michael bio chatper 11 yayayay
1/70
Earn XP
Description and Tags
wait he didnt just spell the word rapper and leave out a p did he.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
71 Terms
colonization
does not cause disease
infection
multiplication of a microbe in a host; produces inflammation.
disease
If the host loses to a microbe during infection. Damage is caused to host tissues and organs.
infectious disease
a pathologic state caused directly by microorganisms or their products.
microbiome
the population of microbes that reside in the body without causing disease.
sites previously known to harbor normal microbiota
Skin and adjacent mucous membranes
Upper respiratory tract
GI tract, including mouth
Outer urethra
External genitalia (RJ doesn’t have this)
Vagina (RJ has this)
External ear canal
External eye
additional sites now thought to harbor some normal microbiota
Lower respiratory tract
Bladder
Breast/breast milk
Amniotic fluids and fetus
sites where microbiota DNA has been detected
Brain
Bloodstream
factors that weaken host defenses
Old age and extreme youth (infancy, prematurity)
Genetic defects in immunity and acquired defects in immunity (AIDS)
Surgery and organ transplants
Underlying disease: cancer, liver malfunction, diabetes
Chemotherapy/immunosuppressive drugs
Physical and mental stress
Pregnancy
Other infections
5 ways newborns acquire microbiota
In Utero
Birth
Milk
Caregivers
Environment
pathogen
relationship with host is parasitic and results in infection and disease
pathogenicity
potential to cause disease (true pathogens, opportunistic pathogens)
virulence
determined by a microbe’s ability to establish itself in a host and cause damage.
virulence factor
any characteristic or structure that contributes to the ability to establish and cause damage
Steps a microbe must take to get to the point where it can cause disease
Finding a portal of entry
Attaching firmly and negotiating the microbiome
Surviving host defenses
Causing damage
Exiting host
polymicrobial
disease caused by the presence of multiple microbes
most infections are ______________
Example: influenza leads to pneumonia
portals of entry
fecal (yum), oral, inhalation (most common), STD, and parenteral
exogenous
Organisms coming from outside the body.
endogenous
Organisms coming from somewhere in the same human host.
infectious dose (ID)
The minimum number of microbes necessary to cause an infection to proceed. Microorganisms with a smaller ________________ have greater virulence,
adhesion
Bacteria, protozoa, and fungi:
Fimbriae (pili)
Surface proteins
Adhesive slimes/capsules
Viruses - specialized receptors
Parasitic worms - suckers, hooks, and barbs.
phagocytes
cells that engulf and destroy host pathogens by means of enzymes and antimicrobial chemicals
antiphagocytic factors
Leukocidins: kill phagocytes outright
Extracellular surface layer (slime or capsule)
Some bacteria survive inside the phagocyte
three ways microbes cause damage to host
Enzymes or toxins (both endotoxins and exotoxins)
Inducing the host’s defenses to respond excessively or inappropriately
Epigenetic changes made to host cells by microbes
exoenzymes
Enzymes secreted by microbes that break down and damage tissues. They dissolve the host’s defense barriers to promote the spread of disease.
Mucinase: digests the protective coating on mucous membranes
Hyaluronidase: digests the substance that cements animal cells together
Coagulase: causes clotting of blood or plasma
Kinase: dissolves fibrin clots
Toxin
a specific chemical product of microbes that is poisonous to other organisms
A _______ is named according to their target:
Neurotoxins act on the nervous system
Enterotoxins act on the intestine
Hemotoxins lyse red blood cells
Nephrotoxins damage the kidneys
exotoxin
small protein produced by bacteria with a specificity for a target
Hemolysins: class of bacterial exotoxin that causes the RBC to hemolyze (burst and release hemoglobin pigment)
endotoxin
Chemical called: Lipopolysaccharide (LPS), part of the outer membrane of gram-negative cell walls
Has a variety of systemic effects on tissues and organs
Causes fever, inflammation, hemorrhage, and diarrhea
sign, symptom, and syndrome
Sign - objective evidence of disease as noted by an observer
Symptom - subjective evidence of disease as sensed by the patient
Syndrome - a disease identified by a certain complex of signs and symptoms
S/S of inflammation
Symptoms - pain and soreness
Signs - Edema, granulomas/abscesses, lymphadenitis
signs of blood infection
Leukocytosis - increase in white blood cell levels
Leukopenia - decrease in white blood cell levels
Septicemia - a general state in which microorganisms are multiplying in the blood and are present in large numbers
Bacteremia or viremia - bacteria or viruses are present in the blood but not multiplying
asymptomatic
no noticeable symptoms are produced while the microbe is active in host tissues, and the host does not seek medical attention.
portals of exit
secretion, excretion, discharge, or sloughed tissue
Respiratory tract, salivary glands, skin cells, fecal matter (yum), urogenital tract, blood.
latency
a dormant state of microbes in certain chronic infectious diseases
sequelae
long-term or permanent damage to tissues or organs caused by infectious disease
Deafness, rheumatic heart disease, arthritis, paralysis
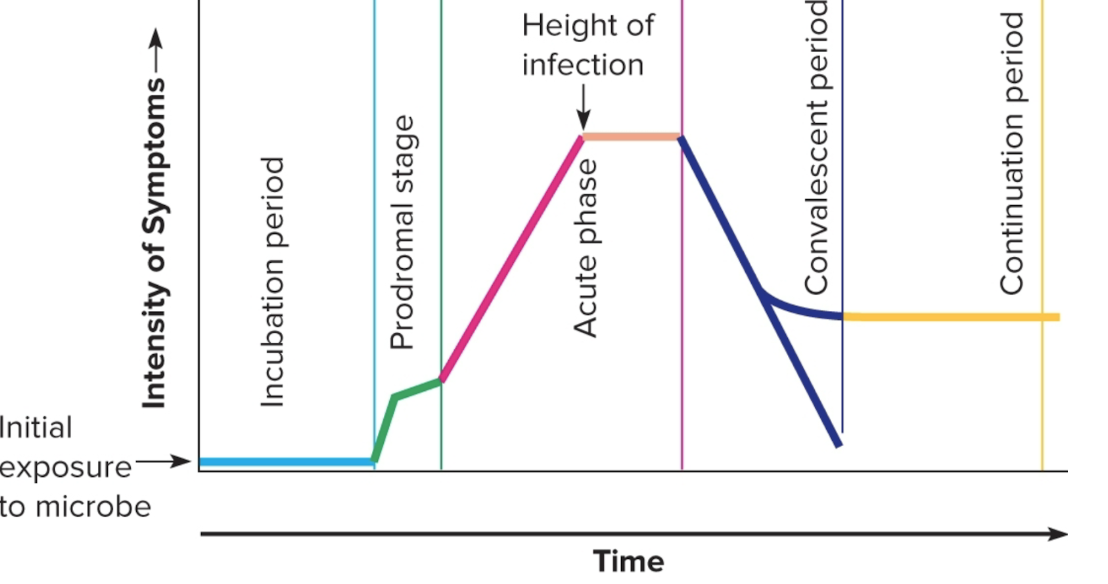
incubation period
First stage of disease
The time from initial contact with the infectious agent to the appearance of symptoms multiplying but not caused enough damage for symptoms
Ranges from several hours to several years
Majority: range from 2 to 30 days
prodromal stage
2nd stage of disease
1 to 2 day period when the earliest notable symptoms of infection appear
Feeling of discomfort: head and muscle aches, fatigue, upset stomach, general malaise
acute phase
3rd stage of disease
Infectious agent multiplies at high levels
Fever and other prominent and specific signs and symptoms
Extremely variable in length of this period
convalescent period
4th stage of disease
Begins to respond to the infection and symptoms decline
Strength and health gradually return
Need to continue antibiotic
continuation phase
5th stage of disease
Only some infections have this phase
Either the organism lingers for months, years, or indefinitely after the patient is well or the organism is gone but symptoms continue
poop phase
6th stage of disease
You poop out the microbe and then eat the poop to cycle back to stage 1.
This is the 5 stages of disease DIAGRAM
What fucking kind of diagram is this?
reservoir
Primary habitat of pathogen, often a human or animal carrier, but can also be soil, water, and plants
transmitter
individual or object from which an infection is acquired
4 types of reservoirs
Animals (nonhuman) - mammals, birds, reptiles
Human (actively ill)
Human (carrier but not ill)
Arthropods
5 types of carriers
Asymptomatic
Incubating
Convalescent
Chronic
Passive
asymptomatic carrier
Infected but show no symptoms of disease.
Gonorrhea, genital herpes with no lesions, HPV
incubating carrier
Spread the infectious agent during the incubation period.
Infectious mononucleosis
convalescent carrier
Recuperating patients without symptoms; they continue to shed viable microbes and convey the infection to others.
Hepatitis A
chronic carrier
Individuals who shelter the infectious agent for a long period after recovery because of the latency of the infectious agent
Tuberculosis, typhoid fever
passive carrier
Medical and dental personnel who must constantly handle patient materials that are heavily contaminated with patient secretions and blood risk picking up pathogens mechanically and accidentally transferring them to other patients
Various healthcare-associated infections
zoonosis
an infection indigenous to animals but naturally transmissible to humans. RJ is a fat, dirty, disgusting slob who poops all day and sniffs his own ballsack.
communicable
a disease in which an infected host can transmit the infectious agent to another host and establish infection in that host
contagious
a disease that is highly communicable, especially through direct contact.
Influenza and measles
noncommunicable
an infectious disease that does not arise through transmission of the infectious agent from host to host
Compromised person is invaded by their own microbiota
Individual has accidental contact with a microbe that exists in a nonliving reservoir
Infected persons do not become a source of disease to others
horizontal transmission
disease is spread through a population from one infected individual to another
Direct contact - close contact
Indirect transmission - an object or substance carries the agent
Vector transmission - arthropods that harbor an infectious agent and transfer it to a human
vertical transmission
disease transmitted from parent to offspring via ovum, sperm, placenta, milk
healthcare associated infection
Infectious diseases acquired or developed during a hospital or health care facility stay
Most common examples:
pneumonia
gastrointestinal illness
UTIs
bloodstream infections
surgical site infections
epidemiology
Study of frequency and distribution of disease and other health-related factors in defined populations
Microbiology, anatomy, physiology, immunology, medicine, psychology, sociology, ecology, and statistics
Florence Nightingale
Laid the foundations of modern epidemiology
Filth contributes to disease
Brought about new methods in military field hospitals
Separating linens and towels for each patient
Cleaning of floors
Unclogging of sewage pipes
Demonstrated that more men died of disease than traumatic injuries
reportable/notifiable diseases
Some diseases must be reported to authorities, and others are reported on a voluntary basis to organizations like the department of public health.
Examples - AIDS, COVID, measles, salmonella, tuberculosis
prevalence
A percentage; total number of cases in population ÷ total number of persons in population × 100
incidence
number of new cases in a designated time period ÷ total number of susceptible persons
Usually reported per 100,000 persons
difference between incidence and prevalence
Incidence = new cases and short time frame
Prevalence = all cases long time frame
mortality rate
Measures the total number of deaths in a population due to a certain disease.
morbidity rate
number of persons afflicted with infectious rates
index case
first case that brought the epidemic to the attention of officials
endemic
an infectious disease that exhibits a relatively steady frequency over a long time period in a particular geographic locale
sporadic
occasional cases are reported at irregular intervals at random locales
epidemic
when statistics indicate that the prevalence of an endemic or sporadic disease is increasing beyond what is expected for a population
pandemic
spread of an epidemic across continents