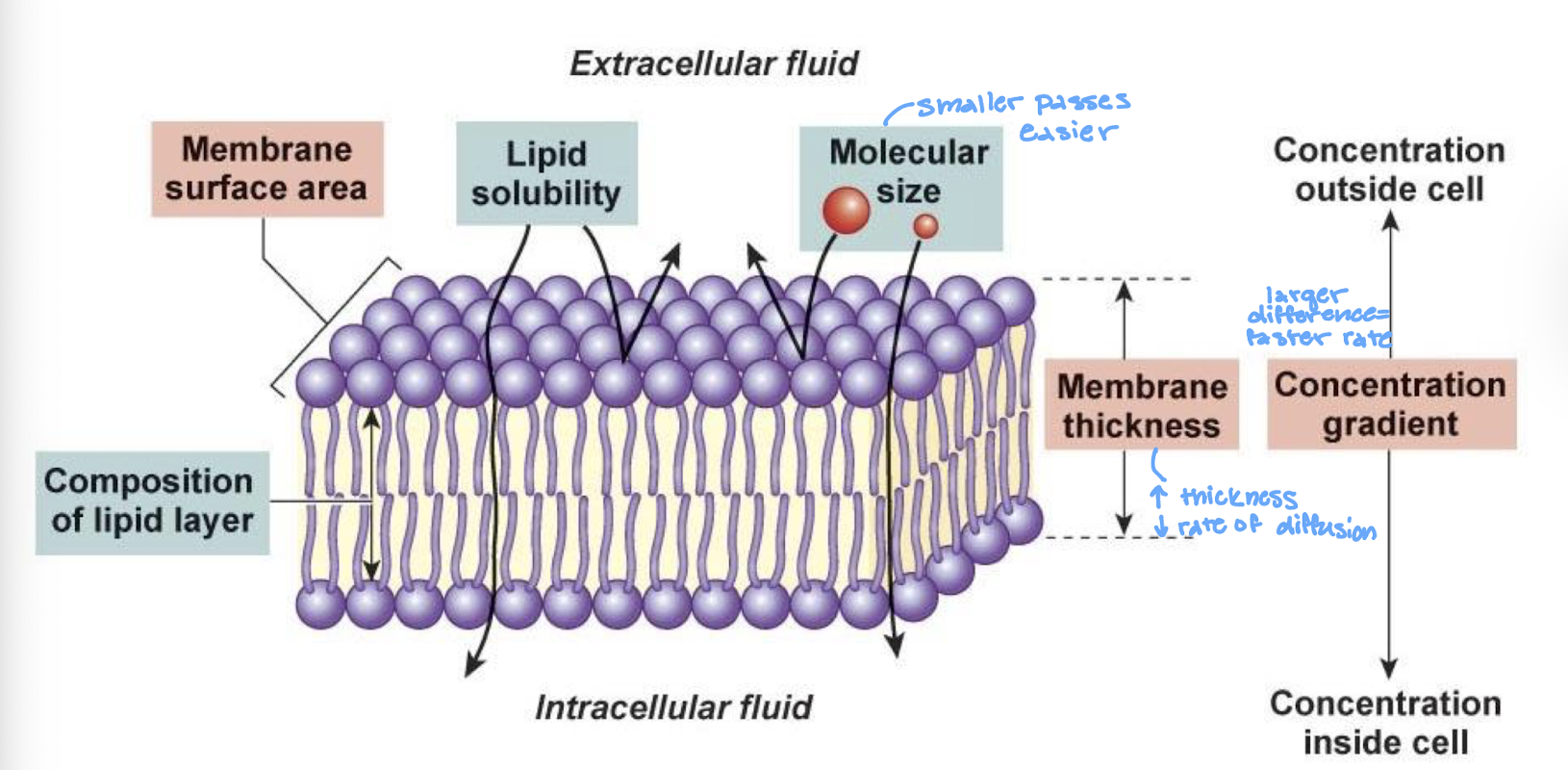
describe Fick’s Law of Diffusion
the rate of diffusion is porptional to (surface area)*(concentration gradient)*(membrane permeability)
rate of diffusion changes based on the composition of lipid layer, membrane surface area, lipid solubility, molecular size, membrane thickness, and the concentration gradient
what are the general properties of diffusion
diffusion uses the kinetic energy of molecular movement and does not require an outside energy source
molecules diffuse from an area of higher concentration to an area of lower concentration
diffusion continues until concentrations come to equilibrium (however molecular movment continues after equilibrium has been reached)
diffusion is faster
along higher concentration gradients
over shorter distnces
at higher temperatures
for small molecules
diffusion can take place in an open system or across a partition that separates two systems
the rate of diffusion through a membrane is faster if
the membrane’s surface area is larger
the membrane is thinner
the concentration gradient is larger
the membrane is more permeable to the molecule
membrane permeability to a molecule depends on
the molecule’s lipid solubillity
the molecule’s size
the lipid composition of the membrane
what are the types of epithelia
exchange epithelium
protective epithelium
secretory epithelium
transporting epithelium
ciliated epithelium
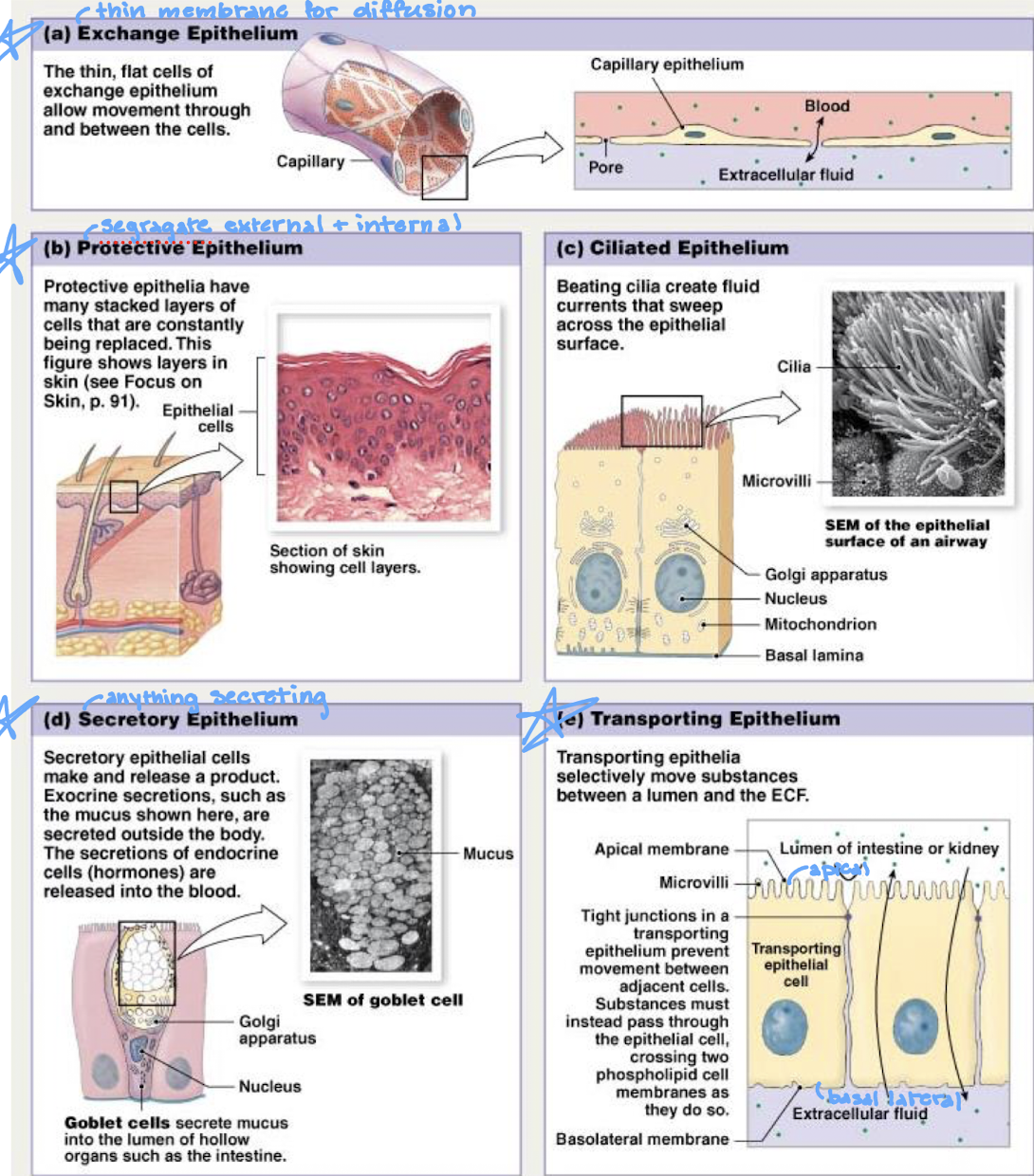
describe exchange epithelium
the thin, flat cells of exchange epithelium allow movement through and between cells
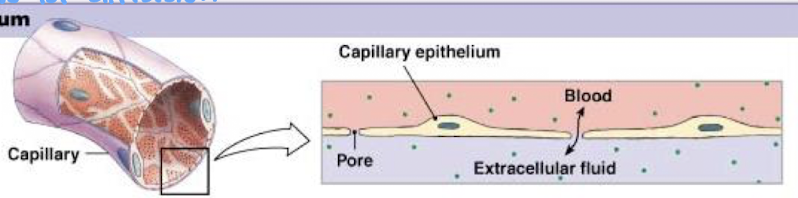
describe the protective epithelium
have many stacked layers of cells that are constantly being replaced
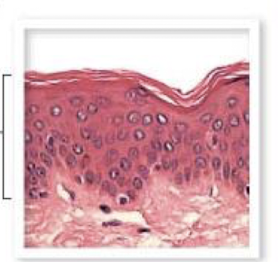
describe the secretory epithelium
make and release a product
describe the transporting epithelium
selectively move substances between a lumen and the ECF
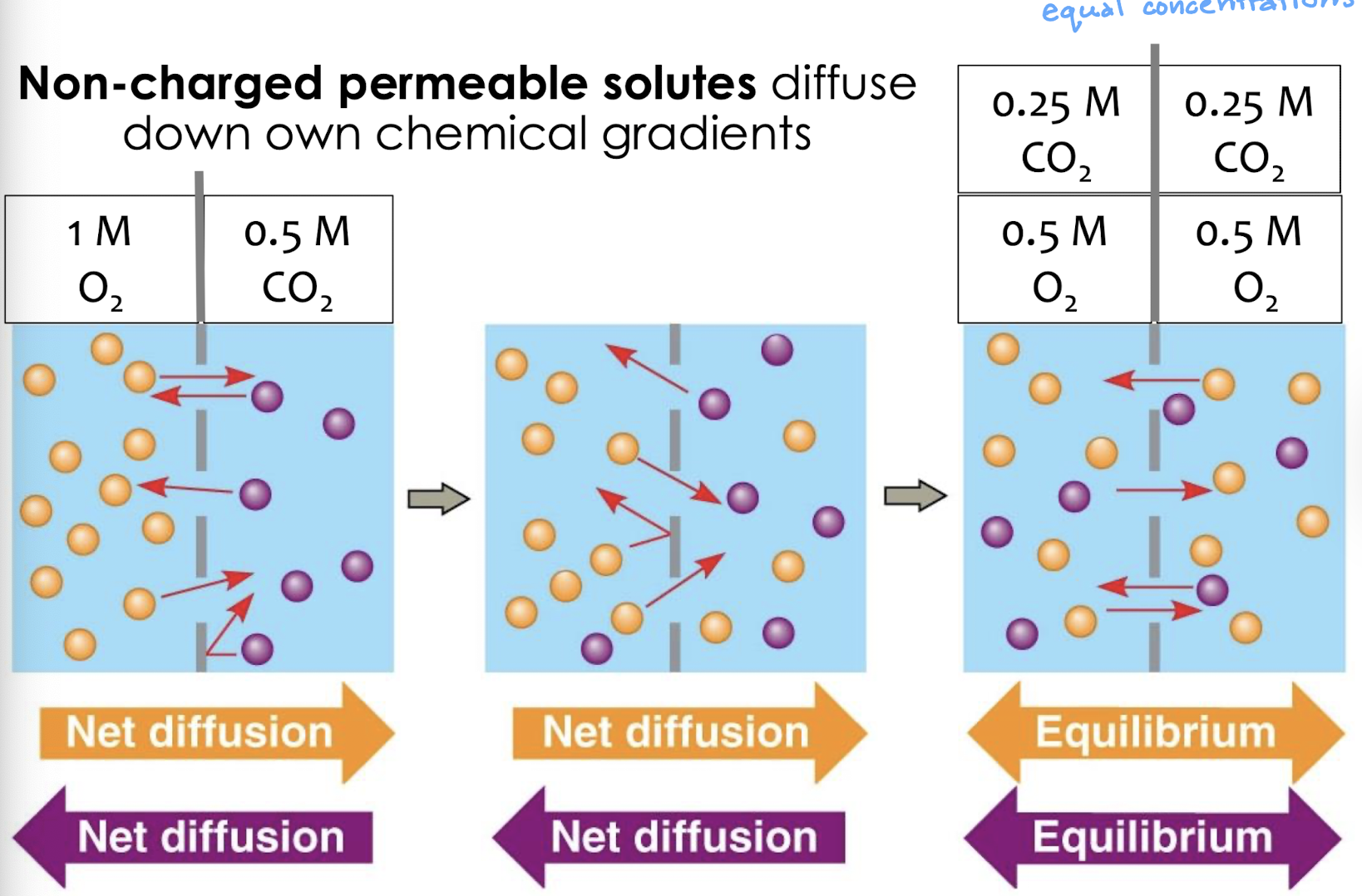
describe the chemical gradients
non-charged permeable solutes diffuse down own chemical gradients
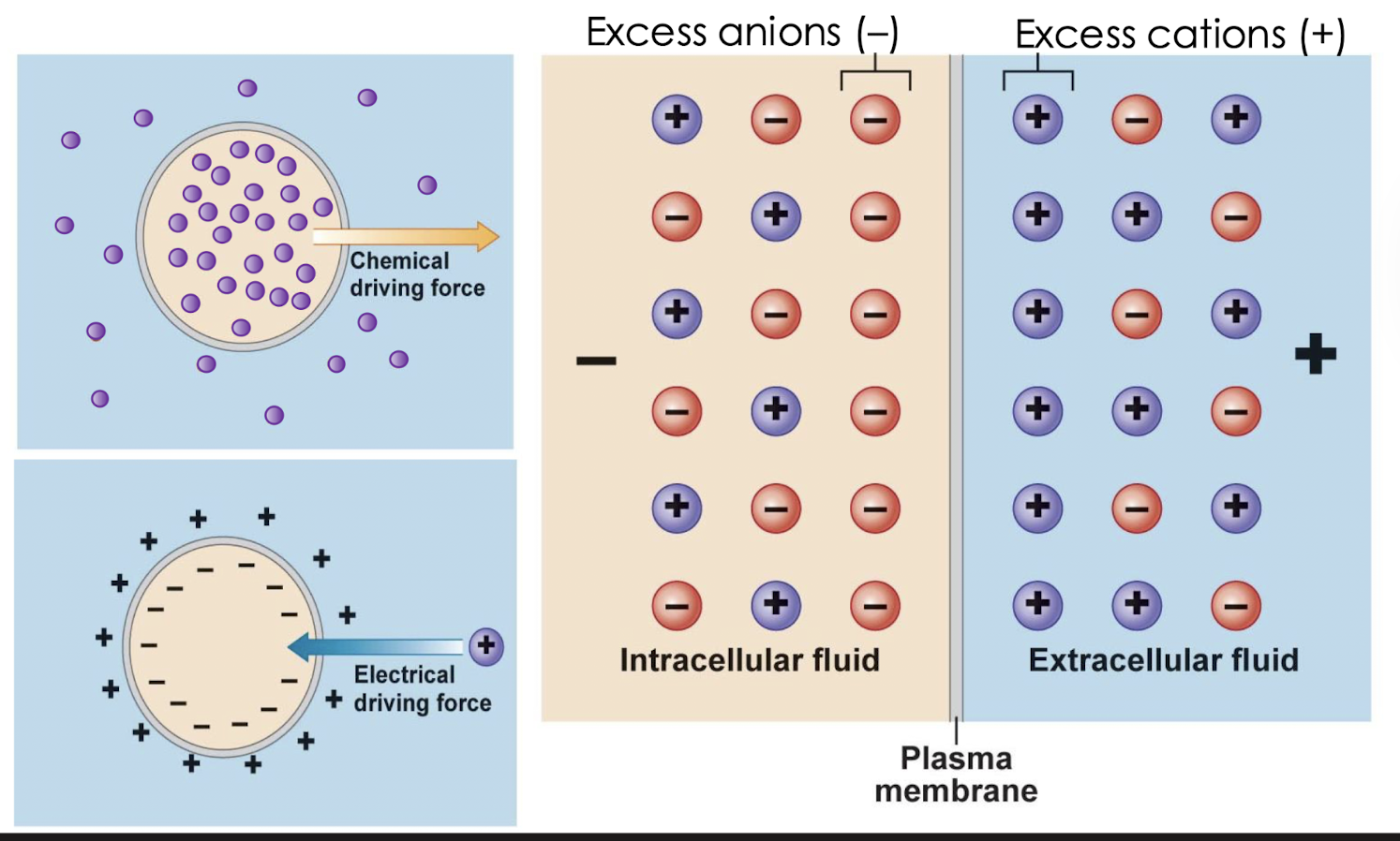
describe the electrochemical gradients
diffusion of charged solutes is affected by own chemical gradient AND overall electrical gradients
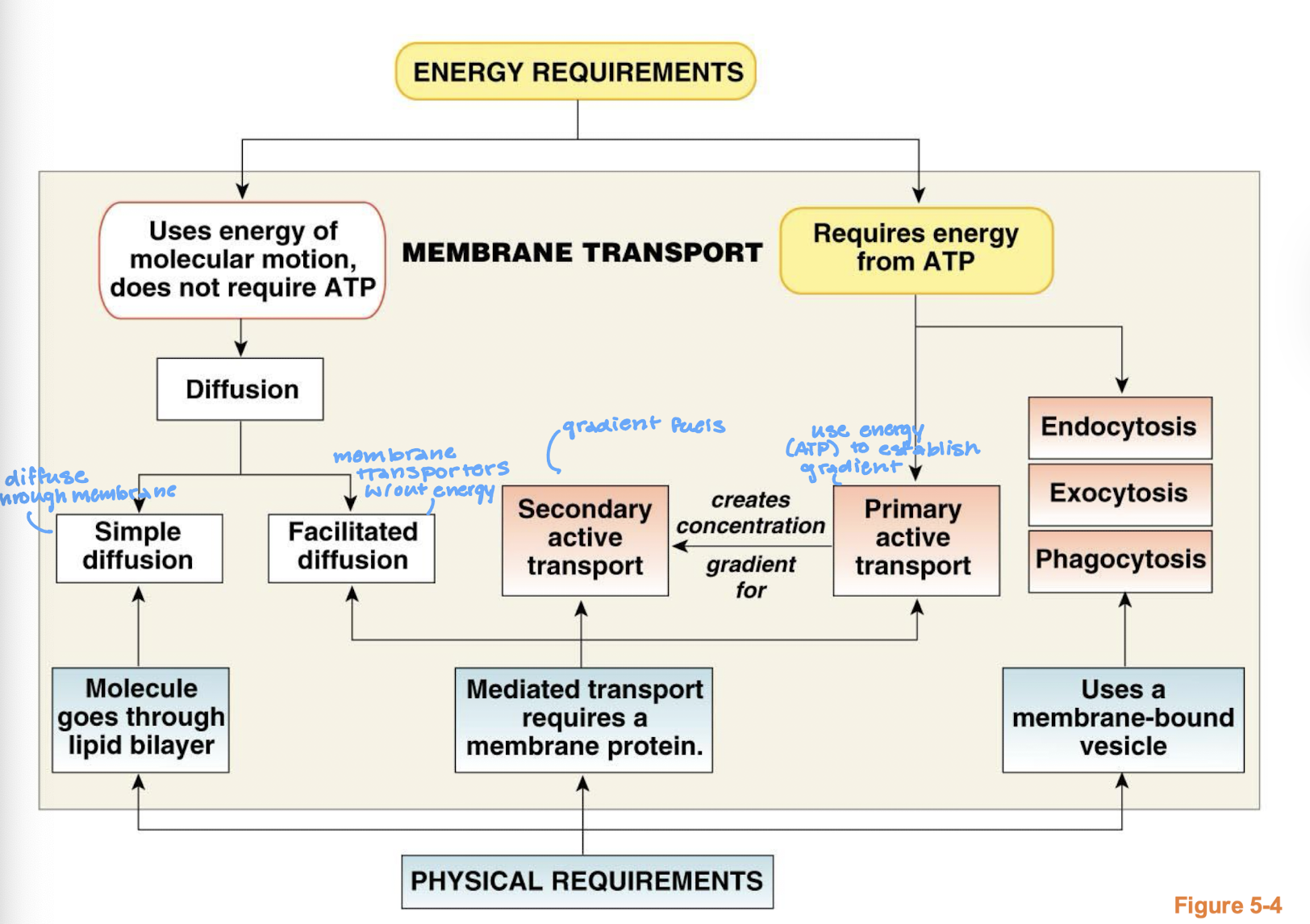
look at this diagram (membrane transport)
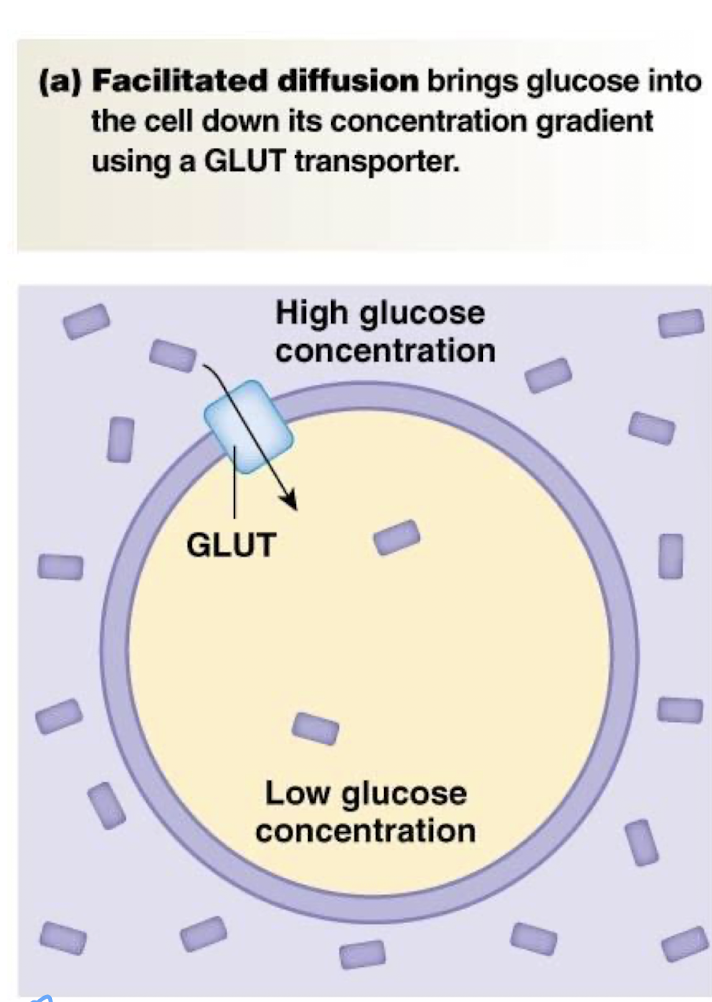
describe facilitated diffusion
passive movement of non-permeable solutes down their own electrochemical gradient using a transport protein imbedded in the cell membrane
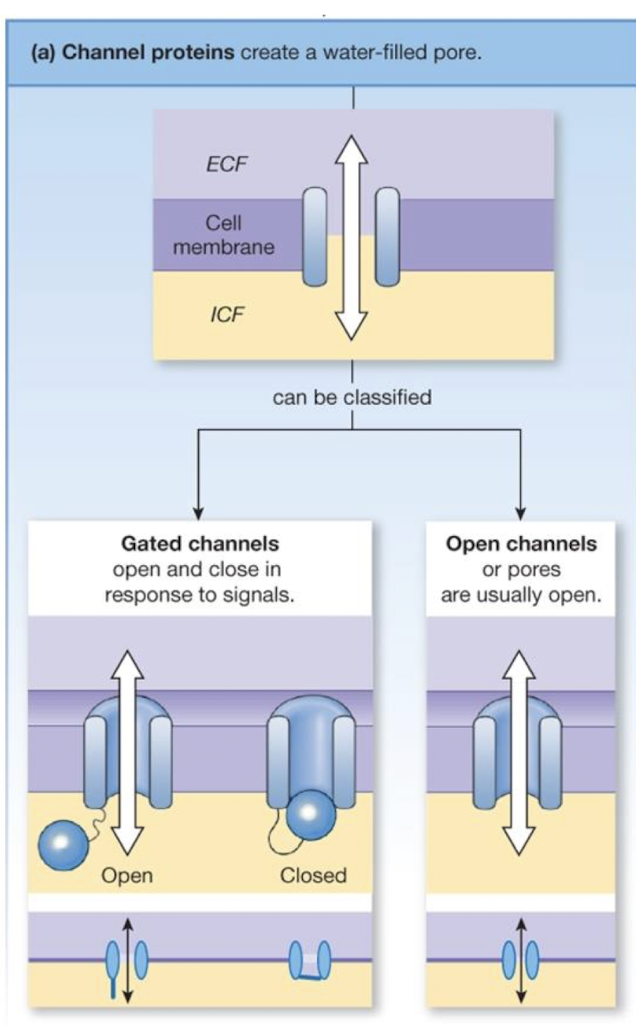
describe channel proteins
used only for facilitated diffusion
allows non-permeable molecules (e.g. ions or glucose) to passively cross the membranes
allows permeable molecules (like water) to diffuse across the membrane more quickly (e.g. aquaporins)
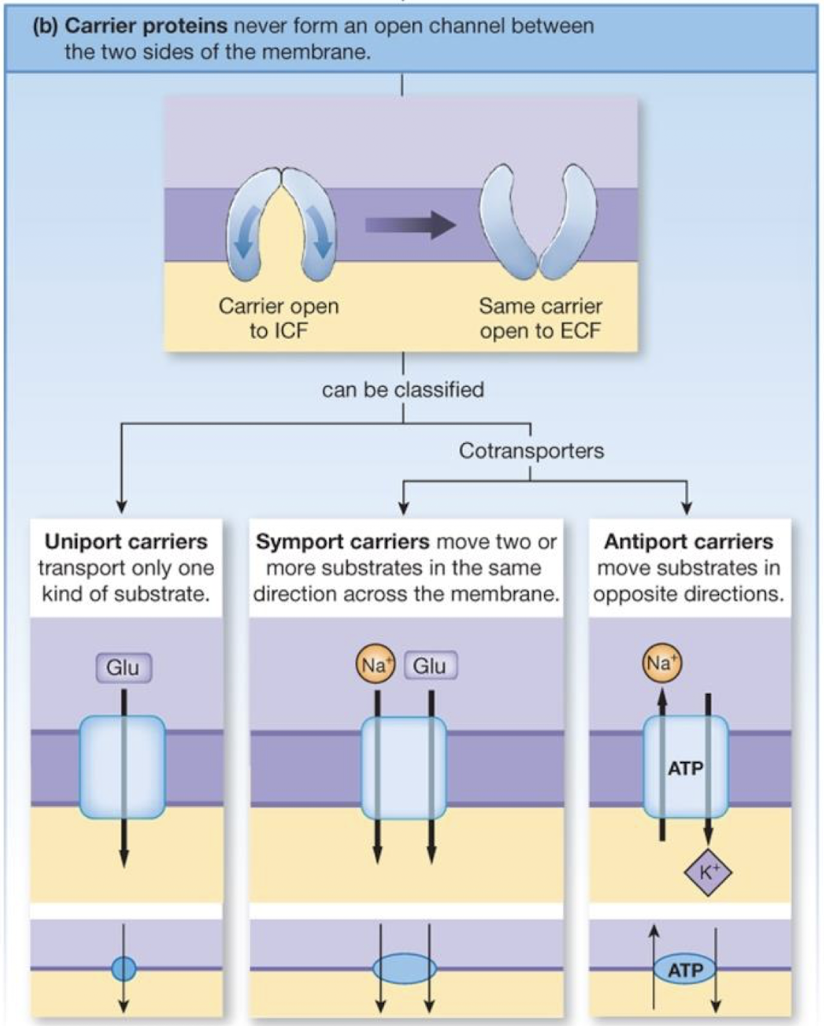
describe carrier proteins
used for facilitated diffusion and active transport
change conformation to allow non-permeable molecules through membrane in a single direction (only open to one side of the membrane at a time)
classified as one of three types (uniport, symport, antiport)
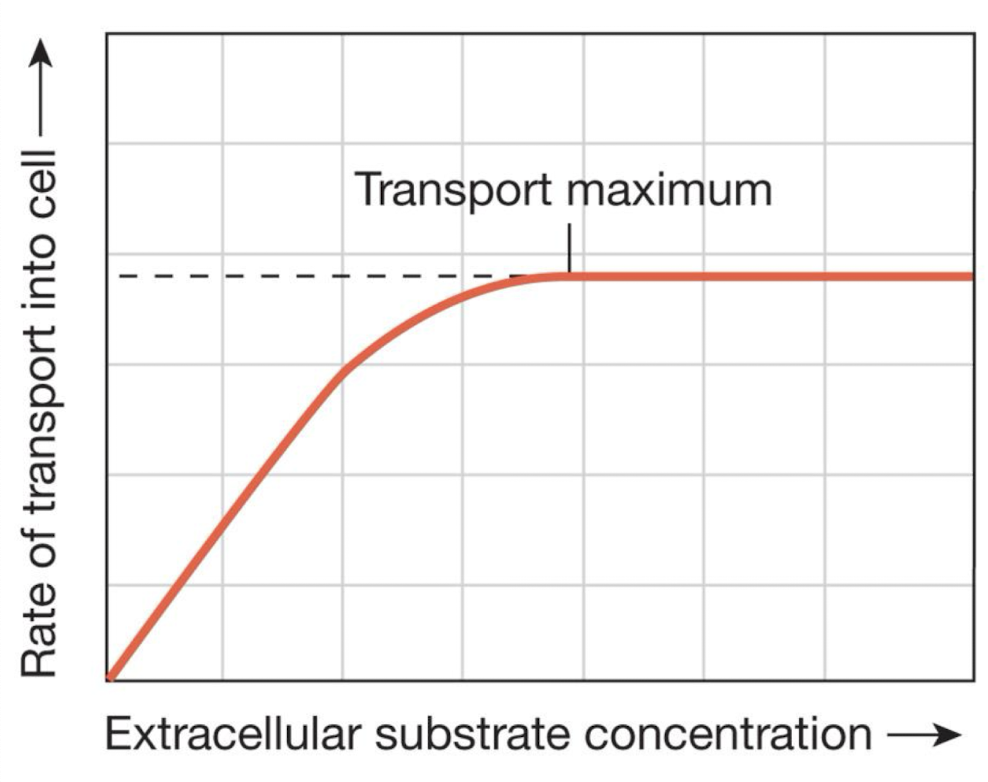
describe carrier saturation
the transport can reach a maximum rate when all the carrier binding sites are filled with substrate
extracellular substrate concentration→transport rate is proportional to substrate concentration until the carriers are saturated
what are the three ways to control channel and carrier proteins
chemically-gated
voltage-gated
mechanically-gated
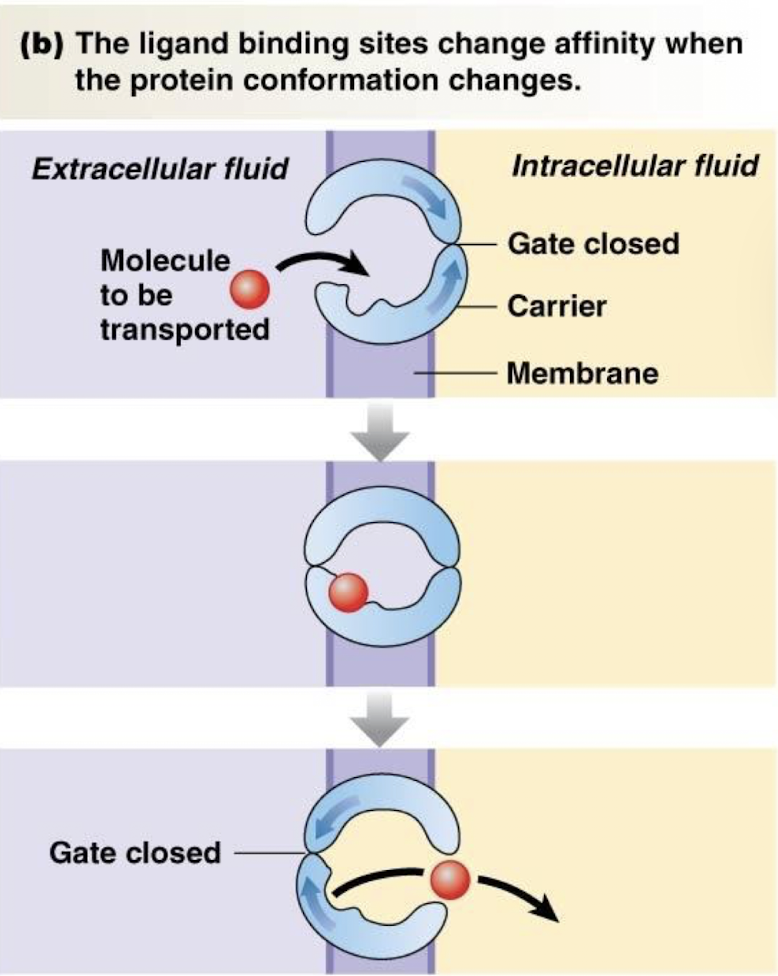
describe chemically-gated
a ligand binds to a receptor on the protein to change its confirmation
describe voltage-gated
a change in the electrical charge across the surrounding membrane changes the protein’s confirmation
describe mechanically-gated
a physical force changes the protein’s conformation
describe active transport
solutes are moved against their electrochemical gradient using energy either stored in the bonds of molecules (e.g. ATP) or released from stored concentration gradients of other molecules across the same membrane
primary = ATP
secondary = concentration gradient of a second substance that is maintained using ATP
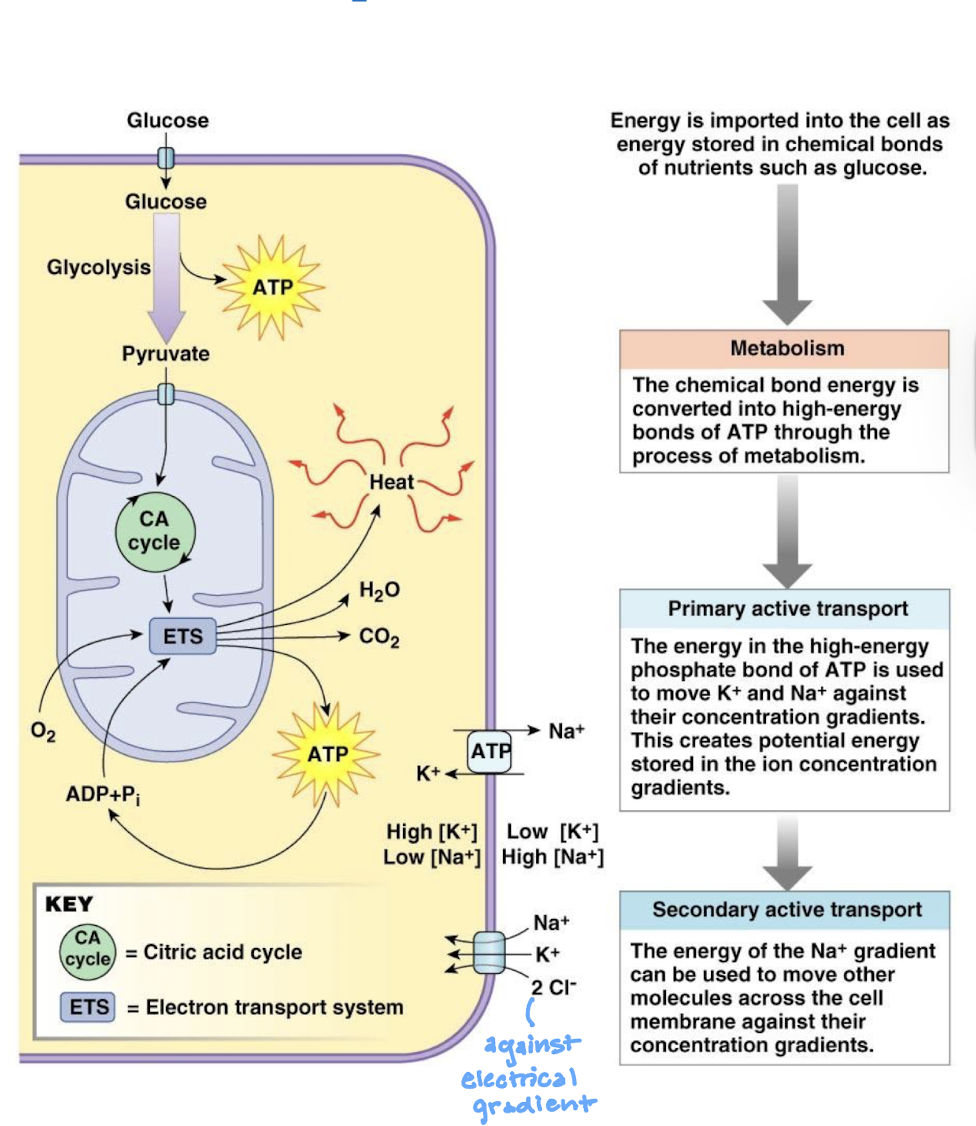
look at the primary active transport of Na+/K+ ATPase pumps
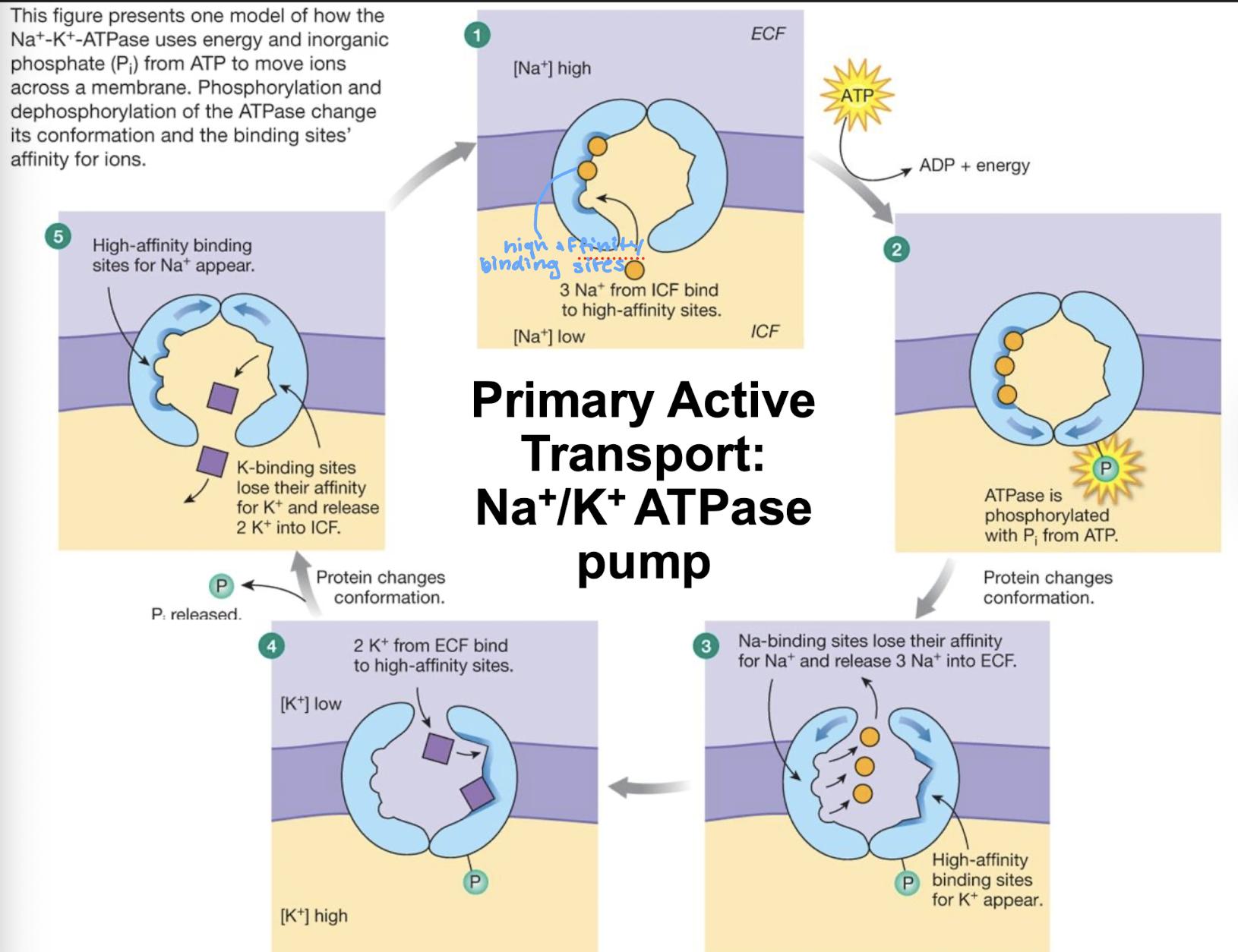
look at the diagram for the secondary active transport of sodium-glucose transporters (SGLT)
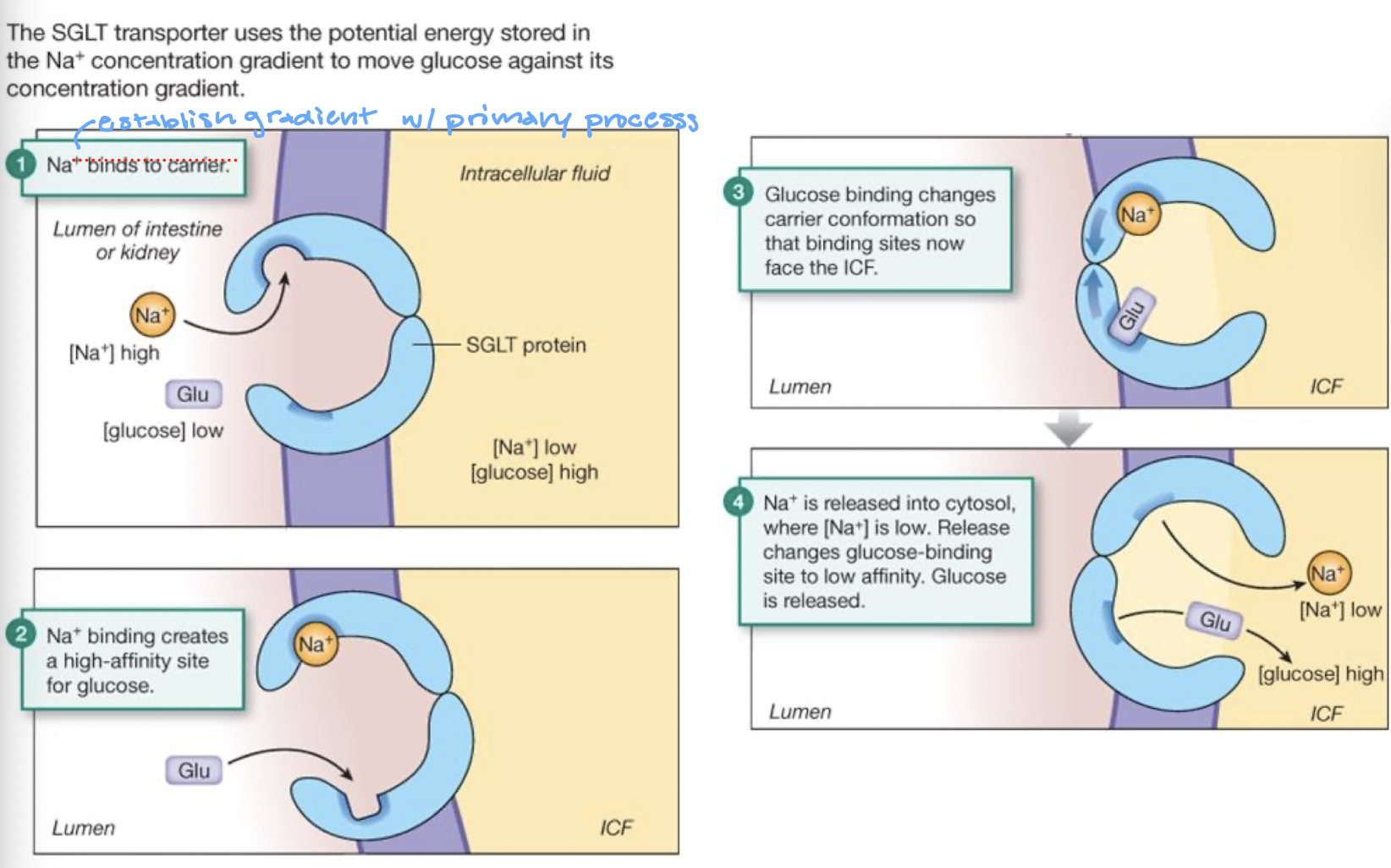
describe the steps in the directional movement of glucose across intestinal epithelium
Na+ glucose symporter brings glucose into cell against its gradient using energy stored in the Na+ concentration gradient
GLUT transporter transfers glucose to ECF by facilitated diffusion
Na+ K+ ATPase pumps Na+ out of the cell, keeping ICF Na+ concentration low
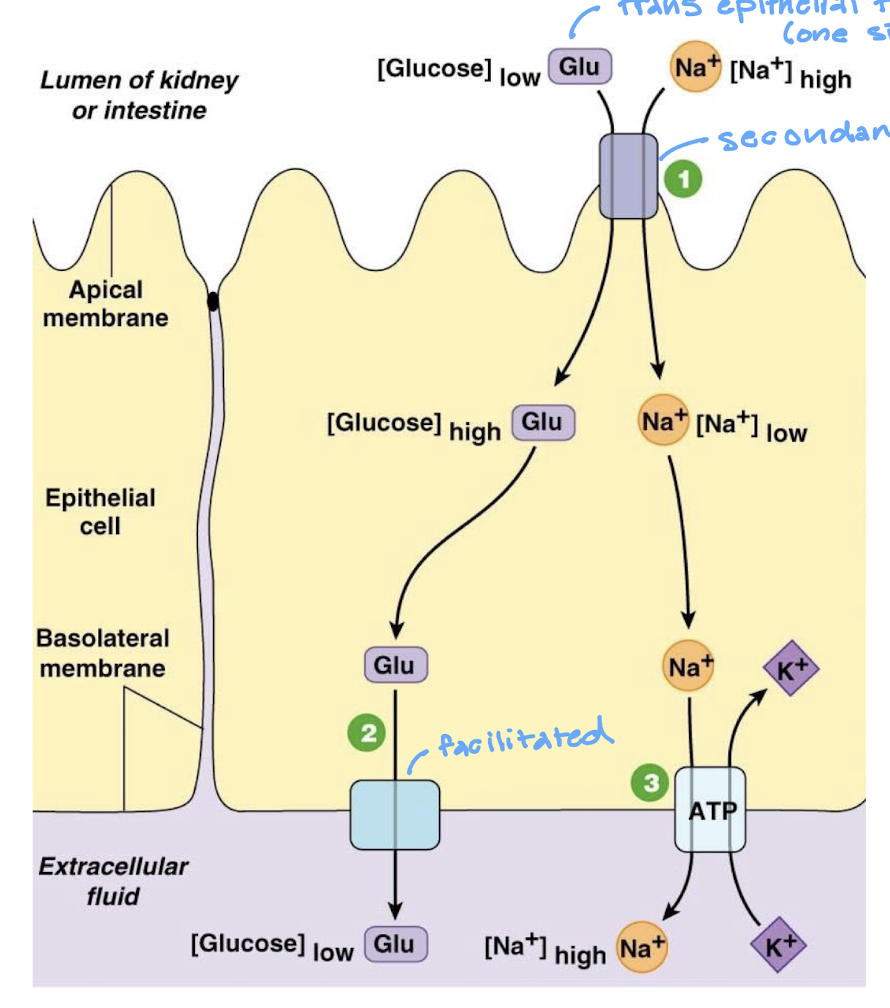
describe transepithelial transport
polarized epithelia have different transport proteins on apical and basolateral membranes
allows selective directional transport across the epithelium
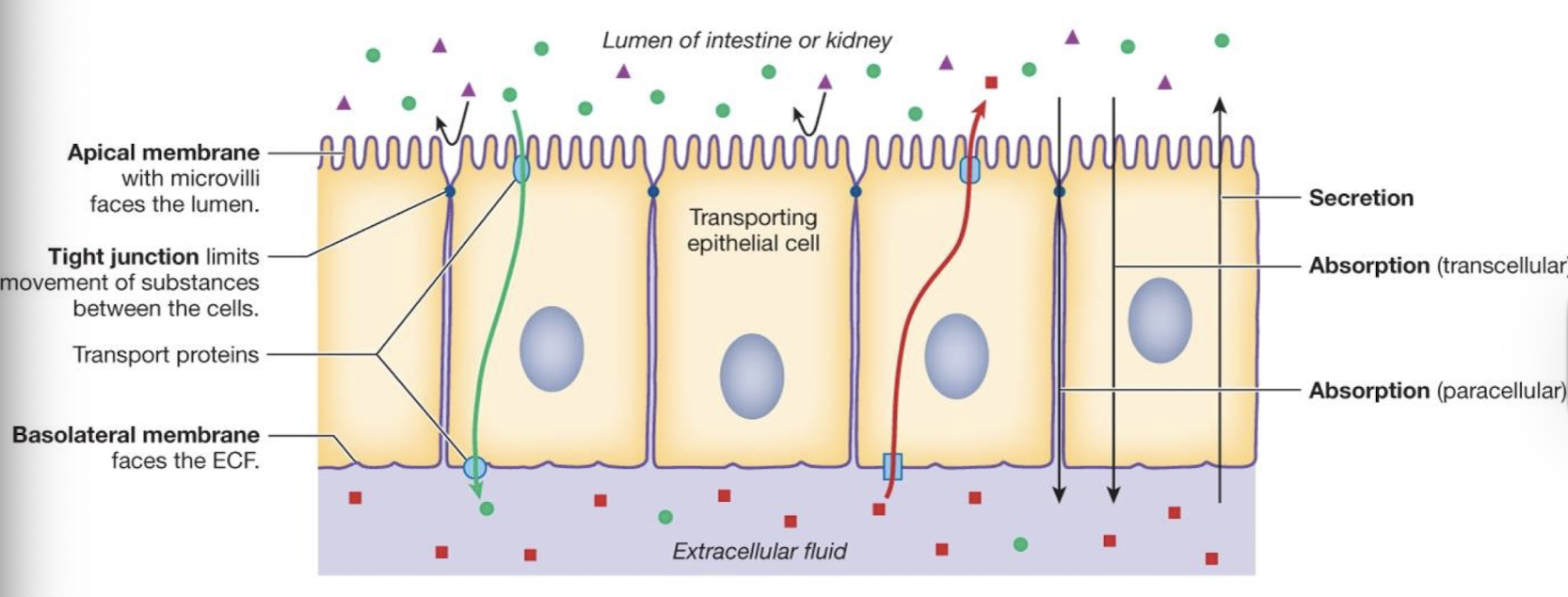
what is absorption with regard to transepithelial transport
transport from lumen to ECF
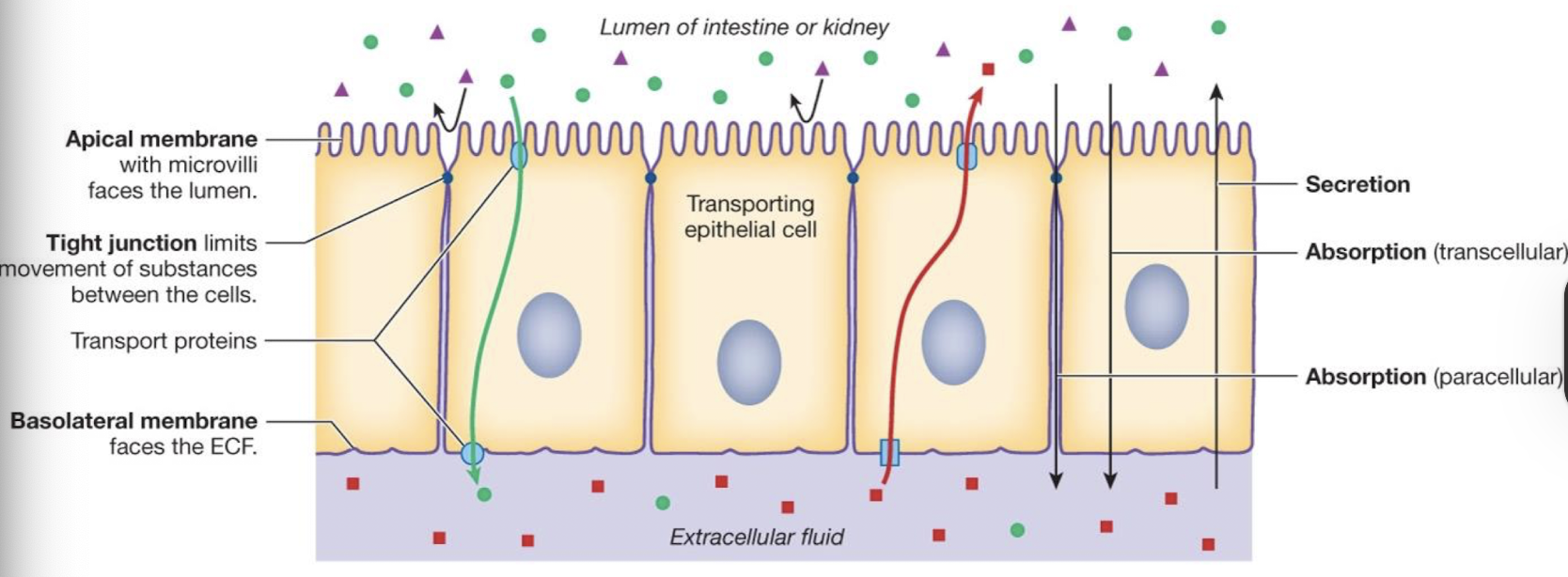
what is secretion with regard to transepithelial transport
transport from ECF to lumen
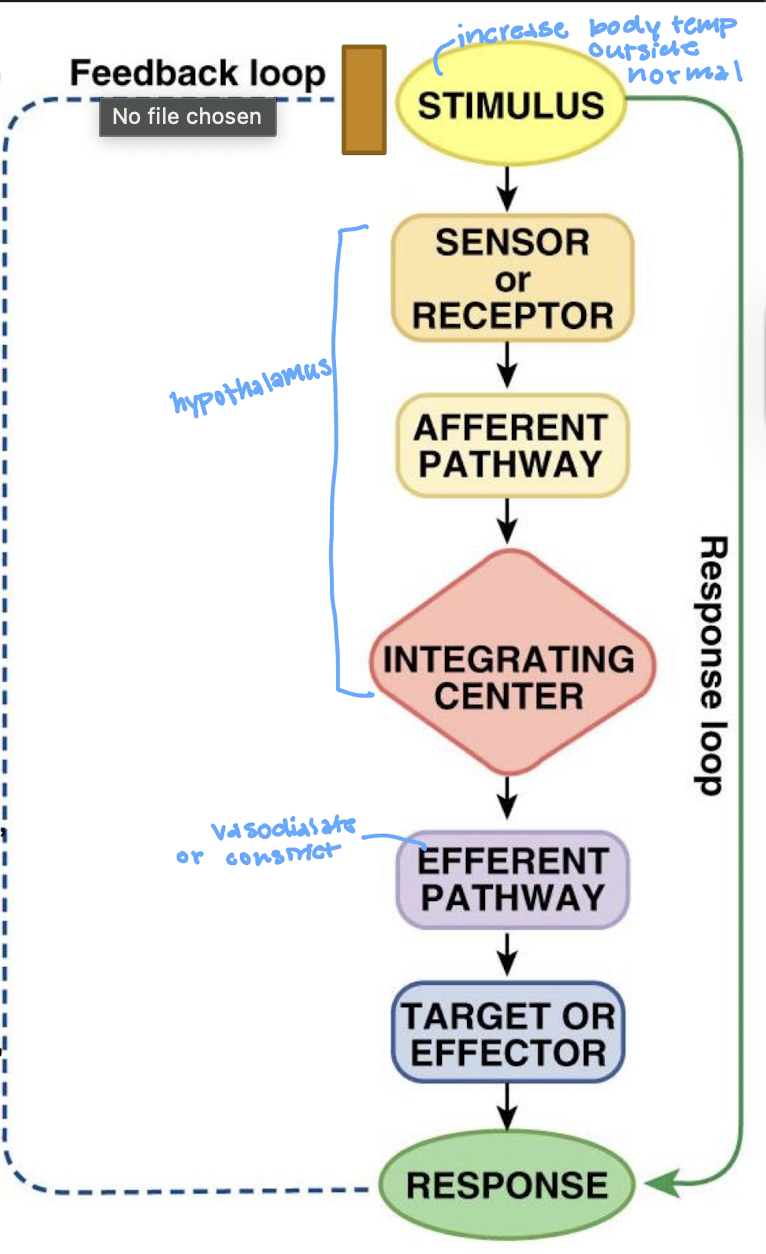
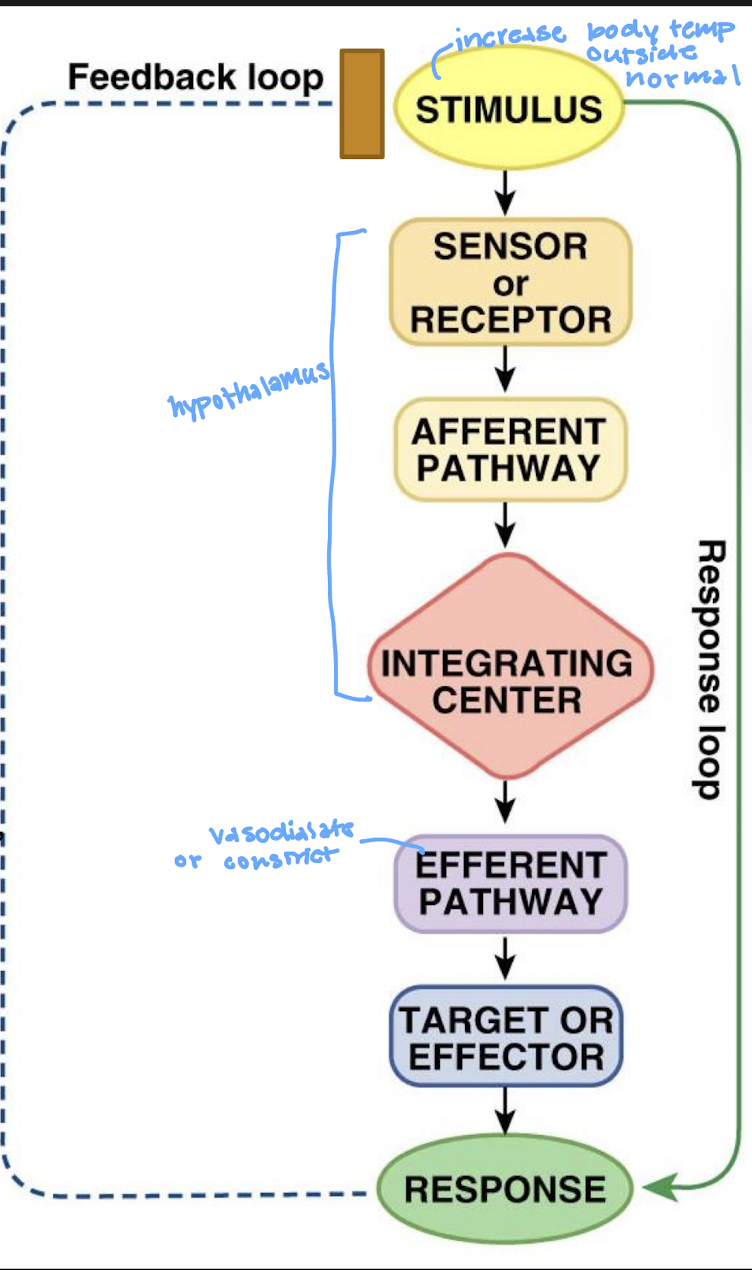
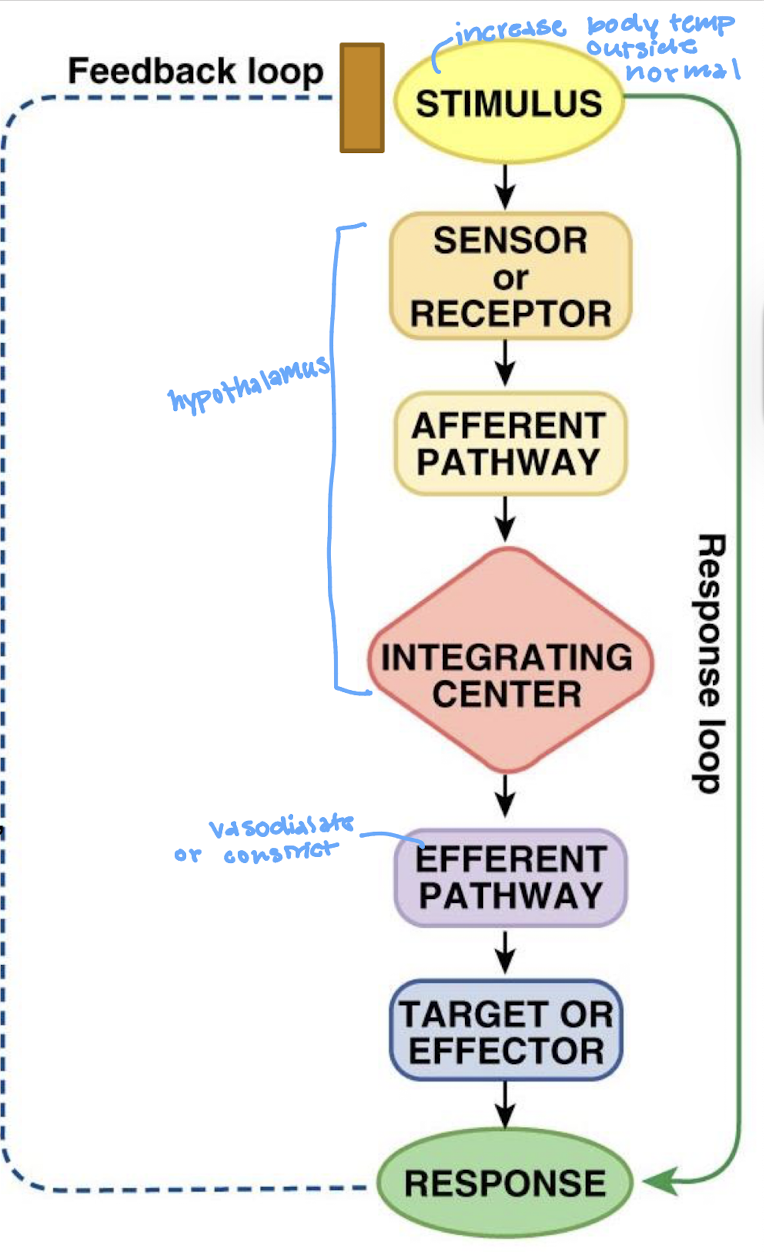
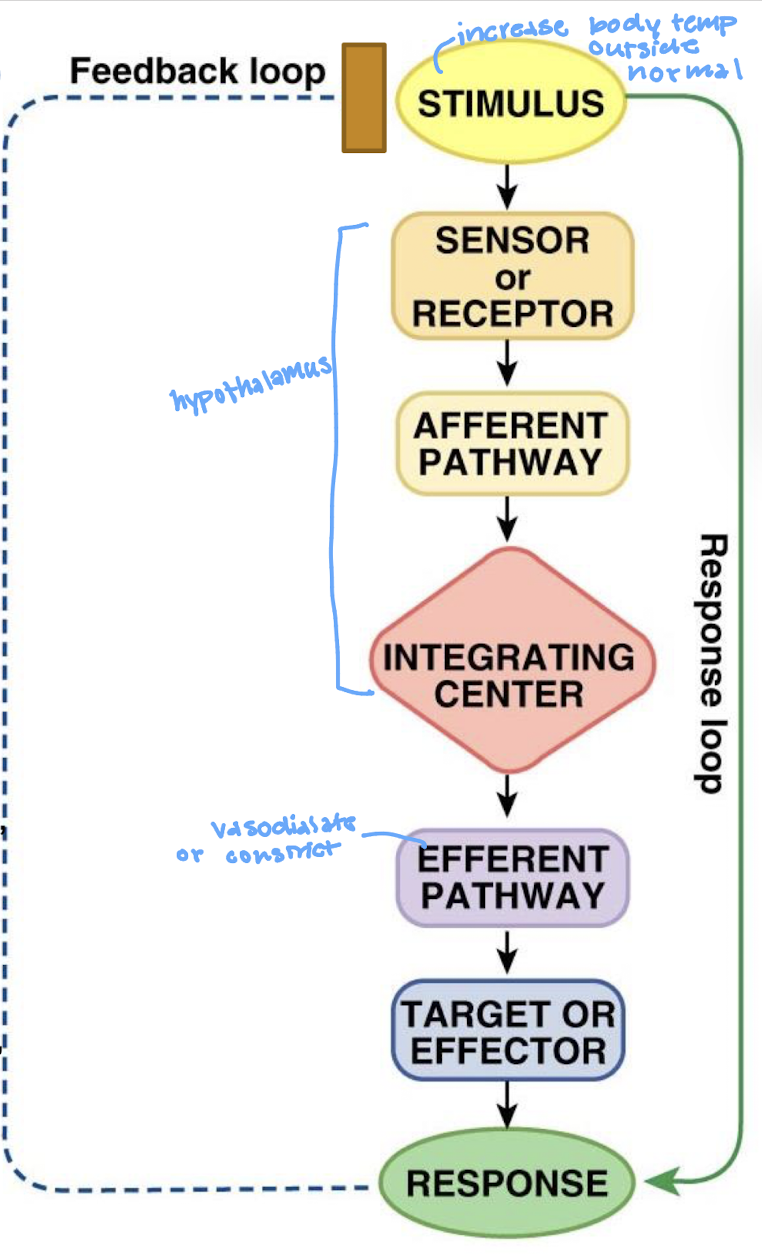
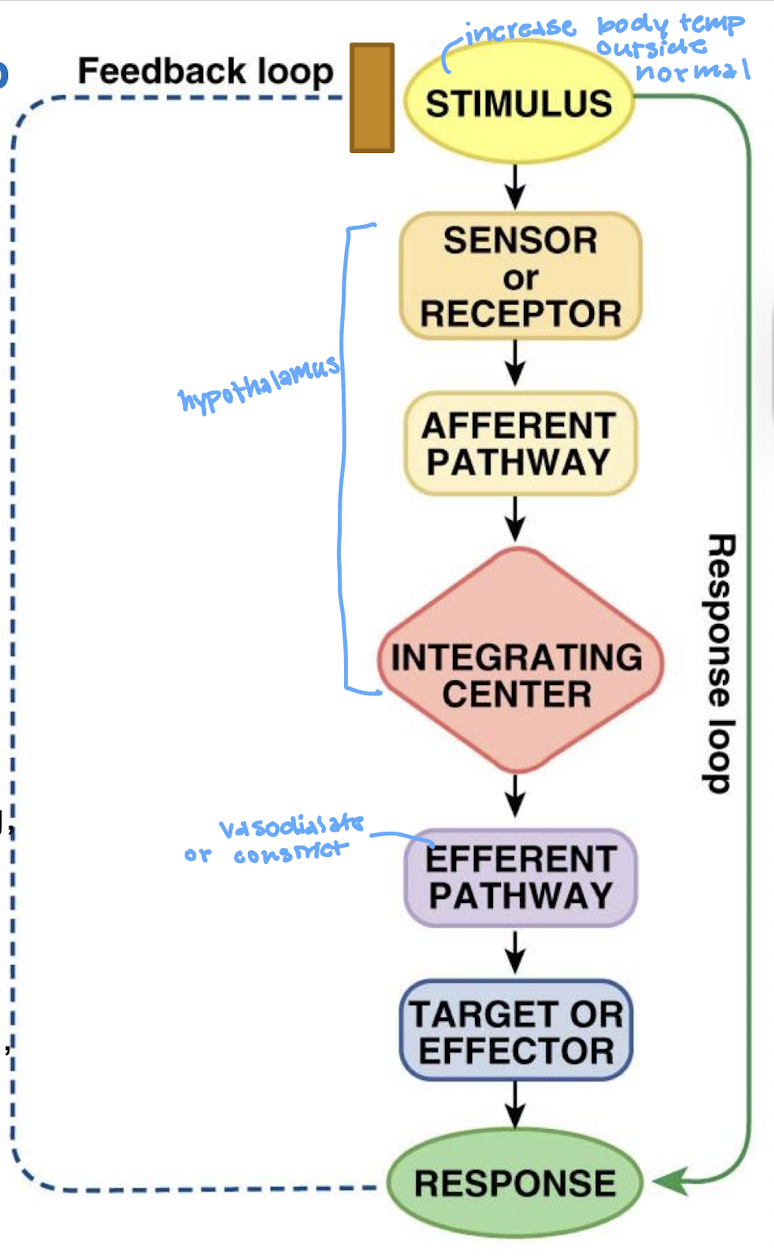
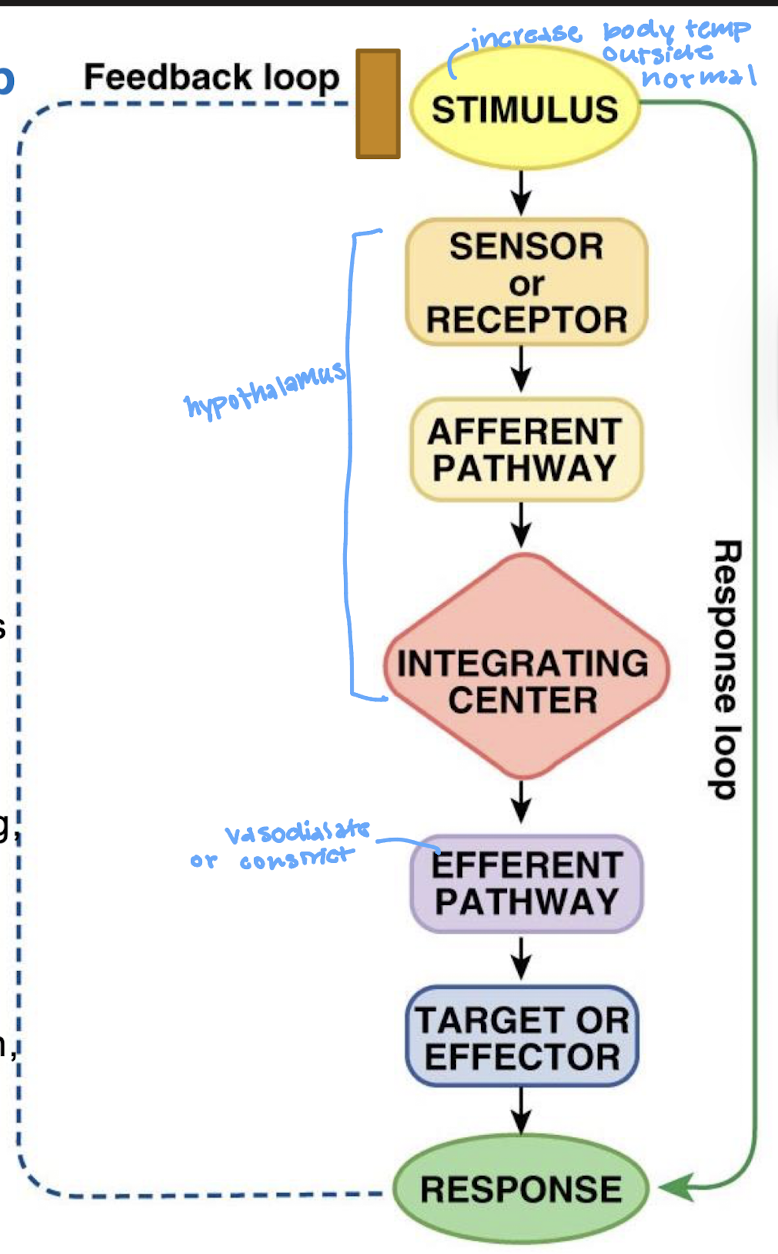
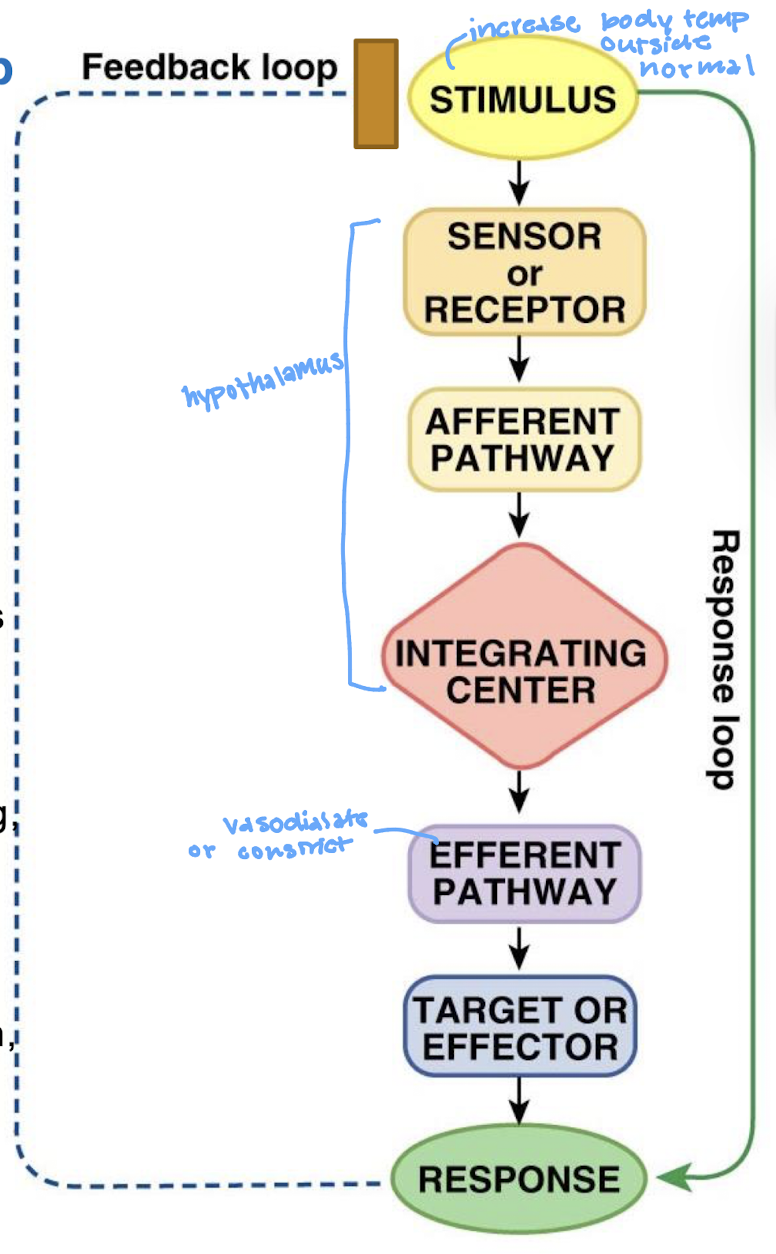
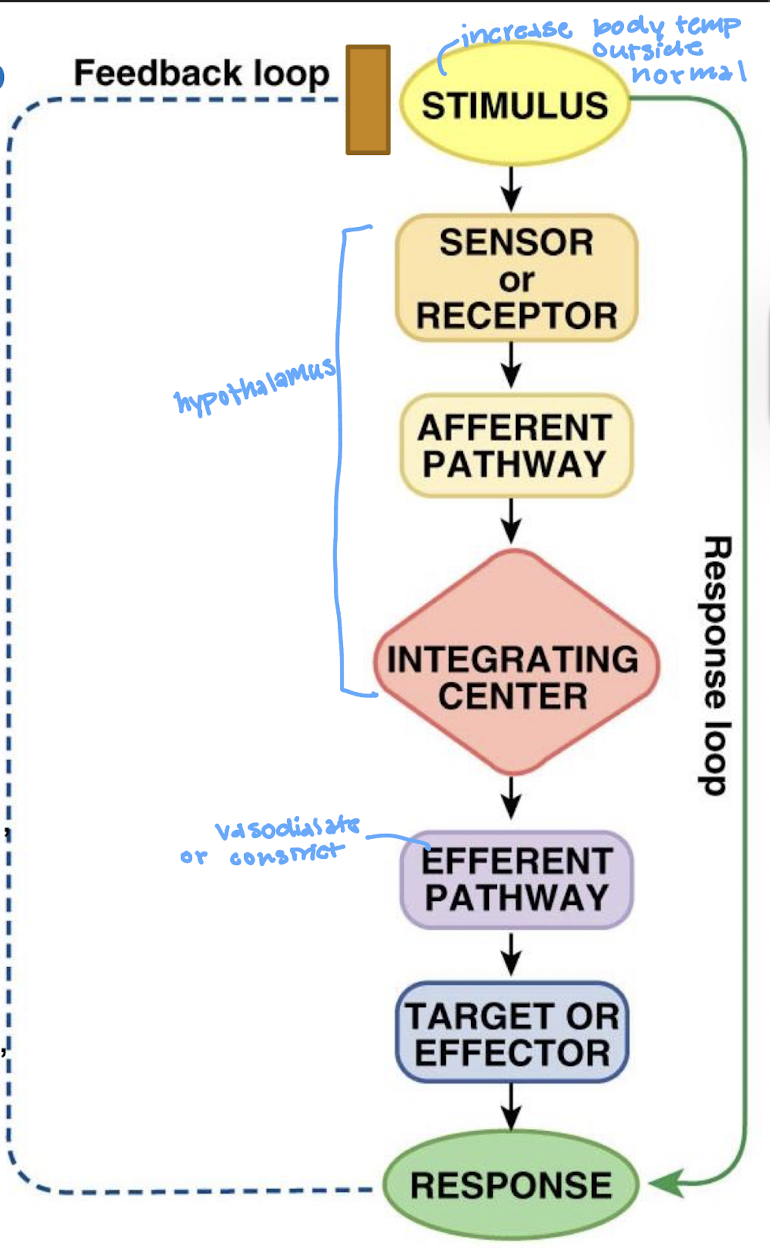
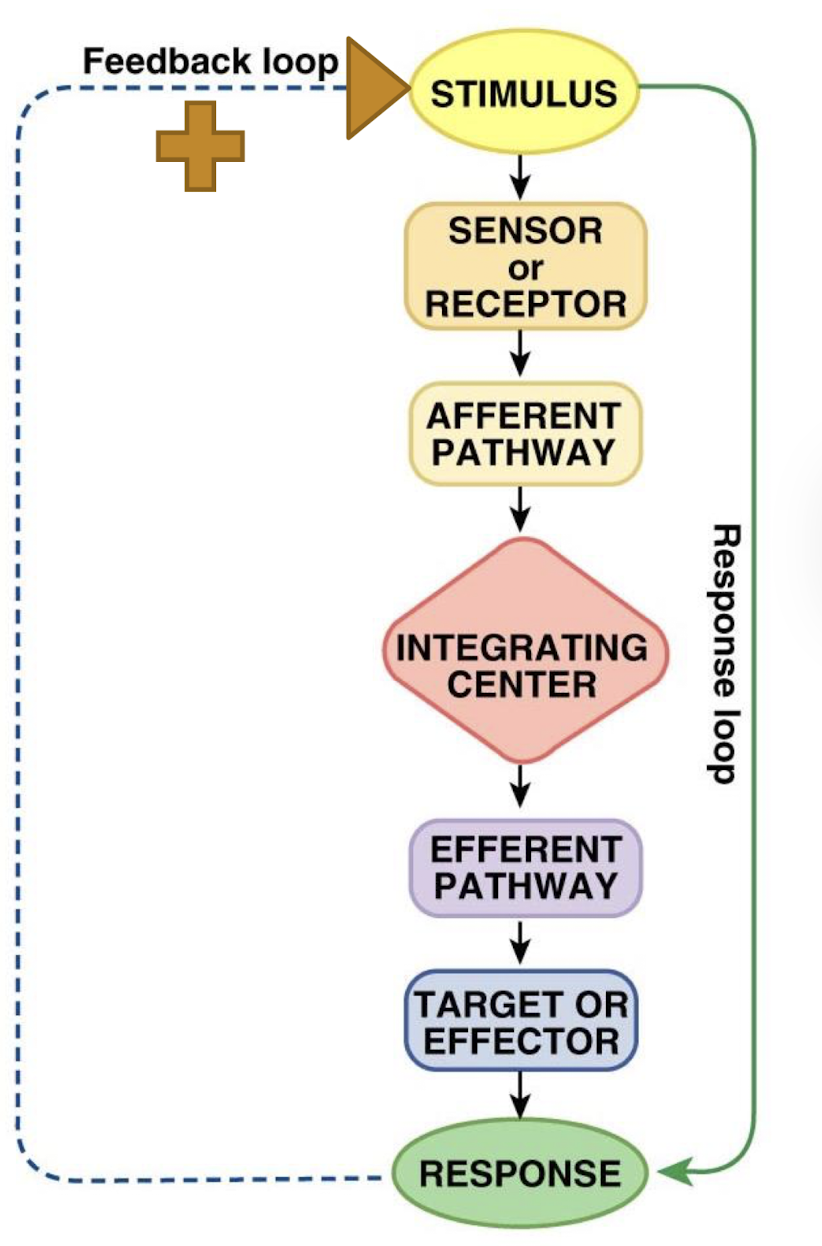
describe the negative feedback loop
homeostatic (i.e. keep regulated variable with a desired optimal range)
a negative feedback response is in the opposite direction of the stimulus
examples: thermoregulation of core body temp and Ca2+ levels in the blood
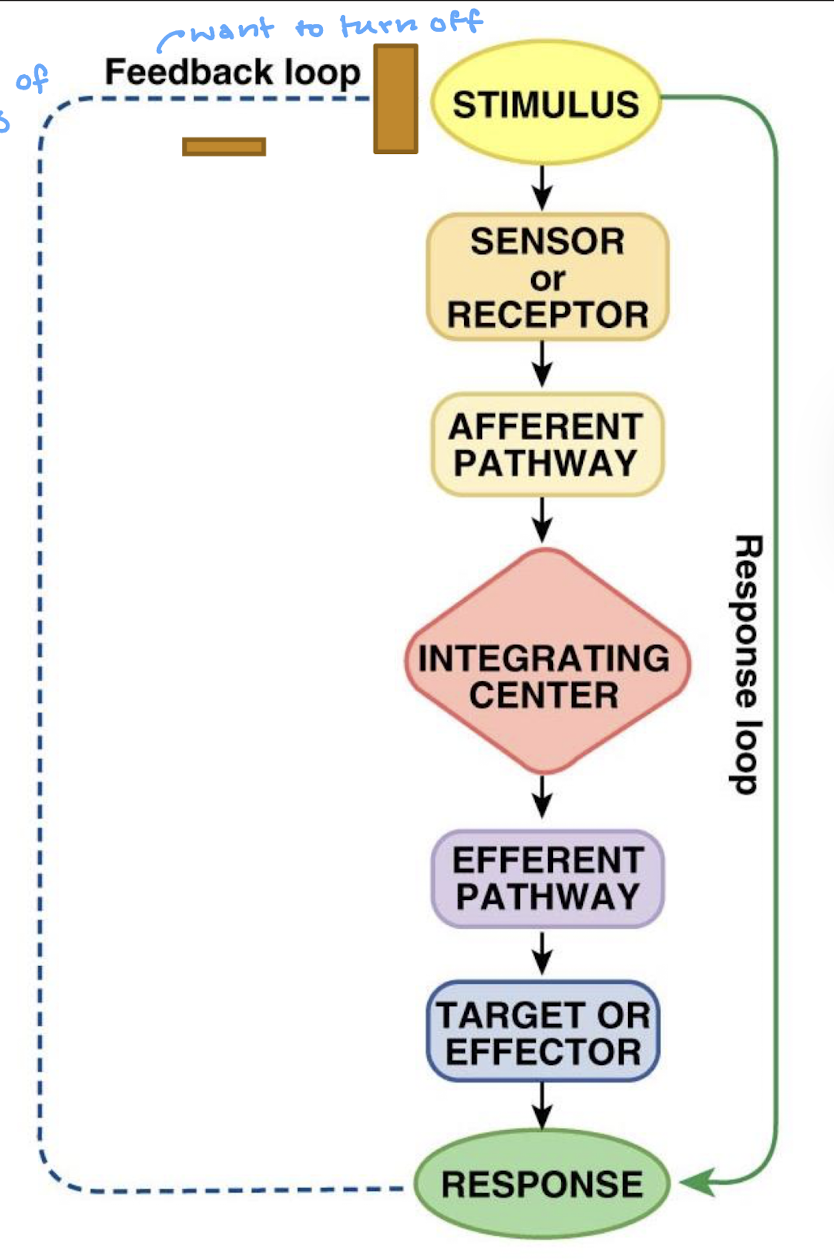
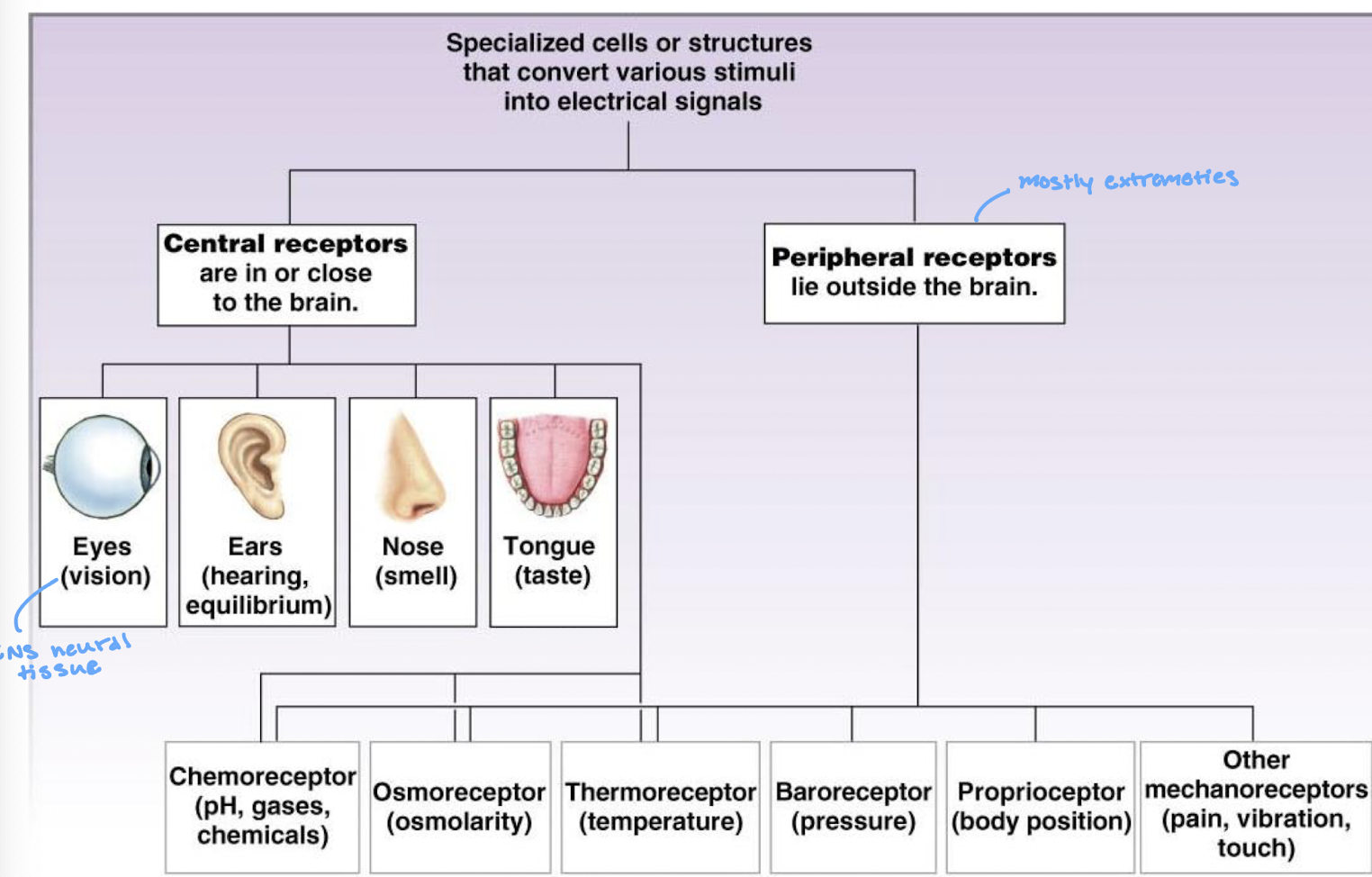
what examples of internal and external sensors/receptors
what is the regulated variable in a feedback loop
variable being monitored and maintained
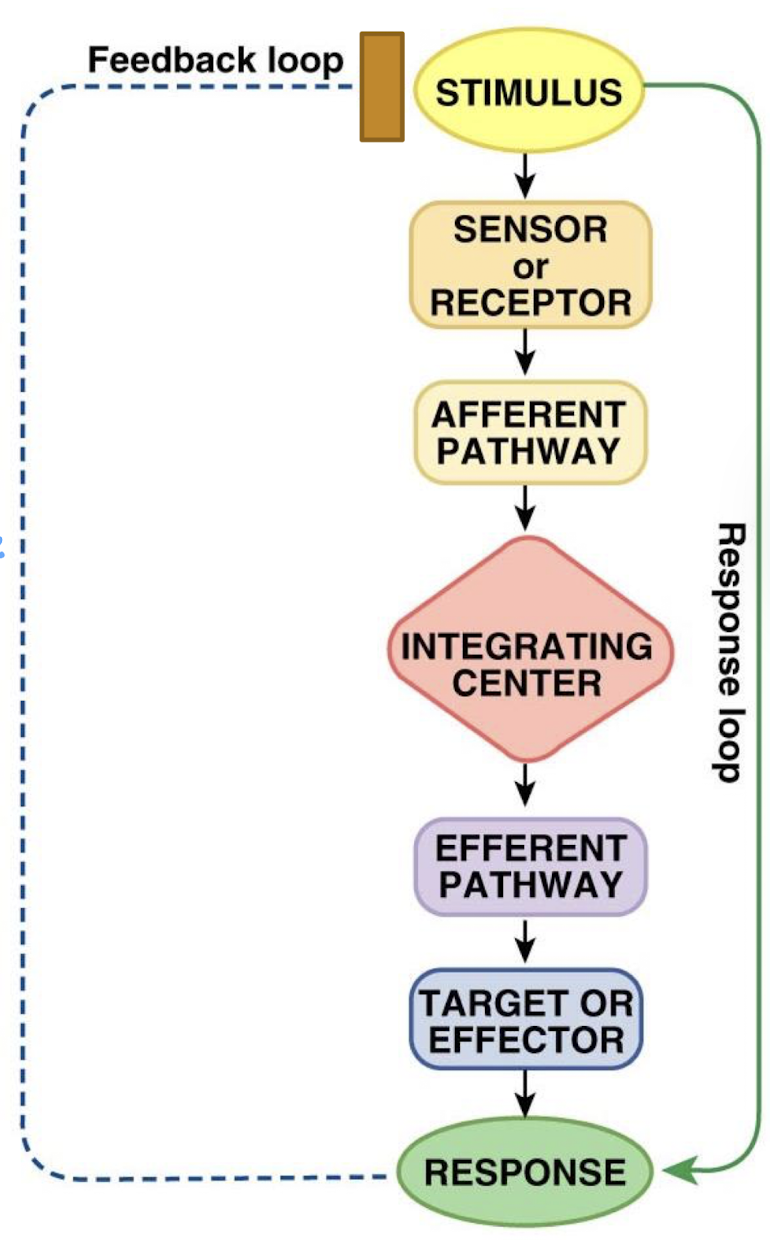
what is the stimulus in a feedback loop
an increase or decrease in regulated variable
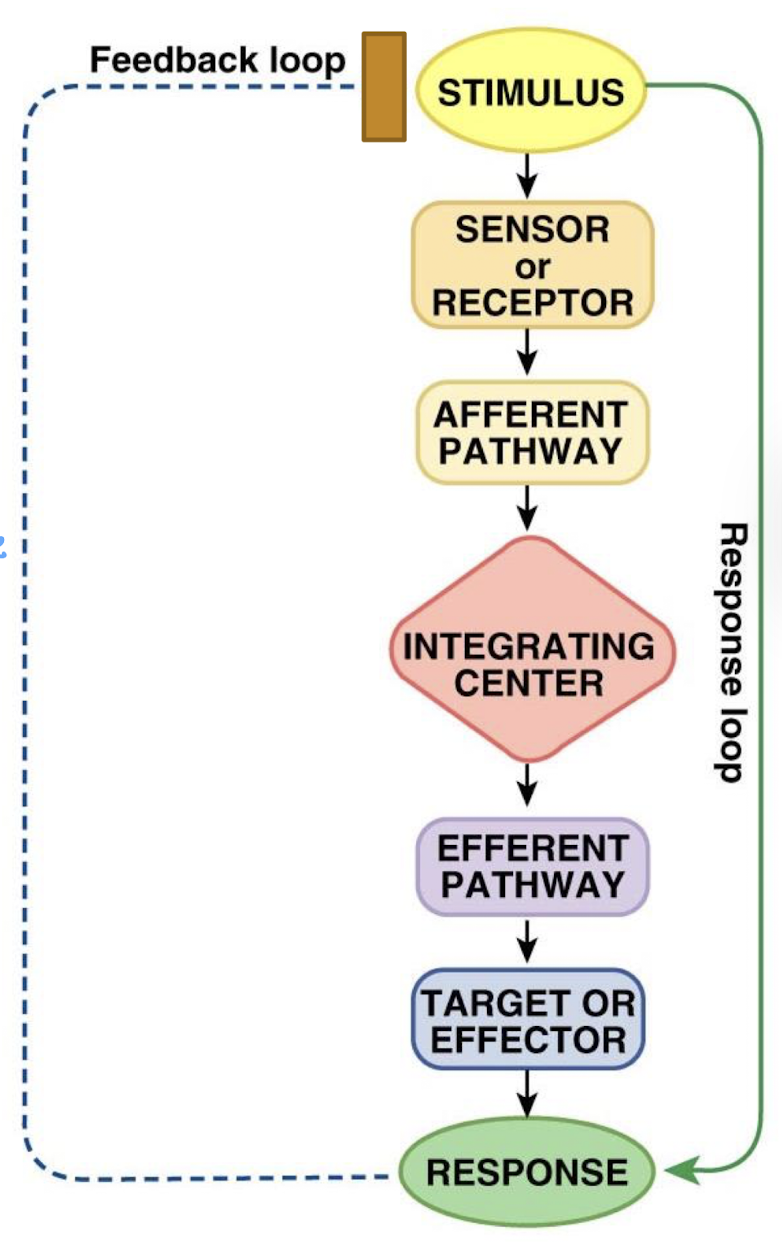
what is the sensor/receptor in a feedback loop
cells measuring the levels of regulated variable (pick up the changes)
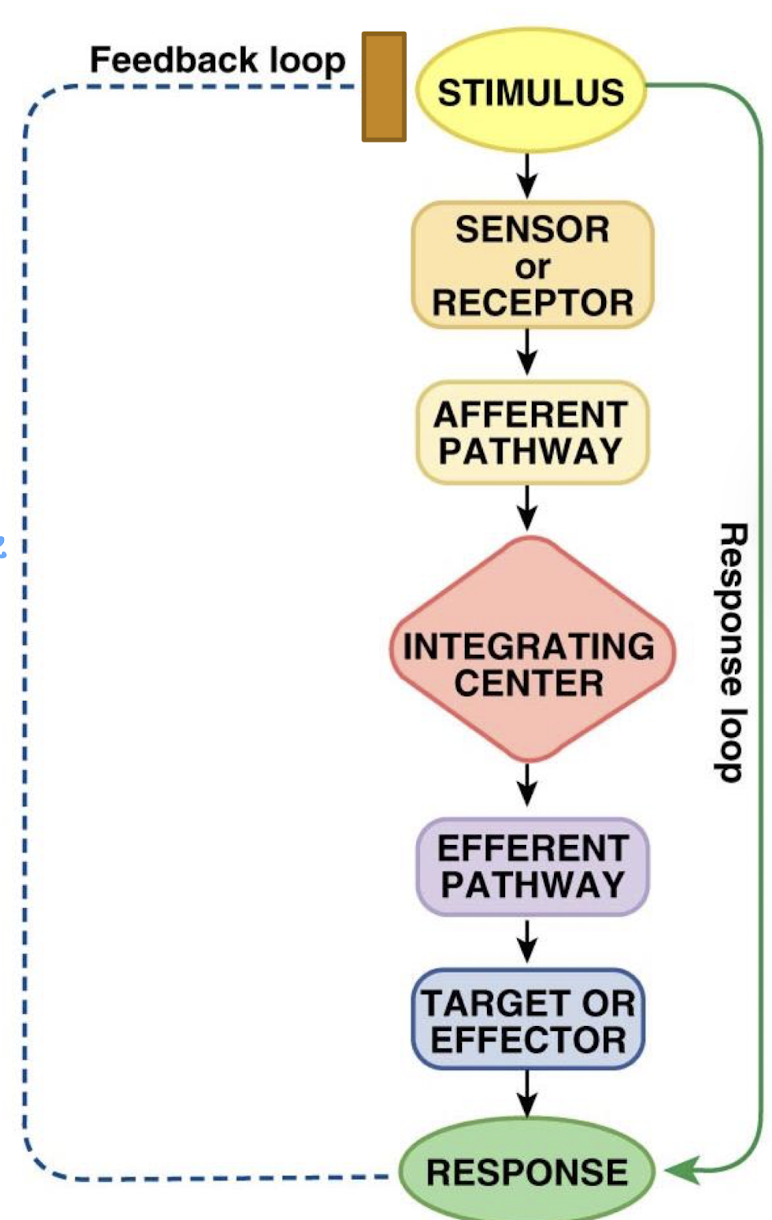
what is the setpoint in the feedback loop
desired value (usually a range) of the regulated variable
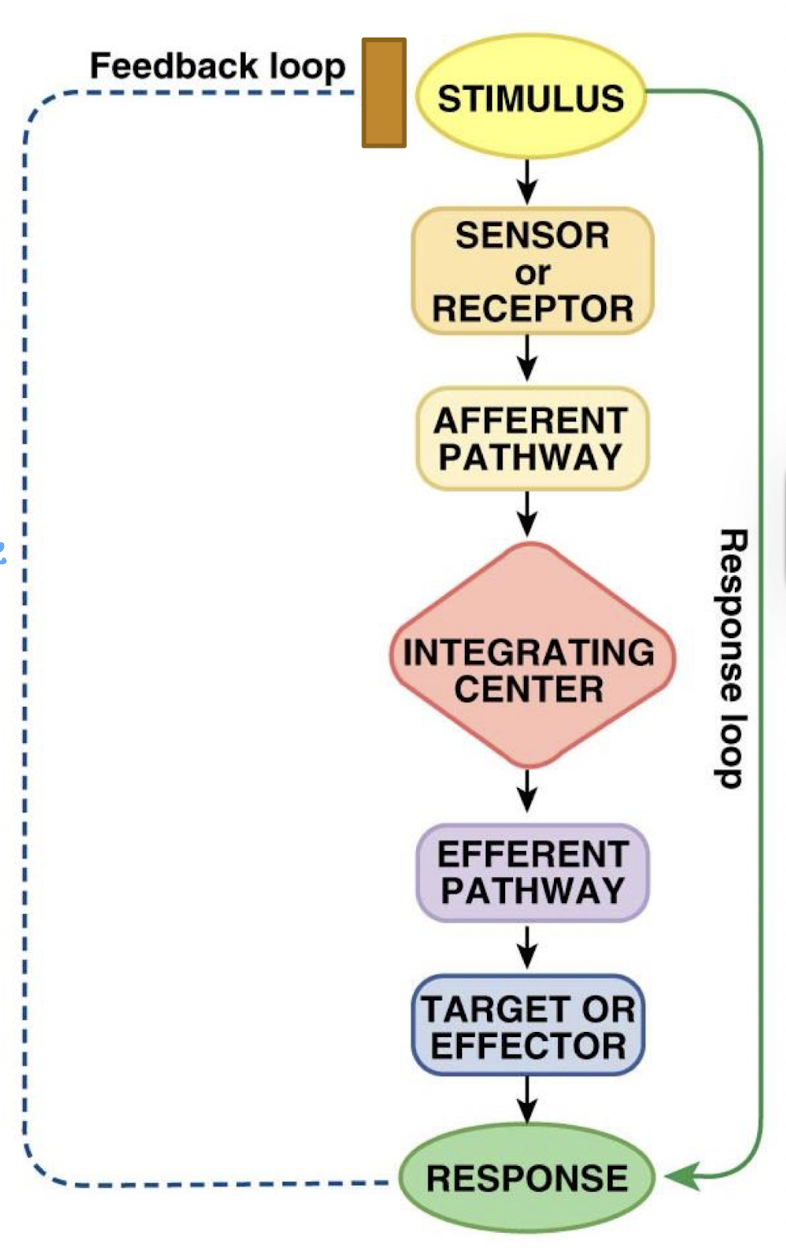
what is the afferent pathway in the feedback loop
nerves that carry signal from sensor to IC (input)
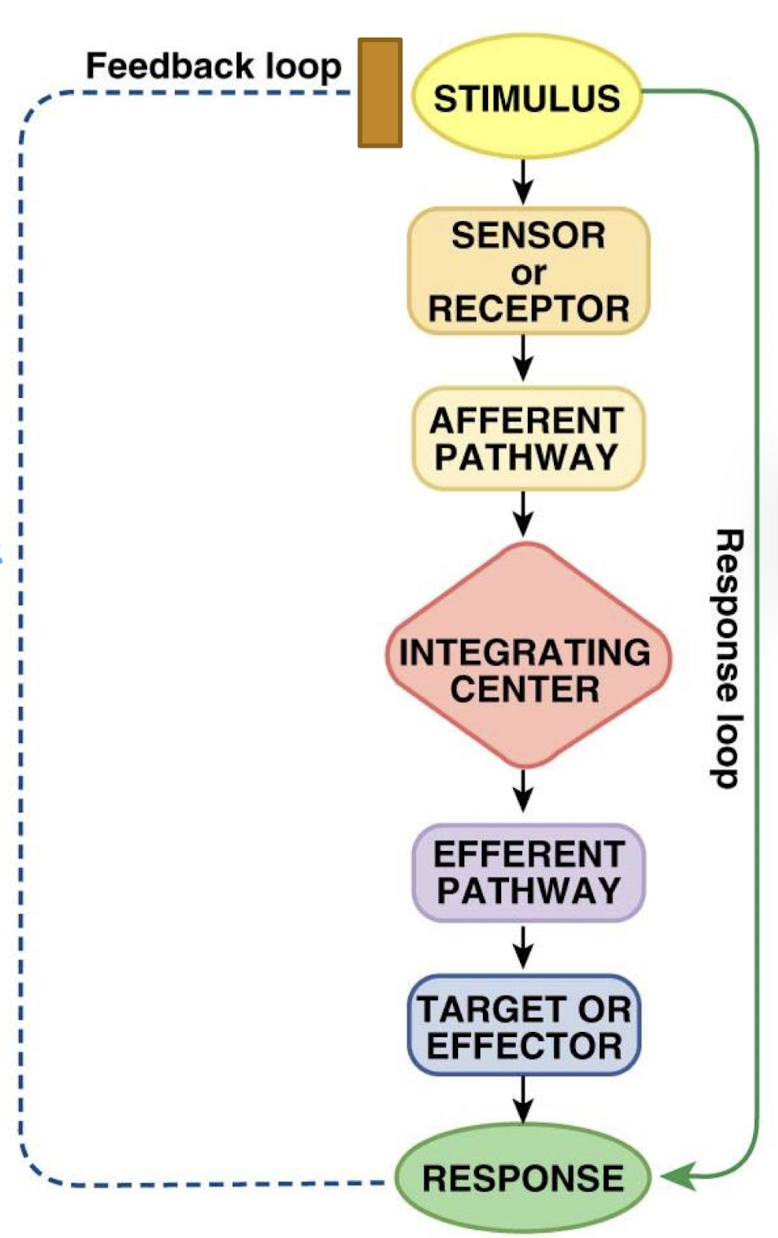
what is the integrating center (IC) in the feedback loop
the tissues, gland, or organ maintaining variable that compares “value” of the regulated variable to the setpoint and determines if any action needs to be taken
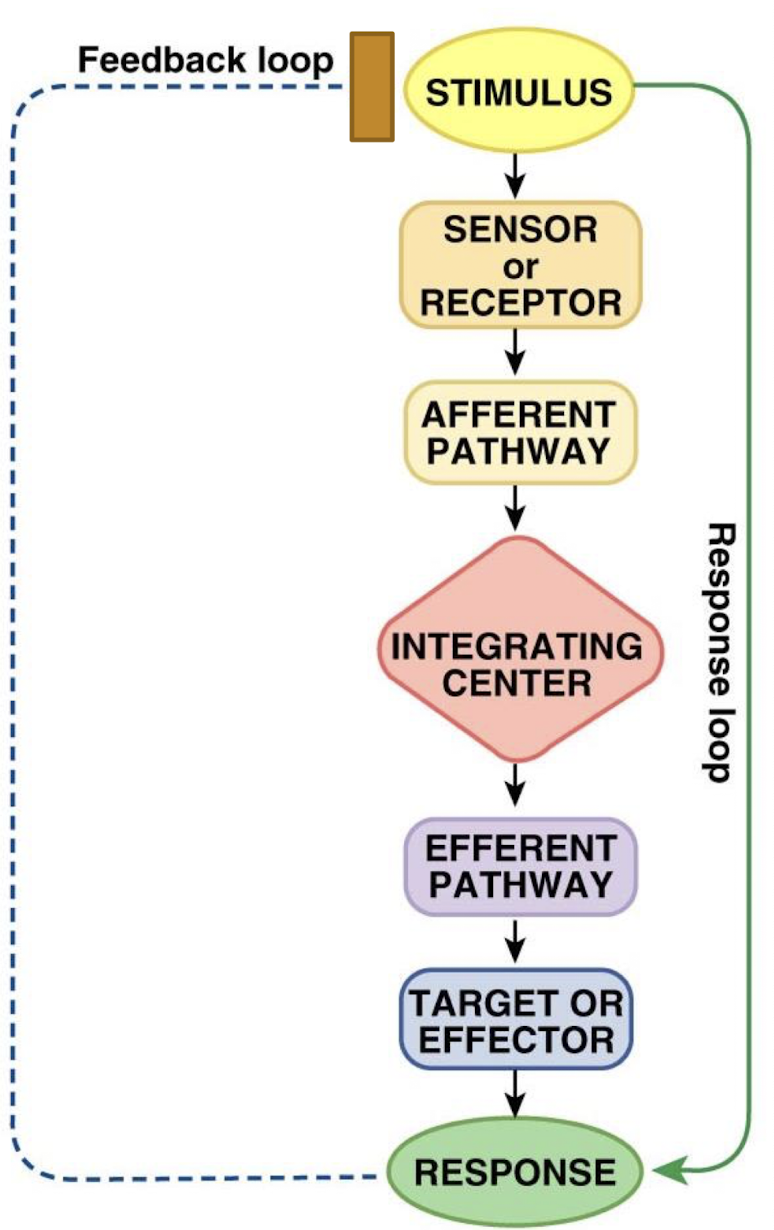
what is the efferent pathway in the feedback loop
hormones or nerves that carry signal from IC to effector tissues (the output)
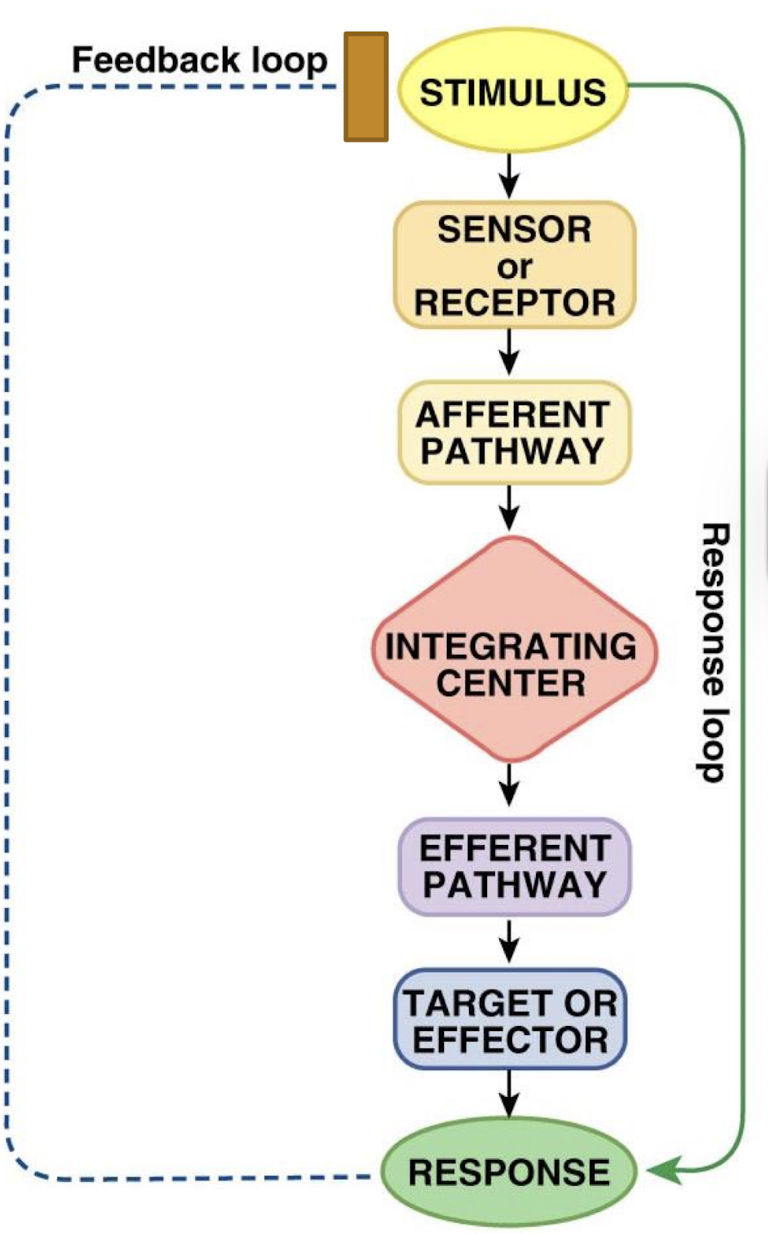
what is the effector in the feedback loop
tissue that carries out response and brings regulated variable back within desired range
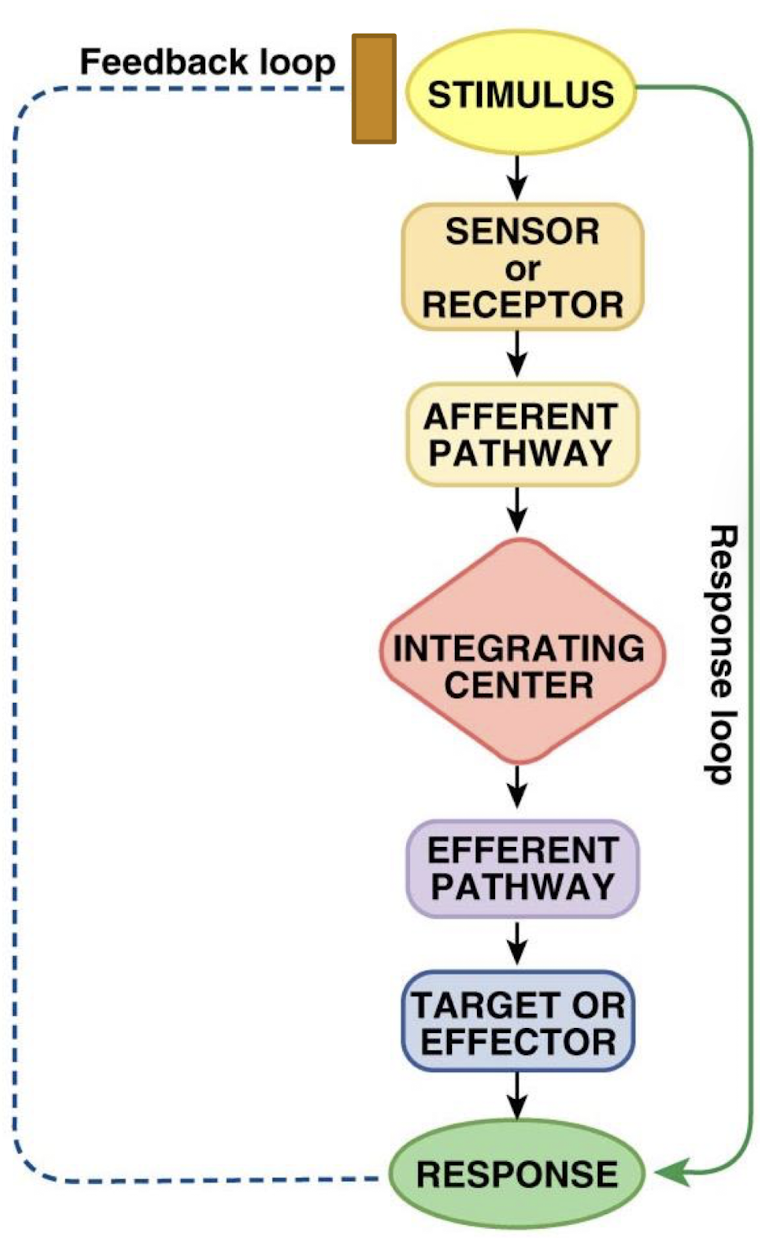
what is the response in the feedback loop
physiological or behavioral change that affects the level of the regulated variable
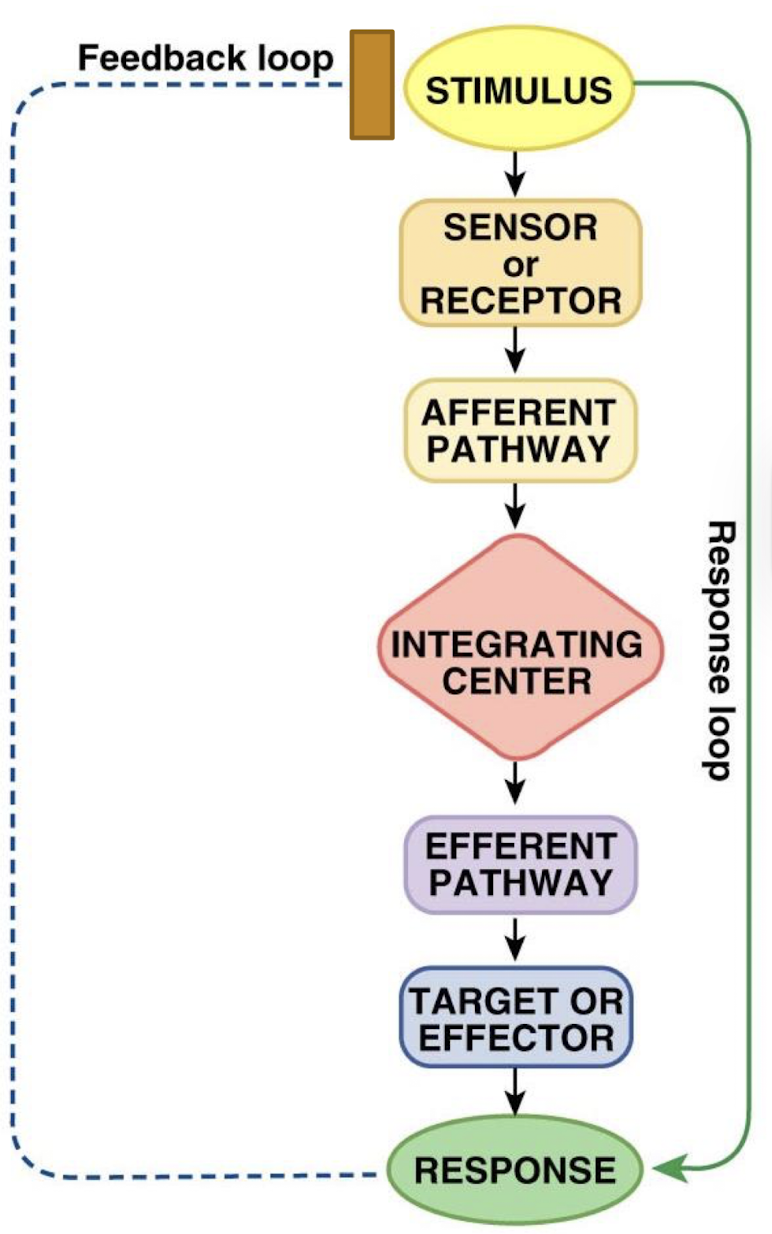
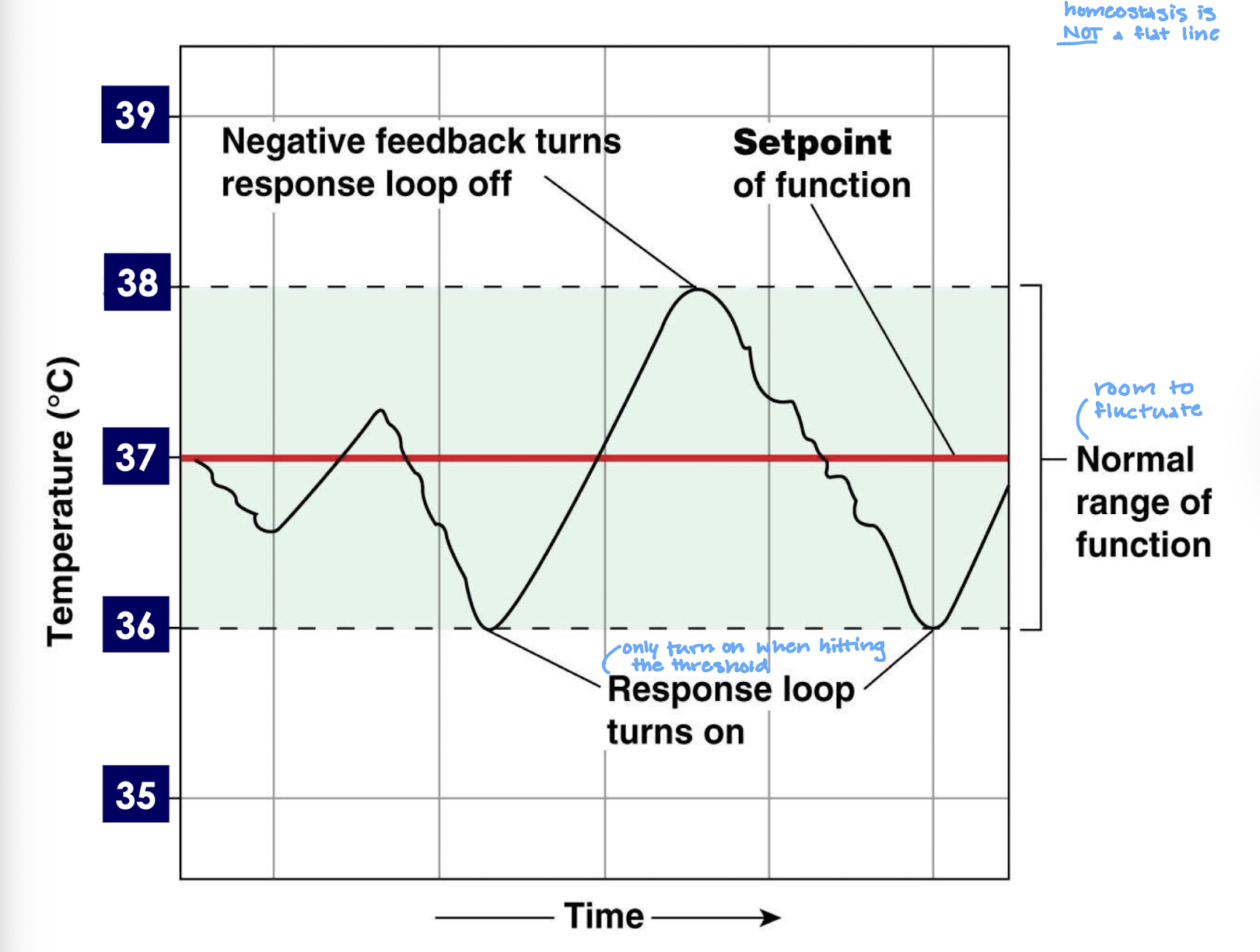
when do negative feedbacks turn response loops on/off
when the behavior (eg temperature) gets to the edge of the normal range of function
how does the body maximize heat loss with thermoregulation
vasodilation of cutaneous blood vessels
increased sweating
behavioral responses
use of fans to increase convective heat loss
immersion in water to increase conductive heat loss
staying out of the sun to prevent radiant heat gain
removing clothes
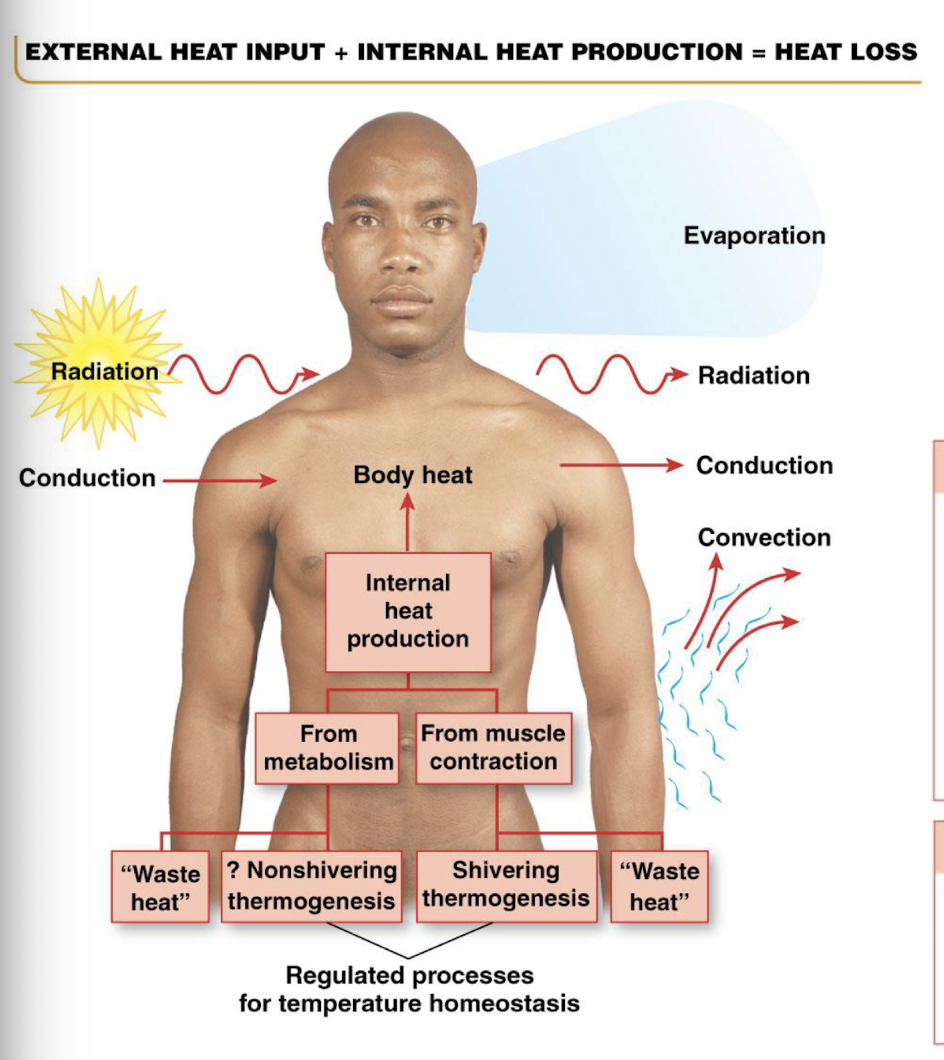
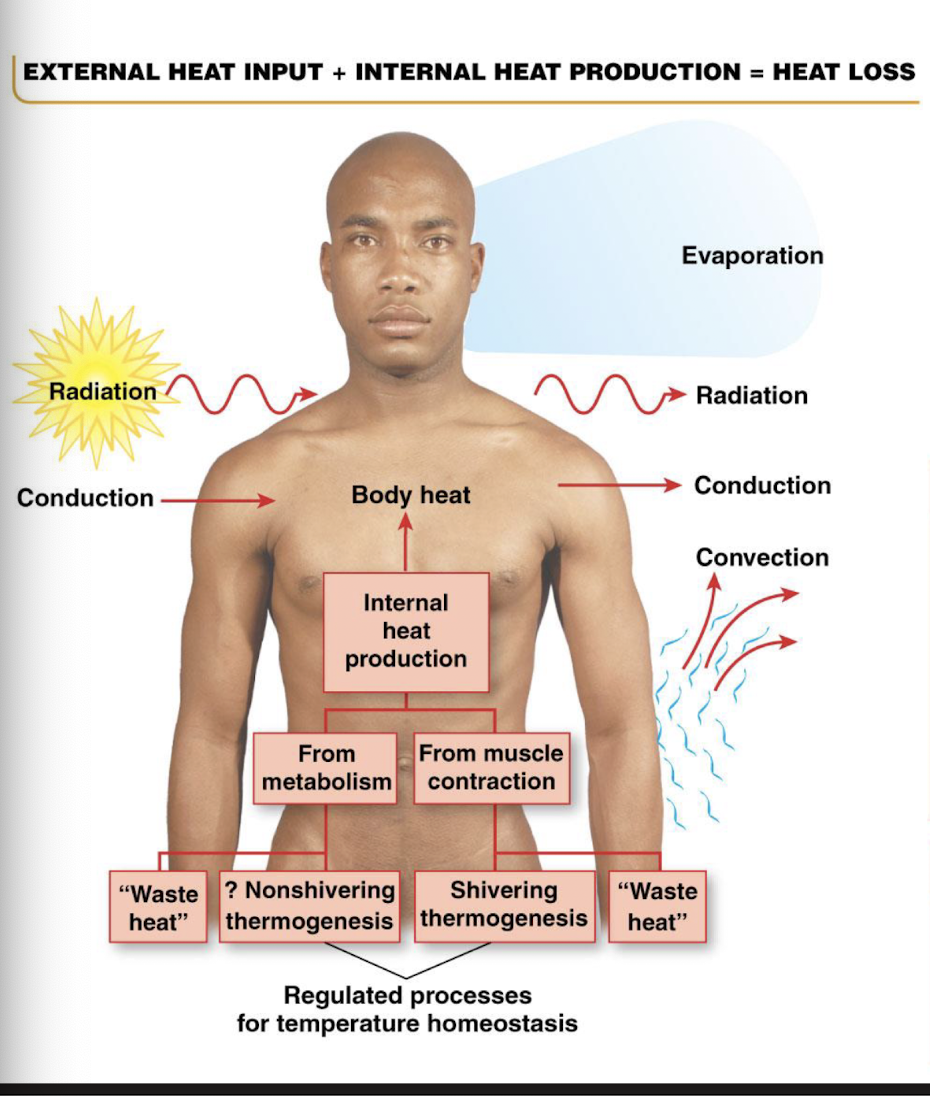
how does the body minimize heat production with thermoregulation
diminished food intake to lessen obligatory heat production
shivering and constricting vessels in response to a fever
behavioral responses
decreased physical activity
what is the regulated variable for thermoregulation for increasing Tb
core body temperature
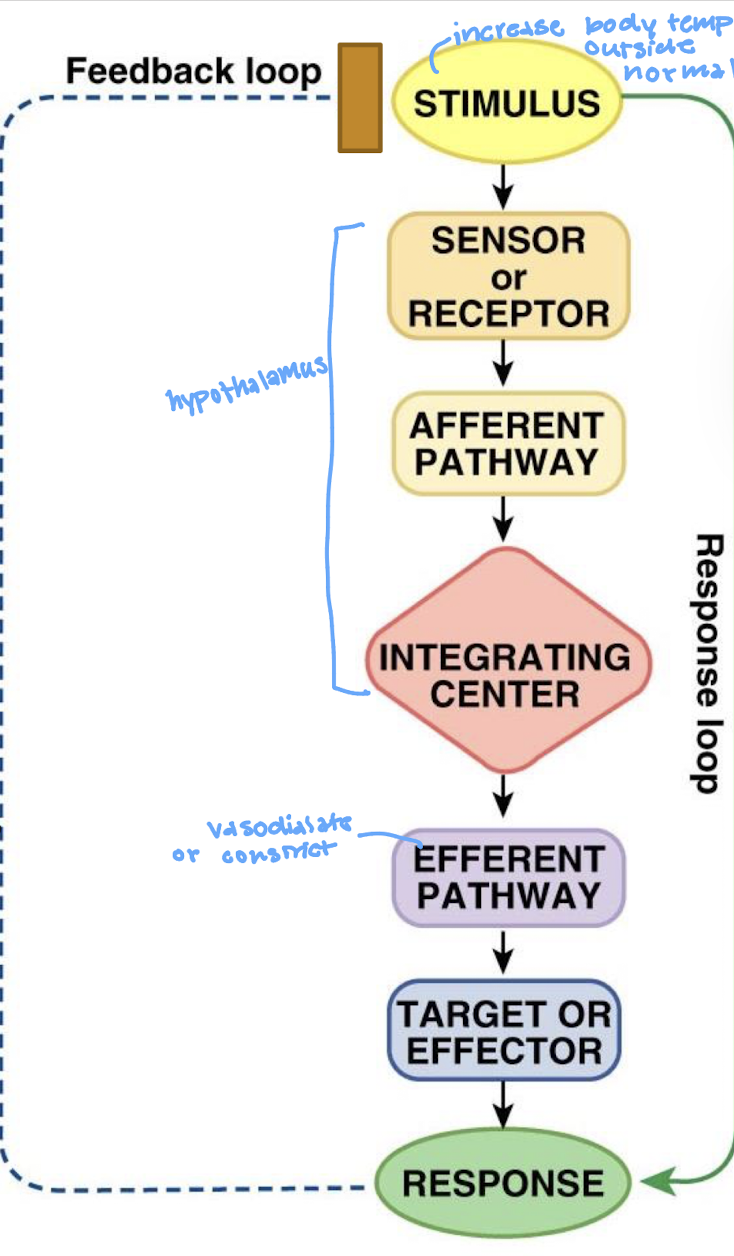
what is the stimulus for thermoregulation for increasing Tb
increase in Tb outside of range
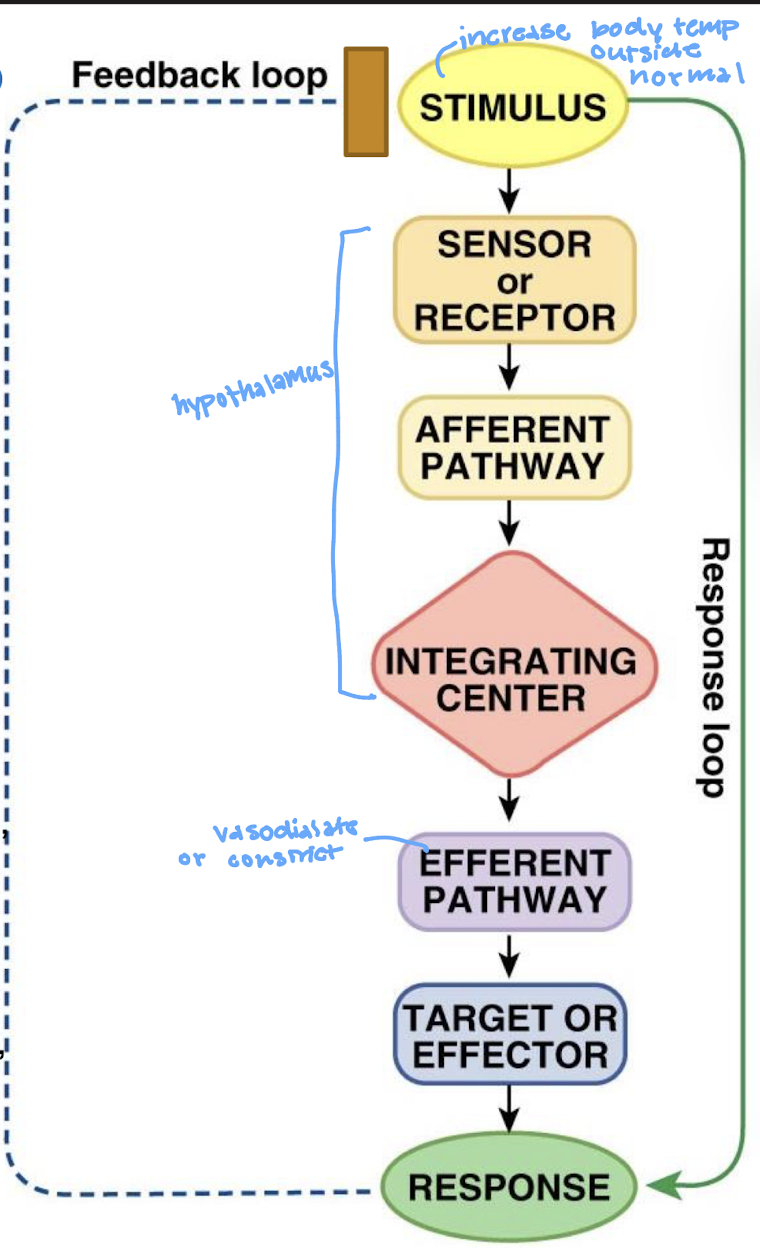
what is the sensor/receptor for thermoregulation for increasing Tb
thermoreceptor cells in the hypothalamus of the brain
what is the setpoint for thermoregulation for increasing Tb
37 degrees celsius
what is the afferent pathway for thermoregulation for increasing Tb
NONE
what is the integrating center for thermoregulation for increasing Tb
same as sensor cells
what is the efferent pathway for thermoregulation for increasing Tb
sympathetic cholinergic neurons regulate fast physiological and behavioral responses
thyroid hormones regulate metabolic pathways
what is the effector for thermoregulation for increasing Tb
arterioles, sweat glands, base of hair follicles
what is the response for thermoregulation for increasing Tb
physiological: increased vasodilation, sweating, pilorelaxation
behavioral: stretch out, decrease activity, decrease food intake, remove clothes, avoid warm environments
metabolic: decrease obligatory heat production
what is the feedback for thermoregulation for increasing Tb
decrease Tb
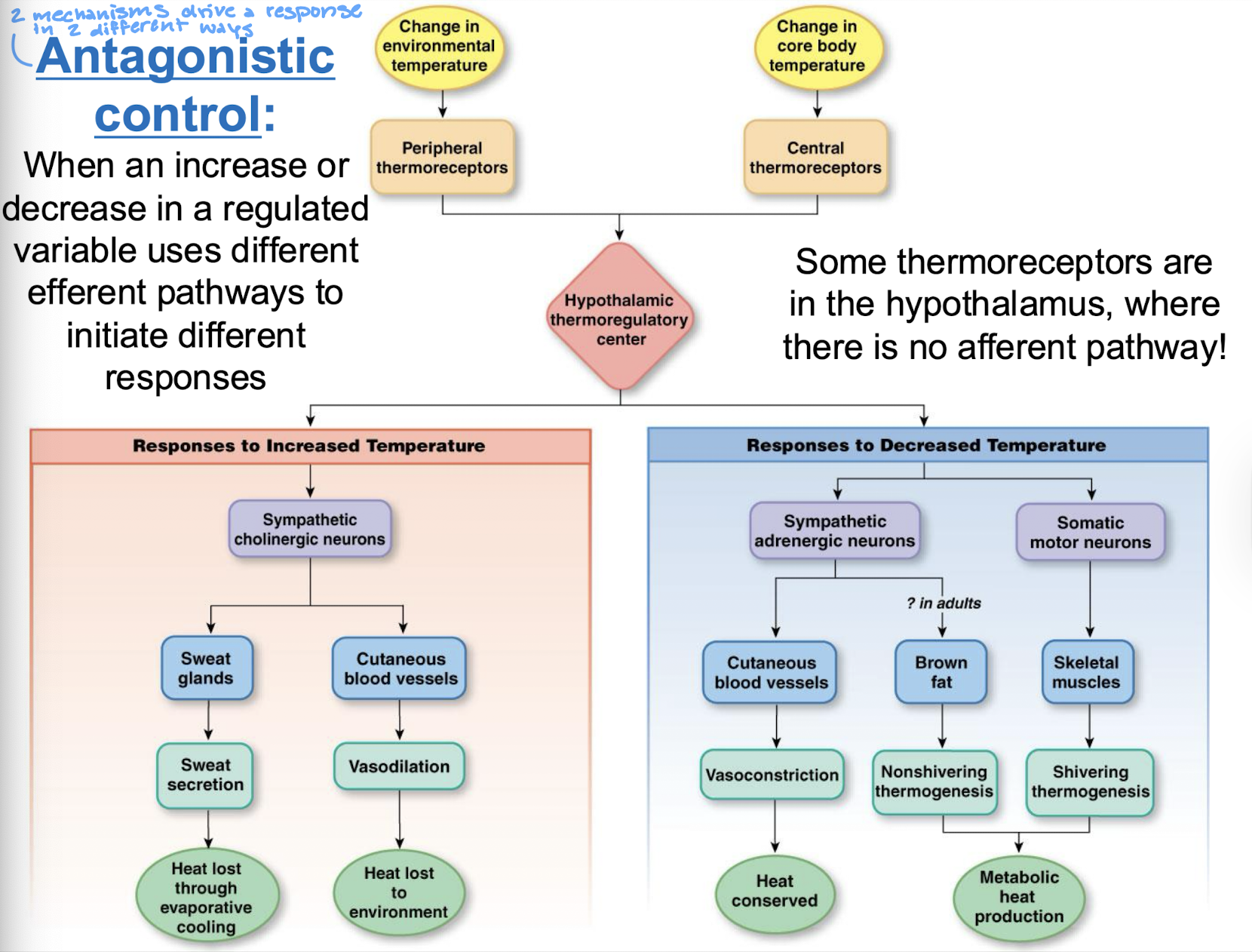
what is an antagonist control
when an increase or decrease in a regulated variable uses different efferent pathways to intiate different responses
what does it mean that acceptable ranges differ
regulated variables can be kept within a very narrow range or a much wider range depending on their importance of constancy
narrow range example:
the set point for blood pH is 7.4 and the acceptable range for pH is only 7.35-7.45
the set point for core temp is 98.8 and the acceptable range for core body temperature is 97-99 degrees F
wide range example
the set point for blood oxygen saturation is about 99nm Hg, and the acceptable range is 60-100 mm Hg
what does it mean that feedback sensitivities differ
variables that drastically impact the functioning of important processes must be maintained within a narrow range and are sensitive to even smaller changes
sensitive feedback example: blood osmolarity feedback loops activates with a 3% change in concentration
robust feedback example: blood O2 saturation feedback loops don’t activate until there is a 40% drop
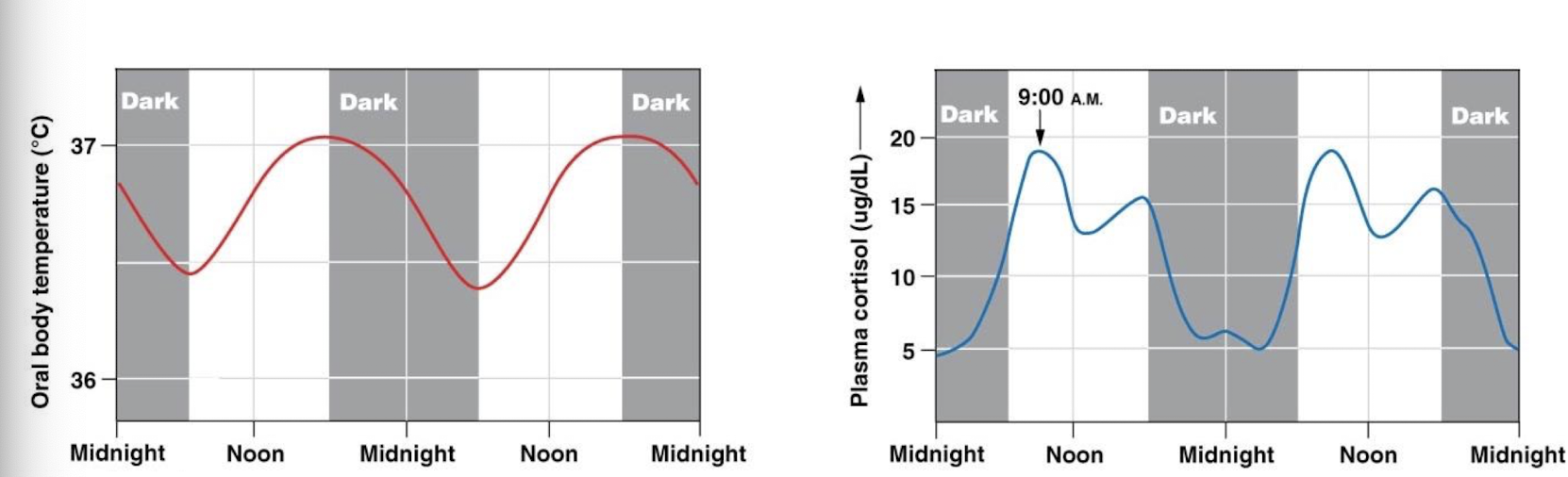
what does it mean that setpoints are not fixed
set points for different individuals can vary
setpoints for an individual can change
increased Tb setpoint during exercise, fever, ovulation
decreased Tb setpoint during sleep and hibernation
circadian rhythms are due to changing setpoints
what does it mean that not everything is regulated
physiological regulation is used to regulate only the most important variables needed to sustain life
the vital list
ions: Na+, K+, Ca2+
gases: O2 and CO2
physical properties: osmolarity, blood pressure, temperature
nutrients: glucose levels (brain fuel)
what are the benefits to regulation
regulation of the internal environment means cells don’t have to withstand changes in their immediate environment
enzymes and other biochemical systems can evolve to work optimally under a specific set of conditions
what are the costs to regulation
it’s EXPENSIVE
it takes a lot of energy to generate and dissipate heat, or maintain ion balance within the body
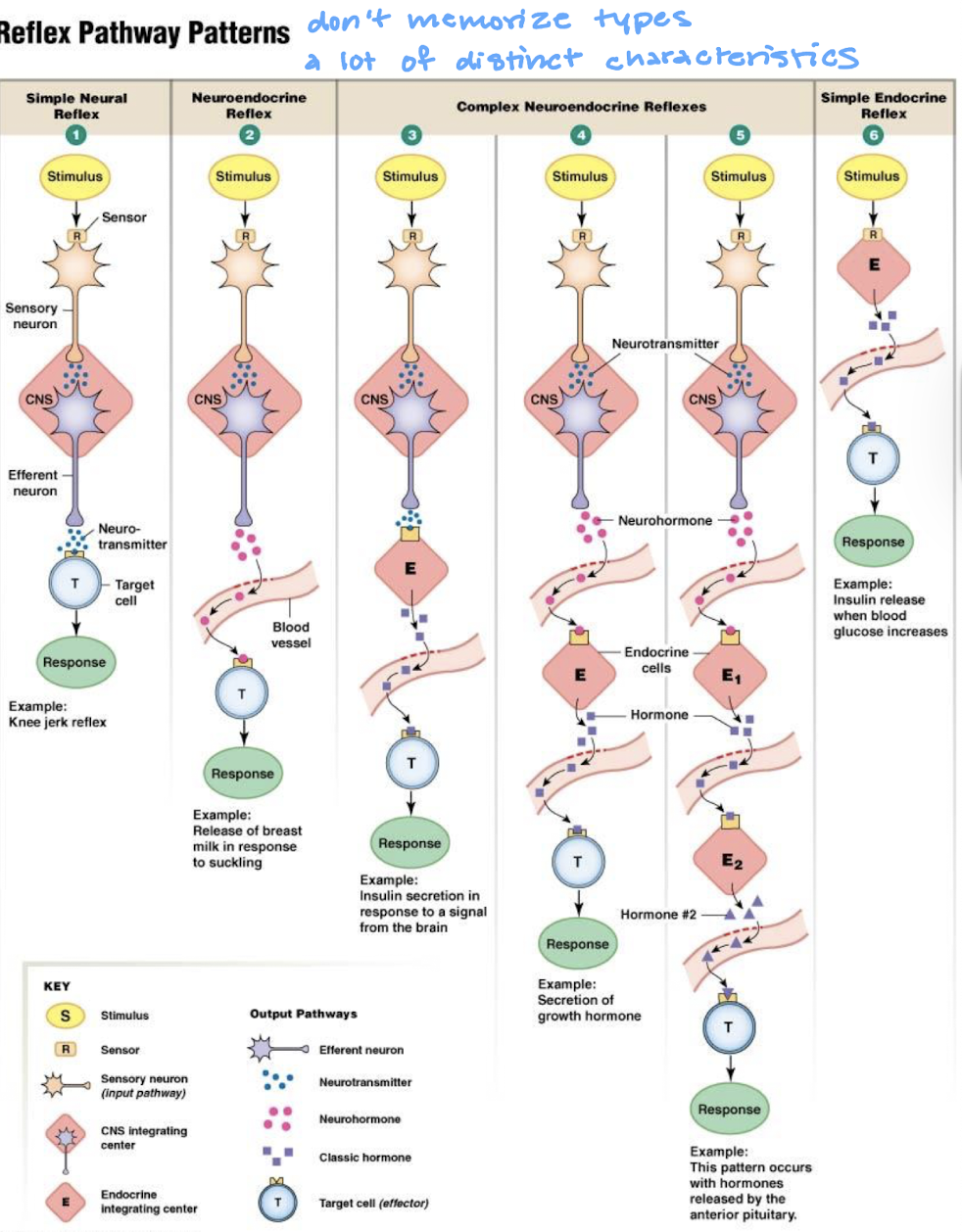
what is meant by feedback loops are not all the same
they may have more than one integrating center
they may have more than one efferent pathway controlled by nerves and/or hormones
they often have multiple response to regulate the variables
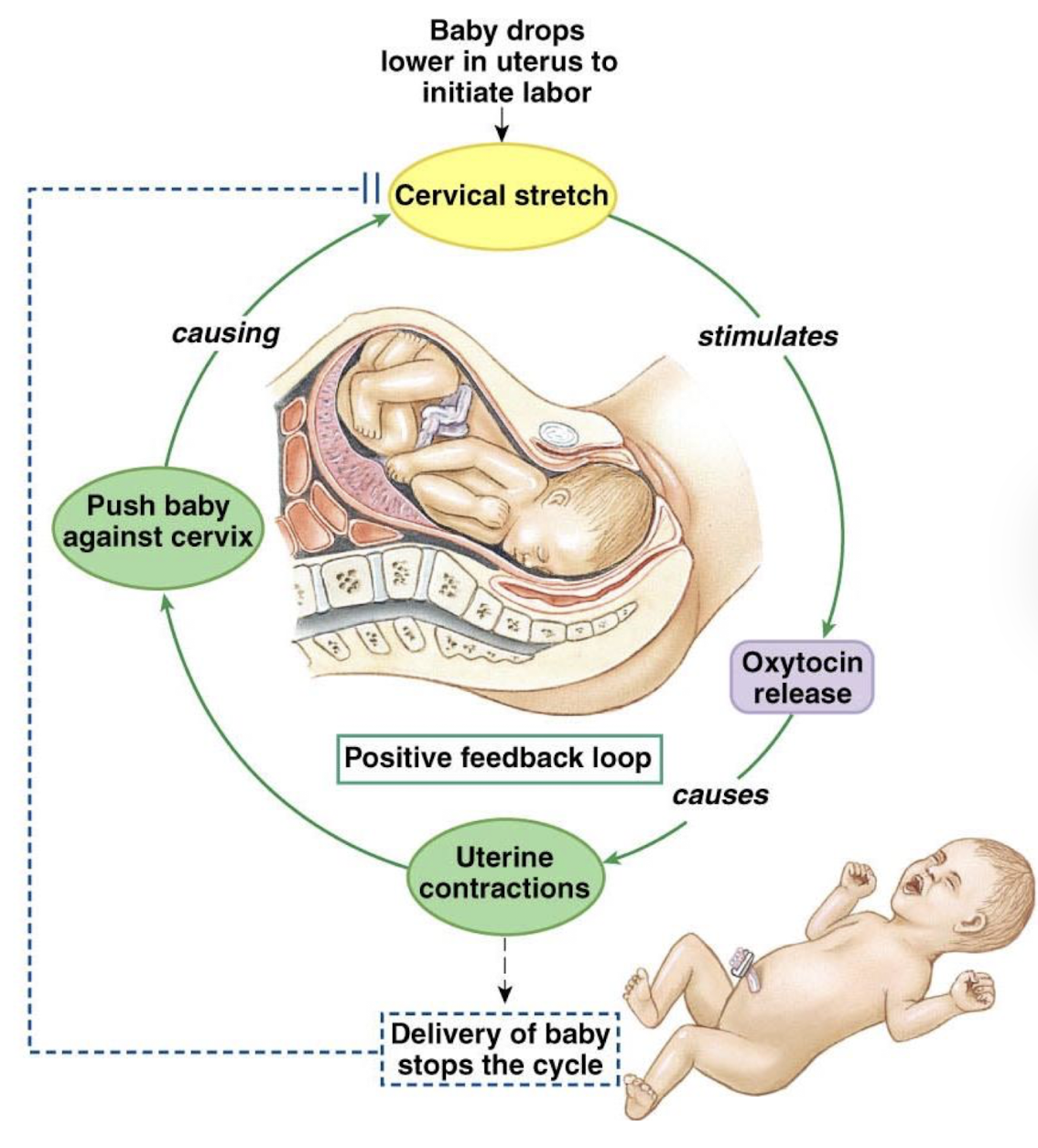
describe positive feedback loops
non-regulatory (i.e. increases the difference between the level of the regulated variable and the setpoint until an external change occurs that restores homeostasis)
response is in the SAME direction as the stimulus
examples
labor and delivery
erections
nerve action potentials
blood clotting
what is the stimulus in labor
cervical stretch
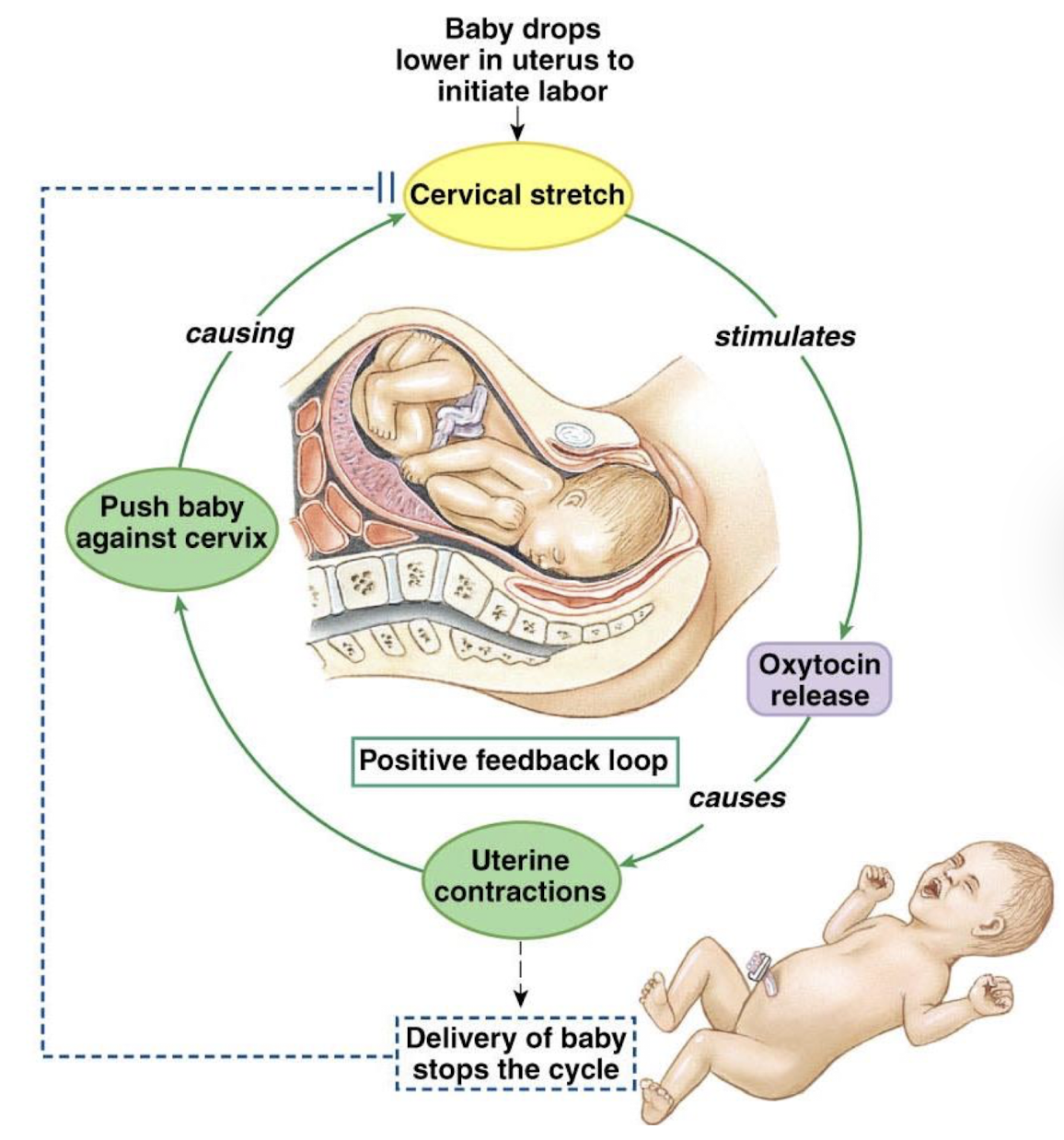
what is the sensor/receptor in labor
stretch receptors in cervix
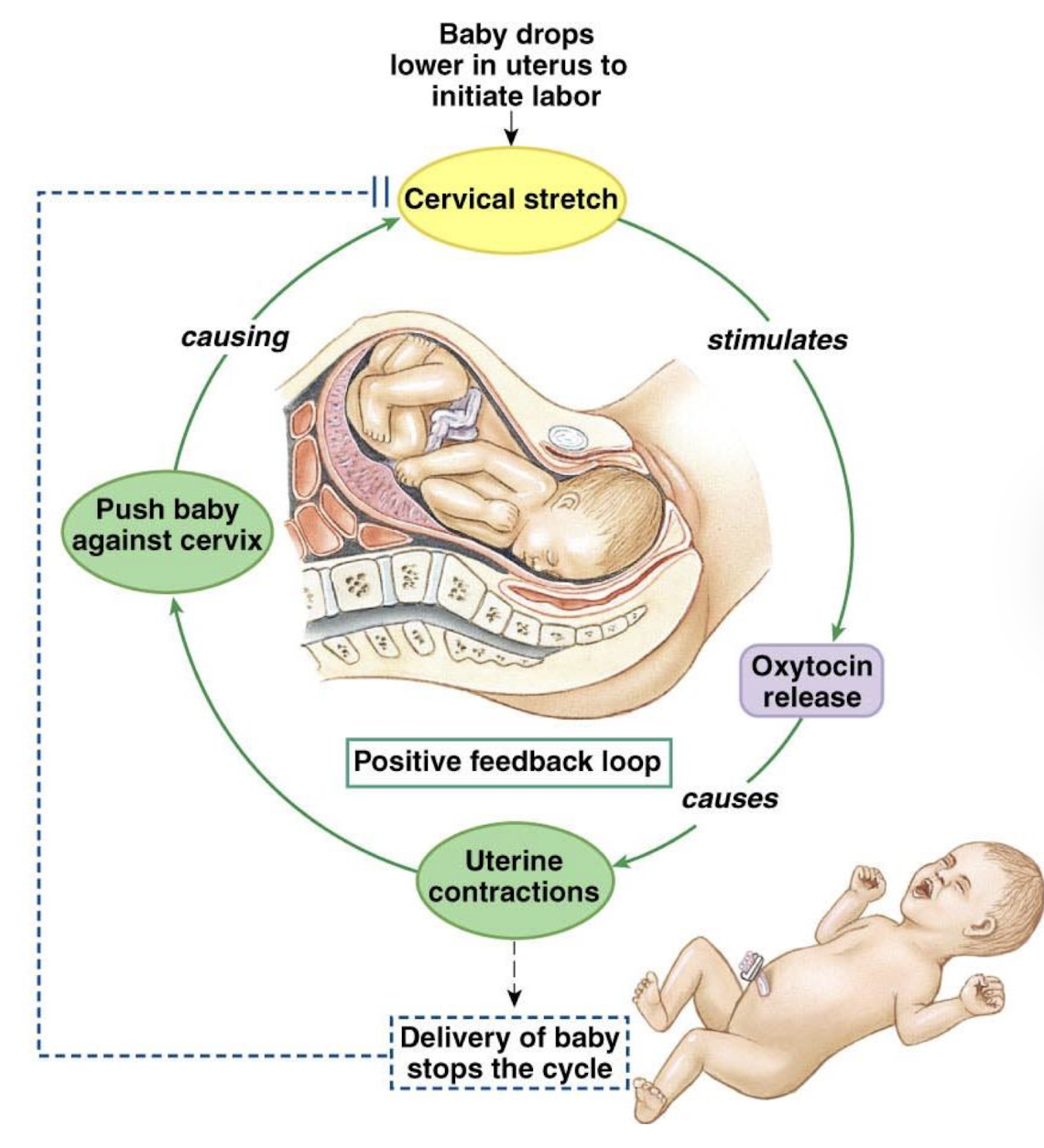
what is the setpoint in labor
no stretch