Chapter 21: The Cardiovascular System: Blood Vessels and Hemodynamics
1/36
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
37 Terms
Describe the structure and function of arteries
Role: Carry blood away from the heart to other organs
Structure: Thick tunica media (consisting of smooth muscle and elastic fibers)
What are two types of arteries?
Elastic (conducting) arteries have large diameters and act as a pressure reservoir, propelling blood forward during ventricular relaxation
Muscular (distributing) arteries are medium-sized and capable of greater vasoconstriction and vasodilation to adjust flow to specific regions
Describe the structure and function of arterioles
Structure: Abundant microscopic vessels that regulate blood flow into capillary networks
Role: Known as resistance vessels because they control flow by altering their diameter
Vasoconstriction increases resistance and decrease flow
Vasodilation increases flow, decreases resistance
Describe the structure and function of capillaries
Structure:
Smallest vessels (5–10 μm in diameter), forming "U-turns" that connect arterial outflow to venous return
Termed exchange vessels, their walls consist only of a single layer of endothelial cells and a basement membrane
Role: Enables exchange of nutrients, gases, and wastes between blood and interstitial fluid
Describe the structure and function of venules
Role: Drain capillary blood and begin the return flow toward the heart
Structure:
Postcapillary venules are porous and significant sites of nutrient exchange and white blood cell emigration
Muscular venules have thicker walls and serve as reservoirs for large volumes of blood
Describe the structure and function of veins
Role: Convey blood from tissues back to the heart
Structure: They have thinner walls and larger lumens than arteries
Many, especially in the limbs, contain valves to prevent the backflow of blood
Outline the vessels through which the blood moves in its passage from the heart to the capillaries and back
Blood moves from the heart through elastic arteries, muscular arteries and arterioles into the capillaries
It returns through post-capillary venules, muscular venules and veins back to the heart
Discuss the pressures that cause movement of fluids between capillaries and interstitial spaces
Movement between capillaries and interstitial spaces is driven by bulk flow (filtration and reabsorption)
Bulk flow = Passive process in which large numbers of ions or particles in a fluid move together in the same direction
Compare and contrast: Filtration vs. Reabsorption
Filtration: Pressure-driven movement of fluid and solutes from blood capillaries into interstitial fluid
Promoted by:
blood hydrostatic pressure (BHP) (~35 mmHg at the arterial end)
interstitial fluid osmotic pressure (IFOP) (~1 mmHg)
Reabsorption: Pressure-driven movement from interstitial fluid into blood capillaries
Promoted by:
blood colloid osmotic pressure (BCOP) (~26 mmHg)
interstitial fluid hydrostatic pressure (IFHP) (~0 mmHg)
What balances filtration and reabsorption?
Net filtration pressure (NFP) determines whether the volumes of blood and interstitial fluid remain steady OR changes
Determines the direction:
Positive (+10 mmHg) at the arterial end (filtration)
Negative (−9 mmHg) at the venous end (reabsorption)
Explain the factors that regulate the volume of blood flow
Total blood flow is cardiac output (CO), determined by heart rate and stroke volume
Distribution to tissues depends on the pressure difference (higher pressure drives more flow) and vascular resistance (higher resistance reduces flow)
Explain how blood pressure changes throughout the cardiovascular system
BP is highest in the aorta (~110/70 mmHg) and falls progressively as it moves through systemic arteries, arterioles, and capillaries (~16 mmHg at the venous end)
It continues to drop in venules and veins, reaching 0 mmHg as it enters the right ventricle
Describe the factors that determine mean arterial pressure and systemic vascular resistance
Mean Arterial Pressure (MAP) is the average arterial pressure, determined by CO and vascular resistance (MAP=CO×R)
Systemic Vascular Resistance (SVR) is the total opposition to flow, determined by blood vessel lumen size, blood viscosity, and total vessel length
Arterioles are the primary regulators of SVR
Describe the relationship between cross-sectional area and velocity of blood flow
Velocity is inversely related to the total cross-sectional area of the vessels
Flow is slowest in the capillaries (where area is greatest), which facilitates material exchange
Describe how blood pressure is regulated
BP is controlled by interconnected systems:
Cardiovascular (CV) center: Located in the medulla oblongata, it receives input from the brain (limbic system, hypothalamus) and sensory receptors (proprioceptors, baroreceptors, chemoreceptors). It provides output via the sympathetic and parasympathetic nervous systems.
Baroreceptor Reflexes: Carotid sinus and aortic reflexes monitor stretch; a fall in BP triggers increased sympathetic stimulation to raise CO and SVR.
Hormones: The RAA system, epinephrine/norepinephrine, and ADH increase BP, while atrial natriuretic peptide (ANP) decreases it
Autoregulation: Tissues automatically adjust local flow based on metabolic needs, responding to physical changes (temperature, stretch) and vasodilating chemicals (NO, H+, K+).
Define pulse
The traveling pressure wave created by the alternate expansion and recoil of elastic arteries
Define systolic BP
The highest pressure attained in arteries during ventricular contraction
Define diastolic BP
The lowest arterial pressure during ventricular relaxation
Define pulse pressure
The difference between systolic and diastolic blood pressure, normally about 40 mmHg
Define shock
Shock is a failure of the cardiovascular system to deliver enough O2 and nutrients to meet the metabolic needs of cells
Describe the four types of shock
Hypovolemic: Caused by decreased blood volume (e.g., hemorrhage).
Cardiogenic: Caused by poor heart function (e.g., heart attack).
Vascular: Caused by inappropriate vasodilation (e.g., severe allergic reaction or bacterial toxins).
Obstructive: Caused by the blockage of blood flow (e.g., pulmonary embolism)
Explain how the body’s response to shock is regulated by negative feedback.
The body initiates compensatory systems to restore volume and pressure:
Activation of the RAA system (conserves salt/water)
Secretion of ADH (conserves water)
Activation of the sympathetic ANS (increases HR, contractility, and causes vasoconstriction)
Define systemic circulation and explain its importance
Systemic circulation includes all vessels carrying oxygenated blood from the left ventricle to capillaries and returning deoxygenated blood to the right atrium.
It is vital for delivering nutrients/oxygen to all body tissues and removing wastes and heat
Identify the four principal divisions of the aorta
Ascending Aorta: The initial segment emerging from the left ventricle.
Arch of the Aorta: The continuation of the ascending aorta that loops to the left.
Thoracic Aorta: The portion of the aorta that descends through the chest, ending at the diaphragm.
Abdominal Aorta: The segment below the diaphragm that descends to the fourth lumbar vertebra
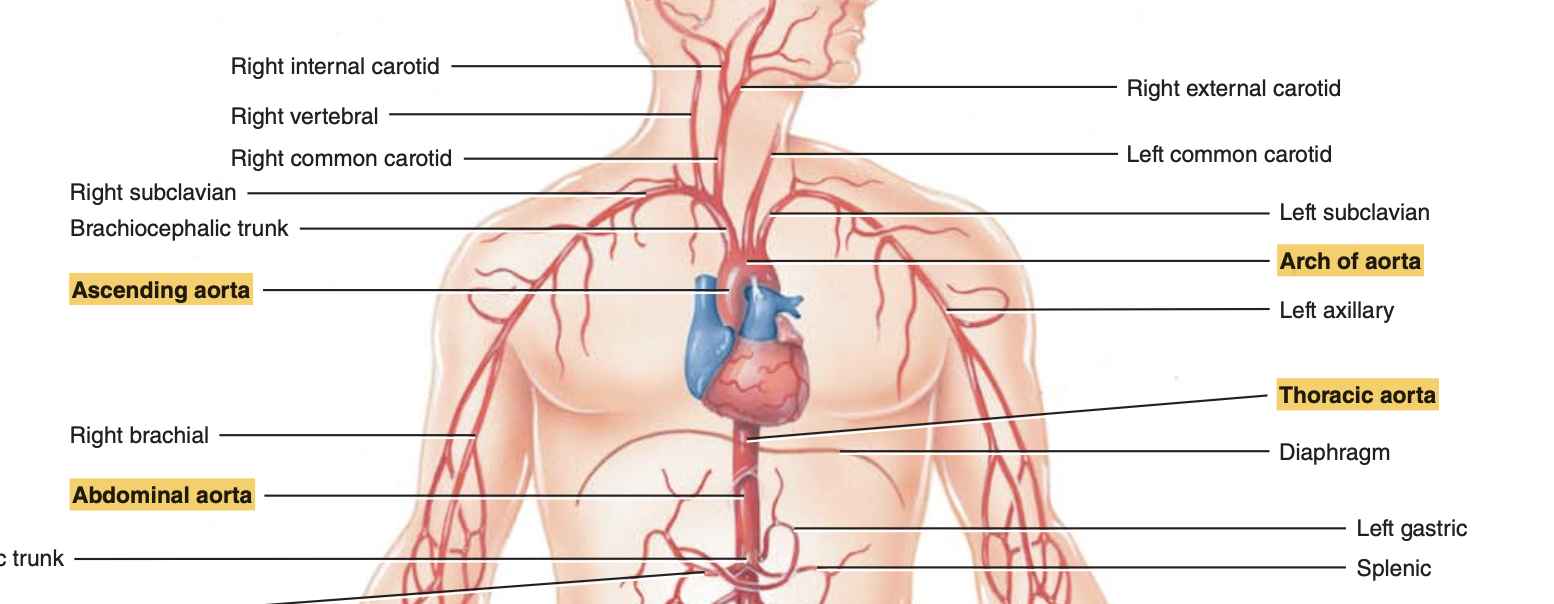
Locate the major arterial branches arising from each division
Ascending: Coronary arteries.
Arch: Brachiocephalic trunk, left common carotid, and left subclavian.
Thoracic: Visceral (pericardial, bronchial, esophageal, mediastinal) and parietal (intercostal, subcostal, phrenic) branches.
Abdominal: Visceral (celiac trunk, mesenterics, renals, gonadal) and parietal (phrenic, lumbar, sacral) branches
Identify the two primary arterial branches of the ascending aorta
Right Coronary Artery: Supplies the myocardium of the right atrium and both ventricles.
Left Coronary Artery: Supplies both ventricles and the left atrium; includes the major "LAD" branch
Identify the three principal arteries that branch from the arch of the aorta.
In order of origination: Brachiocephalic trunk, left common carotid artery, and left subclavian artery
Brachiocephalic Trunk: The first and largest branch; divides into the right subclavian and right common carotid.
Left Common Carotid Artery: Supplies the left side of the head and neck.
Left Subclavian Artery: Distributes blood to the left upper limb
Identify the visceral and parietal branches of the thoracic aorta
Visceral Branches: Supply organs
Includes Pericardial (pericardium), Bronchial (bronchi), Esophageal (esophagus), and Mediastinal (mediastinum tissues) arteries
Parietal Branches: Supply the body wall.
Includes Posterior Intercostal (ribs/muscles), Subcostal (abdominal wall), and Superior Phrenic (diaphragm) arteries
Identify the visceral and parietal branches of the abdominal aorta
Visceral Branches: Include the Celiac trunk (GI tract/spleen), Superior mesenteric (small intestine/colon), Inferior mesenteric (rectum/colon), Suprarenal (adrenals), Renal (kidneys), and Gonadal (testes/ovaries).
Parietal Branches: Include the Inferior phrenic (diaphragm), Lumbar (back muscles/vertebrae), and Median sacral (sacrum/coccyx)
Identify the two major branches of the common iliac arteries
Internal Iliac Arteries: Primary supply for the pelvic muscle wall, pelvic organs, and external genitals.
External Iliac Arteries: Larger branches that follow the pelvic brim and become the femoral arteries in the thigh
Identify the three systemic veins that return deoxygenated blood to the heart.
Coronary Sinus: Receives blood from cardiac veins draining the heart myocardium.
Superior Vena Cava (SVC): Returns blood from the head, neck, upper limbs, and thorax.
Inferior Vena Cava (IVC): Returns blood from the abdomen, pelvis, and lower limbs
Identify the three major veins that drain blood from the head
Internal Jugular Veins: Drains the brain, meninges, and bones of the cranium.
External Jugular Veins: Drains the scalp, skin, and muscles of the head and neck.
Vertebral Veins: Drains the deep neck and cervical vertebrae
Identify the principal veins that drain the upper limbs
Superficial Veins: Cephalic (lateral arm), Basilic (medial arm), and Median antebrachial (forearm).
Deep Veins: Radial and Ulnar (forearm), Brachial (arm), and Axillary (armpit)
Identify the principal veins that drain the abdomen and pelvis
Principal veins include the Inferior Vena Cava, which is joined by the Common iliac, Lumbar (abdominal wall), Gonadal (testes/ovaries), Renal (kidneys), Suprarenal (adrenals), Inferior phrenic (diaphragm), and Hepatic (liver) veins
Describe the importance of the hepatic portal system
It directs venous blood from the GI organs and spleen into the liver before it returns to the heart, allowing the liver to process nutrients and detoxify harmful substances
Explain why pulmonary circulation is important
It transports deoxygenated blood to the lungs to unload CO2 and pick up O2, returning the oxygenated blood to the heart for systemic distribution
Describe the disorders that affect blood vessels
Hypertension: Damaging high blood pressure.
Atherosclerosis: Reduced compliance and stiffening of arterial walls.
Varicose Veins: Dilated veins caused by leaky valves.
Edema: Abnormal increase in interstitial fluid volume
Thrombophlebitis: Inflammation of a vein associated with clot formation