Metabolic Kinetics, Cardiac Conduction, and Balance: Human Physiology Overview
1/119
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
120 Terms
What method is used to estimate energy expenditure through oxygen consumption and carbon dioxide production?
Indirect Calorimetry
What does RER stand for in metabolic studies?
Respiratory Exchange Ratio
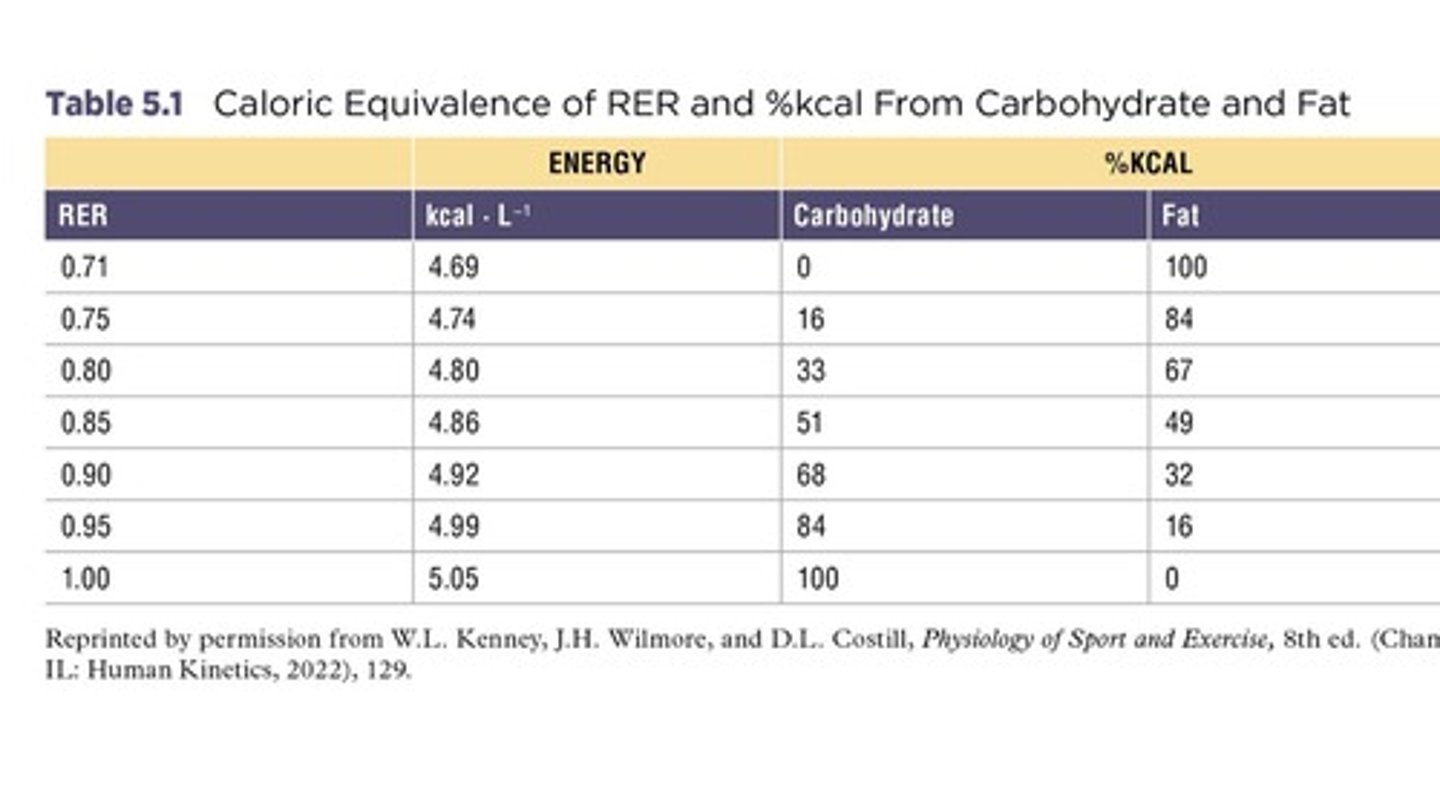
What is the respiratory quotient (RQ)?
The ratio of the amount of CO2 produced divided by the amount of O2 consumed at the cellular level.
What are the atmospheric gas levels of oxygen, CO2, and nitrogen?
20.93% oxygen, 0.03% CO2, and 79.04% nitrogen.
What happens to oxygen and CO2 levels in expired breath?
Expired breath decreases oxygen levels and increases CO2 levels.
What is the significance of RER in basal metabolic rate calculations?
RER is used to calculate the amount of CO2 produced versus O2 consumed.
What does an RER of 1.0 indicate physiologically?
It reflects 100% carbohydrate utilization and increased anaerobic glycolysis.
How can we estimate the percentage of fat versus carbohydrates burned from RER?
An RER of 0.7 implies 100% fat burning; percentages can be calculated using the formula: CHO burned = 100% - % fat burned.
What is the difference between Basal Metabolic Rate (BMR) and Resting Metabolic Rate (RMR)?
BMR is the minimum energy required to sustain vital functions in a fasted state, while RMR is the energy expended while resting quietly.
What factors influence Resting Metabolic Rate (RMR)?
Fat-free mass, organ size, sex, hormonal influences, and age.
What is the typical resting VO2 value for a young adult?
Approximately 0.20-0.30 L/min.
What is the expected RER range at rest?
0.80-0.85.
What is the oxygen deficit in exercise physiology?
A temporary mismatch where energy demand exceeds aerobic supply at the onset of exercise.
What metabolic pathways are involved in energy production?
ATP-PC system, glycolysis, and oxidative phosphorylation.
What is the role of phosphocreatine in energy production?
It helps regenerate ATP quickly during high-intensity exercise.
What physiological changes occur during the transition from rest to exercise?
ATP demand increases instantaneously while VO2 gradually increases, creating an oxygen deficit.
What is the largest consumer of energy at rest?
The liver, accounting for 29-32% of energy consumption.
How does body composition affect RMR?
Higher fat-free mass generally leads to a higher RMR due to increased metabolic activity.
What is the impact of age on RMR?
RMR typically decreases by 1-2% per decade after age 20.
What factors can cause a mismatch between predicted and measured RMR?
Recent food intake, caffeine, exercise, temperature, and individual physiological differences.
What is the significance of measuring expired gases in metabolic studies?
It helps calculate the amount of CO2 produced versus O2 consumed, indicating fuel type used.
What is the role of lactate in energy production?
Lactate accumulates when the body cannot clear it faster than it is produced, especially during anaerobic activity.
What does a higher RER indicate during exercise?
It indicates a greater reliance on carbohydrates as a fuel source.
What physiological factors contribute to energy expenditure at rest?
Organ mass, hormonal influences, and metabolic/mitochondrial factors.
How does sex influence RMR?
Men typically have more muscle mass than women, leading to higher RMR.
What is the caloric equivalent of oxygen consumption?
It shows the kilocalories produced per liter of oxygen consumed.
What is required for oxidative enzymes to activate?
Activation is required for oxidative enzymes.
What must accumulate to stimulate ATP synthase?
ADP and inorganic phosphate (Pi) must accumulate.
What effect does cast have on dehydrogenase activity?
Cast increases dehydrogenase activity.
What is the relationship between cardiac output and muscle blood flow?
Cardiac output and muscle blood flow require ramp time.
How is early ATP supplied during exercise?
Early ATP is supplied by the breakdown of phosphocreatine and fast glycolysis.
What is the O2 deficit in trained individuals?
Trained individuals reach steady state faster, resulting in a smaller O2 deficit.
What is EPOC?
Excess post-exercise oxygen consumption (EPOC) is a function of the intensity and duration of the previous exercise bout.
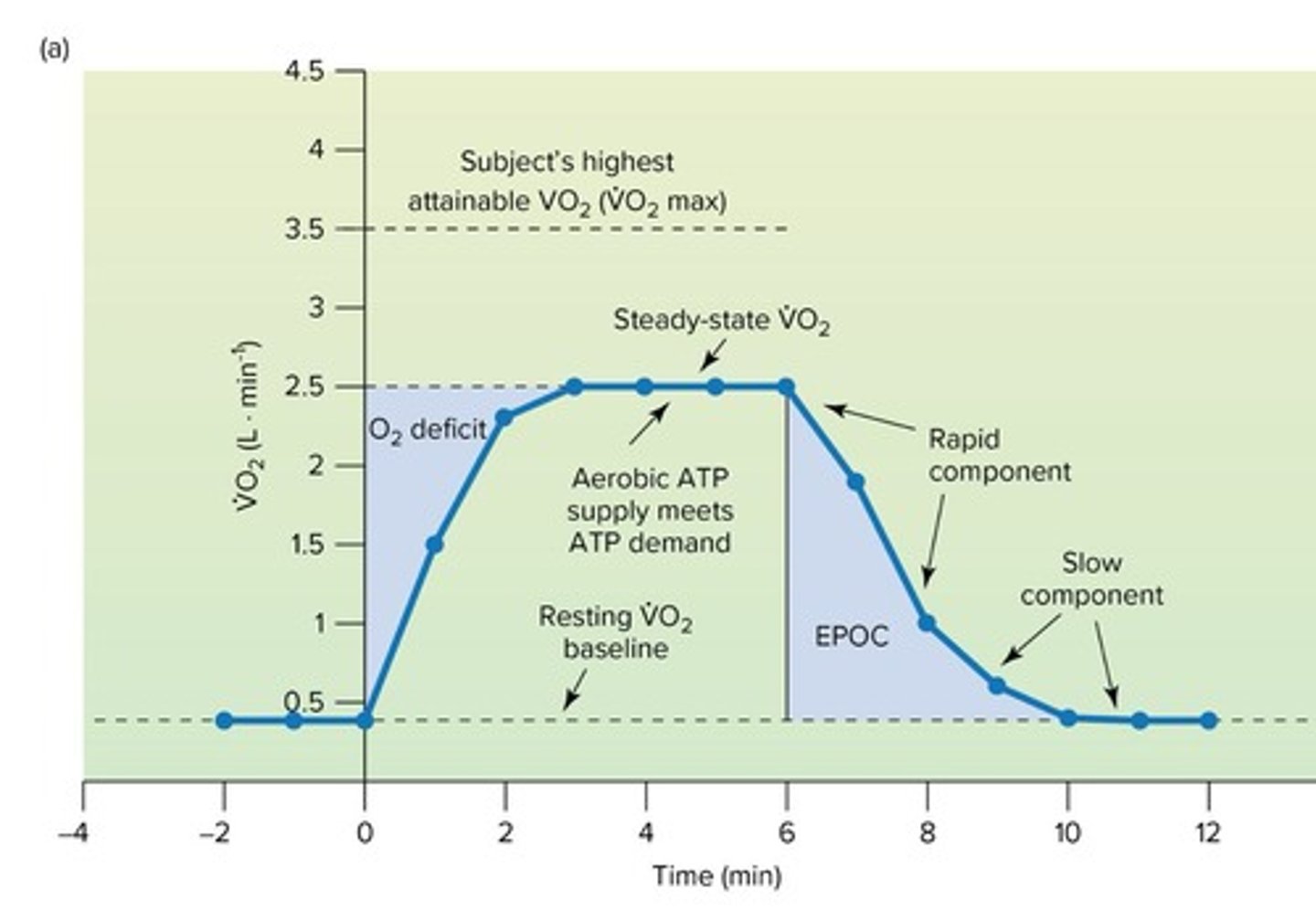
What does the area under the steady-state requirement but above actual VO2 represent?
It represents the O2 deficit.
What factors affect the magnitude of EPOC?
The magnitude reflects the intensity, duration, and fitness level of the exercise.
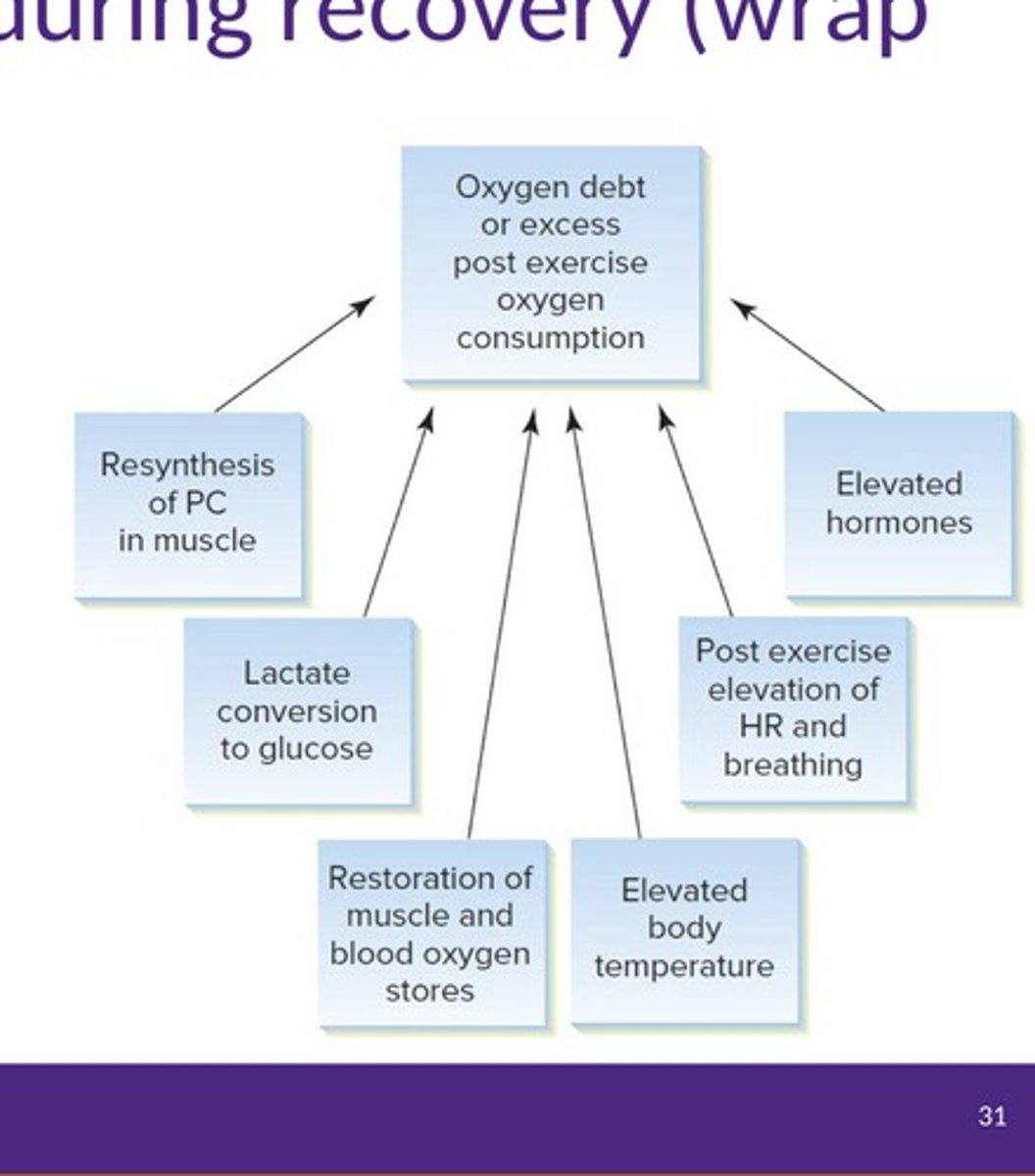
What are the components of recovery after exercise?
Fast and slow recovery components include lactate oxidation, elevated body temperature, and myoglobin O2 restoration.
What is the role of the SA node in the heart?
The SA node initiates the heart's rhythm at a pace of approximately 100 bpm.
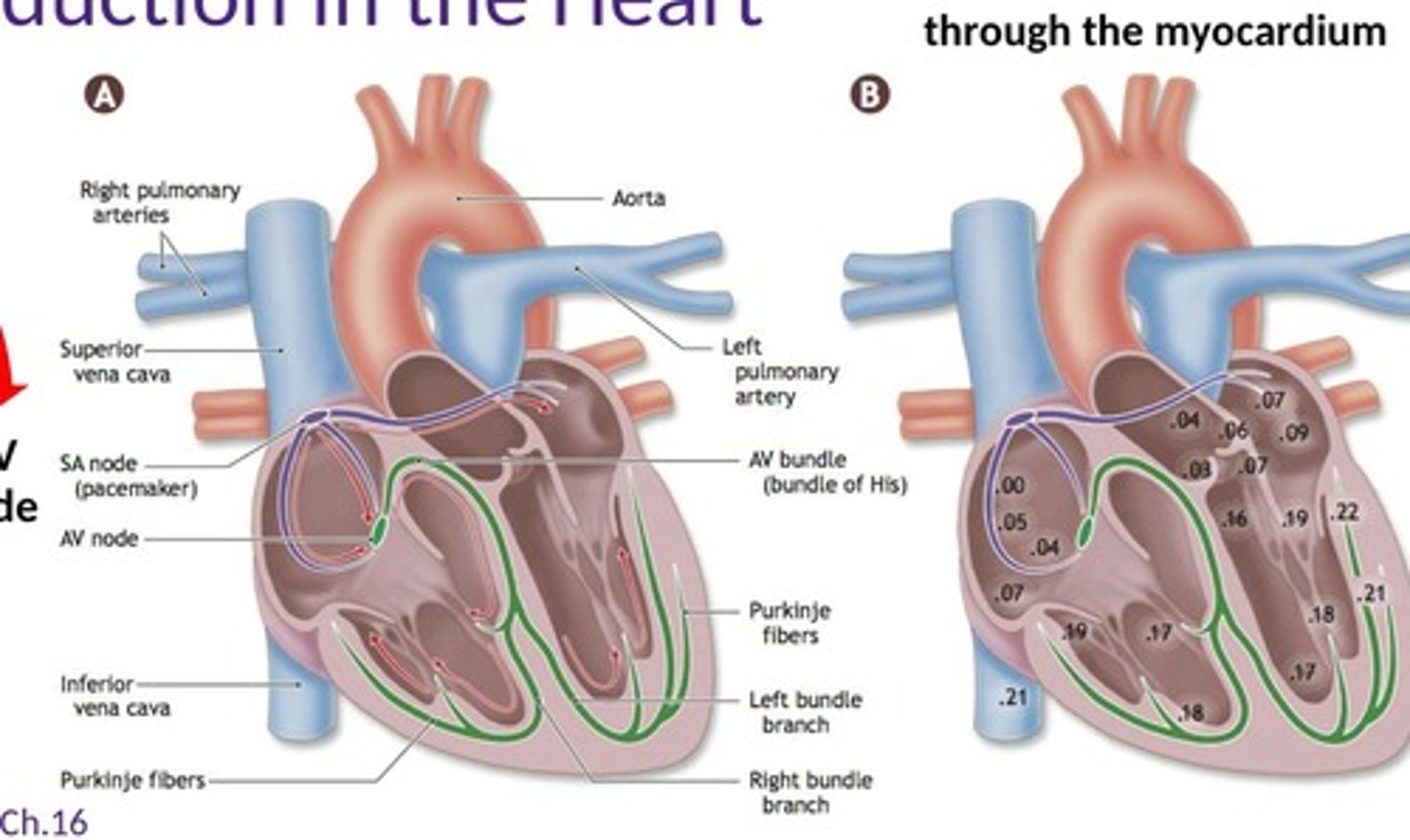
How does the parasympathetic nervous system affect heart rate?
The parasympathetic nervous system slows the heart rate when resting.
What is the function of pacemaker cells in the heart?
Pacemaker cells are responsible for the fastest spontaneous rate of depolarization.
What is the path of conduction in the heart?
Excitation spreads from the SA node to the atria, then to the AV node, and finally to the ventricles via the bundle of His and Purkinje fibers.
What happens during depolarization of cardiac muscle cells?
Depolarization reverses the electrical charge across the cell membrane, leading to contraction.
What is the significance of the ECG?
An electrocardiogram (ECG) assesses the heart's rate, rhythm, and can suggest structural or ischemic changes.
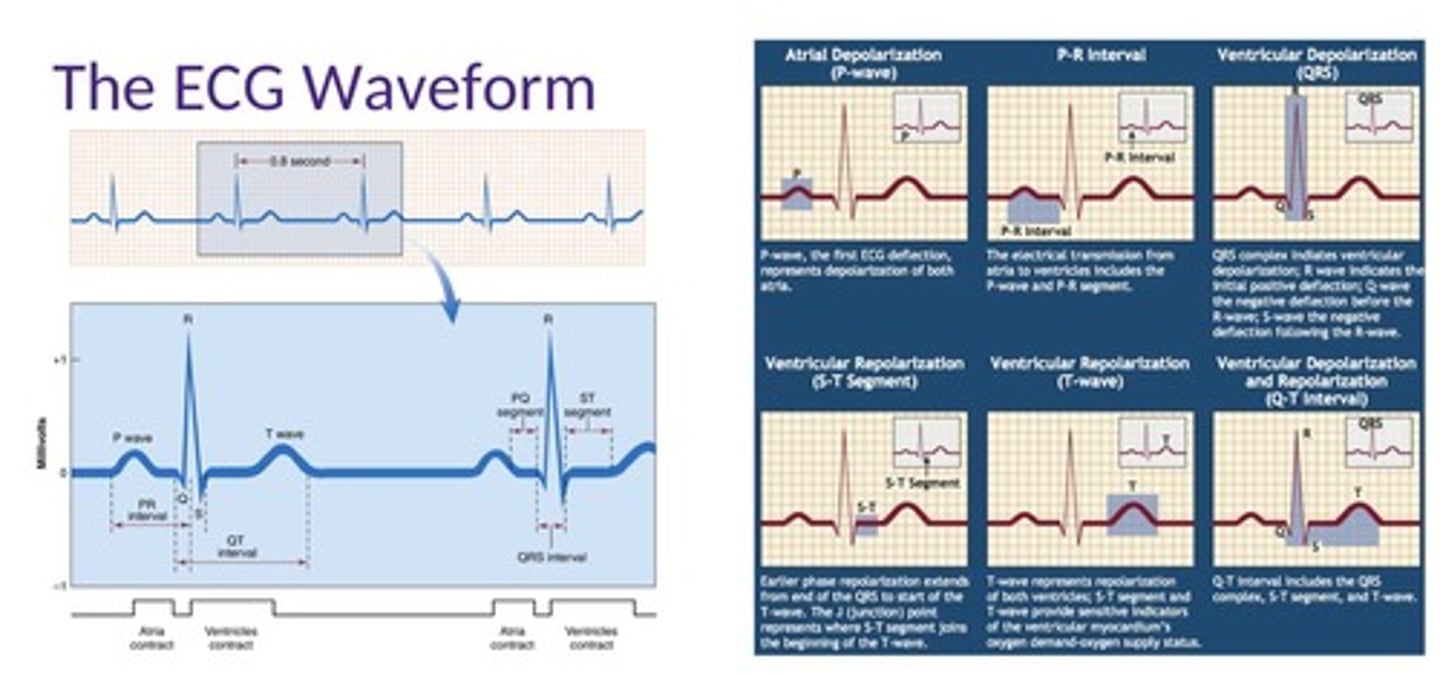
What is the normal cardiac axis direction?
The normal cardiac axis is directed downward and slightly to the left.
What indicates left axis deviation on an ECG?
Left axis deviation is indicated by a QRS axis less than -30 degrees.
What indicates right axis deviation on an ECG?
Right axis deviation is indicated by a QRS axis greater than +90 degrees.
What are the two groups of leads in a 12-lead ECG?
Group 1 is oriented in the frontal plane (I, II, III, aVR, aVL, aVF) and Group 2 is oriented in the horizontal plane (V1, V2, V3, V4, V5, V6).
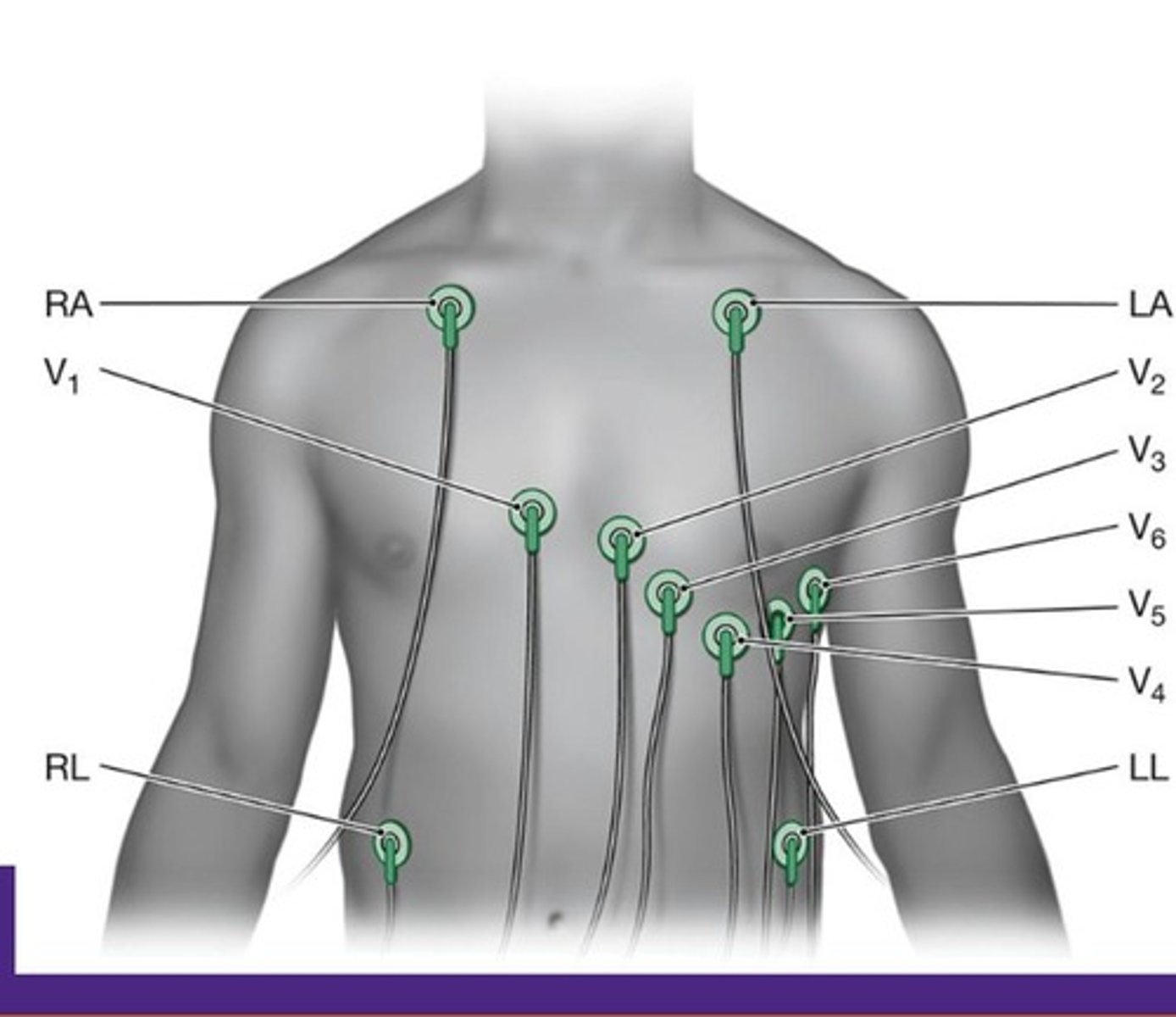
What is the role of augmented leads in ECG?
Augmented leads are combined leads that enhance the electrical signal detection.
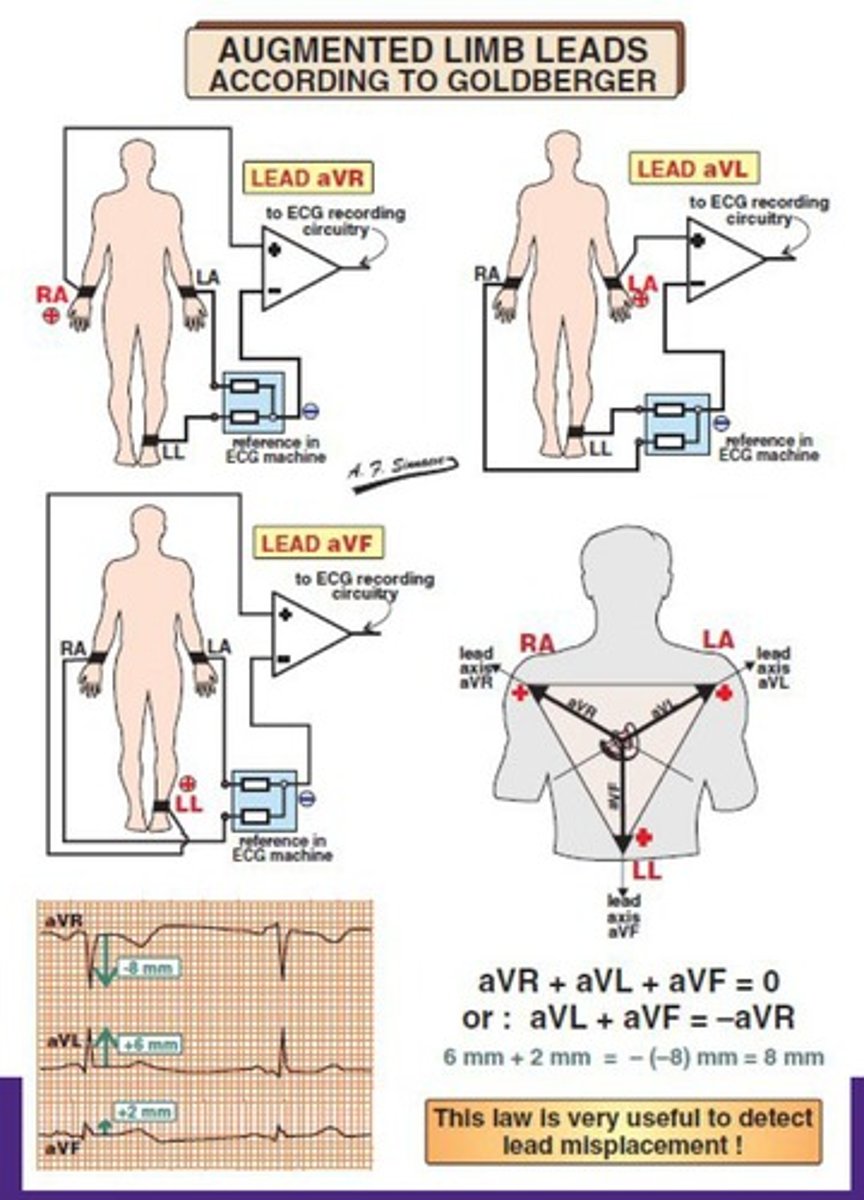
What does the term 'intrinsic regulation of heart rhythm' refer to?
It refers to the heart's ability to maintain its own rhythm, primarily driven by the SA node.
How does training affect vagal tone?
Training increases vagal tone, leading to faster heart rate recovery.
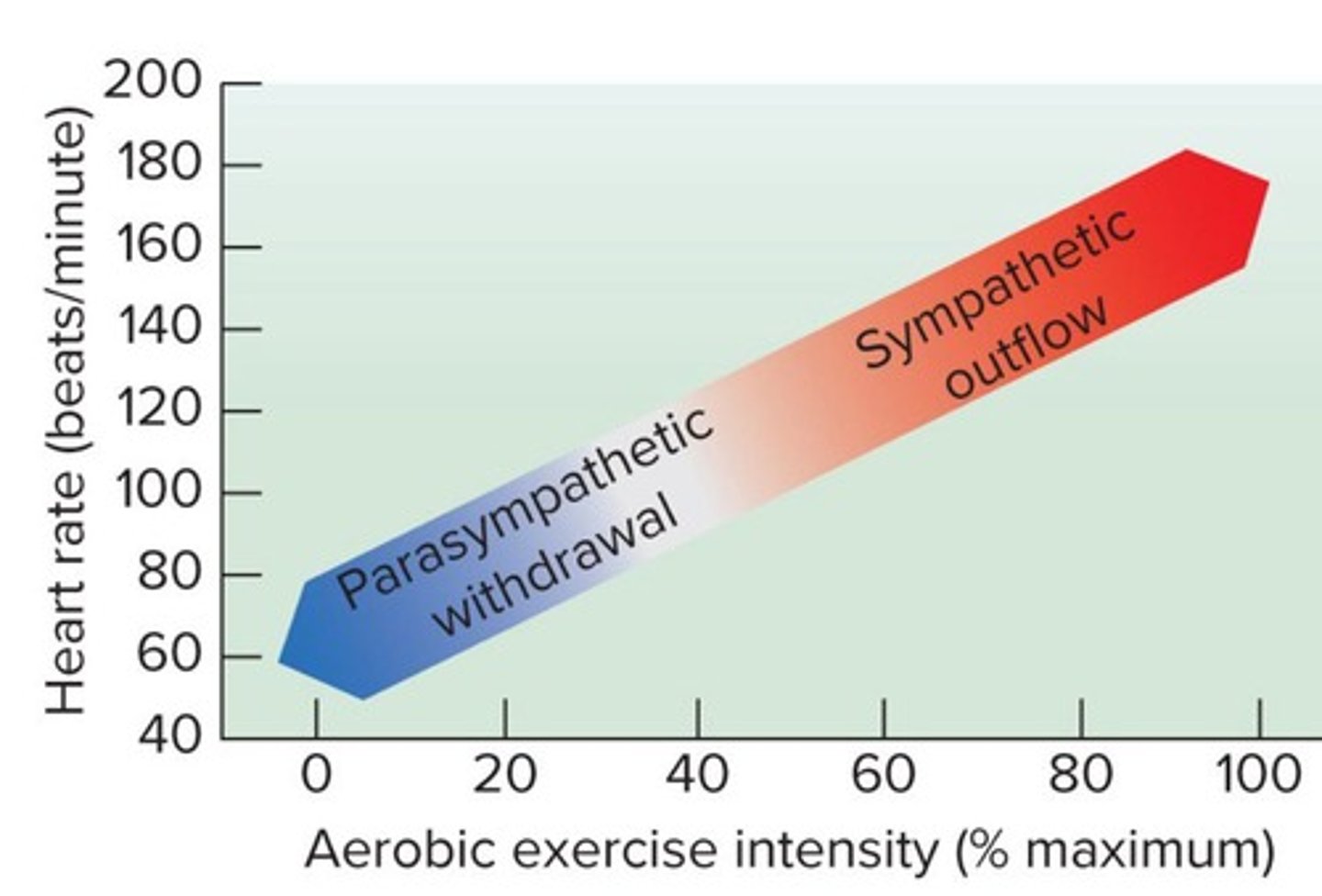
What is the relationship between heart rate and exercise intensity?
Heart rate increases with exercise intensity due to vagal withdrawal and sympathetic input.
What is the role of central command in heart rate modulation?
Central command anticipates the need for increased heart rate during exercise.
What does the electrical activity in the heart precede?
The mechanical events of contraction.
What are the axes of an ECG recording?
Time is on the X-axis and millivolts (mV) are on the Y-axis.
What can clinicians determine from an ECG?
Time delays and quantity of electrical activity.
What are ST segment abnormalities in ECG?
Elevation or depression of the ST segment indicating potential cardiac issues.
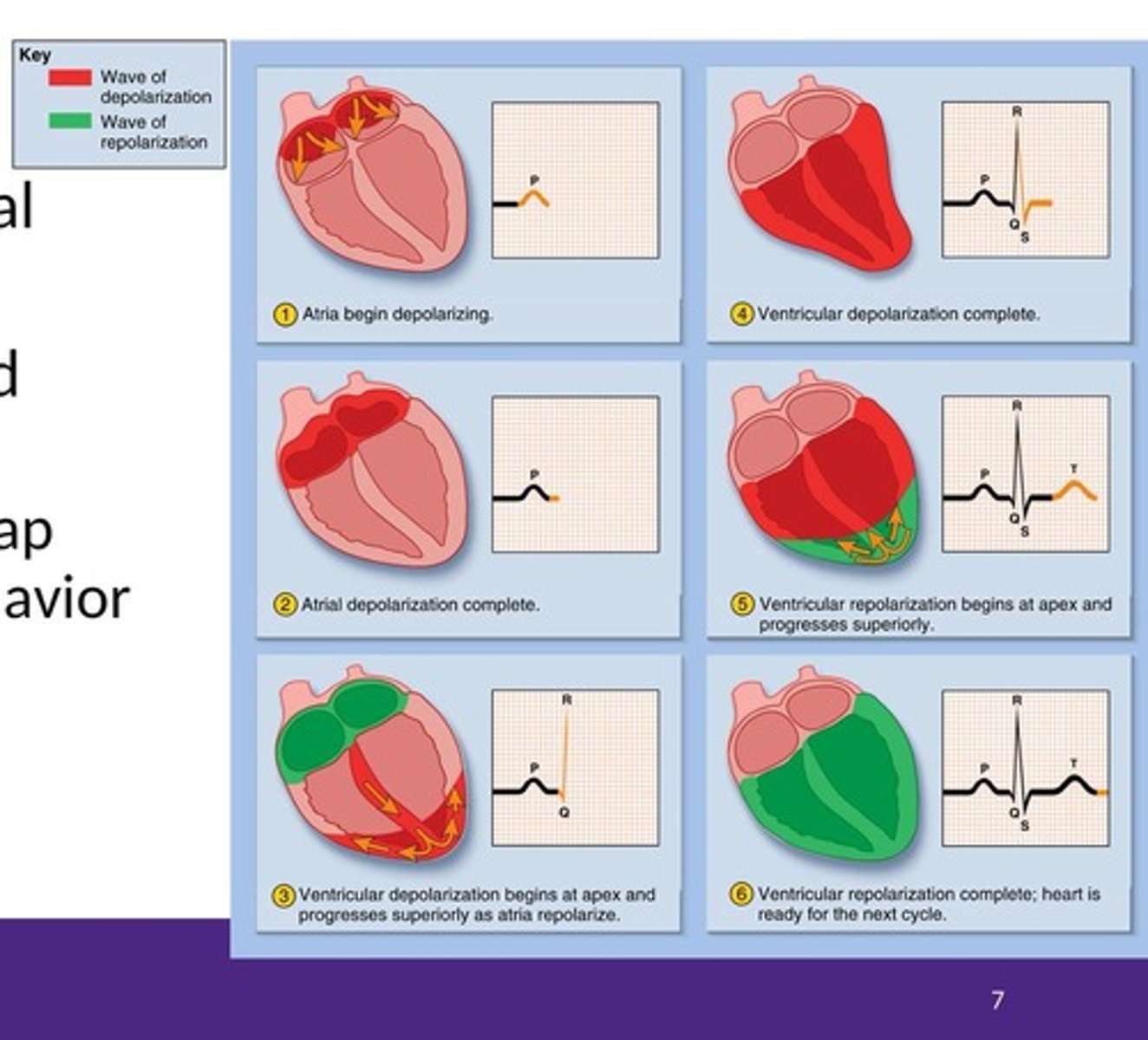
What is the primary function of the nervous system?
To regulate endless bodily functions.
What are the three primary functions of the nervous system?
Monitoring the environment, integrating information, and initiating a response.
What type of neurons relay information to the CNS?
Afferent neurons.
What do efferent neurons do?
Relay signals from the CNS to effector organs.
What is the somatic nervous system responsible for?
Sending signals from the CNS to skeletal muscles for voluntary control.
What does the autonomic nervous system regulate?
Involuntary functions such as cardiac and smooth muscle activity.
What types of sensory receptors are involved in muscle contraction regulation?
Mechanoreceptors and proprioceptors.
What is a reflex?
A rapid, involuntary movement in response to a stimulus.
What is the functional unit of the nervous system?
The neuron (nerve cell).
What are the three distinct regions of a neuron?
Dendrites, cell body, and axon.
What is the role of dendrites in a neuron?
They receive information and convey it to the cell body.
What happens when a signal is strong enough in a neuron?
It passes the signal along to the axon.
What is an action potential?
A reversal of polarity or charge in electric potential in a neuron.
What is the resting membrane potential?
The difference in electrical charge between the inside and outside of a cell.
What causes the resting membrane potential?
Unequal distribution of positive and negative ions across the cell membrane.
What is irritability in neurons?
The ability to respond to a stimulus.
What is conductivity in neurons?
The transmission of an electrical impulse from one location to another.
What is the role of neurotransmitters?
They allow neurons to communicate with each other.
What ions predominate extracellularly in a resting neuron?
Sodium (Na+) and chloride (Cl-) ions
What ions predominate intracellularly in a resting neuron?
Potassium (K+) ions and negatively charged protein anions
What is the function of the sodium-potassium pump in neurons?
It removes three sodium ions from the cell for each potassium ion it brings in, creating a net loss of positive ions and making the interior negatively charged.
What happens when sufficient stimulus is applied to a neuron?
Sodium channels open, allowing positive ions to flow into the neuron, leading to depolarization.
How is an action potential propagated along an axon?
It moves along the entire length of the axon, causing neurotransmitter release from the axon terminal.
What is a synapse?
The gap or junction between the terminal ends of an axon and other neurons, muscle cells, or glands.
What is the neuromuscular junction?
A specialized synapse between a motor neuron and a muscle fiber.
What neurotransmitter is released at the neuromuscular junction?
Acetylcholine (ACh)
What occurs when ACh binds to receptors on the sarcolemma?
It causes changes in ionic permeability, leading to depolarization of the sarcolemma and generation of an action potential.
What is a motor unit?
A motor neuron and the muscle fibers it innervates, serving as the basic unit of contraction.
What is the role of reflexes in movement?
Reflexes maintain posture and mediate responses to stimuli in a coordinated fashion.
What is a reflex arc?
The neural pathway involved in a reflex action, including a receptor, afferent neuron, integration center, efferent neuron, and effector organ.
What are the two types of reflexes?
Autonomic (involving cardiac or smooth muscle and glands) and somatic (resulting in skeletal muscle contraction).
What is the function of the spinal cord in reflex actions?
It connects the peripheral nervous system (PNS) with the brain and serves as the site of reflex integration.
What are ascending tracts in the spinal cord?
Tracts that carry sensory (afferent) information to the brain.
What are descending tracts in the spinal cord?
Tracts that carry motor (efferent) information from the brain to the body.
What is the pyramidal system?
A system composed of neurons whose cell bodies originate in the cerebral cortex and control precise and discrete movements.
What is the extrapyramidal system?
A system that consists of all descending tracts not included in the pyramidal system, controlling muscle tone, posture, and head movements.
What is the role of the integration center in a reflex arc?
It processes the incoming neural signal and connects the afferent neuron with efferent neurons.
What happens when a neuronal action potential reaches the axon terminal?
The neuron membrane increases its permeability, allowing calcium ions to enter.
What is the significance of the neuromuscular junction compared to other synapses?
At the neuromuscular junction, a single presynaptic action potential leads to a postsynaptic action potential, and the synapse can only be excitatory.
What is the role of efferent neurons?
They carry information from the central nervous system (CNS) to muscles or glands.
What is the function of motor neurons?
Efferent neurons that innervate skeletal muscle, classified as alpha or gamma.
What is the role of the dorsal root ganglion?
It contains the cell bodies of afferent neurons in the spinal nerve, part of the PNS.
What is the function of the ventral root of a spinal nerve?
It contains the cell bodies of efferent neurons that exit the spinal cord.
What is the basic unit of contraction in skeletal muscle?
The motor unit.
What is the role of calcium ions in neurotransmitter release?
Increased calcium levels cause synaptic vesicles to migrate to the cell membrane and release neurotransmitters by exocytosis.