Thrombosis, Embolism, Infarction
1/54
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
55 Terms
Thrombosis
An inappropriate activation of normal haemostatic processes, such as formation of a thrombus in uninjured vasculature or thrombotic occlusion of a vessel after relatively minor injury.
Thrombus
Solid mass formed within the vascular system (blood vessel or cardiac chamber) in life from the constituents of flowing blood.
Thrombi have laminations called what
Lines of Zahn
How do lines of Zahn form
Lines of Zahn are produced by alternating pale layers of platelets admixed with fibrin and darker layers containing more red cells.
3 primary influences predisposing to thrombus formation according to Virchow’s triad
1. Endothelial injury
2. Alteration of blood flow (stasis, turbulence)
3. Blood hypercoagulability.
What can cause endothelial injury
hypertension
scarred heart valves
atheroma
cigarette smoke
(shear stress)
Give 2 examples of alteration in blood flow & what problems they cause
Stasis → development of venous thrombi
Turbulence → endothelial injury, forms countercurrents & local pockets of stasis
2 causes of stasis
Inactivity
Mitral valve stenosis → left atrial dilatation
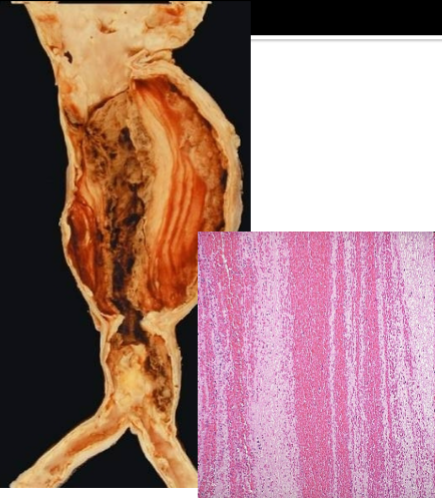
Cause of turbulence
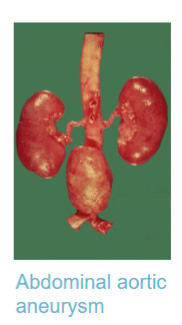
Aneurysms

Superficial venous thrombi rarely embolise but may lead to what
varicose ulcers
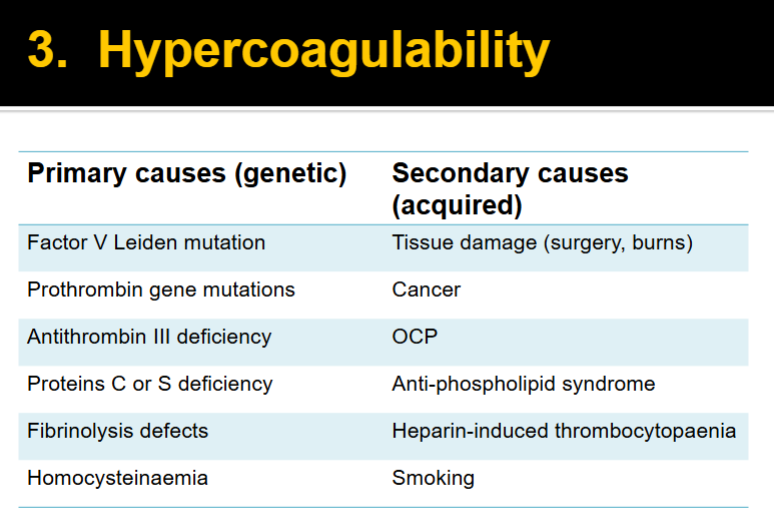
Risk factors for Venous thrombi
immobilisation (e.g. longhaul travel)
post-surgery
OCP
smoking
advanced age
obesity
cancer
pregnancy
inherited
thrombophilia
Most common sites of Arterial thrombi
coronary, cerebral, & femoral arteries
Arterial thrombi are usually superimposed on what
Usually superimposed on an atherosclerotic plaque, but also superimposed on other vascular injury (e.g. vasculitis, trauma).
True/False Arterial thrombi rarely embolise
True
Cardiac thrombi (mural thrombi) most commonly occur after what
atrial fibrillation
after an MI
Is there a risk of embolism with cardiac thrombi
Yes - They may embolise to brain, peripheral arteries, spleen
What are Vegetations
Thrombi which form on cardiac valves. These thrombi may contain bacteria (=bacterial endocarditis) or be sterile (e.g. in acute rheumatic fever).
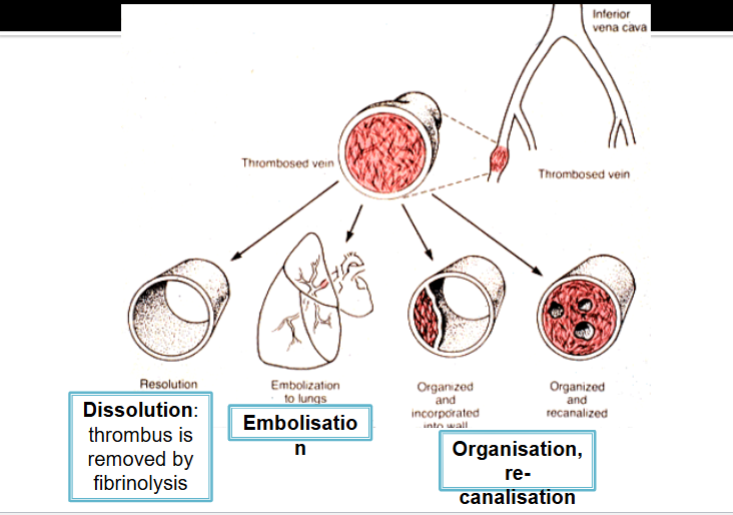
3 possible fates of a thrombus
Name 7 types of emboli
1. Thromboembolus: Virtually 99% of all emboli represent some part of a detached thrombus.
Pulmonary thromboembolus
Systemic thromboembolus
2. Fat/bone marrow embolus
3. Air/nitrogen embolus
4. Cholesterol embolus
5. Amniotic fluid embolus
6. Tumour embolus
7. Foreign matter, e.g. talc in IV drug abusers
>95% of pulmonary thromboembolism cases originate where
Above-knee DVTs
What % of pulmonary thromboembolisms are silent
60-80% are clinically silent because they are small
What is a Saddle embolus & what does it lead to
Large pulmonary embolism (PE) which impacts across the bifurcation of the pulmonary arteries → sudden death due to acute right heart failure
Multiple small emboli: can embolise off a single large mass. What can this lead to?
pulmonary haemorrhage or pulmonary infarction
Multiple emboli over time lead to
pulmonary hypertension and chronic right heart failure
Treatment of DVT/PE (3)
LMW heparin & oral anticoagulant
Thrombolytic therapy in PE with haemodynamic instability
IVC filter (right) indicated if contraindication to/failure of anticoagulation
Where would you find Systemic thromboembolus
Within the arterial circulation
Systemic thromboembolus can lead to what
Infarction
80% of systemic thromboembolus arise from what kind of thrombus
80% arise from intracardiac mural thrombi
Other than intracardiac mural thrombi, what do systemic thromboemboli arise from
Aortic aneurysm
Atherosclerotic plaque fragments (Cholesterol emboli)
Valvular vegetations (endocarditis)
Rarely – paradoxical embolus
Up to 10% - unknown
The majority of intracardiac mural thrombi occur as a result of what 3 things
LV infarction
Atrial dilation
Atrial fibrillation
What is a paradoxical embolism & how does it happen
Normally, venous clots travel to the lungs → pulmonary embolism.
A paradoxical embolism occurs when a venous clot enters the arterial circulation, potentially causing stroke, MI, or limb ischemia.
This can only happen if there is a patent foramen ovale
How does a Fat/bone marrow embolus occur
Fat globules enter the bloodstream through tissue (usually bone marrow or adipose tissue) that has been disrupted by trauma
Occurs after fractures of long bones, e.g. femur.
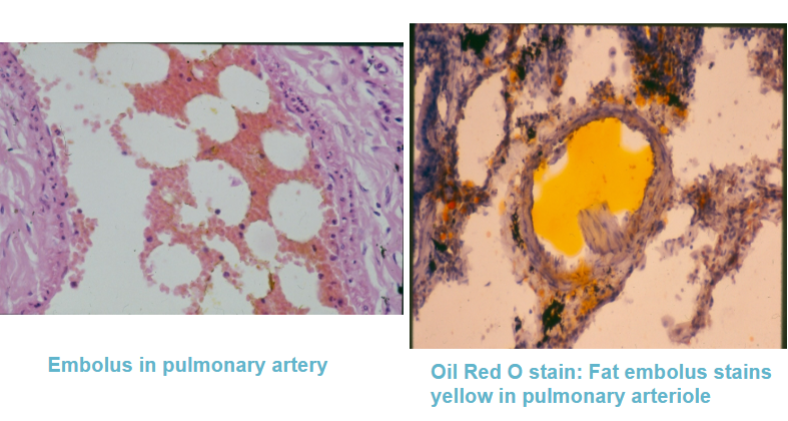
How long after fracture of long bone & with what signs do fat/bone marrow embolus patients present
Presents 1-3 days after injury.
Classic triad – hypoxemia, neurologic abnormalities, petechial rash
Treatment of Fat/bone marrow embolus
Management is supportive (stabilise patient)
Mortality rate of a fat/bone marrow embolus
5-15%
Two conditions necessary for an air embolus to occur
1. direct communication between a source of air and the vasculature
2. pressure gradient favouring the passage of air into the circulation rather than bleeding
Give 3 examples of what could cause an air embolus
surgical procedures
intravenous catheterisation
trauma
barotrauma (divers come up too quick → alveolar rupture & tearing of pulmonary veins)
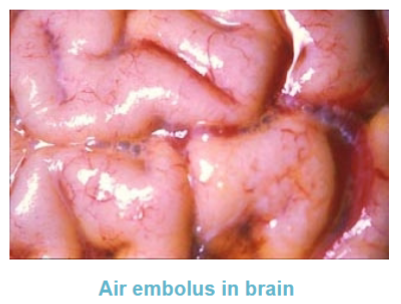
How many ml of air do you need to have a clinical presentation of an air embolus
>100 ml
What can cause an air embolism
Decompression sickness (“the bends”) in divers, also patients requiring positive pressure ventilation.
Rapid ascent can result in expansion of gas in the lungs, alveolar rupture and tearing of pulmonary veins. Alternatively, air bubbles may form in the venous system during ascent
Amniotic fluid embolisms have a high/low prevalence & a high/low mortality rate
Very rare, but has mortality of 20-90%
In an amniotic fluid embolism, how does the amniotic fluid enter the maternal circulation
Amniotic fluid enters the maternal circulation through the endocervical veins, the placental insertion site, or a site of uterine trauma
Signs of amniotic fluid embolism
Precipitates cardiogenic shock
Respiratory failure
Inflammatory response
Ischaemia
Restriction in blood supply (from either reduced arterial flow or reduced venous drainage) which causes oxygen deprivation and results in tissue damage.
Can cell injury due to ischaemia be reversible
Only if blood flow is restored
Reperfusion injury
Cells proceed to die after blood flow resumes after ischemic injury
How do reperfusion injuries happen
1. Re-oxygenation increases generation of oxygen free radicals causing new damage
2. Production of cytokines recruits circulating neutrophils to reperfused tissue resulting in inflammation.
Infarction
An area of ischaemic necrosis caused by occlusion of either the arterial supply or the venous drainage in a particular tissue.
Almost always due to arterial occlusion
If infarction is generally caused by arterial occlusion, what does venous thrombosis usually cause
Venous thrombosis more often induces venous obstruction and congestion rather than infarction
What is the exception to this: Venous thrombosis more often induces venous obstruction and congestion rather than infarction
organs with a single venous outflow channel, e.g. testis or ovary
Name & differentiate between the 2 types of infarcts
Red infarcts
Seen with venous occlusions (testis/ovary)
Seen in loose tissues (lug) which allow blood to collect in infarcted zone
Seen in tissues with dual circulations (lung/liver) allowing flow of blood from the unobstructed vessel into the necrotic zone
White infarcts
Seen in arterial occlusions or solid organs (heart/spleen/kidney)
Solidity of the tissue limits the amount of haemorrhage that can seep into the area
All infarcts tend to be what shape
All infarcts tend to be wedge-shaped, with the occluded vessel at the apex and the periphery of the organ forming the base
The dominant histologic characteristic of infarction is …
ischaemic coagulative necrosis


What are septic infarcts & how do they occur
The infarct gets converted into an abscess
These occur when embolisation occurs by fragmentation of a bacterial vegetation from a heart valve or when microbes seed an area of necrotic tissue.