Lecture 6 Key Points - Hypertension & Hypotension
1/70
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
71 Terms
Hypertension ranges
Elevated blood pressure, often above 130/80 mmHg.
Hypotension ranges
Abnormally low blood pressure, typically below 90/60 mmHg.
Cardiovascular System
System comprising heart, blood, and vessels.
Systolic Pressure
Pressure during peak ventricular contraction.
Diastolic Pressure
Pressure during heart's resting phase.
Systemic Vascular Resistance (SVR)
Total resistance in arterial system.
Pulse Pressure
Difference between systolic and diastolic pressures.
Cardiac Output
Volume of blood pumped by the heart per minute.
Stroke Volume
Blood volume ejected per heartbeat, ~70 mL.
Heart Rate
Number of heartbeats per minute, average ~80 bpm.
Renin-Angiotensin-Aldosterone System
Hormonal system regulating blood pressure and fluid balance.
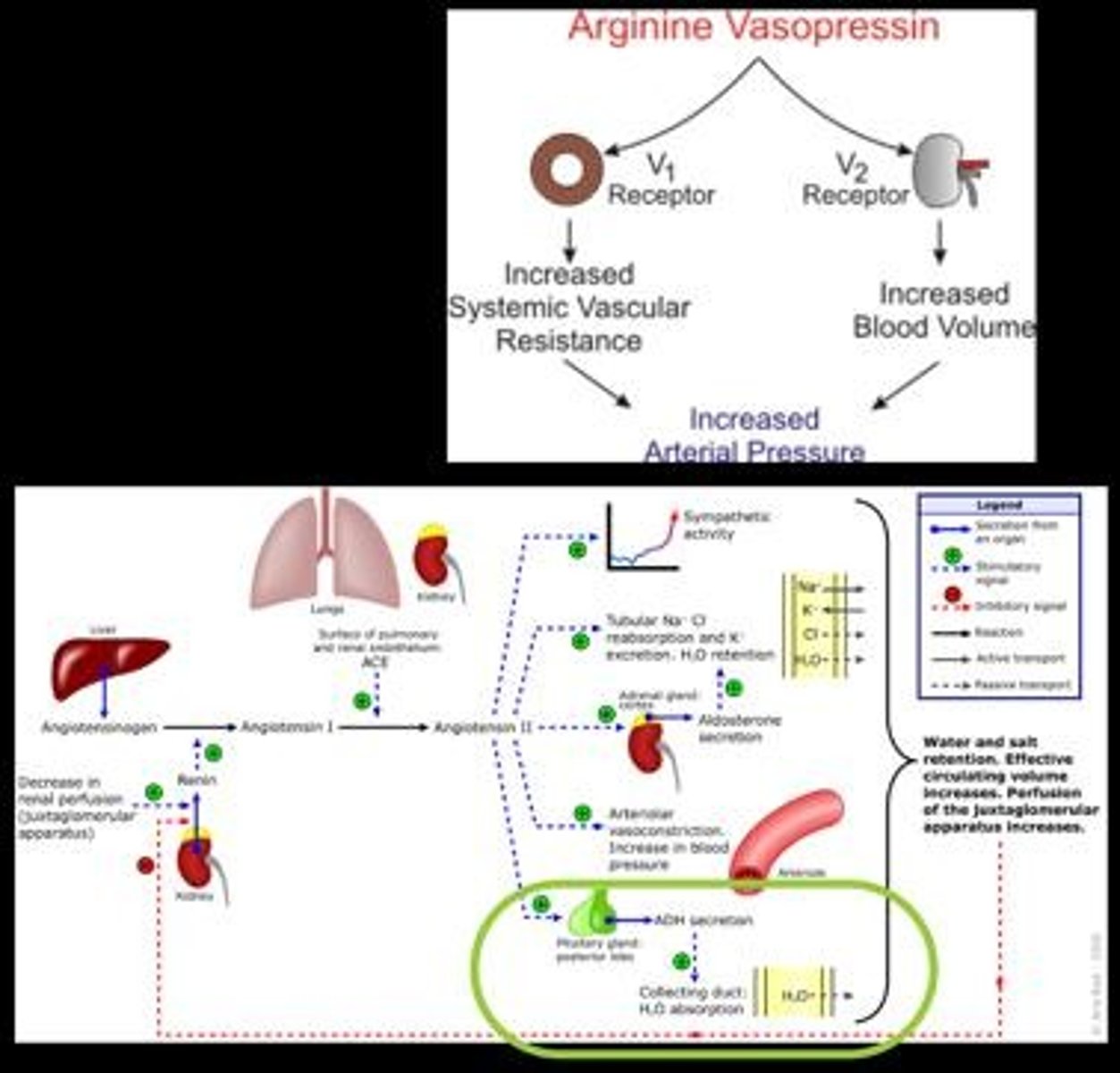
Angiotensin II
Potent vasoconstrictor increasing blood pressure.
Aldosterone
Hormone increasing sodium retention, affecting blood volume.
Vasopressin (ADH)
Hormone promoting water retention, increasing blood volume.
Primary Hypertension
90-95% of cases, cause unknown.
Secondary Hypertension
5-10% of cases, identifiable underlying causes.
Diuretics
First-line hypertension treatment, targets kidneys.
Vascular Resistance
Force opposing blood flow in vessels.
Autonomic Nervous System
Controls involuntary bodily functions, including blood pressure.
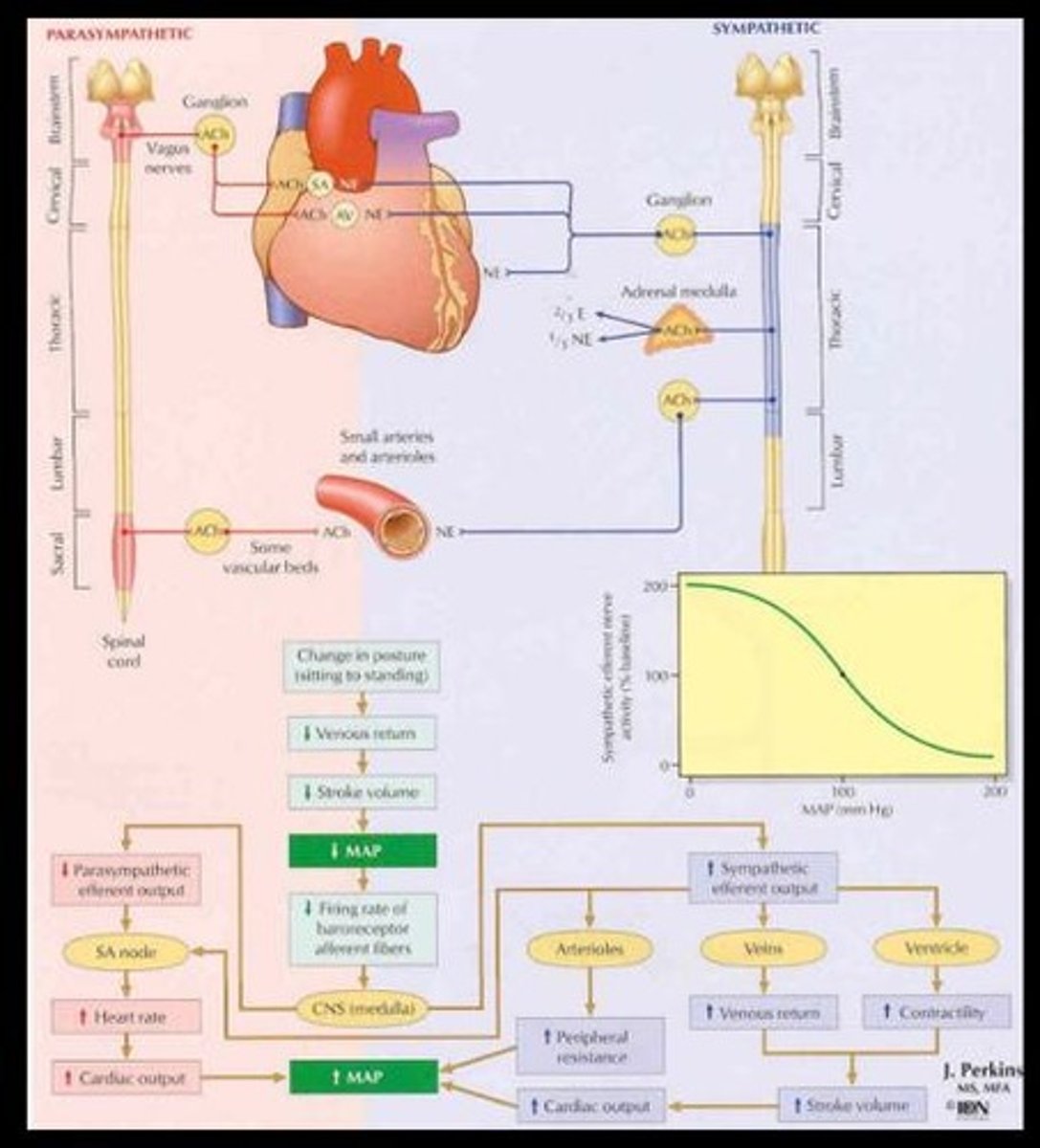
Short-term Regulation of blood pressure
Immediate adjustments via autonomic nervous system.
Intermediate Regulation of blood pressure
Involves hormonal responses to blood pressure changes.
Long-term Regulation of blood pressure
Endocrine adjustments affecting blood volume and pressure.
Thiazides
Most common diuretic class, mild effects.
Hydrochlorothiazide
Common thiazide diuretic, few side effects.
Loop Diuretics
Strong diuretics, potassium-wasting effects.
Furosemide
Loop diuretic, impairs Na+/K+/Cl- cotransporters.
Potassium-Sparing Diuretics
Inhibit Na+/K+ pump, retain potassium.
Spironolactone
Aldosterone antagonist, used in hypertension.
Triamterene
K+ sparing diuretic, often combined with thiazide.
Beta Blockers
Reduce heart rate, blood pressure, cardiac output.
Propranolol
Nonselective beta blocker, used for migraines.
Selective Beta Blockers
Atenolol and Metoprolol, once daily dosing.
ACE Inhibitors
Inhibit RAA system, prevent AT1 to AT2 conversion.
Lisinopril
Common ACE inhibitor, ideal for long-term therapy.
Angiotensin Receptor Antagonists
Inhibit AT2 effects, fewer side effects than ACE.
Losartan
Inhibits AT2 effects, less potent than ACE inhibitors.
Calcium Channel Blockers
Act on vascular smooth muscle, treat hypertension.
Dihydropyridines
Vascular selective CCBs, end in -ipine.
Gingival Hyperplasia
Common in CCB users, resolves after stopping.
Malignant Hypertension
BP > 180/120, medical emergency.
Hypertensive Urgency
> 180/120, asymptomatic, refer to PCP.
Hypertensive Emergency
> 180/120, symptomatic, signs of organ damage.
NSAID Interaction with beta blockers
Prolonged use reduces beta blocker effectiveness.
Rebound Tachycardia
Abrupt cessation of beta blockers causes increased heart rate.
White Coat Hypertension
Elevated BP only in healthcare settings.
Normal BP
Blood pressure outside healthcare settings is normal.
Prevalence of white coat hypertension
Occurs in 15% to 30% of patients.
Dental Appointment Protocol
Measure BP and pulse at every appointment.
Stressful Appointments
Avoid long or stressful dental procedures.
Potential Causes of Hypertension
Includes pain, stress, and anxiety.
Postural hypotension
Drop in BP due to position change.
Vasoconstrictors
Drugs that narrow blood vessels.
Hypertension prevalence
Affects 28% of US population.
Primary diagnosis visits
35 million yearly office visits for hypertension.
Controlled hypertension
Only 35% of patients manage their condition.
Smoking effects
Damages vascular endothelium, increasing hypertension risk.
Atherosclerotic plaques
Cholesterol deposits damaging blood vessels.
Alcohol impact
Contributes to vascular endothelium damage.
Target organ effects of hypertension
Hypertension affects organs like heart and kidneys.
Left ventricular hypertrophy
Heart muscle thickening due to high BP.
Nephrosclerosis
Kidney damage from prolonged hypertension.
Encephalopathy
Brain dysfunction caused by severe hypertension.
Orthostatic hypotension
BP drop upon standing from sitting.
Neurogenic causes of orthostatic hypotension
Blood pressure regulation impairment due to neural issues.
Non-neurogenic causes of orthostatic hypotension
Inadequate BP response despite normal neural function.
Vasovagal syncope
Fainting due to excessive vagal stimulation.
Shock
Life-threatening condition with organ under-perfusion.
Supine hypotensive syndrome
Hypotension in pregnant women due to vena cava compression.
Hemorrhagic shock
Life-threatening condition from significant blood loss.
Acute congestive heart failure
Heart fails to meet metabolic demands.
Acute adrenal insufficiency
Inadequate stress response leading to hypotension.